Orthopedic Ban Review | Dr Hutaif General Orthopedics R -...
14 Apr 2026
56 min read
102 Views

Key Takeaway
This interactive board review contains 100 randomly selected orthopedic surgery questions with clinical images, immediate feedback, and detailed references.
Orthopedic Ban Review | Dr Hutaif General Ort...
00:00
Start Quiz
Question 1High Yield
Which of the following statements is false regarding the use of estrogen therapy to prevent osteoporosis:
Explanation
Estrogen therapy is one of the main therapeutiCinterventions used to prevent osteoporosis in postmenopausal women. Features of estrogen interactions include:
Osteoblasts have estrogen receptors.
Estrogen indirectly affects calcium metabolism by modulating calcium absorption and renal excretion. Estrogen decreases osteoclast activity.
Estrogen prevents osteoporosis in 80% of postmenopausal women.
The protective effect of estrogren therapy ends when therapy is discontinued.
Osteoblasts have estrogen receptors.
Estrogen indirectly affects calcium metabolism by modulating calcium absorption and renal excretion. Estrogen decreases osteoclast activity.
Estrogen prevents osteoporosis in 80% of postmenopausal women.
The protective effect of estrogren therapy ends when therapy is discontinued.
Question 2High Yield
A 75-year-old man is transferred in for management of an infected left total knee arthroplasty (TKA). He has had two irrigation and debridements with polyethylene liner exchanges for a resistant enterococcus bacteria that has been cultured from intraoperative specimens during these procedures. He now has an open wound (Figure
Explanation
No detailed explanation provided for this question.
Question 3High Yield
A 14-year-old girl with a history of multiple food allergies and severe asthma was involved in a motor vehicle accident and sustained an isolated right femur fracture. Which of the following medications is the best choice to control her pain:
Explanation
The goal in this patient is to provide safe, effective, and long-acting analgesia. Meperidine is recommended in this circumstance. It is an opioid that provides intermediate and long-term analgesia. Additionally, it does not cause the associated histamine release and bronchospasm that can occur in patients with asthma and atopia.
Ketamine would provide short-term analgesia, but would also alter the level of consciousness.
Morphine is well known for precipitating bronchospasm in patients with atopia and asthma. Therefore, it would not be the best choice in the scenario presented.
Methohexital (a barbiturate) and midazolam (a benzodiazepine) both cause decreased awareness and have no analgesic properties.
Ketamine would provide short-term analgesia, but would also alter the level of consciousness.
Morphine is well known for precipitating bronchospasm in patients with atopia and asthma. Therefore, it would not be the best choice in the scenario presented.
Methohexital (a barbiturate) and midazolam (a benzodiazepine) both cause decreased awareness and have no analgesic properties.
Question 4High Yield
Figure 8 shows the AP radiograph of a 33-year-old woman who sustained a midshaft clavicle fracture from a motorcycle accident 15 months ago. She continues to have significant pain with activities of daily living. Management should consist of
Explanation
The patient has a symptomatic painful atrophic midclavicular nonunion, and the treatment of choice is rigid internal fixation with a dynamic compression plate and autogenous bone grafting. A tension band effect is desired and achieved by placing the plate superiorly. Excellent success rates of 90% to 100% have been reported using this technique. Intramedullary screw fixation without bone grafting has a decreased success rate. Partial claviculectomy is not a preferred option.
REFERENCES: Jupiter JB, Leffert RD: Non-union of the clavicle: Associated complications and surgical management. J Bone Joint Surg Am 1987;69:753-760.
Simpson NS, Jupiter JB: Clavicular nonunion and malunion: Evaluation and surgical management. J Am Acad Orthop Surg 1996;4:1-8.
REFERENCES: Jupiter JB, Leffert RD: Non-union of the clavicle: Associated complications and surgical management. J Bone Joint Surg Am 1987;69:753-760.
Simpson NS, Jupiter JB: Clavicular nonunion and malunion: Evaluation and surgical management. J Am Acad Orthop Surg 1996;4:1-8.
Question 5High Yield
A 34-year-old woman presents for treatment of pain in the hallux. She notes pain upon weight bearing and wearing high-heel shoes. Upon examination, the range of motion of the hallux metatarsophalangeal (MP) joint is 10° dorsiflexion and 30° plantarflexion, with pain upon passive dorsiflexion. Radiographs demonstrate osteophytes over the dorsal surface of the metatarsal head, maintenance of the joint space, and a metatarsal declination angle of 10°. The first metatarsal is elevated above the second metatarsal at the level of the metatarsal neck by 4 mm. The ideal procedure to correct this problem and alleviate pain is:
Explanation
This patient has mild hallux rigidus with a normal alignment of the first metatarsal. The average elevation of the first metatarsal above the second metatarsal at the level of the metatarsal neck is 7.5 mm, thus, 4 mm is within normal limits. Arthrodesis is not indicated for mild rigidus and osteotomy is indicated only for severe elevation of the first metatarsal. C heilectomy combined with osteotomy of the proximal phalanx (the Moberg osteotomy) is the preferred procedure.
Question 6High Yield
A 13-year-old boy is complaining of elbow and wrist pain following a fall off a bike. Radiographs are taken in the emergency department (Figures 1 through 4). The wrist injury is unstable, and the patient is taken to the operating room for closed reduction and pinning of the distal radius fracture, closed treatment of the proximal fractures. Subsequent to surgery, the patient is noted to have increased irritability and progressively requires more IV pain medication throughout the night. He is anxious, argumentative, and refuses to comply with neurovascular assessments of his upper extremity. What is the best next step in treatment for this patient?

Explanation
■
This patient is manifesting the signs of acute compartment syndrome (ACS). In the pediatric population, the 5 P's are less reliable signs of ACS. Instead, pediatric patients manifest increasing analgesic requirements, agitation, and anxiety in the evolution of ACS. Given this patient's clinical signs and risk factors for developing ACS (increased age/adolescence, male predominance, multiple fractures within an extremity), the appropriate treatment is to proceed with emergent forearm fasciotomies.
Administering diazepam (Valium) for the anxiety only masks the underlying condition, which may result in a poorer prognosis if the diagnosis is further delayed. Providing ice and elevation may be useful to diminish swelling and pain, but will not successfully treat the compartment syndrome. Importantly, the diagnosis of ACS is primarily a clinical one. Measuring compartment pressures may be more useful to help confirm or rule out the diagnosis in an obtunded child or one with severe mental/communication difficulty.
■
This patient is manifesting the signs of acute compartment syndrome (ACS). In the pediatric population, the 5 P's are less reliable signs of ACS. Instead, pediatric patients manifest increasing analgesic requirements, agitation, and anxiety in the evolution of ACS. Given this patient's clinical signs and risk factors for developing ACS (increased age/adolescence, male predominance, multiple fractures within an extremity), the appropriate treatment is to proceed with emergent forearm fasciotomies.
Administering diazepam (Valium) for the anxiety only masks the underlying condition, which may result in a poorer prognosis if the diagnosis is further delayed. Providing ice and elevation may be useful to diminish swelling and pain, but will not successfully treat the compartment syndrome. Importantly, the diagnosis of ACS is primarily a clinical one. Measuring compartment pressures may be more useful to help confirm or rule out the diagnosis in an obtunded child or one with severe mental/communication difficulty.
Question 7High Yield
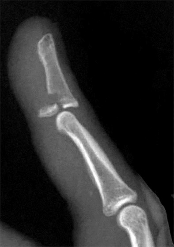
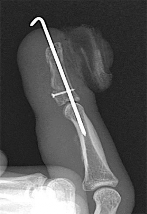
Figure 1 shows a radiograph obtained from an active 30-year-old man who sustained an injury to his ring finger 1 week earlier. The most appropriate treatment is
---
---
Explanation
---
Figure 1 reveals evidence of an intra-articular distal phalanx fracture with a distal interphalangeal (DIP) joint dorsal subluxation. This injury is unstable and requires surgical management for an active individual. Volar distal phalanx fractures are often associated with flexor digitorum profundus avulsion injuries, which are addressed concomitantly. This injury was treated with ORIF of the intra-articular fracture, pinning of the DIP joint, and repair of an avulsed flexor digitorum profundus tendon with a button on the dorsal nail plate, as shown in Figure 2. Splint immobilization would not maintain a reduction of this unstable injury. The terminal tendon is not injured in this patient but is often injured in a dorsal distal phalanx fracture with a volar dislocation. Arthrodesis of the DIP is a salvage procedure and would not be considered acutely.
Figure 1 reveals evidence of an intra-articular distal phalanx fracture with a distal interphalangeal (DIP) joint dorsal subluxation. This injury is unstable and requires surgical management for an active individual. Volar distal phalanx fractures are often associated with flexor digitorum profundus avulsion injuries, which are addressed concomitantly. This injury was treated with ORIF of the intra-articular fracture, pinning of the DIP joint, and repair of an avulsed flexor digitorum profundus tendon with a button on the dorsal nail plate, as shown in Figure 2. Splint immobilization would not maintain a reduction of this unstable injury. The terminal tendon is not injured in this patient but is often injured in a dorsal distal phalanx fracture with a volar dislocation. Arthrodesis of the DIP is a salvage procedure and would not be considered acutely.
Question 8High Yield
A 45-year-old man has had 3 months of increasing upper back pain, “balance" issues, and heaviness in his legs. His physical examination reveals a normal neurological examination, but he is noted to be anemic. His MRI scans and biopsy specimen are shown in Figures 1 through

Explanation
■
The MRI scan reveals a large posterior element tumor, which is compressing the spinal cord. Multiple lesions within the spinal column are consistent with multiple myeloma. Myeloma is a radiosensitive tumor. Additionally, he has a SINS of 6. This score helps the treating physician determine the tumor-related instability of the vertebral column to guide the decision for operative management. A SINS of 0-6 is thought to be stable; 7-12, potentially stable, and >13, unstable. Appropriate treatment in a neurologically intact patient with a radiosensitive tumor with a low SINS would be radiation treatment versus surgical treatment, despite the degree of spinal cord compression.
The MRI scan reveals a large posterior element tumor, which is compressing the spinal cord. Multiple lesions within the spinal column are consistent with multiple myeloma. Myeloma is a radiosensitive tumor. Additionally, he has a SINS of 6. This score helps the treating physician determine the tumor-related instability of the vertebral column to guide the decision for operative management. A SINS of 0-6 is thought to be stable; 7-12, potentially stable, and >13, unstable. Appropriate treatment in a neurologically intact patient with a radiosensitive tumor with a low SINS would be radiation treatment versus surgical treatment, despite the degree of spinal cord compression.
Question 9High Yield
The most common complication after resection of a plantar fibromatosis is:
Explanation
The most common complication after resection of plantar fibromatosis is recurrence. Although other complications (nerve injury and wound dehiscence) do occur, they occur less frequently. The most reliable treatment for plantar fibromatosis is observation and shoe wear modification if the lesion is painful.
Question 10High Yield
Figure 1 is the radiograph of a 12-month-old girl with a history of type 3 fibroblast growth factor receptor mutation, rhizomelic shortening of the limbs, and dwarfism who is noted to have a thoracolumbar kyphosis (TLK) of 25°. Spontaneous resolution of her thoracolumbar kyphosis is closely associated with

Explanation
■
Achondroplasia is a skeletal dysplasia caused by a genetic mutation in the type-3 fibroblast growth factor receptor gene, which leads to abnormal endochondral ossification. Some, but not all physical features of achondroplasia include rhizomelic shortening of the limbs, midface hypoplasia, frontal bossing, lower extremity malalignment, hyperlordosis and TLK (defined as a Cobb angle of 20° or more centered at T12 and L1).
Thoracolumbar kyphosis is a characteristic feature of achondroplasia and thought to be a result of developmental motor delay and hypotonia and disproportionate head size relative to a small chest size. Most patients with achondroplasia develop TLK at about sitting age. Studies have shown that most cases of TLK resolve spontaneously within a year after patients start to walk. Studies suggest that approximately 30% of early TLK cases persist, and a third of these cases progress into severe deformities. Apical vertebral translation, percentage of apical vertebral wedging for vertebral height, and developmental motor delay (not sitting by age 14 months and not walking independently by age 30 months) are shown to be risk factors for TLK to persist. Presence of a vertriculoperitoneal shunt, hydrocephalus, foramen magnum decompression, gender, lumbar lordosis were not associated with unresolved TLK. Although the magnitude of the thoracolumbar kyphosis at presentation(>25°) is cited as a risk factor in some studies, this is not verified in other studies.
■
Achondroplasia is a skeletal dysplasia caused by a genetic mutation in the type-3 fibroblast growth factor receptor gene, which leads to abnormal endochondral ossification. Some, but not all physical features of achondroplasia include rhizomelic shortening of the limbs, midface hypoplasia, frontal bossing, lower extremity malalignment, hyperlordosis and TLK (defined as a Cobb angle of 20° or more centered at T12 and L1).
Thoracolumbar kyphosis is a characteristic feature of achondroplasia and thought to be a result of developmental motor delay and hypotonia and disproportionate head size relative to a small chest size. Most patients with achondroplasia develop TLK at about sitting age. Studies have shown that most cases of TLK resolve spontaneously within a year after patients start to walk. Studies suggest that approximately 30% of early TLK cases persist, and a third of these cases progress into severe deformities. Apical vertebral translation, percentage of apical vertebral wedging for vertebral height, and developmental motor delay (not sitting by age 14 months and not walking independently by age 30 months) are shown to be risk factors for TLK to persist. Presence of a vertriculoperitoneal shunt, hydrocephalus, foramen magnum decompression, gender, lumbar lordosis were not associated with unresolved TLK. Although the magnitude of the thoracolumbar kyphosis at presentation(>25°) is cited as a risk factor in some studies, this is not verified in other studies.
Question 11High Yield
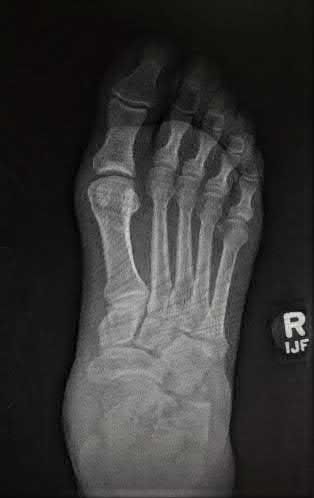
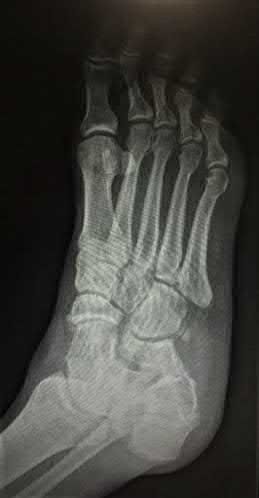
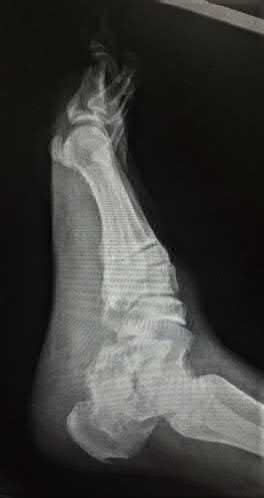
A 30-year-old manual laborer is forced to jump from a collapsing building. He lands on his feet but experiences severe right foot pain. He presents with intact skin, moderate swelling and ecchymosis about the right heel, and global tenderness of the hindfoot. He is otherwise neurovascularly intact. Radiographs of his right foot are shown in Figures A-C. When considering surgery, which of the following is the
only undisputed difference when comparing nonoperative management of this injury to open reduction and internal fixation?
only undisputed difference when comparing nonoperative management of this injury to open reduction and internal fixation?
Explanation
An increased risk of surgical complications and reoperation is the only difference which has been found among patients who have undergone operative versus nonoperative management of displaced intra-articular calcaneal fractures (DIACFs). Differences between all other radiographic, subjective, and standardized functional outcomes remain disputed.
Despite a number of randomized control trials directly comparing operative to nonoperative management of DIACFs, controversy still surrounds the surgical indications. This is thought to be largely due to patient heterogeneity and the impact of age, gender, and other potentially confounding variables such as vocation and socioeconomic status. Furthermore, variability in surgical technique and functional outcome measures used preclude direct comparisons between studies as well as implementation of effective meta-analyses.
Functional outcomes following operative management have been shown to be worse in the older, obese, smoking, manual laborer, and worker’s compensation demographics, albeit only on subgroup analysis and not in direct comparison to a nonoperatively managed matched cohort. Some studies have suggested an improved ability to return to work and decreased risk of subtalar arthritis in operatively-managed DIACFs. However long-term investigations have shown conflicting findings on maintenance of radiographic indices including calcaneal height, width, and Bohler’s angle, regardless of management strategy.
Buckley et al. compared nonoperative management to open reduction and internal fixation of DIACFs. The authors found no significant difference in functional outcomes at a minimum of 2-year follow-up. However, after eliminating the worker’s compensation patients from the analysis, SF-36 and VAS scores were significantly better in the surgical cohort. They supported that the outcomes following operative management were in general superior.
Griffin et al. performed a randomized controlled trial comparing operative to nonoperative management of acute DIACFs. At a minimum two-year follow-up, the authors found that there was no significant difference in any of the functional outcome measures. However, the risk of complications and all-cause reoperation was perhaps not surprisingly significantly higher in the surgical
cohort.
Ibrahim et al. performed a 15-year follow-up of a randomized control trial evaluating the differences between nonoperative and operative management of DIACFs. The findings were similar to their index study, with no significant differences in any of the functional outcomes scores or radiographic parameters. The authors also found no difference in the rate of development in subtalar arthritis. This study has been criticized for the incomplete follow-up data in nearly two-thirds of the original cohort.
In a recent meta-analysis, Ning et al. evaluated studies comparing outcomes following operative versus nonoperative management of DIACFs. The authors found no significant differences in standardized functional outcomes, but they noted that heterogeneity in the outcome measures across studies may contribute to ambiguity in interpreting this finding. Conversely, operatively managed patients were more likely to return to work, but were also more likely to experience complications. The authors concluded that operative management for DIACFs was superior when displacement was outside of acceptable tolerances.
Figures:
Figure A is an AP radiographic of the right foot demonstrating a comminuted DIACF with subluxation of the calcaneocuboid joint.
Figure B is an oblique view of the right foot confirming a depressed posterior facet.
Figure C is a lateral view of the foot showing significant loss of calcaneal height and articular incongruity.
Incorrect Answers:
Answer 1: Previous studies have shown either a comparable or increased risk of development of subtalar arthritis in nonoperatively managed DIACFs.
Answer 3: Most comparative studies have found no significant difference in long-term subjective and functional outcomes between operatively and nonoperatively managed DIACFs. Subgroup analysis supports improved outcomes in select patient demographics with certain injury characteristics, but this remains disputed.
Answer 4: Nonoperatively managed DIACFs have been shown to have greater difficulty with shoe wear but generally a decreased likelihood of returning to work post-operatively.
Answer 5: Studies are conflicting and inconclusive regarding maintenance of radiographic indices such as Bohler’s angle, calcaneal height and width at longterm follow-up regardless of treatment method.
Despite a number of randomized control trials directly comparing operative to nonoperative management of DIACFs, controversy still surrounds the surgical indications. This is thought to be largely due to patient heterogeneity and the impact of age, gender, and other potentially confounding variables such as vocation and socioeconomic status. Furthermore, variability in surgical technique and functional outcome measures used preclude direct comparisons between studies as well as implementation of effective meta-analyses.
Functional outcomes following operative management have been shown to be worse in the older, obese, smoking, manual laborer, and worker’s compensation demographics, albeit only on subgroup analysis and not in direct comparison to a nonoperatively managed matched cohort. Some studies have suggested an improved ability to return to work and decreased risk of subtalar arthritis in operatively-managed DIACFs. However long-term investigations have shown conflicting findings on maintenance of radiographic indices including calcaneal height, width, and Bohler’s angle, regardless of management strategy.
Buckley et al. compared nonoperative management to open reduction and internal fixation of DIACFs. The authors found no significant difference in functional outcomes at a minimum of 2-year follow-up. However, after eliminating the worker’s compensation patients from the analysis, SF-36 and VAS scores were significantly better in the surgical cohort. They supported that the outcomes following operative management were in general superior.
Griffin et al. performed a randomized controlled trial comparing operative to nonoperative management of acute DIACFs. At a minimum two-year follow-up, the authors found that there was no significant difference in any of the functional outcome measures. However, the risk of complications and all-cause reoperation was perhaps not surprisingly significantly higher in the surgical
cohort.
Ibrahim et al. performed a 15-year follow-up of a randomized control trial evaluating the differences between nonoperative and operative management of DIACFs. The findings were similar to their index study, with no significant differences in any of the functional outcomes scores or radiographic parameters. The authors also found no difference in the rate of development in subtalar arthritis. This study has been criticized for the incomplete follow-up data in nearly two-thirds of the original cohort.
In a recent meta-analysis, Ning et al. evaluated studies comparing outcomes following operative versus nonoperative management of DIACFs. The authors found no significant differences in standardized functional outcomes, but they noted that heterogeneity in the outcome measures across studies may contribute to ambiguity in interpreting this finding. Conversely, operatively managed patients were more likely to return to work, but were also more likely to experience complications. The authors concluded that operative management for DIACFs was superior when displacement was outside of acceptable tolerances.
Figures:
Figure A is an AP radiographic of the right foot demonstrating a comminuted DIACF with subluxation of the calcaneocuboid joint.
Figure B is an oblique view of the right foot confirming a depressed posterior facet.
Figure C is a lateral view of the foot showing significant loss of calcaneal height and articular incongruity.
Incorrect Answers:
Answer 1: Previous studies have shown either a comparable or increased risk of development of subtalar arthritis in nonoperatively managed DIACFs.
Answer 3: Most comparative studies have found no significant difference in long-term subjective and functional outcomes between operatively and nonoperatively managed DIACFs. Subgroup analysis supports improved outcomes in select patient demographics with certain injury characteristics, but this remains disputed.
Answer 4: Nonoperatively managed DIACFs have been shown to have greater difficulty with shoe wear but generally a decreased likelihood of returning to work post-operatively.
Answer 5: Studies are conflicting and inconclusive regarding maintenance of radiographic indices such as Bohler’s angle, calcaneal height and width at longterm follow-up regardless of treatment method.
Question 12High Yield
Considering her current symptoms, history, and examination findings, you believe that the most efficacious means with which to address this patient's junctional kyphosis is
Explanation
- revision posterior instrumentation with extension of the fusion to T1 to span the area of junctional kyphosis.
Question 13High Yield
An obtunded 80-year-old man was found alone in his apartment after an apparent fall. A CT scan performed in the emergency department shows that he has an extensile injury of an ankylosed cervical spine. The fracture extends across the ossified C5-C6 disk space and into the lamina of C5. There is 1.5 cm of widening between the C5 and C6 vertebrae anteriorly. The patient's family asks you about the long-term impact of the fracture on his functional capacity and survival. You advise them that patients with fractures of the cervical spine with ankylosing conditions have
Explanation
■
Several studies have found that rates of neurologic deficit and mortality are higher for patients with ankylosing spondylitis and a spinal fracture than for age-matched controls. The 2011 work of Schoenfeld and associates, which directly compared patients with cervical fractures in ankylosed spines to age- and sex-matched controls who also had cervical fractures but no ankylosing condition, demonstrated that those with ankylosing spondylitis were at elevated risk for mortality for up to 2 years after sustaining a fracture. In a study by Westerveld and associates, the rate of neurologic deficit among patients with ankylosing spondylitis and a spinal fracture was 57.1% compared to 12.6% among controls.
Several studies have found that rates of neurologic deficit and mortality are higher for patients with ankylosing spondylitis and a spinal fracture than for age-matched controls. The 2011 work of Schoenfeld and associates, which directly compared patients with cervical fractures in ankylosed spines to age- and sex-matched controls who also had cervical fractures but no ankylosing condition, demonstrated that those with ankylosing spondylitis were at elevated risk for mortality for up to 2 years after sustaining a fracture. In a study by Westerveld and associates, the rate of neurologic deficit among patients with ankylosing spondylitis and a spinal fracture was 57.1% compared to 12.6% among controls.
Question 14High Yield
Which of the following are characteristic of osteoarthritis:
Explanation
The characteristic findings in osteoarthritis are:
Asymmetric loss of the joint space Subchondral sclerosis and cysts Osteophyte formation
As the cartilage degenerates, progressive bone remodeling occurs. The other responses refer to other synovial proliferative disorders:
Pigmented villonodular synovitis: Synovial proliferation, cysts/erosions on both sides of the joint
Rheumatoid arthritis: Synovial proliferation with lymphocytic infiltration, periarticular osteopenia, symmetric joint space loss
C harcot neuropathy: Subluxation, bone fragmentation, dissolution of the articular surfaces
Gout: Periarticular erosions, soft tissue masses, preservation of the articular surfaces
Asymmetric loss of the joint space Subchondral sclerosis and cysts Osteophyte formation
As the cartilage degenerates, progressive bone remodeling occurs. The other responses refer to other synovial proliferative disorders:
Pigmented villonodular synovitis: Synovial proliferation, cysts/erosions on both sides of the joint
Rheumatoid arthritis: Synovial proliferation with lymphocytic infiltration, periarticular osteopenia, symmetric joint space loss
C harcot neuropathy: Subluxation, bone fragmentation, dissolution of the articular surfaces
Gout: Periarticular erosions, soft tissue masses, preservation of the articular surfaces
Question 15High Yield
A 9-year-old boy is injured while playing soccer. His examination reveals painful range of motion
between 5° and 75°. There is tenderness on the medial side of his knee. There is no effusion, a grade 1A Lachman test, and severe pain over the medial epicondyle of the knee. Varus stress is negative and pain is elicited with valgus stress. Initial radiographs were negative for abnormality. What is the most likely area of injury?
between 5° and 75°. There is tenderness on the medial side of his knee. There is no effusion, a grade 1A Lachman test, and severe pain over the medial epicondyle of the knee. Varus stress is negative and pain is elicited with valgus stress. Initial radiographs were negative for abnormality. What is the most likely area of injury?
Explanation
This patient likely has a physeal injury to the distal femoral physis. Stress radiographs or an MRI scan will most reliably reveal this diagnosis. The growth plate, when injured, is most commonly fractured through the hypertrophic zone of cartilage, its weakest point. This patient is optimally treated in a cylindrical or long-leg cast.
Question 16High Yield
Which of the following tumors rarely metastasizes to the spine?
Explanation
Metastatic tumors are the most common tumors found in the spine. Up to 75% of all bony metastases occur in patients with carcinoma of the breast, lung, kidney, prostate, thyroid, and multiple myeloma. Carcinoma of the colon rarely metastasizes to the spine.
Question 17High Yield
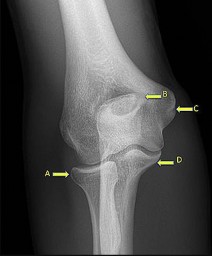
A 24-year-old right-hand-dominant professional baseball pitcher has valgus extension overload (VEO) syndrome of the right elbow, as seen in Figure 7. Which letter in the figure corresponds to the typical area of osteophyte formation in this condition?
Explanation
VEO most commonly is seen in throwers for whom valgus stress across the elbow causes impingement of the posteromedial olecranon tip against the medial wall of the olecranon fossa. With repeated impingement, a bony osteophyte may grow on the olecranon at the site of impingement in this posteromedial region of the olecranon. Bony growth within the olecranon
fossa also has been seen. The distinction between this condition and ulnar collateral ligament injury is difficult to make, but VEO often can be distinguished from UCL injury by determining the exact location of pain a patient experiences. With VEO, the pain typically occurs with direct palpation of the posterior medial tip of the olecranon. The valgus extension overload provocative test also aids in diagnosis. A supervised physical therapy program and arthroscopic surgical decompression when nonsurgical treatment is unsuccessful are typical treatments for this condition.
Locations C and D represent the origin and insertion, respectively, of the elbow medial collateral ligament (MCL) structure, and, although associated MCL pathology can exist in the setting of VEO syndrome, osteophyte formation is not typical in these areas. Location A is the radial head, and although the radiocapitellar joint is a known secondary stabilizer of elbow valgus stress, osteophyte formation in this area is less likely in this clinical scenario.
RECOMMENDED READINGS
8. [Reddy AS, Kvitne RS, Yocum LA, Elattrache NS, Glousman RE, Jobe FW. Arthroscopy of the elbow: a long-term clinical review. Arthroscopy. 2000 Sep;16(6):588-94. ](http://www.ncbi.nlm.nih.gov/pubmed/10976118)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/10976118)
9. [Andrews JR, Craven WM. Lesions of the posterior compartment of the elbow. Clin Sports Med. 1991 Jul;10(3):637-52. Review. PubMed PMID: 1868565.](http://www.ncbi.nlm.nih.gov/pubmed/1868565)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/1868565)
10. [Wilson FD, Andrews JR, Blackburn TA, McCluskey G. Valgus extension overload in the pitching elbow. Am J Sports Med. 1983 Mar-Apr;11(2):83-8. ](http://www.ncbi.nlm.nih.gov/pubmed/6846685)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/6846685)
fossa also has been seen. The distinction between this condition and ulnar collateral ligament injury is difficult to make, but VEO often can be distinguished from UCL injury by determining the exact location of pain a patient experiences. With VEO, the pain typically occurs with direct palpation of the posterior medial tip of the olecranon. The valgus extension overload provocative test also aids in diagnosis. A supervised physical therapy program and arthroscopic surgical decompression when nonsurgical treatment is unsuccessful are typical treatments for this condition.
Locations C and D represent the origin and insertion, respectively, of the elbow medial collateral ligament (MCL) structure, and, although associated MCL pathology can exist in the setting of VEO syndrome, osteophyte formation is not typical in these areas. Location A is the radial head, and although the radiocapitellar joint is a known secondary stabilizer of elbow valgus stress, osteophyte formation in this area is less likely in this clinical scenario.
RECOMMENDED READINGS
8. [Reddy AS, Kvitne RS, Yocum LA, Elattrache NS, Glousman RE, Jobe FW. Arthroscopy of the elbow: a long-term clinical review. Arthroscopy. 2000 Sep;16(6):588-94. ](http://www.ncbi.nlm.nih.gov/pubmed/10976118)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/10976118)
9. [Andrews JR, Craven WM. Lesions of the posterior compartment of the elbow. Clin Sports Med. 1991 Jul;10(3):637-52. Review. PubMed PMID: 1868565.](http://www.ncbi.nlm.nih.gov/pubmed/1868565)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/1868565)
10. [Wilson FD, Andrews JR, Blackburn TA, McCluskey G. Valgus extension overload in the pitching elbow. Am J Sports Med. 1983 Mar-Apr;11(2):83-8. ](http://www.ncbi.nlm.nih.gov/pubmed/6846685)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/6846685)
Question 18High Yield
Figures 1 and 2 are the radiographs of a 55-year-old man who has a 3-year history of right shoulder pain. He has maximized nonoperative management and is interested in operative treatment. He had an open Bankart repair 20 years ago and did well until a few years ago. What is most important to know when deciding on the best surgical treatment for this patient?
Explanation
The radiographs show severe osteoarthritis of the shoulder. The best surgical option would be an arthroplasty. The major determining factor for which type of arthroplasty to choose is the integrity of the rotator cuff tendons. Although the radiographs do not reveal any obvious signs of rotator cuff failure, the patient had had an open Bankart 20 years ago. The integrity of the subscapularis tendon following a previous open shoulder procedure is crucial in deciding which type of arthroplasty to consider. Range of motion and infraspinatus strength do not affect the decision-making process, assuming the rotator cuff is intact. Activity level can be important when deciding whether to proceed with an arthroplasty, but it is not as important as the rotator cuff integrity when choosing which arthroplasty to use.
51
51
Question 19High Yield
Figures 2a and 2b show the clinical photograph and radiograph of a 16-year-old cheerleader who fell on her left lower extremity while performing a pyramid. Following adequate sedation, closed reduction is performed, but an incomplete reduction is noted. What structure is most likely preventing a reduction?
Explanation
The stretched peroneus brevis muscle and tendon follow anterior to the fibula and are most likely incarcerated with reduction. The anterior talofibular ligament is too small to prevent reduction of the ankle joint itself. The extensor digitorum brevis originates from the talus; therefore, it is not involved in the tibiotalar joint. The posterior tibial tendon lies medially and would not be interposed into the ankle joint. Similarly, the anterior tibialis tendon also would not be involved.
REFERENCES: Pehlivan O, Akmaz I, Solakoglu C, et al: Medial peritalar dislocation. Arch Orthop Trauma Surg 2002;122:541-543.
Rivera F, Bertone C, De Martino M, et al: Pure dislocation of the ankle: Three case reports and literature review. Clin Orthop 2001;382:179-184.
REFERENCES: Pehlivan O, Akmaz I, Solakoglu C, et al: Medial peritalar dislocation. Arch Orthop Trauma Surg 2002;122:541-543.
Rivera F, Bertone C, De Martino M, et al: Pure dislocation of the ankle: Three case reports and literature review. Clin Orthop 2001;382:179-184.
Question 20High Yield
A 17-year-old pitcher reports pain over the medial aspect of the elbow that occurs during the acceleration phase of throwing, and it prevents him from throwing at the velocity needed to be competitive. What structure is most likely injured in this patient?


Explanation
DISCUSSION: The anterior bundle of the ulnar collateral ligament of the elbow is the primary constraint to valgus force of the elbow. In pitchers and in overhead athletes, injury to this portion of the ligament results in valgus instability. Reconstruction of the anterior band of the ulnar collateral ligament is necessary in many elite athletic throwers to allow them to return to this competitive activity.
REFERENCES: Azar FM, Andrews JR, Wilk KE, et al: Operative treatment of ulnar collateral ligament injuries of the elbow in athletes. Am J Sports Med 2000;28:16-23.
Cain EL, Dugas JR, Wolf RS, et al: Elbow injuries in throwing athletes: A current concepts review. Am J Sports Med 2003;31:621-635.
Rettig AC, Sherrill C, Snead DS, et al: Nonoperative treatment of ulnar collateral ligament injuries in
throwing athletes. Am J Sports Med 2001 ;29:15-17.
/
Figure 55a Question 55
A 22-year-old male basketball player has had knee pain for the past 3 months. He denies any history of trauma. He has symptoms of catching but no locking. He has rested for 2 weeks but symptoms returned when he resumed sporting activities. Tr and T2-weighted MRI scans are shown in Figures 55a and 55b. What is the most likely diagnosis?
1. #### Locked lateral meniscus tear
2. #### Anterior cruciate ligament tear
3. #### Ganglion cyst of the anterior cruciate ligament
4. #### Synovial osteochondromatosis
5. #### Pigmented villonodular synovitis PREFERRED RESPONSE: 3
DISCUSSION: The MRI scans show a cystic structure within the anterior cruciate ligament. It is fluid filled as seen on the T2 sequence. Ganglion cysts of the cruciate ligaments are rare. The most common presentation is pain with occasional loss of motion. Instability is not a chief complaint and often there is no evidence of laxity on examination. If nonsurgical management fails, arthroscopic debridement of the cyst is the accepted method of treatment.
REFERENCES: Liu SH, Osti L, Mirzayan R: Ganglion cysts of the anterior cruciate ligament: A case report and review of the literature. Arthroscopy 1994; 10:110-112.
Parish EN, Dixon P, Cross MJ: Ganglion cysts of the anterior cruciate ligament: A series of 15 cases. Arthroscopy 2005;21:445-447.
Figure 56
REFERENCES: Azar FM, Andrews JR, Wilk KE, et al: Operative treatment of ulnar collateral ligament injuries of the elbow in athletes. Am J Sports Med 2000;28:16-23.
Cain EL, Dugas JR, Wolf RS, et al: Elbow injuries in throwing athletes: A current concepts review. Am J Sports Med 2003;31:621-635.
Rettig AC, Sherrill C, Snead DS, et al: Nonoperative treatment of ulnar collateral ligament injuries in
throwing athletes. Am J Sports Med 2001 ;29:15-17.
/
Figure 55a Question 55
A 22-year-old male basketball player has had knee pain for the past 3 months. He denies any history of trauma. He has symptoms of catching but no locking. He has rested for 2 weeks but symptoms returned when he resumed sporting activities. Tr and T2-weighted MRI scans are shown in Figures 55a and 55b. What is the most likely diagnosis?
1. #### Locked lateral meniscus tear
2. #### Anterior cruciate ligament tear
3. #### Ganglion cyst of the anterior cruciate ligament
4. #### Synovial osteochondromatosis
5. #### Pigmented villonodular synovitis PREFERRED RESPONSE: 3
DISCUSSION: The MRI scans show a cystic structure within the anterior cruciate ligament. It is fluid filled as seen on the T2 sequence. Ganglion cysts of the cruciate ligaments are rare. The most common presentation is pain with occasional loss of motion. Instability is not a chief complaint and often there is no evidence of laxity on examination. If nonsurgical management fails, arthroscopic debridement of the cyst is the accepted method of treatment.
REFERENCES: Liu SH, Osti L, Mirzayan R: Ganglion cysts of the anterior cruciate ligament: A case report and review of the literature. Arthroscopy 1994; 10:110-112.
Parish EN, Dixon P, Cross MJ: Ganglion cysts of the anterior cruciate ligament: A series of 15 cases. Arthroscopy 2005;21:445-447.
Figure 56
Question 21High Yield
A
B
C
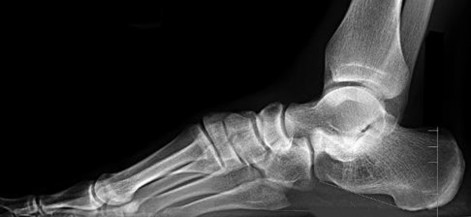
Figures 64a through 64c are the MR images and radiograph of an active 30-year-old man who has been treated for pain in his subtalar joint for 6 months. He has had casting, physical therapy, and bracing but continues to have activity-limiting pain. An injection into the subtalar joint under fluoroscopic guidance temporarily relieved his pain. His best surgical option at this time is
B
C
Figures 64a through 64c are the MR images and radiograph of an active 30-year-old man who has been treated for pain in his subtalar joint for 6 months. He has had casting, physical therapy, and bracing but continues to have activity-limiting pain. An injection into the subtalar joint under fluoroscopic guidance temporarily relieved his pain. His best surgical option at this time is
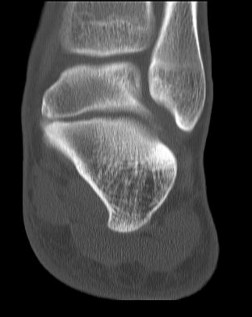
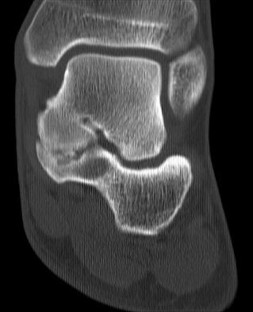
Explanation
When contemplating the causes of subtalar joint degeneration in young patients, an unstable tarsal coalition should be considered in the absence of antecedent trauma. Initial treatment with casting is appropriate because this intervention can relieve symptoms for many patients. There are 2 surgical options for a symptomatic tarsal coalition: bar resection or completion fusion. Risk factors for a poor outcome after bar resection are adult age and a bar that encompasses more than 50% of the middle facet of the subtalar joint. Because this patient has both risk factors, the appropriate procedure is a subtalar fusion.
RECOMMENDED READINGS
[Comfort TK, Johnson LO. Resection for symptomatic talocalcaneal coalition. J PediatrOrthop. 1998 May-Jun;18(3):283-8. PubMed PMID: 9600549. ](http://www.ncbi.nlm.nih.gov/pubmed/9600549)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/9600549)
[Thorpe SW, Wukich DK. Tarsal coalitions in the adult population: does treatment differ from the adolescent? Foot Ankle Clin. 2012 Jun;17(2):195-204. doi: 10.1016/j.fcl.2012.03.004. Epub 2012 Apr 6. Review. PubMed PMID: 22541520. ](http://www.ncbi.nlm.nih.gov/pubmed/22541520)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/22541520)
RECOMMENDED READINGS
[Comfort TK, Johnson LO. Resection for symptomatic talocalcaneal coalition. J PediatrOrthop. 1998 May-Jun;18(3):283-8. PubMed PMID: 9600549. ](http://www.ncbi.nlm.nih.gov/pubmed/9600549)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/9600549)
[Thorpe SW, Wukich DK. Tarsal coalitions in the adult population: does treatment differ from the adolescent? Foot Ankle Clin. 2012 Jun;17(2):195-204. doi: 10.1016/j.fcl.2012.03.004. Epub 2012 Apr 6. Review. PubMed PMID: 22541520. ](http://www.ncbi.nlm.nih.gov/pubmed/22541520)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/22541520)
Question 22High Yield
A right-hand-dominant 45-year-old man sustained an injury to the anterior aspect of his right elbow during sudden elbow flexion while trying to lift a heavy load 3 days ago. He reports the sensation of a sudden, sharp pain at the time of injury, which has since subsided. He has ecchymosis in the anterior and medial elbow regions and has difficulty with resisted forearm supination with the elbow in a flexed position. A diagnosis of an acute distal biceps tendon rupture is made, and, after having a discussion with the patient, surgical treatment is chosen. During surgical reattachment, what is the relationship of the distal biceps tendon within the antecubital fossa to the median nerve and recurrent radial artery before the tendon attaches to the bicipital tuberosity?
Explanation
During surgical repair of a distal biceps tendon rupture, regardless of the surgical approach or technique, an understanding of the regional anatomy is important. The tendon passes distally into the antecubital fossa. The antecubital fossa is defined by the brachioradialis radially and the pronator teres ulnarly. A sheath surrounds the biceps tendon as it passes through the antecubital fossa toward its insertion on the radial tuberosity. The lateral antebrachial cutaneous nerve lies superficially in the subcutaneous tissue of the antecubital fossa. The nerve parallels the brachioradialis. While still superficial, the tendon is contiguous with the lacertus fibrosus that becomes confluent medially with the fascia overlying the flexor-pronator mass. The brachial artery lies just beneath the lacertus fibrosus at the level of the elbow flexion crease. The tendon travels just lateral (radial) to the median nerve within the antecubital fossa and passes posterior (deep) to the recurrent radial artery before it attaches to the radial tuberosity. Full forearm supination allows visualization of the tendinous insertion on the radial tuberosity.
RECOMMENDED READINGS
23. Leslie BM, Ranger H. Biceps tendon and triceps tendon ruptures. In: Baker CL, Plancher KD, eds. _Operative treatment of elbow injuries_. New York: Springer-Verlag; 2002:110-122.
24. [Eames MH, Bain GI, Fogg QA, van Riet RP. Distal biceps tendon anatomy: a cadaveric study. J Bone Joint Surg Am. 2007 May;89(5):1044-9. PubMed PMID: 17473142. ](http://www.ncbi.nlm.nih.gov/pubmed/17473142)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/17473142)
RECOMMENDED READINGS
23. Leslie BM, Ranger H. Biceps tendon and triceps tendon ruptures. In: Baker CL, Plancher KD, eds. _Operative treatment of elbow injuries_. New York: Springer-Verlag; 2002:110-122.
24. [Eames MH, Bain GI, Fogg QA, van Riet RP. Distal biceps tendon anatomy: a cadaveric study. J Bone Joint Surg Am. 2007 May;89(5):1044-9. PubMed PMID: 17473142. ](http://www.ncbi.nlm.nih.gov/pubmed/17473142)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/17473142)
Question 23High Yield
A 32-year-old man underwent a total medial meniscectomy 2 years ago. He now reports pain and recurrent swelling for the past 3 months. Work-up includes full standing hip-knee-ankle radiographs, standing AP radiographs of both knees in full extension, an axial view of the patellofemoral joint, and a 45-degree flexion AP radiograph. Contraindication to meniscus allograft transplantation includes which of the following?
Explanation
DISCUSSION: Flattening of the femoral condyles indicates the onset of significant arthritis of the joint
and is a contraindication to meniscus allograft transplantation. Criteria to proceed with allograft transplantation includes prior total meniscectomy, age of 50 years or younger, BMI of less than 30, clinical symptoms of pain in the involved tibiofemoral compartment, 2 mm or more of tibiofemoral joint space on a 45-degree weight-bearing AP radiograph, ligamentous stability, normal alignment, and no radiographic evidence of advanced arthrosis. Recurrent effusions are associated with chronic meniscus deficiency, and is one criteria for meniscal transplantation. High tibial osteotomy is often considered in conjunction with meniscal transplantation to correct tibiofemoral malalignment.
REFERENCES: Noyes FR, Barber-Westin SD: Meniscus transplantation: Indications, techniques, clinical outcomes. Instr Course Lect 2005;54:341-353.
Kang RW, Lattermann C, Cole BJ: Allograft meniscus transplantation: Background, indications, techniques, and outcomes. J Knee Surg 2006;19:220-230.
and is a contraindication to meniscus allograft transplantation. Criteria to proceed with allograft transplantation includes prior total meniscectomy, age of 50 years or younger, BMI of less than 30, clinical symptoms of pain in the involved tibiofemoral compartment, 2 mm or more of tibiofemoral joint space on a 45-degree weight-bearing AP radiograph, ligamentous stability, normal alignment, and no radiographic evidence of advanced arthrosis. Recurrent effusions are associated with chronic meniscus deficiency, and is one criteria for meniscal transplantation. High tibial osteotomy is often considered in conjunction with meniscal transplantation to correct tibiofemoral malalignment.
REFERENCES: Noyes FR, Barber-Westin SD: Meniscus transplantation: Indications, techniques, clinical outcomes. Instr Course Lect 2005;54:341-353.
Kang RW, Lattermann C, Cole BJ: Allograft meniscus transplantation: Background, indications, techniques, and outcomes. J Knee Surg 2006;19:220-230.
Question 24High Yield
In the surgical correction of a clubfoot, the following clinical or radiographic finding indicates that a child should have a plantar release:
Explanation
Plantarflexion of the first ray, especially if the first ray is not colinear with the talus on the lateral radiograph, should serve as an indication for a plantar release.
Anterior extrusion of the talus is common because of the tightness of the Achilles tendon and the posterior capsule. Inferior subluxation of the calcaneocuboid joint is not a feature of clubfoot.
Medial subluxation of the calcaneocuboid joint, in combination with the clinical appearance of a curved lateral border of the foot, should serve as an indication for a lateral release, not a plantar release.
Inability to dorsiflex the ankle is an indication for a posterior release.
Anterior extrusion of the talus is common because of the tightness of the Achilles tendon and the posterior capsule. Inferior subluxation of the calcaneocuboid joint is not a feature of clubfoot.
Medial subluxation of the calcaneocuboid joint, in combination with the clinical appearance of a curved lateral border of the foot, should serve as an indication for a lateral release, not a plantar release.
Inability to dorsiflex the ankle is an indication for a posterior release.
Question 25High Yield
A 70-year-old woman who underwent total knee replacement 18 months ago has had 3 weeks of moderate
drainage from a previously healed wound. What is the most appropriate treatment?
drainage from a previously healed wound. What is the most appropriate treatment?
Explanation
This situation represents a definitively and chronically infected knee replacement. Antibiotic therapy alone might suppress the infection but would not eradicate it. Debridement and polyethylene exchange would be appropriate treatment for an early postoperative infection. The treatment of choice is to perform a two-stage debridement and reconstruction. Although not among the listed choices, an aspiration or culture could be done presurgically and might help clinicians identify the best antibiotics to treat the condition. Antibiotic selection would not affect the need for the two-stage reconstruction, however.
Question 26High Yield
A 14-year-old girl with a history of aortic root dilation and FBN1 gene mutation and arachnodactyly presents with a thoracolumbar curve of 55°. When compared with patients with adolescent idiopathic scoliosis, the expected outcome with posterior spinal fusion and instrumentation of this patient's scoliosis would be (a) higher
Explanation
■
Marfan syndrome is an autosomal dominant disorder caused by a defect in the FBN1 gene encoding fibrillin1. The main orthopaedic feature of Marfan syndrome is overgrowth of the long bones and related tall stature, chest deformities (pectus carinatum or excavatum), arachnodactyly, protrusio acetabuli, flatfeet, scoliosis and dural ectasia.
Scoliosis in Marfan patients tends to progress rapidly, be less responsive to bracing, and have more revisions and complications as a result of higher rates of cerebrospinal fluid leaks, fixation failure, spine fracture, distal degeneration, proximal add on, and dural ectasia. Fixation failure is likely attributable to osteopenia, dysplastic pedicles, and dysplastic lamina. Dural ectasia, or enlargement of the dural sac, is a highly specific diagnostic feature of Marfan syndrome and is present in more than two-thirds of patients. As the dural sac balloons, it may erode the surrounding bone, which already is weakened by the genetic mutation. These changes pose a challenge to surgical fixation and create a high likelihood of fracture and dural injury. Although some studies report higher blood loss and longer surgical times than in patients with adolescent idiopathic scoliosis, other studies dispute this. Neurological complication and pseudoarthrosis rates have been similar between these two groups of patients.
Marfan syndrome is an autosomal dominant disorder caused by a defect in the FBN1 gene encoding fibrillin1. The main orthopaedic feature of Marfan syndrome is overgrowth of the long bones and related tall stature, chest deformities (pectus carinatum or excavatum), arachnodactyly, protrusio acetabuli, flatfeet, scoliosis and dural ectasia.
Scoliosis in Marfan patients tends to progress rapidly, be less responsive to bracing, and have more revisions and complications as a result of higher rates of cerebrospinal fluid leaks, fixation failure, spine fracture, distal degeneration, proximal add on, and dural ectasia. Fixation failure is likely attributable to osteopenia, dysplastic pedicles, and dysplastic lamina. Dural ectasia, or enlargement of the dural sac, is a highly specific diagnostic feature of Marfan syndrome and is present in more than two-thirds of patients. As the dural sac balloons, it may erode the surrounding bone, which already is weakened by the genetic mutation. These changes pose a challenge to surgical fixation and create a high likelihood of fracture and dural injury. Although some studies report higher blood loss and longer surgical times than in patients with adolescent idiopathic scoliosis, other studies dispute this. Neurological complication and pseudoarthrosis rates have been similar between these two groups of patients.
Question 27High Yield
22
The lesser or small saphenous vein passes along the sural nerve in the mid calf
The lesser or small saphenous vein passes along the sural nerve in the mid calf
Explanation
The sural nerve is at risk when incisions are placed near the Achilles tendon musculotendinous junction of the posterior calf. The nerve, which can be easily identified when the vein is visualized, is at risk during Achilles tendon recession procedures, and the vein provides a landmark with which to identify the nerve.
RECOMMENDED READINGS
1. [Eid EM, Hegazy AM. Anatomical variations of the human sural nerve and its role in clinical and surgical procedures .Clin Anat.2011Mar;24(2):237-45.doi: 10.1002/ ca.21068. Epub 2010 Oct 14.PubMed PMID: 20949489.](http://www.ncbi.nlm.nih.gov/pubmed/20949489)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/20949489)
2. Hoppenfeld S, deBoer P, Buckley R. Surgical Exposures in Orthopaedics. The Anatomic Approach. Philadelphia, PA: Lippincott Williams &Wilkins 2009:585-622.
3. [Aktan Ikiz ZA, Uçerler H, Bilge O. The anatomic features of the sural nerve with an emphasis on its clinical importance. Foot Ankle Int. 2005 Jul;26(7):560-7. PubMed PMID: 16045849.](http://www.ncbi.nlm.nih.gov/pubmed/16045849)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/16045849)
RECOMMENDED READINGS
1. [Eid EM, Hegazy AM. Anatomical variations of the human sural nerve and its role in clinical and surgical procedures .Clin Anat.2011Mar;24(2):237-45.doi: 10.1002/ ca.21068. Epub 2010 Oct 14.PubMed PMID: 20949489.](http://www.ncbi.nlm.nih.gov/pubmed/20949489)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/20949489)
2. Hoppenfeld S, deBoer P, Buckley R. Surgical Exposures in Orthopaedics. The Anatomic Approach. Philadelphia, PA: Lippincott Williams &Wilkins 2009:585-622.
3. [Aktan Ikiz ZA, Uçerler H, Bilge O. The anatomic features of the sural nerve with an emphasis on its clinical importance. Foot Ankle Int. 2005 Jul;26(7):560-7. PubMed PMID: 16045849.](http://www.ncbi.nlm.nih.gov/pubmed/16045849)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/16045849)
Question 28High Yield
-What is the optimal initial treatment for his orthopaedic injuries?
Explanation
No detailed explanation provided for this question.
Question 29High Yield
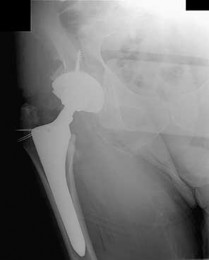
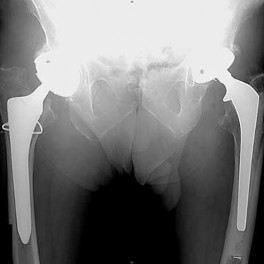
What is the most likely explanation for the change between the initial intraoperative radiograph (Figure 11a) and the radiograph taken 4 weeks after surgery (Figure 11b) in an 87-year-old man who underwent primary hip replacement for osteoarthritis?
Explanation
The image demonstrates subsidence of the femoral implant. The implant subsided because it did not have good initial stability. The tapered femoral implant was placed after initial preparation for an anatomic femoral stem. A limited, nondisplaced femoral neck fracture was encountered during the procedure and treated. Two advantages of tapered stems are the efficient transfer of stress to the proximal femur and the ability to accommodate some subsidence to achieve enhanced stability. Although subsidence of a tapered stem to a more stable position can produce a good result, quality of metaphyseal bone should be considered. Attention to surgical technique remains important to optimize component stability for biological fixation.
RECOMMENDED READINGS
1. Savory CG, Hamilton WG, Engh CA Sr, Della Valle CJ, Rosenberg AG, Galante JO. 15 Hip designs. In: Barrack RL, Booth RE Jr, Lonner JH, McCarthy JC, Mont MA, Rubash HE, eds. Orthopaedic Knowledge Update: Hip and Knee Reconstruction 3.
Rosemont, IL: American Academy of Orthopaedic Surgeons; 2006:345-368.
2. Blaha JD, Borus TA. Press-fit femoral components. In: Callaghan J, Rosenberg A, and Rubash H, eds The Adult Hip. 2nd ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2007:1036-1043.
RECOMMENDED READINGS
1. Savory CG, Hamilton WG, Engh CA Sr, Della Valle CJ, Rosenberg AG, Galante JO. 15 Hip designs. In: Barrack RL, Booth RE Jr, Lonner JH, McCarthy JC, Mont MA, Rubash HE, eds. Orthopaedic Knowledge Update: Hip and Knee Reconstruction 3.
Rosemont, IL: American Academy of Orthopaedic Surgeons; 2006:345-368.
2. Blaha JD, Borus TA. Press-fit femoral components. In: Callaghan J, Rosenberg A, and Rubash H, eds The Adult Hip. 2nd ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2007:1036-1043.
Question 30High Yield
A unilateral "piano key" sign, indicates
Explanation
The piano key sign is a demonstration of instability at the DRUJ, typically seen after healing from a distal radius fracture with an associated ulnar styloid fracture (as in this case) or other wrist injury. The hand is pushed down against a table top, and the distal radius translates dorsally (with the distal ulna apparently moving volarly). In fact, the distal radius is the mobile segment, while the distal ulna is fixed in space. Treatment involves repair or reconstruction of the foveal insertion of the triangular fibrocartilage complex (TFCC) and distal radioulnar ligaments. This type of instability is also common in malunions of the distal radius or distal one-third of the radial shaft (Galeazzi-type fractures). In malunions, DRUJ instability can be treated with a corrective osteotomy of the distal radius to restore the anatomic relationship between the distal ulna and the distal radius at the DRUJ. Radiocarpal and midcarpal instability do not involve the DRUJ. Disruption of the interosseous membrane (in isolation, with intact distal radioulnar ligaments and an intact TFCC) does not lead to translational instability of the DRUJ. Although hypermobility syndrome may lead to ligamentous laxity, it does not lead to unilateral DRUJ instability.
Question 31High Yield
Which of the following describes crevice corrosion:
Explanation
C revice corrosion occurs at the sites of a surface defect in a metal implant. At these defects, changes in pH and electrolyte concentrations cause corrosion.
C ommon examples of crevice corrosion include:
At the interface between an uncemented acetabular component and the cancellous screws (at the contact point where the head of the screw is countersunk into the acetabular shell)
At the interface between a screw head and the plate at the point where the screw head contacts the plate
The other responses refer to:
Galvanic corrosion: Impurities within a metal implant Galvanic corrosion: At sites of electrochemical gradients Fretting corrosion: Relative micromotion under load
Oxidative degradation: Free-radical generation during air sterilization
C orrect Answer: Differences in oxygen tension causing pH and electrolyte changes
C ommon examples of crevice corrosion include:
At the interface between an uncemented acetabular component and the cancellous screws (at the contact point where the head of the screw is countersunk into the acetabular shell)
At the interface between a screw head and the plate at the point where the screw head contacts the plate
The other responses refer to:
Galvanic corrosion: Impurities within a metal implant Galvanic corrosion: At sites of electrochemical gradients Fretting corrosion: Relative micromotion under load
Oxidative degradation: Free-radical generation during air sterilization
C orrect Answer: Differences in oxygen tension causing pH and electrolyte changes
Question 32High Yield
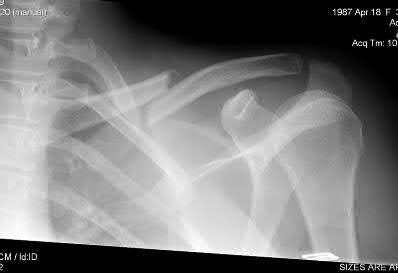
A 22-year-old healthy left hand dominant male presents to the ED with left shoulder pain after falling from an ATV. Figure A is the radiograph of his left clavicle. He is neurovascularly intact and there is no evidence of skin tenting or open fracture. Which of the following most predisposes this patient to nonunion?
Explanation
Displaced clavicle fractures are associated with higher rates of nonunion.
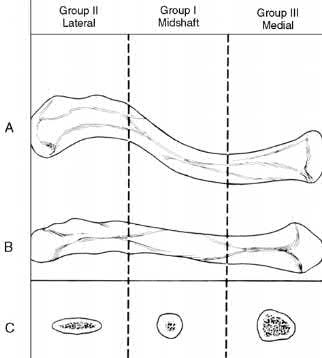
Nonunion occurs in roughly 5-6% of clavicle fractures and can result in slower functional return, poor cosmesis and muscle fatigability. Clavicle fractures can be sub-classified using the Allman classification into medial, diaphyseal, and lateral injuries (Illustration A). The Neer classification for diaphyseal injuries describes fractures as "nondisplaced" (less than 100% displacement) and "displaced" (greater than 100% displacement).
Robinson et al. performed a prospective cohort study to identify risk factors for nonunion after nonoperative management of clavicle fractures. The overall nonunion rate was 6.2% and was highest in lateral third fractures (11.5%).
Diaphyseal fractures had the lowest nonunion rate (4.5%). Additionally, the authors found that the risk for nonunion was increased by advancing age, female gender, fracture displacement, and comminution.
Jorgensen et al. performed a systemic review of the literature looking for predictors of non-union and malunion in mid shaft clavicle fractures treated non-operatively. They found fracture comminution, displacement, older age, female gender, and the presence of smoking to be his factors for non-union. Of these, displacement was the most likely factor that can be used to predict nonunion.
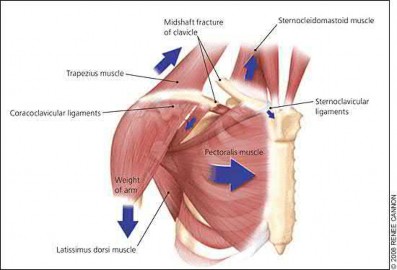
Figure A demonstrates a displaced left clavicle diaphyseal fracture. Note that the medial fragment is displaced superiorly by the deforming force of the sternocleidomastoid. Illustration A represents the Allman classification.
Illustration B demonstrates the deforming forces acting on the clavicle.
Incorrect Answers:
Answer 1: Diaphyseal fractures were demonstrated to have the lowest rate of nonunion when compared to lateral third fractures and medial clavicle fractures.
Answer 3: Advancing age was found to be an independent predictor of nonunion.
Answer 4: Female gender was found to be an independent predictor of nonunion.
Answer 5: Injury to the dominant hand was not found to be associated with an increased risk of non-union.
Nonunion occurs in roughly 5-6% of clavicle fractures and can result in slower functional return, poor cosmesis and muscle fatigability. Clavicle fractures can be sub-classified using the Allman classification into medial, diaphyseal, and lateral injuries (Illustration A). The Neer classification for diaphyseal injuries describes fractures as "nondisplaced" (less than 100% displacement) and "displaced" (greater than 100% displacement).
Robinson et al. performed a prospective cohort study to identify risk factors for nonunion after nonoperative management of clavicle fractures. The overall nonunion rate was 6.2% and was highest in lateral third fractures (11.5%).
Diaphyseal fractures had the lowest nonunion rate (4.5%). Additionally, the authors found that the risk for nonunion was increased by advancing age, female gender, fracture displacement, and comminution.
Jorgensen et al. performed a systemic review of the literature looking for predictors of non-union and malunion in mid shaft clavicle fractures treated non-operatively. They found fracture comminution, displacement, older age, female gender, and the presence of smoking to be his factors for non-union. Of these, displacement was the most likely factor that can be used to predict nonunion.
Figure A demonstrates a displaced left clavicle diaphyseal fracture. Note that the medial fragment is displaced superiorly by the deforming force of the sternocleidomastoid. Illustration A represents the Allman classification.
Illustration B demonstrates the deforming forces acting on the clavicle.
Incorrect Answers:
Answer 1: Diaphyseal fractures were demonstrated to have the lowest rate of nonunion when compared to lateral third fractures and medial clavicle fractures.
Answer 3: Advancing age was found to be an independent predictor of nonunion.
Answer 4: Female gender was found to be an independent predictor of nonunion.
Answer 5: Injury to the dominant hand was not found to be associated with an increased risk of non-union.
Question 33High Yield
A 20-year-old male military recruit reports a 5-day history of progressive deep groin pain that is made worse with weight-bearing activities and running. His initial coronal T2-weighted MRI scan is shown in Figure 75. His initial treatment should consist of which of the following?
Explanation
DISCUSSION: The MRI scan findings and patient history demonstrate a compression-sided femoral neck stress fracture. The stress fracture on the coronal MRI scan involves about one third of the width of the femoral neck. Surgical treatment would be recommended for tension-sided fractures of the femoral neck. The most appropriate initial treatment is protected weight bearing, with close examination and imaging follow-up. Skeletal traction is not currently used for nondisplaced femoral neck stress fractures, and there is no indication
for open reduction and internal fixation. There is no documented role for pulsed ultrasound or calcium supplements in the acute treatment of stress fractures.
REFERENCES: Shin AY, Morin WD, Gorman JD, et al: The superiority of magnetic resonance imaging in differentiating the cause of hip pain in endurance athletes. Am J Sports Med 1996;24:168-176.
Pihlajamaki HK, Ruohola JP, Weckstrom M, et al: Long-term outcome of undisplaced fatigue fractures of the
femoral neck in young male adults. J Bone Joint Surg Br 2006;88:1574-1579.
Valimaki VV, Alfthan H, Lehmuskallio E, et al: Risk factors for clinical stress fractures in male military recruits: A prospective cohort study. Bone 2005;37:267-273.
for open reduction and internal fixation. There is no documented role for pulsed ultrasound or calcium supplements in the acute treatment of stress fractures.
REFERENCES: Shin AY, Morin WD, Gorman JD, et al: The superiority of magnetic resonance imaging in differentiating the cause of hip pain in endurance athletes. Am J Sports Med 1996;24:168-176.
Pihlajamaki HK, Ruohola JP, Weckstrom M, et al: Long-term outcome of undisplaced fatigue fractures of the
femoral neck in young male adults. J Bone Joint Surg Br 2006;88:1574-1579.
Valimaki VV, Alfthan H, Lehmuskallio E, et al: Risk factors for clinical stress fractures in male military recruits: A prospective cohort study. Bone 2005;37:267-273.
Question 34High Yield
Slide 1
A 24-year-old man presents with a short forearm and a hand deformity. The patient is otherwise healthy with no other congenital defects. The clinical appearance of his forearm is shown (Slide). Your diagnosis is:
A 24-year-old man presents with a short forearm and a hand deformity. The patient is otherwise healthy with no other congenital defects. The clinical appearance of his forearm is shown (Slide). Your diagnosis is:
Explanation
This is a classic appearance of a radial club hand, which is often referred to as preaxial longitudinal deficiency. Ulnar club hand and postaxial longitudinal deficiency are synonymous.
Question 35High Yield
The MRI scan of the shoulder shown in Figure 2 was performed with the arm in abduction and external rotation. The image reveals what condition?
Explanation
Internal impingement of the shoulder is now a well-recognized cause of shoulder pain in the throwing athlete. First described by Walch and associates, it involves contact of the rotator cuff and labrum in the maximally externally rotated and abducted shoulder, such as in the late cocking phase of the throwing motion. Schickendantz and associates have shown this contact to be physiologic in most patients and becoming pathologic with repetitive overhead activity.
REFERENCES: Schickendantz MS, Ho CP, Keppler L, Shaw BD: MR imaging of the thrower’s shoulder: Internal impingement, latissimus dorsi/subscapularis strains, and related injuries. Magn Reson Imaging Clin N Am 1999;7:39-49.
Walch G, Boileau P, Noel E, et al: Impingement of the deep surface of the supraspinatus tendon on the posterosuperior glenoid rim: An arthroscopic study. J Shoulder Elbow Surg 1992;1:238-245.
McFarland EG, Hsu CY, Neira C, O’Neil O: Internal impingement of the shoulder: A clinical and arthroscopic analysis. J Shoulder Elbow Surg 1999;8:458-460.
REFERENCES: Schickendantz MS, Ho CP, Keppler L, Shaw BD: MR imaging of the thrower’s shoulder: Internal impingement, latissimus dorsi/subscapularis strains, and related injuries. Magn Reson Imaging Clin N Am 1999;7:39-49.
Walch G, Boileau P, Noel E, et al: Impingement of the deep surface of the supraspinatus tendon on the posterosuperior glenoid rim: An arthroscopic study. J Shoulder Elbow Surg 1992;1:238-245.
McFarland EG, Hsu CY, Neira C, O’Neil O: Internal impingement of the shoulder: A clinical and arthroscopic analysis. J Shoulder Elbow Surg 1999;8:458-460.
Question 36High Yield
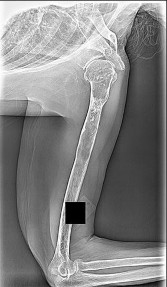
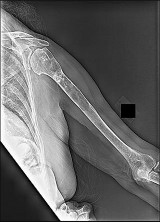
Figures 93a through 93f are radiographs, selected MR imaging sequences, and biopsy specimens of the left humerus of a 76-year-old woman who has experienced long-term left arm pain. She has received previous treatment for osteoarthritis of her left shoulder with nonsteroidal anti-inflammatory drugs and an intra-articular corticosteroid injection for her rotator cuff arthropathy. Recent staging studies show no evidence of metastatic disease. What is the most appropriate next treatment?
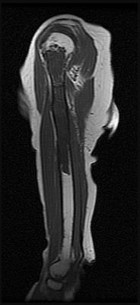

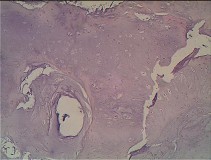
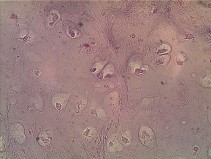
Explanation
This patient’s radiographs, MR imaging, and histologic examination are diagnostic for low-grade chondrosarcoma, which is treated with surgery alone. In this patient, the tumor is entirely intramedullary. Both wide resection and extended intralesional curettage with intraoperative surgical adjuvant treatment are treatment options. Chemotherapy and radiation are not beneficial in the treatment of low-grade chondrosarcoma.
Endoprosthetic reconstruction using a reverse shoulder arthroplasty may be employed when the rotator cuff is deficient for older patients with neoplasms of the proximal humerus. Allograft-prosthetic composite reverse shoulder arthroplasty also has been used with early success.
RECOMMENDED READINGS
92. [Mermerkaya MU, Bekmez S, Karaaslan F, Danisman M, Kosemehmetoglu K, Gedikoglu G, Ayvaz M, Tokgozoglu AM. Intralesional curettage and cementation for low-grade chondrosarcoma of long bones: retrospective study and literature review. World J Surg Oncol. 2014 Nov 10;12:336. doi: 10.1186/1477-7819-12-336. Review. PubMed PMID: 25382793.](http://www.ncbi.nlm.nih.gov/pubmed/25382793)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/25382793)
93. [Di Giorgio L, Touloupakis G, Vitullo F, Sodano L, Mastantuono M, Villani C. Intralesional curettage, with phenol and cement as adjuvants, for low-grade intramedullary chondrosarcoma of the long bones. Acta Orthop Belg. 2011 Oct;77(5):666-9. PubMed PMID: 22187844. ](http://www.ncbi.nlm.nih.gov/pubmed/22187844)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/22187844)
94. [Chalmers PN, Keener JD. Expanding roles for reverse shoulder arthroplasty. Curr Rev Musculoskelet Med. 2016 Mar;9(1):40-8. doi: 10.1007/s12178-016-9316-0. PubMed PMID: 26803609. ](http://www.ncbi.nlm.nih.gov/pubmed/26803609)[View](http://www.ncbi.nlm.nih.gov/pubmed/26803609)
[Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/26803609)
95. [King JJ, Nystrom LM, Reimer NB, Gibbs CP Jr, Scarborough MT, Wright TW. Allograft-prosthetic composite reverse total shoulder arthroplasty for reconstruction of proximal humerus tumor resections. J Shoulder Elbow Surg. 2016 Jan;25(1):45-54. doi: 10.1016/j.jse.2015.06.021. Epub 2015 Aug 6. PubMed PMID: 26256013. ](http://www.ncbi.nlm.nih.gov/pubmed/26256013)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/26256013)
Endoprosthetic reconstruction using a reverse shoulder arthroplasty may be employed when the rotator cuff is deficient for older patients with neoplasms of the proximal humerus. Allograft-prosthetic composite reverse shoulder arthroplasty also has been used with early success.
RECOMMENDED READINGS
92. [Mermerkaya MU, Bekmez S, Karaaslan F, Danisman M, Kosemehmetoglu K, Gedikoglu G, Ayvaz M, Tokgozoglu AM. Intralesional curettage and cementation for low-grade chondrosarcoma of long bones: retrospective study and literature review. World J Surg Oncol. 2014 Nov 10;12:336. doi: 10.1186/1477-7819-12-336. Review. PubMed PMID: 25382793.](http://www.ncbi.nlm.nih.gov/pubmed/25382793)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/25382793)
93. [Di Giorgio L, Touloupakis G, Vitullo F, Sodano L, Mastantuono M, Villani C. Intralesional curettage, with phenol and cement as adjuvants, for low-grade intramedullary chondrosarcoma of the long bones. Acta Orthop Belg. 2011 Oct;77(5):666-9. PubMed PMID: 22187844. ](http://www.ncbi.nlm.nih.gov/pubmed/22187844)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/22187844)
94. [Chalmers PN, Keener JD. Expanding roles for reverse shoulder arthroplasty. Curr Rev Musculoskelet Med. 2016 Mar;9(1):40-8. doi: 10.1007/s12178-016-9316-0. PubMed PMID: 26803609. ](http://www.ncbi.nlm.nih.gov/pubmed/26803609)[View](http://www.ncbi.nlm.nih.gov/pubmed/26803609)
[Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/26803609)
95. [King JJ, Nystrom LM, Reimer NB, Gibbs CP Jr, Scarborough MT, Wright TW. Allograft-prosthetic composite reverse total shoulder arthroplasty for reconstruction of proximal humerus tumor resections. J Shoulder Elbow Surg. 2016 Jan;25(1):45-54. doi: 10.1016/j.jse.2015.06.021. Epub 2015 Aug 6. PubMed PMID: 26256013. ](http://www.ncbi.nlm.nih.gov/pubmed/26256013)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/26256013)
Question 37High Yield
A 45-year-old woman with a history of rheumatoid arthritis has C1-C2 instability with neurologic deterioration. Her posterior atlanto-dens interval is 10 mm. Which fixation technique will be the most biomechanically sound to facilitate fusion across the atlanto-axial junction?
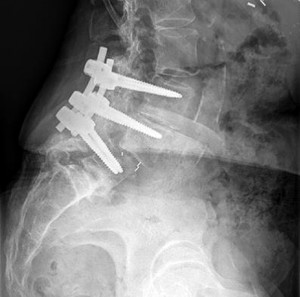
Explanation
C1-C2 transarticular screw fixation is 10-fold stiffer than wiring constructs, particularly in rotation; eliminates the need for postsurgical halo use; and is associated with reported fusion rates to a maximum of 100% for bilateral screws and 95% for unilateral fixation. All of the other fusion techniques mentioned are associated with a pseudarthrosis rate of at least 30%.
RECOMMENDED READINGS
[Stock GH, Vaccaro AR, Brown AK, Anderson PA. Contemporary posterior occipital fixation. J Bone Joint Surg Am. 2006 Jul;88(7):1642-9. PubMed PMID: 16841419. ](http://www.ncbi.nlm.nih.gov/pubmed/16841419)[View Abstract at](http://www.ncbi.nlm.nih.gov/pubmed/16841419)[ ](http://www.ncbi.nlm.nih.gov/pubmed/16841419)[PubMed](http://www.ncbi.nlm.nih.gov/pubmed/16841419)
[Sim HB, Lee JW, Park JT, Mindea SA, Lim J, Park J. Biomechanical evaluations of various c1-c2 posterior fixation techniques. Spine (Phila Pa 1976). 2011 Mar 15;36(6):E401-7. doi: 10.1097/BRS.0b013e31820611ba. PubMed PMID: 21372651. ](http://www.ncbi.nlm.nih.gov/pubmed/21372651)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/21372651)
CLINICAL SITUATION FOR QUESTIONS 37 THROUGH 43
Figure 37 is the lateral radiograph of a 71-year-old woman who has pain with ambulation that improves when she sits down. She had similar symptoms 2 years earlier when she underwent an L3-L5 posterior spinal fusion. Upon examination she has good range of hip and knee motion, 5/5 motor function, and normal sensation of her lower extremities. She has negative bilateral straight-leg raise findings and her knees slightly flex to stand upright
37
RECOMMENDED READINGS
[Stock GH, Vaccaro AR, Brown AK, Anderson PA. Contemporary posterior occipital fixation. J Bone Joint Surg Am. 2006 Jul;88(7):1642-9. PubMed PMID: 16841419. ](http://www.ncbi.nlm.nih.gov/pubmed/16841419)[View Abstract at](http://www.ncbi.nlm.nih.gov/pubmed/16841419)[ ](http://www.ncbi.nlm.nih.gov/pubmed/16841419)[PubMed](http://www.ncbi.nlm.nih.gov/pubmed/16841419)
[Sim HB, Lee JW, Park JT, Mindea SA, Lim J, Park J. Biomechanical evaluations of various c1-c2 posterior fixation techniques. Spine (Phila Pa 1976). 2011 Mar 15;36(6):E401-7. doi: 10.1097/BRS.0b013e31820611ba. PubMed PMID: 21372651. ](http://www.ncbi.nlm.nih.gov/pubmed/21372651)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/21372651)
CLINICAL SITUATION FOR QUESTIONS 37 THROUGH 43
Figure 37 is the lateral radiograph of a 71-year-old woman who has pain with ambulation that improves when she sits down. She had similar symptoms 2 years earlier when she underwent an L3-L5 posterior spinal fusion. Upon examination she has good range of hip and knee motion, 5/5 motor function, and normal sensation of her lower extremities. She has negative bilateral straight-leg raise findings and her knees slightly flex to stand upright
37
Question 38High Yield
Which of the following tumor metastasizes to lungs:
Explanation
Squamous cell carcinoma and basal cell carcinoma do not commonly metastasize to the lungs. Actinic keratoses are premalignant lesions that progress into squamous cell carcinomas. Schwannomas are common benign nerve tumors.
Question 39High Yield
When a patient has acute or chronic anterior shoulder instability, a bony or glenoid reconstructive procedure should be considered in which clinical setting?
Explanation
HAGL lesions may be initially treated without surgery. Recurrent instability in the setting of a HAGL lesion may be treated with a soft-tissue repair. A nonengaging or nontracking Hill-Sachs lesion may be treated with an anterior soft-tissue (Bankart) repair. A tracking or engaging lesion may be treated with a bony glenoid procedure or a soft-tissue procedure plus remplissage. An ALPSA lesion may be treated with a soft-tissue procedure unless it is associated with a glenoid bony defect exceeding 25%. A glenoid bony defect exceeding 25% is associated with substantially higher recurrence than defects smaller than 20%, and consideration for bony glenoid reconstruction is advised.
RECOMMENDED READINGS
73. [Beran MC, Donaldson CT, Bishop JY. Treatment of chronic glenoid defects in the setting of recurrent anterior shoulder instability: a systematic review. J Shoulder Elbow Surg. 2010 Jul;19(5):769-80. doi: 10.1016/j.jse.2010.01.011. Epub 2010 Apr 14. Review. PubMed PMID: 20392650. ](http://www.ncbi.nlm.nih.gov/pubmed/20392650)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/20392650)
74. [Boileau P, Villalba M, Héry JY, Balg F, Ahrens P, Neyton L. Risk factors for recurrence of shoulder instability after arthroscopic Bankart repair. J Bone Joint Surg Am. 2006 Aug;88(8):1755-63. PubMed PMID: 16882898. ](http://www.ncbi.nlm.nih.gov/pubmed/16882898)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/16882898)
RECOMMENDED READINGS
73. [Beran MC, Donaldson CT, Bishop JY. Treatment of chronic glenoid defects in the setting of recurrent anterior shoulder instability: a systematic review. J Shoulder Elbow Surg. 2010 Jul;19(5):769-80. doi: 10.1016/j.jse.2010.01.011. Epub 2010 Apr 14. Review. PubMed PMID: 20392650. ](http://www.ncbi.nlm.nih.gov/pubmed/20392650)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/20392650)
74. [Boileau P, Villalba M, Héry JY, Balg F, Ahrens P, Neyton L. Risk factors for recurrence of shoulder instability after arthroscopic Bankart repair. J Bone Joint Surg Am. 2006 Aug;88(8):1755-63. PubMed PMID: 16882898. ](http://www.ncbi.nlm.nih.gov/pubmed/16882898)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/16882898)
Question 40High Yield
Figure 1 is the radiograph of an 18-year-old right-hand-dominant man who has pain and stiffness 3 months after sustaining an injury to his dominant ring finger while playing basketball. An examination reveals significant proximal interphalangeal (PIP) joint swelling with active and passive PIP joint motion of 15/40 degrees of flexion. What is the best next step?
---
---
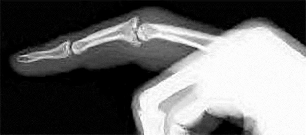
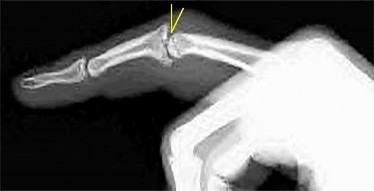
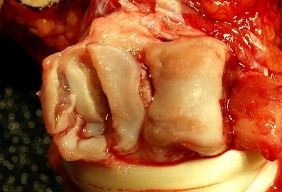
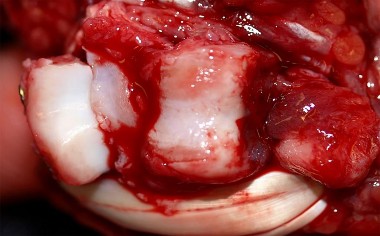




Explanation
This patient has a subacute PIP joint dorsal fracture dislocation with involvement of 50% to 60% of the palmar articular surface of the base of P2. A "V sign" (Figure 2) is evident, indicating dorsal subluxation of the joint. In some cases, an ORIF is possible, but substantial comminution often precludes proper restoration of the critical volar buttress. Therapy is not the answer because the joint is dorsally subluxated and must be corrected. Dynamic external fixation on its own would not result in a reduced joint. The hemi-hamate autograft has proven useful in this type of scenario and serves to restore the volar buttress of P2 using an osteochondral autograft harvested from the distal articular aspect of the hamate at its articulation with the fourth/fifth metacarpal bases. Intraoperative clinical photographs and a postsurgical radiograph are shown in Figures 3 through 5.
---
---
---
---
---
---
---
---
Question 41High Yield
A 75-lb, 10-year-old boy fell and is now unable to walk and has left thigh pain and deformity. He has no other injuries and is otherwise healthy. Radiographs are shown in Figures 93a and 93b. What is the most appropriate management?
Explanation
DISCUSSION: The fracture is best treated with elastic nails. Traction and a spica cast could be used but requires more time in the hospital and the cast increases family inconvenience for 4 to 6 weeks. There are lateral entry nails that could be used, but to date there is still not a long enough follow-up to determine the risk of osteonecrosis. External fixation may be an alternative for a patient with multiple injuries or extensive soft-tissue damage. Open plating could also be used but in the midshaft location, flexible nails are the most appropriate choice and offer the fewest number of potential complications.
REFERENCES: Abel MF (ed): Orthopaedic Knowledge Update: Pediatrics 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2006, pp 271-279.
Buechsenschuetz KE, Mehlman CT, Shaw KJ, et al: Femoral shaft fractures in children: Traction and
casting versus elastic stable intramedullary nailing. J Trauma 2002;53:914-921.
• b
2010 Pediatric Orthopaedic Examination Answer Book • 77
M
Figure 94
REFERENCES: Abel MF (ed): Orthopaedic Knowledge Update: Pediatrics 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2006, pp 271-279.
Buechsenschuetz KE, Mehlman CT, Shaw KJ, et al: Femoral shaft fractures in children: Traction and
casting versus elastic stable intramedullary nailing. J Trauma 2002;53:914-921.
• b
2010 Pediatric Orthopaedic Examination Answer Book • 77
M
Figure 94
Question 42High Yield
**CLINICAL SITUATION**
Figures 1 through 3 are the radiographs of a 25-year-old man who is brought to the emergency department after a motorcycle collision. He is complaining of isolated knee pain. Examination reveals swelling, popliteal ecchymosis, joint line pain, and limited knee joint motion. His pulses and sensation are normal.
Figures 4 through 8 are the axial and coronal CT scan sections of the injury. Intra-operative patient positioning for definitive fixation should be
---
---
---
---
---
---
---
---
Figures 1 through 3 are the radiographs of a 25-year-old man who is brought to the emergency department after a motorcycle collision. He is complaining of isolated knee pain. Examination reveals swelling, popliteal ecchymosis, joint line pain, and limited knee joint motion. His pulses and sensation are normal.
Figures 4 through 8 are the axial and coronal CT scan sections of the injury. Intra-operative patient positioning for definitive fixation should be
---
---
---
---
---
---
---
---
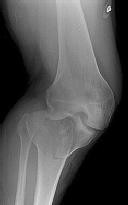
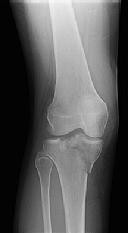
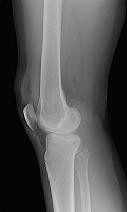
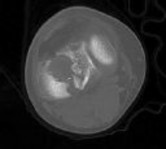
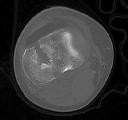
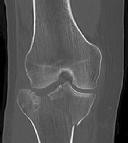
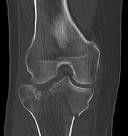
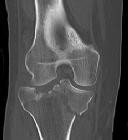
Explanation
Medial plateau fracture dislocations are rare. Failure to recognize this pattern can lead to poor patient outcomes secondary to poor surgical decision making. Pathognomonic findings on the anteroposterior radiograph include an intact lateral column (lateral articular surface still in continuity with tibial shaft), centrolateral articular impaction, shortening, and condylar widening. The medial femoral condyle stays with the fractured medial tibial plateau segment.
Initial management of axially unstable tibial plateau fractures with soft tissue swelling should consist of spanning external fixation and closed manipulative realignment. This allows for soft tissue recovery with the knee joint provisionally stabilized in reduced station. It also provides time for pre-operative planning, which is typically empowered via a CT scan with reconstructions. If the pattern was initially misdiagnosed as a more typically bicondylar tibial plateau fracture, the CT scan will clarify the misconception and allow for better surgical decision making.
Supine positioning is preferred for definitive fixation, but surgical approaches vary. Attempting to stabilize a medial partial articular pattern in the supine position from a lateral utility approach is fraught with difficulties. Lateral locked plating is not designed for this indication. The lateral utility approach allows for visualization of the centrolateral impaction and lateral meniscal peripheral capsular avulsion repair, but when used alone leads to biomechanically unsound implant placement. The primary plate should be on the medial side of the tibia rather than the intact lateral column.
Initial management of axially unstable tibial plateau fractures with soft tissue swelling should consist of spanning external fixation and closed manipulative realignment. This allows for soft tissue recovery with the knee joint provisionally stabilized in reduced station. It also provides time for pre-operative planning, which is typically empowered via a CT scan with reconstructions. If the pattern was initially misdiagnosed as a more typically bicondylar tibial plateau fracture, the CT scan will clarify the misconception and allow for better surgical decision making.
Supine positioning is preferred for definitive fixation, but surgical approaches vary. Attempting to stabilize a medial partial articular pattern in the supine position from a lateral utility approach is fraught with difficulties. Lateral locked plating is not designed for this indication. The lateral utility approach allows for visualization of the centrolateral impaction and lateral meniscal peripheral capsular avulsion repair, but when used alone leads to biomechanically unsound implant placement. The primary plate should be on the medial side of the tibia rather than the intact lateral column.
Question 43High Yield
An 82-year-old man who underwent a primary total knee arthroplasty 11 weeks ago is now seen following a fall from a standing height. A radiograph is shown in Figure 42. Examination reveals a small abrasion of the skin overlying the anterior aspect of the knee. He is able to actively extend the the knee but has a 10-degree extensor lag. Initial management should include which of the following?

Explanation
DISCUSSION: The patient has a periprosthetic fracture of the patella but is able to actively extend his knee. Despite the wide displacement of the fracture fragments, nonsurgical management is recommended given the high risk of complications and problems when open treatment of these fractures is undertaken.
REFERENCES: Ortiguera CJ, Berry DJ: Patellar fracture after total knee arthroplasty. J Bone Joint Surg Am 2002;84:532-540.
Parvizi J, Kim KI, Oliashirazi A, et al: Periprosthetic patella fractures. Clin Orthop Relat Res
2006;446:161-166.
Figure 43a Figure 43b
REFERENCES: Ortiguera CJ, Berry DJ: Patellar fracture after total knee arthroplasty. J Bone Joint Surg Am 2002;84:532-540.
Parvizi J, Kim KI, Oliashirazi A, et al: Periprosthetic patella fractures. Clin Orthop Relat Res
2006;446:161-166.
Figure 43a Figure 43b
Question 44High Yield
A 63-year-old man has long-standing type 2 diabetes. He has had associated ongoing neuropathy for approximately 5 years. He now reports a red, hot, swollen right foot for the past 2 days. You place him supine in your office with the foot elevated for 30 minutes. You return to see that the redness has dissipated. What is the most likely diagnosis?
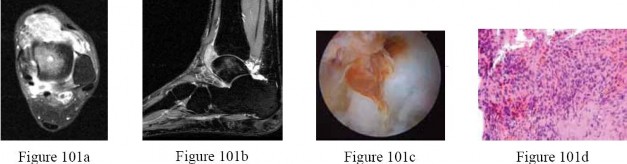
Explanation
Charcot arthropathy is a progressive condition of the musculoskeletal system that is characterized by joint dislocations, pathologic fractures, and debilitating deformities. This disorder results in progressive destruction of bone and soft tissues at weight-bearing joints; in its most severe form, it may cause significant disruption of the bony architecture. In patients with diabetes, the incidence of acute Charcot arthropathy of the foot and ankle ranges from 0.15% to 2.5%. Acute Charcot arthropathy almost always appears with signs of inflammation. Profound unilateral swelling, an increase in local skin temperature (generally, an increase of 3° to 7° above the nonaffected foot’s skin temperature), erythema,joint effusion, and bone resorption in an insensate foot are present. These characteristics, in the presence of intact skin and a loss of protective
sensation, are often pathognomonic of acute Charcot arthropathy.Cellulitis is an infection of the skin and osteomyelitis is an infection of the bone; examination of the limb would remain unchanged after 30 minutes of elevation. Reynaud and Sjogren syndromes are rheumatologic conditions that do not have these symptoms.
CLINICAL SITUATION FOR QUESTIONS 101 THROUGH 103
A 27-year-old woman has had pain in her right ankle for 2 years. Examination reveals a slightly warmjoint, without erythema. Ankle range of motion is limited by pain.
Radiographs are unremarkable.Because management consisting of immobilization, nonsteroidal anti-inflammatory drugs, and physiotherapy has failed to provide relief, MRI scans are obtained and shown in Figures 101a and 101b.An intraoperative image and the histology are shown in Figures 101c and 101d.
---
sensation, are often pathognomonic of acute Charcot arthropathy.Cellulitis is an infection of the skin and osteomyelitis is an infection of the bone; examination of the limb would remain unchanged after 30 minutes of elevation. Reynaud and Sjogren syndromes are rheumatologic conditions that do not have these symptoms.
CLINICAL SITUATION FOR QUESTIONS 101 THROUGH 103
A 27-year-old woman has had pain in her right ankle for 2 years. Examination reveals a slightly warmjoint, without erythema. Ankle range of motion is limited by pain.
Radiographs are unremarkable.Because management consisting of immobilization, nonsteroidal anti-inflammatory drugs, and physiotherapy has failed to provide relief, MRI scans are obtained and shown in Figures 101a and 101b.An intraoperative image and the histology are shown in Figures 101c and 101d.
---
Question 45High Yield
A 12-year-old girl is brought into the office for an examination because of hip pain. She is able to bear weight on the involved limb while using crutches for stability. Radiographs reveal a grade III slip of the capital femoral epiphysis. Recommended treatment for this patient is:
Explanation
In situ fixation provides the best results no matter what the grade of slip.
Question 46High Yield
A 2-year-old child is brought to your office for evaluation of a "big hand." Upon examination, you notice that the child has mildly enlarged ring and small fingers. There is full range of motion without instability. After examination of the patient, you recommend:
Explanation
The child is not ready for surgery. Although surgery may coincide with the patient beginning school, this does not always occur. At this time, additional examination and testing are recommended.
Question 47High Yield
Smoking has been associated with lower fusion rates in both cervical and lumbar fusion. Which of the following statements best describes an explanation for these findings?
Explanation
of the mechanism mediating this effect. Whereas all of the above have been postulated as explanations, more recent studies have
demonstrated that nicotine delivered via a transdermal patch significantly enhanced posterior spinal fusion in rabbits. Thus it appears that the effects of smoking on fracture healing are multifactorial and not yet fully understood.
demonstrated that nicotine delivered via a transdermal patch significantly enhanced posterior spinal fusion in rabbits. Thus it appears that the effects of smoking on fracture healing are multifactorial and not yet fully understood.
Question 48High Yield
Figure 12 is the radiograph of a patient with type 2 diabetes, a body mass index of 42, and an Hgb A1c of 8. What is the most appropriate management for this injury?
Explanation
Several recent studies have shown that while there is an increased risk of complications following ORIF of displaced ankle fractures in diabetic patients compared with nondiabetic patients,the overall risks of treatment are less than that associated with nonsurgical treatment in diabetics. There is also the possibility that ORIF of unstable ankle fractures may forestall the development of Charcot changes in the ankle, although this is not definitively known. Extra rigid fixation may be required because of the patient’s size and poorly controlled diabetes. Nonsurgical management is associated with poorer functional outcomes (due to arthritis secondary to poor reduction of the fracture) and a higher rate of skin breakdown, due to the need for higher skin pressures from the use of highly molded casting used to maintain a closed reduction.
Question 49High Yield
Figures 1 through 3 are the MRI scans of a 26-year-old man who injured his knee wrestling one day prior. He has a moderate effusion, medial knee pain and an inability to extend his knee actively or passively. What is the most appropriate definitive treatment option?
Explanation
The images show a bucket handle medial meniscus tear, which is likely responsible for the block to motion. Therefore, surgery should be recommended with a meniscus repair if possible. Physical therapy or knee aspiration/manipulation under anesthesia is not the best definitive treatment.
Question 50High Yield
A 39-year-old right-hand dominant woman presents with many years of right shoulder instability. She tried physical therapy several times over the years without any benefit. Figure 1 shows her current axillary radiograph. Figures 2 and 3 are representative MR arthrogram images. What is the best treatment plan?
Explanation
4
The question stem describes a patient with long-standing anterior glenohumeral joint instability. The axillary view plain radiograph shows blunting of the anterior glenoid rim. The axial cut from the MR arthrogram shows loss of anterior glenoid contour and tear and medialization of the anteroinferior labrum consistent with anterior glenohumeral joint instability. The sagittal cut shows loss of pear-shaped glenoid. With a patient describing innumerable dislocations and anterior glenoid bone loss, the best option is for coracoid transfer or Latarjet. Open or arthroscopic bankart repair does not address the bone loss. Glenoid osteotomy has been advocated for posterior shoulder instability and glenoid retroversion, which the patient does not have.
The question stem describes a patient with long-standing anterior glenohumeral joint instability. The axillary view plain radiograph shows blunting of the anterior glenoid rim. The axial cut from the MR arthrogram shows loss of anterior glenoid contour and tear and medialization of the anteroinferior labrum consistent with anterior glenohumeral joint instability. The sagittal cut shows loss of pear-shaped glenoid. With a patient describing innumerable dislocations and anterior glenoid bone loss, the best option is for coracoid transfer or Latarjet. Open or arthroscopic bankart repair does not address the bone loss. Glenoid osteotomy has been advocated for posterior shoulder instability and glenoid retroversion, which the patient does not have.
You Might Also Like

Medically Verified Content by
Prof. Dr. Mohammed Hutaif
Consultant Orthopedic & Spine Surgeon

