ABOS Orthopedic Board Review: Bone Dysplasias, HO, GCRG, Gorham's Disease | Part 23
Key Takeaway
Orthopedic Board Review Part 23 covers key topics including metaphyseal dysplasia (Schmid, McKusick), heterotopic ossification (prophylaxis, excision, risk factors), giant cell reparative granuloma (jaw lesions, pathology, treatment), and Gorham's disease (vanishing bone, vascular pathology). This section provides essential knowledge for ABOS exam preparation.
Question 1
A 6-year-old child is diagnosed with Schmid type metaphyseal dysplasia. When discussing the natural history of the condition, the parents ask about the typical age of onset. Compared to other types of metaphyseal dysplasia, how does Schmid type typically present?
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly states that "Schmid-type is transmitted in autosomal dominant manner, and presents later than other types of metaphyseal dysplasia." This later presentation, often in childhood, is a distinguishing feature from types like McKusick, which can be recognized earlier due to more pronounced early childhood features. Options A, B, D, and E are inconsistent with the described presentation.
Question 2
A 1-year-old child with a confirmed diagnosis of metaphyseal dysplasia is experiencing recurrent episodes of pneumonia and persistent diarrhea. The parents are concerned about these ongoing health issues. Which of the following systemic complications are frequently associated with metaphyseal dysplasia in younger children?
View Answer & Explanation
Correct Answer: C
Rationale: The teaching case states that "The disease frequently associates with malabsorption, neutropenia and recurrent infections in younger children." The vignette describes symptoms consistent with these complications (recurrent pneumonia for infections, persistent diarrhea for malabsorption). Recognizing these systemic associations is critical for comprehensive management of patients with metaphyseal dysplasia. The other options are not mentioned as frequent associations in the provided text.
Question 3
A 3-year-old male presents with disproportionate short stature. Physical examination reveals short and pudgy hands, genu varum, and a prominent "rachitic rosary" along the costochondral junctions. Radiographs show metaphyseal shortening of the long bones and phalanges, with normal epiphyses. The family history indicates an autosomal recessive inheritance pattern for this condition.
View Answer & Explanation
Correct Answer: C
Rationale: McKusick type metaphyseal dysplasia, also known as cartilage-hair hypoplasia, is explicitly stated to be transmitted as an autosomal recessive trait. This is a key distinguishing feature of this specific type of metaphyseal dysplasia. Autosomal dominant inheritance (A) is characteristic of Schmid type metaphyseal dysplasia, which presents differently.
Question 4
A 5-year-old female presents with short stature and concerns about the appearance of her hands. On examination, her hands are noted to be short and "puffy." An anteroposterior radiograph of both hands is obtained, as shown. The radiograph demonstrates metaphyseal shortening of the metacarpals and phalanges.
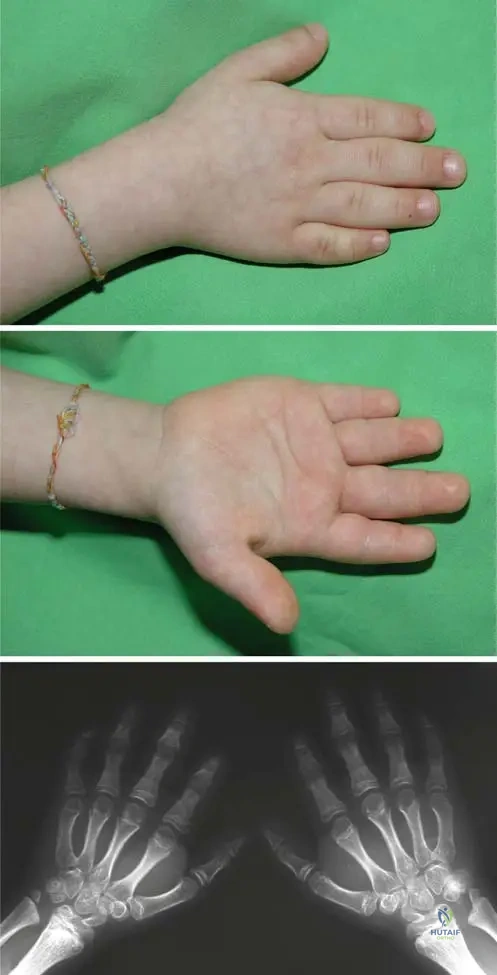
View Answer & Explanation
Correct Answer: C
Rationale: The clinical text explicitly states that "Short and pudgy hands and feet are the typical deformities" for McKusick type metaphyseal dysplasia. The image also visually supports the description of short and puffy hands. Normal hand appearance with wrist swelling (B) is more characteristic of Schmid type, which has milder upper extremity involvement.
Question 5
A 2-year-old male is evaluated for recurrent respiratory infections and short stature. Physical examination reveals a disproportionately short stature, genu varum, and palpable enlargements at the costochondral junctions. Radiographs confirm metaphyseal changes in the long bones. Which of the following terms describes the chest-wall involvement seen in this patient?
View Answer & Explanation
Correct Answer: C
Rationale: The teaching case states, "Chest-wall involvement with enlargement of costochondral junctions causes 'rachitic rosary'." This is a characteristic finding in McKusick type metaphyseal dysplasia. Pectus excavatum (A) and pectus carinatum (B) are different chest wall deformities not specifically mentioned as characteristic of this condition.
Question 6
A 4-year-old female presents with progressive bowing of her legs and short stature. Clinical examination reveals disproportionate short stature and varus deformity of both knees. Radiographs show metaphyseal irregularities in the distal femurs and proximal tibias. Which of the following lower extremity deformities is characteristic of McKusick type metaphyseal dysplasia?
View Answer & Explanation
Correct Answer: B
Rationale: The clinical context explicitly states that McKusick type metaphyseal dysplasia is characterized by "disproportionate short stature, with genu varum and varus ankle deformity." Genu valgum (A) is the opposite deformity. Coxa valga (D) is not mentioned as characteristic, while coxa vara is characteristic of Schmid type.
Question 7
A 6-year-old male is diagnosed with metaphyseal dysplasia. His parents are concerned about the genetic implications for future children. The patient exhibits disproportionate short stature, short and pudgy hands, and genu varum. Radiographs show metaphyseal shortening of tubular bones and normal epiphyses. Given these findings, which genetic inheritance pattern is most likely for this specific type of metaphyseal dysplasia?
View Answer & Explanation
Correct Answer: B
Rationale: The clinical features (disproportionate short stature, short and pudgy hands, genu varum) are classic for McKusick type metaphyseal dysplasia. The text clearly states, "McKusick type also called cartilage-hair hypoplasia, is transmitted as an autosomal recessive trait." Autosomal dominant (A) is characteristic of Schmid type, which has different clinical presentations.
Question 8
A 7-year-old male presents with disproportionate short stature, genu varum, and short, pudgy hands. Radiographs show metaphyseal irregularities of the long bones and phalanges. His presentation is contrasted with another patient who has metaphyseal dysplasia but presents with mild wrist swelling and elbow flexion contractures. Which of the following statements accurately differentiates the upper extremity involvement between McKusick type and Schmid type metaphyseal dysplasia?
View Answer & Explanation
Correct Answer: B
Rationale: The text states, "Short and pudgy hands and feet are the typical deformities" for McKusick type. In contrast, for Schmid type, it notes, "Upper extremity involvement is mild, evidenced by wrist swelling and flexion contractures of the elbows." Therefore, McKusick type has distinct, more pronounced hand deformities, while Schmid type has milder upper extremity issues.
Question 9
A 1-year-old infant is evaluated for failure to thrive and bowing of the legs. Radiographs of the lower extremities reveal characteristic changes in the metaphyses of the long tubular bones, with normal epiphyses. This radiographic pattern is typical for metaphyseal dysplasia. Which of the following best describes the primary radiographic finding in metaphyseal dysplasia?
View Answer & Explanation
Correct Answer: C
Rationale: The teaching case explicitly states, "Metaphyseal dysplasia is characterized by typical radiographical changes in the metaphyses of the short and long tubular bones, with normal epiphyses." This is the defining radiographic feature of the condition. Epiphyseal dysgenesis (A) would imply abnormal epiphyses, which is incorrect for metaphyseal dysplasia.
Question 10
A 9-month-old infant with disproportionate short stature and short, pudgy hands is diagnosed with McKusick type metaphyseal dysplasia. The parents report a history of recurrent infections and poor weight gain. Which of the following systemic associations is frequently observed in younger children with metaphyseal dysplasia, including the McKusick type?
View Answer & Explanation
Correct Answer: B
Rationale: The text states, "The disease frequently associates with malabsorption, neutropenia and recurrent infections in younger children." This is a general association with metaphyseal dysplasia, which includes the McKusick type. The other options are not mentioned as frequent associations in the provided text.
Question 11
A 3-year-old child with McKusick type metaphyseal dysplasia presents with a noticeable deformity of the ankles. On examination, the ankles appear to turn inward. Radiographs confirm metaphyseal changes and reveal distal fibular overgrowth. Which specific ankle deformity is characteristic of McKusick type metaphyseal dysplasia due to this overgrowth?
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly states that McKusick type is characterized by "genu varum and varus ankle deformity due to distal fibular overgrowth." This directly matches the clinical and radiographic findings described. Valgus ankle deformity (D) is the opposite of what is seen.
Question 12
A 5-year-old girl is brought to the clinic due to her short stature. Her height is significantly below the 3rd percentile, and her limbs appear disproportionately short compared to her trunk. Physical examination reveals short and pudgy hands and genu varum. Radiographs show metaphyseal irregularities. What is the characteristic type of short stature observed in McKusick type metaphyseal dysplasia?
View Answer & Explanation
Correct Answer: B
Rationale: The teaching case clearly states, "Disproportionate short stature is characteristic" of McKusick type metaphyseal dysplasia. This means the limbs are shorter in proportion to the trunk. Proportionate short stature (A) would imply all body parts are equally small.
Question 13
A genetic counselor is discussing the prevalence of McKusick type metaphyseal dysplasia with the parents of an affected child. The child presents with short stature, short and pudgy hands, and a "rachitic rosary." The parents are curious about the incidence of this condition in different populations. In which population is the incidence of McKusick type metaphyseal dysplasia notably higher?
View Answer & Explanation
Correct Answer: C
Rationale: The text specifically mentions, "In Amish population the incidence is 1/1,000 live births, but in other populations it is less frequent than the Schmidt type." This highlights a significantly higher incidence in the Amish population compared to others.
Question 14
A pediatrician is reviewing two cases of metaphyseal dysplasia. Patient A, a 6-month-old, presents with severe short stature, recurrent infections, and short, pudgy hands. Patient B, a 5-year-old, presents with milder short stature, wrist swelling, and coxa vara. Based on the typical presentation timing, which patient is more likely to have McKusick type metaphyseal dysplasia?
View Answer & Explanation
Correct Answer: C
Rationale: The text states, "Schmid-type is transmitted in autosomal dominant manner, and presents later than other types of metaphyseal dysplasia." This implies that McKusick type (one of the "other types") would present earlier. Patient A's younger age and severe presentation align with an earlier onset condition like McKusick type, while Patient B's later age and milder upper extremity involvement align with Schmid type.
Question 15
A 4-year-old child with disproportionate short stature is undergoing radiographic evaluation. Clinical examination reveals short and pudgy hands. An anteroposterior radiograph of the hands is obtained. What specific radiographic finding is expected in the hands of a patient with McKusick type metaphyseal dysplasia?

View Answer & Explanation
Correct Answer: C
Rationale: The caption for Fig. 1.25 (the provided image) explicitly states, "Anteroposterior radiograph (c) of both hands. Note the metaphyseal shortening of the metacarpals and phalanges." This is the characteristic radiographic finding in the hands for McKusick type metaphyseal dysplasia. Phalangeal lengthening (E) is the opposite of what is observed.
Question 16
A 2-year-old male is diagnosed with metaphyseal dysplasia based on clinical findings of short stature, genu varum, and radiographic evidence of metaphyseal irregularities in long bones. Which of the following skeletal structures is typically described as normal in metaphyseal dysplasia?
View Answer & Explanation
Correct Answer: C
Rationale: The teaching case states, "Metaphyseal dysplasia is characterized by typical radiographical changes in the metaphyses of the short and long tubular bones, with normal epiphyses." This is a defining characteristic of the condition. The metaphyses (A) are where the changes occur.
Question 17
A 10-year-old boy presents with decreased standing height primarily due to lower extremity involvement, including bowing of the tibia and femur, and a characteristic varus deformity of the hip. His upper extremities show only mild wrist swelling. This presentation is distinct from a younger child with short, pudgy hands and genu varum. Which specific hip deformity is characteristic of Schmid type metaphyseal dysplasia, but NOT typically of McKusick type?
View Answer & Explanation
Correct Answer: B
Rationale: The text states that Schmid type metaphyseal dysplasia presents with "characteristic coxa vara." This specific hip deformity is mentioned in the context of Schmid type and is not listed as a feature of McKusick type. Coxa valga (A) is the opposite deformity.
Question 18
A 7-year-old male is diagnosed with metaphyseal dysplasia. His presentation includes significant bowing of the tibia and femur, and a varus deformity of the knees and ankles. His upper extremity involvement is mild, with some wrist swelling. This clinical picture is consistent with Schmid type metaphyseal dysplasia. Which of the following is a characteristic lower extremity finding in Schmid type, distinguishing it from McKusick type?
View Answer & Explanation
Correct Answer: B
Rationale: The text describes Schmid type as having "bowing of tibia and femur, with characteristic coxa vara." While McKusick type has genu varum, the specific mention of bowing of the tibia and femur is a distinguishing feature of Schmid type. Distal fibular overgrowth (A) is characteristic of McKusick type, causing varus ankle deformity.
Question 19
A 1-year-old infant presents with short stature, recurrent infections, and radiographic evidence of metaphyseal changes in the long bones with normal epiphyses. The clinical picture is consistent with McKusick type. What is the broader category of skeletal disorders to which McKusick type belongs?
View Answer & Explanation
Correct Answer: C
Rationale: The title of the section is "1.2.4 Metaphyseal Dysplasia (McKusick Type)," and the introductory sentence states, "Metaphyseal dysplasia is characterized by typical radiographical changes in the metaphyses..." McKusick type is a specific form of metaphyseal dysplasia. Epiphyseal dysplasia (A) would involve the epiphyses, which are normal in metaphyseal dysplasia.
Question 20
A 3-year-old female with McKusick type metaphyseal dysplasia presents with a varus ankle deformity. Radiographs confirm metaphyseal changes and show a specific abnormality in the distal lower leg contributing to this deformity. What is the underlying anatomical cause of the varus ankle deformity in McKusick type?
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly states that McKusick type is characterized by "genu varum and varus ankle deformity due to distal fibular overgrowth." This directly identifies the cause of the ankle deformity. Fibular shortening (B) would likely lead to a different deformity or leg length discrepancy.
Question 21
A 6-month-old infant is referred for evaluation of short stature and unusual hand appearance. On physical examination, the infant's hands are observed to be short and "puffy." This finding, along with disproportionate short stature and a family history consistent with autosomal recessive inheritance, points towards McKusick type metaphyseal dysplasia. Which of the following best describes the typical clinical appearance of the hands in McKusick type metaphyseal dysplasia?

View Answer & Explanation
Correct Answer: C
Rationale: The text states, "Short and pudgy hands and feet are the typical deformities" for McKusick type metaphyseal dysplasia. The image also clearly depicts short and puffy hands. Normal in appearance (B) would be incorrect, as the hands are a key diagnostic feature.
Question 22
A 34-year-old male presents with progressive stiffness and pain in his right hip 3 months after sustaining a comminuted acetabular fracture treated with open reduction and internal fixation. Physical examination reveals a significant reduction in hip range of motion, particularly in flexion and abduction. Radiographs show mature bone formation bridging the acetabulum and proximal femur. Which of the following is the most appropriate initial medical management for this patient's condition?
View Answer & Explanation
Correct Answer: C
Rationale: Indomethacin, a non-steroidal anti-inflammatory drug (NSAID), is the most commonly used and effective medical prophylaxis for heterotopic ossification (HO) following trauma or surgery, particularly around the hip. It is thought to inhibit osteoblast differentiation and prostaglandin synthesis. High-dose corticosteroids are not indicated for HO prevention or treatment. Bisphosphonates have shown some efficacy in preventing HO in specific contexts but are not first-line. Calcitonin and methotrexate are not standard treatments for HO.
Question 23
A 28-year-old male sustained a severe traumatic brain injury (TBI) and multiple long bone fractures in a motor vehicle accident. Three weeks post-injury, he develops warmth, swelling, and decreased range of motion in his left elbow. Plain radiographs of the elbow are unremarkable. What is the most sensitive diagnostic test to detect early heterotopic ossification in this patient?
View Answer & Explanation
Correct Answer: C
Rationale: A three-phase technetium-99m bone scan is the most sensitive diagnostic test for detecting early, immature heterotopic ossification, often showing increased uptake in the soft tissues before it is visible on plain radiographs. While serum alkaline phosphatase can be elevated in HO, it is not specific and can be elevated for other reasons. C-reactive protein is an inflammatory marker. MRI can show soft tissue changes but is less specific for early HO than a bone scan. CT scans are excellent for visualizing mature HO and surgical planning but are not as sensitive for early, immature HO as a bone scan.
Question 24
A 65-year-old male undergoes a total hip arthroplasty (THA) for severe osteoarthritis. He has a history of previous HO formation after a prior hip surgery. To prevent recurrence of heterotopic ossification, which of the following prophylactic measures is most effective when initiated postoperatively?
View Answer & Explanation
Correct Answer: A
Rationale: Postoperative radiation therapy (XRT) with a single dose of 700-800 cGy, administered within 24-48 hours of surgery, is highly effective in preventing heterotopic ossification, especially in high-risk patients or after HO excision. While Indomethacin is also effective, the question asks for the *most* effective measure for a high-risk patient (history of previous HO). CPM does not prevent HO. Oral corticosteroids and low molecular weight heparin are not indicated for HO prophylaxis.
Question 25
A 45-year-old male with a C5 spinal cord injury sustained 6 months ago presents with progressive loss of motion and pain in his right shoulder. Radiographs confirm extensive heterotopic ossification around the glenohumeral joint, leading to near-complete ankylosis. The patient is otherwise stable and medically optimized. What is the most appropriate timing for surgical excision of the heterotopic ossification?
View Answer & Explanation
Correct Answer: C
Rationale: Surgical excision of heterotopic ossification is generally recommended only after the HO has matured. Radiographic maturity is indicated by corticalization and trabeculation of the HO, and biochemical maturity is suggested by normalization or plateauing of serum alkaline phosphatase levels. Operating on immature HO carries a significantly higher risk of recurrence. Waiting for maturity typically means waiting 6-12 months after the initial injury or onset of HO. Nerve compression is an indication for surgery, but the timing still depends on maturity. Early surgery increases recurrence risk.
Question 26
A 72-year-old female undergoes revision total hip arthroplasty. She has no prior history of heterotopic ossification. To minimize the risk of HO formation, the surgeon plans to administer a prophylactic agent. Which of the following is the most common and generally accepted first-line medical prophylaxis for HO in this setting?
View Answer & Explanation
Correct Answer: D
Rationale: Indomethacin is the most widely studied and commonly used NSAID for the prevention of heterotopic ossification following total hip arthroplasty. It is typically given for 3-6 weeks postoperatively. While other NSAIDs like Ibuprofen and Celecoxib (a COX-2 inhibitor) have also been used, Indomethacin has the strongest evidence base and is considered first-line. Etidronate is a bisphosphonate that has shown some efficacy but is not typically first-line over NSAIDs. Dexamethasone (a corticosteroid) is not used for HO prophylaxis.
Question 27
A 19-year-old male sustained a severe burn injury involving his right elbow. Over the past several weeks, he has developed progressive loss of elbow flexion and extension. Radiographs show extensive heterotopic ossification bridging the anterior aspect of the elbow joint. What is the primary mechanism by which NSAIDs like indomethacin prevent heterotopic ossification?
View Answer & Explanation
Correct Answer: C
Rationale: NSAIDs, including indomethacin, primarily prevent heterotopic ossification by inhibiting prostaglandin synthesis, specifically cyclooxygenase (COX) enzymes. Prostaglandins, particularly PGE2, play a crucial role in the inflammatory cascade that promotes osteoblast differentiation and subsequent bone formation in soft tissues. By inhibiting their synthesis, NSAIDs interfere with this process. They do not primarily inhibit osteoclast activity, suppress fibroblasts, have a direct cytotoxic effect on stem cells, or enhance bone resorption in this context.
Question 28
A 55-year-old male with a history of traumatic brain injury presents with a painful, stiff left knee. Radiographs reveal significant heterotopic ossification around the quadriceps mechanism, limiting knee flexion. The HO appears mature on radiographs. Which of the following is a contraindication to surgical excision of heterotopic ossification?
View Answer & Explanation
Correct Answer: B
Rationale: Immature heterotopic ossification is a strong contraindication to surgical excision because operating on immature HO significantly increases the risk of recurrence. Surgical excision should be delayed until the HO is radiographically and biochemically mature. A history of DVT is a risk factor for surgery but not a contraindication to HO excision itself. Neurological deficits are often associated with HO and are not a contraindication. Age and concomitant osteoarthritis are not contraindications.
Question 29
A 38-year-old male sustained a severe elbow dislocation with associated coronoid and radial head fractures. He underwent open reduction and internal fixation. To prevent heterotopic ossification, the surgeon considers postoperative radiation therapy. What is the typical timing for administering radiation prophylaxis for HO?
View Answer & Explanation
Correct Answer: C
Rationale: Postoperative radiation therapy for HO prophylaxis is most effective when administered within 24-72 hours of surgery. This timing targets the rapidly proliferating mesenchymal stem cells that are differentiating into osteoblasts before significant bone matrix is laid down. Preoperative radiation is also an option, but postoperative is more common. Delaying radiation beyond 72 hours significantly reduces its efficacy.
Question 30
A 22-year-old female with Fibrodysplasia Ossificans Progressiva (FOP) presents with a new flare-up characterized by painful swelling and stiffness in her neck and shoulder. She has a known genetic mutation. Which of the following genes is typically associated with Fibrodysplasia Ossificans Progressiva?
View Answer & Explanation
Correct Answer: C
Rationale: Fibrodysplasia Ossificans Progressiva (FOP) is a rare, autosomal dominant genetic disorder characterized by progressive heterotopic ossification. It is caused by a mutation in the ACVR1 (also known as ALK2) gene, which encodes for a bone morphogenetic protein (BMP) type I receptor. This mutation leads to a gain-of-function, making the receptor hyperactive and promoting aberrant bone formation. COL1A1 is associated with osteogenesis imperfecta. FGFR3 is associated with achondroplasia. SOX9 and RUNX2 are important transcription factors in chondrogenesis and osteogenesis, respectively, but are not the primary gene mutated in FOP.
Question 31
A 58-year-old male with a history of severe traumatic brain injury (TBI) and prolonged coma develops significant heterotopic ossification around his right knee, leading to a fixed flexion contracture. He is undergoing physical therapy, but his range of motion is severely limited. Which of the following is a recognized risk factor for the development of heterotopic ossification?
View Answer & Explanation
Correct Answer: C
Rationale: Traumatic brain injury (TBI) is a well-established and significant risk factor for the development of heterotopic ossification, particularly around large joints. Other major risk factors include spinal cord injury, severe burns, and certain types of orthopedic trauma or surgery (e.g., total hip arthroplasty, elbow trauma). Diabetes, chronic kidney disease, hypothyroidism, and osteoporosis are not recognized as primary risk factors for HO.
Question 32
A 40-year-old male sustained a severe open fracture of the distal humerus and underwent extensive surgical reconstruction. Two months postoperatively, he presents with increasing elbow stiffness and pain. Radiographs show early signs of heterotopic ossification anterior to the elbow joint. What is the Brooker classification system primarily used to grade?
View Answer & Explanation
Correct Answer: C
Rationale: The Brooker classification system is specifically used to grade the severity and extent of heterotopic ossification around the hip joint, typically after total hip arthroplasty or trauma. While HO can occur in other joints, the Brooker classification is not used for them. It is not related to elbow contractures, infection risk, TBI prognosis, or functional outcomes.
Question 33
A 68-year-old male undergoes total hip arthroplasty. He is considered high-risk for heterotopic ossification due to a history of hypertrophic osteoarthritis and prior HO in the contralateral hip. The surgeon decides to use postoperative radiation therapy. What is the typical single dose of radiation (in cGy) used for HO prophylaxis?
View Answer & Explanation
Correct Answer: C
Rationale: The most commonly used and effective single dose of radiation for heterotopic ossification prophylaxis is 700-800 cGy, administered within 24-72 hours postoperatively. This dose has been shown to be effective with minimal side effects. Lower doses may be less effective, and significantly higher single doses are generally not used for prophylaxis due to potential side effects.
Question 34
A 30-year-old male with a T10 spinal cord injury sustained 4 months ago develops progressive pain and swelling in his right knee. Physical examination reveals a warm, firm mass around the knee with significantly restricted range of motion. Radiographs show extensive heterotopic ossification. Which of the following laboratory findings would most likely be elevated in the early, active phase of heterotopic ossification?
View Answer & Explanation
Correct Answer: D
Rationale: Serum alkaline phosphatase (ALP) levels are often elevated during the active, early phase of heterotopic ossification, reflecting increased osteoblastic activity. While not specific to HO, a rising or elevated ALP in the appropriate clinical context can support the diagnosis and indicate active bone formation. ESR can be elevated due to inflammation but is less specific for HO. Serum calcium, phosphate, and PTH are typically normal in HO unless there are other underlying metabolic bone disorders.
Question 35
A 42-year-old male sustained a severe crush injury to his forearm, resulting in multiple fractures and soft tissue damage. He subsequently developed extensive heterotopic ossification around the elbow, leading to severe flexion contracture. He is now 9 months post-injury, and radiographs show mature HO. Surgical excision is planned. What is a common complication following surgical excision of heterotopic ossification, particularly in the elbow?
View Answer & Explanation
Correct Answer: B
Rationale: Ulnar nerve neuropathy is a common complication following surgical excision of heterotopic ossification around the elbow. The ulnar nerve is particularly vulnerable due to its superficial location in the cubital tunnel and its proximity to the HO mass. Careful identification and protection of the nerve are crucial during surgery. While other nerve palsies or vascular injuries can occur, ulnar nerve issues are particularly prevalent in elbow HO excision. Compartment syndrome is an acute post-traumatic or post-surgical complication, not typically a direct complication of HO excision itself.
Question 36
A 25-year-old male sustained a severe burn injury to his left arm and shoulder. Over the past 2 months, he has developed progressive stiffness and pain in his shoulder. Radiographs show early, immature heterotopic ossification around the glenohumeral joint. Which of the following is the most important non-pharmacological intervention in the early management of heterotopic ossification?
View Answer & Explanation
Correct Answer: C
Rationale: Gentle, active and passive range of motion exercises are crucial in the early management of heterotopic ossification. While HO cannot be "stretched away," maintaining joint motion helps prevent severe contractures and ankylosis. Complete immobilization can worsen stiffness. Aggressive passive stretching can exacerbate inflammation and potentially stimulate further HO formation. Cold therapy and ultrasound are not primary interventions for HO itself, though cold may help with inflammation. The goal is to preserve as much functional motion as possible without causing further trauma.
Question 37
A 60-year-old male with a history of severe acetabular fracture treated with ORIF 6 months prior presents with a painful, stiff hip. Radiographs show extensive heterotopic ossification (Brooker Class IV). He is otherwise healthy. What is the primary indication for surgical excision of heterotopic ossification?
View Answer & Explanation
Correct Answer: C
Rationale: The primary indication for surgical excision of heterotopic ossification is significant functional impairment (e.g., severe loss of range of motion limiting activities of daily living) or nerve/vascular compression. The mere radiographic presence of HO, cosmetic deformity, or elevated ALP levels are not sufficient indications for surgery. Surgery is a significant undertaking with risks, and it should only be performed when the benefits of improved function outweigh these risks. Patient request alone is not an indication without functional impairment.
Question 38
A 33-year-old male with a C6 spinal cord injury sustained 8 months ago presents with a painful, swollen left hip. Radiographs show extensive heterotopic ossification. He is currently taking indomethacin for prophylaxis. Which of the following is a common side effect of long-term NSAID use for HO prophylaxis that must be monitored?
View Answer & Explanation
Correct Answer: B
Rationale: Gastrointestinal ulceration and bleeding are well-known and common side effects of long-term NSAID use, including indomethacin, due to their inhibition of prostaglandin synthesis which protects the gastric mucosa. Patients on NSAIDs for HO prophylaxis require monitoring for GI symptoms and may need concomitant gastroprotective agents. While NSAIDs can affect renal function (leading to hyperkalemia in some cases) and rarely liver function, GI issues are the most common and significant concern. Hypoglycemia and bone marrow suppression are not typical side effects of NSAIDs.
Question 39
A 70-year-old female undergoes total hip arthroplasty. She has no specific risk factors for heterotopic ossification. The surgeon decides to use a prophylactic regimen. Which of the following is considered a relative contraindication to the use of NSAIDs for HO prophylaxis?
View Answer & Explanation
Correct Answer: C
Rationale: Active peptic ulcer disease is a relative contraindication to NSAID use due to the increased risk of gastrointestinal bleeding and perforation. NSAIDs inhibit prostaglandin synthesis, which is crucial for maintaining the integrity of the gastric mucosa. While age over 65 increases the risk of NSAID side effects, it's not an absolute contraindication. Hypertension, mild osteoarthritis, and previous appendectomy are not contraindications.
Question 40
A 29-year-old male sustained a severe open fracture of the tibia and fibula. He subsequently developed heterotopic ossification around the ankle joint, causing pain and limited dorsiflexion. The HO is radiographically mature. Which of the following cell types is primarily responsible for the formation of heterotopic ossification?
View Answer & Explanation
Correct Answer: D
Rationale: Heterotopic ossification is characterized by the aberrant differentiation of mesenchymal stem cells (MSCs) into osteoblasts and chondrocytes within soft tissues, leading to the formation of mature lamellar bone. These MSCs are typically found in perivascular niches or are recruited to sites of injury. Osteoclasts are involved in bone resorption. Chondrocytes are involved in cartilage formation, which can be an intermediate step in HO (endochondral ossification). Fibroblasts are involved in scar tissue formation. Macrophages are immune cells involved in inflammation.
Question 41
A 50-year-old male with a history of severe burns to his upper extremities develops progressive stiffness and pain in both elbows due to extensive heterotopic ossification. He is 1 year post-burn injury, and radiographs confirm mature HO. He is undergoing physical therapy. What is the primary goal of surgical excision of heterotopic ossification?
View Answer & Explanation
Correct Answer: D
Rationale: The primary goal of surgical excision of heterotopic ossification is to alleviate nerve or vascular compression and to improve functional range of motion, thereby enhancing the patient's quality of life and ability to perform activities of daily living. Complete eradication of all ectopic bone is often not achievable or necessary. While improving range of motion is a goal, restoration of *full, pain-free* range of motion is often unrealistic. Prevention of future HO formation is addressed by prophylaxis, not the excision itself. Reduction of ALP levels is a biochemical marker, not a surgical goal.
Question 42
A 45-year-old male develops new bone formation in the soft tissues surrounding his elbow following a complex fracture and surgical fixation. This process leads to significant stiffness and pain.
View Answer & Explanation
Correct Answer: C
Rationale: Heterotopic ossification (HO) is characterized by the formation of mature lamellar bone in non-osseous soft tissues. This process involves the differentiation of mesenchymal stem cells into osteoblasts, a classic example of metaplasia, where one mature cell type is replaced by another mature cell type. Hyperplasia refers to an increase in the number of cells, while neoplasia refers to uncontrolled, abnormal cell growth (tumor formation). Dysplasia refers to abnormal cell development or organization, and aplasia is the failure of an organ or tissue to develop.
Question 43
A 28-year-old male sustained a severe traumatic brain injury (TBI) and multiple long bone fractures in a motor vehicle accident. Six weeks post-injury, he develops progressive stiffness and decreased range of motion in his hips and shoulders, with palpable firm masses.
View Answer & Explanation
Correct Answer: B
Rationale: In patients with traumatic brain injury, the severity of the neurological injury, often quantified by a low Glasgow Coma Scale (GCS) score, is a significant risk factor for heterotopic ossification. Other risk factors include prolonged coma, spasticity, and associated long bone fractures. Early mobilization is generally beneficial and not a risk factor. Prophylactic antibiotics and normothermia are not directly linked to HO risk.
Question 44
A 35-year-old male with a T6 complete spinal cord injury sustained 3 months ago presents with swelling, warmth, and decreased range of motion in his right hip. Radiographs show early signs of new bone formation around the hip joint.
View Answer & Explanation
Correct Answer: C
Rationale: For patients with spinal cord injury (SCI), a complete SCI is a stronger predictor for the development of heterotopic ossification compared to an incomplete SCI. The severity of neurological deficit, spasticity, and autonomic dysreflexia are all associated with an increased risk of HO. Early rehabilitation is generally encouraged and not a risk factor. Corticosteroids are not typically used for HO prophylaxis and age over 60 is not a specific risk factor for SCI-related HO.
Question 45
A 60-year-old male undergoes a total hip arthroplasty (THA) for severe osteoarthritis. Postoperatively, he develops progressive hip stiffness. Radiographs show mature heterotopic bone formation bridging the joint.
View Answer & Explanation
Correct Answer: D
Rationale: Following total hip arthroplasty, the hip joint itself, specifically the periarticular soft tissues around the hip capsule and abductor muscles, is the most commonly affected anatomical location by heterotopic ossification. While HO can occur in other joints after trauma or surgery, the hip is the most frequent site of concern after THA.
Question 46
A 40-year-old male, 4 weeks after sustaining multiple fractures in a motor vehicle accident, complains of increasing pain, swelling, and warmth around his left elbow. He also notes a progressive loss of elbow range of motion.
View Answer & Explanation
Correct Answer: C
Rationale: The most common early clinical signs of heterotopic ossification are localized inflammation, presenting as erythema, swelling, warmth, and pain. These symptoms often precede significant radiographic changes and are indicative of the active, immature phase of HO formation. Progressive loss of joint range of motion is also a key symptom. Crepitus and joint instability are less common early signs, and numbness (nerve compression) is a later complication.
Question 47
A 55-year-old male, 2 weeks post-op from an acetabular fracture fixation, develops unexplained fever, localized warmth, and decreased hip range of motion. Initial plain radiographs are unremarkable.
View Answer & Explanation
Correct Answer: C
Rationale: Bone scintigraphy using Technetium-99m is the most sensitive imaging modality for detecting early, immature heterotopic ossification. It can show increased osteoblastic activity and uptake as early as 7-10 days post-injury, often before any changes are visible on plain radiographs. While MRI and CT can show soft tissue changes, they are less specific for early bone formation activity. Plain radiographs only become positive once the HO is sufficiently mineralized.
Question 48
A 70-year-old female, 6 months after a total hip arthroplasty, presents with severe hip stiffness. Plain radiographs reveal dense, well-corticated bone bridging the joint.
View Answer & Explanation
Correct Answer: C
Rationale: A CT scan is considered the gold standard for assessing the maturity and precise extent of heterotopic ossification, particularly when surgical excision is being planned. It provides detailed three-dimensional anatomical information, allows for accurate measurement of bone density (to confirm maturity), and helps delineate the relationship of the HO to neurovascular structures. Plain radiographs are useful for initial detection and grading but lack the detail of CT for surgical planning.
Question 49
A 50-year-old male is scheduled for a revision total hip arthroplasty, and he has a history of severe heterotopic ossification after his primary THA. The surgeon plans pharmacological prophylaxis.
View Answer & Explanation
Correct Answer: C
Rationale: Non-steroidal anti-inflammatory drugs (NSAIDs), particularly indomethacin, are the most commonly used pharmacological agents for prophylaxis against heterotopic ossification. They work by inhibiting prostaglandin synthesis, which plays a critical role in the inflammatory cascade leading to HO. Warfarin and aspirin are anticoagulants, prednisone is a corticosteroid (not primary HO prophylaxis), and gabapentin is for neuropathic pain.
Question 50
A 30-year-old male with a history of severe TBI and previous HO formation is undergoing open reduction and internal fixation of a complex elbow fracture. The surgeon plans to use prophylactic radiation.
View Answer & Explanation
Correct Answer: C
Rationale: For prophylactic radiation therapy to prevent heterotopic ossification, the optimal timing is typically within 24-72 hours postoperatively. This window allows the radiation to target the rapidly proliferating mesenchymal stem cells before they fully differentiate into osteoblasts and begin significant bone formation. Preoperative radiation can also be effective but is less common. Radiation administered much later postoperatively is less effective as HO formation is already underway.
Question 51
A 48-year-old male is prescribed indomethacin after an acetabular fracture fixation to prevent heterotopic ossification.
View Answer & Explanation
Correct Answer: B
Rationale: NSAIDs like indomethacin prevent heterotopic ossification primarily by inhibiting cyclooxygenase (COX) enzymes, thereby blocking the synthesis of prostaglandins. Prostaglandins, particularly PGE2, are potent mediators of inflammation and play a crucial role in the early stages of HO formation by promoting the differentiation of mesenchymal stem cells into osteoblasts. While NSAIDs may have some effect on stem cell differentiation, their main mechanism is through prostaglandin inhibition. Direct osteoclast inhibition is the primary mechanism of bisphosphonates.
Question 52
A 25-year-old male with a severe elbow injury developed extensive heterotopic ossification, severely limiting his range of motion. Radiographs show mature, well-corticated bone.
View Answer & Explanation
Correct Answer: C
Rationale: The general recommendation for the timing of surgical excision of heterotopic ossification is once the bone is radiographically mature. Maturity is indicated by dense, well-corticated bone on plain radiographs, often confirmed by a quiescent bone scan (no increased uptake). Operating on immature HO carries a significantly higher risk of recurrence. While waiting a year post-injury is a common guideline, the key factor is radiographic maturity, which can sometimes occur earlier or later.
Question 53
A 65-year-old male, 3 months after a total hip arthroplasty, has radiographs showing islands of bone within the soft tissues around the hip, but no bridging of the joint.
View Answer & Explanation
Correct Answer: B
Rationale: The Brooker classification system for heterotopic ossification around the hip is as follows: * Grade 0: No HO. * Grade I: Islands of bone within the soft tissues, but no functional bridging of the joint. * Grade II: Bone spurs from the pelvis or femur, leaving at least 1 cm between opposing surfaces. * Grade III: Bone spurs from the pelvis or femur, reducing the space between opposing surfaces to less than 1 cm. * Grade IV: Apparent bony ankylosis of the joint. Based on the description of "islands of bone within the soft tissues... but no bridging of the joint," this corresponds to Grade I.
Question 54
A 38-year-old male with extensive heterotopic ossification around his elbow after a severe fracture now presents with numbness and tingling in his hand, along the ulnar nerve distribution.
View Answer & Explanation
Correct Answer: C
Rationale: A common complication of significant heterotopic ossification, particularly around joints like the elbow (where the ulnar nerve is superficial), is nerve compression. The expanding mass of heterotopic bone can impinge upon adjacent nerves, leading to symptoms such as numbness, tingling, and weakness in the distribution of the affected nerve. Pathological fracture, joint infection, avascular necrosis, and DVT are less direct or common complications of HO itself.
Question 55
A 16-year-old athlete sustains a direct blow to his quadriceps muscle during a football game. Weeks later, he develops a painful, firm mass within the muscle. Radiographs show calcification.
View Answer & Explanation
Correct Answer: C
Rationale: Myositis Ossificans Traumatica (MOT) is a specific form of heterotopic ossification that occurs within muscle tissue, typically after direct trauma. While generalized HO can occur in various periarticular soft tissues (e.g., joint capsules, ligaments), MOT is specifically characterized by bone formation within the muscle belly. Both are benign, localized, and acquired conditions. Neither is infectious.
Question 56
A 55-year-old male undergoes surgical excision of mature heterotopic ossification around his elbow. He is at high risk for recurrence.
View Answer & Explanation
Correct Answer: C
Rationale: To minimize the risk of recurrence after surgical excision of heterotopic ossification, postoperative prophylaxis with either radiation therapy (usually a single dose within 24-72 hours) or NSAIDs (e.g., indomethacin for 3-6 weeks) is strongly recommended. These measures target the inflammatory and cellular processes that lead to HO formation. Immediate postoperative physical therapy is important for range of motion but does not prevent recurrence. Strict immobilization can actually contribute to stiffness and potentially HO formation.
Question 57
A 14-year-old female presents with a 4-month history of painless swelling of her anterior mandible. Clinical examination reveals a firm, non-tender expansion of the alveolar process. Radiographic imaging demonstrates a well-defined, expansile, multilocular radiolucent lesion in the symphyseal region, crossing the midline. There is no evidence of cortical breach or root resorption.
View Answer & Explanation
Correct Answer: C
Rationale: Giant cell reparative granuloma (GCRG) is a benign, non-neoplastic lesion most commonly found in the jaws, particularly the anterior mandible, often crossing the midline in adolescents and young adults. Its characteristic radiographic appearance is a well-defined, expansile, multilocular radiolucency. Ameloblastoma is typically seen in older patients and often in the posterior mandible, though it can be multilocular. Aneurysmal bone cyst can occur in the jaws but GCRG is more specific to this presentation and location.
Question 58
A 10-year-old male presents with a slowly enlarging, asymptomatic mass in his left maxilla. Intraoral examination shows a firm, non-tender swelling of the gingiva and alveolar bone. CT scan reveals an expansile, lytic lesion with thin cortical bone expansion in the anterior maxilla. Biopsy demonstrates numerous multinucleated giant cells, spindle-shaped stromal cells, and areas of hemorrhage and hemosiderin deposition.
View Answer & Explanation
Correct Answer: D
Rationale: The histological description of numerous multinucleated giant cells, spindle-shaped stromal cells, hemorrhage, and hemosiderin is classic for giant cell reparative granuloma (GCRG). The clinical presentation in a young patient with an expansile jaw lesion further supports this. Giant cell tumor of bone is rare in the jaws and typically occurs in epiphyses of long bones in older adults. Brown tumor would require evidence of hyperparathyroidism, and while histologically similar, the clinical context is key. Cherubism is a genetic condition with bilateral jaw involvement.
Question 59
A 22-year-old female undergoes incisional biopsy of an expansile, lytic lesion in her posterior mandible. Histopathological examination reveals a cellular lesion composed of numerous multinucleated giant cells uniformly distributed within a background of plump spindle-shaped stromal cells. Foci of hemorrhage and hemosiderin are noted. Which of the following is the most appropriate initial management strategy for this lesion, assuming a diagnosis of giant cell reparative granuloma?
View Answer & Explanation
Correct Answer: E
Rationale: For giant cell reparative granuloma (GCRG), the primary treatment is surgical curettage, often with adjunctive measures such as cryotherapy or chemical cautery (e.g., Carnoy's solution) to reduce recurrence rates. En bloc resection is generally reserved for aggressive or recurrent lesions due to its morbidity. Radiation and chemotherapy are not indicated for this benign lesion. Intralesional corticosteroids have been used in some cases, but curettage remains the mainstay of treatment.
Question 60
A 16-year-old male presents with a recurrent, expansile lesion in his anterior mandible, previously treated with curettage for giant cell reparative granuloma 18 months ago. The lesion is now larger and more aggressive radiographically. Which of the following factors is most strongly associated with recurrence of giant cell reparative granuloma?
View Answer & Explanation
Correct Answer: C
Rationale: Aggressive clinical behavior, rapid growth, and larger lesions are associated with a higher recurrence rate for giant cell reparative granuloma (GCRG). Younger age (under 20) is also often associated with more aggressive lesions and higher recurrence. Maxillary lesions can be more challenging to treat but are not inherently more recurrent than mandibular lesions. Hemorrhage is a common histological feature and not a specific predictor of recurrence. Unilocular lesions are generally less aggressive than multilocular ones.
Question 61
A 12-year-old girl is diagnosed with a giant cell reparative granuloma in her left posterior mandible. Prior to definitive surgical treatment, her pediatrician requests a consultation regarding potential systemic associations. Which of the following systemic conditions should be ruled out due to its potential to present with histologically similar lesions?
View Answer & Explanation
Correct Answer: C
Rationale: Brown tumors of hyperparathyroidism are histologically indistinguishable from giant cell reparative granulomas (GCRG) and other giant cell lesions. Therefore, it is crucial to rule out primary hyperparathyroidism by checking serum calcium, phosphorus, and parathyroid hormone (PTH) levels, especially in cases of multiple or unusual giant cell lesions. The other conditions listed do not typically present with giant cell lesions that mimic GCRG.
Question 62
A 19-year-old male presents with a 6-month history of progressive swelling of his right anterior maxilla. Radiographs show a well-defined, expansile radiolucent lesion. An incisional biopsy confirms giant cell reparative granuloma. Which of the following statements best describes the biological nature of giant cell reparative granuloma?
View Answer & Explanation
Correct Answer: B
Rationale: Giant cell reparative granuloma (GCRG) is widely considered a reactive lesion rather than a true neoplasm. It is thought to arise in response to local trauma, hemorrhage, or inflammation, leading to a reparative process involving giant cells. It has no metastatic potential and a very low risk of malignant transformation. It is not a hamartoma or an infectious granuloma.
Question 63
A 13-year-old female presents with a 2-month history of mild pain and swelling in her left posterior mandible. Panoramic radiograph reveals a unilocular, well-demarcated radiolucency with sclerotic borders, displacing the inferior alveolar nerve canal. Biopsy confirms giant cell reparative granuloma. What is the most common location for giant cell reparative granuloma in the jaws?
View Answer & Explanation
Correct Answer: C
Rationale: Giant cell reparative granuloma (GCRG) has a strong predilection for the jaws, with the anterior mandible (symphyseal and parasymphyseal regions) being the most common site. While it can occur in other parts of the jaws, including the posterior mandible and maxilla, the anterior mandible is classically described as its primary location, often crossing the midline.
Question 64
A 17-year-old male is diagnosed with an aggressive giant cell reparative granuloma in his anterior mandible, causing significant cortical expansion and root resorption of adjacent teeth. Surgical curettage is planned. Which of the following adjunctive therapies is commonly used during curettage to reduce the risk of recurrence?
View Answer & Explanation
Correct Answer: C
Rationale: Cryotherapy (using liquid nitrogen) is a common adjunctive therapy used during curettage of giant cell reparative granulomas (GCRG) to destroy residual cells and reduce the risk of recurrence. Other adjunctive measures include chemical cautery (e.g., Carnoy's solution). Systemic bisphosphonates are used for giant cell tumors of bone, not typically GCRG. The other options are not standard adjunctive therapies for GCRG.
Question 65
A 25-year-old female presents with a 9-month history of a slowly growing, firm mass in her anterior maxilla. Radiographs show a well-defined, expansile, unilocular radiolucency. Biopsy confirms giant cell reparative granuloma. Which of the following features, if present, would suggest a more aggressive variant of GCRG?
View Answer & Explanation
Correct Answer: C
Rationale: Aggressive giant cell reparative granulomas (GCRG) are characterized by rapid growth, larger size, cortical perforation, root resorption, and a higher tendency for recurrence. Unilocular appearance and absence of pain are typically associated with less aggressive lesions. While GCRG can occur in the maxilla and in patients over 25, these factors alone do not define an aggressive variant as strongly as rapid growth and cortical destruction.
Question 66
A 15-year-old male is diagnosed with a giant cell reparative granuloma in his anterior mandible. He has no other medical conditions. Which of the following genetic syndromes is NOT typically associated with multiple giant cell lesions in the jaws?
View Answer & Explanation
Correct Answer: C
Rationale: Cherubism, Noonan syndrome, Jaffe-Campanacci syndrome, and Ramon syndrome (a variant of Cherubism) are all associated with multiple giant cell lesions in the jaws, often histologically similar to giant cell reparative granuloma. Neurofibromatosis Type 2 is primarily associated with schwannomas and meningiomas, not giant cell lesions of the jaws.
Question 67
A 10-year-old girl presents with a firm, non-tender swelling of her right anterior maxilla. Radiographic imaging shows an expansile, multilocular radiolucent lesion. An incisional biopsy is performed. Histologically, the lesion shows numerous multinucleated giant cells, spindle cell stroma, and areas of hemorrhage. Which of the following immunohistochemical markers is typically NOT helpful in distinguishing giant cell reparative granuloma from other giant cell lesions?
View Answer & Explanation
Correct Answer: A
Rationale: CD68 is a marker for macrophages and histiocytes, and it will be positive in the multinucleated giant cells of giant cell reparative granuloma (GCRG), giant cell tumor of bone (GCTB), and brown tumor, making it non-specific for differentiation. H3.3 G34W mutation is a specific marker for giant cell tumor of bone, which is typically negative in GCRG. p63 is positive in the stromal cells of GCTB but less consistently in GCRG. Vimentin and alpha-1-antitrypsin are generally positive in the stromal cells of GCRG but are not highly specific for distinguishing it from other giant cell lesions in the way H3.3 G34W is for GCTB.
Question 68
A 16-year-old male presents with a 3-month history of painless swelling in his left anterior mandible. Panoramic radiograph reveals a well-defined, expansile, multilocular radiolucent lesion. The patient's serum calcium and PTH levels are within normal limits. An incisional biopsy confirms giant cell reparative granuloma. What is the most appropriate long-term follow-up strategy for this patient after successful surgical curettage?
View Answer & Explanation
Correct Answer: C
Rationale: Giant cell reparative granuloma (GCRG) has a recurrence rate ranging from 10-20%, particularly for aggressive lesions or in younger patients. Therefore, regular follow-up is essential. Bi-annual (every 6 months) clinical and radiographic examination for at least 3-5 years is generally recommended to detect any recurrence early. Annual follow-up for 1-2 years might be insufficient for some cases, while lifelong surveillance is typically excessive for a benign lesion.
Question 69
A 20-year-old female presents with a 5-month history of a slowly enlarging mass in her anterior mandible. Radiographs show an expansile, multilocular radiolucency. Biopsy reveals features consistent with giant cell reparative granuloma. Which of the following is a key histological feature that helps differentiate GCRG from a true giant cell tumor of bone (GCTB)?
View Answer & Explanation
Correct Answer: C
Rationale: Abundant hemorrhage, hemosiderin deposition, and reactive bone formation are characteristic features of giant cell reparative granuloma (GCRG) and are less prominent or absent in true giant cell tumors of bone (GCTB). While both lesions have multinucleated giant cells and a spindle cell stroma, in GCTB, the giant cells are typically more uniformly distributed and numerous, and the stromal cells are neoplastic. The stromal cells in GCRG are reactive. Osteoid formation is not a primary differentiating feature.
Question 70
A 12-year-old boy is diagnosed with a giant cell reparative granuloma in his right maxilla. The lesion is causing displacement of developing tooth buds. The parents are concerned about the potential for future dental complications. Which of the following is a common dental complication associated with giant cell reparative granuloma in the jaws?
View Answer & Explanation
Correct Answer: C
Rationale: Giant cell reparative granuloma (GCRG), being an expansile lesion within the bone, commonly causes displacement of adjacent teeth and resorption of their roots. It can also interfere with the eruption of permanent teeth. The other options are not typically associated complications of GCRG.
Question 71
A 17-year-old female presents with a 4-month history of a slowly enlarging, firm swelling of her left anterior mandible. Radiographs show a well-defined, expansile, multilocular radiolucency. An incisional biopsy is performed, confirming giant cell reparative granuloma. Which of the following is the most appropriate initial imaging modality for evaluating the extent of a suspected giant cell reparative granuloma in the jaws?
View Answer & Explanation
Correct Answer: A
Rationale: Plain radiographs, such as panoramic views for the entire mandible and maxilla, and periapical views for specific tooth-related details, are the initial and most common imaging modalities for evaluating suspected jaw lesions like giant cell reparative granuloma (GCRG). They provide good detail of bone changes, lesion boundaries, and relationship to teeth. CT scans are often used for more detailed assessment of cortical integrity and soft tissue extension, but plain radiographs are typically the first step. MRI is excellent for soft tissue but less specific for initial bone architecture. PET and bone scans are generally for metastatic workup or metabolic activity, not initial diagnosis of benign jaw lesions. Ultrasound has limited utility for intraosseous lesions.
Question 72
A 14-year-old male presents with a recurrent giant cell reparative granuloma in his anterior mandible, despite two previous curettages with adjunctive cryotherapy. The lesion is now causing significant bone destruction and tooth loss. Which of the following treatment options might be considered for this aggressive, recurrent lesion?
View Answer & Explanation
Correct Answer: C
Rationale: For aggressive, recurrent giant cell reparative granulomas (GCRG) that have failed conservative surgical approaches, en bloc resection (radical excision) may be considered, especially if the lesion is causing significant morbidity and bone destruction. Observation is not appropriate for a recurrent, aggressive lesion. Systemic bisphosphonates are not standard for GCRG. Radiation therapy is generally avoided due to the risk of malignant transformation in benign lesions, especially in young patients. Intralesional calcitonin has been explored but is not a primary treatment for aggressive recurrence.
Question 73
A 19-year-old female is diagnosed with a giant cell reparative granuloma in her left posterior mandible. The lesion is asymptomatic and appears as a well-defined, unilocular radiolucency on panoramic radiograph. Given the benign nature of GCRG, what is the primary goal of surgical treatment?
View Answer & Explanation
Correct Answer: C
Rationale: The primary goals of surgical treatment for giant cell reparative granuloma (GCRG) are to completely remove the lesion, preserve adjacent vital structures (e.g., teeth, nerves), and prevent recurrence. While cosmetic improvement may be a secondary benefit, it's not the primary goal. GCRG has a very low risk of malignant transformation, so prevention is not a primary concern. It is not a tumor in the neoplastic sense, and chemotherapy is not indicated.
Question 74
A 15-year-old male presents with a 6-month history of a slowly enlarging, painless swelling in his anterior mandible. Radiographs show a well-defined, expansile, multilocular radiolucency. Biopsy confirms giant cell reparative granuloma. Which of the following cell types is considered the neoplastic or proliferative component in a true giant cell tumor of bone, but is merely reactive in giant cell reparative granuloma?
View Answer & Explanation
Correct Answer: C
Rationale: In giant cell tumor of bone (GCTB), the spindle-shaped mononuclear stromal cells are considered the neoplastic component, and they are responsible for the proliferation and production of osteoclast-activating factors that lead to the formation of multinucleated giant cells. In contrast, in giant cell reparative granuloma (GCRG), the stromal cells are reactive fibroblasts or myofibroblasts, and the multinucleated giant cells are thought to be reactive osteoclast-like cells. The giant cells themselves are generally considered reactive in both lesions, but their proliferation is driven by the stromal cells.
Question 75
A 13-year-old female is diagnosed with a giant cell reparative granuloma in her anterior mandible. The lesion is relatively small and asymptomatic. Her parents are hesitant about immediate surgery. Which of the following non-surgical treatment modalities has shown some promise in managing smaller, less aggressive giant cell reparative granulomas?
View Answer & Explanation
Correct Answer: B
Rationale: Intralesional corticosteroid injections have been reported as a non-surgical treatment option for smaller, less aggressive giant cell reparative granulomas (GCRG), particularly in cases where surgery might be challenging or in very young patients. The mechanism is thought to involve inhibition of osteoclast activity and inflammation. Systemic corticosteroids are not typically used for GCRG. Oral NSAIDs provide symptomatic relief but do not treat the lesion. Antibiotics are for infection, and bisphosphonates are not standard for GCRG.
Question 76
A 16-year-old male presents with a 5-month history of a slowly enlarging, firm swelling in his left anterior mandible. Radiographs show an expansile, multilocular radiolucency. An incisional biopsy confirms giant cell reparative granuloma. Which of the following is the most important factor in preventing recurrence of giant cell reparative granuloma after surgical treatment?
View Answer & Explanation
Correct Answer: C
Rationale: The most critical factor in preventing recurrence of giant cell reparative granuloma (GCRG) is the completeness of lesion removal during surgery. Incomplete curettage leaves residual cells that can lead to recurrence. While factors like patient age (younger patients have higher recurrence) and lesion size/aggressiveness can influence recurrence rates, thorough surgical excision is paramount. Post-operative medications or lesion location are less impactful than the completeness of removal.
Question 77
A 14-year-old male presents with a several-month history of painless swelling in his left distal phalanx. Radiographs reveal a well-defined, expansile, lytic lesion within the bone, without significant periosteal reaction. Biopsy shows numerous multinucleated giant cells within a spindle cell stroma, associated with areas of hemorrhage and hemosiderin deposition. Which of the following best describes the nature of this lesion?
View Answer & Explanation
Correct Answer: B
Rationale: Giant cell reparative granuloma (GCRG) is widely considered a benign, reactive lesion rather than a true neoplasm. It is often associated with a history of trauma or hemorrhage, which is thought to initiate the reparative process. The histological findings described are classic for GCRG. Option A is incorrect as GCRG is benign. Options C, D, and E describe other types of lesions not consistent with GCRG.
Question 78
A 10-year-old girl presents with a slowly enlarging, firm mass in her right hand. Radiographs demonstrate an expansile, lytic lesion involving the metacarpal shaft. Histological examination confirms a giant cell reparative granuloma. While GCRG can occur in various locations, which of the following is considered one of the most common sites for this lesion, particularly in the craniofacial region?
View Answer & Explanation
Correct Answer: C
Rationale: Giant cell reparative granuloma (GCRG) is most commonly found in the jaw bones, particularly the mandible and maxilla, where it is often referred to as central giant cell granuloma. While it can occur in the small bones of the hands and feet (as in the vignette), the jaw bones are the most classic location. The other options are less common sites for GCRG.
Question 79
A 16-year-old male presents with mild pain and swelling in his left foot. Radiographs reveal a well-circumscribed, expansile, lytic lesion in the third metatarsal, with a "soap-bubble" appearance. There is no evidence of periosteal reaction or cortical breach. Based on the clinical and radiographic findings, a giant cell reparative granuloma is suspected. Which of the following is a characteristic radiographic feature of GCRG?
View Answer & Explanation
Correct Answer: C
Rationale: Giant cell reparative granuloma typically presents radiographically as a well-defined, expansile lytic lesion. It can be unilocular or multilocular, with the latter sometimes described as having a "soap-bubble" appearance. Sclerotic margins (A) are not typical, nor is aggressive periosteal reaction (B), sunburst pattern (D), or a predominantly sclerotic appearance (E).
Question 80
A 12-year-old female undergoes biopsy for an expansile lytic lesion in her proximal phalanx of the thumb. The pathologist describes a lesion characterized by a proliferation of spindle-shaped stromal cells, numerous multinucleated giant cells, areas of hemorrhage, and hemosiderin deposition. These findings are consistent with a giant cell reparative granuloma. What is the primary cellular component that gives this lesion its name?
View Answer & Explanation
Correct Answer: C
Rationale: The defining histological feature of a giant cell reparative granuloma, and indeed what gives it its name, is the presence of numerous multinucleated giant cells (osteoclast-like cells) within a background of spindle-shaped stromal cells. While fibroblasts (D) and osteoblasts (A) may be present in the reactive bone formation, they are not the primary defining cellular component. Chondrocytes (B) and plasma cells (E) are not characteristic.
Question 81
A 9-year-old boy presents with pain and swelling in his left distal radius. Radiographs show an expansile, lytic lesion with cortical thinning. MRI reveals fluid-fluid levels within the lesion. Biopsy is performed, and the pathologist notes numerous multinucleated giant cells, spindle cell stroma, and areas of hemorrhage, but also large blood-filled cystic spaces. Which of the following is the most important differential diagnosis to consider given these findings, especially the fluid-fluid levels?
View Answer & Explanation
Correct Answer: C
Rationale: The presence of fluid-fluid levels on MRI is highly suggestive of an aneurysmal bone cyst (ABC). Both GCRG and ABC contain multinucleated giant cells and hemorrhage, making their differentiation challenging, sometimes requiring careful histological assessment for the characteristic large, blood-filled cystic spaces of ABC. Osteosarcoma (A) and Ewing sarcoma (B) are malignant and typically have more aggressive radiographic features. NOF (D) and SBC (E) generally have different histological and radiographic appearances.
Question 82
A 25-year-old woman presents with knee pain and a lytic lesion in the epiphysis of her distal femur, extending into the metaphysis. Biopsy reveals numerous multinucleated giant cells. The pathologist notes that the giant cells are uniformly distributed and very numerous, with prominent nuclei, and the stromal cells are plump and ovoid. While giant cell reparative granuloma is in the differential, what other lesion, typically found in skeletally mature patients and often epiphyseal, must be carefully distinguished histologically?
View Answer & Explanation
Correct Answer: C
Rationale: Giant cell tumor (GCT) is a critical differential diagnosis for giant cell reparative granuloma (GCRG), especially in older patients and when the lesion is epiphyseal. Histologically, GCT typically shows a more uniform distribution of very numerous, larger giant cells with prominent nuclei, and the stromal cells are neoplastic and plump. In contrast, GCRG giant cells are often smaller, less numerous, and more clustered around areas of hemorrhage, with a more reactive spindle cell stroma. Chondroblastoma (A) is also epiphyseal but has chondroid matrix. Fibrous dysplasia (B), osteoid osteoma (D), and enchondroma (E) have distinct histological features.
Question 83
A 13-year-old boy is diagnosed with a giant cell reparative granuloma in his calcaneus after presenting with heel pain. The lesion is well-defined and expansile. After confirming the diagnosis with biopsy, what is generally considered the primary surgical treatment for symptomatic or progressive giant cell reparative granuloma?
View Answer & Explanation
Correct Answer: C
Rationale: For most giant cell reparative granulomas, especially in non-critical locations, intralesional curettage is the primary surgical treatment. This involves scraping out the lesion from within the bone. Wide en bloc resection (A) is typically reserved for aggressive or recurrent lesions, or those in anatomically challenging areas. Amputation (B), radiation therapy (D), and chemotherapy (E) are not standard treatments for benign GCRG.
Question 84
A 7-year-old girl develops a giant cell reparative granuloma in her distal phalanx following a crush injury to her finger. This clinical scenario highlights a common hypothesis regarding the etiology of GCRG. Which of the following is most strongly implicated in the pathogenesis of giant cell reparative granuloma?
View Answer & Explanation
Correct Answer: C
Rationale: Giant cell reparative granuloma is widely believed to be a reactive process, often triggered by trauma or hemorrhage. The lesion represents an exuberant reparative response to local injury. This is supported by its histological features (hemorrhage, hemosiderin, reactive bone) and clinical associations. Genetic mutations (A), chronic infections (B), autoimmune responses (D), and nutritional deficiencies (E) are not considered primary etiological factors for GCRG.
Question 85
A 15-year-old boy is diagnosed with a giant cell reparative granuloma of the calcaneus. He has no significant past medical history. Considering the typical demographics for this lesion, which age group is most commonly affected by giant cell reparative granuloma?
View Answer & Explanation
Correct Answer: B
Rationale: Giant cell reparative granuloma predominantly affects children and young adults, typically under the age of 20. This demographic profile is consistent with its reactive nature, often following trauma. While it can occur at any age, it is much less common in older adults or infants. This helps differentiate it from other giant cell-rich lesions like Giant Cell Tumor, which peaks in the 3rd-4th decades.
Question 86
A 10-year-old girl presents with a painful, swollen finger. Radiographs show an expansile, lytic lesion in the proximal phalanx. Biopsy confirms giant cell reparative granuloma. While the jaw bones are a classic site, GCRG is also relatively common in which other specific anatomical region, as illustrated by this case?
View Answer & Explanation
Correct Answer: C
Rationale: Beyond the jaw bones, the small bones of the hands and feet (phalanges, metacarpals, metatarsals) are the next most common sites for giant cell reparative granuloma. The vignette directly describes a lesion in the proximal phalanx, fitting this pattern. The other listed locations are much less common for GCRG.
Question 87
A 19-year-old male has a lytic lesion in his distal tibia. Histological examination reveals numerous multinucleated giant cells. To differentiate giant cell reparative granuloma from a true giant cell tumor (GCT), the pathologist carefully examines the giant cells and stromal cells. Which of the following histological features is more characteristic of GCRG compared to GCT?
View Answer & Explanation
Correct Answer: C
Rationale: In giant cell reparative granuloma, the multinucleated giant cells are often smaller, less numerous, and tend to be clustered around areas of hemorrhage or hemosiderin deposition, with a more reactive spindle cell stroma. In contrast, giant cell tumor (GCT) typically shows a more uniform distribution of very numerous, larger giant cells with prominent nucleoli (A), and the stromal cells are neoplastic and plump (B). High mitotic activity (D) is more concerning for malignancy, and osteoid matrix (E) suggests an osteoblastic lesion.
Question 88
A 14-year-old girl underwent curettage for a giant cell reparative granuloma in her calcaneus. Six months later, she presents with recurrent pain and swelling at the same site, and follow-up radiographs show enlargement of the previously treated lesion. What is the approximate recurrence rate for giant cell reparative granuloma after intralesional curettage?
View Answer & Explanation
Correct Answer: C
Rationale: While generally benign, giant cell reparative granuloma can recur after intralesional curettage, with reported recurrence rates typically ranging from 10% to 20%. Incomplete removal of the lesion is a common reason for recurrence. Higher recurrence rates (D, E) are more typical of aggressive giant cell tumors, while very low rates (A, B) are less common for GCRG.
Question 89
A 17-year-old male presents with a recurrent giant cell reparative granuloma in his distal phalanx, 18 months after initial curettage. The lesion is symptomatic and progressively enlarging. What is the most appropriate next step in management for a recurrent, symptomatic GCRG?
View Answer & Explanation
Correct Answer: B
Rationale: For recurrent, symptomatic giant cell reparative granuloma, repeat intralesional curettage is often the next step. Adjuvant therapies such as bone grafting, phenol, or cryotherapy may be considered to reduce recurrence risk, especially in challenging locations. Observation (A) is not appropriate for a symptomatic, enlarging recurrence. Amputation (D) is overly aggressive for a benign lesion. Chemotherapy (C) and radiation therapy (E) are not standard treatments for GCRG due to its benign nature and potential side effects.
Question 90
A 10-year-old boy presents with a several-month history of a slowly growing, firm mass in his left foot. Radiographs show a well-defined, expansile lytic lesion in the cuboid bone, causing significant cortical thinning but no breach. This expansile nature is a common feature of giant cell reparative granuloma. What does this expansile growth pattern imply about the lesion's interaction with the bone cortex?
View Answer & Explanation
Correct Answer: B
Rationale: The expansile nature of giant cell reparative granuloma indicates a slow, continuous growth that causes remodeling and thinning of the cortical bone from within, rather than rapid destruction or invasion. This is characteristic of many benign, slow-growing intraosseous lesions. Rapid destruction (A) or invasion (D) would suggest a more aggressive or malignant process. Formation of new bone on the outer surface (C) is periosteal reaction, and complete replacement (E) is not typical for an expansile benign lesion.
Question 91
A 45-year-old woman with a history of chronic kidney disease and secondary hyperparathyroidism presents with a lytic lesion in her distal radius. Biopsy reveals numerous multinucleated giant cells, spindle cell stroma, and areas of hemorrhage. While giant cell reparative granuloma is a consideration, what other giant cell-rich lesion, directly related to her systemic condition, must be ruled out?
View Answer & Explanation
Correct Answer: C
Rationale: A Brown tumor is a focal lesion of bone caused by excessive osteoclastic activity due to hyperparathyroidism. Histologically, it is rich in multinucleated giant cells and can be indistinguishable from giant cell reparative granuloma without clinical context and biochemical evaluation (parathyroid hormone, calcium, phosphate levels). Given the patient's history of chronic kidney disease and secondary hyperparathyroidism, a Brown tumor is a critical differential diagnosis. The other options are not directly related to hyperparathyroidism or have distinct histological features.
Question 92
A 6-year-old boy presents with a painful, swollen finger after falling off his bicycle a month prior. Radiographs show an expansile lytic lesion in the proximal phalanx. Biopsy confirms giant cell reparative granuloma. The temporal relationship between the injury and the lesion's presentation supports which aspect of GCRG's pathogenesis?
View Answer & Explanation
Correct Answer: C
Rationale: The history of trauma preceding the development of the lesion strongly supports the theory that giant cell reparative granuloma is a reactive process, often initiated by local injury or hemorrhage. This is a key aspect of its pathogenesis, distinguishing it from true neoplasms. Options A, B, D, and E are inconsistent with the current understanding of GCRG etiology.
Question 93
A 13-year-old girl presents with a firm, non-tender swelling of her left ring finger. Radiographs show a well-defined, expansile, lytic lesion involving the entire proximal phalanx. There is no periosteal reaction. A biopsy is performed, confirming giant cell reparative granuloma. Which of the following bones is most commonly affected by GCRG in the appendicular skeleton?
View Answer & Explanation
Correct Answer: D
Rationale: While the jaw bones are the most common overall site, in the appendicular skeleton, giant cell reparative granulomas are most frequently found in the small tubular bones of the hands and feet, particularly the phalanges, metacarpals, and metatarsals. The vignette itself describes a lesion in the proximal phalanx, which is a classic location. The long bones (A, B, C) and pelvis (E) are much less common sites for GCRG.
Question 94
A 10-year-old boy is diagnosed with a giant cell reparative granuloma in his mandible. The lesion is small, asymptomatic, and discovered incidentally. While surgical curettage is a common treatment, what non-surgical management option has shown some efficacy, particularly for jaw lesions, and might be considered for an asymptomatic, stable lesion?
View Answer & Explanation
Correct Answer: B
Rationale: For giant cell reparative granulomas, especially in the jaw, intralesional steroid injections have been reported to be effective in some cases, leading to regression of the lesion. This can be an alternative to surgery, particularly for smaller or asymptomatic lesions, or in anatomically challenging areas. Observation (E) could also be considered for asymptomatic, stable lesions, but steroid injections offer an active non-surgical intervention. Antibiotics (A), bisphosphonates (C), and radiation (D) are not standard treatments for GCRG.
Question 95
A 7-year-old boy presents with a lytic lesion in his distal tibia. Radiographs show a well-defined, eccentric, lytic lesion with a sclerotic rim, located in the metaphysis. Histology reveals spindle cells, giant cells, and areas of hemorrhage. While GCRG is a consideration, what other common benign lytic lesion in children, often with a similar radiographic appearance (eccentric, sclerotic rim), should be included in the differential diagnosis?
View Answer & Explanation
Correct Answer: C
Rationale: Non-ossifying fibroma (NOF), also known as fibrous cortical defect, is a very common benign lesion in children, typically found eccentrically in the metaphysis of long bones (like the distal tibia) and characterized by a well-defined lytic appearance with a sclerotic rim. While histologically different (NOF has storiform fibrous tissue and fewer, smaller giant cells), its radiographic presentation can overlap with GCRG, especially in the differential for lytic lesions in children. Osteosarcoma (A) and Ewing sarcoma (B) are malignant. SBC (D) is typically centrally located and lacks a sclerotic rim. Osteoid osteoma (E) is sclerotic with a nidus.
Question 96
A 25-year-old male presents with progressive pain and swelling in his left thigh over several months. Radiographs show extensive osteolytic changes in the proximal femur with concentric narrowing of the femoral neck.
View Answer & Explanation
Correct Answer: C
Rationale: The clinical presentation of progressive pain and swelling with extensive osteolytic changes, particularly with concentric narrowing as shown in the image, is characteristic of Gorham’s disease (massive osteolysis). Osteosarcoma and chondrosarcoma typically present with more aggressive features, often with periosteal reaction or matrix mineralization. Fibrous dysplasia usually has a ground-glass appearance. Paget's disease involves both lytic and blastic phases, often with bone enlargement, which is not described here.
Question 97
A 30-year-old female presents with chronic pain in her humerus. Radiographs reveal progressive resorption of the bone diaphysis. Biopsy reveals a sponge-like consistency grossly.
View Answer & Explanation
Correct Answer: C
Rationale: Gorham’s disease is characterized by massive, progressive osteolytic changes, which can lead to complete resorption of bone diaphysis as seen in advanced cases. Gross pathology often describes a sponge-like consistency. The other options do not typically present with this specific combination of progressive massive osteolysis and gross pathological findings.
Question 98
A 40-year-old male presents with new-onset weakness and numbness in his lower extremities. Imaging reveals extensive osteolytic changes in a vertebral body. Which of the following is a characteristic microscopic finding for the most likely diagnosis?
Question 98
A 35-year-old male presents with progressive pain and swelling in his left shoulder. Radiographs reveal extensive osteolytic changes involving the humerus, with a "vanishing bone" appearance. Biopsy shows vascular proliferation within the bone marrow. Which of the following best describes the primary pathological process in Gorham's disease?
View Answer & Explanation
Correct Answer: C
Rationale: Gorham's disease is characterized by the proliferation of benign vascular channels (angiomatous spaces) within the bone, which leads to progressive bone resorption and osteolysis. The microscopic examination shows varying amounts of vascular changes without reactive bone formation. Main Distractor: Option B is incorrect because while osteoclastic activity is involved in bone resorption, the primary driver in Gorham's disease is the abnormal vascular proliferation, not a systemic hormonal dysregulation like parathyroid hormone.
Question 98
A 42-year-old female presents with new-onset weakness and numbness in her lower extremities. She has a history of chronic back pain. Imaging reveals extensive osteolytic changes in several vertebral bodies of the lumbar spine. Based on the clinical context of Gorham's disease, what is the most likely cause of her neurological symptoms?
View Answer & Explanation
Correct Answer: E
Rationale: The case description explicitly states, "Lesions of the vertebral column may cause neurologic findings." This directly links vertebral involvement in Gorham's disease to neurological symptoms. Main Distractor: Option B, pathological fracture and instability, is a plausible consequence of extensive osteolysis and could lead to neurological symptoms. However, the provided text directly attributes neurologic findings to "lesions of the vertebral column," which encompasses the destructive process itself and its direct impact, rather than solely focusing on fracture as the mechanism.
Question 98
A 28-year-old male is diagnosed with Gorham's disease affecting his pelvis. Initial radiographs show patchy lytic lesions. He is followed over several years. What radiographic change is expected to occur over time in the involved bone?
View Answer & Explanation
Correct Answer: C
Rationale: The disease is described as involving "massive, progressive osteolytic changes" and radiographs show "extensive osteolytic changes of the involved bone." Fig. 8.62 further illustrates "complete resorption of diaphysis," indicating the progressive and extensive nature of the osteolysis. Main Distractor: Option D is incorrect. While the text mentions "Over time, sclerotic bone may accompany healing," this refers to a later, potential healing phase, not the primary progressive change which is osteolysis. The initial and predominant radiographic feature is progressive bone destruction.
Question 98
A bone biopsy is performed on a 19-year-old patient suspected of having Gorham's disease in the distal femur. Upon gross examination of the specimen, what characteristic finding would the pathologist most likely report?
View Answer & Explanation
Correct Answer: C
Rationale: The case text explicitly states under "Pathology": "Gross specimens have a sponge-like consistency." Main Distractor: Option B, a soft, gelatinous texture, might seem plausible for a vascular lesion, but the specific and unique descriptor provided in the text for Gorham's disease is "sponge-like consistency," which is more precise.
Question 98
A 50-year-old male presents with chronic hip pain. Radiographs show significant lytic destruction in the proximal femur with concentric narrowing of the femoral neck. A biopsy is performed. Microscopic examination of the bone tissue would most likely reveal which of the following?

View Answer & Explanation
Correct Answer: C
Rationale: The text states, "Microscopic examination shows varying amounts of vascular changes... Note the cavernous angiomatous spaces." Fig. 8.63 further illustrates this. This is a hallmark microscopic feature of Gorham's disease. Main Distractor: Option A, abundant reactive bone formation, is incorrect because the text specifically states, "Microscopic examination shows varying amounts of vascular changes without reactive bone formation."
Question 98
A 30-year-old patient undergoes a bone biopsy for a progressive lytic lesion in the tibia. The pathologist notes vascular proliferation. To confirm a diagnosis of Gorham's disease and differentiate it from other vascular lesions, which microscopic feature is critical to observe or, more importantly, *not* observe?
View Answer & Explanation
Correct Answer: B
Rationale: The text and Fig. 8.63 specifically state, "Endothelial cells show no cytological atypia." This benign nature of the endothelial cells is crucial in distinguishing Gorham's disease from malignant vascular tumors. Main Distractor: Option A, presence of osteoid seams, is not directly mentioned as a distinguishing feature in the context of Gorham's pathology. The absence of reactive bone formation is mentioned, which is different from osteoid seams.
Question 98
A 17-year-old athlete presents with insidious onset of pain and swelling in his forearm, several months after a minor fall. Radiographs show progressive osteolysis of the radius. Given the potential diagnosis of Gorham's disease, what historical factor is frequently reported by patients?
View Answer & Explanation
Correct Answer: C
Rationale: The case description explicitly states, "Many patients report antecedent trauma." Main Distractor: Option A, family history, is incorrect as Gorham's disease is described as an "idiopathic process," implying no clear genetic predisposition or familial pattern.
Question 98
A 38-year-old female presents with a several-month history of worsening pain and swelling in her left thigh. Radiographs demonstrate complete resorption of the diaphysis of the left femur. What additional radiographic finding might be observed in the local region in Gorham's disease?
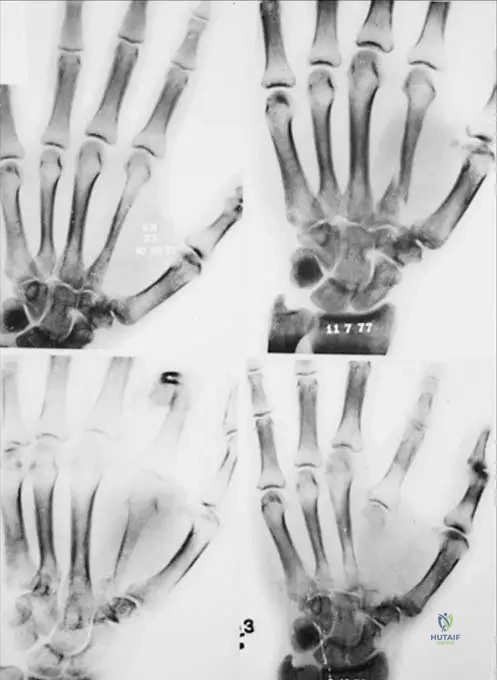
View Answer & Explanation
Correct Answer: B
Rationale: The text states, "Local soft tissues may also be involved." This indicates that the disease process is not always confined strictly to the bone. Main Distractor: Option A, periosteal new bone formation, is generally associated with reactive processes or infection, which is not characteristic of Gorham's disease; the text emphasizes the lack of reactive bone formation.
Question 98
A 25-year-old male is diagnosed with Gorham's disease after presenting with progressive bone loss in his humerus. Based on the provided description, how is Gorham's disease primarily classified?
View Answer & Explanation
Correct Answer: C
Rationale: The first sentence of the case description clearly states, "Gorham’s disease is an idiopathic process involving massive, progressive osteolytic changes." Main Distractor: Option A, a primary bone malignancy, is incorrect because the pathology explicitly states "Endothelial cells show no cytological atypia," indicating a benign process, not malignant.
Question 98
A 15-year-old patient is diagnosed with Gorham's disease affecting the scapula. The parents inquire about the long-term course of the disease. Which statement best describes the typical progression of the osteolytic changes?
View Answer & Explanation
Correct Answer: B
Rationale: The description states, "Gorham’s disease is an idiopathic process involving massive, progressive osteolytic changes." This highlights the key characteristic of the disease's progression. Main Distractor: Option C, stabilization after initial rapid bone loss, is incorrect as the disease is described as "progressive," implying ongoing rather than self-limiting or stabilizing destruction.
Question 98
A 60-year-old patient presents with chronic hip pain. Radiographs show significant lytic destruction in the proximal femur with concentric narrowing of the femoral neck, as depicted in the image. This finding is characteristic of which aspect of Gorham's disease?

View Answer & Explanation
Correct Answer: C
Rationale: The image (Fig. 8.57) shows "Lytic destruction in the proximal femur with concentric narrowing of the femoral neck," which is a direct visual representation of the "massive, progressive osteolytic changes" that define Gorham's disease. Main Distractor: Option B, malignant bone tumor infiltration, is incorrect. While it can cause lytic lesions, Gorham's disease is a benign vascular process, and the pathology explicitly states no cytological atypia, ruling out malignancy.
Question 98
A 45-year-old male presents with a "vanishing bone" phenomenon in his left leg. An AP radiograph of the left femur, as shown, demonstrates complete resorption of the diaphysis. This radiographic appearance is a hallmark of Gorham's disease and signifies what?

View Answer & Explanation
Correct Answer: B
Rationale: The image (Fig. 8.62) shows "complete resorption of diaphysis," which is an extreme manifestation of the "massive, progressive osteolytic changes" characteristic of Gorham's disease. This represents extensive and advanced destruction. Main Distractor: Option D, early stages of bone healing, is incorrect. The image clearly shows severe bone loss, which is the opposite of early healing. While sclerotic bone may accompany healing later, complete resorption is a destructive phase.
Question 98
A bone biopsy from a patient with suspected Gorham's disease reveals the microscopic features shown in the image, characterized by cavernous angiomatous spaces. What is a key characteristic of the endothelial cells lining these spaces in Gorham's disease?

View Answer & Explanation
Correct Answer: C
Rationale: The text accompanying Fig. 8.63 explicitly states, "Endothelial cells show no cytological atypia." This benign nature is a defining feature of Gorham's disease. Main Distractor: Option A, they exhibit significant cytological atypia, is the direct opposite of the described pathology and would suggest a malignant vascular tumor rather than Gorham's disease.
Question 98
A pathologist is reviewing a bone biopsy from a patient with extensive osteolysis. The microscopic findings include vascular changes and cavernous angiomatous spaces. To support a diagnosis of Gorham's disease, the pathologist would specifically note the absence of which feature?
View Answer & Explanation
Correct Answer: B
Rationale: The text states, "Microscopic examination shows varying amounts of vascular changes without reactive bone formation." The absence of reactive bone formation is a key diagnostic characteristic. Main Distractor: Option A, endothelial cell proliferation, is incorrect because vascular changes and angiomatous spaces imply endothelial cell proliferation, which is a *present* feature, not an absent one.
Question 98
A 30-year-old patient presents with symptoms related to Gorham's disease. The specific complaints vary widely depending on the affected anatomical site. Which of the following is NOT listed as a general clinical symptom in the provided text?
View Answer & Explanation
Correct Answer: D
Rationale: The text states, "Clinical symptoms vary depending on the anatomic site, with many patients reporting pain, swelling, and mechanical symptoms. Lesions of the vertebral column may cause neurologic findings." Fever is not mentioned as a clinical symptom. Main Distractor: Option A, pain, is incorrect as it is explicitly listed as a common clinical symptom.
Question 98
A 22-year-old patient with Gorham's disease affecting the femur is being monitored with serial radiographs. While the disease is characterized by progressive osteolysis, what radiographic change is noted to potentially occur over time, suggesting a phase of resolution or healing?
View Answer & Explanation
Correct Answer: C
Rationale: The text states, "Over time, sclerotic bone may accompany healing." This indicates a potential late-stage radiographic finding distinct from the initial progressive osteolysis. Main Distractor: Option B, complete disappearance of the affected bone, is a description of the *progression* of osteolysis (as seen in Fig. 8.62), not a sign of healing or resolution.
Question 98
A 40-year-old male presents with a several-month history of worsening pain in his arm. Radiographs show extensive bone loss in the humerus. The primary characteristic of the osteolysis seen in Gorham's disease is described as:
View Answer & Explanation
Correct Answer: B
Rationale: The introductory sentence defines the disease: "Gorham’s disease is an idiopathic process involving massive, progressive osteolytic changes." Main Distractor: Option A, localized and self-limiting, is incorrect because the disease is described as "massive" and "progressive," indicating widespread and ongoing destruction, not a limited or resolving process.
Question 98
A microscopic examination of a bone biopsy from a patient with Gorham's disease reveals vascular changes within the bone marrow. Which specific cell type is primarily involved in forming these characteristic vascular structures?
View Answer & Explanation
Correct Answer: C
Rationale: The text mentions "vascular changes" and "cavernous angiomatous spaces," and specifically states, "Endothelial cells show no cytological atypia." Endothelial cells are the cells that line blood vessels and form vascular structures. Main Distractor: Option B, osteoblasts, are bone-forming cells, and the pathology of Gorham's disease is characterized by the *absence* of reactive bone formation, making osteoblasts not primarily involved in the characteristic vascular changes.
Question 98
A 29-year-old female undergoes a bone biopsy for a lytic lesion in her humerus. Microscopic examination reveals numerous vascular spaces. The image provided shows these spaces. What is the specific descriptive term used for these vascular spaces in the context of Gorham's disease?

View Answer & Explanation
Correct Answer: C
Rationale: The text accompanying Fig. 8.63 explicitly states, "Note the cavernous angiomatous spaces." This is the precise pathological description of the vascular lesions. Main Distractor: Option A, capillary hemangiomas, is a general term for a type of vascular lesion, but "cavernous angiomatous spaces" is the specific and more accurate descriptor provided in the case for Gorham's disease.
Question 98
A 33-year-old male presents with a several-month history of progressive pain and weakness in his right leg. Radiographs show extensive osteolytic changes in the tibia. Based on the overall description of Gorham's disease, which statement best summarizes its fundamental nature?
View Answer & Explanation
Correct Answer: C
Rationale: This option synthesizes the key elements from the text: "idiopathic process," "vascular changes" (benign vascular proliferation), and "massive, progressive osteolytic changes" (progressive bone resorption). Main Distractor: Option A, a neoplastic process characterized by malignant endothelial cell proliferation, is incorrect. The text clearly states it's an "idiopathic process" and that "Endothelial cells show no cytological atypia," ruling out malignancy.
Question 99
A 35-year-old male presents with progressive pain and swelling in his left shoulder. Radiographs reveal extensive osteolytic changes involving the humerus, with a "vanishing bone" appearance. Biopsy shows vascular proliferation within the bone marrow. Which of the following best describes the primary pathological process in Gorham's disease?
View Answer & Explanation
Correct Answer: C
Rationale: Gorham's disease is characterized by the proliferation of benign vascular channels (angiomatous spaces) within the bone, which leads to progressive bone resorption and osteolysis. The microscopic examination shows varying amounts of vascular changes without reactive bone formation. Main Distractor: Option B is incorrect because while osteoclastic activity is involved in bone resorption, the primary driver in Gorham's disease is the abnormal vascular proliferation, not a systemic hormonal dysregulation like parathyroid hormone.
Question 100
A 42-year-old female presents with new-onset weakness and numbness in her lower extremities. She has a history of chronic back pain. Imaging reveals extensive osteolytic changes in several vertebral bodies of the lumbar spine. Based on the clinical context of Gorham's disease, what is the most likely cause of her neurological symptoms?
View Answer & Explanation
Correct Answer: E
Rationale: The case description explicitly states, "Lesions of the vertebral column may cause neurologic findings." This directly links vertebral involvement in Gorham's disease to neurological symptoms. Main Distractor: Option B, pathological fracture and instability, is a plausible consequence of extensive osteolysis and could lead to neurological symptoms. However, the provided text directly attributes neurologic findings to "lesions of the vertebral column," which encompasses the destructive process itself and its direct impact, rather than solely focusing on fracture as the mechanism.
