Humeral Shaft Fractures: Expert Insights on Diagnosis & Treatment
Key Takeaway
In this comprehensive guide, we discuss everything you need to know about Humeral Shaft Fractures: Expert Insights on Diagnosis & Treatment. Shaft fractures humeral are common injuries, representing 3-5% of all fractures. They typically occur in the humerus shaft, from the pectoralis major insertion to the supracondylar ridge, with 60% involving the middle third. Injury mechanisms include direct trauma or indirect forces, like falls. Patients present with pain, swelling, and deformity, requiring careful neurovascular assessment, especially for radial nerve function.
Introduction and Epidemiology
Humeral shaft fractures represent a significant portion of orthopedic trauma, accounting for approximately 3 percent to 5 percent of all skeletal fractures. The overall incidence is estimated at 14.5 per 100,000 individuals annually. These injuries exhibit a classic bimodal age distribution. A distinct peak in the third decade of life is predominantly observed in males, typically resulting from high-energy trauma such as motor vehicle collisions or sports-related injuries. A secondary peak occurs in the seventh and eighth decades, predominantly in females, typically secondary to low-energy falls reflecting underlying osteoporotic bone changes.
While the vast majority of these fractures are closed injuries, open fractures constitute 2 percent to 10 percent of cases and require emergent surgical evaluation. The anatomic distribution of humeral diaphyseal fractures is heavily weighted toward the middle third of the diaphysis, which accounts for 60 percent of cases. The proximal third accounts for 30 percent, and the distal third comprises the remaining 10 percent.
The mechanism of injury dictates the resulting fracture pattern. Direct trauma to the brachium, which is the most common etiology, typically produces transverse or highly comminuted fracture patterns. Indirect trauma, such as a fall on an outstretched hand, imparts torsional and bending forces that result in spiral or oblique fracture configurations. Furthermore, extreme muscular contraction, such as that seen in competitive arm wrestling or overhead throwing athletes, can generate sufficient rotational torque to produce spiral fractures of the humeral shaft.

Initial clinical evaluation must be meticulous. Patients present with profound localized pain, gross deformity, swelling, and shortening of the affected extremity. A comprehensive neurovascular examination is paramount, with a specific focus on radial nerve motor and sensory function, given its intimate anatomic relationship with the posterior and lateral humerus. In scenarios involving high-energy crush injuries or extreme swelling, serial examinations are indicated to monitor for compartment syndrome, supplemented by invasive compartment pressure measurements if clinical suspicion remains high.
Soft tissue integrity must be scrutinized. Superficial abrasions must be carefully differentiated from true open fractures. If an open fracture with potential intra-articular extension is suspected, an intra-articular saline load test performed via an injection distant from the traumatic wound can definitively rule out joint communication by demonstrating fluid extravasation.
Surgical Anatomy and Biomechanics
A profound understanding of humeral shaft anatomy and its associated musculotendinous attachments is essential for predicting fracture displacement, planning surgical approaches, and executing anatomic reduction. The humeral diaphysis extends from the superior border of the pectoralis major insertion proximally to the supracondylar ridge distally. Morphologically, the cross-sectional anatomy transitions from a robust, cylindrical shape proximally to a narrower, flattened triangular shape distally. This transition has critical implications for intramedullary nail sizing and the contouring of extra-articular plates.

The vascular supply to the humeral diaphysis is primarily derived from perforating branches of the brachial artery. The principal nutrient artery enters the medial aspect of the humerus just distal to the midshaft. Surgical stripping of the periosteum during open reduction and internal fixation must be minimized to preserve this tenuous endosteal and periosteal blood supply, thereby mitigating the risk of iatrogenic nonunion.
Musculotendinous attachments exert predictable deforming forces on fracture fragments based on the anatomic level of the fracture:
* Fractures proximal to the pectoralis major insertion: The proximal fragment is abducted and externally rotated by the rotator cuff musculature, while the distal fragment is displaced medially by the pectoralis major.
* Fractures between the pectoralis major and deltoid insertions: The proximal fragment is adducted by the pectoralis major, latissimus dorsi, and teres major. The distal fragment is abducted by the deltoid and translated proximally by the biceps and triceps.
* Fractures distal to the deltoid insertion: The proximal fragment is abducted by the deltoid, while the distal fragment is shortened and translated proximally by the combined pull of the biceps and triceps.

The radial nerve is the most critical neurovascular structure at risk during both the initial injury and subsequent surgical intervention. The nerve courses along the posterior aspect of the humerus within the spiral groove, passing from medial to lateral. It pierces the lateral intermuscular septum to enter the anterior compartment. Topographically, the radial nerve can be reliably identified 14 to 15 cm proximal to the lateral epicondyle and 20 to 21 cm proximal to the medial epicondyle. Fractures of the distal third of the humerus, particularly spiral oblique patterns (Holstein-Lewis fractures), carry a high risk of radial nerve entrapment within the fracture site.

Indications and Contraindications
The management of humeral shaft fractures requires a nuanced decision-making process balancing the inherent healing capacity of the humerus against the morbidity of surgical intervention. Historically, non-operative management with functional bracing (Sarmiento bracing) has been the gold standard for isolated, closed humeral shaft fractures, yielding union rates exceeding 90 percent.
Acceptable radiographic alignment parameters for non-operative management include:
* Less than 20 degrees of anterior angulation
* Less than 30 degrees of varus or valgus angulation
* Less than 3 centimeters of longitudinal shortening
Surgical intervention is reserved for specific clinical scenarios where conservative management is either contraindicated or has a high probability of failure.
| Management Strategy | Primary Indications | Relative Contraindications |
|---|---|---|
| Non Operative Bracing | Closed, isolated fractures meeting acceptable alignment criteria; High surgical risk patients. | Open fractures; Vascular injury; Polytrauma; Non-compliant patients; Severe soft tissue injury preventing brace fit. |
| Open Reduction Internal Fixation | Failure of closed reduction; Open fractures; Vascular injury requiring repair; Floating elbow; Bilateral humerus fractures; Pathologic fractures; Segmental fractures. | Severe osteopenia compromising screw purchase; Active local infection; Critical soft tissue compromise over proposed incision. |
| Intramedullary Nailing | Pathologic fractures; Segmental fractures; Polytrauma requiring rapid stabilization; Osteopenic bone (relative). | Narrow medullary canal; Pre-existing shoulder or elbow arthropathy; Active medullary infection. |
| External Fixation | Severe contaminated open fractures; Damage control orthopedics in hemodynamically unstable polytrauma; Burn injuries over the brachium. | Definitive fixation in compliant patients (due to pin tract infection risk and joint stiffness). |

The presence of a primary radial nerve palsy is generally not an absolute indication for immediate surgical exploration in closed fractures, as up to 90 percent of these represent neuropraxia that will spontaneously recover. However, a secondary radial nerve palsy that develops after closed reduction attempts strongly suggests iatrogenic nerve entrapment and mandates urgent surgical exploration and stabilization.
Pre Operative Planning and Patient Positioning
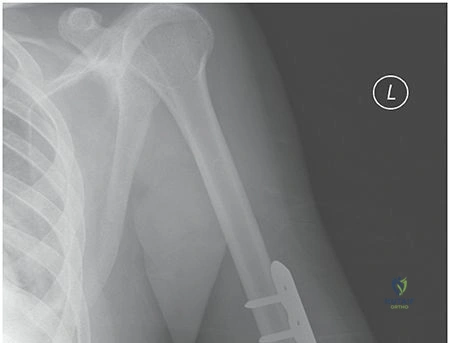
Comprehensive radiographic evaluation is mandatory prior to surgical intervention. Standard orthogonal anteroposterior and lateral radiographs of the entire humerus must be obtained, ensuring clear visualization of both the glenohumeral and ulnohumeral joints. In cases of severe comminution or when intra-articular extension is suspected, a computed tomography scan is highly recommended to delineate fracture morphology and guide implant selection. Traction radiographs can also be beneficial in complex, shortened fractures to better understand the native bone length and fracture configuration.

Implant selection should be tailored to the fracture pattern, anatomic location, and bone quality. Broad 4.5 mm dynamic compression plates or locking compression plates are the workhorse implants for diaphyseal fixation. Pre-operative templating ensures appropriate plate length, aiming for a minimum of six, and ideally eight, cortices of fixation proximal and distal to the fracture zone.
Patient positioning is dictated by the chosen surgical approach and the planned fixation modality:
* Supine or Beach Chair Position: Utilized for the anterolateral approach or antegrade intramedullary nailing. The arm is draped free on a radiolucent hand board. This position allows excellent access to the proximal and middle thirds of the humerus.
* Lateral Decubitus Position: The patient is placed in the lateral position with the operative arm draped over a sterile bolster or supported by an articulated arm holder. This provides unparalleled access for the posterior approach, ideal for distal third fractures.
* Prone Position: An alternative for the posterior approach, offering excellent visualization of the posterior humerus and radial nerve, though airway management and ventilation require careful anesthesia coordination.
Fluoroscopy must be positioned to allow unhindered orthogonal views of the entire humerus without compromising the sterile field. The C-arm is typically brought in from the contralateral side or parallel to the operative bed, depending on the specific room setup and patient positioning.
Detailed Surgical Approach and Technique
The surgical management of humeral shaft fractures demands meticulous soft tissue handling, precise identification of neurovascular structures, and adherence to biomechanical principles of fracture fixation.
Anterolateral Approach
The anterolateral approach is highly versatile, providing excellent exposure of the proximal and middle thirds of the humeral diaphysis. The incision is centered over the lateral border of the biceps muscle belly. Proximally, the internervous plane lies between the deltoid (axillary nerve) and the pectoralis major (medial and lateral pectoral nerves). Distally, the approach utilizes an intermuscular plane rather than a true internervous plane, splitting the brachialis muscle longitudinally.
Because the medial half of the brachialis is innervated by the musculocutaneous nerve and the lateral half by the radial nerve, splitting the muscle belly longitudinally allows access to the anterior humerus while protecting the radial nerve laterally. The periosteum is elevated only as much as necessary to achieve reduction and plate application. Retractors must be placed with caution, particularly on the lateral aspect of the humerus, to avoid iatrogenic compression of the radial nerve.

Posterior Approach
The posterior approach is the gold standard for distal third humeral shaft fractures and scenarios requiring radial nerve exploration, such as a Holstein-Lewis fracture. The incision is made in the posterior midline of the arm. The deep dissection can be performed via a triceps-splitting or a triceps-sparing (paratricipital) technique.
In the triceps-splitting approach, the long and lateral heads of the triceps are identified, and the interval between them is developed. The medial head of the triceps is then split longitudinally in the midline to expose the posterior humerus. The radial nerve and profunda brachii artery must be identified early in the dissection as they cross the posterior humerus from medial to lateral in the spiral groove. The nerve is carefully mobilized and protected with vessel loops.
The triceps-sparing approach involves mobilizing the entire triceps muscle belly medially or laterally, preserving the extensor mechanism's integrity, which may result in improved postoperative triceps strength and reduced elbow stiffness.
Plate Osteosynthesis Technique
For simple transverse or short oblique fractures, absolute stability is desired to promote primary bone healing. This is achieved through anatomic reduction and rigid fixation using a 4.5 mm narrow or broad plate. If the fracture pattern allows, an interfragmentary lag screw should be placed to generate compression across the fracture site, followed by a neutralization plate.
For highly comminuted or segmental fractures, relative stability is preferred to promote secondary bone healing via callus formation. A bridge plating technique is employed, bypassing the zone of comminution. The plate is fixed proximally and distally, preserving the soft tissue envelope and vascular supply to the comminuted fragments. Locking screws may be utilized in osteoporotic bone or very short end segments to enhance construct stability.

Intramedullary Nailing Technique
Intramedullary nailing offers a biomechanically favorable load-sharing construct and can be performed via antegrade or retrograde techniques.
Antegrade nailing requires an entry point at the greater tuberosity or the articular surface of the humeral head, depending on the specific nail design. The rotator cuff must be incised, which carries a known risk of postoperative shoulder pain and dysfunction. The canal is reamed sequentially, and the nail is inserted and locked proximally and distally. Care must be taken during distal interlocking to avoid injury to the musculocutaneous or radial nerves.
Retrograde nailing avoids the rotator cuff but requires an entry point in the distal humerus, typically just proximal to the olecranon fossa. This approach carries a risk of iatrogenic supracondylar fracture and may lead to elbow stiffness. It is often preferred in polytrauma patients where the supine position is required for concurrent procedures, or in distal third fractures where antegrade nailing provides insufficient distal fixation.

Complications and Management
Despite meticulous surgical technique, the management of humeral shaft fractures is associated with several well-documented complications. Early recognition and appropriate salvage strategies are critical for optimizing patient outcomes.
| Complication | Incidence | Etiology and Risk Factors | Management and Salvage Strategies |
|---|---|---|---|
| Radial Nerve Palsy | 11% to 18% | Trauma at injury (Holstein-Lewis); Iatrogenic stretch during retraction; Entrapment during reduction. | Primary palsy: Observation, baseline EMG at 6 weeks. Secondary palsy: Urgent surgical exploration. Late failure to recover: Tendon transfers (e.g., Pronator teres to ECRB). |
| Nonunion | 2% to 10% | Soft tissue interposition; Inadequate fixation stability; Excessive periosteal stripping; Infection; Smoking. | Hypertrophic: Improve mechanical stability (exchange nailing or rigid plating). Atrophic: Debridement, rigid plating, and autologous bone grafting (iliac crest). |
| Infection | 1% to 3% | Open fractures; Prolonged surgical time; Poor soft tissue envelope; Medical comorbidities (Diabetes). | Superficial: Oral or IV antibiotics. Deep: Urgent surgical irrigation and debridement, retention of stable hardware, removal of loose hardware with external fixation, tailored IV antibiotics. |
| Joint Stiffness | 10% to 15% | Prolonged immobilization; Intra-articular hardware penetration; Rotator cuff violation (antegrade nails). | Aggressive early physical therapy; Capsular release for refractory adhesive capsulitis; Hardware removal if impinging on joint mechanics. |
| Malunion | 5% to 10% | Inadequate reduction; Failure of conservative bracing; Premature weight-bearing. | Often well-tolerated due to compensatory shoulder motion. Corrective osteotomy reserved for severe symptomatic deformity (>30 degrees angulation). |
Radial nerve palsy remains the most scrutinized complication. The majority of primary palsies are neuropraxias that resolve spontaneously within 3 to 4 months. If clinical recovery is not evident by 6 to 12 weeks, electromyography and nerve conduction studies are indicated to assess for subclinical reinnervation. If no recovery is noted by 6 months, surgical exploration and potential nerve grafting or tendon transfers are warranted.
Nonunion of the humeral shaft presents a significant clinical challenge. Atrophic nonunions, characterized by a lack of callus formation and tapered bone ends, indicate a biological failure. Treatment requires meticulous debridement of fibrous tissue, opening of the medullary canal, rigid internal fixation with dual plating or a robust 4.5 mm plate, and the application of autologous bone graft to stimulate osteogenesis. Hypertrophic nonunions indicate a mechanical failure and typically resolve with improved rigid stabilization alone.
Post Operative Rehabilitation Protocols
Postoperative rehabilitation must be carefully tailored to the stability of the surgical construct, bone quality, and concomitant injuries. The primary goal of early rehabilitation is the prevention of shoulder and elbow stiffness, which are common sequelae of humeral shaft fractures regardless of the management modality.
In the immediate postoperative phase (Days 1 to 14), the operative extremity is typically supported in a sling for comfort. Active and active-assisted range of motion exercises for the wrist and hand are initiated immediately to prevent dependent edema and distal stiffness. Pendulum exercises for the glenohumeral joint and gentle active-assisted range of motion for the elbow are commenced within the first postoperative week, provided rigid internal fixation was achieved.
During the intermediate phase (Weeks 2 to 6), formal physical therapy focuses on restoring full passive and active range of motion of the shoulder and elbow. Weight-bearing through the operative extremity is strictly prohibited. Isometrics for the deltoid, biceps, and triceps can be introduced as pain allows.
In the late rehabilitation phase (Weeks 6 to 12), radiographic evaluation is performed to assess for progressive callus formation and fracture consolidation. Once clinical and radiographic signs of healing are evident, progressive resistance exercises and strengthening protocols are initiated. Patients may gradually transition to weight-bearing activities. Return to heavy manual labor or high-impact sports is typically restricted until complete radiographic union is achieved, which often requires 3 to 6 months.
Summary of Key Literature and Guidelines
The academic discourse surrounding humeral shaft fractures is rich with high-quality evidence guiding clinical decision-making. The foundational work by Sarmiento et al. established functional bracing as a highly effective, safe, and cost-efficient modality for closed humeral shaft fractures, demonstrating union rates exceeding 95 percent with excellent functional outcomes. This remains a cornerstone of orthopedic teaching, emphasizing that not all displaced fractures require surgical intervention.
In the realm of operative management, the debate between plate osteosynthesis and intramedullary nailing has been extensively studied. A landmark meta-analysis by Bhandari et al. compared dynamic compression plating with intramedullary nailing. The study concluded that while both modalities achieve high union rates, intramedullary nailing is associated with a higher risk of shoulder impingement and a slightly elevated risk of reoperation. Conversely, plate osteosynthesis carries a higher risk of iatrogenic radial nerve palsy, particularly when utilizing the posterior approach.
Regarding radial nerve management, Shao et al. conducted a comprehensive systematic review detailing the natural history of radial nerve palsy associated with humeral shaft fractures. Their findings reinforced the paradigm of expectant management for primary closed injuries, demonstrating an overall spontaneous recovery rate of over 70 percent, thereby discouraging routine immediate surgical exploration unless specific indications (such as an open fracture or secondary palsy) are present.
Current clinical practice guidelines from major orthopedic societies, including the Orthopaedic Trauma Association (OTA) and the American Academy of Orthopaedic Surgeons (AAOS), synthesize this literature, recommending individualized treatment plans based on fracture morphology, patient physiology, and surgeon expertise. The consensus strongly supports shared decision-making, weighing the predictable surgical risks against the prolonged recovery and potential malunion associated with conservative management.
