00:00
Start Quiz
Question 26
Figure 17 shows the radiograph of a 2-year-old girl who sustained a fracture of the femur in a fall while walking with her parents. History reveals that this is her third long bone fracture, having sustained a humerus fracture 1 year ago and a fracture of the opposite femur 9 months ago. There is no family history of any similar problem. Examination reveals distinctly blue sclerae, normal appearing teeth, and no skin lesions. What is the most likely cause of this patient's disorder?
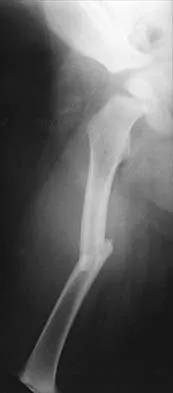
Explanation
Osteogenesis imperfecta (OI) is a genetically determined disorder of type I collagen synthesis that is characterized by bone fragility. This patient has had three fractures of the long bones by age 2 years, with the last one occurring after relatively minor trauma. The patient's history and clinical features are consistent with a diagnosis of Sillence type IA OI. Type I OI is the mildest and most common form. Inheritance is autosomal-dominant; however, as in this patient, new mutations are frequent. Type I is subclassified into the A type (absence of dentinogenesis imperfecta) and B type (presence of dentinogenesis imperfecta). The sclerae are blue, and the first fractures usually occur in the preschool years after walking has begun. Cells from individuals with type I OI largely demonstrate a quantitative defect of type I collagen; they synthesize and secrete about half the normal amount of type I procollagen. Qualitative mutations that lead to an abnormal type I procollagen molecule result in more severe types of the disorder. There are no indications that this child has been abused. Radiographs of the femur show no evidence of rickets, pyknodysostosis, or osteopetrosis. Morquio syndrome, characterized by excess excretion of keratin sulfate in the urine, is not associated with bone fragility. Kocher MS, Shapiro F: Osteogenesis imperfecta. J Am Acad Orthop Surg 1998;6:225-236. Sillence DO, Senn A, Danks DM: Osteogenesis imperfecta: An expanding panorama of variants. Clin Orthop 1981;159:11-25.
Question 27
An 8-year-old boy with severe hemophilia A (factor VIII) and no inhibitor is averaging eight transfusions per month for bleeding into the right ankle. Examination shows synovial hypertrophy; range of motion consists of 0 degrees of dorsiflexion and 20 degrees of plantar flexion. The patient's knees, elbows, and left ankle have no restriction of motion. Standing radiographs of the right ankle are shown in Figure 18. Management should consist of
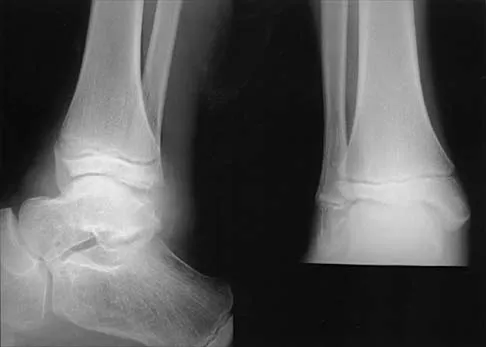
Explanation
The patient has bilateral hypertrophic synovitis that is causing repeated hemarthroses and progressive arthropathy. Ankle synovectomy in patients with hemophilia is effective in significantly reducing the rate of joint bleeding and in slowing the progression of the arthropathy; therefore, bilateral synovectomies is the treatment of choice. Range of motion can be effectively maintained after ankle synovectomy. Bracing and prophylactic transfusions would be ineffective at this time. Ankle arthrodesis should be reserved for patients with severe pain. Compared with patients who have juvenile rheumatoid arthritis, patients with hemophilia generally do not have involvement of the subtalar joint and rarely require a pantalar arthrodesis. Greene WB: Synovectomy of the ankle for hemophilic arthropathy. J Bone Joint Surg Am 1994;76:812-819.
Question 28
Figures 19a through 19c show radiographs of the cervical spine of an asymptomatic patient with Down syndrome who wants to participate in a Special Olympics running event. The neurologic examination is normal. Management should consist of
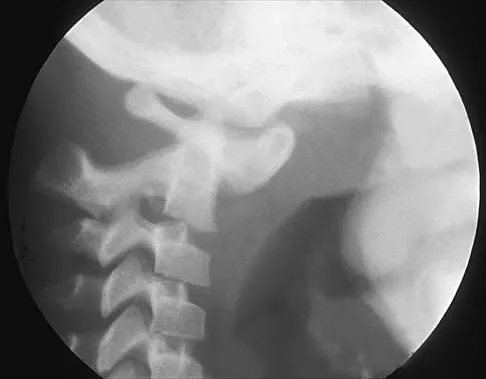
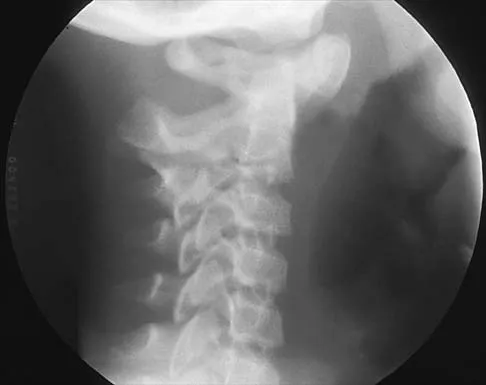
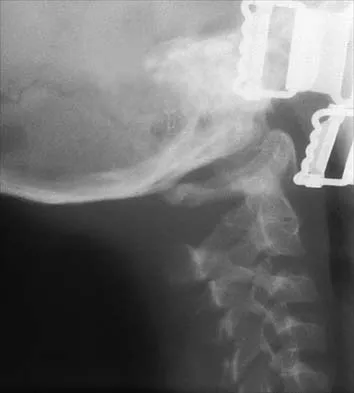
Explanation
An atlanto-dens interval (ADI) of up to 4 mm in children is considered normal. Children with Down syndrome have increased ligamentous laxity, with atlantoaxial instability occurring in as many as 15% to 20% of patients. These patients are at risk for catastrophic injury following minor trauma and should be routinely screened for instability, generally beginning when the patient starts to walk. Patients with an ADI of greater than 5 mm should avoid contact sports and high-risk activities such as gymnastics, diving, the high jump, and the butterfly stroke. The American Academy of Pediatrics Committee of Sports Medicine and Fitness guidelines recommend that lateral views of the cervical spine in neutral, flexion, and extension should be obtained in all children with Down syndrome who wish to participate in sports. Patients with normal radiographs and examinations do not need repeat radiographs, although some authors suggest that instability increases with age, and therefore recommend repeat radiographs every 5 years. Cervical spine fusion in patients with Down syndrome has a high rate of complications and should be performed only on patients with symptoms and evidence of myelopathy. American Academy of Pediatrics Committee of Sports Medicine and Fitness: Atlantoaxial instability in Down syndrome. Pediatrics 1995;96:151-154. Copley LA, Dormans JP: Cervical spine disorders in infants and children. J Am Acad Orthop Surg 1998;6:204-214.
Question 29
Compared with amputation, limb salvage for osteosarcoma of the distal end of the femur will result in
Explanation
Major advances in diagnostic imaging, neoadjuvant chemotherapy, and surgical techniques have allowed limb salvage to be performed as an alternative to amputation in children with osteosarcoma. The outcome of treatment of nonmetastatic, high-grade osteosarcoma of the distal femur was studied in 227 patients from 26 institutions. The authors found no difference in the long-term survival or quality of life between patients treated with limb salvage and those treated with amputation. Patients treated with limb salvage had a higher rate of reoperation, but a better functional outcome. Rougraff BT, Simon MA, Kneisl JS, Greenberg DB, Mankin HJ: Limb salvage compared with amputation for osteosarcoma of the distal end of the femur: A long-term oncological, functional, and quality-of-life study. J Bone Joint Surg Am 1994;76:649-656.
Question 30
Examination of a 7-year-old boy reveals 20 degrees of valgus following a lawn mower injury to the lateral femoral epiphysis. Treatment consists of total distal femoral epiphyseodesis and varus osteotomy. Following surgery, he has a limb-length discrepancy of 3 cm and 5 degrees of genu valgum. Assuming that he undergoes no further treatment, the patient's predicted limb-length discrepancy at maturity would be how many centimeters?
Explanation
The distal femoral epiphysis grows approximately 1 cm per year and in boys, growth ceases at approximately age 16 years. Therefore, the patient's limb-length discrepancy at maturity would be 12 cm (9 cm plus the 3-cm discrepancy he has from the previous surgery). Little DG, Nigo L, Aiona MD: Deficiencies of current methods for the timing of epiphyseodesis. J Pediatr Orthop 1996;16:173-179.
Question 31
When the iliac apophysis starts ossifying in the normal adolescent, growth of the sitting height or trunk height is characterized by
Explanation
Studies by Anderson and associates have resulted in a growth-remaining chart for sitting height that shows an increase of 3 to 5 cm in girls and an increase of 5 to 8 cm in boys. Future growth of the spine may impact brace longevity and fit. Anderson M, Hwang SC, Green WT: Growth of the normal trunk in boys and girls during the second decade of life: Related to age, maturity, and ossification of the iliac epiphyses. J Bone Joint Surg Am 1965;47:1554-1564.
Question 32
A 10-year-old girl was thrown over the handlebars of her bicycle and landed directly on her left shoulder. She was treated with a figure-of-8 strap and analgesics. Follow-up examination 2 weeks later reveals that the lateral end of the clavicle is superiorly dislocated relative to the acromion. A radiograph of the shoulder shows calcification lateral to the coracoid process at the level of the acromion, and the clavicle is superiorly displaced. Management should consist of
Explanation
In adults, a direct blow on the acromion usually results in an acromioclavicular dislocation. In children, however, the usual injury from this mechanism is a physeal fracture of the lateral clavicle. The clavicular shaft fragment, analogous to the metaphyseal portion of a physeal fracture, herniates through the periosteum, leaving the distal periosteal sleeve in contact with the lateral (distal) physeal fragment. The treatment of choice is immobilization until the patient is pain-free. Falstie-Jensen S, Mikkelsen P: Pseudodislocation of the acromioclavicular joint. J Bone Joint Surg Br 1982;64:368-369.
Question 33
Figures 20a and 20b show the radiographs of an obese 15-year-old boy who has severe left groin pain and is unable to bear weight following a minor injury. Treatment should consist of
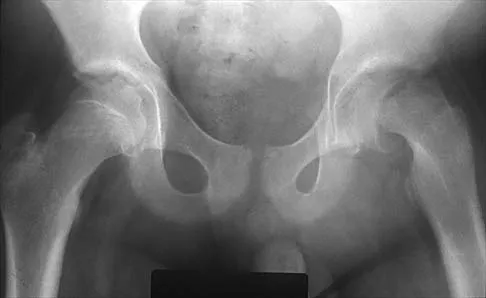
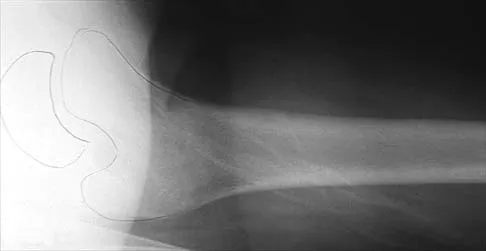
Explanation
The radiographs and history are consistent with an acute unstable slipped capital femoral epiphysis. Aronson and Loder documented an increased rate of osteonecrosis associated with manipulative reduction. They recommended bed rest with skin traction to allow the synovitis to resolve, followed by in situ pinning. They noted, however, that many of these slips reduced with anesthesia and positioning on a fracture table. Biomechanic studies have shown a slight increased resistance to shear stress when two screws are used, but it is unknown if this is significant in the clinical setting. Open epiphyseodesis does not provide postoperative stability; therefore, adjunctive fixation or immobilization is required. Numerous studies have noted the inadvisability of using multiple screws. Casting has a high rate of complications, including chondrolysis and progression of the slip. Aronson DD, Loder RT: Treatment of the unstable (acute) slipped capital femoral epiphysis. Clin Orthop 1996;322:99-110. Karol LA, Doane RM, Cornicelli SF, Zak PA, Haut RC, Manoli A II: Single versus double screw fixation for treatment of slipped capital femoral epiphysis: A biomechanical analysis. J Pediatr Orthop 1992;12:741-745.
Question 34
What is the recommended treatment of a skeletally immature 12-year-old boy who has an anterior cruciate ligament-deficient knee?
Explanation
Traditional surgeries for anterior cruciate ligament-deficient knees carry the potential risk of premature physeal closure in young athletes. Therefore, most surgeons are reluctant to recommend intra-articular reconstruction using bone tunnels with bone-patellar tendon-bone autografts or hamstring tendons. The current recommendation for young athletes is activity modification, rehabilitation, and functional bracing until the patient is near skeletal maturity. At that time, for the very symptomatic patient, the treatment of choice is intra-articular repair of the anterior cruciate ligament. If a skeletally immature patient continues to have instability despite rehabilitation and bracing, a modification of the femoral tunnel to the over-the-top position will not place the lateral femoral physis at risk for premature closure and deformity. A centrally placed tibial tunnel will minimize the risk of angular deformity and minimize limb-length discrepancy if physeal arrest occurs. Barry P: Anterior cruciate ligament injuries, in Andrews JR, Timmerman LA (eds): Diagnostic and Operative Arthroscopy. Philadelphia, Pa, WB Saunders, 1997, p 358. McCarroll JR, Shelbourne KD, Porter DA, Rettig AC, Murray S: Patellar tendon graft reconstruction for midsubstance anterior cruciate ligament rupture in junior high school athletes: An algorithm for management. Am J Sports Med 1994;22:478-484. Nottage WM, Matsuura PA: Management of complete traumatic anterior cruciate ligament tears in the skeletally immature patient: Current concepts and review of the literature. Arthroscopy 1994;10:569-573.
Question 35
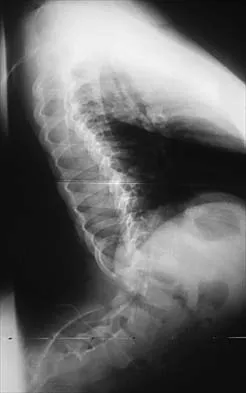
Figures 21a and 21b show the radiographs of a 12-year-old patient with an L4-level myelomeningocele who has scoliosis that has been slowly progressing for the past several years. There has been no loss of motor function. An MRI scan shows no syringomyelia or increased hydrocephalus. Management should consist of
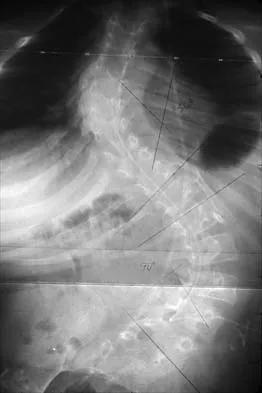
Explanation
Scoliosis is a common occurrence in children with myelomeningocele, with the incidence increasing as the neurologic level moves cephalad. The rate of pseudarthrosis for isolated anterior or posterior fusions has been reported as high as 75%. The combination of anterior and posterior fusions with some type of instrumentation has been shown to decrease the rate of pseudarthrosis to 20%. Brace treatment in smaller curves can be used as a temporizing measure to delay surgery, but as with idiopathic scoliosis, the brace is ineffective for larger curves. Observation is not indicated with a curve of this magnitude. Ward WT, Wenger DR, Roach JW: Surgical correction of myelomeningocele scoliosis: A critical appraisal of various spinal instrumentation systems. J Pediatr Orthop 1989;9:262-268.
Question 36
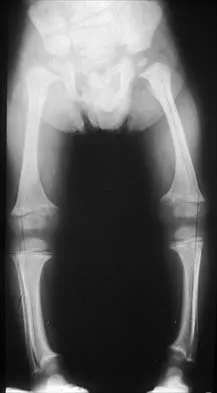
A 3-year-old child is referred for evaluation of bowed legs. History reveals no dietary deficiencies; however, family history is significant for several members with bowed legs. Examination reveals genu varum, and the child is in the 5th percentile for height and weight. Laboratory studies show normal renal function, a normal calcium level, a decreased phosphate level, and an elevated alkaline phosphatase level. A plain radiograph of the lower extremities is shown in Figure 22. What is the most likely diagnosis?
Explanation
The differential diagnosis of genu varum includes physiologic genu varum, Blount's disease, skeletal dysplasia, and metabolic bone disease. Children with Blount's disease are generally in the 95th percentile for height and weight, and usually multiple family members are not affected. The radiographs show widening of the physis and metaphyseal flaring. In Blount's disease, the characteristic radiographic changes involve only the tibia, and at this age, most commonly show beaking of the medial metaphysis. Skeletal dysplasias, such as chondrometaphyseal dysplasia, are associated with short stature, and the radiographic changes are similar to those seen here. However, laboratory studies in these children will be within normal limits. Children with chronic renal disease will often be of short stature, and the radiographic findings are again similar to those shown here. However, BUN and creatinine levels are elevated and phosphate levels are elevated rather than decreased in children with renal disease. The absence of dietary deficiencies and positive family history rules out vitamin D-deficient rickets. There are four types of vitamin D-resistant rickets: failure of production of 1,25-dihydroxy vitamin D, phosphate diabetes (hypophosphatemic rickets), end organ insensitivity to vitamin D, and renal tubular acidosis. All types of vitamin D-resistant rickets are resistant to treatment with physiologic doses of vitamin D. The patient's clinical picture, family history, laboratory studies, and radiographs are most consistent with hypophosphatemic rickets. This entity is inherited as a sex-linked dominant trait. Evans GA, Arulanantham K, Gage JR: Primary hypophosphatemic rickets: Effect of oral phosphate and vitamin D on growth and surgical treatment. J Bone Joint Surg Am 1980;62:1130-1138. Loeffler RD Jr, Sherman FC: The effect of treatment on growth and deformity in hypophosphatemic vitamin D-resistant rickets. Clin Orthop 1982;162:4-10. Loder RT, Johnston CE II: Infantile tibia vara. J Pediatr Orthop 1987;7:639-646.
Question 37
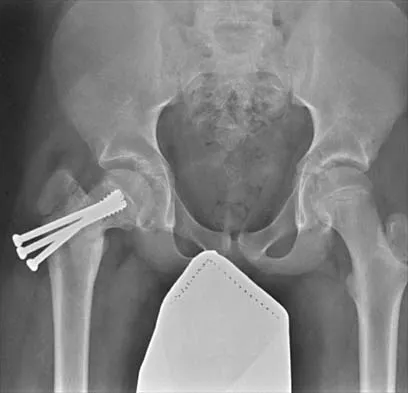
A 14-year-old boy sustained a femoral neck fracture in a fall from a tree and underwent open reduction and internal fixation 6 months ago. Follow-up examination now reveals an antalgic Trendelenburg gait and painful range of motion. A radiograph is shown in Figure 23, and a CT scan shows a nonunion. Treatment should consist of
Explanation
The coxa vara deformity and fracture nonunion should be treated simultaneously; therefore, the treatment of choice is curettage of the nonunion, intertrochanteric valgus osteotomy, and revision internal fixation. In addition, valgus osteotomy will convert the shear forces across the nonunion to compression, aiding in healing of the nonunion. None of the other procedures addresses both issues, and hip fusion is inappropriate under these conditions. Lam SF: Fractures of the neck of the femur in children. J Bone Joint Surg Am 1971;53:1165-1179.
Question 38
A 22-month-old child has scrapes and bruises on his head and a severe deformity of the forearm after being thrown from a car as an unrestrained passenger in a motor vehicle accident. Examination reveals a Glasgow Coma Scale score of 12. Prior to treatment of the forearm, management should include
Explanation
As CT scanning has become available, the use of radiographs of the skull has decreased in importance for evaluation of head trauma. The indications for CT scanning for suspected head trauma include any degree of obtundation, focal neurologic deficit, history of a high-velocity injury, amnesia for the injury, progressive headache, persistent vomiting, children younger than age 2 years, serious facial injury, posttraumatic seizure, skull penetration, or a Glasgow Coma Scale score of 13 or less. Evidence of improved outcome with use of steroids in head trauma is lacking. Steroids are useful for increased intracranial pressure caused by brain tumors or abscesses. High-dose IV methylprednisolone is indicated for spinal cord trauma and improves the ultimate degree of recovery of function. When herniation is suspected in a patient with asymmetric neurologic findings or the patient's condition is deteriorating rapidly, a mannitol infusion may be used. Hall DE: Head injuries, in Hoekelman RA (ed): Primary Pediatric Care. St Louis, Mo, Mosby, 1997, pp 1709-1712. Nelson WE, Behrman RE, Kliegman RM (eds): Nelson Essentials of Pediatrics. Philadelphia, Pa, WB Saunders, 1998, p 712.
Question 39
Examination of a 5-year-old boy with amyoplasia shows a flexion contracture of 70 degrees of the right knee. The active arc of motion is from 70 degrees to 90 degrees, and the opposite knee has a flexion contracture of 10 degrees. Both hips are dislocated with flexion contractures of 10 degrees, passive hip motion is from 10 degrees to 90 degrees of flexion, and the feet are plantigrade and easily braceable. Despite a daily stretching program, the parents and physical therapists note that it is increasingly difficult for him to walk because of the flexion contracture of the right knee. Management of the knee flexion contracture should now include
Explanation
Most children with amyoplasia are ambulatory and when a decrease in function occurs because of a severe contracture, it must be addressed. A radical posterior soft-tissue release, including the posterior knee capsule and often the collateral ligaments and the posterior cruciate ligament, is needed to obtain extension. After the age of 1 year, aggressive physical therapy will do little to correct a contracture. Botulinum toxin A is indicated for spasticity and is contraindicated with severe contractures. Supracondylar femoral extension osteotomy works well, but will remodel at an average rate of 1 degree per month, which is not considered ideal in a young patient. Gradual correction with a circular ring external fixator is an option, but a soft-tissue release will also most likely be needed for a contracture of this severity. Sarwark JF, MacEwen GD, Scott CI Jr: Amyoplasia (a common form of arthrogryposis). J Bone Joint Surg Am 1990;72:465-469. DelBello DA, Watts HG: Distal femoral extension osteotomy for knee flexion contracture in patients with arthrogryposis. J Pediatr Orthop 1996;16:122-126.
Question 40
A 13-year-old girl who is 2 years postmenarche has been referred for management of scoliosis. She denies any history of back pain. Radiographs show a right thoracic curve of 35 degrees. She has a Risser sign of 4 and a bone age of 15.5 years. Management should consist of
Explanation
Because the patient is skeletally mature with a curve of less than 40 degrees, there is no benefit to bracing and surgery is not indicated. Management should consist of observation and follow-up radiographs in 6 months. Lonstein JE, Carlson JM: The prediction of curve progression in untreated idiopathic scoliosis during growth. J Bone Joint Surg Am 1984;66:1061-1071.
Question 41
In children with isolated zone II lacerations of the flexor tendon, poor digital motion is best correlated with
Explanation
In a recent study on restoration of motion following zone I and zone II flexor tendon repairs in children, age was found to have no effect on the results of zone II tendon repairs. Early passive motion offered no better results than immobilization for 3 weeks. Immobilization for more than 4 weeks correlated with poorer results.
Question 42
In a longitudinal study of children with spastic diplegia, analysis of long-term function will most likely reveal
Explanation
In a longitudinal study of 18 patients with spastic diplegia over a period of 32 months, three-dimensional gait analysis revealed a deterioration of gait stability with increases in double support time and decreases in single support time. Kinematic data also identified a loss of excursion about the knee, ankle, and pelvis. Interestingly, the static examination of the children showed a decrease in the popliteal angle over time. The authors concluded that ambulatory ability tends to worsen over time in children with spastic diplegia.
Question 43
Examination of a 7-year-old girl with myelomeningocele reveals calcaneal deformities of both feet. She ambulates on both extremities wearing ankle-foot orthoses and has no upper extremity aids. She has grade 5/5 motor strength to the tibialis anterior muscles and absent motor strength to the triceps surae. There is no varus or valgus deformity of the hindfoot, and the skin over the heels is intact; however, mild callosities are present. Management should consist of
Explanation
A calcaneal deformity of the foot may occur in children who have low lumbar myelomeningocele. Strong dorsiflexors overcome a weak or absent gastrocnemius-soleus complex, leading to downward growth of the calcaneal apophysis. The deformity is usually progressive and does not respond to nonsurgical management. Most authorities recommend transfer of the tibialis anterior muscle through the interosseous membrane to the posterior aspect of the calcaneus. This procedure has been reported to be effective in limiting progression of the deformity. An extra-articular subtalar arthodesis, a treatment option for valgus deformity of the hindfoot, is not indicated. Similarly, Achilles tendon tenodesis to the fibula, an option for managing valgus of the ankle, is not indicated. Calcaneal osteotomy may be used in older children with severe calcaneal deformity. Stott NS, Zionts LE, Gronley JK, Perry J: Tibialis anterior transfer for calcaneal deformity: A postoperative gait analysis. J Pediatr Orthop 1996;16:792-798.
Question 44
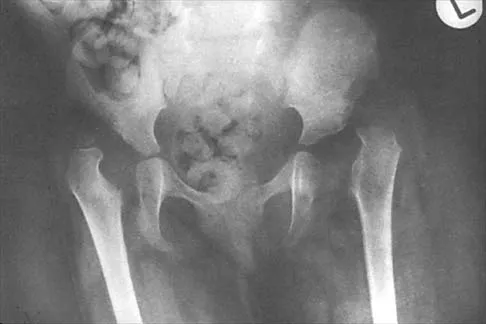
Figure 24 shows the radiograph of a 4-year-old girl with spina bifida. Examination reveals an L3 motor level, excellent sitting and standing balance, and satisfactory range of motion at the hips. Management should consist of
Explanation
Children with spina bifida and bilateral symmetrical dislocation of the hips usually do not require treatment. A level pelvis and good range of motion of the hips are more important for ambulation than reduction of bilateral hip dislocations. Because the patient has good sitting and standing balance and good range of motion, maintenance of that range of motion and symmetry is more important than reduction. Surgery is not recommended.
Question 45
Posterior spinal fusion for scoliosis should be performed on a patient with Duchenne muscular dystrophy when
Explanation
Progressive scoliosis develops in most patients with Duchenne muscular dystrophy. The onset of spinal deformity typically follows the cessation of walking, and curves can be expected to progress about 10 degrees per year. Posterior spinal fusion with instrumentation should be performed as soon as a curve of 25 degrees or greater is documented and before deterioration of pulmonary function (a FVC of less than 30%) precludes surgery. Patients with kyphotic posture tend to progress more rapidly than those with lordotic posture. Brace treatment is contraindicated because it is not definitive and it may mask curve progression while pulmonary function is concomitantly worsening. Beaty JH (ed): Orthopaedic Knowledge Update 6. Rosemont, Ill, American Academy of Orthopaedic Surgeons, 1999, pp 635-651.
Question 46
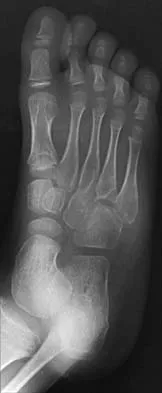
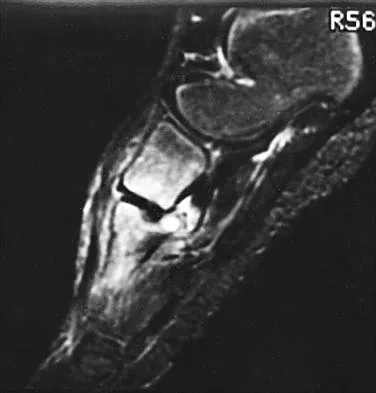
Figures 25a and 25b show the radiograph and MRI scan of a 7 1/2-year-old boy who has been limping for 1 year. His pain has worsened over the past 2 weeks, and his parents note swelling over the dorsum of the foot for the past 4 days. Examination reveals no fever, and laboratory studies show a WBC of 6,700/mm3, an erythrocyte sedimentation rate of 26 mm/h, and a normal C-reactive protein level. What is the most likely diagnosis?
Explanation
The diagnosis of tuberculous osteomyelitis in children is often delayed. In one series of 23 children, the average interval between the onset of symptoms and definite diagnosis was 4.3 months. In these patients, the presenting signs and symptoms were found to be mild, with the most common signs being localized swelling (69.6%) and a painful disability of the involved limbs (65.2%). A mild elevation of the erythrocyte sedimentation rate may be present, but the C-reactive protein level is usually normal. In patients who have osteoarticular tuberculosis, an MRI scan generally shows large intra-articular effusions, periarticular osteoporosis, and gross thickening of the synovial membrane. Differential diagnosis between tuberculosis and pyogenic arthritis is difficult, and an accurate diagnosis usually requires biopsy of synovial tissue. Aspiration of synovial fluid often results in insufficient information to make a diagnosis. Treatment generally consists of surgical debridement and combined antituberculous chemotherapy with isoniazid, ethambutol, and rifampin. Wang MN, Chen WM, Lee KS, Chin LS, Lo WH: Tuberculous osteomyelitis in young children. J Pediatr Orthop 1999;19:151-155.
Question 47
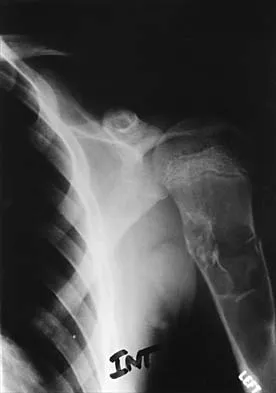
A 10-year-old boy who plays baseball reports acute pain after throwing a softball from the outfield to second base. A radiograph is shown in Figure 26. Management should consist of
Explanation
The patient has a fracture through a unicameral bone cyst, as evidenced by the "falling leaf" sign on the radiograph. Following healing of the fracture, treatment should consist of corticosteroid injection or bone marrow injection. Some cysts heal with the fracture and do not require injections. Biopsy is unnecessary because the radiograph shows that the cyst is benign. Curettage and bone grafting are seldom necessary because these cysts regularly heal with injections. Corticosteroids are useful when injected into the cyst, but are not used systemically. Pulsed electromagnetic fields have not been used therapeutically in this condition.
Question 48
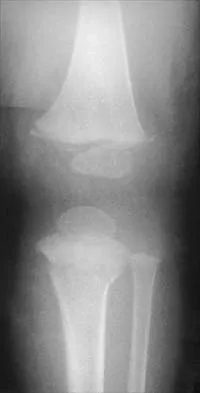
The mother of an otherwise healthy 1-month-old infant reports that he is not moving his left leg after falling from his high chair 2 days ago. He has a temperature of 99.5 degrees F (37.5 degrees C). Examination reveals that the left thigh is moderately tender to palpation. Because the infant is apprehensive, range of motion is difficult to quantify, but appears to be normal at the hips and ankles. Range of motion of the left knee is approximately 25 degrees to 90 degrees. A radiograph of the leg is shown in Figure 27. Management should consist of
Explanation
The patient has a bucket-handle fracture of the distal femur with bilateral corner fractures of the distal femur and a transverse fracture of the proximal tibia. These fractures are virtually pathognomonic of child abuse. The infant should be admitted to the hospital, and child protection services should be notified for investigation of possible abuse. A skeletal survey should be obtained, along with laboratory studies that include a CBC, a platelet count, a prothrombin time, a partial thromboplastin time, and a bleeding time. Akbarnia BA: The role of the orthopaedic surgeon in child abuse, in Morrissy RT, Weinstein SL (eds): Lovell & Winter's Pediatric Orthopaedics, ed 4. Philadelphia, Pa, Lippincott-Raven, 1996, pp 1315-1334.
Question 49
A 12-year-old girl with juvenile rheumatoid arthritis (JRA) has had chronic pain and synovitis about the knee that is now well-controlled medically. Examination reveals 20 degrees of valgus at the knee. Knee range of motion shows 10 degrees to 90 degrees of flexion. Treatment should consist of
Explanation
Children with JRA frequently have valgus in association with hypervascularity because of chronic inflammation. This is normally caused by overgrowth of the medial femoral epiphysis. Staple hemiepiphyseodesis, if done early, can reverse the deformity. Osteotomy is usually unnecessary at this age, and there is a risk of stiffness of the knee following the procedure. Synovectomy may be helpful but will not prevent or correct a deformity.
Question 50
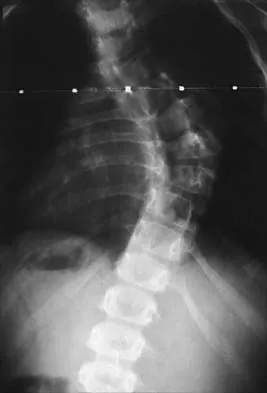
Figure 28 shows the radiograph of a 6-year-old girl who has a right thoracic scoliosis that measures 60 degrees. Examination shows multiple cafe-au-lait spots, and family history reveals that the child's mother has the same disorder. The gene responsible for this disorder codes for
Explanation
The patient has the dystrophic type of scoliosis seen in patients with neurofibromatosis type I (NF-1). The NF-1 gene is located on chromosome 17 and codes for neurofibromin, believed to be a tumor-suppresser gene. Abnormalities in the dystrophin gene are seen in Duchenne muscular dystrophy and Becker muscular dystrophy. A mutation in the frataxin gene is responsible for Friedreich ataxia. The most common type of hereditary motor and sensory neuropathy (Charcot-Marie-Tooth), HMSN type IA is caused by a complete duplication of the peripheral myelin protein gene. A defect in the cellular sulfate transport protein results in undersulfation of proteoglycans seen in diastrophic dysplasia.
