Posterior Cruciate Ligament Injuries: Advanced Physical Examination, Diagnostics, and Natural History
Key Takeaway
Diagnosing posterior cruciate ligament (PCL) injuries requires meticulous physical examination to avoid mistaking a posteriorly subluxed tibia for an anterior cruciate ligament tear. By assessing the normal 5 to 10 mm anterior tibial step-off, utilizing stress radiography, and understanding the natural history of PCL deficiency, orthopaedic surgeons can accurately identify these injuries and prevent long-term degenerative articular changes.
INTRODUCTION TO POSTERIOR CRUCIATE LIGAMENT INJURIES
The posterior cruciate ligament (PCL) is the primary restraint to posterior tibial translation, providing approximately 95% of the total restraining force against posterior displacement of the tibia relative to the femur. Despite its robust biomechanical properties—boasting a cross-sectional area significantly larger than that of the anterior cruciate ligament (ACL)—the PCL is susceptible to rupture under specific high-energy trauma or hyperflexion mechanisms.
Historically, PCL injuries have been underdiagnosed or misdiagnosed in the acute setting. The subtlety of clinical signs, combined with the complex interplay of the posterolateral corner (PLC) and medial-sided structures, demands a rigorous, evidence-based approach to physical examination and diagnostic imaging. Furthermore, the natural history of the PCL-deficient knee remains a topic of intense academic debate, with clinical trajectories ranging from asymptomatic functional adaptation to rapid, debilitating osteoarthritis. This comprehensive masterclass delineates the critical nuances of physical examination, advanced imaging modalities, and the natural history of PCL injuries to guide orthopaedic residents, fellows, and practicing consultants in optimal patient management.
MECHANISM OF INJURY
Understanding the mechanism of injury is paramount for maintaining a high index of suspicion for PCL disruption. As a rule, "isolated" tears of the PCL are relatively rare; the vast majority of these ruptures are associated with medial or lateral compartment disruptions, particularly the posterolateral corner.
Clinically, isolated tears of the PCL are typically generated by two primary mechanisms:
* The Dashboard Injury: A direct, high-energy blow to the anterior aspect of the proximal tibia while the knee is flexed (e.g., striking the dashboard in a motor vehicle collision). This drives the tibia posteriorly, catastrophically loading the anterolateral (AL) and posteromedial (PM) bundles of the PCL.
* Fall on a Flexed Knee: A lower-energy, athletic injury where the patient falls directly onto the tibial tubercle with the knee hyperflexed and the foot in plantarflexion.
* Hyperextension: Often associated with combined ACL and PCL injuries, severe hyperextension can rupture the PCL once the ACL has failed.
CLINICAL PEARL:
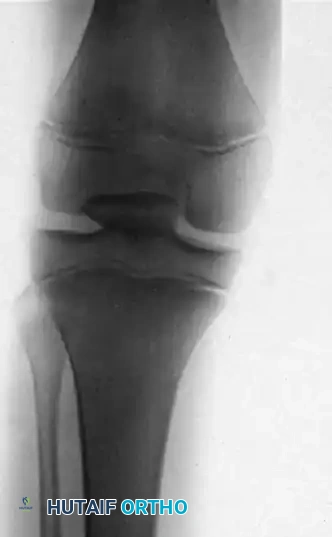
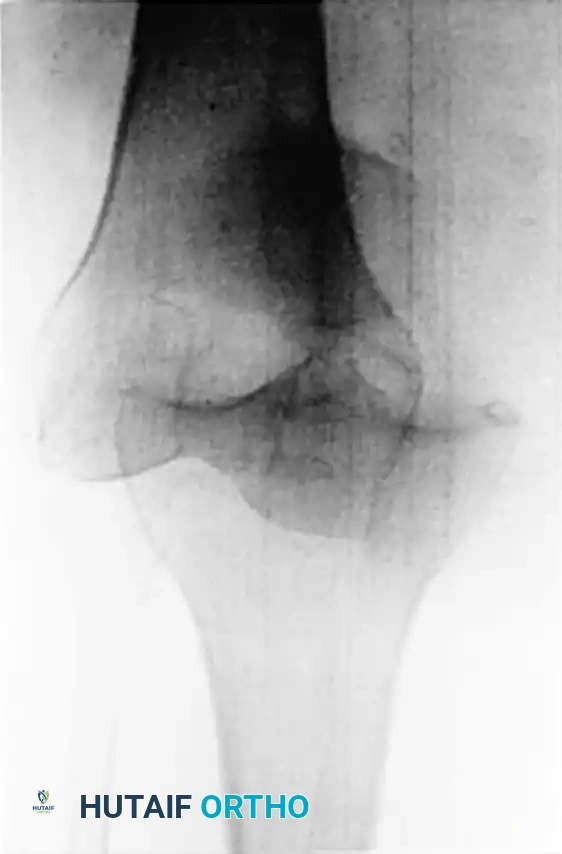
Isolated PCL disruptions can be exceedingly difficult to diagnose acutely due to hemarthrosis, muscle guarding, and the absence of gross multidirectional instability. Always scrutinize acute knee radiographs for a bony avulsion fragment originating from the posterior tibial sulcus, which definitively indicates a PCL injury and may alter the surgical algorithm toward acute primary repair.
ADVANCED PHYSICAL EXAMINATION
The physical examination of a suspected PCL injury requires a systematic approach, meticulous patient positioning, and an intimate understanding of knee kinematics. The examiner must evaluate not only the PCL but also the collateral ligaments and the posterolateral corner to rule out multiligamentous knee injuries (MLKI).
The Posterior Drawer Test and the "Pseudolaxity" Pitfall
The posterior drawer test is the most sensitive and specific clinical maneuver for diagnosing a PCL tear. However, the true direction of translation of the tibia is frequently misinterpreted by inexperienced clinicians.
When a patient with a PCL-deficient knee lies supine, gravity and the resting tone of the hamstring muscles cause the proximal tibia to subluxate posteriorly. If the examiner fails to recognize this abnormal starting position, the application of further posterior stress may not produce any additional translation. This leads to a false-negative posterior drawer test.
Conversely, when the examiner applies an anterior force to this posteriorly subluxed tibia, the tibia translates anteriorly to its normal, neutral anatomic position. The examiner feels this excursion, misinterprets the reduction of the tibia as pathological anterior laxity, and erroneously diagnoses an ACL injury.
SURGICAL PITFALL:
The "False Anterior Drawer" is a classic diagnostic trap. The examiner does not realize that the tibia is simply moving from a posteriorly subluxed position to neutral, rather than from neutral to an anteriorly subluxed position. Misdiagnosing a PCL tear as an ACL tear can lead to catastrophic surgical planning, including inappropriate graft placement and failure of reconstruction.
Assessing the Tibial Step-Off
To prevent diagnostic confusion, the examiner must establish the neutral resting position of the knee before applying any dynamic stress. This is achieved by assessing the anterior tibial step-off.
- Positioning: Place both of the patient's knees in the drawer position (hips flexed to 45 degrees and knees flexed to 90 degrees).
- Palpation: The examiner places their thumbs on the anteromedial and anterolateral joint lines of each knee, sliding distally from the medial femoral condyle to the medial tibial plateau.
- Normal Anatomy: In a healthy knee, the anterior medial tibial plateau rests approximately 5 to 10 mm anterior to the medial femoral condyle.
- Pathologic Anatomy: With a PCL injury, this anterior offset is lost. The tibia sags posteriorly, and the anterior tibial plateau appears flush with, or even posterior to, the medial femoral condyle.
Grading PCL Laxity
Once the resting position is established, the posterior drawer test is performed and graded based on the position of the medial tibial plateau relative to the medial femoral condyle:
* Grade I (Partial Tear): 0 to 5 mm of posterior translation. The tibia remains anterior to the medial femoral condyle (the normal step-off is diminished but not lost).
* Grade II (Complete Isolated Tear): 6 to 10 mm of posterior translation. The anterior tibia becomes flush with the medial femoral condyle.
* Grade III (Combined Injury): Greater than 10 mm of posterior translation. The anterior tibia translates posterior to the medial femoral condyle. A Grade III injury almost universally indicates a combined PCL and posterolateral corner (PLC) or medial collateral ligament (MCL) injury.
Adjunctive Clinical Tests
- Posterior Sag Sign (Godfrey's Test): The patient's hips and knees are flexed to 90 degrees, and the examiner supports the patient's heels. A visible posterior drop (sag) of the proximal tibia confirms PCL deficiency.
- Quadriceps Active Test: With the knee flexed to 90 degrees and the tibia in its posteriorly subluxed resting position, the patient is asked to actively contract their quadriceps (e.g., by attempting to slide their foot down the examination table against resistance). The patellar tendon vector pulls the tibia anteriorly, reducing it to the neutral position. A visible anterior shift is pathognomonic for a PCL tear.
- Dial Test: Essential for differentiating an isolated PCL tear from a combined PCL/PLC injury. External rotation of the tibia is measured at 30 degrees and 90 degrees of knee flexion. Increased external rotation (>10 degrees compared to the contralateral side) at 90 degrees only suggests an isolated PCL injury; increased rotation at both 30 and 90 degrees indicates a combined PCL and PLC injury.
DIAGNOSTIC IMAGING PROTOCOLS
While a meticulous physical examination is the cornerstone of diagnosis, advanced imaging is required to quantify laxity, evaluate concomitant intra-articular pathology, and formulate a definitive surgical plan.
Stress Radiography
Stress radiography is a highly objective, reproducible, and invaluable tool in the diagnosis and quantification of PCL injuries. It is particularly useful for differentiating between partial and complete tears, and for monitoring the progression of laxity over time.
Hewett et al. established a rigorous protocol for stress radiography in patients with isolated unilateral PCL tears. Their methodology and findings are foundational to modern orthopaedic practice:
* Protocol: An 89-N posterior load is applied to the proximal tibia (often utilizing a Telos stress device or kneeling views) with the knee positioned in 70 degrees of flexion. A lateral radiograph is then obtained.
* Comparative Efficacy: Stress radiographs were compared with KT-1000 arthrometer measurements and clinical posterior drawer test results. Stress radiography was found to be statistically superior to both modalities in accurately quantifying posterior tibial translation.
* Diagnostic Thresholds: An increased side-to-side difference in posterior translation of 8 mm or more on stress radiographs is highly indicative of a complete PCL rupture. Measurements between 0 and 7 mm typically represent partial tears or attenuated ligaments.
CLINICAL PEARL:
The KT-1000 arthrometer, while historically popular for ACL evaluation, is notoriously unreliable for PCL injuries due to the difficulty in establishing a consistent neutral starting point and the interference of the patellofemoral joint during posterior translation. Rely on stress radiography for objective quantification of PCL laxity.
Magnetic Resonance Imaging (MRI)
MRI is the gold standard for the non-invasive evaluation of the PCL and is routinely obtained in all suspected cases.
* Reliability: MRI studies are exceptionally reliable for the diagnosis of acute PCL tears—often cited as being more accurate for the PCL than for the ACL. The normal PCL appears as a thick, continuous, low-signal-intensity band on T1 and T2-weighted sagittal images.
* Acute vs. Chronic: In the acute setting, a tear manifests as discontinuity, intrasubstance high signal (edema/hemorrhage), or a thickened, amorphous ligament. In chronic settings, the PCL may heal in an elongated position, appearing structurally intact but functionally incompetent.
* Associated Pathology: While associated meniscal disease is much less common with PCL injuries than with ACL injuries, MRI is critical for identifying concomitant chondral lesions, bone bruises (typically anterior tibia and patella from the dashboard mechanism), and posterolateral corner disruptions. If an MRI reveals repairable meniscal or chondral lesions, surgical intervention for these lesions is indicated, which subsequently lowers the threshold for concurrent PCL reconstruction to protect the intra-articular repairs.
THE NATURAL HISTORY OF THE PCL-DEFICIENT KNEE
The natural history of the disrupted posterior cruciate ligament remains one of the most debated topics in sports medicine. Unlike the ACL-deficient knee, which predictably leads to recurrent instability and secondary meniscal tears, the trajectory of the PCL-deficient knee varies considerably among patients.
The Spectrum of Clinical Outcomes
Some investigators have described cohorts of untreated patients who remain highly functional with minimal symptoms many years after their initial injury. These patients often possess excellent dynamic quadriceps control, which compensates for the loss of the static posterior restraint.
Conversely, other longitudinal studies report a grim prognosis for the conservatively managed PCL. Significant osteoarthritic changes in knees with chronic PCL deficiency have been reported in an exceptionally high percentage (up to 80%) of patients when repair or reconstruction is delayed beyond 4 years.
Biomechanical Consequences of PCL Deficiency
To understand this clinical dichotomy, one must examine the altered kinematics of the PCL-deficient knee:
* Posterior Tibial Sag: The chronic posterior subluxation of the tibia alters the resting contact points between the femur and the tibia.
* Medial Compartment Overload: The posterior shift of the tibia causes the medial femoral condyle to ride anteriorly on the medial tibial plateau, ascending the anterior upslope of the medial meniscus. This drastically increases contact pressures in the medial tibiofemoral compartment, leading to accelerated articular cartilage wear.
* Patellofemoral Kinematics: To counteract the posterior tibial sag, the quadriceps muscle must work overtime. This chronic, increased quadriceps tension significantly elevates patellofemoral joint reaction forces, predisposing the patient to severe anterior knee pain and patellofemoral chondromalacia.
Clinical Presentation of Chronic Deficiency
Most literature regarding ACL insufficiency emphasizes functional instability (giving way). In stark contrast, functional instability may not be the major symptom of an isolated PCL insufficiency.
Patients with chronic PCL deficiency typically present with:
* Anterior Knee Pain: Secondary to patellofemoral overload.
* Medial Joint Line Aching: Exacerbated during activity, particularly deceleration, descending stairs, or walking down inclines.
* Recurrent Effusions: A hallmark of progressive articular cartilage degeneration.
SURGICAL WARNING:
Do not wait for radiographic evidence of osteoarthritis before considering surgical intervention in a symptomatic patient. Pain, aching during activity, and recurrent effusions are the direct result of articular cartilage degeneration, which begins at a microscopic and biochemical level several years before joint space narrowing or osteophytes become evident on standard radiographs.
CLINICAL DECISION MAKING AND TREATMENT ALGORITHMS
The management of PCL injuries must be highly individualized, taking into account the grade of the injury, the chronicity, the presence of concomitant injuries, and the patient's functional demands.
Non-Operative Management
Isolated Grade I and Grade II PCL tears are traditionally managed non-operatively. The protocol involves:
* A period of immobilization in full extension (to eliminate the posterior sag caused by hamstring tension).
* Aggressive physical therapy focusing on quadriceps strengthening, which acts as a dynamic synergist to the PCL.
* Avoidance of isolated hamstring strengthening in the early rehabilitation phase.
Operative Indications
Surgical reconstruction of the PCL is generally indicated in the following scenarios:
* Combined Ligamentous Injuries: Any PCL tear associated with a PLC, MCL, or ACL injury (Grade III laxity).
* Bony Avulsion Fractures: Acute avulsions from the tibial insertion should be primarily repaired with lag screws or suture anchors to restore native anatomy.
* Symptomatic Chronic Isolated Tears: Patients with isolated PCL tears who fail conservative management and develop progressive medial or patellofemoral pain, recurrent effusions, or functional instability.
* Concomitant Intra-articular Pathology: If a patient requires surgery for a repairable meniscus tear or a significant chondral defect, concurrent PCL reconstruction is strongly considered to restore normal joint kinematics and protect the repair from abnormal shear forces.
CONCLUSION
The evaluation and management of posterior cruciate ligament injuries demand a high level of clinical acumen. The orthopaedic surgeon must master the nuances of the physical examination—specifically recognizing the posteriorly subluxed starting position to avoid the pitfall of the false anterior drawer. Utilizing stress radiography provides objective, quantifiable data that surpasses traditional arthrometric measurements, while MRI remains indispensable for evaluating the entire joint envelope.
Although the natural history of the isolated PCL tear is variable, the biomechanical reality of medial compartment and patellofemoral overload cannot be ignored. By identifying patients at risk for early degenerative arthritis and intervening appropriately, surgeons can alter the natural history of the PCL-deficient knee, preserving joint longevity and optimizing patient function.
📚 Medical References
- PCL injuries with associated pathology: long-term results, Orthopedics 14:687, 1991.
- Berg EE: Posterior cruciate ligament tibial inlay reconstruction, Arthroscopy 11:69, 1995.
- Bergfeld JA, Graham SM, Parker RD, et al: A biomechanical comparison of posterior cruciate ligament reconstructions using singleand double-bundle tibial inlay techniques, Am J Sports Med 33:976, 2005.
- Bosworth DM, Bosworth BM: Use of fascia lata to stabilize the knee in cases of ruptured crucial ligaments, J Bone Joint Surg 18:178, 1936.
- Boynton MD, Tietjens BR: Long-term follow-up of untreated isolated posterior cruciate ligament–defi cient knee, Am J Sports Med 24:306, 1996.
- Burks RT, Schaffer JJ: A simplifi ed approach to the tibial attachment of the posterior cruciate ligament, Clin Orthop Relat Res 254:216, 1990.
- Castle TH Jr, Noyes FR, Grood ES: Posterior tibial subluxation of the posterior cruciate–defi cient knee, Clin Orthop Relat Res 284:193, 1992.
- Clancy WG Jr, Bisson LJ: Double-tunnel technique for reconstruction of the posterior cruciate ligament, Oper Tech Sports Med 7:110, 1999.
- Clancy WG Jr, Shelbourne KD, Zoellner GB, et al: Treatment of knee
You Might Also Like