Elbow Contracture Release: Medial Over-the-Top Approach Masterclass
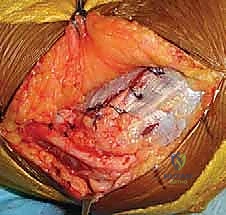
Key Takeaway
This masterclass details the medial over-the-top approach for elbow contracture release. Fellows will learn intricate surgical anatomy, meticulous patient positioning, and a step-by-step intraoperative execution, including ulnar nerve management and capsule excision. We cover critical pearls, potential pitfalls, and comprehensive postoperative care, ensuring a thorough understanding of this challenging procedure for restoring elbow motion.
Introduction and Epidemiology
Elbow contracture represents a profoundly debilitating condition that significantly impairs upper extremity function, limiting a patient's ability to position the hand in space for activities of daily living. The normal functional arc of elbow motion is generally accepted to be between 30 and 130 degrees of flexion, with 50 degrees of pronation and 50 degrees of supination. Loss of this functional arc, whether through trauma, degenerative joint disease, inflammatory arthropathy, or central nervous system injury, often necessitates surgical intervention when nonoperative measures are exhausted.
Multiple techniques have been described for the release of elbow contractures, encompassing open lateral, medial, posterior, and arthroscopic approaches. The medial approach provides the distinct advantage of direct access to both the anterior and posterior aspects of the ulnohumeral joint while simultaneously allowing for direct visualization, decompression, and management of the ulnar nerve. Concomitant ulnar neuropathy is frequently observed in the setting of severe elbow contracture, making the medial approach particularly advantageous.
Medial-based releases have evolved significantly over the past several decades. The approach was initially proposed by Wilner, whose technique involved medial epicondylectomy and wide dissection to achieve soft tissue release. Recognizing the morbidity associated with epicondylectomy, Weiss and Sachar subsequently described splitting the flexor-pronator mass rather than performing a complete release or epicondylectomy, thereby preserving the dynamic stabilizers of the medial elbow. Mansat et al popularized this approach specifically to deal with extrinsic contractures of the elbow coupled with ulnar nerve involvement. Furthermore, Itoh et al and Wada et al underscored the biomechanical importance of the posterior oblique band of the medial collateral ligament, identifying it as a critical structure that must be addressed and released if a severe extension contracture exists.

Surgical Anatomy and Biomechanics
A profound understanding of medial elbow anatomy is mandatory to safely navigate the medial approach, perform an adequate capsular release, and avoid catastrophic iatrogenic instability or neurologic injury. The medial compartment of the elbow encompasses the medial side of the ulnohumeral joint, the medial collateral ligament complex, the flexor-pronator mass, the ulnar nerve, and the medial antebrachial cutaneous nerve.
Medial Ulnohumeral Articulation
The medial ulnohumeral joint is composed of the medial column of the distal humerus, the medial epicondyle, the medial aspect of the proximal ulna, and the coronoid process. The highly congruent nature of the ulnohumeral articulation provides primary skeletal stability to the elbow. Osteophyte formation in the coronoid fossa anteriorly or the olecranon fossa posteriorly frequently contributes to intrinsic mechanical blocks to motion.

Medial Collateral Ligament Complex
The medial collateral ligament serves as the primary restraint to valgus stress at the elbow and consists of three distinct parts anterior, posterior, and transverse segments.
The anterior bundle is the most discrete and biomechanically critical component. It originates from the anteroinferior surface of the medial epicondyle—importantly, not from the condylar elements of the trochlea just inferior to the axis of rotation—and inserts onto the sublime tubercle of the anteromedial coronoid. The anterior bundle must be meticulously preserved during contracture release to prevent iatrogenic valgus instability.
The posterior portion, often referred to as the posterior oblique band, is essentially a thickening of the posterior capsule. It is well defined only when the elbow is in approximately 90 degrees of flexion. Because this band becomes taut in flexion, contracture of the posterior oblique band is a primary anatomic driver of extension loss.
The transverse component, sometimes known as Cooper's ligament, spans from the coronoid to the tip of the olecranon. It originates and inserts on the same bone (the ulna) and therefore appears to contribute little or nothing to elbow stability.

Flexor Pronator Mass
The flexor-pronator mass provides dynamic valgus stability to the elbow and serves as the superficial muscular layer encountered during the medial approach. It includes the pronator teres, which is the most proximal of the flexor-pronator group. Just inferior to the origin of the pronator teres at the anteroinferior aspect of the medial epicondyle originates the flexor carpi radialis.
The palmaris longus muscle arises from the medial epicondyle and from the intermuscular septa it shares with the flexor carpi radialis and flexor carpi ulnaris. The flexor carpi ulnaris is the most posterior of the common flexor tendons, originating from both the medial epicondyle and from the medial border of the coronoid and proximal medial aspect of the ulna. Deep to these structures lies the flexor digitorum superficialis, which is the deepest muscle originating from the common flexor tendon but remains superficial to the flexor digitorum profundus.

Neurologic Structures
The ulnar nerve rests on the posterior aspect of the medial epicondyle within the cubital tunnel. While it is in close proximity to the medial collateral ligament, it is not intimately related to the fibers of the anterior bundle itself. The nerve is susceptible to compression at multiple sites, including the arcade of Struthers, the medial intermuscular septum, Osborne's ligament, and the deep flexor-pronator aponeurosis.
The medial antebrachial cutaneous nerve courses anterior to the medial epicondyle and provides sensation to the medial forearm. Its branches are highly variable and are frequently encountered during the superficial dissection of the medial approach. Injury to these branches can result in painful neuroma formation.

Indications and Contraindications
Surgical release of an elbow contracture via a medial approach is primarily indicated when nonoperative modalities have failed and the patient exhibits a functional deficit. The medial approach is specifically favored when there is concomitant ulnar nerve symptomatology or when the primary pathology is localized to the medial compartment, such as medial heterotopic ossification.
| Parameter | Operative Indications | Non Operative Indications | Contraindications to Release |
|---|---|---|---|
| Clinical Presentation | Functional arc loss (<30 to 130 degrees) failing conservative therapy | Mild stiffness, early post-traumatic phase (<6 months), functional ROM maintained | Active joint infection, severe medical comorbidities |
| Neurologic Status | Concomitant ulnar neuropathy requiring decompression/transposition | Intact neurologic function (though not a contraindication to non-op) | - |
| Bony Pathology | Medial heterotopic ossification, prominent medial osteophytes | Minimal bony block, primarily soft tissue contracture responsive to splinting | Severe articular destruction (indicates need for arthroplasty), joint instability |
| Patient Factors | Highly motivated, compliant with rigorous postoperative rehabilitation | Poor compliance, inability to tolerate dynamic splinting | Non-compliant patient, severe cognitive impairment |

Pre Operative Planning and Patient Positioning
Thorough preoperative planning is essential for anticipating the anatomic distortions commonly seen in the stiff elbow. The surgeon must differentiate between extrinsic causes of stiffness (capsular contracture, ligamentous shortening, heterotopic ossification) and intrinsic causes (articular step-off, osteophytes, loose bodies, cartilage loss).
Imaging and Diagnostic Studies
Diagnosis of the contracture is usually made by identifying a characteristic history, such as prior trauma or prolonged immobilization, and performing a meticulous physical examination documenting the exact arc of motion and neurologic status.
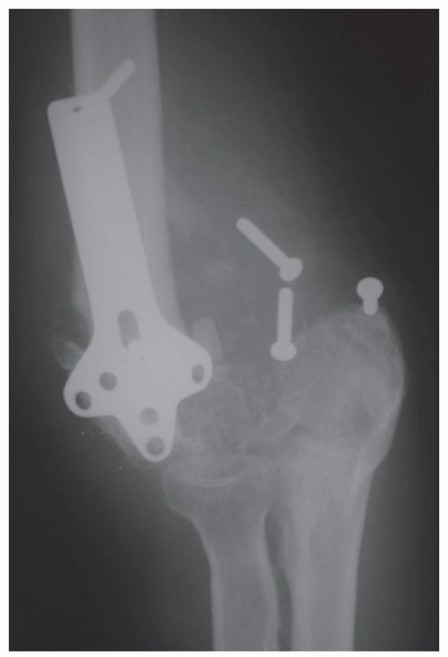
Joint involvement is confirmed by plain radiographs. The anteroposterior view provides good visualization of the joint line and medial/lateral gutters. The lateral view is critical as it can demonstrate osteophytes on the coronoid and at the tip of the olecranon, which act as mechanical blocks to flexion and extension, respectively, even when the central joint space is preserved.
The details of the extent of any bony involvement, including complex heterotopic ossification or intra-articular loose bodies, are best observed on computed tomography. Three-dimensional CT reconstructions are highly recommended for preoperative spatial mapping of heterotopic bone. Transverse imaging by magnetic resonance imaging has little use in our practice for the evaluation of elbow contracture, as it provides inferior bony detail compared to CT and rarely alters the surgical plan for capsular release.
Preoperative electromyography and nerve conduction studies should be obtained if the patient exhibits any clinical signs of ulnar neuropathy, establishing a baseline prior to surgical intervention.

Nonoperative Management
Several options have been proposed for the treatment of elbow contracture prior to considering surgical release. Nonoperative treatment with mobilization of the elbow through the use of alternating flexion and extension splints or dynamic splints can provide a good result if it is initiated soon after the contracture develops.
Manipulation with the patient under anesthesia has also been recommended historically; however, this carries significant risks. Severe loss of motion, iatrogenic fractures, and catastrophic ulnar nerve injury have been reported following aggressive manipulation. Recently, botulinum toxin has been used to release muscle contracture in order to facilitate elbow rehabilitation and regain motion, particularly in patients with central nervous system injury or severe spasticity.

Patient Positioning and Anesthesia
The procedure is typically performed under general anesthesia, often supplemented with a regional block (e.g., supraclavicular or axillary nerve block) for postoperative pain control. It is critical that the regional block does not obscure the postoperative evaluation of the ulnar nerve if a transposition is performed.
The patient is positioned supine on the operating table. The operative arm is draped free and positioned across the chest. Alternatively, the patient can be placed in the lateral decubitus position with the arm resting over a sterile bolster. A sterile tourniquet is applied to the proximal arm to ensure a bloodless surgical field, which is vital for identifying neurovascular structures and assessing the adequacy of the capsular release.

Detailed Surgical Approach and Technique
The medial approach to the stiff elbow requires systematic dissection, meticulous hemostasis, and sequential release of the contracted tissues while protecting the stabilizing ligaments.
Incision and Superficial Dissection
A standard medial utility incision is utilized, centered over the medial epicondyle. The incision extends approximately 5 to 7 centimeters proximally along the medial intermuscular septum and 5 to 7 centimeters distally along the course of the flexor carpi ulnaris.
During the superficial dissection, subcutaneous flaps are elevated. The surgeon must remain vigilant for branches of the medial antebrachial cutaneous nerve. These branches typically cross the operative field transversely or obliquely just distal to the medial epicondyle. They must be identified, mobilized, and protected with vessel loops to prevent painful postoperative neuromas.

Ulnar Nerve Management
The first deep structure to be formally addressed is the ulnar nerve. Given the high association of ulnar nerve symptoms with elbow contracture and the risk of traction injury during subsequent capsular release and postoperative rehabilitation, the nerve must be completely decompressed.
The nerve is identified proximally along the medial border of the triceps and traced distally into the cubital tunnel. The arcade of Struthers and the medial intermuscular septum are excised to prevent kinking of the nerve if it is to be transposed. Distally, the fascia of the flexor carpi ulnaris (Osborne's ligament) is released, and the two heads of the flexor carpi ulnaris are split to fully decompress the nerve as it enters the forearm.
Depending on the degree of preoperative neuropathy, the anticipated gain in flexion, and the stability of the nerve within the cubital tunnel after decompression, the surgeon must decide between an in situ decompression and an anterior transposition (subcutaneous, intramuscular, or submuscular). In the setting of a severe contracture release, an anterior subcutaneous transposition is frequently performed to remove the nerve from the zone of posterior scar tissue and prevent tension during terminal flexion.

Deep Dissection and Capsular Release
Once the ulnar nerve is protected, attention is turned to the flexor-pronator mass. The technique described by Weiss and Sachar is generally preferred to minimize morbidity. A longitudinal split is made in the flexor-pronator mass, typically between the pronator teres and the flexor carpi radialis, or directly through the common tendon, exposing the anterior joint capsule.
The brachialis muscle is carefully elevated off the anterior capsule using a periosteal elevator. Retractors are placed anteriorly to protect the median nerve and brachial artery, which lie immediately anterior to the brachialis.
An anterior capsulectomy is then performed. The thickened, contracted anterior capsule is excised from medial to lateral. It is crucial to identify and preserve the anterior bundle of the medial collateral ligament during this step. The anterior bundle lies immediately deep to the flexor-pronator mass origin on the anteroinferior medial epicondyle.

Following the anterior release, attention is directed posteriorly. The triceps is elevated from the posterior humerus, and a posterior capsulotomy is performed. As emphasized by Itoh et al and Wada et al, the posterior oblique band of the medial collateral ligament is a critical structure to identify and release if an extension contracture exists. This band is incised to allow the ulnohumeral joint to hinge open into extension.

Bony Decompression
Soft tissue release alone is frequently insufficient if bony impingement exists. The coronoid process is inspected through the anterior arthrotomy. Any hyperplastic bone or osteophytes on the tip of the coronoid that impinge within the coronoid fossa during flexion are excised using a rongeur or an osteotome.
Similarly, the olecranon fossa is inspected through the posterior arthrotomy. Fibrous tissue, heterotopic ossification, and loose bodies are aggressively cleared from the olecranon fossa. Osteophytes on the tip of the olecranon are resected to restore terminal extension.

Following completion of the soft tissue and bony releases, the elbow is taken through a full range of motion. The surgeon must verify that the mechanical blocks have been eliminated and that the anterior bundle of the medial collateral ligament remains competent. If the ulnar nerve was transposed, its tracking is observed throughout the arc of motion to ensure no kinking or subluxation occurs.
The wound is thoroughly irrigated. Hemostasis is achieved following tourniquet deflation, which is critical to prevent postoperative hematoma formation—a known catalyst for recurrent stiffness and heterotopic ossification. A closed suction drain is frequently placed prior to layered closure.

Complications and Management
Surgical release of the stiff elbow is a technically demanding procedure associated with a distinct complication profile. Meticulous surgical technique and strict adherence to anatomic planes are required to minimize these risks.
| Complication | Incidence / Risk Factors | Management and Salvage Strategy |
|---|---|---|
| Ulnar Neuritis / Injury | Most common complication. Risk increased with severe preoperative contracture and excessive traction. | Prevent via routine decompression/transposition. Treat post-op neuritis with gabapentinoids, NSAIDs. Revision neurolysis if symptoms persist. |
| Medial Instability | Iatrogenic transection of the anterior bundle of the MCL during anterior capsulectomy. | Intraoperative recognition requires primary repair. Postoperative instability may necessitate formal MCL reconstruction using autograft. |
| Hematoma Formation | Inadequate hemostasis post-tourniquet deflation. | Meticulous intraoperative hemostasis, use of closed suction drains. Evacuation required if hematoma compromises the wound or neurologic status. |
| Recurrent Stiffness | Poor compliance with rehab, inadequate initial release, prolonged immobilization. | Aggressive static progressive splinting. Revision release if refractory, though outcomes diminish with subsequent surgeries. |
| Heterotopic Ossification | High-energy trauma, traumatic brain injury, burns. | Prophylaxis with Indomethacin or single-dose localized radiation therapy. Delayed surgical excision once bone is metabolically mature. |

Post Operative Rehabilitation Protocols
The success of an elbow contracture release is intrinsically tied to the postoperative rehabilitation protocol. The surgical intervention merely resets the baseline; the rehabilitation maintains it.
Immediate postoperative mobilization is paramount. Patients are typically placed in a bulky compressive dressing with an anterior plaster splint holding the elbow in extension to maximize the stretch on the anterior soft tissues, which are prone to rapid recurrent contracture.
Active and active-assisted range of motion exercises are initiated within the first 24 to 48 hours postoperatively. Continuous passive motion machines may be utilized in the inpatient setting, though their long-term superiority over dedicated active therapy remains debated in the literature.
Pain management is a critical component of the rehabilitation phase. The use of indwelling regional nerve catheters (e.g., supraclavicular or infraclavicular) allows for aggressive therapy by minimizing patient guarding and pain-induced muscle spasm.
Upon discharge, patients are transitioned to a static progressive splinting program. Dynamic splinting may also be employed, but static progressive splinting is generally favored for its ability to provide a sustained, low-load stretch leading to plastic deformation of the healing collagen matrix without inciting an inflammatory response. Splints are typically worn at night and during periods of rest, alternating between flexion and extension depending on the patient's specific deficits.
Prophylaxis against heterotopic ossification is routinely administered, particularly in high-risk patients. This generally consists of a continuous course of oral Indomethacin for 3 to 6 weeks postoperatively, or alternatively, a single fraction of localized external beam radiation therapy administered within the first 72 hours following surgery.
Summary of Key Literature and Guidelines
The evolution of the medial approach for elbow contracture is well documented in the orthopedic literature.
Wilner's early descriptions of medial epicondylectomy highlighted the utility of the medial approach but were fraught with complications related to flexor-pronator weakness and medial instability.
Weiss and Sachar revolutionized the approach by demonstrating that the flexor-pronator mass could be split longitudinally, providing excellent access to the anterior capsule without compromising the dynamic medial stabilizers.
Mansat et al further defined the indications for the medial approach, emphasizing its superiority in managing extrinsic contractures complicated by ulnar neuropathy. Their work solidified the routine management of the ulnar nerve during contracture release.
Finally, the biomechanical and clinical studies by Itoh et al and Wada et al brought critical attention to the posterior oblique band of the medial collateral ligament. Their findings established that failure to release this specific anatomic structure is a primary cause of persistent extension deficits following operative intervention.
Collectively, these foundational studies dictate current best practices: meticulous protection of the anterior bundle of the medial
Clinical & Radiographic Imaging
















You Might Also Like