00:00
Start Quiz
Question 51
Figure 16 shows the radiograph of a 56-year-old man who has neck pain after a rollover accident on his lawnmower. The injury appears to be isolated, and he is neurologically intact. Management of the fracture should consist of
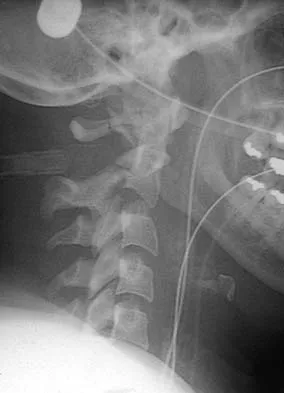
Explanation
The radiograph shows a type IIa Hangman's fracture, and the classic treatment is halo vest immobilization. Traction should be avoided in type IIa injuries because of the risk of overdistraction. A lesser form of immobilization such as a hard collar or a Minerva jacket can be used for nondisplaced (type I) fractures. Surgery generally is reserved for type III fractures (includes C2-3 facet dislocation), or extenuating circumstances such as multiple trauma or other fractures of the cervical spine that require surgical stabilization. Levine AM, Edwards CC: The management of traumatic spondylolisthesis of the axis. J Bone Joint Surg Am 1985;67:217-226.
Question 52
Degenerative spondylolisthesis of the cervical spine is most commonly seen at which of the following levels?
Explanation
Degenerative spondylolisthesis of the cervical spine is seen almost exclusively at C3-4 and C4-5; this is in contrast to degenerative changes, which are most commonly seen at C5-6 and C6-7. Tani T, Kawasaki M, Taniguchi S, et al: Functional importance of degenerative spondylolisthesis in cervical spondylotic myelopathy in the elderly. Spine 2003;28:1128-1134.
Question 53
Thoracic disk herniations are most frequently found in what area of the spine?
Explanation
Although thoracic disk herniations have been reported at all levels of the thoracic spine, more than two thirds are found at T9-T12, which is the more mobile lower third of the thoracic region. Belanger TA, Emery SE: Thoracic disc disease and myelopathy, in Frymoyer JW, Wiesel SW (eds): The Adult and Pediatric Spine. Philadelphia, PA, Lippincott Williams and Wilkins, 2004, pp 855-864.
Question 54
In a patient who has had low back pain for less than 2 weeks, which of the following findings is an indication for continued observation and symptomatic treatment rather than more aggressive evaluation and/or treatment?
Explanation
An inability to participate in athletics generally is considered an indication for continued symptomatic treatment only. All of the other answers suggest the possibility of more significant pathology that may require more urgent treatment. Frymoyer JW: Back pain and sciatica. N Engl J Med 1988;318:291-300.
Question 55
Radiographs of an 80-year-old woman with back pain reveal a compression fracture. Which of the following imaging studies best evaluates the acuity of the fracture?
Explanation
The best method of evaluating the acuity of osteoporotic compression fractures is to look for edema in the vertebral body. This is best accomplished with a STIR-weighted MRI scan. Bone scans can show increased uptake at the site of fracture for many months after the fracture. T1-weighted MRI scans show loss of normal marrow fat that may not necessarily correspond with acuity of the fracture. CT scans and radiographs show fracture deformity but cannot be used to judge acuity. Phillips FM: Minimally invasive treatments of osteoporotic vertebral compression fractures. Spine 2003;28:S45-S53.
Question 56
A 24-year-old professional football player underwent surgery for a symptomatic cervical disk herniation with radiculopathy 9 months ago. A current radiograph is shown in Figure 17. He has normal neurologic findings, no pain, and full range of motion. A CT scan shows a solid fusion. When can he expect to return to play?
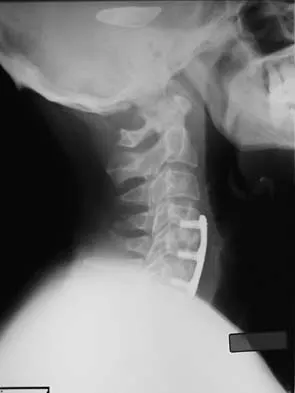
Explanation
The radiograph shows that the two-level anterior cervical diskectomy and fusion has healed. In addition, the patient has good range of motion and the neurologic examination is normal. Based on these findings, the patient can return to play immediately. Patients with one- or two-level anterior cervical diskectomies and fusions that have healed fully can return to play. Any loss of motion, persistent neurologic deficit, or significant adjacent segment degeneration may preclude a player from returning. Thomas B, McCullen GM, Yuan HA: Cervical spine injuries in football players. J Am Acad Orthop Surg 1999;7:338-347.
Question 57
When treating thoracic disk herniations, which of the following surgical approaches has the highest reported rate of neurologic complications?
Explanation
Numerous surgical approaches have been used for thoracic diskectomy, including the most recent VATS. One of the first approaches described, posterior laminectomy, involves manipulation of the spinal cord, which the other approaches avoid. The posterior approach had dismal results, including further neurologic deterioration and even paralysis. Belanger TA, Emery SE: Thoracic disc disease and myelopathy, in Frymoyer JW, Wiesel SW (eds): The Adult and Pediatric Spine. Philadelphia, PA, Lippincott Williams and Wilkins, 2004, pp 855-864. Benjamin V: Diagnosis and management of thoracic disc disease. Clin Neurosurg 1983;30:577-605. Russell T: Thoracic intervertebral disc protrusion: Experience of 67 cases and review of the literature. Br J Neurosurg 1989;3:153-160.
Question 58
When harvesting iliac crest bone graft during a posterior spinal decompression and fusion, injury to what structure can result in painful neuromas or numbness over the skin of the buttocks?
Explanation
The superior cluneal nerves (L1, L2, and L3) are most at risk when harvesting iliac crest bone graft during a posterior decompression and fusion. These nerves pierce the lumbodorsal fascia and cross the posterior iliac crest, beginning 8 cm lateral to the posterior superior iliac spine. The ilioinguinal nerve is more at risk during exposure of the anterior ilium during retraction of the iliacus and abdominal wall muscles. Iliohypogastric nerve injury may arise in a similar fashion to ilioinguinal neuralgia. The lateral femoral cutaneous nerve lies in close proximity to the anterior superior iliac spine and is also at risk with anterior iliac crest bone graft harvesting. The superior gluteal nerve courses through the sciatic notch and supplies motor branches to the gluteus medius, minimus, and tensor fascia lata muscles. Injury results in hip abduction weakness. An HS: Principles and Techniques of Spine Surgery. Baltimore, MD, Williams and Wilkins 1998, pp 770-773. Kurz LT, Garfin SR, Booth RE Jr: Harvesting autogenous iliac bone grafts: A review of complications and techniques. Spine 1989;14:1324-1331.
Question 59
A 42 year-old-woman who underwent surgery for lumbar scoliosis 2 years ago now has fixed sagittal plane imbalance and severe back pain. Which of the following is considered a contraindication to isolated pedicle subtraction osteotomy for the treatment of iatrogenic flatback syndrome in this patient?
Explanation
Pedicle subtraction osteotomy is the preferred osteotomy technique for the treatment of many patients with iatrogenic flatback syndrome. In the presence of an anterior pseudarthrosis, however, it must be done in conjunction with an anterior procedure. Prior laminectomy is not a contraindication. Significant correction, usually averaging about 30 degrees, can be obtained through each osteotomy. Osteotomies should be performed at L2 or below in the presence of kyphosis at the thoracolumbar junction. The pedicle subtraction technique is preferred with vascular calcifications because it does not lengthen the anterior column, which could risk vascular injury. Potter BK, Lenke LG, Kuklo TR: Prevention and management of iatrogenic flatback deformity. J Bone Joint Surg Am 2004;86:1793-1808.
Question 60
A 42-year-old man sustained a burst fracture at L2 in a motor vehicle accident. Examination reveals that he is neurologically intact. Figure 18 shows a cross-sectional CT scan through the fracture. If the fracture is managed nonsurgically for the next 2 years, the retained fragments can be expected to
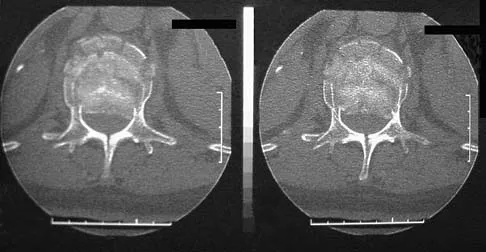
Explanation
Numerous articles have reported that both surgical and nonsurgical management of burst fractures are associated with resolution of impingement at long-term follow-up. If the patient is neurologically intact and appropriately treated at the time of injury, neurologic deterioration is not expected nor is there a risk of injury to the dural sac. The retained fragments can be expected to gradually resorb and widen the spinal canal. Mumford J, Weinstein JN, Spratt KF, et al: Thoracolumbar burst fractures: The clinical efficacy and outcome of nonoperative management. Spine 1993;18:955-970.
Question 61
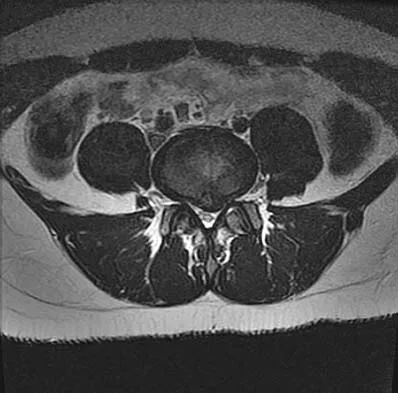
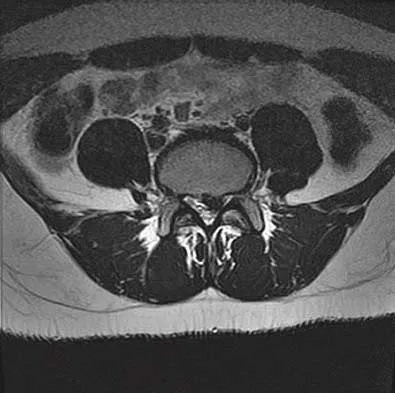
A 50-year-old man reports the onset of back pain and incapacitating pain radiating down his left leg posterolaterally and into the first dorsal web space of his foot 1 day after doing some yard work. He denies any history of trauma. Examination reveals ipsilateral extensor hallucis longus weakness. MRI scans are shown in Figures 19a through 19c. What nerve root is affected?
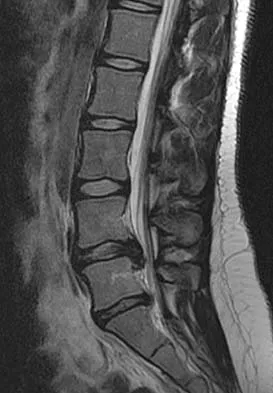
Explanation
The MRI scans clearly show an extruded L4-5 disk that is affecting the L5 root on the left side. In addition, the L5 root has a cutaneous distribution in the first dorsal web space. S1 affects the lateral foot, and L4 affects the medial calf. An HS: Principles and Techniques of Spine Surgery. Baltimore, MD, Williams and Wilkins, 1998, pp 98-100.
Question 62
Which of the following pharmacologic agents is most likely to adversely affect the success rate of bony union after lumbar arthrodesis?
Explanation
Glassman and associates reported a significantly higher pseudarthrosis rate when ketorolac was used postoperatively compared to a similar group of patients who were not given ketorolac. Animal studies from the same institution support these clinical findings. To reduce narcotic dosage, nonsteroidal anti-inflammatory drugs (NSAIDs) have been promoted as an adjunct for postoperative analgesia in patients undergoing spinal fusion. However, a high failure rate of arthrodesis has been associated with postoperative use of NSAIDs. The analgesics oxycodone hydrochloride, hydrocodone/acetaminophen, and tramadol, as well as the tricyclic antidepressant imipramine, have not been shown to inhibit fusion. Glassman SD, Rose SM, Dimar JR, et al: The effect of postoperative nonsteroidal anti-inflammatory drug administration on spinal fusion. Spine 1998;23:834-838.
Question 63
A 69-year-old woman is seen in the emergency department with a bilateral C5-6 facet dislocation and complete quadriplegia after falling down a flight of stairs. After initial evaluation and treatment by the trauma service, she is moved to the intensive care unit. Examination reveals a blood pressure of 90/50 mm/Hg, a pulse rate of 50/min, a respiration rate of 12/min, and urine output of 1 mL/kg/h. Her hemodynamic status should be addressed by
Explanation
The patient's heart rate is not responding to hypotension with tachycardia, as would be expected in the event of hypovolemic shock. Additionally, the adequate urine output suggests proper fluid resuscitation. Instead, she is bradycardic, possibly indicating neurogenic shock and loss of sympathetic tone to the heart. A Swan-Ganz catheter should be used to help differentiate these problems and guide appropriate fluid resuscitation and use of vasopressor agents. Hadley MN: Management of acute spinal cord injuries in an intensive care unit or other monitored setting. Neurosurgery 2002;50:S51-S57.
Question 64
What region of the spine is most susceptible to changes in the vascular supply to the spinal cord during an anterior approach?
Explanation
The thoracic spinal cord is characterized by a variable and, at times, complicated blood supply. The artery of Adamkiewicz, also known as the great anterior medullary artery, most typically arises off the left side of the aorta between T8 and T12. It represents the sole medullary blood supply to the thoracic spine. When this artery is divided or injured, the blood supply to the thoracic cord may be interrupted. It is important to avoid electocautery of blood vessels within or near the thoracic foramen because this is a site of important, albeit limited, collateral circulation. Sharma M, Anderson FC: Spinal vascular lesions, in Frymoyer JW, Wiesel SW (eds): The Adult and Pediatric Spine. Philadelphia, PA, Lippincott Williams and Wilkins, 2004, pp 301-306.
Question 65
What is the most common presenting sign or symptom in an adult with lumbar pyogenic infection?
Explanation
Pain is very common but is often nonspecific; therefore, the diagnosis of spinal infection is often delayed. Fever and sepsis can occur but are not common. Neurologic manifestations also can occur but are absent in most patients. In findings reported by Carragee, the urinary tract is a common source for hematogenous spinal infection, but the source was found in only 27% of 111 patients. Direct inoculation during spinal surgery is uncommon. Carragee EJ: Pyogenic vertebral osteomyelitis. J Bone Joint Surg Am 1997;79:874-880. Frazier DD, Campbell DR, Garvey TA, et al: Fungal infections of the spine: Report of eleven patients with long-term follow-up. J Bone Joint Surg Am 2001;83:560-565.
Question 66
The natural history of cervical spondylolytic myelopathy is best described as
Explanation
The natural history of cervical myelopathy has been described by Lees and Turner as exacerbations of symptoms followed by often long periods of static or deteriorating function (or very rarely improvement). This stepwise pattern of decreasing function has been corroborated by Clarke and Robinson. These authors described long periods of stable neurologic function, sometimes lasting for years, in about 75% of their patients. In the majority of the patients, however, the condition deteriorated between quiescent streaks. About 20% of their patients showed a slow, steady progression of symptoms and signs without a stable period, and 5% had rapid deterioration of neurologic function. Emery SF: Cervical spondylotic myelopathy: Diagnosis and treatment. J Am Acad Orthop Surg 2001;9:376-388. Lees F, Turner JA: The natural history and prognosis of cervical spondylosis. Brit Med J 1963;2:1607-1610.
Question 67
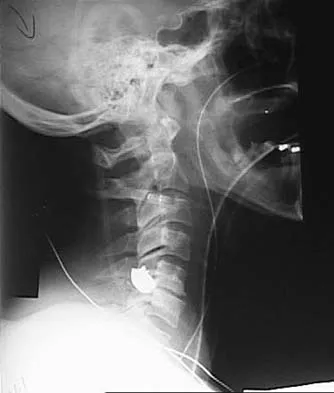
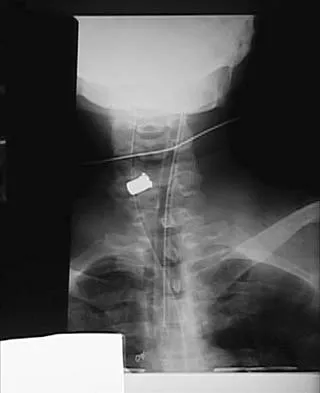
Figures 20a and 20b show lateral and AP radiographs of a 49-year-old man who sustained a gunshot wound through the left shoulder. He reports neck pain and examination reveals weakness in all four extremities. What is the priority of evaluation?
Explanation
The projectile entered the left shoulder and traveled to the right neck; therefore, a high incidence of suspicion must be directed to the airway, great vessels of the neck, and contents of the mediastinum. Immediate assessment of airway, breathing, and circulation takes priority, followed by examination of the neurologic status and other systems, as determined by the examination findings. Subcommittee on ATLS of the American College of Surgeons Committee on Trauma 1993-1997, Spine and Spinal Cord Trauma; Advanced Trauma Life Support Student Manual, ed 6, 1997. International Standards for Neurological and Functional Classification of Spinal Cord Injury. American Spinal Injury Association and International Medical Society of Paraplegia (ASIA/IMSOP).
Question 68
A 35-year-old woman undergoes an L4-5 anterior fusion via a left retroperitoneal approach. Postoperative examination reveals that her right foot is cool and pale. Her neurologic examination is normal, and her pedal pulses are asymmetric. What is the most likely reason for the right foot finding?
Explanation
The lower extremity symptoms are consistent with a sympathectomy that is the result of an injury to the sympathetic chain, ipsilateral to the approach along the anterior border of the lumbar spine. This results in a warm, red foot, which creates the appearance that the normal cooler foot may have compromised circulation. The latter generally attracts greater attention because of the risks associated with limb ischemia. The condition usually is self-limited and does not require any specific treatment. Rothman RH, Simeone FA (eds): The Spine, ed 4. Philadelphia PA, WB Saunders, 1999, p1550.
Question 69
What type of thoracolumbar spinal injury is associated with an increased risk of neurologic deterioration following admission to the hospital?
Explanation
Gertzbein's Scoliosis Research Society Morbidity and Mortality report noted that neurologic deterioration developed in approximately 16% of patients who were hospitalized with fracture-dislocations of the thoracolumbar spine, a particular concern with rotational burst fractures (AO type C). Patients with standard burst fractures and Chance fractures had a markedly lower incidence of neurologic involvement and tended to remain neurologically stable. Gertzbein SD: Neurologic deterioration in patients with thoracic and lumbar fractures after admission to the hospital. Spine 1994;19:1723-1725.
Question 70
A 30-year-old man has had a 3-day history of severe, incapacitating lower back pain without radiation. He reports improvement with rest. He denies any history of trauma, has no constitutional symptoms, and his neurologic examination is normal. What is the best course of action?
Explanation
There are no red flags in the history or examination to warrant MRI. Limited bed rest (less than 3 days) has been shown to be more beneficial to early recovery compared with prolonged bed rest (more than 7 days). No data support the use of epidural or facet steroid injections for acute low back pain.
Question 71
Which of the following patient factors is associated with recurrent radicular pain following lumbar diskectomy for sciatica?
Explanation
A large annular defect at the site of a lumbar disk herniation is associated with persistent radicular pain postoperatively. Large sequestered herniations and a positive SLR preoperatively correlate with good outcomes after diskectomy. Neither symptoms of more than 3 months' duration nor preoperative epidural steroid injections correlate with postoperative results after diskectomy. Carragee EJ, Han MY, Suen PW, et al: Clinical outcomes after lumbar discectomy for sciatica: The effects of fragment type and anular competence. J Bone Joint Surg Am 2003;85:102-108.
Question 72
Figure 21 shows the tomogram of a 26-year-old woman who sustained an axial load injury to her neck in a fall off a horse. What ligament is injured?

Explanation
Levine and Edwards, in their description of the classic C1 burst (Jefferson) fracture, noted that spread of the lateral masses of more than 7 mm is indicative of a transverse ligament rupture. Long-term C1-C2 instability, however, has not been described with this fracture pattern. Although long-term traction followed by halo vest immobilization has been described as the best technique for achieving an ideal result, treatment of this injury remains somewhat controversial. Levine AM, Edwards CC: Fractures of the atlas. J Bone Joint Surg Am 1991;73:680-691.
Question 73
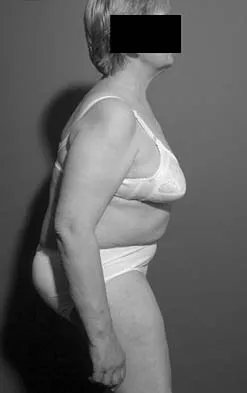
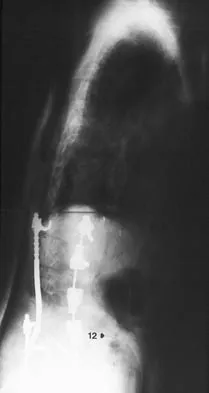
Based on the findings shown in Figures 22a and 22b, corrective surgery to obtain maximal safe correction and optimal instrumentation fixation should be performed at which of the following locations?
Explanation
The clinical photograph and radiograph show an iatrogenic flatback deformity with loss of the normal lumbar lordosis. The safest correction for this malalignment typically is performed away from the spinal cord in the midlumbar spine, most commonly at L2 or L3. The more distal the correction is performed, the more sagittal plane translation of the C7 plumb line with respect to the posterior sacrum. Performing the osteotomy too distally, however, makes it difficult to obtain adequate distal fixation. Shufflebarger HL, Clark CE: Thoracolumbar osteotomy for postsurgical sagittal imbalance. Spine 1992;17:S287-S290.
Question 74
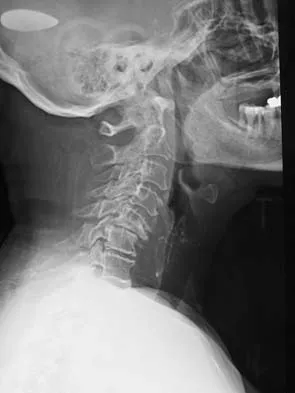
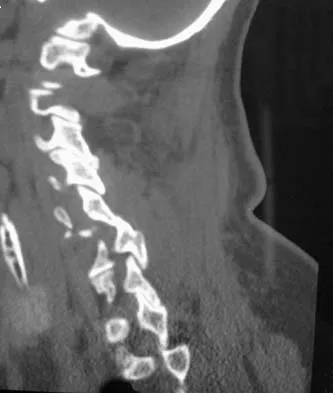
A 65-year-old woman has significant neck pain after falling and striking her head. A radiograph and sagittal CT scan are shown in Figures 23a and 23b. What is the most likely diagnosis?
Explanation
The radiograph shows a displacement of C5 on C6 of approximately 25%. The CT scan shows a perched facet at C5-6. There is no evidence of a facet fracture. A bilateral facet dislocation would show a displacement of more than 50%. Rothman RH, Simeone FA (eds): The Spine, ed 4. Philadelphia PA, WB Saunders, 1999, pp 927-937.
Question 75
Immediately after undergoing lumbar instrumentation, a patient reports severe right leg pain and has 4+/5 weakness. Figure 24 shows an axial CT scan of L5. Exploratory surgery will most likely reveal
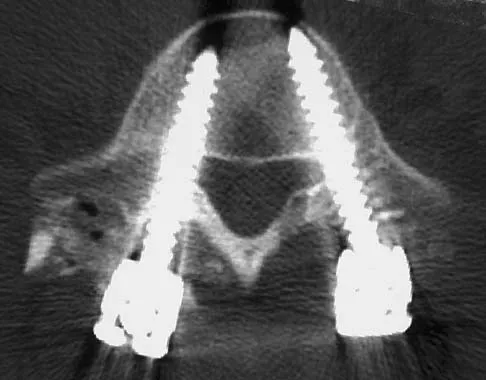
Explanation
The most common finding at exploration of an inappropriately placed pedicle screw is displacement of the nerve. Pedicle breach is common, ranging from 2% to 20%, but most are asymptomatic. All of the choices are possible, but in a large series conducted by Lonstein and associates, the authors reported that displacement of the root, most often medial, was the most common finding. Laceration, contusion, or transfixion usually was not seen. Spinal fluid leakage occurs less frequently and is not expected in the minimal broach illustrated. Esses SI, Sachs BL, Dreyzin V: Complications associated with the technique of pedicle screw fixation: A selected survey of ABS members. Spine 1993;18:2231-2238. Laine T, Lund T, Ylikoski M, et al: Accuracy of pedicle screw insertion with and without computer assistance: A randomised controlled clinical study in 100 consecutive patients. Eur Spine J 2000;9:235-240.
