Hybrid Primary Total Hip: A Solution for Complex Joint Pain
Introduction and Epidemiology
Primary total hip arthroplasty (THA) stands as one of the most consistently successful surgical interventions in orthopedic surgery, delivering profound pain relief and restoration of function for patients afflicted with debilitating hip pathologies. While the spectrum of THA constructs encompasses fully cemented and fully uncemented designs, each with its own established advantages, disadvantages, and specific indications, the hybrid THA paradigm presents a compelling alternative. This construct, defined by the coupling of a cemented femoral stem with an uncemented acetabular component, is specifically tailored for a discerning subset of patients presenting with what can be characterized as complex joint pain, often rooted in compromised femoral bone quality and/or specific anatomical challenges.
The rationale behind the hybrid THA lies in its strategic capitalization on the distinct biomechanical properties and fixation mechanisms of its constituent components. The cemented femoral stem offers immediate, robust mechanical stability, which is particularly advantageous in scenarios of poor bone stock, osteopenia, osteoporosis, or distorted femoral canal anatomy where primary uncemented fixation might be suboptimal or fraught with increased risk of intraoperative fracture or early subsidence. Concurrently, the uncemented acetabular cup relies on biological fixation, promoting long-term osseointegration and adaptability, particularly in younger, more active patients or those with good acetabular bone quality capable of supporting bone ingrowth. This dual-strategy approach aims to mitigate the individual limitations of fully cemented or fully uncemented constructs in specific patient profiles.
Historically, Sir John Charnley's seminal work in the 1960s cemented the supremacy of mechanical fixation, establishing low-friction arthroplasty with cemented components as the benchmark for THA. However, subsequent clinical experience illuminated concerns regarding the long-term integrity of the cement-bone interface, particularly the prevalence of aseptic loosening and osteolysis, especially in younger, more active demographics who exerted higher cyclic loads across the construct. This spurred the profound evolution of uncemented designs, which sought to achieve biological fixation through bone ingrowth into porous-coated surfaces, circumventing the perceived longevity issues of cement. The hybrid construct emerged from this evolutionary synthesis, recognizing that a "one-size-fits-all" approach to fixation might not be optimal and that tailoring the fixation strategy for each bone segment (femur and acetabulum) based on patient-specific factors – including age, bone mineral density, femoral canal morphology, and activity demands – could yield superior long-term outcomes for specific patient cohorts.
Epidemiologically, the global incidence of hip osteoarthritis, post-traumatic arthritis, osteonecrosis, and other degenerative or destructive hip conditions necessitating THA continues its upward trajectory. This trend is predominantly driven by an aging global population, increased life expectancy, and a rising prevalence of comorbidities such as obesity. While contemporary practice has seen a predominant shift towards fully uncemented THA in many regions, particularly in younger and middle-aged patients with good bone quality, hybrid constructs retain a significant, evidence-based role. They are particularly relevant in patient cohorts characterized by osteopenia, osteoporosis, severe proximal femoral deformity (e.g., severe coxa vara/valga, previous fracture malunion), Dorr Type C femurs, or other scenarios where a durable cement mantle can provide superior initial stability, optimized load transfer, and reduced risk of intraoperative complications or early mechanical failure. The phrase "complex joint pain" in this context thus refers not merely to the severity of discomfort, but rather to the underlying anatomical and bone quality challenges that complicate standard implant selection and fixation strategies.
Surgical Anatomy and Biomechanics
A thorough understanding of the regional surgical anatomy and the biomechanical principles governing implant fixation is paramount for successful hybrid THA. This section delineates the critical anatomical considerations and the biomechanical rationale for the hybrid construct.
Femoral Anatomy and Bone Quality Assessment
The proximal femur presents a complex anatomical and biomechanical landscape. Its morphology, particularly the diaphyseal and metaphyseal regions, dictates femoral stem selection and preparation. The Dorr classification of the proximal femur (Types A, B, and C) is a critical radiographic tool for assessing bone quality and canal morphology.
* Dorr Type A: Characterized by a "champagne flute" appearance with thick cortices and a narrow intramedullary canal, typically associated with good bone quality.
* Dorr Type B: Displays intermediate cortical thickness and canal flare.
* Dorr Type C: Features "stovepipe" morphology with thin cortices and a wide, often sclerotic, intramedullary canal, commonly seen in osteoporotic patients.
In osteoporotic or Dorr Type C femurs, the attenuated cortical bone and widened canal provide a suboptimal substrate for press-fit uncemented stem fixation, increasing the risk of intraoperative fracture, subsidence, and aseptic loosening. A well-pressurized cement mantle in this scenario offers immediate, circumferential load transfer to the weaker bone, distributing stresses more evenly and enhancing initial stability. This negates the reliance on biological ingrowth, which is often compromised in poor bone quality. Understanding the anteversion of the femoral neck, typically 10-20 degrees, is also crucial for correct stem orientation.
Acetabular Anatomy and Pelvic Support
The acetabulum, formed by the fusion of the ilium, ischium, and pubis, is the concave articular surface for the femoral head. Its orientation (anteversion and inclination) and the integrity of its bone stock are critical. The anterior and posterior columns of the acetabulum, as described by Judet, provide crucial structural support. For uncemented acetabular components, the integrity and density of the cancellous bone within the acetabular vault are paramount to achieve adequate primary mechanical stability through press-fit and screw fixation (if necessary). Secondary biological fixation through osseointegration relies on viable bone apposition to the porous coating. Deficiencies in acetabular bone stock due to osteolysis, dysplasia, or trauma may necessitate augmentation or alternative fixation strategies, although a well-vascularized host bone bed is always preferred for uncemented fixation. The relationship of the acetabulum to the sciatic nerve, obturator nerve, and external iliac vessels must be meticulously understood to avoid iatrogenic injury.
Soft Tissue Structures and Internervous Planes
Knowledge of the surrounding musculature, neurovascular structures, and internervous planes is essential for safe and effective surgical access. Key structures include:
* Muscles: Gluteus maximus, medius, and minimus; piriformis and other short external rotators; iliopsoas; rectus femoris; adductors.
* Nerves: Sciatic nerve (most commonly injured), femoral nerve, superior gluteal nerve (supplies gluteus medius/minimus and tensor fascia lata), obturator nerve, lateral femoral cutaneous nerve.
* Vessels: Femoral artery and vein, superior and inferior gluteal arteries.
The chosen surgical approach dictates the specific soft tissue dissection and the internervous planes utilized, influencing potential complications and post-operative recovery.
Biomechanics of Hybrid THA Components
Cemented Femoral Stem Biomechanics
The primary advantage of a cemented femoral stem is its immediate mechanical interlocking with the host bone via a polymethylmethacrylate (PMMA) cement mantle. This interdigitation into the cancellous bone provides excellent initial stability, which is particularly beneficial in osteoporotic bone where the modulus of elasticity mismatch between the implant and bone can be detrimental to direct uncemented fixation. The cement acts as a viscoelastic intermediary, distributing stresses more evenly to the bone and reducing micromotion at the bone-cement interface. Key biomechanical considerations include:
* Cement Mantle Thickness and Integrity: A uniform 2-5mm cement mantle is ideal for optimal stress distribution and prevention of fracture.
* Pressurization: Proper cement pressurization during insertion is vital to achieve deep penetration into the cancellous bone interstices, maximizing the interdigitation zone and mechanical strength.
* Load Transfer: Cemented stems achieve load transfer predominantly through the calcar (proximal load transfer) and distally through the stem, minimizing "stress shielding" of the proximal femur observed in some stiff uncemented stems.
* Subsidence: While slight early subsidence can occur, a well-cemented stem exhibits excellent resistance to progressive subsidence, which is a common concern in poorly fixed uncemented stems in osteoporotic bone.
Uncemented Acetabular Cup Biomechanics
Uncemented acetabular components achieve primary stability through mechanical interference (press-fit) with the reamed acetabular bed, often augmented by ancillary screw fixation. Secondary stability is achieved through biological osseointegration into the porous surface coating.
* Primary Stability: Crucial for allowing bone ingrowth to occur without excessive micromotion, which can lead to fibrous tissue formation instead of bone. Press-fit typically involves undersizing the reamed cavity by 1-2mm relative to the cup diameter.
* Bone Ingrowth: Requires viable, vascularized host bone and a porous surface architecture with pore sizes generally ranging from 50-500 µm to facilitate osteoblast migration and bone formation.
* Load Transfer: Uncemented cups transfer load directly to the surrounding acetabular bone, relying on the bone's inherent strength.
* Modularity: The ability to select different bearing surfaces (e.g., ceramic-on-ceramic, ceramic-on-polyethylene, metal-on-polyethylene) allows for customization based on patient activity levels, age, and risk of wear.
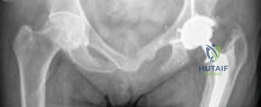
This image depicts a typical hybrid THA construct, showcasing a cemented femoral stem and an uncemented acetabular cup. The distinct fixation mechanisms are visually apparent.
Indications and Contraindications
The judicious selection of a hybrid THA construct requires a meticulous assessment of patient-specific factors, balancing the advantages of both cemented femoral and uncemented acetabular components against potential risks.
Operative Indications for Hybrid THA
Hybrid THA is often indicated in scenarios where there is a clear disparity in bone quality or anatomical suitability between the femur and the acetabulum.
Primary Degenerative and Inflammatory Arthritis
- Severe Osteoarthritis with Compromised Femoral Bone Quality: Patients with advanced primary osteoarthritis who also exhibit osteopenia, osteoporosis, or Dorr Type C femoral bone morphology are prime candidates. The cemented stem provides reliable initial fixation where an uncemented stem would be at high risk of subsidence or fracture.
- Rheumatoid Arthritis and other Inflammatory Arthropathies: These conditions often lead to systemic bone loss and severe osteopenia, making cemented femoral fixation a safer and more predictable option for immediate stability. The acetabular bone, however, may still be suitable for biological ingrowth.
- Post-Traumatic Arthritis: Cases where previous femoral fractures or surgical interventions have left a distorted femoral canal or compromised bone stock, but the acetabulum remains relatively intact.
Avascular Necrosis and Femoral Head Pathology
- Avascular Necrosis (AVN) with Femoral Head Collapse: When AVN has led to significant collapse of the femoral head, necessitating arthroplasty, a hybrid construct can be beneficial, especially if the patient is relatively young but has concomitant femoral bone fragility or a challenging canal.
Specific Femoral Anatomical Challenges
- Dorr Type C Femur: As discussed, this morphology is a strong indication for a cemented femoral stem due to the thin cortices and wide canal, which provide poor purchase for press-fit uncemented stems.
- Proximal Femoral Deformity: Conditions like severe coxa vara or valga, or malunion from previous fractures, can create an irregular femoral canal. Cemented stems can conform to these irregularities more effectively, providing better fill and load transfer than standard uncemented stems.
- Previous Femoral Hardware: Removal of prior plates, screws, or intramedullary nails can leave defects or altered bone density in the femoral canal, which a cemented stem can manage more predictably.
- Need for Immediate Full Weight-Bearing with Compromised Femur: In certain elderly or frail patients, immediate full weight-bearing is crucial for rehabilitation, even if femoral bone quality is poor. A robustly cemented stem allows for this, while the acetabular side, if healthy, benefits from biological ingrowth.
Revision Scenarios
- Femoral Revision with Extensive Bone Loss: In some limited femoral revision cases where bone grafting or impaction grafting is used, a cemented stem can provide the necessary stability. However, fully cemented revision stems or impaction grafting with cement are also alternatives. This can be a niche indication in hybrid context where the acetabulum is revised to uncemented.
Contraindications for Hybrid THA
Absolute Contraindications
- Active Local or Systemic Infection: Any active infection, regardless of the construct, is an absolute contraindication to elective THA due to the high risk of periprosthetic joint infection (PJI).
- Rapidly Progressive Neurological Disease: Conditions that preclude safe ambulation or compliance with post-operative precautions (e.g., severe Parkinson's disease, uncontrolled stroke with severe hemiparesis).
- Inability to Comply with Post-Operative Protocols: Patients with severe cognitive impairment or lack of social support may struggle with rehabilitation requirements.
- Malignancy at Surgical Site: Uncontrolled primary or metastatic disease involving the hip joint.
Relative Contraindications
- Severe Acetabular Bone Loss or Defects: If the acetabular bone stock is severely deficient (e.g., Paprosky Type III defects, extensive osteolysis) to the extent that biological ingrowth is unlikely, an uncemented acetabular component may be contraindicated. In such cases, a cemented cup, acetabular cage, or custom component might be necessary.
- Severe Peripheral Vascular Disease: Compromised vascularity can impair wound healing and bone ingrowth.
- Compromised Skin or Soft Tissue Integrity: Local skin lesions, severe burns, or previous radiation therapy in the hip region increase the risk of wound complications and infection.
- Allergy to Implant Materials: Rare, but patients with known allergies to nickel, chromium, or cobalt may require specific implant choices.
Table 1: Operative vs. Non-Operative Indications for Hybrid THA
| Category | Operative Indications for Hybrid THA | Non-Operative Indications / Contraindications for Hybrid THA |
|---|---|---|
| Primary Disease | Severe OA with Osteoporosis/Osteopenia | Mild to Moderate OA (non-surgical candidates) |
| Rheumatoid Arthritis (with femoral fragility) | ||
| Avascular Necrosis (femoral head collapse with poor femur) | ||
| Post-traumatic Arthritis (with distorted femoral canal) | ||
| Femoral Anatomy | Dorr Type C Femur (thin cortices, wide canal) | Dorr Type A Femur (typically suited for uncemented stem) |
| Severe Proximal Femoral Deformity | ||
| Previous Femoral Hardware or Bone Defects | ||
| Acetabular Bone | Adequate Acetabular Bone Quality for Press-Fit/Ingrowth | Severe Acetabular Bone Loss (Paprosky Type III) |
| Patient Factors | Elderly, Frail patients needing immediate weight-bearing | Active Infection (local/systemic) |
| High-demand, younger patient (acetabular side only) | Rapidly Progressive Neurological Disease | |
| Inability to Comply with Rehab | ||
| Uncontrolled Medical Comorbidities |
Pre Operative Planning and Patient Positioning
Thorough preoperative planning is fundamental to achieving a successful outcome in hybrid THA, minimizing complications, and optimizing component placement, leg length equality, and hip biomechanics.
Patient Assessment and Optimization
A comprehensive medical and surgical history, physical examination, and review of comorbidities are essential. Optimization of medical conditions, such as diabetes control (HbA1c < 7.0%), management of anemia, and smoking cessation, is critical to reduce perioperative risks. Nutritional status assessment is important, especially in frail or cachectic patients. Patients should be counseled regarding expectations, rehabilitation, and potential risks. Preoperative dental evaluation is recommended to address potential sources of infection.
Radiographic Planning and Templating
High-quality imaging is indispensable. Standard views include:
* Anteroposterior (AP) Pelvis with both hips: Essential for assessing hip center of rotation, leg length discrepancy, femoral head migration, osteophyte formation, and overall pelvic obliquity. This view allows comparison of both hips and identifies any pelvic tilt.
* Frog-leg Lateral View: Provides an additional perspective of the proximal femur and hip joint.
* Cross-table Lateral View of the Affected Hip: Crucial for assessing femoral anteversion and posterior osteophyte burden.
Digital templating is the gold standard for preoperative planning. It allows for:
* Component Sizing: Accurate estimation of femoral stem and acetabular cup sizes.
* Offset Restoration: Planning to restore the natural femoral and global hip offset, which is crucial for abductor muscle tension and hip stability.
* Leg Length Assessment: Precise planning to correct or prevent leg length discrepancy.
* Femoral Canal Morphology: Detailed assessment of the femoral canal (Dorr classification, cortical thickness) to guide cemented stem selection (e.g., straight, bowed, collared, collarless). The stem should provide adequate fill in the diaphysis and a robust cement mantle.
* Acetabular Bone Stock: Evaluation of acetabular osteophytes, bone defects, and the integrity of the anterior and posterior columns.
* Trialing: Digital manipulation of template components to simulate intraoperative sizing and placement.
For complex cases involving significant deformity, previous surgery, or profound bone loss, Computed Tomography (CT) scans with 3D reconstructions may be necessary to better define anatomy, assess bone stock, and aid in custom implant design if required. Magnetic Resonance Imaging (MRI) can be useful for evaluating soft tissue pathology or early stages of AVN.

Pre-operative templating showing planned component sizes and positions for a THA.
Patient Positioning
The choice of patient positioning depends on the selected surgical approach. Meticulous positioning is critical to provide optimal surgical exposure, facilitate accurate component placement, and prevent iatrogenic injury.
Lateral Decubitus Position (for Posterior/Posterolateral Approaches)
- Setup: Patient is positioned on their side with the affected hip superior. Bean bag or specialized hip positioners are used to stabilize the torso and pelvis.
- Support: Anterior and posterior pelvic support (e.g., sacral and pubic posts) prevent rotation and ensure the pelvis remains perpendicular to the floor, crucial for accurate acetabular orientation.
- Lower Extremity Management: The unaffected leg is flexed and abducted, often placed in a well-padded trough or held by an assistant. The affected leg is prepared free, allowing full range of motion for intraoperative trials.
- Nerve Protection: Axillary roll, padding of dependent bony prominences (fibula head for common peroneal nerve, ulnar nerve at elbow) are essential.
Supine Position (for Direct Anterior or Anterolateral Approaches)
- Setup: Patient lies flat on their back. A fracture table may be used for direct anterior approach to facilitate leg manipulation and traction, or the patient can be positioned on a standard operating table with a bump under the ipsilateral hip.
- Support: Pelvic stabilizers are used to prevent rotation.
- Lower Extremity Management: Both legs are prepared free. For direct anterior approach, the leg can be manipulated off the side of the table for femoral exposure.
- Nerve Protection: Padding under the sacrum, careful attention to the lateral femoral cutaneous nerve with direct anterior approaches.
Regardless of the position, ensuring unrestricted access to the surgical field, maintaining sterility, and preventing neurovascular injury are paramount.
Detailed Surgical Approach and Technique
The execution of a hybrid THA demands meticulous surgical technique, with precise attention to bone preparation, cementation, and uncemented component impaction. While the specific approach may vary based on surgeon preference and patient anatomy, the fundamental principles of component fixation remain consistent. This section outlines a general step-by-step technique, emphasizing aspects critical to the hybrid construct.
Approach Selection
The choice of surgical approach influences exposure, potential for soft tissue damage, and post-operative recovery.
* Posterior/Posterolateral Approach: Widely used, offers excellent exposure of both the acetabulum and femur. It involves detaching the short external rotators and posterior capsule, which are typically repaired.
* Anterolateral Approach: Involves splitting the gluteus medius and minimus, potentially affecting abductor function. Offers good stability.
* Direct Anterior Approach: Muscle-sparing, allows fluoroscopic guidance, but has a steep learning curve and can be challenging for femoral exposure, especially in larger patients or those with deformities.
For illustrative purposes, we will describe key steps generally applicable, with emphasis on component-specific techniques.
Incision and Dissection
- Skin Incision: A curvilinear incision centered over the greater trochanter for posterior/posterolateral approaches, or an anterior incision parallel to the anterior superior iliac spine for direct anterior approach.
- Fascia Lata: Incision of the fascia lata in line with the skin incision.
- Muscle and Capsule Exposure:
- Posterior: Detach gluteus maximus fibers, expose the short external rotators (piriformis, gemelli, obturator internus, quadratus femoris) which are then released from their insertions on the greater trochanter, often with a cuff of bone, and tagged for later repair. The posterior capsule is then incised.
- Anterior: Interval between tensor fascia lata and sartorius (direct anterior), or between tensor fascia lata and gluteus medius (anterolateral).
Femoral Neck Osteotomy and Hip Dislocation
- Dislocation: The hip is dislocated, typically with controlled internal rotation and adduction for a posterior approach, or external rotation for an anterior approach.
- Femoral Neck Osteotomy: Using the templated level, the femoral neck is osteotomized. Careful preservation of the capsule and soft tissues for subsequent repair is important. The excised femoral head is then removed from the field.

Image demonstrating the femoral head osteotomy during THA.
Acetabular Preparation and Uncemented Cup Insertion
- Exposure: The acetabulum is cleared of remaining soft tissue, osteophytes, and the labrum to expose the true bony rim.
- Reaming: Progressive reaming of the acetabulum is performed using hemispherical reamers, starting with a size smaller than the planned cup and increasing incrementally. Reaming continues until healthy, bleeding subchondral bone is exposed concentrically. The reaming typically undersizes the final cup by 1-2mm to achieve a robust press-fit. Correct inclination (40-45 degrees) and anteversion (15-20 degrees) are critical for stability.
- Hole Drilling (if indicated): For added primary stability in cases of poor bone quality or large defects, screw holes may be drilled in the superior-posterior quadrant, avoiding the "safe zone" (anterior-inferior quadrant) to minimize neurovascular injury.
- Cup Impaction: The uncemented acetabular cup is then firmly impacted into the reamed acetabular bed, ensuring complete seating and achieving solid primary mechanical stability. Auditory and tactile feedback (a solid thud) confirms good impaction.
- Screw Insertion (if indicated): If screws are used, they are inserted to augment primary fixation.
- Liner Insertion: The polyethylene or ceramic liner is then impacted into the acetabular shell. Care is taken to ensure correct orientation if an asymmetric liner is used.
Image illustrating the reaming of the acetabulum to prepare for cup insertion.

Image showing the insertion of an uncemented acetabular cup into the reamed acetabulum.
Femoral Preparation and Cemented Stem Insertion
- Canal Preparation: The femoral canal is prepared sequentially.
- Broaching/Reaming: The canal is initially opened with a box osteotome or small reamer. Progressive broaches or reamers are then used to create a cavity that corresponds to the planned cemented stem, ensuring adequate cancellous bone removal to allow for a uniform cement mantle.
- Canal Plug: An intramedullary cement restrictor (plug) is inserted distally to the planned stem tip position to ensure retrograde cement pressurization.
- Pulsatile Lavage: Thorough cleaning of the femoral canal with pulsatile lavage is critical to remove bone marrow, fat, and debris, which can compromise cement penetration and bonding.
- Drying: The canal is meticulously dried with sponges or compressed air.
- Cement Mixing and Insertion:
- Mixing: Bone cement (PMMA) is mixed according to manufacturer instructions. Vacuum mixing is preferred to reduce porosity and increase mechanical strength.
- Insertion: Once the cement reaches a doughy consistency, it is delivered into the femoral canal retrogradely using a cement gun, starting from the distal plug and filling proximally. This technique ensures optimal pressurization and interdigitation.
- Stem Insertion: The selected cemented femoral stem is then carefully inserted into the cement-filled canal, ensuring correct alignment, anteversion, and depth based on templating. The stem should be inserted smoothly to avoid generating high pressures that could cause cement extravasation or reduce effective pressurization. Excess cement extruded around the stem is removed.
- Cement Curing: The stem is held in place until the cement fully polymerizes and hardens (exothermic reaction). This usually takes several minutes. Final removal of any remaining extruded cement.
Image depicting the preparation of the femoral canal for a cemented stem, including the insertion of the cement restrictor.
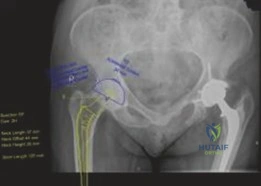
Image illustrating the retrograde delivery of bone cement into the femoral canal via a cement gun.
Image showing the insertion of a cemented femoral stem into the prepared canal, with excess cement being removed.
Trial Reduction and Final Reduction
- Trial Components: Trial femoral head and stem are assembled, and a trial reduction is performed.
- Assessment: Critical assessment of:
- Stability: Range of motion and stability in various positions (flexion, extension, internal/external rotation, abduction/adduction).
- Leg Length: Comparison with the contralateral limb and preoperative measurements.
- Offset: Restoration of femoral and global offset to optimize abductor mechanics and prevent impingement.
- Definitive Components: Once optimal parameters are achieved with trials, the definitive femoral head (ceramic or metal) is impacted onto the femoral trunnion.
- Final Reduction: The definitive components are carefully reduced.
Wound Closure
- Capsular/Rotator Repair: The short external rotators and posterior capsule (if detached) are meticulously repaired to enhance hip stability, particularly important for posterior approaches.
- Layered Closure: The wound is closed in layers: deep fascia, subcutaneous tissue, and skin. Drains may be used based on surgeon preference and intraoperative bleeding.
Complications and Management
Despite the high success rates of THA, complications can arise, some of which are unique to the hybrid construct or have different incidences. Proactive identification and appropriate management are paramount.
Intraoperative Complications
- Periprosthetic Fractures: Can occur during reaming, broaching, or stem insertion (femoral) or during reaming or cup impaction (acetabular).
- Management: Minor fractures may be managed non-operatively, or with cerclage wires or cables. Larger fractures may require plate fixation or revision to a different stem design.
- Neurovascular Injury: Sciatic nerve palsy (most common), femoral nerve palsy, or damage to major vessels.
- Management: Immediate recognition, nerve exploration if indicated, conservative management initially. Vascular injuries require immediate repair.
- Cement Extravasation: Cement can extravasate into the soft tissues, potentially compressing nerves or vessels.
- Management: Careful removal of excess cement before hardening. If nerve compression is suspected postoperatively, exploration may be warranted.
- Acetabular Perforation: Reaming or screw placement can perforate the acetabulum into the pelvis.
- Management: Minor perforations may be observed. Larger ones may require bone grafting or special fixation.
Early Postoperative Complications (Within 3 Months)
- Hip Dislocation: Incidence varies by approach (posterior > anterior). Often related to malposition of components, inadequate soft tissue repair, or patient non-compliance with precautions.
- Management: Closed reduction is usually attempted first. Recurrent dislocations may require surgical revision (component re-orientation, modular head exchange, constrained liner, or soft tissue repair).
- Periprosthetic Joint Infection (PJI): A devastating complication. Can be acute (<3 weeks) or subacute (3 weeks to 3 months).
- Management: Acute infections may be managed with irrigation and debridement (I&D) and component retention with antibiotic therapy. Subacute and chronic infections typically require two-stage revision arthroplasty.
- Deep Venous Thrombosis (DVT) and Pulmonary Embolism (PE): Thromboembolic events remain a significant risk.
- Management: Prophylactic anticoagulation is standard. Symptomatic DVT/PE require therapeutic anticoagulation.
- Leg Length Discrepancy (LLD): Can lead to gait abnormalities and back pain.
- Management: Small discrepancies are often tolerated. Larger or symptomatic LLD may require shoe lifts; rarely, revision surgery for severe cases.
- Nerve Palsy: Often due to stretch injury during dislocation or limb lengthening.
- Management: Conservative with observation and physical therapy. Most resolve spontaneously.
- Hematoma: Collection of blood in the surgical site.
- Management: Small hematomas often resolve. Large or symptomatic hematomas may require drainage.
Late Postoperative Complications (>3 Months)
- Aseptic Loosening: The most common long-term failure mechanism.
- Acetabular: Failure of biological ingrowth or subsequent osteolysis around the uncemented cup.
- Femoral: Cement-bone interface failure, stem fracture, or cement mantle fracture.
- Management: Symptomatic loosening requires revision arthroplasty, often of the specific failing component.
- Periprosthetic Fracture (Type B2/B3/C): Occur around a well-fixed or loose stem.
- Management: Requires surgical stabilization (plating, cabling, revision to longer stem) and bone grafting.
- Osteolysis: Granulomatous inflammatory reaction to wear debris (polyethylene, metal, ceramic particles) causing bone resorption.
- Management: Regular radiographic surveillance. Small, stable lesions may be observed. Progressive lesions or those compromising implant fixation require debridement, bone grafting, and potentially component revision.
- Implant Wear: Degradation of bearing surfaces (e.g., polyethylene liner wear).
- Management: Revision of the worn component, often just the liner exchange.
- Heterotopic Ossification (HO): Formation of mature lamellar bone in non-osseous tissues.
- Management: Prophylaxis (NSAIDs, radiation therapy) in high-risk patients. Symptomatic HO may require surgical excision after maturation.
- Chronic Pain: Can be multifactorial (component malposition, infection, loosening, nerve entrapment, muscle imbalance).
- Management: Thorough investigation to identify etiology. May involve conservative measures, injections, or revision surgery.
Table 2: Common Complications of Hybrid THA
| Complication | Incidence (approximate range) | Salvage Strategies |
|---|---|---|
| Hip Dislocation | 0.5-5% | Closed reduction, external bracing, component revision, constrained liner |
| Periprosthetic Infection (PJI) | 0.5-2% | I&D with component retention (acute), two-stage revision (chronic) |
| Aseptic Loosening (Femoral) | 0.5-3% (10-year) | Femoral revision with new cemented or uncemented stem, bone grafting |
| Aseptic Loosening (Acetabular) | 0.5-2% (10-year) | Acetabular revision with new uncemented/cemented cup, bone grafting |
| Periprosthetic Fracture | 0.5-2% | ORIF with cables/plates, revision to longer stem, bone grafting |
| Deep Venous Thrombosis (DVT) | 1-5% (symptomatic) | Anticoagulation (prophylactic and therapeutic) |
| Pulmonary Embolism (PE) | <1% | Anticoagulation, IVC filter (rarely) |
| Leg Length Discrepancy | 1-10% (symptomatic) | Shoe lift, physical therapy, rarely revision |
| Nerve Palsy | 0.5-2% | Observation, physical therapy, nerve exploration (rarely) |
| Heterotopic Ossification (HO) | 5-20% (radiographic) | Prophylaxis (NSAIDs, XRT), surgical excision (symptomatic) |
Post Operative Rehabilitation Protocols
Post-operative rehabilitation is crucial for optimizing functional recovery, restoring strength, and ensuring the long-term success of a hybrid THA. Protocols generally emphasize early mobilization, pain management, and progressive strengthening while respecting hip precautions tailored to the surgical approach. Given the robust immediate fixation of the cemented femoral stem, accelerated weight-bearing protocols are often permissible.
Immediate Postoperative Period (Days 0-7)
- Pain Management: A multimodal analgesic approach is initiated, often including regional nerve blocks (e.g., adductor canal block), NSAIDs (if no contraindications), acetaminophen, and opioid sparing agents. Adequate pain control is essential for early mobilization.
- Weight-Bearing Status: For hybrid THA, the cemented femoral stem typically allows for immediate full weight-bearing as tolerated from post-operative day 0 or 1, assuming stable fixation intraoperatively. This contrasts with some uncemented stems where protected weight-bearing might be employed initially.
- Mobilization: Physical therapy begins immediately.
- Bed Mobility: Instruct patient in safe transfers in and out of bed.
- Gait Training: Ambulation with an assistive device (walker, crutches) is initiated. Focus on proper gait mechanics, maintaining hip precautions.
- Range of Motion (ROM): Gentle active and passive ROM exercises within prescribed limits.
- Muscle Activation: Isometric gluteal sets, quadriceps sets, ankle pumps to prevent DVT.
- Hip Precautions: Dependent on the surgical approach:
- Posterior/Posterolateral: Avoid hip flexion beyond 90 degrees, internal rotation, and adduction past midline.
- Anterolateral/Direct Anterior: Often have fewer or no specific rotational precautions, but excessive extension/external rotation may be restricted initially.
- DVT Prophylaxis: Continued pharmacological and mechanical prophylaxis (TED hose, SCDs).
- Wound Care: Daily inspection of the surgical site.
Early Rehabilitation Phase (Weeks 1-6)
- Progression of Ambulation: Gradual reduction in assistive device use as strength and balance improve. Goal is often cane or no device by 4-6 weeks for uncomplicated cases.
- Strengthening: Introduction of progressive resistive exercises for hip abductors, adductors, flexors, extensors, and knee musculature. Examples include:
- Light resistance band exercises.
- Gentle weight-bearing exercises (mini-squats, heel raises).
- Therapeutic exercises for core stability.
- Functional Mobility: Practice activities of daily living (ADLs) such as dressing, bathing, stair climbing, and getting in/out of a car, always adhering to precautions.
- Balance Training: Begin with static balance exercises and progress to dynamic balance activities.
- Pain and Swelling Management: Continue monitoring and managing pain; use cryotherapy for swelling.
Intermediate Rehabilitation Phase (Weeks 6-12)
- Advanced Strengthening: Increase intensity and complexity of strengthening exercises.
- Theraband exercises with increased resistance.
- Light weights for hip and knee musculature.
- Progression to single-leg stance exercises.
- Gait Refinement: Focus on normalizing gait pattern, improving stride length, and minimizing compensatory movements.
- Activity Progression: Introduction of low-impact activities such as swimming, cycling (stationary), and elliptical trainer. Avoid high-impact activities.
- Proprioception and Balance: Advanced balance exercises, uneven surface ambulation.
- Discontinuation of Precautions: Depending on surgeon preference, stability of the hip, and patient progress, some hip precautions may be discontinued after 6-12 weeks, particularly if the posterior capsule and rotators were meticulously repaired.
Long-Term Rehabilitation and Return to Activity (Beyond 12 Weeks)
- Maintenance Program: Patients are encouraged to continue a home exercise program focusing on strength, flexibility, and cardiovascular fitness.
- Return to Sports/Activities:
- Low-Impact: Walking, golf (with precautions), cycling, swimming, doubles tennis are generally safe.
- Moderate-Impact (Caution): Skiing, singles tennis, hiking.
- High-Impact (Generally Discouraged): Running, jumping sports, contact sports. These activities impose excessive forces that can accelerate implant wear and increase the risk of loosening or periprosthetic fracture.
- Patient Education: Emphasis on protecting the joint, avoiding falls, maintaining a healthy weight, and adherence to follow-up schedules. Patients should be educated on the signs of potential complications (infection, loosening) and when to seek medical attention.
Summary of Key Literature and Guidelines
The evolution of THA has been marked by continuous refinement, and the hybrid construct represents a mature strategy backed by decades of clinical experience and robust evidence. Key literature and established guidelines inform its appropriate application.
Historical Context and Evolution
The foundational work of Sir John Charnley established the principles of low-friction arthroplasty with cemented fixation. His long-term results, demonstrating excellent survivorship of cemented stems, particularly the Charnley Elite stem, set the benchmark for joint replacement. However, concerns regarding cement-bone interface failure in younger, more active patients propelled the development of uncemented technology, notably pioneered by groups such as the Harris Hip Team and the DePuy/Porous-Coated Anatomic (PCA) design. The hybrid concept arose from the recognition that different bone stocks and physiological demands might necessitate distinct fixation strategies for the acetabulum and femur. Early hybrid designs, combining a cemented femoral stem with an uncemented acetabular component, showed promising results, particularly in specific patient demographics.
Clinical Outcomes and Survivorship
Numerous long-term studies have evaluated the survivorship and functional outcomes of hybrid THA, often comparing them to fully cemented or fully uncemented constructs.
* Cemented Femoral Stems: Meta-analyses and national joint registry data (e.g., National Joint Registry for England, Wales, Northern Ireland, and the Isle of Man; Australian Orthopaedic Association National Joint Replacement Registry) consistently demonstrate excellent long-term survivorship for well-fixed, modern cemented femoral stems in appropriate patient populations, often exceeding 90-95% at 10-15 years. They are particularly favored in older patients and those with compromised femoral bone quality (Dorr Type C).
* Uncemented Acetabular Cups: Modern uncemented acetabular components also exhibit high survivorship rates, often comparable to cemented cups, relying on successful biological ingrowth. Long-term studies show survivorship exceeding 90% at 10-15 years, with the primary concern being osteolysis from polyethylene wear debris, though this has been mitigated by advanced bearing surfaces (highly cross-linked polyethylene, ceramics).
Studies specifically on hybrid THA have shown:
* Comparable Overall Survivorship: Hybrid THA often demonstrates overall survivorship rates comparable to fully cemented or fully uncemented THA in carefully selected patient groups.
* Reduced Femoral Loosening in Specific Cohorts: For patients with significant femoral osteopenia or Dorr Type C femurs, cemented femoral stems in a hybrid construct have been shown to have lower rates of aseptic loosening compared to uncemented stems in similar bone, highlighting the benefit of the cement mantle in weak bone.
* Advantages in Revision: The ability to selectively revise a single component, if one fails while the other remains well-fixed, can be an advantage. For instance, if the acetabular cup loosens but the cemented stem remains stable, only the cup needs revision.
Current Guidelines and Consensus
While no single global guideline dictates universal implant choices, various orthopedic societies and expert panels offer recommendations that support the role of hybrid THA:
* Patient-Specific Approach: A consensus exists for a patient-specific approach to implant selection, considering age, bone quality, activity level, and comorbidities.
* Elderly and Osteoporotic Patients: For elderly patients or those with poor femoral bone quality (osteopenia/osteoporosis, Dorr Type C), cemented femoral stems are often recommended due to their proven long-term durability and immediate stability. The hybrid approach allows for the benefits of uncemented acetabular fixation in such patients if their acetabular bone is adequate.
* Younger Patients: While fully uncemented THA is frequently preferred in younger, active patients with good bone stock, the hybrid option might be considered if femoral anatomy presents specific challenges that would compromise uncemented femoral fixation, while still leveraging the biological ingrowth of an uncemented acetabulum.
* Bearing Surfaces: Guidelines emphasize the selection of appropriate bearing surfaces (e.g., ceramic-on-polyethylene or ceramic-on-ceramic) for durability and reduced wear rates, irrespective of the fixation strategy.
Future Directions
Research and development continue to enhance THA outcomes:
* Advanced Materials: Development of new porous coatings, bioactive surfaces, and improved polyethylene formulations for reduced wear and enhanced osseointegration.
* Surgical Navigation and Robotics: Increasing adoption of computer navigation and robotic assistance for precise component positioning and alignment, potentially reducing variability and improving long-term survivorship.
* Custom Implants: 3D printing and custom implant technologies for highly complex anatomies or revision scenarios.
* Perioperative Optimization: Enhanced recovery after surgery (ERAS) protocols, multimodal pain management, and prehabilitation continue to improve patient experience and outcomes.
In conclusion, hybrid primary total hip arthroplasty remains a valuable and evidence-based solution for complex joint pain, particularly in patients with compromised femoral bone quality where the robust immediate fixation of a cemented femoral stem offers distinct advantages, while leveraging the biological benefits of an uncemented acetabular component. Its continued judicious application, guided by meticulous patient selection and refined surgical technique, ensures optimal long-term outcomes.
Clinical & Radiographic Imaging