Orthopedic Board Exam MCQs: Arthroplasty & Trauma Practice | Part 156

Key Takeaway
This page offers Part 156 of an OITE & AAOS Orthopedic Board Review quiz. It provides 100 verified, high-yield MCQs, formatted like official exams, with detailed explanations. Designed for orthopedic residents and surgeons, it's crucial for board certification exam preparation.
About This Board Review Set
This is Part 156 of the comprehensive OITE and AAOS Orthopedic Surgery Board Review series authored by Dr. Mohammed Hutaif, Consultant Orthopedic & Spine Surgeon.
This set has been strictly audited and contains 100 100% verified, high-yield multiple-choice questions (MCQs) modelled on the exact format of the Orthopaedic In-Training Examination (OITE) and the American Academy of Orthopaedic Surgeons (AAOS) board examinations.
How to Use the Interactive Quiz
Two distinct learning modes are available:
- Study Mode — After selecting an answer, you immediately see whether you are correct or incorrect, together with a full clinical explanation and literature references.
- Exam Mode — All feedback is hidden until you click Submit & See Results. A live timer tracks elapsed time. A percentage score and detailed breakdown are displayed upon submission.
Pro Tip: Use keyboard shortcuts A–E to select options, F to flag a question for review, and Enter to jump to the next unanswered question.
Topics Covered in Part 156
This module focuses heavily on: Arthroplasty, Elbow, Fracture, Hip, Infection, Knee, Revision, Shoulder, Tumor.
Sample Questions from This Set
Sample Question 1: Figures 9a and 9b show the radiographs of a 75-year-old man who underwent a revision total knee arthroplasty with a long-stemmed tibial component. In rehabilitation, he reports fullness and tenderness in the proximal medial leg (at the knee...
Sample Question 2: A 51-year-old man sustained an open fracture of his tibia in Korea 42 years ago. An infection developed and it was resolved with surgical treatment. For the past 6 months, an ulcer with mild drainage has developed over the medial tibia. The...
Sample Question 3: Serum phosphate levels are high.Tumoral calcinosis is a heritable condition that is characterized by periarticular metastatic calcification. Most patients are black, and the inheritance is usually autosomal recessive. Metastatic calcificati...
Sample Question 4: -Where is the physis with the highest growth rate (in mm per year) located?...
Sample Question 5: If a surgeon inadvertently burrs through the midlateral wall of C5 during a anterior corpectomy, what structure is at greatest risk for injury? Review Topic...
Why Active MCQ Practice Works
Evidence consistently demonstrates that active recall through spaced MCQ practice yields substantially greater long-term retention than passive reading alone (Roediger & Karpicke, 2006). All questions in this specific module have been algorithmically verified for clinical integrity and complete explanations.
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
Figures 9a and 9b show the radiographs of a 75-year-old man who underwent a revision total knee arthroplasty with a long-stemmed tibial component. In rehabilitation, he reports fullness and tenderness in the proximal medial leg (at the knee). The strategy that would best limit this postoperative problem is use of
Explanation
REFERENCE: Gustke K: Cemented tibial stems are not requisite in revision. Orthopedics 2004;27:991-992.
Question 2
A 51-year-old man sustained an open fracture of his tibia in Korea 42 years ago. An infection developed and it was resolved with surgical treatment. For the past 6 months, an ulcer with mild drainage has developed over the medial tibia. The ulcer is small and there is minimal erythema at the ulcer site. A radiograph and MRI scan are shown in Figures 43a and Figure 43b. Initial cultures show Staphylococcus aureus susceptible to the most appropriate antibiotics. Laboratory studies show an erythrocyte sedimentation rate of 70 mm/h. What is the most appropriate surgical treatment at this time?
Explanation
REFERENCES: Patzakis MJ, Zalavras CG: Chronic posttraumatic osteomyelitis and infected nonunion of the tibia: Current management concepts. J Am Acad Orthop Surg 2005;13:417-427.
Beals RK, Bryant RE: The treatment of chronic open osteomyelitis of the tibia in adults.
Clin Orthop Relat Res 2005;433:212-217.
Question 3
Serum phosphate levels are high. Tumoral calcinosis is a heritable condition that is characterized by periarticular metastatic calcification. Most patients are black, and the inheritance is usually autosomal recessive. Metastatic calcifications occur around joints and in the skin, marrow, teeth, and blood vessels. The periarticular masses may grow quite large and are attached to the fascia, but they are extra-articular. The masses may occur at the shoulder, hip, and elbow. Radiographically: The masses are composed of heavy, amorphous calcification in nodules. Laboratory:
Explanation
Question 4
-Where is the physis with the highest growth rate (in mm per year) located?
Explanation
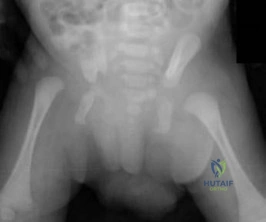
Question 5
If a surgeon inadvertently burrs through the midlateral wall of C5 during a anterior corpectomy, what structure is at greatest risk for injury? Review Topic
Explanation
(SBQ12SP.54) Integrity of the posterior ligamentous complex (PLC) is a critical predictor of spinal fracture stability. Components of the PLC include the supraspinous ligament, interspinous ligament, ligamentum flavum and: Review Topic
Facet joint capsules
Facet joint capsules, and facet joints
Facet joint capsules, facet joints, and the posterior longitudinal ligament
Facet joint capsules, and the posterior longitudinal ligament
Posterior longitudinal ligament
Components of the PLC include the supraspinous ligament, interspinous ligament, ligamentum flavum and facet joint capsules.
Numerous methods have been used to evaluate for PLC injury. Palpation is unreliable and has low accuracy. Radiographs can show characteristic flexion-distraction fracture patterns with widening or malaligment of the spinous processes. Computed tomography (CT) is more reliable than radiographs to provide indirect evidence of ligament injury. Magnetic resonance image (MRI) can provide direct evidence of soft-tissue injury, making it the preferred method in diagnosing ligamentous injury. However, MRI may not always be utilized due to situations involving emergency operations or contraindications to MRI, such as certain metal implants.
Vaccaro et al. introduced a new classification system for thoracolumbar injuries, TLICS, based on morphological appearance, integrity of the posterior ligamentous complex, and neurological status. They advocate use of the system for nonoperative versus operative decision making and communication between surgeons.
Varccaro et al. sought to determine the accuracy of magnetic resonance imaging (MRI) in diagnosing injury of the posterior ligamentous complex (PLC) in patients with thoracolumbar trauma. Forty-two patients with 62 levels of injury were studied. The sensitivity for the various PLC components ranged from 79% (left facet capsule) to 90% (interspinous ligament). The specificity ranged from 53% (thoracolumbar fascia) to 65% (ligamentum flavum). They concluded that the integrity of the PLC as determined by MRI should not be used in isolation to determine treatment.
Incorrect Answers:
Question 6
Which of the following diagnostic studies best distinguishes Ewing’s sarcoma from small cell osteosarcoma?
Explanation
REFERENCES: Perotti D, Corletto V, Giardini R, Parafioriti A, Fossati-Bellani F, Luksch R: Retrospective analysis of ploidy in primary osseous and extraosseous Ewing family tumors in children. Tumori 1998;84:493-498.
Riley RD, Burchill SA, Abrams KR, Heney D, Sutton AJ, Jones DR, et al: A systematic review of molecular and biological markers in tumours of the Ewing’s sarcoma family. Eur J Cancer 2003;39:19-30.
Menendez LR (ed): Orthopaedic Knowledge Update: Musculoskeletal Tumors. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 11-20.
Question 7
The photomicrograph seen in Figure 41 shows which of the following conditions?
Explanation
REFERENCES: Krall RA, Kostianovsky M, Patchefsky AS: Synovial sarcoma: A clinical, pathological and ultrastructural study of 26 cases supporting the recognition of a monophasic variant. Am J Surg Pathol 1981;5:137-151.
Wright PH, Sim FH, Soule EH, Taylor WF: Synovial sarcoma. J Bone Joint Surg Am 1982;64:112-122.
Question 8
- The Magnetic resonance imaging signal characteristics of a high-grade soft-tissue sarcoma are best described as
Explanation
other characteristics, such as size, pattern of growth, integrity of natural boundaries, and homogeneity.
Intravenous contrast agents are not necessary to evaluate neurovascular structures. Both the T1 & T2 weighted images are essential to detect and characterize soft tissue lesions.
Most Tumors have long T1 and T2 relaxation times, therefore, in most instances signal intensity alone is of limited benefit. Exceptions are lipoma, hematoma, intra-lesional hemorrhage.
Hemorrhage may occur in some soft tissue lesions, especially sarcomas, leading to the low T1 and high T2 intensity sound on MR. Miller, indicates that Water, CSF, acute hemorrhage and soft tissue tumors appear dark on T1 and light on T2.
Question 9
A 23-year-old student complains of recurrent left shoulder instability. He first dislocated his shoulder in high school while playing lacrosse and was managed with physical therapy. A second dislocation occurred one year later while skiing. He has since sustained two more dislocations and says that his shoulder feels “loose.” Examination reveals grade II anterior load and shift, positive apprehension and relocation tests, and normal rotator cuff strength. An MRI arthrogram is ordered and surgical treatment is recommended. What factor would most strongly represent an indication for a procedure including bone augmentation (e.g. Latarjet) rather than a soft-tissue-only stabilization (isolated labral repair/capsulorrhaphy)?
Explanation
glenoid bone augmentation. A large Hill-Sachs lesion may be an indication for glenoid augmentation, primarily if it is in a location/orientation that engages the anterior glenoid rim. These are referred to as “off-track” lesions. Of these choices, the strongest indication for a Latarjet coracoid transfer or similar bone augmentation (other options include iliac crest autograft or distal tibial allograft) is high-grade glenoid bone loss. Classically, this is performed through an open approach, although arthroscopic techniques are increasing in popularity. Although the critical amount of bone loss is debated, most surgeons and studies suggest a cut-off of approximately 20% to 25%, above
which isolated soft-tissue stabilization alone is less likely to be successful in the long-term.
Question 10
A 67-year-old man with right shoulder osteoarthritis (OA) remains symptomatic despite a course of nonsurgical treatment. A CT scan of the shoulder shows eccentric posterior glenoid wear with 10° of retroversion. What is the appropriate management of this glenoid bone loss during surgery for an anatomic total shoulder arthroplasty?
Explanation
glenoid bone grafting may be considered for glenoid retroversion >15°.
Question 11
A 17-year-old high school football player sustains a traumatic anterior shoulder dislocation, resulting in a small bony Bankart lesion and small Hill-Sachs lesion. The patient undergoes an arthroscopic Bankart repair with incorporation of the bone fragment and returns to play football the following year. He has a recurrent dislocation at football practice but decides to finish the football season before considering additional treatment. He sustains nine additional dislocations, with the last dislocation occurring while sleeping.What diagnostic test is most appropriate when planning revision surgery?
Explanation
more likely to have pain after surgery. Age and activity level are lesser influences on satisfaction.
Question 12
Which of the following factors is associated with the worst prognosis in soft-tissue sarcomas?
Explanation
REFERENCES: Collin C, Goobold J, Hadju SI, Brennan MF: Localized extremity soft tissue sarcoma: An analysis of factors affecting survival. J Clin Oncol 1987;5:601-612.
Eilber FC, Rosen G, Nelson SE, et al: High-grade extremity soft tissue sarcomas: Factors predictive of local recurrence and its effect on morbidity and mortality.
Ann Surg 2003;237:218-226.
Question 13
A baseball player reports a dull pain in the posterior aspect of his throwing arm. Examination reveals decreased internal rotation and prominence of the inferomedial corner of the scapula. An MRI scan suggests a partial-thickness tear of the posterior supraspinatus tendon. Successful treatment would most likely include which of the following? Review Topic
Explanation
required, and capsulolabral imbrication is more consistent with the surgical treatment for multidirectional instability.
Question 14
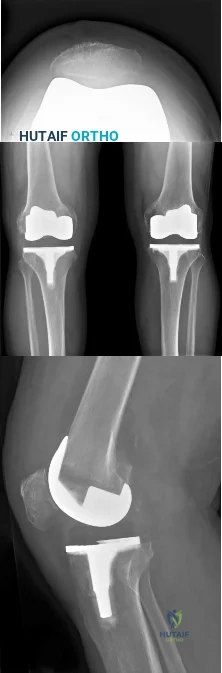
Polyethylene wear of the bearing surface has been recognized as a mode of failure in total knee arthroplasty; therefore, many patients are offered polyethylene exchange. In terms of success rates, this surgical procedure has been reported to have a
Explanation
REFERENCES: Wasielewski RC, Parks N, Williams I, et al: Tibial insert undersurface as a contributing source of polyethylene wear debris. Clin Orthop 1997;345:53-59.
Engh GA, Koralewicz LM, Pereles TR: Clinical results of modular polyethylene insert exchange with retention of total knee arthroplasty components. J Bone Joint Surg Am 2000;82:516-523.
Question 15
A 12-year-old girl has had progressive left knee pain for the past 4 months. She reports that the pain is unrelated to activity, and she has no history of fever or recent infections. Examination reveals full range of motion of the knee but tenderness along the medial joint line. Plain radiographs and MRI scans are shown in Figures 39a through 39d. A biopsy specimen of the lesion is shown in Figure 39e. Treatment should include
Explanation
REFERENCE: Springfield DS, Capanna R, Gherlinzoni F, Picci P, Campanacci M: Chondroblastoma: A review of seventy cases. J Bone Joint Surg Am 1985;67:748-755.
Question 16
-Figure 235 is the radiograph of a 75-year-old woman who is seen in the emergency department following a low-energy fall. What is the most appropriate treatment based on her radiographic findings?
Explanation
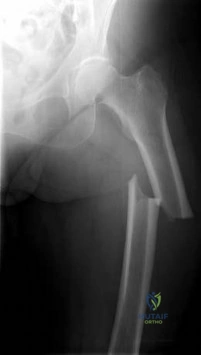
Question 17
-Assuming that the lesion can be covered appropriately and there is no drainage from the lesion, when should the patient be allowed to safely return to wrestling?
Explanation
This patient has cellulitis, which is typically caused by group A Streptococcus or Staphylococcus. The patient’s lack of improvement with first-line antibiotics is concerning for methicillin-resistant Staphylococcus aureus (MRSA) infection. MRSA cellulitis is becoming more prevalent in young athletes,and a high index of suspicion is required to provide appropriate intervention during this
aggressive disease process. The diagnosis is typically made clinically without the use of cultures. Oral trimethoprimsulfamethoxazole (a sulfonamide-class drug) double strength twice daily for 10 to 14 days or doxycycline (a tetracycline-class drug) 100 mg twice daily for 10 to 14 days are recommended for first-line treatment of suspected MRSA cellulitis. There is no indication to proceed with irrigation and debridement; however, if the patient develops a soft-tissue abscess or the underlying joint becomes involved, this would be an appropriate intervention. Switching the athlete to an IV cephalosporin (cefazolin) is not likely to be effective against the presumed resistant bacteria.
Ciprofloxacin (a fluoroquinolone-class drug) is effective against many bacteria, but not MRSA. The current recommendation for wrestlers with cellulitis is that return to competition be allowed after 72 hours of antibiotic treatment if there has been no extension of the cellulitis for 48 hours, the lesion can be covered, and there is no drainage from the lesion. The other responses are not current recommendations for return to competition.
Question 18
A 75-year-old woman undergoes hybrid total hip arthroplasty for osteoarthritis. A postoperative radiograph obtained in the recovery room is shown in Figure 18. Treatment should now consist of
Explanation
REFERENCES: Lee SR, Bostrom MP: Periprosthetic fractures of the femur after total hip arthroplasty. Instr Course Lect 2004;53:111-118.
Kelley SS: Periprosthetic femoral fractures. J Am Acad Orthop Surg 1994;2:164-172.
Berry DJ: Management of periprosthetic fractures: The hip. J Arthroplasty 2002;17:11-13.
Question 19
A 35-year-old laborer who sustained a forefoot injury 10 years ago has returned to work but reports a progressively painful deformity of the hallux and continued midfoot pain that is aggravated by weight-bearing activities. Shoe wear modifications have failed to provide relief. Direct palpation reveals no pain at the first metatarsocuneiform joint. A radiograph is shown in Figure 11. What is the next most appropriate step in management?
Explanation
REFERENCES: Kitaoka HB, Patzer GL: Arthrodesis versus resection arthroplasty for failed hallux valgus operations. Clin Orthop 1998;347:208-214.
McGarvey WC, Braly WG: Bone graft in hindfoot arthrodesis: Allograft vs autograft. Orthopedics 1996;19:389-394.
Ouzounian TJ: Metatarsophalangeal arthrodesis for salvage of failed hallux valgus surgery. Foot Ankle Clin 1997;2:741-752.
Question 20
Which of the following factors is most critical to the success of a meniscal allograft transplantation?
Explanation
cryopreservation of the graft to ensure cell viability is not necessary. There is a limited immune response to musculoskeletal allografts; therefore, immunosuppression, as is required for visceral organ transplantation, is not indicated.
Question 21
Osteoarthritic cartilage is characterized by decreased
Explanation
Chondrocytes in OA are much more metabolically active than those of normal cartilage. Studies reveal measuring the levels of utilization on sulfate and H-glucosamine informing components of cartilage matrix. The amount of DNA also rises in OA cartilage most noticeable at the articular chondrocyte.
The synthesis of hyaluronate increases. Recent data suggests 1) hyaluronate that is synthesized is abnormal and, hence, does not allow aggregation; or 2) The excess synthesis is a response to a rapid degradation of synthesized product. This is in light of the fact that synthesis increases, yet concentration of hyaluronate decreases.
The correct answer is that proteoglycan content decreases. The synthesis of proteoglycan increases in OA, but due to the increased rate of breakdown of proteoglycan there is a net result of lowered proteoglycan content.
Question 22
Figure 21 shows the radiograph of an 18-year-old man who was brought to the emergency department with shoulder pain following a rollover accident on an all-terrain vehicle. Examination reveals a fracture with massive swelling; however, the skin is intact and not tented over the fracture. Based on these findings, initial management should consist of
Explanation
REFERENCES: Iannotti JP, Williams GR (eds): Disorders of the Shoulder. Philadelphia, PA, Lippincott, 1999, pp 632-635.
Ebraheim NA, An HS, Jackson WT, et al: Scapulothoracic dissociation. J Bone Joint Surg Am 1988;70:428-432.
Question 23
Figure 38 shows the radiograph of a 75-year-old woman who has had right shoulder pain, difficulty sleeping on the affected arm, and difficulties performing activities of daily living for the past 6 weeks. Initial nonsurgical management includes analgesics, a subacromial cortisone injection, and gentle range-of-motion exercises. However, these modalities have failed to provide relief, and the patient reports that she is unable to elevate her arm. Her pain is worse and she would like the most reliable treatment method for pain relief and functional improvement. What is the best surgical treatment?
Explanation
REFERENCES: Favard L, Lautmann S, Sirveaux F, et al: Hemiarthroplasty versus reverse arthroplasty in the treatment of osteoarthritis with massive rotator cuff tear, in Walch G, Boileau P, Mole D (eds): 2000 Shoulder Prosthesis Two to Ten Year Follow-Up. Montpellier, France, Sauramps Medical, 2001, pp 261-268.
Frankle M, Siegal S, Pupello D, et al: The reverse shoulder prosthesis for glenohumeral arthritis associated with severe rotator cuff deficiency: A minimum two-year follow-up study of sixty patients. J Bone Joint Surg Am 2005;87:1697-1705.
Werner CM, Steinmann PA, Gilbart M, et al: Treatment of painful pseudoparesis due to irreparable rotator cuff dysfunction with the Delta III reverse-ball-and-socket total shoulder prosthesis. J Bone Joint Surg Am 2005;87:1476-1486.
Question 24
What is the most common associated pathology in patients who have suprascapular nerve entrapment secondary to ganglion cysts?
Explanation
REFERENCES: Fehrman DA, Orwin JF, Jennings RM: Suprascapular nerve entrapment by ganglion cysts: A report of six cases with arthroscopic findings and review of the literature. Arthroscopy 1995;11:727-734.
Iannotti JP, Ramesey ML: Arthroscopic decompression of a ganglion cyst causing suprascapular nerve compression. Arthroscopy 1996;12:739-745.
Moore TP, Fritts HM, Quick DC, Buss DD: Suprascapular nerve entrapment caused by supraglenoid cyst compression. J Shoulder Elbow Surg 1997;6:455-462.
Question 25
The diagnosis of an infection after total knee arthroplasty is most reliably proven based on what single study?
Explanation
REFERENCES: Windsor RE, Bono JV: Infected total knee replacements. J Am Acad Orthop Surg 1994;2:44-53.
Windsor RE, Insall JN, Urs WK, et al: Two-stage reimplantation for the salvage of total knee arthroplasty complicated by infection: Further follow-up and refinement of indications. J Bone Joint Surg Am 1990;72:272-278.
Question 26
A 72-year-old female presents to your office with a 24-month old painful nonunion of a 3-part fracture of the proximal humerus. She has been treated conservatively with range of motion exercises but continues to complain of debilitating pain and dysfunction. Operative management should include:

Explanation
The referenced article by Cheung et al reviews treatment options for proximal humeral nonunions and reports successful use of arthroplasty in treating elderly osteoporotic proximal humeral nonunions as a pain relieving procedure.
Dines reported a case series of 20 chronic post-traumatic proximal humerus fractures including nonunions that were treated with shoulder arthroplasty achieving fair to excellent results in 90% at mid-term follow-up
Question 27
An 18-year-old football player has intense pain and is unable to bear weight on the right knee after being tackled from the front. A posterior knee dislocation is reduced on the field. Because the game took place in a remote location, the patient is not examined in the emergency department until 5 hours after the injury. Examination now shows a grossly swollen knee with moderate ischemia in the lower leg. Posterior tibial and dorsalis pedis pulses are diminished. The best course of action should be to
Explanation
REFERENCES: Kremchek TE, Welling RE, Kremchek EJ: Traumatic dislocation of the knee. Orthop Rev 1989;18:1051-1057.
Reckling FW, Peltier LF: Acute knee dislocations and their complications. J Trauma 1969;9:181-191.
Question 28
Which of the following is helpful on physical examination to diagnose a fixed posterior shoulder dislocation? Review Topic
Explanation
Question 29
0 mmol/L (normal < 2.5), 1 hour postinjury it was 3.5 mmol/L, and it is now 5 mmol/L. His core temperature is 93 degrees F (34 degrees C). What is the most appropriate management for the femoral shaft fracture at this point?
Explanation
Question 30
A 37-year-old man has had isolated chronic knee swelling for the past 6 months. He denies any history of specific trauma. Examination reveals a large effusion with a stable knee, but the remainder of the examination is normal. Plain radiographs are unremarkable. An MRI scan reveals a large effusion without meniscal injury. An arthroscopic image of the suprapatellar pouch is shown in Figure 23. What is the most likely diagnosis?
Explanation
REFERENCES: Flandry FC, Hughston JC, Jacobson KE, Barrack RL, McCann SB, Kurtz DM: Surgical treatment of diffuse pigmented villonodular synovitis of the knee. Clin Orthop 1994;300:183-192.
Zvijac JE, Lau AC, Hechtman KS, Uribe JW, Tjin-A-Tsoi EW: Arthroscopic treatment of pigmented villonodular synovitis of the knee. Arthroscopy 1999;15:613-617.
Question 31
A 70-year-old man undergoes removal of an infected total hip arthroplasty (THA) and insertion of an articulating antibiotic-loaded spacer to treat a deep periprosthetic hip infection. While in a nursing home receiving intravenous antibiotics 3 weeks after surgery, the patient trips and falls. Examination reveals swelling in the mid and distal thigh, intact skin and neurovascular structures, and severe pain with knee or hip movement. Radiographs of the femur are shown in Figures 1 through 4. What is the most appropriate treatment for the fracture below the implant?
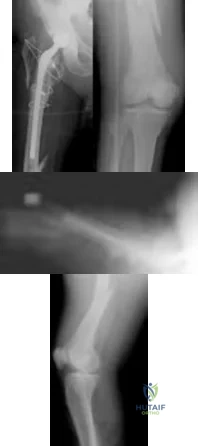
Explanation
This patient has a type C periprosthetic femoral fracture. The articulating spacer is not involved in the fracture, which is well distal to the implant. The most appropriate treatment is open reduction and internal fixation of the fracture. Traction is not appropriate for this fracture because the injury can be treated surgically despite the history of previous hip infection. Traction would also be needed for at least 5 weeks and would delay the surgical treatment of the periprosthetic fracture until the time of second-stage revision THA. The fracture is fairly distal, and revision to a longer antibiotic-loaded implant or uncemented stem is not suitable for this fracture pattern, because it extends well past the isthmus. A femoral stem in the distal fragment would provide little stability for the fracture. Removal of the articulating spacer and reimplantation using a long-stem fluted uncemented hip replacement is not appropriate, because it would be premature to reimplant the man's hip while he is still receiving treatment for a deep hip infection.
Question 32
The most appropriate next surgical procedure is
Explanation
This patient’s arthritis likely has progressed to the lateral compartment. The location and degree of local pain and tenderness are the most important physical findings. History and physical findings indicate arthritis progression to the lateral and anterior compartments. This scenario suggests the need for conversion of the unicompartmental arthroplasty to TKA.
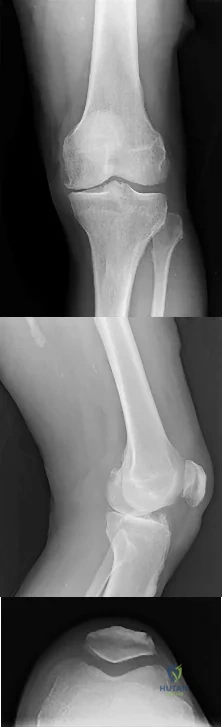
Question 33
A 35-year-old male sustains a posterior column/posterior wall acetabular fracture. Which of the following is the preferred approach for open treatment of this injury?

Explanation
Question 34
Figure 16 shows the radiograph of a 75-year-old man who has progressive groin pain and a limp following total hip replacement. At revision surgery, the anterior and posterior columns of the acetabulum are noted to be intact. The optimal surgical technique for acetabular component reconstruction is a
Explanation
REFERENCES: Petrera P, Rubash HE: Revision total hip arthroplasty: The acetabular component. J Am Acad Orthop Surg 1995;3:15-21.
Lachiewicz PF, Poon ED: Revision of a total hip arthroplasty with a Harris-Galante porous-coated acetabular component inserted without cement: A follow-up note on the results at five to twelve years. J Bone Joint Surg Am 1998;80:980-984.
Question 35
What clinical finding is associated with the least favorable prognosis in an adolescent patient who has been diagnosed with a high-grade osteosarcoma of the distal femur?
Explanation
REFERENCE: Mirra JM: Bone Tumors: Clinical, Radiologic, and Pathologic Correlation. Philadelphia, PA, Lea and Febiger, 1989, pp 344-350.
Question 36
- A 17-year old boy who sustained a closed clavicle fracture after he was ejected from an all-terrain vehicle was treated with a figure-of-8 brace 1 year ago. He now reports continuous pain at the site of the fracture and is unable to actively raise his arm above his head. A radiograph is shown in Figure 1. Management should now include
Explanation
Selection (1) would not provide adequate fixation to promote healing. (2) Electrical stimulation would not be sufficient for the above reasons. (3) Resection of the distal clavicle would not be indicate for this case because it promote further instability of the clavicle and increasing the affected forces to the clavicle.
(5) Kirschner wire fixation with bone graft, the author stated would provide fixation, but they achieved better results with plate fixation and bone graft Question 6 -
A 75-year-old woman sustains a fracture below the level of a total hip prosthesis. Radiographs demonstrate loosening of the prosthetic component. Treatment should consist of
a cast brace
a spica cast
plate fixation
allograft strut fixation
long stem revision
The key to this question lies in the radiographic evidence of loosening of the prosthetic component. The long stem revision is clearly indicated in this case because of various factors, one decreases impingement of the loose stem against the lateral femoral cortex. A non-surgical approach in the elderly patient will only increase the many risk factors such as atelectasis, pneumonia, and thromboembolic disease.[Instructional Course 44 pg. 293-303]
Question 37
A 75-year-old woman who sustained a fall now reports neck pain and upper extremity weakness. Examination reveals 4 of 5 strength in the upper extremities and 5 of 5 strength in the lower extremities. Radiographs show multilevel degenerative disk disease. An MRI scan is shown in Figure 96. Her clinical presentation is most compatible with which of the following? Review Topic
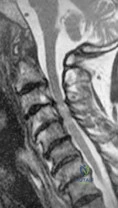
Explanation
Question 38
A teenage female is referred to you for evaluation of curvature in her back that was discovered on routine school screening. She is diagnosed with adolescent idiopathic scoliosis. In which of the following scenarios is a bracing program the most appropriate treatment? Review Topic
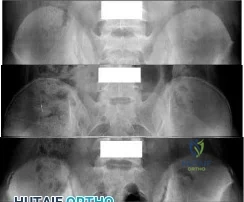
Explanation
The treatment of adolescent idiopathic scoliosis (AIS) depends on the magnitude and location of curve as well skeletal maturity of the patient. For curves less than 20 degrees, observation is appropriate until skeletal maturity, with closer intervals during
times of peak growth. Curves between 20-25 and 45 degrees in patients who are Risser stage 0,1 or 2 are best treated with bracing to stop progression. Curves with an apex at T7 or below are typically treated with a Boston brace. Curves over 50 degrees generally warrant a discussion about surgery to prevent progression past maturity.
In a landmark study, Weinstein et al. evaluated both a randomized and preference based cohort of bracing versus observation. The trial was stopped early due to efficacy of bracing. The rate of treatment success was 72% after bracing and 48% after observation. Treatment success was strongly correlated to time of brace wear.
Schlenzka et al. reviewed indications, treatment, and complications associated with brace treatment of AIS. They state that further evidence is necessary to evaluate the efficacy of bracing in AIS.
Figure 1, 2, and 3 are radiographs depicting Risser stage 0, 1, and 4 respectively. Illustration B shows radiographs of all Risser stages. Illustration C is the Lenke classification system for idiopathic scoliosis.
Incorrect Answers:
Question 39
All of the following techniques can help to prevent apex-anterior angulation during intramedullary nailing of proximal one-third tibia fractures EXCEPT:

Explanation
Question 40
A researcher is working on Medication A, a drug FDA-approved for the treatment of osteoporosis in men and women. It is an anti-resorptive agent that inhibits the formation, function and survival of osteoclasts. It does not bind to calcium hydroxyapatite. At 1-year after the initial dose, tissue levels are non-detectable. It can be used in the presence of cancer metastases to bone. What is Medication A? Review Topic
Explanation
Denosumab is a human monoclonal antibody against RANKL. By binding RANKL, it prevents interaction of RANKL with RANK (on OC and osteoclast precursors, OCP), and inhibits OC-mediated bone resorption, and the formation, function and survival of OC. In contrast, bisphosphonates bind to calcium hydroxyapatite in bone, and decrease resorption by decreasing function and survival (but not formation) of OC.
Vaananen et al. reviewed the cell biology of OC. During bone resorption, 3 membrane domains appear: ruffled border, sealing zone and functional secretory domain. The resorption cycle starts with migration, bone attachment, polarization (formation of membrane domains), dissolution of hydroxyapatite, degradation of organic matrix, removal of degradation products from resorption lacuna, and apoptosis of the OC or return to the non-resorbing stage.
Boyce et al. reviewed the regulation of osteoclasts and their functions. OCPs are held in bone marrow by chemokines e.g. stroma-derived factor-1 (SDF1) and attracted to blood by sphingosine-1 phosphate (S1P) (increased in synovial fluid of patients with RA). All aspects of osteoclast formation and functions are regulated by M-CSF and RANKL. More recent studies indicate that osteoclasts and their precursors regulate immune responses and osteoblast formation and functions by means of direct cell-cell contact through ligands and receptors, such as ephrins and Ephs, and semaphorins and plexins, and through expression of clastokines.
Warriner and Saag reviewed the diagnosis and treatment of osteoporosis. They defined osteoporosis as T-score of = -2.5 or a history of fragility fracture. Incident hip and vertebral fractures increase future risk of these fractures (hazard ratio 7.3 and 3.5, respectively).
Cummings et al. compared subcutaneous denosumab (60mg every 6mths) vs placebo in prevention of fractures in 7868 osteoporotic (T-score -2.5 to -4.0) postmenopausal women. They found that denosumab reduced risk of vertebral fracture by 68% (risk ratio, 0.32), hip fracture by 40% (hazard ratio 0.6), nonvertebral fracture by 20% (hazard ratio 0.8). There was no increased risk of cancer, infection, delayed fracture healing, cardiovascular disease, osteonecrosis of the jaw or adverse reactions. They concluded that it was useful for reduction of fractures in osteoporotic women.
The video shows the action of denosumab (prolia). Illustration A shows the different osteoclast zones.
Incorrect Answers:
Question 41
A 71-year-old woman who reports long-term use of oral steroids for asthma is referred for treatment of a distal humerus fracture. Radiographs reveal diffuse osteopenia and a severely comminuted intra-articular fracture. What is the most appropriate treatment?
Explanation
REFERENCES: Kamineni S, Morrey BF: Distal humeral fractures treated with noncustom total elbow replacement. J Bone Joint Surg Am 2004;86:940-947.
Frankle MA, Herscovici D Jr, DiPasquale TG, et al: A comparison of open reduction and internal fixation and primary total elbow arthroplasty in the treatment of intraarticular distal humerus fractures in women older than 65. J Orthop Trauma 2003;17:473-480.
Garcia JA, Mykula R, Stanley D: Complex fractures of the distal humerus in the elderly: The role of total elbow replacement as primary treatment. J Bone Joint Surg Br 2002;84:812-816.
Question 42
What is the prognosis for ambulation, from best to worst, for patients with an incomplete spinal cord injury?
Explanation
REFERENCES: Apple DF: Spinal cord injury rehabilitation, in Herkowitz HN, Garfin SR, Balderston RA, Eismont FJ, Bell GR, Wiesel SW (eds): Rothman-Simeone The Spine, ed 4. Philadelphia, PA, WB Saunders, 1999, pp 1130-1131.
Northrup BE: Evaluation and early treatment of acute injuries to the spine and spinal cord, in Clark CR (ed): The Cervical Spine, ed 3. Philadelphia, PA, Lippincott Raven, 1998, pp 544-545.
Question 43
Clinical studies on the use of topical and intravenous (IV) forms of tranexamic acid (TXA) administration demonstrate which results?
Explanation
Numerous studies have demonstrated efficacy of both IV and topical administration of TXA for decreasing blood loss and transfusion rates. Several studies have shown no significant difference between TXA IV and topical administration in decreasing blood loss or lowering transfusion rates. Inconclusive evidence shows that IV administration of TXA places individuals at higher risk for a thromboembolic event. Both IV and topical TXA are equally effective in decreasing blood loss and minimizing transfusion rates.
Question 44
-What is the diagnosis?
Explanation
Salter-Harris type II fracture of the proximal humerus
Question 45
A right-handed 44-year-old construction worker reports pain and limited range of motion in his right elbow that has limited his ability to work for the past year. Examination reveals range of motion from 60 to 90 degrees, and he has pain at the extremes of flexion and extension. Pronation and supination are minimally restricted. Anti-inflammatory drugs have failed to provide relief. A radiograph is shown in Figure 8. Management should now consist of
Explanation
REFERENCES: Antuna SA, Morrey BF, Adams RA, et al: Ulnohumeral arthroplasty for primary degenerative arthritis of the elbow: Long-term outcome and complications. J Bone Joint Surg Am 2002;84:2168-2173.
Phillips NJ, Ali A, Stanley D: Treatment of primary degenerative arthritis of the elbow by ulnohumeral arthroplasty: A long-term follow-up. J Bone Joint Surg Br 2003;85:347-350.
Question 46
What percent of patients initially diagnosed with classic, high-grade osteosarcoma of the extremity have visible evidence of pulmonary metastasis on CT of the chest?
Explanation
REFERENCES: Kaste SC, Pratt CB, Cain AM, et al: Metastases detected at the time of diagnosis of primary pediatric extremity osteosarcoma at diagnosis: Imaging features. Cancer 1999;86:1602-1608.
Link MP, Goorin AM, Miser AW, et al: The effect of adjuvant chemotherapy on relapse-free survival in patients with osteosarcoma of the extremity. N Engl J Med 1986;314:1600-1606.
Question 47
He reports that he had no problems with the knee until 6 weeks ago when he noted the gradual onset of pain following a colonoscopy. Examination reveals a painful, swollen knee. Knee aspiration reveals a WBC count of 40,000/mm3. Management should consist of
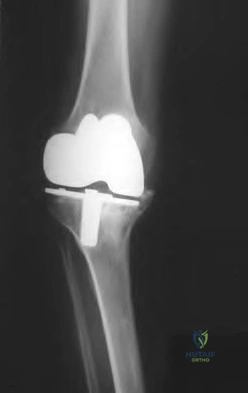
Explanation
has been used successfully when the duration of symptoms is 3 weeks or less. Long-term suppressive antibiotics are most commonly used when the patient’s medical condition precludes further surgery. Delayed reimplantation has been shown to be superior to immediate reimplantation in multiple studies. Little data support the use of arthroscopic irrigation and debridement.
Question 48
Figure 68 shows the MRI scan of a 13-year-old boy who has had knee pain and swelling following training lessons for ski racing for the past 6 months. The only abnormal finding on physical examination is an effusion. Management should consist of
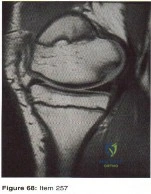
Explanation
Question 49
In a patient with a soft-tissue sarcoma treated by wide excision and radiation therapy, the risk of subsequent fracture is probably most influenced by
Explanation
REFERENCES: Bell RS, O’Sullivan B, Nguyen C, et al: Fractures following limb-salvage surgery and adjuvant irradation for soft-tissue sarcoma. Clin Orthop 1991;271:265-271.
Lin PP, Boland PJ, Healey JH: Treatment of femoral fractures after irradiation. Clin Orthop 1998;352:168-178.
Question 50
A 45-year-old man who is a smoker has a significant hemothorax and bilateral closed femoral fractures. On insertion of a chest tube, 1,100 mL of blood was returned. He has had 75 mL of chest tube output over the last 2 hours while being resuscitated in the ICU. His base deficit is now 2 and his urine output has been 3 mL/kg over the last hour. What is the next most appropriate step in management?
Explanation
REFERENCES: Nork SE, Agel J, Russell GV, et al: Mortality after reamed intramedullary nailing of bilateral femur fractures. Clin Orthop Relat Res 2003;415:272-278.
Pape HC, Zelle BA, Hildebrand F, et al: Reamed femoral nailing in sheep: Does irrigation and aspiration of intramedullary contents alter the systemic response? J Bone Joint Surg Am 2005;87:2515-2522.
Question 51
A 40-year-old right-handed professional football player reports persistent right wrist pain after falling during a game 5 days ago. A radiograph is shown in Figure 21. Management should consist of
Explanation
REFERENCES: Cohen MS: Ligamentous injuries of the wrist in the athlete. Clin Sports Med 1998;17:533-552.
Taleisnik J: Carpal instability. J Bone Joint Surg Am 1988;70:1262-1268.
Question 52
A 73-year-old man who underwent repair of the left rotator cuff 6 years ago reports good pain relief but notes residual weakness of the left shoulder, especially with overhead tasks. He denies having pain at night and has minimal discomfort with activities of daily living but is dissatisfied with his shoulder strength. Radiographs show an acromiohumeral interval of 2 mm. Appropriate management should consist of
Explanation
REFERENCES: Bigliani LU, Cordasco FA, McIlveen SJ, Musso ES: Operative treatment of failed repairs of the rotator cuff. J Bone Joint Surg Am 1992;74:1505-1515.
DeOrio JK, Cofield RH: Results of a second attempt at surgical repair of a failed initial rotator-cuff repair. J Bone Joint Surg Am 1984;66:563-567.
Gerber C, Vinh TS, Hertel R, Hess CW: Latissimus dorsi transfer for the treatment of massive tears of the rotator cuff: A preliminary report. Clin Orthop 1988;232:51-61.
Question 53
What is the most important feature in choosing an outcome instrument to assess shoulder disorders?
Explanation
REFERENCES: Leggin BG, Iannotti JP: Shoulder outcome measurement, in Iannotti JP, Williams GR (eds): Disorders of the Shoulder: Diagnosis and Management. Philadelphia, PA, Lippincott Williams and Wilkins, 1999, p 1027.
Norris TR (ed): Orthopaedic Knowledge Update: Shoulder and Elbow. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1997, pp 47-55.
Question 54
A 45-year-old man with a painful varus knee is being considered for an upper tibial osteotomy. Which of the following factors is considered the most compelling argument against this procedure?
Explanation
REFERENCE: Kelly MA: Nonprosthetic management of the arthritic knee, in Callaghan JJ, Dennis DA, Paprosky WG, Rosenberg AG (eds): Orthopaedic Knowledge Update: Hip and Knee Reconstruction. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1995, pp 245-249.
Question 55
Figures 38a and 38b
Explanation
Inversion of the ankle can cause various injuries about the foot and ankle, all via the same mechanism. Fifth metatarsal base avulsion (Figure 35) fractures can be treated with use of a walking boot until pain subsides. Jones fractures (Figure 36) can be treated with surgical or nonsurgical treatment, although young, active patients are perhaps better treated with ORIF, which can decrease disability time. Treatment of an anterior process calcaneus fracture (Figure 37) is similar to that for a fifth metatarsal base avulsion fracture. Figures 38a and 38b show a calcaneal fracture-dislocation, which necessitates ORIF.
RECOMMENDED READINGS
Schepers T, Backes M, Schep NW, Carel Goslings J, Luitse JS. Functional outcome following a locked fracture-dislocation of the calcaneus. Int Orthop. 2013 Sep;37(9):1833-8. PubMed PMID: 23959223. View Abstract at PubMed
Polzer H, Polzer S, Mutschler W, Prall WC. Acute fractures to the proximal fifth metatarsal bone: development of classification and treatment recommendations based on the current evidence. Injury. 2012 Oct;43(10):1626-32. doi: 10.1016/j.injury.2012.03.010. Epub 2012 Mar 30. Review. PubMed PMID: 22465516. View Abstract at PubMed
Roche AJ, Calder JD. Treatment and return to sport following a Jones fracture of the fifth metatarsal: a systematic review. Knee Surg Sports Traumatol Arthrosc. 2013 Jun;21(6):1307-15. doi: 10.1007/s00167-012-2138-8. Epub 2012 Sep 6. Review. PubMed PMID: 22956165. View Abstract at PubMed
Berkowitz MJ, Kim DH. Process and tubercle fractures of the hindfoot. J Am Acad Orthop Surg. 2005 Dec;13(8):492-502. Review. PubMed PMID: 16330511. View Abstract at PubMed
Question 56
A 2-day-old infant has the hyperextended knee deformity shown in Figure 7. No other deformities are found on examination. A radiograph shows that the ossified portion of the proximal tibia is slightly anterior to that of the distal femur. Management should consist of
Explanation
REFERENCES: Ko JY, Shih CH, Wenger DR: Congenital dislocation of the knee. J Pediatr Orthop 1999;19:252-259.
Johnson E, Audell R, Oppenheim WL: Congenital dislocation of the knee. J Pediatr Orthop 1987;7:194-200.
Roy DR, Crawford AH: Percutaneous quadriceps recession: A technique for management of congenital hyperextension deformities of the knee in the neonate. J Pediatr Orthop
1989;9:717-719.
Question 57
During establishment of an anterior portal for hip arthroscopy, what structure is at greatest risk for injury? Review Topic
Explanation
Question 58
An osteoprogenitor cell is expected to commit to a bone lineage in the presence of what transcription factor?
Explanation
C/EBPa are transcription factors leading to adipocytes, MyoD promotes myoblasts, and Sox 9 corresponds to chondroblasts.
Question 59
The postoperative neurologic prognosis of a patient who has a tumor that is compressing the spinal cord and causing a neurologic deficit depends primarily on the
Explanation
REFERENCES: Weinstein JN: Differential diagnosis and surgical treatment of primary benign and malignant neoplasms, in Frymoyer JW (ed): The Adult Spine: Principles and Practice. New York, NY, Raven Press, 1991, vol 1, pp 829-860.
Siegal T, Siegal T: Current considerations in the management of neoplastic spinal cord compression. Spine 1989;14:223-228.
Question 60
A 77-year-old man with diabetes mellitus has had a nonhealing Wagner grade I ulcer under the medial sesamoid for the past 3 months. He smokes tobacco regularly. He has undergone several debridements and total contact casting. Examination reveals no palpable pulses. He has no erythema or purulence, and he is afebrile. Radiographs reveal no abnormalities. What is the best initial diagnostic test to help determine why the ulcer has failed to heal?
Explanation
REFERENCE: Brodsky JW: Evaluation of the diabetic foot. Instr Course Lect 1999;48:289-303.
Question 61
An 8-year-old sustains the injury shown in Figures A and B. Postoperative radiographs are shown in Figures C and D. After cast removal and in-office k-wire removal, elbow range of motion is found to be between 20-80 degrees of flexion. How soon after surgery is range of motion expected to be >90% of normal? Review Topic
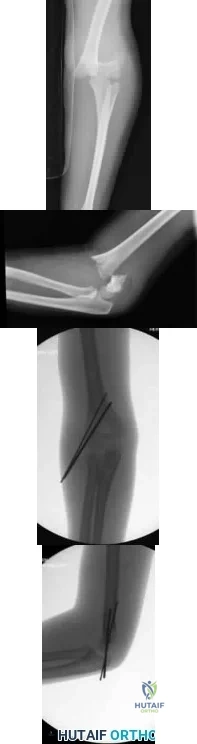
Explanation
Displaced pediatric supracondylar elbow fractures are often treated with closed reduction and percutaneous pinning. Risk of stiffness is low considering the extra-articular nature of the injury. Utility of physical therapy to improve range of motion after operative treatment of this injury is not supported in the literature.
Zionts et al. retrospectively evaluated elbow stiffness after treatment for pediatric supracondylar fractures. Ninety-four percent of normal range of motion was restored by 6 months after the operative procedure. Further improvement occurs up to one-year postoperatively
Lee et al. surveyed 76 orthopaedic surgeons on their treatment of pediatric supracondaylar injuries. They noted that general orthopaedic surgeons used passive exercises to assist with elbow stiffness after operative management of pediatric supracondylar fractures. In contrast, pediatric orthopaedists used active range of motion to improve elbow motion.
Keppler et al. retrospectively reviewed patients who had sustained supracondaylar fractures to ascertain the effect of postoperative physical therapy. At one year follow up, there was no difference in motion between patients who had received physical therapy and those who had not.
Figures A and B demonstrate the AP and lateral radiographs of a pediatric supracondylar fracture. Figures C and D are the postoperative radiographs after closed reduction and percutaneous pinning of the elbow injury.
Incorrect Answers:
(SBQ13PE.13) A 17-month-old boy is referred to your clinic by his pediatrician for a workup of "bowed legs." The patient's mother states that she has other children that grew out of it by age 3 or 4. Examination of the patient reveals a child whose measurements reside in the 75% percentile for height and weight. His gait appears appropriate for a toddler without varus thrust. Supine measurements show 10-degrees of symmetric, bilateral genu varus. Appropriate workup includes: Review Topic
Longterm clinical and radiographic monitoring to plan for guided growth until skeletal maturity
X-rays today and at age 4 to assure resolution of his genu varum
Genetic screening for metabolic causes of Rickets
Vitamin D levels drawn today and weekly 50,000 IU vitamin D injections assuming the value is low
Clinical observation and follow up to monitor resolution of genu varum
This patient has physiologic genu varum or tibia vara, which is common in toddlers less than 2 years of age. The mainstay of treatment is simple observation, as there is predictable resolution of this alignment as children
There are numerous etiologies of genu varum in children. Most common in the children under age 2 is a predictable pattern of genu varum and internal torsion in the first year or so after beginning to walk. Persistence of genu varum, severe (>20 degrees) or worsening deformity, limb asymmetry or varus thrust gait, and low height and weight percentiles should trigger further workup with x-rays and metabolic or genetic screening. A family history of genu varum is non-specific, and in isolation, does not indicate heritable causes of genu varum.
Kling and Hensinger's review article highlights normal angular and torsional deviations in growing children, including genu varum and genu valgum as well as hip and hind foot deformities. They emphasize that understanding the natural history of these deformities in growing children helps the treating physician identify those who need more than simple observation of their malalignment.
Staheli et al. published normal values of rotational profile physical exam maneuvers (including thigh foot axis, transmalleolar axis, prone internal and external hip rotation) to better understand the predictable changes in different age groups.
Birch provides an update on current treatment of Blount's disease. He suggests further radiographic evaluation in ambulatory infants with asymmetric varus deformity or varus deformity that persists after age 18 months. If these findings are present, radiographs are recommended. If the X-rays reveal metaphyseal-diaphyseal angle
>16° on AP radiographs and confirm the diagnosis of infantile Blount disease, he recommends anti-varus long leg bracing during ambulation for patients aged <=3 years with progressive deformity, clear radiographic evidence of infantile Blount disease, or lateral thrust with ambulation.
Illustration A shows pathologic metaphyseal beaking common in Blount's disease. There are no pathognomonic x-ray findings in physiological bowing as presented in this question.
Incorrect Answers:
Question 62
An osteoconductive bone graft material has which of the following properties?
Explanation
substitution, which allows for graft incorporation. An osteoinductive graft will stimulate the recruitment of progenitor cells that can differentiate into osteoblastic cells. Specific BMPs are osteoinductive. Osteogenic material contains viable cells with the ability to form bone. The ability to provide osteoprogenitor cells is only seen in fresh autograft. Other grafts rely on the recruitment of host progenitor cells to differentiate.
Question 63
A 10-year-old girl has been unable to walk for the past 5 days because of bilateral hip pain. Administration of IV morphine has provided some pain relief. She is afebrile. History reveals that she had an upper respiratory tract infection 3 weeks ago that resolved uneventfully. Examination reveals moderate pain with internal rotation and abduction, while log rolling maneuvers do not cause significant pain. An MRI scan shows a small effusion of one hip; however, a bone scan and plain radiographs are normal. Initial laboratory studies showed a markedly elevated WBC count, which subsequently declined to normal levels with IV antibiotics. Current studies show an erythrocyte sedimentation rate (ESR) of 100 mm/h. Aspiration of the hip obtains 3 mL of fluid; Gram stain is negative for bacteria, but a cell count shows a WBC count of 16,500/mm 3 . Streptozyme titer of the peripheral blood is 200 units (normal is less than 100 units). Management should now consist of
Explanation
REFERENCES: De Cunto CL, Giannini EH, Fink CW, et al: Prognosis of children with poststreptococcal reactive arthritis. J Pediatr Infect Dis 1988;7:683-686.
Haueisen DC, Weiner DS, Weiner SD: The characterization of “transient synovitis of the hip” in children. J Pediatr Orthop 1986;6:11-17.
Question 64
Of the following variables, which has the strongest influence on external fixator stiffness?
Explanation
Question 65
Figure 17 shows the radiograph of an 11-year-old boy with Duchenne muscular dystrophy who has been nonambulatory for the past 2 years. Management of the spinal deformity should consist of
Explanation
REFERENCES: Sussman M: Duchenne muscular dystrophy. J Am Acad Orthop Surg 2002;10:138-151.
Mubarek SJ, Morin WD, Leach J: Spinal fusion in Duchenne muscular dystrophy: Fixation and fusion to the sacropelvis? J Pediatr Orthop 1993;13:752-757.
Question 66
A 48-year-old woman reports bilateral thigh pain that is limiting her function as a librarian. A radiograph and a bone scan are shown in Figures 23a and 23b. What is the most likely diagnosis?
Explanation
REFERENCES: Resnick D: Diagnosis of Bone and Joint Disorders, ed 3. Philadelphia, PA,
WB Saunders, 1995, pp 956-957.
Wheeless’ Textbook of Orthopaedics: Acetabular Protrusio. www.wheelessonline.com/ortho/acetabular_protrusio
Question 67
Benign Ethnic Neutropenia is more common in males.
Explanation
Access to pediatric orthopaedic management has been well investigated. Numerous Level 4 studies have shown that orthopaedic offices in urban and rural areas prefer treating patients with private insurance over patients with Medicaid.
Iobst et al. telephoned 100 urban and rural orthopaedic outpatient offices to schedule an appointment for a 10-year-old patient with a forearm fracture. They showed that 8/100 offices would schedule an appointment within 1 week to the child with Medicaid insurance, as compared to 36/100 that gave an appointment to a child with private insurance.
Pierce et al. contacted 42 orthopaedic practices to schedule an appointment for a 14- year-old patient with an ACL injury. They showed that 38/42 offices scheduled an appointment for the child within 2 weeks with private insurance. This compared to 6/42 that scheduled an appointment for a similar child with Medicaid.
Incorrect Answers:
The perioperative use of which medication has been shown to increase the risk of post-operative infection following orthopaedic procedures in patients with rheumatoid arthritis (RA)?
Naproxen
Leflunomide
Sulfasalazine
Etanercept
Aspirin
Of the medications listed, only etanercept has been shown to increase the risk of post- operative infection following orthopaedic procedures in patients with RA.
Etanercept is a TNF-alpha antagonist with a short half-life that is administered once or twice weekly in patients with RA. Since TNF-alpha plays a central role in the pathogenesis of RA and is instrumental in causing joint destruction, the inhibition of this molecule has shown excellent results in controlling disease. The most powered study on TNF-alpha inhibitor use in the perioperative period following an orthopaedic procedures demonstrated a significant increase in
post-operative infection.
Howe et al. review the medical management of patients with RA who underwent orthopaedic procedures. They state that while there is conflicting information regarding TNF-alpha antagonists, they recommend holding them prior to major orthopaedic interventions.
Giles et al. review 91 patients with rheumatoid arthritis who underwent an orthopaedic procedure. They found TNF-alpha inhibitor therapy to be significantly associated with the development of a serious postoperative infection (p=.041)
Perhala et al. review 61 patients with RA who were treated with methotrexate during the perioperative period surrounding a total joint arthroplasty. They
failed to find a significant increase in complications in this patient group, stating the perioperative use of methotrexate does not affect wound healing or increase the likelihood of periprosthetic infection.
Illustration A shows the site of action of TNA-alpha inhibitors in the RA pathway.
Incorrect Answers:
Communication breakdown is the leading cause of which of the following?
Delayed diagnoses
Medication errors
Surgical site infections
1 and 2
All of the above
Communication failures are the leading cause of wrong side surgeries, medication errors and diagnostic delays.
Poor communication sets up environments in which medical errors can take place. Per the Joint Commission, medical errors may be the among the top 10 causes of death in the United States. Establishing open lines of communication is critical to reduce the risk of error and enhance patient safety.
Gandhi et al. designed a framework to study missed or delayed diagnoses and their causes. The most significant factors contributing to errors were poor handoffs, failures in judgment, failures in memory and failures in knowledge.
O’Daniel et al. review the importance of professional communication and collaborative team efforts. They note that patient safety is at risk when poor communication is in place. The leading cause for medication errors, treatment delays and wrong-site surgeries is communication failure.
Illustration A shows the leading causes of death in the United States. This includes “preventable errors” as a cause.
Incorrect Answers:
treatment, medication errors and wrong side surgery
Which of the following is true regarding osteoprotegerin (OPG)?
It is secreted by osteoclasts
It increases bone resorption
Binds to prostoglandin E2 before stimulating osteoclasts
Osteoprotegerin knock-out mice develop osteopetrosis
Binds to and sequesters RANKL
Osteoprotegerin is a decoy receptor for RANKL. Binding to RANKL causes decreased production of osteoclasts by inhibiting the differentiation of osteoclast precursors.
Bone resporption/remodeling is a complex process regulated by a large variety of molecules. Molecules that have shown to inhibit osteoclasts include OPG, calcitonin, estrogen, TGF-B, and IL-10. Corticosteroids have been shown to decrease production of OPG, thereby enhancing osteoclast formation and longevity. Prolia, or denosumab, is a newly approved drug used to treat osteoporosis and has a mechanism of action similar to osteoprotegerin
(inhibits binding of RANKL to RANK).
Boyle et al. review osteoclast differentiation and activation. The authors state that targeted disruption of OPG causes increased osteoclastogenesis and/or activation resulting in osteopenia.
Illustration A shows how OPG binds to RANKL inhibiting the stimulation of osteoclasts.
Incorrect Answers:
A 55-year-old woman has T-score -2.0 at the femoral neck. According to the World Health Organization Fracture Risk Assessment Tool (FRAX), she has a ten- year probability of sustaining a hip fracture of 1.5% and a ten-year probability of sustaining a major osteoporotic fracture of 8.9%. Which of the following statements is true regarding her antiresorptive therapy management?
Antiresorptive therapy should be started based on her T-score
Antiresorptive therapy should be started based on her risk of hip fracture alone
Antiresorptive therapy should be started based on her risk of major osteoporotic fracture alone
Antiresorptive therapy should not be started
Antiresorptive therapy should be started based on her risks of both hip fracture and major osteoporotic fracture
This patient has osteopenia. Assessment by FRAX shows that ten-year risk of hip fracture is less than 3% and her ten-year risk of major osteoporosis- related fracture is less than 20%. Therefore, antiresorptive therapy is not indicated at this time.
According to the 2008 National Osteoporosis Foundation guidelines, pharmacologic treatment for osteoporosis should be considered if patients are
postmenopausal women or men greater than 50 years old AND meet one of the following criteria: (1) they have a prior hip or vertebral fracture, (2) they have a T score -2.5 or less at the femoral neck or spine, (3) they have a T score between -1.0 and -2.5 at the femoral neck or spine AND a 10-year risk of hip fracture greater than 3% or 10-year risk of major osteoporosis-related fracture greater than 20%.
FRAX (World Health Organization Fracture Risk Assessment Tool) calculates
year risk of fracture based on the following variables: age, sex, race, height, weight, BMI, history of fragility fracture, parental history of hip fracture, use of oral glucocorticoids, secondary osteoporosis and alcohol use to calculate 10-year risk of fracture.
Unnanuntana et al. reviewed the assessment of fracture risk. Besides FRAX score and T-score, they discussed biochemical markers of bone formation and resorption, which are useful for monitoring the efficacy of antiresorptive / anabolic therapy, and may help identify patients at high risk for fracture.
Ekman et al. reviewed the role of the orthopaedic surgeon in minimizing mortality and morbidity associated with fragility fractures. The surgeon should consider prescribing appropriate medications, physical therapy, assessing fall risk and preventing falls and changing lifestyle factors (exercise, smoking and alcohol).
Illustration A shows the FRAX online tool (http://www.shef.ac.uk/FRAX/tool.aspx?country= =9).Illustration B shows the clinical risk factors considered in FRAX calculation.
Incorrect Answers:
A 32-year-old runner sustains a trimalleolar left ankle fracture. She undergoes open reduction and internal fixation and is kept non- weightbearing after surgery. At 2 months, what changes will occur in the articular cartilage of both her knees as a result of her current weightbearing regimen?
Cartilage thickening in the left (ipsilateral) knee and no change in cartilage thickness in the right (contralateral) knee
Cartilage thinning in both knees
Cartilage thinning in the left (ipsilateral) knee and no change in cartilage thickness in the right (contralateral) knee
Cartilage thinning in the left (ipsilateral) knee and increased cartilage thickness in the right (contralateral) knee
Increased cartilage thickness in both knees
After a period of off-loading, the off-loaded limb will experience cartilage thinning. The contralateral limb will not demonstrate any cartilage changes.
Physiologic loading of cartilage increases proteoglycan synthesis and cell proliferation and is chondroprotective. Joint immobilization leads to cartilage thinning, tissue softening, and reduced proteoglycan content, leading to cartilage erosion. Joint overuse leads to cartilage damage (in vitro only).
Hinterwimmer et al. examined cartilage atrophy after partial load bearing
using quantitative MRI. They found cartilage thinning in all knee compartments (greatest thinning, medial tibia; least thinning, patella). There was no change in cartilage morphology in the contralateral knee.
Sun reviewed the relationship between mechanical loading and cartilage degeneration. In OA, cartilage breakdown occurs at the articular surface, and is then fueled by synovial proteases and cytokines. In RA, synovial cells and macrophages are the source of degradative enzymes and incite cartilage destruction.
Milward-Sadler et al. examined mRNA levels following mechanical stimulation in normal and osteoarthritic chondrocytes. Normal chondrocytes showed increased aggrecan mRNA and decreased matrix metalloproteinase 3 (MMP-3) mRNA after stimulation. This
chondroprotective response was absent in osteoarthritic chondrocytes.
Illustration A shows pro- and anti-inflammatory mechanisms of mechanical loading on chondrocytes. Underloading and overloading induce cartilage damage through pathways involving the upregulation of MMPs and ADAMTSs (ADAMTS, a disintegrin and metalloproteinase with thrombospondin motifs, or aggrecanase). Physiological loading blocks these increases.
Incorrect Answers:
A morbidly obese 40-year-old man is scheduled to undergo hemilaminectomy for resection of an painful osteoid osteoma of the T6 lamina. He is positioned prone on a Jackson table and localization is performed with intraoperative fluoroscopy prior to the start of the case. At close to the end of the case, intraoperative frozen section reveals only normal bone fragment from the resected lamina. A probe is placed and a cross-table lateral radiograph reveals that the T7 lamina was resected instead of T6. At this point, the surgeon should
do all of the following EXCEPT
Complete the surgery
Abort the case and obtain further imaging
Apologize to the patient and family
Formally document the error in the operative report
Inform the patient and family immediately after the operation
Fluoroscopic localization of the correct thoracic vertebra can be difficult in the obese
patient. Upon detection of wrong level surgery, he should not abort the case. Rather, he should perform the desired procedure at the correct site, and advise the patient and family upon completion.
Adverse events are inevitable. The correct action following wrong-site surgery is to perform the desired procedure at the correct site followed by frank and honest communication with the patient/family. Open, honest communication favorably affects patient behavior, health outcomes, patient satisfaction, and often reduces the incidence of medical professional liability actions. The
discussion should include a disclosure of known facts and an explanation as to the likely cause, as well as ongoing treatment, follow up care, and prognosis.
The AAOS Information Statement about Wrong Site Surgery identifies 3 treatment steps following discovery of an error during surgery under general anesthesia: Return the patient to his preoperative condition, perform the correct procedure at the correct site, and advise the patient and family of what occurred and the likely consequences, if any, of the wrong- site surgery.
The AAOS Information Statement on Communicating Adverse Events states that the surgeon has an ethical and professional obligation to disclose the error to the patient and/or family. Disclosure should include what happened, why it happened, health implications, and what measures are being instituted to prevent recurrences.
Incorrect Answers:
All of the following are Standards of Professionalism relating to interactions with industry for practicing orthopaedic surgeons EXCEPT:
Decline gifts from industry with a market value over $100 (unless they are medical textbooks or patient educational materials)
Disclose to the patient any financial arrangements with industry that relates to the patient's treatment
Accept no direct financial inducements from industry for utilizing a particular implant
Disclose any relationship with industry to colleagues who may be influenced by your work
Decline to participate in industry sponsored non-CME courses or
conferences
The AAOS has adopted the Standards of Professionalism (SOP). These SOP’s establish mandatory, minimum levels of acceptable conduct for fellows and members of the AAOS to engage in relationships with industry. There are 17 standards with relation to industry. Answer choice 5 is not a SOP as surgeons are allowed to participate in or consult in meetings that are conducive to the effective exchange of information. The SOP also stipulate that tuition, travel, and modest hospitality (including meals and receptions) are allowed to attend an industry-sponsored non-CME course.
A prospective randomized trial is conducted to test the efficacy of Vitamin C versus placebo in treating patients who develop chronic regional pain syndrome (CRPS) after distal radius fractures. At first follow-up, the rates of CRPS are 1% and 9% in the study and placebo group, respectively. Which statistical test is most appropriate to determine significance?
Single factor analysis of variance
Chi-square test
Student t-test
Mann-Whitney rank sum test
Wilcoxon rank sum test
In the study provided, we need to determine whether distributions of categorical variables differ from one another. The appropriate study is the chi- square test.
Data can be classified as numerical (continuous) or categorical (proportional). Responses to such questions as "What is your major?" or Do you own a car?" are categorical because they yield data such as "biology" or "no." In contrast, responses to such questions as "How tall are you?" or "What is your G.P.A.?" are numerical. When comparing two independent means from numeric data, a t-test is performed. However, if categorical data is being compared, the chi- square test will determine if the proportions are really different.
Kocher et al. review basic clinical epidemiology and biostatistics relevant to orthopaedic surgery. Amongst other things, they describe that data can be summarized in terms of measures of central tendency, such as mean, median, and mode, and in terms of measures of dispersion, such as range, standard deviation, and percentiles.
Illustration A shows an algorithm for determining which test to use for varying data. Incorrect Answers:
distributed.
A 35-year-old patient is involved in a motor vehicle accident and sustains multiple fractures including a closed comminuted proximal meta-diaphyseal tibia fracture. The surgeon is considering bridge plating the fracture using a minimally invasive approach. Which of the following is true regarding bridge plating?
A locked plate construct (locked screws) or hybrid construct (locked and non- locked screws) is necessary.
Periosteal stripping is performed through two incisions proximal and distal to the fracture.
Bridge plating is performed following direct reduction of the fracture.
AO Type A diaphyseal fractures are best treated with this technique.
Bridge plating with a long working length creates a flexible, axially stable construct.
In bridged plating, only the most proximal and distal screw holes are filled. This creates a flexible, axially stable construct.
Bridge plating is applicable to all long-bone fractures with complex fragmentation and where intramedullary nailing or conventional plate fixation is not suitable. The construct preserves the blood supply to the fracture fragments as the fracture site is undisturbed during the operative procedure. It provides RELATIVE stability, allowing for some motion at the fracture site, leading to callus formation and secondary bone healing. The construct is FLEXIBLE because of increased distance between the 2 screws closest to the fracture (long working length), allowing for stress distribution and permitting more motion at the fracture site. The construct is also AXIALLY STABLE because the plate acts as an extramedullary splint and resists axial compression.
Livani et al. advocate using an anterior or antero-lateral approach for minimally invasive plating of the humerus. They recommend that distal access is obtained first, allowing identification of the lateral antebrachial cutaneous nerve. For distal fractures, they recommend extending the plate down to the lateral column.
Apivatthakakul et al. defined minimally-invasive plate osteosynthesis (MIPO) danger zones from the lateral epicondyle. They found the musculocutaneous nerve averaged 18- 43% of the humeral length, the danger zone for the radial nerve averaged 36-59% of the humeral length, and the most dangerous screws that penetrated or touched the radial nerve lay 47-53% of the humeral length.
Illustration A shows a distal tibia fracture. Illustration B shows radiographs 5 months after bridge plating of this fracture. There is callus formation, characteristic of indirect bone healing.
periosteal blood supply is critical.
Which of the following components of bone is most responsible for compressive strength?
Type I collagen
Osteocalcin
Proteoglycans
Osteonectin
Osteopontin
Proteoglycans, in addition to calcium hydroxyapatite [Ca10(PO4)6(OH)2], are most responsible for providing compressive strength.
Bone is composed of both organic and inorganic components. Inorganic components include calcium hydroxyapatite and osteocalcium phosphate. Organic components include collagen, proteoglycans, matrix proteins, cytokines and growth factors. While Type I collagen is responsible for providing the tensile strength of bone, proteoglycans and calcium hydroxyapatite [Ca10(PO4)6(OH)2] are most responsible for providing compressive strength. Proteoglycans contain a core protein with various
numbers of covalently attached side chains of glycosaminoglycans. In addition to providing compressive strength, they are also responsible for binding growth factors and inhibiting mineralization.
Knothe et al. review the osteocyte. They discuss that osteocytes are the most abundant
cells in bone, are actively involved in maintaining the bony matrix, and may act as mechanosensors.
Illustration A shows a proteoglycan aggregate, which can form when individual molecules link onto a chain of hyaluronic acid.
Incorrect Answers:
A prospective, randomized controlled trial of 150 patients undergoing total hip arthroplasty is performed to test whether repair of the capsule during a posterior approach reduces post-operative dislocations in the first three months. The study found no difference in dislocation rate if the capsule was repaired versus not repaired (p =
.34). Subsequently, a multicenter follow-up study of 2000 patients showed that repairing the capsule led to a decreased dislocation rate
in the first three months (p = .03). Assuming the second study reflects reality, which of the following errors occurred in the first study?
Observer bias
Type-II error
Alpha error
Type-I error
Confounding error
In this situation, the null hypothesis was accepted when it should have been rejected.
This is a type-II error.
A study can have two types of errors. Type-I errors, or alpha errors, occur when the null hypothesis is rejected when it should have been accepted. The alpha level refers to the probability of a type-I error. By convention, the alpha level of significance is set at 0.05, which means that we accept the finding of a significant association if there is less than a one in twenty chance that the observed association was due to chance alone. Type-II errors, or beta errors, occur when the null hypothesis is accepted when it should be rejected. This
often occurs when studies are underpowered. In the example above, the null hypothesis is that repair of the capsule does not reduce dislocations within the first three months. Since the first study did not show a statistically significant difference, the null hypothesis was accepted. Since a more powered study showed that repair of the capsule does reduce dislocations, the null hypothesis should have been rejected in the initial study (if it was adequately powered).
Fosgate et al. review the importance of sample size calculations when performing research. They state that sample size ensures statistical significance if the subsequent data collection is perfectly consistent with the assumptions made for the sample size calculation (assuming power was set as
50% or greater).
Illustration A shows the difference between type-I and type-II errors. Video V is a lecture discussing statistical definition review of PPV, NPV, sensitivity and specificity.
Incorrect Answers:
that properly constructed studies attempt to avoid.
Which of the following is a potential cause of fretting corrosion?
The micromotion at the femoral head-neck junction in a modular total hip replacement
A stainless-steel cerclage wire is in contact with a titanium-alloy femoral stem
Friction between polyethylene liner and femoral head leading to osteolysis
The formation of pits within a stainless-steel plate and the subsequent release of metal ions
The formation of an adherent oxide coating on titanium implants
Micromotion at the femoral head-neck junction can lead to fretting corrosion, one of the most common causes of failure of a modular implant.
Modular components give surgeons excellent intraoperative flexibility, but are susceptible to various types of corrosion. While titanium and cobalt-chrome contain a protective surface oxide layer, continued micromotion at the modular junction may disrupt the protective layer leading to fretting corrosion, defined as micromotion at contact sites under load. This may eventually lead to a painful synovitis that necessitates a revision procedure.
Srinivasan et al. review modularity in total hip arthroplasty. Amongst other things, they discuss the modularity of the femoral head/neck junction, describing the morse taper interlocking system that provides both axial and rotational stability.
Illustration A shows an example of corrosion at the head/neck junction of a total hip arthroplasty.
Incorrect Answers:
Which of the following situations is most likely to decrease sentinel event errors?
Physician and nurse training is lengthened by 20%
Resident hours are decreased to 55 hours per week
An environment is created where all members of the healthcare team feel empowered to express their concerns and beliefs
Holding individuals responsible for errors in clinical judgement
Physicians and nurses are assigned to a smaller number of patients
Creating an environment where all members of the healthcare team feel empowered to express their beliefs increases communication, the key element in decreasing sentinel events.
Research has shown that 70% of sentinel event errors are caused by improper communication. Specific ways to improve communication include effective clinical handover between shifts and breaking down the "hierarchy" so that all members of the team can discuss their expectations and concerns. Barriers to effective communication include distractions, cultural differences, power distance relationships, time pressures, and lack of organization.
Leonard et al. describe specific clinical experiences in the application of surgical briefings, properties of high reliability perinatal care, the value of critical event training and simulation, and benefits of a standardised communication process in the care of patients transferred from hospitals to skilled nursing facilities. They recommend embedding standardized tools and behaviors to bridge differences in communications styles between clinicians.
Incorrect Answers:
Which of the following side effects is most strongly associated with the use of NSAIDs?
Hepatic dysfunction
Renal impairment
Prolonged QTc
Seizures
Hematuria
All NSAIDs have the potential to cause serious renal impairment.
NSAIDs work by inhibiting the cyclooxygenase pathway (COX), which is comprised of the COX-1 and COX-2 pathways. The COX-1 pathway is involved in prostaglandin E2– mediated gastric mucosal protection and thromboxane effects on coagulation, while the COX-2 pathway is mainly involved with the modulation of pain and fever without effect on platelet function. While selective COX-2 inhibitors have a decreased side effect profile, all NSAIDS
have the potential to cause renal impairment and their use should be limited in patients with underlying renal disease.
Horlocker et al. review multimodal pain management in the perioperative setting of a total joint arthroplasty. Specifically, they note that NSAIDs should be used cautiously in patients with underlying renal dysfunction who are to undergo a procedure with major blood loss.
Griffin et al. reviewed 1,799 patients hospitalized for acute renal failure. They found that NSAIDs increased the risk of renal failure by 58% and that NSAID use resulted in 25 excess hospital admissions per 10,000 years of use.
Illustration A shows the COX pathways and their inhibition by NSAIDs. Incorrect Answers:
It is recommended that invasive dental work be completed prior to the initiation of which of the following medications?
Glucosamine
Cholecalciferol
Levothyroxine
Teriparatide
Bisphosphonates
Bisphosphonate therapy combined with invasive dental work increases the risk for development osteonecrosis of the jaw.
Bisphosphonates are a class of drugs that prevent bone mass loss by inhibiting osteoclast resorption. They are used in the treatment of vertebral compression fractures, non- vertebral fragility fractures, osteogenesis imperfecta, multiple myeloma, and avascular necrosis. Because bisphosphonates have been associated with osteonecrosis of the jaw, it is suggested that all invasive
dental work be completed prior to initiation of treatment.
Pazianas et al. (2011) review the safety profile of bisphosphonates. Specifically, they cite gastrointestinal discomfort, atypical femur fractures, osteonecrosis of the jaw, ocular inflammation, and musculoskeletal pain as common side effects. They state there is limited evidence surrounding
bisphosphonate's association with esophageal cancer and atrial fibrillation.
Pazianas et al. (2007) reviewed 11 publications that reported 26 cases of osteonecrosis of the jaw following initiation of bisphosphonate treatment. Age
>60 years, female sex, and previous invasive dental treatment were the most common characteristics of those who developed ONJ.
Illustration A shows the various bisphosphonates and their mechanisms of action. Illustration B shows an example of osteonecrosis of the jaw, a side effect that has been linked to bisphonphonate treatment.
Incorrect Answers:
Figures A and B show radiographs of a 24-year-old female with a soccer injury. A physical examination reveals an isolated, closed injury with no clinical features of neurovascular injury or compartment syndrome. She has been consented to be treated with intramedullary nail fixation. A pre-operative note by the anaesthesiology team makes reference to the patients fair skin and natural red-hair color. How will this information affect the post-operative management of this patient?
Longer duration of anticoagulation due to increased risk of DVT
Avoiding anticoagulation medications due to increased risk of bleeding
Require higher dosages of post-operative analgesia
Longer period of non-weight bearing on surgical limb
Avoiding opioids due to higher risk of unrecognized allergies
Female patients with natural red-hair may require higher dosages of post- operative analgesia compared to other hair types.
Melanocortin-1-receptor (MC1R) is one of the key proteins involved in hair color and skin tone. Mutations of the MC1R alleles can render this protein non- functional, which results in a phenotype of red-hair and fair skin. Mutations of the MC1R have shown to modulate the pain response and opioid efficacy in these patients. Women are more commonly affected and often require more anaesthetic and higher dosages of opioid to achieve comparable MAC level and pain-relief, respectively, as women with other hair types.
Liem et al. showed that a greater concentration of induction and maintenance agents (sevoflurane and desflurane, respectively) were required to sustain comparable MAC levels in red-haired patients as dark haired patients.
Fillingim et al. reviewed the affect of gender, sex and pain. They concluded there is a biopsychosocial element of pain that is perceived differently by men and women. In terms of postoperative and procedural pain, the outcome might be more severe in women than men.
Delaney et al. looked at the involvement of the melanocortin-1 receptor in acute pain in mice. They found that while the MC1R is better known as a gene involved in mammalian hair colour, it was shown to be involved in the pain pathway of inflammatory but not neuropathic origin. Mutations of MC1R showed increased tolerance to noxious pain stimulus in mice.
Figures A and B are AP and lateral radiographs of a left tibia. There is a low energy, distal third shaft fracture with no cortical apposition on the AP view.
Incorrect Answers:
Which of the following medications used for thromboprophylaxis following orthoapedic surgery is a direct inhibitor of factor Xa?
Dextran
Rivaroxaban (Xarelto)
Coumadin
Fondaparinux (Arixtra)
Aspirin
Rivaroxaban (Xarelto), an oral anticoagulant, is a direct inhibitor of factor Xa.
Rivaroxaban (Xarelto) is a member of a new class of oral, direct (antithrombin- independent) factor Xa inhibitors, which restrict thrombin generation both in vitro and in vivo. Inhibition of Factor Xa interrupts the intrinsic and extrinsic pathway of the blood coagulation cascade, inhibiting both thrombin formation and development of thrombi.
Eriksson et al. compare rivaroxaban to enoxaparin for the prevention of symptomatic venous embolism following total hip arthroplasty. Major venous thromboembolism occurred in 4 of 1686 patients (0.2%) in the rivaroxaban group and in 33 of 1678 patients (2.0%) in the enoxaparin group. Additionally, major bleeding events were similar between the two groups.
Illustration A shows the mechanisms of action of various agents used for thromboprophylaxis.
Incorrect Answers:
as Protein C and Protein S.
The origin of bovine derived grafts is particularly important to which of the following religious groups?
Christianity
Islam
Hinduism
Buddhism
Judaism
The origin of bovine-derived surgical implants should be discussed in further detail with patients ascribing to Hinduism.
Patients come from a variety of religious backgrounds. Depending on a patient’s religion, the origin of surgical implants may have implications for their use. In Hinduism, bovine animals are considered sacred. Use of cow by- products is considered purifying in nature. Subsequently, the origin of bovine derived implants should be discussed with patients ascribing to Hinduism.
Easterbrook et al. evaluated the utility of porcine and bovine surgical implants amongst those of Jewish, Muslim and Hindu faiths. Hindu religious leaders, who were surveyed, did not approve of the use of bovine surgical implants.
Enoch et al. evaluated the acceptability of biological products amongst various religious groups. The Hindu religious leaders were found to not have an objection to the use of biological implants derived from cows.
Illustration A shows a clinical photo of a fetal bovine derived dermal substitute. Incorrect Answers:
Immunological testing of anti-cyclic citrullinated peptide antibodies (anti- CCP) is most commonly used for the diagnosis and prognosis of which immunological condition?
Ankylosis spondylitis
Rheumatoid arthritis
Psoriatic arthritis
Systemic lupus erythematosus
Reiter's syndrome
Anti-cyclic citrullinated peptide antibodies (anti-CCP) are commonly used as a marker for the diagnosis and prognosis of rheumatoid arthritis (RA).
Immunological studies are commonly performed to investigate cases of suspected rheumatoid arthritis. Rheumatoid factor has historically been used as a primary marker for RA. However, in more recent years, the use of anti- CCP antibodies has shown to be as sensitive as, and more specific than, rheumatoid factor (RF) in early and fully established disease. In general, anti-
CCP assays equate to a sensitivity of 50-75% and a specificity of 90-95%. High levels of anti-CCP have been shown to be indicative of a more erosive disease process and may be detected before the onset of arthritis.
Gardner and Kadel reviewed the laboratory studies most commonly used in rhuematologic diseases. Standard ordering for clinically suspected RA include Rf, anti- CCP, ESR/CRP as well as other markers of autoimmune diseases such as antinuclear antibodies, anticardiolipin antibodies and lupus anticoagulant, HLA-B27, and uric acid levels.
Illustration A shows the sensitivity and specificity of anti-CCP vs. RF in a variety of autoimmune diseases.
Incorrect Answers:
Vitamin C has been shown to decrease the likelihood of which of the following complications following surgery on the foot and ankle in non-diabetic patients?
Nonunion
Complex Regional Pain Syndrome, type II
Malunion
Complex Regional Pain Syndrome, type I
Wound infection
Vitamin C has been shown to decrease the likelihood of developing complex regional pain syndrome (CRPS), type 1, when given post-operatively to patients undergoing foot and ankle and wrist surgery.
CRPS is a frequent post-operative complication, with rates varying from 10-
37%. Type I CRPS does not have an identifiable nerve lesion, while type II has an identifiable nerve lesion. Multiple studies have shown that vitamin C decreases rates of CRPS following distal radius fractures, and more recently, the same has been shown following foot and ankle surgery. While the exact mechanism of CRPS is unknown, vitamin C has been shown to reduce lipid peroxidation, scavenge hydroxyl radicals, protect the capillary endothelium, and inhibit vascular permeability. All of these characteristics of vitamin C may play a role in modulating the pain pathway.
Zollinger et al. perform a double-blind, prospective, multicenter trial where
416 patients with 427 wrist fractures were randomly allocated to treatment with placebo or treatment with 200, 500, or 1500 mg of vitamin C daily for fifty days. The prevalence of complex regional pain syndrome was 2.4% in the vitamin C group and 10.1% in the placebo group.
Besse et al. compare two groups of patients undergoing surgery on the foot and ankle to determine the effect of vitamin C on the development of CRPS, type I. CRPS type I occurred in 18 cases (9.6%) in the group not given vitamin C, and 4 cases (1.7%) in the group given vitamin C.
Illustration A shows an example of a limb affected by CRPS. Note the increased swelling, a common physical exam finding in patients afflicted with the disease.
Incorrect Answers:
A 25-year-old Spanish speaking male presents to the emergency department 6 hours after sustaining the injury seen in Figure A. He is grossly intoxicated and screaming in pain. Physical examination reveals a closed injury with overlying muscular compartments that are extremely firm to palpation. After sedating the patient, measurements of the intracompartmental pressures were all found to be
>75mmHg. His wife is Spanish speaking and expected to arrive to the hospital in 2-3 hours with a relative to help with translation. No medical translator is
available. You attempt to outline the risk and benefits of surgery to the patient, but the he repeatedly interrupts you and yells out ,"No surgery!". An English-Spanish speaking friend is with the patient and says that he has known the patient for over 2 years and will help with any decision making. What would be the next most appropriate step in the management of this patient?
Delay surgery to monitor the patient for impending compartment syndrome
Proceed with surgery with urgent fasciotomy after documenting the necessity of treatment without consent
Delay the surgery until the wife arrives and able to give informed consent with the aid of a translator
Proceed with surgery for urgent fasciotomy after obtaining informed consent from the patients friend
Respect the patients autonomy and reassess the patient in the morning when he demonstrates capacity to accurately comprehend the proposed treatment
This patient is presenting with compartment syndrome of the right tibia. In a situation of required surgery for limb threatening injury without available legal consent the surgeon should confirm and document the necessity of care with a fellow colleague.
Physicians are responsible for whether a patient is able to reasonably understand their medical condition and the nature of any proposed medical procedure, including the risks, benefits, and available alternatives. If the patient lacks this capacity, disclosure imposed by the doctrine of informed
consent are excused because irreparable harm that may result from the physician’s hesitation to provide treatment. Detailed documentation is also important. In addition, the attending physician should contact the Risk Management Dept at the hospital for support prior to surgical intervention or have a medical translator involved to ensure information is being translated properly.
Katz et al. reviewed the medical decision making process of Hispanic people. They showed that Hispanic people are more likely to permit their physician to take the predominant role in making health decisions compared to Non- Hispanic people.
Figure A shows a comminuted tibia and fibula fracture. Incorrect Answers
A Spanish speaking child sustained the injury seen in Figure A after a fall at school. He was casted in the emergency department without the assistance of an interpreter and advised to return to see an orthopaedic surgeon in 1 week. However, the family returns to the emergency department with the child 3 months later, still in the cast. What is the most likely reason the child did not attend the recommended orthopaedic follow-up visit.?
The child is a victim of neglect
The child had no symptoms of pain
He was allowed to return to school wearing the cast
Concerns of cost
Follow-up instructions were not effectively communicated
The most likely reason the child did not attend the recommended orthopaedic follow-up visit was a language barrier preventing effective communication of the intended follow-up instructions.
Communication skills and cultural competence is a key element in good orthopaedic care. Poor communication can often lead to devastating outcomes. In this example, poor communication resulted in this patient being lost to
follow-up. Language barriers must be accommodated and alternative methods of communication must be utilized.
Levinson et al. examined how patients present their medical issues in clinical encounters and how physicians respond to these clues in routine primary care and surgical settings. They showed that good communication relies mostly on the physicians ability to identify patient clues within the clinical encounter.
Poor communication between the physician tended to delay clinical visits, poor follow-up and unsatisfactory outcomes.
Figure A is an AP radiograph of the elbow in a skeletally immature patient. Figure B is a lateral radiograph of the elbow with a posterior fat pad sign, suggestive of an occult fracture.
Incorrect Answers:
A 25-year-old female presents to the emergency room within increasing left shoulder pain after walking into a door 5 months ago. She previously sustained a femoral fracture 2 years ago after tripping on a rug. Relevant skeletal survey radiographs and tissue biopsy results are shown in Figures A through D. Laboratory investigations show normal glomerular filtration rate and creatinine clearance. Dual energy x-ray absorptiometry (DEXA) scan shows T-score of -1.4 and
-1.2 at the hip and lumbar spine, respectively. Which of the following laboratory values in Figure E most likely reflects this patient's condition?
A
B
C
D
E
This patient has primary hyperparathyroidism. Laboratory investigations are likely to show elevated serum intact parathyroid hormone (PTH), alkaline phosphatase (ALP) and ionized serum calcium, and low serum phosphate.
Primary hyperparathyroidism is most commonly caused by a single adenoma (80-90%). Besides the signs and symptoms of hypercalcemia, patients present
with calcification of menisci and articular cartilage, erosions in hand bones, "salt and pepper skull", and brown tumors (osteoclastomas), which appear as lytic regions expanding the cortex and causing pathological fractures, so named because of hemosiderin deposition.
Singhal et al. reviewed primary hyperparathyroidism. They advocate routine serum calcium levels for patients with pathologic fractures. If this is elevated, total and ionized calcium and intact PTH levels should be obtained. They feel that surgery for orthopaedic stabilization and parathyroidectomy should be performed simultaneously for better outcome.
Mankin et al. reviewed metabolic bone disease. They suggest that patients with mild disease with normal calcium levels do not require treatment. For patients with high calcium levels, treatment should include maintenance of fluid balance, localization and removal of the adenoma, bony stabilization, and medications (calcitonin, estrogen, bisphosphonates, and calcimimetics such as cinacalcet).
Figure A is an AP radiograph showing a lytic expansile lesion with pathological fracture in metadiaphyseal region of left humerus with similar lesion in the
fifth posterior rib. Figure B is an AP radiograph showing a lytic expansile lesion in the third metacarpal of the right hand and the fifth metacarpal of the left hand. Figure C is a low power micrograph of a brown tumor demonstrating a central zone of bone resorption, and filling with fibroblastic tissue, with a peripheral rim of osteoid production. Figure D is a high power micrograph of a brown tumor. In areas of bone resorption, there are numerous osteoclast-like giant cells amidst a fibrous stroma. This is unlike a true giant cell tumor, which lacks a fibrogenic stroma.
Incorrect Answers:
and impaired 1,25-dihydroxyvitamin D production by the diseased kidneys. This patient has normal renal function. Answer 3: Elevated PTH, ALP, serum calcium and phosphate occur in tertiary hyperparathyroidism. This again occurs in chronic renal disease after prolonged chronic secondary hyperparathyroidism or after renal transplantation, where the parathyroid glands become autonomous and PTH levels do not normalize. This patient has normal renal function.
elevated.
FOR ALL MCQS CLICK THE LINK ORTHO MCQ BANK
Question 68
- The Injury Severity Score (ISS), using point scores from five different body systems, is a method that aids in predicting the chances of mortality in a patient with multiple injuries by
Explanation
Question 69
Figure 11 shows the radiograph of an 18-year-old soccer player who reports recurrent lateral foot pain after sustaining an inversion injury. History reveals that 6 months ago he had been treated in a non-weight-bearing cast for a fifth metatarsal fracture. Management should consist of
Explanation
REFERENCES: Torg JS, Balduini FC, Zelko RR, Pavlov H, Peff TC, Das M: Fractures of the base of the fifth metatarsal distal to the tuberosity: Classification and guidelines for nonsurgical and surgical management. J Bone Joint Surg Am 1984;66:209-214.
DeLee JC: Fractures and dislocations of the foot, in Mann R, Coughlin M (eds): Surgery of the Foot and Ankle, ed 6. St Louis, MO, Mosby, 1993, pp 1465-1503.
Question 70
An 80-year-old African American woman who lives in a large city is scheduled for total hip arthroplasty to address primary osteoarthritis. Part of the presurgical protocol includes nasal swab screening to assess for methicillin-resistant Staphylococcus aureus (MRSA) colonization. Which demographic factor places this patient at highest risk for a positive result?
Explanation
Demographic factors are associated with increased risk for MRSA colonization, so it is important to identify vulnerable patients. Female gender and advanced age reduce the risk for colonization, whereas African American race increases this risk. Urban environments do not influence MRSA colonization.
Question 71
All of the following are characteristic of end-stage septic shock EXCEPT?

Explanation
Question 72
Figure 56 is the radiograph of an otherwise healthy 3-year-old boy who fell and sustained the isolated injury shown. What is the best treatment modality?
Explanation
At 3 years of age, children do well with nonsurgical treatment with early spica casting and early mobilization. There is no indication to perform surgical stabilization in such a closed isolated injury. The fracture is not shortened unacceptably according to clinical practice guidelines, and traction for this fracture is unnecessary. Traction also may be problematic for the family and healthcare system.
RESPONSES FOR QUESTIONS 57 THROUGH 62
Cortical thickening in the region of the lesion
Erosive metaphyseal lesion with loss of cortical integrity
Normal bony anatomy on radiographs
Diffuse articular erosion with loss of joint space
Round, expansive, well-circumscribed metaphyseal lesion with thinning of the cortex
Eccentric well-circumscribed metaphyseal lesion with a scalloped border
Match the orthopaedic condition described below with the expected radiographic finding listed above.
Question 73
What mechanism of injury is most likely to cause a fracture of the anteromedial facet of the coronoid?
Explanation
(SBQ12TR.86) Figure A shows intraoperative radiographs of a 45-year-old patient with a left elbow injury. What would be the next most appropriate step in this patients care?
Early range of motion
Hinged elbow brace for 4 weeks
Repair lateral collateral ligament
Remove and upsize implant
Remove and downsize implant
The intraoperative images are consistent with overstuffing of the ulnohumeral joint during a radial head replacement. The most appropriate next step would be removing and downsizing the implant.
Overstuffing the radiohumeral joint by >2.5 mm can significantly alter elbow kinematics. It has also shown to lead to pain and early joint disease. The most sensitive method to assess for overstuffing of the joint is by direct visualisation intraoperatively. This can be performed by visualising the lateral aspect of the ulnohumeral joint when the radial head is resected and comparing this to when the trial radial head is reduced in place. In comparison, radiographic asymmetry of the medial ulnohumeral joint has been shown to be less sensitive. Radiographic findings of incongruity of ulnohumeral joint only occurs when significant overlengthening of the radius occurs.
Frank et al. examined the effect of radial head thickness in seven cadaver specimens. They found that incongruity of the medial ulnohumeral joint would only become apparent radiographically after overlengthening of the radius by >or=6 mm.
Doornberg et al. examined seventeen computed tomography scans of the elbow to investigate the height of the radial head relative to the lateral edge and central ridge of the coronoid process. They found that the radial head was on average only 0.9 mm more proximal than the lateral edge of the coronoid process.
Figure A shows intraoperative radiographs of a patient that has undergone a radial head arthroplasty. There is significant widening of the medial ulnohumeral joint on an AP radiograph as well as widening of the ulnohumeral joint on the lateral radiograph,
Incorrect Answers:
Question 74
006%-3.4 %. The typical skin flora includes staph and strep as well as P. acnes, which has a propensity for the shoulder. Because it is an anaerobic organism, cultures may only become positive after 7-21 days.
Explanation
A 47-year-old, healthy, active patient presents with a sub-acute, full-thickness supraspinatus tear. His physical examination reveals significant weakness and pain with abduction. There was no glenohumeral instability. Radiographs demonstrate a type 1 acromion. An MRI scan shows a crescent shaped tear with 2-cm of tendinous retraction and no tendinous fatty changes. A subacromial corticosteroid injection 6 weeks ago provided him with 24 hours of pain relief but no improvement in strength. What would be the most appropriate treatment option?
Repeat subacromial corticosteriod injection

Biological augmentation of rotator cuff with porcine small intestine xenograft Rotator cuff repair

Rotator cuff repair plus acromioplasty

Rotator cuff repair, remplissage procedure, bicep tenodesis and distal clavicle excision
This patient has an isolated supraspinatus rotator cuff tear with symptomatic weakness. The most appropriate treatment would be isolated rotator cuff repair.
The primary purpose of rotator cuff repair is to restore muscle function. Secondary outcomes include reduction of pain and prevention of irreversible cuff changes, specifically muscular atrophy. Non-operative treatment ( exercise, therapy and pain medications) are recommended for partial thickness tears. The indication of surgical repair includes, isolated supraspinatus weakness +/- pain
that correlates with MRI imaging of a respective full thickness tear. Routine acrominoplasty is not recommended in conjunction with rotator cuff repair, especially with no previous symptoms of impingement.
Pedowitz et al. developed clinical practice guidelines for the treatment of rotator cuff pathology. The strongest supporting evidence in current literature was given a grade of 'moderate' with four treatment recommendations. These were,
Exercise and non-steroidal anti-inflammatory drugs can be used to manage partial thickness tears,

Routine acromioplasty is not required the time of cuff repair,
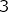
Non-cross-linked, porcine small intestine submucosal xenograft patches should not be used to manage cuff tears, and

Surgeons can advise patients that workers' compensation status correlates with a less favorable outcome after rotator cuff surgery.
Illustration A shows the different shapes of rotator cuff tears. Incorrect Answers:
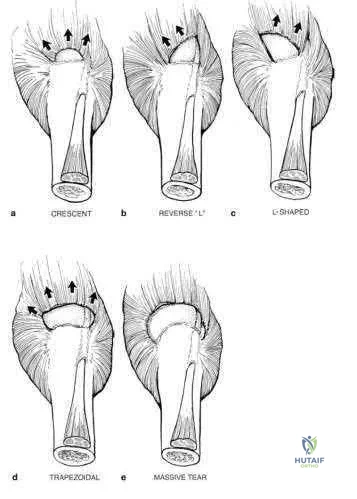
A 12-year-old baseball pitcher describes progressive worsening of medial elbow pain on
his throwing side. Examination reveals normal elbow range of motion. He is tender over the medial elbow to palpation. A dynamic ultrasound of his elbow shows no evidence of medial widening with valgus stress. His radiograph is shown in Figure A and an MRI is shown in Figure B. What is the most likely cause of his symptoms?
Displaced medial epicondyle avulsion fracture Medial apophysitis
Medial ulnar collateral ligament tear
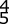
Valgus extension overload with olecranon osteophytes Ulnar neuritis
The clinical presentation is consistent with Little League Elbow caused by medial apophysitis. Little League elbow is a general term explaining medial elbow pain in adolescent pitchers. The underlying pathology can include medial epicondyle stress fractures, avulsion fractures of the medial epicondyle, ulnar collateral ligament (UCL) injuries, or medial epicondyle apophysitis. In order to identify the underlying cause it is important to first rule out injury to the MCL by looking for medial widening on stress radiographs or dynamic ultrasound, or valgus instability on physical exam. Radiographs are useful to look for avulsion fractures or subtle physeal widening commonly seen with apophysitis.
Wei et al. obtained radiographs and magnetic resonance imaging on nine adolescent pitchers with a clinical diagnosis of Little League Elbow. They found radiographic findings in 4/9 and MRI findings in 6/9 patients. They emphasized that the MRI did not change management in any patients. Cain et al. review the different elbow conditions seen in throwing athletes. They emphasize the need to understand the underlying pathophysiology in order to treat and make appropriate changes to the biomechanics of the pitching technique.
Figure A shows an AP radiograph with slight widening of the apophysis, but no evidence of avulsion fracture. Figure B is an MRI which shows signal consistent with edema of the medial epicondyle apophysis.
Incorrect Answers:
The other responses are all typical throwing elbow conditions, but are much less common than apophysitis in the adolescent thrower.
What is the primary function of the structure labeled with an asterisk in Figure A?
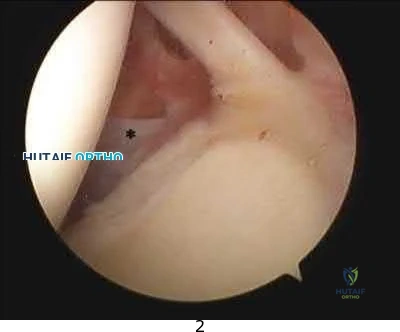
Prevents inferior translation of the humerus with the arm by the side Provides internal rotation of the humerus

Prevents anterior translation of the humerus with the arm in 45 degrees of abduction Prevents anterior translation of the humerus with the arm in 90 degrees of abduction Provides supination of the forearm and elbow flexion
The labeled structure is the middle glenohumeral ligament (MGHL) of the shoulder. The primary function of the MGHL is to prevent anterior translation of the humeral head with the arm in 45-60 degrees of abduction.
This structure originates from the glenoid labrum and inserts medial to the lesser tuberosity running obliquely across the subscapularis. The size of the structure may be variable and there are recognized normal anatomic variants ( including a cord like MGHL in the Buford complex). It is important to be able to recognize the MGHL and differentiate this from the subscapularis, IGHL, SGHL, and other intraarticular structures in the shoulder to be able to perform effective and precise arthroscopic procedures.
Burkhart et al. describe the function of the glenohumeral ligaments in anterior shoulder instability, noting that the MGHL provides a restraint to anterior translation with the arm in 45-60 degrees of abduction.
Wang et al. discuss microdamage to the inferior glenohumeral ligament from a basic science perspective, indicating that over time it may stretch and compromise it's function in restraining humeral translation.
Figure A is an arthroscopic image of the intraarticular structures of the shoulder with an asterisk on the MGHL.
Incorrect Answers (these are labeled on Illustration A, with the exception of the subscapularis which is difficult to visualize):

In which of the following clinical circumstances would it be appropriate to eccentrically ream the anterior glenoid?

year-old male undergoing a shoulder arthroplasty due to rotator cuff arthropathy 65-year-old female with a glenoid retroversion of 13-degrees undergoing shoulder arthroplasty

year-old female with humeral anteversion of 13-degrees undergoing shoulder arthroplasty

year-old female with glenoid retroversion of 25-degrees undergoing shoulder arthroplasty

year-old male with significant glenoid bone stock deficiency and severe osteoarthritis
The surgeon should consider eccentrically reaming the anterior glenoid when performing a total shoulder arthroplasty on a patient with a retroverted glenoid due to posterior deficiency associated with osteoarthritic changes which is most consistent with answer choice #2.
Normal version of the glenoid is 0-3 degrees of retroversion, but when doing a total shoulder the goal should be to place the glenoid component in neutral to slight anteversion. Reaming the anterior glenoid to neutral is a technique to be considered by the operative surgeon when presented with a patient undergoing total shoulder arthroplasty with a retroverted glenoid, as failure to perform this step increases the chance for glenoid loosening. If reaming down the anterior glenoid will take away too much bone stock (down to the coracoid process), one may consider bone grafting the posterior glenoid. To perform a total shoulder arthroplasty patients will need a functioning rotator cuff and appropriate glenoid bone stock.
Clavert et al. performed cadaveric analysis to simulate glenoid retroversion of greater than 15 degrees and found that retroversion to this degree cannot be safely corrected with eccentric anterior reaming when using a glenoid component with peripheral pegs due to penetration into the glenoid vault.
Nowak et al. used 3D-CT models of patients with advanced shoulder osteoarthritis with varying degrees of glenoid retroversion and simulated glenoid resurfacing. They found that smaller size glenoid components may allow for greater version correction when using in-line pegged components, as they would be less likely to result in peg penetration.
Illustration A shows >25 degrees of glenoid retroversion seen by axial radiograph of the shoulder in a patient with advanced osteoarthritis. In this case, anterior glenoid reaming is not the correct answer and a posterior glenoid allograft reconstruction would be appropriate.
Incorrect Answers:
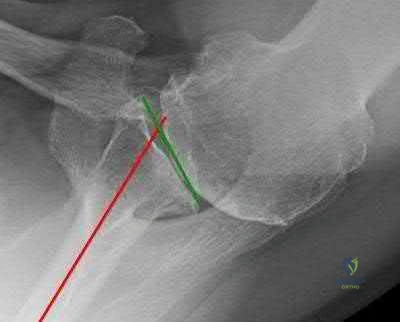
A 44-year-old left-hand dominant carpenter experienced immediate left elbow pain after trying to stop a heavy object from falling two days ago. Figure A shows a clinical image of the patient upon presentation. Physical exam shows full strength with wrist flexion, wrist extension, and pronation, but notable weakness with supination of the forearm. Sensory exam shows no deficits in the forearm or hand. There is a negative milking maneuver test and a positive hook test. Radiographs are shown in Figure B. What is the next most appropriate step in management?
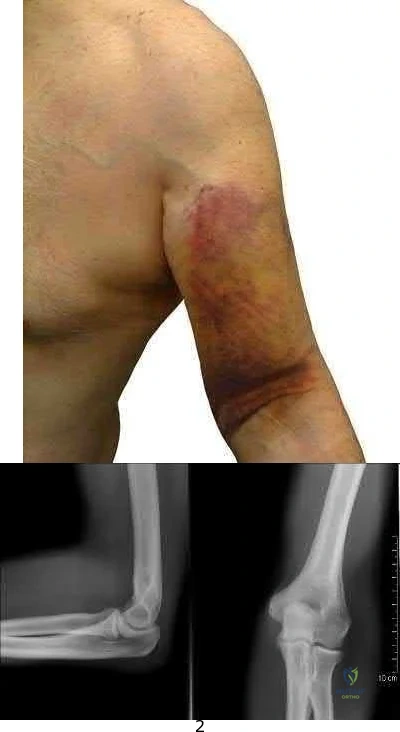
Sling use as needed for comfort and progressive physical therapy Allograft reconstruction of the distal biceps tendon
Ulnar collateral ligament reconstruction Distal biceps tendon avulsion repair Brachioradialis and ECRB avulsion repair
Distal biceps tendon avulsion repair is the most appropriate next step in management.
Distal biceps tendon ruptures occur most commonly in middle-aged men and usually involve the dominant extremity. The mechanism of injury is usually a single traumatic event with eccentric force on the flexed elbow.
Sutton et al. authored a Level 5 review of distal biceps tendon ruptures. They discuss that nonsurgical management of distal biceps tears is appropriate in the low-demand or medically ill patient. Surgical repair improves elbow flexion strength by 30% and supination strength by 40% compared to nonoperative management.
O'Driscoll et al. conducted a Level 2 study examining the accuracy of the hook test for distal biceps rupture diagnosis. They found that the hook test was abnormal in 33 of 33 (100%) patients with complete biceps avulsions, and intact in 12 of 12 (100%) with partial detachments.
Figure A is a clinical image demonstrating ecchymosis in the distal arm and antecubital fossa. Figure B shows normal elbow radiographs. Illustration A shows a normal hook test with an intact distal biceps insertion.
Incorrect Answers:
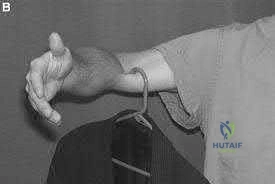
Early reverse total shoulder designs (before the development of the Grammont-style prosthesis) had a high failure rate due to early loosening of the glenoid component. What biomechanical feature accounted for this problem?

Glenoid component did not have a neck Humeral component too horizontal Center of rotation too lateral
Center of rotation too anterior Center of rotation too inferior
Early reverse ball-and-socket designs failed because their center of rotation remained lateral to the scapula, which limited motion and produced excessive torque on the glenoid component, leading to early loosening. The first modern reverse prosthesis was designed by Paul Grammont. According to Boileau et al., Grammont's design "introduced 2 major innovations (1) a large glenoid hemisphere with no neck and (2) a small humeral cup almost horizontally oriented with a nonanatomic inclination of 155 degrees, covering less than half of the glenosphere. This design medializes the center of rotation compared to earlier versions which minimizes torque on the glenoid component. Furthermore, the humerus is lowered relative to the acromion, restoring and even increasing deltoid tension. The Grammont reverse prosthesis imposes a new biomechanical environment for the deltoid muscle to act, thus allowing it to compensate for the deficient rotator cuff muscles." According to Gerber, "moving the center of rotation more medial and distal as well as implanting a large glenoid hemisphere that articulates with a humeral cup in 155 degrees of valgus are the biomechanical keys to sometimes spectacular short- to midterm results".
Which of the following preoperative factors is a contraindication to total shoulder arthroplasty?

Passive external rotation less than 10 degrees Eccentric posterior glenoid erosion
A 2-cm full-thickness supraspinatus tendon tear Inflammatory arthritis

A preganglionic brachial plexus injury
A preganglionic brachial plexus palsy, otherwise known as a root avulsion injury, presents with a flail arm and has a poor prognosis for recovery of motor function. Patients with brachial plexus palsies are not candidates for total shoulder arthroplasty due to the substantial motor and sensory deficits associated with these injuries.
In contrast, patients with a preoperative loss of passive external rotation, posterior glenoid erosion, a reparable full-thickness rotator cuff tear isolated to the supraspinatus tendon, and inflammatory arthritis are not contraindicated for a total shoulder arthroplasty.
Iannotti et al. performed a Level I prospective study in 118 patients who underwent either a total shoulder arthroplasty or a shoulder hemiarthroplasty for primary osteoarthritis. The presence of a reparable full-thickness rotator cuff tear did not adversely affect outcomes in either group but rather provided better active external rotation in the cohort receiving total shoulder arthroplasties. The authors concluded that a reparable tear of supraspinatus is not a contraindication to the use of a glenoid component.
Norris et al. compared outcomes of total shoulder arthroplasty and hemiarthroplasty performed for primary osteoarthritis in 160 patients. There were no differences in postoperative pain, function, ASES scores, or range of motion between groups for patients with reparable rotator cuff tears. The authors concluded that minor thinning and small tears of the rotator cuff can be adequately addressed at the time of surgery without adversely affecting outcomes.
Illustration A is a cervical T2 axial MRI which shows a cervical root avulsion, a form of preganglionic brachial plexus injury. Notice the perineural hyperintensity.
Incorrect Answers:
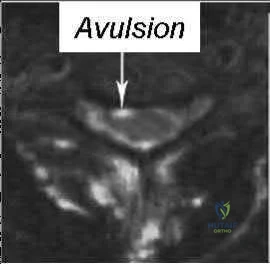
A 42-year-old male sustains a flail chest injury and subsequently undergoes operative stabilization of his chest wall. At first follow-up, the inferior angle of his ipsilateral scapula translates medially with any attempt at overhead activity. Injury to which of the following structures would cause this abnormality?

Spinal accessory nerve C8 and T1 nerve roots
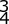
Upper and lower subscapular nerves Thoracodorsal nerve

Long thoracic nerve
The clinical vignette describes medial scapular winging, which is seen after injury to the long thoracic nerve.
Medial scapular winging due to a long thoracic nerve palsy can be seen after repetitive stretching in athletes, with direct compression injury, or even iatrogenically during surgical procedures to the lateral thorax. Injury to the long thoracic nerve will eliminate the function of the serratus anterior,
which acts to protract the scapula laterally and upward and stabilize the vertebral border of scapula. This results in upper extremity weakness in forward elevation or abduction as the scapula is not stabilized against the thorax.
Meininger et al. report that lesions of the long thoracic nerve and spinal accessory nerves are the most common cause of scapular winging, although numerous underlying etiologies have been described. They report patients describe diffuse neck pain, shoulder girdle discomfort, upper back pain, and weakness with abduction and overhead activities. They also report that most cases are treated nonsurgically.
Wiater et al. review injuries to the spinal accessory nerve which causes dysfunction of the trapezius and subsequent lateral scapular winging. They note that the superficial course of the spinal accessory nerve in the posterior cervical triangle makes it susceptible to injury, and iatrogenic injury to the nerve after a surgical procedure is one of the most common causes of trapezius palsy. Most injuries are treated nonoperatively, but the Eden-Lange procedure, in which the insertions of the levator scapulae, rhomboideus minor, and rhomboideus major muscles are transferred, relieves pain, corrects deformity, and improves function in patients with irreparable injury to the spinal accessory nerve.
Illustration A shows a clinical photo of medial scapular winging, while illustration B shows a clinical photo of lateral scapular winging. Illustration C shows the long thoracic nerve during a rib fixation procedure, with the nerve sitting directly on top of the serratus anterior. The trapezius is overlying the scapula at the bottom of the photo, and the patient's head is to the right of the photo. Incorrect Answers:
A patient sustains a distal biceps brachii tendon rupture. If treated non-operatively, the greatest loss of strength would be seen with which activity?

Forearm supination Forearm pronation

Elbow flexion
Shoulder forward flexion Shoulder internal rotation
While both elbow flexion and forearm supination strength are affected, there is a greater percentage loss of supination strength. Patients may complain of weakness and fatigue with rotational activities such as using a screwdriver. The primary elbow flexor is actually the brachialis, and therefore less weakness in flexion is reported.
Patterson reviewed distal biceps ruptures and found nonsurgical treatments had 21 55% loss of supination strength and 8 36% loss of flexion strength.
Klonz reviewed anatomic and non-anatomic repairs and found better results with anatomic repairs with 91% return of supination strength and 96% return of flexion strength. Supination strength after nonanatomic repair did not improve in 4 of 8 patients (42%-56% of the uninjured arm).
A 27-year-old right hand dominant construction worker falls off a scaffold onto his outstretched arm. Figure A exhibits the radiograph taken at a local emergency room.
Following treatment, he is placed in a sling and follows up at your office two weeks later. He complains of a feeling that his arm is going to 'pop out'. Which specific physical examination finding is likely to be present?
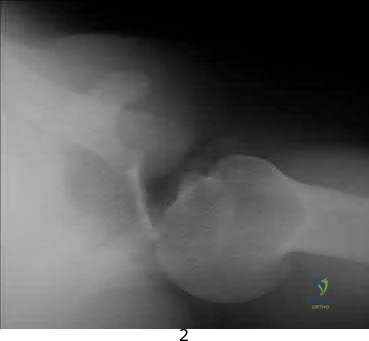
Hornblower's Test Jobe's Test
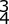
Apprehension Sign with shoulder abducted and externally rotated Speed's Test

Kim's Test
The patient suffered a posterior shoulder dislocation, likely injuring the posterior capsule and/or labrum. Out of all the answer choices, Kim's test assesses posterior structures. Thus, Kim's test is the physical examination finding most likely to be present.
Posterior dislocations occur less frequently than anterior dislocations, and are often missed. Following closed reduction, persistent instability can occur, usually associated with posterior capsular or labral pathology. Posteriorly directed provocative maneuvers, such as the Kim test can be positive.
Robinson et al. performed an epidemiologic analysis on 120 posterior dislocations. Recurrent instability occurred at a rate of 17.7%. Risk factors for recurrent instability included age less than 40-years-old, dislocation during seizure, and a large reverse Hill-sachs (>1.5 cm3). Kim et al. describe the Kim lesion, a separation between the posteroinferior labrum and the articular cartilage without complete detachment of the labrum, which cause persistent posterior instability.
Figure A depicts a posterior dislocation on xray. Illustration A depicts the Kim test, which is performed by having the patient seated, arm at 90° abduction, followed by flexing the shoulder to 45° forward flexion while simultaneously applying axial load on the elbow and posterior-inferior force on the upper humerus. The test is positive when there is pain. Video 1 depicts the proper way to perform a Kim Test.
Incorrect answers:
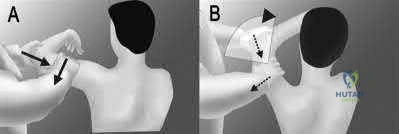
A 27-year-old male bodybuilder presents to the office with vague, deep shoulder pain and weakness with his bench press. His examination is somewhat difficult due to his large size, but no significant abnormal findings are noted. Radiographs are normal, and an MRI arthrogram is shown in Figure A. Which of the following is the most likely etiology of his complaints?
Pectoralis major rupture Supraspinatus partial thickness tear SLAP lesion
Tendonitis of the long head of the biceps Posterior labral tear
The clinical presentation and MRI are consistent with a Posterior labral tear.
Posterior labral tears are commonly seen in individuals that have repeated posteriorly-directed stress across their glenohumeral joint (football linemen, bodybuilders). These patients will often present with ill-described pain deep in their shoulder joint, along with decreases in shoulder strength. Focused shoulder examinations, such as the Jahnke Jerk Test or Push-pull test, can elicit pain from posterior labral tears; however, the sensitivity and specificity of these tests remain under question.
Mair et al. reviewed the outcome of posterior labral injuries in nine athletes who underwent arthroscopic repair with a bioabsorbable tack after failure of conservative management; all were
able to return to contact sports. They note that posteriorly applied forces can result in a shear-type vector that can cause posterior labral tears without capsular injury.
Bradley et al. reviewed 91 athletes with unidirectional recurrent posterior shoulder instability that were treated with an arthroscopic posterior capsulolabral reconstruction. They found that significant improvements in stability, pain, and function at a mean of 27 months postoperatively. Eightynine percent of the patients were able to return to their sport.
Figure A shows an axial MRI arthrogram of the shoulder with a posterior labral tear and an associated paralabral cyst. Illustration A is another axial shoulder MRI arthrogram cut showing a posterior labral tear (red arrow) and an associated paralabral cyst (yellow arrows).
Incorrect Answers:
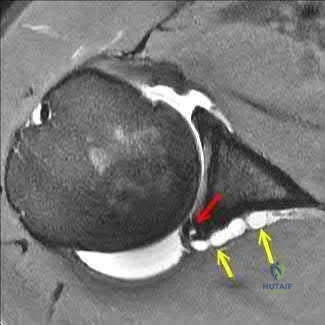
A patient sustains a full thickness tear of their teres minor. Which of the following test/signs would most likely be positive in this patient?

Jobe's test Belly press test
Internal rotation lag sign Hornblower's sign Hawkin's sign
Hornblower's test is completed by asking the patient to hold their shoulder in 90 degrees of abduction and 90 degrees of external rotation. The test is positive if the arm falls into internal rotation or they are unable to actively externally rotate against resistance. This suggests teres minor pathology.
There are various tests/signs used by clinicians to detect rotator cuff pathology. The teres minor is innervated by the axillary nerve and functions to externally rotate the humerus. The hornblower's test/sign has various descriptions, but all act to determine external rotation weakness. In addition to being sensitive and specific for teres minor pathology, it can also be positive with posterior supraspinatus tears.
Walch et al. review 54 patients that underwent repair of combined supraspinatus and infraspinatus rotator-cuff tears. They found that the hornblower's sign was highly sensitive and specific for irreparable degeneration of the teres minor, while the dropping-sign was highly sensitive and specific for irreparable degeneration of the infraspinatus.
Hertel et al. prospectively review 100 patients with painful shoulders and impingement syndrome. They compared various lag signs (ERLS-external rotation lag sign, IRLS-internal rotation lag sign, drop sign) to the Jobe and lift-off signs. The ERLS was less sensitive but more specific than the
Jobe sign for the supraspinatus/infraspinatus. The drop sign was the least sensitive but was as specific as the ERLS. The IRLS was as specific but more sensitive than the lift-off sign for subscapularis tears.
Illustration A shows another variation of the hornblower's sign as originally desbribed by Arthui et
positive if the patient is unable to do this without abducting the affected arm and demonstrates the difficulty in raising the hand to the mouth in the absence of external rotation of the shoulder. The video provided shows how to perform both variations of the hornblower's test.
Incorrect Answers:
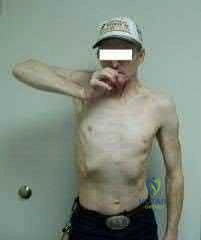
Reverse total shoulder arthroplasty combined with latissimus dorsi transfer would be
most appropriate for which of the following patients?
year-old male with post-traumatic shoulder arthritis after a four-part proximal humerus fracture with no motor dysfunction

year-old male with grade 4 shoulder arthritis with severe deltoid muscle dysfunction secondary to a stroke

year-old female with significant rotator cuff arthropathy, a negative Hornblower sign and less than 5 degrees of external rotation lag

year-old female with pseudoparesis of anterior elevation and external rotation, narrowing of gleno-humeral joint and acetabularization of the acromion

year-old male with grade 4 shoulder arthritis and an isolated supraspinatus tear
Reverse total shoulder arthroplasty combined with latissimus dorsi transfer would be most appropriate in a patient with pseudoparesis of anterior elevation and external rotation, in the setting of shoulder arthritis (narrowing of glenohumeral joint and acetabularization of the acromion).
Combining a latissimus dorsi tendon transfers with reverse total shoulder arthroplasty (R-TSA) helps to restore control of active external rotation. Dysfunction with external rotation can be determined clinically with external rotation lag sign, a positive Hornblower's sign, and radiographically with fatty degeneration of the teres minor classified as stage 2 or greater according to the system of Goutallier et al. or Fuchs et al.
Gerber et al. found that R-TSA with combined lat dorsi transfer yielded minimal improvements in external rotation ROM (13 deg to 19 deg) compared to increases in shoulder ROM in flexion (94 deg to 137 deg) and abduction (87 deg to 145 deg), with this procedure.
Boileau et al. examined 17 consecutive patients treated with reverse shoulder arthroplasty and latissimus dorsi and teres major transfer (L'Episcopo). They found that external rotation increased from -21 degrees to 13 degrees (+34 degrees ). They recommend transferring both the LD and TM, rather than the LD alone as it results in better active external rotation.
Illustration A is a radiograph showing a right reverse total shoulder replacement. Illustration B shows a cadaveric image of the positioning of the latissimus dorsi tendon transfer prior to implantation of the reverse total shoulder components.
Incorrect Answers
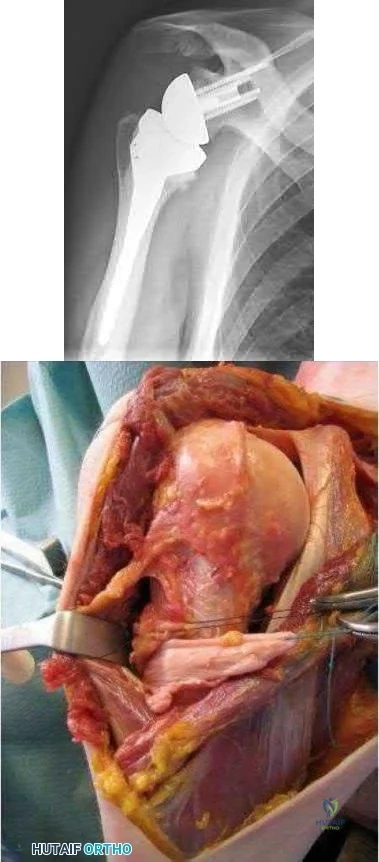
Figure A and B are MRI images of a 42-year-old male with symptoms of right shoulder neuropathy. If this patient has an abnormality detected on EMG and nerve conduction testing, which of the following nerves is most likely to be involved?
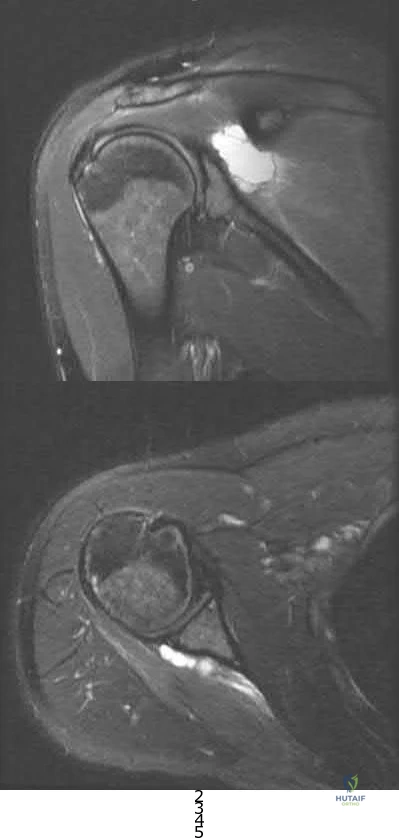
Subscapular nerve Axillary nerve Musculocutaneous nerve Suprascapular nerve Long thoracic nerve
This patient is presenting with suprascapular nerve compression secondary to a spinoglenoid cyst. Injuries of the posterior shoulder joint capsule or posterior-superior labrum can result in spinoglenoid cysts. They may lead to suprascapular nerve palsy.
Patients will present with characteristic findings of external rotation
( infraspinatus) weakness when the cyst is isolated in the spinoglenoid notch. If the cyst is located in the suprascapular notch, both external rotation weakness and abduction (supraspinatus) weakness will be present. Electromyography and MRI are the investigations of choice in depicting the etiology of this mononeuropathy.
Piatt et al. found posterosuperior labral tears in 65/73 patients who had spinoglenoid notch cysts. All patients presented with should pain and weakness. Patients undergoing surgical intervention by drainage or excision +/- arthroscopic labral repair had a better outcome than non-operative care.
Westerheide et al. reported fourteen patients who underwent arthroscopic decompression of ganglion cysts associated with suprascapular neuropathy. All patients had a labral tear intraoperatively with arthroscopic drainage and labral repair. There was not recurrence at an average of 51 months of followup.
Piasecki et al. reviewed suprascapular neuropathy. Causes include:nerve entrapment along this path, particularly at the vulnerable suprascapular and spinoglenoid notch, as well as extrinsic compression by soft-tissue masses.
Figures A is a coronal MRI showing a large hyperintense mass medial to the glenoid articulation. Figure B shows an axial MRI of the lesion posterior to the glenoid. Illustration A shows a diagram of the posterior right shoulder. The suprascapular nerve can be seen traveling through the spinoglenoid notch. Incorrect Answers:
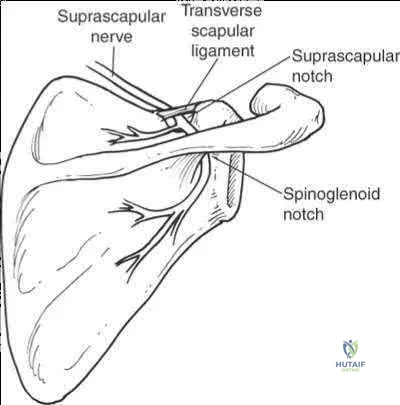
A 12-year-old right-hand-dominant pitcher presents with progressive right shoulder pain. He is now unable to pitch. He is tender to palpation over the lateral shoulder and has pain with rotation. An AP radiograph of the affected shoulder is shown in Figures A and a contralateral radiograph is shown in Figure B. What is the most likely diagnosis?
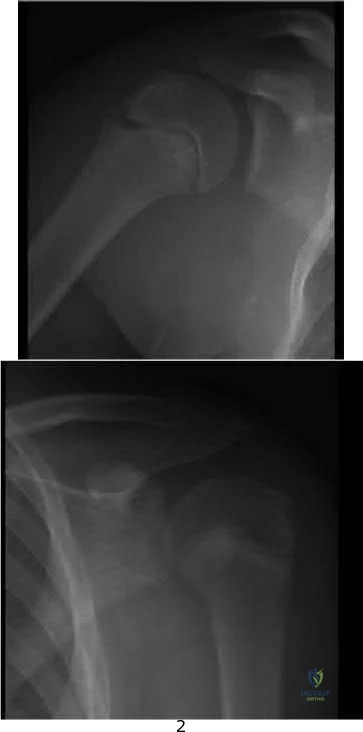
Septic arthritis of the shoulder SLAP tear
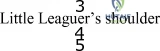
External impingement Internal impingement
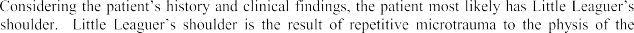
proximal humerus. Patients may report a recent increase in pitching regimen. On examination, there is focal tenderness at the level of the physis. Treatment focuses on rest, physical therapy and a progressive throwing program. Pitching is often stopped for 2-3 months during rehabilitation.
Chen et al. review shoulder and elbow injuries in the young athlete. Little
Leaguer's shoulder results from epiphyseal lysis secondary to microtrauma. Pain over the anterolateral shoulder may be elicited on examination. The mainstay of treatment is 2-3 months of rest and return to pitching via a progressive throwing program.
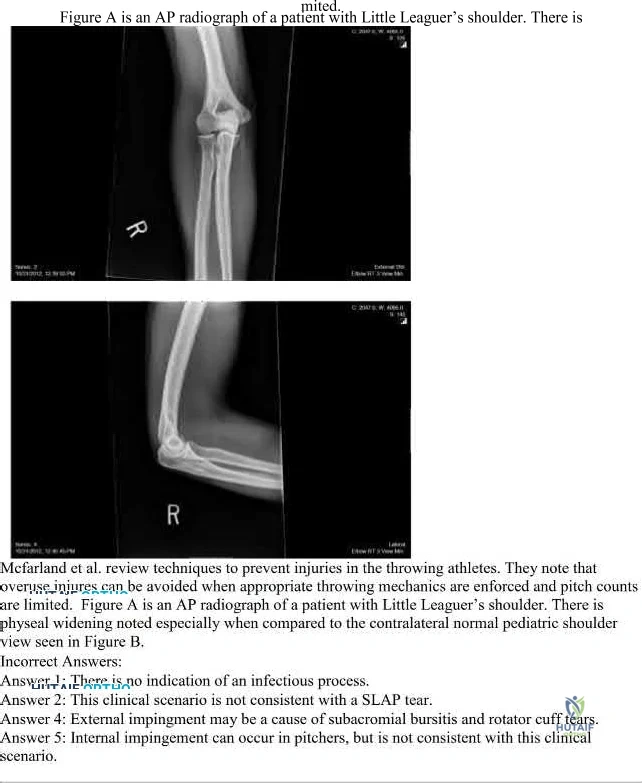
Mcfarland et al. review techniques to prevent injuries in the throwing athletes. They note that overuse injures can be avoided when appropriate throwing mechanics are enforced and pitch counts are li
physeal widening noted especially when compared to the contralateral normal pediatric shoulder view seen in Figure B.
Incorrect Answers:
A 35-year-old carpenter has pain in the antecubital fossa that is worse with turning a screwdriver. He has undergone non-operative treatment for 6 months without relief. On physical examination his hook test is normal and there is pain and weakness with resisted supination. Radiographs are shown in Figures A-C. A MRI of the right elbow is shown in Figure D. The next most appropriate treatment is?
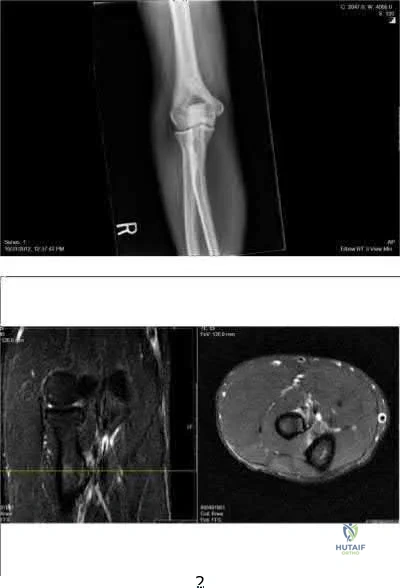
Exploration of the radial tunnel Superficial radial neurectomy

Detachment and repair of the biceps tendon Transfer of the biceps to the brachialis EMG with nerve conduction study
While complete trauamtic rupture of the distal biceps is more common, partial tears have been reported in the literature. The most common presentation is pain in the antecubital fossa worse with resisted supination.
Conservative management consists of NS
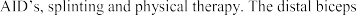
Transfer to the brachialis improves flexion strength but not supination.
Ramsey et al present a review article on distal biceps tendon injuries. They state that the most successful management of partial distal biceps tears that have failed conservative management is to surgically treat it like a complete rupture with release and surgical reattachment of the distal biceps to the radial tuberosity.
Figures A-C are normal radiographs of the elbow. Figure D is a crossreferenced axial and coronal T2 MRI that demonstrates increased signal and partial distal biceps tendon tearing. Illustration C shows the resected region of distal biceps tendon in the same patient and had an excellent functional outcome following distal biceps release and surgical reattachment with 2 double-loaded suture anchors.
Video V demonstrates The hook test for detecting complete distal biceps tendon avulsions.

A 49-year-old man sustains a dislocation of his left elbow that is successfully reduced and splinted. He misses his scheduled follow-up appointments and returns 6 weeks later. He is immediately enrolled in a course of vigorous physical therapy. At a repeat visit at 6 months, examination reveals that he lacks 40 degrees of elbow extension, and has flexion to 80 degrees. He is taken to the operating room for surgical release. Figures A and B are diagrams depicting the ligamentous attachments about the elbow. To restore elbow flexion, in addition to releasing the articular capsule, which ligament should be released?
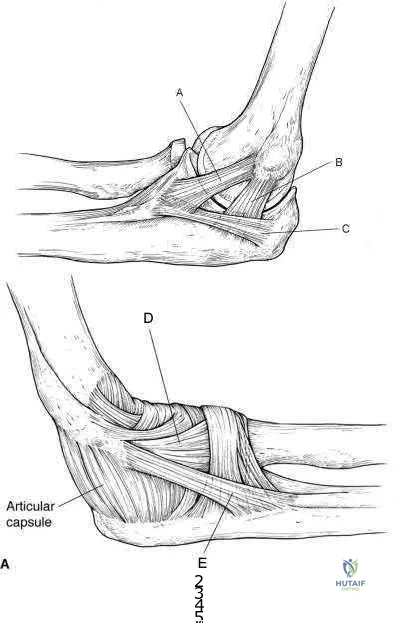
Ligament A Ligament B Ligament C Ligament D Ligament E
In addition to capsular release, the posterior band of the medial collateral ligament (MCL) should be released.
The posterior band of the MCL is attached dorsal to the axis of rotation and has greater variation in length. It increases in length by 9 mm between 60° and 120° of flexion. Posterior band contracture leads to loss of elbow flexion. In contrast, the anterior band of the MCL (AMCL) maintains a constant length ( isometric) throughout the entire arc of movement. Anterior capsule contracture leads to loss of extension.
Wada et al. treated 14 elbows with post traumatic contracture. Through a medial incision, the ulnar nerve was freed and the posterior band and posteromedial joint capsule were excised. Mean flexion increased from 89° preop to 127° postop. Anterior capsulectomy was performed for limited extension.
Morrey et al. studied structures providing stability about the elbow. They found that the anterior capsule stabilizes the elbow to varus-valgus stress in extension, not in flexion. The anterior band of the MCL is a primary stabilizer, especially in flexion.
Figures A and B are medial and lateral illustrations of the elbow, respectively, depicting the ligamentous attachments. Illustrations A and B are radiographs are 3D CT reconstruction images of the left elbow, respectively, showing heterotopic ossification around the posterior band of the MCL.
Incorrect Answers:
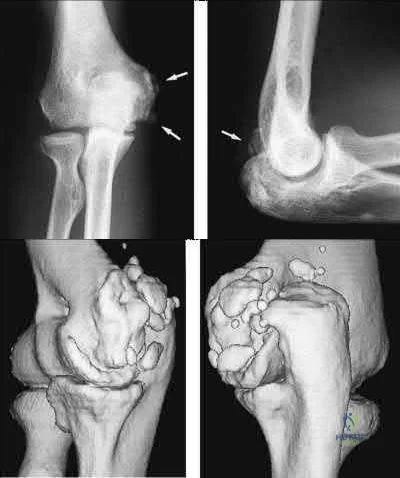
A 23-year-old male sustains a dislocation of his elbow that was successfully closed reduced in the emergency room. 3 months later, the patient presents with pain and a catching sensation in his elbow. On physical exam, he is noted to have a positive lateral pivot-shift test. Incompetence of which of the following ligaments in Figure A is most commonly associated with his condition?
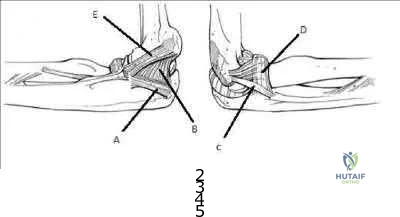
A B C D E
The patient is presenting with symptoms and physical exam consistent with posterolateral rotatory instability. Injury to the lateral ulnar collateral ligament
( LUCL), labeled C in Figure A, allows an abnormal external rotation
( supination) of the ulna on the humerus. This results in posterolateral rotatory instability. Posterolateral rotatory instability often presents as pain and recurrent clicking, snapping, clunking, or locking of the elbow. It should be noted that frank dislocations are not the most common presenting symptom. The physical exam is usually benign except for a positive lateral pivot-shift test or posterolateral rotatory drawer test. While injury to the LUCL is thought to be the primary pathology, other ligamentous stabilizers of the elbow may play a role.
Mehta et al. review posterolateral rotatory instability of the elbow. They state the instability usually results from an elbow dislocation with subsequent failure to heal of the ligamentous structures.
Patients with recurrent instability often require surgical intervention, as bracing is typically cumbersome and ineffective.
The video provided shows how to perform the lateral pivot-shift test. The patient is placed in the supine postion with forearm overhead and elbow extended. The elbow is then supinated with force and flexed to >40° while a valgus load applied. A positive result is palpable / visible clunk as the ulna and radius reduce suddenly. Illustration A shows the posterolateral rotatory drawer test.
External rotation and posterior forces are applied to the forearm attempting to sublux the radius posterior to the capitellum.
Incorrect Answers:
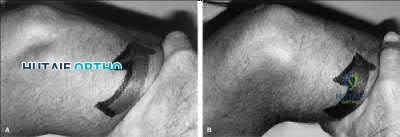
Figure A is the MR image of the left shoulder of an active 47year-old painter who has been experiencing shoulder pain for 9 months. In addition to the finding shown in Figure A, MRI examination of the intra-articular portion of the biceps tendon shows fraying greater than 50%. He has not obtained relief from an 8 month course of non-operative management including non-steroidal antiinflammatory medications, physical therapy and corticosteroid injection. What is the best next step in treatment?
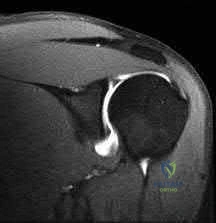
New course of physical therapy

Activity shutdown with 6 weeks sling immobilization
Arthroscopic superior labrum anterior to posterior (SLAP) tear repair Arthroscopic debridement and possible biceps tenotomy versus tenodesis

Arthroscopic rotator cuff repair and acromioplasty
This patient has a Type II SLAP lesion. These should only rarely be repaired in patients older than 40 years of age. If a source of pain refractory to nonoperative management, biceps tenotomy or tenodesis should be considered.
SLAP repair for Type II SLAP lesions is a procedure that has enjoyed a high success rate in young patients. These are generally not indicated for repair in patients greater than 40 years of age due to high rate of stiffness postoperatively. A subset of patients continue to do poorly after SLAP repair. Poor range of motion and the development of post-surgical adhesive capsulitis is often an etiology for poor results. Arthrofibrosis recalcitrant to diligent therapy over many months can be treated with arthroscopic capsular release. This is predicated on failure of a dedicated course of physical therapy as part of a non-operative management course lasting greater than six months. As the propensity for stiffness increases with age, consideration should be treated with SLAP tear debridement and biceps tenotomy or tenodesis in patients greater than 40 years old. Tenotomy or tenodesis, however, can be effective at providing pain relief in the presence of proximal biceps tendon pathology.
Katz et al. reviewed 34 patients who presented to their group for management of failed SLAP repair. 50% were Worker's Compensation cases. The mean age at the time of initial SLAP repair was 43 years. They treated these patients conservatively initially followed by revision surgery in 21 cases. All completed a course of physical therapy initially. They concluded that once a patient has failed SLAP repair, there is a high chance of further conservative treatment failing. Although revision surgery improves outcomes, 32% will continue to have a "suboptimal" result. Holloway et al. reviewed 50 patients who underwent arthroscopic capsular release for adhesive capsulitis, comparing three groups: (1) post-surgical; (2) post-fracture; and (3) idiopathic adhesive capsulitis. All patients had completed supervised physical therapy and a home exercise program for at least one year. They concluded that arthroscopic capsular release improved range of motion equally for all three groups but patients in the post-surgical group had poorer subjective pain, function and satisfaction scores.
Figure A is an MRI showing a Type II SLAP tear. Illustration A shows the classification of SLAP lesions.
Incorrect Answers:
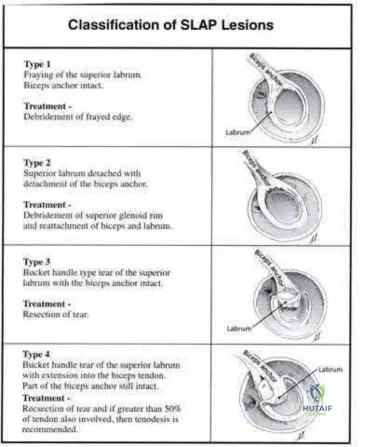
A 30-year-old man undergoes arthroscopic Bankart repair for recurrent anterior dislocation. He continues to experience instability postoperatively. Examination reveals a positive apprehension test. Radiographs of both shoulders are seen in Figure A. CT scan of his left shoulder is seen in Figure B. What is the best treatment option?
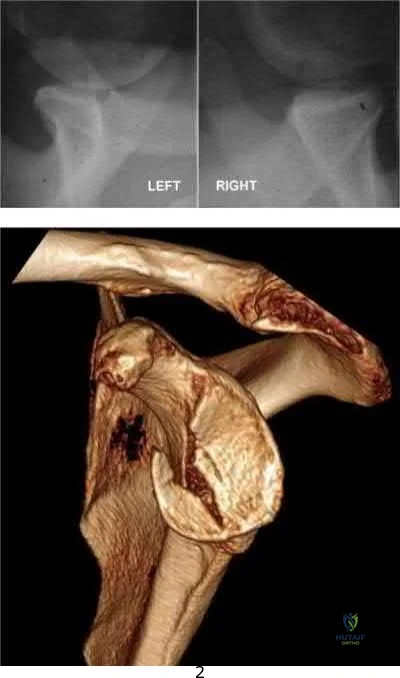
Bankart repair

Humeral head bone augmentation Remplissage
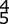
Coracoid autograft Connolly procedure
This patient has anterior glenoid bone deficiency (inverted pear glenoid) from a large bony Bankart lesion that was not adequately addressed in the index procedure. This is best treated with bony augmentation using the Latarjet vascularized coracoid transfer.
Patients with glenoid bone defects >20-30% have a high recurrence rate
(>60%) after Bankart repair alone. Bone grafting is necessary to offer containment. Autograft options include coracoid transfer (such as the Latarjet procedure which extends the articular arc and creates a conjoined tendon sling) and iliac crest bone grafting.
Burkhart et al. addressed glenohumeral bone defects. They advise that significant bone deficits cannot be adequately addressed via arthroscopic Bankart repair alone. The Latarjet transfer creates an extra-articular platform to extend the articular arc of the glenoid.
Hantes et al. assessed Latarjet repairs using CT. They found that there is almost complete repair of a 25% to 30% glenoid defect when using the Latarjet procedure.
Figure A comprises comparison Bernageau view glenoid profile radiographs of both shoulders.
Figure B is a 3D reconstruction CT with showing glenoid bone deficiency (inverted pear deformity) with a large bony Bankart lesion. Illustration A shows the method of obtaining a Bernageau glenoid profile view. Illustration B shows the "cliff sign" of anterior glenoid bone loss.
Illustration C depicts the Latarjet procedure. Illustration D depicts reduction in the articular arc with anterior glenoid loss.
Incorrect Answers:
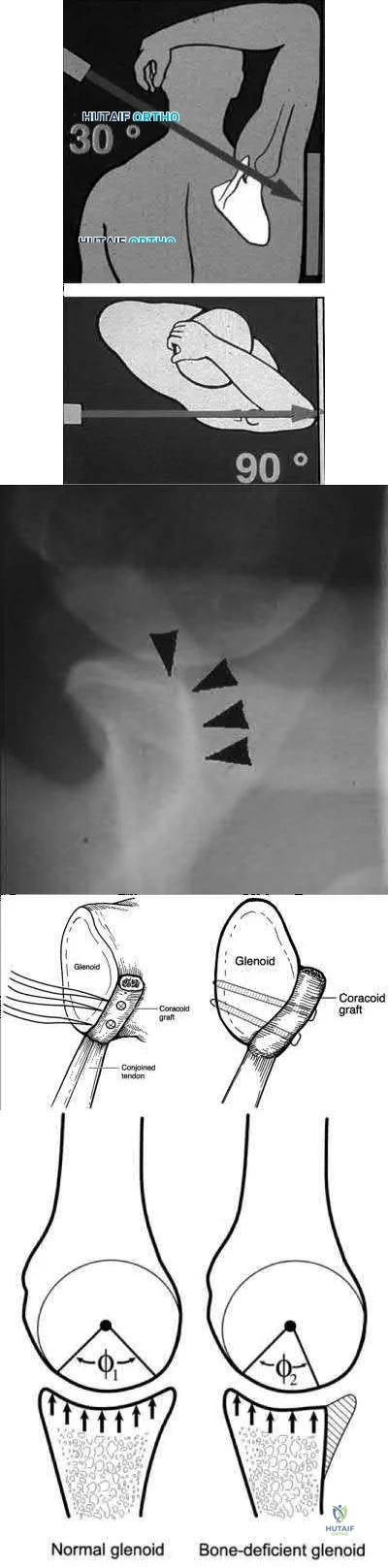
Figure A shows an arthroscopic picture of a 62-year-old male undergoing repair of a torn subscapularis tendon. In the image shown, G represents the glenoid, H represents the humeral head, and the dotted line represents the superolateral border of the subscapularis tendon. Which two ligaments form the structure marked with the asterisk?
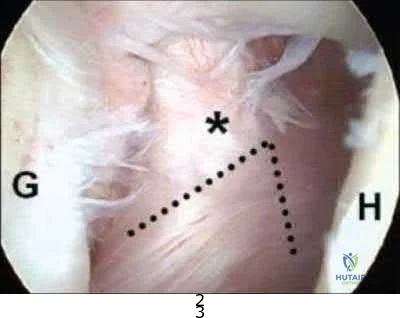
Inferior and middle glenohumeral ligaments Middle and superior glenohumeral ligaments Coracohumeral and coracoacromial ligaments
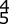
Coracohumeral and superior glenohumeral ligaments Superior and inferior glenohumeral ligaments
The coracohumeral and superior glenohumeral ligaments form a complex that marks the superolateral margin of the subscapularis tendon.
In chronic or degenerative tears, the subscapularis will often retract medially and become scarred to the deltoid fascia. This makes identification difficult during arthroscopic repair. The coracohumeral and superior glenohumeral ligaments form a complex that inserts on the superolateral margin of the subscapularis. This "comma sign" can usually be identified during arthroscopic repair making identification of the subscapularis tendon an easier task.
Burkhart and Brady present surgical pearls for arthroscopic repairs of the subscapularis. Amongst other things, they state the subscapularis is almost always repairable with proper mobilization, but an Achilles tendon allograft or a subcoracoid pectoralis major transfer may be used for a severely degenerated subscapularis.
Lo and Burkhart describe the comma sign for repair of chronic subscapularis tears. They describe how the superior glenohumeral ligament/coracohumeral ligament complex and subscapularis tendon are intimately associated, and often tear off the humerus while remaining attached to each other. This complex, when torn, forms a "comma sign," that marks the superior and lateral margins of the subscapularis tendon.
Illustration A shows why the convergence of the superior glenohumeral and coracohumeral ligaments on the superolateral border of the subscapularis is referred to as the "comma sign." Incorrect Answers:
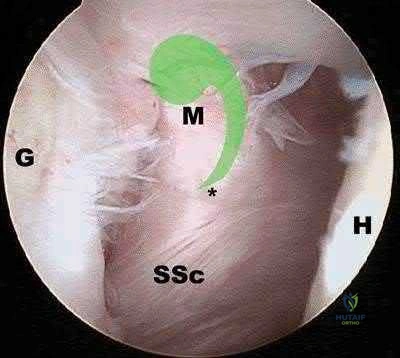
A 52-year-old man sustained the left elbow injury shown in Figure A while playing basketball 2.5 months ago. He underwent the procedure shown in Figure B. Post-operatively he was mobilized in a hinged brace. On examination today, his arc of elbow flexion is 75 degrees with loss of 45 degrees of full extension. His Disabilities of the Arm, Shoulder and Hand (DASH) Outcome Measure score is 45 points. What initial treatment option will likely provide the greatest improvement in this patients DASH score and functional range of motion?
Self-directed exercise therapy Supervised exercise therapy
Supervised exercise therapy with static progressive elbow splinting Continuous passive motion device

Closed manipulation under anesthesia
The clinical presentation is consistent with post-traumatic elbow stiffness following an elbow fracture-dislocation. Supervised exercise therapy with static elbow splinting over a 6 month period
has shown to have a significant improvement on DASH scores and functional range of motion (ROM) in patients with post-traumatic elbow stiffness.
Post-traumatic elbow stiffness is often difficult to manage. The ultimate goal of treatment is to restore a functional range of elbow motion (30° to 130°). Nonoperative modalities are considered the first-line of treatment. Aggressive physical therapy has traditionally been advocated. However, the use of static progressive elbow splinting with a turnbuckle, alongside aggressive physical therapy, has shown to provide better functional outcomes. Treatment is usually maintained over a period of 6-12 months. Surgery is considered when nonoperative therapy fails.
Doornberg et al. looked at a retrospective case series of 29 patients with posttraumatic elbow stiffness. They showed that static progressive splinting can help gain additional motion when standard exercises fail to produce additional improvements.
Lindenhovius et al. randomized sixty-six patients with post-traumatic elbow stiffness into static progressive elbow splint therapy or dynamic elbow splinting over a 12 month period. There was no significant difference in outcomes between treatment modalities. ROM increased by 40° vs. 39° at six months, respectively. DASH scores improved from 50 vs 45 at enrollment to 32 vs. 25 at six months, respectively.
Figure A shows a posterior elbow dislocation with an associated medial epicondyle fracture. Figure B shows ORIF of the fracture seen in Figure A. Illustration A shows a static progressive turnbuckle elbow splint used for posttraumatic elbow stiffness.
Incorrect Answers:
tissues, causing hemarthrosis and additional fibrosis in the joint.
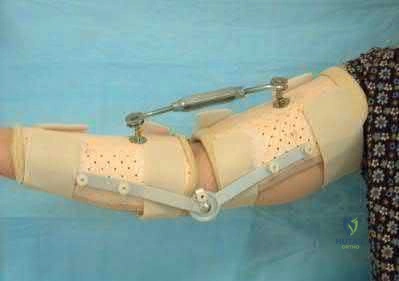
A 25-year-old right-hand baseball pitcher presents with persistent shoulder pain for the past several months in his dominant throwing arm. On physical examination, he is found to have full arc of motion with the exception of an internal rotation deficit of 30 degrees compared to his contralateral side. He is asked to complete the exercise shown in the video in Figure V. This form of rehabilitation is meant to address pathology in which anatomic structure?

Superior glenohumeral ligament Middle glenohumeral ligament
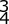
Anterior band of the inferior glenohumeral ligament Superior band of the inferior glenohumeral ligament

Posterior band of the inferior glenohumeral ligament
tissues in patients demonstrating symptoms of internal impingement. The sleeper stretch helps to address posterior tightness and the only posterior structure listed in the responses is the posterior band of the inferior glenohumeral ligament (posterior IGHL).
Internal impingement is a significant cause of pain in throwing athletes. It results from impingement of the articular undersurface of the posterior supraspinatus against the posteriorsuperior glenoid.
This is thought to be secondary to tightness in the posterior soft tissues including the capsule and posterior band of the IGHL. The mainstay of non-operative management is posterior capsular stretching with the sleeper stretches and cross-body adduction stretches. Heyworth et al. review the etiology, diagnosis and management of internal impingement of the shoulder. They note that repetitive contact between greater tuberosity and glenoid rim posterosuperiorly lead to impingement of the posterior rotator cuff and labrum. This occurs when the arm is externally rotated and abducted.
Tyler et al. reviewed the effects of posterior capsular stretching on alleviating symptoms in patients with internal impingement. Twenty-
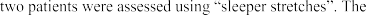
Figure V is a video that demonstrates the sleeper stretch to address tightness of the posterior soft tissues. The arm is forward flexed 90 degrees and the patient lies on his side in order to stabilize the scapula while the arm is internally rotated. Illustration A depicts the sleeper stretch.
Incorrect Answers:
not the focus of the sleeper stretch.
A 28-year-old professional baseball pitcher sustains a complete rupture of his ulnar collateral ligament. He is neurovascularly intact on exam. Which of the following surgical reconstruction techniques has been shown to result in the lowest complication rate and best patient outcome?

Splitting of flexor-pronator mass, figure-of-8 graft fixation. Splitting of flexor-pronator mass, docking graft fixation.
Splitting of flexor-pronator mass, docking graft fixation, ulnar nerve transposition. Detachment of flexor-pronator mass, figure-of-8 graft fixation, ulnar nerve transposition.

Detachment of flexor-pronator mass, docking graft fixation, ulnar nerve transposition.
Ulnar collateral ligament (UCL) reconstruction using a flexor-pronator musclesplitting approach and a docking graft fixation technique are associated with the lowest complication rate and best patient outcomes.
Vitale et al. performed a systematic review of retrospective cohort studies evaluating UCL reconstruction techniques in overhead athletes. They demonstrated that the flexor-pronator musclesplitting approach was associated with better outcomes than detachment of the flexorpronator mass, had a lower rate of postoperative ulnar neuropathy, and a lower overal complication rate. They also found fixation of the graft utilizing the docking technique was associated with better outcomes than the figure-of-8 technique. Abandoning the obligatory ulnar nerve transposition was associated with improved patient outcomes (89% vs. 75%) and a lower rate of postoperative ulnar neuropathy (4% vs. 9%).
Rettig et al performed a case series review of 31 overhead throwing athletes with ulnar collateral ligament injuries managed nonoperatively with 3 months rest followed by rehabilitation exercises. They concluded that 42% of athletes were able to return to their previous level of competition at an average of 6 months from diagnosis (earlier than reconstruction). The authors were unable to identify any patient-specific factors (duration of symptoms, age, acuity of onset) that would predict the success of nonoperative treatment.
Illustration A shows the figure-of-8 (Jobe) graft fixation technique. It is performed by passing the tendon graft through two bone tunnels in the medial epicondyle of the humerus and through one tunnel in the ulnar sublime tubercle. The graft is then sutured to itself in a figure-of-8 configuration. Illustration B shows the docking graft fixation technique. The graft is placed in a triangular configuration through a single humeral tunnel. The suture limbs are then brought out through two separate bone holes and tied over a bony bridge on the superior aspect of the medial epicondyle.
Incorrect Answers:
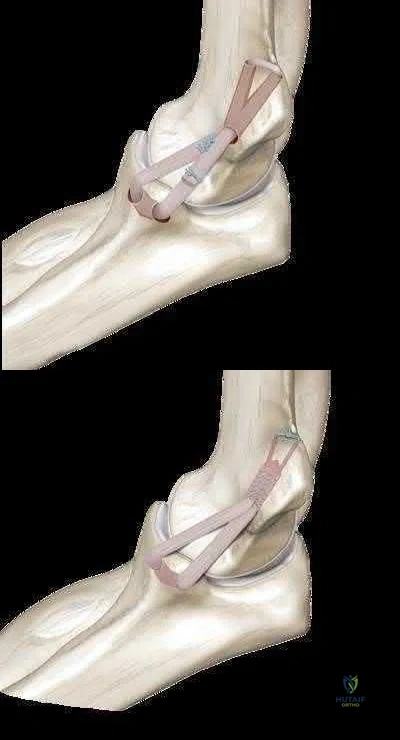
The right shoulder exercise seen in Figure A will put the LEAST amount of stretch on which structure?
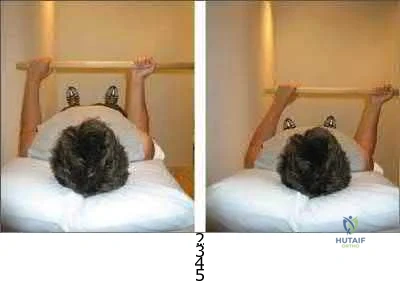
Inferior glenohumeral ligament Coracohumeral ligament Anterior-superior capsule Superior glenohumeral ligament Posterior capsule
Shoulder wand exercises, as shown in Figure A, are used to increase external range of motion of the shoulder. With the arm adducted and the elbow flexed, this exercise will put the LEAST amount of stretch on the posterior capsule.
External rotation shoulder wand exercises are commonly used for the treatment of adhesive capsulitis. Adhesive capsulitis is most commonly caused by contracture of the rotator interval. The rotator interval includes the anterior-superior capsule, superior glenohumeral ligament, coracohumeral ligament and long head biceps tendon. The structure most commonly contracted is the anterior-superior capsule, which limits external rotation when the arm is adducted. Kuhn et al. showed that in the neutral position, each ligament except the posterior capsule significantly affected the torque required for external rotation. The greatest effect on resisting external rotation at 0 degrees of abduction was the entire inferior glenohumeral ligament > coracohumeral ligament
> anterior band of the inferior glenohumeral ligament > superior and middle glenohumeral ligament.
Harryman et al. looked at the role of the rotator interval capsule in passive motion and stability of the shoulder. They found operative alteration of this capsular interval was found to affect flexion, extension, external rotation, and adduction of the humerus with respect to the scapula. Limitation of external motion was increased by operative imbrication of the rotator interval and decreased by sectioning of the rotator interval capsule.
Kim et al. reviewed shoulder MRIs to determine if abnormalities of the rotator interval were correlated with chronic shoulder instability. They found a significantly larger rotator interval height, rotator interval area, and rotator interval index in patients with chronic anterior shoulder instability compared to patients without instability.
Figure A shows a patient performing an exercise to increase right shoulder external rotation with a wand/stick. The right arm is fully adducted by her side, and her elbow flexed at 90 degrees.
Incorrect Answers:
) A 55-year-old male returns for followup 3 months after reverse shoulder arthroplasty. He reports limited function of his right shoulder but no antecedent trauma. A radiograph of his shoulder is shown in Figure A. All of the following variables are associated with this complication EXCEPT:
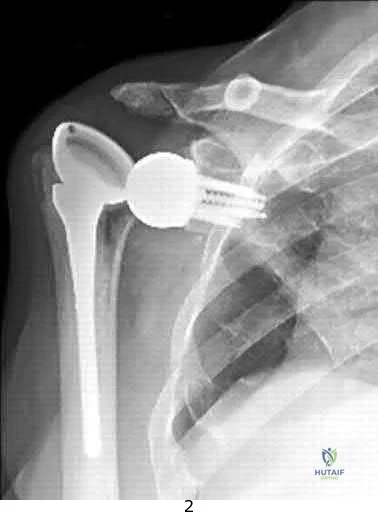
History of malunited proximal humerus fracture Proximal humeral bone loss
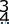
Failed primary arthroplasty Rheumatoid arthritis

Fixed preoperative glenohumeral dislocation
Rheumatoid arthritis is not associated with reverse shoulder arthroplasty (RSA) dislocation. RSA dislocation is a known complication of RSA. Risks include proximal humeral bone loss, chronic fracture sequelae with malunited/ununited tuberosities, failed previous arthroplasty, and fixed glenohumeral dislocation preoperatively. An irreparable subscapularis tears may be less of an issue with newer implant designs.
Trappey et al. studied instability and infection rates after RSA. They found that the rate of instability was similar in primary and revision surgery, but the rate of infection was higher in revision surgery. Instability was highest in the fracture sequelae group because of malunited tuberosities, contractures and proximal humeral bone loss.
Favre et al. examined the effect of component positioning on RSA stability.
They found that humeral version was more important than glenoid version. Stability is improved with the humerus in neutral or slight anterversion. They recommend avoiding retroversion >10deg. Edwards et al. examined subscapularis insufficiency and the risk of RSA dislocation. They found that of 138 RSA, all 7 dislocations occurred in patients with an irreparable subscapularis.
Dislocation was also more likely in patients with complex diagnoses, including proximal humeral nonunion, fixed dislocation, and failed prior arthroplasty.
Figure A shows reverse shoulder arthroplasty dislocation. Incorrect Answers:
) A 45-year-old man complains of chronic right shoulder pain. He has a history of chronic steroid use because of asthma. He recently completed a course of physical therapy
and has given up his job as a laborer in favor of a desk job. Examination reveals diminished shoulder abduction strength. A radiograph of his shoulder is shown in Figure A. Which of the following surgical treatment options (Figures B through F) is the most appropriate?
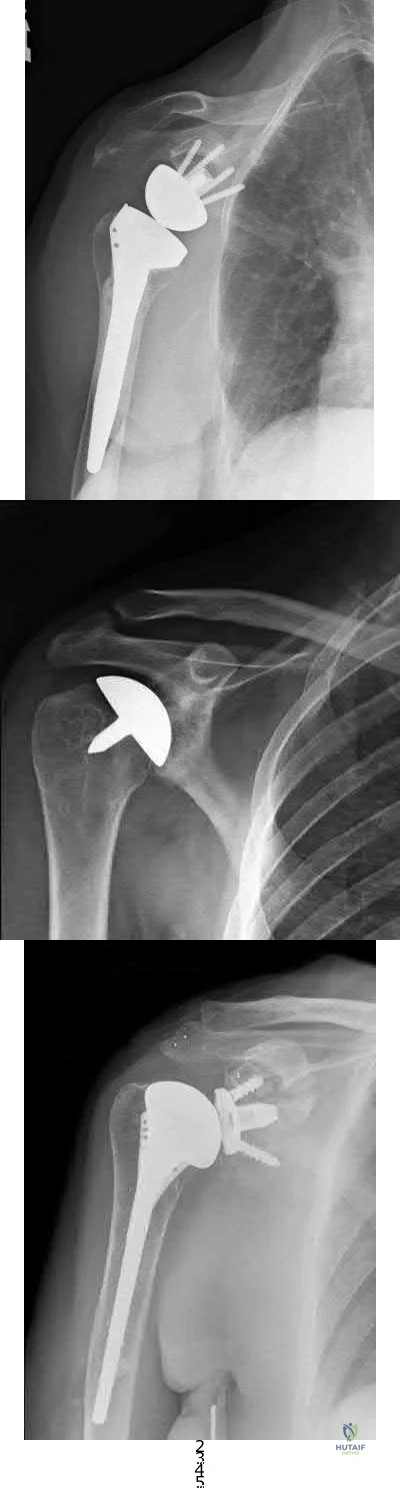
Figure B Figure C Figure D Figure E Figure F
This patient has early stage avascular necrosis (AVN) of the humeral head without subchondral collapse/flattening, likely related to chonic steroid use.
Core decompression is indicated.
Treatment of humeral head AVN is dependent on Cruess Stage. Precollapse stages (Stage I and II) may be treated by core decompression and joint preservation. Hemiarthroplasty is used for Stage III-IV disease. Total shoulder arthroplasty is used for Stage V disease. Resurfacing may be used for Stage III disease with focal chondral defects and sufficient remaining epiphyseal bone stock for fixation.
Harreld et al. reviewed humeral head AVN. They advocate attempting core decompression and arthroscopy for Stage III disease, and then tailoring resurfacing or replacement depending on defect size.
Smith et al. reviewed 31 hemiarthroplasties for steroid-related AVN (6 Stage III, 16 Stage IV, 5 Stage V). Unsatisfactory results were found in 45%. This was associated with glenoid cartilage wear over time. However, they still believed hemiarthroplasty was appropriate for younger active patients with stage III or stage IV disease.
LaPorte et al. performed core decompression for various stages of AVN.
Results were successful in 94%, 88%, 70% and 14% of Ficat-Arlet Stages I, II, III and IV humeral head AVN respectively, and more successful for nonsteroid related cases compared with steroidrelated cases. They recommend this treatment for Stages I-III.
Figure A comprises a radiograph showing Cruess Stage II disease ("snowcap" sign indicating sclerosis, preservation of the head contour and absence of subchondral collapse, left), a T1weighted
MRI (center) and T2-weighted fat saturated MRI (right) showing a variegated pattern of osteonecrosis, but with preservation of normal head contour. Figure B shows core decompression. Figure C shows hemiarthroplasty. Figure D shows reverse shoulder arthroplasty. Figure E shows resurfacing. Figure F shows total shoulder arthroplasty. Illustration A depicts the Cruess staging system. Illustration B shows a possible algorithm for management where they use the Ficat stages adapted from the hip.
Incorrect Answers:
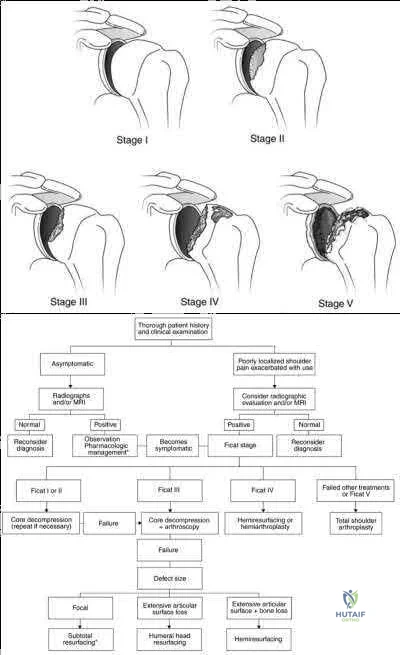
A 56-year-old otherwise healthy woman undergoes uncomplicated arthroscopic repair of a full-thickness rotator cuff tear. Prior to the procedure, the patient had attempted a long,
protracted course of physical therapy in an attempt to regain function without surgery. At her 10 day post-operative visit, she tearfully informs you that she cannot see her physical therapist because she has used up her 24-visit allotment for the year. She has 4 more weeks
until her insurance year turns over, and she does not have the financial means to pay out of pocket. What is the best next course of action?
Request a peer-to-peer review for authorization of additional visits or else the patient is likely to have a poor result

Provide a brief explanation and sheet of exercises for periscapular and cuff strengthening exercises using a resistance band
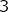
Test her range of motion and strength, and if limited, have her return weekly to your clinic for a guided home rehabilitation program

Explain to her that seeing a physical therapist during the first 6 weeks following cuff repair will not affect her range of motion one year removed from surgery

Give her a prophylactic corticosteroid injection to avoid early post-operative adhesive capsulitis
Early motion following rotator cuff repair has not been shown to impact range of motion and stiffness at one year post-operative clinical examinations.
Stiffness is a complication of protecting rotator cuff repairs from early re-tear with sling immobilization. However, with sling immobilization of up to 6 weeks, there is evidence of no increase in long-term stiffness. Accordingly, supervised physical therapy is not required in the first 6 weeks following arthroscopic rotator cuff repairs in order to obtain a good result.
Parsons et al. retrospectively reviewed 43 patients with full-thickness cuff tears who underwent a conservative early-postoperative protocol involving sling immobilization for 6 weeks with no formal therapy during that time. 10 /43 patient were characterized as stiff at their 6-week postoperative visit. At one year, there was no difference in the range of motion of the early stiff group compared to the non-stiff group.
Trenerry et al. collected prospective data on 209 consecutive patients undergoing primary rotator cuff repair. They found that patients in the stiffest quartile of range of motion testing at 6 weeks progressively regained range of motion by a post-operative visit at 72 weeks. The predictor of slowest recovery of early post-operative stiffness was found to be an internal rotation deficit with the patient reaching behind his or her back.
Incorrect Answers:
1: Early supervised physical therapy has not been shown to be essential to obtaining good motion post-operatively.
2 and 3: Strength testing and home strengthening programs in the early postoperative period would put the repair at risk for early failure.
5: Prophylactic corticosteroids are not indicated for prevention of postoperative stiffness, and furthermore, could theoretically interfere with healing.
A 62-year-old woman presents with chronic shoulder pain. On physical exam, she has anterior shoulder pain and her symptoms are reproduced with provocative testing of the biceps including supination against resistance and forward flexion of the shoulder against resistance. Internal and external rotation are painful, but her range of motion is intact. Shoulder radiograph and MRI images are shown in Figures A-E. Which of the following statements is true regarding the patient's condition?
Her clinical examination is most consistent with a SLAP tear, which should be repaired. Her biceps pathology is due to her partial tearing of her subscapularis

She has isolated degenerative biceps tendonosis and an injection may cure her symptoms

She has end-stage rotator cuff arthropathy and should consider a reverse total shoulder arthroplasty

Her subacromial impingement is causing her biceps tendon sheath to be inflamed
The subscapularis tendon is the most important medial restraint to subluxation or dislocation of the long head of the biceps tendon (LHBT).
Anterior shoulder pain and positive provocative biceps clinical examination tests are common in patients with concomitant rotator cuff pathology. A consequence of subscapularis tendon tears -even partial tears - is that the LHBT can subluxate medially out of the intertubercular groove, as the subscapularis tendon is the most important restraint to medial instability of the LHBT. This instability can cause both pain and inflammation around the biceps tendon, leading to pain with resisted supination (Yergason's test) or resisted forward flexion (Speeds' test).
Walch et al. wrote a case series on 71 cases of biceps tendon instability. They found that dislocated LHBTs were associated with partial or complete subscapularis tears in 96% of cases.
Maier et al. published clinical results of treating acute traumatic medial LHBT instability with open repair of the subscapularis tendon and stabilization of the LHBT. They showed equivalent functional clinical outcomes to biceps tenotomy or tenodesis, with improved cosmesis and decreased muscle cramping.
Figures A and B show Grashey and axillary lateral views of the patient and demonstrate an os acromiale. Figures C, D, and E are axillary T2 MRI images. Figure C shows the tendon of the long head of the biceps in the distal aspect of the biceps grove. Moving proximally, Figure D shows the tendon subluxated onto the lesser tubercle and Figure E shows it fully dislocated medially.
Incorrect Answers:
A 78-year-old male presents to clinic 4 weeks after left total shoulder arthroplasty. He has not been wearing his sling and reports that he developed increased pain after slipping in the shower. He used the arm to catch himself from falling. On examination, he can flex the shoulder to 70 degrees, limited by pain. Active external rotation with arm at the side is 50 degrees and active internal rotation is 5 degrees. Passive external rotation is to 80 degrees. A radiograph of the left shoulder is shown below in Figure A. What other complaint is the patient most likely to have?
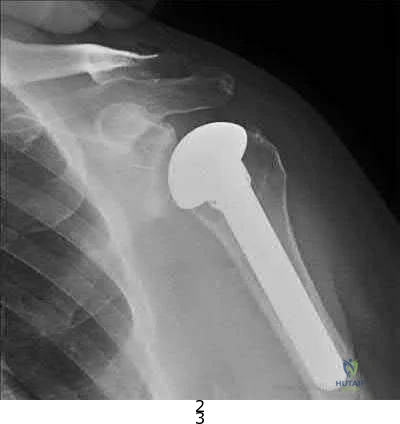
Pain with palpation of the bicipital groove Pain with palpation over the subdeltoid bursa Sensory loss over the lateral shoulder
Sensation of shoulder instability with external rotation Sensation of shoulder instability with internal rotation
The clinical presentation is consistent with a tear of the subscapularis, which is a well-described complication after total shoulder arthroplasty. The most likely additional complaint this patient will have is anterior shoulder instability, noticeable with external rotation of the shoulder.
Total shoulder arthroplasty is the preferred treatment for glenohumeral arthritis in patients with intact rotator cuff and good glenoid bone stock. The surgical approach involves detaching the subscapularis and capsule from the anterior humerus and dislocating the humeral head anteriorly. Post operatively, external rotation is limited to protect the subscapularis repair. If there is suspicion of a postoperative subscapularis tear, and ultrasound can be performed to confirm the diagnosis.
Miller et al. reported 7 cases of subscapularis tendon rupture after total shoulder arthroplasty, all of which were subsequently repaired. Decreased functional outcomes were observed in these patients, with lengthening techniques to address internal rotation contractures and prior surgery involving the subscapularis tendon as risk factors for rupture
Westoff et al. performed static and dynamic ultrasounds on 22 patients after total shoulder arthroplasty evaluating for numerous periarticular pathologies. The authors concluded that sonography is a useful tool for evaluation of periimplant tissues after TSA.
Figure A shows an intact left total shoulder arthroplasty without evidence of fracture, dislocation, or hardware loosening. Illustration A shows the incision for the subscapularis tendon during TSA. Incorrect Answers:
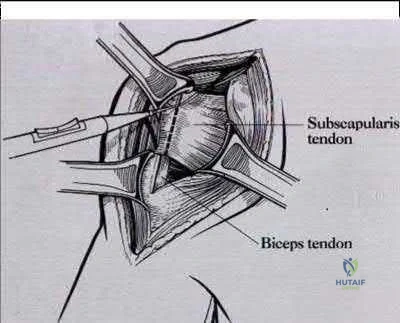
A 25-year-old lineman is referred to your office for a second opinion. 1 year ago, he underwent an arthroscopic procedure for shoulder instability. He complains of persistent sense of instability despite the surgery. Which of the following is a contraindication to revision arthroscopic labral repair for recurrent anterior glenohumeral instability?
Glenoid bone loss of 10%
Capsular attenuation from prior thermal capsulorraphy Anterior labral periosteal sleeve avulsion (ALSPA ) lesion Glenoid labral articular defect (GLAD) lesion

Combined Superior Labrum from Anterior to Posterior tear (SLAP) and recurrent Bankart lesion
Capsular attenuation or postthermal capsular necrosis from prior thermal capsulorraphy is a contraindicated to arthroscopic repair.
Thermal capsulorrhaphy utilizes heat generated by radiofrequency or laser ablation to cause capsular shrinkage in an effort to treat shoulder instability. However, high recurrence rates have been found, especially around two to three weeks after the index procedure, when the capsular tissue is the weakest. In the setting of recurrence following thermal capsulorrhaphy, open revision is recommended.
Creighton et al. reported on a series of 18 patients undergoing revision arthroscopic stabilization. Of the 18, 3 failed with recurrent instability, all with previous thermal capsulorrhaphy. Miniaci et al. reviewed the outcomes following thermal capsulorrhaphy noting high rates of recurrent instability, especially in the setting of initial treatment for multidirectional instability. Park et
al. reported on a series of 14 patients undergoing revision following thermal capsulorrhaphy. Ten out of 14 patients had signs of capsular thinning, insufficiency and attenuation.
Wong et al. surveyed 379 shoulder surgeons on the complications following thermal capsulorrhaphy. Capsular insufficiency and thinning were commonly associated with recurrent instability.
Hecht et al. performed thermal capsulorrhaphy and biomechanical analysis of the capsule in a sheep model. The authors found that the capsule was weakest at the 2-3 week post-operative timepoint, leading to the highest rate insufficiency, attenuation and mechanical failure at this time.
Incorrect answers:
A 47-year-old landscaper presents with worsening left shoulder pain and weakness. Three years ago, he injured the left shoulder in a fall and elected for nonoperative
management to minimize time off from work. Physical therapy was effective until 6 months ago when his shoulder function worsened to the point that he is now unable to work.
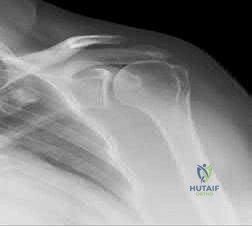
Examination of his active range of motion reveals forward elevation 120° with pain, abduction 100°, IR at neutral to T8 and ER at neutral 5°. He has a positive ER lag sign and Hornblower's sign. Belly press and lift-off tests are normal. A recent radiograph is shown in Figures A. MRI images are shown in Figures B and C. Which of the following is the best treatment option?
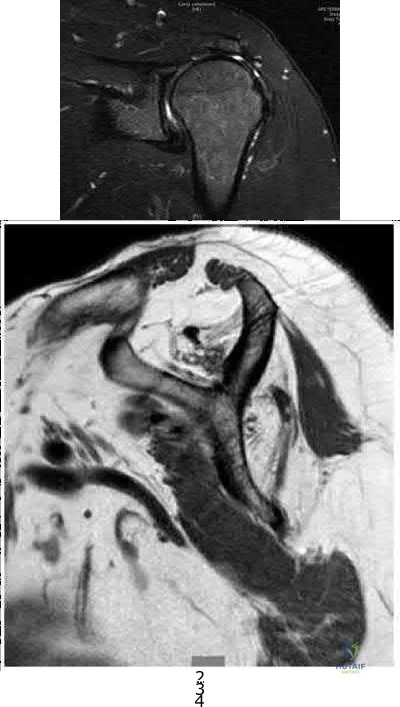
Continue physical therapy Latissimus dorsi transfer Arthroscopic rotator cuff repair Pectoralis major transfer

Reverse total shoulder arthroplasty
This patient has a chronic massive posterosuperior rotator cuff tear with marked atrophy, tendon retraction and loss of external rotation strength that is impacting his daily life. The best treatment option for this middle-aged laborer with an irreparable posterosuperior rotator cuff tear is a latissimus dorsi transfer to restore external rotation strength and motion.
Irreparable rotator cuff tears are marked by: (1) Superior displacement of the humeral head (AHI < 5-7mm), (2) Fatty infiltration of the rotator cuff muscles ( Goutallier stage 3-4), (3) Increased duration of the tendon tear and (4) Profound external rotation weakness. These findings are predictive of poorquality tissue and stiffness of the muscle-tendon unit, not amenable to primary repair. In this setting, a latissimus dorsi transfer can be utilized to restore shoulder strength, function and improve pain. Relative contraindications include subscapularis deficiency, deltoid deficiency, pseudoparalysis of the shoulder and advanced glenohumeral arthritis.
Gerber et al. performed a case series analysis of 67 patients with irreparable rotator cuff tears managed with latissimus dorsi transfer. Patients with an intact subscapularis demonstrated improvement in pain, range of motion and strength postoperatively, while no improvement was noted in patients with subscapularis deficiency. The authors conclude that latissimus dorsi transfer should not be performed in the setting of poor subscapularis function.
Iannotti et al. found that better clinical results following latissimus dorsi transfer were associated with: preserved active shoulder range of motion and strength (specifically forward elevation > 90° and external rotation > 20°), synchronous firing of the transferred latissimus dorsi muscle and male gender.
Figure A is an AP radiograph of the left shoulder with superior migration of the humeral head (AHI
< 5mm) and no evidence of glenohumeral arthritis. Figures B and C show a retracted posterosuperior rotator cuff tear and Goutallier stage 4 atrophy (more fat than muscle) of the supraspinatus, infraspinatus and teres minor, rendering this tear irreparable. Illustration A shows a latissimus dorsi transfer. The latissimus dorsi tendon is positioned over the top of the humeral head, covering most of the rotator cuff defect. The tendon is then secured to the subscapularis tendon edge and lesser tuberosity anteriorly, the remnant supraspinatus and infraspinatus tendons medially, and the greater tuberosity laterally.
Incorrect Answers:
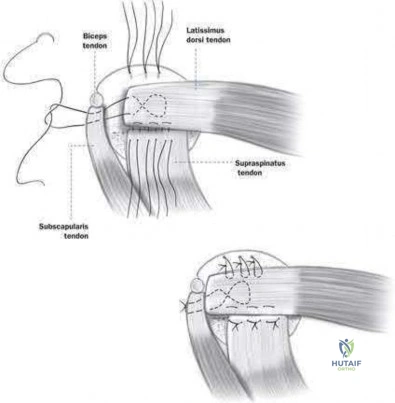
A collegiate swimmer develops medial winging of the scapula. If the EMG and nerve conduction studies are abnormal, the most likely nerve roots to be involved are?
C7, C8, T 1 C6, C7, C 8 C5, C6, C 7 C4, C5, C 6 C3, C4, C 5
Classic medial winging of the scapula is due to paralysis of the serratus anterior muscle which is supplied by the long thoracic nerve which holds the scapula to the chest wall and prevents the inferior angle of the scapula from migrating medially. It is innervated by the long thoracic nerve (C5, 6, 7).
Surgical treatment may include partial pec major transfer. Lateral winging may be caused by spinal accessory nerve palsy (CN XI, also ventral ramus C2,3,4). The nerve may be injured during neck surgery. This causes trapezius weakness, allowing the inferior pole of the scapula to migrate laterally. The modified Eden-Lange procedure may be used for this type of winging.
Gregg et al. describes paralysis of the serratus muscle in young athletes which they felt was due to repetitive traction. Full recovery usually occurs in an average of 9 months, and they recommend that surgical methods of treatment should be reserved for patients in whom function fails to return after a twoyear period.
Foo et al. describes a larger cohort of 20 patients again treated expectantly with observation and physical therapy. They reported consistent recovery but that it can take up to 2 years.
Illustration A shows a clinical photo of medial scapular winging. Illustration V is an instructional video of scapular winging. It begins with a clinical video of the condition.
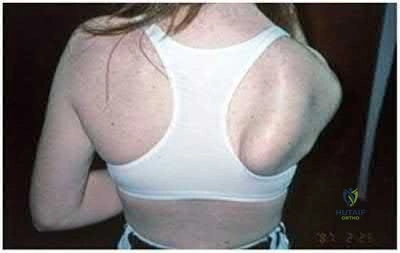
A 62-year-old man complains of shoulder pain for 2 years. He has had 1 course of intra articular sodium hyaluronate and 6 weeks of physical therapy with little relief. Examination reveals diminished arm flexion and abduction secondary to pain. Radiographs of his shoulder are shown in Figures A and B. According to the American Academy of Orthopaedic Surgeons Clinical Practice Guidelines, what is the next best step?
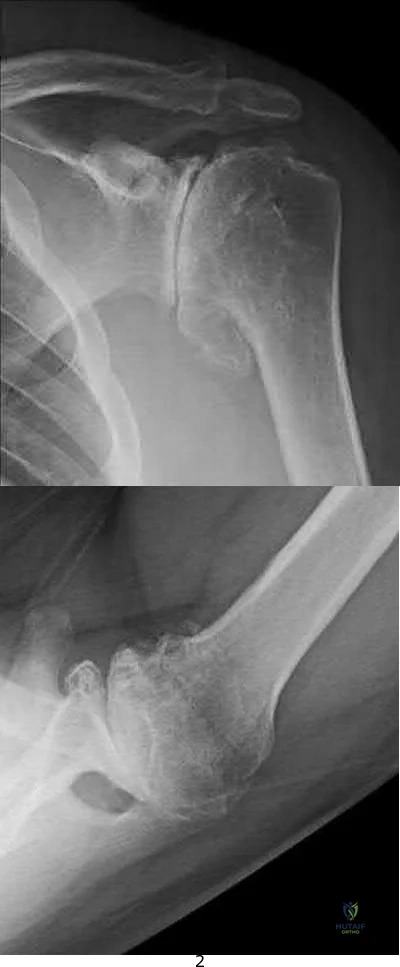
Humeral head replacement arthroplasty Hemiarthroplasty and ream-and-run glenoid procedure

Cuff tear arthropathy (CTA) prosthesis
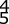
Total shoulder arthroplasty with a metal-backed cemented glenoid component Total shoulder arthroplasty with an all-polyethylene cemented glenoid component
This patient has end-stage glenohumeral osteoarthritis (GH OA). According to the AAOS CPG, total shoulder arthroplasty (TSA) is recommended using an allpolyethylene cemented glenoid component.
TSA is indicated for cases of end-stage GH OA. It is preferred to hemiarthroplasty. It is contraindicated in cases with insufficient glenoid bone stock (glenoid wear to the level of the coracoid), rotator cuff arthropathy or irreparable cuff tears and deltoid dysfunction. It provides good pain relief and has good survival at 10 years (>90%).
Radnay et al. performed a systematic review involving 1952 patients comparing TSA with humeral head replacement (HHR). They found that TSR provided greater pain relief, range of motion, patient satisfaction, and had lower revision rates. They recommend TSA over HHR for GH OA. Izquierdo et al. described the AAOS Clinical Practice Guidelines (CPG) regarding treatment of GH OA. This is summarized in Illustration A.
Figures A and B show end-stage GH OA with large osteophytes and subchondral sclerosis. There is significant glenoid wear and posterior subluxation (Walch B glenoid deformity). Illustration A is a table summarizing the AAOS CPG on treatment of GH OA. Illustration B shows a CTA humeral component. It is not paired with a glenoid component.
Incorrect Answers:
Metal-backed glenoids have higher rates of revision than all-polyethylene glenoids.
Posterior glenohumeral dislocations are as common as anterior dislocations in which of the following patient groups?
Football players
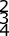
Marfan's syndrome patients Renal failure patients Epilepsy patients

Women
Millett et al and Robinson et al provide review articles on posterior shoulder dislocations, which are rare clinical entities that occur during seizures and electrocution (due to tetanic muscle contraction) or as a result of high energy trauma. Robinson et al noted that poor prognostic factors associated with posterior shoulder dislocation include late diagnosis, large bony defect of humeral head, associated proximal humerus fracture, and need for arthroplasty. In Gerber's series, posterior dislocations occurred with equal frequency to anterior in a cohort of epilepsy patients.
What nerve is injured most commonly during the superficial dissection when repairing a distal biceps rupture through a single incision anterior approach?

Medial antebrachial cutaneous nerve Lateral antebrachial cutaneous nerve Superficial radial nerve

Ulnar nerve

Posterior interosseous nerve
The lateral antebrachial cutaneous nerve (LABCN) is at risk during the superficial dissection when repairing a distal biceps rupture through a single incision anterior approach.
The LABCN is the terminal cutaneous branch of the musculocutaneous nerve, which supplies sensation to the volar-lateral aspect of the forearm. The LABCN pierces the deep fascia of the arm lateral to the musculotendinous junction of the distal biceps tendon after lying on top or piercing through the brachialis muscle. It exits the arm and lies in the subcutaneous tissues of the antecubital fossa. It is important to retract this nerve laterally during the approach to the distal biceps tendon.
Cohen describes the importance of identifying the LABCN during the superficial dissection as injury to this nerve is not uncommon (5-7%). Injury to the PIN (5 %) is devastating and occurs with retractor placement during the deep dissection and the use of suspensory fixation on the posterior cortex of the radius.
The review article by Ramsey et al covers the surgical anatomy and complications of biceps surgery, including injury to the LABCN.
Illustration A shows the LABCN relative to the anterolateral approach to the elbow which is commonly used to repair distal biceps avulsions. Illustration B shows the close proximity of the LABCN to the distal biceps in a human specimen.
Incorrect Responses:
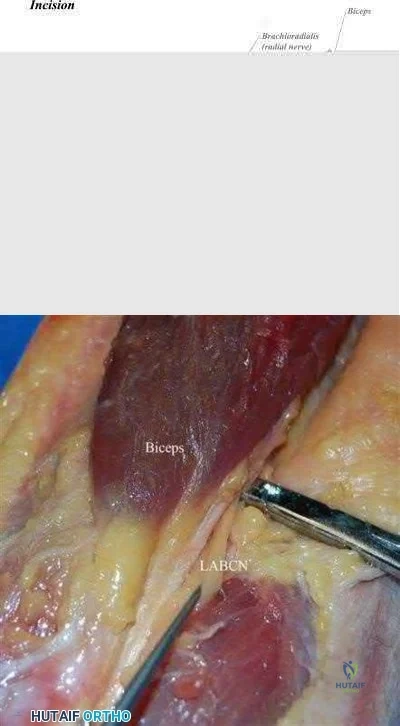
An MRI of the shoulder in a patient with chronic quadrilateral space syndrome is most likely to show which of the following?
Increased intra-capsular volume Loss of intra-capsular volume Fatty atrophy of the infraspinatus Fatty atrophy of the teres minor

Fatty atrophy of the latissimus dorsi
Quadrilateral space syndrome involves dysfunction of the axillary nerve, perhaps by entrapment or compression, resulting in the functional denervation of the teres minor.
The quadrilateral space is a potential space formed by the long head of the triceps medially, the humerus laterally, the teres minor above, and the teres major below. The axillary nerve and posterior circumflex humeral artery travel through this space.
The Sanders article describes the MRI appearance, which is that the muscle appears streaked with white on MRI and atrophied (See illustration A) consistent with fatty atrophy. Sanders group report this finding in 3% of shoulder MRIs. The posterior circumflex humeral artery also travels with the axillary nerve as it travels through this space. Loss of capsular volume on an arthrogram study is suggestive of adhesive capsulitis.
Illustration B is a diagram which shows the borders of the quadrilateral (or quadrangular) space.
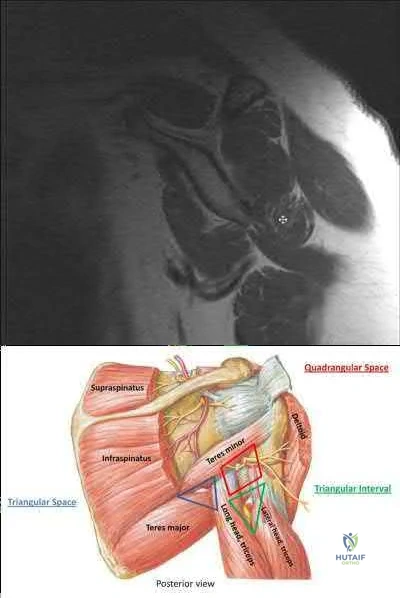
A 21-year-old collegiate volleyball player is noted to have weakness in external rotation and isolated atrophy of the infraspinatus on physical examination as seen in Figure A. An axial MRI image is shown in Figure B. This clinical condition is most likely caused by compression of the:
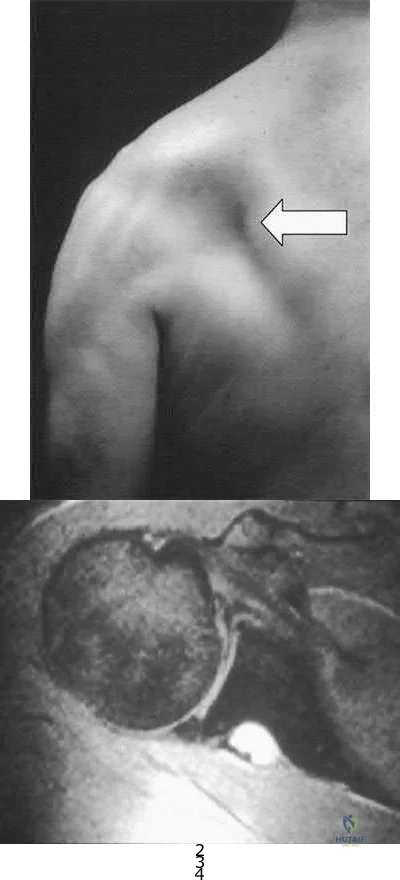
Axillary nerve at the triangular space Suprascapular nerve in the suprascapular notch Axillary nerve in the quadrangular space Suprascapular nerve in the spinoglenoid notch

Long thoracic nerve anterior to the scalenus and the first rib and posterior to the clavicle
The clinical presentation is consistent for a suprascapular neuropathy caused by compression of the suprascapular nerve by a cyst in the spinoglenoid notch.
The suprascapular nerve arises from the upper trunk of the brachial plexus with contributions from C5-6. It travels through the suprascapular notch of the scapula where it gives motor branches to the supraspinatus then around the spinoglenoid notch where it innervates the infraspinatus.
Compression of the nerve at the suprascapular notch will cause denervation and atrophy of both the supraspinatus and infraspinatus while compression at the spinoglenoid notch affects the infraspinatus in isolation. This is commonly seen in overhead athletes who sustain a SLAP tear and resultant spinoglenoid notch cyst as seen in the MRI. This will cause weakness and atrophy of the infraspinatus and can be noted both clinically and radiographically. Appropriate operative management is still not clear in the literature with some authors reporting a need for labral repair + cyst decompression and others reporting good outcomes with labral repair alone. Other cases have been treated with needle aspiration.
The cited reference by Cummins et al reviews the various causes, diagnosis, and treatment of suprascapular neuropathy.
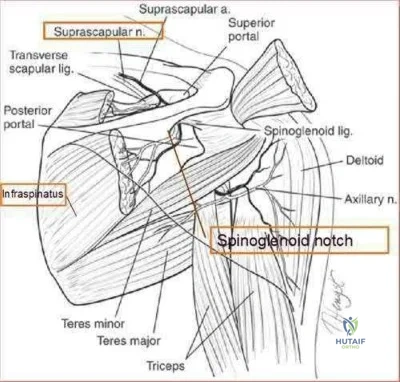
The reference by Martin et al is a retrospective study of the results of nonoperative treatment of suprascapular neuropathy in which 5 had excellent results and 7 had good results.
Which of the following provocative tests would most likely be positive in a patient with medial epicondylitis?

Resisted forearm pronation and wrist flexion with a clenched fist Resisted forearm supination and wrist extension with a clenched fist Dynamic valgus stress test
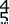
Milking maneuver Pinch grip test
A provocative test for medial epicondylitis can be elicited by applying resistance to a patient with their fist clenched, wrist flexed and pronated.
Medial epicondylitis is an overuse syndrome of the flexor-pronator mass. The pronator teres (PT) and flexor carpi radialis (FCR) are thought to be most affected with this condition. It is most common in the dominant arm and occurs with activities that require repetitive wrist flexion/forearm pronation. Patients are most tender over the origin of PT and FCR at the medial epicondyle.
Resisting a patient with their fist clenched, wrist flexed and pronated can cause worsening of their pain. This maneuver can be used as a provocative test for this condition.
Cain et al. reviewed elbow injuries in throwing athletes. They comment that the common flexorpronator muscle origin provides dynamic support to valgus stress in the throwing elbow, especially during early arm acceleration and help produce wrist flexion during ball release.
Amin et al. reviewed the evaluation and management of medial epicondylitis. They report that medial epicondylitis typically occurs in the fourth through sixth decades of life, the peak working years, and equally affects men and women. Physical therapy and rehabilitation is the main aspect of recovery from medial epicondylitis, once acute symptoms have been alleviated.
Illustration A shows a video of this provocative test for medial epicondylitis. Incorrect Answers:
A 72-year-old woman presents for follow-up after elbow surgery. Her radiographs are shown in Figures A and B. Which of the following pre-operative diagnoses is a relative contraindication to the use of this prosthesis design?

Acute intra-articular distal humerus fracture Malunited intra-articular distal humerus fracture Late-stage rheumatoid arthritis
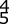
Post-traumatic bony ankylosis Osteoarthritis
This patient has had an unconstrained total elbow arthroplasty (TEA).
Unconstrained TEA is least preferred for late-stage rheumatoid arthritis where there is significant capsuloligamentous instability and bony erosion.
Unconstrained (unlinked or resurfacing prosthesis) TEA depend on intact bony and ligamentous constraints for stability. These are appropriate for humeroulnar conditions with intact collateral ligaments and radiocapitellar articulation e.g. osteoarthritis, post-traumatic arthritis, intra-articular distal humerus fracture, and malunion of the distal humerus. Conditions with increased risk of
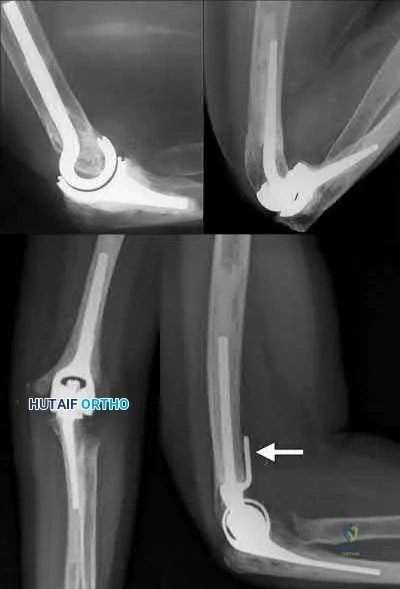
instability (ligamentous injury, rheumatoid arthritis) will benefit from a linked or semiconstrained prosthesis.
Mansat et al. reviewed the Coonrad-Morrey linked (semi-constrained) TEA implant in 70 patients after 5 years. They found that patients with inflammatory arthritis had higher function than those with traumatic conditions
( fractures, nonunions and post-traumatic arthritis). Survival rate was 98% and 91 % at 5 and 10 years, respectively. They concluded that this implant provided satisfactory treatment for different indications although radiolucent lines and bushing wear were a concern.
Hildebrand et al. reviewed the functional outcome of the Coonrad-Moorey prosthesis in 51 elbows after 50 months. The inflammatory arthritis group had higher performance scores than the traumatic/post-traumatic conditions group. Isometric extensor torque was found to be less than the nonoperated side. Radiolucency was noted in 11 elbows.
Figures A and B show an unconstrained TEA with radial head replacement. Illustration A shows more examples of unconstrained TEA. Illustration B shows a semiconstrained TEA. The arrow points to the anterior flange. Illustration C shows radiolucent lines around the stems. Illustration D shows severe bushing wear leading to locking mechanism failure. Illustration E is a table comparing linked and unlinked implants.
Incorrect Answers:
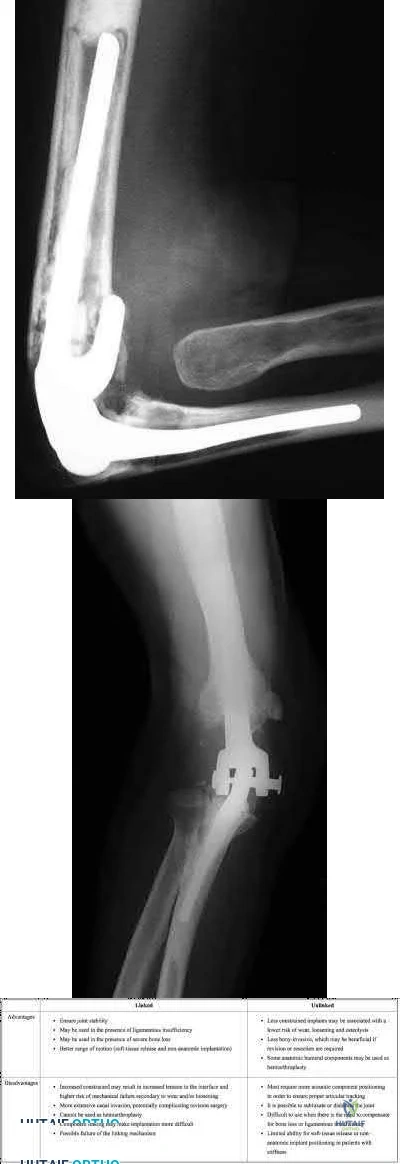
A professional baseball team has several pitchers with complaints of velocity loss with their pitches and shoulder pain of their dominant shoulders during spring training. Pitch counts are properly monitored. The average glenohumeral internal rotation deficit on the pitching staff is 45 degrees. The best intervention would be:
Pitchers throwing less fastballs and more changeups
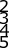
Evaluate the pitchers elbows for ulnar collateral ligament acute ruptures. Increasing the weight training for the deltoid and latissimus dorsi muscles Focused stretches and therapies that address posterior capsular tightness Firing the general manager for finding pitchers that "lose their stuff"
Glenohumeral Internal Rotation Deficit (GIRD) is a phenomenon that occurs in baseball pitchers and is due to posterior capsular tightness. Treatment should begin with a therapy program addressing the pathologic posterior capsule.
GIRD is a phenomenon that is frequently found in high-level overhead throwing athletes, predominantly baseball pitchers. It is defined as the measured difference in internal rotation between the non-dominant arm and dominant arm. Worsening range of motion deficits are seen with increased repetitions, both over a single season and a career. GIRD > 25º is associated with development of shoulder pathologies or pain requiring periods of inactivity. Cessation of overhead throwing activities and initiation of a stretching program to address posterior capsular contractures is largely effective (90% in some series).
Burkhart et al. reviewed the conditions associated with high-level overhead throwing athletes shoulders, culminating in a theory of pathologic progression to "dead arm syndrome" (loss of velocity and effective pitching). Their theory attributes adaptive hyperexternal rotation (occurs during late-cocking / early acceleration phases of pitching) to lead to posterior-inferior capsular contracture and GIRD. Subsequent injuries to anterior structures - including SLAP lesions - would then occur.
Illustration A is a cartoon depiction of how to perform the sleeper stretch. This is a common component of a pitcher's maintenance stretching program.
Incorrect Answers:
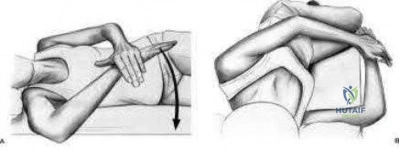
A 68-year-old man presents with severe right shoulder pain. He had a prolonged course of physical therapy and received several cortisone injections for his pain without improvement. Examination reveals pseudoparalysis of the right shoulder with a 20-degree external rotation lag with the shoulder adducted. With the shoulder placed in 90 degrees of abduction, he can actively externally rotate his shoulder. The patient was treated with a medialized reverse prosthesis shown in Figure A. Which of the following statement is true regarding this treatment option?
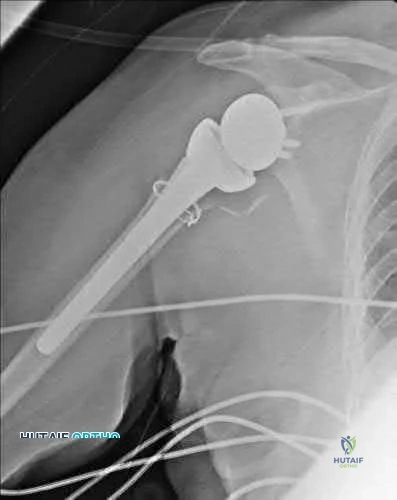
It is contraindicated in patients with shoulder pseudoparalysis

It can be used in patients with deltoid dysfunction when combined with latissimus dorsi transfer It shifts the center of rotation of the shoulder superior and lateral
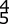
The risk of scapular notching is increased with inferior placement of the glenoid component The risk of instability is increased with an irreparable subscapularis
The clinical presentation is consistent with a patient with pseudoparalysis that was treated with a reverse total shoulder arthroplasty (RTSA). The risk of postoperative instability is increased in patients with an irrepairable subscapularis when a medialized reverse prosthesis is used. Answers 1-4 are false statements.
RTSA is most commonly indicated for rotator cuff arthropathy. However, indications for use now include shoulder pseudoparalysis, anterosuperior escape of the humeral head, acute 3 or 4-part proximal humerus fractures, and greater tuberosity fracture nonunions. Contraindications to RTSA included deltoid dysfunction, insufficient glenoid bone stock, and bony deficiency of the acromion. Edwards et al. prospectively evaluated the risk of shoulder dislocation after reverse TSA. They found a significantly increased risk of dislocation (p=0.012) in patients with an irreparable subscapularis at time of surgery. There were no dislocations in the reparable group. Dislocations were more likely in patients with proximal humeral nonunions and failed prior arthroplasty. Mulieri et al. looked at the use of reverse TSA in patients with irreparable massive rotator cuff tears without evidence of glenohumeral arthritis. All outcomes were improved postoperatively, and they advocate
for reverse TSA in this subset of patients. Survivorship was over 90% at more than 4 years average follow up.
Boileau et al. evaluated the clinical outcomes of isolated biceps tenotomy/tenodesis in patients with massive rotator cuff tears and a biceps lesion. They found that the procedure can effectively treat pain and improve function in these patients. There was no difference in patients undergoing tenotomy versus tenodesis.
Figure A is a right shoulder radiograph status post RTSA with components in adequate position. Incorrect Answers:
Figure A shows immediate post-operative radiographs of a 75year-old patient with primary osteoarthritis. She presents 3 years later with increasing pain and weakness in the shoulder despite home physical therapy. Examination reveals limited active range of motion, with forward elevation of 80 degrees and external rotation of 50 degrees. Her deltoid function is intact. Repeat radiographs are seen in Figure B. Which treatment option would provide the best functional outcome for this patient?
Open tendon transfer
Corticosteriod injection and supervised physical therapy
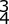
Open rotator cuff repair, subacromial decompression and distal clavical excision Revision to reverse shoulder arthroplasty

Revision to cuff arthropathy hemiarthroplasty
This patient presents with failed total shoulder arthroplasty. The best treatment option for functional outcome would be revision to reverse shoulder arthroplasty (rTSA).
RTSA is considered a viable treatment option for patients with failed shoulder arthroplasty. It allows for improved arm elevation and abduction in the setting of nonfunctional rotator cuff muscles, as seen in this example. Despite the expanding indications for rTSA, there are high complication rates in the revision setting. Complication rates for rTSA after failed shoulder arthroplasty have been reported to be between 11-36%. This procedure should, therefore, be performed by surgeons with extensive training in reconstructive shoulder arthroplasty.
Patel et al. retrospectively reviewed 31 patients (mean age, 68.7 years) who underwent rTSA for treatment of a failed shoulder arthroplasty. They found the greatest improvement with active forward elevation from 44° preoperatively to 108 ° postoperatively (P < .001). Complications occurred in 3 patients with periprosthetic fracture.
Hattrup et al. reviewed a series of 19 patients that underwent open rotator cuff repair after shoulder arthroplasty. Out of the 19 patients only 4 shoulders were successfully repaired. They concluded that successful rotator cuff repair after shoulder arthroplasty is possible but failure is more common. Figure A shows a left total shoulder arthroplasty that is well reduced in the glenoid. Figure B shows antero-superior escape of the prosthesis, indicative of a massive rotator cuff tear.
Incorrect Answers:
A 35-year-old man awoke following a night of heavy drinking with severe right shoulder pain and inability to raise his arm above his head. A radiograph from the emergency room is provided in Figure A. He was treated with a sling for a diagnosis of rotator cuff tear. Six weeks later, he complains of continued pain and difficulty using the arm. Which of the following is the next best step in management?
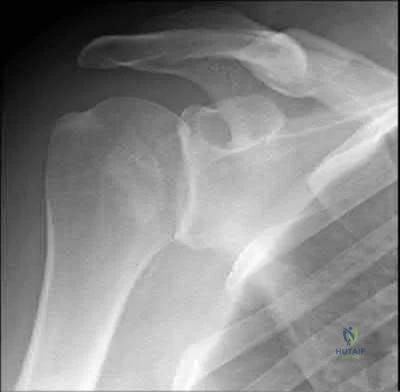
Physical therapy for range of motion followed by rotator cuff and deltoid strengthening exercises

Axillary radiograph of the shoulder
EMG to evaluate the suprascapular and axillary nerves Arthroscopic rotator cuff repair

Open subacromial decompression and latissimus dorsi transfer for massive cuff tear
The radiograph demonstrates overlap of the humeral head and glenoid suggesting shoulder dislocation. An Axillary radiograph is necessary to evaluate concentric reduction vs. dislocation of the shoulder. An example is provided in illustration A. Posterior shoulder dislocations can be easily be missed without the proper orthogonal views of the shoulder. Perron reviews the proper identification and emergency room care of posterior shoulder dislocation. Richardson found axillary radiographs to be more sensitive than trans-scapular radiographs for identifying posterior shoulder dislocations.
Recent randomized controlled trials comparing early passive range of motion to 6 weeks of immobilization after successful arthroscopic rotator cuff repair concluded that, compared to immobilization, early passive range of motion resulted in:
Higher Constant scores at 12 months

Increased rates of re-rupture as determined by ultrasound Equivalent functional outcomes

Less pain at 6 months

Inceased range of motion at 12 months
A series of high-quality RCTs have demonstrated that early passive range of motion has equivalent functional outcomes when compared to 6 weeks of immobilization after arthroscopic rotator cuff surgery.
Traditionally, most surgeons recommended early post-operative range of motion exercises for their patients in order to prevent adhesions and ultimately stiffness. However, recent evidence has found that there is no difference in the healing rate, range of motion or functional outcome between patients who undergo early versus delayed (i.e. initial 6 weeks of immobilization) passive range of motion exercises after arthroscopic rotator cuff repair.
Kim et al. conducted a randomized controlled trial comparing early passive range of motion vs. immobilization in 106 patients who underwent arthroscopic repair for full-thickness rotator cuff tears. They found that there was no clinically or statistically significant difference between the two groups in pain, healing or function.
Keener et al. also conducted a randomized controlled trial of 124 patients who were undergoing arthroscopic repair of a full-thickness rotator cuff tear and found no difference between early and delayed range of motion in healing and functional outcome.
Cuff & Pupello also compared early vs. delayed range of motion during the post-operative rehabilitation phase in a randomized controlled trial of 68 individuals undergoing arthroscopic rotator cuff repair and found no significant difference in range of motion or healing.
Incorrect Answers:
A 49-year-old male presents with right shoulder pain and weakness after undergoing open cervical lymph node biopsy approximately one year ago. A pertinent finding from the physical exam is seen in Figure A, with the patients arms by his side. Physical exam finding with the arms in a position of 90 degrees of forward elevation and 10 degrees of external rotation are shown in Figure B.
What nerve is most likely injured?
Long thoracic Suprascapular Spinal accessory Axillary Thoracodorsal
The patient is presenting with LATERAL scapular winging which is a result of injury to the spinal accessory nerve and resultant trapezius muscle palsy.
The spinal accessory nerve is fundamental to scapulothoracic function and essential for scapulohumeral rhythm. This nerve is vulnerable along its superficial course. The majority of injuries to the spinal accessory nerve are iatrogenic and occur secondary to head and neck surgery. There is often a marked delay in recognition and initiating treatment. Surgical treatment with the Eden-Lange transfer lateralizes the levator scapulae and rhomboids (transfer from medial border to lateral border)
Camp et al. reviewed the results of 111 patients who underwent operative management of a lesion to the spinal accessory nerve. They found that the majority (~80%) of injuries were sustained iatrogenically and that diagnosis was delayed for approximately 12 months.
Pikkarainen et al. reviewed the natural history of isolated serratus palsy. They found that symptoms mostly recover in 2 years, but at least one-fourth of the patients will have long-lasting symptoms, especially pain.
Figure A depicts a patient with lateral scapular winging. Figure B demonstrates physical exam of this patient with their arms in a position of 90 degrees of forward elevation and 10 degrees of external rotation. Illustration A highlights the difference between medial and lateral scapular winging. Illustration B depicts another example of a patient with lateral scapular winging.
Incorrect Answers:
An injury to the long thoracic nerve would result in serratus anterior palsy which would lead to MEDIAL scapular winging.

An injury to the suprascapular nerve would result in weakness and wasting of the supraspinatus and/or infraspinatus.
Question 75
Gaucher’s disease is manifested by reticuloendothelial system macrophage accumulation of
Explanation
REFERENCES: Beatty JH: Orthopaedic Knowledge Update 6. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1999, pp 247-252.
Goldblatt J, Sacks S, Beighton P: The orthopedic aspects of Gaucher disease. Clin Orthop 1978;137:208-214.
Beutler E: Gaucher’s disease. N Engl J Med 1991;325:1354-1360.
Question 76
- Which of the following surgical approaches to the hip is associated with the highest incidence of heterotopic ossification?
Explanation
Prevention:
incision choice: ilioinguinal if possible
radiation
indocin (give pepcid with it)
Question 77
..First-line treatment recommendations include
Explanation
Ultrasound
MRI scan of the thigh
Chest CT scan and whole-body bone scan
Positron emission tomography (PET) scan
Presurgical radiation therapy
Marginal resection
Radical resection and postsurgical radiation
Transverse incision centered over the mass
Incision centered over the mass in line with long axis of limb
Sentinel node biopsy
Core needle biopsy
For each soft-tissue mass clinical scenario or question below, match the most appropriate next evaluation or treatment step listed above.
Question 78
An 8-year-old boy reports ankle pain after striking the ground with the medial aspect of his foot while attempting to kick a soccer ball. Radiographs reveal slight distal tibial physeal widening but no other abnormalities. In treating this injury, which of the following associated conditions is most likely present but may be missed without careful evaluation?
Explanation
REFERENCES: Phan VC, Wroten E, Yngve DA: Foot progression angle after distal tibial physeal fractures. J Pediatr Orthop 2002;22:31-35.
Brook GJ, Greer RB: Traumatic rotational displacements of the distal tibial growth plate. J Bone Joint Surg Am 1970;52:1666-1668.
Question 79
A 40-year-old woman has a symptomatic mass on the anterior aspect of the ankle. She reports no constitutional symptoms. An MRI scan is shown in Figure 12. What is the most likely diagnosis?
Explanation
REFERENCES: Kransdorf MJ, Jelinek JS, Moser RP Jr, et al: Soft tissue masses: Diagnosis using MR imaging. Am J Roentgenol 1989;153:541-547.
Wetzel LH, Levine E: Soft-tissue tumors of the foot: Value of MR imaging for specific diagnosis. Am J Roentgenol 1990;155:1025-1030.
Gerster JC, Landry M, Dufresne L, Meuwly JY: Imaging of tophaceous gout: Computed tomography provide specific images compared with magnetic resonance imaging and ultrasonography. Ann Rheum Dis 2002;61:52-54.
Question 80
A B Figures 82a and 82b are the clinical photograph and radiograph of a 60-year-old man with a 30-year history of diabetes complicated by borderline chronic renal failure, heart failure controlled by medication, and bilateral lower extremity neuropathy. He is currently wheelchair bound because of his cardiopulmonary limitations, but uses his legs for transfers. He has had a progressive left ankle deformity that has progressed to the point at which he cannot use his leg for pivot transfers. He is adamant that something should be done to improve his living situation. Which surgical option can best achieve his goal of using the leg for transfers?
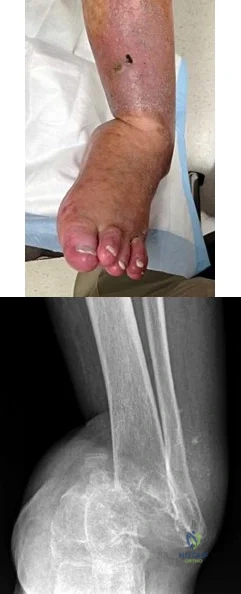
Explanation
The indications for surgery in a Charcot joint are an unbraceable deformity or recurrent ulceration despite use of adequate bracing. Any significant varus/valgus deformity of the ankle or hindfoot (as in this patient) is unbraceable, whereas midfoot Charcot deformities usually can be treated nonsurgically. The goal of surgery is to provide a stable aligned foot and ankle to permit activities and reduce risk for recurrent ulceration. This does not mean that there has to be a radiographic fusion because many patients with diabetes achieve a stable nonunion without pain. The only surgical construct that will provide long-term inherent stability and alignment in this situation is use of a hindfoot fusion rod. It provides better stability and purchase than screw fixation and can be left in indefinitely (unlike an external fixator).
RECOMMENDED READINGS
Dalla Paola L, Volpe A, Varotto D, Postorino A, Brocco E, Senesi A, Merico M, De Vido D, Da Ros R, Assaloni R. Use of a retrograde nail for ankle arthrodesis in Charcot neuroarthropathy: a limb salvage procedure. Foot Ankle Int. 2007 Sep;28(9):967-70. PubMed PMID: 17880869. View Abstract at PubMed
Pinzur MS. Benchmark analysis of diabetic patients with neuropathic (Charcot) foot deformity. Foot Ankle Int. 1999 Sep;20(9):564-7. PubMed PMID: 10509683. View Abstract at PubMed Pinzur M. Surgical versus accommodative treatment for Charcot arthropathy of the midfoot. Foot Ankle Int. 2004 Aug;25(8):545-9. PubMed PMID: 15363375. View Abstract at PubMed
CLINICAL SITUATION FOR QUESTIONS 83 THROUGH 87
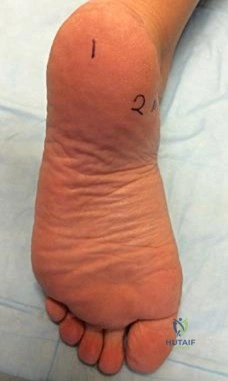
Figures 83a and 83b are the clinical photographs of a 42-year-old woman with a BMI of 31 who has had a 1-year history of right heel pain.
A
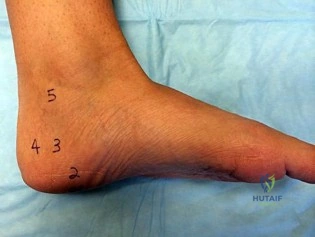
B
Question 81
A 6-year-old boy is being treated for acute hematogeneous osteomyelitis of the distal femur with intravenous antibiotics. The best method to determine the success or failure of initial treatment is by serial evaluations of which of the following studies?
Explanation
REFERENCES: Unkila-Kallio L. Kallio MJ, Eskola J, et al: Serum C-reactive protein, erythrocyte sedimentation rate, and white blood cell count in acute hematogenous osteomyelitis of children. Pediatrics 1994;93:59-62.
Herring JA(ed): Tachdjian’s Pediatric Orthopaedics, ed 4. Philadelphia. PA. WB Saunders, 2008, pp 2090-2100.
AL-Madena Copy
Question 82
A 72-year-old active man has shoulder pain after undergoing an explantation of an anatomic shoulder arthroplasty 6 months prior with an antibiotic cement spacer placed. The patient has 60° of forward flexion, 40° of external rotation, and a positive belly press with limited internal rotation. A recent work-up for continued infection is negative, and a follow-up MRI reveals grade 2 atrophy of the supraspinatus and grade 3 atrophy of the subscapularis with tendon retraction to the glenoid rim. What is the best next step in definitive management?
Explanation
is not indicated for this otherwise active patient.
Question 83
A 54-year-old man undergoes uneventful anterior cervical diskectomy and interbody fusion at C4-5 for focal disk herniation and C5 radiculopathy. At the 3-week follow-up examination, the patient reports a persistent cough. Pulmonary evaluation reveals a mild but persistent aspiration. Laryngoscopy reveals partial paralysis of the left vocal cord, most likely caused by
Explanation
REFERENCES: Apfelbaum RI, Kriskovich MD, Haller JR: On the incidence, cause, and prevention of recurrent laryngeal nerve paralysis during anterior cervical spine surgery. Spine 2000;25:2906-2912.
Jewett BA, Menico GA, Spengler DM, Coleman SC, Netterville JL: Vocal Cord Paralysis Following Anterior Cervical Spine Surgery. Paper presented at the annual meeting or the Cervical Spine Research Society, December 2000, Charleston SC, Paper #7.
Question 84
The primary function of structure “A” in Figure 29 is to limit
Explanation
REFERENCES: Sugita T, Amis AA: Anatomic and biomechanical study of the lateral collateral and popliteofibular ligaments. Am J Sports Med 2001;29:466-472.
Veltri DM, Deng XH, Torzilla PA, et al: The role of the cruciate and posterolateral ligaments in stability of the knee: A biomechanical study. Am J Sports Med 1995;23:436-443.
Question 85
What is the most frequent complication following primary total hip arthroplasty?
Explanation
REFERENCES: Eftekhar N: Total Hip Arthroplasty. St Louis, MO, Mosby,1993, pp 1445-1676.
Koval KJ (ed): Orthopaedic Knowledge Update 7. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 56, 417-451.
FOR ALL MCQS CLICK THE LINK ORTHO MCQ BANK
Question 86
Figure 83a shows an axillary radiograph and Figures 83b and 83c show axial MR arthrograms of a 20-year-old collegiate offensive lineman who has shoulder pain while pass-blocking. He sustained a shoulder injury 3 months earlier when he "jammed it." Prior to this injury, he denies any pain or instability in either shoulder. Despite undergoing rehabilitation with a physical therapist and trainer and abstaining from playing for 6 weeks, he is currently unable to play because of his symptoms. Examination reveals full active range of motion, a positive jerk test which reproduces his symptoms, and a grade 2 posterior translation of the humeral head with load and shift testing which also reproduces his symptoms. What is the best management option to allow him to return to his pre-injury function next season? Review Topic
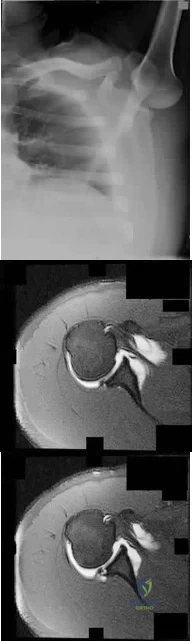
Explanation
Question 87
Patients who sustain bilateral femoral shaft fractures when compared to unilateral femur fractures have higher rates of the following EXCEPT:

Explanation
Question 88
A 32-year-old man has a Glasgow Coma Scale score of 8 and an open pelvic fracture. The patient’s family reports that he is a Jehovah’s Witness. Initial hemodynamic instability has resolved. In the operating room during a washout, the patient’s blood pressure becomes unstable. What is the most appropriate action?
Explanation
REFERENCES: Jimenez R, Lewis VO (eds): Culturally Competent Care Guidebook. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2007.
Jehovah’s Witnessess Official Web Site: Medical Care and Blood, 2008, http://www.watchtower.org/e/medical_care_and_blood.htm
Question 89
Delayed-onset muscle soreness (DOMS) is initially evident at the muscle tendon junction and can spread throughout the entire muscle. It is primarily associated with what type of exercise? Review Topic
Explanation
Question 90
What neurovascular structure is at greatest risk when creating a proximal anterolateral elbow arthroscopy portal? Review Topic
Explanation
Question 91
A 35-year-old man is brought to the emergency department following a motorcycle accident. He is breathing spontaneously and has a systolic blood pressure of 80 mm Hg, a pulse rate of 120/min, and a temperature of 98.6° F (37° C). Examination suggests an unstable pelvic fracture; AP radiographs confirm an open book injury with vertical displacement on the left side. Ultrasound evaluation of the abdomen is negative. Despite administration of 4 L of normal saline solution, he still has a systolic pressure of 90 mm Hg and a pulse rate of 110. Urine output has been about 20 mL since arrival 35 minutes ago. What is the next best course of action?
Explanation
REFERENCE: Mayo K, Kellam JK: Pelvic ring disruptions, in Browner BD (ed): Skeletal Trauma, ed 3. Philadelphia, PA, WB Saunders, 2003, pp 1052-1108.
Question 92
An otherwise healthy 78-year-old woman has low back and buttock pain. Rectal examination reveals a large sacral mass. Figures 7a and 7b show a CT scan and a sagittal MRI scan of the lumbosacral spine. A biopsy specimen is shown in Figure 7c. What is the most likely diagnosis?
Explanation
REFERENCES: Mindell ER: Chordoma. J Bone Joint Surg Am 1981;63:501-505.
Samson IR, Springfield DS, Suit HD, Mankin HJ: Operative treatment of sacrococcygeal chordoma: A review of twenty-one cases. J Bone Joint Surg Am 1993;75:1476-1484.
Question 93
-Figures a and b are the posteroanterior and lateral radiographs of a 13-year-old girl with a progressive curve despite bracing with a thoracolumbosacral orthosis. Examination reveals no pain or neurologic findings. The lumbar curve measures 59 degrees and the thoracic curve measures 52 degrees.The most appropriate treatment is
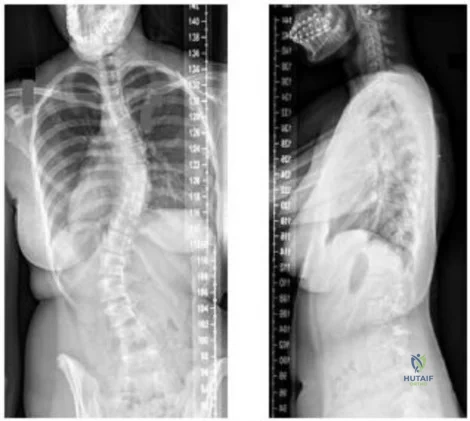
Explanation
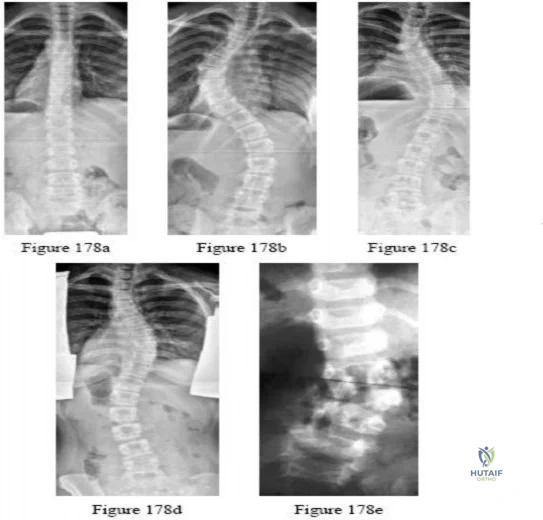
Question 94
A 25-year-old man has a mass on the medial aspect of the left knee. He reports that the mass has been present for several years, but a recent increase in physical activity has resulted in periodic tenderness. Radiographs are shown in Figures 13a and 13b. What is the most likely diagnosis?
Explanation
REFERENCES: Menendez LR (ed): Orthopaedic Knowledge Update: Musculoskeletal Tumors. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 103-111.
Parsons TW: Benign bone tumors, in Fitzgerald R Jr, Kaufer H, Malkani A (eds): Orthopaedics. Philadelphia, PA, Mosby International, 2002, pp 1027-1035.
Question 95
Figures 1 and 2 show the intraoperative photographs obtained during surgical treatment for de Quervain tendonitis. For orientation purposes, dorsal is at the top. Figure 1 is obtained just after the initial first extensor compartment release, and Figure 2 shows the floor of the first extensor compartment. If the structure marked by the black dot is not addressed, the most common postoperative problem would be
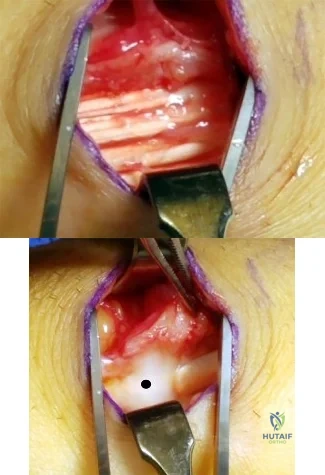
Explanation
The black dot identifies an accessory compartment of the extensor pollicis brevis (EPB) tendon. The incidence of accessory EPB compartment in patients undergoing surgical treatment for de Quervain syndrome ranges from 46% to 60%. Failure to release this compartment at the time of initial surgery can cause persistent postoperative pain. The patient would not experience altered sensation if this compartment were not released. Altered sensation would most commonly occur following injury to the dorsal radial sensory nerve branch during surgery. EPB tendon subluxation also would not occur should the accessory compartment not be released. For EPB tendon subluxation to occur, its own compartment would need to be released first. Finally, EPB tendon rupture would be an extremely uncommon complication of failure to release the accessory compartment.
Question 96
Which of the following regions in the growth plate is commonly affected in a Salter-Harris type II injury? Review Topic
Explanation
Question 97
Figure 4 shows the AP radiograph of a 28-year-old woman who has had moderate pain in the left hip for the past year. Nonsurgical management has failed to provide relief. She denies any history of hip pain, pathology, or trauma. Management should consist of
Explanation
REFERENCES: Trousdale RT, Ekkernkamp A, Ganz R, Wallrichs SL: Periacetabular and intertrochanteric osteotomy for the treatment of osteoarthrosis in dysplastic hips. J Bone Joint Surg Am 1995;77:73-85.
Pemberton PA: Pericapsular osteotomy of the ilium for the treatment of congenital subluxation and dislocation of the hip. J Bone Joint Surg Am 1965;47:65-86.
Question 98
A type 2A hangman’s fracture, which has the potential to overdistract with traction, has which of the following hallmark findings?
Explanation
REFERENCES: Garfin SR, Vaccaro AR (eds): Orthopaedic Knowledge Update: Spine. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1997, pp 197-217.
Levine AM, Edwards CC: The management of traumatic spondylolisthesis of the axis. J Bone Joint Surg Am 1985;67:217-226.
Question 99
A patient who sustained injuries in a motorcycle accident 30 minutes ago has significant motor and sensory deficits corresponding to a C6 level of injury. A lateral radiograph obtained during the initial on-scene evaluation reveals bilateral jumped facets at C5-C6; this appears to be an isolated injury. The patient is awake and alert. The next step in management of the dislocation should consist of
Explanation
REFERENCES: Delamarter RB, Sherman J, Carr JB: Pathophysiology of spinal cord injury: Recovery after immediate and delayed decompression. J Bone Joint Surg Am
1995;77:1042-1049.
Star AM, Jones AA, Cotler JM, Balderston RA, Sinha R: Immediate closed reduction of cervical spine dislocations using traction. Spine 1990;15:1068-1072.
Eismont FJ, Arena MJ, Green BA: Extrusion of an intervertebral disc associated with traumatic subluxation or dislocation of cervical facets: Case report. J Bone Joint Surg Am
1991;73:1555-1560.
Question 100
Which of the following bearing surface combinations has shown the lowest in vivo wear rates in total hip arthroplasty?
Explanation
REFERENCES: Beaty JH (ed): Orthopaedic Knowledge Update 6. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1999, pp 47-53.
Jazrawi LM, Kummer FJ, DiCesare PE: Alternative bearing surfaces for total joint arthroplasty. J Am Acad Orthop Surg 1998;6:198-203.
