Sternoclavicular Joint Dislocations: Epidemiology, Surgical Anatomy, and Critical Complications
Key Takeaway
Sternoclavicular (SC) joint dislocations are uncommon but critical shoulder girdle injuries, often high-energy. They are classified as anterior (most common) or posterior, with posterior dislocations posing significant "hidden dangers" due to their proximity to vital mediastinal structures like major blood vessels, necessitating thorough clinical assessment for associated life-threatening complications.
Sternoclavicular Joint Dislocations: Spot the Hidden Dangers
Introduction & Epidemiology
Sternoclavicular (SC) joint dislocations, while relatively uncommon, represent a critical injury due to their potential for severe life-threatening complications, particularly with posterior displacement. They account for approximately 3% of all shoulder girdle injuries and less than 1% of all joint dislocations. These injuries are typically classified based on the direction of clavicular displacement relative to the sternum: anterior (most common, ~90%) or posterior (less common, ~10%). Both types are usually the result of high-energy trauma, often indirect mechanisms, though direct blows can occur.
Mechanisms of Injury:
*
Indirect Trauma:
*
Anterior Dislocations:
Most commonly result from an indirect force to the posterolateral aspect of the shoulder, driving the clavicle anteriorly and medially (e.g., fall on an outstretched arm with the shoulder abducted and extended). A direct blow to the anteromedial clavicle can also cause anterior displacement.
*
Posterior Dislocations:
Typically result from an indirect force to the anterolateral shoulder, compressing the shoulder and driving the clavicle posteriorly and medially (e.g., dashboard injury, direct blow to the top of the shoulder with the arm adducted and flexed). This mechanism compresses the shoulder girdle, translating the medial clavicle posteriorly.
*
Direct Trauma:
A direct blow to the medial clavicle can also cause either anterior or posterior displacement depending on the vector.
Classification:
*
Acute:
Less than 3 weeks post-injury.
*
Subacute:
3 weeks to 3 months post-injury.
*
Chronic:
Greater than 3 months post-injury.
*
Traumatic:
Resulting from specific injury.
*
Non-traumatic:
Spontaneous, inflammatory, degenerative.
The high-energy nature of these injuries, especially posterior dislocations, mandates a thorough clinical assessment for associated injuries, particularly those involving vital mediastinal structures. Failure to recognize the severe implications of posterior dislocations can lead to catastrophic outcomes.
Surgical Anatomy & Biomechanics
The sternoclavicular joint is a diarthrodial, saddle-type synovial joint with a unique anatomy that belies its critical biomechanical role as the sole bony articulation between the upper extremity and the axial skeleton. Despite its small size, it withstands significant forces.
Bony Anatomy:
*
Medial Clavicle:
The medial end of the clavicle is convex longitudinally and concave transversely. It articulates with the manubrium.
*
Manubrium:
The clavicular notch of the manubrium is reciprocally concave longitudinally and convex transversely.
*
First Costal Cartilage:
The articular capsule of the SC joint attaches to the first rib's costal cartilage, which contributes to joint stability.
Ligamentous Anatomy (Primary Stabilizers):
The SC joint possesses a robust ligamentous complex, making it inherently stable.
*
Anterior Sternoclavicular Ligament:
Broad, strong fibers running from the anterior aspect of the medial clavicle to the anterior manubrium. It resists posterior translation and superior displacement, and limits protraction. It is generally stronger than the posterior ligament.
*
Posterior Sternoclavicular Ligament:
Similar to the anterior ligament but courses posteriorly. It is crucial for resisting anterior translation and limiting retraction. It is thinner and weaker than its anterior counterpart, making it more susceptible to injury in posterior dislocations. The critical relationship of this ligament to the mediastinal structures makes posterior SC joint instability particularly dangerous.
*
Interclavicular Ligament:
Connects the superior aspects of the medial ends of both clavicles, crossing the superior aspect of the manubrium. It primarily resists inferior displacement and provides additional stability against superior translation of the clavicle.
*
Costoclavicular Ligament (Rhomboid Ligament):
This is the primary static stabilizer of the SC joint and often considered extracapsular. It consists of two laminae (anterior and posterior) extending from the inferior surface of the medial clavicle to the superior surface of the first rib. It strongly resists superior displacement of the clavicle and provides significant resistance to anterior, posterior, and medial translation, as well as axial rotation. Its integrity is paramount for SC joint stability.
Articular Disc:
An intra-articular fibrocartilaginous disc is present in the majority of SC joints. It attaches superiorly to the medial clavicle, inferiorly to the first costal cartilage, and circumferentially to the joint capsule. It acts as a shock absorber, incongruity reducer, and pivot point, further enhancing stability and distributing forces. It also divides the joint into two separate synovial cavities.
Biomechanics:
The SC joint allows for significant range of motion in multiple planes:
* Elevation/Depression: Up to 45-60 degrees.
* Protraction/Retraction: Up to 30 degrees.
* Axial Rotation: Up to 30-45 degrees, primarily occurring with arm elevation and rotation.
These motions are crucial for full shoulder girdle function. The costoclavicular ligament is the primary restraint to superior translation, while the anterior and posterior SC ligaments resist anterior and posterior translation, respectively. Complete disruption of these ligaments, particularly the costoclavicular, leads to significant instability.
Adjacent Vital Structures (Hidden Dangers):
The immediate proximity of the posterior aspect of the SC joint to critical mediastinal structures defines the "hidden dangers" of posterior dislocations. These include:
*
Vascular Structures:
Subclavian artery and vein, brachiocephalic (innominate) artery and vein, common carotid arteries, internal jugular veins.
*
Respiratory Structures:
Trachea, pleura (apex of the lung), potential for pneumothorax/hemothorax.
*
Gastrointestinal Structures:
Esophagus.
*
Neurological Structures:
Brachial plexus (inferior trunk), phrenic nerve, recurrent laryngeal nerve (especially on the left).
*
Other:
Thoracic duct (left side).
Injury to any of these structures can result in life-threatening hemorrhage, airway obstruction, dysphagia, or neurological deficit. Therefore, a high index of suspicion and thorough investigation are paramount for posterior SC joint dislocations.
Indications & Contraindications
Treatment for SC joint dislocations is dictated by the direction of displacement, chronicity, patient symptoms, and presence of associated neurovascular or visceral injury.
Non-Operative Indications:
*
Acute Anterior SC Joint Dislocations:
* Most anterior dislocations are managed non-operatively, regardless of reducibility, as they rarely cause functional impairment or chronic pain.
* Closed reduction may be attempted but is often unstable and difficult to maintain. Even if reduced, recurrence is common but usually asymptomatic.
* Initial management involves ice, analgesia, and a sling for comfort for 1-3 weeks. Gradual return to activities as tolerated.
*
Stable Chronic Anterior SC Joint Dislocations:
* Patients with minimal pain, good function, and no significant cosmetic deformity are managed symptomatically.
*
Asymptomatic Posterior SC Joint Dislocations (Very Rare/Controversial):
* Extremely rare scenario. If a posterior dislocation is identified incidentally and is asymptomatic, stable, and causes no mediastinal compression, non-operative management might be considered in carefully selected, low-demand patients, though this is highly atypical. Most posterior dislocations are symptomatic and pose risks.
Operative Indications:
*
Acute Posterior SC Joint Dislocations:
*
Absolute Indication:
Presence of neurovascular compromise (e.g., subclavian artery/vein compression, pulsatile mass, diminished pulses, neurologic deficit), airway compromise (dyspnea, stridor), esophageal injury (dysphagia, odynophagia), or pneumothorax/hemothorax. These necessitate emergent closed or open reduction.
*
Relative Indication:
All symptomatic posterior dislocations are generally recommended for reduction due to the risk of delayed complications, even if initially asymptomatic. Persistent pain or cosmetic deformity.
*
Irreducible Anterior SC Joint Dislocations:
* Rarely irreducible by closed means. If significant cosmetic deformity, pain, or functional impairment persists despite conservative measures, surgical intervention may be considered.
*
Chronic Symptomatic Instability (Anterior or Posterior):
* For patients with persistent pain, instability, clicking, or functional limitation despite adequate non-operative management for chronic dislocations (usually 3-6 months), reconstructive surgery is indicated. This typically involves ligament reconstruction.
*
Associated Fractures:
* Fractures of the medial clavicle or manubrium requiring surgical stabilization, especially if complicated by dislocation.
*
Growth Plate Injuries (Physeal Fractures):
* In skeletally immature patients, Salter-Harris Type I or II injuries of the medial clavicular physis may mimic true SC joint dislocations. Posterior displacement often requires reduction due to risks, while anterior displacement can be managed non-operatively.
Table 1: Operative vs. Non-Operative Indications for SC Joint Dislocations
| Feature/Condition | Non-Operative Management | Operative Management |
|---|---|---|
| Acute Anterior Dislocation | Initial treatment for most cases. Sling, analgesia, ROM. | Rarely, if significant cosmetic deformity, persistent pain/dysfunction, or irreducible (very rare). |
| Chronic Anterior Dislocation | Asymptomatic, mild pain, acceptable function/cosmesis. | Persistent, debilitating pain, significant cosmetic deformity, functional instability despite conservative treatment for 3-6 months. Reconstruction indicated. |
| Acute Posterior Dislocation | Almost never (unless extremely rare, asymptomatic, stable, no compromise). | Absolute: Any neurovascular (subclavian, brachiocephalic, carotid, jugular, brachial plexus) or visceral (trachea, esophagus, pleura) compromise/symptoms. Relative: All symptomatic cases, persistent pain, cosmetic deformity, irreducible closed reduction. |
| Chronic Posterior Dislocation | Rarely (if completely asymptomatic and no compromise). | Persistent pain, instability, functional limitations, or concern for late-onset visceral/neurovascular compromise. Reconstruction indicated. |
| Associated Fractures | Stable, minimally displaced fractures. | Displaced medial clavicle fractures requiring stabilization, unstable fractures leading to joint instability. |
| Physeal Injuries | Anteriorly displaced physeal fractures (Salter I/II). | Posteriorly displaced physeal fractures due to risk of vital structure compromise. |
Pre-Operative Planning & Patient Positioning
Thorough pre-operative planning is paramount, especially for posterior dislocations, given the potential for severe complications.
Diagnostic Imaging:
*
Plain Radiographs:
Anteroposterior (AP) and lateral views are often insufficient due to bony overlap. A "serendipity view" (AP with 40-degree cephalic tilt) is essential as it projects the medial clavicles above the sternum, allowing for comparison of superior-inferior alignment. An oblique view (specifically the "Heinig view") can also be helpful.
*
Computed Tomography (CT) Scan:
The gold standard for diagnosing and characterizing SC joint dislocations.
Axial cuts provide detailed information on the direction and degree of displacement relative to the manubrium. Coronal and sagittal reconstructions further clarify the injury. For posterior dislocations, a CT angiogram (CT-A) with IV contrast is mandatory to assess for impingement, compression, or laceration of mediastinal vessels and to evaluate the proximity of the clavicle to the trachea, esophagus, and lung apex. This allows for detailed visualization of the "hidden dangers."
*
Magnetic Resonance Imaging (MRI):
Useful for assessing soft tissue injuries, including ligamentous tears (anterior/posterior SC ligaments, costoclavicular ligament, articular disc), muscle contusions, and associated brachial plexus injuries. May be considered if soft tissue pathology is suspected or if plain films/CT are equivocal. However, it is less critical than CT for initial bony assessment and mediastinal structures.
*
Chest Radiograph:
May be obtained to rule out pneumothorax or hemothorax, particularly in posterior dislocations.
Consultations:
*
Thoracic Surgery/Vascular Surgery:
For any posterior dislocation, especially if CT-A demonstrates proximity or compression of major vessels/airway, or if an open reduction is planned. Their expertise may be required for vascular control or repair.
*
Anesthesiology:
Crucial for managing complex cases, potential for rapid blood loss, and ensuring a secure airway (e.g., fiberoptic intubation if airway compromise is suspected).
*
General Surgery/ENT:
If esophageal or tracheal injury is suspected.
Pre-Operative Considerations:
*
Type and Screen/Crossmatch:
Essential for posterior dislocations due to the risk of major hemorrhage.
*
Discussion of Risks:
Comprehensive discussion with the patient about the potential for neurovascular or visceral injury, even during reduction maneuvers.
*
Concomitant Injuries:
Evaluate for other traumatic injuries, especially if high-energy trauma.
Patient Positioning:
*
Supine Position:
Standard for all SC joint procedures.
*
Shoulder Roll/Bolster:
Placed longitudinally between the scapulae to facilitate posterior extension of the shoulders, which can aid in reduction and open up the operative field.
*
Head Position:
Turned away from the operative side to allow adequate access.
*
Draping:
Wide sterile prep and drape, often including the ipsilateral upper extremity free-draped to allow manipulation for reduction and evaluation of pulses. The entire chest and neck should be prepped, allowing for potential extension of the incision or emergent thoracotomy/sternotomy if necessary.
*
Monitoring:
Standard anesthetic monitoring. Consider arterial line for continuous blood pressure monitoring in high-risk cases.
*
Fluoroscopy:
C-arm fluoroscopy should be readily available and draped sterilely for intraoperative confirmation of reduction and hardware placement.
Detailed Surgical Approach / Technique
Surgical management of SC joint dislocations primarily aims for stable reduction and restoration of joint stability while minimizing morbidity. The chosen technique depends on the type, chronicity, and associated injuries.
1. Acute Posterior SC Joint Dislocations (Emergent)
The primary goal is gentle, stable reduction. Closed reduction is typically attempted first, followed by open reduction if unsuccessful or if concerns for mediastinal compromise persist.
-
Closed Reduction:
- Technique 1 (Adduction and Traction): Patient supine with bolster. Surgeon stands on the ipsilateral side. The arm is adducted, extended, and externally rotated to create tension on the costoclavicular ligament. Strong longitudinal traction is applied to the arm. Simultaneously, an assistant applies gentle downward pressure on the ipsilateral shoulder, while the surgeon manipulates the medial clavicle superiorly and anteriorly.
- Technique 2 (Towel Clip/Fingers): After general anesthesia and muscle relaxation, a sterile towel clip (or two fingers of the surgeon) can be carefully placed behind the medial clavicle. Gentle anterior traction is applied. This method is controversial due to the proximity of vital structures and should only be performed by experienced surgeons with vascular/thoracic surgery backup immediately available. Careful tactile feedback is critical to avoid placing the clip too deeply.
- Technique 3 (Figure-of-8 Strap/Sling): While rarely used in acute settings due to variable success, a figure-of-8 strap can provide prolonged gentle traction in specific cases.
- Confirmation: Reduction is confirmed by palpation, observation of restored sternal notch symmetry, and intraoperative fluoroscopy or repeat CT scan.
- Stability: If reduced, stability is assessed. Many acute posterior dislocations are stable after reduction. If unstable, percutaneous K-wire fixation (controversial, see below) or open reconstruction may be necessary.
-
Open Reduction: Indicated if closed reduction fails, if mediastinal compromise persists, or if there's a need for direct visualization/repair of vital structures.
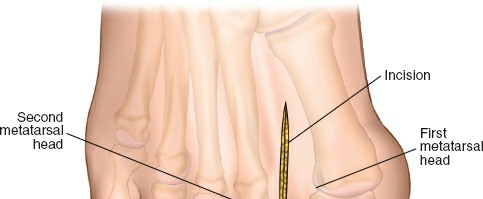
- Incision: Transverse incision (Langer's lines) approximately 5-7 cm long centered over the SC joint, or a longitudinal incision along the medial clavicle and sternal border, allowing for extension if needed.
-
Dissection:
- Skin and subcutaneous tissue. Identify and protect the supraclavicular nerves.
- Careful dissection through the platysma.
- Incise the anterior capsule and periosteum.
- Retract the sternocleidomastoid muscle (SCM) as needed.
- CRITICAL STEP for posterior dislocations: If posterior displacement, the medial clavicle is typically overriding the manubrium posteriorly. The posterior SC ligament is ruptured. With extreme caution, develop a plane posterior to the medial clavicle. Always have vascular/thoracic surgery present or on immediate standby. A finger can be used to palpate posterior structures and protect them during reduction.
- Reduction: Gentle traction on the arm in abduction and extension, while the surgeon directly manipulates the clavicle anteriorly.
-
Stabilization (if unstable post-reduction):
- Suture Repair: If the posterior capsule and costoclavicular ligament remnants are adequate, primary repair using non-absorbable sutures (e.g., 2-0 or #1 braided polyester) to reconstruct the posterior capsule and reinforce the anterior capsule.
-
Ligament Reconstruction (for severe instability/chronic cases):
Autograft (semitendinosus, palmaris longus, gracilis) or allograft (tibialis anterior, Achilles) can be used to reconstruct the costoclavicular ligament and/or the SC joint capsule.
- Technique: Drill tunnels in the medial clavicle and first rib/manubrium to pass the graft. The graft is then tensioned and secured (e.g., with interference screws, suture anchors, or direct suture repair) to restore stability. This is often performed as a figure-of-8 reconstruction across the joint.
-
Internal Fixation (Controversial/Limited Role):
- K-wires: Previously used, but highly discouraged due to significant complication rates , including migration into mediastinal structures (heart, great vessels, lung). If used in specific, carefully selected cases (e.g., skeletally immature patients without reconstructable ligaments), they must be bent at both ends to prevent migration and removed at 4-6 weeks. They offer no rotational stability.
- Plates/Screws: Generally avoided directly across the SC joint due to the complex biomechanics, risk of hardware failure, and limited bone stock for fixation. May be used for associated clavicle or manubrial fractures.
- Suture Anchors: Can be used in the manubrium or medial clavicle to reattach torn ligaments or graft material.
2. Acute Anterior SC Joint Dislocations
- Closed Reduction: Often attempted but difficult to maintain. Performed by applying direct pressure over the medial clavicle.
-
Open Reduction & Stabilization:
Rarely indicated in acute settings. If reduction is genuinely irreducible or if there's persistent, severe pain/dysfunction.
- Approach similar to posterior dislocation.
- Primary repair of anterior capsule and costoclavicular ligament. If irreducible, may indicate interposition of capsule or articular disc.
- Stabilization techniques similar to posterior dislocations, with emphasis on preventing anterior displacement.
3. Chronic Symptomatic SC Joint Instability (Anterior or Posterior)
These cases almost invariably require open reconstruction to restore stability and alleviate symptoms.
- Debridement: Removal of hypertrophic scar tissue, degenerative articular disc fragments, and any osteophytes.
- Medial Clavicle Resection Arthroplasty (for degenerative arthritis/some chronic anterior instability): Resection of 1-2 cm of the medial clavicle, combined with interpositional tissue (e.g., muscle flap, tendon, or synthetic mesh) to prevent bony impingement. This is primarily a salvage procedure for pain rather than instability.
-
Ligament Reconstruction:
This is the mainstay for chronic instability.
- Graft Choice: Autografts (semitendinosus, palmaris longus, gracilis) are preferred. Allografts can be used if autograft harvest is contraindicated or in revision cases.
-
Technique (often a Figure-of-8):
- The graft is passed through drill holes in the medial clavicle and anchored to the manubrium and/or first rib.
- A common technique involves drilling two divergent tunnels (2.5-3.5mm) in the medial clavicle, and one or two tunnels in the manubrium and/or the first rib.
- The graft is then woven through these tunnels, creating a figure-of-8 pattern around the repaired joint, aiming to recreate the function of the costoclavicular and sternoclavicular ligaments.
- The graft is tensioned and secured with non-absorbable sutures, interference screws, or staple fixation.
- The joint is usually held in a reduced position (often slight retraction and depression) during graft tensioning.
- Capsular Repair: Concomitant repair of the remaining capsule should always be performed.
Internervous Planes:
The surgical approach for SC joint surgery does not typically utilize a distinct internervous plane. The dissection involves:
* Skin and subcutaneous tissue.
* Platysma.
* Retraction of sternocleidomastoid muscle (innervated by accessory nerve CN XI and C2-C3 spinal nerves).
* Deep to the SCM, the surgical approach directly enters the region of the SC joint capsule. Care is taken to identify and protect the internal jugular vein and common carotid artery laterally, and the neurovascular structures posteriorly.
Critical Intraoperative Considerations:
*
Vascular/Airway Control:
For posterior dislocations, immediate access to thoracic/vascular surgery is non-negotiable. Have suction, vascular clamps, and sternotomy tray readily available.
*
Pneumothorax:
Maintain a high index of suspicion. Post-operative chest X-ray is often warranted.
*
Recurrent Laryngeal Nerve:
Right recurrent laryngeal nerve loops around the subclavian artery; left loops around the aortic arch. Injury is rare but possible during deep posterior dissection.
*
Stabilization:
Ensure adequate reduction and stable fixation without placing hardware across the joint, if possible, or using temporary hardware that is carefully monitored and removed.
Complications & Management
Complications following SC joint dislocations can range from minor to life-threatening, particularly with posterior dislocations.
Table 2: Common Complications, Incidence, and Salvage Strategies
| Complication | Incidence | Management / Salvage Strategy |
|---|---|---|
| Neurovascular Injury | 5-10% (posterior dislocations) | Emergent surgical exploration and repair/ligation. Consultation with vascular/thoracic surgery. Pre-op CT-A crucial. May require sternotomy/thoracotomy. |
| Airway/Esophageal Injury | Rare, but critical (posterior dislocations) | Emergent surgical consultation (thoracic/ENT/GI). Airway management (intubation, tracheostomy), esophageal repair. Requires multidisciplinary approach. |
| Pneumothorax/Hemothorax | 1-3% (posterior dislocations) | Chest tube insertion. Close monitoring. Surgical repair of pleural defect if persistent air leak. |
| Recurrence/Persistent Instability | Varies widely (up to 50% for closed reduction of anterior; ~5-15% for surgical reconstruction) | Non-operative: For asymptomatic or minimally symptomatic recurrences, particularly anterior. Operative: If symptomatic, revise primary repair or perform formal ligament reconstruction using autograft/allograft. Consider medial clavicle resection arthroplasty for chronic symptomatic pain with degenerative changes. |
| Chronic Pain/Degenerative Arthritis | Common post-trauma; higher with chronic instability | Non-operative: NSAIDs, physical therapy, intra-articular steroid injections. Operative: Medial clavicle resection arthroplasty (for intractable pain), or revision ligament reconstruction if instability is the primary cause. |
| Hardware Migration/Failure | High with K-wires (up to 50%); lower with suture/graft fixation | Hardware removal. If instability recurs, consider revision ligament reconstruction. If K-wire migration into mediastinum, emergent surgical removal by experienced vascular/thoracic surgeon. |
| Infection | <1-2% | Superficial: Wound care, antibiotics. Deep: Irrigation and debridement, IV antibiotics, hardware removal (if present and stable joint), repeat reconstruction if necessary. |
| Wound Complications | 5-10% (dehiscence, seroma, hematoma) | Local wound care, drainage, sterile dressings. Revision closure if significant dehiscence. |
| Nerve Injury | Rare (supraclavicular, recurrent laryngeal, phrenic) | Supraclavicular: Symptomatic management, nerve blocks. Recurrent laryngeal/Phrenic: ENT/Thoracic consultation. Voice therapy for RLN. Diaphragmatic pacing for phrenic if severe. |
| Nonunion/Malunion (of associated fractures) | Rare | Nonunion: Revision fixation with bone grafting. Malunion: Osteotomy if symptomatic. |
Specific Considerations:
*
K-wire migration:
This is a historically significant and potentially fatal complication. K-wires should generally be avoided across the SC joint. If used, they must be bent proximally and distally to prevent migration and removed at the earliest safe time (4-6 weeks).
*
Irreducible dislocations:
Often due to interposition of the articular disc, capsule, or rarely, tendons (e.g., subclavius). Requires open reduction.
*
Post-traumatic osteolysis of the medial clavicle:
A rare, painful condition that may require medial clavicle resection.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is crucial for optimizing outcomes, restoring function, and preventing recurrence after SC joint surgery. Protocols vary based on the specific procedure (reduction with simple repair vs. ligament reconstruction) and surgeon preference.
General Principles:
*
Protection:
Initial protection of the surgical repair to allow tissue healing.
*
Gradual Mobilization:
Progressive restoration of range of motion.
*
Progressive Strengthening:
Rebuilding muscular support.
*
Return to Activity:
Phased return to functional activities and sports.
Typical Protocol for SC Joint Reconstruction/Stabilization:
Phase 1: Protection & Early Motion (Weeks 0-6)
*
Immobilization:
Sling or figure-of-8 bandage for 4-6 weeks, with strict instructions to avoid abduction and external rotation, especially for posterior repairs. For anterior repairs, avoid extreme protraction. For ligament reconstructions, a full-time sling is often maintained for 4-6 weeks.
*
Pain Management:
Analgesics, ice.
*
Early Range of Motion (ROM):
*
Passive Range of Motion (PROM):
Gentle, pain-free pendulum exercises. Scapular mobilizations.
*
Elbow/Wrist/Hand ROM:
Active exercises to prevent stiffness.
*
Cervical Spine ROM:
Active, pain-free.
*
Precautions:
* NO active shoulder elevation beyond 30-45 degrees.
* NO active external rotation.
* NO lifting with the affected arm.
* Avoid direct pressure on the joint.
Phase 2: Progressive Motion & Light Strengthening (Weeks 6-12)
*
Discontinue Sling (gradually):
Typically around week 6, depending on pain and healing.
*
Active-Assisted Range of Motion (AAROM):
Progress from PROM to AAROM and then to gentle AROM for shoulder flexion, abduction (limited to 90 degrees), and internal/external rotation (within pain-free limits).
*
Scapular Stabilization:
Gentle isometric exercises (e.g., scapular squeezes).
*
Isometric Strengthening:
Light isometric deltoid and rotator cuff exercises, avoiding positions that stress the SC joint.
*
Core Strengthening:
Maintain overall fitness.
*
Precautions:
* Avoid sudden or forceful movements.
* No heavy lifting or overhead activities.
* Continue to protect against direct trauma to the joint.
Phase 3: Intermediate Strengthening & Advanced Motion (Weeks 12-24)
*
Full AROM:
Aim for full, pain-free active range of motion of the shoulder.
*
Progressive Strengthening:
* Begin light resistance exercises for rotator cuff (internal/external rotation with band), deltoid, and scapular stabilizers.
* Progress to isotonic exercises as tolerated.
* Introduce closed kinetic chain exercises (e.g., wall pushes, plank variations).
*
Proprioception/Neuromuscular Control:
Exercises to improve joint awareness and stability.
*
Precautions:
* Gradual increase in resistance.
* Avoid contact sports or high-impact activities.
Phase 4: Return to Activity/Sport (Months 6+)
*
Advanced Strengthening:
Progress to sport-specific or activity-specific strengthening.
*
Plyometrics:
For athletes, introduce controlled plyometric exercises.
*
Agility & Sport-Specific Drills:
Gradually reintroduce specific movements required for the patient's desired activities.
*
Return to Contact Sports/Heavy Lifting:
Typically not before 6 months, and often 9-12 months post-reconstruction, after achieving full strength, range of motion, and confidence, and with clinical assessment of joint stability.
Key Points:
*
Patient Compliance:
Critical for success.
*
Individualization:
Protocols must be tailored to the patient's individual progress, pain levels, and specific surgical procedure.
*
Communication:
Close collaboration between the surgeon, physical therapist, and patient.
Summary of Key Literature / Guidelines
The literature on SC joint dislocations, while not as voluminous as other shoulder injuries, consistently highlights the critical distinction between anterior and posterior dislocations in terms of management and potential morbidity.
1. Diagnosis:
*
CT scan with IV contrast is the gold standard
for evaluating SC joint dislocations, particularly posterior displacements, providing crucial information on joint displacement and proximity/compression of mediastinal structures. (J Trauma. 2004;57(5):1018-22; J Bone Joint Surg Am. 2000;82(9):1227-36).
* The
serendipity view
on plain radiographs is a helpful initial screening tool but lacks sensitivity and specificity compared to CT.
2. Management of Anterior Dislocations:
*
Non-operative management is generally the preferred approach for acute anterior SC joint dislocations.
Closed reduction, even if successful, often results in recurrence without significant functional impairment or pain (Clin Orthop Relat Res. 2003;(411):110-8).
* Surgical intervention for anterior dislocations is typically reserved for
chronic, symptomatic instability
or significant cosmetic deformity unresponsive to conservative measures. Medial clavicle resection arthroplasty or ligament reconstruction are the primary surgical options (J Bone Joint Surg Am. 2011;93(12):1128-34).
3. Management of Posterior Dislocations:
*
All symptomatic acute posterior SC joint dislocations warrant emergent reduction.
The presence of neurovascular or visceral compromise necessitates urgent intervention (J Bone Joint Surg Am. 2000;82(9):1227-36).
*
Closed reduction
should be attempted under general anesthesia with muscle relaxation, often with vascular/thoracic surgery backup, due to the critical structures involved (J Orthop Trauma. 2017;31 Suppl 3:S30-S35). Techniques involving arm traction and direct manipulation are safer than those utilizing a towel clip behind the clavicle.
*
Open reduction
is indicated if closed reduction fails or if there is persistent mediastinal compromise.
*
Stabilization:
If reduced posterior dislocations are unstable, or in chronic cases, ligament reconstruction using autograft (e.g., semitendinosus, palmaris longus) or allograft is the current standard. Techniques involve creating a figure-of-8 pattern to recreate the costoclavicular and sternoclavicular ligaments (J Shoulder Elbow Surg. 2013;22(2):e1-e11; J Bone Joint Surg Am. 2014;96(10):855-64).
*
Internal fixation with K-wires is strongly discouraged
due to a high rate of severe complications, including migration into the mediastinum (J Bone Joint Surg Am. 1999;81(5):675-81). If used (e.g., in physeal injuries), they must be bent and removed early.
4. Pediatric SC Joint Injuries:
* In skeletally immature patients, what appears to be an SC joint dislocation is often a
Salter-Harris Type I or II epiphyseal fracture
of the medial clavicle. The medial clavicular physis is the last physis to close (around 20-25 years of age).
* Posterior displacement of the epiphysis requires careful reduction due to the same risks as true posterior dislocations in adults (J Bone Joint Surg Am. 2005;87(11):2521-8). Anteriorly displaced physeal injuries are usually treated non-operatively.
5. Outcomes:
* Outcomes for anterior dislocations treated non-operatively are generally good, with high patient satisfaction despite frequent residual deformity.
* Outcomes for surgically managed posterior dislocations are generally favorable when vital structures are protected and stable reduction/fixation is achieved. However, the potential for catastrophic complications remains a significant concern.
* Chronic instability, both anterior and posterior, often responds well to reconstructive surgery, with significant pain relief and functional improvement reported in the literature (J Bone Joint Surg Am. 2011;93(12):1128-34).
In summary, the academic literature underscores the necessity of a high index of suspicion, meticulous diagnostic imaging, and careful surgical planning, particularly for posterior SC joint dislocations, to mitigate the "hidden dangers" associated with this challenging injury.
You Might Also Like