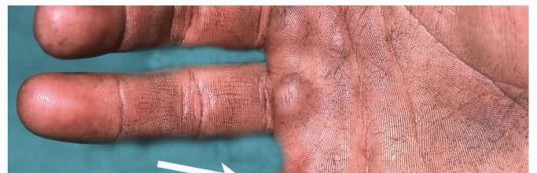
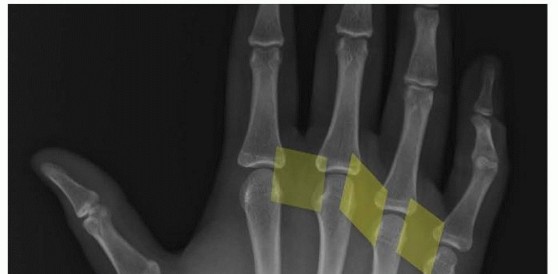
Soft Tissue Mallet Finger: Comprehensive Review of Anatomy, Classification, & Management
Key Takeaway
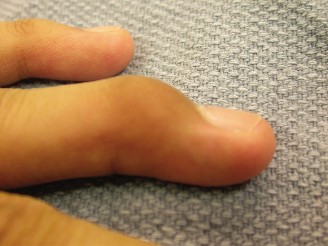
Soft tissue mallet finger, a Doyle Type I injury, involves terminal extensor tendon disruption at the DIP joint, causing a flexion deformity. It's a common hand injury, typically managed non-operatively with continuous DIP joint splinting in extension for 6-8 weeks to allow tendon healing and prevent secondary deformities like swan neck.
Introduction & Epidemiology
Soft tissue mallet finger, a common closed extensor mechanism injury of the distal interphalangeal (DIP) joint, results from disruption of the terminal extensor tendon without significant bony avulsion. This injury leads to an inability to actively extend the DIP joint, resulting in a characteristic flexion deformity. While seemingly innocuous, if left untreated or improperly managed, it can lead to persistent extensor lag, functional impairment, and secondary deformities such as a swan neck deformity.
Epidemiologically, mallet finger is one of the most frequently encountered tendon injuries of the hand. It typically occurs due to sudden, forceful flexion of an actively extended DIP joint, often when an object strikes the fingertip (e.g., "jamming" a finger during sports, tucking in a bed sheet). The injury can affect individuals of all ages, though a bimodal distribution is often observed, with peaks in athletic young adults and middle-aged to elderly individuals who may have less resilient collagen or osteopenia. The long finger and ring finger are most commonly affected, reflecting their frequent involvement in daily activities and sports.
Classification systems for mallet finger injuries often include both bony and soft tissue components. The
Doyle classification
is widely utilized:
*
Type I
: Soft tissue avulsion of the terminal extensor tendon from its insertion on the distal phalanx. This is the primary focus of this review.
*
Type II
: Bony avulsion fracture of the dorsal aspect of the distal phalanx, involving less than 30% of the articular surface.
*
Type III
: Bony avulsion fracture involving more than 30% of the articular surface, often associated with DIP joint subluxation.
*
Type IV
: Epiphyseal fracture in children (Salter-Harris type I or II).
For Type I injuries, the decision-making process between non-operative and operative management revolves around the acuity of the injury, the degree of extensor lag, associated deformities, and patient factors, emphasizing the importance of a thorough understanding of the underlying anatomy and biomechanics.
Surgical Anatomy & Biomechanics
A comprehensive understanding of the anatomy and intricate biomechanics of the extensor mechanism at the DIP joint is paramount for effective management of soft tissue mallet finger. The extensor mechanism is a complex aponeurosis formed by the confluence of intrinsic and extrinsic muscles, allowing for coordinated finger movement.
The extensor digitorum communis (EDC) tendon, an extrinsic muscle, splits into three slips at the proximal phalanx: a central slip that inserts on the middle phalanx (extending the PIP joint) and two lateral bands. These lateral bands course distally, join the tendons of the intrinsic muscles (lumbricals and interossei), and reunite to form the terminal extensor tendon (also known as the conjoint tendon or distal aponeurosis). The terminal extensor tendon inserts broadly onto the dorsal base of the distal phalanx, extending to the germinal matrix of the nail.
Crucial supporting structures include:
*
Triangular Ligament
: Located dorsally, it stabilizes the lateral bands, preventing their volar subluxation and maintaining their position for efficient DIP joint extension.
*
Retinacular Ligaments
: Oblique and transverse retinacular ligaments influence joint movement and contribute to the overall balance. The transverse retinacular ligament prevents dorsal migration of the lateral bands.
The biomechanics of DIP joint extension rely solely on the integrity and effective pull of the terminal extensor tendon. The central slip extends the PIP joint, and the lumbricals and interossei contribute to MCP joint flexion and PIP/DIP extension. In a soft tissue mallet injury (Type I), the terminal extensor tendon is ruptured from its insertion, disrupting the extensor moment arm at the DIP joint. This disruption leaves the DIP joint extension unopposed, and the powerful pull of the flexor digitorum profundus (FDP) tendon, which inserts on the volar aspect of the distal phalanx, creates the characteristic flexion deformity.
If left untreated, chronic extensor lag can lead to secondary deformities:
*
Swan Neck Deformity
: The flexion deformity at the DIP joint can lead to hyperextension of the PIP joint due to altered biomechanics, particularly if the central slip remains intact and the lateral bands shift dorsally over the PIP joint axis. This is often exacerbated by intrinsic muscle tightness.
*
Pseudoboutonnière Deformity
: While less common in pure soft tissue mallet, chronic imbalance can sometimes lead to a milder form of a PIP extension deficit.
Innervation of the digital extensor mechanism is primarily from the posterior interosseous nerve (a branch of the radial nerve) for the extrinsic extensors, and the ulnar and median nerves for the intrinsic muscles. Vascular supply to the tendons is segmental, primarily from dorsal arterial networks, which must be respected during surgical dissection.
Indications & Contraindications
The management of soft tissue mallet finger primarily involves non-operative splinting. Surgical intervention is reserved for specific circumstances where conservative treatment has failed or is unlikely to succeed, or in complex presentations.
Non-Operative Indications
The vast majority of acute soft tissue mallet injuries (Doyle Type I) are successfully managed non-operatively. The core principle is continuous immobilization of the DIP joint in full extension or slight hyperextension (0-10 degrees) for a prolonged period, typically 6 to 8 weeks, followed by a gradual weaning phase. The PIP joint should be left free to allow full range of motion.
- Acute Soft Tissue Mallet Injuries : Any closed Type I injury presenting within a few weeks of onset.
- Patient Compliance : Patients who are motivated and understand the critical importance of continuous splint wear.
- Minimal Extensor Lag : Ideally, full passive extension is achievable, with an extensor lag often less than 40-50 degrees.
- Absence of Secondary Deformity : No fixed swan neck deformity at presentation.
Operative Indications
Surgical management for soft tissue mallet finger aims to restore the extensor mechanism’s integrity and stability. It is generally considered for:
- Failed Non-Operative Management : Persistent extensor lag of more than 15-20 degrees after an adequate course of continuous splinting (typically 8 weeks, followed by night splinting).
- Chronic Soft Tissue Mallet : Injuries presenting late (e.g., >3 months) with significant extensor lag and often associated scarring or tendon retraction.
- Fixed Swan Neck Deformity : Cases where the mallet finger has led to a fixed hyperextension deformity of the PIP joint, requiring a combined approach to address both deformities.
- Irreducible DIP Joint Subluxation : Although more common with bony mallet fractures, severe soft tissue injuries can sometimes result in chronic subluxation that is not amenable to closed reduction and splinting.
- Open Mallet Injuries : Lacerations over the DIP joint with extensor tendon disruption, which require surgical debridement and primary repair to prevent infection and facilitate healing.
- Significant Initial Extensor Lag : While often treated non-operatively, a very severe initial extensor lag (e.g., >50 degrees), suggesting extensive retraction, might be an early consideration for surgical repair, particularly in high-demand patients, though this remains debated.
Contraindications
Absolute contraindications to surgery are rare but include:
- Active Infection : Uncontrolled infection in the operative field.
- Poor Skin Quality/Viability : Conditions precluding wound closure or adequate healing.
- Severe Comorbidities : Medical conditions that significantly increase surgical risk, outweighing potential benefits.
- Unrealistic Patient Expectations : Patients expecting full, pre-injury function in chronic or complex cases.
Relative contraindications include:
* Patient unwillingness to comply with post-operative rehabilitation.
* Mild, asymptomatic extensor lag that does not significantly impact function.
The decision to proceed with surgery should always involve a careful risk-benefit analysis and thorough discussion with the patient regarding potential outcomes and the demands of post-operative rehabilitation.
| Indication Category | Non-Operative Management (Splinting) | Operative Management (Surgical Repair) |
|---|---|---|
| Acuity | Acute (within 4-6 weeks of injury) | Chronic (>3 months), or failed acute non-operative management |
| Injury Type | Closed, isolated Type I (soft tissue) mallet | Open Type I mallet, persistent extensor lag after non-op treatment |
| Extensor Lag | Any degree, provided passively correctable to full extension | Persistent lag >15-20 degrees after adequate splinting, severe initial lag |
| Associated Deformity | None, or flexible swan neck deformity (PIP not fixed) | Fixed swan neck deformity, chronic irreducible DIP subluxation |
| Joint Stability | Stable DIP joint, no subluxation | Irreducible DIP subluxation (rare for pure soft tissue) |
| Patient Factors | Compliant, motivated patient, low functional demand if lag persists | High functional demand, non-compliant with splinting (less ideal) |
| Tissue Status | Healthy, viable tissues | Significant scarring, poor tendon quality requiring repair/reconstruction |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is critical for optimizing outcomes in soft tissue mallet finger repair. This involves a comprehensive patient assessment, careful imaging review, and consideration of the surgical approach.
Pre-Operative Assessment
-
Clinical Examination
:
- History : Elicit the mechanism of injury, date of injury, prior treatments, and current functional limitations. Document hand dominance and occupation.
- Inspection : Observe the resting posture of the affected finger, noting the characteristic DIP joint flexion deformity.
- Palpation : Assess for tenderness over the dorsal aspect of the DIP joint.
-
Range of Motion
:
- Active DIP Extension Lag : Measure the angle of flexion at the DIP joint when the patient attempts active extension. This is the primary measure of the mallet deformity.
- Passive DIP Motion : Gently extend the DIP joint to assess full passive extension. In soft tissue mallet, full passive extension should be achievable. Inability to passively extend suggests joint contracture, which may require additional releases.
- Adjacent Joint Motion : Assess PIP and MCP joint range of motion to identify any secondary stiffness or the presence of a swan neck deformity (PIP hyperextension, often with decreased PIP flexion).
- Neurovascular Status : Document sensation and capillary refill in the affected digit.
-
Imaging
:
- Plain Radiographs : Standard AP, lateral, and oblique views of the affected digit are mandatory. These are crucial to rule out bony avulsion fractures (Doyle Type II, III, IV), DIP joint subluxation, and pre-existing arthritis. A true lateral view is essential to accurately assess the joint alignment and presence of bony avulsion. For pure soft tissue mallet, radiographs will typically show no significant bony pathology.
- MRI : Generally not indicated for routine soft tissue mallet finger. It may be considered in very chronic, complex cases with ambiguous diagnoses or to assess the extent of tendon retraction and scarring, but it adds significant cost and is rarely needed for surgical decision-making in Type I injuries.
- Patient Factors : Discuss patient expectations, functional goals, and the commitment required for post-operative rehabilitation. Assess for comorbidities that may affect wound healing or anesthetic risk (e.g., diabetes, peripheral vascular disease, smoking).
Anesthesia
- Regional Anesthesia : A brachial plexus block (e.g., axillary block) or wrist block is often preferred. This provides excellent intraoperative analgesia, post-operative pain control, and motor paralysis, facilitating visualization and repair.
- General Anesthesia : May be used based on patient preference, surgeon preference, or if a regional block is contraindicated or unsuccessful.
- Local Anesthesia with Sedation : Digital blocks can be used for very minor procedures, but are generally insufficient for complex repairs due to the need for a bloodless field and extensive dissection.
Patient Positioning
- Position : The patient is typically positioned supine on the operating table.
- Arm Preparation : The affected arm is abducted and placed on a radiolucent hand table, allowing full access to the hand and fingers.
- Tourniquet : An upper arm pneumatic tourniquet is routinely used to create a bloodless field, which is essential for clear visualization of the delicate extensor mechanism. The tourniquet time should be monitored.
- Sterile Preparation and Draping : The hand and forearm are prepped with an antiseptic solution (e.g., povidone-iodine or chlorhexidine) and sterilely draped, ensuring exposure of the entire digit and potential donor sites if grafting is anticipated.
- Magnification : Use of surgical loupes (2.5x to 4.5x magnification) is highly recommended to aid in the precise identification of tendon ends and meticulous repair.
Detailed Surgical Approach / Technique
Surgical repair of soft tissue mallet finger aims to restore the integrity of the terminal extensor tendon, re-establish active DIP joint extension, and prevent secondary deformities. The technique varies based on the acuity of the injury, extent of retraction, and tissue quality.
Principles of Repair
- Direct Repair : Whenever feasible, direct end-to-end repair of the ruptured tendon is the preferred method, especially in acute or subacute cases where tissue quality is good and retraction is minimal.
- Tension-Free Repair : The repair should be performed with minimal tension to promote healing and reduce the risk of re-rupture.
- Sufficient Immobilization : The DIP joint must be adequately immobilized post-operatively to protect the repair during the healing phase.
Incision
Several incision types can be used, with the choice often dictated by surgeon preference and the chronicity of the injury.
*
Dorsal Longitudinal Incision
: A straight longitudinal incision centered over the DIP joint allows good exposure and can be extended proximally or distally if needed. Care must be taken to avoid injury to the underlying tendon. This can sometimes lead to scar contracture, particularly if placed directly over the joint.
*
Transverse Incision
: A curved transverse incision just distal to the DIP joint crease, or a straight transverse incision at the DIP joint level. Provides good cosmetic outcome but may limit exposure in complex cases.
*
Dorsal Y-V Plast
(or Z-plasty modification): Can be utilized in chronic cases with associated skin contracture, allowing for lengthening of the dorsal skin and better exposure.
Regardless of the choice, incision planning should account for neurovascular bundles and the potential for scar contracture.
Dissection
- Skin and Subcutaneous Dissection : Incise the skin and carefully dissect through the subcutaneous tissue. Identify and protect the dorsal digital nerves, which are superficial and run along the sides of the digit. Using loupes is invaluable here.
- Exposure of Extensor Mechanism : Carefully identify the ruptured extensor tendon. In acute cases, the torn ends may be relatively easy to find, with the proximal end often retracted slightly. In chronic cases, the proximal tendon end may be significantly retracted (often proximally to the PIP joint level) and embedded in scar tissue. The distal stump is usually very short, often a thin flap of tissue still attached to the distal phalanx.
- Debridement : Gently debride any frayed, necrotic, or excessively scarred tissue from the tendon ends to provide healthy tissue for repair. Avoid aggressive debridement that would shorten the tendon excessively.
Repair Technique
The goal is to re-establish the attachment of the terminal extensor tendon to the distal phalanx.
-
Identification and Mobilization
:
- Locate the distal attachment site on the dorsal aspect of the distal phalanx. This may require gentle elevation of residual tendon fibers.
- Locate the retracted proximal tendon stump. This may necessitate gentle probing proximally along the dorsal aspect of the middle phalanx. Once found, mobilize it sufficiently to allow for tension-free advancement to the distal phalanx.
-
Tendon-to-Bone Reattachment (Direct Repair) :
- This is the most common technique for acute and subacute soft tissue mallets.
- Drill Holes : Create two small drill holes (e.g., 22G needle, 0.028-inch K-wire) in the dorsal aspect of the distal phalanx, just distal to the DIP joint. These holes should exit through the volar cortex or nail plate, creating bone tunnels.
- Suture Placement : Use a strong, non-absorbable monofilament suture (e.g., 4-0 or 5-0 Prolene, FiberWire). A modified Kessler or Krackow stitch is often employed in the proximal tendon stump for secure purchase. The sutures are then passed through the drill holes in the distal phalanx.
- Reattachment : The sutures are brought out volarly, tied over a button on the volar aspect of the fingertip, or tied directly over the nail plate with a felt pad for protection. This technique securely pulls the tendon stump down to its anatomical insertion. Alternatively, suture anchors can be used to reattach the tendon directly to the bone without drilling through the entire phalanx.
- Tendon-to-Tendon Repair : In situations where a sufficient distal tendon stump remains (rare in Type I, more common in lacerations), a direct tendon-to-tendon repair can be performed using various techniques (e.g., modified Kessler, Bunnell, locking loop). This usually requires protection of the repair by transarticular K-wire fixation.
-
Tendon Advancement/Shortening (for Chronic Cases) :
- For chronic injuries with significant retraction and scar tissue, direct reattachment may lead to excessive tension.
- The tendon may be advanced distally and reattached to the distal phalanx as described above. If the tendon is attenuated or excessively long due to scar, a segment may be resected to restore appropriate tension, followed by direct end-to-end repair.
- Lateral Band Involvement : In some chronic cases, the lateral bands may become thickened or adherent, contributing to persistent extensor lag. Release of these adhesions or selective shortening may be considered.
-
Tendon Grafting (for Large Gaps/Poor Tissue Quality) :
- If there is a substantial gap or the native tendon tissue is severely compromised, a tendon graft may be necessary. Common donor sites include the palmaris longus, plantaris, or extensor indicis proprius.
- The graft is interwoven into the proximal tendon stump and distally secured to the distal phalanx using the bone tunnel technique or suture anchors. This is a more complex procedure with longer rehabilitation.
-
Reinforcement : In some cases, local tissue flaps (e.g., parts of the dorsal capsule, tenodesis using a portion of the lateral band) can be used to reinforce the repair, though this is less common for isolated soft tissue mallet.
Internal Fixation (K-wire)
After the tendon repair, transarticular K-wire fixation of the DIP joint is almost always performed to protect the repair and maintain the joint in the desired position during healing.
*
Positioning
: The DIP joint is gently placed in full extension or slight hyperextension (0-10 degrees). Over-extension should be avoided to prevent skin complications or volar plate injury.
*
K-wire Placement
: A single 0.035-inch (0.9 mm) or 0.045-inch (1.1 mm) K-wire is typically used.
*
Dorsal-Volar Approach
: The K-wire is inserted through the dorsal aspect of the distal phalanx, across the DIP joint, and into the middle phalanx. The entry point should avoid the nail matrix and tendon repair.
*
Lateral-Lateral Approach
: Less common for mallet finger, but involves placing two small K-wires laterally, crossing the joint. This may be preferred if the dorsal approach compromises the repair or nail matrix.
*
Confirmation
: Confirm proper K-wire position with intraoperative fluoroscopy or radiographs to ensure the joint is adequately immobilized and the wire does not impinge on articular surfaces or neurovascular structures. The wire should be bent and cut short outside the skin to prevent migration and allow easy removal.

Closure
- Layered Closure : Once the repair and K-wire fixation are complete, the wound is irrigated. The subcutaneous tissue and skin are meticulously closed in layers using fine sutures (e.g., 5-0 absorbable for subcutaneous, 5-0 or 6-0 non-absorbable for skin).
- Dressings : A sterile dressing is applied, typically a non-adherent dressing directly over the wound, followed by gauze and a light compressive bandage. A protective splint may be applied over the dressing to augment the K-wire fixation and provide further support to the finger, particularly for the PIP joint to prevent swan necking.
Complications & Management
Despite meticulous surgical technique and diligent post-operative care, complications can occur after soft tissue mallet finger repair. It is crucial for the orthopedic surgeon to be aware of these potential issues, their incidence, and appropriate management strategies.
| Complication | Incidence | Management / Salvage Strategies |
|---|---|---|
| Extensor Lag / Re-rupture | Most common (5-20%), higher in chronic cases | Mild lag (<15°) : Continue therapy, extended splinting (night, activity-specific). Moderate-Severe lag (>15° or re-rupture) : Re-evaluation of compliance; revision surgery (redo repair if possible, tendon advancement, tenodesis using local tissue or graft, or ultimately DIP fusion for severe functional deficit). |
| Infection | Low (1-5%), higher with open injuries | Superficial : Oral antibiotics, local wound care. Deep : Surgical debridement, intravenous antibiotics, hardware removal (if K-wire), culture-specific antibiotic therapy. May require wound VAC or staged reconstruction. |
| Stiffness / Loss of Motion | Common (10-30%), particularly flexion | DIP Flexion Contracture : Aggressive hand therapy, serial casting/splinting, dynamic splinting. PIP Hyperextension (Swan Neck) : PIP flexion splinting, extensor tenolysis at PIP joint, intrinsic release, thenar muscle transfer, or lateral band reconstruction for fixed deformities. DIP Arthrofibrosis : Tenolysis, capsulotomy. |
| Nail Deformity | Variable (5-15%), often cosmetic | Hook Nail / Ridging : Often transient. If persistent and problematic, nail bed revision, nail plate removal, or osteotomy of distal phalanx. Non-adherence : Patient education, conservative management. |
| Skin Necrosis / Wound Issues | Low (1-3%), higher in smokers/diabetics | Local wound care, serial debridement. If significant, requires skin grafting, local flap coverage (e.g., V-Y advancement, cross-finger flap) for wound closure. Cessation of smoking. |
| Pain / Hardware Complications | Variable, related to K-wire use | K-wire Migration/Breakage : Early removal of hardware, replace if necessary. Pin Tract Infection : Local wound care, oral antibiotics, K-wire removal. Nerve Irritation (Dorsal Digital Nerve) : Observation, anti-neuropathic agents. If persistent, nerve release/neurolysis or excision of painful neuroma. Tenderness over Repair : Anti-inflammatory medication, local massage. |
| Swan Neck Deformity | Secondary deformity if mallet is untreated/failed | Prophylaxis : Proper post-op care focusing on PIP joint range. Flexible Deformity : PIP flexion splinting, intrinsic stretching. Fixed Deformity : Often requires complex reconstruction, including PIP volar plate tenodesis, intrinsic release, or PIP arthrodesis in severe, recalcitrant cases. Addressing the underlying mallet deformity (if not already done) is paramount. |
| Hypersensitivity/CRPS | Rare (<1%) | Aggressive physical therapy, pain management (neuropathic medications, sympathetic blocks), psychological support. Early diagnosis and intervention are key. |
Specific Considerations for Management
Extensor Lag/Re-rupture
: This is the most common reason for unsatisfactory outcomes. It can result from inadequate immobilization, excessive post-operative stress, poor tissue quality, or technical error during repair.
* Initial management involves stricter adherence to rehabilitation protocols, including prolonged splinting.
* For persistent, functionally significant lag, revision surgery may be considered. Options include repeat direct repair, tendon advancement (if proximal tissue allows), tenodesis (using a portion of the lateral band or a small palmaris longus graft), or, in cases of severe, irreparable damage with significant functional impairment, DIP joint arthrodesis (fusion) in a functional position (typically 10-15 degrees of flexion).
Stiffness and Loss of Motion
: While protecting the DIP repair, it is crucial to encourage full range of motion at the PIP and MCP joints. Prolonged, rigid immobilization of all joints can lead to diffuse stiffness.
* Early, controlled motion of uninvolved joints is key.
* For DIP flexion stiffness, aggressive hand therapy, dynamic splinting, or serial casting may be needed.
* Surgical intervention (tenolysis or capsulotomy) for severe, fixed contractures is a last resort.
Nail Deformity : Disruption of the germinal matrix during injury or surgery can lead to nail growth abnormalities. Most are cosmetic and resolve over time. In rare cases, revision of the nail bed or distal phalanx osteotomy may be considered.
K-wire Complications : Pin tract infections are managed with local wound care and oral antibiotics; wire removal is indicated if infection persists or deepens. K-wire migration or breakage requires removal. Nerve injury from pin placement, while rare, may necessitate observation or surgical exploration.
Swan Neck Deformity
: This secondary deformity results from an imbalance in the extensor mechanism, with volar plate laxity at the PIP joint and overactivity of the central slip, leading to PIP hyperextension and compensatory DIP flexion. It can be a consequence of untreated or failed mallet finger.
* Prevention involves strict mallet splinting and monitoring of PIP joint posture.
* Management often requires a multi-faceted approach, addressing both the mallet deformity and the PIP joint hyperextension. PIP flexion splinting, intrinsic muscle release, or formal PIP joint volar plate tenodesis (e.g., using a FDS slip or static tenodesis with a wire) may be necessary.
Thorough patient education regarding potential complications, their prevention, and the importance of adhering to rehabilitation protocols is essential for managing expectations and optimizing outcomes.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is a critical determinant of outcome following soft tissue mallet finger repair. The protocol aims to protect the surgical repair while restoring functional range of motion and strength. Strict adherence to a phased, controlled program, often guided by a certified hand therapist, is essential.
Phase 1: Immobilization (Weeks 0-6)
The primary goal of this phase is to protect the surgically repaired terminal extensor tendon, allowing for initial healing, while preventing stiffness in uninvolved joints.
-
DIP Joint Immobilization
:
- The DIP joint is maintained in full extension or slight hyperextension (0-10 degrees) via the transarticular K-wire or a custom-molded thermoplastic splint (Stack splint or similar dorsal/volar splint).
- If a K-wire is present, the splint primarily augments protection and reminds the patient of the injury.
- Crucial Principle : Absolutely no active or passive DIP joint flexion is permitted. The patient must be meticulously educated on this, particularly for activities of daily living.
-
PIP and MCP Joint Motion
:
- Active and passive range of motion exercises for the PIP and MCP joints are immediately encouraged to prevent stiffness.
- Focus : Full flexion and extension of PIP and MCP joints, avoiding any strain on the DIP joint.
-
Edema Control
:
- Elevation of the hand (above heart level).
- Gentle compression dressings (avoiding excessive pressure on the K-wire or DIP joint).
- Gentle retrograde massage (proximal direction) to reduce swelling.
-
Wound Care
:
- Keep the surgical site clean and dry.
- Monitor for signs of infection (redness, swelling, pain, discharge).
- Patient Education : Reinforce the importance of protection, proper splint wear, and adherence to the activity restrictions.
Phase 2: Protected Motion (Weeks 6-12)
This phase transitions from rigid immobilization to controlled, guarded motion, gradually increasing the stress on the healing tendon.
- K-wire Removal (if present) : Typically performed at 6 weeks post-operatively.
-
DIP Joint Motion
:
- Initiate Passive DIP Flexion : Very gentle, controlled passive flexion of the DIP joint is started, gradually increasing the range. The therapist guides this, ensuring the movement is pain-free and does not cause excessive tension on the repair.
- Initiate Active DIP Extension : Active DIP extension against gravity, up to the full extension endpoint, is encouraged.
- Avoid Active DIP Flexion : Active, unresisted DIP flexion is still restricted.
-
Splinting Regimen
:
- Night Splinting : Continue DIP joint extension splinting during sleep for an additional 4-6 weeks (total 10-12 weeks from surgery).
- Protective Splinting : Wear the DIP extension splint during high-risk activities, sports, or during situations where accidental impact is possible.
- Continue PIP/MCP ROM : Maintain full range of motion for adjacent joints.
-
Scar Management
:
- Gentle scar massage once the wound is well-healed to prevent adhesions and soften scar tissue.
- Topical silicone products may be used.
Phase 3: Strengthening & Return to Activity (Weeks 12+)
The final phase focuses on restoring full strength, endurance, and function, with a gradual return to unrestricted activities.
-
Gradual Increase in DIP Motion
:
- Progress from passive/active assisted DIP flexion to active, unresisted DIP flexion.
- Gradually discontinue all protective splinting as active motion improves and pain subsides.
-
Strengthening Exercises
:
- Begin with gentle isometric exercises for DIP extension and flexion.
- Progress to light resistive exercises using therapeutic putty, rubber bands, or light weights, focusing on both extensor and flexor strength.
- Emphasize grip strength and overall hand function.
-
Functional Activities
:
- Progressive integration into daily activities, occupational tasks, and sport-specific drills.
- Educate the patient on proper body mechanics and protective measures to prevent re-injury.
-
Monitoring
:
- Regular assessment of extensor lag, range of motion, and pain levels.
- Adjust the protocol based on individual patient progress and healing response.
- Full recovery of pre-injury strength and range of motion can take several months.
Key Principles for Rehabilitation
:
*
Communication
: Close collaboration between the surgeon and hand therapist is paramount.
*
Patient Education and Compliance
: The success of the rehabilitation program heavily relies on the patient's understanding and strict adherence to the prescribed exercises and restrictions.
*
Gradual Progression
: Advancement through phases should be based on clinical healing and functional improvement, not solely on timeframes.
*
Individualization
: Protocols are guidelines; adjustments must be made for individual patient needs, comorbidities, and the specific surgical technique employed.
Summary of Key Literature / Guidelines
The management of soft tissue mallet finger (Doyle Type I) is well-established, with the vast majority of literature supporting non-operative splinting as the first-line treatment. Surgical intervention is typically reserved for specific indications as outlined.
Non-Operative Management
:
The cornerstone of mallet finger treatment since its earliest descriptions, continuous immobilization of the DIP joint in extension (or slight hyperextension) for 6-8 weeks, followed by night-time splinting for an additional 2-4 weeks, remains the gold standard for acute soft tissue injuries. Studies by
Smirk and McMahon (2001)
and
Lubahn et al. (1986)
underscore the high success rates (typically 80-90%) with proper splinting and patient compliance. The critical factor is continuous wear; even brief periods of DIP joint flexion during the initial healing phase can compromise the repair. Various splint designs (Stack splints, custom thermoplastic splints) have similar efficacy, with patient comfort and compliance being key differentiators.
Surgical Management (Indications and Outcomes)
:
While primary repair of acute soft tissue mallet finger is less common than splinting, it finds its niche in select circumstances.
*
Chronic Mallet Deformities
: For cases presenting late with persistent, functionally significant extensor lag (>15-20 degrees) after failed conservative treatment, surgical reconstruction offers a viable option. Authors like
Wehbe and Schneider (1989)
have detailed various techniques for reconstruction of the extensor mechanism.
*
Techniques
: Direct end-to-end repair with suture anchors or pull-out sutures through drill holes in the distal phalanx is a common approach. For retracted or attenuated tendons, advancements, tendon shortening, or interpositional grafting (e.g., palmaris longus) have been described.
Ismail et al. (2014)
reviewed surgical options for chronic mallet finger, highlighting the complexity and the often varied outcomes compared to acute splinting.
*
Open Injuries
: Acute open mallet finger lacerations require surgical debridement and primary repair, irrespective of the degree of lag, to prevent infection and restore tendon integrity.
*
Associated Deformities
: Mallet finger can lead to secondary swan neck deformity.
Belsky et al. (1989)
described the pathogenesis and management strategies for swan neck deformities secondary to mallet finger, often involving a combination of DIP joint repair and PIP joint volar plate procedures or intrinsic muscle releases.
Complications and Salvage
:
The literature consistently reports that complications such as persistent extensor lag, stiffness (particularly DIP flexion loss), and nail deformities are the most common challenges.
*
Extensor Lag
: Recurrent extensor lag is the most frequent reason for dissatisfaction post-surgery.
Crawford and Dawson (2007)
reviewed factors affecting outcomes, emphasizing the importance of patient compliance and precise surgical technique. Salvage options range from prolonged splinting for mild cases to revision surgery (repeat repair, tenodesis, or fusion) for significant functional deficits.
*
Stiffness
: Protocols emphasizing early, protected PIP and MCP joint motion are crucial to minimize overall hand stiffness.
Dinopoulos et al. (2004)
discussed the balance between protection of the repair and prevention of stiffness.
*
Infection and Hardware-related Issues
: These are less frequent but can significantly impact outcomes, necessitating prompt identification and appropriate management (antibiotics, debridement, hardware removal).
General Guidelines and Consensus
:
* Most orthopedic and hand surgery guidelines strongly advocate for non-operative management of acute, closed soft tissue mallet finger injuries, citing its high success rate and low complication profile.
* Surgical intervention is largely reserved for failed conservative treatment, chronic cases with significant functional impairment, open injuries, or those associated with complex secondary deformities like fixed swan neck.
* The choice of surgical technique depends heavily on the individual pathology, surgeon experience, and patient factors. Regardless of the approach, meticulous surgical technique and a structured, therapist-supervised post-operative rehabilitation program are critical for optimal outcomes.
* Patient education regarding the prolonged healing process, the importance of adherence to protocols, and realistic expectations is paramount in achieving satisfactory results.
In conclusion, the management of soft tissue mallet finger is an excellent example of the effectiveness of conservative treatment for a common injury, with surgery acting as a crucial, albeit secondary, option for specific, challenging presentations.
You Might Also Like