Making a Complex Regional Pain Syndrome Diagnosis: Avoid Overdiagnosis
Key Takeaway
This article provides essential research regarding Making a Complex Regional Pain Syndrome Diagnosis: Avoid Overdiagnosis. Diagnosing Complex Regional Pain Syndrome (CRPS) now uses refined criteria, addressing previous IASP guidelines that led to overdiagnosis due to low specificity. Current methods for this pain syndrome making involve grouping symptoms into distinct categories, such as pain processing, vasomotor dysfunction, edema, and motor/trophic changes. This improves diagnostic accuracy and differentiation from other conditions.
-
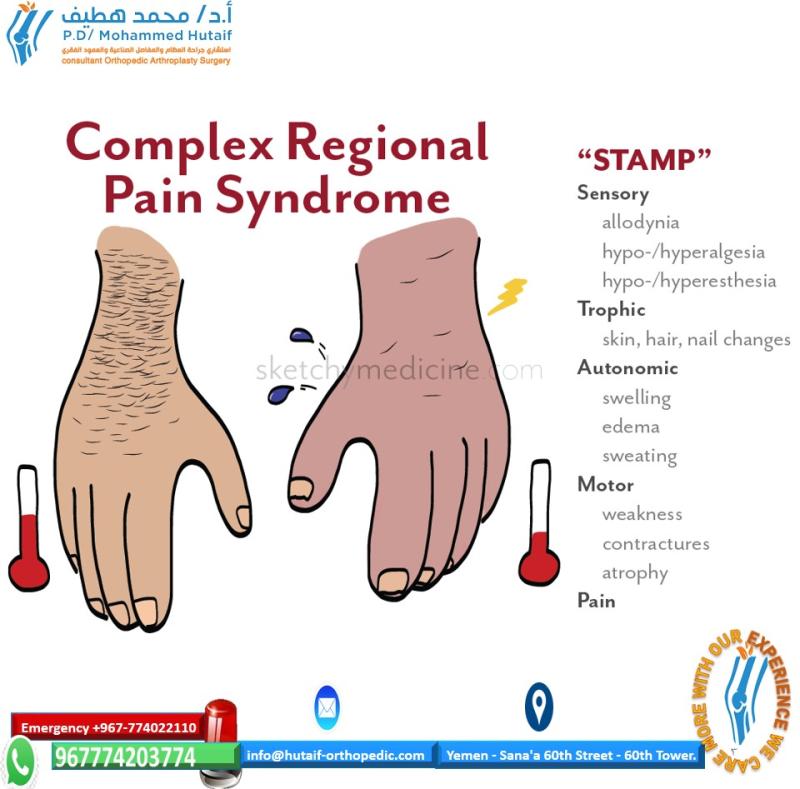
Complex Regional Pain Syndrome MAKING A DIAGNOSIS
Considerable confusion has been generated by a failure
to understand the recent work from the IASP. In 1994, when the IASP
produced the new diagnostic entity of CRPS, it was descriptive, and
general and based on a consensus.119
Deliberately, it did not imply any etiology or pathology (including any
direct role for the SNS). The intention was to provide an officially
endorsed set of standardized diagnostic criteria to improve clinical
communication and facilitate research.118
In other words, this was intended as a starting point from which
individual researchers could move forward. It was not thought of as a
mature clinical diagnostic device.
Since their original publication, the diagnostic
criteria have been validated, refined, and developed. The validation
studies suggest that the original criteria are adequately sensitive within the context of a pain clinic
(i.e., they rarely miss a case of actual CRPS); however, the criteria
cause problems of overdiagnosis because of poor specificity.58,80
Comparison of CRPS patients to other proved pain states, such as
chronic diabetic patients with ascending symmetric pain, whose
neuropathy is confirmed by nerve conduction studies, also show that the
criteria are very sensitive but have low specificity, so that a
diagnosis of CRPS may be erroneous in up to 60% of cases.22
Other problems are evident. For example, the criteria
assume that any sign or symptom of vasomotor, sudomotor, and
edemarelated change is sufficient to justify the diagnosis and there is
no possibility of providing greater diagnostic or prognostic accuracy
by observing more than one of these features. An additional weakness is
the failure to include motor or trophic signs and symptoms. Numerous
studies have described various signs of motor dysfunction (e.g.,
dystonia, tremor) as important characteristics of this disorder, and
trophic changes have frequently been mentioned in historical clinical
descriptions.26,28 These differentiate CRPS from other pain syndromes.58,138
Finally, the wording of the criteria permits diagnosis based solely on
patientreported historical symptoms. This may be inappropriate in the
context of litigation.
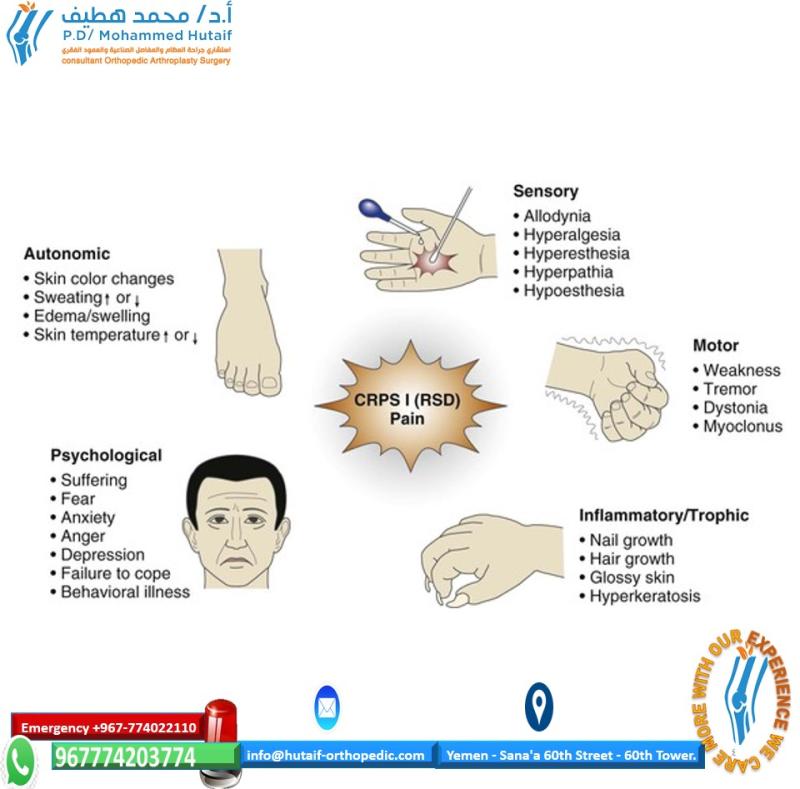
Factor analysis of 123 CRPS patients has indicated that the features cluster into four statistically distinct subgroups.80 - A set of signs and symptoms indicating abnormalities in pain processing (e.g., allodynia, hyperalgesia, hyperpathia)
- Skin color and temperature changes, indicating vasomotor dysfunction
- Edema and abnormalities of sweating
-
Motor and trophic signs and symptoms
The statistical separation of edema and sudomotor
dysfunction from vasomotor instability and the finding of motor and
trophic abnormalities are at variance with the original IASP criteria,
which were therefore modified22,58,80 (Table 23-3).
The important changes are inclusion of clinical signs, their separation
from symptoms, and the inclusion of features of motor abnormalities and
trophic changes. Intriguingly, these subgroups are virtually identical
to those suggested by our group a decade earlier.3
Statistical analysis has been undertaken to investigate
sensitivity and specificity of decision rules for diagnosis of CRPS
compared to neuropathic pain of a proved non-CRPS cause using these
criteria22 (Table 23-4).
These propose different diagnostic criteria depending on the clinical
circumstances. Thus, for purely clinical diagnosis, the criteria
provide a sensitivity of 0.85 and a specificity of 0.69, whereas for
research diagnosis, the criteria provide a sensitivity of 0.70 and
specificity of 0.94, because, in the former circumstance, one wishes to
avoid failing to offer treatment to a possible candidate while in the
latter situation one is more concerned to be investigating a
homogeneous group in whom the diagnosis cannot be in doubt.
It is critical to understand that the Bruehl modification of the original IASP criteria24 given in Table 23-3 apply to the diagnosis of CRPS within a pain clinic setting
and are therefore intended to differentiate CRPS from other causes of
chronic pain within that setting. They do not apply directly to the
diagnosis of CRPS within the context of an orthopaedic practice. The
reason for this apparent conundrum is that the precise nature of CRPS
remains unclear and it is therefore a diagnosis of exclusion.
Conditions from which CRPS must be distinguished in a pain clinic
(e.g., neuropathic pain in association with diabetic neuropathy) are
different from those which apply in an orthopaedic or fracture clinic
(e.g., soft tissue infection or stress fracture). Therefore, the
diagnostic criteria must be slightly different, just as slightly
different criteria are required within a pain clinic for diagnosis of
CRPS depending on whether the diagnosis is being made for clinical or
research purposes.
Atkins et al.2,3,4 proposed a set of diagnostic criteria for CRPS specifically in an orthopaedic context(Table 23-5).
These were derived empirically from a less formal but similar process
to the IASP consensus approach. The criteria were designed as far as
possible to be objective, but the patient’s veracity was assumed, so no
attempt was made to separate reports of vasomotor or sudomotor
abnormalities from observation of them. A number of the criteria are
quantifiable,2,3,51 which allows their powerful use to investigate treatment.53,54,105
The original criteria were developed in the context of CRPS of the hand
following Colles’ fracture of the wrist, but they have subsequently
been generalized for use in the diagnosis of CRPS in other orthopaedic
scenarios and in the lower limb.13,135
Diagnosis by these criteria, when used after Colles’ fracture, maps
virtually exactly with the Bruehl criteria, suggesting their
reliability.147
Clinical Diagnosis in an Orthopaedic Setting
1. Pain
A history of excessive pain is elicited. Abnormalities
of pain perception are examined in comparison with the opposite normal
side. Excessive tenderness is found by squeezing digits in the affected
part between thumb and fingers. This may be quantitated using
dolorimetry but this is usually a research tool.4,6
Allodynia is demonstrated by fine touch and hyperalgesia using a pin.
Hyperpathia is examined by serial fine touch or pin prick.
TABLE
23-3 Modified International Association for the Study of Pain
Diagnostic Criteria for Complex Regional Pain Syndrome (CRPS)
| General definition of the syndrome
CRPS describes
an array of painful conditions that are characterized by a continuing
(spontaneous and/ or evoked) regional pain that is seemingly
disproportionate in time or degree to the usual course of any known
trauma or other lesion. The pain is regional (not in a specific nerve
territory or dermatome) and usually has a distal predominance of
abnormal sensory, motor, sudomotor, vasomotor, and/or trophic findings.
The syndrome shows variable progression over time.
To make the
clinical
diagnosis, the following criteria must be met (sensitivity of 0.85 specificity of 0.69)
1. | Continuing pain, which is disproportionate to any inciting event
2. | Must report at least one symptom in
three of the four
following categories:
| | Sensory
| | | Reports of hyperesthesia and/or allodynia
| | Vasomotor
| | | Reports of temperature asymmetry and/or skin color changes and/or skin color asymmetry
| | Sudomotor/edema
| | | Reports of edema and/or sweating changes and/or sweating asymmetry
| | Motor/trophic
| | | Reports of
decreased range of motion and/or motor dysfunction (weakness, tremor,
dystonia) and/ or trophic changes (hair, nail, skin)
3. | Must display at least one sign at time of evaluation in
two or more
of the following categories:
| | Sensory
| | | Evidence of
hyperalgesia (to pinprick) and/or allodynia (to light touch and/or
temperature sensation and/or deep somatic pressure and/or joint
movement)
| | Vasomotor
| | | Evidence of temperature asymmetry (>1°C) and/or skin color changes and/or asymmetry
| | Sudomotor/edema
| | | Evidence of oedema and/or sweating changes and/or sweating asymmetry
| | Motor/trophic
| | | Evidence of
decreased range of motion and/or motor dysfunction (weakness, tremor,
dystonia) and/or trophic changes (hair, nail, skin)
4. | There is no other diagnosis that better explains the signs and symptoms.
For
research
purposes, diagnostic decision rule should be at least one symptom
in all four
symptom categories and at least one sign (observed at evaluation) in
two or more sign categories (sensitivity of 0.70, specificity of 0.94).
From Bruehl et al.22 and Harden et al.80
2a. Vasomotor instability
Vasomotor instability is often transitory and so it may
not be present at the time of examination. If the patient is reliable,
then a history confirms its presence. Visual inspection is the usual
means of diagnosis.
Thermography can be used to quantitate temperature
difference between the limbs. This is greater in CRPS than other pain
syndromes,128,162
and this can be used to distinguish CRPS from other causes of
neuropathic pain. However, thermography has not been validated within
an orthopaedic context and must therefore be used with caution. It is
not usually used in an orthopaedic context.
2b. Abnormal sweating
Whether this feature should be considered with vasomotor instability as proposed by Atkins et al.3,6 or should be with edema as suggested recently by Harden et al.80
is not yet clear. As for vasomotor instability, the feature is
inconstant and it may be necessary to rely on history. Excessive
sweating is usually clinically obvious. In a doubtful case, the
resistance to a biro or pencil gently stroked across the limb is
useful. The extent of sweating can be quantified by iontophoresis but
this is rarely undertaken.
3. Edema and swelling
This is usually obvious on inspection. In the hand, it
may be quantified by hand volume measurement. Similarly, skinfold
thickness and digital circumference may be measured.3,6
4. Loss of joint mobility and atrophy
Loss of joint mobility is usually diagnosed by standard
clinical examination. The range of finger joint movement may be
accurately quantified.3,6,51 As outlined here, atrophy will affect every tissue within the limb.
5. Bone changes
Radiographic appearances and bone scans are discussed
earlier. CRPS does not cause arthritis and joint space is preserved.
Sudeck’s technique of assessing bone density by radiographing two
extremities on one plate120,145 remains
useful but densitometry is not usually helpful.156 A normal bone scan without radiographic osteoporosis virtually excludes adult CRPS.
TABLE
23-4 Diagnostic Sensitivity and Specificity for the International
Association for the Study of Pain Modified Criteria (see Table 23-3)
in Distinguishing Patients with Complex Regional Pain Syndrome (CRPS)
from Patients with Neuropathic Pain from a Documented Non-CRPS Cause
| --- | Decision rule | Sensitivity | Specificity |
| --- | --- | --- |
| 2 + sign categories and 2 + symptom categories | 0.94 | 0.36 |
| 2 + sign categories and 3 + symptom categories | 0.85 | 0.69 |
| 2 + sign categories and 4 symptom categories | 0.70 | 0.94 |
3 + sign categories and 2 + symptom categories <td align="right" colspan="1" rowspan="1" style="border-style: solid; border-color: rgb(221, 221, 221); box-si
You Might Also Like