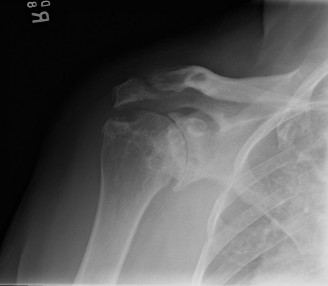
Complex Intra-Articular Distal Radius Fracture: Case Study of Failed Volar Tilt Restoration
Key Takeaway
Failed closed reduction of an intra-articular distal radius fracture manifests as persistent dorsal angulation, inadequate volar tilt restoration, and articular step-off on post-reduction imaging. These issues confirm insufficient anatomical alignment, necessitating operative intervention for optimal functional outcomes and to prevent complications.
Patient Presentation & History
A 58-year-old right-hand dominant female presented to the emergency department following a fall from standing height onto an outstretched right hand (FOOSH). The mechanism was low-energy, occurring while stepping off a curb. She reported immediate, severe pain, swelling, and deformity in her right wrist, rendering it unusable. There was no associated loss of consciousness, head trauma, or other injuries.
Her past medical history is significant for well-controlled Type 2 Diabetes Mellitus managed with Metformin and essential hypertension managed with Amlodipine. She has no known allergies. Surgical history includes an uncomplicated appendectomy 20 years prior. She is a non-smoker and denies regular alcohol consumption. She lives independently and is actively employed in an administrative role requiring proficient right-hand function for computer work. She reports no prior injuries or surgeries to either wrist.
Upon initial assessment in the emergency department, closed reduction was attempted under procedural sedation (conscious sedation with midazolam and fentanyl) using sustained manual traction and direct manipulation. Despite initial temporary improvement in gross alignment, subsequent post-reduction radiographs demonstrated persistent dorsal angulation and inadequate restoration of volar tilt, specifically measured at -12 degrees (dorsal angulation), with an articular step-off of 3mm. The patient experienced significant pain during the procedure, and a second attempt was deemed unlikely to yield superior results without formal anesthesia. Given the persistent deformity and articular incongruity, the decision for operative intervention was made.
Clinical Examination
Upon presentation, the patient was alert and oriented, in acute distress secondary to pain.
Inspection: Gross "dinner fork" deformity was evident on the radial aspect of the right wrist, consistent with dorsal displacement of the distal radius fragment. Significant soft tissue swelling was present around the wrist and distal forearm, extending into the hand. Ecchymosis was noted volarly and dorsally. The skin envelope was intact, without evidence of open wounds, blistering, or tenting. The digits were well perfused, and her nail beds were pink with brisk capillary refill.
Palpation: Marked tenderness was elicited over the distal radius and radiocarpal joint. Palpable crepitus was present with any attempt at wrist motion. The radial pulse was strong and readily palpable; the ulnar pulse was also present. Sensation to light touch was intact across all dermatomes (median, ulnar, and radial nerve distributions). The ulnar styloid was tender to palpation, indicating a possible concomitant fracture. There was no evidence of acute compartment syndrome, with soft, compressible muscle compartments and no pain out of proportion to injury.
Range of Motion (ROM): Active and passive range of motion of the wrist was severely limited due to pain and gross instability. Finger flexion and extension were full, though painful, with good grip strength noted for a brief squeeze, indicating intact long flexor and extensor tendons. Elbow and shoulder ROM were full and pain-free.
Neurological Assessment:
*
Median Nerve:
Sensation intact in the thumb, index, middle, and radial half of the ring finger. Motor function: thumb opposition (Opponens Pollicis) and abduction (Abductor Pollicis Brevis) were intact against resistance. FPL strength was 5/5.
*
Ulnar Nerve:
Sensation intact in the little finger and ulnar half of the ring finger. Motor function: finger abduction/adduction (Dorsal/Palmar Interossei) and little finger abduction (Abductor Digiti Minimi) were intact against resistance.
*
Radial Nerve:
Sensation intact in the dorsal first web space. Motor function: wrist extension (ECRL/ECRB) and thumb extension (EPL/EPB) were limited by pain but gross function appeared present.
No signs of acute carpal tunnel syndrome were present at the time of examination.
Vascular Assessment: Radial and ulnar pulses were 2+ bilaterally. Capillary refill was brisk (<2 seconds) in all digits.
Imaging & Diagnostics
Initial Radiographs (Post-Reduction Attempt):
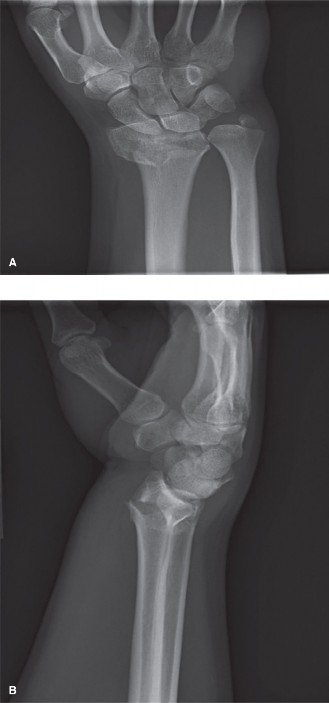
An initial series of radiographs (PA, lateral, and oblique views) of the right wrist was obtained following the unsuccessful closed reduction attempt. These films confirmed a dorsally displaced, comminuted, intra-articular distal radius fracture.

- PA View: Demonstrated significant radial shortening of approximately 5 mm (compared to the contralateral side), a radial inclination of 12 degrees (normal 21-25 degrees), and extensive comminution involving the metaphysis and articular surface. A non-displaced ulnar styloid base fracture was also noted.
- Lateral View: The critical finding was persistent dorsal angulation, measured at -12 degrees (loss of normal 11-12 degrees volar tilt). This indicated failure to restore the anatomical volar tilt despite the reduction maneuver. A significant dorsal cortical comminution and displacement of the lunate facet fragment were evident.
- Oblique Views: Further highlighted the comminuted nature of the articular surface.
Computed Tomography (CT) Scan:
Given the intra-articular involvement and the persistent articular step-off on plain radiographs, a non-contrast CT scan of the right wrist was ordered for detailed characterization of the fracture morphology and pre-operative planning.

-
Axial, Coronal, and Sagittal Views with 3D Reconstructions:
The CT scan provided invaluable detail. It confirmed a multi-fragmentary, intra-articular distal radius fracture with a specific "die-punch" component involving the lunate facet.
- Articular Step-Off: Measured up to 3mm at the lunate facet and 2mm at the scaphoid facet.
- Fragment Rotation: Crucially, the CT demonstrated significant pronation of the distal fragment, contributing to the persistent dorsal angulation and loss of volar tilt. This rotational component is often underestimated or missed on plain radiographs and is a primary reason why simple traction fails to restore anatomical volar tilt. The lunate facet fragment was displaced and rotated.
- Metaphyseal Comminution: Extensive comminution of the dorsal and volar cortices, with a significant metaphyseal void dorsally.
- DRUJ: The distal radioulnar joint (DRUJ) appeared congruent but the ulnar styloid fracture was clearly visualized, raising concern for potential intrinsic ligamentous instability of the DRUJ once the distal radius was reduced.
Templating:
Based on the CT findings, pre-operative templating was performed. A volar locking plate system was identified as the preferred fixation method, specifically an anatomically pre-contoured variable-angle locking plate designed for volar distal radius fixation. Consideration was given to the appropriate plate length to achieve adequate screw purchase proximally and distally, while avoiding impingement. Screw lengths were estimated based on CT measurements. The need for potential bone graft or bone graft substitute to fill the metaphyseal void was also considered during planning.
Differential Diagnosis
The presentation of acute wrist pain, swelling, and deformity following a FOOSH mechanism necessitates consideration of several potential diagnoses.
| Condition | Etiology/Mechanism | Key Clinical Findings | Key Imaging Findings (X-ray, CT) | Management Approach |
|---|---|---|---|---|
| 1. Distal Radius Fracture | Low/high-energy FOOSH; direct impact. Often osteoporotic in older adults. | Acute pain, swelling, gross deformity ("dinner fork" with dorsal displacement, "garden spade" with volar), tenderness, limited ROM. Neurovascular status often compromised acutely. | Loss of radial length, inclination, and volar tilt. Cortical disruption, comminution (metaphyseal/articular), articular step-off/gap. Concomitant ulnar styloid fracture common. CT crucial for intra-articular detail. | Non-operative (cast/splint) for stable, minimally displaced fractures or those adequately reduced closed. Operative (ORIF with volar locking plate, external fixation, percutaneous pinning) for unstable, significantly displaced, or intra-articular fractures, or failed closed reduction. |
| 2. Scaphoid Fracture | FOOSH (typically wrist hyperextension, ulnar deviation). Most common carpal fracture. | Acute pain in anatomical snuffbox, tenderness over scaphoid tubercle. Pain with resisted pronation or ulnar deviation. Less obvious deformity. | Often subtle or occult on initial X-rays; may require repeat X-rays in 10-14 days, MRI, or CT for definitive diagnosis. Can be associated with distal radius fractures. | Non-operative (thumb spica cast) for stable, non-displaced fractures. Operative (percutaneous screw fixation, open reduction and internal fixation) for displaced fractures, proximal pole fractures, or those with delayed union risk. High risk of avascular necrosis. |
| 3. Carpal Dislocation/Fracture-Dislocation (e.g., Perilunate Dislocation) | High-energy FOOSH (hyperextension, ulnar deviation, intercarpal supination). | Severe pain, profound swelling, often obvious wrist deformity. Limited ROM. Higher incidence of median nerve compromise (acute carpal tunnel syndrome). | Characteristic disruption of carpal arcs (Gilula's lines). Dorsal displacement of carpus relative to lunate. May involve associated fractures (scaphoid, triquetrum). Lateral view crucial for diagnosis. | Urgent closed reduction followed by surgical stabilization (often ORIF of associated fractures, ligament repair/reconstruction). High potential for chronic instability and arthritis if not anatomically reduced. Emergent if neurovascular compromise. |
| 4. Acute Carpal Tunnel Syndrome | Can be secondary to acute distal radius fracture due to swelling, hematoma, or direct compression from displaced fragments. | Paresthesias/numbness in median nerve distribution (thumb, index, middle, radial ring fingers). Weakness/loss of thumb opposition/abduction. Positive Tinel's sign over carpal tunnel. | Imaging for distal radius fracture or other underlying cause. Nerve conduction studies (NCS) typically not performed acutely. | Emergent carpal tunnel release if significant neurovascular deficit or progressive symptoms. Otherwise, supportive care, elevation, splinting, and close monitoring with definitive fracture management. |
Based on the clinical presentation and definitive imaging, the primary diagnosis was a highly comminuted, intra-articular distal radius fracture (Frykman Type VIII, AO/OTA 23-C3.3) with significant loss of volar tilt and articular congruity, confirmed by CT scan, which failed closed reduction. While scaphoid fracture and carpal dislocations were considered in the initial differential, they were ruled out by the detailed imaging. The patient did not exhibit signs of acute carpal tunnel syndrome requiring emergent release prior to fracture fixation.
Surgical Decision Making & Classification
The decision for operative management was predicated on several factors indicating an unstable fracture pattern unsuitable for non-operative treatment and the failure of closed reduction to achieve acceptable radiographic parameters.
Indications for Operative Intervention in this Case:
1.
Failed Closed Reduction:
Despite an attempt at closed reduction, post-reduction radiographs demonstrated persistent loss of volar tilt (-12 degrees dorsal angulation), radial shortening of 5mm, and an articular step-off of 3mm. These parameters are well outside the generally accepted criteria for stable reduction (e.g., volar tilt >0 degrees, radial shortening <3-5mm, articular step-off <1-2mm).
2.
Intra-articular Comminution:
The CT scan clearly demonstrated significant comminution of both the lunate and scaphoid facets, with a "die-punch" component, indicating high risk for post-traumatic arthritis if articular congruity is not restored.
3.
Fragment Rotation/Pronation:
The CT also highlighted the rotational component of the distal fragment (pronated malalignment), which is inherently difficult to correct and maintain with closed methods. This specific pathology contributes significantly to the failure of traction to restore volar tilt.
4.
Patient Demands:
As a right-hand dominant individual in an administrative role, optimal functional recovery was critical. Achieving anatomical reduction is paramount for long-term function and minimizing the risk of complications such as malunion and post-traumatic arthrosis.
Fracture Classification:
*
AO/OTA Classification:
The fracture was classified as
23-C3.3
.
*
23:
Distal forearm segment.
*
C:
Complete articular fracture (articular surface and metaphysis involved).
*
3:
Multi-fragmentary (highly comminuted) intra-articular fracture.
*
.3:
Involves both lunate and scaphoid facets, with significant metaphyseal comminution.
This classification highlights the severity and complexity, guiding the choice of open reduction and internal fixation.
-
Frykman Classification: Based on the involvement of both the radiocarpal and distal radioulnar joints, and the comminution, this would be classified as Frykman Type VIII (intra-articular fracture of the distal radius extending into the DRUJ, with an associated ulnar styloid fracture).
-
Fernandez Classification: This system classifies distal radius fractures based on the predominant injury mechanism. This case presented features consistent with a Type III (Compression/Shear Fracture) due to the "die-punch" component and articular comminution. The persistent dorsal angulation and loss of volar tilt also suggest a strong hyperextension component, but the articular involvement leans towards compression.
The comprehensive imaging, particularly the CT scan, provided crucial insights into the precise fracture morphology, the degree of articular involvement, and the rotational malalignment of the distal fragment, which collectively dictated the need for open reduction and internal fixation with a volar locking plate to restore anatomical alignment and stability.
Surgical Technique / Intervention
The patient was scheduled for open reduction and internal fixation (ORIF) of the right distal radius fracture.
Pre-Operative Preparation:
After obtaining informed consent, the patient was taken to the operating theatre. Prophylactic intravenous antibiotics (Cefazolin 2g) were administered.
Anesthesia and Positioning:
The patient received a regional anesthetic block (interscalene block for supra-clavicular and axillary block) in combination with general anesthesia. She was positioned supine on the operating table with the right arm extended onto a radiolucent hand table. A tourniquet was applied to the upper arm and inflated to 250 mmHg after exsanguination with an Esmarch bandage. The entire limb was prepped and draped in a sterile fashion, allowing free access for fluoroscopy. The C-arm was positioned to obtain true PA, lateral, and oblique views of the wrist without repositioning the patient.
Surgical Approach (Volar Henry Approach):
1.
Incision:
A curvilinear skin incision of approximately 6-8 cm was made on the volar aspect of the distal forearm, extending from the level of the flexor crease of the wrist proximally along the radial border of the flexor carpi radialis (FCR) tendon.
2.
Dissection:
Subcutaneous tissues were carefully dissected. The palmar cutaneous branch of the median nerve was identified and protected, often lying radially to the FCR tendon. The flexor carpi radialis (FCR) tendon sheath was incised longitudinally, and the FCR tendon was retracted ulnarly.
3.
Exposure of Radial Artery and Median Nerve:
The radial artery was identified along the radial border of the FCR sheath and protected radially. Deeper dissection revealed the median nerve, which was gently retracted ulnarly, along with the flexor pollicis longus (FPL) muscle belly.
4.
Pronator Quadratus (PQ) Muscle Reflection:
The pronator quadratus (PQ) muscle was identified, originating from the distal ulna and inserting onto the distal radius. A meticulous L-shaped incision was made through the PQ, with the horizontal limb along its distal insertion onto the radius and the vertical limb along its ulnar border. The PQ was then carefully elevated subperiosteally from distal to proximal, hinged on its ulnar attachment. This exposed the volar surface of the distal radius and the fracture site.
Reduction Techniques:
The specific challenge in this case was the persistent loss of volar tilt due to the pronated and dorsally impacted distal fragment. Simple traction had failed, as it does not adequately address the rotational malalignment or the dorsal impaction.
1.
Initial Disimpaction and Provisional Traction:
Gentle longitudinal traction was applied to the hand to disimpact the fracture fragments and restore some radial length. This was maintained with finger traps if necessary, but carefully to avoid over-distraction.
2.
Direct Visualization and Manipulation:
With the PQ reflected, the fracture fragments were directly visualized. A small dental pick or blunt elevator was used to meticulously disengage impacted fragments.
3.
Correction of Rotational Malalignment:
This was the critical step for restoring volar tilt. The distal fragment was grasped with a bone clamp or held with K-wires inserted as joy-sticks. The fragment was
supinated
(or derotated from its pronated position) while simultaneously applying
dorsal pressure
to the distal fragment. This maneuver is crucial to bring the articular surface back into a neutral or slightly volar-tilted position relative to the diaphyseal axis. The tendency for gravity or soft tissue attachments to pull the fragment into pronation and dorsal tilt must be overcome.
4.
Articular Reduction:
Under fluoroscopic guidance (PA and lateral views), the articular fragments, particularly the lunate facet (die-punch fragment), were directly reduced using small K-wires, blunt elevators, or specific articular clamps. The goal was to achieve an articular step-off of less than 1mm. Temporary K-wires were used to stabilize key articular fragments to the radial shaft or to each other.
5.
Metaphyseal Void Management:
After articular reduction, a significant metaphyseal void was noted dorsally and volarly due to the comminution. To prevent collapse and maintain reduction, a cancellous bone graft (either allograft chips or a synthetic bone graft substitute) was gently packed into the metaphyseal defect to provide structural support and promote healing.
Fixation Construct (Volar Locking Plate):
1.
Plate Selection and Positioning:
An anatomically contoured, variable-angle volar locking plate (e.g., from the Stryker VariAx 2, DePuy Synthes DVR, or Acumed Acu-Loc systems) was selected. The plate was provisionally positioned on the volar aspect of the distal radius. The proximal edge of the plate was positioned just proximal to the watershed line to avoid potential impingement on the flexor pollicis longus (FPL) tendon while still allowing for adequate screw length in the distal fragment.
2.
Proximal Fixation:
The plate was secured to the radial shaft proximally with non-locking cortical screws or locking screws, ensuring bicortical purchase.
3.
Distal Fixation:
Under fluoroscopic control, variable-angle locking screws were inserted into the distal fragments, targeting the subchondral bone for maximum stability. Screw trajectory was carefully planned to avoid penetrating the joint surface or impinging on the DRUJ.
4.
Final Checks:
Fluoroscopy was used extensively during the entire reduction and fixation process to confirm:
*
PA View:
Radial length (restored to within 1-2mm of contralateral side), radial inclination (restored to 21-25 degrees), and absence of articular step-off.
*
Lateral View:
Restoration of normal volar tilt (10-15 degrees), absence of articular step-off, and appropriate screw lengths (all screws subchondral but not penetrating joint). The critical volar tilt was confirmed at +12 degrees.
*
Oblique Views:
Confirmed absence of residual fragment displacement.
*
DRUJ Stability:
The distal radioulnar joint was assessed by pronating and supinating the forearm while compressing the ulna to the radius. It was found to be stable after fixation of the radius. The ulnar styloid fracture was not significantly displaced and was deemed stable, requiring no separate fixation.
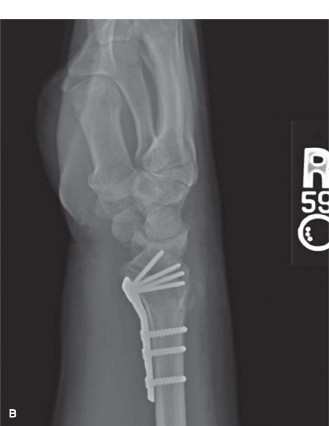
Closure:
Once satisfactory reduction and fixation were confirmed, the tourniquet was deflated. Hemostasis was achieved. The pronator quadratus muscle was meticulously repaired over the volar plate using absorbable sutures. This repair is crucial to help prevent volar tendon irritation or rupture from direct contact with the plate, and may contribute to distal radioulnar joint stability. The subcutaneous tissues were closed, followed by skin closure with interrupted non-absorbable sutures. A sterile dressing was applied, and the wrist was immobilized in a neutral volar splint.
Post-Operative Protocol & Rehabilitation
Immediate Post-Operative Phase (Days 0-7):
*
Immobilization:
A well-padded volar wrist splint or sugar tong splint was applied for comfort and edema control, maintaining the wrist in a neutral position.
*
Pain Management:
Multimodal analgesia regimen including oral opioids, NSAIDs (if not contraindicated), and acetaminophen.
*
Edema Control:
Strict elevation of the hand above heart level, active finger, elbow, and shoulder range of motion exercises were initiated immediately to reduce swelling and prevent stiffness in adjacent joints. Ice packs were applied as tolerated.
*
Neurovascular Monitoring:
Close monitoring of neurovascular status, including sensation, motor function, and capillary refill.
*
Wound Care:
The dressing was kept clean and dry. Sutures were typically removed at 10-14 days post-op.
Early Rehabilitation Phase (Weeks 1-6):
*
Splint Removal & Hand Therapy Referral:
At 1-2 weeks, once soft tissue swelling had subsided and wound healing was progressing, the splint was typically removed. The patient was referred for formal hand therapy.
*
Gentle Active ROM:
Under the guidance of a hand therapist, active range of motion for the wrist was initiated (flexion, extension, radial and ulnar deviation, pronation, and supination). Passive range of motion was introduced cautiously based on fracture stability and surgeon preference.
*
Tendon Gliding Exercises:
To prevent adhesions and maintain tendon excursion.
*
Scar Management:
Gentle scar massage commenced after suture removal to prevent adhesions.
*
Progressive Loading:
Avoidance of heavy lifting or weight-bearing through the wrist was strictly enforced. Light activities of daily living were gradually reintroduced.
Intermediate Rehabilitation Phase (Weeks 6-12):
*
Increased ROM:
The focus shifts to maximizing wrist and forearm range of motion. Dynamic splinting may be used if significant stiffness persists.
*
Strengthening:
Progressive strengthening exercises were initiated using light resistance, putty, resistance bands, and gradually introducing light weights (e.g., 0.5-1 kg).
*
Functional Activities:
Activities mimicking work and daily tasks were incorporated into the therapy program.
*
Radiographic Follow-up:
Follow-up radiographs at 6 weeks and 12 weeks to assess fracture healing and maintenance of reduction.
Late Rehabilitation Phase (Beyond 12 Weeks):
*
Return to Full Activity:
Once radiographic evidence of healing is present and strength and ROM are optimized, a gradual return to full activity, including sports or manual labor, is permitted. This is individualized based on patient progress and fracture union.
*
Advanced Strengthening:
Continued progressive resistance exercises.
*
Monitoring for Complications:
Long-term monitoring for potential complications such as post-traumatic arthritis, nonunion, malunion, complex regional pain syndrome (CRPS), tendon irritation/rupture, or hardware-related issues. Hardware removal is considered only if symptomatic.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls:
- Comprehensive Pre-operative Planning: A detailed understanding of the fracture morphology using high-quality radiographs and, crucially, a CT scan , is paramount for intra-articular and comminuted distal radius fractures. CT identifies articular step-offs, fragment rotation (especially pronation of the distal fragment), and metaphyseal defects that impact reduction strategy.
- Address Rotational Malalignment for Volar Tilt: The primary reason "traction fails volar tilt" is the often-overlooked pronated rotation of the distal fragment. Simple ligamentotaxis with traction primarily restores length but does not correct this rotation or dorsal impaction. Direct visualization and manipulation, specifically supination of the distal fragment combined with dorsal pressure , are essential to achieve anatomical volar tilt.
- Anatomical Reduction of Articular Surface: Strive for less than 1mm of articular step-off. Use joy-stick K-wires or small elevators for fragment-specific reduction, especially of the lunate facet (die-punch) fragments.
- Volar Plate Positioning ("Watershed Line"): The distal edge of the volar locking plate must be positioned proximal to the critical "watershed line" of the distal radius to prevent impingement and friction on the flexor pollicis longus (FPL) and other flexor tendons, which can lead to tenosynovitis or rupture. However, it must be distal enough to provide adequate purchase in the subchondral bone. Careful fluoroscopic assessment in the lateral view is necessary.
- Pronator Quadratus Repair: Meticulous repair of the pronator quadratus muscle flap over the volar plate is crucial. It serves as a soft tissue buffer, minimizing tendon irritation, and may contribute to distal radioulnar joint (DRUJ) stability.
- Assess DRUJ Stability: Always assess DRUJ stability intraoperatively after definitive fixation of the distal radius. If unstable, consider further intervention (e.g., TFCC repair, temporary K-wire fixation across the DRUJ).
- Bone Graft for Metaphyseal Void: In cases of significant metaphyseal comminution and bone loss, packing the defect with cancellous bone graft (autograft or allograft) or bone graft substitute can provide structural support, prevent secondary collapse, and promote healing.
- Early Mobilization (if stable): If stable fixation is achieved, early, protected active range of motion, guided by a hand therapist, can significantly improve functional outcomes, reduce stiffness, and minimize the risk of Complex Regional Pain Syndrome (CRPS).
Pitfalls:
- Inadequate Reduction: The most common pitfall. Relying solely on traction and failing to address the pronated and dorsally impacted distal fragment leads to persistent loss of volar tilt, radial shortening, and articular incongruity. These malunions are often poorly tolerated and can lead to pain and post-traumatic arthritis.
- Over-Distraction: Excessive traction during reduction can lead to ligamentotaxis with gapping, potentially resulting in nonunion, delayed union, or permanent carpal ligament laxity and instability.
-
Hardware Impingement/Prominence:
- Volar: A plate positioned too distally or proud can lead to severe flexor tendon irritation or rupture (especially FPL), requiring hardware removal.
- Dorsal: Screws penetrating the dorsal cortex can irritate extensor tendons or impinge dorsally during wrist extension.
- Articular Penetration by Screws: Screws that are too long can penetrate the articular cartilage, causing pain, crepitus, and accelerated post-traumatic arthritis. Intraoperative fluoroscopy with multiple views (PA, true lateral, 45-degree pronated oblique, 45-degree supinated oblique) is essential to confirm appropriate screw length and trajectory.
- Nerve Injury: Iatrogenic injury to the palmar cutaneous branch of the median nerve or the superficial radial nerve during the approach is a risk. Careful dissection and retraction are necessary.
- Complex Regional Pain Syndrome (CRPS): A devastating complication. Characterized by disproportionate pain, swelling, skin changes, and functional limitation. Early recognition and aggressive multimodal treatment are crucial. Vigilant post-operative pain control and early mobilization can help mitigate this risk.
- Malunion/Nonunion: Despite ORIF, severe comminution or poor bone quality can predispose to malunion or nonunion. Regular radiographic follow-up is necessary.
- Infection: As with any open procedure, surgical site infection remains a risk, despite prophylactic antibiotics.
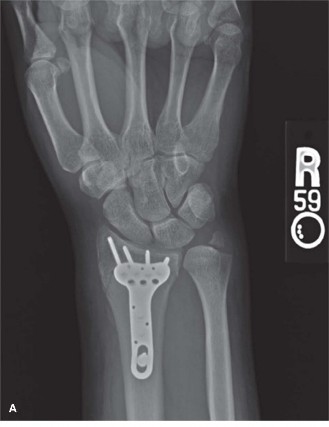
Clinical & Radiographic Imaging
You Might Also Like