00:00
Start Quiz
Question 76
A 4-year-old boy sustained a nondisplaced, but complete, fracture of the left proximal tibial metaphysis 1 year ago. The fracture healed uneventfully in an anatomic position. Examination of the injured extremity now reveals 18 degrees of valgus compared with 3 degrees of valgus on the opposite side. Management should now include
Explanation
The development of a valgus deformity after this type of fracture is a well-known occurrence, and the patient's parents should be informed about this risk. In a patient who is age 4 years, the natural history is one of gradual correction by the development of a physiologic varus deformity at the distal tibial physis; therefore, no active intervention is needed at this time. Bracing has no effect on the deformity, and the child is too young for any procedure on the growth plate. Proximal tibial osteotomy is reserved until the patient nears skeletal maturity because of the risk of recurrence of the deformity. Lateral stapling can be done near skeletal maturity if the deformity persists, but this is unlikely to be necessary. Zionts LE, MacEwen GD: Spontaneous improvement of posttraumatic tibia valga. J Bone Joint Surg Am 1986;68:680-687.
Question 77
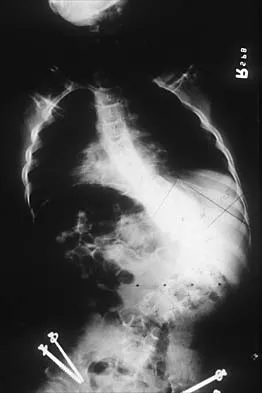
A 16-year-old boy with spastic quadriplegic cerebral palsy has been referred for evaluation and management of scoliosis. His parents report increasing problems with sitting balance, positioning, and hygiene because of the deformity. The radiograph shown in Figure 46 reveals a lordoscoliosis of 105 degrees with marked pelvic obliquity. Attempts at correcting the pelvic obliquity on supine bending radiographs show significant rigidity. Management should consist of
Explanation
Spinal stabilization is the treatment of choice in patients with severe scoliosis who have progressive positioning, sitting balance, and/or hygiene problems despite maximal nonsurgical management. Pelvic rigidity and marked frontal plane deformity necessitate anterior and posterior procedures so as to maximize correction and fusion. Weinstein SL (ed): The Pediatric Spine: Principles and Practice. New York, NY, Raven Press, 1994, pp 977-997.
Question 78
A 10-year-old boy reports a gradual onset of weakness; however, he is fully ambulatory. History reveals that he has a 17-year-old brother who has just stopped walking because of a similar condition. Laboratory studies show a creatine kinase level of 5,480 IU/L (normal 25 to 232 IU/L), and examination shows a slightly positive Gower sign. What is the most likely diagnosis?
Explanation
The patient has Becker muscular dystrophy. Patients with this condition have a slower rate of progression of disease compared with patients who have Duchenne muscular dystrophy, and walking may continue into the late teens. The creatine kinase level is not as high as in Duchenne muscular dystrophy, which can range from 20,000 to 30,000 IU/L. Becker muscular dystrophy is allelic to Duchenne muscular dystrophy, resulting in a mutation in the dystrophin gene. Myotonic dystrophy is characterized by a progressive inability to relax the muscles after contracture. The Gower sign is not helpful in this disease. Patients with Charcot-Marie-Tooth disease, one type of which is also known as HMSN type II, do not have elevated creatine kinase levels and usually present with a foot deformity. Spinal muscular atrophy, type II, usually presents with severe weakness in the second year of life. Matsuo M: From molecular diagnosis to gene therapy. Brain Dev 1996;18:167-172. Darras BT: Molecular genetics of Duchenne and Becker muscular dystrophy. J Pediatr 1990;117:1-15.
Question 79
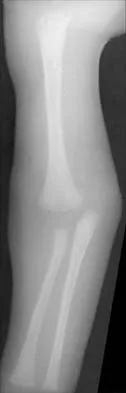
Figure 47 shows the radiograph of a 2-day-old girl who has been referred for swelling and limited use of the right upper extremity. The second of twins, the infant was breech and delivered with forceps at age 38 weeks, weighing 5.37 lb. Difficulty in moving the arm was noted shortly after birth. Examination shows no active motion of the shoulder, elbow, or wrist. Active finger flexion and extension are present. The elbow is mildly swollen, and passive motion shows lack of full extension of 20 degrees, lack of full flexion of 15 degrees, and no restriction of pronation or supination. What is the most likely diagnosis?
Explanation
Fractures involving the entire distal humeral physis may be a complication of a difficult delivery. Basing the diagnosis on radiographs can be difficult at this age because the secondary ossification center of the lateral condyle has not developed. The key to the diagnosis is the constant relationship of the radius and ulna, with medial and posterior displacement of the forearm relative to the humerus. An ultrasound can be obtained to confirm the diagnosis in newborns. Because the fracture is through cartilage, examination may reveal only mild swelling, and crepitation may be muffled or not apparent. The lack of apparent active motion of the shoulder, elbow, and wrist is secondary to pseudoparalysis. Child abuse is a common mechanism of this injury in a child who is age 1 month to age 3 years. Beaty JH, Wilkins KE: Fractures involving the entire distal humeral physis, in Rockwood CA, Wilkins KE, Beaty JH (eds): Fractures in Children, ed 4. Philadelphia, Pa, Lippincott-Raven, 1996, vol 3, pp 790-801. Dias JJ, Lamont AC, Jones JM: Ultrasonic diagnosis of neonatal separation of the distal humeral epiphysis. J Bone Joint Surg Br 1988;70:825-828.
Question 80
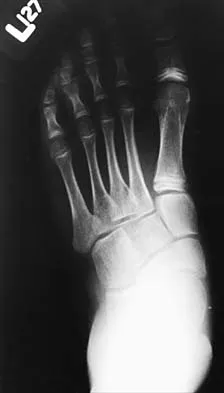
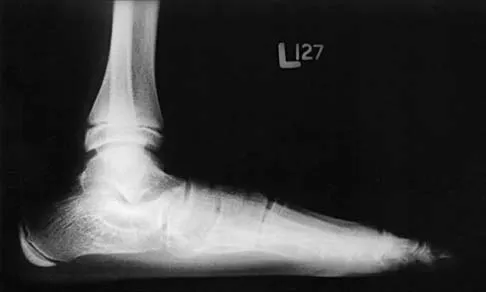
Examination of a 12-year-old girl with a painful flatfoot deformity reveals tenderness in the region of the sinus tarsi and no appreciable subtalar motion. Radiographs are shown in Figures 48a through 48c. Two attempts to relieve her symptoms by cast immobilization fail to relieve the pain. Management should now consist of
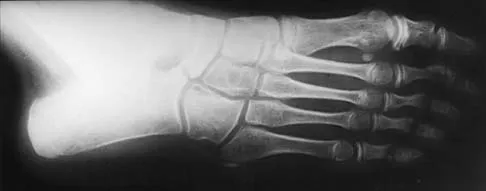
Explanation
Surgical treatment is indicated for a symptomatic tarsal coalition that has failed to respond to nonsurgical management. In this patient, the radiographs reveal a calcaneonavicular coalition and no degenerative changes. The patient is symptomatic, and two attempts at use of a short leg walking cast have failed to provide relief. For calcaneonavicular coalitions, good results have been reported following resection and interposition of the extensor digitorum brevis. A retrospective study of this procedure achieved good to excellent results in 58 of 75 feet (77%). Degenerative arthritis or persistent pain following resection of a coalition is a reasonable indication for a triple arthodesis. A medial closing wedge osteotomy of the calcaneus may be indicated for a rigid flatfoot with severe valgus deformity. There are no studies documenting the long-term effectiveness of a manipulation under general anesthesia for this condition. Gonzalez P, Kumar SJ: Calcaneonavicular coalition treated by resection and interpostion of the extensor digitorum brevis muscle. J Bone Joint Surg Am 1990;72:71-77.
Question 81
When counseling a patient with hypophosphatemic rickets, which of the following scenarios will always result in a child with the same disorder?
Explanation
Hypophosphatemic rickets is an inherited disorder that is transmitted by a unique sex-linked dominant gene. Therefore, if a male patient has a female offspring, his affected X chromosome will be transmitted and all of his female children will have hypophosphatemic rickets. All male offspring of a male patient will be unaffected. All offspring of a female patient have a 50% chance of having the disorder. Understanding the inheritance of hypophosphatemic rickets facilitates early diagnosis and early treatment. Medical treatment with phosphorus and some types of vitamin D (most authors recommend calcitriol) improves, but does not fully correct, the mineralization defect in hypophosphatemic rickets. However, if medical treatment is begun before the child begins walking, the growth plate is then adequately protected and a bowleg deformity will most likely be prevented. Evans GA, Arulanantham K, Gage JR: Primary hypophosphatemic rickets: Effect of oral phosphate and vitamin D on growth and surgical treatment. J Bone Joint Surg Am 1980;62:1130-1138.
Question 82
A 15-year-old boy with Duchenne muscular dystrophy has a progressive scoliosis that now measures 55 degrees. He is in foster care and is no longer ambulatory. Because posterior spinal fusion with instrumentation is the recommended treatment, the patient participates in a thorough discussion of the risks and benefits of the procedure. However, he refuses the surgery. The physician should now
Explanation
Traditionally, patients have been viewed as ignorant about medical matters and ill-equipped to determine what is in their best interest. This has been especially true for minors. However, recent informed consent policies are now based on the patient's right to self-determination. While most spinal surgeons would agree that spinal fusion improves pulmonary function, sitting balance, and comfort, they would also agree that this comes at considerable risk in a patient with compromised pulmonary function and ultimately, a terminal condition. With increasing frequency, young people older than age 14 years are gaining greater autonomy in decision making about their health care matters. This includes do not resuscitate orders when young patients are terminally ill, as well as in less serious situations. Surgery could be performed with the permission of the legal guardians; however, in this situation it is preferable to follow the patient clinically until he consents to surgery along with the legal guardians. Bracing is contraindicated. Reich WT (ed): Encyclopedia of Bioethics. New York, NY, Simon and Schuster, 1995, pp 1256-1265. Confidential health services for adolescents. Council on Scientific Affairs, American Medical Association. JAMA 1993;269:1420-1424.
Question 83
Figure 49 shows the radiograph of a 3-year-old child with progressive bowlegs. Laboratory studies show a calcium level of 9.5 mg/dL (normal 9.0 to 11.0 mg/dL), a phosphorus level of 4.2 mg/dL (normal 3 to 5.7 mg/dL), and an alkaline phosphatase level of 305 IU/L (normal 104 to 345 IU/L). What is the most likely diagnosis?
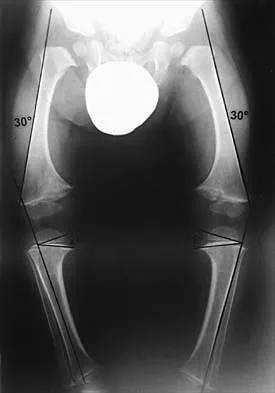
Explanation
The patient has bowlegs associated with very wide physes, particularly noted at the hips. The widening of the growth plates is a classic sign of rickets; however, the normal levels of calcium, phosphorus, and alkaline phosphatase rule out both nutritional and hypophosphatemic rickets. Patients with nutritional rickets or hypophosphatemic rickets have hypophosphatemia and increased alkaline phosphatase levels. Jansen metaphyseal dysostosis has very severe radiographic findings that are not found in this patient; however, these radiographic findings are classic for Schmid metaphyseal dysostosis. This disorder is caused by a mutation in the gene for type X collagen, which is found only in the growth plates of growing children. Lachman RS, Rimoin DL, Spranger J: Metaphyseal chondrodysplasia - Schmid type: Clinical and radiographic delineation with a review of the literature. Pediatr Radiol 1988;18:93-102.
Question 84
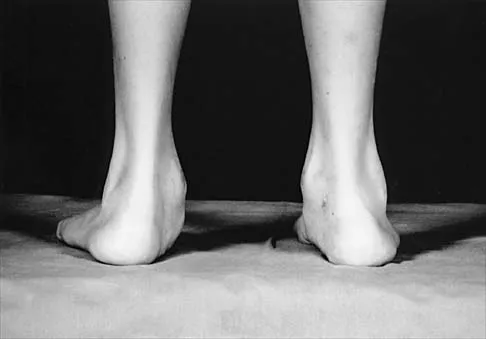
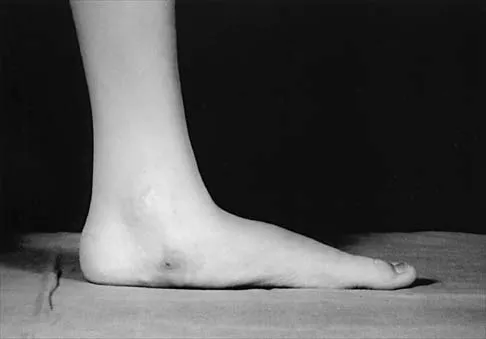
Figures 50a and 50b show the standing clinical photographs of a 12-year-old boy who has had increasing pain in the left foot for the past 9 months. He reports that the pain is activity related, aching in nature, and localized to the medial aspect of the midfoot and hindfoot. History reveals that he sustained a puncture wound located superior and posterior to the medial malleolus from a plate glass window 18 months ago. Examination reveals no restriction of ankle or subtalar motion, normal neurovascular status, no masses, and a well-healed 1.5-cm laceration posterior to the superior aspect of the medial malleolus. Inversion strength of the foot is decreased to grade 3/5. Radiographs of the foot show no bony abnormalities. Treatment should consist of
Explanation
The photographs show a planovalgus posture of the foot. The foot deformity and decreased inversion strength are secondary to laceration of the posterior tibial tendon 18 months ago. If the injury had been recognized acutely, optimal treatment would have consisted of repair of the tendon; however, contracture now precludes that possibility. Therefore, transfer of the flexor digitorum longus or flexor hallucis longus is the preferred treatment. In adults with posterior tibial dysfunction, the entire tendon is typically degenerated and the transfer must be anchored through a drill hole in the navicular. In this patient, the distal end of the posterior tibial tendon is a satisfactory insertion site. Lengthening osteotomy of the calcaneus could be combined with the tendon transfer if the patient had a fixed deformity of the foot. UCBL orthoses and an ankle-foot orthosis are not considered good long-term solutions for a 12-year-old patient. Mosca VS: Flexible flatfoot and skewfoot, in Drennan JC (ed): The Child's Foot and Ankle. New York, NY, Raven Press, 1992, pp 355-376.
Question 85
Which of the following clinical scenarios represents an appropriate indication for convex hemiepiphysiodesis/hemiarthrodesis in the treatment of a child with a congenital spinal deformity?
Explanation
Convex hemiarthrodesis and hemiepiphysiodesis are procedures designed to gradually reduce curve magnitude in congenital scoliosis because of hemivertebrae. They are used to surgically create an anterior and posterior bar to arrest growth on the convexity of the existing deformity. Success of the technique is predicated on continued growth on the concave side of the deformity. Prerequisites for this procedure include curves of limited length (less than or equal to five vertebrae), curves of reasonable magnitude (less than 70 degrees), absence of kyphosis, concave growth potential, and appropriate age (younger than age 5 years).
Question 86
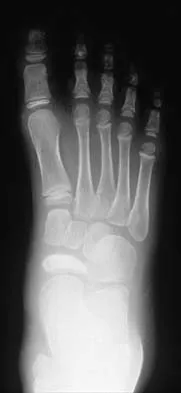
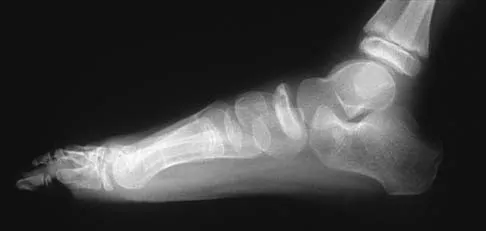
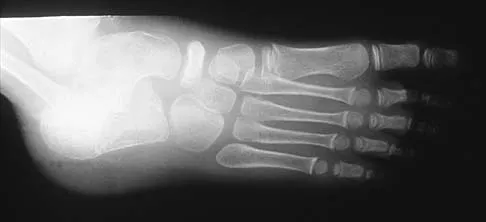
Figures 51a through 51c show the radiographs of a 7-year-old soccer player who reports a gradual onset of midfoot pain that began shortly after the start of soccer season. He states that the pain is worse with activity and is partially alleviated by rest. Examination reveals soft-tissue swelling, and tenderness and warmth in the region of the talonavicular and navicular cunieform joints. Management should consist of
Explanation
Osteochondrosis of the tarsal navicular (Kohler disease) is an infrequent cause of midfoot pain in children, and the etiology is unknown. The typical radiographic findings include flattening and irregular ossification of the tarsal navicular. The medial cunieform and talus maintain their normal articular contours. The acute process is best treated with rest and immobilization. A short leg walking cast results in relief of pain and a quicker return to activity compared with orthotics, although long-term success is similar with either method of treatment. Children may return to activities when the symptoms subside. The radiographic appearance of the talus begins to normalize by about 8 to 10 months following the onset of symptoms.
Question 87
A 10-year-old child with cerebral palsy undergoes bilateral hamstring lengthening for severe knee flexion contractures, and knee immobilizers are applied postoperatively. Examination at the initial postoperative check 2 hours after surgery reveals that she can dorsiflex her toes on the right foot, but not on the left foot. The physician should now
Explanation
Children with cerebral palsy are often difficult to examine. However, this patient clearly has a peroneal nerve deficit, most likely from the acute stretch after the hamstring lengthening. The nerve has the best chance of recovery if it is relaxed by flexing the knee. Once the nerve has recovered, gradual knee extension can be accomplished. Aspden RM, Porter RW: Nerve traction during correction of knee flexion deformity: A case report and calculation. J Bone Joint Surg Br 1994;76:471-473.
Question 88
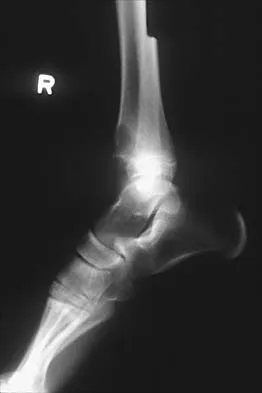
Figures 52a and 52b show the plain radiographs of a 12-year-old girl who has right distal leg pain. She reports that symptoms are present with weight-bearing activities and improve with rest. Examination reveals diffuse tenderness over the distal tibial metaphysis and mild swelling. A photomicrograph of the biopsy specimen is shown in Figure 52c. What is the most likely diagnosis?
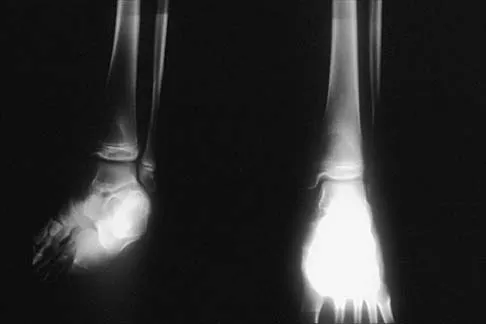
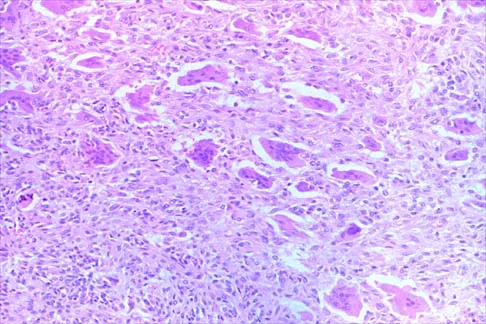
Explanation
This lytic lesion is in the epiphyseal-metaphyseal region of the distal tibia. The most common lesion in this area is a giant cell tumor. Although these lesions are most commonly seen in adults, they can also occur in the skeletally immature patient. The photomicrograph shows a lesion with multiple giant cells, the nuclei of which are similar to those in the background stroma; this finding is characteristic of giant cell tumors. Giant cells can be seen in many benign lesions, including aneurysmal bone cysts, Brown tumors, and eosinophilic granuloma. These lesions usually have fewer giant cells with less nuclei. The location of this lesion in the epiphyseal-metaphyseal area is not seen in aneurysmal bone cysts, unicameral bone cysts, Ewing's sarcoma, or eosinophilic granuloma.
Question 89
A 15-year-old boy with epilepsy who is treated with phenytoin sustains a vertebral compression fracture during a breakthrough seizure. Radiographs of the spine reveal generalized osteopenia. What is the most likely cause of the osteopenia?
Explanation
As a side effect of treatment, phenytoin induces osteomalacia, or rickets, in growing children, through interference with metabolism of vitamin D. Oral supplementation of vitamin D can minimize this effect in patients who are undergoing prolonged treatment with phenytoin.
Question 90
Figure 53 shows the pedigree of a family with an unusual type of muscular dystrophy. This pedigree is most consistent with what type of inheritance pattern?
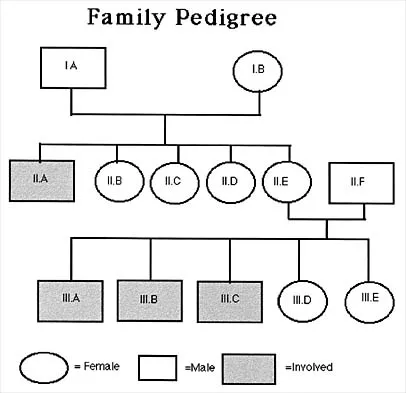
Explanation
The pedigree documents involvement of male offspring only, and it also shows transmission through an uninvolved female carrier. This inheritance pattern is most consistent with a x-linked recessive inheritance. It would be inconsistent with a dominant inheritance pattern unless there was incomplete penetrance. Autosomal-recessive inheritance would be possible only if the family member labeled II.F was also a carrier of the same gene; however, this is unlikely. Mitochondrial inheritance is possible, but as with autosomal patterns, mitochondrial inheritance normally affects both male and female offspring. It is transmitted only through the maternal line.
Question 91
Which of the following is considered the most accurate test to determine the amount of limb-length discrepancy in a patient with a knee flexion contracture of 35 degrees?
Explanation
Flexion contractures and angular deformities of a limb cause inaccurate limb-length measurement results with most clinical methods. A CT scanogram is more accurate than standard scanograms for determining limb length in patients with knee flexion contractures of 30 degrees or more. The cost and time necessary to complete the examinations are comparable, but the CT scanogram delivers only 20% of the radiation needed for standard scanograms. Aaron A, Weinstein D, Thickman D, Eilert R: Comparison of orthoroentgenography and computed tomography in the measurement of limb-length discrepancy. J Bone Joint Surg Am 1992;74:897-902.
Question 92
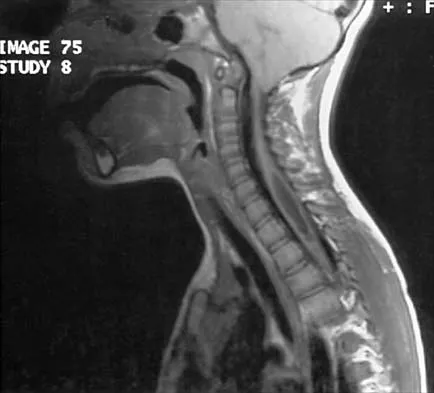
Figures 54a and 54b show the radiograph and MRI scan of a 7-year-old boy who has a painful right thoracic scoliosis that measures 35 degrees. Neurologic examination is normal. Management should consist of
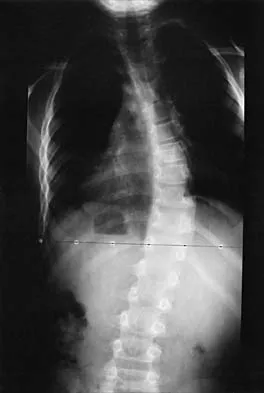
Explanation
Because hydrosyringomyelia, with or without an Arnold-Chiari malformation, is now being recognized as the etiology of many infantile and juvenile idiopathic scolioses, management should consist of a neurosurgical consultation. Observation with follow-up radiographs is not an option in curves of this magnitude. A technitium Tc 99m bone scan is unnecessary because the etiology of the curve has been identified. Although spinal fusion may be needed in the future, it should not be undertaken before the neurosurgical problem has been addressed. Zadeh HG, Sakka SA, Powell MP, Mehta MH: Absent superficial abdominal reflexes in children with scoliosis: An early indicator of syringomyelia. J Bone Joint Surg Br 1995;77:762-767. Schwend RM, Hennrikus W, Hall JE, Emans JB: Childhood scoliosis: Clinical indications for magnetic resonance imaging. J Bone Joint Surg Am 1995;77:46-53.
Question 93
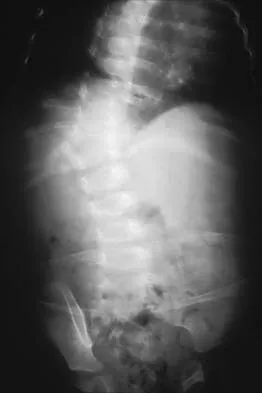
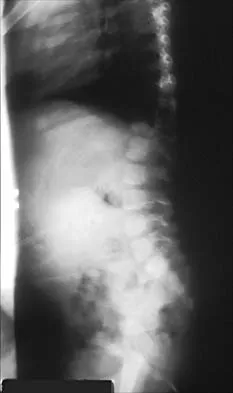
A 10-month-old girl has the spinal deformity shown in Figures 55a and 55b with no apparent neurologic finding. The next step in evaluation should be to obtain
Explanation
Approximately 60% of patients with a congenital spine abnormality have associated malformations outside the spinal column. Genitourinary abnormalities are probably the most common, occurring in up to 37% of patients. These are usually anatomic anomalies, such as renal agenesis, duplication, fusion, and ectopia. A genitourinary ultrasound is the least invasive screening tool. Other associated anomalies include cervical vertebral abnormalities, VATER syndrome, and intraspinal abnormalities such as diastematomyelia. An MRI scan is not recommended as part of the screening examination; however, if the patient had neurologic signs or symptoms, an MRI scan would be indicated. Beals RK, Robbins JR, Rolfe B: Anomalies associated with vertebral malformations. Spine 1993;18:1329-1332.
Question 94
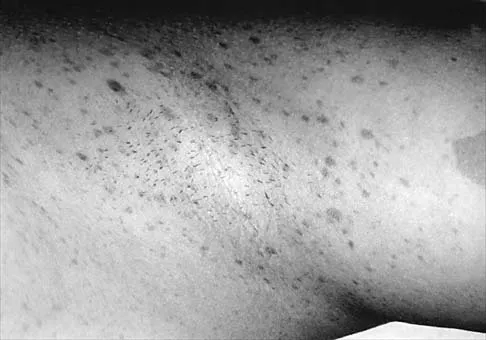
A 12-year-old girl has scoliosis at T5-T10 that measures 62 degrees. A clinical photograph of the axilla is shown in Figure 56. Management should consist of
Explanation
Neurofibromatosis type 1 (NF-1) is an autosomal-dominant disorder affecting about 1 in 4,000 people. NF-1 causes tumors to grow along various types of nerves and affects the development of non-nervous tissues, such as bone and skin. The gene for NF-1 is located on the long arm of chromosome 17 and codes the protein neurofibromin. Research indicates that NF-1 acts as a tumor-suppressor gene and, as such, plays an important role in the control of cell growth and differentiation. Axillary and inguinal freckling is considered a good diagnostic marker for NF-1. The hyperpigmented spots that measure from 2 mm to 4 mm may be congenital, but these typically appear and increase later in life. Scoliosis is the most common musculoskeletal disorder of NF-1. The curves are frequently dystrophic, kyphotic, and have a high risk of pseudarthrosis following spinal fusion. Anterior and posterior spinal fusion with rigid posterior segmental instrumentation is the treatment of choice. Goldberg Y, Dibbern K, Klein J, Riccardi VM, Graham JM Jr: Neurofibromatosis type 1: An update and review for the primary pediatrician. Clin Pediatr 1996;35:545-561.
Question 95
A 12-year-old girl has bilateral developmentally dislocated hips. History reveals no previous treatment, and she reports no discomfort. Good long-term clinical results are most likely to occur with
Explanation
The natural history of complete developmental dislocation of the hip is dependent on two factors: bilaterality and the presence or absence of a false acetabulum. Patients with bilateral dislocations may have low back pain because of hyperlordosis, but they tend to have less disability than patients with unilateral dislocations who have secondary problems related to limb-length inequality. Degenerative joint disease and clinical disability are most likely to develop in patients with completely dislocated hips and well-developed false acetabula. In a 12-year-old child who has bilateral developmental hip dislocations, it would be difficult to obtain surgical treatment results that are better than the natural history of the disorder. Abductor strengthening exercises are unlikely to influence the long-term outcome in this disorder. Surface replacements are not indicated in young asymptomatic patients. Weinstein SL: Natural history of congenital hip dislocation (CDH) and hip dysplasia. Clin Orthop 1987;225:62-76.
Question 96
Thyroid hormone regulates skeletal growth at the physis by stimulation of
Explanation
Children with hypothyroidism have delayed bone age, reduced thickness of the physis, disorganization of the cartilage columns of the physis, and impaired differentiation of proliferating chondrocytes into hypertrophic cells. As a result, these children have severe growth retardation, and slipped capital femoral epiphysis may develop because of mechanical weakening of the physis. Thyroid hormone regulates terminal differentiation of the growth plate chondrocytes, with a resultant increase in type X collagen and alkaline phosphatase. These substances are important factors in matrix mineralization. Insulin-like growth factors and FGF-2 appear to act synergistically to stimulate mitotic activity of the growth plate chondrocytes. TGF-beta= and PTHrP stimulate proteoglycan synthesis and mitotic activity of the chondrocytes and inhibit type X collagen and alkaline phosphatase activity. Ballock RT: Regulation of skeletal growth and maturation by thyroid hormone, in Buckwalter JA, Ehrlich MG, Sandell LJ, Trippel SB (eds): Skeletal Growth and Development: Clinical Issues and Basic Science Advances. Rosemont, Ill, American Academy of Orthopaedic Surgeons, 1998, pp 301-317. Rosier RN, O'Keefe RJ, Reynolds PR, Hicks DG, Puzas JE: Expression and function of TGF-beta= and PTHrP in the growth plate, in Buckwalter JA, Ehrlich MG, Sandell LJ, Trippel SB (eds): Skeletal Growth and Development: Clinical Issues and Basic Science Advances. Rosemont, Ill, American Academy of Orthopaedic Surgeons, 1998, pp 285-299.
Question 97
A newborn has an anterolateral bow of the tibia and a duplication of the great toe. Which of the following conditions will develop as the infant grows?
Explanation
Anterolateral bowing of the tibia is normally associated with congenital pseudarthrosis of the tibia. This, in turn, is associated with neurofibromatosis. Posterior bowing is more benign and usually corrects spontaneously. However, anterolateral bowing also corrects spontaneously, and the limb-length discrepancy may be the only remaining sequela when associated with duplication of the great toe. Lisch nodules and axillary freckling are pathognomonic findings in neurofibromatosis but would not be expected in this patient because this type of tibial deformity is not associated with neurofibromatosis.
Question 98
During stabilization of a slipped capital femoral epiphysis, the screw penetrates into the joint. The screw is repositioned so that it is within the femoral head. This transient penetration of the hip joint will most likely lead to
Explanation
Chondrolysis may be associated with unrecognized permanent penetration of the joint space by a pin or screw. However, transient penetration by the guide wire or screw is not associated with this problem. One study described 11 hips in which there was transient intraoperative penetration of the joint space by a guide wire or screw. These patients were followed for at least 2 years, with none showing any clinical or radiographic evidence of chondrolysis. Another retrospective study of 55 slipped epiphyses described 11 hips with transient intraoperative pin penetration, with none showing development of chondrolysis. There are no studies to suggest that transient pin penetration leads to osteonecrosis, stiffness, or premature physeal closure. Zionts LE, Simonian PT, Harvey JP Jr: Transient penetration of the hip joint during in situ cannulated-screw fixation of slipped capital femoral epiphysis. J Bone Joint Surg Am 1991;73:1054-1060.
Question 99
The mother of a 3-month-old infant states that she has difficulty positioning the infant's legs during diaper changes. Examination reveals limited abduction of both hips and a negative Ortolani sign. A radiograph reveals bilaterally dislocated hips. Initial management consists of guided reduction in a Pavlik harness, with weekly follow-up. Figures 57a and 57b show the radiograph and CT scan obtained after 6 weeks in the harness. Management should now consist of
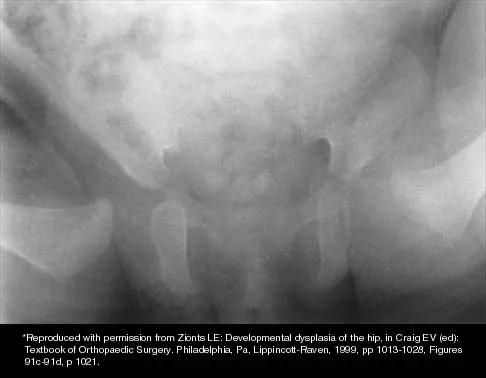
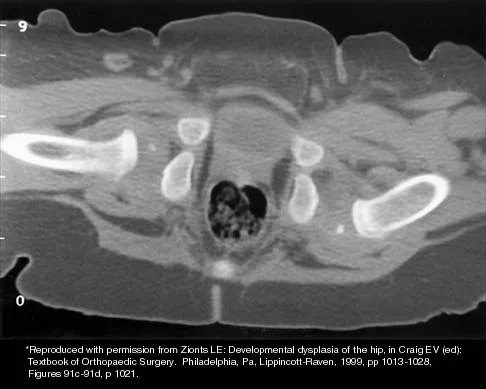
Explanation
In an infant younger than age 6 months with a complete dislocation of the hip that is not initially reducible, the Pavlik harness may be used for a trial of guided reduction. When the harness is used in these patients, the infant should be followed at weekly intervals to see if reduction has been achieved. If the hip does not reduce after 3 to 4 weeks of harness wear, the harness should be discontinued, and closed or open reduction should be considered to avoid secondary deformation of the posterolateral acetabulum, also known as Pavlik harness pathology. Changing to other abduction braces is not indicated. Jones GT, Schoenecker PL, Dias LS: Developmental hip dysplasia potentiated by inappropriate use of the Pavlik harness. J Pediatr Orthop 1992;12:722-726. Atar D, Lehman WB, Grant AD: Pavlik harness pathology. Isr J Med Sci 1991;27:325-330.
Question 100
A 6-year-old boy with severe spastic quadriplegic cerebral palsy is nonambulatory. Examination reveals 10 degrees of hip abduction on the left and 30 degrees on the right with the hips and knees extended. The Thomas test shows 20 degrees of flexion bilaterally, and Ely test results are 3+/4 bilaterally. Radiographs show a center edge angle of 0 degrees on the left and -10 degrees on the right. The neck shaft angles are 170 degrees bilaterally. Which of the following procedures would offer the best results?
Explanation
The patient has bilateral subluxated hips, with nearly vertical neck shaft angles; therefore, the treatment of choice is varus derotation osteotomy. Shortening of the bone on one or both sides may be necessary to allow adequate range of motion postoperatively. In patients this age and with this degree of bony deformity, soft-tissue releases are not likely to lead to hip stability. Botulinum toxin has been shown to be effective in the treatment of ankle equinus, but its efficacy in other areas has not been demonstrated as yet. The indications for obturator neurectomy are unclear at present. Proximal femoral resection is a salvage procedure for long-standing hip dislocations that are symptomatic and not reconstructable. Tylkowski CM, Rosenthal RK, Simon SR: Proximal femoral osteotomy in cerebral palsy. Clin Orthop 1980;151:183-192.
