Hybrid Primary Total Hip: A Solution for Complex Joint Pain
Key Takeaway
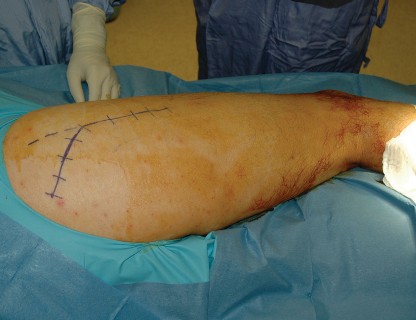
Looking for accurate information on Hybrid Primary Total Hip: A Solution for Complex Joint Pain? A primary total hip arthroplasty treats severe hip osteoarthritis. A "hybrid" approach typically involves an uncemented acetabular component and a cemented femoral component. This method aims to provide optimal fixation and long-term stability, relieving pain and improving mobility for patients like the 86-year-old woman described, who suffered from debilitating right hip pain.
Hybrid Primary Total Hip: A Solution for Complex Joint Pain
Introduction & Epidemiology
Primary total hip arthroplasty (THA) is one of the most successful surgical interventions in terms of pain relief and functional restoration for patients suffering from debilitating hip pathologies. While fully cemented and fully uncemented THA constructs each possess distinct advantages and indications, the hybrid THA —characterized by a cemented femoral stem and an uncemented acetabular component—emerges as a compelling solution for a specific subset of patients presenting with complex joint pain. This construct leverages the immediate, reliable stability of a cemented femoral stem, which is particularly beneficial in cases of compromised femoral bone quality, while capitalizing on the long-term biological fixation and adaptability of an uncemented acetabular cup.
Historically, Sir John Charnley's pioneering work established cemented fixation as the gold standard for THA. However, concerns regarding long-term cement-bone interface failure and aseptic loosening, particularly in younger, more active patients, spurred the development of uncemented designs that relied on biological ingrowth. The hybrid construct arose from a synthesis of these experiences, recognizing that optimal fixation strategies might differ between the acetabulum and the femur depending on patient-specific factors such as age, bone quality, and activity demands.
Epidemiologically, the incidence of hip osteoarthritis and other arthritic conditions necessitating THA continues to rise globally, driven by an aging population and increasing rates of obesity. While the majority of primary THAs today utilize uncemented components, hybrid constructs maintain a significant role, particularly in patient cohorts with osteopenia, osteoporosis, or specific femoral deformities where a durable cement mantle can provide superior initial stability and load transfer. The phrase "complex joint pain" in this context refers to situations where standard approaches might be suboptimal, compelling a surgeon to consider a hybrid approach for a more predictable and robust reconstruction.
Surgical Anatomy & Biomechanics
A thorough understanding of hip joint anatomy and biomechanics is paramount for successful primary THA. The hip is a diarthrodial ball-and-socket joint, providing both stability and mobility.
Acetabular Anatomy
The acetabulum is formed by the fusion of the ilium, ischium, and pubis. Its articular surface, the lunate facies, is crescent-shaped and covered by articular cartilage, encompassing approximately 180 degrees of the femoral head. The non-articular acetabular fossa contains the ligamentum teres and fat pad. Key anatomical landmarks for acetabular component positioning include:
*
Anterior Inferior Iliac Spine (AIIS):
Origin of the rectus femoris and iliofemoral ligament.
*
Transverse Acetabular Ligament (TAL):
Defines the inferior border of the lunate surface, crucial for identifying the true acetabular floor and preventing oversized reaming inferiorly.
*
Acetabular Teardrop:
Radiographic landmark reflecting the anterior column of the acetabulum and ischial spine.
*
Kohler's Line:
Radiographic line from the pelvic brim to the medial aspect of the ischial body, used to assess acetabular protrusion.
Proper restoration of acetabular inclination (typically 40-45 degrees from the transverse pelvic axis) and anteversion (15-20 degrees) is critical for hip stability, range of motion, and minimizing wear.
Femoral Anatomy
The proximal femur consists of the femoral head, neck, and shaft.
*
Femoral Head:
Spherical, covered by articular cartilage, articulating with the acetabulum.
*
Femoral Neck:
Connects the head to the shaft, typically angled at 125-135 degrees (neck-shaft angle) and with 10-20 degrees of anteversion relative to the transcondylar axis.
*
Greater Trochanter:
Provides insertion for gluteus medius and minimus (abductors).
*
Lesser Trochanter:
Provides insertion for the iliopsoas (major hip flexor).
*
Femoral Canal:
The intramedullary canal, whose morphology (Dorr classification: Type A - champagne flute, Type B - normal, Type C - stovepipe) influences cemented stem selection and technique. A Dorr Type C femur, characterized by a wide diaphyseal canal and thin cortices, often favors a cemented femoral stem for reliable fixation.
Musculature & Neurovascular Structures
- Gluteal Muscles (Abductors): Gluteus medius and minimus are critical for gait stability. Deltoid-like action on the hip.
- Deep External Rotators: Piriformis, gemelli, obturator internus, quadratus femoris. Often encountered and sometimes partially released in posterior approaches.
-
Neurovascular Bundles:
- Sciatic Nerve: Most commonly injured nerve in THA, coursing posterior to the hip joint. Risk factors include excessive leg lengthening, posterior approach, hematoma.
- Femoral Nerve: Anterior to the hip, rarely injured with standard approaches, but vulnerable during anterior approaches or with excessively medial retractors.
- Obturator Nerve: Medial to the hip, risk during acetabular reaming or medial screw placement.
Biomechanics of THA
The primary biomechanical goals of THA are:
1.
Restoration of Joint Center of Rotation:
Moving the center of rotation superiorly and medially increases joint contact forces. An ideal placement matches the native hip's center, minimizing stress on the prosthesis and host bone.
2.
Restoration of Femoral Offset:
The horizontal distance from the center of the femoral head to the axis of the femoral shaft. Critical for tensioning the abductor muscles, influencing gait, stability, and prosthetic loosening.
3.
Restoration of Leg Length:
Discrepancy can lead to gait abnormalities, back pain, and nerve palsy. Meticulous templating and intraoperative assessment are crucial.
4.
Component Fixation:
*
Uncemented Acetabular Cup:
Relies on biological ingrowth into a porous surface. Requires a precise press-fit for initial stability and bone apposition.
*
Cemented Femoral Stem:
Achieves immediate mechanical interlock with host bone via a polymethylmethacrylate (PMMA) mantle. Optimal cement technique (distal plug, pulsed lavage, pressurization, vacuum mixing) creates a durable interface, particularly advantageous in osteoporotic bone where biological ingrowth might be delayed or insufficient.

Indications & Contraindications
The decision to proceed with a hybrid primary THA is multifactorial, balancing patient-specific characteristics with implant biomechanics and long-term goals.
Operative Indications for Hybrid THA
A hybrid construct is often favored when there are specific concerns regarding femoral bone quality or patient longevity and activity levels that warrant the unique advantages of this combined fixation strategy.
-
Severe Primary or Secondary Osteoarthritis:
- Disabling pain, stiffness, and functional limitation refractory to extensive non-operative management.
- Radiographic evidence of severe joint space narrowing, subchondral sclerosis, osteophytes, and/or subchondral cysts.
-
Avascular Necrosis (AVN) of the Femoral Head:
- Especially with advanced collapse (Ficat Stage III/IV) and significant pain. A cemented stem can provide reliable fixation despite potentially compromised femoral head/neck bone.
-
Post-Traumatic Arthritis:
- Following acetabular or proximal femoral fractures, or other significant hip trauma.
-
Inflammatory Arthropathies:
- Rheumatoid arthritis, ankylosing spondylitis, psoriatic arthritis leading to debilitating joint destruction. These conditions often present with osteopenic bone, where a cemented stem can offer superior initial stability.
-
Developmental Dysplasia of the Hip (DDH) or Legg-Calve-Perthes Disease:
- With subsequent severe degenerative changes and often associated with abnormal femoral canal morphology or poor bone stock.
-
Compromised Femoral Bone Quality (Dorr Type C or Osteoporosis):
- This is a primary indication for a cemented femoral stem. A wide, stovepipe femoral canal (Dorr Type C) or severe osteoporosis makes achieving adequate press-fit and primary stability with an uncemented stem challenging. Cement provides a predictable and immediate robust fixation.
-
Younger, Active Patients with Adequate Acetabular Bone:
- While uncemented stems are often chosen for younger patients, a hybrid approach allows for the benefits of uncemented acetabular fixation (biological ingrowth, ease of bearing surface revision) while addressing concerns about femoral fixation in cases with less than ideal femoral cancellous bone density or unusual canal geometry.
-
Certain Anatomical Variations or Deformities:
- Post-slipped capital femoral epiphysis (SCFE) or prior femoral osteotomies can alter femoral canal anatomy, sometimes making cemented fixation more predictable.
Contraindications
Contraindications generally apply to all forms of THA, with some nuances for hybrid constructs.
-
Absolute Contraindications:
- Active Infection: Current or recent periprosthetic joint infection (PJI) or other active systemic infection. This requires eradication before elective arthroplasty.
- Rapidly Progressive Neurological Disease: Conditions like advanced Parkinson's disease, severe uncontrolled multiple sclerosis, or progressive muscular dystrophy, which would severely compromise rehabilitation and functional outcomes.
- Severe Vascular Compromise: Insufficient blood supply to the limb to support healing.
- Uncontrolled Systemic Medical Conditions: Severe cardiac, pulmonary, renal, or hepatic disease that poses an unacceptable anesthetic or surgical risk.
- Skeletally Immature Patient: Except in rare, highly specific circumstances (e.g., severe tumor resection) typically requiring specialized revision surgery.
-
Relative Contraindications:
- Morbid Obesity: Increases surgical complexity, complication rates (infection, dislocation, DVT/PE), and potential for earlier implant failure.
- Severe Muscle Weakness or Paralysis: May limit functional recovery despite successful arthroplasty.
- Patient Non-compliance or Unrealistic Expectations: Critical for successful rehabilitation and long-term outcomes.
- Psychiatric Instability or Cognitive Impairment: May hinder adherence to post-operative protocols.
- Severe Osteopenia/Osteoporosis (for uncemented cup): While the hybrid addresses the femoral side, if acetabular bone is severely compromised, an uncemented cup may not achieve sufficient primary stability for ingrowth. However, techniques like screw augmentation or augments can mitigate this.
Summary of Operative vs. Non-Operative Indications
| Operative Indications for Hybrid THA | Non-Operative Considerations (Failed Before THA) |
|---|---|
| Severe primary or secondary osteoarthritis with disabling pain and functional limitation, refractory to non-operative treatment. | Pharmacotherapy (NSAIDs, analgesics, neuropathic pain adjuncts) |
| Avascular necrosis of the femoral head with advanced collapse or severe pain. | Physical therapy, activity modification, assistive devices (cane, walker) |
| Post-traumatic arthritis. | Intra-articular injections (corticosteroids, hyaluronic acid) |
| Inflammatory arthropathies (e.g., rheumatoid arthritis) with joint destruction and associated osteopenia. | Weight management and dietary modifications |
| Select cases of developmental dysplasia of the hip (DDH) or Legg-Calve-Perthes disease with severe degenerative changes. | Lifestyle modification, patient education regarding joint protection |
| Compromised femoral bone quality (Dorr Type C, severe osteoporosis) where reliable cemented fixation is preferred. | |
| **Younger, active patients where biological ingrowth of acetabular component is desired, combined with femoral factors favoring cementation |
Clinical & Radiographic Imaging
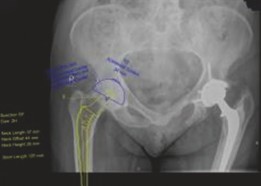

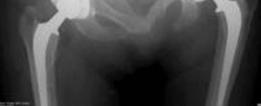

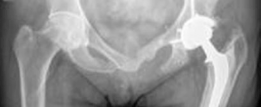
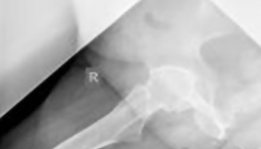
You Might Also Like