Total Ankle Arthroplasty: Specific Implants, Surgical Techniques, and Clinical Outcomes

Key Takeaway
Total ankle arthroplasty (TAA) has evolved significantly, offering a viable alternative to arthrodesis for end-stage ankle arthritis. This guide reviews the biomechanics, surgical techniques, and clinical outcomes of prominent TAA systems, including the Agility, Scandinavian Total Ankle Replacement (STAR), and Buechel-Pappas prostheses. Understanding the specific design rationales, bone resection requirements, and complication profiles of these implants is critical for orthopedic surgeons optimizing patient outcomes and implant survivorship.
INTRODUCTION TO TOTAL ANKLE ARTHROPLASTY
The surgical management of end-stage ankle arthritis has undergone a paradigm shift over the last three decades. While ankle arthrodesis remains a highly reliable procedure for pain relief, it inherently sacrifices tibiotalar motion, leading to altered gait biomechanics and accelerated adjacent-segment degeneration (specifically in the subtalar and talonavicular joints). Total Ankle Arthroplasty (TAA) has emerged as a biomechanically superior alternative for appropriately selected patients, aiming to preserve functional range of motion, restore normal gait kinematics, and protect adjacent hindfoot joints from premature arthropathy.
The evolution of TAA implants from highly constrained, cemented first-generation designs (which suffered catastrophic failure rates due to aseptic loosening) to modern second- and third-generation unconstrained or semi-constrained, cementless designs represents a triumph of orthopedic bioengineering. Modern implants rely on precise anatomical alignment, biological osseointegration, and sophisticated bearing designs to minimize stress transfer to the bone-prosthesis interface.
This comprehensive guide meticulously evaluates three historically and clinically significant TAA systems: the Agility, the Scandinavian Total Ankle Replacement (STAR), and the Buechel-Pappas prostheses.
AGILITY TOTAL ANKLE ARTHROPLASTY
Biomechanics and Implant Design
The Agility Total Ankle System is a fixed-bearing, two-component prosthesis. Its design philosophy centers on a semi-constrained articulation where the ultra-high-molecular-weight polyethylene (UHMWPE) insert is rigidly locked into the titanium tibial tray.
The articulation features partial conformity between the tibial polyethylene and the metallic talar component. This partial conformity is a deliberate biomechanical compromise: it allows for a degree of rotational and translational freedom, thereby decreasing the sheer stress transferred to the critical bone-prosthesis interface. However, this reduced conformity inherently increases contact stresses within the polyethylene, theoretically elevating the risk of accelerated volumetric wear.
Clinical Pearl: The defining architectural requirement of the Agility system is the necessity of a distal tibiofibular syndesmosis fusion. By fusing the syndesmosis, the implant utilizes the fibula to provide a wider, more stable structural base for the broad tibial component, effectively mitigating the risk of tibial subsidence.
Surgical Technique and Positioning
Patient Positioning and Approach:
1. The patient is positioned supine with a bump under the ipsilateral hip to internally rotate the leg to a neutral mechanical axis.
2. A standard anterior longitudinal approach is utilized, exploiting the internervous plane between the Extensor Hallucis Longus (EHL) and the Extensor Digitorum Longus (EDL).
3. The superficial peroneal nerve and the deep peroneal nerve/anterior tibial artery bundle must be meticulously protected.
Bone Resection and Syndesmotic Fusion:
The Agility implant requires a significantly larger talar resection compared to modern bone-sparing designs.
1. An external distractor is mandatory to open the joint space, allowing for the relatively aggressive, flat bone cuts required for the components.
2. The medial cortex of the fibula and the lateral cortex of the tibia are decorticated.
3. Bone graft (often harvested from the resected talus or distal tibia) is packed into the syndesmotic interval.
4. Trans-syndesmotic fixation (typically utilizing robust cortical screws) is placed to compress the arthrodesis site, ensuring a rigid construct to support the oversized tibial tray.
Clinical Outcomes and Complications
Long-term data on the Agility prosthesis reveals a complex profile of high patient satisfaction juxtaposed with notable radiographic and surgical complication rates.

Knecht et al. reported intermediate results at an average follow-up of 9 years in 132 patients. The clinical success was evident, with 92% of patients satisfied with their outcome and 97% willing to recommend the procedure. However, the radiographic and revision data highlighted inherent design challenges:
* Major Revision Rate: 11%
* Secondary Procedures: 27% (32 of 132 patients) required additional operations.
* Radiographic Lucencies: A staggering 76% of ankles demonstrated periprosthetic lucencies, raising concerns about long-term aseptic loosening.
Spirt et al. evaluated 306 ankles at a mean follow-up of 33 months. They reported a 28% reoperation rate (most frequently for arthroscopic or open debridement of impingement), a 10% revision-to-fusion rate, and a 5-year implant survival rate of 80%. Interestingly, older age was a protective factor, with elderly patients demonstrating a lower risk of reoperation and failure.
Kopp et al. reviewed 43 ankles at an average 44.5-month follow-up. While patient satisfaction remained exceptionally high at 97.5%, the complication profile persisted:
* 85% exhibited radiographic lucencies.
* 23% required a second operation.
* Intraoperative malleolar fractures occurred (three medial, one lateral), necessitating immediate internal fixation.
* Three syndesmosis fusions progressed to nonunion, a critical failure given the implant's reliance on fibular support.
Surgical Warning: The learning curve for the Agility system is steep. Literature consistently demonstrates a sharp decrease in complications, particularly malleolar fractures and syndesmotic nonunions, as surgeon volume and familiarity with the aggressive bone resections increase.
SCANDINAVIAN TOTAL ANKLE REPLACEMENT (STAR)
Biomechanics and Implant Design
The Scandinavian Total Ankle Replacement (STAR) represents a fundamental shift in TAA philosophy. It is a mobile-bearing, three-component design consisting of a cementless tibial flat plate, a highly polished talar component, and a freely mobile UHMWPE meniscus interposed between them.

Kinematic Decoupling:
The mobile polyethylene component allows for minimal constraint at the flat tibial interface. This unconstrained articulation effectively decouples rotational and translational forces, drastically reducing stress transfer to the tibial bone-prosthesis interface—a primary cause of aseptic loosening in fixed-bearing designs.
Conversely, the inferior surface of the polyethylene is highly conforming to the central ridge of the talar component. This high conformity maximizes contact area, theoretically reducing contact stresses and minimizing superior-to-inferior polyethylene wear.
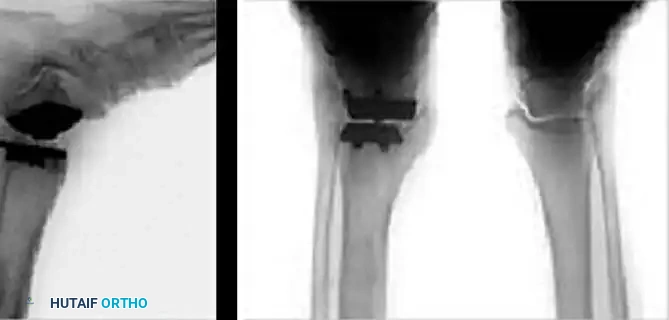
Pitfall: While the mobile bearing reduces interface stress, the unconstrained flat tibial articulation can lead to increased "backside wear" of the polyethylene and offers less inherent anterior-to-posterior stability, relying heavily on the integrity of the patient's collateral ligaments.
Surgical Technique and Positioning
Implantation of the STAR prosthesis is highly bone-conserving compared to the Agility system.
1. Approach: A standard anterior approach is utilized.
2. Bone Resection: The talar cuts are minimal, preserving the structural integrity of the talar neck and body. The system does require resurfacing of the medial and lateral talar facets to accommodate the highly conforming talar component.
3. Ligamentous Balancing: Because the implant is unconstrained, meticulous soft-tissue balancing is paramount. Coronal plane deformities must be corrected through medial or lateral ligamentous releases or adjunctive osteotomies to prevent asymmetrical loading.
Clinical Outcomes and Complications
The STAR prosthesis has one of the most robust bodies of literature in foot and ankle surgery, spanning both its original cemented iteration and its modern cementless (hydroxyapatite/titanium porous coated) design.
Cemented STAR Outcomes:
Kofoed et al. reported on 52 patients with the early cemented STAR, comparing osteoarthritis (OA) and rheumatoid arthritis (RA) cohorts. At 14 years, survivorship was highly comparable: 72.7% for OA and 75.5% for RA. The revision/arthrodesis rate was slightly higher in the OA group (24%) compared to the RA group (19%).
In a subsequent study of 100 patients (mixed cemented and uncemented) at a 6-year follow-up, Kofoed demonstrated that age was not a strict contraindication. Patients under 50 years had a 13% revision/fusion rate, statistically indistinguishable from the 11% rate in patients over 50 years.
Uncemented STAR Outcomes:
Wood et al. evaluated 200 patients with the modern uncemented STAR (112 RA, 56 OA, 25 post-traumatic arthritis) at a mean 46-month follow-up.
* Survivorship: 87.9% at 8 years.
* Revision Rate: 7% required revision or fusion, with an additional 4% undergoing secondary surgeries.
* Complications: Intraoperative malleolar fractures were a notable risk (9 fractures: 8 medial, 1 lateral). Postoperatively, 10 additional medial malleolar fractures occurred.
* Edge-Loading: Nine patients exhibited edge-loading, a phenomenon where coronal malalignment causes the mobile bearing to subluxate or load asymmetrically, leading to rapid catastrophic wear.
* Wound Healing: Delayed wound healing was significantly more prevalent in the RA cohort, whereas persistent pain and stiffness were more common in the post-traumatic arthritis group.
Anderson et al. reported a more guarded outcome in 51 patients with the uncemented STAR, noting a 24% revision rate and a 5-year survival rate of 70%. Despite this, 31 of 51 patients remained satisfied. Notably, preoperative and postoperative range of motion did not differ significantly, emphasizing that TAA primarily provides pain relief rather than massive gains in arc of motion.
BUECHEL-PAPPAS TOTAL ANKLE ARTHROPLASTY
Biomechanics and Implant Design
The Buechel-Pappas (BP) arthroplasty is another mobile-bearing, three-component system, but it features distinct anatomical and structural variations from the STAR.
The BP system is minimally constrained and fully conforming. Its defining characteristic is the deep central sulcus of the talar component, which articulates with a corresponding convexity on the inferior surface of the polyethylene bearing.
* Bone Preservation: Unlike the STAR, the BP talar component does not require resurfacing of the medial and lateral talar facets. This preserves vital talar bone stock, which is highly advantageous in the event of future revision. However, this design provides less total surface area for biological ingrowth.
* Tibial Stem: The tibial component features an intramedullary stem designed to provide enhanced mechanical support and resist subsidence in the softer metaphyseal bone of the distal tibia.
Surgical Technique
The surgical approach mirrors the standard anterior incision, but the preparation of the tibia is unique.
1. Anterior Cortical Window: To accommodate the tibial stem, a precise anterior cortical window must be created in the distal tibia.
2. Stem Implantation: The medullary canal is prepared, and the stemmed tibial tray is impacted into place. This requires meticulous trajectory planning to avoid breaching the posterior tibial cortex or inducing a sagittal plane malalignment.
3. Talar Preparation: The talar dome is resected with a simple flat cut, preserving the gutters.
Clinical Outcomes and Complications
Buechel et al. reported on 50 patients (33 post-traumatic arthritis, 8 OA, 7 RA, 2 talar osteonecrosis) with a mean follow-up of 5 years. The clinical results were highly favorable:
* Clinical Scores: 88% achieved good or excellent results, 6% fair, and 6% poor.
* Survivorship: The implant demonstrated an impressive 93.5% survivorship rate at 10 years.
* Revision Rate: Only 2 of 50 patients (4%) required revision surgery.
* Complications: Similar to other systems, medial malleolar fractures were the most common structural complication, occurring in three patients during the postoperative period. The preservation of the medial facet during talar preparation may alter stress distribution, contributing to this risk.
POSTOPERATIVE PROTOCOL AND REHABILITATION
Regardless of the specific implant utilized, strict adherence to a phased postoperative rehabilitation protocol is critical for soft-tissue healing, osseointegration, and the restoration of functional kinematics.
Phase I: Tissue Healing (Weeks 0-2)
* The patient is placed in a bulky, well-padded short leg splint in neutral dorsiflexion.
* Strict non-weight-bearing (NWB) status is enforced to protect the fragile anterior incision and allow early osseointegration of the cementless components.
* Strict elevation is mandated to mitigate edema and prevent wound dehiscence—the most dreaded early complication of the anterior approach.
Phase II: Early Mobilization (Weeks 2-6)
* Sutures are removed at 2 to 3 weeks once the incision is fully sealed.
* The patient is transitioned to a removable Controlled Ankle Motion (CAM) boot.
* Progressive partial weight-bearing is initiated, advancing to full weight-bearing as tolerated by week 6.
* Active range of motion (ROM) exercises (dorsiflexion and plantarflexion) are initiated out of the boot to prevent capsular contracture. Inversion and eversion are generally restricted to protect the malleoli and collateral ligaments.
Phase III: Strengthening and Proprioception (Weeks 6-12+)
* The CAM boot is gradually weaned.
* Physical therapy focuses on closed-chain strengthening, proprioceptive retraining, and gait normalization.
* High-impact activities (running, jumping) are permanently restricted to prevent accelerated polyethylene wear and implant subsidence.
CONCLUSION
Total Ankle Arthroplasty is a highly sophisticated, technically demanding procedure that offers profound pain relief and functional preservation for patients with end-stage ankle arthritis. The Agility, STAR, and Buechel-Pappas systems each represent distinct biomechanical philosophies—from fixed-bearing syndesmotic fusion models to unconstrained, bone-sparing mobile bearings.
While modern cementless designs have drastically improved long-term survivorship, orthopedic surgeons must remain vigilant regarding implant-specific complications, including radiographic lucencies, edge-loading, and malleolar stress fractures. Meticulous patient selection, precise surgical execution, and rigorous postoperative management remain the cornerstones of success in total ankle arthroplasty.
You Might Also Like