Upper Extremity Replantation: Surgical Principles and Microvascular Techniques
Key Takeaway
Upper extremity replantation demands meticulous microvascular expertise and a multidisciplinary team approach. Successful outcomes hinge on strict patient selection, minimizing warm ischemia time, and precise surgical execution. This guide details the critical indications, contraindications, and step-by-step surgical protocols required to restore optimal function and sensibility following traumatic amputations of the hand and upper limb.
THE REPLANTATION TEAM AND INFRASTRUCTURE
Replantation of amputated upper extremity parts is a highly complex, resource-intensive endeavor that must be performed exclusively by surgeons fellowship-trained in hand and upper extremity surgery. Furthermore, digital replantation requiring the operating microscope mandates a surgeon who has demonstrated the ability to perform reliable microvascular anastomoses with a predictable patency rate of 90% or greater.
Although a single surgeon supported by highly trained and motivated assistants can perform a replantation, the current standard of care strongly favors the use of rotating surgical teams. Replantation procedures frequently exceed 12 hours; fatigue significantly degrades microvascular precision. During the microvascular portions of the procedure, at least one of the scrubbed surgeons must be highly proficient in microvascular and microneural repairs.
Institutional infrastructure is equally critical. The replantation service must provide:
* 24/7 Coverage: Rotating availability of microsurgeons without interruption.
* Specialized Personnel: Scrub nurses and surgical assistants intimately familiar with the sequence of events, micro-instruments, and specialized equipment.
* Facility Support: Dedicated surgical suites, an intensive care unit (ICU) available around the clock, and specialized anesthesia personnel adept at prolonged regional and general anesthesia, fluid management, and vasospasm prevention.
GENERAL CONSIDERATIONS AND PATIENT SELECTION
The overarching philosophy of replantation is that the anticipated functional outcome must surpass that of a well-fitted prosthesis or a revised amputation stump. The difference in functional gain must justify the significant surgical risk, prolonged operative time, extensive rehabilitation, and economic expense.
The potential for the replanted part to regain useful motion and sensibility must be rigorously assessed before committing the patient to a grueling reconstructive course.
Clinical Pearl: Survival of the replanted part is not the sole metric of success. A viable but insensate, stiff, and painful appendage is a functional liability that impairs the overall use of the extremity.
The following factors must be systematically evaluated:
* Age of the patient
* Severity and mechanism of injury (guillotine vs. crush vs. avulsion)
* Level of amputation and specific part amputated
* Interval between amputation and replantation (warm vs. cold ischemia time)
* Presence of multiple or bilateral amputations
* Segmental injuries to the amputated part (multilevel trauma)
* Patient’s physiological status, including concomitant life-threatening injuries
* Rehabilitation potential (cognitive capacity, compliance, and occupational demands)
* Economic and psychosocial factors
INDICATIONS AND CONTRAINDICATIONS
Because the final decision regarding replantation is a shared responsibility between the patient and the surgeon, absolute indications are rare. However, established guidelines dictate current best practices.
Age Considerations
Replantations have been successfully performed in patients ranging from a few weeks old to octogenarians.
Pediatric Patients:
The young patient poses unique technical challenges, particularly in digital replantations, due to the diminutive size of their vessels. Vessel diameter in children may be as small as 0.5 mm, making it exceedingly difficult to place a microvascular clamp on the distal segment. In such cases, either a volar venous anastomosis or controlled bleeding (via medicinal leeches or systemic heparin) is necessary to manage venous outflow. Postoperative anxiety in children can also precipitate severe vasospasm.
Despite these challenges, children possess profound neuroplasticity and regenerative capabilities. Most authors consider replantation over amputation for almost any part in a child. The success rate of distal fingertip replantations in children is notably higher than in adults.
Elderly Patients:
The upper age limit for replantation is not strictly defined by chronological age, but rather by physiological status. Poor peripheral nerve regeneration and a high propensity for joint stiffness severely limit functional outcomes in the elderly. Replantation above the elbow, through the elbow, or through the proximal forearm yields dismal hand function in older patients. However, preserving the elbow joint in anticipation of a subsequent below-elbow amputation may be indicated to allow for superior prosthetic fitting. Distal injuries (at or beyond the tendinous portion of the forearm) carry a better prognosis for sensory and motor return, making older patients viable candidates for distal replantations.
Severity and Mechanism of Injury
The mechanism of injury directly dictates the zone of vascular trauma and the prognosis for survival and function.
1. Clean, Sharp "Guillotine" Amputations: Offer the best prognosis. The zone of injury is minimal, requiring little bone shortening or vessel debridement.
2. Minimal Local Crush Amputations: Favorable, provided the crushed segments of vessels are adequately resected and bypassed with interpositional vein grafts.
3. Avulsion Amputations: Carry a guarded prognosis. Ring avulsion-degloving injuries feature extensive intimal damage stretching far beyond the visible skin laceration (the "red line" sign). While revascularization is possible, complete degloving often necessitates extensive vein grafting. The functional outlook is highly uncertain. Ring avulsion amputations through the joint are usually best treated by terminal amputation and closure.
4. Contaminated Injuries: Amputations heavily contaminated with soil (especially barnyard injuries) carry an unacceptably high risk of clostridial myonecrosis (gas gangrene) and severe deep infections. These are generally relative contraindications to replantation.
Level of Injury and Part Amputated
Proximal Amputations (Shoulder to Proximal Forearm):
Replantation near the shoulder carries a poor prognosis for hand function due to unpredictable nerve regeneration over long distances, irreversible intrinsic muscle atrophy, and severe joint stiffness. Amputations through the humerus, elbow, and proximal forearm have potential for success primarily in young, healthy patients with clean, sharp injuries. The patient must have the physiological reserve to await prolonged nerve regeneration.
Distal Amputations (Distal Forearm, Wrist, and Hand):
Replantation at the distal forearm, wrist, metacarpals, or digits should be aggressively pursued, as the potential for sensory and motor return is excellent.

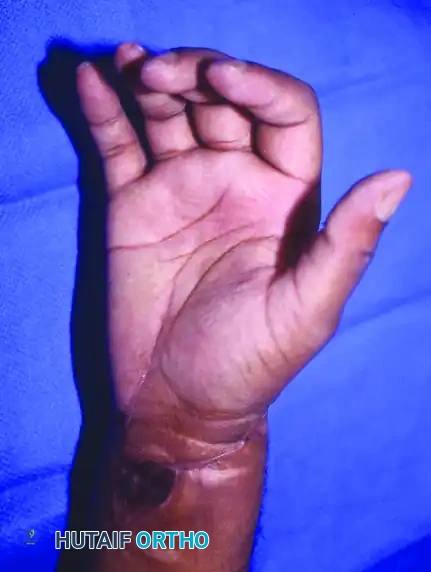
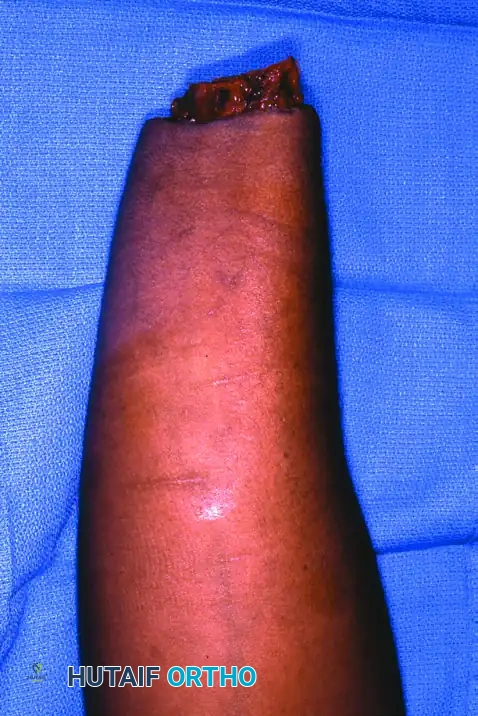
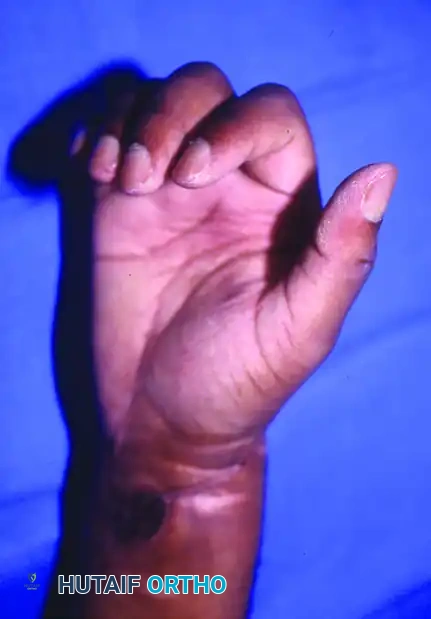
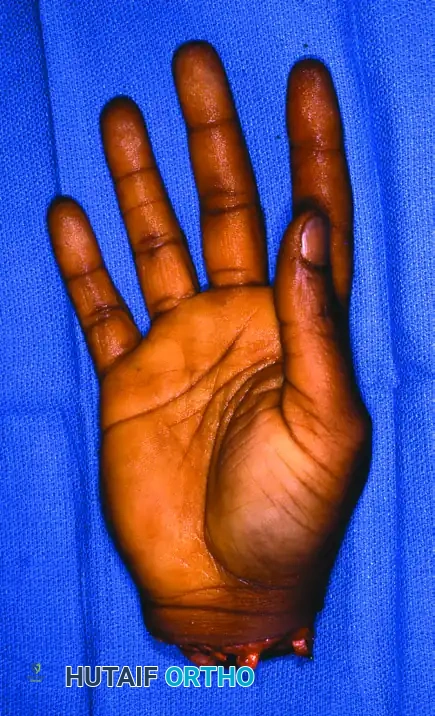
Figure 63-12: Hand replantation sequence demonstrating a sharp amputation at the wrist level, followed by successful revascularization and excellent postoperative flexion and extension.
The Thumb:
Thumb amputations at almost any level are an absolute indication for replantation. The thumb provides 40% to 50% of total hand function. Even in the presence of nerve and tendon avulsion or joint destruction, a revascularized thumb can be functionally restored later with nerve grafts, neurovascular island pedicle transfers, and tendon transfers.
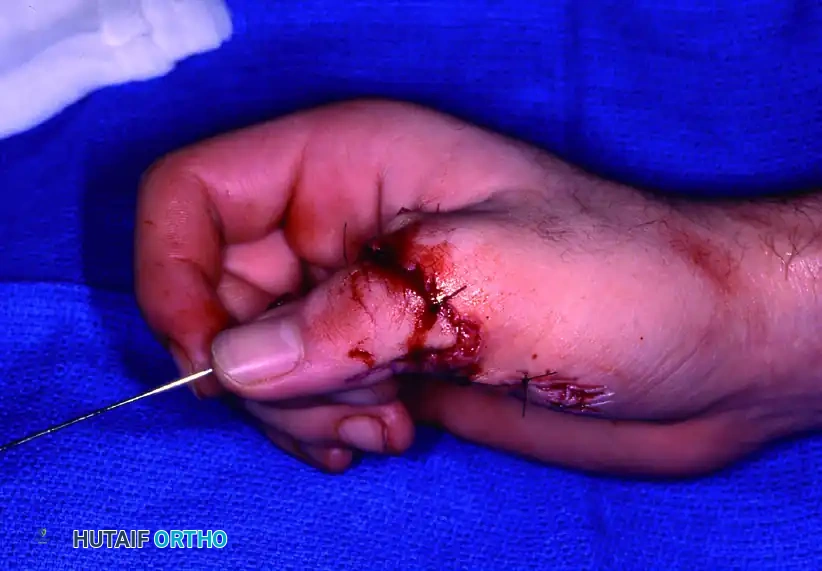
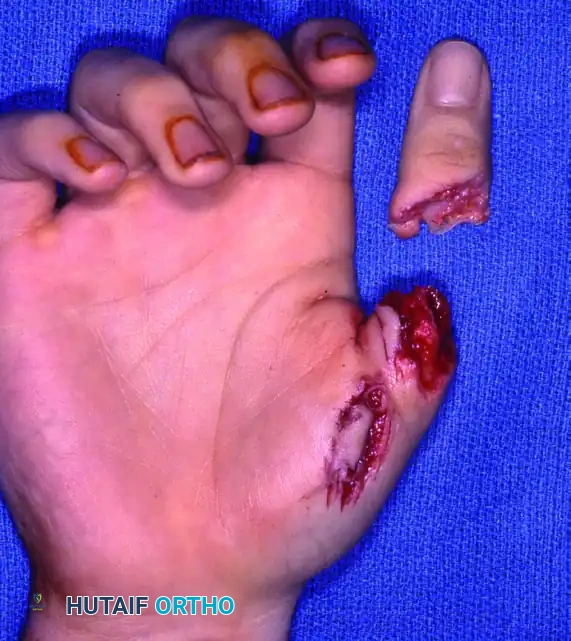
Figure 63-13: Thumb replantation. The thumb's critical role in pinch and grasp makes its salvage paramount, even in complex crush-avulsion scenarios.
Single vs. Multiple Digits:
Replantation of single and multiple digits distal to the flexor digitorum superficialis (FDS) insertion generally yields satisfactory function. However, amputations proximal to the PIP joint often result in a stiff digit that impairs the overall function of the hand by obstructing the adjacent healthy fingers.
While single-digit replantations (other than the thumb) are often discouraged, exceptions exist: musicians, specialized occupations, children, aesthetic concerns, or cases where the remaining attached digits are severely damaged.
In multiple-digit amputations, the goal is to restore a functional tripod pinch and power grip. Replanting at least two digits in the long and ring positions provides the best functional opposition to the thumb.
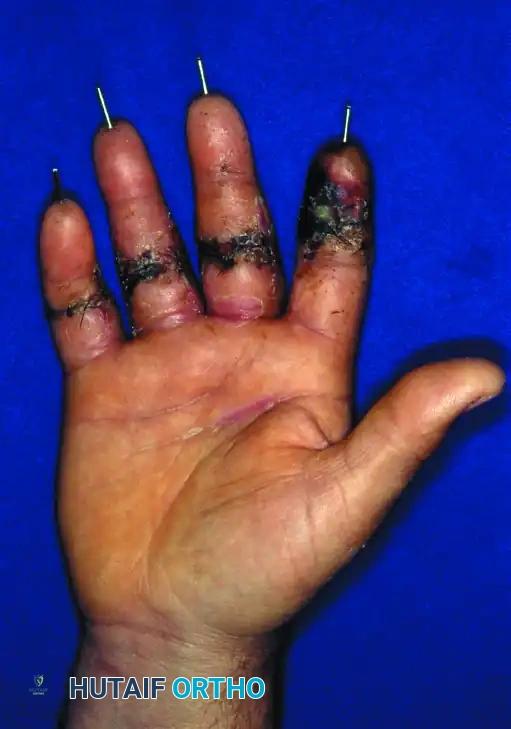
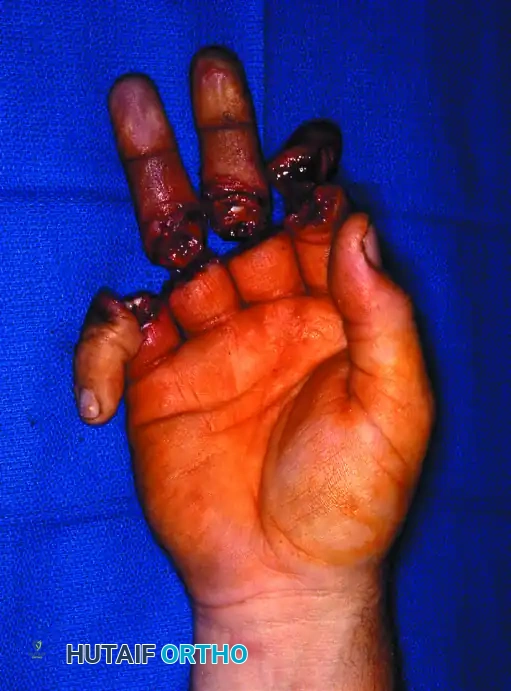
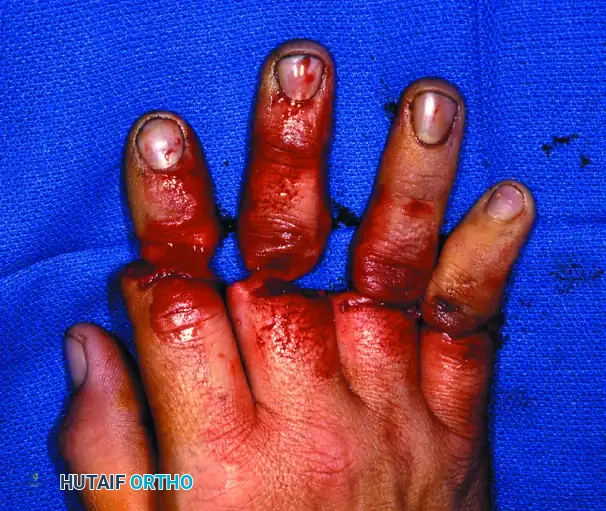
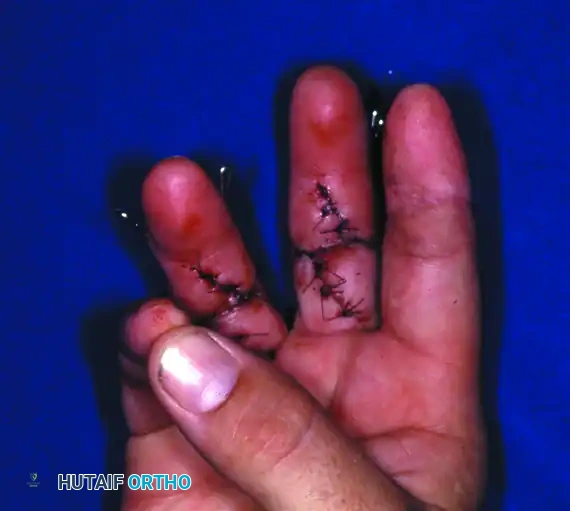
Figure 63-14: Multiple-digit replantation in a 20-year-old man with a saw injury. Amputations distal to the FDS insertion allow for excellent sensory return and useful finger flexion/extension.
Warm Ischemia (Anoxic) Time
Ischemia time is a critical determinant of both part survival and systemic patient safety.
* Muscle-Containing Parts (Proximal to Palm): Irreversible necrotic changes begin in skeletal muscle after 6 hours of warm ischemia (20°C to 25°C). With proper cooling (4°C), this window can be extended to 12 hours. Replanting a proximal part with significant necrotic muscle risks severe ischemia-reperfusion injury, leading to myoglobinuria, metabolic acidosis, hyperkalemia, acute renal failure, and potentially fatal arrhythmias.
* Non-Muscle Parts (Digits): Digits lack skeletal muscle bellies and are highly resistant to ischemia. Allowable warm ischemia time is up to 8 hours. With strict cooling to 4°C, successful digital replantations have been reported after more than 30 hours of ischemia.
Surgical Warning: Never place an amputated part directly on ice or in water. The part should be wrapped in saline-moistened gauze, placed in a sealed watertight plastic bag, and then that bag should be immersed in a slurry of ice and water to maintain a temperature of exactly 4°C without causing frostbite.
Conditions Precluding Replantation
- Concomitant Life-Threatening Injuries: Patients requiring emergent intracranial, thoracic, or intra-abdominal lifesaving surgeries cannot undergo immediate replantation. Digits may be cooled to 4°C and saved for delayed replantation if the patient stabilizes.
- Preexisting Vascular Disease: Patients with severe peripheral vascular disease, diabetes mellitus, rheumatoid arthritis, lupus erythematosus, or significant atherosclerosis are poor candidates. Their vessels often exhibit severe intimal disease under the microscope, precluding successful anastomosis.
- Severe Medical Illness: Uncompensated coronary artery disease, recent myocardial infarction, or severe COPD increases the anesthetic risk of a 12-hour surgery to unacceptable levels.
- Psychiatric Illness: Self-inflicted amputations during acute psychotic episodes carry a high risk of postoperative self-mutilation and non-compliance with rehabilitation. True inadvertent accidents in compensated psychiatric patients may be considered, but require profound clinical judgment.
STEP-BY-STEP SURGICAL APPROACH
The sequence of repair in replantation is designed to establish a stable skeletal foundation, restore tendon continuity, and minimize ischemia time. The standard sequence is: Bone → Extensor Tendons → Flexor Tendons → Arteries → Nerves → Veins → Skin.
1. Bone Shortening and Fixation
Adequate bone shortening is the most critical step to ensure tension-free vascular and neural anastomoses. Attempting to bridge gaps under tension invariably leads to vasospasm and thrombosis.
* Shorten the bone ends symmetrically using an oscillating saw.
* Fixation must be rapid and rigid. Longitudinal Kirschner wires (K-wires), crossed K-wires, or intraosseous wiring are preferred for digits. Plates and screws may be used for forearm and humeral amputations.
2. Tendon Repair
- Extensor Tendons: Repaired using a core suture technique (e.g., figure-of-eight or modified Kessler) with non-absorbable braided suture.
- Flexor Tendons: Repaired using a robust 4-strand or 6-strand core suture to allow for early active mobilization protocols. The flexor sheath is vented if necessary to prevent bowstringing or constriction.
3. Arterial Anastomosis
- The operating microscope is brought into the field.
- Vessels are meticulously debrided back to healthy intima. The "ribbon sign" or "red line" indicates intimal damage requiring further resection.
- If primary anastomosis is impossible without tension, reversed interpositional vein grafts (harvested from the volar forearm or foot) are mandatory.
- Anastomosis is performed using 9-0 or 10-0 nylon on a micro-spatula needle. The back-wall technique or triangulation technique is utilized to prevent catching the posterior wall.
- Release the micro-clamps and confirm pulsatile flow and distal perfusion.
4. Nerve Repair
- Primary epineurial repair is performed using 9-0 or 10-0 nylon.
- If a gap exists, nerve conduits or autologous nerve grafts (e.g., sural nerve or medial antebrachial cutaneous nerve) are utilized. Tension-free coaptation is essential for axonal regeneration.
5. Venous Anastomosis
- Venous outflow is critical. The rule of thumb is to repair two veins for every one artery to prevent venous congestion.
- Veins are highly thin-walled and require meticulous handling.
- If adequate veins cannot be found (especially in distal fingertip amputations), the nail bed may be scored to allow controlled bleeding, supported by the application of medicinal leeches (Hirudo medicinalis).
6. Skin Closure and Fasciotomy
- Skin is closed loosely. Tight closures cause venous compression and subsequent flap failure.
- If swelling is significant, skin grafts or dermal substitutes are used to cover exposed vessels.
- Prophylactic fasciotomies of the hand and forearm are mandatory in proximal replantations with prolonged ischemia times to prevent compartment syndrome.
POSTOPERATIVE PROTOCOLS AND REHABILITATION
The postoperative environment must be strictly controlled to prevent vasospasm and thrombosis.
Environmental and Systemic Management
- Temperature Control: The patient's room must be kept warm (above 75°F / 24°C). The replanted part is kept elevated and exposed under a warming light or Bair Hugger.
- Vasospasm Precautions: Absolute prohibition of smoking, nicotine patches, and caffeine. Visitors must be restricted to reduce patient stress.
- Anticoagulation: Protocols vary by institution but typically include Aspirin (81-325 mg daily). Dextran 40 or systemic Heparin infusions may be used in cases of crush injury or marginal venous outflow.
- Monitoring: Continuous monitoring via surface temperature probes, pulse oximetry, or implantable Doppler probes. A drop in temperature of >2°C or an absolute temperature <30°C demands immediate evaluation for vascular compromise.
Rehabilitation
Rehabilitation begins once vascular stability is assured (typically post-operative day 5-7).
* Early Phase: Controlled passive motion protocols (e.g., modified Kleinert or Duran protocols) are initiated to prevent tendon adhesions while protecting the microvascular anastomoses.
* Late Phase: Active range of motion, sensory re-education, and strengthening. Full functional recovery may take 12 to 18 months, heavily dependent on the rate of nerve regeneration (approximately 1 mm per day).
> Pitfall: Failure to aggressively manage postoperative pain and anxiety can lead to profound sympathetic discharge, resulting in irreversible arterial vasospasm and loss of the replanted part. Adequate regional analgesia (e.g., continuous indwelling brachial plexus catheters) is highly recommended.
You Might Also Like