Ring Finger Fracture Management: CRPP Techniques, Surgical Anatomy & Biomechanics
Key Takeaway
Closed Reduction and Percutaneous Pin Fixation (CRPP) is a minimally invasive treatment for unstable or displaced ring finger fractures, including metacarpal and phalangeal types. It preserves soft tissue, reduces surgical time, and often allows earlier mobilization than open surgery. Success depends on meticulous technique, accurate reduction, and stable pin placement, critical for preserving hand function and preventing malunion.
Introduction & Epidemiology
Fractures of the ring finger, encompassing both metacarpal and phalangeal bones, are a common presentation in orthopedic trauma. These injuries often result from direct impact, crushing forces, or axial loading, frequently observed in athletic activities, industrial accidents, and altercations. While any digit can be affected, the ring finger, particularly its metacarpal, is statistically among the most frequently injured in the hand, often secondary to a "boxer's fracture" mechanism involving the metacarpal neck. Phalangeal fractures of the ring finger can occur at the proximal, middle, or distal phalanx, impacting articular surfaces or the shaft.
The functional significance of the ring finger within the hand's kinetic chain necessitates precise anatomical reduction and stable fixation to preserve grip strength, dexterity, and overall hand function. Malunion, particularly rotational malalignment or excessive angulation, can lead to significant functional impairment, including scissoring deformities, decreased range of motion, and persistent pain.
Closed reduction and percutaneous pin fixation (CRPP) is a widely utilized and effective treatment modality for unstable, irreducible, or significantly displaced ring finger fractures that do not warrant open reduction and internal fixation (ORIF). CRPP offers the advantages of being minimally invasive, preserving soft tissue integrity, reducing surgical time, and often allowing for earlier mobilization compared to more extensive open approaches. However, its success is contingent upon meticulous surgical technique, accurate reduction, stable pin placement, and appropriate post-operative management. This review aims to provide an exhaustive, high-yield guide for orthopedic surgeons, residents, and medical students on the insights into reduction and percutaneous pin treatment of ring finger fractures.
Surgical Anatomy & Biomechanics
A thorough understanding of the anatomical and biomechanical nuances of the ring finger is paramount for successful fracture management.
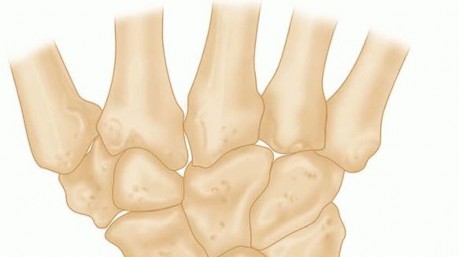
Metacarpals
The fourth (ring) metacarpal articulates proximally with the capitate and hamate, forming the carpometacarpal (CMC) joint. This joint allows for limited motion, primarily flexion/extension and some rotation, which contributes to the hand's arching and grip capabilities. The base of the fourth metacarpal has distinct facets for articulation with the hamate and a small facet for the third metacarpal. The shaft is triangular in cross-section proximally and cylindrical distally. The neck is the narrowest part, just proximal to the head, and is a common site for fractures due to its stress concentration. The metacarpal head is convex and articulates with the concave base of the proximal phalanx, forming the metacarpophalangeal (MCP) joint.
Key Biomechanical Considerations for Metacarpal Fractures:
*
Dorsal Angulation
: Metacarpal neck fractures typically result in apex-dorsal angulation due to the pull of the intrinsic muscles (interossei) and the flexor digitorum profundus (FDP) and superficialis (FDS) tendons causing volar displacement of the distal fragment.
*
Rotational Stability
: The intrinsic muscles (dorsal and palmar interossei) insert onto the proximal phalanges and the extensor hood, influencing both flexion and extension, and playing a critical role in rotational stability. Rotational malalignment of the fourth metacarpal can lead to "scissoring" of the digits when making a fist.
*
Extensor Hood Mechanism
: The extensor digitorum communis tendon overlies the metacarpal neck and head, stabilized by the sagittal bands, which can sometimes interfere with closed reduction.
Phalanges
The ring finger comprises three phalanges: proximal, middle, and distal.
*
Proximal Phalanx
: Articulates with the metacarpal head proximally (MCP joint) and the middle phalanx distally (proximal interphalangeal, PIP, joint). Its shaft is generally rectangular.
*
Middle Phalanx
: Articulates with the proximal phalanx proximally (PIP joint) and the distal phalanx distally (distal interphalangeal, DIP, joint). The FDS tendon inserts on its base.
*
Distal Phalanx
: Articulates with the middle phalanx proximally (DIP joint) and terminates distally as the ungual tuberosity. The FDP tendon inserts on its base, and the terminal extensor tendon (part of the extensor mechanism) inserts on its dorsal base.
Key Biomechanical Considerations for Phalangeal Fractures:
*
Tendon Forces
:
*
Proximal Phalanx Fractures
: The intrinsic muscles (interossei and lumbricals) exert a deforming force, causing apex-volar angulation in shaft fractures, as they insert on the proximal phalanx. The FDS and FDP tendons exert a flexor moment.
*
Middle Phalanx Fractures
: Fractures proximal to the FDS insertion (proximal 2/3) typically result in apex-dorsal angulation due to the unopposed pull of the central slip of the extensor mechanism. Fractures distal to the FDS insertion (distal 1/3) often result in apex-volar angulation due to the FDP pulling the distal fragment volarly.
*
Distal Phalanx Fractures
: Primarily impacted by the FDP and terminal extensor tendons. Mallet finger deformity can result from terminal extensor avulsion fractures.
*
Ligamentous Stability
: Collateral ligaments (radial and ulnar) at the MCP, PIP, and DIP joints provide critical mediolateral stability. The volar plates at the MCP, PIP, and DIP joints prevent hyperextension and provide stability. Articular fractures involving these structures can lead to joint instability.
*
Rotational Deformity
: Even minor rotational malalignment in phalangeal fractures can lead to significant functional impairment, as it affects the cascade of finger flexion and can cause digit overlap (scissoring). This is critical to assess during reduction.
Indications & Contraindications
The decision between operative and non-operative management, particularly concerning the use of CRPP for ring finger fractures, depends on a careful evaluation of fracture characteristics, patient factors, and surgeon expertise.
Operative Indications (CRPP Focus)
Percutaneous pinning is primarily indicated for closed, unstable fractures that can be anatomically reduced by closed means.
-
Unstable Fractures
:
- Irreducible by Closed Means : Despite adequate analgesia and manipulation, the fracture cannot be reduced to an acceptable alignment.
- Tendency to Displace After Reduction : Fractures that reduce well but redisplace immediately or soon after reduction once external forces are removed (e.g., due to strong muscle pull or fracture morphology).
-
Significant Angulation (after closed reduction attempts)
:
- Metacarpal Neck/Shaft : Persistent dorsal angulation typically exceeding 30-40 degrees for the fourth metacarpal. Greater angulation is often tolerated in the fourth and fifth metacarpals compared to the second and third due to inherent CMC joint mobility.
- Phalangeal Shaft : Persistent angulation exceeding 10-20 degrees in the proximal or middle phalanges. Articular step-off or gapping >1mm.
- Rotational Malalignment : Any clinically significant rotational deformity (e.g., scissoring or crossover of digits upon fist formation) is an absolute indication for operative intervention, as even minor rotational malunion can cause severe functional deficit.
- Shortening : Metacarpal shortening greater than 2-3 mm, particularly if accompanied by angulation or malrotation. Significant shortening of a phalanx can disrupt extensor and flexor tendon mechanics.
- Comminuted Fractures : While comminution often favors ORIF, some patterns, particularly those with a large, reducible main fragment and smaller comminuted pieces, can be stabilized with judicious pinning.
- Open Fractures : After thorough debridement and irrigation, unstable open fractures can be stabilized with percutaneous pins, often as a temporary measure or definitive fixation depending on soft tissue status.
- Articular Fractures : Select intra-articular fractures (e.g., small, displaced volar plate avulsion fractures of the PIP joint, or minimally comminuted base fractures) that can be anatomically reduced closed and require stabilization.
Contraindications
While CRPP is versatile, certain situations contraindicate its use or favor alternative methods.
-
Absolute Contraindications :
- Gross Contamination/Infection : Active infection in the surgical field (relative, open debridement first).
- Severe Comminution Preventing Stable Reduction : If closed reduction cannot achieve a stable, anatomic alignment due to extensive comminution, CRPP will likely fail. This typically necessitates ORIF.
- Non-Reducible Articular Fractures : Intra-articular fractures with significant displacement, step-off, or impaction that cannot be anatomically reduced by closed manipulation. These require direct visualization for reduction and fixation.
- Significant Soft Tissue Loss/Damage : Compromised soft tissues or extensive open wounds might preclude pin placement or increase infection risk.
-
Relative Contraindications :
- Patient Factors : Poor bone quality (severe osteoporosis) might lead to poor pin purchase. Uncooperative patient or inability to comply with post-operative care.
- Surgeon Experience : Inexperienced surgeons might opt for ORIF in complex cases to ensure anatomical reduction and fixation, as CRPP requires skill in closed reduction maneuvers and fluoroscopic interpretation.
Table: Operative vs. Non-Operative Indications
| Indication Category | Operative Management (CRPP Recommended) | Non-Operative Management (Conservative) |
|---|---|---|
| Fracture Stability | Unstable (tends to redisplace after reduction), irreducible closed fractures. | Stable, minimally displaced fractures that maintain acceptable alignment after closed reduction (if needed) without fixation. |
| Angulation (Post-Reduction) | Metacarpal Neck/Shaft : >30-40 degrees (4th MC). Phalangeal Shaft : >10-20 degrees (proximal/middle phalanx). Articular : Any intra-articular step-off or gapping >1mm that is reducible. | Metacarpal Neck/Shaft : <30-40 degrees (4th MC), or acceptable based on patient age/activity. Phalangeal Shaft : <10-20 degrees. Minimally displaced articular fractures without functional impairment. |
| Rotational Malalignment | Any clinically significant rotational malalignment (e.g., scissoring upon fist formation). | No rotational malalignment. |
| Shortening | >2-3 mm of shortening, especially if combined with angulation or malrotation. | <2-3 mm of shortening, without significant functional impact. |
| Open Fractures | All open fractures (after appropriate debridement and irrigation) to stabilize the skeletal injury. | Not applicable for open fractures. |
| Comminution | Select comminuted patterns where a stable, anatomical reduction can be achieved closed. | Grossly comminuted fractures where stable reduction is impossible with CRPP (often requiring ORIF). |
| Patient Factors | High functional demand, professional athletes, patients requiring early return to specific activities, non-compliance with conservative treatment (relative indication). | Low functional demand, elderly patients with significant comorbidities where surgery poses greater risk, compliant patients capable of protecting the injury. |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is crucial to optimize surgical outcomes and minimize complications.
Pre-Operative Planning
-
Clinical Assessment
:
- Thorough history taking, including mechanism of injury, hand dominance, occupation, and functional demands.
- Neurovascular examination: Assess sensation, motor function, and capillary refill to rule out nerve or vascular injury. Note any open wounds or signs of compartment syndrome.
- Soft tissue envelope assessment: Note swelling, ecchymosis, and skin integrity. Significant swelling may delay surgery or necessitate staged procedures.
- Rotational assessment: Carefully evaluate for rotational deformity by asking the patient to make a gentle fist, observing the convergence of fingertips to the scaphoid tubercle and any scissoring of the injured digit relative to adjacent digits.
-
Radiographic Evaluation
:
-
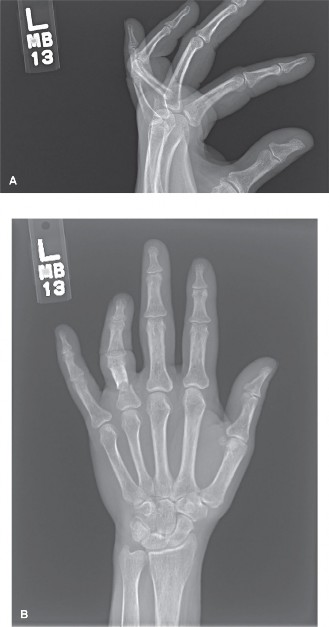
Standard Views
: Obtain high-quality posteroanterior (PA), lateral, and oblique radiographs of the hand or affected digit.
- PA View : Assesses shortening, angulation in the coronal plane, and transverse displacement.
- Lateral View : Crucial for assessing angulation in the sagittal plane (dorsal/volar angulation). For metacarpals, a true lateral may require individual digit views. For phalanges, a true lateral of the affected digit is essential to assess angulation relative to its articulation.
- Oblique Views : Provide additional information about fracture configuration, especially for spiral or oblique patterns.
- Special Views : For complex articular fractures or when comminution obscures visualization, a fine-cut Computed Tomography (CT) scan may be beneficial to delineate fracture lines, joint involvement, and articular step-off. This is particularly useful for PIP joint fractures.
-
Standard Views
: Obtain high-quality posteroanterior (PA), lateral, and oblique radiographs of the hand or affected digit.
-
Hardware Selection
:
- K-wires : Most commonly, 0.035-inch (0.9 mm) or 0.045-inch (1.1 mm) K-wires are used. Thinner wires are used for phalanges and children, while thicker wires may be necessary for larger metacarpals or to provide greater stability. Select appropriate length K-wires.
- Tools : Power drill with slow speed, K-wire cutters, needle holders for bending wires.
-
Anesthesia
:
- Regional anesthesia (e.g., axillary block, supraclavicular block) is often preferred, providing good intraoperative analgesia and post-operative pain control without systemic side effects.
- General anesthesia may be chosen for patient preference, prolonged cases, or when regional block is contraindicated.
- A Bier block (intravenous regional anesthesia) can also be used for shorter procedures.
- Tourniquet : A pneumatic tourniquet applied to the upper arm or forearm is essential to maintain a bloodless field, which significantly aids in visualization and precise pin placement. The tourniquet time should be monitored.
Patient Positioning
- Setup : The patient is positioned supine on the operating table.
- Arm Position : The affected arm is abducted on a specialized hand table, providing stable support and easy access for the surgical team and fluoroscopy unit.
- Draping : The hand and forearm are sterilely prepped and draped, isolating the surgical field while allowing adequate exposure for fluoroscopy. Ensure that the C-arm can be positioned for both AP and true lateral views of the affected digit without contamination.
- Fluoroscopy : The image intensifier (C-arm) should be readily available and positioned to allow for immediate intraoperative radiographic assessment in multiple planes (AP, lateral, oblique). This facilitates accurate reduction and confirmation of pin placement.
Detailed Surgical Approach / Technique
The goal of CRPP is to achieve and maintain an anatomical reduction with minimal soft tissue disruption. This requires precise reduction maneuvers and meticulous K-wire placement under fluoroscopic guidance.
1. Anesthesia and Preparation
- Administer chosen anesthetic.
- Inflate tourniquet to appropriate pressure (e.g., 250 mmHg for normotensive adults).
- Perform thorough antiseptic skin preparation (e.g., povidone-iodine or chlorhexidine) from the elbow to the fingertips.
- Drape the hand and forearm sterilely, exposing the surgical site and allowing for fluoroscopy.
2. Reduction Maneuvers
The specific maneuver depends on the fracture location and deformity. Intraoperative fluoroscopy is indispensable for confirming reduction.
Metacarpal Neck/Shaft Fractures (Boxer's Fracture type)
-
Traction and Flexion
: Apply longitudinal traction to the affected digit. For metacarpal neck fractures, the
Jahss maneuver
is classic:
- Flex the MCP joint to 90 degrees.
- Apply direct volar pressure over the dorsal apex of the fracture fragment (the metacarpal head).
- Simultaneously apply axial pressure to the flexed proximal phalanx to "cup" the metacarpal head and push it dorsally. This maneuver uses the proximal phalanx as a lever.
- Direct Manipulation : For shaft fractures, direct manipulation of the fracture fragments with digital pressure can assist reduction.
- Rotational Assessment : Crucially, after preliminary reduction, flex all fingers simultaneously to observe the "cascade." The fingertips should converge towards the scaphoid tubercle without scissoring or crossing. Any malrotation needs immediate correction.
- Fluoroscopic Confirmation : Obtain AP and true lateral views to confirm satisfactory reduction in terms of angulation, shortening, and translation.
Phalangeal Fractures
- Traction and Counter-Traction : Apply longitudinal traction to the digit with counter-traction at the wrist or palm.
-
Specific Angulation Correction
:
- Proximal Phalanx Shaft : Often apex-volar angulation. Apply dorsal pressure to the apex of the fracture and maintain traction.
- Middle Phalanx Shaft : If apex-dorsal (proximal to FDS insertion), apply volar pressure to the apex. If apex-volar (distal to FDS insertion), apply dorsal pressure to the apex.
- Rotational Assessment : Absolutely critical. Flex all digits to assess the cascade. The nail beds should be in the same plane.
- Fluoroscopic Confirmation : AP and true lateral views are mandatory. A perfect lateral view of the phalanx is essential to visualize true sagittal angulation.
3. Percutaneous Pin Fixation (K-wire Placement)
Once an anatomical reduction is achieved and confirmed fluoroscopically, pins are inserted to maintain stability. The number, diameter, and configuration of pins depend on the fracture pattern and surgeon preference.
Metacarpal Fractures
-
Retrograde Intramedullary Pinning (Most Common)
:
- Maintain reduction.
- Insert a 0.035" or 0.045" K-wire dorsally through the metacarpal head, just distal to the fracture site, aiming proximally. Start just lateral or medial to the extensor tendon to avoid direct impingement.
- Advance the wire under fluoroscopic guidance across the fracture site, into the medullary canal of the proximal fragment.
- The wire should achieve bicortical purchase in the proximal fragment for optimal stability but avoid exiting the bone proximally into the carpus if possible. If a long wire is needed, it can be cut flush with the skin or bent and buried.
- Typically, two crossed K-wires provide good rotational and angular stability. The second wire is inserted similarly, often from the opposite side of the metacarpal head, crossing the first wire within the medullary canal or parallel in a different trajectory.
- Ensure pins do not interfere with adjacent digits or tendons.
-
Trans-Metacarpal Pinning (for severe instability or comminution)
:
- One or two K-wires are inserted from the injured metacarpal across the intermetacarpal space into a stable adjacent metacarpal (e.g., from 4th to 3rd metacarpal).
- This provides robust stability but restricts motion of the adjacent digit. Pins are typically placed more proximally in the metacarpal shaft.
- Antegrade Pinning (less common for neck fractures) : Wires are inserted through the metacarpal base proximally and advanced distally across the fracture. This may be used for more distal shaft fractures or certain base fractures.

Figure 1: Intraoperative fluoroscopic image demonstrating percutaneous K-wire fixation for an unstable metacarpal neck fracture of the ring finger. Note the two crossed K-wires providing stability after closed reduction.
Phalangeal Fractures
-
Longitudinal Intramedullary Pinning
:
- Most commonly used for transverse or short oblique shaft fractures.
- Insert a K-wire (e.g., 0.035") from the tip of the affected finger (distal phalanx or fingertip if fracture is more distal) or through the fracture site.
- Advance the pin across the fracture into the medullary canal of the proximal fragment. Aim for bicortical purchase.
- Ensure the pin does not cross the PIP or DIP joint if possible, unless the joint itself is unstable or part of the fracture pattern (e.g., volar plate avulsion).
-
Crossed K-wires
:
- Similar to metacarpals, two K-wires are inserted obliquely, one from each side of the fractured segment, crossing at the fracture site.
- Effective for oblique or spiral fractures, or those with significant rotational instability. Entry points should be carefully selected to avoid neurovascular bundles.
-
Dorsal Blocking Pins (for volar plate avulsion fractures of PIP joint)
:
- Small articular fragments, particularly those involving the volar plate at the PIP joint, can be reduced and held with a small K-wire (e.g., 0.028" or 0.035") inserted across the PIP joint to block hyperextension, allowing the volar plate to heal. The PIP joint is typically held in 20-30 degrees of flexion.
-
Pin Insertion Technique
:
- Use a power drill at a slow speed to prevent thermal necrosis of bone.
- Advance wires steadily under fluoroscopic visualization in both AP and lateral planes.
- Ensure bicortical purchase in at least one fragment for stability.
- Check rotational alignment again with a full finger cascade after pin insertion.
- Cut pins leaving 5-10 mm protruding from the skin or bend them 90 degrees and cut flush to the skin. This facilitates removal and reduces irritation. The choice depends on surgeon preference and expected pin removal timeline.
4. Post-Fixation Assessment
- Fluoroscopy : Re-evaluate fracture reduction in AP, lateral, and oblique views. Confirm pin position, length, and stability.
- Clinical Assessment : Release tourniquet. Check capillary refill and sensation. Re-assess active range of motion of uninvolved digits. Re-check the digital cascade for rotational alignment.
5. Dressing and Splinting
- Apply sterile dressings around the pin exit sites (e.g., with petrolatum gauze) to minimize infection risk.
- Apply a sterile bulky dressing.
- Immobilize the hand and digits in an intrinsic plus position (MCPs flexed 70-90 degrees, IPs extended) with a dorsal or volar splint, molded to maintain the reduction and protect the pins. For metacarpal fractures, the wrist is often included. For phalangeal fractures, the splint may be limited to the affected digit and adjacent digits (buddy taping).
- Provide appropriate instructions for pin site care and warning signs of infection.
Complications & Management
While generally safe and effective, percutaneous pinning is associated with potential complications, which orthopedic surgeons must recognize and manage.
| Complication | Incidence (Approx.) | Management / Salvage Strategy |
|---|---|---|
| Malunion (Angulation, Rotation, Shortening) | 10-20% (variable) | Mild (functional/cosmetic deficit) : Observation, hand therapy, patient education. Moderate to Severe (functional impairment, scissoring) : Corrective osteotomy (often after fracture healing) with internal fixation, followed by rehabilitation. Prevention is key: meticulous reduction and stable fixation. |
| Nonunion | <5% | Early (asymptomatic) : Extended immobilization, bone stimulator. Established (symptomatic, persistent gap) : Surgical intervention – debridement of fibrous tissue, bone grafting (autograft or allograft), revision internal fixation (plates, screws, IM nails). |
| Pin Tract Infection | 5-10% | Superficial (localized erythema, minor discharge) : Pin site care, local antibiotics (topical/oral). Deep (cellulitis, abscess, osteomyelitis) : Pin removal, IV antibiotics (culture-directed), surgical debridement if abscess or osteomyelitis. |
| Tendon Adhesions / Stiffness | Common (variable, often minor) | Prevention : Early controlled range of motion (if stability allows), appropriate splinting. Management : Aggressive hand therapy (active and passive ROM, scar massage), dynamic splinting. Refractory : Tenolysis, capsulectomy. |
| Nerve Injury (Digital Nerves) | Rare (<1%) | Mild (neuropraxia) : Observation, serial neurological exams. Severe (axonotmesis, neurotmesis) : Exploration, neurolysis, or nerve repair/grafting if transection suspected. Prevention: careful pin placement, awareness of neurovascular bundles. |
| Vascular Injury | Very Rare | Minor (hematoma) : Observation. Significant (ischemia) : Urgent exploration, vascular repair. |
| Hardware Failure / Migration | <5% | Migration (non-threatening) : Observation, early pin removal if healed. Migration (threatening structures, loss of reduction) : Pin removal, re-reduction, re-pinning or alternative fixation. Breakage : Pin removal (may require open approach for retained fragments). |
| Refracture | Rare | After pin removal : Re-reduction and re-fixation (often with more stable ORIF), extended immobilization. During fixation : Re-evaluation of stability, revision fixation. |
| Complex Regional Pain Syndrome (CRPS) | <5% | Prevention : Early recognition, adequate pain control, gentle mobilization, psychological support. Management : Multimodal approach – physical/occupational therapy, pain medications (neuropathic agents, NSAIDs), sympathetic nerve blocks, psychological counseling. |
| Prominent Hardware / Pin Irritation | Common | Local discomfort : Conservative management (padding). Significant irritation : Early pin removal once fracture is stable. |
| Growth Plate Arrest (in children) | Rare | Prevention : Careful pin placement avoiding physes in pediatric patients. Management : Dependent on skeletal maturity and severity of growth arrest (e.g., epiphysiodesis of contralateral limb to equalize length, or limb lengthening). |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is integral to optimizing functional outcomes after CRPP of ring finger fractures. Protocols are tailored based on fracture stability, specific digit involved, pin configuration, and surgeon preference. The general principles aim to protect the fracture fixation while initiating controlled motion to prevent stiffness.
Phase 1: Immobilization and Early Protection (0-3/4 weeks)
- Goals : Maintain fracture reduction, protect fixation, minimize edema, prevent stiffness in uninvolved joints.
-
Immobilization
:
- The hand is typically immobilized in a custom-molded splint (dorsal or volar), maintaining the intrinsic plus position (MCPs 70-90° flexion, IPs near full extension) for metacarpal fractures.
- For phalangeal fractures, the splint may be molded to the affected digit and potentially buddy-taped to an adjacent stable digit.
- Splint removal is strictly for hygiene and pin site care, performed by the patient or caregiver as instructed.
-
Edema Management
:
- Elevation of the hand above heart level (e.g., resting on pillows).
- Gentle, active range of motion (AROM) of uninvolved joints (shoulder, elbow, wrist, thumb, and adjacent uninvolved fingers) to promote circulation and reduce swelling.
- Pin Site Care : Daily cleaning of pin entry sites with sterile saline or antiseptic solution as instructed to prevent infection. Observe for signs of infection (redness, swelling, pus).
- Patient Education : Instruct on warning signs of infection, loss of sensation, increased pain, or splint issues. Emphasize activity modification and avoidance of heavy lifting or grasping.
- Radiographic Follow-up : Weekly or bi-weekly radiographs (AP/lateral) to monitor fracture healing and maintenance of reduction.
Phase 2: Pin Removal and Progressive Mobilization (3/4 - 6 weeks)
- Goals : Initiate gentle controlled motion of the injured digit, improve range of motion, and begin strengthening.
-
Pin Removal
:
- Typically, K-wires are removed between 3 to 6 weeks post-operatively, once radiographic signs of early union are visible (e.g., bridging callus). The exact timing depends on the fracture pattern and perceived stability.
- Pin removal is usually performed in an outpatient setting without anesthesia, often with local anesthetic if desired.
-
Post-Pin Removal Mobilization
:
- Controlled AROM/PROM : Immediately after pin removal, begin gentle active and passive range of motion exercises for the affected MCP and IP joints.
- Buddy Taping : Continue buddy taping the injured finger to an adjacent digit to provide dynamic support and prevent scissoring or rotational forces during early movement.
- Splinting : A protective removable splint may be continued between exercise sessions, especially at night, for another 2-3 weeks to prevent re-injury during sleep.
- Edema and Scar Management : Continue edema control. Begin scar massage and desensitization if surgical incisions were made or pin tracts are tender.
- Therapist Involvement : Referral to a certified hand therapist (CHT) is highly recommended at this stage for guided, progressive rehabilitation. The CHT can implement specific exercises, joint mobilization techniques, and fabricate dynamic splints if needed.
Phase 3: Strengthening and Functional Integration (6-12+ weeks)
- Goals : Restore full range of motion, improve grip and pinch strength, achieve full functional use of the hand.
-
Progressive Strengthening
:
- Once pain-free range of motion is well-established, gradually introduce strengthening exercises using putty, resistance bands, and light weights.
- Focus on both intrinsic and extrinsic muscle groups of the hand and forearm.
- Advanced ROM : Continue with more vigorous AROM and PROM exercises, focusing on any lingering deficits. Joint mobilization techniques by the therapist may be employed.
- Functional Activities : Incorporate task-specific exercises relevant to the patient's occupation, hobbies, or sports.
-
Return to Activity
:
- Gradual return to light duty work or activities.
- Full return to demanding activities, contact sports, or heavy labor is typically allowed once full strength and pain-free range of motion are achieved, and radiographic healing is complete (often 10-12+ weeks, but varies).
- Long-Term Follow-up : Monitor for potential complications such as stiffness, pain, or signs of malunion or nonunion. Continued exercises may be necessary for several months.
Throughout all phases, patient compliance and close communication between the surgeon and hand therapist are critical for successful outcomes.
Summary of Key Literature / Guidelines
Closed reduction and percutaneous pinning (CRPP) remains a cornerstone in the management of unstable metacarpal and phalangeal fractures of the ring finger. Its effectiveness is well-documented in the orthopedic literature, supported by decades of clinical experience and numerous studies.
- Early Pioneers : The principles of hand fracture management, including the importance of anatomical reduction and stable fixation, were established by early hand surgeons. Classic techniques, such as the Jahss maneuver for metacarpal neck fractures, highlight the ingenuity in achieving closed reduction.
- Metacarpal Fractures : For unstable metacarpal neck and shaft fractures, particularly of the fourth and fifth metacarpals, CRPP is a preferred method due to its minimally invasive nature and ability to achieve satisfactory stability. Studies by London (1961) , Jahss (1938) , and later comprehensive reviews (e.g., Belsky et al., 1984; Foucher et al., 2005 ) have emphasized acceptable functional outcomes with CRPP, provided strict criteria for reduction and stable fixation are met. The tolerable angulation for the ring metacarpal (up to 30-40 degrees dorsally) is higher than for the central metacarpals due to the inherent mobility of the 4th and 5th carpometacarpal joints, a concept crucial for guiding treatment decisions. However, rotational malalignment is consistently highlighted as intolerable.
- Phalangeal Fractures : For unstable phalangeal shaft fractures (proximal and middle phalanx), CRPP is effective in maintaining reduction and preventing rotational deformities. Eaton (1970s) and Bilos and Herman (1974) contributed significantly to understanding the biomechanics and management of these fractures. The critical consideration in phalangeal fractures is the prevention of stiffness and tendon adhesions, which can be mitigated by careful pin placement to avoid crossing joint lines unnecessarily and facilitating early, controlled mobilization. For intra-articular fractures (e.g., volar plate avulsions), small K-wires can be used as blocking pins or for direct fragment fixation to restore joint congruity and stability, as described by Weiss et al. (2000) .
-
Advantages of CRPP
:
- Minimally Invasive : Reduced soft tissue dissection, theoretically lower risk of infection compared to ORIF, less scar formation.
- Preservation of Vascularity : Maintains blood supply to fragments, which is critical for healing.
- Shorter Operative Time : Often quicker than ORIF.
- Cost-Effective : Generally less expensive than plate and screw fixation.
-
Limitations and Considerations
:
- Dependence on Closed Reduction : Requires a fracture to be amenable to closed reduction. Irreducible fractures or those with interposed soft tissue may require ORIF.
- Risk of Pin Tract Infection : While generally low, this remains a concern.
- Pin Complications : Pin loosening, migration, or breakage.
- Less Rigid Fixation : Compared to plate and screw fixation, K-wires provide less rigid stability, often necessitating post-operative immobilization and potentially delaying early aggressive rehabilitation.
- Current Guidelines and Trends : Modern hand surgery emphasizes early mobilization where possible to prevent stiffness. While plate and screw fixation provides more rigid stability and facilitates immediate motion, CRPP remains the gold standard for many unstable fractures, particularly when comminution or soft tissue compromise makes ORIF less desirable, or when the fracture pattern is simple and amenable to percutaneous techniques. The choice between CRPP and ORIF is increasingly dictated by fracture stability after reduction, patient factors, and the surgeon's experience. The American Society for Surgery of the Hand (ASSH) and American Academy of Orthopaedic Surgeons (AAOS) guidelines generally support CRPP for suitable fracture patterns, emphasizing restoration of length, alignment, and rotation.
In conclusion, CRPP is a valuable and frequently employed technique for ring finger fractures. Its success hinges on a profound understanding of hand anatomy and biomechanics, meticulous surgical execution, and diligent post-operative care. While not without potential complications, when appropriately indicated and performed, CRPP yields excellent functional outcomes, allowing patients to regain the critical dexterity and strength of their dominant hand. Continued refinement of techniques and careful patient selection remain paramount.
You Might Also Like