Complex Index Finger MCP & PIP Joint Injuries: Diagnosis, Surgical Anatomy, and Management
Key Takeaway
Complex index finger MCP and PIP joint injuries involve intricate damage to articular surfaces, ligaments, and soft tissues from high-energy trauma. Accurate diagnosis, vital for preserving hand function, necessitates understanding their epidemiology, detailed surgical anatomy, and biomechanics. Meticulous management prevents chronic pain and functional impairment.
Introduction & Epidemiology
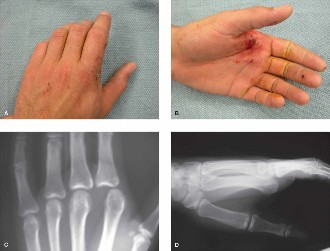
Complex injuries to the joints of the index finger represent a significant challenge in hand surgery, demanding meticulous diagnosis and precise surgical management to preserve critical hand function. The index finger, being the primary digit for precision grip and fine motor tasks, holds paramount importance in daily activities and professional occupations. Injuries can range from isolated ligamentous tears and irreducible dislocations to highly comminuted intra-articular fractures and fracture-dislocations involving either the metacarpophalangeal (MCP) or proximal interphalangeal (PIP) joint.
The etiology of these complex injuries is diverse, frequently involving high-energy trauma such as axial loading, hyperextension, rotational forces, or direct impact. Common scenarios include sports-related injuries (e.g., ball sports, contact sports), falls onto an outstretched hand, and industrial accidents. Epidemiological data highlight the PIP joint as the most frequently injured joint in the hand, with dislocations and fracture-dislocations being prevalent. While MCP joint dislocations are less common, they often present with unique challenges due to entrapment of surrounding soft tissues. Intra-articular fractures, particularly pilon fractures of the proximal or middle phalanx, or condylar fractures of the metacarpal head or proximal phalanx, carry a high risk of post-traumatic arthritis and chronic stiffness if not anatomically reduced and stably fixed.
The complexity of these injuries often stems from a combination of articular surface disruption, ligamentous instability, capsular tearing, and potential involvement of the extensor or flexor tendon mechanisms. Accurate and timely diagnosis is paramount, as missed or inadequately treated injuries can lead to chronic pain, joint instability, progressive stiffness, and debilitating functional impairment, severely impacting a patient's quality of life and vocational capacity. This comprehensive review focuses on the academic and surgical considerations for diagnosing and managing complex injuries of the index finger's MCP and PIP joints, emphasizing high-yield anatomical, biomechanical, and technical aspects critical for orthopedic surgeons, residents, and medical students.
Surgical Anatomy & Biomechanics
A profound understanding of the intricate anatomy and biomechanics of the index finger's MCP and PIP joints is foundational to both accurate diagnosis and successful surgical intervention for complex injuries.
Metacarpophalangeal (MCP) Joint of the Index Finger
The MCP joint is a condylar joint, allowing for flexion/extension, abduction/adduction, and circumduction. Its stability is derived from both bony congruence and a robust ligamentous-capsular complex.
- Bony Anatomy: The convex metacarpal head articulates with the concave base of the proximal phalanx. The metacarpal head has two condyles separated by a shallow groove.
- Joint Capsule: A thin, loose capsule permits a wide range of motion.
- Volar Plate: A strong fibrocartilaginous structure located on the volar aspect of the joint. It is firmly attached to the proximal phalanx base (distal insertion) and loosely connected to the metacarpal neck (proximal insertion) via a membranous attachment. It prevents hyperextension and provides a floor for the flexor tendons.
-
Collateral Ligaments (Radial and Ulnar):
These are the primary stabilizers against varus and valgus stress. Each collateral ligament consists of a cord portion and an accessory portion.
- Cord Portion: Originates from the dorsal aspect of the metacarpal head and inserts onto the volar aspect of the proximal phalanx base. These cords are taut in flexion and lax in extension, a crucial biomechanical feature allowing finger spread in extension and firm grip in flexion.
- Accessory Portion: Originates more volarly on the metacarpal head and inserts into the volar plate. These are taut in extension and lax in flexion.
- Extensor Mechanism: The extensor digitorum communis (EDC) tendon divides into three slips (a central slip to the middle phalanx, two lateral slips that join to form the terminal tendon to the distal phalanx). At the MCP joint, the sagittal bands, which originate from the volar plate and deep transverse metacarpal ligament, encircle the metacarpal head and insert into the extensor tendon, stabilizing its position dorsally over the joint.
- Flexor Tendons: The flexor digitorum superficialis (FDS) and flexor digitorum profundus (FDP) tendons run within the flexor sheath volar to the joint, providing flexion power.
- Neurovascular Bundles: Digital nerves and arteries run along the radial and ulnar aspects of the digits, vulnerable during surgical approaches.
Proximal Interphalangeal (PIP) Joint of the Index Finger
The PIP joint is a true hinge joint, allowing primarily flexion and extension. It is remarkably stable due to its constrained bony articulation and powerful ligamentous restraints.
- Bony Anatomy: The trochlea of the proximal phalanx head articulates with the base of the middle phalanx. The trochlea has a central groove fitting into a ridge on the middle phalanx base, enhancing stability.
- Joint Capsule: Relatively thick and taut.
- Volar Plate: Extremely robust and thick, firmly attached to both the proximal and middle phalanges. It is the primary restraint against hyperextension and dorsal dislocation. Its proximal attachment contains check-rein ligaments, fibrous extensions that restrict its proximal excursion.
- Collateral Ligaments (Radial and Ulnar): Strongest in the hand, these ligaments originate from the head of the proximal phalanx and insert onto the base of the middle phalanx, volar to the axis of rotation. They are taut throughout the range of motion, providing critical stability against varus/valgus stress.
- Extensor Mechanism: At the PIP joint level, the central slip of the extensor tendon inserts onto the dorsal base of the middle phalanx, providing extension. The lateral bands pass distally, joining to form the terminal tendon. The triangular ligament connects the lateral bands dorsally.
- Flexor Tendons: FDS inserts into the middle phalanx, FDP into the distal phalanx.
- Neurovascular Bundles: Similar to the MCP joint, these run along the sides.
Biomechanical Implications for Injury
Understanding these structures is critical for diagnosing injury patterns:
- MCP Joint: Hyperextension can lead to volar plate rupture and irreducible dorsal dislocation due to volar plate interposition. Varus/valgus stress can injure collateral ligaments. Avulsion fractures of the volar plate or collateral ligament insertions are common.
- PIP Joint: Dorsal dislocations are very common due to hyperextension, often with volar plate avulsion. Lateral dislocations involve collateral ligament rupture. Axial loading can cause pilon fractures of the middle phalanx base or condylar fractures of the proximal phalanx head, leading to significant articular incongruity and instability. The central slip of the extensor mechanism can avulse, leading to a Boutonnière deformity.

A detailed anatomical overview, potentially depicting the ligamentous structures and joint capsule of the PIP joint, is essential for comprehending the mechanisms of complex injury patterns and planning appropriate surgical interventions. The above image could represent such a detailed view.
Indications & Contraindications
The decision-making process for managing complex index finger joint injuries involves a careful assessment of patient factors, injury characteristics, and functional demands. The primary goal is to restore anatomical congruence, stability, and optimal function while minimizing complications.
Operative Indications
Surgical intervention is generally indicated for complex injuries where conservative management is unlikely to achieve a stable, congruent, and functional joint. Specific indications include:
-
Irreducible Dislocations:
- MCP Joint: Often due to interposition of the volar plate, flexor tendons, or a sagittal band, creating a "buttonhole" deformity that blocks reduction. Chronic dislocations (beyond 2-3 weeks) often require open reduction due to soft tissue contracture.
- PIP Joint: Less common than irreducible MCP, but can occur with incarcerated volar plate or collateral ligament.
-
Unstable Intra-articular Fractures:
- Articular Step-Off: Displacement of articular fragments exceeding 1-2 mm, significantly increasing the risk of post-traumatic arthritis.
- Joint Incongruity/Subluxation: Persistent subluxation or dislocation after reduction attempts, indicating severe instability.
- Large Articular Fragment: A single articular fragment compromising >25-30% of the joint surface, especially if displaced.
- Condylar Fractures: Displaced unicondylar or bicondylar fractures of the metacarpal head or proximal phalanx (PIP joint) that lead to instability or malrotation.
- Pilon Fractures: Comminuted intra-articular fractures of the proximal or middle phalanx base.
- Fracture-Dislocations: Combined articular fracture and joint dislocation that is unstable, irreducible, or has significant articular disruption. These are particularly challenging due to dual insult to bony and ligamentous structures.
- Open Fractures/Dislocations: Require urgent debridement and stabilization to prevent infection and facilitate healing.
-
Significant Ligamentous Instability:
- Complete Collateral Ligament Rupture: Demonstrated by significant laxity (>20-30 degrees angulation compared to contralateral) under stress, especially for active individuals.
- Volar Plate Avulsion: Large, displaced avulsion fractures from the middle phalanx base (PIP joint) or proximal phalanx base (MCP joint) resulting in persistent instability or hyperextension.
- Central Slip Avulsion: Displaced avulsion of the central slip of the extensor mechanism at the PIP joint, leading to a Boutonnière deformity.
- Failed Closed Reduction: When closed reduction is unsuccessful or the reduction cannot be maintained.
- Rotational Malalignment: Even minor degrees of rotational malunion can lead to scissoring of digits and significant functional impairment.
Non-Operative Indications
Conservative management is appropriate for stable injuries without significant articular disruption or irreducible deformity.
- Stable, Reducible Dislocations: Once reduced, if the joint maintains stability through the full range of motion or with protective splinting, non-operative management is considered.
-
Minimally Displaced or Stable Fractures:
- Extra-articular fractures without significant displacement or rotational deformity.
- Intra-articular fractures with <1 mm articular step-off and no instability.
- Stable avulsion fractures (e.g., small volar plate avulsions) without joint instability.
- Stable Ligamentous Sprains: Grade I and II collateral ligament sprains without significant joint laxity.
- Patients with Significant Comorbidities: Those who are high surgical risks or have limited functional demands where the risks of surgery outweigh potential benefits.
- Patient Preference: After a thorough discussion of risks, benefits, and alternatives, a patient may opt for non-operative management, understanding the potential for suboptimal outcomes.
Contraindications
Absolute contraindications to surgical intervention are rare but primarily include:
- Active Infection: Uncontrolled local or systemic infection in the operative field.
- Severe Crushing Injury: Irreparable soft tissue damage, severe comminution with no reconstructible fragments, or critical vascular compromise where salvage is not feasible.
- Severe Medical Comorbidities: Unstable medical conditions that preclude safe anesthesia and surgery.
- Profound Osteopenia: Poor bone quality that would preclude stable implant fixation (though alternative techniques like K-wire arthrodesis might still be possible).
- Established Severe Osteoarthritis: In cases of end-stage post-traumatic arthritis, arthrodesis or arthroplasty might be more appropriate primary interventions rather than fracture fixation and ligament repair.
Table: Operative vs. Non-Operative Indications
| Feature | Operative Indications | Non-Operative Indications |
|---|---|---|
| Dislocations |
- Irreducible dislocations (MCP: volar plate interposition; PIP: incarcerated structures)
- Chronic dislocations (>2-3 weeks) |
- Stable, reducible dislocations, maintaining congruence after reduction |
| Intra-articular Fractures |
- Articular step-off >1-2 mm
- Joint incongruity/subluxation - Displaced condylar fractures - Displaced pilon fractures - Large (>25-30%) articular fragments with displacement/instability - Rotational malalignment |
- Articular step-off <1 mm
- Minimally displaced stable fractures - No joint incongruity or instability after initial treatment |
| Ligamentous Injuries |
- Complete collateral ligament ruptures with significant instability (>20-30° laxity)
- Displaced volar plate avulsion fractures causing instability - Displaced central slip avulsion causing Boutonnière deformity |
- Grade I-II collateral ligament sprains without significant laxity
- Small, non-displaced volar plate avulsion fractures without instability |
| Fracture-Dislocations |
- Unstable or irreducible fracture-dislocations
- Significant articular surface disruption - Open fracture-dislocations |
- Stable fracture-dislocations with minimal articular involvement (rare)
- Those manageable by closed reduction and stable immobilization |
| General |
- Failed closed reduction
- Open injuries - Progressive deformity - Anticipated poor functional outcome with non-operative management |
- Stable injuries in patients with high surgical risk
- Patient preference after comprehensive discussion - Low functional demands where residual stiffness or mild instability is tolerable (in specific, selected cases and with patient understanding of sequelae) |
Pre-Operative Planning & Patient Positioning
Thorough pre-operative planning is the cornerstone of successful management for complex index finger joint injuries. It minimizes intra-operative surprises, optimizes surgical efficiency, and enhances patient outcomes.
Diagnostic Imaging
Beyond clinical examination, imaging is critical for defining the injury.
-
Standard Radiographs:
Anteroposterior (AP), lateral, and true oblique views are mandatory.
- Lateral View: Crucial for assessing joint congruence, identifying dorsal or volar dislocations, and evaluating articular step-off in the sagittal plane.
- Oblique Views: Can highlight subtle condylar fractures or avulsion fragments missed on standard AP/lateral.
- Stress Radiographs: May be indicated for suspected collateral ligament injuries to quantify instability, although clinical stress testing is often sufficient.
-
Computed Tomography (CT) Scan:
- Indications: Absolutely essential for all suspected intra-articular fractures or complex fracture-dislocations.
- Value: Provides detailed information on fracture configuration, comminution, fragment size, location, displacement, and articular step-off in three dimensions. This guides the choice of surgical approach and fixation strategy. 3D reconstructions are particularly useful for understanding the complex geometry of condylar or pilon fractures.
-
Magnetic Resonance Imaging (MRI):
- Indications: Primarily for soft tissue injuries where diagnosis is uncertain or surgical planning requires specific detail (e.g., complete collateral ligament ruptures without bony avulsion, volar plate tears, central slip avulsions, extensor tendon entrapment in MCP dislocations).
- Value: Delineates ligamentous, tendinous, and capsular structures, and can identify occult contusions or osteochondral lesions.
- Fluoroscopy: Used intra-operatively to confirm reduction and fixation.
Surgical Planning
Based on comprehensive imaging, a detailed surgical plan should be formulated.
-
Approach Selection:
The chosen approach (dorsal, volar, mid-axial) depends on the specific injury pattern, location of fragments, and structures requiring repair.
- Dorsal Approach: Best for dorsal fracture-dislocations, pilon fractures of the phalanx base, and extensor mechanism repair.
- Volar Approach: Preferred for volar plate avulsions, irreducible volar dislocations, and specific volar condylar fractures. Requires careful neurovascular and flexor tendon protection.
- Mid-axial Approach: Useful for direct access to collateral ligaments or lateral condylar fractures.
-
Implant Selection:
Determine the specific hardware needed:
- K-wires: For temporary fixation, definitive fixation of small fragments, tension band wiring, or arthrodesis.
- Mini-screws: 1.0 mm, 1.3 mm, or 1.5 mm cortical screws or headless compression screws for articular fragments, condylar fractures.
- Mini-plates: 1.3 mm or 1.5 mm plates (e.g., locking plates, L-plates, T-plates, buttress plates) for unstable metaphyseal or diaphyseal extensions, or highly comminuted articular segments.
- Suture Anchors: For ligamentous avulsions (collateral ligaments, volar plate, central slip).
- External Fixation: Occasionally for highly comminuted, unstable injuries, especially pilon fractures with soft tissue compromise (e.g., small joint distraction fixators).
- Reduction Strategy: Plan the sequence of reduction maneuvers (traction, direct manipulation, use of joystick K-wires).
- Soft Tissue Management: Anticipate the need for capsular repair, ligament reconstruction, or tendon repair.
- Bone Grafting: Consider autograft or allograft for significant bone loss, particularly in metaphyseal defects associated with intra-articular fractures.
- Tourniquet Time: Estimate surgical duration to manage tourniquet time.
Patient Positioning and Setup
Proper positioning ensures optimal exposure, patient safety, and surgeon comfort.
- Anesthesia: Regional anesthesia (e.g., axillary block) is often preferred for prolonged procedures, providing both intra-operative anesthesia and post-operative analgesia. General anesthesia is an alternative.
- Positioning: Supine on the operating table with the arm extended on a specialized hand table. The elbow should be comfortable.
- Tourniquet: A pneumatic tourniquet is applied to the upper arm for a bloodless field, typically inflated to 250 mmHg or 100 mmHg above systolic pressure.
- Sterile Field: Standard sterile preparation and draping of the hand and forearm, allowing for full range of motion of the digits.
- Magnification: Use of loupes (2.5x-4.5x magnification) is highly recommended for detailed micro-surgical work in the confined spaces of finger joints.
- Image Intensifier (Fluoroscopy): Essential for intra-operative verification of reduction and hardware placement.
Detailed Surgical Approach / Technique
The surgical technique for complex index finger joint injuries must be tailored to the specific pathology, aiming for anatomical reduction, stable fixation, and early mobilization.
General Principles
- Bloodless Field: Tourniquet use is standard.
- Magnification: Essential for meticulous dissection and visualization of small structures.
- Atraumatic Technique: Handle soft tissues delicately to preserve vascularity and promote healing.
- Anatomical Reduction: Restore articular congruity and overall alignment.
- Rigid Fixation: Achieve stable osteosynthesis to allow early controlled motion.
- Soft Tissue Repair: Reconstruct or repair damaged ligaments and capsule to restore stability.
Surgical Approaches
-
Dorsal Approach (for PIP/MCP joint dorsal fracture-dislocations, Pilon fractures, Extensor Tendon Injuries)
- Incisions: Often an "S" or "lazy S" shaped incision (proximal phalanx) or a longitudinal incision curving around the extensor mechanism (MCP). A straight dorsal incision over the PIP joint can be used, but risks scar contracture.
-
Dissection:
- Carefully elevate full-thickness skin flaps.
- Identify and protect the digital neurovascular bundles radially and ulnarly.
- For PIP Joint: If the central slip is intact, make a longitudinal incision directly over the dorsal aspect of the central slip, or a transverse incision to detach its insertion (requiring subsequent repair). If the central slip is ruptured or avulsed, expose and manage accordingly. In a dorsal fracture-dislocation, the central slip and lateral bands may be displaced laterally. The dorsal capsule is often torn.
- For MCP Joint: Incise through the sagittal band or elevate it to expose the joint. The extensor tendon can be mobilized radially or ulnarly, or split longitudinally.
- Exposure: Once the capsule is incised or elevated, the articular surface is exposed. This approach provides excellent visualization of dorsal articular fragments and the condyles.
-
Volar Approach (for Volar Plate Avulsions, Irreducible Volar Dislocations, Volar Condylar Fractures)
- Incisions: Z-plasty or Brunner incision (zigzag) to prevent scar contracture across flexion creases. A mid-lateral incision can also provide volar access indirectly.
-
Dissection:
- Carefully identify and protect the digital neurovascular bundles along the sides of the flexor sheath.
- For PIP Joint: Incise the A2 pulley (proximal phalanx) or A4 pulley (middle phalanx) if necessary, being mindful of flexor tendon mechanics. Retract flexor tendons radially or ulnarly. The volar plate will be encountered.
- For MCP Joint: Similar care with neurovascular bundles. Retract the flexor tendons. The volar plate and accessory collateral ligaments will be encountered.
- Exposure: Direct visualization of the volar plate and any volar articular fragments.
-
Mid-Axial (Mid-Lateral) Approach (for Collateral Ligament Repairs, Lateral Condylar Fractures)
- Incisions: A straight longitudinal incision along the mid-axial line of the phalanx.
- Dissection: Elevate skin and subcutaneous tissue. Carefully separate the neurovascular bundle from the flexor sheath volarly. Dorsally, the lateral band of the extensor mechanism is identified. The collateral ligament lies between these planes.
- Exposure: Provides direct access to the collateral ligaments and lateral aspects of the joint.
Reduction and Fixation Techniques (Examples for specific complex injuries)
1. PIP Joint Dorsal Fracture-Dislocation (Pilon Fracture of Middle Phalanx Base)
This highly unstable injury often involves a dorsal articular fragment of the middle phalanx base, disruption of the central slip, and loss of articular congruence.
- Approach: Dorsal approach.
-
Procedure:
- Expose Joint: Elevate skin flaps. Identify and retract lateral bands if needed. The central slip may be avulsed or lacerated.
- Fragment Reduction: The key is to reduce the often comminuted articular fragment. Use fine instruments or K-wire joysticks to manipulate the fragments. A small "push-off" fragment may be present.
- Restoration of Articular Congruence: Once the main articular fragment (or fragments) are reduced, temporary K-wire fixation can stabilize them to the main body of the middle phalanx. Ensure no articular step-off.
-
Fixation:
- Mini-screws: For larger, reducible fragments, 1.0 or 1.3 mm cortical or headless compression screws can provide stable fixation. Insert from dorsal to volar, avoiding joint penetration.
- Mini-plates: For more comminuted metaphyseal extension or if screw fixation is insufficient, a small dorsal locking plate (e.g., 1.3 mm) can buttress the dorsal cortex and maintain reduction.
- K-wires: Used for smaller fragments, or as lag screws in conjunction with a tension band. Can also be used for temporary transarticular pinning to maintain reduction (often removed early to prevent stiffness).
- External Fixation: In severe comminution or soft tissue compromise, a small joint distraction external fixator can provide indirect reduction and maintain joint space and length, allowing for ligamentotaxis. This is typically combined with limited internal fixation.
- Soft Tissue Repair: Repair the central slip if avulsed or lacerated (e.g., using suture anchors or direct repair). Repair the joint capsule.
2. MCP Joint Irreducible Dorsal Dislocation
This typically involves the volar plate or a flexor tendon interposing within the joint.
- Approach: Volar approach (preferred for direct visualization of entrapped structures). Alternatively, a dorsal approach can be used, but visualization of the volar plate may be limited.
-
Procedure (Volar):
- Expose Volar Plate: Identify and protect neurovascular bundles. Retract flexor tendons. The volar plate will be seen entrapped between the metacarpal head and proximal phalanx base.
- Release Entrapment: Carefully excise or incise the membranous attachment of the volar plate to the metacarpal neck. The collateral ligaments may also be tightly stretched around the metacarpal head, forming a "buttonhole."
- Reduction: Once the entrapped structures are released, the joint can usually be reduced by longitudinal traction and gentle flexion.
- Stability Assessment: Test stability. Usually, the joint is stable after reduction, and no fixation is needed.
- Repair: Repair the incised volar plate or capsule if possible, ensuring it does not re-interpose.
3. Proximal Phalanx Condylar Fractures (MCP or PIP Joint)
These are challenging due to small fragment size and rotational instability.
- Approach: Dorsal or mid-axial, depending on fracture location (radial or ulnar condyle).
-
Procedure:
- Expose Fracture: Carefully dissect, protecting extensor mechanism and collateral ligaments.
- Fragment Reduction: Use small pointed reduction clamps, K-wire joysticks, or fine dental picks to anatomically reduce the condylar fragment. Rotational alignment is critical.
-
Fixation:
- Mini-screws: One or two 1.0 mm or 1.3 mm headless compression screws or standard cortical screws, inserted perpendicular to the fracture plane, provide excellent compression and rotational stability. Ensure screw heads are countersunk and do not protrude into the articular surface.
- K-wires: Transarticular K-wires may be used temporarily to maintain reduction while screws are placed. Definitive K-wire fixation can be used for very small fragments or where screw fixation is not feasible, often combined with a tension band wire.
- Transcondylar K-wires: For bicondylar fractures, two K-wires can be inserted from opposite sides across the fracture line, then across the joint to the opposite side of the adjacent phalanx (crossed K-wires).

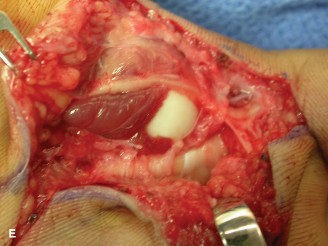
This image could depict a surgical view of a condylar fracture of the proximal phalanx, illustrating the delicate reduction with small instruments and subsequent fixation with mini-screws or K-wires. The precise alignment of articular fragments is paramount for successful outcome in such complex intra-articular injuries.
Soft Tissue Closure
- Capsule and Ligament Repair: Close joint capsule and repair any significant collateral ligament tears with non-absorbable sutures (e.g., 4-0 Ethibond or FiberWire).
- Tendon Repair: Repair any incised or damaged extensor tendons (e.g., central slip) using fine non-absorbable sutures (e.g., 4-0 Prolene or FiberWire) in a modified Kessler or Bunnell technique.
- Skin Closure: Close skin meticulously with fine sutures (e.g., 5-0 or 6-0 Nylon). Apply a sterile dressing and splint in a position of safety (MCP flexion, PIP extension).
Complications & Management
Despite meticulous surgical technique and comprehensive post-operative care, complications can arise following complex index finger joint injury management. Anticipation and prompt management are crucial for mitigating adverse outcomes.
Common Complications
-
Stiffness/Loss of Motion (Most Common):
- Incidence: Very high, especially with PIP joint injuries, prolonged immobilization, or severe intra-articular comminution. Can range from mild restriction to severe ankylosis.
- Etiology: Adhesions (tendinous, capsular, periarticular), articular incongruity, post-traumatic arthritis, prolonged edema, CRPS.
-
Management:
- Early & Aggressive Hand Therapy: Crucial for preventing and treating stiffness.
- Dynamic/Static Progressive Splinting: To regain lost range of motion (ROM).
- Manipulation Under Anesthesia (MUA): For dense adhesions or early capsular contracture, often followed by aggressive therapy.
- Surgical Arthrolysis: Open or arthroscopic release of adhesions and capsule contracture. Indicated after conservative measures fail, typically 3-6 months post-injury.
-
Post-Traumatic Arthritis:
- Incidence: High following intra-articular fractures, particularly those with residual articular step-off or incongruity.
- Etiology: Persistent articular surface damage, altered joint mechanics, chronic inflammation.
-
Management:
- Conservative: NSAIDs, corticosteroid injections, activity modification.
-
Surgical:
- Arthroplasty: For MCP joint, silicone or pyrolytic carbon implants. For PIP joint, less successful but can be considered in select cases.
- Arthrodesis: Fusion of the joint, providing a stable, painless, but immobile joint. Often the salvage procedure for severe, painful arthritis, especially for the PIP joint in functional positions.
-
Nonunion/Malunion:
- Incidence: Nonunion is less common in phalangeal fractures but can occur with inadequate fixation, poor vascularity, or infection. Malunion is more common, particularly rotational or angular deformities.
- Etiology: Insufficient reduction or fixation, bone loss, infection, poor healing potential.
-
Management:
- Nonunion: Revision osteosynthesis (re-fixation), potentially with bone grafting.
- Malunion: Corrective osteotomy and re-fixation, typically for symptomatic angular or rotational deformities that cause functional impairment (e.g., scissoring).
-
Hardware-Related Complications:
- Incidence: Common.
- Etiology: Prominent hardware causing soft tissue irritation, K-wire migration or breakage, screw loosening or breakage.
- Management: Symptomatic hardware removal after fracture union, typically 3-6 months post-surgery.
-
Infection:
- Incidence: Relatively low in elective hand surgery (<2%), but higher in open fractures or prolonged procedures.
- Etiology: Contamination during surgery, compromised soft tissue.
- Management: Debridement, irrigation, cultures, appropriate antibiotic therapy, potentially hardware removal if stable fracture union achieved.
-
Neurovascular Injury:
- Incidence: Rare but possible, particularly with complex dislocations, extensive dissection, or misplaced hardware.
- Etiology: Laceration, contusion, compression of digital nerves or arteries.
- Management: Immediate exploration and repair if identified intra-operatively. Observation for neurapraxia. Surgical neurolysis or nerve grafting for persistent deficits.
-
Complex Regional Pain Syndrome (CRPS) Type I:
- Incidence: Variable, but a known complication of upper extremity trauma and surgery.
- Etiology: Multifactorial, involving neuropathic, inflammatory, and psychological components.
- Management: Multidisciplinary approach: early recognition, aggressive physical therapy, pain management (NSAIDs, gabapentin, tricyclic antidepressants, regional blocks), psychological support.
-
Recurrent Instability/Dislocation:
- Incidence: Can occur with inadequate ligament repair, capsular laxity, or hardware failure.
- Management: Revision ligament reconstruction or capsulorrhaphy. In severe cases, arthrodesis may be considered.
-
Tendon Adhesion/Rupture:
- Incidence: Adhesions are common. Rupture is rarer.
- Etiology: Surgical trauma, prolonged inflammation, infection, prominent hardware.
- Management: Tenolysis for adhesions. Surgical repair/reconstruction for ruptures.
Table: Common Complications, Incidence, and Salvage Strategies
| Complication | Incidence | Salvage Strategies |
|---|---|---|
| Stiffness / Loss of Motion | High (especially PIP joint, 30-70%) | Intensive hand therapy, dynamic/static progressive splinting, manipulation under anesthesia (MUA), surgical arthrolysis (open or arthroscopic). |
| Post-Traumatic Arthritis | Moderate to High (15-50% in intra-articular) | Conservative management (NSAIDs, injections), activity modification, arthroplasty (MCP > PIP), arthrodesis (PIP preferred for stability/pain relief, also MCP if arthroplasty fails/contraindicated). |
| Nonunion / Malunion | Low (nonunion: <5%); Moderate (malunion: 5-20%) | Nonunion: Revision ORIF with bone grafting. Malunion: Corrective osteotomy with ORIF, especially for symptomatic rotational or angular deformity causing impingement or scissoring. |
| Hardware-Related Complications | High (often elective removal: 20-40%) | Symptomatic hardware removal (typically after fracture union, 3-6 months post-op). Revision fixation for hardware failure if fracture nonunion. |
| Infection | Low (<2% clean cases; higher in open injuries) | Debridement, irrigation, wound cultures, appropriate systemic antibiotics. Potential hardware removal, especially if stable union or non-critical to stability. |
| Neurovascular Injury | Low (<1%) | Immediate exploration and microsurgical repair (if observed intra-op). Post-op: observation, neurolysis, nerve grafting for persistent deficits. |
| Complex Regional Pain Syndrome (CRPS) Type I | Variable (5-15% after hand trauma/surgery) | Multidisciplinary approach: early physical/occupational therapy, pain management (pharmacologic, regional blocks), psychological support, sympathetic blocks. |
| Recurrent Instability / Dislocation | Low (5-10%) | Revision ligament repair/reconstruction (e.g., free tendon graft), capsulorrhaphy. In severe, recalcitrant cases, arthrodesis. |
| Tendon Adhesion / Rupture | Adhesions: Moderate (10-20%); Rupture: Low (<1%) | Adhesion: Intensive hand therapy, tenolysis (surgical release). Rupture: Primary repair (if acute), tendon graft reconstruction (if chronic defect), or tendon transfer. |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is as critical as the surgical procedure itself in achieving optimal functional outcomes for complex index finger joint injuries. The goal is to safely restore range of motion, strength, and dexterity while protecting the surgical repair. Protocols are individualized based on the specific injury, surgical technique, and stability of fixation.
General Principles
- Early Controlled Motion: For most stable fixations, early controlled active and passive range of motion is initiated to prevent stiffness and promote articular cartilage health.
- Protection of Repair: The intensity and type of exercises are carefully graded to protect healing bone, ligaments, and tendons.
- Edema Control: Crucial throughout the rehabilitation process to prevent stiffness and secondary complications.
- Pain Management: Adequate pain control facilitates active participation in therapy.
- Patient Education: Patients must understand the importance of adherence to the protocol and activity restrictions.
- Hand Therapist Involvement: Close collaboration with a specialized hand therapist is indispensable.
Phases of Rehabilitation
Phase 1: Immobilization/Protection Phase (Weeks 0-3/4)
- Goal: Protect the repair, reduce swelling, maintain adjacent joint motion.
-
Immobilization:
-
Splinting:
Typically a custom orthosis (thermoplastic splint) is fabricated immediately post-op.
- For MCP Joint Injuries: Usually immobilized with the MCP joint in 70-90 degrees of flexion and the PIP/DIP joints in full extension (position of safety) for approximately 3-4 weeks. This position minimizes collateral ligament contracture.
- For PIP Joint Injuries: Immobilized in 20-30 degrees of flexion. The specific splint design (e.g., dorsal blocking splint for volar plate repair, extension block splint for dorsal fracture-dislocation) will depend on the injury and stability of fixation.
- Buddy Taping: May be used to the adjacent middle finger for added protection while allowing some controlled motion in the uninjured fingers.
-
Splinting:
Typically a custom orthosis (thermoplastic splint) is fabricated immediately post-op.
-
Exercises:
- Edema Management: Elevation, gentle compression, retrograde massage.
- Active Range of Motion (AROM): For uninvolved joints (wrist, elbow, shoulder) and the DIP joint if the PIP is immobilized.
- Passive Range of Motion (PROM): For the injured joint, if indicated and deemed safe by the surgeon and therapist (e.g., controlled arc of motion within the splint).
- Light Gripping: Non-resistive squeezing of a soft sponge to maintain forearm muscle tone (avoiding torque on the injured finger).
- Weight Bearing: None on the affected finger.
- Wound Care: Maintain clean, dry dressings. Monitor for signs of infection.
Phase 2: Early Mobilization/Controlled Motion Phase (Weeks 3/4-8)
- Goal: Gradually increase joint range of motion, prevent adhesions, and improve soft tissue glide.
- Splinting: The static splint may be continued between exercise sessions. Dynamic or static-progressive splinting may be introduced to regain specific ranges of motion (e.g., extension block splint gradually increased for PIP flexion).
-
Exercises:
- AROM: Gradually increase active flexion and extension for the injured MCP or PIP joint within prescribed limits. Gentle place and hold exercises.
- PROM: Gentle passive stretching and joint mobilization performed by the therapist, respecting tissue healing limits.
- Tendon Gliding Exercises: To prevent adhesions of flexor and extensor tendons.
- Soft Tissue Mobilization: Scar massage to prevent scar tethering.
- Desensitization: If nerve irritation or hypersensitivity is present.
- Strength: Begin very light isometric exercises if appropriate.
- Function: Encourage light functional use within pain limits (e.g., buttoning a shirt).
Phase 3: Strengthening and Functional Integration Phase (Weeks 8-12+)
- Goal: Restore full range of motion, improve strength, endurance, and dexterity. Return to full activities.
- Splinting: Discontinue most splinting, except possibly for night-time wear if residual contracture exists.
-
Exercises:
- Progressive Strengthening: Isometric, then isotonic exercises using therapy putty, hand exercisers, and light weights. Focus on grip, pinch, and individual finger strength.
- Advanced ROM: Continue stretching and mobilization to achieve full functional range.
- Dexterity and Coordination: Fine motor activities, object manipulation, writing.
- Proprioceptive Exercises: Balance and coordination tasks.
-
Activity Progression:
- Gradual return to light occupational tasks and recreational activities.
- Sport-specific training, if applicable, typically not before 3-4 months post-op for contact sports or activities involving repetitive gripping.
- Hardware Removal: If hardware is prominent or causing symptoms, it may be removed after bone healing is confirmed (typically 3-6 months post-op), potentially followed by a brief period of therapy.
Specific Considerations for MCP vs. PIP Joint
- MCP Joint: Tends to be more forgiving with stiffness due to its greater inherent laxity. However, achieving full MCP flexion is crucial for power grip. The "position of safety" (MCP flexion, PIP/DIP extension) minimizes collateral ligament contracture and is often used for immobilization.
- PIP Joint: Extremely prone to stiffness. Early, controlled motion is paramount. Prolonged immobilization can quickly lead to irreversible contracture, particularly in extension. The rehabilitation is often more intensive and protracted for PIP injuries.
Summary of Key Literature / Guidelines
The management of complex index finger joint injuries continues to evolve, guided by advancements in surgical techniques, implant technology, and a deeper understanding of hand biomechanics. While no single universally accepted guideline covers all complex finger joint injuries, several key principles and literature insights underpin current best practices.
-
Anatomical Reduction and Stable Fixation for Intra-Articular Fractures:
The overwhelming consensus in the literature, supported by clinical studies and biomechanical research, emphasizes the critical importance of achieving anatomical reduction of articular surfaces and providing stable internal fixation for intra-articular fractures (e.g., condylar fractures, pilon fractures). Residual articular step-off exceeding 1-2 mm is consistently correlated with increased rates of post-traumatic arthritis and poor functional outcomes.
- References: Landmark studies by Belsky et al. (1984) and Hastings and Carroll (1988) on condylar fractures highlight the technical demands and need for precise fixation. Newer literature on headless compression screws and miniature plate systems has demonstrated improved stability and reduced implant prominence compared to older techniques.
-
Early Motion is Key (Especially for PIP Joint):
The PIP joint's propensity for stiffness is well-documented. Early controlled active range of motion, initiated as soon as surgical fixation allows, is consistently advocated to prevent capsular and ligamentous contracture and promote cartilage nutrition. This is often achieved through dynamic splinting or carefully monitored active exercise programs.
- References: Studies by Green and Rowland (2005) and Freeland and Latenser (2007) emphasize early protected motion protocols for PIP fracture-dislocations to mitigate stiffness while ensuring stability.
-
Management of Irreducible Dislocations:
The literature consistently supports open reduction for irreducible MCP and PIP dislocations. The common causes of irreducibility (e.g., volar plate interposition at the MCP, collateral ligament or volar plate incarceration at the PIP) necessitate direct surgical intervention to release the entrapped structures.
- References: Kaplan's classic description (1957) of the pathological anatomy of irreducible MCP dislocation remains foundational, informing current surgical approaches.
-
Role of Advanced Imaging:
The use of CT scans for complex intra-articular fractures is now standard of care, providing essential pre-operative detailed visualization of fracture patterns and comminution that plain radiographs cannot offer. MRI is valuable for soft tissue injuries (e.g., collateral ligaments, central slip avulsions) where clinical diagnosis is ambiguous or surgical planning requires specific detail.
- References: Multiple contemporary reviews on hand trauma imaging support the routine use of CT for complex articular fractures of the hand and wrist.
-
External Fixation for Severe Fracture-Dislocations:
For highly comminuted PIP joint fracture-dislocations, particularly pilon fractures with significant bone loss or soft tissue compromise, distraction external fixation (e.g., Suzuki frame, mini-hinged external fixators) combined with limited internal fixation can be a valuable tool. It maintains joint space, length, and provides stability via ligamentotaxis, facilitating early motion.
- References: Suzuki et al. (1994) described the technique of dynamic external fixation for PIP fracture-dislocations, which has been refined and widely adopted.
-
Salvage Procedures:
In cases of severe post-traumatic arthritis, chronic instability, or failed reconstruction, the literature supports arthrodesis (fusion) as a reliable salvage procedure for the index finger joints, particularly the PIP joint, to provide a stable, pain-free digit in a functional position. Arthroplasty (joint replacement) can be considered for the MCP joint in select patients with low demands, but outcomes for PIP arthroplasty are generally less predictable.
- References: Various long-term outcome studies on arthrodesis versus arthroplasty for finger joint arthritis provide evidence for these distinct indications.
In summary, the literature underscores that successful management of complex index finger joint injuries hinges on a precise pre-operative assessment (including advanced imaging), an individualized surgical plan to achieve anatomical reduction and stable fixation, meticulous surgical technique, and an aggressive yet protective post-operative rehabilitation protocol. The choice between various surgical and non-surgical modalities is dictated by the specific injury pattern, patient factors, and the surgeon's experience, always aiming to restore the intricate balance of stability and mobility essential for optimal hand function.
Clinical & Radiographic Imaging
You Might Also Like
