00:00
Start Quiz
Question 51
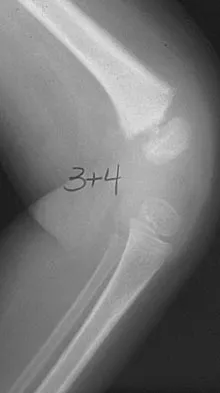
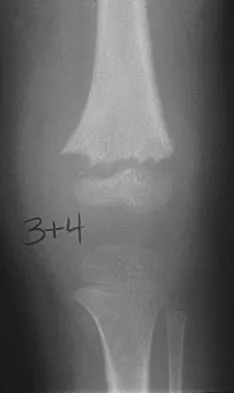
A 10-year-old boy with an L1 myelomeningocele has a low-grade fever and a swollen thigh that is warm to touch and erythematous. AP and lateral radiographs are shown in Figures 24a and 24b. Management should consist of
Explanation
Fractures of the long bones are common in patients with myelodysplasia, and the frequency of fracture increases with higher level defects. Fractures also occur following surgery and immobilization secondary to disuse osteoporosis. The response to the fracture (swelling, fever, warmth, erythema) is often confused with infection, osteomyelitis, or cellulitis. Management should consist of a short period of immobilization in a well-padded splint. Long-term casting results in further osteopenia and repeated fractures. Lock TR, Aronson DD: Fractures in patients who have myelomeningocele. J Bone Joint Surg Am 1989;71:1153-1157.
Question 52
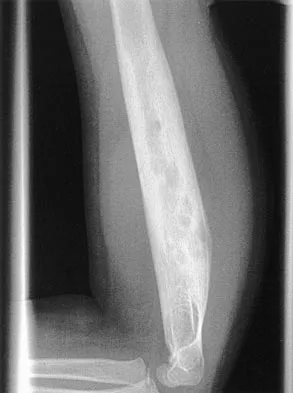
A 6-year-old African-American boy with sickle cell disease has had pain and limited use of his right arm for the past 3 days. History reveals that he sustained a humeral fracture approximately 3 years ago. A lateral radiograph is shown in Figure 25. Based on these findings, a presumptive diagnosis of chronic osteomyelitis is made. What are the two most likely organisms?
Explanation
The risk of Salmonella osteomyelitis is much greater in patients with sickle cell disease than the general population. The exact reason for this increased risk is still unclear, but it appears to be associated with an increased incidence of gastrointestinal microinfarcts and abscesses. Both Staphylococcus aureus and Salmonella have been mentioned as the most prevalent causative organisms. Piehl FC, David RJ, Prugh SI: Osteomyelitis in sickle cell disease. J Pediatr Orthop 1993;13:225-227. Givner LB, Luddy RE, Schwartz AD: Etiology of osteomyelitis in patients with major sickle hemoglobinopathies. J Pediatr 1981;99:411-413. Epps CH Jr, Bryant DD III, Coles MJ, Castro O: Osteomyelitis in patients who have sickle-cell disease: Diagnosis and management. J Bone Joint Surg Am 1991;73:1281-1294.
Question 53
A 7-year-old child is unresponsive, tachycardic, and has a systolic blood pressure of 50 mm Hg after being struck by a car. The patient is intubated and venous access is obtained. The secondary survey reveals an unstable pelvis. Despite adequate resuscitation, the patient continues to be hemodynamically unstable. What is the best course of action?
Explanation
The patient is hemodynamically unstable, so any treatment should be aimed at stabilization. Airway, breathing, and circulation are the most important areas to control initially; the patient has been intubated and has adequate venous access. Despite fluid resuscitation, the child remains hypotensive, indicating continued blood loss. With an unstable pelvic fracture there can be significant hemorrhage. Decreasing the pelvic volume can decrease blood loss related to the pelvic fracture. This can be done in the emergency department by applying a pelvic sling. Other means of decreasing pelvic volume include a pelvic clamp, a simple anterior frame pelvic external fixator, or a simple sheet tied around the pelvis. These maneuvers may stabilize the patient so that further evaluation and treatment can be undertaken. All of the other choices will delay stabilization and should be postponed until the patient is stabilized. Torode I, Zieg D: Pelvic fractures in children. J Pediatr Orthop 1985;5:76-84. Eichelberger MR, Randolph JG: Pediatric trauma-initial resuscitation, in Moore EE, Eisman B, Van Way CE (eds): Critical Decisions in Trauma. St Louis, MO, CV Mosby, 1984, p 344.
Question 54
A 3-year-old boy with severe cerebral palsy is unable to sit independently and does not crawl. Examination reveals a 40-degree hip flexion contracture by the Thomas test and 25 degrees of passive abduction. A radiograph of the pelvis shows subluxation of both hips, with a migration index of 30%. Management should consist of
Explanation
Progressive hip subluxation occurs in up to 50% of children with spastic quadriparesis. The subluxation is the result of chronic muscle hypertonicity, especially in the adductor muscle group. In time, the constant muscle tension will lead to dislocation, dysplastic changes in the acetabulum, and erosive changes in the cartilage of the femoral head. Many of these children will experience pain. Two recent studies have shown that early soft-tissue releases can successfully prevent progressive subluxation in children who are younger than age 4 years and who have a Reimers index (migration index) of less than 40%. Botulinum toxin A injections may reduce tone in the adductors for 4 to 6 months, but it is difficult to inject into the iliopsoas. Additionally, there are no long-term studies documenting the efficacy of botulinum toxin A to treat progressive hip subluxation in patients who have spastic quadriparesis. In general, proximal femoral osteotomy, combined with soft-tissue release as necessary, is indicated in older children (older than age 4 years) with progressive subluxation. Although selective dorsal rhizotomy has been used in nonambulatory patients, outcomes are less well documented than in ambulatory patients. There are no studies documenting the effect of selective dorsal rhizotomy on progressive hip subluxation in nonambulatory children. Miller F, Cardoso Dias R, Dabney KW, et al: Soft-tissue release for spastic hip subluxation in cerebral palsy. J Pediatr Orthop 1997;17:571-584.
Question 55
The parents of a 3-year-old girl who has had pain and swelling in the right ankle for the past 3 months now report that she has a limp and that the right knee and both ankles are painful and swollen. The limp and difficulty walking are most severe in the morning when the child first gets out of bed and are also more severe after extended walking. The parents deny fever, chills, weight loss, or night pain. Examination shows mild swelling and slightly restricted motion of the right knee and both ankles but is otherwise normal. In addition to initiation of treatment, the child should be referred to which of the following specialists?
Explanation
Pauciarticular juvenile rheumatoid arthritis (JRA) is the most common subgroup of JRA. It typically presents between the ages of 2 to 4 years with a mild swelling of one to four joints. Girls are affected four times more often than boys. The ankle and knee are commonly involved, and limping is typically worse in the morning and after extended activity. The diagnosis of pauciarticular JRA is typically one of exclusion because laboratory studies, including erythrocyte sedimentation rate and rheumatoid factor, are usually within normal limits. Pauciarticular JRA has the highest incidence of chronic uveitis, and in the subgroup with elevated antinuclear antibody (ANA) titers, the incidence is 75%. In JRA, uveitis usually occurs after the onset of synovitis but may precede the joint symptoms. At the early stage of uveitis, the patient is asymptomatic. If the eye condition is not detected and treated, progressive loss of vision may occur. Orthopaedic surgeons may be instrumental in making the diagnosis of pauciarticular JRA. Pauciarticular JRA is not associated with conditions that require input from the other specialists. Carey TP: Inflammatory arthritides: Juvenile rheumatoid arthritis, seronegative spondyloarthropathies, transient synovitis, hemophilic arthropathy, in Fitzgerald RH, Kaufer H, Malkani AL (eds): Orthopaedics. St Louis, MO, Mosby, 2002, pp 1315-1321.
Question 56
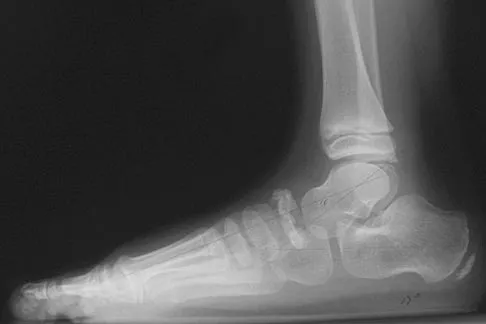
A 9-year-old boy has pain over the midfoot medially with activity. Based on the findings shown in Figures 26a and 26b, which of the following is considered the most effective short-term management?
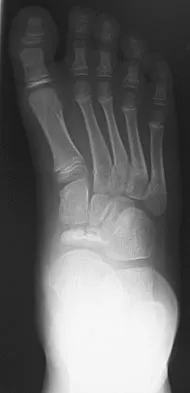
Explanation
While Kohler's disease has a benign course, temporary cast immobilization has been shown to result in a shortened duration of symptoms. Core decompression or other surgery is not warranted because of the benign nature. Shoe inserts may be beneficial, but there are no studies to support their use. Borges JL, Guile JT, Bowen JR: Kohler's bone disease of the tarsal navicular. J Pediatr Orthop 1995;15:596-598.
Question 57
During the first 2 years of life, which of the following actions is most responsible for increasing structural stability of the physis?
Explanation
The zone of Ranvier provides the earliest increase in strength of the physis. During the first year of life, the zone spreads over the adjacent metaphysis to form a fibrous circumferential ring bridging from the epiphysis to the diaphysis. This ring increases the mechanical strength of the physis. The zone also helps the physis grow latitudinally. In turn, the increased width of the physis helps the physis further resist mechanical forces. The change in shape of the physis to its progressively more undulating form is also a factor in increasing physeal strength, but this occurs over a longer period of time, as the child's activity level increases. The undulations of the physis seen in some growth plates also add to stability but to a lesser extent. The other changes contribute little toward increasing physeal strength. Burkus J, Ogden J: Development of the distal femoral epiphysis: A microscopic morphological investigation of the zone of Ranvier. J Pediatr Orthop 1984;4:661-668.
Question 58
Because the patient shown in Figure 27 can no longer fit in shoes, treatment of the deformity should consist of
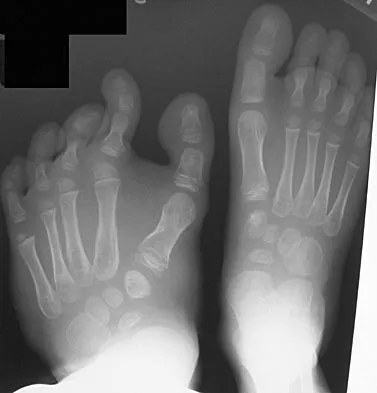
Explanation
In local gigantism, a ray resection allows proper fitting of shoes. The ray resection narrows the foot and shortens the length. The foot may require further surgery with growth. Debulking, physeal arrest, and distal phalanx amputation are unlikely to be effective. Turra S, Santini S, Cagnoni G, Jacopetti T: Gigantism of the foot: Our experience in seven cases. J Pediatr Orthop 1998;18:337-345.
Question 59
Examination of a 9-year-old girl who injured her left elbow in a fall reveals tenderness and swelling localized to the medial aspect of the elbow. Motor and sensory examinations of the hand are normal, and circulation is intact. A radiograph is seen in Figure 28. Management should consist of
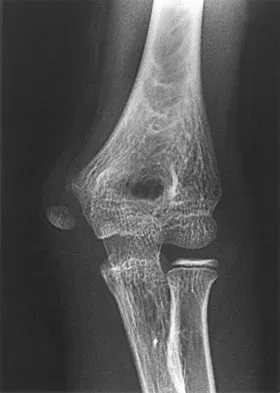
Explanation
Avulsion fractures of the medial epicondyle are caused by a valgus stress applied to the immature elbow and usually occur in children between the ages of 9 and 14 years. Long-term studies have shown that isolated fractures of the medial epicondyle with between 5 to 15 mm of displacement heal well. Brief immobilization (1 to 2 weeks) in a long arm cast or splint yields results similar to open reduction and internal fixation. Fibrous union of the fragment is not associated with significant symptoms or diminished function. Surgical excision of the fragment yielded the worst results in one study and should be avoided. Open reduction is best reserved for those injuries in which the medial epicondylar fragment becomes entrapped in the elbow joint during reduction and cannot be extracted by closed manipulation. Farsetti P, Potenza V, Caterini R, Ippolito E: Long-term results of treatment of fractures of the medial humeral epicondyle in children. J Bone Joint Surg Am 2001;83:1299-1305.
Question 60
A 2-year-old child has refused to bear weight on his leg for the past 2 days. His parents report that he will crawl, has no fever, and has painless full range of motion of his hip and knee. Examination reveals no deformity or bruising, but there is mild swelling and tenderness over the anterior tibia. C-reactive protein, WBC count, and erythrocyte sedimentation rate studies are normal. Radiographs are negative. What is the best course of action?
Explanation
Despite the negative radiographic findings, the child's age and presentation are most consistent with a toddler's fracture. There is often not a witnessed injury. The differential diagnosis of infection is unlikely given that the child is afebrile and shows no signs of illness. Immobilization will make the child more comfortable and will often allow weight bearing. Repeat radiographs at the end of treatment will show a healing fracture and confirm the diagnosis. Aspiration of the tibial metaphysis would be indicated to obtain material for culture. The bone scan and MRI would show abnormalities, but these studies are nonspecific, costly, and time-consuming. Occasionally, oblique radiographs will show the fracture. Halsey MF, Finzel KC, Carrion WV, Haralabatos SS, et al: Toddler's fracture: Presumptive diagnosis and treatment. J Pediatr Orthop 2001;21:152-156.
Question 61
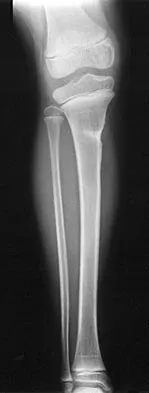
A 7-year-old girl sustains the fracture shown in Figure 29a. Casting results in uneventful healing. Ten months later, the patient has a progressive valgus deformity of the right lower extremity. A radiograph is shown in Figure 29b. Management should now consist of
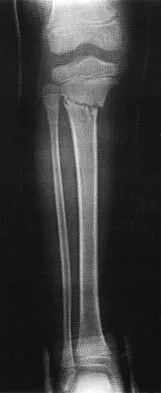
Explanation
Although fractures of the proximal tibial metaphysis in young children appear innocuous, development of a progressive valgus deformity is possible despite adequate and appropriate treatment. When treating a child with this injury, it is prudent to warn the parents that a valgus deformity of the tibia may develop. The most likely cause is asymmetric growth of the proximal tibial physis. Because spontaneous angular improvement can be expected in most patients, surgery to correct these deformities should be delayed at least 2 to 3 years and should be limited to patients who have symptoms. There are no studies that document the efficacy of bracing for this deformity. Tuten HR, Keeler KA, Gabos PG, et al: Posttraumatic tibia valga in children: A long-term follow-up note. J Bone Joint Surg Am 1999;81:799-810.
Question 62
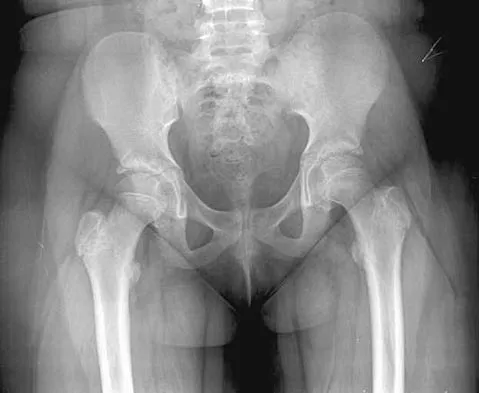
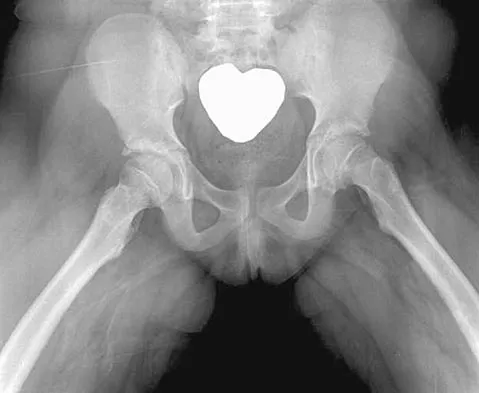
An obese 10-year-old boy has had left groin pain and a limp for the past 2 months. Examination reveals decreased abduction and internal rotation. Laboratory studies show normal renal function and an elevated thyroid-stimulating hormone (TSH) level. AP and frog lateral radiographs of the pelvis are shown in Figures 30a and 30b. What is the best course of action?
Explanation
The radiographs show a grade I slipped capital femoral epiphysis (SCFE) that is classified as stable because the child is able to bear weight. The elevated TSH level indicates possible hypothyroidism. SCFE usually occurs in boys age 12 to 14 years. Because of the patient's young age and hypothyroidism, he is at increased risk for slippage of the contralateral hip; therefore, prophylactic pinning of the uninvolved side also should be considered. Because of the risk of slip progression, crutch treatment and nonsteroidal anti-inflammatory drugs are not indicated. Realignment osteotomy is not indicated for grade I SCFE. Traction to reduce the slip, followed by pinning, has been advocated for unstable slips but is not indicated here. Loder RT, Wittenberg B, DeSilva G: Slipped capital femoral epiphysis associated with endocrine disorders. J Pediatr Orthop 1995;15:349-356.
Question 63
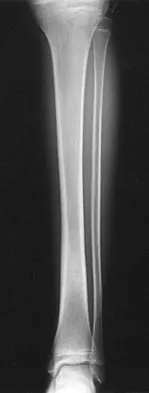
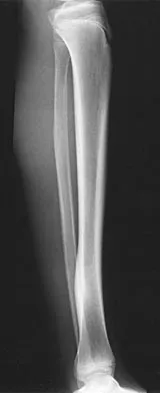
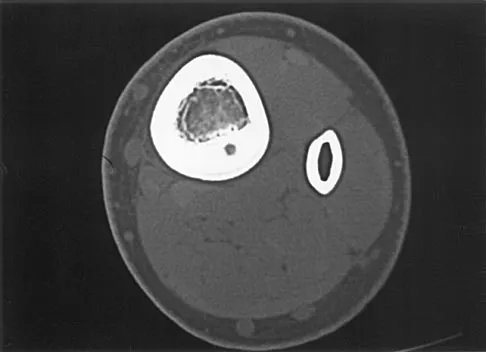
A 7-year-old boy has had chronic left leg pain that is worse at night but is not activity related. Use of nonsteroidal anti-inflammatory drugs for the past 6 months has failed to provide relief. A CBC count with differential, erythrocyte sedimentation rate, and C-reactive protein are within normal limits. Radiographs and a CT scan are shown in Figures 31a through 31c. Management should consist of
Explanation
Osteoid osteomas are painful bone lesions, with radiographs revealing a dense sclerotic cortex surrounding a small radiolucency or nidus. Symptoms often are worse at night but usually are not activity related. While treatment in the past has consisted of open en bloc excision, current means of removal include percutaneous drilling under CT guidance and percutaneous radiofrequency coagulation. Success rates of percutaneous treatment are comparable to those seen following open procedures. The characteristic radiographic appearance of this lesion usually obviates the need for biopsy. Because the lesion is not caused by pyogenic organisms, antibiotics are not indicated. Donahue F, Ahmad A, Mnaymneh W, Pevsner NH: Osteoid osteoma: Computed tomography guided percutaneous excision. Clin Orthop 1999;366:191-196.
Question 64
In patients with neurofibromatosis, what is the most important sign of impending rapid progression of a spinal deformity?
Explanation
Neurofibromatosis can progress very rapidly. Rib penciling is the only singular prognostic factor. Significant progression has been observed in 87% of the curves with three or more penciled ribs. The other factors are often present but do not have a high correlation with rapid, severe progression. Crawford AH, Schorry EK: Neurofibromatosis in children: The role of the orthopaedist. J Am Acad Orthop Surg 1999;7:217-230.
Question 65
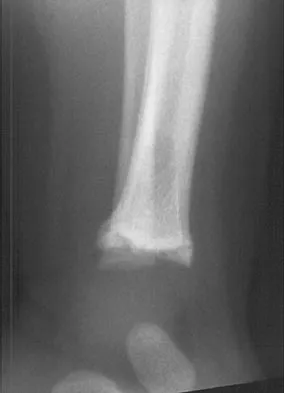
The fracture shown in Figure 32 is strongly indicative of what diagnosis?
Explanation
Fractures that occur through the primary spongiosa at the subphyseal region of the metaphysis are highly specific for child abuse. On radiographic studies, the metaphyseal lucency in these injuries may appear as either the so-called "bucket-handle" or "metaphyseal corner" fracture. These fractures are not typical features of osteogenesis imperfecta or vitamin D-resistant rickets. The ingestion of lead may lead to thick, transverse bands of increased density at the distal metaphysis. Fractures in the subphyseal region of the metaphysis are not typically seen in children who have osteomyelitis. Kocher MS, Kasser JR: Orthopaedic aspects of child abuse. J Am Acad Orthop Surg 2000;8:10-20.
Question 66
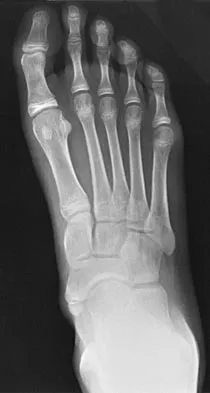
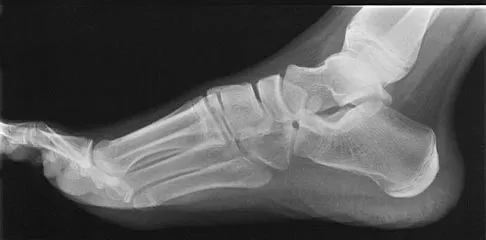
Figures 33a and 33b show the radiographs of a 10-year-old girl who reports a 4-month history of medial foot pain after she was kicked while playing soccer. The pain is worse with activity and partially relieved by rest. Examination reveals tenderness directly over a prominent navicular tuberosity. Management should consist of
Explanation
An accessory tarsal navicular is located at the medial tuberosity of the navicular bone. Nearly all children and adolescents who have a symptomatic accessory tarsal navicular bone become asymptomatic when they reach skeletal maturity. Initial management should include activity restrictions, shoe modification to avoid pressure over the prominent navicular, and non-narcotic analgesics. Although anecdotal, the use of arch supports may be helpful. When pain is refractory to these methods, a short period of cast immobilization may be useful. Surgery should be reserved for patients who have disabling symptoms despite a prolonged period of nonsurgical management. When surgery is indicated, simple excision of the accessory navicular is recommended. Sella EJ, Lawson JP, Ogden JA: The accessory navicular synchondrosis. Clin Orthop 1986;209:280-285.
Question 67
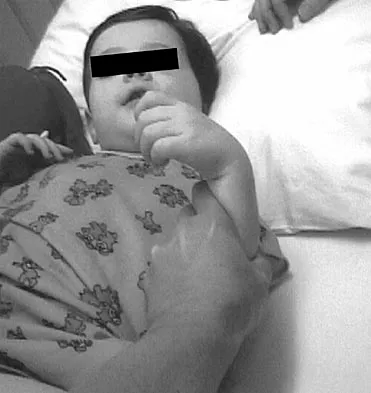
An 18-month-old child with obstetrical palsy has a maximum external rotation as shown in Figure 34. The parents should be advised that without surgical treatment the likelihood that glenoid dysplasia will develop is approximately what percent?
Explanation
Based on the available literature, the probability of development of glenoid dysplasia in the setting of a significant limitation of external rotation is close to 70%. Humeral dysplasia is also likely and can be managed surgically. Efforts are being made to identify procedures that will prevent glenoid dysplasia and help maintain function. Pearl ML, Edgerton BW: Glenoid deformity secondary to brachial plexus birth palsy. J Bone Joint Surg Am 1998;80:659-667. Waters PM, Smith GR, Jaramillo D: Glenohumeral deformity secondary to brachial plexus birth palsy. J Bone Joint Surg Am 1998;80:668-677.
Question 68
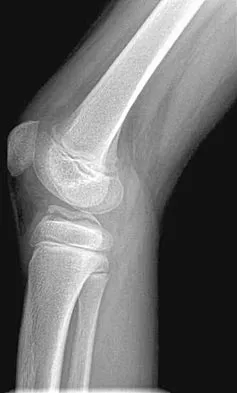
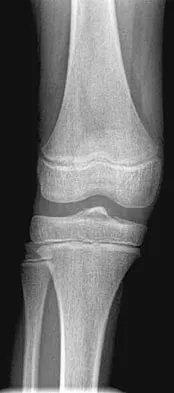
A 10-year-old boy has a painful, swollen knee after falling off his bicycle. Examination reveals no other injuries. Radiographs are shown in Figures 35a and 35b. Initial management of this fracture should consist of
Explanation
The radiographs show a minimally displaced fracture of the tibial eminence, which is classified as a McKeever type II injury. In a number of studies, it has been found that most of these fractures will reduce with extension of the knee. This is often made easier with evacuation of the hemarthrosis. The position of knee immobilization is controversial, with some authors preferring full extension and others preferring 20 degrees of flexion. Flexion to 90 degrees will further displace the fragment. If the fragment does not reduce or if the patient has a McKeever type III or IV injury, reduction and internal fixation are required. This can be done with either an open or an arthroscopic procedure. Excision of the fragment is not indicated. Meyers MH, McKeever FM: Fractures of the intercondylar eminence of the tibia. J Bone Joint Surg Am 1970;52:1677-1684. Wiley JJ, Baxter MP: Tibial spine fractures in children. Clin Orthop 1990;255:54-60 Janarv PM, Westblad P, Johansson C, Hirsch G: Long-term follow-up of anterior tibial spine fractures in children. J Pediatr Orthop 1995;15:63-68.
Question 69
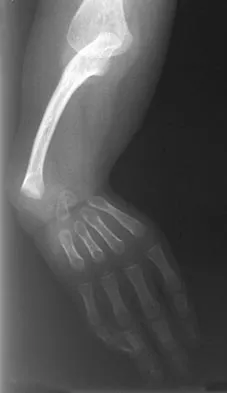
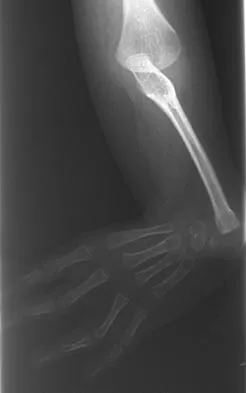
Figures 36a and 36b show the radiographs of a 3-year old child who has a congenital upper extremity deformity. Which of the following features would be a major contraindication to a centralization procedure?
Explanation
The patient has bilateral absent radii or radial clubhand. Patients who lack elbow flexion take advantage of the hand position to reach their mouths, and a centralization procedure would take away that ability. This procedure can be performed on patients with partial to complete absence of the radius. A hypoplastic thumb can be addressed at a staged procedure; it does not represent a contraindication to centralization. Complete thumb absence can be addressed by pollicizing the index ray. Green DP: Operative Hand Surgery, ed 2. New York, NY, Churchill Livingstone, 1988, pp 269-271.
Question 70
Examination of a 4-year old child with obstetrical palsy reveals weak deltoids, pectoralis major strength of 4-5, and normal hand function. External rotation of the shoulder is limited. What is the most appropriate surgical procedure to restore external rotation?
Explanation
Transfer of the latissimus dorsi and teres major to the posterior rotator cuff will restore external rotation and some abduction. The procedure should be performed in children who are approximately age 4 years, following spontaneous recovery and prior to significant stiffness. External rotation osteotomy is more appropriate for an older child. Fusion should not be performed until skeletal maturity. Distal biceps rerouting restores pronation for a supination deformity. Latissimus dorsi and teres major transfer to the subscapularis would accentuate the internal rotation. In younger patients without significant bony deformity, a subscapularis slide or lengthening can restore external rotation. Strecker WB, McAllister JW, Manske PR, Schoenecker PL, Dailey LA: Sever-L'Episcopo transfers in obstetrical palsy: A retrospective review of twenty cases. J Pediatr Orthop 1990;10:442-444.
Question 71
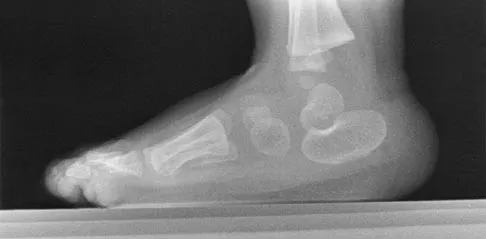
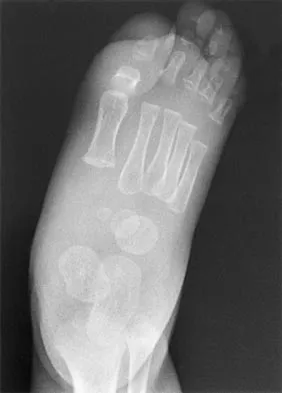
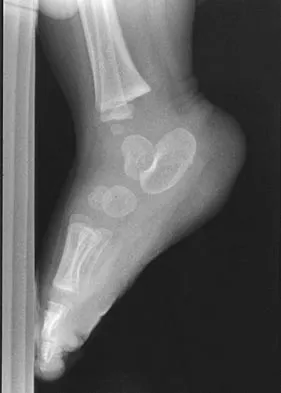
A 7-month-old girl has had a severe flatfoot deformity since birth. The talar head is prominent in the medial plantar arch of the foot. No other deformities of the spine or extremities are present. Motor and sensory examinations of the extremities are normal. Figures 37a through 37c show simulated weight-bearing AP and lateral radiographs and a planter flexion lateral view. What is the most likely diagnosis?
Explanation
Congenital vertical talus is a fixed dorsal dislocation of the talonavicular joint with equinus of the ankle joint. The AP radiograph shows valgus of the midfoot and an increased talocalcaneal angle; the lateral radiograph shows a vertically positioned talus and equinus of the ankle joint, and the plantar flexion lateral view shows that the talonavicular joint does not reduce. A line drawn through the long axis of the talus passes below the long axis of the first metatarsal. Initial management should consist of serial casting to stretch the dorsal soft-tissue structures; surgery eventually will be required to reduce the talonavicular joint. The differential diagnosis of congenital vertical talus includes pes calcaneovalgus, flexible pes planus, and peroneal spastic flatfoot. Pes calcaneovalgus, flexible pes planus, congenital short Achilles tendon, and peroneal spastic flatfoot would not show resistent dorsal dislocation of the navicular on the plantar flexion view. Kodros SA, Dias LS: Single-stage surgical correction of congenital vertical talus. J Pediatr Orthop 1999;19:42-48.
Question 72
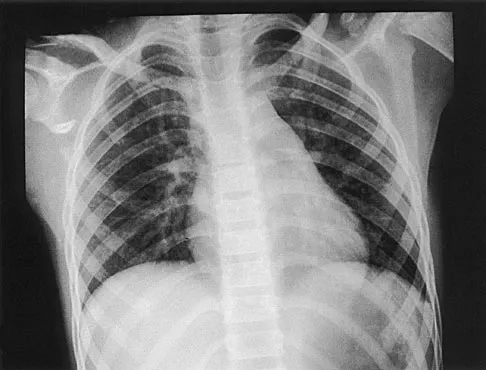
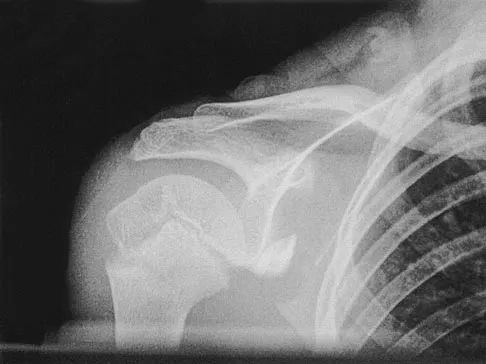
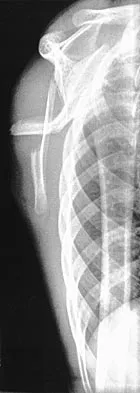
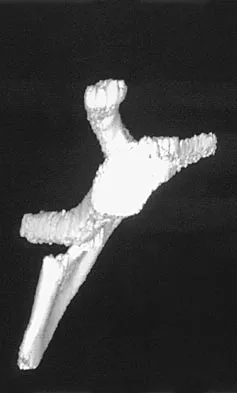
A 12-year-old boy has severe left shoulder pain after being struck by an automobile. A chest radiograph, AP and lateral radiographs, and a CT scan with three-dimensional reconstruction of the scapula are shown in Figures 38a through 38d. Management should consist of
Explanation
Scapular body fractures in children are rare and are often associated with other injuries of the chest and thorax. Management is generally nonsurgical, unless the injury is open, and usually consists of support with a sling and gentle range-of-motion exercises to minimize shoulder stiffness. Green N, Swiontkowski M: Skeletal Trauma in Children, ed 2. Philadelphia, PA, WB Saunders, 1998, vol 3, pp 319-341.
Question 73
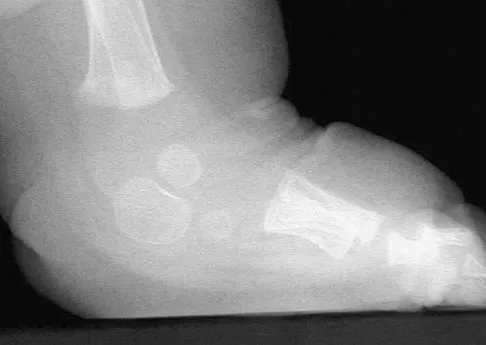
Figure 39 shows the radiograph of a 4-month old infant who has been undergoing weekly casting since birth for a congenital equinovarus deformity. Management should now consist of
Explanation
The radiograph shows the development of a rocker-bottom foot deformity. A rocker-bottom foot occurs in the treatment of clubfoot when casting is continued in the presence of a very tight gastrocnemius-soleus complex and an uncorrected hindfoot. While there are some preliminary reports on using Botox injection and continued casting for the equinus deformity, most authors recommend posterior or posterior medial release. Percutaneous tenotomy has been recently recommended with the resurgence of the Ponsetti technique. Lehman WB, Atar D: Complications in the management of talipes equinovarus, in Drennan JC (ed): The Child's Foot and Ankle. New York, NY, Raven Press, 1992, pp 135-136. Herring JA: Tachdjian's Pediatric Orthopedics, ed 4. Philadelphia, PA, WB Saunders, 2002, pp 927-935.
Question 74
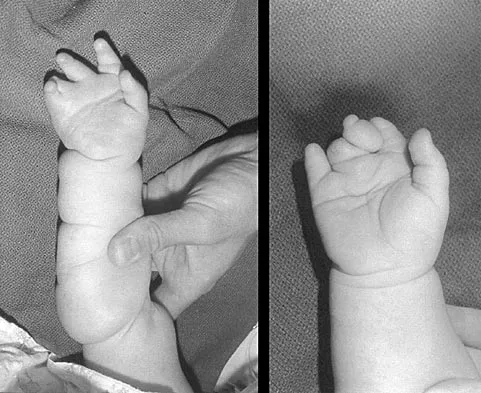
A 1-year-old infant has the hand deformities shown in Figure 40. What pathologic process is the most likely cause of these deformities?
Explanation
Streeter's dysplasia is clearly related to rupture of the amnion in utero and is now most commonly referred to as premature amnion rupture sequence. The deformities arise from amniotic bands that wrap about protruding parts and from uterine packing because of the accompanying oligohydramnios. Clubfoot can develop as a result of the latter mechanism. Three limb involvement is most commonly seen, along with syndactyly. Treatment involves resection of bands and Z-plasty of skin. The disease is not genetic and has not been related to teratogen exposure or to iatrogenic influences such as amniocentesis. Developmental field disruption is not seen in this disease, and the growth potential of the involved parts is normal unless neurovascular disruption has arisen from band formation.
Question 75
A 13-year-old girl with hallux valgus reports pain after playing basketball. Radiographs show a hallux valgus angle of 20 degrees, an intermetatarsal angle of 11 degrees, a distal metatarsal articular angle of 10 degrees, and a congruent joint. Management should consist of
Explanation
Shoe wear modification is the most appropriate management based on the patient's age, high activity level, and relatively minor symptoms. She also has a mild hallux valgus. Normal radiographic measurements are an intermetatarsal angle of less than 9 degrees, a hallux valgus angle of less than 15 degrees, and a distal metatarsal articular angle of less than 9 degrees. Surgical procedures should be reserved for patients with more severe or progressive deformities. Stephens HM: Bunions, in Fitzgerald RH, Kaufer H, Malkani AL (eds): Orthopaedics. St Louis, MO, Mosby, 2002, pp 1510-1519.
