Posterolateral Approach to Ankle: Pilon & Posterior Malleolus Fracture Management
Key Takeaway
The posterolateral approach to the ankle is a critical surgical strategy for directly addressing complex pilon and posterior malleolus fractures. It ensures superior visualization for anatomical reduction and stable fixation. This is vital for restoring articular congruity, syndesmotic stability, and preventing long-term sequelae like post-traumatic arthritis.
Introduction & Epidemiology
The posterolateral approach to the ankle is a critical surgical strategy for addressing complex fractures involving the posterolateral aspect of the distal tibia (pilon) and the posterior malleolus. Historically, posterior malleolus fractures, often associated with syndesmotic injuries and rotational forces, were frequently managed indirectly or through medial/anterolateral approaches, leading to challenges in direct reduction and stable fixation. Similarly, posterolateral pilon fractures, characterized by unique fragment morphology and articular displacement, often eluded adequate management via traditional anterior or medial incisions.
Improved understanding of ankle fracture biomechanics, advanced imaging techniques, particularly computed tomography (CT), and the development of specialized instrumentation and plating systems have led to a resurgence and refinement of posterior surgical approaches. The posterolateral approach offers direct visualization and facilitates anatomical reduction and stable internal fixation of these difficult-to-access fragments, crucial for restoring articular congruity and overall ankle stability.
Epidemiologically, ankle fractures are among the most common long bone injuries, with an increasing incidence, particularly in older populations. Posterior malleolus fractures account for 7-44% of all ankle fractures, with varying reported frequencies depending on the classification system and inclusion criteria. Pilon fractures, representing high-energy injuries to the distal tibia, comprise approximately 7-10% of all tibial fractures. The posterolateral fragment pattern in both posterior malleolus and pilon fractures often results from external rotation and abduction forces, sometimes with an axial load component, leading to impaction and comminution that necessitates precise surgical intervention to prevent long-term sequelae such as post-traumatic arthritis and chronic instability.
The growing recognition of the impact of residual posterior malleolar displacement on ankle stability and the articular surface, coupled with the ability of the posterolateral approach to directly address these fragments, has firmly established its role in the orthopedic surgeon's armamentarium for ankle trauma.
Surgical Anatomy & Biomechanics
A thorough understanding of the regional anatomy and the biomechanical implications of posterior fragment injuries is paramount for safe and effective utilization of the posterolateral approach.
Surgical Anatomy
The posterolateral approach navigates a relatively safe internervous and internervascular plane, minimizing direct muscle dissection and critical neurovascular structure compromise when performed meticulously.
-
Bony Structures:
- Distal Tibia (Pilon): The posterior aspect of the distal tibia forms the posterior articular roof of the ankle joint. Fractures in this region can involve significant articular impaction and comminution. The posterolateral aspect specifically includes the incisura fibularis (fibula notch) and the insertion of the posterior inferior tibiofibular ligament (PITFL).
- Posterior Malleolus: This is the posterior lip of the distal tibia, varying in size and morphology. It serves as the primary attachment site for the PITFL, a critical component of the syndesmosis. Large posterior malleolar fragments, particularly those involving >25-30% of the articular surface, often indicate significant syndesmotic instability due to disruption of the PITFL attachment.
- Fibula: The lateral malleolus articulates with the fibular notch of the tibia. Its integrity is crucial for syndesmotic stability. The posterolateral approach provides excellent access to the posterior aspect of the fibula, facilitating combined fixation of lateral malleolar fractures or posterior fibular plating when indicated.
- Talus: The trochlea of the talus articulates with the distal tibia and fibula. Restoration of the tibiotalar relationship is the primary goal of fracture fixation.
-
Soft Tissue Structures:
- Skin and Subcutaneous Tissue: The incision is made through these layers. Careful attention must be paid to soft tissue handling to prevent wound complications.
-
Nerves:
- Sural Nerve: This purely sensory nerve runs superficially along the posterolateral aspect of the lower leg, typically coursing with the small saphenous vein. It is vulnerable during the skin incision and initial dissection, especially at the level of the ankle joint. It should be identified and protected, usually retracted anteriorly with the peroneal tendons.
- Posterior Tibial Nerve: Located more medially and deep, within the tarsal tunnel (posterior to the medial malleolus), it is generally not at direct risk with a strictly posterolateral approach.
-
Vessels:
- Small Saphenous Vein: Accompanies the sural nerve and is similarly vulnerable. It can be ligated if necessary, but preservation is preferred.
- Peroneal Artery: Located deep in the posterior compartment, more medially. Not typically at risk.
- Posterior Tibial Artery: Located medially in the tarsal tunnel. Not at risk.
-
Tendons:
- Achilles Tendon: Forms the posterior boundary of the approach. Retracted medially.
- Flexor Hallucis Longus (FHL): Located deep and medial to the Achilles, it runs through its own groove on the posterior tibia. It is sometimes exposed during deeper dissection of pilon fractures but generally preserved.
- Peroneal Tendons (Longus and Brevis): Run laterally and anteriorly to the incision. These are mobilized and retracted anteriorly to expose the posterior aspect of the distal tibia and fibula. Their sheath is typically incised longitudinally.
- Flexor Digitorum Longus (FDL) and Tibialis Posterior (TP): Located more medially and deeper within the posterior compartment, they are generally not directly exposed or at risk with the posterolateral approach.
-
Ligaments:
- Posterior Inferior Tibiofibular Ligament (PITFL): The primary ligament attaching to the posterior malleolus. Disruption or avulsion of this ligament is a key indicator of syndesmotic instability and its integrity must be assessed. Direct repair or reattachment is often required.
- Transverse Ligament: A deep portion of the PITFL, also critical for syndesmotic stability.
- Intermalleolar Ligament: Connects the distal tibia and fibula, often disrupted in syndesmotic injuries.
Biomechanics
-
Posterior Malleolus Fractures:
- Mechanism: Typically caused by external rotation with or without axial load. The talus rotates externally, impacting the posterior aspect of the distal tibia.
- Stability: The PITFL is the primary stabilizer of the posterior syndesmosis. Displaced posterior malleolus fractures imply disruption of the PITFL (either avulsion from the tibia or fibula, or mid-substance tear). This directly affects syndesmotic stability. Large posterior fragments can also lead to posterior talar subluxation.
- Articular Congruity: Significant displacement of the posterior malleolus fragment (e.g., >25-30% of articular surface, or >2mm step-off/gap) can lead to incongruity of the tibiotalar joint, increasing contact pressures and predisposing to post-traumatic arthritis.
-
Posterolateral Pilon Fractures:
- Mechanism: High-energy axial compression combined with rotational and shear forces. The posterolateral fragment pattern often results from the talus driving superiorly and posteriorly, impacting the distal tibia.
- Stability: These fractures involve portions of the articular surface and metaphysis. They can be highly unstable due to comminution and impaction. The extent of articular disruption and metatarsal-diaphyseal dissociation dictates the overall stability.
- Articular Congruity: The primary biomechanical concern is the restoration of the articular surface and axial alignment. Displaced fragments lead to joint incongruity, altered load distribution, and subsequent degenerative changes.
The posterolateral approach allows direct assessment and manipulation of these critical structures, enabling precise anatomical reduction and stable fixation, which are paramount for restoring normal ankle kinematics and long-term function.
Indications & Contraindications
The decision to utilize a posterolateral approach for ankle fractures is based on a meticulous evaluation of fracture morphology, associated injuries, patient factors, and the surgeon's experience. Advanced imaging, particularly CT, is indispensable for this assessment.
Indications
Operative Indications (Posterolateral Approach)
-
Displaced Posterior Malleolus Fractures:
- Fragment Size: Generally accepted threshold is >25-30% of the distal tibial articular surface involved. Some authors advocate for operative fixation for fragments as small as 10-15% if significant displacement (>2mm) or syndesmotic instability is present.
- Displacement: Any articular step-off or gap greater than 2mm, or any posterior talar subluxation.
- Associated Syndesmotic Instability: When associated with a fibula fracture and/or deltoid ligament injury, a displaced posterior malleolus fragment often implies syndesmotic instability, necessitating direct reduction and stabilization of the posterior malleolus.
- Inability to Achieve/Maintain Closed Reduction: If closed reduction and casting fail to achieve anatomical reduction of the posterior fragment, operative intervention is indicated.
-
Posterolateral Pilon Fractures:
- Articular Displacement: Displaced articular fragments requiring direct visualization and reduction. The posterolateral fragment in pilon fractures can be distinct and challenging to access anteriorly.
- Comminution and Impaction: While comminution may dictate staged management, the posterolateral approach provides the best exposure for direct reduction and support of the posterolateral articular segment.
- Fracture-Dislocations: Often requiring open reduction due to significant displacement and soft tissue interposition.
-
Specific Fracture Patterns:
- "Posterolateral Fragment" of the Distal Tibia: This is a distinct fragment pattern, often involving the entire posterolateral corner of the distal tibia, including the fibular incisura. It often accompanies fibular fractures and requires direct posterolateral stabilization.
- Combined Malleolar Fractures: When a significant posterior malleolus fracture coexists with lateral (and sometimes medial) malleolar fractures, the posterolateral approach can be combined with other incisions or utilized for primary posterior fixation.
Non-Operative Indications
- Minimally Displaced Posterior Malleolus Fractures: Small posterior malleolus fragments (<10-15% of articular surface) without significant displacement (<2mm) or evidence of syndesmotic instability.
- Non-displaced or stable Pilon Fractures: Extremely rare for posterolateral pilon fractures; usually implies a very minimal, stable injury without articular step-off.
- High Surgical Risk Patients: Patients with severe medical comorbidities that contraindicate surgery, provided the fracture is stable and minimally displaced.
- Severe Soft Tissue Compromise: In rare instances where soft tissue envelope prohibits surgery and internal fixation, external fixation or conservative management may be considered as a temporizing or definitive measure, though this often results in suboptimal outcomes for displaced articular fractures.
Contraindications
Absolute Contraindications
- Active Infection at the Surgical Site: Increases the risk of osteomyelitis and deep surgical site infection.
-
Severe Soft Tissue Compromise:
- Gross Contamination in Open Fractures: Requires initial debridement and delayed definitive fixation.
- Extensive Blistering/Skin Necrosis: The skin envelope must be viable for surgery. Staged management (external fixation, soft tissue healing) is essential.
- Irremediable Medical Comorbidities: Conditions that render the patient unfit for anesthesia and surgery (e.g., severe cardiac decompensation, uncontrolled sepsis).
Relative Contraindications
- Significant Peripheral Vascular Disease: Compromised healing potential and increased risk of wound complications. A vascular consult is essential.
- Uncontrolled Diabetes Mellitus: Poor glycemic control significantly increases infection and wound complication rates.
- Severe Osteopenia/Osteoporosis: May make stable fixation challenging; alternative fixation strategies or adjunctive bone augmentation may be considered.
- Patient Non-Compliance: May compromise post-operative rehabilitation and outcomes.
- Extensive Comminution with Bone Loss: While fixation is often attempted, severe bone loss may require bone grafting or consider primary arthrodesis in select cases, though this is rare for primary treatment of posterior malleolus.
Table: Operative vs. Non-Operative Indications
| Feature | Operative Indication (Posterolateral Approach) | Non-Operative Indication |
|---|---|---|
| Posterior Malleolus | - Fragment size >25-30% (some sources >10-15%) of articular surface. | - Fragment size <10-15% of articular surface. |
| - Articular step-off/gap >2mm. | - Articular step-off/gap <2mm. | |
| - Posterior talar subluxation. | - No talar subluxation. | |
| - Associated syndesmotic instability. | - No syndesmotic instability. | |
| - Inability to achieve/maintain closed reduction. | - Anatomical or near-anatomical reduction achieved and maintained with casting/boot. | |
| Posterolateral Pilon | - Displaced articular fragments requiring direct visualization. | - Extremely rare (e.g., minimally displaced, stable fissure fracture without articular step-off). Typically requires operative stabilization due to high-energy mechanism and articular involvement. |
| - Any significant articular step-off or axial malalignment. | ||
| Soft Tissue Envelope | - Stable and viable soft tissue envelope. | - Severe soft tissue compromise (e.g., extensive blistering, gross contamination in open fractures) preventing immediate internal fixation (often indicates staged approach with external fixation rather than definitive non-operative management). |
| Patient Factors | - Medically optimized patient suitable for anesthesia and surgery. | - Severe medical comorbidities precluding surgery (rarely a primary indication for non-operative management of a significantly displaced fracture). |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is critical for optimizing outcomes and minimizing complications with the posterolateral approach.
Pre-Operative Planning
-
Clinical Assessment:
- Neurovascular Status: Thorough assessment of distal pulses, sensation (especially sural nerve distribution), and motor function.
- Soft Tissue Envelope: Inspection for swelling, ecchymosis, blistering, or open wounds. Severe swelling or blistering necessitates delayed surgery, often with a period of elevation, ice, and immobilization (e.g., posterior splint, external fixator) until the "wrinkle sign" returns.
- Pain and Deformity: Document initial presentation.
-
Imaging Review:
- Plain Radiographs: AP, lateral, and mortise views are initial steps. They provide information on overall alignment, fibula fracture pattern, and gross displacement. The lateral view is crucial for assessing posterior malleolus size and displacement.
-
Computed Tomography (CT) Scan:
Absolutely essential
for posterolateral pilon and posterior malleolus fractures.
- 3D Reconstruction: Provides invaluable information on fracture morphology, fragment size, number, and location (especially of the posterior malleolus and posterolateral pilon fragments).
- Articular Surface: Clearly delineates articular step-off, impaction, and comminution, which may be missed on plain radiographs.
- Syndesmosis: Helps assess the integrity of the fibular incisura and the attachment of the PITFL.
- Surgical Approach Selection: Confirms the appropriateness of the posterolateral approach by identifying fragment patterns best addressed posteriorly.
- MRI: Rarely indicated acutely for fracture assessment. May be useful in chronic instability cases or to evaluate extensive soft tissue damage if the diagnosis is unclear, but not routinely needed for acute fracture planning.
-
Surgical Timing:
- Acute vs. Delayed: Most ankle fractures are typically managed acutely (within 24-48 hours) if the soft tissues allow. High-energy pilon fractures or those with severe soft tissue compromise often require staged management, beginning with external fixation and delaying definitive internal fixation until the soft tissue swelling has subsided (e.g., 7-14 days).
- Open Fractures: Require immediate surgical debridement. Definitive fixation may be delayed.
-
Templating and Implant Selection:
- Plates: Consider posterior antiglide plates (e.g., 1/3 tubular plate), locking plates specifically designed for posterior malleolus or posterior pilon fragments (e.g., "posterior pilon plates"), and conventional locking plates for fibula fixation. Pre-contoured plates often conform well to the anatomy.
- Screws: Lag screws (partially threaded) for interfragmentary compression. Cortical screws for plate fixation. Screw lengths and trajectories should be planned based on CT.
- Syndesmotic Fixation: If syndesmotic instability persists after posterior malleolus fixation (less common if the PITFL is adequately repaired/reduced), consider syndesmotic screw (e.g., 3.5mm, 4.5mm) or suture-button fixation.
- Bone Graft: Autograft (e.g., iliac crest, distal tibia, calcaneus) or allograft may be needed for significant metaphyseal defects in pilon fractures to support the reduced articular fragments.
-
Operating Room Setup:
- Fluoroscopy: Essential for intraoperative imaging (AP, lateral, mortise views, Broch's view for posterior malleolus).
- Tourniquet: Standard for ankle surgery to optimize visualization and minimize blood loss.
- Instrument Tray: Small fragment set, mini-fragment set, reduction clamps (pointed, ball-spiked), elevators (Freer, periosteal), small osteotomes.
Patient Positioning
The choice of patient position is crucial for optimal exposure and surgeon comfort. Both prone and lateral decubitus positions have advantages.
-
Prone Position (Most Common for Posterolateral Approach):
-
Advantages:
- Excellent direct visualization of the entire posterior aspect of the distal tibia and fibula.
- Allows for easy access to the lateral malleolus if a combined lateral plate is required for fibular fixation.
- The leg rests naturally, allowing stable positioning for fluoroscopy.
-
Disadvantages:
- More challenging for anesthetic access to the airway if intubated.
- Requires careful padding of pressure points (chest rolls, knees, ankles) to prevent nerve compression (e.g., common peroneal nerve at fibular head, ulnar nerve).
- Can be challenging for obese patients.
-
Setup:
- Patient is placed prone on the operating table.
- Bolsters (e.g., chest rolls) are placed longitudinally to support the torso, allowing the abdomen to hang free and minimize vena caval compression.
- Knees are slightly flexed with soft padding.
- Ankles are supported, with the foot slightly dorsiflexed or in neutral.
- A well-padded tourniquet is applied high on the thigh.
- Fluoroscopy unit is positioned on the contralateral side of the table for easy C-arm access.
-
Advantages:
-
Lateral Decubitus Position:
-
Advantages:
- Easier anesthetic access to the airway.
- May be more comfortable for certain patients.
- Allows for access to the medial malleolus if a combined medial approach is also needed.
-
Disadvantages:
- Requires careful draping and positioning to ensure stable access to the posterolateral aspect.
- The leg needs to be supported in a specific manner (e.g., with a leg holder) to maintain adequate exposure, which can sometimes interfere with C-arm access or require a second assistant.
- Access to the anterior/medial ankle may be easier, but direct visualization posteriorly can be more challenging than in prone.
-
Setup:
- Patient is placed in a lateral decubitus position on the contralateral side of the injured ankle (e.g., right ankle injury, left lateral decubitus).
- Pillows/bolsters are used for support between the legs and under the upper arm.
- A beanbag or specialized leg holder can help stabilize the leg.
- The injured leg is flexed at the hip and knee, with the foot draped freely or positioned in a stirrup that allows for rotation.
- Tourniquet applied high on the thigh.
- Fluoroscopy unit positioned accordingly.
-
Advantages:
Regardless of position, ensure adequate padding, confirm neurovascular integrity pre- and post-positioning, and prepare the surgical field meticulously to ensure sterile conditions and optimal visualization.
Detailed Surgical Approach / Technique
The detailed surgical technique for the posterolateral approach involves precise dissection, anatomical reduction of fragments, and stable internal fixation.
1. Incision and Initial Dissection
- Incision: A longitudinal incision is made along the posterolateral aspect of the distal leg, extending from approximately 8-10 cm proximal to the tip of the lateral malleolus to the level of the calcaneus. The incision typically runs just medial to the palpable border of the fibula and lateral to the Achilles tendon.
- Skin and Subcutaneous Tissue: Carefully incise the skin and subcutaneous tissue. Identify and protect the sural nerve and small saphenous vein , which lie superficially in this plane. These structures typically run between the Achilles tendon and the peroneal tendons and should be mobilized and retracted anteriorly with the peroneal tendons.
- Deep Fascia: Incise the deep fascia longitudinally, just anterior to the Achilles tendon and posterior to the peroneal compartment.
2. Internervous Plane & Exposure
-
Identify the Interval:
The key internervous and internervascular plane for this approach is between the:
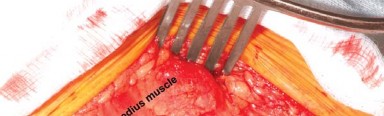
- Medially/Posteriorly: Achilles tendon and flexor hallucis longus (FHL) muscle belly.
- Anterolaterally: Peroneal tendons (longus and brevis) and their muscle belly.
-
Mobilization and Retraction:
- Carefully release the sheath of the peroneal tendons posteriorly.
- The peroneal tendons are then gently retracted anteriorly using blunt retractors (e.g., Hohmanns, army-navy, or self-retaining retractors), revealing the posterior aspect of the distal fibula and the posterior face of the tibia.
- The Achilles tendon and FHL muscle are retracted medially .
- Exposure of Fibula and Tibia: This interval directly exposes the posterior aspect of the distal fibula and the posterior facet of the distal tibia (posterior malleolus/pilon). The posterior inferior tibiofibular ligament (PITFL) and the transverse ligament insertion sites on the posterior malleolus will be visible.
3. Fracture Reduction
- Debridement: Remove any hematoma, loose bone fragments, or soft tissue interposition that may impede reduction.
- Direct Visualization: The primary advantage of this approach is direct visualization of the articular surface of the posterior malleolus and posterolateral pilon fragments.
-
Reduction Techniques for Posterior Malleolus:
- Large Fragment: If the posterior malleolus is a single, large fragment, use a ball-spiked pusher or a small pointed reduction clamp to manipulate it directly back into anatomical position. Gentle traction on the foot can help de-impact fragments.
- Impaction: For impacted fragments, a small osteotome or Freer elevator can be used to disimpact and elevate the articular surface. Ensure the articular surface is fully restored.
- Temporary Fixation: Once anatomical reduction is achieved, maintain it with temporary K-wires (e.g., 1.2-1.6mm) drilled from posterior to anterior into the distal tibia, ensuring they are not within the intended screw path.
- Syndesmotic Assessment: Assess syndesmotic stability after reduction and temporary fixation of the posterior malleolus. Often, reduction of the posterior malleolus (and repair of PITFL) restores syndesmotic stability.
-
Reduction Techniques for Posterolateral Pilon Fractures:
- Fragment Identification: Identify all major fragments, especially the key articular segment.
- Indirect Reduction (if needed): Traction, manipulation of the foot, and gentle external rotation can help reduce gross displacement.
- Direct Reduction: Use elevators, small reduction clamps, and bone hooks to restore the articular surface and metaphyseal alignment. For impacted areas, elevate the articular fragments and consider bone grafting if there is a significant underlying metaphyseal defect.
- Restoration of Fibular Length: If a fibula fracture is present, ensure its length and rotation are restored first, as this can help guide the reduction of the posterior tibial fragments (often performed via the same posterolateral incision, plating the posterior aspect of the fibula).
- Temporary Fixation: Use K-wires to hold reduced fragments.
4. Internal Fixation
The choice of fixation varies depending on the fracture pattern and surgeon preference.
-
Posterior Malleolus Fixation:
- Lag Screws: For large, single fragments, use one or two 3.5mm or 4.0mm partially threaded cancellous lag screws. These are typically inserted from posterior to anterior, angling slightly superiorly and anteriorly, engaging the strong anterior tibial cortex. Ensure screws are perpendicular to the fracture plane for optimal compression.
- Posterior Antiglide Plate: A 1/3 tubular plate or a specialized posterior malleolus locking plate can be applied to the posterior aspect of the tibia. This provides buttress support to the posterior fragment, preventing posterior displacement. Screws are placed through the plate into the main tibial metaphysis and diaphysis. This plate also serves as a tension band to compress lag screws if used.
- Positioning: The plate should be contoured to fit the posterior aspect of the tibia and extend proximally enough to achieve good purchase in the bone. Ensure no impingement with the FHL tendon sheath.
-
Posterolateral Pilon Fixation:
- Lag Screws: Interfragmentary lag screws are used for primary articular reduction and compression of large fragments.
- Locking Plate Fixation: Specialized posterior pilon plates (often pre-contoured) or conventional locking plates are used to buttress the articular fragments and provide stable fixation to the metaphysis and diaphysis. These plates are applied to the posterior or posterolateral surface of the distal tibia.
- Screw Trajectory: Screws must be carefully aimed to avoid articular penetration. Use fluoroscopy in multiple planes.
- Bone Grafting: If significant metaphyseal bone loss or impaction exists beneath reduced articular fragments, bone graft (autograft or allograft) should be placed to provide structural support and prevent collapse. This is particularly important in high-energy pilon fractures.
- Fibula Fixation: If the fibula is fractured, it can often be fixed through the same incision by extending the exposure laterally to plate the posterior aspect of the fibula. This is often performed first to establish fibular length.
-
Syndesmotic Fixation (if necessary):
- After posterior malleolus fixation, reassess syndesmotic stability using intraoperative stress tests (e.g., external rotation stress, cotton test).
- If instability persists, additional fixation may be needed. This is less common after direct posterior malleolus fixation with PITFL repair.
- Options: 3.5mm or 4.5mm tricortical syndesmotic screw (typically 1-2 cm above the tibiotalar joint line, through 3 or 4 cortices) or suture-button construct (e.g., TightRope).
5. Intraoperative Fluoroscopy
-
Obtain AP, lateral, and mortise views to confirm:
- Anatomical reduction of all fragments.
- Appropriate plate and screw positioning.
- No articular screw penetration.
- Restoration of overall alignment and mortise integrity.
- Syndesmotic reduction.
- Broch's View: A specific lateral oblique view (approximately 30-45 degrees internal rotation from true lateral) can be useful to better visualize the posterior malleolus fragment and confirm reduction.
6. Wound Closure
- Irrigation: Thoroughly irrigate the wound with sterile saline.
- Drain: A small suction drain may be considered if significant bleeding is anticipated, especially in complex pilon fractures, but it is not always necessary for posterior malleolus fractures.
- Deep Fascia: Close the deep fascia over the peroneal tendons meticulously.
- Subcutaneous Tissue: Approximate the subcutaneous tissue.
- Skin: Close the skin with staples or sutures, ensuring tension-free closure. Apply a sterile dressing and a well-padded posterior splint in a neutral position.
Throughout the procedure, meticulous soft tissue handling, careful hemostasis, and precise anatomical reduction under direct visualization are key to achieving optimal functional outcomes and minimizing complications.
Complications & Management
Despite meticulous surgical technique, complications can occur following the posterolateral approach to the ankle. Awareness of these potential issues and their management is crucial.
Common Complications
-
Sural Nerve Injury:
- Incidence: Highly variable, reported from 5-30%. Can range from temporary neurapraxia to permanent transection.
- Mechanism: Direct injury during skin incision or superficial dissection, or entrapment/stretch injury from retraction.
- Symptoms: Sensory deficit (numbness, tingling) along the lateral aspect of the foot and ankle, potentially chronic neuropathic pain.
-
Management:
- Prevention: Careful identification and protection of the nerve during initial dissection.
- Intraoperative: If transected, consider direct repair or nerve graft depending on the gap. If severely stretched, neurolysis.
- Post-operative: Conservative management for neurapraxia (observation, NSAIDs). For persistent symptoms or neuroma formation, surgical exploration, neurolysis, or neuroma excision/relocation may be required. Referral to a peripheral nerve specialist may be indicated.
-
Wound Complications:
- Incidence: 5-15%, higher in pilon fractures, diabetics, smokers, and patients with significant soft tissue injury. Includes dehiscence, infection, and necrosis.
- Mechanism: Poor soft tissue handling, excessive tension, hematoma, infection, compromised vascularity.
- Symptoms: Erythema, swelling, discharge, pain, fever (for infection); wound gapping, tissue non-viability.
-
Management:
- Prevention: Careful incision planning, gentle tissue handling, meticulous hemostasis, layered tension-free closure, proper post-operative wound care.
- Dehiscence: Local wound care, serial debridement, secondary closure, or delayed skin grafting/flaps for large defects.
- Superficial Infection: Oral antibiotics, local wound care.
- Deep Infection: Surgical debridement, intravenous antibiotics, potentially hardware removal (once fracture is healed), antibiotic beads, or negative pressure wound therapy.
-
Nonunion/Malunion:
- Incidence: Nonunion <5% for posterior malleolus; malunion incidence varies but can be significant, especially in pilon fractures if anatomical reduction is not achieved.
- Mechanism: Inadequate reduction, insufficient stability of fixation, poor bone healing potential, infection, large bone defect.
- Symptoms: Persistent pain, deformity, instability, functional limitation.
-
Management:
- Prevention: Anatomical reduction, stable fixation, appropriate bone graft for defects.
- Nonunion: Surgical revision with debridement, stable internal fixation, and bone grafting (autograft preferred).
- Malunion: Corrective osteotomy (if symptomatic and functional deficit) or arthrodesis for severe malunion with debilitating arthritis.
-
Post-Traumatic Arthritis (PTA):
- Incidence: Up to 50% for pilon fractures, 10-20% for posterior malleolus, especially with residual articular step-off.
- Mechanism: Residual articular incongruity, cartilage damage at time of injury, altered joint mechanics.
- Symptoms: Chronic pain, stiffness, swelling, decreased range of motion.
-
Management:
- Prevention: Paramount - anatomical articular reduction is key.
- Early: Activity modification, NSAIDs, intra-articular injections (corticosteroids, hyaluronic acid).
- Advanced: Arthroscopic debridement, osteochondral grafting (if focal), distraction arthroplasty, ankle arthrodesis, or total ankle arthroplasty (for severe, diffuse PTA in suitable candidates).
-
Hardware Irritation:
- Incidence: Common, 10-20%, especially with plates or screws prominent under the skin.
- Mechanism: Prominent hardware causing impingement or irritation of soft tissues or skin.
- Symptoms: Localized pain, tenderness, skin irritation, sometimes bursitis.
- Management: Hardware removal after fracture healing (typically 6-12 months post-op).
-
Syndesmotic Malreduction:
- Incidence: 5-10% of cases involving syndesmotic injury, even after posterior malleolus fixation.
- Mechanism: Inadequate reduction of the posterior malleolus and PITFL, or malreduction of associated fibula fracture. Can also occur if an additional syndesmotic screw is improperly placed.
- Symptoms: Persistent pain, instability, limited range of motion, post-traumatic arthritis.
-
Management:
- Prevention: Intraoperative fluoroscopic assessment (e.g., perfect mortise, Cotton test), direct visualization of PITFL.
- Revision: If symptomatic, malreduced syndesmosis may require revision surgery, including hardware removal, repeat reduction, and stable fixation (screw or suture button).
-
Deep Vein Thrombosis (DVT) / Pulmonary Embolism (PE):
- Incidence: DVT 1-20% (clinical vs. asymptomatic), PE <1%.
- Mechanism: Immobility, surgical trauma, hypercoagulable state.
- Symptoms: DVT: calf pain, swelling, tenderness. PE: dyspnea, chest pain, cough, hypoxemia.
-
Management:
- Prevention: Standard DVT prophylaxis (pharmacological, mechanical).
- Treatment: Anticoagulation.
Table: Common Complications, Incidence, and Salvage Strategies
| Complication | Approximate Incidence | Salvage Strategies |
|---|---|---|
| Sural Nerve Injury | 5-30% | - Observation for neurapraxia (NSAIDs) |
| - Surgical exploration, neurolysis, neuroma excision/relocation for persistent symptoms. | ||
| Wound Complications | 5-15% | - Local wound care, antibiotics (superficial) |
| (Dehiscence, Infection, Necrosis) | - Surgical debridement, IV antibiotics, negative pressure wound therapy (deep infection) | |
| - Secondary closure, skin grafting, flap coverage (dehiscence/necrosis) | ||
| Nonunion / Malunion | <5% / Variable | - Nonunion: Revision fixation, debridement, bone grafting. |
| - Malunion: Corrective osteotomy, ankle arthrodesis. | ||
| Post-Traumatic Arthritis (PTA) | 10-50% | - Conservative management (NSAIDs, injections, activity modification) |
| - Arthroscopic debridement, osteochondral grafting | ||
| - Ankle arthrodesis, total ankle arthroplasty (end-stage) | ||
| Hardware Irritation | 10-20% | - Hardware removal (after fracture healing) |
| Syndesmotic Malreduction | 5-10% | - Revision surgery: hardware removal, repeat reduction, appropriate fixation (screw or suture button) |
| Deep Vein Thrombosis (DVT) | 1-20% | - Anticoagulation therapy |
| Pulmonary Embolism (PE) | <1% | - Anticoagulation therapy, supportive care |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation following the posterolateral approach aims to restore ankle function, strength, and range of motion while protecting the healing fracture. Protocols are tailored to individual patient factors, fracture stability, and fixation achieved. The following outlines a general, progressive guideline.
Phase 1: Immobilization & Early Healing (Weeks 0-6/8)
- Goal: Protect surgical repair, minimize pain and swelling, maintain soft tissue mobility.
-
Immobilization:
- Immediately post-op: Well-padded posterior splint (neutral dorsiflexion/plantarflexion) for 2-3 weeks.
- Transition to: Removable walking boot (CAM walker) at 2-3 weeks, allowing for wound checks and gentle exercises.
-
Weight Bearing:
- Non-Weight Bearing (NWB): Essential for 6-8 weeks, or longer for complex pilon fractures or if significant comminution/bone graft was utilized.
- Emphasis on: Touch-down weight bearing (TDWB) only for balance if using crutches/walker.
-
Pain & Swelling Management:
- Elevation above heart level (especially for the first 1-2 weeks).
- Ice therapy.
- Prescribed analgesia.
-
Exercises (Non-Weight Bearing):
- Week 0-2: Gentle toe wiggles, isometric quad and gluteal contractions. Avoid active ankle plantar/dorsiflexion to protect the posterior structures.
-
Week 2-6/8:
In the walking boot (removed for exercises):
- Gentle active and passive range of motion (ROM) of the ankle (dorsiflexion, plantarflexion, inversion, eversion) within pain-free limits. Avoid aggressive stretching or stress on posterior structures.
- Subtalar joint mobilization.
- Knee and hip ROM exercises.
- Upper extremity strengthening.
- Non-weight bearing core exercises.
- Wound Care: Regular wound checks, dressing changes, staple/suture removal around 2-3 weeks.
Phase 2: Controlled Weight Bearing & Progressive Strengthening (Weeks 6/8 - 12)
- Goal: Gradually restore full weight bearing, improve ankle ROM, initiate gentle strengthening.
-
Weight Bearing:
- Gradual progression from NWB to Partial Weight Bearing (PWB) in the walking boot at 6-8 weeks, based on radiographic healing and clinical comfort.
- PWB progression: Typically 25% for 1-2 weeks, then 50% for 1-2 weeks, then 75% for 1-2 weeks, advancing to full weight bearing (FWB) over 4-6 weeks.
- Once FWB is achieved, transition out of the boot to supportive shoes (e.g., athletic trainers).
-
Exercises:
- ROM: Continue and progress active and passive ankle ROM, aiming for near-normal range. Manual therapy for joint mobilization as tolerated.
-
Strengthening (Begin gentle isometrics, then progress):
- Ankle isometrics (plantarflexion, dorsiflexion, inversion, eversion).
- Theraband exercises (gentle resistance).
- Gastroc/soleus stretches.
- Proprioceptive exercises (e.g., single leg balance, wobble board standing) as tolerated in the boot and then in shoes.
- Gait Training: Focus on normal gait mechanics with crutches, progressing to single crutch, then no aids.
Phase 3: Advanced Strengthening & Functional Return (Weeks 12 - 6 Months)
- Goal: Achieve full ankle ROM and strength, restore balance and proprioception, prepare for return to activity.
- Weight Bearing: Full weight bearing in supportive shoes.
-
Exercises:
- Strength: Progress resistance exercises (Theraband, resistance machines, calf raises – bilateral to unilateral, heel-toe raises).
- Proprioception: Advanced balance exercises, single-leg stance with perturbations.
- Plyometrics (if applicable and appropriate for injury type/patient): Controlled jumping and landing drills (initiate only after significant strength and stability achieved, typically >4-5 months).
- Agility Drills: Ladder drills, cone drills, figure-of-eight patterns.
- Endurance: Cycling, swimming, elliptical trainer.
-
Activity-Specific Training:
- Gradual return to sport-specific activities, ensuring adequate strength, stability, and pain-free range of motion.
- Emphasis on proper warm-up, cool-down, and stretching.
Phase 4: Return to Sport / Long-Term (Months 6+)
- Goal: Full unrestricted return to activities and sport, maintain long-term ankle health.
- Return to Sport: Guided by physician and physical therapist. Criteria often include full pain-free ROM, symmetrical strength (>90% compared to contralateral side), good balance, and successful completion of sport-specific drills.
- Long-Term: Continue home exercise program, particularly strengthening and proprioceptive exercises, to minimize risk of reinjury and manage any residual symptoms. Monitor for signs of post-traumatic arthritis.
Important Considerations:
- Individualization: Protocols must be individualized. High-energy pilon fractures with extensive comminution or bone grafting may require longer NWB periods and slower progression.
- Pain as a Guide: Pain should always be respected. Exercises should not exacerbate pain significantly.
- Radiographic Healing: Progression through weight-bearing phases should be confirmed by radiographic evidence of fracture healing.
- Surgeon Communication: Close communication between the surgeon, physical therapist, and patient is essential for optimal outcomes.
Summary of Key Literature / Guidelines
The evolution of the posterolateral approach for ankle fractures, particularly those involving the posterior malleolus and posterolateral pilon, is supported by a growing body of literature highlighting its advantages in specific fracture patterns.
-
Direct Visualization and Anatomical Reduction:
- Seminal works by authors like Gardner et al. (2006, 2008) have emphasized the importance of direct visualization and anatomical reduction of posterior malleolus fragments. Their biomechanical studies demonstrated that direct reduction and stable fixation of the posterior malleolus significantly improve syndesmotic stability compared to indirect reduction or isolated syndesmotic screw fixation when the PITFL is disrupted.
- The literature consistently highlights that residual articular step-off, even as small as 1-2 mm, correlates with increased risk of post-traumatic arthritis and poor functional outcomes. The posterolateral approach offers the best means to achieve and verify anatomical reduction of these fragments.
-
Role of CT Imaging:
- Multiple studies underscore the indispensable role of pre-operative CT imaging for all complex ankle fractures, especially those involving the posterior malleolus and pilon. CT allows for precise mapping of fracture lines, fragment size and orientation, articular involvement, and helps in planning the optimal surgical approach (e.g., identifying the posterolateral fragment that dictates this approach).
- Historically, plain radiographs often underestimated the size and displacement of posterior fragments. CT has been instrumental in changing surgical paradigms to favor direct fixation.
-
Fragment Size for Operative Intervention:
- While historically a 25-30% involvement of the articular surface was the most common threshold for posterior malleolus fixation, recent literature suggests that smaller fragments may warrant fixation if they are displaced (>2mm step-off/gap) or contribute to syndesmotic instability.
- A study by Vrahas et al. demonstrated that even smaller, displaced posterior malleolus fragments can significantly compromise stability. This shift towards lower thresholds for operative intervention is largely facilitated by the enhanced visualization and stability offered by the posterolateral approach.
- For pilon fractures, any significant articular displacement (typically >1-2mm) is an indication for operative management, and the posterolateral approach is crucial for specific fragment types.
-
Comparison to Other Approaches:
- The posterolateral approach is increasingly recognized as superior to an anterolateral or medial approach for posterior malleolus and posterolateral pilon fragments due to direct access, allowing for anatomical reduction under direct vision and rigid fixation. Indirect reduction techniques, particularly for large or impacted fragments, are often unreliable in achieving and maintaining anatomical congruity.
- Studies comparing posterior versus anterior approaches for posterior malleolus have shown reduced rates of malreduction with direct posterior approaches.
-
Fixation Principles:
- The use of antiglide plates or anatomically contoured locking plates applied to the posterior aspect of the tibia is well-supported. These plates provide buttress support and enhance stability, particularly for comminuted or impacted fragments.
- Interfragmentary lag screws provide compression and are critical for large, well-defined fragments.
- Attention to fibular length and rotation is paramount, and the posterolateral approach often allows for simultaneous fixation of fibular fractures, further simplifying the procedure for combined injuries.
-
Outcomes and Complications:
- Modern literature supports good to excellent functional outcomes when anatomical reduction and stable fixation are achieved via the posterolateral approach. However, the complexity of pilon fractures still carries a higher risk of post-traumatic arthritis.
- Complication rates, particularly sural nerve injury and wound complications, are well-documented and require careful surgical technique and patient selection to mitigate.
- Despite these risks, the benefits of anatomical reduction and stable fixation, leading to better long-term functional results and lower rates of post-traumatic arthritis, generally outweigh the risks of the approach when appropriately indicated.
In conclusion, the posterolateral approach has cemented its position as a preferred technique for specific, challenging ankle fracture patterns. Its efficacy is rooted in the principles of direct visualization, anatomical reduction, and stable internal fixation, all of which are strongly supported by current orthopedic literature and best practice guidelines. Continued refinement of surgical techniques, implant design, and post-operative rehabilitation protocols will further optimize patient outcomes.
You Might Also Like