Orthopedic Board Review MCQs: Hip & Knee Arthroplasty, Sports Medicine | Part 99
Key Takeaway
This page presents Part 99 of an orthopedic surgery board review quiz. It features 50 high-yield multiple-choice questions (MCQs) designed for orthopedic residents and surgeons preparing for their OITE and AAOS board certification exams. The interactive format includes study and exam modes to enhance preparation.
Orthopedic Board Review MCQs: Hip & Knee Arthroplasty, Sports Medicine | Part 99
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
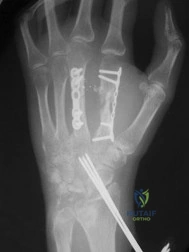
A 22-year-old female collegiate soccer player sustains a non-contact twisting injury to her right knee and feels a 'pop'. Radiographic evaluation is obtained in the emergency department as shown below.
Based on the pathognomonic radiographic finding, which of the following injury mechanisms most accurately describes the etiology of the associated primary ligamentous pathology?

Explanation
Question 2
A 62-year-old male presents for revision of his total hip arthroplasty (THA). He originally received a ceramic-on-ceramic bearing. During the procedure, the surgeon notes a catastrophic fracture of the ceramic femoral head.
After a thorough synovectomy, which of the following is the most appropriate management regarding the new bearing surface, assuming the acetabular shell and femoral stem are well-fixed?
Explanation
Question 3
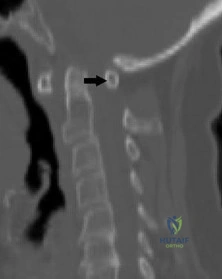
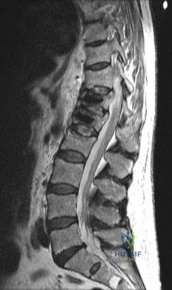
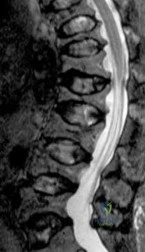
A 45-year-old construction worker complains of posterior knee pain and a feeling of 'giving way'. An MRI of the knee is shown.
Which of the following biomechanical phenomena is the most direct consequence of the pathology demonstrated?
Explanation
Question 4
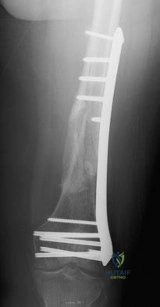
A 55-year-old male with a history of a high tibial osteotomy (HTO) 10 years ago now requires a total knee arthroplasty (TKA) for severe osteoarthritis.
What is the most significant intraoperative challenge the surgeon should anticipate, and what is an appropriate maneuver to address it?
Explanation
Question 5
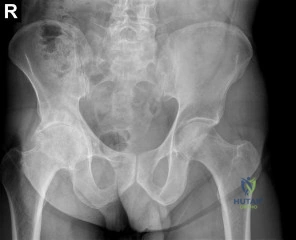
A 25-year-old professional hockey player presents with chronic, deep groin pain exacerbated by hip flexion and internal rotation.
Imaging demonstrates a classic pistol-grip deformity. Which of the following represents the primary mechanism of articular cartilage damage in this condition?
Explanation
Question 6
A 68-year-old female presents to the clinic complaining of a painful popping sensation at the anterior aspect of her knee when extending from a flexed position, one year after an uncomplicated posterior-stabilized total knee arthroplasty (PS-TKA).
What is the primary etiology of this specific complication?
Explanation
Question 7
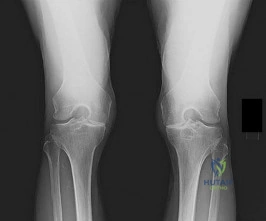
A 60-year-old male with medial compartment osteoarthritis of the knee undergoes evaluation for a unicompartmental knee arthroplasty (UKA).
According to standard Kozinn and Scott criteria, which of the following is an absolute contraindication to performing a medial UKA?
Explanation
Question 8
A 74-year-old female presents to the emergency department after a ground-level fall. Five years ago, she underwent an uncomplicated cementless THA.
Radiographs reveal a periprosthetic femur fracture extending around the distal tip of the femoral stem. The stem is visibly loose on radiographs with subsidence. What is the most appropriate surgical treatment?
Explanation
Question 9
A 16-year-old female basketball player suffers recurrent lateral patellar dislocations. An MRI reveals an avulsion of the Medial Patellofemoral Ligament (MPFL) at its femoral origin.
In an MPFL reconstruction, correct femoral tunnel placement is critical. Where is the anatomical femoral attachment of the MPFL (Schöttle's point) located radiographically on a true lateral view?
Explanation
Question 10
A 66-year-old male with a history of long-segment lumbar spine fusion (L2-S1) presents for a primary total hip arthroplasty (THA) for end-stage osteoarthritis. Which of the following adjustments to the acetabular component orientation is most appropriate to minimize the risk of posterior dislocation when the patient transitions from standing to sitting?
Explanation
Question 11
During a primary posterior-stabilized (PS) total knee arthroplasty, the surgeon places trial components. Upon assessment of gap kinematics, the joint space is symmetrically balanced and stable in full extension, but tight and difficult to flex past 90 degrees. Which of the following is the most appropriate next surgical step to balance the knee?
Explanation
Question 12
A 54-year-old male presents with a painful total hip arthroplasty 5 years postoperatively. His bearing surface is a metal-on-polyethylene construct. Radiographs show a well-fixed stem and cup with no osteolysis. Joint aspiration is negative for infection, but fluid analysis is black and turbid. Blood tests reveal significantly elevated cobalt levels with normal chromium levels. What is the most likely diagnosis?
Explanation
Question 13
According to the 2018 International Consensus Meeting (ICM) criteria for Periprosthetic Joint Infection (PJI), which of the following synovial fluid biomarkers acts as a highly specific indicator of PJI, functioning as an antimicrobial peptide released by neutrophils?
Explanation
Question 14
A 12-year-old male baseball player presents with vague, activity-related right knee pain. Radiographs demonstrate a classic Osteochondritis Dissecans (OCD) lesion. Assuming the most common anatomic location for this lesion, which of the following best describes its position?
Explanation
Question 15
During a primary anterior cruciate ligament (ACL) reconstruction, the surgeon must decide on graft choice. From a purely biomechanical standpoint, which of the following common graft choices possesses the highest ultimate tensile load at the time of time zero testing?
Explanation
Question 16
In the manufacturing of highly cross-linked polyethylene (HXLPE) for total hip arthroplasty, the irradiation process creates free radicals that improve wear resistance but risk long-term oxidation and structural failure. To eliminate these free radicals, the material is often remelted or annealed. Which of the following mechanical properties is most significantly DECREASED as a direct result of this cross-linking and remelting process?
Explanation
Question 17
A 28-year-old female sustains a complete tear of her anterior cruciate ligament (ACL) and requires reconstruction. The pivot shift test is positive on examination. Which anatomic structure dynamically causes the visible 'clunk' or reduction of the tibia during the pivot shift maneuver as the knee is transitioned from extension to flexion?
Explanation
Question 18
A 35-year-old male with a history of a severe nickel allergy requires a primary total knee arthroplasty for post-traumatic osteoarthritis. Standard cobalt-chromium (CoCr) implants contain small amounts of nickel. To avoid a type IV hypersensitivity reaction, which of the following is the most appropriate alternative femoral component material?
Explanation
Question 19
A 19-year-old football player sustains a complex knee injury involving an acute grade III medial collateral ligament (MCL) tear and a complete ACL rupture. Based on current literature and sports medicine guidelines, what is the most broadly accepted initial treatment strategy for this combined injury?
Explanation
Question 20
A surgeon utilizes the direct anterior approach (DAA) for a total hip arthroplasty using the internervous plane between the tensor fasciae latae (TFL) and the sartorius. During deep dissection, a nerve passing over the anterior aspect of the iliacus muscle is at risk of iatrogenic traction injury. What is the clinical consequence of an injury to this specific nerve?
Explanation
Question 21
During a primary posterior-stabilized total knee arthroplasty (TKA), after the preliminary bone cuts have been made, trial components are placed. The surgeon notes that the joint is tight in 90 degrees of flexion but symmetric and well-balanced in full extension. Which of the following is the most appropriate next step to correct this mismatch?
Explanation

Question 22
A 68-year-old male is scheduled to undergo a total hip arthroplasty (THA). He previously underwent a T10-to-pelvis posterior spinal fusion. Which of the following describes the most likely spinopelvic kinematics when this patient transitions from a standing to a seated position, and what is the corresponding implication for acetabular component positioning?
Explanation
Question 23
When performing a medial patellofemoral ligament (MPFL) reconstruction, identifying the correct anatomic femoral attachment is critical to ensure anisometry is minimized. Radiographically, Schottle's point represents the ideal femoral origin. Which of the following best describes the radiographic location of Schottle's point on a true lateral radiograph of the knee?
Explanation

Question 24
A 55-year-old female presents with progressive groin pain 6 years after an uncomplicated metal-on-polyethylene total hip arthroplasty utilizing a modular titanium stem and a large-diameter cobalt-chromium head. Inflammatory markers are normal and an aspiration is negative for infection. MRI with MARS sequencing reveals a large, thick-walled cystic mass communicating with the joint. Serum ion levels show Cobalt is 8.5 ppb and Chromium is 1.1 ppb. What is the most likely pathophysiologic mechanism for her condition?
Explanation
Question 25
A 25-year-old male presents with a chief complaint of profound loss of knee flexion 8 months following an anterior cruciate ligament (ACL) reconstruction using a bone-patellar tendon-bone autograft. He states the knee feels 'locked' whenever he tries to bend it past 80 degrees.
Based on the radiographic principles of ACL graft placement, what is the most likely technical error leading to this specific complication?

Explanation
Question 26
A 62-year-old female presents with an audible and palpable 'catch' in her knee 14 months after a primary posterior-stabilized total knee arthroplasty. The catching occurs consistently when the knee moves from 45 degrees of flexion to 30 degrees of flexion during active extension. Range of motion is 0 to 120 degrees. Radiographs show well-fixed components with no signs of loosening. What is the anatomic basis for this phenomenon?
Explanation
Question 27
A 74-year-old female presents for revision total hip arthroplasty due to severe aseptic loosening of her acetabular component. Preoperative radiographs demonstrate more than 3 cm of superomedial migration of the cup. The teardrop is completely obliterated, and Kohler's line is crossed, indicating extensive medial wall destruction. Based on the Paprosky classification of acetabular defects, what is her defect type?
Explanation

Question 28
A 45-year-old female with a BMI of 32 presents with sudden onset posteromedial knee pain after stepping off a curb. She has no prior history of knee trauma.
MRI reveals a full-thickness radial tear of the medial meniscus at its posterior attachment to the tibia, with 4 mm of meniscal extrusion. Biomechanically, what is the consequence of this injury on the medial compartment?

Explanation
Question 29
According to the 2018 Musculoskeletal Infection Society (MSIS) / International Consensus Meeting (ICM) criteria, which of the following sets of synovial fluid laboratory values is the threshold for diagnosing a chronic periprosthetic joint infection in a total knee arthroplasty?
Explanation
Question 30
A 42-year-old male undergoes a primary THA using a ceramic-on-ceramic bearing. One year postoperatively, he complains of a loud, high-pitched squeaking noise coming from his hip when he walks, bend over, or performs deep squats. He denies pain. Radiographs demonstrate the acetabular cup is positioned in 60 degrees of inclination and 35 degrees of anteversion. What is the primary tribological mechanism leading to squeaking in this scenario?
Explanation
Question 31
A 28-year-old male sustains a high-energy multi-ligament knee injury following a motorcycle collision.
Clinical and MRI evaluation reveals a Schenck KD III-L injury (disruption of the ACL, PCL, and the posterolateral corner/LCL). He has intact pulses with normal ABIs. Which associated neurologic injury is most frequently seen with this specific ligamentous injury pattern?

Explanation
Question 32
A 70-year-old female experiences a catastrophic disruption of her patellar tendon 3 months following a revision total knee arthroplasty. Primary repair is deemed impossible due to poor tissue quality. The surgeon plans an extensor mechanism reconstruction using a synthetic mesh (e.g., Marlex mesh). During the procedure, what is the critical step regarding the positioning of the knee when tensioning and securing the mesh to ensure clinical success?
Explanation
Question 33
The direct anterior approach (DAA) to the hip is increasingly popular for primary THA due to its use of a true internervous and intermuscular plane. Which of the following accurately describes the superficial internervous plane utilized in the direct anterior approach?
Explanation
Question 34
A 22-year-old collegiate hockey player presents with chronic, insidious onset groin pain exacerbated by hip flexion and internal rotation.
Radiographs demonstrate an aspherical femoral head-neck junction with an alpha angle of 65 degrees. He is diagnosed with Cam-type femoroacetabular impingement (FAI). During hip arthroscopy, which pattern of intra-articular damage is most characteristically observed in isolated Cam FAI?

Explanation
Question 35
Understanding normal native knee kinematics is essential for optimizing total knee arthroplasty design. During normal active knee flexion from 0 degrees to 120 degrees, which of the following describes the characteristic motion of the tibiofemoral contact points in the axial plane?
Explanation
Question 36
An 82-year-old female sustains a mechanical fall 8 years following a primary cementless total hip arthroplasty.
Radiographs reveal a periprosthetic femur fracture that originates at the tip of the stem and extends proximally. The stem is visibly loose, migrating distally by 1 cm. The proximal femoral bone stock demonstrates substantial osteolysis but the diaphyseal bone distal to the fracture is robust. According to the Vancouver classification, what is the type of fracture and the most appropriate definitive management?

Explanation
Question 37
A 19-year-old female presents with recurrent episodes of lateral patellar dislocation. Conservative management with physical therapy and bracing has failed. Advanced imaging is obtained to assess risk factors for patellofemoral instability. Which of the following anatomic parameters is a primary indication for adding a tibial tubercle medialization osteotomy (e.g., Fulkerson osteotomy) to a medial patellofemoral ligament (MPFL) reconstruction?
Explanation
Question 38
A 65-year-old female requires a primary total knee arthroplasty for end-stage osteoarthritis. During her preoperative evaluation, she reports a severe, blistering skin reaction to cheap jewelry and watch bands. She believes she has a 'metal allergy'. According to the American Academy of Orthopaedic Surgeons (AAOS) guidelines, what is the most appropriate management regarding component selection?
Explanation
Question 39
A dual mobility cup is utilized in a 71-year-old male undergoing revision total hip arthroplasty for recurrent instability. Three years later, he presents with acute hip pain and shortening of the limb after a minor twisting injury. Radiographs show eccentric seating of the metallic femoral head within the acetabular cup, creating a 'bubble sign', but the large polyethylene bearing remains contained within the metal acetabular shell. What is the most specific complication unique to dual mobility bearings that has occurred?
Explanation

Question 40
A 40-year-old male manual laborer with symptomatic, isolated medial compartment knee osteoarthritis and a mechanical varus axis of 8 degrees is undergoing a medial opening-wedge high tibial osteotomy (HTO). To achieve optimal offloading of the diseased medial compartment without causing excessive lateral compartment overload, the mechanical axis should be corrected to pass through a specific anatomic coordinate on the tibial plateau. What is the standard target point for the mechanical axis post-correction?
Explanation
Question 41
An 18-year-old female collegiate soccer player sustains an anterior cruciate ligament (ACL) tear. She wishes to undergo reconstruction that offers the lowest rate of re-rupture to ensure she can return to high-demand sports. Which of the following graft choices is most statistically supported to minimize her risk of graft failure?
Explanation
Question 42
During a primary total knee arthroplasty, the surgeon assesses the gaps and finds the knee is well-balanced in extension but unacceptably tight in flexion. Which of the following intraoperative modifications will best address this imbalance without altering the extension gap?
Explanation
Question 43
A 65-year-old male presents 8 years post-total hip arthroplasty (metal-on-polyethylene bearing with a 36-mm cobalt-chrome head) with new-onset groin pain. Serum inflammatory markers are normal. MRI with metal artifact reduction shows a solid cystic mass adjacent to the hip joint. Joint aspiration yields cloudy fluid with a negative culture. What is the most likely diagnosis?
Explanation
Question 44
During a primary posterior-stabilized total knee arthroplasty, the surgeon checks the gap kinematics with trial components. The extension gap is perfectly balanced, but the flexion gap is excessively tight. Which of the following is the most appropriate surgical step to achieve a balanced knee?
Explanation
Question 45
A 68-year-old female presents with an inability to actively extend her knee 3 weeks after a primary total knee arthroplasty. Imaging reveals well-fixed components and a complete mid-substance patellar tendon rupture. What is the most reliable surgical treatment?
Explanation
Question 46
A 75-year-old male sustains a fall 5 years after receiving a primary cementless total hip arthroplasty. Radiographs demonstrate a displaced spiral fracture around the distal tip of the femoral stem. The stem has subsided 15 mm and appears loose. What is the Vancouver classification and appropriate management?
Explanation
Question 47
A 45-year-old male undergoes arthroscopy for a medial meniscus posterior root tear. Which of the following best describes the biomechanical consequence of this specific pathology if left untreated?
Explanation
Question 48
When performing a medial patellofemoral ligament (MPFL) reconstruction, anatomic femoral tunnel placement is critical to prevent graft anisometry. According to Schöttle, where is the ideal radiographic femoral attachment point?
Explanation
Question 49
A 62-year-old male with a metal-on-polyethylene total hip arthroplasty presents with new-onset groin pain. Radiographs show well-fixed components with no osteolysis. Serum cobalt levels are significantly elevated, while chromium levels are normal. An MRI with metal artifact reduction shows a cystic pseudotumor. What is the most likely diagnosis?
Explanation
Question 50
According to the 2018 International Consensus Meeting (ICM) criteria, which of the following is considered an absolute major criterion for the diagnosis of periprosthetic joint infection (PJI)?
Explanation
Question 51
In the context of anterior cruciate ligament (ACL) reconstruction, which of the following patients has the strongest indication for a concomitant lateral extra-articular tenodesis (LET) or anterolateral ligament (ALL) reconstruction?
Explanation
Question 52
A patient dislocates their total hip arthroplasty anteriorly during extension and external rotation. Which of the following component malpositions is most commonly associated with this specific direction of instability?
Explanation
Question 53
A 65-year-old female presents with an audible and palpable 'pop' in her knee when extending from a flexed position, 1 year after a posterior-stabilized total knee arthroplasty. What is the most likely etiology of this phenomenon?
Explanation
Question 54
Which of the following best describes the pathomechanics of pincer-type femoroacetabular impingement (FAI)?
Explanation
Question 55
A 24-year-old male sustains a multiligament knee injury resulting in a KD-III L classification (ACL, PCL, and posterolateral corner disruption). He is at highest risk for injury to which of the following neurovascular structures?
Explanation
Question 56
Manufacturers often add Vitamin E to highly cross-linked polyethylene (HXLPE) liners used in total hip arthroplasty. What is the primary biomaterial purpose of this addition?
Explanation
Question 57
Kinematic alignment in total knee arthroplasty aims to differ from traditional mechanical alignment primarily by doing which of the following?
Explanation
Question 58
When evaluating an osteochondritis dissecans (OCD) lesion of the medial femoral condyle, which of the following factors is the most reliable predictor of successful healing with non-operative management?
Explanation
Question 59
A 55-year-old female presents with persistent anterior groin pain exacerbated by active straight leg raise 6 months after a total hip arthroplasty. What is the most common iatrogenic cause of this condition?
Explanation
Question 60
Compared to traditional first-generation Autologous Chondrocyte Implantation (ACI), what is the primary technical advantage of Matrix-induced Autologous Chondrocyte Implantation (MACI)?
Explanation
Question 61
During open surgical repair of a chronic proximal hamstring avulsion, careful retractor placement is required to protect the sciatic nerve. Anatomically, what is the normal relationship of the sciatic nerve to the ischial tuberosity?
Explanation
Question 62
A patient with a history of severe contact dermatitis to cheap jewelry requires a total knee arthroplasty. To prevent a severe metal hypersensitivity reaction, the surgeon should utilize implants specifically avoiding which of the following elements?
Explanation
Question 63
The anterior cruciate ligament (ACL) is composed of two primary bundles. Which of the following statements correctly describes their biomechanical behavior during knee range of motion?
Explanation
Question 64
A 65-year-old male presents with new-onset right groin pain 5 years after an uncomplicated metal-on-polyethylene total hip arthroplasty. Inflammatory markers are normal. Aspiration yields cloudy fluid with negative cultures, but significantly elevated cobalt levels compared to chromium. What is the primary mechanism of failure?
Explanation
Question 65
In anterior cruciate ligament (ACL) reconstruction, which of the following autografts possesses the highest ultimate tensile load?
Explanation
Question 66
During a posterior-stabilized total knee arthroplasty, the surgeon uses spacer blocks and notes that both the flexion and extension gaps are excessively tight and symmetric. Which of the following is the most appropriate next step in balancing the knee?
Explanation
Question 67
A 70-year-old female is evaluated for a total hip arthroplasty (THA). Radiographs reveal a prior L2-S1 posterior spinal fusion. Standing and sitting lateral spinopelvic radiographs demonstrate a change in pelvic tilt of 5 degrees. Based on her spinopelvic biomechanics, what THA component positioning strategy is recommended to minimize dislocation risk?
Explanation
None
