Comprehensive Introduction and Patho-Epidemiology
The evolution of total hip arthroplasty (THA) represents one of the most successful interventions in modern medicine, fundamentally altering the trajectory of debilitating hip pathology. While Sir John Charnley’s pioneering work with polymethylmethacrylate (PMMA) bone cement established the foundation of modern hip arthroplasty, the paradigm has progressively shifted toward uncemented, biologically fixed implants. This transition was driven by the long-term challenges associated with cemented stems, particularly in younger, higher-demand patients who exhibited unacceptable rates of aseptic loosening secondary to cement mantle fatigue and osteolysis. Uncemented THA relies on achieving an initial mechanical press-fit, followed by secondary biologic fixation through osseointegration—either via bone ingrowth into porous surfaces or bone ongrowth onto roughened topographies.
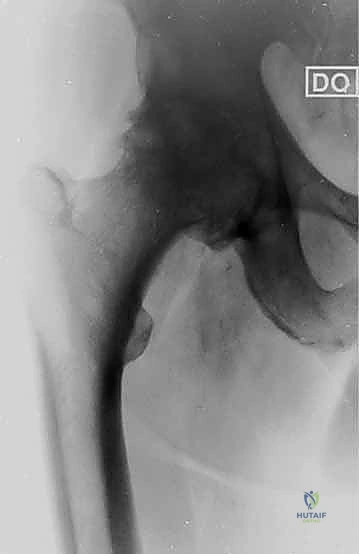
Understanding the patho-epidemiology of the conditions necessitating uncemented THA is critical for appropriate patient selection and surgical planning. Primary osteoarthritis remains the most prevalent indication, characterized by progressive articular cartilage degradation, subchondral sclerosis, osteophyte formation, and eventual joint space obliteration. The etiology is multifactorial, encompassing genetic predisposition, mechanical overload, and subtle morphological abnormalities such as femoroacetabular impingement (FAI) or mild developmental dysplasia of the hip (DDH). Inflammatory arthropathies, such as rheumatoid arthritis and ankylosing spondylitis, present unique challenges, often featuring osteopenic bone, protrusio acetabuli, and altered soft-tissue compliance, which can complicate the initial press-fit required for uncemented components.
Furthermore, the rising incidence of secondary osteoarthritis due to osteonecrosis (avascular necrosis) of the femoral head, particularly in patients with a history of corticosteroid use, alcohol abuse, or trauma, necessitates a robust, durable arthroplasty solution. These patients are typically younger and demand a construct capable of withstanding decades of cyclic loading. Uncemented THA, utilizing highly cross-linked polyethylene or ceramic-on-ceramic bearing surfaces, offers a biologically sound and mechanically durable reconstruction. The success of this procedure, however, is not merely a function of advanced implant metallurgy and tribology; it is intrinsically dependent on the surgeon’s mastery of three-dimensional anatomy, meticulous soft-tissue handling, and precise execution of osseous preparation to optimize the biomechanical environment for long-term survivorship.

Detailed Surgical Anatomy and Biomechanics
Osseous and Articular Anatomy
A profound comprehension of the complex, three-dimensional anatomy of the pelvis and proximal femur is non-negotiable for the arthroplasty surgeon. The acetabulum is a hemispherical cavity formed by the confluence of the ilium, ischium, and pubis, uniting at the triradiate cartilage. During surgical exposure, the surgeon must visualize the entire periphery of the acetabulum, including the robust superior dome, the anterior and posterior walls, and the medial wall. The radiographic "teardrop"—a U-shaped density representing the medial aspect of the acetabular fossa and the lateral aspect of the obturator canal—serves as the definitive landmark for establishing the inferior and medial boundaries of acetabular reaming. Failure to accurately identify and respect the teardrop can result in superiorly or laterally malpositioned components, or catastrophic medial wall blowouts.
The proximal femur is equally complex, featuring a distinct diaphyseal-metaphyseal mismatch that dictates the selection of the femoral implant design. The femoral neck projects anteromedially from the intertrochanteric line, with a native anteversion typically ranging from 10 to 15 degrees and a neck-shaft angle averaging 130 degrees. The greater trochanter serves as the critical insertion site for the hip abductors (gluteus medius and minimus), while the lesser trochanter is the attachment point for the iliopsoas. When preparing the femur for an uncemented stem, the surgeon must appreciate the dense cortical bone of the calcar femorale medially, which provides essential support for the implant, and the variable geometry of the femoral canal (e.g., Dorr types A, B, and C), which influences the choice between proximally coated, fully coated, or modular stem designs to achieve optimal cortical engagement.
Neurovascular Topography and Risk Zones
Navigating the surgical field requires a heightened awareness of the surrounding neurovascular structures to prevent devastating iatrogenic injuries. In the direct lateral approach, the superior gluteal nerve is of paramount concern. This nerve exits the pelvis through the greater sciatic notch, superior to the piriformis, and travels anteriorly between the gluteus medius and minimus, supplying both muscles and the tensor fasciae latae. The main trunk is located approximately 3 to 5 centimeters proximal to the tip of the greater trochanter. Extending the gluteus medius split proximally beyond this safe zone risks denervating the anterior portion of the abductor complex, leading to a persistent, debilitating Trendelenburg gait.
Other critical neurovascular entities include the lateral femoral cutaneous nerve, which courses variably over the anterior superior iliac spine and can be compromised during superficial dissection, resulting in meralgia paresthetica. Medially, the obturator nerve and vessels are vulnerable if retractors are placed too aggressively over the transverse acetabular ligament or if reaming breaches the quadrilateral plate. Posteriorly, the sciatic nerve is intimately related to the posterior column and the short external rotators. While less directly exposed in a lateral approach compared to a posterior approach, the sciatic nerve remains at risk from over-lengthening of the limb, excessive posterior retractor placement, or extrusion of bone debris or cement (in hybrid cases) into the posterior soft tissues. Anteriorly, the femoral nerve and artery are separated from the joint by the iliopsoas muscle but must be respected when placing anterior acetabular retractors.
Biomechanical Principles of Reconstruction
The overarching goal of total hip arthroplasty is the precise restoration of normal hip biomechanics, which requires re-establishing the center of rotation, optimizing femoral offset, and equalizing leg lengths. The hip joint functions as a class I lever, where the fulcrum is the center of the femoral head, the effort is the abductor musculature, and the load is the body weight. Medializing the acetabular component to the level of the true cotyloid fossa decreases the lever arm of the body weight, thereby reducing the joint reactive forces acting across the bearing surface. This medialization must be balanced against the need to preserve adequate anterior and posterior column bone stock.
Femoral offset, defined as the perpendicular distance from the center of rotation of the femoral head to the anatomical axis of the femur, is critical for maximizing the abductor moment arm. Restoring or slightly increasing the native offset enhances abductor efficiency, reduces the force required to stabilize the pelvis during the single-leg stance phase of gait, and decreases the risk of impingement and subsequent dislocation. Conversely, failing to restore offset leads to abductor weakness, increased joint reactive forces, and a higher propensity for instability. Leg length restoration is intimately tied to offset and center of rotation; the surgeon must utilize preoperative templating and intraoperative landmarks (e.g., the distance from the lesser trochanter to the center of rotation) to ensure symmetric leg lengths, recognizing that minor discrepancies are often tolerated better than significant offset deficiencies or instability.

Exhaustive Indications and Contraindications
The decision to proceed with an uncemented total hip arthroplasty must be predicated on a rigorous clinical and radiographic evaluation, confirming that the patient's pathology is severe, functionally limiting, and refractory to exhaustive conservative management. The primary indication is end-stage degenerative joint disease—encompassing primary osteoarthritis, secondary osteoarthritis (e.g., post-traumatic, dysplastic), inflammatory arthropathies, and advanced osteonecrosis—that significantly impairs the patient's activities of daily living, causes intractable pain (often night pain), and diminishes overall quality of life. The patient must have completed a comprehensive trial of non-operative modalities, including weight optimization, activity modification, targeted physical therapy, non-steroidal anti-inflammatory drugs (NSAIDs), and potentially intra-articular corticosteroid injections, without sustained relief.
A meticulous physical examination is essential to confirm the hip as the primary pain generator and to assess the functional status of the surrounding musculature. The Trendelenburg test is critical for evaluating the integrity of the abductor mechanism; a positive test, indicated by a pelvic drop on the contralateral side during a single-leg stance, suggests abductor insufficiency, which may influence the choice of surgical approach and postoperative rehabilitation. The hip flexion-internal rotation test (often analogous to the FADIR test) is highly sensitive for intra-articular hip pathology; reproduction of the patient's characteristic groin pain strongly correlates with hip joint disease. The surgeon must also carefully evaluate for fixed deformities (flexion contractures, limb length discrepancies) and perform a thorough neurological assessment to rule out extrinsic sources of pain, such as lumbar spinal stenosis or radiculopathy, which frequently coexist with hip osteoarthritis in the elderly population.
While uncemented THA is widely applicable, specific patient factors may render it inappropriate or necessitate alternative techniques (e.g., cemented fixation). Absolute contraindications are primarily related to active infection or severe medical comorbidities that preclude safe anesthesia and surgery. Relative contraindications often revolve around bone quality and the ability to achieve a secure initial press-fit. Severe osteoporosis, prior pelvic irradiation, or extensive cystic disease of the acetabulum or proximal femur may compromise the mechanical stability of an uncemented implant, increasing the risk of intraoperative periprosthetic fractures or early aseptic loosening.
| Category | Specific Condition | Clinical Rationale and Management Strategy |
|---|---|---|
| Absolute Contraindications | Active systemic or local infection (e.g., active PJI, untreated osteomyelitis) | Risk of seeding the new implant is unacceptably high. Requires infectious disease clearance and potentially staged management if revising. |
| Absolute Contraindications | Neuropathic arthropathy (Charcot joint) | Severe lack of proprioception leads to rapid, catastrophic mechanical failure and dislocation. Arthrodesis or specialized constrained constructs may be required. |
| Absolute Contraindications | Severe, uncorrectable medical comorbidities | High perioperative mortality risk (e.g., recent myocardial infarction, severe uncompensated heart failure). |
| Relative Contraindications | Severe osteoporosis (Dorr Type C bone) | High risk of intraoperative calcar fracture during broaching and failure of biologic ingrowth. Consider cemented femoral stem. |
| Relative Contraindications | Prior pelvic radiation therapy | Irradiated bone has diminished osteogenic potential and poor vascularity, compromising osseointegration of uncemented cups. |
| Relative Contraindications | Inadequate abductor musculature (e.g., polio, severe neurologic deficit) | High risk of recurrent dislocation and severe limp. May require a constrained liner, dual mobility construct, or alternative procedure. |
Pre-Operative Planning, Templating, and Patient Positioning
Radiographic Protocols and Digital Templating
The foundation of a flawless surgical execution is laid long before the incision, beginning with meticulous preoperative planning and templating. High-quality, standardized radiographs are mandatory. The standard series must include a low-anteroposterior (AP) view of the pelvis centered over the symphysis pubis, allowing for assessment of pelvic obliquity, bilateral hip comparison, and evaluation of the contralateral joint. Additionally, an AP view of the affected hip, taken with the femur internally rotated 10 to 15 degrees, is crucial. This internal rotation compensates for the native femoral anteversion, bringing the femoral neck into the true coronal plane, thereby providing an accurate representation of the neck-shaft angle, offset, and medullary canal geometry. A cross-table lateral or frog-leg lateral view is also required to assess the anterior femoral bow, posterior osteophytes, and three-dimensional canal morphology.
Digital templating has largely superseded acetate overlays, offering enhanced precision and the ability to dynamically adjust implant parameters. The templating process begins with the acetabulum. The surgeon identifies the radiographic teardrop, the ilioischial line, and the superior acetabular rim. The goal is to select a hemispherical cup size that maximizes contact with the native subchondral bone while medializing the center of rotation to the anatomic hip center, typically restoring the hip center to a point slightly lateral and superior to the teardrop. The cup is templated at an inclination of 40 degrees and an anteversion of 15 to 20 degrees. Once the acetabular center of rotation is established, femoral templating commences. The surgeon selects a stem size that achieves cortical contact in the targeted fixation zone (metaphyseal or diaphyseal, depending on the implant philosophy) while restoring the native femoral offset and establishing symmetric leg lengths. The level of the femoral neck resection is carefully measured relative to a fixed landmark, usually the lesser trochanter, to guide the intraoperative osteotomy.
Patient Positioning and Operating Room Setup
Proper patient positioning is a critical, often underappreciated, step that directly influences the accuracy of component orientation and the ease of surgical exposure. For the direct lateral (modified Hardinge) approach, the patient is positioned supine on a standard operating table. The supine position offers distinct advantages, including straightforward assessment of leg lengths and pelvic alignment, and excellent access to the airway for the anesthesia team. It is imperative that the pelvis is level in both the coronal and sagittal planes. Any undetected pelvic tilt or obliquity will translate directly into errors in acetabular component positioning; for instance, an unrecognized posterior pelvic tilt will result in an inadvertently retroverted cup placement.
To ensure rigid pelvic stabilization, a sacral post or a specialized pelvic positioning device is frequently employed. A well-leg holder may be utilized for the contralateral limb, allowing the operative leg to be freely manipulated through a full range of motion. The operative field must be widely prepped and draped to allow for extensile measures should complications arise, such as the need to extend the incision proximally for pelvic fixation or distally for a diaphyseal fracture. The surgeon must verify that the operative leg can be easily adducted and externally rotated, as these maneuvers are essential for dislocating the hip and exposing the proximal femur during the lateral approach. Before the incision is made, a final time-out is conducted, and the surgeon visually and palpably confirms the bony landmarks: the anterior superior iliac spine, the greater trochanter, and the shaft of the femur.
Step-by-Step Surgical Approach and Fixation Technique
Incision, Superficial Dissection, and Deep Exposure
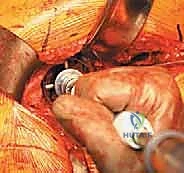
The direct lateral approach, commonly a modification of the Hardinge technique, provides excellent exposure of both the acetabulum and the proximal femur while maintaining the integrity of the posterior capsule, thereby significantly reducing the risk of postoperative posterior dislocation. The skin incision is centered over the lateral aspect of the greater trochanter, extending proximally along the axis of the femur toward the iliac crest and distally along the femoral shaft. The length of the incision is dictated by patient body habitus and the complexity of the reconstruction, but the fundamental principle is to achieve adequate visualization without unnecessary soft-tissue trauma. Sharp dissection is carried down through the subcutaneous fat, maintaining meticulous hemostasis to prevent postoperative hematoma formation.
The fascia lata is identified and incised longitudinally in line with the skin incision. Proximally, this split extends into the gluteus maximus fascia. Retraction of the fascial flaps exposes the underlying vastus lateralis distally and the gluteus medius proximally. The critical step of this approach is the splitting of the abductor mechanism. The interval between the anterior one-third and posterior two-thirds of the gluteus medius is identified. Using electrocautery, the muscle fibers are split longitudinally. It is imperative to limit the proximal extent of this split to no more than 3 to 5 centimeters proximal to the tip of the greater trochanter to avoid transecting the superior gluteal nerve, which would result in catastrophic denervation of the anterior abductors. The split is continued distally, elevating the anterior portion of the gluteus medius and the underlying gluteus minimus off the anterior capsule, and partially reflecting the origin of the vastus lateralis from the vastus ridge.

Capsulotomy, Dislocation, and Femoral Neck Osteotomy
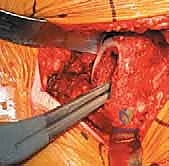
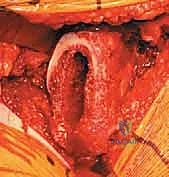
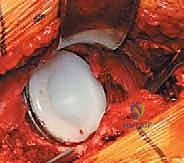
With the anterior capsule fully exposed, a robust capsulotomy or capsulectomy is performed. A T-shaped or H-shaped capsulotomy is common, allowing for wide reflection of the capsular flaps to expose the femoral head and neck. The hip is then dislocated anteriorly by applying a combination of external rotation, adduction, and extension to the operative limb. If the hip is ankylosed or severe osteophytes prevent atraumatic dislocation, an in situ femoral neck osteotomy may be required to avoid iatrogenic fracture of the femur or acetabulum.
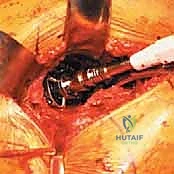
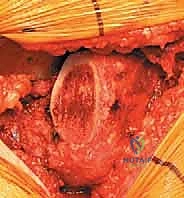
Once dislocated, the proximal femur is elevated, and the site for the femoral neck osteotomy is identified based on preoperative templating. The distance from the lesser trochanter to the planned cut is measured using a calibrated ruler or specialized jig. The osteotomy is executed using an oscillating saw, typically aiming for an angle that matches the collar of the chosen femoral component (often 45 degrees relative to the femoral shaft). The cut must be precise; an excessively high cut may lead to a varus stem position or limb lengthening, while a cut that is too low may compromise metaphyseal support and lead to subsidence. After the osteotomy, the femoral head is removed using a corkscrew and passed off the field.
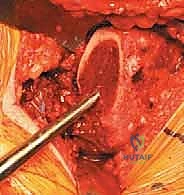
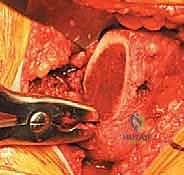
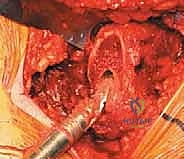
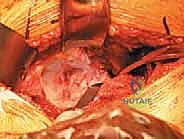
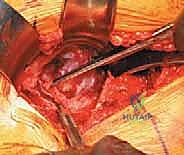
Acetabular Preparation and Component Implantation
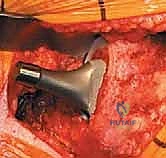
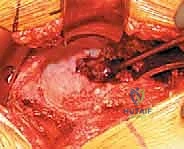
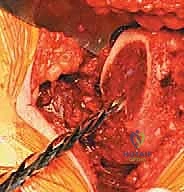
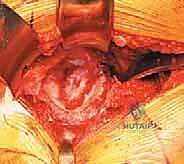
Attention is now directed to the acetabulum. Meticulous retractor placement is the key to achieving 360-degree visualization. An anterior retractor (e.g., a blunt Hohmann) is placed over the anterior rim to retract the iliopsoas and anterior capsule. A superior retractor is positioned under the gluteus medius to expose the dome. An inferior retractor is carefully placed beneath the transverse acetabular ligament, protecting the obturator neurovascular bundle, and a posterior retractor is used to displace the femur posteriorly. The labrum is completely excised using electrocautery or a curved osteotome, and the pulvinar (fat pad) within the cotyloid fossa is removed with a curette. Identifying the true floor of the acetabulum—the radiographic teardrop—is essential to prevent lateralized cup placement.
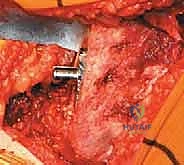
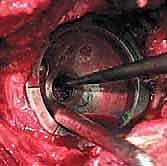
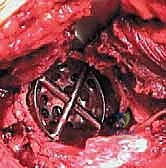
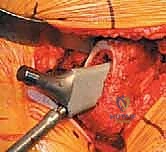
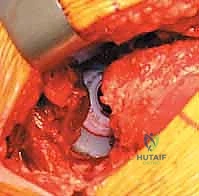
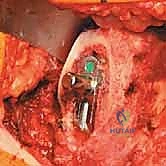
Reaming of the acetabulum commences with a small cheese-grater reamer directed medially to deepen the socket down to the true floor, removing medial osteophytes. Once the medial wall is established, sequentially larger reamers are used, directing the reamer in the planned trajectory of final cup placement (typically 40 degrees of inclination and 15-20 degrees of anteversion). Reaming continues until healthy, bleeding subchondral bone is exposed concentrically, maximizing the surface area for osseointegration. For an uncemented press-fit cup, the final reamer is typically 1 to 2 millimeters smaller than the actual implant size, depending on the bone quality and the specific implant design. The porous-coated titanium cup is then impacted into place. The surgeon assesses the stability of the press-fit through tactile feedback and attempts to distract the cup. Supplemental fixation with cancellous screws may be utilized if the initial press-fit is deemed tenuous, directing screws into the safe zone of the posterior-superior quadrant to avoid neurovascular injury. A highly cross-linked polyethylene or ceramic liner is then seated and impacted into the titanium shell.
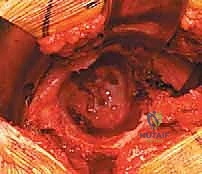

Femoral Preparation, Trialing, and Final Insertion
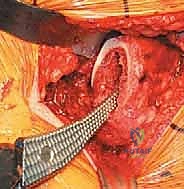
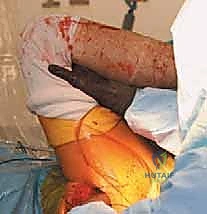
The operative limb is repositioned to expose the proximal femur. In the direct lateral approach, the leg is typically adducted, externally rotated, and hyperextended, allowing the proximal femur to be delivered anteriorly. A box osteotome is used to open the femoral canal, taking care to lateralize the entry point into the greater trochanter to prevent varus malalignment of the stem. A canal finder or tapered awl is introduced to identify the intramedullary axis.
Sequential broaching of the femur is performed, starting with the smallest broach and progressing to the templated size. The broach must be advanced in the correct version (typically 10-15 degrees of native anteversion) and alignment. The surgeon relies on auditory and tactile feedback; a change in pitch during impaction indicates cortical contact. Broaching is complete when the broach achieves absolute rotational and axial stability within the canal and the proximal medial aspect of the broach sits flush with the calcar resection. A trial neck and head are assembled onto the final broach, and the hip is reduced.
A comprehensive trial reduction is performed to assess stability, offset, and leg length. The hip is taken through a full range of motion, checking for impingement in flexion/internal rotation and extension/external rotation. Soft tissue tension is evaluated by applying longitudinal traction; the joint should distract slightly (1-2 mm) but demonstrate robust resistance to subluxation. Leg lengths are compared by palpating the medial malleoli or utilizing intraoperative referencing pins. Once the optimal modular head size and neck length are determined, the hip is dislocated, the trial components are removed, and the final porous-coated uncemented stem is impacted into the canal. The final ceramic or metal head is impacted onto the trunnion after ensuring the morse taper is clean and dry. The hip is reduced for the final time, the wound is copiously irrigated, and a meticulous layered closure is performed, paying special attention to the robust repair of the split gluteus medius and fascial layers to prevent postoperative abductor weakness.
Complications, Incidence Rates, and Salvage Management
Despite meticulous technique, total hip arthroplasty carries inherent risks, and the surgeon must be prepared to manage both intraoperative and postoperative complications. Intraoperative periprosthetic fractures are a particular concern with uncemented stems, especially during the impaction of a press-fit component into sclerotic or osteoporotic bone. Calcar fractures are the most common, occurring in approximately 1% to 3% of primary cases. If identified intraoperatively, an undisplaced calcar fracture can often be managed with cerclage wiring and progression to a fully coated or modular stem to bypass the defect. Acetabular fractures during cup impaction are rare but devastating; they require immediate recognition, potential supplemental screw fixation, or conversion to a multi-hole revision shell.
Clinical & Radiographic Imaging Archive