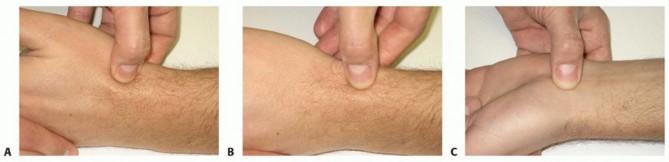
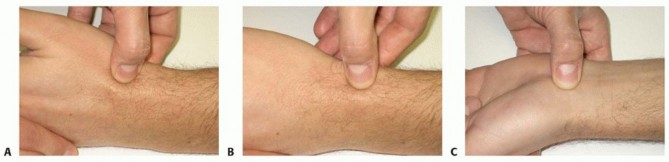
7 Effective Ways to Fix Your Finger Sprain Fast (With Pictures)
Key Takeaway
In this comprehensive guide, we discuss everything you need to know about 7 Simple Ways to Fix Your Finger Sprain: Heal Fast & Easy. Effective ways to fix finger sprains involve immediate R.I.C.E. therapy: Rest the injured finger, apply ice for 10-15 minutes, compress it, and elevate to reduce swelling. Over-the-counter anti-inflammatory medications or topical creams can manage pain and inflammation. For severe symptoms like unnatural bending, extreme swelling, or discoloration, consult a doctor immediately to prevent complications.
Introduction and Epidemiology
Ligamentous injuries of the digits, colloquially categorized as finger sprains, encompass a highly variable spectrum of soft tissue disruptions affecting the interphalangeal and metacarpophalangeal joints of the hand. While frequently dismissed by patients as minor or self-limiting trauma, these injuries possess a profound potential to cause enduring functional impairment, chronic pain, and debilitating joint stiffness if not subjected to rigorous clinical evaluation and precise management. Because the human hand relies on an exquisitely balanced biomechanical envelope to execute both fine motor tasks and powerful grip, an algorithmic, meticulous approach to diagnosis and intervention is mandatory for the orthopedic or hand surgeon.
Epidemiologically, ligamentous disruptions of the hand are ubiquitous across both athletic and occupational demographics. They are predominantly sustained via contact sports, occupational hazards, or falls onto an outstretched hand (FOOSH), subjecting the digit to sudden axial loading, torsional stress, or forced hyperextension. The proximal interphalangeal (PIP) joint represents the most frequently injured articulation in the hand, largely due to its exposed position and its role as the primary fulcrum for digital flexion. Additionally, acute rupture of the ulnar collateral ligament (UCL) of the thumb metacarpophalangeal (MCP) joint—historically termed "gamekeeper's thumb" or "skier's thumb"—constitutes a highly prevalent and clinically critical injury pattern. Conversely, isolated sprains of the distal interphalangeal (DIP) joint are comparatively rare, owing to the short lever arm of the distal phalanx and the robust stabilization provided by the terminal extensor and flexor digitorum profundus (FDP) tendons.
The diagnostic imperative lies in differentiating a stable, partial ligamentous sprain (Grade I or II) from a complete, structurally unstable rupture (Grade III) that may necessitate operative repair. The acute clinical presentation is typically characterized by localized edema, ecchymosis, fusiform swelling, and exquisite point tenderness over the affected ligamentous footprint. Evaluating the degree of functional deficit—ranging from mild guarding to a complete inability to generate pinch or grip strength—is essential for prognosticating and formulating a treatment algorithm.

The Eaton and Littler classification system remains the foundational orthopedic framework for evaluating PIP joint injuries, specifically addressing volar plate avulsions and complex fracture-dislocations.
* Type I: Involves a hyperextension injury resulting in a partial tear or longitudinal split of the volar plate without frank dislocation. The joint remains stable through a full active range of motion.
* Type II: Characterized by a complete avulsion of the volar plate from its distal insertion at the base of the middle phalanx, often accompanied by a transient dorsal dislocation. The joint typically reduces congruently but may exhibit hyperextension laxity.
* Type III: Represents a fracture-dislocation involving the volar base of the middle phalanx. This is further stratified into Type IIIa (stable, involving less than 40% of the volar articular surface) and Type IIIb (unstable, involving greater than 40% of the articular surface, leading to dorsal subluxation of the middle phalanx). Accurate classification dictates the critical divergence between non-operative dorsal extension block splinting and surgical osteosynthesis or arthroplasty.
Surgical Anatomy and Biomechanics
A sophisticated comprehension of the microanatomy and kinematic behavior of the digital articulations is a prerequisite for executing effective surgical repairs and reconstructive procedures. Each joint is governed by a precise interplay between the osseous architecture, the collateral ligament complexes, the volar plate, and the dynamic tendinous stabilizers.
Metacarpophalangeal Joint Anatomy and Biomechanics
The MCP joints are diarthrodial condyloid articulations facilitating a multi-planar arc of motion, including flexion, extension, abduction, adduction, and circumduction. The metacarpal head is asymmetric, being wider volarly than dorsally, which creates a critical "cam effect."
- Collateral Ligament Complex: This is bifurcated into two distinct anatomical and functional bands.
- Proper Collateral Ligament (PCL): Originates from the dorsal-lateral aspect of the metacarpal head and inserts onto the volar-lateral base of the proximal phalanx. Due to the cam effect of the metacarpal head, the PCL is lax in extension (permitting abduction/adduction) and maximally taut in 70 to 90 degrees of flexion, providing critical stability during power grip.
- Accessory Collateral Ligament (ACL): Originates volarly to the PCL and inserts broadly onto the volar plate and the deep transverse metacarpal ligament. The ACL is taut in extension and lax in flexion.
- Volar Plate: A dense, fibrocartilaginous structure that reinforces the palmar joint capsule, preventing hyperextension. It is firmly anchored to the proximal phalanx but possesses a membranous, proximal attachment to the metacarpal neck, allowing it to glide during flexion.
- Thumb MCP Joint Specifics: The thumb MCP joint is uniquely constrained and relies heavily on the UCL to resist valgus stress during lateral pinch maneuvers. A complete rupture of the thumb UCL often involves the interposition of the adductor pollicis aponeurosis between the torn ligament ends (the Stener lesion), which physically precludes anatomic healing and serves as an absolute indication for surgical intervention.
Proximal Interphalangeal Joint Anatomy and Biomechanics
The PIP joints function as ginglymus (hinge) joints, restricted almost entirely to the sagittal plane (flexion and extension). Unlike the MCP joints, the condyles of the proximal phalanx are concentric, meaning the collateral ligaments maintain relatively constant tension throughout the entire arc of motion.
- Collateral Ligaments: The radial and ulnar collateral ligaments are the primary static restraints against varus and valgus deviation, respectively. Both the PCL and ACL components remain engaged throughout flexion and extension, contributing to the inherent rigidity of the PIP joint.
- Volar Plate and Check-Rein Ligaments: The PIP volar plate is a robust, rigid cartilaginous structure at its distal insertion on the middle phalanx. Proximally, it bifurcates into two distinct, stout ligamentous bands known as the check-rein ligaments, which anchor firmly to the periosteum of the proximal phalanx. These check-reins are the primary static stabilizers preventing PIP hyperextension.
- The Critical Corner: This is a vital biomechanical concept referring to the anatomical confluence where the proper collateral ligament, accessory collateral ligament, and the volar plate converge at the volar-lateral base of the middle phalanx. Disruption of this "critical corner" results in profound, multi-planar rotary instability that is poorly tolerated and often requires surgical reconstruction.
Distal Interphalangeal Joint Anatomy
The DIP joint mimics the ginglymus architecture of the PIP joint but is anatomically distinct in that its volar plate lacks the proximal check-rein extensions. Stability is conferred primarily by the dynamic forces of the terminal extensor tendon dorsally and the FDP tendon volarly, supplemented by the proper collateral ligaments laterally. Because of the robust soft-tissue envelope and the short lever arm of the distal phalanx, isolated, surgically actionable ligamentous ruptures at the DIP joint are exceedingly uncommon.
Indications and Contraindications
Clinical decision-making in the management of digital ligamentous trauma hinges upon a precise assessment of joint stability, both clinically and radiographically. The overarching objective is the restoration of a concentrically reduced, stable, and painless joint capable of a functional arc of motion. Overtreatment of stable sprains with surgery or prolonged immobilization reliably induces iatrogenic stiffness, whereas conservative management of grossly unstable lesions precipitates chronic subluxation, profound weakness, and early-onset post-traumatic arthrosis.
Operative Versus Non Operative Management Parameters
| Clinical Scenario | Recommended Management | Rationale |
|---|---|---|
| Grade I or II Collateral Ligament Sprain | Non-Operative | Microscopic or partial tearing with a firm endpoint on clinical stress testing. Demonstrates excellent healing potential with buddy taping and immediate, protected early active motion. |
| Grade III Thumb Ulnar Collateral Ligament Tear | Operative | Complete rupture frequently results in a Stener lesion (interposition of the adductor aponeurosis). This anatomic block prevents ligamentous apposition, leading to chronic valgus instability and severe pinch weakness if not surgically repaired. |
| Volar Plate Avulsion with Stable Joint (Eaton I/II) | Non-Operative | The joint maintains concentric reduction through a full active arc of motion. Effectively managed with dorsal extension block splinting, progressively decreasing the extension block over 3-4 weeks. |
| Volar Plate Avulsion with Unstable Joint (Eaton IIIb) | Operative | The joint subluxates dorsally during extension due to loss of the volar buttress. Typically involves an articular fracture fragment exceeding 40% of the middle phalanx base, necessitating open reduction internal fixation (ORIF) or volar plate arthroplasty. |
| Irreducible Dislocation | Operative | Closed reduction is physically blocked by soft tissue interposition. Offending structures typically include the volar plate, flexor tendons, lumbricals, or the lateral bands of the extensor mechanism. |
| Chronic Symptomatic Instability | Operative | Indicated following the failure of an exhaustive conservative management trial, characterized by recurrent "giving way," persistent pain, and objectively compromised grip or key pinch strength. |
Contraindications to Surgical Intervention
Absolute contraindications to acute surgical repair include the presence of active local or systemic infection, severe crush injuries with compromised soft-tissue envelopes precluding safe incision, and severe medical comorbidities that contraindicate anesthesia.
Relative contraindications include a non-compliant patient profile; postoperative success is heavily dependent on strict adherence to complex, phased rehabilitation protocols. Furthermore, in patients presenting with severe, pre-existing osteoarthritis of the affected joint, primary ligament repair is generally contraindicated. Restoring soft-tissue stability to a biologically degraded, arthritic joint will fail to alleviate pain and will likely exacerbate stiffness. In such scenarios, primary arthrodesis (joint fusion) is the salvage procedure of choice.
Pre Operative Planning and Patient Positioning
Thorough preoperative planning requires a systematic integration of the physical examination findings, precise stress testing, and appropriate diagnostic imaging to formulate a definitive surgical strategy.
Clinical Evaluation and Stress Testing
The cornerstone of the physical examination is provocative stress testing of the collateral ligaments and the volar plate. For the PIP and MCP joints, varus and valgus stress must be applied sequentially in both full extension and 30 degrees of flexion.
* Testing in 30 degrees of flexion isolates the Proper Collateral Ligament (PCL).
* Testing in full extension evaluates the Accessory Collateral Ligament (ACL) and the volar plate.
A diagnosis of a complete Grade III rupture is strongly suggested by the absence of a firm endpoint or asymmetric laxity exceeding 15 to 20 degrees when compared to the contralateral, uninjured digit.
When evaluating the thumb MCP joint for UCL integrity, patient guarding and pain can frequently mask true instability. If the examination is equivocal, a local anesthetic block (e.g., a median and ulnar nerve block at the wrist, or a localized digital block) is strongly recommended to eliminate muscular guarding and facilitate an accurate, objective stress examination.
Imaging Modalities
Standard radiographic evaluation—comprising posteroanterior (PA), true lateral, and oblique views—is mandatory to exclude avulsion fractures, subtle subluxations, and concomitant osseous pathology. The true lateral radiograph is of paramount importance for evaluating the concentricity of the PIP joint. The presence of a "V-sign" (an asymmetric, V-shaped widening of the dorsal joint space) is pathognomonic for dorsal subluxation of the middle phalanx and indicates profound volar plate and collateral ligament incompetence.
In scenarios of suspected complete thumb UCL rupture where plain radiographs demonstrate no osseous avulsion, advanced imaging via ultrasound or magnetic resonance imaging (MRI) is highly indicated. High-resolution ultrasound, when performed by an experienced musculoskeletal sonographer, is highly sensitive and specific for identifying the Stener lesion dynamically. MRI remains the gold standard for providing unparalleled visualization of the ligamentous disruption, localizing the retracted stumps, and assessing the integrity of the adductor aponeurosis and volar plate.
Anesthesia and Patient Positioning
Surgical intervention can be successfully executed under traditional regional anesthesia (e.g., axillary or supraclavicular brachial plexus blocks) or by utilizing the Wide Awake Local Anesthesia No Tourniquet (WALANT) technique. The WALANT approach, utilizing a mixture of lidocaine and epinephrine, is increasingly recognized as the gold standard for hand ligament repairs. It eliminates the need for a tourniquet, reduces anesthesia-related risks, and crucially allows the surgeon to assess the dynamic stability of the repair intraoperatively by having the patient actively move the digit through a full range of motion prior to skin closure.
The patient is positioned supine with the operative extremity extended onto a radiolucent hand table. If a traditional anesthetic approach is selected, a well-padded pneumatic upper arm tourniquet is applied to maintain a bloodless field. Intraoperative fluoroscopy (C-arm) must be draped and readily available to confirm joint concentricity, hardware trajectory, and the absence of intra-articular penetration.
Detailed Surgical Approach and Technique
The operative strategy and surgical dissection vary significantly based on the specific anatomical joint and the ligamentous structure compromised. The subsequent sections delineate the precise operative management of the most frequently encountered surgical finger sprains.
Ulnar Collateral Ligament Repair of the Thumb
Surgical intervention for a complete thumb UCL rupture, particularly when complicated by a Stener lesion, is designed to anatomically restore the ligamentous footprint at the volar-ulnar base of the proximal phalanx.
- Incision and Dissection: A lazy-S or gently curved chevron incision is mapped over the dorsal-ulnar aspect of the thumb MCP joint. The incision design must avoid crossing the joint flexion crease at a perpendicular angle to mitigate the risk of postoperative scar contracture.
- Sensory Nerve Protection: Meticulous blunt dissection is employed within the subcutaneous tissue to isolate and protect the terminal sensory branches of the superficial radial nerve. Iatrogenic injury to these branches invariably leads to highly morbid, painful neuroma formation.
- Identifying the Adductor Aponeurosis: The adductor aponeurosis is clearly delineated. In the presence of a classic Stener lesion, the proximal stump of the avulsed UCL will be visualized displaced superficially and proximally, resting over the proximal edge of the adductor aponeurosis.
- Arthrotomy and Joint Inspection: The adductor aponeurosis is longitudinally incised parallel to the extensor pollicis longus (EPL) tendon. This exposes the underlying joint capsule and the torn UCL. The joint space is thoroughly irrigated and inspected for occult osteochondral shear fractures.
- Preparation of the Footprint: The anatomic insertion site at the volar-ulnar base of the proximal phalanx is aggressively debrided of fibrous tissue and lightly decorticated with a curette or burr to expose a bleeding, cancellous bony bed, thereby optimizing biological healing.
- Ligament Fixation: A micro-suture anchor (typically ranging from 1.3 to 1.5 millimeters in diameter, depending on bone stock) is deployed into the prepared bony footprint. The non-absorbable sutures are passed through the distal end of the torn ligament utilizing a locking Krackow or grasping mattress stitch configuration to ensure robust hold.
- Tensioning and Closure: The MCP joint is concentrically reduced and held in approximately 10 to 15 degrees of flexion with a slight ulnar deviation force applied. The sutures are tensioned and tied, securing the ligament flush against the decorticated bone. The adductor aponeurosis is then meticulously repaired over the reconstructed ligament using absorbable sutures to restore dynamic stabilization.
Proximal Interphalangeal Joint Volar Plate Repair
Operative intervention for PIP joint volar plate injuries is reserved for irreducible dislocations, unstable fracture-dislocations (Eaton Type IIIb), or chronic volar plate incompetence resulting in a symptomatic swan neck deformity.
- Incision: A volar Bruner zigzag incision is executed, centered directly over the PIP joint. The apices of the triangular flaps should extend precisely to the mid-axial lines to prevent vascular compromise of the skin flaps.
- Neurovascular Protection: The volar skin flaps are elevated, and the radial and ulnar neurovascular bundles are meticulously identified, mobilized, and gently retracted laterally using vessel loops.
- Flexor Tendon Sheath Approach: The fibrous flexor tendon sheath is exposed. The C1 and C2 cruciate pulleys, along with the A3 pulley, are identified. Depending on the required proximal-distal exposure, the sheath can be opened through the C1/C2 interval, or the A3 pulley can be incised along its lateral attachment and reflected.
- Retraction of Flexor Tendons: The flexor digitorum superficialis (FDS) and flexor digitorum profundus (FDP) tendons are retracted laterally. This maneuver exposes the volar aspect of the PIP joint capsule and the avulsed volar plate.
- Fracture Management and Ligament Repair: If a large, structurally integral volar base fracture fragment is present (typically >40% of the articular surface), it is anatomically reduced and fixed using mini-fragment screws (1.0mm - 1.3mm) or multiple fine Kirschner wires. If the fragment is small, severely comminuted, or avascular, it is excised. The volar plate is then advanced distally into the resultant bony defect at the base of the middle phalanx (volar plate arthroplasty).
- Fixation Technique: Fixation of the advanced volar plate is achieved using either a classic pull-out wire/suture technique tied over a dorsal cortical button, or, more ubiquitously in contemporary practice, utilizing twin micro-suture anchors placed into the volar base of the middle phalanx.
- Assessment of Stability: Following secure repair, the joint is taken through a full passive range of motion to confirm concentric reduction without any dorsal subluxation or hinging. If residual instability is detected, a temporary transarticular Kirschner wire may be placed to hold the joint in 20-30 degrees of flexion for 3 weeks, although this significantly elevates the risk of profound postoperative stiffness.
Proximal Interphalangeal Joint Collateral Ligament Repair
Acute surgical repair of the PIP joint collateral ligaments is an infrequent requirement, as the vast majority of these injuries heal with robust scar tissue under conservative management. However, operative repair is indicated for gross, multi-planar instability associated with soft tissue interposition, or in the context of chronic, symptomatic collateral laxity.
- Incision: A mid-axial incision is utilized on the affected side of the digit. The dissection plane must remain strictly dorsal to the neurovascular bundle and volar to the lateral band of the extensor mechanism.
- Exposure: The transverse retinacular ligament is sharply incised, allowing the lateral band to be mobilized and retracted dorsally. This exposes the underlying collateral ligament complex and the joint capsule.
- Repair: The avulsed or ruptured ends of the ligament are identified. Clean mid-substance tears can be repaired directly utilizing non-absorbable figure-of-eight or mattress sutures. Avulsions from the proximal phalanx origin or the middle phalanx insertion are reattached using micro-suture anchors.
- Reconstruction: In scenarios of chronic instability where the native ligament is severely attenuated, retracted, or absent, a free tendon graft (commonly the palmaris longus or a harvested slip of the flexor carpi radialis) is required to reconstruct the collateral ligament. The graft is routed through precisely drilled bone tunnels in the proximal and middle phalanges to recreate the anatomic origins and insertions, typically secured with interference screws or suspensory buttons.
Complications and Management
The surgical management of finger sprains and ligamentous disruptions is fraught with a distinct and challenging set of potential complications. The hand surgeon must constantly navigate the delicate, often contradictory balance between achieving rigid structural stability and preserving functional mobility.
Common Complications and Salvage Strategies
| Complication | Estimated Incidence | Pathophysiology | Salvage and Management Strategies |
|---|---|---|---|
| Postoperative Stiffness | 20% - 40% | Formation of dense adhesions between the repaired ligament, the joint capsule, and the surrounding gliding tendons; often exacerbated by prolonged or rigid immobilization. | Aggressive, supervised hand therapy utilizing dynamic or static progressive splinting. Surgical tenolysis and capsulotomy may be indicated if conservative measures plateau after 6 months. |
| Recurrent Instability | 5% - 10% | Mechanical failure of the suture anchor, biological attenuation of the repaired ligament, non-compliance with rehab, or unrecognized concomitant injuries (e.g., occult fractures). | Revision ligament repair, autograft/allograft tendon reconstruction, or ultimately joint arthrodesis in cases complicated by severe secondary degenerative changes. |
| Superficial Infection | 2% - 5% | Bacterial colonization of the surgical incision. Often exacerbated by aggressive early motion protocols that cause micro-dehiscence of the wound edges. | Targeted oral or intravenous antibiotic therapy combined with local wound care. Hardware removal is rarely necessary unless a deep, intra-articular infection is confirmed. |
| Neuroma Formation | 1% - 3% | Iatrogenic traction, laceration, or entrapment of the dorsal sensory branches of the radial or ulnar nerves during surgical exposure. | Initial conservative management with desensitization therapy and gabapentinoids. Refractory cases require surgical exploration, neuroma excision, and burying the proximal nerve stump into local muscle or bone (TMR or RPNI techniques). |
| Complex Regional Pain Syndrome (CRPS) | 1% - 2% | An exaggerated, pathological inflammatory and neuropathic autonomic response to the initial surgical trauma. | Requires a high index of suspicion for early recognition. Management involves aggressive multimodal pain control, stellate ganglion blocks, and relentless continuous active motion therapy. |
Stiffness remains the most ubiquitous, frustrating, and challenging complication following surgical intervention in the small joints of the hand. The PIP joint is notoriously susceptible to severe flexion contractures due to the rapid scarring of the volar plate and collateral ligaments. Prevention is heavily reliant on meticulous, atraumatic surgical technique, minimizing unnecessary soft tissue stripping, and the prompt initiation of early protected motion protocols. When severe, functionally limiting stiffness persists despite exhaustive conservative therapy and splinting, a staged surgical approach involving hardware removal, radical capsulotomy, and flexor/extensor tenolysis may be indicated. However, patients must be explicitly counseled preoperatively that achieving a "normal" arc of motion following salvage tenolysis is highly improbable.
Post Operative Rehabilitation Protocols
The ultimate functional success of any ligamentous repair in the hand is inextricably linked to the execution of a highly structured postoperative rehabilitation protocol. The prevailing philosophy in modern orthopedic hand surgery has shifted away from prolonged rigid immobilization, favoring a transition to early protected motion as rapidly as the biomechanical strength of the surgical repair will permit.
For thumb UCL repairs, the thumb is typically immobilized in a rigid thumb spica splint or cast for four weeks postoperatively. Crucially, the interphalangeal joint of the thumb is left free to prevent adhesions of the extensor pollicis longus and flexor pollicis longus tendons. At the four-week mark, the rigid immobilization is transitioned to a removable, custom thermoplastic orthosis, and active range of motion of the MCP joint is initiated under the guidance of a certified hand therapist. Passive stretching and aggressive strengthening exercises are strictly delayed until six to eight weeks postoperatively to protect the healing ligamentous footprint. Unrestricted pinch and power grip activities, as well as a return to high-impact contact sports, are generally permitted at ten to twelve weeks, often with prophylactic taping or bracing.
Following PIP joint volar plate repairs or reconstructions, the rehabilitation protocol is dictated entirely by the intraoperative stability of the repair. A dorsal extension block splint is universally employed. The splint is initially fabricated at an angle that maintains a concentric joint reduction—typically 20 to 30 degrees of flexion. Active flexion within the confines of the splint is encouraged immediately (often on postoperative day one or two) to facilitate flexor tendon gliding and prevent restrictive adhesions. Each week, the extension block is progressively reduced by 10 degrees, allowing the joint to gradually achieve full extension. By four to six weeks, the splint is discontinued during the day, and buddy taping to the adjacent digit is utilized. Dynamic extension splinting may be cautiously introduced at six to eight weeks if a residual, rigid flexion contracture is present.
Collateral ligament repairs of the PIP and DIP joints are generally managed with buddy taping to the adjacent, uninjured digit. This allows for early active flexion and extension while effectively protecting the joint against deleterious varus and valgus shear stresses. A custom static orthosis may be utilized at night to maintain full extension and prevent the development of flexion contractures during sleep.
Summary of Key Literature and Guidelines
The academic foundation and evidence-based algorithms for the management of finger sprains and ligamentous injuries are built upon several landmark anatomical and clinical studies that remain highly relevant to contemporary practice.
Stener's seminal 1962 publication fundamentally elucidated the pathoanatomy of the displaced ulnar collateral ligament of the thumb. His work conclusively demonstrated that the interposition of the adductor aponeurosis physically prevents spontaneous ligamentous healing, thereby mandating surgical intervention. This anatomical concept remains the primary physiological driver for the operative management of Grade III thumb UCL injuries today.
The management of PIP joint injuries is heavily influenced by the foundational work of Eaton and Littler, who defined the anatomical basis for volar plate avulsions and complex fracture-dislocations. Their classification system continues to serve as the universal language guiding the decision between conservative dorsal extension block splinting and surgical stabilization. Furthermore, Hastings and Carroll provided critical biomechanical insights into the PIP joint, emphasizing the paramount importance of the collateral ligament and volar plate confluence at the "critical corner" in maintaining multi-planar digital stability.
Current guidelines from the American Society for Surgery of the Hand (ASSH) emphasize the critical importance of early, accurate diagnosis utilizing targeted stress testing and appropriate advanced imaging modalities. The consensus strongly supports conservative management with early protected motion for stable sprains, reserving surgical intervention for specific, well-defined indications such as Stener lesions, irreducible dislocations, and grossly unstable fracture-dislocations. Finally, the paradigm shift towards Wide Awake Local Anesthesia No Tourniquet (WALANT) techniques for ligament repairs represents a significant recent advancement in the hand surgery literature. This technique allows for real-time intraoperative assessment of repair stability, thereby facilitating more aggressive, tailored early motion protocols and ultimately optimizing patient outcomes.