Question 1
During primary total knee arthroplasty, what is the maximum distance the joint line can be raised or lowered before poor motion, joint instability, and increased chance of revision occur?
Explanation
Positioning of the femoral and tibial components is a common cause of early failure of total knee arthroplasty. Two modes of possible position are raising or lowering the joint line from its anatomic level. Raising or lowering the joint line beyond an established threshold can cause limited range of motion, poor patellar function, and possible instability. It has been determined that a threshold of approximately 8 mm provides consistently good results after knee arthroplasty.
Question 2
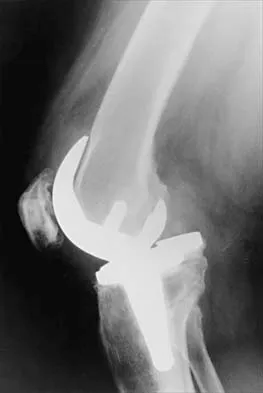
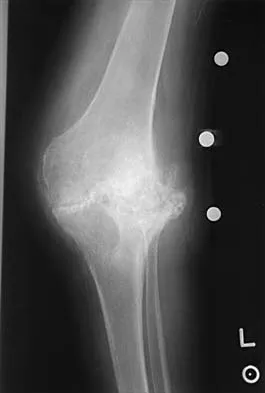
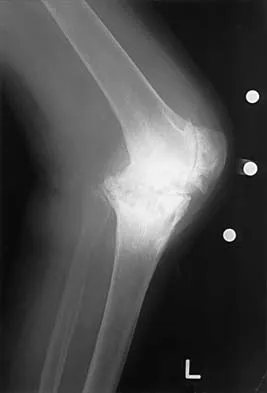
Figure 1 shows the radiograph of an 18-year-old patient who has severe knee pain. Treatment consisting of osteotomy should be perfomed
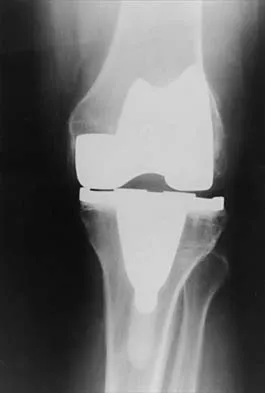
Explanation
Very large corrections of tibial deformity can be achieved at or just below the tibial tubercle. This level of osteotomy maintains the relationship between the tubercle and the rest of the joint, does not alter patellofemoral mechanics, and avoids complicating possible future conversion to total knee arthroplasty. High tibial osteotomy is contraindicated for large corrections because of excessive elevation of the tibial tubercle and overhang of the lateral plateau. Correction in the tibial diaphysis creates a zig zag pattern in the tibia by correcting below the deformity and risks nonunion in cortical bone. There is no evidence that the femur is deformed; therefore, femoral osteotomy is not indicated.
Question 3
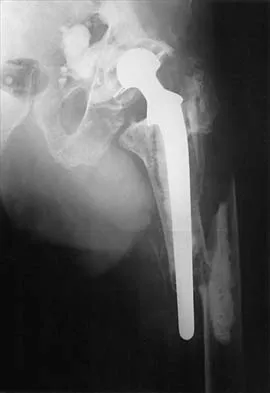
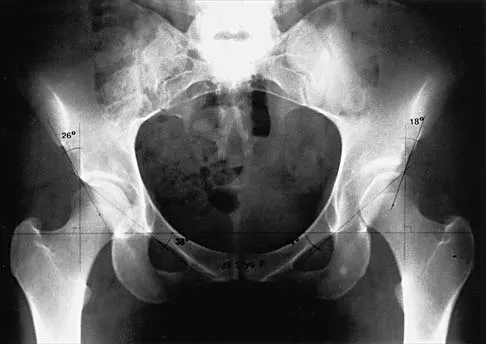
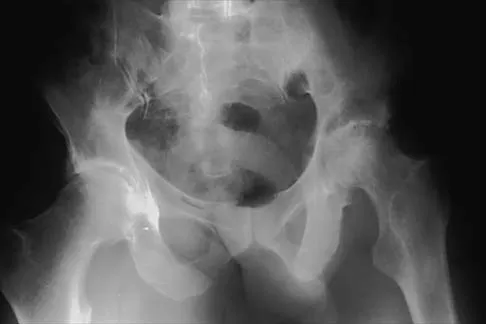
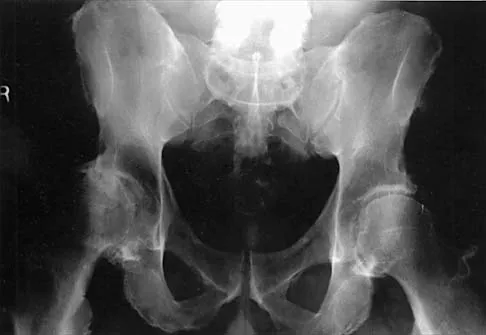
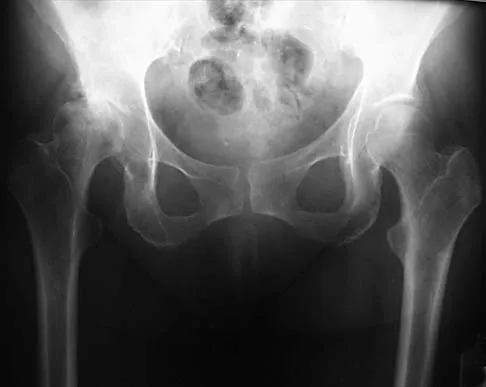
Figure 2 shows the AP radiograph of an 18-year-old woman with progressive and severe right hip pain. Nonsteroidal anti-inflammatory drugs no longer control her pain. What is the next most appropriate step in management?
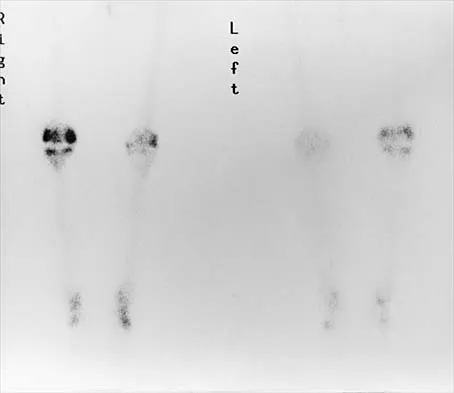
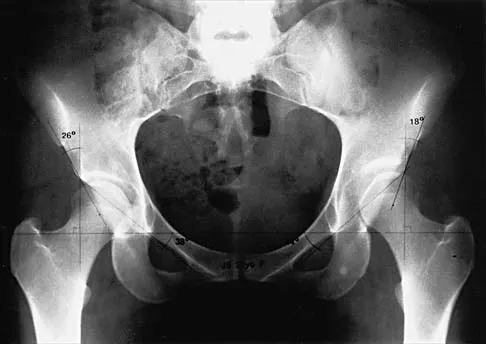
Explanation
A concentric hip with acetabular dysplasia in a symptomatic patient is best treated by periacetabular osteotomy. The Salter osteotomy is less optimal because the method has limited correction, is uniaxial, cannot be tailored to the deformity, and lateralizes the entire hip joint, thereby increasing the joint reactive forces. Because the hyaline cartilage of the joint is histologically normal, rotating the hyaline cartilage into an optimal position is preferable to augmenting the acetabulum with a shelf or by Chiari osteotomy. Varus intertrochanteric osteotomy has no significant role in the treatment of acetabular dysplasia. Total hip arthroplasty may be required in the future but should not be the first choice.
Question 4
Which of the following findings is a prerequisite for a high tibial valgus osteotomy for medial compartment gonarthrosis?
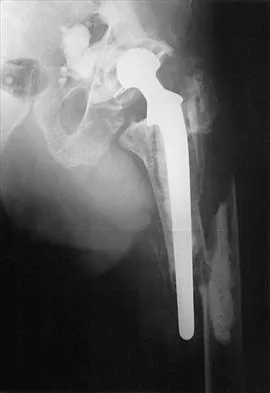
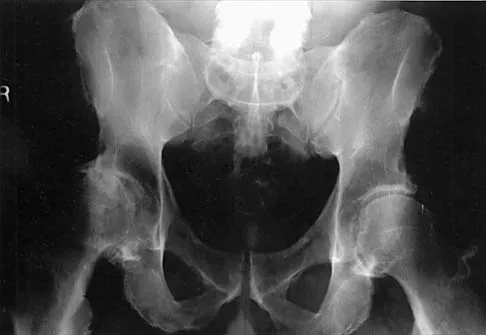
Explanation
The indications for high tibial valgus osteotomy include a physiologically young age, arthritis confined to the medial compartment, 10 to 15 degrees of varus alignment on weight-bearing radiographs, a preoperative arc of motion of at least 90 degrees, flexion contracture of less than 15 degrees, and a motivated, compliant patient. Contraindications include lateral compartment narrowing of the articular cartilage, lateral tibial subluxation of greater than 1 cm, medial compartment bone loss, ligamentous instability, and inflammatory arthritis. Naudie D, Bourne RB, Rorabeck CH, Bourne TT: The Insall Award: Survivorship of the high tibial valgus osteotomy. A 10- to 22-year followup study. Clin Orthop 1999;367:18-27.
Question 5
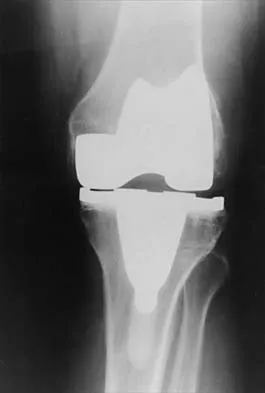
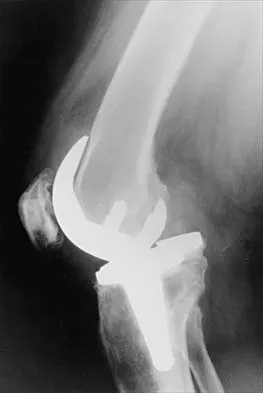
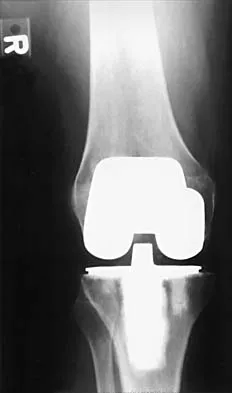
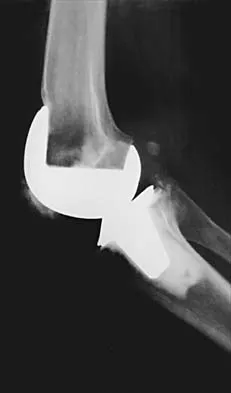
Figures 3a and 3b show the current radiographs of a 58-year-old man who underwent total knee arthroplasty with a cruciate ligament sparing prosthesis 7 years ago. Examination reveals boggy synovitis and moderate pain, particularly anteriorly. Management should consist of
Explanation
3b The patient has symptoms of synovitis that are most likely the result of the release of particles from the tibial polyethylene. While observation may be warranted in a completely asymtomatic knee, some intervention is indicated for this patient as there is clear radiographic evidence of lysis in both the tibia and femur. The decision about the extent of the revision should be made at the time of surgery. A limited incision technique is not indicated. Grafting (or using graft substitute) the defect is the most appropriate approach for treating the osteolytic lesions. While a posterior stabilized prosthesis might be the solution, surgical findings might dictate otherwise.
Question 6
What is the main benefit of using metal-backed tibial components in total knee arthroplasty?
Explanation
In a normal knee, the hard subchondral bone helps to distribute loads across the joint surface. A metal-backed tibial component in total knee arthroplasty decreases the compressive stresses on the underlying, softer cancellous bone by distributing the load over a larger surface area, particularly when one condyle is loaded. Although metallic base plates also increase the tensile forces on the other condyle when one is loaded and may decrease the thickness of the polyethylene tray, these are not benefits. Compressive forces on the polyethylene tray are increased with metal backing. The conformity of the articular surfaces is not affected by metal backing of the tibial component.
Question 7
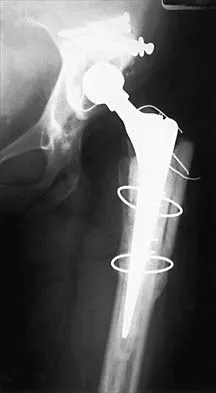
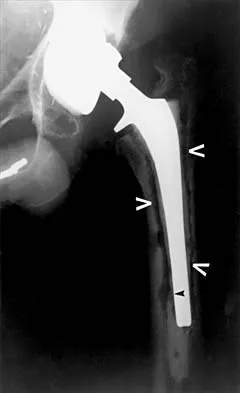
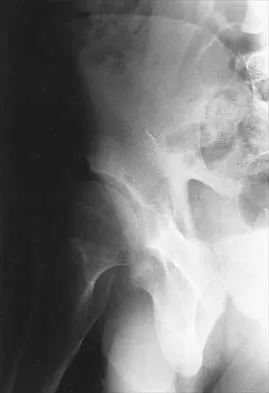
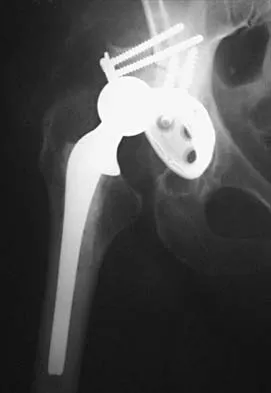
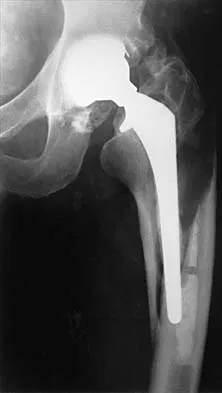
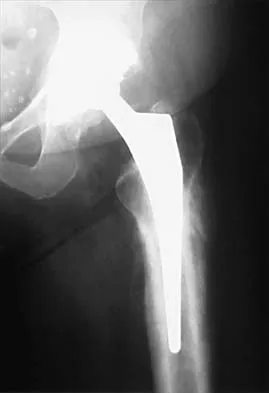
Figures 4a and 4b show the radiographs of a 32-year-old man who has right groin pain with activity or prolonged standing. Which of the following factors would not prohibit consideration of acetabular liner exchange and grafting of the defects?
Explanation
4b Polyethylene particles generated as mechanical wear debris can be phagocytized by macrophages and enter a metabolically active state that releases cytokines, causing periprosthetic bone resorption. Significant osteolysis can occur in the pelvis with a porous-coated cementless socket without loosening of the component. If the acetabular component is modular, well positioned, well-designed with a good survivorship record, and remains undamaged after liner removal, the polyethylene liner can be exchanged and the lytic defects can be debrided and bone grafted. This implant is well positioned, has a good survivorship record, a good locking mechanism, and is modular. The hip arthroplasty needs to be aseptic for consideration of liner exchange. Maloney WJ, Herzwurm P, Paprosky W, Rubash HE, Engh CA: Treatment of pelvic osteolysis associated with a stable acetabular component inserted without cement as part of a total hip replacement. J Bone Joint Surg Am 1997;79:1628-1634.
Question 8
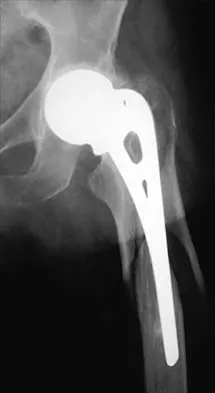
A patient who underwent total knee arthroplasty 6 years ago now reports knee pain for the past 3 days following dental surgery. Cultures of the aspirate are positive for Staphylococcus epidermidis. Management should consist of
Explanation
The patient has an early prosthesis infection as a result of hematogenous seeding from dental surgery. Irrigation and debridement with polyethylene exchange and IV antibiotics have been successful in early postoperative infections; it is less likely to be effective for a late hematogenous infection. Immediate total component exchange also may be effective, but it should be reserved for failure of irrigation and debridement. Pellicci PM, Tria AJ Jr, Garvin KL (eds): Orthopaedic Knowledge Update: Hip and Knee Reconstruction 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2000, pp 323-337.
Question 9
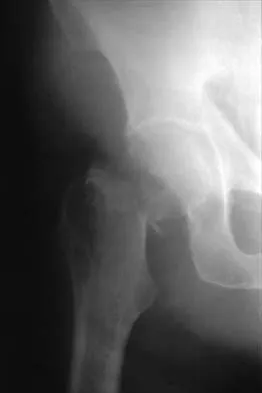
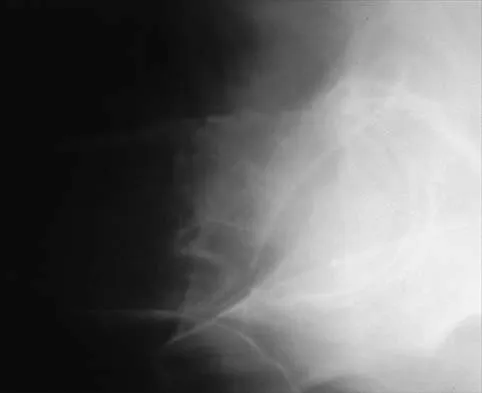
A 32-year-old woman with systemic lupus erythematosus treated with methotrexate and oral corticosteroids reports right groin pain with ambulation and night pain. Examination reveals pain with internal and external rotation and flexion that is limited to 105 degrees because of discomfort. Laboratory studies show a serum WBC of 9.0/mm3 and an erythrocyte sedimentation rate of 35 mm/h. Figures 5a and 5b show AP and lateral radiographs of the right hip. Further evaluation should include
Explanation
5b The radiographs show Ficat and Arlet stage 2 osteonecrosis. The femoral head remains round, and there are sclerotic changes in the superolateral quadrant. Patients with systemic lupus erythematosus are at risk for osteonecrosis because of prednisone use and the underlying metabolic changes associated with the condition (hypofibrinolysis and thrombophilia). MRI is the best diagnostic method for detecting osteonecrosis, with a greater than 98% sensitivity and specificity. For this patient, an MRI can assess the contralateral hip for any involvement and can quantify the extent of the lesion. Mont MA, Jones LC, Sotereanos DG, Amstutz HC, Hungerford DS: Understanding and treating osteonecrosis of the femoral head. Instr Course Lect 2000;49:169-185.
Question 10
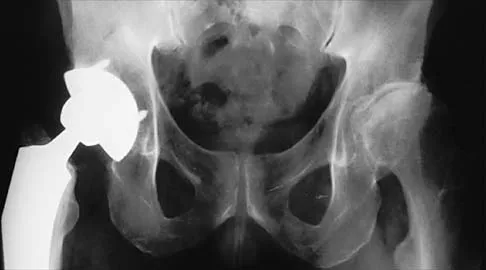
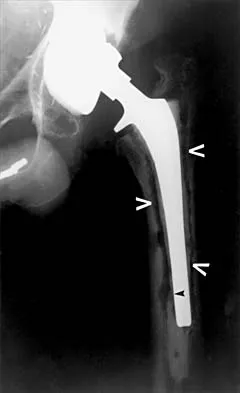
An otherwise healthy 57-year-old man has persistent, severe hip pain after undergoing total hip arthroplasty 3 months ago. What is the next most appropriate step in management?
Explanation
Any patient who is severely symptomatic this quickly after surgery must be evaluated for infection. Loosening is also a possible cause, but infection must be ruled-out. Bone scans are not helpful at this early postoperative stage. Normal laboratory values argue strongly against infection, but when abnormal, need to be supplemented with a hip aspiration. Aspiration remains the most selective and sensitive measure, especially when linked to a WBC count of the synovial tissues in the joint. There is no indication for an antiobiotic trial because it may make future culture sensitivity more difficult. Drancourt M, Stein A, Argenson JN, et al: Oral rifampin plus ofloxacin for treatment of staphylococcus-infected orthopedic implants. Antimicrob Agents Chemother 1993;37:1214-1218. Duncan CP, Beauchamp C: A temporary antibiotic-loaded joint replacement system for the management of complex infections involving the hip. Orthop Clin North Am 1993; 24: 751-759.
Question 11
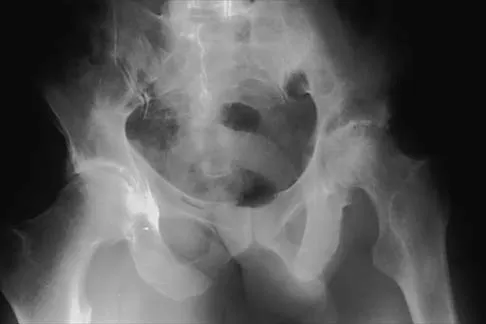
A 61-year-old man reports right hip pain and limited motion after undergoing total hip arthroplasty for posttraumatic arthritis 1 year ago. Figure 6 shows an AP radiograph of the pelvis. To improve motion and relieve pain, management should consist of
Explanation
The patient has symptomatic grade IV Brooker heterotopic ossification. Once the bone has matured, it can be excised. Surgical excision should be combined with postoperative irradiation to avoid recurrence. Pharmacologic and irradiation intervention are not successful beyond the perioperative period unless they are combined with surgical excision of mature heterotopic ossification. Koval KJ (ed): Orthopaedic Knowledge Update 7. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 417-451.
Question 12
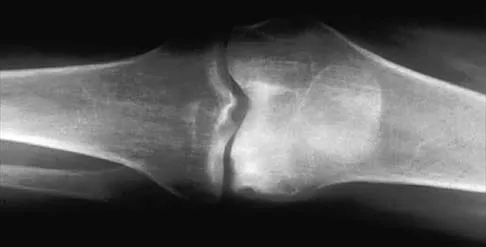
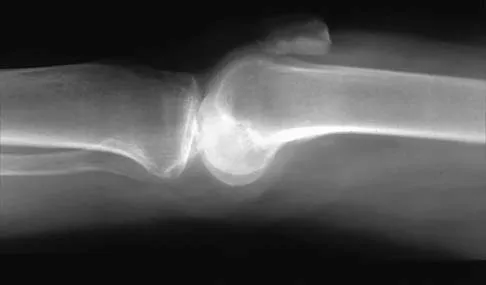
Osteolysis after total knee arthroplasty can be minimized through prosthetic design features such as
Explanation
The incidence of osteolysis is minimal in studies reporting the use of all polyethylene or monolithic metal-backed tibial components. Osteolysis has been reported in patients with total knee arthroplasties using cementless implants with modular components. Micromotion between the tibial tray and the polyethylene results in backside wear, leading to osteolysis. Osteolysis also has been reported in cemented posterior cruciate-substituting modular components. O'Rourke and associates reported a 16% incidence of osteolysis in patients with a posterior stabilized implant because of the use of modular polyethylene and the subsequent abrasive wear. Oxidation of the polyethylene that is the result of the method of sterilization and shelf life has also been implicated in the high incidence of osteolysis, along with patient factors such as activity level and weight.
Question 13
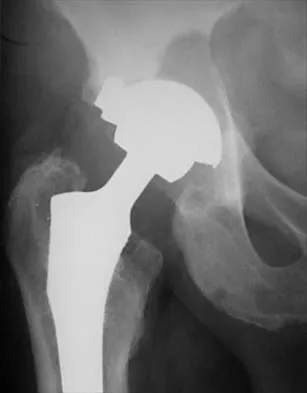
What type of cementless femoral fixation results in the highest rate of distal femoral osteolysis?
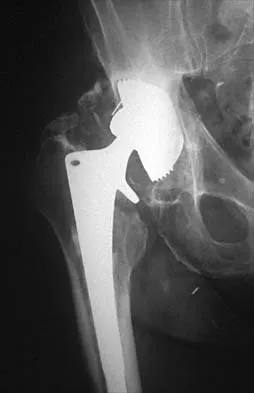
Explanation
Despite the relatively few problems with porous-coated cementless stems, stress shielding and thigh pain do occur. One design feature of proximally coated stems that has been associated with a higher incidence of distal osteolysis is the presence of noncircumferential proximal porous coating. Tapered, modular with sleeve, and hydroxyapatite proximally porous-coated stems have all performed well. Fully porous-coated straight stems have a high survivorship rate as well. Pellicci PM, Tria AJ Jr, Garvin KL (eds): Orthopaedic Knowledge Update: Hip and Knee Reconstruction 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2000, pp 175-180. Koval KJ (ed): Orthopaedic Knowledge Update 7. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 417-451.
Question 14
When performing a total knee arthroplasty using modular components, what is the minimum recommended thickness of an ultra-high molecular weight polyethylene insert for a tibial component?
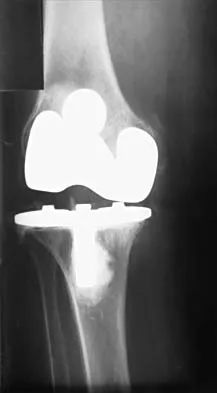
Explanation
Polyethylene wear has been identified as a major contributor to failure of total knee implants, of which thickness is an important factor. Several studies have shown that the minimum thickness should be 6 to 8 mm. While Wright and Bartel have shown that 6 to 8 mm has been recommended as the minimum thickness of an ultra-high molecular weight polyethylene insert for a tibial component in total knee arthroplasty, more recent work by Meding and associates and Worland and associates has verified the clinical efficacy of 4 mm of polyethylene in compression-molded anatomic graduated nonmodular components. Bartel DL, Bicknell VL, Wright TM: The effect of conformity, thickness, and material on stresses in ultra-high molecular weight components for total joint replacement. J Bone Joint Surg Am 1986;68:1041-1051. Wright TM, Bartel DL: The problem of surface damage in polyethylene total knee components. Clin Orthop 1991;273:261-263. Meding JB, Ritter MA, Faris PM: Total knee arthroplasty with 4.4 mm of tibial polyethylene: 10-year followup. Clin Orthop 2001;388:112-117.
Question 15
During total knee arthroplasty using a posterior cruciate-retaining design, excessive tightness in flexion is noted, while the extension gap is felt to be balanced. Which of the following actions will effectively balance the knee?
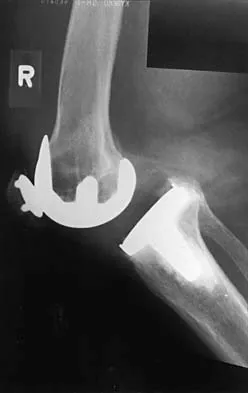
Explanation
Excessive flexion gap tightness can be addressed with a variety of techniques; including: (a) recess and release the posterior cruciate ligament; (b) resect a posterior slope in the tibia; (c) avoid an oversized femoral component that moves the posterior condyles more distally; (d) resect more posterior femoral condyle and use a smaller femoral component placed more anteriorly; and (e) release the tight posterior capsule and balance the collateral ligaments.
Question 16
What is the dominant component of articular cartilage extracellular matrix by weight?
Explanation
Articular cartilage is a highly organized viscoelastic material, and load transmission depends on the specific composition of the extracellular matrix. Articular cartilage is devoid of neural, lymphatic, and blood vessel tissue. The extracellular matrix consists of water, proteoglycans, and collagen. Water comprises most of the wet weight (65% to 80%). Type II collagen comprises 95% of the collagen. The collagen and proteoglycan (keratan sulfate and chondroitin sulfate) matrix and its high water content are responsible for the mechanical properties of the articular cartilage. Buckwalter JA, Mankin HJ: Articular cartilage: Degeneration and osteoarthritis, repair, regeneration, and transplantation. Inst Course Lect 1998;47:487-504.
Question 17
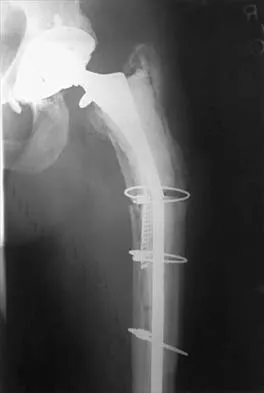
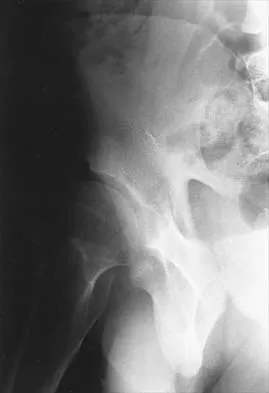
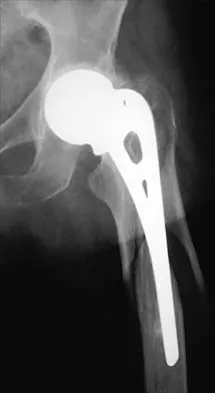
A 70-year-old man underwent primary total knee arthroplasty 3 months ago. Figures 7a and 7b show the radiograph and clinical photograph following incision and drainage of the wound 1 week ago. Aspiration of the joint reveals methicillin-sensitive Staphylococcus aureus. What is the next most appropriate step in management?
Explanation
7b The overriding factor determining treatment in this case is the appearance of the surgical wound. Based on MacPhearson's work, this "C" wound is best managed with two-stage exchange. The functional outcome is markedly diminished following a knee arthrodesis compared to revision knee arthroplasty. Harwin SF: The diagnosis and management of infected total knee replacement. Seminars Arthroplasty 2002;13:9-22. Goldmann RT, Scuderi GR, Insall JN: 2-stage reimplantation for infected total knee replacement. Clin Orthop 1996;331:118-124.
Question 18
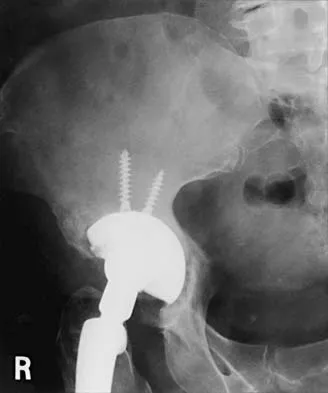
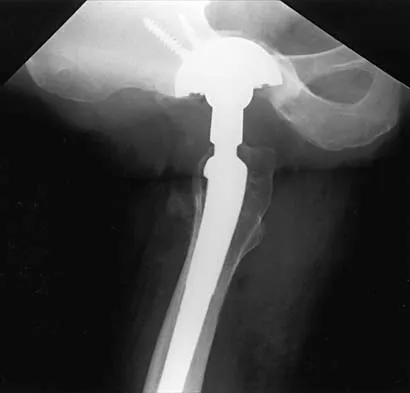
A 35-year-old male laborer with isolated posttraumatic degenerative arthritis of the right hip undergoes the procedure shown in Figure 8. What is the most appropriate position of the right lower extremity?
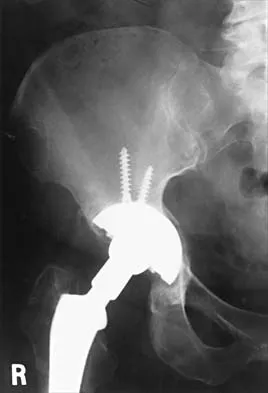
Explanation
The primary indication for hip arthrodesis is isolated unilateral hip disease in a young, active patient. Avoiding abductor damage and preserving proximal femoral anatomy are imperative to allow conversion to a future total hip arthroplasty. Optimal positioning is 30 degrees of flexion to allow swing-through. Neutral abduction and adduction and slight external rotation allow the most efficient gait while allowing sufficient support in stance. A small degree of adduction is acceptable for a successful hip arthrodesis. Callaghan JJ, Brand RA, Pedersen DR: Hip arthrodesis: A long term follow-up. J Bone Joint Surg Am 1985;67:1328-1335.
Question 19
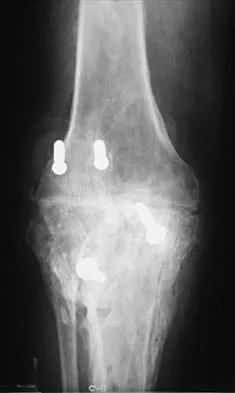
Which of the following factors can contribute to patellar subluxation following routine total knee arthroplasty?
Explanation
Excessive resection of the lateral facet of the patella can lead to subluxation. Rotational alignment of the components can have a significant impact on patellar tracking. Internal rotation of the femoral component leads to more lateral alignment of the patella within the trochlear groove. Internal rotation and medial placement of the tibial component results in lateralization of the tibial tubercle with an increase in the Q angle. Excessive valgus alignment of the mechanical axis, or insufficient correction of preoperative valgus, has a similar effect on the Q angle, and both can result in a higher rate of tracking problems.
Question 20
When an adult hip is surgically dislocated for relief of femoro-acetabular impingment, what is the risk of postoperative iatrogenic osteonecrosis?
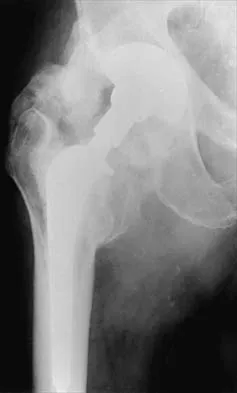
Explanation
In a report of more than 70 hips treated by surgical dislocation, iatrogenic osteonecrosis failed to develop in any of the hips.
Question 21
What is the most frequent late complication of cementless fixation in total knee arthroplasty?
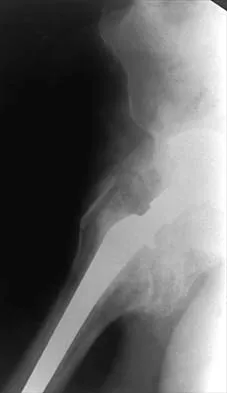
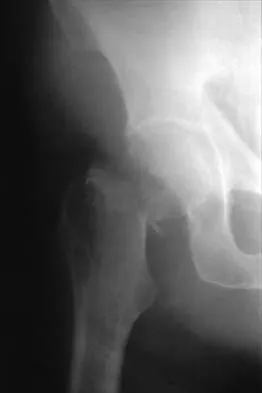
Explanation
The incidence of osteolysis, particularly around fixation screws in the tibia, can be as high as 30%. Stable femoral component fixation is generally maintained. Infection, subluxation of the patella, and stiffness can occur with either cemented or cementless fixation. Peters PC, Engh GA, Dwyer KA, Vinh TN: Osteolysis after total knee arthroplasty without cement. J Bone Joint Surg Am 1992;74:864-876.
Question 22
In the treatment of acetabular dysplasia, what type of pelvic osteotomy leaves the "teardrop" in its original position and redirects the acetabulum?
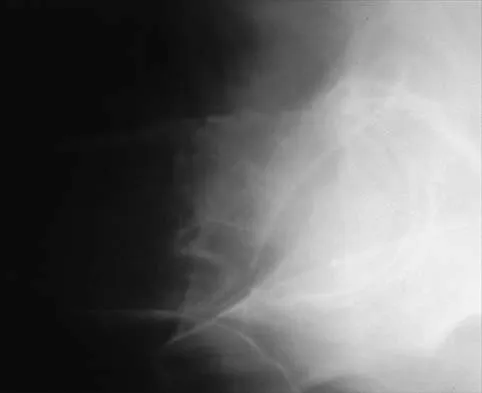
Explanation
The dial or spherical osteotomy leaves the medial wall or teardrop in its original position and, as a result, is intra-articular. The other pelvic osteotomies (except Chiari) redirect the acetabulum, including the medial wall. The Chiari osteotomy improves coverage without redirecting the acetabulum within the pelvis, and it leaves the teardrop in the same place. Lack W, Windhager R, Kutschera HP, Engel A: Chiari pelvic osteotomy for osteoarthritis secondary to hip dysplasia: Indications and long-term results. J Bone Joint Surg Br 1991;73:229-234. Ganz R, Klaue K, Vinh TS, Mast JW: A new periacetabular osteotomy for the treatment of hip dysplasias: Technique and preliminary results. Clin Orthop 1988;232:26-36.
Question 23
What is the correct order of the elastic modulus of the following materials from greatest to least?
Explanation
In Young's modulus of elasticity, E is a measure of the stiffness of a material and its ability to resist deformation. In the elastic region of the stress-stain curve, E = stress/strain. The moduli of elasticity for these materials are alumina ceramic = 380 Gigapascals (GPa), cobalt-chromium = 210 GPa, stainless steel = 190 GPa, titanium = 116 GPa, and PMMA = 1.1 to 4.1 GPa. Buckwalter JA, Einhorn TA, Simon SR (eds): Orthopaedic Basic Science, ed 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2000, pp 182-215.
Question 24
Compared to similar patients who do not donate autologous blood, patients with normal baseline hemoglobin who donate autologous blood prior to undergoing primary total hip arthroplasty are likely to
Explanation
Billote and associates compared patients with normal baseline hemoglobin levels who did and did not donate autologous blood prior to total hip arthroplasty. No patients received allogeneic blood perioperatively, and the autologous donors had significantly lower hemoglobin levels at the time of surgery and in the recovery room. Of the autologous donors, 69% received an autologous transfusion. The authors concluded that autologous donation was unnecessary in patients undergoing primary total hip arthroplasty who had a normal hemoglobin. Billote D, Glisson SN, Green D, Wixson RL: A prospective, randomized study of preoperative autologous donation for hip replacement surgery. J Bone Joint Surg Am 2002;84:1299-1304.
Question 25
Which of the following best describes the resultant forces on an increased offset stem when compared with a standard offset stem?
Explanation
The increased emphasis on restoring offset in total hip arthroplasty has implications for the forces applied to the components and the fixation interfaces. Static analysis has shown that with an increased affect, joint reaction force on the articulation is decreased. When the resultant load on the hip is "out of plane" (ie, directed anterior to posterior), there is increased torsion where the stem is turned into more retroversion. Buckwalter JA, Einhorn TA, Simon SR (eds): Orthopaedic Basic Science, ed 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2000, pp 134-180. Hurwitz DE, Andriaacchi TP: Biomechanics of the hip, in Callaghan J, Rosenberg AG, Rubash HE (eds): The Adult Hip. Philadelphia, PA, Lippincott-Raven , 1998.
Finish Exam?
You cannot change answers after submitting.
