Question 51
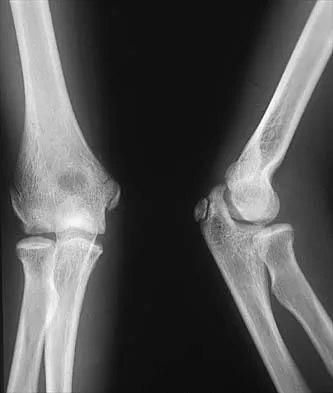
A 14-year-old girl has a painful hallux valgus deformity that has not responded to shoe modifications. Figure 21 shows a standing AP radiograph. What is the most appropriate surgical procedure?
Explanation
The radiograph reveals an increased first-second intermetatarsal angle and a congruent metatarsophalangeal joint with an abnormal distal metatarsal articular angle. Correction of both of these abnormalities requires a proximal and distal first metatarsal osteotomy. Coughlin M: Juvenile bunions, in Coughlin MJ, Mann RA (eds): Surgery of the Foot and Ankle, ed 6. St Louis, MO, Mosby, 1993, pp 297-339.
Question 52
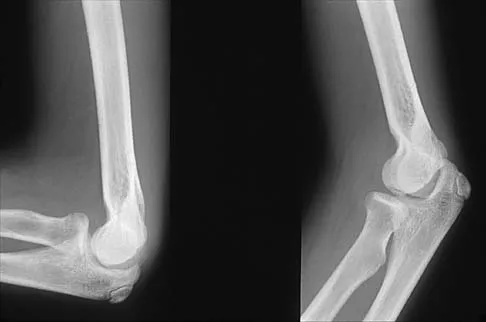
Figure 22 shows the radiograph of a 7-year-old boy who underwent retrograde elastic nailing of a femoral shaft fracture. What is the most common problem following this procedure?
Explanation
Several large clinical studies have shown that the most common problem after elastic nailing of a femoral shaft fracture is persistent pain and irritation at the nail insertion site. Unacceptable shortening and malunion are very rare in a 7-year-old patient. Rotational malalignment also is unusual. Osteonecrosis has been reported in solid antegrade nailing but not with elastic nailing of femoral shaft fractures in skeletally immature patients. Flynn JM, Luedtke LM, Ganley TJ, et al: Comparison of titanium elastic nails with traction and a spica cast to treat femoral fractures in children. J Bone Joint Surg Am 2004;86:770-777. Flynn JM, Hresko T, Reynolds RA, et al: Titanium elastic nails for pediatric femur fractures: A multicenter study of early results with analysis of complications. J Pediatr Orthop 2001;21:4-8.
Question 53
A newborn girl with an isolated unilateral dislocatable hip is placed in a Pavlik harness with the hips flexed 100 degrees and at resting abduction. Figure 23 shows an ultrasound obtained 2 weeks later. What is the next step in management?
Explanation
The infant has a well-positioned hip in the Pavlik harness and treatment should be continued in the current position. The success rate is over 90% with the use of this device for a dislocatable hip. Ultrasound is a useful tool to confirm appropriate positioning of the cartilaginous femoral head during treatment. If the femoral head is not reduced after 2 to 3 weeks in the harness, this mode of treatment should be abandoned. Forceful extreme abduction can cause osteonecrosis of the femoral epiphysis and should be avoided. Closed reduction, arthrography, and spica casting are indicated if the hip cannot be maintained in a reduced position with the harness. Lehmann HP, Hinton R, Morello P, et al: Developmental dysplasia of the hip practice guideline: Technical report. Committee on Quality Improvement, and Subcommittee on Developmental Dysplasia of the Hip. Pediatrics 2000;105:E57.
Question 54
During the early swing phase of the normal gait cycle, what lower extremity muscle is primarily contracting?
Explanation
Electromyography during walking reveals the tibialis anterior muscle is active during early swing, allowing the foot to clear the ground. All of the other muscles are quiet, as the limb moves forward through space with minimal muscular effort. The other muscles are primarily active during weight acceptance or push-off. Gage JR: An overview of normal walking. Instr Course Lect 1990;39:291-303.
Question 55
A 6-month-old child is seen in the emergency department with a spiral fracture of the tibia. The parents are vague about the etiology of the injury. There is no family history of a bone disease. In addition to casting of the fracture, initial management should include
Explanation
Unwitnessed spiral fractures should raise the possibility of child abuse, especially prior to walking age. With nonaccidental trauma being considered in the differential diagnosis, a skeletal survey is indicated to determine if there are other fractures in various stages of healing. Kempe CH, Silverman FN, Steele BF, et al: The battered-child syndrome. JAMA 1962;181:17-24.
Question 56
What is the primary indication for performing an arthroscopic synovectomy on a patient with hemophilia that is the result of factor VIII deficiency?
Explanation
Improved medical management has changed musculoskeletal outcomes for individuals with hemophilia. Patients with severe hemophilia receiving prophylactic administration of factor VIII may never develop a target joint that requires further orthopaedic intervention. Patients with moderate hemophilia and those patients with severe hemophilia not receiving prophylactic treatment will still develop joints that have recurrent hemarthroses. When recurrent hemarthrosis continues despite optimal medical management, synovectomy is indicated. While synovectomy is predictable in its ability to decrease joint bleeding, it does not necessarily improve joint range of motion or prevent the development of hemophilic arthropathy over time. It will not reverse articular damage to the joint once it has developed. Dunn AL, Busch MT, Wyly JB; et al: Arthroscopic synovectomy for hemophilic joint disease in a pediatric population. J Pediatr Orthop 2004;24:414-426.
Question 57
The rate of complications after in situ pinning of a chronic slipped capital femoral epiphysis is highest with placement of the screw in what quadrant of the femoral head?
Explanation
The rate of complications increases as the pin moves farther from the ideal position, which is the center of the head. This is the strongest argument for the use of a single pin. The highest rate of complications, primarily osteonecrosis and pin penetration, is associated with pin placement in the anterior superior quadrant. Raney EM, Ogden JA: Slipped capital femoral epiphysis. Current Ortho 1995;9:111-116.
Question 58
What is the incidence and significance of anterior cruciate ligament laxity following tibial eminence fractures in skeletally immature individuals?
Explanation
Measurable anterior cruciate ligament laxity, while frequently seen after tibial eminence fractures, usually does not cause symptoms. It is found even in patients whose fractures have been anatomically reduced and fixed, leading to speculation that it is due to stretching of the ligament at the time of injury. Willis R, Blokker C, Stall TM, et al: Long-term follow-up of anterior eminence fractures. J Pediatr Orthop 1993;13:361-364.
Question 59
A full-term newborn has webbing at the knees, rigid clubfeet, a Buddha-like posture of the lower extremities, and no voluntary or involuntary muscle action at and below the knees. Radiographs of the spine and pelvis reveal an absence of the lumbar spine and sacrum. What maternal condition is associated with this diagnosis?
Explanation
The history, physical examination, and radiographic findings are consistent with type IV sacral agenesis or caudal regression syndrome. These children are born with no lumbar spine or sacrum. The T12 vertebra is often prominent posteriorly. Popliteal webbing and knee flexion contractures are common with this diagnosis. There is a higher incidence of this diagnosis when the mother has diabetes mellitus. Maternal drug abuse and alcoholism can produce phenotypically unique children but without the findings described here. Maternal idiopathic scoliosis is not associated with caudal regression syndrome. Chan BW, Chan KS, Koide T, et al: Maternal diabetes increases the risk of caudal regression caused by retinoic acid. Diabetes 2002;51:2811-2816.
Question 60
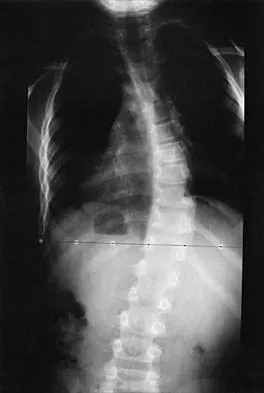
Figure 24 shows the sitting AP and lateral spinal radiographs of a nonambulatory 12½-year-old boy with Duchenne muscular dystrophy who is being evaluated for scoliosis. The lumbar curve from T12 to L5 measures 36 degrees, and the thoracic curve from T3 to T12 measures 24 degrees on the AP radiograph. He has 5 degrees of pelvic obliquity. His forced vital capacity is 45% of predicted for height and weight. What is the most appropriate treatment for the spinal deformity?
Explanation
Posterior spinal fusion is the treatment of choice for scoliosis in patients with Duchenne muscular dystrophy once they are no longer able to walk. This treatment improves quality of life and upright wheelchair positioning. Its effect on pulmonary function is less clear, as pulmonary function will continue to decline because of the underlying muscle disease. While bracing and wheelchair modifications may slow the progression of the curve, progression will continue. Surgical intervention at this stage does not have to include the pelvis, which, in general, is indicated in curves of greater than 40 degrees, and when pelvic obliquity is greater than 10 degrees. Fixation to the pelvis should also be considered in lumbar curves where the apex is lower than L1. Surgical treatment usually can be safely performed if the vital capacity is greater than 35%. Hahn GV, Mubarak SJ: Muscular dystrophy, in Weinstein SL (ed): The Pediatric Spine, ed 2. Philadelphia, PA, Lippincott Williams & Wilkins, 2001, pp 819-832.
Question 61
A 3-year-old child has refused to walk for the past 2 days. Examination in the emergency department reveals a temperature of 102.2 degrees F (39 degrees C) and limited range of motion of the left hip. An AP pelvic radiograph is normal. Laboratory studies show a WBC count of 9,000/mm3, an erythrocyte sedimentation rate (ESR) of 65 mm/h, and a C-reactive protein level of 10.5 mg/L (normal < 0.4). What is the next most appropriate step in management?
Explanation
Examination reveals an irritable hip, creating a differential diagnosis of transient synovitis versus pyogenic hip arthritis. Kocher and associates described four criteria to help predict the presence of infection: inability to bear weight, fever, ESR of more than 40 mm/h, and a peripheral WBC count of more than 12,000/mm3. This patient meets three of the four criteria, with a positive predictive value of 73% to 93% for joint infection. Therefore, aspiration of the hip is warranted, with a high likelihood that emergent hip arthrotomy will be indicated. Ideally, intravenous antibiotics should be administered after culture material has been obtained from needle aspiration of the hip. An urgent bone scan is better indicated as a screening test for sacroiliitis or diskitis. If the arthrocentesis proves negative, CT or MRI of the pelvis may be indicated to rule out a pelvic or psoas abscess. Del Beccaro MA, Champoux AN, Bockers T, et al: Septic arthritis versus transient synovitis of the hip: The value of screening laboratory tests. Ann Emerg Med 1992;21:1418-1422. Kocher MS, Mandiga R, Zurakowski D, et al: Validation of a clinical prediction rule for the differentiation between septic arthritis and transient synovitis of the hip in children. J Bone Joint Surg Am 2004;86:1629-1635.
Question 62
A 2-year-old girl has had a swollen right knee for the past 7 weeks. There is no history of significant trauma, and she has not had a fever or been ill. Her parents report that she is stiff in the morning but otherwise does not report pain. A CBC count and erythrocyte sedimentation rate are normal. Treatment with naproxen at appropriate doses for the past 2 weeks has resulted in some improvement. Radiographs show only soft-tissue swelling. Examination reveals a healthy-appearing child with a warm and swollen right knee that is only slightly tender but lacks full extension by 20 degrees. What is the next most appropriate step in management?
Explanation
Up to 30% of children with juvenile rheumatoid arthritis (increasingly known now as juvenile idiopathic arthritis or JIA) already have potentially damaging uveitis at the time of diagnosis. This patient has typical oligoarticular JRA (JIA) and therefore is at significant risk for uveitis. MRI, radioisotope scanning, or an ACE level most likely would not provide additional useful diagnostic information because intra-articular derangement, osteomyelitis, or sarcoidosis are all unlikely. Arthrocentesis and triamcinolone hexacetonide joint injection might be indicated if continued use of nonsteroidal medication does not result in improvement, but should be held off for at least an additional 4 to 6 weeks to see if continued use of naproxen results in control of the arthritis. Wolf MD, Lichter PR, Ragsdale CG: Prognostic factors in the uveitis of juvenile rheumatoid arthritis. Ophthalmology 1987;94:1242. Cassidy JT, Petty RE: Textbook of Pediatric Rheumatology. Philadelphia, PA, WB Saunders, 2001, p 220.
Question 63
A 12-year-old girl has back pain after falling 20 feet and landing in the sitting position. She has no fractures or other injuries, and her neurologic examination is normal. A lateral radiograph, transverse CT scan, and reformatted sagittal CT scan are shown in Figures 25a through 25c. Which of the following methods is associated with the best long-term outcome?
Explanation
25b 25c The patient has a displaced burst fracture. Fusion with instrumentation has shown better results than casting alone. Posterior fusion with instrumentation, with sagittal plane correction, yields the best results. Decompression occurs indirectly with correction of the kyphosis. Anterior decompression is unnecessary. Lalonde F, Letts M, Yang JP, et al: An analysis of burst fractures of the spine in adolescents. Am J Orthop 2001;30:115-120. Clark P, Letts M: Trauma to the thoracic and lumbar spine in the adolescent. Can J Surg 2001;44:337-345.
Question 64
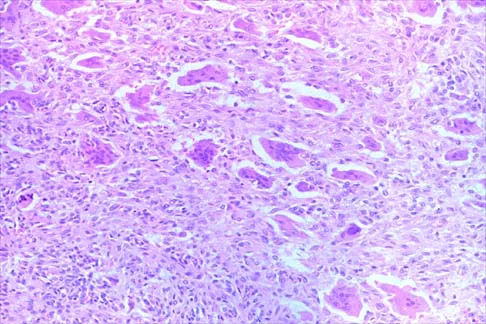
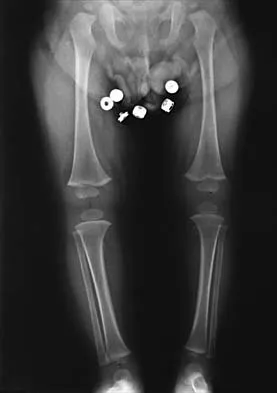
Figure 26 shows the radiograph of an otherwise healthy Caucasian 5-year-old boy who has a painless limp. What is the best treatment option?
Explanation
The prognosis of Legg-Perthes disease in children younger than age 6 years is good. There is no indication that surgical treatment will improve the outcome. Range-of-motion exercises to prevent contracture may be helpful. Herring JA, Kim HT, Browne R: Legg-Calve-Perthes disease: Prospective multicenter study of the effect of treatment on outcome. J Bone Joint Surg Am 2004;86:2121-2134.
Question 65
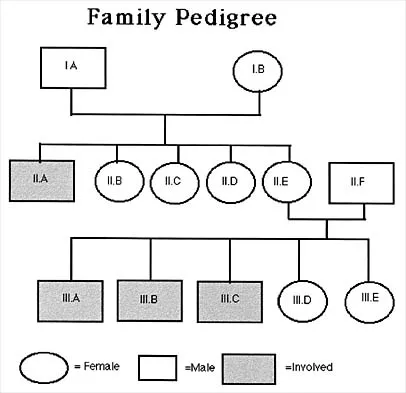
A 12-year-old girl who has a history of frequent tripping and falling also has bilateral symmetric hand weakness, high arched feet, absent patellar and Achilles tendon reflexes, and excessive wear on the lateral border of her shoes. She reports that she has multiple paternal family members with similar deformities. She most likely has a defect of what protein?
Explanation
The girl shows clinical features of hereditary motor sensory neuropathy type 1, Charcot-Marie-Tooth disease. The most common type of this autosomal-dominant disease is due to an underlying defect in the gene coding for peripheral myelin protein-22 on chromosome 17. Many other less common mutations have been identified in this family of neuropathies. Dystrophin is a protein that is abnormal in Duchenne's muscular dystrophy, which affects males and is diagnosed earlier. Type I collagen is defective in osteogenesis imperfecta. Alpha-L-iduronidase is defective in mucopolysaccharidosis type I, Hurler's syndrome. Defective cartilage oligomeric matrix protein is associated with some forms of multiple epiphyseal dysplasia. Patel PI, Roa BB, Welcher AA, et al: The gene for the peripheral myelin protein PMP-22 is a candidate for Charcot-Marie-Tooth disease type 1A. Nat Genet 1992;1:159-165.
Question 66
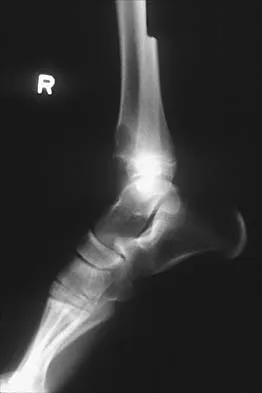
A 12-year-old boy with an ankle fracture undergoes closed reduction under sedation in the emergency department. Figure 27 shows a lateral radiograph of the ankle after two attempts at closed reduction. Based on these findings, treatment should now consist of
Explanation
The widening of the physis associated with incomplete reduction of this fracture suggests that periosteum is interposed at the fracture site. Clinical and animal study findings suggest that the interposed periosteum may lead to premature physeal closure. Repeated forceful attempts at reduction may subject the physis to further injury and should be avoided. Growth problems are common in children with Salter-Harris type I fractures of the lower extremities. Nonunions are rare in children with Salter-Harris type I fractures. Barmada A, Gaynor T, Mubarak SJ: Premature physeal closure following distal tibial physeal fractures: A new radiographic predictor. J Pediatr Orthop 2003;23:733-739.
Question 67
A 9-year-old girl has pain over the fifth toe that is aggravated by shoe wear. Clinical photographs are shown in Figures 28a and 28b. Treatment of this deformity should consist of
Explanation
28b The major obstacle to overcome in the surgical treatment of this cock-up deformity is recurrence. Dorsal releases can be performed; however, chronic dislocation of the fifth MTP joint usually needs to be addressed with plantar release as well. Chronic dorsal soft-tissue contractures may be overcome with translation of the toe into a plantar-based incision, as described originally by Cockin and accredited to Butler. This is the treatment of choice. Resection of the proximal phalanx improves symptoms but induces a secondary deformity; this procedure is usually reserved for skeletally mature individuals. Black GB, Grogan DP, Bobechko WP: Butler arthroplasty for correction of adducted fifth toe: A retrospective study of 36 operations between 1968 and 1982. J Pediatr Orthop 1985;5:439-441. Paton RW: V-Y plasty for correction of varus fifth toe. J Pediatr Orthop 1990;10:248-249.
Question 68
What acetabular procedure for developmental dysplasia of the hip does not require a concentric reduction of the femoral head in the acetabulum?
Explanation
All of the reorientation innominate osteotomies require a concentric reduction of the hip. The Staheli shelf procedure may be performed even with the hip subluxated, but it is a salvage procedure that covers a portion of the femoral head with capsular fibrocartilage rather than hyaline cartilage. Staheli LT, Chew DE: Slotted acetabular augmentation in childhood adolescence. J Pediatr Orthop 1992;12:569-580.
Question 69
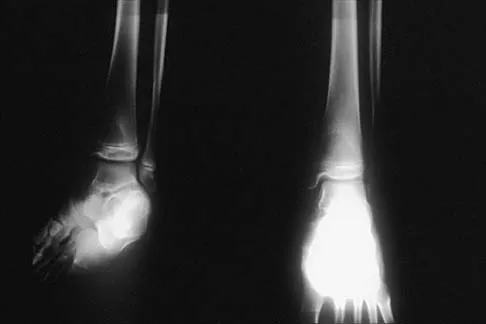
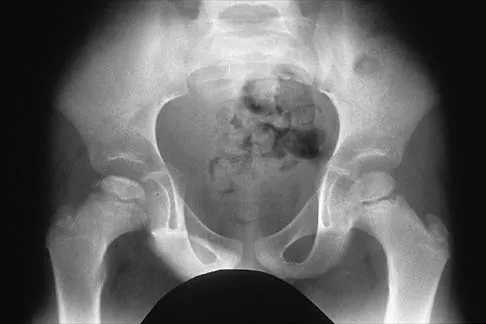
Figure 29 shows the AP radiograph of a 14-year-old boy. The radiographic findings are most consistent with what pathologic process?
Explanation
The severe depression of the proximal medial tibial epiphysis is most consistent with the diagnosis of neglected infantile Blount's disease. Blount's disease in adolescents produces a deformity in the metaphyseal region. Septic arthritis and JRA affect both sides of the joint. Hemophilia produces a characteristic widening of the intercondylar notch. Thompson GH, Carter JR: Late-onset tibia vara (Blount's Disease). Clin Orthop 1990;255:24-35.
Question 70
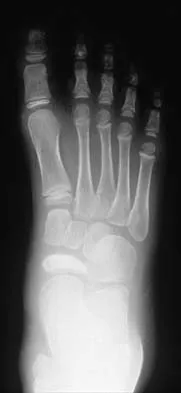
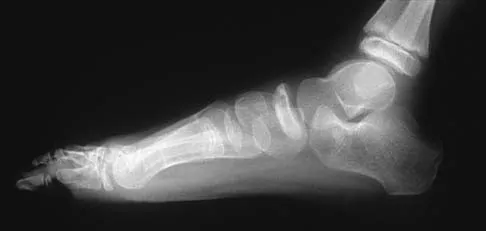
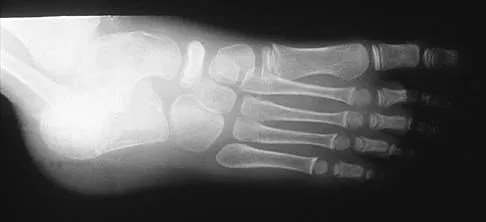
A 5-year-old boy has had pain in the right foot for the past month. Examination reveals tenderness and mild swelling in the region of the tarsal navicular. Radiographs are shown in Figure 30. Management should consist of
Explanation
The child has the classic findings of Kohler's disease or osteochondrosis of the tarsal navicular. The cause of this condition is not known, but osteonecrosis and mechanical compression have been proposed. Children generally report midfoot pain over the tarsal navicular and limping. Physical findings include tenderness, swelling, and occasionally redness in the region of the tarsal navicular. Radiographs show sclerosis and narrowing of the tarsal navicular. The natural history of the condition is spontaneous resolution and reconstitution of the navicular. Symptomatic treatment with restriction of weight bearing or casting is recommended. Karp M: Kohler's disease of the tarsal scaphoid. J Bone Joint Surg 1937;19:84-96.
Question 71
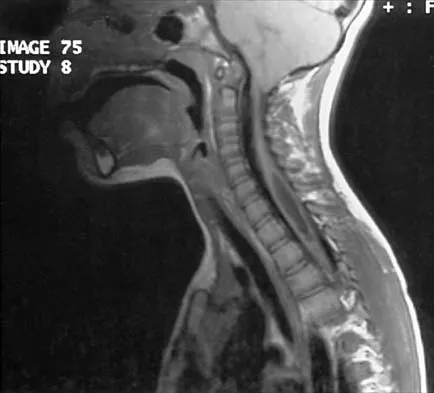
A 9-year-old child sustained a fracture-dislocation of C-5 and C-6 with a complete spinal cord injury. What is the likelihood that scoliosis will develop during the remaining years of his growth?
Explanation
The incidence of late spinal deformity after complete spinal cord injury in children depends on the level of the spinal cord injury and the age of the patient at the time of injury. If a cervical level injury occurs before age 10 years, paralytic scoliosis will develop in virtually 100% of patients. Brown JC, Swank SM, Matta J, et al: Late spinal deformity in quadriplegic children and adolescents. J Pediatr Orthop 1984;4:456-461. Lancourt JE, Dickson JH, Carter RE: Paralytic spinal deformity following traumatic spinal-cord injury in children and adolescents. J Bone Joint Surg Am 1981;63:47-53.
Question 72
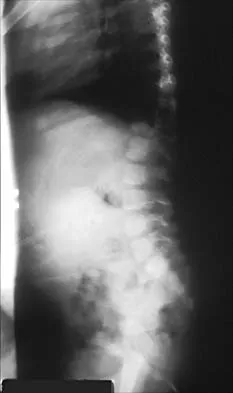
Figures 31a and 31b show the radiograph and MRI scan of an otherwise normal 3-month-old infant who has a spinal deformity. MRI reveals no intraspinal anomalies. What is the next step in management?
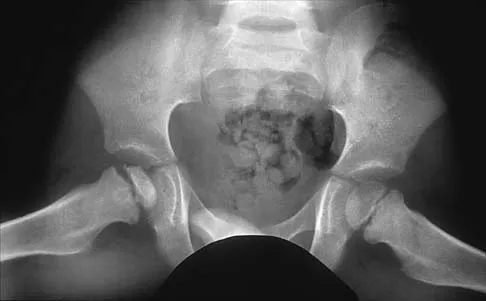
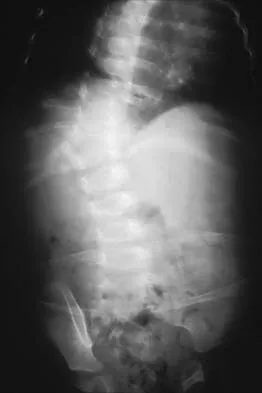
Explanation
31b Congenital scoliosis in an infant warrants evaluation of the renal, cardiac, and neurologic systems because frequently there is concurrent pathology. Progression in this instance is possible but not certain; therefore, progression must be documented prior to any surgical intervention. Close observation with serial radiographs every 4 to 6 months is appropriate. All of the surgical options listed may be reasonable choices in the future, but cardiac evaluation is the most important issue at this time. Basu PS, Elsebaie H, Noordeen MH: Congenital spinal deformity: A comprehensive assessment at presentation. Spine 2002;27:2255-2259.
Question 73
A 22-month-old girl has cerebral palsy. Which of the following findings is a good prognostic indicator of the child's ability to walk in the future?
Explanation
For the parachute test, the examiner holds the child prone and then lowers the child rapidly toward the floor. The parachute reaction is normal or positive if the child reaches toward the floor. The Moro or startle reflex should not be present beyond age 6 months. Asymmetric tonic neck reflex, extensor thrust, and absent foot placement are abnormal findings at any age. Bleck EE: Orthopaedic Management in Cerebral Palsy. Lavenham, Suffolk, The Lavenham Press, 1987, pp 121-139.
Question 74
The husband of a 22-year-old woman has hypophosphatemic rickets. The woman has no orthopaedic abnormalities, but she is concerned about her chances of having a child with the same disease. What should they be told regarding this disorder?
Explanation
Hypophosphatemia is a rare genetic disease usually inherited as an X-linked dominant trait. The fact that the woman has no skeletal manifestations would indicate that the husband has the X-linked mutation. The disease is more severe in boys than it is in girls. The husband will not transmit the disease to his sons. However, all of their daughters will be affected either with the disease or as carriers. If the woman has the disease or the trait, there is a 50% chance that her sons will inherit the disease and a 50% chance that her daughters will be carriers or have a milder form of the disease. Parents should be advised to have genetic counseling so they can be informed when deciding whether to have children. Herring JA: Metabolic and endocrine bone diseases, in Tachdjian's Pediatric Orthopaedics, ed 3. New York, NY, WB Saunders, 2002, pp 1685-1743. Sillence DO: Disorders of bone density, volume, and mineralization, in Rimoin DL, Conner JM, Pyerite RE, et al (eds): Principles and Practice of Medical Genetics, ed 4. New York, NY, Churchill Livingstone, 2002.
Question 75
A 9-year-old boy sustained a traumatic brain injury and right lower extremity trauma in an accident involving a motor vehicle and a pedestrian. Initial evaluation in the emergency department reveals an obtunded patient who is breathing spontaneously and withdraws appropriately to painful stimuli. After initial resuscitation and stabilization, a CT scan reveals a right parietal intracranial hemorrhage. Radiographs of the swollen right thigh are shown in Figures 32a and 32b. Management of the fractured femur should ultimately consist of
Explanation
32b A child with a traumatic brain injury generally achieves significant neurologic recovery and has a more favorable prognosis than an adult. Early stabilization of fractures facilitates transportation of the child for diagnostic tests and decreases the incidence of shortening and malunion. Surgical treatment of the fracture is indicated when cerebral perfusion pressure has stabilized. Casting or traction is not the most appropriate treatment of a femoral fracture in a child of this age with a brain injury. Fracture reduction is difficult to maintain if the brain injury leads to spasticity, and transportation within the hospital for tests is more difficult. Insertion of a reamed antegrade intramedullary nail inserted at the piriformis fossa is associated with a small risk of osteonecrosis of the femoral head. The transverse femoral fracture in this patient is ideally suited for stabilization with flexible intramedullary nails. Ligier and associates treated 123 femoral shaft fractures in children with flexible intramedullary nails, including 35 patients with head injury. In one patient with hemiplegia and a urinary tract infection, a deep wound infection developed, necessitating nail removal. The remaining patients all healed without major complications. Heinrich and associates treated 78 diaphyseal femoral fractures with flexible intramedullary nails, including 14 with head injury. No major complications were reported and all fractures healed. Tolo VT: Management of the multiply injured child, in Rockwood CA, Wilkins KE, Beaty JH (eds): Fractures in Children, ed 4. Philadelphia, PA, Lippincott-Raven, 1996, pp 83-95. Ligier JN, Metaizeau JP, Prevot J, et al: Elastic stable intramedullary nailing of femoral shaft fractures in children. J Bone Joint Surg Br 1988;70:74-77. Heinrich MS, Drvaric DM, Darr K, et al: The operative stabilization of pediatric diaphyseal femur fractures with flexible intramedullary nails: A prospective analysis. J Pediatric Orthop 1994;14:501-507.
Finish Exam?
You cannot change answers after submitting.
