OITE & ABOS Orthopedic Board Prep: Adult Reconstruction, Trauma & Upper Extremity MCQs Part 140
Key Takeaway
This page offers Part 140 of a comprehensive OITE & ABOS Orthopedic Surgery Board Review. Featuring 100 verified, high-yield MCQs on topics like Arthroplasty, Elbow, and Hip, it's designed for orthopedic residents and surgeons. Utilize study or exam mode with detailed explanations for rigorous board certification preparation.
About This Board Review Set
This is Part 140 of the comprehensive OITE and AAOS Orthopedic Surgery Board Review series authored by Dr. Mohammed Hutaif, Consultant Orthopedic & Spine Surgeon.
This set has been strictly audited and contains 100 100% verified, high-yield multiple-choice questions (MCQs) modelled on the exact format of the Orthopaedic In-Training Examination (OITE) and the American Academy of Orthopaedic Surgeons (AAOS) board examinations.
How to Use the Interactive Quiz
Two distinct learning modes are available:
- Study Mode — After selecting an answer, you immediately see whether you are correct or incorrect, together with a full clinical explanation and literature references.
- Exam Mode — All feedback is hidden until you click Submit & See Results. A live timer tracks elapsed time. A percentage score and detailed breakdown are displayed upon submission.
Pro Tip: Use keyboard shortcuts A–E to select options, F to flag a question for review, and Enter to jump to the next unanswered question.
Topics Covered in Part 140
This module focuses heavily on: Arthroplasty, Elbow, Fracture, Hip, Infection, Shoulder.
Sample Questions from This Set
Sample Question 1: Figures below show the AP and lateral radiographs obtained from a 54-year-old woman who has worseninggroin pain 18 months after a primary left total hip arthroplasty. The pain is worst when climbing stairs, when rising from a seated positio...
Sample Question 2: Figure 10 is the radiograph of a 44-year-old man with a long-standing history of severe hip pain and a limp. Which clinical scenario most likely could occur when performing total hip arthroplasty on this patient?...
Sample Question 3: After excising a mass from the thigh that was thought to be a lipoma, the pathology reveals that the mass is a high-grade sarcoma. Subsequent treatment should include...
Sample Question 4: A 42-year-old man reports persistent arm pain after undergoing intramedullary nailing of a humeral shaft fracture 13 months ago.Physical exam shows near normal shoulder and elbow range-of-motion. Infection work-up is normal. A radiograph is...
Sample Question 5: Anotherwisehealthyyear-oldwomanhaspain2yearsaftertotalhiparthroplasty.Theclinicalphotographinbelowdemonstratesherskinenvelope,andassociatedradiograph.HerC-reactive proteinlevelisnormal,andhererythrocytesedimentationrateismildlyelevated.Thew...
Why Active MCQ Practice Works
Evidence consistently demonstrates that active recall through spaced MCQ practice yields substantially greater long-term retention than passive reading alone (Roediger & Karpicke, 2006). All questions in this specific module have been algorithmically verified for clinical integrity and complete explanations.
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
Figures below show the AP and lateral radiographs obtained from a 54-year-old woman who has worsening groin pain 18 months after a primary left total hip arthroplasty. The pain is worst when climbing stairs, when rising from a seated position, and during resisted hip flexion. Her pain improved early after surgery but did not completely resolve. Her C-reactive protein and erythrocyte sedimentation rate results of less than 1 mg/dL and 10 mm/hr, respectively, were obtained in the office. What is the best next step?
Explanation
Iliopsoas impingement is a potential cause of persistent groin pain after a total hip arthroplasty. This patient’s history gives groin pain with resisted hip flexion and during activities that require this level of function. The radiographs depict an acetabular component with substantial retroversion. Typical options for the management of iliopsoas tendon impingement include injections, tenotomy, and acetabular revision. Recently, Chalmers and associates reported more predictable groin pain resolution with 8 mm or more of anterior acetabular component when overhang was revised. The radiographs clearly show more retroversion, with a cup prominence of more than 8 mm anteriorly. MRI with MARS could potentially help in the diagnosis of this impingement but would not help in management (option A). An ultrasound- guided injection would need to be administered into the iliopsoas tendon sheath to be of help and, in this case, would likely be performed for diagnostic purposes due to the extreme anterior overhang (option C). Option D would be useful for mild cases of iliopsoas impingement but likely would not help much in this more extreme case.
Question 2
Figure 10 is the radiograph of a 44-year-old man with a long-standing history of severe hip pain and a limp. Which clinical scenario most likely could occur when performing total hip arthroplasty on this patient?
Explanation
The radiograph reveals hip dysplasia. Patients with hip dysplasia and severe limb shortening are at high risk for sciatic nerve palsy from overlengthening. Overmedializing the acetabular component is not the preferred response because overlateralization is more of a concern if the cup is placed in the pseudoacetabulum instead of in the true acetabulum. Placing the hip center too inferior is not the preferred response because the concern in this scenario is placing the hip center too superior if the cup is placed in the pseudoacetabulum or if a large-diameter cup is used. Acetabular fractures are possible because of osteoporotic bone at the true hip center, but is less likely than overlengthening of the extremity.
CLINICAL SITUATION FOR QUESTIONS 11 THROUGH 13
Figures 11a and 11b are the radiographs of a 35-year-old woman with end-stage debilitating osteoarthritis of the right hip. She is contemplating total hip arthroplasty (THA). She has a history of right hip dysplasia and underwent hip osteotomy as an adolescent. Over the years, she has failed nonsurgical treatment including weight loss, activity modifications, and intra-articular injections. Her infection workup reveals laboratory findings within defined limits.
Question 3
After excising a mass from the thigh that was thought to be a lipoma, the pathology reveals that the mass is a high-grade sarcoma. Subsequent treatment should include
Explanation
REFERENCES: Noria S, Davis A, Kandel R, et al: Residual disease following unplanned excision of soft-tissue sarcoma of an extremity. J Bone Joint Surg Am 1996;78:650-655.
Bell RS, O’Sullivan B, Liu FF, et al: The surgical margin in soft-tissue sarcoma. J Bone Joint Surg Am 1989;71:370-375.
Question 4
A 42-year-old man reports persistent arm pain after undergoing intramedullary nailing of a humeral shaft fracture 13 months ago. Physical exam shows near normal shoulder and elbow range-of-motion. Infection work-up is normal. A radiograph is shown in Figure
Explanation
Rubel et al in a combined cadaveric and clinical study comparing one versus two plate constructs for humeral nonunions found that the two plate construct was significantly stiffer, but had no difference in healing rate compared with a single plate construct; 92% of the humeral shaft nonunion patients went onto union with rigid plate fixation.
Ring et al successfully treated a cohort of osteoporotic humeral shaft nonunions with locked plating. They
report 100% union rate with locking plate fixation of these humeral shaft nonunions, with use of autograft in >50% of their cases. Subjective shoulder scores were excellent or good in 22 of 24 patients.
Brinker and O'Connor analyzed the current available evidence for exchange nailing of nonunions and could not recommend this treatment for humeral shaft nonunions.
OrthoCash 2020
Question 5
An otherwise healthy year-old woman has pain 2 years after total hip arthroplasty. The clinical photograph in below demonstrates her skin envelope, and associated radiograph. Her C-reactive protein level is normal, and her erythrocyte sedimentation rate is mildly elevated. The white blood cell count is normal. Hip aspiration attempted under fluoroscopy generates no fluid. What is the best definitive treatment?
Explanation
This patient clearly has a chronically infected total hip arthroplasty, indicated by the open, draining sinus, as well as trochanteric bone resorption on radiographs, and two years of pain. Recently, specific guidelines have been published to better help the clinician define infection. Repeating the hip aspiration is unnecessary, because infection is already evident. Initiating a wound care consult would not address the underlying infection. The determination whether to retain the components or perform a two-stage exchange is based more on the acuity of infection. In this particular case, the patient is chronically infected. Irrigation and debridement with a liner exchange and retention of the components are reserved for the acute setting.
Question 6
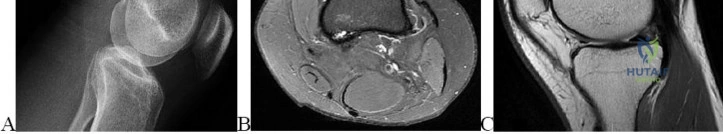
An 80-year-old man has had increasing shoulder pain for the past 4 months. He reports that it began with soreness and stiffness after chopping some wood. A coronal MRI scan is shown in Figure 16. Initial management should consist of
Explanation
REFERENCES: Rockwood CA Jr, Williams GR Jr, Burkhead WZ Jr: Debridement of degenerative, irreparable lesions of the rotator cuff. J Bone Joint Surg Am 1995;77:857-866.
Beaty JH (ed): Orthopaedic Knowledge Update 6. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1999, pp 299-312.
Question 7
Which of the following factors will adversely affect bone ingrowth in a revision porous-coated stem?
Explanation
REFERENCES: Berry DJ, Harmsen WS, Ilstrup D, Lewallen DG, Cabanela ME: Survivorship of uncemented proximally porous-coated femoral components. Clin Orthop 1995;319:168-177.
Cook SD, Thomas KA, Haddad RJ Jr: Histologic analysis of retrieved human porous-coated total joint components. Clin Orthop 1988;234:90-101.
Spector M: Historical review of porous-coated implants. J Arthroplasty 1987;2:163-177.
Question 8
Which of the following is most predictive of a medial side ankle injury in the presence of a fibula fracture above the level of the joint?
Explanation
REFERENCES: McConnell T, Creevy W, Tornetta P III: Stress examination of supination external rotation-type fibular fractures. J Bone Joint Surg Am 2004:86;2171-2178.
Kristensen KD, Hansen T: Closed treatment of ankle fractures: Stage II supination-eversion fractures followed for 20 years. Acta Orthop Scand 1985;56:107-109.
Michelson JD: Fractures about the ankle. J Bone Joint Surg Am 1995;77:142-152.
Question 9
What is the most prevalent adverse event associated with allogeneic blood transfusion?
Explanation
REFERENCES: Aubuchon JP, Birkmeyer JD, Busch MP: Safety of the blood supply in the United States: Opportunities and controversies. Ann Intern Med 1997;127:904-909.
Popovsky MA, Whitaker B, Arnold NL: Severe outcomes of allogeneic and autologous blood donation: Frequency and characterization. Transfusion 1995;35:734-737.
Question 10
Which of the following zones of articular cartilage has the highest concentration of proteoglycans?
Explanation
Question 11
A 12-year-old boy with an ankle fracture undergoes closed reduction under sedation in the emergency department. Figure 27 shows a lateral radiograph of the ankle after two attempts at closed reduction. Based on these findings, treatment should now consist of Review Topic
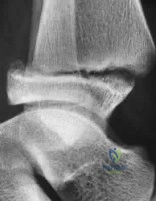
Explanation
Question 12
Figure 35 shows the lateral radiograph of a 15-year-old basketball player who felt a dramatic pop in his knee when landing after a lay-up. The patient reports that he cannot bear weight on the injured extremity. Management should consist of
Explanation
REFERENCES: Ogden JA, Tross RB, Murphy MJ: Fractures of the tibial tuberosity in adolescents. J Bone Joint Surg Am 1980;62:205-215.
Pape JM, Goulet JA, Hensinger RN: Compartment syndrome complicating tibial tubercle avulsion. Clin Orthop 1993;295:201-204.
Question 13
5 standard deviations below young normals (< -2.5). The Z-score represents a comparison to age-matched normals.
Explanation
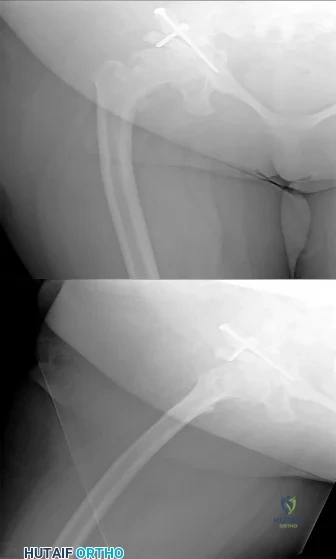
This patient has an impending subtrochanteric femur fracture and should be stabilized with cephalomedullary nailing.
Bisphosphonates have been shown to prevent osteoporotic fractures. They suppress osteoclastic recruitment and activity and induce apoptosis of osteoclasts. However, they have also been associated with subtrochanteric femur fractures. Cortical stress reactions in the form of lateral cortical thickening have been documented when radiographs were performed during the prodromal period preceding these fractures. If radiographs are obtained and demonstrate lateral cortical thickening in the presence of thigh pain, the entire femur should be stabilized with prophylactic cephalomedullary nailing to prevent fracture.
Shane et al. performed a review of atypical subtrochanteric and diaphyseal
femoral fractures. They report that long-term bisphosphonate use is associated with these injuries. Bisphosphonates localize in areas that are developing stress fractures and suppress intracortical remodeling. When bisphosphonate use has stopped, the risk of fracture decreases over time. They conclude that teriparatide may advance the healing of atypical femur fractures after surgical treatment.
Koh et al. studied the natural history of femoral stress lesions associated with bisphosphonate therapy. They determined certain features that predispose to complete stress fractures. They found all patients had thigh pain before fracture. They conclude that cortical stress reactions associated with prolonged antiresorptive therapy and the "dreaded black line" should be prophylactically stabilized to avoid a complete fracture.
Figure A is a radiograph of the proximal femur demonstrating lateral cortical thickening with the "dreaded black line." Illustration A is the same image with an arrow indicating the "dreaded black line."
Incorrect Answers:
Which of the following statements regarding bone mineral density (BMD) is true?
The 2017 American College of Rheumatology/American Association of Hip and Knee Surgeons Guideline for the Perioperative Management of Antirheumatic Medication states that hydroxychloroquine can be continued and etanercept
should be held for 2 weeks prior to undergoing total hip arthroplasty.
Patients with rheumatoid arthritis (RA) report high satisfaction following hip or knee replacement despite the higher rates of infection, dislocation, and readmission rates. Patients with RA may present on a variety of different biologic and nonbiologic medications used to control their systemic RA.
Optimal preoperative management of these immunosuppressant medications may help mitigate some of the risks of postoperative complications in RA patients.
Singh et al. reviewed the evidence surrounding the benefits and harms of various antirheumatic medications. They found evidence for traditional DMARDs, biologic agents, and nonbiologic agents in acute and established RA totaling 74 recommendations. They concluded that these recommendations are not prescriptions and that ultimate decision making should be patient- specific in a shared-decision
making process between the patient and physician.
Goodman et al. performed a multistep literature review on optimal antirheumatic medication management prior to joint replacement surgery. They were able to provide recommendations on when to continue, when to withhold, and when to restart these medications, and the optimal perioperative dosing of glucocorticoids. They concluded that these guidelines will help physicians manage antirheumatic medications at the time of elective THA or TKA.
Incorrect Answers:
An 83-year-old woman presents complaining of thigh pain. The pain has been progressing over the last few months. She denies any night chills or recent weight loss. She has smoked 1 pack per day for the last 40 years. Her current medications are alendronate and citalopram. Her current imaging is shown in Figure A. What is the next best step in treatment?
The patient is presenting with complex regional pain syndrome (CRPS) type 1 after a distal 1/3 tibial shaft fracture. The best diagnostic test for this is a thorough history and physical exam.
CRPS is a disorder of increased sympathetic activity in a region of prior trauma. Cases can be classified as type 1, where there is no demonstrable nerve damage, or type 2, where a specific nerve is affected. Patients will typically present with cool and mottled skin that atrophic and absent of hair. Many times the affected limb will be noticeably cooler than the contralateral side. In advanced stages, there will be joint contractures and extensive osteopenia on radiographs. Several diagnostic aids have been developed, but remain inadequate to diagnostic sensitivity compared to a thorough history and physical.
Shah et al. reviewed the diagnosis and treatment of CRPS. The authors reported that sweat quantification testing, skin thermography, and electromyography may be useful aids in diagnosis, but there is a lack of diagnostic sensitivity to make these tests reliable. The authors concluded that evidence suggests gabapentin, prazosin, propranolol, nifedipine, and mexiletine are the best medications for treatment.
Hogan et al. reviewed the diagnosis and treatment of CRPS. The authors reported that the most sensitive means for diagnosis is a good history and physical exam as there is no single test to confirm the diagnosis. The authors recommended a multidisciplinary team approach including pain specialists, physical therapists, and orthopedic surgeons as syndrome response to medications is variable.
Figures A and B demonstrate an AP and lateral radiograph of the right tibia and fibula with a distal 1/3 tibia fracture. Illustration A depicts that Lankford and Evans classification for CRPS.
Incorrect Answers:
A 72-year-old female with rheumatoid arthritis is scheduled to undergo total hip arthroplasty. She presents for her preoperative visit and asks about dosing of her antirheumatic medications. She currently takes etanercept weekly and hydroxychloroquine daily. Which of the following is the best dosing recommendation for her antirheumatic medications prior to surgery?
the entire right lower extremity, with sensitivity to cold temperatures. Physical exam demonstrates hyperesthesia of the extremity, thin and shiny appearing skin, cyanotic appearing with skin cool to the touch. What is the likely diagnosis and what is the best diagnostic test?
In a 5-year-old female without a history of trauma or rashes and with persistent oligoarthritis that improves during the day, the most likely diagnosis is juvenile idiopathic arthritis (JIA). Early-onset JIA is associated with chronic uveitis.
JIA is defined by the American College of Rheumatology as persistent arthritis and swelling in one or more joints for 6 weeks or longer in a patient younger than 16 years of age. It is a diagnosis of exclusion, usually entailing pattern recognition after a thorough history and physical exam. Serologic studies, including rheumatoid factor (RF), antinuclear antibody (ANA), and HLA-B27, may be helpful to rule out other etiologies (septic arthritis, systemic lupus erythematosus, rheumatic fever); however, these are neither sensitive nor specific. In patients with JIA, evaluation for possible uveitis by an ophthalmologist should be considered. Although this patient could have Lyme disease given the likely recent exposure to ticks during her camping trip, the lack of a rash, unresponsiveness to antibiotics, and polyarthritic nature make it less likely.
Arvikar et al. compared clinical features of systemic autoimmune arthritides to those of Lyme arthritis. They found that patients with Lyme arthritis usually had a clinical picture of monoarticular knee arthritis, whereas patients with systemic autoimmune arthritis manifested with polyarthritis. They concluded that systemic autoimmune arthritis with or without a history of Lyme disease should be treated with disease-modifying antirheumatic drugs (DMARDs).
Punaro et al. reviewed common rheumatologic conditions in children who may present to orthopaedic surgeons. For JIA, they reported a typical history of oligoarthritis for 6 weeks or more in a white female patient, with a peak onset between ages 1 and 3 years. Uveitis was typically chronic, bilateral, and asymptomatic. They concluded that while serologic tests were useful in
excluding other diagnoses, they were less useful in confirming JIA.
Incorrect Answers:
A 40-year-old patient sustains the injury in Figures A and B six months ago and underwent the appropriate fixation method. The patient is continuing to experience a tremendous amount of pain in
returning from summer camp. She denies any antecedent trauma, fevers, or rashes. Antibiotics prescribed by her primary care doctor have provided no significant relief, but she reports feeling better at
the end of the day. Labs reveal a negative rheumatoid factor. Which of the following is most commonly associated with her diagnosis?
The hardware shown in Figure A is a tension band plate. It is able to perform its function due to the Hueter-Volkmann Law.
Bones undergo continuous remodeling and turnover which are sensitive to the surrounding mechanical environment. Bone remodeling is governed by Wolff’s law, while the mechanical influence on longitudinal bone growth is controlled by the Hueter– Volkmann law. Wolff’s law relates to the adaptation of bone to its mechanical environment, and involves bone apposition stimulated by intermittent increased stress and bone resorption following reduced intermittent stress. The Hueter–Volkmann law relates to immature bone growth suppression through sustained compressive loading and growth acceleration by reduced loading or distraction.
Villemure et al. performed a review of growth plate mechanics and mechanobiology. They report that growth plates are sensitive to the surrounding mechanical environment. There are a number of clinical conditions of the skeleton that are thought to result from abnormal mechanical loading conditions influencing longitudinal growth prior to skeletal maturity, such as clubfoot (associated with limb position in utero), slipped capital femoral epiphysis, tibia vara, spondylolisthesis, and scoliosis.
Shabtai et al. performed a review of the limits of growth modulation using tension band plates in the lower extremities. Tension band plates have been found to be safe and effective at correcting pediatric frontal plane angular deformities. They found that the success rate for idiopathic cases nears 100%. The success rate for pathologic cases is lower and they have a higher complication rate. They conclude that tension band plates are a reasonable option for all but the most extreme frontal and sagittal plane deformities.
Figure A is a bilateral knee radiograph of a pediatric patient with tension band plates on the right tibia. Illustration A is a bilateral knee radiograph of the same pediatric patient.
The physis appears to have partially closed down and the angle of the screws has changed. One of the screws has broken which happens frequently.
Incorrect Answers:
A 5-year-old girl presents with an 8-week history of pain and swelling in the right knee, right shoulder, and left elbow after
Limb buds develop at 4 weeks and are first able to be visualized by transvaginal ultrasound at 8 weeks.
In a developing fetus, limb buds form at 26 days. The development of the limb is guided by a complex interaction of gene transcription factors and regulatory loops. The most important genes in limb development are sonic hedgehog (SHH), HOX genes, and WNT genes. Ultrasound evaluation is increasingly
being utilized to diagnose and guide treatment for developmental anomalies of a fetus. The limb buds of the fetus can be first seen at 8 weeks of gestation.
Krakow et al. reported on the prenatal diagnosis of fetal developmental dysplasias. They found that differentiating these disorders in the prenatal period can be challenging because they are rare and because many of the ultrasound findings are not necessarily pathognomic for a specific disorder.
Oetgen et al. authored a review on prenatal diagnosis of musculoskeletal conditions. They note that ultrasonography is a safe and cost-effective tool used to prenatally detect common musculoskeletal conditions such as clubfoot, skeletal dysplasias, limb-length discrepancies, spinal abnormalities, and hand and other upper extremity deformities.
Illustration A is a pictorial representation of limb bud formation Incorrect Answers:
The hardware shown in Figure A relies on which of the following principles to achieve its function?
Both Hemophilia A and B are inherited by X-linked recessive patterns. Hemophilia A is caused by factor VIII deficiency, whereas hemophilia B is caused by factor IX deficiency.
Factor VIII deficiency, also known as Hemophilia A, most commonly affects males due to the X-linked recessive inheritance pattern and occurs with a frequency of 1:5000 males. Factor IX deficiency, also known as hemophilia B, also only affects males due to X-linked recessive inheritance, with a frequency of 1:30000 males. Both disorders commonly present with recurrent spontaneous hemarthroses that affect large joints, typically the knee, leading to chronic synovitis and eventually joint destruction. Initial treatment involves factor replacement to within 60% normal, joint aspiration, and immobilization until the physical exam is normal. Treatment for chronic synovitis involves radiosynovectomy, open synovectomy, or arthroscopic synovectomy. End- stage joint destruction requires reconstructive surgery with aggressive factor replacement pre- and postoperatively.
Luck et al. performed a review on hemophilic arthropathy and recommended treatment options for hemophilic arthropathy. The authors recommend that infants get
primary prophylaxis with factor replacement prior to developing a "target" joint. In patients that experience a hemarthrosis, factor replacement with joint aspiration and immobilization until a normal physical exam are paramount for reducing chronic synovitis. Synovectomy, either arthroscopic or open, is recommended for chronic synovitis to reduce the progression of arthropathy. Then arthroplasty is reserved for end-stage joint destruction characteristic of recurrent synovitis.
Zingg et al. performed a retrospective review of 43 consecutive TKA in patients with hemophilic arthropathy. At 9.5 years follow-up there were two hematogenous infections, three revisions, 94% good-to-excellent patient- reported outcomes, and significantly increased ROM compared to preoperative examination. The authors concluded that TKA remains a successful option for end-stage arthropathy for hemophiliacs, but outcomes do not reach the level of non-hemophiliacs.
Journeycake et al. performed a retrospective review on 28 arthroscopic synovectomies performed on pediatric hemophiliac patients with chronic synovitis. At 5-years follow-up 76% of affected joints had stable or improved levels of function. The authors concluded that arthroscopic synovectomy provides a reliable means for limiting current hemorrhage in the affected joint and improving ROM.
Illustration A depicts a pedigree with an X-linked recessive inheritance pattern. Notice how only males are affected, but women can be carriers. Illustration B depicts the process by which recurrent hemarthroses leading to chronic synovitis and then arthropathy.
Incorrect Answers:
deficiency of von Willibrand factor; which assists in platelet adhesion. It is inherited in autosomal recessive pattern with the gene locus found on chromosome 12.
In terms of fetal limb bud development, which of the following is true?
Fluoroquinolones such as levofloxacin act by block DNA replication by inhibiting DNA gyrase.
Fluoroquinolone antibiotics are bactericidal, and their mechanism of action works through the inhibition of DNA gyrase. Side effects of fluoroquinolones include inhibition
of early fracture healing through toxic effects on chondrocytes and increased rates of tendinitis, with a special predilection for the Achilles tendon.
Levine et al. published a review on fluoroquinolones. They report that fluoroquinolones act by inhibiting DNA topoisomerases such as DNA gyrase (topoisomerase II). Due to increasing antibiotic resistance, their use is limited to specific clinical scenarios.
Additionally, their use in children is restricted due to a potential for growth disturbance and cartilage damage.
Perry et al. performed an experimental study on the inhibition of fracture healing by levofloxacin and trovafloxacin in rats. They found that experimental fractures systemically exposed to levofloxacin or trovafloxacin have diminished healing during the early stages of fracture repair. They, therefore, concluded that the administration of quinolones during early fracture repair may compromise fracture healing in humans.
Illustration A is an image illustrating the targets of the various antibiotic classes. Incorrect Answers:
Which of the following bleeding disorders is caused by an X- linked recessive mutation?
An isotonic muscle contraction is a muscle contraction with constant tension such as the upwards and downwards motions of a biceps curl.
The word “isotonic” is derived from two Greek words: “iso”, meaning “same”, and “tonikos” meaning “tension”. An isotonic muscle contraction is one during which the muscle maintains the same tension as it shortens. There are two types of isotonic contractions: concentric and eccentric. In a concentric isotonic contraction, the muscle shortens while contracting. In an eccentric isotonic contraction, the muscle lengthens during contraction.
Ashe et al. review exercise programs used in physical therapy. They report that muscle strengthening can be classified into isotonic, isometric, and isokinetic contractions.
Isotonic exercises involve the development of muscular force through range of motion or movement. Isokinetic exercises involve the force generation at a constant speed.
Isometric exercises involve the development of force without movement, as in tensing and holding a muscle
at a certain part of the range.
Illustration A is an image which illustrates the difference between isotonic and isometric contractions.
Incorrect Answers:
Which of the following correctly describes a class of antibiotics and its mechanism of action?
The third step in applying EBM is to appraise the evidence.
Evidence-based medicine (EBM) refers to an explicit process of using and evaluating information to make medical decisions. When applying EBM in practice, there are 5 steps that should be followed: 1) formulate an answerable question, 2) gather evidence, 3) appraise the evidence, 4)
implement the evidence, and 5) evaluate the process to determine the efficacy of the proposed treatment.
Bernstein published a review on EBM. He advocates for the use of a five-step process for sound decision making: formulate answerable questions, gather evidence, appraise the evidence, implement the valid evidence, and evaluate the process.
Spindler et al. published a review on reading and reviewing the orthopaedic literature. They focus on the third step of EBM: appraising the evidence. They report that systematic review assists the orthopaedic surgeon in interpreting study results and in understanding the relative validity of these results in the hierarchy of evidence.
Illustration A is a table listing the 5 steps of EBM.
Incorrect Answers:
4: Gathering evidence is the second step of EBM.
Which of the following activities describes an isotonic muscle contraction?
On average, physicians interrupt patients within 23 seconds of their interview.
The patient-physician interaction often begins with an initial "survey of problems" through an open-ended question designed to give the patient the freedom to speak and explain
their reason for seeking care. This is followed by a set of focused or closed-ended questions designed to elicit additional details and clarification. Unfortunately, physicians are often quick to interrupt or redirect patients prior to the completion of their reason for seeking care. This practice may lead to missed information, poor communication, and poor
patient satisfaction. Time constraints on physicians may contribute to this behavior. Marvel et al. looked at 264 patient-physician interviews by board-certified family practice physicians. They found patients' initial statement of concern were only complete 28% of the time with an average physician redirection
time of 23.1 seconds. They found patients only needed an additional 6 seconds to complete their statement of concern compared to those who were
redirected by the physician. They conclude that obtaining a complete patient agenda takes little time and can improve interview efficacy and increase data collection.
Incorrect Answers:
When applying evidence-based medicine (EBM) in practice, there are 5 steps that should be followed. Which of the following describes the third step?
For upper extremity surgery, the majority of narcotic pills prescribed by hand surgeons are not consumed by patients.
Patients in the United States are treated very aggressively for pain control. This is due, in part, to The Joint Commission, which has controversially identified pain as the "5th vital sign." An opioid epidemic has ensued which has been linked to a decreased the life expectancy in the United States for three consecutive years beginning in 2014. As a result, unused prescription pain medication following upper extremity surgery represents a liability for patients and surgeons. Following simple soft tissue surgeries (trigger finger, carpal tunnel, mass removal) patients typically only require pain
medication for 2-3 days, and there is no difference in pain control between narcotic or anti-inflammatory medication.
Stanek et al. implemented a standardized postoperative opioid prescription protocol for a group of academic hand surgeons. They found that the protocol decreased the opioid prescription size by 15%, prescription variability, and decreased refills. The authors recommend the development of specific prescription guidelines.
Rodgers et al. interviewed 250 patients after upper extremity surgery about opioid consumption. They reported that patients most frequently received 30 narcotic pills, which provided relief in 92% of cases. The authors found that patients undergoing bone procedures used on average 14 pills, most patients took medication for less than two days post-operatively, and the number of pills consumed on average was 10, with 19 pills unused. As a result, the authors advocated for more limited narcotic prescriptions post-operatively.
Weinheimer et al. randomized patients undergoing hand surgery to receive either Norco or acetaminophen/ibuprofen. They found no difference in time until patients were pain- free, average VAS scores, or the absolute number of those patients who were pain-free. They did find that the narcotic group experienced more adverse side effects (23% vs 3%), ultimately recommending for limiting narcotics post-operatively.
Incorrect answers:
During a new patient office visit, a physician asks an initial open- ended question to the patient. On average, how much time elapses before the physician redirects the patient's initial statement of concern?
The patient’s laboratory workup is likely to reveal hypovitaminosis D. Metabolic and endocrine abnormalities should be considered in patients who exhibit poor fracture healing, especially in those who lack history and exam findings suggestive of infection.
In addition to ruling out infection, a nonunion workup should include tests to identify metabolic and endocrine abnormalities. 25-hydroxyvitamin D3, synthesized from cholecalciferol in the liver, is the laboratory study of choice to determine vitamin D deficiency. Low vitamin D is a common, and easily treated, form of malnourishment in orthopedic trauma patients. Other important factors that can negatively impact fracture healing include protein malnourishment, diabetes mellitus, nicotine use, and HIV.
Warner et al. showed perioperative vitamin D deficiency correlated with
inferior clinical outcomes in patients who underwent operative fixation of ankle fractures. Of the 98 patients studied, 36 (37%) were found to be deficient in vitamin D (<20 ng/ml) and 31 (32%) were found to have a vitamin D insufficiency (> 20 ng/ml, <30 ng/ml). They concluded insufficient vitamin D may result in worse outcomes in orthopedic trauma patients recovering from fracture fixation.
Brinker et al. reviewed metabolic and endocrine abnormalities in 37 patients with nonunions. Inclusion criteria were: 1) an unexplained nonunion that occurred despite adequate reduction and stabilization; 2) history of multiple low-energy fractures with at
least one nonunion; or 3) a nonunion of a nondisplaced pubic rami or sacral ala fracture. Of the 37 patients who met screening criteria, 31 (84%) had metabolic or endocrine abnormalities. Vitamin D deficiency, discovered in 25 of 37 patients (68%), was the most common newly diagnosed abnormality. The authors conclude all patients with nonunion who meet their screening criteria should be referred to an endocrinologist.
Bishop et al. reviewed the assessment of compromised fracture healing and advocate for a metabolic and endocrine workup in the presence of nonunion. If an endocrinology consultation is unavailable, the initial laboratory screening should include 25- hydroxyvitamin D, calcium, thyroid-stimulation hormone, phosphorus, and alkaline phosphatase levels. They also emphasize that the presence of normal inflammatory markers does not exclude the possibility of infection, which should remain in consideration until fracture union and resolution of symptoms.
Incorrect Answers
However, the rate of infection is lower than hypovitaminosis D and both can occur simultaneously.
A hand surgeon plans on performing a carpal tunnel release on a healthy 45- year-old female. Which of the following is true regarding pain management for this case in the post-operative setting?
The ideal scenario to use the ANOVA test is when comparing parametric continuous data (i.e. BMI) for three or more groups.
In statistical analyses, data can be described as discrete (categorical, ordinal) or continuous. Discrete data are observations that can be expressed as categories such as gender, race, or disease status. Continuous data, such as age, are observations for which the difference between the numbers have meaning on a numerical scale. The ANOVA test is used to compare differences in mean values (i.e. continuous data) when there are more than two independent sample groups. When discrete data is compared in the setting of two or more independent sample groups, the chi-squared (parametric) or Fischer's exact test (non-parametric) may be utilized.
Kuhn et al. reviewed statistical tests when discrete data are analyzed. They reported that data may be either discrete (i.e. categorical) or continuous (i.e. age, BMI, height). They presented examples of tests used for discrete data including the chi-square test and Fischer's exact test. They emphasized the importance of scrutinizing the data presented prior to selecting a statistical test.
Greenfield et al. reviewed statistical tests when continuous data are analyzed. They reported that statistical tests for continuous data must be used if the outcome of interest is a comparison of sample means for data that are continuous (i.e. the height of populations). They discuss one-sample t-tests, independent two-sample t-tests, paired t- tests, and ANOVA.
Illustration A demonstrates an algorithm that is helpful in selecting the correct statistical test.
Incorrect Answers:
A 40-year-old Hispanic male presents with persistent pain seven months after open reduction internal fixation of a closed distal tibial fracture. His postoperative course was unremarkable and weight- bearing was resumed at six weeks. Exam reveals a well-healed incision with tenderness at the fracture site. There is no swelling or erythema. Radiographs demonstrate intact hardware and an oligotrophic nonunion. Laboratory workup is most likely to support which of the following interventions:
General anesthesia carries an increased risk of thromboembolism compared to spinal anesthesia. The remaining statements are false.
There have been multiple factors that demonstrate an increased risk of venous thromboembolism (VTE). Some of these risk factors include a previous VTE, obesity (BMI
> 30), surgery type (i.e. total joint arthroplasty),
hypercoagulable states (i.e. cancer, inheritable traits), myocardial infarction (MI), congestive heart failure, family history of VTE, hormone replacement therapy, elevated hormone conditions, varicose veins, and general anesthesia (increased risk compared to epidural/spinal anesthesia). Current AAOS guidelines recommend mechanical prophylaxis in all total hip and knee arthroplasty patients and chemoprophylaxis is recommended, but no optimal regimen is recommended. Chemical prophylaxis should be individualized for each patient and their risk factors.
Geerts et al. put forth their recommendations on the prevention of VTE from the American College of Chest Physicians in 2008. Some of the important points include aspirin not being recommended as a monotherapy (this recommendation was changed in 2012 and is now accepted as monotherapy), recommendation for mechanical prophylaxis, and recommendation for routine chemoprophylaxis for elective hip and knee arthroplasty for a minimum of 10 days.
Caprini et al. retrospectively reviewed 939 patients with either a DVT, PE, or PE and DVT and their treatment. They found that there was lower than anticipated use of low molecular weight heparin, insufficient bridging of patients to warfarin, and insufficient continuation of anticoagulation following hospitalization. They concluded that hospitals need to re-evaluate adherence to VTE treatment guidelines and develop strategies to optimize therapy.
Incorrect Answers:
An orthopedic surgery intern is preparing to perform statistical analyses for his research project. He presents to the department statistician inquiring about the Analysis of Variance (ANOVA) test. Which of the following below is the ideal scenario to use the ANOVA test?
While almost all patients undergoing major orthopaedic procedures receive VTE prophylaxis, this is often not within the ACCP post-operative VTE prophylaxis guidelines.
VTE events typically occur following hospital discharge, within the first 2 to 6 weeks following surgery. Risk is increased with major orthopaedic surgery due to greater soft tissue disruption, venous stasis from limb manipulation, and post-operative immobility. VTE following major orthopaedic hip and knee surgery represents not only a significant cause of postoperative morbidity and mortality but contributes a substantial economic burden. Prophylaxis is the single-most-important factor mitigating the risk of VTE. Therefore adherence to the AAOS and ACCP guidelines is recommended.
Friedman et al. evaluated compliance of physicians with American College of Chest Physicians (ACCP) post-operative VTE prophylaxis guidelines following TKA and THA. The authors found moderate compliance overall, with 47% of THA and 61% of TKA patients receiving appropriate prophylaxis in terms of type, duration, start time, and dose. Compliance with Warfarin use was the lowest, while that with low-molecular-weight heparin was significantly higher. They concluded that while almost all patients received prophylaxis, this was often not within the guidelines.
Oster et al. investigated the economic consequences of VTE following major orthopaedic hip or knee surgery. The authors found that 2.2% of patients developed clinically significant VTE, 62% after hospital discharge and that patients who developed in-hospital VTE had a significantly longer length of hospital stay and associated costs than those that did out-of-hospital and were later readmitted. They concluded that the economic impact of VTE was
substantial regardless of setting.
Incorrect answers:
Which of the following statements is true as it relates to the risk of thromboembolism?
Those utilizing opioids prior to elective hip and knee arthroplasty are at elevated risk of complications. Weaning opioids preoperatively has been shown to improve postoperative outcomes.
Nonoperative management of osteoarthritis (OA) is focused on reducing pain and limiting functional impairment with medications, physical therapy, activity modification, weight
loss, and intra-articular corticosteroid injections.
Pharmacologic management of OA includes NSAIDs and tramadol (per the AAOS CPGs). Opioids have been increasingly used for OA despite the lack of evidence behind their usage. Chronic opioid usage may improve OA-related pain but it has been associated with numerous adverse effects and worse musculoskeletal treatment outcomes.
Gaffney et al. in their review of perioperative pain management for hip and knee arthroplasty, describe the role of opioids, cryotherapy, acetaminophen, NSAIDs, tramadol, anticonvulsants, spinal analgesia, epidural analgesia, peripheral nerve blocks, and periarticular injections. They recommend IV dexamethasone on POD1, scheduled Tylenol, scheduled NSAIDs (Celebrex vs naproxen vs ketorolac), and PRN tramadol, oxycodone, or hydromorphone for breakthrough pain.
Nguyen et al. performed a retrospective matched cohort comparing patients undergoing hip or knee arthroplasty who were either opioid-naive, chronic opioid users, or chronic opioid users weaned of opioids preoperatively. They found that chronic opioid users who were able to reduce their preoperative opioid use by half prior to arthroplasty had outcomes (SF12 physical component and WOMAC) superior to those who were unable to decrease preoperative opioid use.
Sing et al. performed a retrospective review including 1263 patients undergoing primary THA or TKA, finding that patients who utilized opioids preoperatively had elevated postoperative pain, consumed a greater amount of morphine equivalents, walked fewer meters, had a longer postoperative length of stay, were more likely to be discharged to a care facility, and had 4-
5x greater 90d complications. They conclude that opioid users are a high-risk group.
Incorrect answers:
Which of the following is true regarding venous thromboembolism (VTE) following major orthopaedic hip or knee surgery?
This patient has developed CRPS following fixation of a distal radius fracture. All of the above are characteristics of CRPS except for decreased perfusion to the fingertips.
CRPS is divided into two general categories: Type I, occurring in the absence of a specific nerve injury, and Type II, resulting from presence of a specific nerve injury. The incidence is 6-26 cases per 100,000 person-years, mostly affecting females (4:1), and smokers. The International Association of the Study of Pain (IASP) has developed the Budapest Criteria for the diagnosis of CRPS. These include sensory (reports of hyperesthesia and/or allodynia), vasomotor (reports of temperature asymmetry and/or skin color changes and/or skin color asymmetry), sudomotor/edema (reports of edema and/or sweating changes and/or sweating asymmetry), and motor (reports of decreased ROM, weakness, or trophic changes to hair or nails) changes. Vitamin C following distal
radius fracture fixation has been suggested as preventative, though still somewhat controversial. Following development of CRPS, treatment includes psychotherapy, occupational therapy, sympathetic blockade, and antidepressants.
Birklein and Schlereth comprehensively review CRPS. The authors describe how after a trauma there is an abundance of inflammatory mediators which stimulate the peripheral nerves. In addition, the proinflammatory cytokine network stimulates bone cell and fibroblast proliferation and potentially endothelial dysfunction. They note that these molecular changes lead to autonomic disturbances and an overwhelming pain response.
Koh et al. also present a review of CRPS. The authors stress that CRPS is a clinical diagnosis and one of exclusion. They discuss that CRPS is best treated within a multidisciplinary team including orthopaedic surgeons, pain management, therapy, and psychological services. Early diagnosis is furthermore critical. Finally, the authors advocated vitamin C administration on the day of fracture as prophylaxis against CRPS.
Incorrect answers:
A 65-year old male with worsening right hip osteoarthritis has failed nonsurgical management and would like to proceed with total hip arthroplasty. He has consulted with a pain management specialist and is treating his pain with opioids. If he is able to successfully decrease the amount of opioids he takes preoperatively by 50%, what effect would that have on his postoperative functional outcome?
Etanercept is a biologic disease modifying anti-rheumatic drug (DMARD) which works by binding and inhibiting TNF-a, in effect suppressing the autoimmune response associated with rheumatoid arthritis (RA).
There are a number of DMARDs commonly used in the medical management of RA. TNF- a is a frequent target, given its pivotal role as one of the major cytokines driving the progression of RA. Etanercept is one example of a TNF-a inhibitor that is often used to treat RA, juvenile RA, psoriatic arthritis, and ankylosing spondylitis. Infliximab, adalimimab, golimumab are other
commonly used TNF-a inhibitors. Before initiating these medications, patients and physicians should be aware of the possibility of reactivation of latent tuberculosis as well
as increased rates of infection and lymphomas with long- term use.
Saleh et al. reviewed the perioperative management of RA patients. They note that patients that are maintained on etanercept perioperatively have a significantly increased rate of perioperative infection. The authors discuss recommendations that etanercept be held at least one half-life prior to surgery and in some instances up to 4-5 half-lives before surgery. They recommend restarting the medication at 2 weeks post-operatively so long as the surgical sites are healing uneventfully.
Nikiphorou et al. evaluated the impact of biologic agents on the surgical treatment of RA. The authors discussed that although rates of major joint replacements (THA/TKA) for osteoarthritis are increasing, the rates of THA/TKA for RA has been essentially unchanged over >10 years. They concluded that effective medical management of RA has led to fewer orthopedic surgeries being performed in the RA population.
Incorrect Answers:
A 60-year-old female underwent open reduction and internal fixation of a distal radius fracture 3 weeks ago. She returns to your clinic and appears anxious. She complains of pain and difficulty sleeping. When you remove her splint her entire hand and wrist are sensitive. You suspect that she has developed complex regional pain syndrome (CRPS). All of the following are common signs or symptoms of CRPS EXCEPT:
All of the statements listed above are true EXCEPT for answer 2 - BMP-2 is not FDA indicated for single-level posterolateral lumbar fusions.
Bone morphogenetic proteins are a member of the TGF-beta superfamily. It is an osteoinductive material that induces mesenchymal stems cells to differentiate into bone- forming osteoblasts. There has been an increasing amount of literature published around its use in long bone procedures, spinal procedures, and nonunions. Currently, the FDA indications for rhBMP-2 are acute open tibial shaft fractures treated within 14 days and single level ALIFs with a lumbar tapered fusion device.
Hsu et al. authored a systematic review including 6 articles on the cost- effectiveness of BMP-2 compared to iliac crest bone graft (ICBG) in lumbar and cervical arthrodesis procedures. They conclude that in lumbar arthrodesis procedures BMP-2 is only cost- effective when taking into account societal costs such as productivity and lost wages.
Carreon et al. performed a cost-utility analysis on an RCT that they performed comparing BMP-2 to ICBG in posterolateral lumbar fusions. There are more complications, increased need for additional treatment and revision surgery in patients over 60 years old receiving ICBG compared with rhBMP-2/ACS, which account for an increased cost utility for the ICBG group.
Glassman et al., in the paper that the aforementioned study worked off of, performed an RCT of rhBMP-2/ACS (Infuse bone graft) versus iliac crest bone
graft (ICBG) for lumbar spine fusion in patients over 60 years of age. They conclude that BMP-2 is a viable ICBG replacement in older patients in terms of safety, clinical efficacy, and cost-effectiveness.
Cheng et al. looked at the osteogenic activity of fourteen different BMPs on mesenchymal progenitor cells. They found BMP-2, 6, and 9 induced high levels of alkaline phosphatase activity in pluripotent stem cells. They conclude BMP-
2, 6, and 9 may play important roles in inducing osteoblast differentiation of mesenchymal stem cells.
Illustration A (Cheng et al.) is a figure demonstrating the distinct osteogenic activity of human BMPs. BMP-2, 6, and 9 are the most potent agents to induce osteoblast lineage differentiation of mesenchymal progenitor cells while most BMPs can promote the terminal differentiation of committed osteoblast precursors.
Incorrect answers:
Which of the following medications specifically target tumor necrosis factor alpha (TNF-a)?
Fretting corrosion results from the relative micromotion between two affixed materials placed under a load and is characterized by the formation of pits,
grooves, and oxide debris. This may be seen at modular junctions.
The process of fretting corrosion involves the physical disruption of the passivated layer at the junction of two materials due to friction caused by micromotion under pressure.
The increased surface roughness and release of metallic oxide debris may then, in turn, lead to other types of corrosion such as crevice corrosion. Fretting corrosion has been described at the head-neck junction in total hip arthroplasty, and the risk is increased with an increasing number of component interfaces.
Brown et al. describe fretting corrosion within the context of modular hip tapers. The authors note that while modularity increases versatility, this comes at the cost of interfacial corrosion which may result in both device failure as well as the release of metal ions with local soft tissue reactions. They conclude that longer neck extension was associated with increased fretting corrosion
and that this can potentially be mitigated by increasing the stability of the interface.
Goldberg et al. performed in vitro corrosion testing of modular hip tapers. The authors found that once fretting corrosion created an environment suitable for crevice corrosion, corrosion continued regardless of continued mechanical loading. They concluded that mechanical loading had a significant impact on initiating the corrosion process.
Incorrect Answers:
temperature cycling causing rapid expansion/contraction of the metal. This may be a consideration during the manufacturing process of implants but is not seen in vivo.
When considering using recombinant human BMP-2 in orthopaedic surgery, all of the following are true EXCEPT:
The null hypothesis in this randomized controlled trial is that there is no difference in cement penetration during TKA with or without tourniquet use. As there was significant crossover (tourniquet use in the "no tourniquet" cohort), accepting the null hypothesis when it is false would result in beta (type 2) error.
In hypothesis testing, the assertion that the observed findings did not occur by chance alone but rather occurred because of a true association between variables is confirmed or rejected. By convention, the null hypothesis suggests that there is no significant association between variables while the alternative hypothesis suggests that there is a significant association. Alpha (type 1) error occurs when the null hypothesis is rejected
when it is, in fact, true (false positive effect). Beta (type 2) error occurs when the null hypothesis is
accepted when it is, in fact, false (false negative effect).
Kocher et al. reviewed power analyses, statistical errors, and the concept of statistical power. They discuss that beta represents the chance of a type II error, while alpha represents the chance of a type I error, and that conventionally beta is set at 0.2 and alpha at 0.05. The authors recommended that when a study observes no difference, the power of the study, or (1 - beta), should be reported.
Lochner et al. investigated the rates of beta error in randomized controlled trials in orthopedic trauma. They reported a 90% beta error rate in these trials, which exceeds accepted standards. The authors recommended that future authors perform pre-study power and sample-size calculations to
reduce these rates.
Illustration A shows a Bayesian analysis table demonstrating the relationship between alpha, beta, and the null hypothesis.
Incorrect Answers:
Which of the following types of corrosion is defined by the formation of pits, grooves, and oxide debris due to the relative micromotion between two affixed materials placed under a load?
Tobramycin is an aminoglycoside that acts primarily by disrupting protein synthesis through irreversibly binding to 30S ribosomal subunit, leading to altered cell membrane permeability, disruption of the cell envelope, and eventual cell death.
Exchange nailing with an antibiotic-impregnated intramedullary nail is often implemented in the treatment of chronic osteomyelitis with septic tibial nonunion as it provides both fracture stabilization and antibiotic elution. Vancomycin and tobramycin are often added to the polymethylmethacrylate (PMMA) cement for broad-spectrum coverage.
Vancomycin disrupts cell-wall synthesis in a time-dependent manner by binding to the D- Ala-D-Ala terminal of the growing peptide. It is extremely effective in gram-positive bacteria, but ineffective against gram-negative bacilli due to its large size. Conversely, tobramycin is effective against gram-negative organisms, and works chiefly through the inhibition of bacterial protein synthesis by irreversibly binding to the 30S ribosomal subunit.
Jaeblon et al. reviews the contemporary use of PMMA in orthopaedic surgery. The authors discuss the utility of PMMA as a delivery vehicle for antibiotics, eluting from both the surface and pores of the cement as well as the microcracks within it, while simultaneously eliminating dead space. They conclude that tobramycin is popular because it comes in powder form, which is easy to mix, and because of its broad spectrum activity, which includes antipseudomonal coverage. Moreover, it has been shown to potentiate the elution of other antibiotics, such as vancomycin.
McNamara et al. reviews the mechanism of Vancomycin. The authors report how this antibiotic has increased in importance in the last decade due to the growing resistance of many gram-positive bacteria to β-lactam antibiotics. They discuss that vancomycin is a large, complex, tricyclic glycopeptide molecule that works primarily through disruption of the biosynthesis of peptidoglycan, the major structural polymer of the gram-positive
bacterial cell walls, through binding to the D-alanyl-D-alanine terminal of cell wall precursor units. The authors conclude that unlike penicillins and cephalosporins, cross- resistance with vancomycin does not develop, because vancomycin acts against different stages of cell wall synthesis and different specific targets.
Nana et al. discusses the high affinity of microorganisms to adhere to foreign materials commonly used in orthopedics, including cobalt-chromium, titanium, polyethylene, and PMMA cement through the formation of biofilms. The
authors report that S. aureus and S. epidermidis are the most common biofilm-forming bacteria found in orthopedics, and, when combined with P. aeruginosa, they represent nearly 75% of biofilm infections. They conclude that while no current guidelines exist for treating these infections, recent studies have shown that biofilm growth can be fully inhibited when PMMA is mixed with both daptomycin and gentamicin.
Figures A and B are the AP and lateral radiographs of an infected nonunion of a tibial shaft fracture treated initially with an intramedullary nail.
Figure C is an axial CT image illustrating the tibial fracture nonunion.
Incorrect Answers:
A randomized controlled trial is undertaken to investigate whether tourniquet use increases cement penetration during total knee arthroplasty. Approximately 40% of the patients that were initially randomized to the "no tourniquet" group had tourniquets placed intraoperatively due to difficulty with visualization. Intent- to- treat analysis was conducted and the results showed no difference in the rates of cement penetration. What statistical term best applies if these results are accepted at face value?
Sclerostin is a direct antagonist of the Wnt/β-catenin pathway and thus a key regulator of the formation of mineralized bone matrix and bone mass. Anti- sclerostin antibodies result in inactivation of sclerostin, thereby promoting the anabolic Wnt/β-catenin pathway and resulting in INCREASED bone density
Sclerostin is a glycoprotein encoded by the SOST gene and produced primarily by osteocytes. It acts as a negative regulator of bone mass by directly antagonizing Wnt binding to the LRP5/6 receptor, thereby leading to β-catenin degradation and reduction of Wnt-target gene expression. This results in anti- anabolic properties, including inhibition of osteoblastic differentiation, bone formation, and loss of inhibition of osteoblast and osteocyte apoptosis. Genetic mutations resulting in loss of function or decreased expression of SOST have been linked to endosteal hyperostosis, increased bone mass, and increased bone density (as with Van Buchem disease and sclerosteosis). As a result, new immunotherapies targeting sclerostin (such as Romosozumab and
Blosozumab) are being investigated for their utility toward treating osteoporosis and have shown promising results.
Recker et al. presented a double-blinded phase 2 randomized controlled trial of blosozumab in the treatment of low bone mineral density in postmenopausal women. The authors found that administration of the monoclonal antibody resulted in significant dose- dependent increases in bone mineral density at the spine and hip. The authors concluded that the anti-sclerostin antibody was effective in the treatment of low bone mineral density in postmenopausal women.
Illustration A is a comparison of the unsuppressed Wnt pathway (left) with the Wnt- antagonized pathways (right). Sclerostin binds the LRP5/6 receptor in the place of Wnt, leading to the release of the destruction complex and β-catenin degradation. In the absence of sclerostin, the β-catenin translates into the nucleus and promotes downstream transcription of Wnt target genes.
Incorrect Answers:
sclerostin lead to an under- or uninhibited Wnt/β-catenin pathway and thereby INCREASED bone mass, such as would be seen in Van Buchem disease or sclerosteosis.
Figures A through C are the radiographs and CT scan of a 33- year-old male who was treated 13-months ago for an open tibial shaft fracture. He has received several courses of intravenous antibiotics for chronic osteomyelitis. Despite continued treatment with IV antibiotics, his inflammatory markers remain elevated. The decision is made to proceed with irrigation and debridement, nail removal with exchange for a polymethylmethacrylate intramedullary nail with vancomycin and tobramycin. What is the primary mechanism of action of tobramycin?
Lubricin is a hyaluronic acid-binding proteoglycan found in synovial fluid that reduces the coefficient of friction between the surfaces of the joint.
Lubricin reduces the friction between the surfaces in the joint, leading to decreased shear forces transmitted to the hyaline cartilage. It is a glycoprotein that is produced by the chondrocytes in the superficial zone and is not a primary component of the extracellular matrix. A deficiency in lubricin has
been associated with early-onset arthritis.
Schumacher et al. first discovered what is now known to be "lubricin" by studying the superficial zone of bovine articular cartilage. The authors noted that the chondrocytes in this zone secreted this proteoglycan. In addition, they found that this molecule, or a very similar molecule, was present in synovial fluid and moreover could serve as a functional metabolic marker for chondrocytes of the superficial zone of articular cartilage.
Jay et al. analyzed the synovial fluid in both normal and lubricin-deficient samples and found that the subdiffusive and elastic behavior of synovial fluid, at physiological shear rates, was absent in fluid from a patient who lacked lubricin. They concluded that lubricin provided synovial fluid with an ability to dissipate strain energy induced by physiologic motion, which is a chondroprotective feature distinct from boundary lubrication.
Incorrect Answers:
osteoblastogenesis.
Which of the following is accurate regarding sclerostin?
In the days following an intra-articular injury, the following substances are produced, contributing to articular cartilage damage and the eventual formation of post-traumatic arthritis: IL-1ß, TNF-a, nitric oxide, matrix metalloproteinases, aggrecans, and damage-associated molecular patterns.
Immediately following an intra-articular fracture, there is mechanical damage and necrosis of articular cartilage. Traditionally, orthopaedic surgeons are
taught that the most critical factor in affecting the outcomes of these patients is the accuracy of the articular reduction and restoration of the mechanical alignment. However, even in expertly reduced fractures, some patients experience poor outcomes and develop progressive, debilitating osteoarthritis. More recently, researchers have looked at inflammatory events that may also contribute to arthritis and ways to modulate these events.
Olson et al. provide a review article on the role of cytokines in post-traumatic arthritis. They note that, despite accurate articular reductions, many patients go on to develop
arthritic changes, often indistinguishable from primary OA. While mechanical alignment and structural damage are sometimes responsible, the cascade of cytokines and other signaling molecules listed above serve to catalyze these intra-articular events; developing ways to blunt this inflammatory response is of great interest.
Lewis et al. examined the relationship of inflammatory and post-traumatic arthritis in a rodent model. Tibial plateau fractures were induced in C57BL/6 and MRL/MpJ "superhealer" mice, which were killed at different time-points. Synovial fluid was inspected post-mortem for cytokine analysis, as well as gross specimens, and it was determined that an association exists between joint tissue inflammation and the development and progression of post- traumatic arthritis in mice.
Figure A is an XR of a tibial plateau fracture. Figure B is an XR of a knee demonstrating post-traumatic arthritis. Illustration A is a table of several cytokines and their functions. Illustration B is a timeline of intra-articular pathogenic events following an injury. Illustration C is a diagram showing various cellular events and pathogenic mechanisms in the acute aftermath following an intra-articular injury.
Incorrect Answers:
blood vessels, IL-8 is chemotactic, BMP2 plays a role in the development of bone and cartilage, BMP5 plays a role in cartilage development, and M-CSF causes hematopoietic stem cells to differentiate into macrophages or other related cells.
A 45-year-old patient presents to your clinic for evaluation of knee pain. He has been told he has osteoarthritis and has significant pain with knee range of motion. Which of the following components of synovial fluid is most responsible for reducing the coefficient of friction in a native knee joint?
This player has sustained a tear of the medial collateral ligament (MCL). The MCL is a ligament which inserts indirectly into bone through Sharpey's fibers.
Ligaments can insert on bone either indirectly and directly. Indirect is the most common and is a fibrous insertion. The superficial fibers of the tendon insert into the periosteum, while the deep fibers insert directly into the bone. These
deep fibers are called Sharpey's fibers and are made of type I collagen. The direct insertion has both deep and superficial fiber insertions as well. Direct insertions are fibrocartilaginous and consist of four transitional zones of increasing stiffness that allow force dissipation.
Lu et al. performed a review to determine the functional attachments of soft tissue to bone. They report that a specialized interface, called an insertion site or enthesis, integrates
tendon or ligament to bone and serves to facilitate joint motion. Fibrous (indirect) insertions typically occur over large areas, presumably to distribute force and reduce stress, and are characterized by perforating mineralized collagen fibers.
Cole et al. performed a review of fixation of soft tissues to bone. They report that recreation of the enthesis relies on adequate biologic healing afforded by adequate initial fixation. The healing pattern associated with direct soft–tissue- to-bone repair, such as rotator cuff repair, is different from that associated
with fixation within bone tunnels (ex. ACL reconstruction). The process of tendon healing within osseous tunnels occurs over time.
Lui et al. performed a review of the biology and augmentation of tendon-bone insertion repair. They report that when a ligament runs parallel to the bone, like the MCL, the insertion is more likely to be indirect. When a ligament enters the bone perpendicularly, such as the ACL, the insertion is direct. Indirect insertions may be elevated off the bone without cutting the ligament itself while direct insertions require cutting the substance of the ligament to detach it.
Figure A is a T2-weighted, coronal MRI demonstrating a tear of the MCL. Illustration A is a polarized photomicrograph demonstrating Sharpey fibers, indicated by the white arrows. G represents tendon, while B represents bone (Liu et al.). Illustration B is a Safranin-O-staining photomicrograph of a direct tendon insertion site (Liu et al.).
Illustration C is an H&E photomicrograph of the same direct tendon insertion site (Liu et al.). B represents bone, CFC represents calcified fibrocartilage, UCFC represents uncalcified fibrocartilage, and T represents tendon.
Incorrect Answers:
A 32-year-old male sustains the injury shown in Figure A. He undergoes surgical fixation with subsequent removal of hardware. He does well for 10 years and then presents to your office with increasing left knee stiffness and pain for the last 6 months. He reports no constitutional symptoms or recent trauma. His physical exam is notable for well-healed incisions, a mild effusion, no ligamentous instability, and 5-100 degrees of range of motion. An XR is obtained and shown in Figure B. Which of the following correctly lists the cytokines produced following the initial injury that may contribute to the findings shown in Figure B and the patient's current symptoms?
imaging is shown in Figure A. Which of the following correctly classifies the injured structure and its indirect insertion into bone?
Hypertrophic nonunions are described as having abundant callous formation without bony bridging at the fracture site and rarely require an increase in bone biology to achieve fracture healing.
A nonunion is defined as a fracture that has not healed and has no further capacity to heal without further intervention. Nonunions are typically classified as hypertrophic, oligotrophic, and atrophic. Hypertrophic nonunions show clear
evidence of ability to heal without bridging of fracture gaps. Atrophic nonunions show no evidence of biologic healing and no bridging of fracture gaps. Oligotrophic nonunions tend to fall somewhere in between hypertrophic and atrophic nonunions with some evidence of biologic activity however incomplete healing. Understanding these characteristics allows for proper identification of the nonunion and selection of appropriate intervention with regard to increasing bone biology and fracture stability to achieve healing.
Bishop et al. review the diagnosis and assessment of delayed bone healing through a systematic approach to help surgeons determine appropriate interventions to achieve healing. They state biologic capacity, fracture stability, deformity, infection, and host status should all be considered closely prior to establishing a plan of management for a nonunion.
Babhulkar et al. reviewed 113 patients diagnosed and treated for nonunions including 61 hypertrophic and 52 atrophic nonunions. They found all patients healed with improved function and pain following treatment of their nonunions. They found residual problems related to joint stiffness, limb length
discrepancy, and angular deformity.
Illustration A shows a hypertrophic nonunion of a tibial shaft fracture treated nonoperatively. Illustration B shows an atrophic nonunion following open reduction internal fixation of a humeral shaft fracture.
Incorrect Answers:
A 20-year-old male collegiate football player sustained a knee injury. His
The arrow is pointing to the superficial zone of articular cartilage in Figure A. The superficial zone of articular cartilage has the highest content of collagen and the lowest content of proteoglycans relative to the other zones.
Normal articular cartilage can be divided into 3 zones and the tidemark based on the shape of the chondrocytes and the orientation of the type II collagen. The zones, in order from closest to the joint surface, are superficial zone, intermediate (transitional) zone, and deep zone. The superficial zone has the highest content of collagen and lowest content of proteoglycans of all the zones; in contrast, the deep zone has the lowest content of collagen and the highest content of proteoglycans. The intermediate zone has amounts of collagen and proteoglycans that reside between those found in the superficial and deep zones.
Ulrich-Vinther et al. reviewed the biology of articular cartilage. They noted three distinct zones of articular cartilage that are separated from the subchondral bone by the tidemark. The authors noted that tissue engineering approaches are being used in an effort to regenerate damaged articular cartilage due to injury or aging.
Jeffery et al. studied the three-dimensional architecture of bovine articular cartilage with scanning electron microscopy. They noted that the collagen was ordered in different morphologies in each zone of articular cartilage. The authors concluded that the three- dimensional organization of collagen is important when considering cartilage structure and function.
Illustration A demonstrates the zones of articular cartilage and their spacial relationship. Illustration B shows the relationship between collagen and proteoglycans
within articular cartilage.
Incorrect Answers:
While planning for revision of a failed open reduction internal fixation you are planning to increase mechanical stability across the fracture site. In addition to addressing stability, which of the following fracture scenarios is least likely to require additional bone biology in order to achieve healing?
A is characterized by:
PROMIS is a useful orthopaedic patient-reported outcomes measure (PROM) that can assess disease specific and general health questions, validated for use in foot and ankle, upper extremity, and spine patients.
Multiple tools have been developed to asses patient-reported outcomes, however, some of these are narrow in scope, cumbersome to administer, and less useful in orthopedics. PROMIS was developed by a team of NIH researchers to address these shortcomings. Domains include physical, mental, and social health. PROMIS utilizes computer adaptive testing software (CAT), allowing for fewer questions and more accurate measurements. Additionally, results are reported as T-scores, allowing for easy interpretation.
Brodke et al. provide an overview of PROMIS. They report that this tool was developed to be easy to administer and broad in scope, utilizing item response theory. This validated tool is reliable in assessing specific function of the upper and lower extremities, as well as underlying health traits.
McCormick et al. described PROM used in spine surgery. They reinforce that the benefit of PROM is to gather insight into subjective measures not typically captured in traditional research, looking at such factors as general health quality, function, and pain. The authors also note the importance of these tools as greater emphasis is placed on quality of care and patient experience.
Godil et al. studied instruments to accurately measure quality and outcomes in lumber spine surgical registries. They conducted a prospective cohort study of
58 patients undergoing TLIF for lumbar degenerative spondylolisthesis and administered several PROs. They concluded that the ODI was the best measure assessing pain and disability in lumbar surgery, citing its validity and responsiveness in measuring the effectiveness of lumbar fusion; EuroQOL-5D (EQ-5D) was found to be the best, the most valid, and responsive measure of improvement for health-related quality of life.
Illustration A is a chart depicting the main domains and subcategories analyzed with PROMIS.
Incorrect Answers:
The layer of articular cartilage that the arrow points to in Figure
As part of the World Health Organization (WHO) Surgical Safety Checklist, all of the answers listed are methods to prevent wrong-site surgery EXCEPT marking an "X" on the operative extremity. Patients should be marked unambiguously, with either a "yes" or the surgeon's initials in permanent marker, prior to induction of anesthesia.
The WHO developed the Surgical Safety Checklist in an effort to improve the safety of patients undergoing surgery. Implementation of this checklist has resulted in improved clinician safety attitudes, as well as decreased patient morbidity and mortality. A time-out or group huddle occurs prior to induction with the patient, prior to incision, and prior to the patient leaving the operating room; all team members have an opportunity to speak up and discuss any concerns during this process. The American Academy of Orthopaedic Surgeons suggest the following to prevent wrong-site surgery: Surgical team engagement, patient confirmation, signing the surgical site (in the visible
surgical field or inline with the planned incision) with a permanent marker with the patient's assistance, and utilizing separate time-outs in the case of separate surgical procedures/sites.
Haynes et al. looked at changes in safety attitude, morbidity, and mortality following implementation of the WHO Surgical Safety Checklist. They administered a survey pre- and post-intervention at 8 hospitals. Post- intervention, they found an overall improvement in safety attitudes and found that this was correlated with a reduction in post-operative complication rates.
Gillespie at al. reviewed the evidence of implementing a surgical safety checklist. They utilized a realist synthesis methodology in this study. They concluded that intervention methods and implementation strategies were not well described in the literature, surgical checklists appear to be more successful when physicians are leading their implementation, and that greater participation and ownership of safety checklists can be expected by physicians are actively engaged in their development and implementation.
Illustration A is the WHO Surgical Safety Checklist. Illustration B is an example of the correct way to mark a patient for a right shoulder surgery for a planned deltopectoral incision.
Incorrect Answers:
Which of the following instruments incorporates both general disease and disease-specific measures and has been validated for use in patients with spine, foot and ankle, and upper extremity conditions?
This patient has a catastrophic ceramic component failure and requires a thorough debridement and revision with a head and liner exchange.
Ceramic bearings in hip arthroplasty are recognized for their superior wear properties and low-friction. However, ceramics are also brittle, have a high modulus of elasticity, and are prone to fracture under certain circumstances. Catastrophic bearing failure is not as common in newer-generation ceramics, as first-generation products were more prone to failure due to flaws in the manufacturing process. Squeaking is a known complication of ceramic-on- ceramic bearings and may be associated with catastrophic failure. Obesity, trauma, and component malposition have been linked to failure, and revision procedures should address any component malposition.
Malem et al. describe a case report of a catastrophic ceramic-on-ceramic total hip replacement failure presenting as a squeaking hip. Within 5 years of her index surgery, the patient developed a painful, squeaking hip with a limited range of motion. At the time of revision, she was found to have a broken femoral head, black wear debris, and a completely worn acetabular component, suggesting that a squeaking ceramic-on-ceramic hip replacement may be a sign of catastrophic failure.
Stanat et al. provide a meta-analysis and review of squeaking in 3rd and 4th generation ceramic-on-ceramic total hip replacements. They conclude that the only significant patient- associated risk factor for squeaking was body mass index. In terms of implant type and surgical factors, they found that the presence of a Stryker Accolade stem was associated with an increased incidence of squeaking; cup version was not associated with a higher incidence of squeaking in their analysis.
Figure A is a radiograph demonstrating ceramic fracture and displacement of the femoral component in relation to the acetabular component; ceramic fragments are present around the femoral neck and cup. The partially radiolucent head is a tip-off to the older generation ceramics. Illustration A is an intra-operative photograph demonstrating a fractured ceramic femoral head. Illustration B is a revision of the hip in Figure A utilizing ceramic-on- ceramic components. Illustration C (Traina et al.) is a treatment algorithm when ceramic bearing failure is suspected.
Incorrect Answers:
All of the following can be done to improve patient safety and prevent wrong site surgery EXCEPT:
Nitrogen-containing bisphosphonates exert their action by inhibiting farnesyl pyrophosphate synthase.
Nitrogen-containing bisphosphonates inhibit osteoclasts which leads to increased bone mass and reduced bone turnover. They act on the cholesterol biosynthesis pathway enzyme, farnesyl pyrophosphate synthase. By inhibiting this enzyme in the osteoclast, they interfere with geranylgeranylation (attachment of the lipid to regulatory proteins), which causes osteoclast inactivation. Non-nitrogen containing bisphosphonates are metabolized in the cell to compounds that replace the terminal pyrophosphate moiety of ATP, forming a nonfunctional molecule that competes with ATP in the cellular energy metabolism. Due to this disruption in metabolism, the osteoclast
initiates apoptosis and dies, leading to an overall decrease in the breakdown of bone. Examples of nitrogen-containing bisphosphonates are alendronate, risedronate, pamidronate, and zolendronate. Examples of non-nitrogen containing bisphosphonates are tiludronate, clodronate, etidronate.
Reszka et al. performed a review of bisphosphonates. They report that they bind to the bone mineral, which localizes their action to the target tissue. They are rapidly cleared from the circulation via renal excretion, which minimizes exposure of all other organs.
They do not easily penetrate cell membranes, which reduces exposure to non-target tissues. They also report that alendronate and risedronate are the only pharmacologic agents shown to prevent spine and nonvertebral fractures associated with postmenopausal and glucocorticoid-induced osteoporosis.
Luo et al. performed a systematic review to determine the efficacy and safety of alendronate for adult AVN treatment. They found most studies suggested a positive short-term efficacy of alendronate treatment in reducing pain, improving articular function, slowing of bone collapse progression, and delaying the need for arthroplasty. There were no severe adverse effects associated with alendronate treatment observed and most of the included studies suggested the use of alendronate in early AVN with a small necrotic lesion to achieve better outcomes.
Illustration A (Reszka et al.) details the nitrogen and non-nitrogen containing bisphosphonates and their chemical structures. Illustration B is the mevalonate pathway, showing the action of a nitrogen-containing bisphosphonate.
Incorrect Answers:
A 60-year-old patient presents to clinic complaining of left hip squeaking and stiffness following a ceramic-on-ceramic total hip replacement five years earlier. Initially, he was extremely pleased with the operation, but these symptoms of squeaking and stiffness have developed fairly abruptly over the past 6 months. On physical exam, he has a well-healed incision, a 1 centimeter leg length discrepancy (left shorter than right), decreased hip flexion, and decreased internal rotation. A radiograph is shown in Figure A. C- reactive protein is 0.2 mg/dL (nl <0.9 mg/dL) and erythrocyte sedimentation rate is 5 mm/hr (nl 0-15 mm/hr). What would you recommend for this patient?
in the red box?
Aspirin inhibits the aggregation of platelets, which are shown in Figure C.
The coagulation cascade is a complex interaction of multiple clotting factors which ultimately leads to the aggregation of platelets to form a clot. The end result of the clotting cascade leads to the conversion of prothrombin to thrombin, causing the formation of fibrin and the subsequent aggregation of platelets in a clot. Aspirin irreversibly blocks the formation of thromboxane A2 in platelets, which inhibits platelet aggregation and thus the formation of a clot.
Hyers reviewed the mechanism of action of various anticoagulants and the pathophysiology of venous thromboembolism. He noted that while deep vein thrombosis and pulmonary embolism resulted in significant morbidity and mortality in the United States, novel anticoagulants have recently been developed that hold promise for new therapeutic options.
Brown pooled the results of 14 randomized controlled trials examining venous thromboembolism (VTE) rates. Their analysis showed that VTE rates were not significantly different when aspirin was used for anticoagulation compared with vitamin K antagonists or low molecular weight heparin (LMWH). The authors concluded that aspirin could be used for VTE prophylaxis after major orthopaedic surgery.
Figure A shows a plasma cell. Figure B shows a neutrophil. Figure C shows arrows pointing to platelets in a peripheral blood smear. Figure D features a basophil, and figure E shows an osteoclast. Illustration A shows the mechanism of action of aspirin.
Incorrect Answers:
A man with osteonecrosis of the hip is treated with a medication which inhibits the pathway shown in Figure A. Which of the following medications best matches this mechanism of action of the medication
Demineralized bone matrix (DBM) is both osteoconductive and osteoinductive.
DBM is made from the acidic extraction of bone matrix from allograft. It removes the minerals and leaves the collagenous and noncollagenous structure and proteins. It is osteoconductive and osteoinductive as it contains collagen, bone morphogenic proteins (BMPs), transforming growth factor-beta (TGF-β), and residual calcium. It does not contain mesenchymal precursor cells or impart structural support.
Ripamonti et al. performed a review of regenerative medicine and tissue engineering of bone. They report that the understanding of bone formation by autoinduction has been pivotal for setting the rules for tissue engineering. An extracellular matrix combined with TGF-β is capable of performing this task.
Grabowski et al. review bone graft and bone graft substitutes. They report that DBM is both osteoinductive and osteoconductive. DBM provides varying degrees of osteoconductive potential based on the carrier material chosen.
They also report that given the techniques used for demineralization are proprietary, the actual techniques are not published, and the process is not regulated. They conclude that the actual concentration of BMPs is varied when comparing various lots of the same preparation.
Figure A is a coronal CT slice demonstrating a depression fracture of the lateral tibial plateau.
Incorrect Answers:
Aspirin exerts its primary effect on which of the following cells (identified by black arrows)?
FOR ALL MCQS CLICK THE LINK ORTHO MCQ BANK
Question 14
A 10-year-old boy with severe hemophilia A (factor VIII) sustained an injury to his right forearm 2 hours ago when a classmate fell on his arm during a scuffle. Examination reveals moderate swelling in the forearm, decreased sensation in the distribution of the median and ulnar nerves, and pain on passive extension of the fingers. What is the most appropriate sequence of treatment?
Explanation
REFERENCES: Greene WB: Diseases related to the hematopoietic system, in Morrissy RT, Weinstein SL (eds): Lovell & Winter’s Pediatric Orthopaedics, ed 4. Philadelphia, Pa, Lippincott-Raven, 1996, pp 345-391.
Greene WB, McMillan CW: Nonsurgical management of hemophilic arthropathy, in Barr JS (ed): Instructional Course Lectures 38. Park Ridge, Ill, American Academy of Orthopaedic Surgeons, 1989, pp 367-381.
Naranja RJ Jr, Chan PS, High K, Esterhai JL Jr, Heppenstall RB: Treatment considerations in patients with compartment syndrome and an inherited bleeding disorder. Orthopedics 1997;20:706-711.
Question 15
A 23-year-old woman with a history of bilateral recurrent ankle sprains, progressive cavovarus feet, and a family history of high arches and foot deformities is seen for evaluation. Management consisting of bracing and physical therapy has been poorly tolerated. Heel varus is partially corrected with a Coleman block. There are thick calluses under the first metatarsal heads. Sensation to touch and Weinstein monofilament is normal. Tibialis anterior and peroneus brevis are weak but present. What is the most appropriate management?
Explanation
REFERENCES: Younger AS, Hansen ST Jr: Adult cavovarus foot. J Am Acad Orthop Surg 2005;13:302-315.
Sammarco GJ, Taylor R: Cavovarus foot treated with combined calcaneus and metatarsal ostetotomies. Foot Ankle Int 2001;22:19-30.
Richardson EG (ed): Orthopaedic Knowledge Update: Foot and Ankle 3. Rosemont, IL,
American Academy of Orthopaedic Surgeons, 2003, pp 135-143.
Question 16
An anterior approach to the sacroiliac joint is indicated with which of the following concomitant injuries?

Explanation
Question 17
A 14-year-old gymnast presents after a fall from the balance beam with a hyperextension injury to her left knee. She could ambulate with pain but was unable to continue exercise due to pain. On examination she has a swollen knee with painful
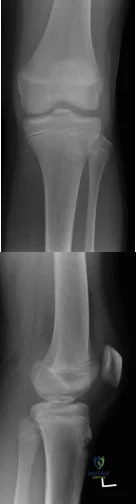
Explanation
Tibial eminence fractures are rare but occur more often in pediatric populations, often in the setting of sports-related injuries. Debate continues over operative vs nonoperative treatment, as well as fixation type (screw vs suture) for openly treated fractures. Past evidence suggested closed treatment was adequate but there has been an increase in operative management. Closed treatment is suggested for minimally displaced fractures (Type I and reducible Type II) and open treatment for completely displaced fractures (non-reducible Type II and Type III).
Wilfinger et al provide the results of a closed reduction protocol at their institution including 38 patients with long term followup. All patients underwent aspiration and closed reduction in the OR under fluoroscopic guidance followed by long leg casting in hyperextension and graduated weight bearing over weeks. No patients complained of persistent pain, swelling, giving way, or disability at follow up.
However, Edmonds et al in a retrospective review compare open reduction internal fixation (ORIF), arthroscopic-assisted internal fixation (AAIF), and closed reduction with casting (CRC) for pediatric patients with displaced tibial spine fractures. They report improved reduction but also increased arthrofibrosis in ORIF and AAIF groups
compared to CRC, but of the 24% of patients with long term followup results, there was no difference in functional outcomes across all 3 groups. There was a 17% rate of later operation for the CRC group patients. They suggest closed treatment for fractures with <5mm displacement, otherwise ORIF or AAIF.
Gans et al conducted a systematic review focused on the questions of open vs closed reduction, and screw vs suture fixation. The 26-article review found insufficient evidence to have any clear recommendations. They did find reduced laxity and improved range of motion for minimally displaced fractures that had an open reduction, and that completely displaced fractures treated nonoperative had higher rates of nonunion.
Figures A and B are AP and lateral knee radiographs demonstrating a moderately displaced (Meyers and McKeever Type II) tibial spine fracture in a skeletally immature patient.
Incorrect Responses
Question 18
Figures 163a through 163c show the radiograph and MRI scans of a 45-year-old woman with severe right arm pain. She has had symptoms for 6 months without resolution despite multiple nonsurgical treatments. Examination reveals weakness in the right triceps and wrist flexors with decreased sensation in the middle finger and a positive Spurling's sign. What is the most appropriate treatment for the patient's symptoms? Review Topic
Explanation
Question 19
A 78-year-old man has a history of worsening bilateral calf pain with activity. MRI scans are shown in Figures 31a through 31d. His symptoms are not improved with forward flexion of the lumbar spine. His lower extremity pain is relieved when he sits or ceases activity. Which of the following tests would be most helpful in establishing a diagnosis? Review Topic
Explanation
Decreased range of motion and hip joint pain, especially in internal rotation and abduction, are common findings in patients with degenerative arthritis of the hip. While post-myelography CT has been found superior to MRI as a single study for the preoperative planning of decompression for lumbar spinal stenosis, it will not assist in differentiating vascular from neurogenic claudication.
Question 20
In obstetrical brachial plexus palsy, which of the following signs is associated with the poorest prognosis for recovery in a 2-month-old infant?
Explanation
REFERENCES: Clarke HM, Curtis CG: An approach to obstetrical brachial plexus injuries. Hand Clin 1995;11:563-581.
Narakas AO: Injuries to the brachial plexus, in Bora FW (ed): The Pediatric Upper Extremity: Diagnosis and Management. Philadelphia, PA, WB Saunders, 1986, p 247.
Question 21
Plate fixation of olecranon fractures is recommended over tension band wire fixation when
Explanation
Question 22
A 50-year-old woman has a painful hallux valgus and a painful callus beneath the second metatarsal head. A radiograph is shown in Figure 46. To correct these problems, treatment of the great toe deformity should consist of
Explanation
REFERENCE: Sangeorzan BJ, Hansen ST Jr: Modified Lapidus procedure for hallux valgus. Foot Ankle 1989;9:262-266.
Question 23
An active 60-year-old man is evaluated 4 years following surgical correction of a hallux valgus deformity. The patient reports that a hallux varus deformity developed rapidly following his initial surgery. Conservative management consisting of wider shoes, toe strapping, and anti-inflammatory drugs has failed to provide relief. Examination reveals a hallux varus deformity with restricted painful motion of the metatarsophalangeal joint and callus formation under the second metatarsal head. What is the next most appropriate step in management?
Explanation
REFERENCES: Kitaoka HB, Patzer GL: Arthrodesis versus resection arthroplasty for failed hallux valgus operations. Clin Orthop 1998;347:208-214.
Ouzounian TJ: Metatarsophalangeal arthrodesis for salvage of failed hallux valgus surgery. Foot Ankle Clin 1997;2:741-752.
Question 24
Figure 54 is the lateral radiograph of a 55-year-old man who is evaluated for a 2-year history of pain and stiffness of his right metatarsophalangeal (MTP) joint. Upon examination he has dorsal bossing, severe crepitation, and pain with passive range of motion. There is pain with the "grind" test. Dorsiflexion is limited to 0 degrees. No sesamoid tenderness is present. What is the most appropriate surgical treatment?
Explanation
The radiograph reveals end-stage degenerative changes of the first MTP joint with a dorsal loose body. MTP arthritis and decreased joint dorsiflexion is referred to as hallux rigidus. A chevron bunionectomy is used to correct hallux valgus deformity without arthritis. The cheilectomy is used in lesser degrees of joint destruction. Resection of the proximal phalanx results in a floppy toe and is generally not recommended.
RECOMMENDED READINGS
McNeil DS, Baumhauer JF, Glazebrook MA. Evidence-based analysis of the efficacy for operative treatment of hallux rigidus. Foot Ankle Int. 2013 Jan;34(1):15-32. doi: 10.1177/1071100712460220. Review. PubMed PMID: 23386758.
View Abstract at PubMed
Deland JT, Williams BR. Surgical management of hallux rigidus. J Am Acad Orthop Surg. 2012 Jun;20(6):347-58. doi: 10.5435/JAAOS-20-06-347. Review. PubMed PMID: 22661564.
View Abstract at PubMed
CLINICAL SITUATION FOR QUESTIONS 55 THROUGH 58
Figures 55a and 55b are the anteroposterior and lateral radiographs of a 57-year-old man who fell off of a ladder 10 days ago and landed on his left foot. He is now unable to weight bear on the left. He has no history of trauma to this foot, and his medical history is unremarkable. Upon examination his left foot is swollen and tender. Pulses and sensation are intact.
A B
Question 25
What imaging study should be obtained next to further evaluate this patient? Review Topic
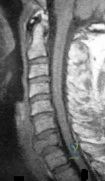
Explanation
Question 26
An adult patient with a grade I isthmic spondylolisthesis at L5-S1 is most likely to have weakness of the
Explanation
REFERENCES: Spivak JM, Connolly PJ (eds): Orthopaedic Knowledge Update: Spine 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2006, pp 311-317.
Lauerman WC, Cain JE: Isthmic spondylolisthesis in the adult. J Am Acad Orthop Surg 1996;4:201-208.
Question 27
-What is the most appropriate initial treatment?
Explanation
Based upon the history and description of the wound, this patient has sustained a frostbite injury to the anterior skin without evidence of infection. Frostbite, a thermal injury to local tissues, can be classified into first-, second-, third-, and fourth-degree injuries. First-degree injuries are characterized by a central whitish area surrounded by erythema. Second- and third-degree injuries are characterized by blisters that appear within the first 24 hours. Second-degree blisters are clear or cloudy, while third-degree blisters are hemorrhagic. Fourth-degree injuries are characterized by tissue necrosis. Treatment of a frostbite injury should begin as soon as it is identified, even if severity has not been determined. Treatment includes protection against mechanical irritation and keeping the injured area away from heat. The limb should be elevated and clear blisters debrided; dark blisters should be drained but not debrided. Topical treatment includes aloe application every 6 hours (silver sulfadiazine for open wounds). Nonsteroidal anti-inflammatory drugs can be given along with PCN G (500,000 U) or clindamycin (600 mg) IV every 6hours for 48 to 72 hours as prophylaxis against infection.Multiple skin incisions on the front of the knee place the skin at healing risk after surgery.
Skin oxygenation is further compromised by a lateral release, which disrupts the superior lateral geniculate artery in the peripatellar vascular anastomosis. When addressing compromised perfusion to the skin, the orthopaedic surgeon may consider not performing a lateral release, using the medial parapatellar incision,and/or not using a tourniquet during surgery. In this patient, the use of cold therapy further compromised perfusion to the skin. This patient’s wound does not reflect infection, but rather frostbite from the compromised skin perfusion and the application of cold therapy.
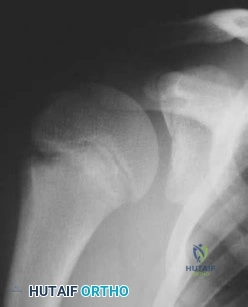
The physiologic responses to the effects of freezing temperatures on limbs have been categorized into 4 phases. Phase I, cooling and freezing, is characterized by vasoconstriction and vasospasm. The freezing results in mechanical destruction of cell membranes in endothelial cells in small capillaries. Phase II,rewarming, initiates as heat absorbed by the limb begins an exothermic reaction as extracellular and intracellular crystals melt. Intracellular swelling occurs and small capillaries become highly permeable,resulting in extravasation of fluid and causing edema and blisters. Phase III is characterized by progressive tissue injury resulting from inflammation, vascular stasis, and thrombosis leading to ischemia.Phase IV is recovery that can progress along 3 potential pathways: complete healing, healing with later sequelae, or early tissue necrosis leading to gangrene.
CLINICAL SITUATION FOR QUESTIONS 85 THROUGH 87
Figure 85 is the radiograph of a 13-year-old right-handed baseball player who has experienced 2 months of right-dominant shoulder pain. As a pitcher, he says he cannot “throw hard” without pain, and he develops a dull ache if he throws more than 15 pitches.
Question 28
Fixed hyperextension of the metatarsophalangeal joint is associated with
Explanation
REFERENCES: Marks RM: Anatomy and pathophysiology of lesser toe deformities. Foot Ankle Clin 1998;3:199-213.
Myerson MS, Shereff MJ: The pathological anatomy of claw and hammer toes. J Bone Joint Surg Am 1989;71:45-49.
Question 29
A 45-year-old man sustains a low-velocity gunshot wound to the base of the right thumb. The open wound is allowed to heal by secondary intention, resulting in a contracture of the first web space. Clinical photographs are shown in Figures 49a through 49c. Treatment should now consist of
Explanation
REFERENCES: Buchler U, Frey HP: Retrograde posterior interosseous flap. J Hand Surg Am 1991;16:283-292.
Brunelli F, Valenti P, Dumontier C, et al: The posterior interosseous reverse flap: Experience with 113 flaps. Ann Plast Surg 2001;47:25-30.
Question 30
When the elbow is extended and an axial load is applied, what percent of stress distribution occurs across the ulnohumeral and radiohumeral articular surface, respectively?
Explanation
REFERENCES: Halls AA, Travill R: Transmission of pressure across the elbow joint. Anat Rec 1964;150:243.
Morrey BF (ed): The Elbow and Its Disorders, ed 3. Philadelphia, PA, WB Saunders, 2000.
Question 31
While lifting weights, a patient feels a pop in his arm. He has the deformity shown in Figure 30. If left untreated, the patient will have the greatest deficiency in
Explanation
REFERENCES: Baker BE, Bierwagen D: Rupture of the distal tendon of the biceps brachii: Operative versus non-operative treatment. J Bone Joint Surg Am 1985;67:414-417.
D’Arco P, Sitler M, Kelly J, et al: Clinical, functional, and radiographic assessments of the conventional and modified Boyd-Anderson surgical procedures for repair of distal biceps tendon ruptures. Am J Sports Med 1998;26:254-261.
Pearl ML, Bessos K, Wong K: Strength deficits related to distal biceps tendon rupture and repair: A case report. Am J Sports Med 1998;26:295-296.
Question 32
What is the most likely cause of recurrent symptoms following excision of a third web space neuroma?
Explanation
REFERENCES: Beskin JL: Recurrent interdigital neuromas, in Nunley JA, Pfeffer GB, Sanders RW, Trepman E (eds): Advanced Reconstruction: Foot and Ankle. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2004, pp 481-484.
Amis JA, Siverhus SW, Liwnicz BH: An anatomic basis for recurrence after Morton’s neuroma excision. Foot Ankle 1992;13:153-156.
Question 33
During a knee arthroscopy on a 38-year-old patient with isolated medial knee pain and no lateral symptoms, a routine examination of the lateral compartment reveals a discoid lateral meniscus. The discoid lateral meniscus is not torn. Based on these findings, what is the most appropriate action? Review Topic
Explanation
Question 34
A 10-year-old girl who is Risser stage 0 has back deformity associated with neurofibromatosis type 1 (NF1). She has no back pain. Examination shows multiple cafe-au-lait nevi with normal lower extremity neurologic function and reflexes. Standing radiographs of the spine show a short 50-degree right thoracic scoliosis with a kyphotic deformity of 55 degrees (apex T8). A 10-degree progression in scoliosis has occurred during the past 1 year. There is no cervical deformity. MRI shows mild dural ectasia, primarily in the upper lumbar region. Management should consist of Review Topic
Explanation
Question 35
-A 42-year-old woman has had right wrist pain for 2 years. She tried splint wear and naproxen and has had 3 steroid injections, each time experiencing less relief.
Explanation
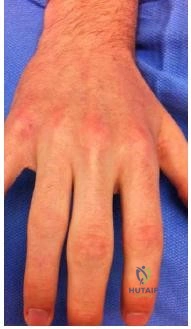
Question 36
Figures 46a through 46e show the radiographs of a 22-year-old man who injured his wrist in a motorcycle accident. He has no other injuries. What is the best course of action?
Explanation
REFERENCES: Dumontier C, Meyer ZU, Reckendorf G, et al: Radiocarpal dislocations: Classification and proposal for treatment: A review of twenty-seven cases. J Bone Joint Surg Am 2001;83:212.
Bilos ZJ, Pankovich AM, Yelda S: Fracture-dislocation of the radiocarpal joint: A clinical study of five cases. J Bone Joint Surg Am 1977;59:198-203.
Question 37
14A 14B An 18-year-old man was involved in an altercation during which he sustained the injuries shown in Figures 14a and 14b. His Glasgow Coma Scale (GCS) score is 11 (a GCS score of 9-12 indicates moderate head injury). The neurosurgeons elect to not place an intracranial pressure (ICP) monitor. The patient responds appropriately to stimuli and is hemodynamically stable. What is the most appropriate initial treatment?
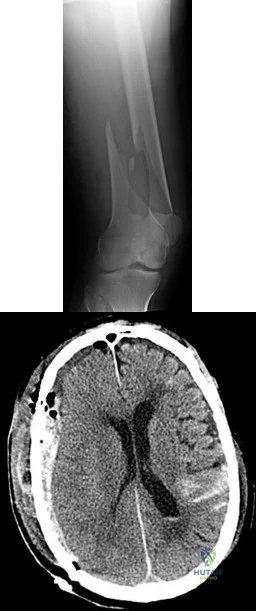
Explanation
Although management of femoral shaft fractures in patients with head injuries remains controversial, most practitioners agree that "damage-control principles" are appropriate for patients with evolving head injuries. This patient has a subarachnoid hemorrhage and a decreased GCS but is responding appropriately. The best treatment is a damage-control approach for the femur that will cause minimal blood loss and allow the brain injury (and swelling) to equilibrate. External fixation can be performed expeditiously and with minimal blood loss, which will reduce further injury to the brain. Special attention should be paid to maintaining cerebral perfusion pressure higher than 70 mmHg. Admission to the intensive care unit is recommended for monitoring of this injury. Knee immobilizers are not tolerated well by young muscular men with femur shaft fractures. A GCS score of 11 or higher can be observed without ICP monitoring.
RECOMMENDED READINGS
Flierl MA, Stoneback JW, Beauchamp KM, Hak DJ, Morgan SJ, Smith WR, Stahel PF. Femur shaft fracture fixation in head-injured patients: when is the right time? J Orthop Trauma. 2010 Feb;24(2):107-14. PubMed PMID: 20101135. View Abstract at PubMed
Roberts CS, Pape HC, Jones AL, Malkani AL, Rodriguez JL, Giannoudis PV.Damage control orthopaedics: evolving concepts in the treatment of patients who have sustained orthopaedic trauma. Instr Course Lect. 2005;54:447-62. Review. PubMed PMID: 15948472. View Abstract at PubMed
Question 38
Figures 1a and 1b are the recent radiographs of an 82-year-old man with rheumatoid arthritis who underwent total knee arthroplasty (TKA) 18 years ago. These radiographs reveal osteolysis with loosening of the tibial component. Aspiration and laboratory study findings for infection are negative. During the revision TKA, treatment of tibial bone loss should consist of
Explanation
Video 1 for reference
For severe tibial defects (Anderson Orthopaedic Research Institute [AORI] types 2 and 3), metaphyseal fixation is necessary to achieve construct fixation during revision TKA. Metaphyseal fixation may be achieved with cement, structural allograft, or conical metallic implants. The major concerns regarding structural allograft are graft resorption and mechanical failure and technical issues related to fashioning the graft and obtaining a good host-allograft interface. In a systematic review, porous metal cones were associated with a decreased loosening rate in AORI 2 and 3 defects compared to structural allografts. Metallic trabecular metal cones and metaphyseal porous coated sleeves provide a stable construct with which to support the tibial component during revision TKA. Clinical results with these devices include good metaphyseal fixation for severe tibial bone defects.
Question 39
A polytrauma patient sustains a right bicondylar tibial plateau fracture and a right humeral shaft fracture both treated with open reduction and internal fixation. He also underwent statically locked intramedullary nailing of a left femoral shaft fracture. What is the appropriate weightbearing status?
Explanation
Tingstad et al found favorable results of immediate weightbearing on humeral shaft fractures treated with plating and full weightbearing did not have any effect on the union or malunion rates.
Brumback et al evaluated the feasibility, safety and efficacy of immediate
weightbearing after treatment of femoral shaft fractures with statically locked IM nail. All the patients went on to union and no loss of fixation occurred.
OrthoCash 2020
Question 40
A 15-year-old girl with a midshaft fibular lesion has histologic findings consistent with Ewing’s sarcoma. Following induction chemotherapy, local control typically consists of
Explanation
REFERENCES: Nesbit ME Jr, Gehan EA, Burgert EO Jr, et al: Multimodality therapy for the treatment of primary, non-metastatic Ewing’s sarcoma of the bone: A long-term follow-up of the first intergroup study. J Clin Oncol 1990;8:1664-1674.
Simon M, Springfield D, et al: Ewing’s Sarcoma: Surgery for Bone and Soft Tissue Tumors. Philadelphia, PA, Lippincott Raven, 1998, p 296.
Question 41
Figure 7 shows the MRI scan of a 23-year-old competitive rugby player who has anterior ankle pain and swelling. He states that he has been playing for many years and has sprained his ankle several times. Examination will reveal what specific hallmark feature?
Explanation
REFERENCES: Ogilvie-Harris DJ, Mahomed N, Demaziere A: Anterior impingement of the ankle of the ankle treated by arthroscopic removal of bony spurs. J Bone Joint Surg Br 1993;75:437-440.
Cannon LB, Hackney RG: Anterior tibiotalar impingement associated with chronic ankle instability. J Foot Ankle Surg 2000;39:383-386.
Question 42
A 78-year-old woman has a history of chronic low back pain. She denies any extremity problems. Her pain is worse in the morning, and gets better, although it does not go away, as the day goes on. An MRI scan of the lumbar spine is shown in Figure 88. She denies any acute worsening of her symptoms, although in general, her symptoms are slowly worsening. She takes nonsteroidal anti-inflammatory drugs as needed for her pain, but otherwise takes no other medications. What is the next most appropriate step in management? Review Topic
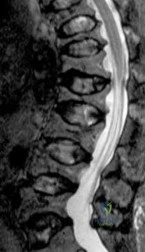
Explanation
Question 43
Which of the following prophylactic regimens for the prevention of deep venous thrombosis after knee arthroplasty has received a grade 1A recommendation in favor of its use from the American College of Chest Physicians (ACCP) in the 2004 guidelines?
Explanation
REFERENCE: Geerts WH, Pineo GF, Heit JA, et al: Prevention of venous thromboembolism: The seventh ACCP Conference on antithrombotic and thrombolytic therapy. Chest 2004;126:338S-400S.
Question 44
A 56-year-old man who tripped and fell out of his golf cart onto his right shoulder 4 days ago now reports mild pain while chipping. Examination reveals mild bruising over the lateral clavicle but good shoulder range of motion and strength. A radiograph is shown in Figure 9. Appropriate treatment at this time should include which of the following?
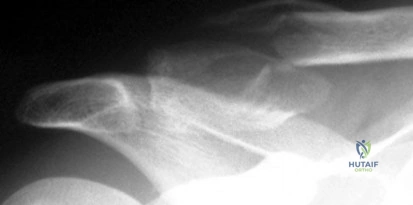
Explanation
Question 45
A hip compression screw is placed in a test jig and a bending load is applied to the tip of the screw. After the load is released, the screw returns completely to its original shape. What is this type of deformation called?
Explanation
Question 46
A 15-year-old boy has had pain in the right knee for the past 3 months. He denies any history of trauma. Examination reveals a firm mass in the distal thigh; the remainder of the examination is unremarkable. A radiograph is shown in Figure 24. What further work-up should be completed prior to biopsy?
Explanation
REFERENCES: Simon MA, Finn HA: Diagnostic strategy for bone and soft tissue tumors. J Bone Joint Surg Am 1993;75:622-631.
Simon M, Springfield D, et al: Biopsy: Surgery for Bone and Soft Tissue Tumors. Philadelphia, PA, Lippincott Raven, 1998, p 6.
Question 47
A 4-year-old boy who was struck by a motor vehicle has a right pneumothorax requiring placement of a chest tube, an open (Gustilo) grade IIIA midshaft fracture of the left femur, and a closed displaced subtrochanteric fracture of the right femur. He also sustained a subdural hematoma that requires neurosurgical intervention. In addition to irrigation and debridement of the left femur, treatment should include
Explanation
Question 48
A 30-year-old man who underwent an anterior lumbar diskectomy and fusion at L4-5 and L5-S1 through an anterior retroperitoneal approach 1 month ago now reports he is unable to obtain and maintain an erection. The most likely cause of this condition is
Explanation
REFERENCES: Flynn JC, Price CT: Sexual complications of anterior fusion of the lumbar spine. Spine 1984;9:489-492.
Johnson RM, McGuire EJ: Urogenital complications of anterior approaches to the lumbar spine. Clin Orthop 1981;154:114-118.
Question 49
Figures A and B are radiographic images of an 85-year-old woman with isolated left hip pain. She describes a non-syncopal fall from standing 4 hours ago. Physical examination reveals pain with log-rolling the left thigh and the inability to bear weight on the affected leg. The radiologist reports no fracture in the left hip. What would be the next best step? Review Topic
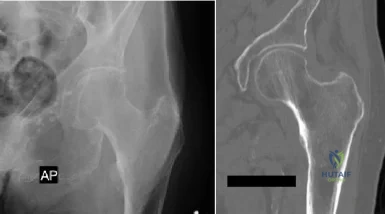
Explanation
Moderate evidence supports MRI as the advanced imaging of choice for diagnosis of presumed hip fracture not apparent on initial radiographs. MRI has been shown to be able to detect occult fractures earlier than bone scan, with better spatial resolution. Usually the MRI should be obtained in less than 24 hours from the time of injury. For situations in which MRI is not immediately available, bone scan can be considered after 72 hours form the time of injury. However, this may compromise patient care and put the patient at risk of fracture displacement.
Cannon et al. reviewed the imaging of choice in occult hip fracture. They showed that physical examination yields a poor sensitivity identifying occult hip fractures, with log-rolling and straight-leg raise as 50% and 70%, respectively. The most sensitive modality for occult fracture identification was MRI.
Iwata et al. retrospectively reviewed a cohort of 35 patients with clinically suspected fractures of the hip that underwent MRI. All radiographs were negative. In 26 of these patients, a T1-weighted coronal MRI showed a hip fracture with 100% sensitivity.
Roberts et al. reviewed the 2015 AAOS Clinical Practice Guideline: Management of Hip Fractures in the Elderly. They report moderate evidence that supports MRI as the advanced imaging of choice for diagnosis of presumed hip fractures not apparent on initial radiographs.
Figure A is a AP radiograph of the left hip and pelvis. Apart from a healed fracture of the ischiopubic rami and generalized osteopenia, there is no obvious hip fracture. Figure B is a coronal CT image that does not demonstrate evidence of an acute hip fracture. Illustration A is a T1 weighted MR image that shows a non displaced fracture (white arrow) through the intertrochanteric region of the left proximal femur.
Incorrect Answers:
(SBQ12TR.32) A 20-year-old male is taken to the emergency department following a motorcycle collision with the injury seen in Figures A and B. He undergoes serial debridements with placement of an antibiotic bead pouch, followed by intramedullary nailing and free tissue transfer. His preoperative examination is notable for absent plantar sensation. Which of the following is predictive of a worse long term outcome in this patient?
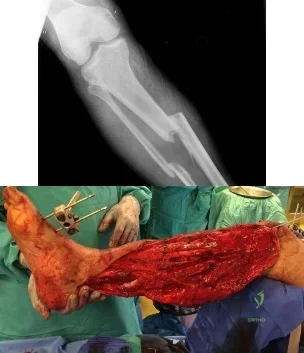
Absent plantar sensation at presentation
Depression at 3 months post-injury
Use of an intramedullary nail
Free tissue transfer instead of rotational flap
Need for multiple debridements
The presence of depression at the 3 months post-injury is a significant predictor of worse long term outcome as well as lower return to work rates in patients that present with limb threatening lower extremity trauma.
The findings of the Lower Extremity Assessment Project (LEAP study) has challenged many of the long-held beliefs of lower extremity trauma surgery, including the concept that patients with absent plantar sensation should undergo immediate amputation . The LEAP study has also brought to light the importance of socioeconomic and psychosocial factors in patient outcomes following these injuries.
Bosse et al analyzed a subgroup of 55 patients from the LEAP study with absent plantar sensation at presentation. Those patients that underwent limb salvage despite absent sensation (n=26) had no significant difference in functional outcome when compared with either insensate patients who underwent amputation or a matched control group of sensate patients with similar injuries. All but one patient in the salvage group had return of some sensation at 2-year follow up and the authors concluded that an insensate plantar foot at presentation should not be included in the algorithm for amputation.
Mackenzie and Bosse reviewed the results of the LEAP study with particular emphasis on the social and economic variables that influence outcomes in severe lower extremity. The authors note that 19% of patients screened positive for severe depression. The presence of anxiety, pain and depression at 3 months post-injury were significant predictors of poor outcome
Incorrect Answers:
tissue for type IIIB tibia fractures. Answer 5: The number of debridements has not been shown to influence outcome.
Question 50
Which of the following is considered a risk factor for the development of low back pain?
Explanation
REFERENCE: Koval KJ (ed): Orthopaedic Knowledge Update 7. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 627-643.
Question 51
An adult patient with a grade I isthmic spondylolisthesis at L5-S1 is most likely to have weakness of the Review Topic
Explanation
Question 52
The therapeutic effect of etanercept in the treatment of rheumatoid arthritis is primarily mediated through
Explanation
REFERENCES: Weinblatt ME, Kremer JM, Bankhurst AD, et al: A trial of etanercept, a recombinant tumor necrosis factor receptor: Fc fusion protein, in patients with rheumatoid arthritis receiving methotrexate. N Engl J Med 1999;340:253-259.
Buckwalter JA, Einhorn TA, Simon SR (eds): Orthopaedic Basic Science: Biology and Biomechanics of the Musculoskeletal System, ed 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2000, pp 489-530.
Question 53
A 13-year-old girl with Down syndrome has bilateral chronic patellar dislocations. She denies knee pain. She is able to straighten her knees and walks with a symmetric but awkward gait. She does not flex her knees in midstance. Examination reveals that the patellae cannot be brought into a reduced position. Management should consist of
Explanation
REFERENCES: Dugdale TW, Renshaw TS: Instability of the patellofemoral joint in Down syndrome. J Bone Joint Surg Am 1986;68:405-413.
Mendez AA, Keret D, MacEwen GD: Treatment of patellofemoral instability in Down’s syndrome. Clin Orthop 1988;234:148-158.
Question 54
A 23-year-old woman with recurrent anterior instability undergoes an open Bankart procedure. Six months after surgery the patient reports shoulder
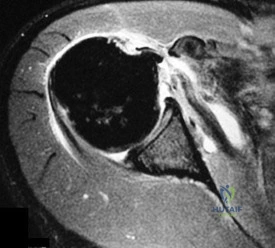
Explanation
Question 55
Which of the following lumbar disk components has the highest tensile modulus to resist torsional, axial, and tensile loads? Review Topic
Explanation
Question 56
Of all the pelvic ring injury types, anteroposterior compression type III pelvic ring injuries have the highest rate of which of the following?

Explanation
Question 57
Compared with percutaneous pinning with Kirschner wires (K-wires), the treatment of metacarpal neck fractures with cannulated intramedullary screws is associated with
Explanation
In a biomechanical study, headless compression screws showed superior load to failure, higher three-point bending strength, and greater strength in axial loading compared with percutaneous K-wire fixation for metacarpal neck fractures. Headless compression screws provide greater initial stability to allow earlier motion in the postoperative period. No data comparing infection rates between the two methods of fixation are available; however, it is assumed that K-wires placed outside of the skin would have increased rates of infection. Neither fixation method would increase the time to healing.
Question 58
273 In an athlete who has full, painless range of motion and a normal neurological examination, which of the following is considered an absolute contraindication to participation in a collision sport such as football?
Explanation
Thomas BE, et al. Cervical spine injuries in football players. J AM Acad Orthop Surg 1999;7:338-347
Torg JS et al: Neurapraxia of the cervical spinal with transientquadriplegia. JBJS Am 1986:68:1354-
Question 59
Osteoclasts originate from which of the following cell types?
Explanation
REFERENCES: Zaidi M, Blair HC, Moonga BS, et al: Osteoclastogenesis, bone resorption, and osteoclast-based therapeutics. J Bone Miner Res 2003;18:599-609.
Brinker MR: Bone (Section 1), in Miller M (ed): Review of Orthopaedics, ed 2. Philadelphia, PA, WB Saunders, 1996, pp 1-35.
Zuscik MJ, Drissi MH, Reynolds PR, et al: Molecular and cell biology in orthopaedics, in Einhorn TA, O’Keefe RJ, Buckwalter JA (eds): Orthopaedic Basic Science: Foundations of Clinical Practice, ed 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2006,
in press.
Question 60
A 55-year-old woman with a 15-year history of systemic lupus erythematosus has had left shoulder pain for the past 3 months. She reports that the pain has grown progressively worse over the past few months, and her shoulder function is severely limited. She is presently being treated with azathioprine and has used corticosteroids in the past. AP and axillary radiographs are shown in Figures 19a and 19b, and MRI scans are shown in Figures 19c and 19d. Which of the following forms of management will yield the most predictable pain relief and return of shoulder function?
Explanation
REFERENCES: Hattrup SJ, Cofield RH: Osteonecrosis of the humeral head: Results of replacement. J Shoulder Elbow Surg 2000;9:177-182.
L’Insalata JC, Pagnani MJ, Warren RF, et al: Humeral head osteonecrosis: Clinical course and radiographic predictors of outcome. J Shoulder Elbow Surg 1996;5:355-361.
Cruess RL: Steroid-induced avascular necrosis of the head of the humerus: Natural history and management. J Bone Joint Surg Br 1976;58:313-317.
Question 61
A 16-year-old girl sustains the closed injury shown in Figure 1. On physical examination, she is found to have a complete radial nerve palsy. Her fracture is treated nonsurgically, and her nerve palsy is followed clinically for improvement. What muscle is most likely to improve last as her nerve recovers?
Explanation
Question 62
A coach of three football teams—the B team, junior varsity team, and varsity team—wants to study the average times in the 40-yard dash for his players. Which test would help him determine if the mean 40-yard dash times for the athletes on one team are different from those on the other teams?
Explanation
Question 63
Which of the following is considered a contraindication to the use of a reverse total shoulder arthroplasty? Review Topic
Explanation
Question 64
-The center of rotation of the knee can be best described as
Explanation
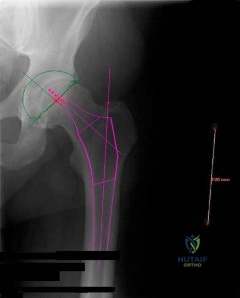
Question 65
-A 37-year-old woman has a 2-month history of weakness in thumb and finger extension, but has normal radial deviation during extension of the wrist. An MRI scan of her forearm shows no abnormality. She does not recall any traumatic event. Needle electromyography findings show fibrillations and reduced
Explanation

Question 66
..Figures 83a and 83b are the radiographs of a 53-year-old otherwise healthy homemaker who had a syncopal episode and sustained a ground-level fall and injury to her right elbow. She presently admits to right elbow pain, swelling, and an inability to bend her elbow. What is the best initial treatment for this injury?
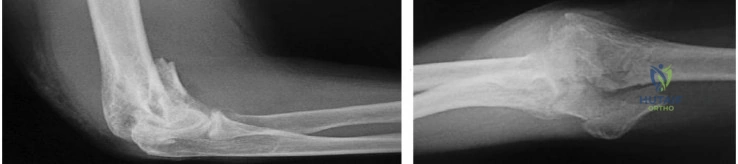
Explanation
Figure 84 is the glenoid CT scan of a 20-year-old man who dislocated his shoulder anteriorly while playing football. He had persistent instability 2 months after the injury, but he did not have a sulcus sign or posterior instability. He underwent an arthroscopic Bankart repair with 4 bioabsorbable anchors with simple sutures through the labrum and capsule.
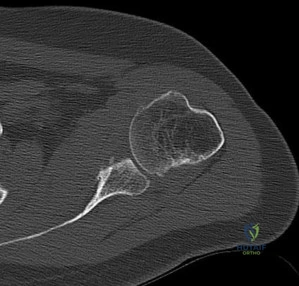
He did not have an engaging Hill-Sachs lesion, the rotator cuff was unremarkable, and the capsule was not torn from the humerus. After surgery, he did well for 6 months until he jumped into a lake and again dislocated his shoulder anteriorly. He says his shoulder no longer felt stable after his reduction.
Question 67
An active, right-handed 71-year-old woman fell on her left shoulder and sustained the injury shown in the radiographs in 52a and 52b and the CT scan in 52c. Management should consist of
Explanation
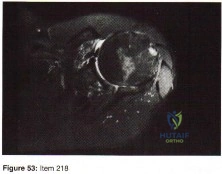
Question 68
….Figures 83a through 83c are the radiograph and MRI scans of a 16-year-old girl who had posterior knee pain after a dance recital 3 weeks ago; the pain resolved 1 week ago with ibuprofen use. What is the appropriate treatment for this patient?
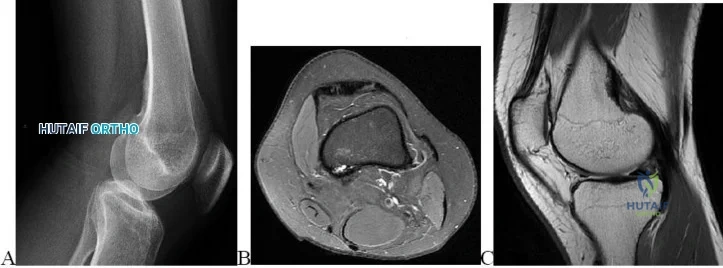
Explanation
Figures 84a and 84b are the CT and MRI scans of a 17-year-old girl with a painful lumbosacral scoliosis that has been present for 12 months. Examination is notable only for pain over the left sacral region and a postural scoliosis leaning away from this side.
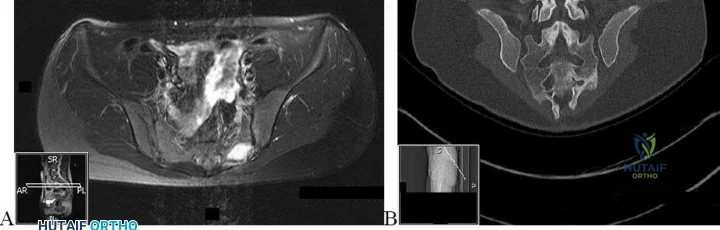
Question 69
-The main blood supply to the capital femoral epiphysis in a 10-year-old child is supplied from the
Explanation
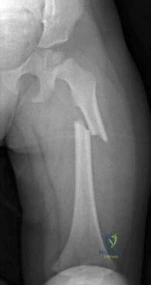
Question 70
A researcher decides she wants to look at the current total number of patients who have methicillin-resistant Staphylococcus aureus (MRSA) infections in a hospital on 1 particular day. What is the researcher measuring?
Explanation
Question 71
An 82-year-old man has had episodic right thigh pain after undergoing a total hip arthroplasty 10 years ago. Initial postoperative radiographs are shown in Figures 26a and 26b, and current radiographs are shown in Figures 26c and 26d. What is the most likely cause of his pain?
Explanation
REFERENCES: Engh CA, Massin P, Suthers KE: Roentgenographic assessment of biologic fixation of porous-surface femoral components. Clin Orthop Relat Res 1990;257:107-128.
Engh CA, Hooten JP, Zettl-Schaffer KF, et al: Evaluation of bone ingrowth in proximally and extensively porous-coated anatomic medullary locking prostheses retrieved at autopsy. J Bone Joint Surg Am 1995;77:903-910.
Question 72
Which of the following articulation couplings shows the lowest coefficient of friction as tested in the laboratory?
Explanation
REFERENCES: Cuckler JM, Bearcroft J, Asgian CM: Femoral head technologies to reduce polyethylene wear in total hip arthroplasty. Clin Orthop 1995;317:57-63.
Sharkey PF, Hozack WJ, Dorr LD, Maloney WJ, Berry D: The bearing surface in total hip arthroplasty: Evolution or revolution, in Price CT (ed): Instructional Course Lectures 49. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2000, pp 41-56.
Question 73
- A consecutive series of 50 patients is randomized to receive either treatment A or treatment B. At a 10-year follow up, patient satisfaction with treatment is measured. Which of the following statistical calculations will provide the most information regarding the magnitude of possible differences between the two groups of patients?
Explanation
Question 74
What is the minimum hours per day of wear that has been correlated with the effectiveness of bracing on curve progression in idiopathic scoliosis? Review Topic
Explanation
Question 75
A soccer player who sustained a twisting injury to the right ankle while making a cut is unable to bear weight and has diffuse tenderness over the anterior and lateral aspects of the ankle. Examination also shows a positive squeeze test. Plain radiographs and a stress radiograph are shown in Figures 26a through 26c. Radiographs of the leg and knee are normal. What is the most appropriate management?
Explanation
REFERENCES: Boytim MJ, Fisher DA, Neumann L: Syndesmotic ankle sprains. Am J Sports Med 1991;19:294-298.
Miller CD, Shelton WR, Barrett GR, et al: Deltoid and syndesmosis ligament injury of the ankle without fracture. Am J Sports Med 1995;23:746-750.
Question 76
In a statement put forth by AAOS, the role of the orthopaedic surgeon in the face of domestic and family abuse includes all of the following EXCEPT: Review Topic
Explanation
The statement put forth by the AAOS implores the orthopaedic surgeon to be aware of the integral components to identify, document, and care for minors, elders, and/or partners who are victims of domestic abuse.
Zilmer et al. in a JAAOS review and the basis for the AAOS statement emphasizes the ability to identify abuse, which includes, but is not limited to frequent/multiple injuries, temporal abnormalities in multiple injuries, frequent visits/utilization of the emergency department, and/or unusual injuries/fracture patterns not consistent with the clinical picture. Meticulous documentation is of paramount importance, in addition to communicating your concerns to the appropriate emergency department personnel.
Incorrect answers:
Question 77
- A 14-year-old girl has idiopathic scoliosis with a 52-degree right thoracic curve and a 36-degree left lumbar curve. The rotation of the apical vertebra appears greater in the thoracic curve. A sagittal view radiograph shows the spine to be virtually straight. The iliac apophyses are Risser 2. Treatment should consist of
Explanation
Question 78
Figure 6 shows an object being held in an outstretched hand. To offset the moment created by the object (ignoring the weight of the forearm), the biceps must generate a force of
Explanation
REFERENCES: An KN, Chao ES, Kaufman KR: Analysis of muscle and joint loads, in Mow VC, Hayes WC (eds): Basic Orthopaedic Biomechanics, ed 2. New York, NY, Lippincott-Raven, 1997, pp 1-14.
Buckwalter JA, Einhorn TA, Simon SR (eds): Orthopaedic Basic Science: Biology and Biomechanics of the Musculoskeletal System, ed 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2000, pp 134-143.
Question 79
A 6-year-old boy with spastic diplegic cerebral palsy has a crouched gait. Examination reveals hip flexion contractures of 15 degrees and popliteal angles of 70 degrees. Equinus contractures measure 10 degrees with the knees extended. Which of the following surgical procedures, if performed alone, will worsen the crouching?
Explanation
REFERENCES: Gage JR: Distal hamstring lengthening/release and rectus femoris transfer, in Sussman MD (ed): The Diplegic Child. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1992, pp 324-326.
Bleck EE: Orthopaedic Management of Cerebral Palsy, in Saunders Monographs in Clinical Orthopaedics. Philadelphia, PA, WB Saunders, vol 2, 1979.
Question 80
A patient undergoes hip arthroscopy, and the pathology is seen in Figure 18. What is the most likely diagnosis?
Explanation
REFERENCE: Byrd JWT: Operative Hip Arthroscopy. New York, NY, Thieme Medical Publishers, 1998, pp 93-104.
Question 81
You are interested in learning a new technique for minimally invasive total knee arthroplasty. The Keyhole Genuflex system seems appealing to you because the instrumentation comes with wireless controls. Which of the following represents an acceptable arrangement?
Explanation
Question 82
A 72-year-old man with diabetic neuropathy and 5 degrees of valgus talar tilt; he has pursued nonsurgical treatment for 30 years and now has unrelenting pain
Explanation
Arthritis of the ankle and hindfoot can pose challenges. Depending upon patient age, comorbidities, and alignment, a variety of surgical interventions may be offered. A total ankle replacement may be considered for patients older than 60 years of age who have minimal misalignment and low-demand lifestyles. In all other cases, ankle fusion must be considered. The nonsurgical care of ankle arthritis includes anti-inflammatory medication, intra-articular steroid injections, bracing with customized products such as the Arizona brace, or a molded foot and ankle orthosis.
Patients with diabetes and Charcot arthropathy may be treated nonsurgically with total-contact casting during acute and active or "hot" phases and accommodative shoes during consolidation and stable or "cool" phases. When the patient has recurrent ulcers or major anatomy changes, surgical intervention must be considered. Tibiotalocalcaneal fusion helps to realign the foot and ankle and make it more braceable in the setting of ankle and hindfoot Charcot disease.
RECOMMENDED READINGS
Queen RM, Adams SB Jr, Viens NA, Friend JK, Easley ME, Deorio JK, Nunley JA. Differences in outcomes following total ankle replacement in patients with neutral alignment compared with tibiotalar joint malalignment. J Bone Joint Surg Am. 2013 Nov 6;95(21):1927-34. doi: 10.2106/JBJS.L.00404. PubMed PMID: 24196462. View Abstract at PubMed
Nunley JA, Caputo AM, Easley ME, Cook C. Intermediate to long-term outcomes of the STAR Total Ankle Replacement: the patient perspective. J Bone Joint Surg Am. 2012 Jan 4;94(1):43-8. doi: 10.2106/JBJS.J.01613. PubMed PMID: 22218381. View Abstract t PubMed
Saltzman CL, Mann RA, Ahrens JE, Amendola A, Anderson RB, Berlet GC, Brodsky JW, Chou LB, Clanton TO, Deland JT, Deorio JK, Horton GA, Lee TH, Mann JA, Nunley JA, Thordarson DB, Walling AK, Wapner KL, Coughlin MJ. Prospective controlled trial of STAR total ankle replacement versus ankle fusion: initial results. Foot Ankle Int. 2009 Jul;30(7):579-96. doi: 10.3113/FAI.2009.0579. PubMed PMID: 19589303. View Abstract at PubMed
Faraj AA, Loveday DT. Functional outcome following an ankle or subtalar arthrodesis in adults. Acta Orthop Belg. 2014 Jun;80(2):276-9. PubMed PMID: 25090803. View Abstract at PubMed Grear BJ, Rabinovich A, Brodsky JW. Charcot arthropathy of the foot and ankle associated with rheumatoid arthritis. Foot Ankle Int. 2013 Nov;34(11):1541-7. doi: 10.1177/1071100713500490. Epub 2013 Jul 30. PubMed PMID: 23900228. View Abstract at PubMed
Question 83
A 30-year-old patient has wrist pain. A radiograph and biopsy specimen are shown in Figures 34a and 34b. What is the most likely diagnosis?
Explanation
REFERENCES: Bieselker JL, Marcove RC, Huvos AG, Mike V: Aneurysmal bone cyst: A Clinico-pathologic study of 66 cases. Cancer 1973;26:615.
Martinez V, Sissons HA: A review of 123 cases including primary lesions and those secondary to other bone pathology. Cancer 1988;61:2291.
Question 84
The spinal cord terminates as the conus medullaris at what vertebral level in adults? Review Topic 1 T12
Explanation
Question 85
The most appropriate surgical approach includes which of the following? Review Topic
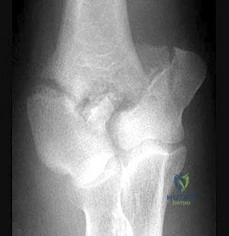
Explanation
Question 86
A patient who underwent an L5-S1 diskectomy 18 months ago has persistent pain in the left leg. Figures 9a and 9b show postoperative axial T 1 -weighted MRI scans at the L5-S1 level without and with gadolinium. What is the most likely diagnosis?
Explanation
REFERENCES: Babar S, Saifuddin A: MRI of the post-discectomy lumbar spine. Clin Radiol 2002;57:969-981.
Kikkawa I, Sugimoto H, Saita K, et al: The role of Gd-enhanced three-dimensional MRI fast low-angle shot (FLASH) in the evaluation of symptomatic lumbosacral nerve roots. J Orthop Sci 2001;6:101-109.
Vroomen PC, Van Hapert SJ, Van Acker RE, et al: The clinical significance of gadolinium enhancement of lumbar disc herniations and nerve roots on preoperative MRI. Neuroradiology 1998;40:800-806.
Question 87
Five weeks after the patient completes a 6-week course of antibiotics, his ESR is 24 mm/h and CRP level is 10 mg/L, which is similar to the levels at 6 weeks. What is the most appropriate treatment at this time?
Explanation
This patient has both serologic and synovial fluid findings that are concerning for indolent infection. He was taking antibiotics at the time of aspiration. The AAOS clinical practice guideline, The Diagnosis of Periprosthetic Joint Infections of the Hip and Knee, suggests that patients discontinue antibiotics for a minimum of 2 weeks and that a repeat aspiration should be performed in cases of contradictory findings. In this situation, the cell count is elevated
along with an elevated ESR and CRP level. As a result, the appropriate treatment at this time is to reaspirate his hip.
This patient has a periprosthetic joint infection with a draining sinus tract. He has had symptoms for several months and, as a result, irrigation and debridement are not indicated. A single-stage surgery may be performed in some centers for healthy patients with susceptible organisms. However, single-stage reconstructions are generally performed with cemented implants in patients without a draining sinus tract. A 2-stage procedure with an antibiotic spacer is the surgical treatment modality most likely to eradicate this infection.
Serologic findings have significantly improved since the time of the prior surgical procedure. Surgical intervention does not need to be delayed until these values have completely normalized.
Question 88
Figures 1 through 3 demonstrate the radiographs obtained from a 45-year-old construction worker who has wrist pain, loss of motion, and loss of strength. Nonsurgical measures have failed, and the patient requests surgery. What is the best surgical option for this patient?
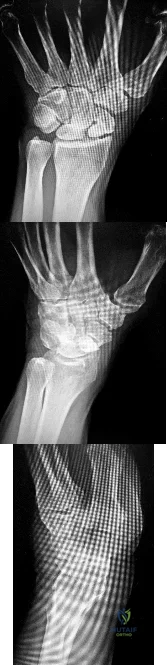
Explanation
This patient has a physically demanding occupation. His radiographs show a long-standing nonunion with avascular necrosis and collapse of the proximal pole. This condition is referred to as a scaphoid nonunion advanced collapse wrist (SNAC). He has advanced arthritis of the capitolunate joint, but the radiolunate joint is preserved. The best option for him would be scaphoid excision with four-corner fusion. Proximal row carpectomy, would be incorrect because of the advanced arthritis of the capitolunate joint. This procedure relies on normal cartilage/joint articulation of the capitate as well as of the lunate fossa of the distal radius. Proximal pole scaphoid excision alone would not address the advanced arthritis of the capitolunate joint. Scaphoid fixation with bone grafting would not address the midcarpal arthritis and advanced proximal pole collapse.
Question 89
A 14-year-old girl reports hip pain that is exacerbated by weight bearing. A radiograph and biopsy specimen are shown in Figures 16a and 16b. The best course of management should be
Explanation
REFERENCES: Azouz EM, Karamitsos C, Reed MH, Baker L, Kozlowski K, Hoeffel JC: Types and complications of femoral neck fractures in children. Pediatr Radiol 1993;23:415-420.
Hecht AC, Gebhardt MC: Diagnosis and treatment of unicameral and aneurysmal bone cysts in children. Curr Opin Pediatr 1998;10:87-94.
Question 90
A 20-year-old man sustains the injury shown in Figures 1a and 1b in a motorcycle accident. In addition to a prompt closed reduction, his outcome might be optimized by
Explanation
REFERENCE: Saltzman C, Marsh JL: Hindfoot dislocations: When are they not benign? J Am Acad Orthop Surg 1997;5:192-198.
Question 91
A 20-year-old college athlete is seen for follow-up after sustaining an injury at football practice 2 days ago. He reports that he tackled a player and felt neck pain and numbness in both arms. The numbness resolved within seconds, but his neck remains painful and stiff. He denies any history of neck pain or injury. Examination reveals limited neck motion. The neurologic examination and radiographs are normal. MRI scans of the cervical spine are shown in Figure 34. During counseling, the patient, his family, and his coach should be informed that he has an acute cervical disk herniation and cannot play
Explanation
REFERENCES: Morganti C, Sweeney CA, Albanese SA, Burak C, Hosea T, Connolly PJ: Return to play after cervical spine injury. Spine 2001;26:1131-1136.
Vaccaro AR, Watkins B, Albert TJ, Pfaff WL, Klein GR, Silber JS: Cervical spine injuries in athletes: Current return-to-play criteria. Orthopedics 2001;24:699-705.
Question 92
Pelvic packing for a hemodynamically unstable patient with a pelvic ring fracture is best described by which of the following techniques?
Explanation
Question 93
A 47-year-old woman has had a 1-month history of left hip and medial thigh pain that is exacerbated by sitting. Laboratory studies show a total protein level of 8.2 g/dL (normal 6.0 to 8.0) and an immunoglobulin G (IGG) level of 2,130 mg/dL (normal 562 to 1,835). A radiograph, CT scan, and biopsy specimen are shown in Figures 38a through 38c. What is the most likely diagnosis?
Explanation
REFERENCE: Mirra J: Bone Tumors: Clinical, Radiologic, and Pathologic Correlations. Philadelphia, PA, Lea & Febiger, 1989, vol 2, ch 16.
Question 94
- To maximally resist apex anterior angulation in the tibia, the pins of a unilateral external fixator should be oriented in which of the following planes?
Explanation
Question 95
A 10-year-old girl has been unable to walk for the past 5 days because of bilateral hip pain. Administration of IV morphine has provided some pain relief. She is afebrile. History reveals that she had an upper respiratory tract infection 3 weeks ago that resolved uneventfully. Examination reveals moderate pain with internal rotation and abduction, while log rolling maneuvers do not cause significant pain. An MRI scan shows a small effusion of one hip; however, a bone scan and plain radiographs are normal. Initial laboratory studies showed a markedly elevated WBC count, which subsequently declined to normal levels with IV antibiotics. Current studies show an erythrocyte sedimentation rate (ESR) of 100 mm/h. Aspiration of the hip obtains 3 mL of fluid; Gram stain is negative for bacteria, but a cell count shows a WBC count of 16,500/mm 3 . Streptozyme titer of the peripheral blood is 200 units (normal is less than 100 units). Management should now consist of
Explanation
REFERENCES: De Cunto CL, Giannini EH, Fink CW, et al: Prognosis of children with poststreptococcal reactive arthritis. J Pediatr Infect Dis 1988;7:683-686.
Haueisen DC, Weiner DS, Weiner SD: The characterization of “transient synovitis of the hip” in children. J Pediatr Orthop 1986;6:11-17.
Question 96
A 14-year-old boy reports progressive right wrist pain. Radiographs are shown in Figure 3a, and a photomicrograph is shown in Figure 3b. What is the most likely diagnosis?
Explanation
REFERENCES: Lersundi A, Mankin HJ, Mourikis A, et al: Chondromyxoid fibroma: A rarely encountered and puzzling tumor. Clin Orthop Relat Res 2005;439:171-175.
Menendez LR (ed): Orthopaedic Knowledge Update: Musculoskeletal Tumors. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 103-111.
Question 97
Following a chevron bunionectomy performed through a dorsal approach, a patient has persistent numbness on the dorsal and medial aspect of the hallux. What nerve has most likely been injured?
Explanation
REFERENCE: Miller SD: Dorsomedial cutaneous nerve syndrome: Treatment with nerve transection and burial into bone. Foot Ankle Int 2001;22:198-202.
Question 98
Reconstruction of the injured structure is performed. After surgery, the patient initially notes limitation in motion, and later develops recurrent instability of the knee. Which factor most likely contributed to the development of instability?
Explanation
The anteromedial bundle originates on the anterior and proximal aspect of the lateral femoral condyle and inserts on the anteromedial aspect of the anterior cruciate ligament (ACL) footprint on the proximal tibia. The posterolateral bundle originates posterior and distal to 63 the anteromedial bundle and inserts on the posterolateral aspect of the tibial footprint. The fibers are parallel when the knee is in an extended position. As the knee moves into flexion,
the fibers of the anteromedial bundle rotate externally with respect to the posterolateral bundle. The anteromedial bundle is tensioned in both flexion and extension. The posteromedial bundle is tensioned in extension, but relaxes as the knee moves into flexion.
The lateral meniscus is more commonly injured with an acute injury to the ACL. The medial meniscus is injured more commonly when the ACL is chronically unstable.
The ACL is an intra-articular and intrasynovial structure. It is innervated by posterior articular branches from the tibial nerve. Innervation of the ACL involves several types of mechanoreceptors (Ruffini, Pacini, Golgi tendon, and free-nerve endings) that may contribute to proprioceptive function of the knee and modulation of quadriceps function.
Injury to the ACL is predominantly associated with instability to anterior translation of the tibia in extension. The ACL plays a secondary role to limit internal rotation of the tibia, and a loss of ACL stability is confirmed by the reduction of the tibia from a position of anterior translation and internal rotation (pivot shift). The radiographs demonstrate anterior placement of the femoral tunnel. The convex shape of the lateral femoral condyle can make it more difficult to visualize the anatomic femoral origin of the ACL. Failure to identify the
anatomic footprint can result in anterior placement of the femoral tunnel. Anterior ACL graft placement can result in its impingement against the posterior cruciate ligament and early limitation of knee flexion. Over time, impingement on the graft may result in stretching of the graft and recurrent knee instability symptoms.
RECOMMENDED READINGS
Duthon VB, Barea C, Abrassart S, Fasel JH, Fritschy D, Ménétrey J. Anatomy of the anterior cruciate ligament. Knee Surg Sports Traumatol Arthrosc. 2006 Mar;14(3):204-13. Epub 2005 Oct 19. Review. PubMed PMID: 16235056. View Abstract at PubMed
Zantop T, Petersen W, Sekiya JK, Musahl V, Fu FH. Anterior cruciate ligament anatomy and function relating to anatomical reconstruction. Knee Surg Sports Traumatol Arthrosc. 2006 Oct;14(10):982-92. Epub 2006 Aug 5. Review. PubMed PMID: 16897068. View Abstract at PubMed
Question 99
In total knee arthroplasty, in vitro testing has shown that cross-linking can diminish the rate of polyethylene wear by 30% to 80%. What other change in material properties is possible when polyethylene is highly cross-linked?
Explanation
The most important concern regarding highly cross-linked polyethylene relates to decreased mechanical properties. Cross-linking results in reduced ductility, tensile strength, and fatigue crack propagation resistance. These problems have not been shown to cause implant failure in the most recent clinical trials, but they remain the most important mechanical issues associated with current material processing methods.
Question 100
A 32-year-old man sustained an L1 burst fracture with 90% canal compromise, intact posterior elements, and kyphosis of 25% at the L1 level. He has an incomplete neurologic injury. Definitive management should consist of
Explanation
REFERENCES: Kaneda K, Abumi K: Burst fractures with neurologic deficits of the thoracolumbar spine. J Bone Joint Surg Am 1997;79:69-83.
McGuire R Jr: The role of anterior surgery in the treatment of thoracolumbar fractures. Orthopedics 1997;20:959-962.
