Elbow Arthroplasty's Journey: From History to Current Designs
Key Takeaway
Learn more about Elbow Arthroplasty's Journey: From History to Current Designs and how to manage it. Elbow arthroplasty j evolved from the failures of non-replacement surgeries to treat elbow pathologies. Early metallic, rigid hinged devices faced high failure rates due to poor implant fixation and design. The modern era began with polymethylmethacrylate (PMMA) for implant fixation, leading to a deeper understanding of elbow biomechanics and improved implant designs, including unlinked "resurfacing" approaches.
Introduction and Epidemiology
Normal elbow function requires a pain-free, mobile, and stable articulation to position the hand in space for activities of daily living. Historically, achieving this triad in the setting of severe articular destruction proved exceptionally challenging. Prior to the advent of modern total elbow arthroplasty, surgical management relied heavily on nonarthroplasty techniques. Resection arthroplasty, interposition arthroplasty utilizing fascia lata or Achilles tendon allografts, and arthrodesis predominated the surgical landscape. While arthrodesis provided stability and pain relief, it severely compromised upper extremity function by eliminating the critical arc of motion necessary for feeding and personal hygiene. Conversely, resection and interposition arthroplasties often sacrificed stability for mobility, resulting in a flail, painful joint.
The development of total elbow arthroplasty was borne out of the distinct failures of these nonreplacement surgeries to effectively treat articular and periarticular pathologies. The epidemiological profile of patients requiring elbow arthroplasty has shifted significantly over the past several decades. Historically, the primary indication was end-stage inflammatory arthropathy, specifically rheumatoid arthritis. The systemic nature of rheumatoid arthritis frequently resulted in profound symmetric joint destruction, making these patients the primary candidates for early arthroplasty designs.
However, with the advent of disease-modifying antirheumatic drugs and biologic therapies, the incidence of severe rheumatoid elbow destruction has precipitously declined. Concurrently, the demographic landscape has shifted toward the aging population, leading to a marked increase in the utilization of total elbow arthroplasty for acute, comminuted distal humerus fractures in osteoporotic bone, post-traumatic osteoarthritis, and distal humerus nonunions. This paradigm shift from low-demand inflammatory arthritis patients to higher-demand post-traumatic and fracture patients has continuously driven the evolution of implant design and surgical technique.

Historical Evolution of Elbow Arthroplasty
Early efforts at elbow arthroplasty were characterized by a fundamental misunderstanding of elbow kinematics. The elbow was erroneously felt to function as a simple, rigid hinge. Initial designs in the mid-20th century were characterized by metallic, nylon, rubber, or acrylic hemiarthroplasties of the distal humerus or proximal ulna. These early total elbow arthroplasties were rigid, fully constrained metallic hinged devices.
Crucially, these early designs predated the introduction of polymethylmethacrylate bone cement. Fixation of these implants to the host bone was achieved through uncemented intramedullary stems or extramedullary supports screwed directly into the cortical bone. The clinical results were predictably disastrous. Instability, early aseptic loosening, unpredictable ranges of motion, and catastrophic periprosthetic fractures limited the success of these implants. Poor implant fixation to bone, combined with inferior implant design that failed to account for out-of-plane forces, contributed to unacceptably high failure rates.

Surgical Anatomy and Biomechanics
A comprehensive understanding of elbow anatomy and biomechanics is paramount for modern arthroplasty success. The elbow is a highly constrained trochoginglymoid joint, comprising the ulnohumeral, radiohumeral, and proximal radioulnar articulations.
Osseous Articulations and Kinematics
The ulnohumeral joint acts primarily as a hinge (ginglymus), allowing flexion and extension, while the radiohumeral and proximal radioulnar joints function as a pivot (trochoid), permitting pronation and supination. The instant center of rotation of the elbow is located at the center of the trochlea, collinear with the anterior-inferior aspect of the medial epicondyle and the center of the capitellum.
The period following the failure of early rigid hinges was characterized by a rapid evolution in the understanding of elbow biomechanics. A growing body of biomechanical and clinical data demonstrated that a simple hinge did not adequately replicate the mechanics of the elbow. The normal ulnohumeral articulation exhibits approximately 3 to 4 degrees of varus-valgus laxity and rotational toggle during the arc of motion. Out-of-plane motion must be accounted for in implant design to prevent the transmission of eccentric forces directly to the implant-bone interface, which inevitably leads to loosening.

Ligamentous Constraints
The stability of the native elbow relies on both static and dynamic restraints. The primary static restraints are the ulnohumeral articulation, the medial collateral ligament complex, and the lateral collateral ligament complex. The anterior bundle of the medial collateral ligament is the primary restraint to valgus stress, while the lateral ulnar collateral ligament is the primary restraint to varus and posterolateral rotatory instability.
The failure of early efforts at arthroplasty led to two distinct approaches to modern implant design based on the management of these ligamentous constraints Unlinked resurfacing designs and Linked semiconstrained designs.

Unlinked Resurfacing Designs
In unlinked, or resurfacing, designs, the articular surface of the joint is resurfaced with preservation of the native collateral ligaments. Success with these implants depends entirely on the integrity of the soft tissue envelope, the presence of adequate bone stock to support the prosthesis, and the precise geometry of the articulation. The contribution of the intact soft tissues to absorbing the forces across the elbow is believed to result in lower rates of implant loosening. Classic examples include the Capitellocondylar and Souter-Strathclyde prostheses. However, these implants are technically demanding to insert, require perfect ligamentous balancing, and are prone to postoperative instability if the soft tissue envelope is compromised.

Linked Semiconstrained Designs
Linked, or semiconstrained, designs were developed to address the instability associated with unlinked implants while avoiding the aseptic loosening seen in early rigid hinges. Stability is achieved through a coupled articulation between the humeral and ulnar components via a locking pin or snap-fit mechanism. Crucially, this linkage is designed to be sloppy, allowing 7 to 10 degrees of varus-valgus and rotational laxity. The ulnohumeral articulation tracks within the tolerance of the implant, implying that the surrounding muscular envelope counters some of the forces across the elbow, effectively offloading the bone-cement interface.

Indications and Contraindications
The indications for total elbow arthroplasty have expanded, but patient selection remains the most critical determinant of long-term success. The surgeon must carefully weigh the functional demands of the patient against the known lifecycle and lifting restrictions associated with elbow arthroplasty.
Operative Indications and Alternatives
| Clinical Scenario | Operative Indication for Arthroplasty | Non-Operative or Alternative Surgical Options |
|---|---|---|
| Rheumatoid Arthritis | End-stage joint destruction, pain refractory to medical management, severe instability. | DMARDs, biologic agents, synovectomy with radial head excision (for early stages). |
| Post Traumatic Osteoarthritis | Severe pain and functional limitation in older, low-demand patients. | NSAIDs, intra-articular injections, interposition arthroplasty (younger patients), arthrodesis (high-demand laborers). |
| Acute Distal Humerus Fracture | Comminuted, intra-articular fractures in osteoporotic bone where stable internal fixation is impossible (typically >65 years old). | Open Reduction Internal Fixation (ORIF) if bone stock permits, cast immobilization (non-ambulatory/high surgical risk). |
| Distal Humerus Nonunion | Symptomatic nonunion with poor bone stock, failed prior osteosynthesis. | Revision ORIF with autologous bone grafting (if adequate bone stock exists). |
Absolute and Relative Contraindications
Absolute contraindications to total elbow arthroplasty include active or recent intra-articular infection, profound neuromuscular dysfunction leading to a flail extremity, and Charcot neuroarthropathy. Performing an arthroplasty in a neuropathic joint universally leads to rapid implant loosening and catastrophic failure.
Relative contraindications include a history of prior joint infection, inadequate soft tissue coverage requiring complex flap reconstruction prior to implantation, and young patient age or high functional demands. Patients must be willing to adhere to permanent lifting restrictions (typically 5 pounds repetitive, 10 pounds maximum single lift) to prevent aseptic loosening. Therefore, heavy laborers or individuals reliant on their upper extremities for weight-bearing (e.g., paraplegic patients utilizing manual wheelchairs) are generally poor candidates.

Pre Operative Planning and Patient Positioning
Meticulous preoperative planning is required to anticipate challenges related to bone loss, deformity, and implant sizing.
Imaging and Templating
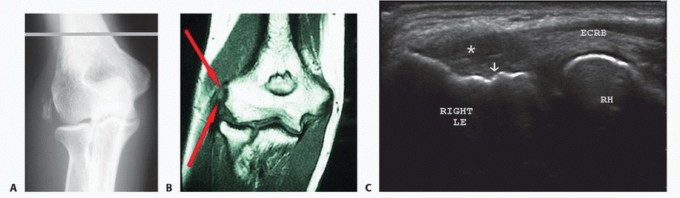
Standard radiographic evaluation includes true anteroposterior and lateral views of the elbow. In cases of acute trauma, traction views may be necessary to delineate fracture fragments and assess the remaining osseous columns. A computed tomography scan is highly recommended in cases of post-traumatic osteoarthritis or revision surgery to quantify bone stock, identify occult deformity, and assess the medullary canals.
Preoperative templating is essential. The surgeon must evaluate the diameter and bowing of the humeral and ulnar canals. The ulnar canal is particularly challenging; it exhibits a complex three-dimensional bow, curving laterally and posteriorly. Failure to recognize this anatomy during canal preparation frequently leads to cortical perforation. Templating also aids in determining the level of the joint line and the need for structural bone grafting, particularly when utilizing implants with an anterior flange designed to counteract posterior and rotational forces.

Patient Positioning Setup
The procedure may be performed with the patient in the lateral decubitus position with the arm draped over a radiolucent post, or in the supine position with the arm brought across the chest. The lateral decubitus position offers excellent visualization of the posterior aspect of the elbow and facilitates access to the ulnohumeral joint. A sterile tourniquet is typically applied to the proximal arm to maintain a bloodless surgical field, though it should be deflated prior to closure to achieve meticulous hemostasis, given the high risk of postoperative hematoma in this poorly padded region.
Detailed Surgical Approach and Technique
The modern era of total elbow replacement was initiated with the introduction of polymethylmethacrylate for implant fixation. Surgical technique must prioritize meticulous handling of the soft tissues, precise bone preparation, and optimal cementation practices.
Incision and Ulnar Nerve Management
A universal posterior approach is utilized. The incision is typically centered over the olecranon, curving slightly medially to avoid placing the scar directly over the bony prominence. Full-thickness fasciocutaneous flaps are elevated to preserve the tenuous vascular supply to the skin.
Management of the ulnar nerve is a critical early step. The nerve is identified proximally in the triceps interval and traced distally through the cubital tunnel to its first motor branches in the flexor carpi ulnaris. While some surgeons advocate for in-situ decompression, routine anterior transposition (subcutaneous or subfascial) is generally preferred to remove the nerve from the zone of injury, prevent traction during joint dislocation, and avoid encasement in postoperative scar tissue.

Triceps Management Strategies
Exposure of the joint requires mobilization of the triceps mechanism. Several techniques exist, each with specific advantages and morbidities:
- Triceps Reflecting (Coonrad-Morrey): The triceps is elevated from medial to lateral in continuity with the anconeus and the periosteum of the proximal ulna. This provides excellent exposure and preserves the continuity of the extensor mechanism, though repair can be tenuous.
- Triceps Sparing (Bryan-Morrey): The triceps is mobilized laterally without detachment from the olecranon. This is technically demanding but eliminates the risk of postoperative triceps rupture. It is particularly useful in fracture cases where the olecranon is intact.
- Triceps Splitting: A midline split is made through the triceps tendon, continuing distally to the olecranon. This provides direct access to the joint but can compromise the extensor mechanism if not meticulously repaired.
- Triceps Peeling (Campbell): The triceps tendon is sharply detached from the olecranon. This approach provides unparalleled exposure but carries the highest risk of postoperative triceps insufficiency and requires prolonged postoperative immobilization.

Joint Preparation and Implantation
Following joint exposure and excision of the collateral ligaments (if a linked implant is chosen), the distal humerus is prepared. The center of the trochlea is identified to establish the anatomic axis. The humeral canal is opened and reamed. The distal humerus is then resected using cutting jigs to accommodate the implant. In modern linked designs, an anterior flange is incorporated into the humeral component. This flange is felt to counteract posterior and rotational forces across the elbow, contributing significantly to the prevention of implant loosening. The anterior cortex of the distal humerus is prepared to receive this flange, and structural autograft (often obtained from the resected trochlea) is placed behind the flange. Incorporation and hypertrophy of this bone graft behind the anterior flange over time proves its biomechanical utility in stress transfer.
Preparation of the ulna requires precise identification of the medullary canal. The starting point is typically at the base of the coronoid, not the tip of the olecranon. Reaming must follow the lateral and posterior bow of the ulna. A burr is often used to open the canal, followed by sequential broaching.
Once trial reduction confirms adequate tracking, stability, and restoration of the joint line, the definitive implants are cemented. The canals are thoroughly irrigated and dried. Polymethylmethacrylate cement is injected in a retrograde fashion using a cement gun and pressurized. The implants are inserted, and the linkage mechanism (e.g., locking pin) is engaged. The triceps mechanism is then meticulously repaired using heavy non-absorbable sutures passed through transosseous drill holes in the olecranon.

Complications and Management
Despite significant advancements in implant design and surgical technique, total elbow arthroplasty remains associated with a higher complication rate compared to hip or knee arthroplasty. The subcutaneous nature of the joint, complex biomechanics, and often compromised host tissues contribute to this risk profile.
Common Complications and Salvage Strategies
| Complication | Estimated Incidence | Etiology and Risk Factors | Salvage Strategy |
|---|---|---|---|
| Infection | 3% - 8% | Thin soft tissue envelope, rheumatoid arthritis, prior surgeries, prolonged operative time. | Acute: Irrigation and debridement with modular exchange. Chronic: Two-stage revision with antibiotic spacer, or resection arthroplasty/amputation if bone stock is unsalvageable. |
| Aseptic Loosening | 5% - 15% (at 10 years) | Eccentric loading, poor cementation technique, failure to adhere to lifting restrictions, high-demand patient. | Revision arthroplasty with longer stems, impaction bone grafting, or strut allografts. |
| Ulnar Neuropathy | 5% - 10% | Traction injury during exposure, compression by hematoma, thermal injury from cement, encasement in scar. | Observation for neuropraxia. Surgical exploration and neurolysis/transposition if symptoms are progressive or refractory. |
| Triceps Insufficiency | 2% - 5% | Failure of triceps repair (especially in peeling approaches), over-resection of the olecranon. | Primary repair with augmentation (e.g., Achilles allograft, anconeus rotation flap). Often requires prolonged immobilization. |
| Periprosthetic Fracture | 2% - 5% | Osteoporosis, stress risers at the tip of the prosthesis, forceful manipulation during surgery. | ORIF with cerclage cables/plates if the implant is stable. Revision to a longer stemmed implant if the component is loose. |
The management of deep periprosthetic joint infection is particularly challenging. The elbow lacks redundant soft tissue, making wound healing difficult. A two-stage revision strategy remains the gold standard for chronic infections, utilizing an articulating or static antibiotic-loaded polymethylmethacrylate spacer prior to reimplantation.
Post Operative Rehabilitation Protocols
Postoperative rehabilitation must balance the need for early range of motion to prevent stiffness with the necessity of protecting the soft tissue repair, particularly the triceps mechanism.
In the immediate postoperative period, the arm is typically placed in a well-padded posterior splint in approximately 60 to 70 degrees of flexion. The splint is maintained for 3 to 7 days to allow for initial wound healing and reduction of edema.
If a triceps-sparing approach was utilized, active and active-assisted range of motion for flexion and extension can be initiated within the first week. Pronation and supination are also encouraged. If the triceps was reflected or peeled and subsequently repaired, active extension is strictly prohibited for 6 weeks to prevent catastrophic rupture of the repair. During this period, patients may perform active flexion and passive extension in a gravity-eliminated plane.
Strengthening exercises are delayed until 8 to 12 weeks postoperatively. It is imperative that the surgeon explicitly educates the patient regarding permanent activity modifications. Total elbow arthroplasty is in a period of refinement, but it is not designed to withstand heavy loading. Patients are universally restricted to lifting no more than 5 pounds repetitively and 10 pounds for a single event. Activities that subject the elbow to high impact or torsional loads (e.g., golf, tennis, chopping wood) are strongly discouraged to maximize the survivorship of the implant.
Summary of Key Literature and Guidelines
The journey from historical nonarthroplasty procedures to current semiconstrained designs represents a triumph of biomechanical engineering and surgical innovation. Clinical experience has clearly demonstrated the design features that are acknowledged to contribute to success.
The transition from rigid hinges to the "sloppy hinge" concept championed by Morrey and colleagues fundamentally altered the survivorship of these implants. By allowing the ulnohumeral articulation to toggle slightly within the constraints of the linkage, eccentric forces are dissipated into the surrounding soft tissues rather than being transmitted directly to the cement-bone interface.
Furthermore, the incorporation of the anterior flange into modern linked humeral designs has been a critical refinement. Biomechanical studies have validated that this flange effectively counteracts the posterior directed forces that occur during elbow extension, which were a primary driver of humeral component loosening in earlier designs. The observed incorporation and hypertrophy of the bone graft placed behind this anterior flange provides in vivo proof of its load-bearing function.
While total elbow arthroplasty continues to undergo refinement, current semiconstrained designs utilizing polymethylmethacrylate fixation offer reliable pain relief and functional restoration for patients with severe articular destruction, provided rigorous adherence to surgical technique and strict patient selection criteria are maintained. Future advancements will likely focus on improving bearing surfaces to reduce wear debris, enhancing biologic fixation options for younger patients, and refining instrumentation to minimize bone resection and optimize implant alignment.
You Might Also Like