00:00
Start Quiz
Question 76
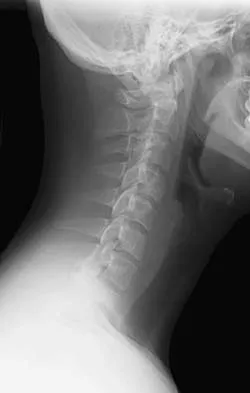
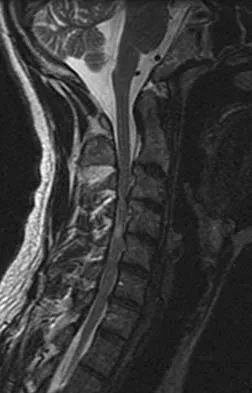
Figures 25a and 25b show the radiograph and MRI scan of a 48-year-old man who reports increasing unsteadiness in his gait and hand clumsiness. Examination reveals a positive Hoffmann's reflex bilaterally, positive clonus, and a spastic gait. Management should consist of
Explanation
The patient has a congenitally small spinal canal with secondary multilevel degenerative changes causing stenosis and cord compression across multiple segments, including directly posterior to the vertebral bodies. A multilevel diskectomy may address the cord compression at the disk level, but not posterior to the bodies, and most likely would be inadequate. The patient has significant stenosis distal to C5, necessitating a more extensive surgical approach than simply C3-C5. Because the patient's cervical lordosis is preserved, a posterior procedure such as laminoplasty or laminectomy would allow the cord to fall away from the anterior pathology and afford decompression. Cervical myelopathy does not tend to resolve, and there is a significant risk for progression; therefore, surgical management usually is recommended. Edwards CC II, Riew KD, Anderson PA, et al: Cervical myelopathy: Current diagnostic and treatment strategies. Spine J 2003;3:68-81.
Question 77
Lumbar disk replacement has been shown to offer which of the following results?
Explanation
There is no clear evidence that disk replacement results in pain relief that is superior to fusion. Pain relief appears to be equivalent with these two procedures. No study has clearly demonstrated that normal segmental motion has been consistently restored. Preexisting facet arthropathy is considered to be a contraindication to disk replacement. Comparative long-term data demonstrating a reduced incidence of adjacent segment disease compared to fusion are not yet available. Geisler FH, Blumenthal SL, Guyer RD, et al: Neurological complications of lumbar artificial disc replacement and comparison of clinical results with those related to lumbar arthrodesis in the literature. J Neurosurg Spine 2004;1:143-154.
Question 78
When performing the exposure for an anterior approach to the cervical spine, the surgical dissection should not enter the plane between the trachea and the esophagus and excessive retraction should be avoided to prevent injury to the
Explanation
The recurrent laryngeal nerve lies between the trachea and the esophagus. The vagus nerve lies in the carotid sheath. The sympathetic trunk lies anterior to the longus colli muscles. The hypoglossal and superior laryngeal nerves are both at risk during the exposure but are not located between the trachea and the esophagus. Flynn TB: Neurologic complications of anterior cervical interbody fusion. Spine 1982;7:536-539.
Question 79
A 39-year-old man reports low back pain, lower extremity numbness, and urinary retention after being injured in a motor vehicle accident 1 day ago. He is able to walk but is in pain. A straight leg raise results in increased back pain, and examination reveals that perianal sensation is decreased. Placement of a urinary catheter results in 500 mL of urine. What is the next most appropriate step in management?
Explanation
Acute cauda equina syndrome, including saddle hypesthesia and bowel/bladder incontinence, is a red flag that demands emergent evaluation with MRI and urgent surgery if compression is confirmed. Results appear to be improved if surgery is performed within 48 hours. The other treatment approaches listed are not indicated if a cauda equina syndrome is present. Ahn UM, Ahn NU, Buchowski JM, et al: Cauda equina syndrome secondary to lumbar disc herniation: A meta-analysis of surgical outcomes. Spine 2000;25:1515-1522. Shapiro S: Medical realities of cauda equina syndrome secondary to lumbar disc herniation. Spine 2000;25:348-351.
Question 80
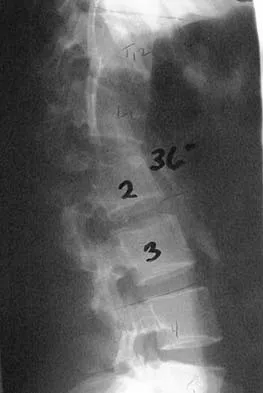
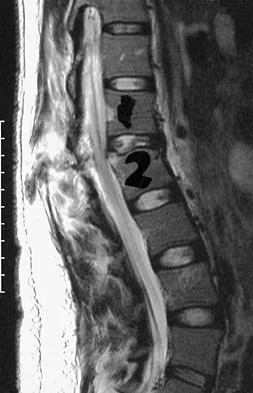
Figures 26a and 26b show the radiograph and MRI scan of an 18-year-old man who fell from a trampoline. Examination reveals exquisite local tenderness at the thoracolumbar junction, but he is neurologically intact. Management should consist of
Explanation
Based on the radiographic findings of marked disruption of the posterior ligamentous complex with a relatively small anterior bony fracture, the patient has a classic Chance-type ligamentous flexion-distraction injury. The pathology is mostly in soft tissues with limited healing potential. The treatment of choice is posterior reconstruction of the tension band with a short segment fusion with instrumentation. Casting or bracing may result in a painful kyphosis with ligamentous insufficiency. The anterior bony column is mostly intact, so anterior reconstruction is not necessary. Carl AL: Adult spine trauma, in DeWald RL (ed): Spinal Deformities: A Comprehensive Text. New York, NY, Thieme, 2003, pp 406-423.
Question 81
A 17-year-old high school football player is seen for follow-up after sustaining an injury 3 days ago. He reports that he tackled a player, felt numbness throughout his body, and could not move for approximately 15 seconds. A spinal cord injury protocol was initiated on the field. Evaluation in the emergency department revealed a normal neurologic examination and full painless neck motion. He states that he has no history of a similar injury. An MRI scan of the cervical spine is normal. During counseling, the patient and his family should be informed that he has sustained
Explanation
The long-term effect of transient quadriplegia is unknown. Based on a history of one brief episode of transient quadriplegia and normal examination and MRI findings, the risk of permanent spinal cord injury with a return to play is low. There is a risk of recurrent episodes of transient quadriplegia after the initial episode. Morganti C, Sweeney CA, Albanese SA, et al: Return to play after cervical spine injury. Spine 2001;26:1131-1136. Odor JM, Watkins RG, Dillin WH, et al: Incidence of cervical spinal stenosis in professional and rookie football players. Am J Sports Med 1990;18:507-509. Torg JS, Naranja RJ Jr, Palov H, et al: The relationship of developmental narrowing of the cervical spinal canal to reversible and irreversible injury of the cervical spinal cord in football players. J Bone Joint Surg Am 1996;78:1308-1314.
Question 82
Which of the following is considered a contraindication to cement injection techniques, such as kyphoplasty or vertebroplasty, in the treatment of osteoporotic compression fractures?
Explanation
When retropulsion of the posterior vertebral wall is present, nothing prohibits the cement from following the path of least resistance into the canal or from pushing a bone fragment further into the canal; most clinicians consider it a contraindication to these techniques. Patient age itself is not a contraindication as long as there are no medical contraindications to surgery. An acute fracture in a patient who remains immobile and hospitalized because of pain may be a good indication for such a technique. Prior compression fracture and older compression fractures are not contraindications, but pain relief may be less predictable. Phillips FM, Pfeifer BA, Leiberman IH, et al: Minimally invasive treatment of osteoporotic vertebral compression fractures: Vertebroplasty and kyphoplasty. Instr Course Lect 2003;52:559-567. Truumees E, Hilibrand A, Vaccaro AR: Percutaneous vertebral augmentation. Spine J 2004;4:218-229.
Question 83
Chronic anterior donor site pain following the harvest of autologous iliac crest bone graft for use during anterior cervical diskectomy and fusion is reported by approximately what percent of patients?
Explanation
Four years after surgery, more than 90% of patients are satisfied with the cosmetic appearance of the iliac donor site scar. Approximately 25% still have pain and/or functional difficulty, including 12.7% who still report difficulty with ambulation, 11.9% difficulty with recreational activities, 7.5% with sexual intercourse, and 11.2% require pain medication for iliac donor site symptoms. Silber JS, Anderson DG, Daffner SD, et al: Donor site morbidity after anterior iliac crest bone harvest for single-level anterior cervical discectomy and fusion. Spine 2003;28:134-139.
Question 84
When treating osteoporosis with alendronate, what is the most common side effect?
Explanation
Alendronate is a second-generation bisphosphonate, and it can cause epigastric distress in up to 30% of patients. This side effect can be minimized by gradually building up to therapeutic doses over a period of 4 to 8 weeks. Marshall JK, Rainsford KD, James C, et al: A randomized controlled trial to assess alendoronate-associated injury of the upper gastrointestinal tract. Aliment Pharmacol Ther 2000;14:1451-1457.
Question 85
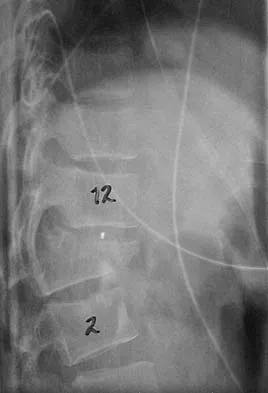
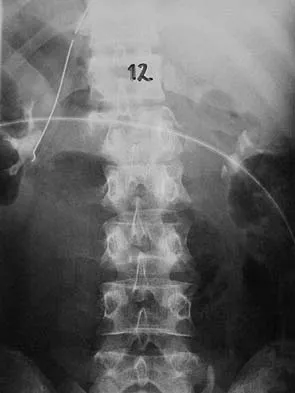
Figures 27a and 27b show the radiographs of a 32-year-old woman who was involved in a high-speed motor vehicle accident. She is neurologically intact. After stabilization and assessment, treatment should consist of
Explanation
The radiographs show a fracture-dislocation with translation in both the coronal and sagittal planes, evidence of significant instability requiring surgical stabilization. Anterior instrumentation is not as effective as posterior instrumentation in restoring stability, and because there is little bony destruction, the anterior column can be successfully reconstructed with simple realignment. The treatment of choice is multisegment posterior fusion with instrumentation. Lewandrowski KU, McLain RF: Thoracolumbar fractures: Evaluation, classification, and treatment, in Frymoyer JW, Wiesel SW (eds): The Adult and Pediatric Spine. Philadelphia, PA, Lippincott Williams and Wilkins, 2004, pp 817-843.
Question 86
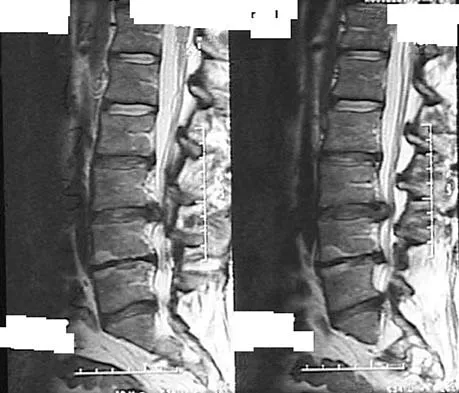
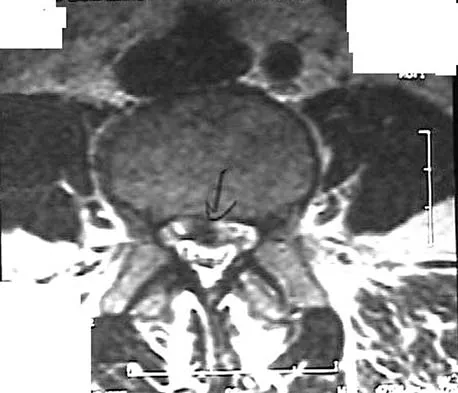
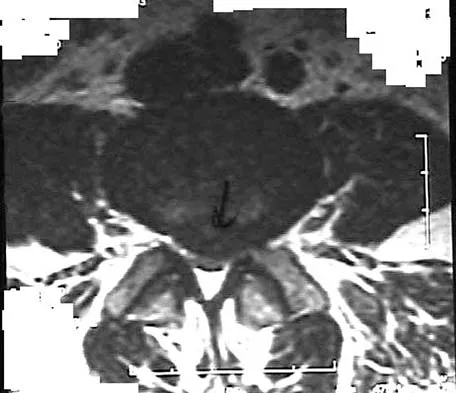
Figures 28a through 28c show the MRI scans of a 30-year-old woman who weighs 290 lb and has low back and left leg pain. She also reports frequent urinary dribbling, which her gynecologist has advised her may be related to obesity. Examination will most likely reveal
Explanation
The patient will most likely exhibit ipsilateral weakness of the tibialis anterior. Gaenslen's test is designed to detect sacroiliac inflammation as a source of low back pain. Beevor's sign tests the innervation of the rectus abdominus and paraspinal musculature (L1 innervation). The extensor hallucis longus is predominantly innervated by L5. The peroneals are predominantly innervated by S1. Hoppenfeld S: Physical Examination of the Spine and Extremities. Appleton, WI, Century-Crofts, 1976.
Question 87
Which of the following statements regarding conus medullaris syndrome is most accurate?
Explanation
Conus medullaris syndrome most frequently occurs as a result of trauma or with a disk herniation at L1, resulting in a lower motor neuron syndrome but with a poor prognosis for recovery of bowel and bladder dysfunction. The conus region, as the termination of the spinal cord, contains the motor cell bodies of the sacral roots. The syndrome is usually a sacral level neural injury; therefore, lower extremity weakness is uncommon. Haher TR, Felmly WT, O'Brien M: Thoracic and lumbar fractures: Diagnosis and management, in Bridwell KH, Dewald RL, Hammerberg KW, et al (eds): The Textbook of Spinal Surgery, ed 2. New York, NY, Lippincott Williams & Wilkins, 1977, pp 1773-1778.
Question 88
Which of the following factors has the greatest effect on the pull-out strength of a lumbar pedicle screw?
Explanation
All of the factors listed contribute to some extent to the pull-out strength of lumbar pedicle screws, but bone mineral density correlates most precisely. Wittenberg RH, Shea M, Swartz DE, et al: Importance of bone mineral density in instrumented spine fusions. Spine 1991;16:647-652.
Question 89
An inverted radial reflex is associated with
Explanation
An inverted radial reflex is a hypoactive brachioradialis reflex in combination with involuntary finger flexion. It is a spinal cord "release" sign and is associated with upper motor neuron pathology as seen in cervical stenosis with myelopathy. Radiculopathy is characterized by a diminished reflex but no finger flexion. Peripheral neuropathy is not associated with any reflex change. Parsonage-Turner syndrome is an idiopathic brachial neuritis. Clark CR (ed): The Cervical Spine, ed 3. Philadelphia, PA, Lippincott Williams & Wilkins, 1998, p 762.
Question 90
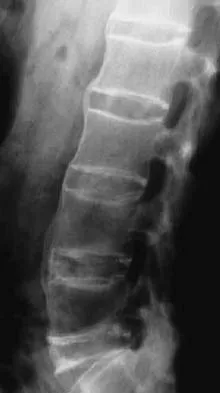
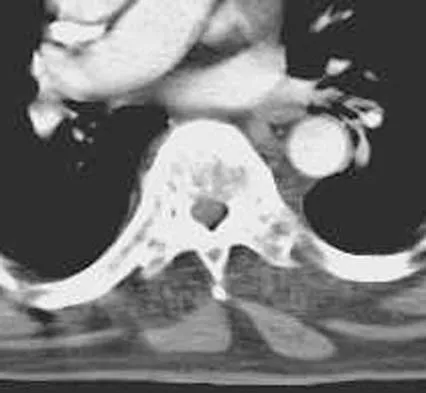
Figures 29a and 29b show the radiograph and CT scan of a 48-year-old man who has diffuse spinal pain. What is the most likely diagnosis?
Explanation
The studies show marginal syndesmophyte formation characteristic of ankylosing spondylitis. These patients typically have diffuse ossification of the disk space without large osteophyte formation. DISH typically presents with large osteophytes, referred to as nonmarginal syndesmophytes. In this patient, the zygoapophyseal joints are fused rather than degenerative as would be seen in rheumatoid arthritis, and the costovertebral joints are also fused. Osteopetrosis does not normally ankylose the disk space. McCullough JA, Transfeldt EE: Macnab's Backache, ed 3. Baltimore, MD, Williams and Wilkins, 1997, pp 190-194.
Question 91
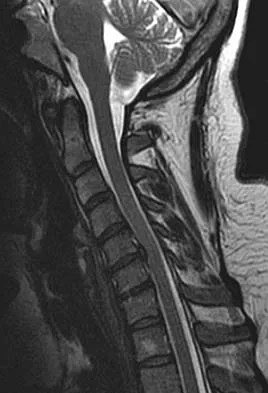
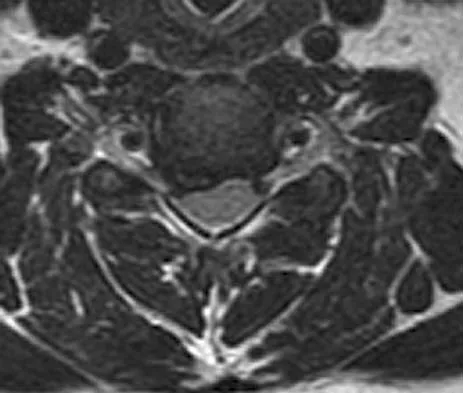
The cervical disk herniation shown in the MRI scans in Figures 30a and 30b will most likely create which of the following constellations of symptoms?
Explanation
The MRI scans reveal a right-sided C5-6 herniated nucleus pulposus. A disk herniation in this region encroaches on the C6 root and is accompanied by a sensory change along the thumb and index finger, alterations in the brachioradialis reflex, and possible wrist extension weakness. Although the nerve root associated with the vertebral body passes above the pedicles such that the C6 root passes above the C6 pedicle, it is still the C6 root that is encroached on because the herniation affects the exiting root rather than the traversing root as seen in the lumbar spine. Klein JD, Garfin SR: Clinical evaluation of patients with suspected spine problems, in Frymoyer JW (ed): Adult Spine: Principles and Practice, ed 2. Philadephia, PA, Lippincott-Raven, 1997, pp 319-330.
Question 92
A 21-year-old man has had posterior neck discomfort for the past 6 months. A whole-body bone scan and a cervical single-photon emission CT reveal increased activity at the C7 spinous process. MRI reveals multifocal involvement of the spinous process lamina and facet of C7. A CT-directed needle biopsy reveals osteoblastoma. What is the best course of action?
Explanation
En bloc excision is the recommended treatment of osteoblastoma. Treatment should consist of en bloc removal of the lamina, facet, and spinous process. Facet removal would necessitate fusion. Radiation therapy is not recommended. Intralesional curettage has a high rate of recurrence. Bridwell KH, Ogilvie JW: Primary tumors of the spine, in Bridwell KH, DeWald RL (eds): The Textbook of Spinal Surgery. Philadelphia, PA, JB Lippincott, 1991, vol 2, pp 1143-1174.
Question 93
What is the most likely consequence of a vertebral compression fracture associated with osteoporosis?
Explanation
After an osteoporotic vertebral compression fracture, the risk of subsequent fractures at adjacent levels increases. This is felt to be the result of a shifting of the sagittal alignment more anteriorly, putting more stress on the osteopenic vertebral bodies and their anterior cortices. Pain generally resolves with rest, but this may take weeks or months. It has been demonstrated experimentally that osteoporotic vertebral bodies are actually less stiff and weaker after a compression fracture; therefore, deformity predisposes to further deformity. The extensor musculature often fatigues over time and usually does not hypertrophy. Frontal plane deformity is a rare development. Heaney RP: The natural history of vertebral osteoporosis: Is low bone mass an epiphenomenon? Bone 1992;13:S23-S26.
Question 94
What is the most appropriate treatment for a chordoma involving the sacrum?
Explanation
Chordomas are very radio- and chemotherapy resistant; therefore, en bloc resection with a negative margin is the preferred treatment. Lesions at or below S3 can be resected without compromising pelvis stability, and continence usually is maintained. The mean survival rate for patients with sacral chordomas is approximately 7 years. Patients with chordoma of the mobile (cervical, thoracic, or lumbar) spine have a mean survival rate of approximately 5 years. This difference is most likely the result of an earlier diagnosis. Fardin DF, Garfin SR, Abitbol J, et al (eds): Orthopaedic Knowledge Update: Spine 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 123-133. Stener B, Gunterberg B: High amputation of the sacrum for extirpation of tumors: Principles and technique. Spine 1978;3:351-366.
Question 95
A 62-year-old woman has back pain and right L2 radicular pain. MRI scans suggest a neoplastic lesion at L2, and a bone scan is negative except at L2. History reveals that she was treated for breast cancer without known metastatic disease 12 years ago and is thought to be free of disease. What is the next most appropriate step in management?
Explanation
Because of the long disease-free interval, it cannot be assumed that this is breast cancer. The lesion could represent metastasis from a new primary tumor or could itself be a primary tumor. CT-guided biopsy will most effectively identify the lesion and guide treatment options. Depending on the specific diagnosis, any of the other options may be appropriate.
Question 96
A 60-year-old woman with rheumatoid arthritis has atlanto-axial instability and basilar invagination. What MRI findings would suggest the need for cervical fusion?
Explanation
The cervical medullary junction should be 135 degrees or greater. An angle of 125 degrees suggests compression of the cervical medullary junction. Other findings supporting surgical intervention include a cord diameter in flexion of less than 6 mm or less than 13 mm of space available for the cord. Clark CR (ed): The Cervical Spine, ed 3. Philadelphia, PA, Lippincott Williams & Wilkins, 1998, pp 700-701. Monsey RB: Rheumatoid arthritis of the cervical spine. J Am Acad Orthop Surg 1997;5:240-248.
Question 97
Which of the following statements is most accurate regarding undetected intraoperative surgical glove perforation?
Explanation
The incidence of undetected intraoperative surgical glove perforation has been demonstrated at approximately 8.5%, occurring most frequently on the index finger or left hand of the assistant surgeon. The frequency of glove perforation is higher in surgeries lasting longer than 3 hours. Al-Habdan I, Sadat-Ali M: Glove perforation in pediatric orthopaedic practice. J Pediatr Orthop 2003;23:791-793.
Question 98
Which of the following is NOT considered a risk factor for nonunion of a type II odontoid fracture?
Explanation
Although obesity can make brace or halo wear difficult, it has not been associated with an increased risk for nonunion. Carson GD, Heller JG, Abitbol JJ, et al: Odontoid fractures, in Levine AM, Eismont FJ, Garfin SR, et al (eds): Spine Trauma. Philadelphia, PA, WB Saunders, 1998, pp 235-238.
Question 99
A 27-year-old woman has a bilateral C5-C6 facet dislocation and quadriparesis after being involved in a motor vehicle accident. Initial management consisted of reduction with traction, but she remains a Frankel A quadriplegic. To facilitate rehabilitation, surgical stabilization and fusion is planned. From a biomechanical point of view, which of the following techniques is the LEAST stable method of fixation?
Explanation
In two different biomechanical studies performed in both bovine and human cadaveric spines, all posterior techniques of stabilization were found to be superior to anterior plating in flexion-distraction injuries of the cervical spine. These injuries usually have an intact anterior longitudinal ligament that allows posterior fixation to function as a tension band. Anterior plating with grafting destroys this last remaining stabilizing structure and does not allow for a tension band effect because all of the posterior stabilizing structures have been destroyed with the injury. In clinical practice, however, anterior plating can be effective in the treatment of this injury with appropriate postoperative orthotic management. Sutterlin CE III, McAfee PC, Warden KE, et al: A biomechanical evaluation of cervical spine stabilization methods in a bovine model: Static and cyclical loading. Spine 1988;13:795-802.
Question 100
Which of the following findings is considered a poor prognostic factor for postoperative neurologic recovery in patients with rheumatoid arthritis?
Explanation
When markedly diminished space available for the cord (demonstrated by a posterior atlantoaxial interval of less than 10 mm) is seen, there is a poor prognosis for recovery (25% of Ranawat class IIIb patients) following surgery. A posterior atlantoaxial interval of 14 mm or less is a predictor of increased risk of paralysis, but patients with an interval between 10 mm and 14 mm have a greater chance of recovery. Space available for the cord that is at least 14 mm is not associated with an increased risk of neurologic deficit. Boden SD, Dodge LD, Bohlman HH, et al: Rheumatoid arthritis of the cervical spine: A long-term analysis with predictors of paralysis and recovery. J Bone Joint Surg Am 1993;75:1282-1297.
