Medial Hip Approach & Obturator Division: Anatomy, Indications, and Surgical Technique
Key Takeaway
The medial hip (Ludloff) approach is used for specific indications like congenital dislocation of the hip (CDH), tumor excision, and managing adductor spasticity via obturator nerve division. It provides direct access to inferomedial capsule and adductors, requiring precise knowledge of neurovascular anatomy, including obturator nerve branches, for safe execution.
Mastering Obturator Division in the Medial Hip Approach
Introduction & Epidemiology
The medial approach to the hip, originally described by Ludloff in the early 20th century, represents a foundational technique in orthopedic surgery for specific indications where direct access to the inferomedial capsule and adductor compartment is paramount. Historically, its primary utility was in the open reduction of congenital dislocation of the hip (CDH), particularly in infants and young children presenting with flexed, abducted, and externally rotated deformities. The approach provides an unparalleled direct view of critical soft tissue impediments to reduction, such as the psoas tendon and hypertrophied adductor musculature.
Beyond pediatric hip pathology, the versatility of the medial approach has expanded to address a range of conditions. It offers a direct route for biopsy and excision of tumors originating from the inferior aspect of the femoral neck or medial proximal femoral shaft, locations often challenging to access via conventional anterior or posterior approaches. Furthermore, it is the preferred approach for targeted adductor releases and obturator neurectomy, procedures critical for managing severe adductor spasticity seen in conditions such as cerebral palsy, stroke, or spinal cord injury. This focused neurotomy or tenotomy aims to alleviate disabling scissoring gait, improve hygiene, and reduce pain.
While less frequently employed than global approaches to the hip, mastering the medial approach, and specifically the division of the obturator nerve, is essential for orthopedic surgeons managing a diverse patient population, particularly those with complex pediatric hip deformities and adult spasticity. Its precise anatomical exposure minimizes collateral damage, making it an indispensable tool in the experienced surgeon's armamentarium.
Surgical Anatomy & Biomechanics
A thorough understanding of the intricate neurovascular and muscular anatomy of the medial thigh is critical for safe and effective execution of the Ludloff approach, particularly when performing obturator division.
Bony Landmarks
The primary bony landmarks are the pubic tubercle and the pubic ramus, which serve as the origin points for the adductor musculature. The ischial tuberosity lies more posteriorly and inferiorly, providing origin for the hamstring and adductor magnus.
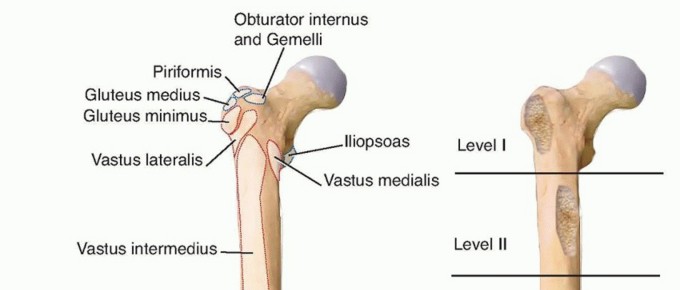
Musculature
The adductor compartment of the thigh comprises several muscles, arranged in layers, all contributing to hip adduction, flexion, and medial rotation:
*
Superficial Layer
:
*
Adductor Longus
: Originates from the pubic body just inferior to the pubic crest, inserting into the linea aspera of the femur. It is the most anterior and easily palpable adductor.
*
Gracilis
: The most medial muscle, originating from the inferior pubic ramus and inserting into the anteromedial aspect of the tibia (pes anserinus).
*
Middle Layer
:
*
Pectineus
: Originates from the pectineal line of the pubis, inserting onto the pectineal line of the femur. It is positioned lateral to the adductor longus.
*
Adductor Brevis
: Deep to the pectineus and adductor longus, originating from the inferior pubic ramus and inserting into the linea aspera.
*
Deep Layer
:
*
Adductor Magnus
: The largest adductor, with a broad origin from the inferior pubic ramus and ischial tuberosity, and an extensive insertion along the linea aspera and adductor tubercle. It has both adductor and hamstring portions.
*
Obturator Externus
: This deep external rotator originates from the external surface of the obturator membrane and surrounding bone, inserting into the trochanteric fossa of the femur. It is a key landmark in deep dissection during hip reduction.
*
Iliopsoas
: While primarily a hip flexor, the psoas tendon runs anterior to the hip joint capsule and can become a significant impediment to reduction in DDH, requiring release.
Neurovascular Structures
The medial approach necessitates careful identification and protection of vital neurovascular structures:
*
Femoral Neurovascular Bundle
: Located laterally to the operative field, within the femoral triangle. This bundle contains the femoral nerve, artery, and vein. Retraction laterally is crucial.
*
Obturator Nerve
: This nerve originates from the lumbar plexus (L2-L4) and typically enters the thigh via the obturator foramen. It divides into an anterior and a posterior branch:
*
Anterior Division
: Runs between the adductor longus and adductor brevis. It innervates the adductor longus, gracilis, and adductor brevis (partially), and provides a cutaneous branch to the medial thigh.
*
Posterior Division
: Pierces the obturator externus and runs between the adductor brevis and adductor magnus. It innervates the adductor magnus and adductor brevis (partially), and the obturator externus. It also supplies the hip joint capsule.
*
Accessory Obturator Nerve
: Present in a variable percentage of individuals (up to 30%), originating from L3-L4. It runs over the superior pubic ramus, deep to the pectineus, and provides branches to the pectineus and hip joint. If present, it often lies lateral to the main obturator nerve and should be considered during extensive adductor releases.
*
Obturator Artery and Vein
: These vessels accompany the obturator nerve through the obturator foramen and should be identified and protected, or ligated if necessary for exposure.
Biomechanics
Adductor muscle function is critical for hip stability, gait, and control of abduction/adduction. In conditions like cerebral palsy or stroke, spasticity of the adductors can lead to:
*
Scissoring Gait
: Bilateral adduction and internal rotation that interferes with ambulation.
*
Difficulty with Hygiene
: Inability to adequately abduct the hips for perineal care.
*
Pain
: Due to muscle spasm or secondary hip subluxation/dislocation.
*
Progressive Hip Deformity
: Persistent adduction forces can lead to femoral head migration, acetabular dysplasia, and eventual hip dislocation, particularly in the growing child with neuromuscular imbalance.
Obturator neurectomy and adductor tenotomy aim to disrupt the pathological adduction forces. By selectively weakening or denervating the adductors, the biomechanical balance around the hip can be restored, facilitating abduction, improving gait, and preventing or managing hip dislocation. The choice between anterior, posterior, or complete obturator nerve division depends on the specific muscles requiring denervation and the degree of spasticity.
Indications & Contraindications
The medial approach to the hip is a targeted intervention with specific indications, primarily related to addressing soft tissue contractures, providing access to medial bony structures, or managing spasticity.
Indications
-
Open Reduction of Congenital Dislocation of the Hip (CDH) / Developmental Dysplasia of the Hip (DDH)
:
- Especially in children up to approximately 18-24 months of age, or in cases where closed reduction has failed due to specific soft tissue impediments.
- Provides excellent exposure for release of the psoas tendon, which commonly blocks reduction by encircling the femoral neck.
- Facilitates release of taut adductor muscles, allowing for safer reduction and stable positioning.
- Allows direct visualization and removal of other intracapsular impediments like the pulvinar, ligamentum teres, or an inverted labrum.
- Psoas Release : For contractures contributing to hip flexion deformity, particularly in DDH or certain neuromuscular conditions.
- Adductor Tenotomy/Release : For severe adductor contracture or spasticity leading to scissoring gait, pain, or difficulties with hygiene. Often combined with obturator neurectomy.
-
Obturator Neurectomy
:
- Selective or complete division of the obturator nerve (anterior and/or posterior divisions) to reduce adductor spasticity in patients with cerebral palsy, stroke, traumatic brain injury, or spinal cord injury.
- Aims to improve gait, facilitate transfers, aid in perineal hygiene, and alleviate pain from muscle spasm.
- The upper part of the approach allows for identification and division of the obturator nerve.
-
Biopsy and Treatment of Tumors
:
- Access to the inferior portion of the femoral neck and medial aspect of the proximal femoral shaft for biopsy or resection of benign or malignant lesions that are difficult to reach via other approaches.
- Can also be utilized for certain osteotomies in the proximal medial femur.
Contraindications
- Active Infection : Local or systemic infection poses a significant risk of surgical site infection.
- Severe Scarring/Previous Surgery : Extensive scarring from prior operations in the groin region can obliterate anatomical planes, making dissection hazardous and increasing the risk of neurovascular injury.
- Unsuitable Patient Positioning : Inability to achieve the necessary flexed, abducted, and externally rotated position due to severe fixed deformities or patient intolerance.
- Pathology Best Addressed by Other Approaches : For example, primary acetabular pathologies, posterior femoral neck fractures, or large posterior tumors are better accessed via other surgical windows.
- Lack of Clear Indication for Adductor Release or Obturator Neurectomy : For spasticity, non-operative management (e.g., botulinum toxin injections, physical therapy) should be exhausted or deemed ineffective before surgical intervention.
Operative vs. Non-Operative Indications
| Indication Category | Operative Approach (Medial Hip) | Non-Operative Management |
|---|---|---|
| Developmental Dysplasia of the Hip (DDH) | Failed closed reduction, irreducible dislocation, persistent instability after non-operative attempts, presence of identified soft tissue blocks (psoas, adductors, capsule). | Pavlik harness, abduction bracing, close observation for mild dysplasia. |
| Adductor Spasticity / Contracture | Severe, intractable spasticity leading to functional impairment (scissoring gait), pain, hygiene issues, progressive hip subluxation/dislocation, failure of conservative measures. | Physical therapy, stretching, bracing, oral antispasmodics, botulinum toxin injections, intrathecal baclofen pump. |
| Hip Tumors | Suspicion of malignancy requiring biopsy, symptomatic benign tumors, tumors located on the inferior femoral neck or medial proximal shaft requiring resection. | Observation for asymptomatic benign lesions, systemic chemotherapy/radiation for certain malignancies where surgery is not primary. |
| Persistent Psoas Contracture | Contracture significantly impeding hip flexion/extension, contributing to dislocation or pain, failure of conservative measures. | Physical therapy, stretching, botulinum toxin injections. |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning and precise patient positioning are crucial for maximizing exposure, minimizing complications, and ensuring optimal outcomes with the medial approach.
Pre-Operative Planning
-
Clinical Assessment
:
- Thorough history and physical examination, focusing on hip range of motion, stability, and neurological status (for spasticity cases, assess adductor tone and function).
- For DDH, evaluate reducibility, abduction deficits, and limb length discrepancy.
- For tumors, assess mass characteristics, pain, and neurological compromise.
-
Imaging Review
:
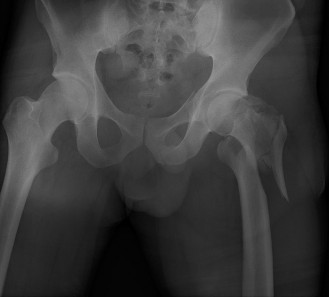
- Radiographs : Anteroposterior pelvis and frog-leg lateral views are standard for DDH, assessing femoral head coverage, acetabular index, and Shenton's line. For tumors, plain films can reveal bony involvement.
- Ultrasound : Essential for DDH diagnosis and monitoring in infants, providing dynamic assessment of hip stability.
- MRI : Highly valuable for visualizing soft tissue impediments (psoas, labrum, pulvinar) in DDH, defining tumor extent, and assessing neurovascular structures.
- CT Scan : Useful for detailed bony anatomy, especially for complex DDH or tumor involving the femoral neck/pelvis.
-
Neurophysiological Assessment (for Spasticity)
:
- EMG studies can confirm adductor hyperactivity.
- Diagnostic nerve blocks (e.g., lidocaine into the obturator nerve) can predict functional improvement post-neurectomy and confirm the nerve's contribution to spasticity.
- Anesthetic Consultation : Discuss potential blood loss (especially in tumor cases), pain management, and specific requirements for patient positioning.
- Equipment Check : Ensure availability of appropriate retractors (e.g., small Hohmanns, army-navy), cautery, nerve stimulator (if desired for obturator identification), and orthopedic instrumentation.
Patient Positioning
The patient is placed
supine
on the operating table. The affected hip is then positioned in
flexion, abduction, and external rotation
.
*
Maintaining Position
:
* A sandbag or bolster is typically placed under the ipsilateral buttock to internally rotate the pelvis and present the adductor region.
* The affected leg is draped free. The foot of the affected side should lie along the medial side of the contralateral knee or distal thigh.
* The knee is flexed, and the hip is abducted maximally to stretch the adductor muscles, making them prominent and facilitating identification.
* In cases of fixed deformity (e.g., severe adduction contracture), achieving this ideal position may not be entirely possible. The position is then determined by the maximal comfortable and safe range of motion achievable.
* Ensure proper padding of all pressure points, especially the contralateral leg and foot.
*
C-arm Access
: Verify that fluoroscopic imaging can be obtained intraoperatively without repositioning, particularly for DDH reduction or tumor localization.

Proper patient positioning for the medial approach to the hip, demonstrating hip flexion, abduction, and external rotation with the foot placed against the contralateral knee.
Detailed Surgical Approach / Technique
The medial approach (Ludloff) is executed with precision, focusing on identifying the internervous planes and critical neurovascular structures to achieve the surgical objective.
1. Incision
The incision choice depends on the specific pathology and surgeon preference:
*
Longitudinal Incision
: Often preferred for extensive exposure, particularly for CDH reduction or large tumors. It typically extends from the pubic tubercle inferiorly along the medial aspect of the thigh for approximately 4-8 cm, following the course of the adductor longus.
*
Transverse Incision
: A shorter transverse incision in the groin crease is sometimes used for isolated adductor release and obturator neurectomy, particularly when combined with other procedures like a proximal femoral osteotomy. This offers better cosmetic results but limited deeper exposure.
* For obturator neurectomy combined with adductor release, the original description notes a short transverse or longitudinal incision in the groin that permits division of the adductors close to their pelvic origin, an area often with less bleeding.
2. Superficial Dissection
- The incision is carried through the skin and subcutaneous tissue.
- Careful hemostasis is maintained. Superficial veins, if encountered, are coagulated or ligated.
- The fascia of the adductor compartment is incised.
- The long and prominent tendon of the adductor longus is identified. It typically runs obliquely from the pubis distally. The gracilis muscle is found medial to the adductor longus.

Initial dissection demonstrating the identification of the adductor longus and gracilis muscles. The internervous plane for deeper access is typically found between the adductor longus and pectineus or adductor brevis.
3. Internervous Plane and Deep Dissection
The key to this approach lies in identifying the internervous plane.
*
Ludloff's original description
: The internervous plane lies between the adductor longus and the pectineus laterally. The adductor longus is retracted medially, and the pectineus is retracted laterally.
*
Alternative Plane
: Some surgeons prefer the plane between the adductor longus (retracted medially) and the adductor brevis (retracted laterally). This plane allows direct access to the anterior division of the obturator nerve and deeper structures.
* Once the desired plane is established, a blunt dissection is performed, meticulously separating the muscle bellies.
4. Adductor Release (if indicated)
- If adductor contracture is present, the adductor longus, gracilis, and adductor brevis can be released.
- This is typically performed by tenotomy close to their pubic origins. A subperiosteal release from the pubic bone provides a complete release.
- Care must be taken to avoid injury to the pubic periosteum, as this can lead to heterotopic ossification.

Depicts the division of the adductor longus tendon near its origin from the pubic bone. This is a common first step in adductor release.
5. Identification and Division of the Obturator Nerve
This is a critical step, especially for managing spasticity.
* After retracting the adductor longus medially and the pectineus/adductor brevis laterally, the fascia overlying the obturator nerve is encountered.
* The
anterior division of the obturator nerve
is typically found running between the adductor longus and adductor brevis. It is often accompanied by an artery and vein.
* The
posterior division
lies deeper, often piercing or running behind the obturator externus muscle, and is typically found between the adductor brevis and adductor magnus.
* A nerve stimulator can be invaluable to confirm the identity of the nerve branches by eliciting adductor contraction.
*
Selective Neurectomy
:
* If only the adductor longus, gracilis, and pectineus are targeted, only the anterior division may be divided.
* For more profound spasticity or involvement of adductor brevis/magnus, both anterior and posterior divisions are typically divided.
* The divisions are carefully isolated, elevated, and divided, often with a segment excised to prevent re-innervation.
* The accompanying obturator vessels should be identified and carefully ligated or coagulated if they need to be divided for exposure, though often they can be preserved.
* Attention must be paid to the potential presence of an
accessory obturator nerve
, which lies more laterally and may need to be addressed if identified and contributing to spasticity.

Illustrates deeper dissection, exposing the neurovascular structures. The obturator nerve and its branches are carefully identified within the adductor compartment.

Close-up view of the obturator nerve, showing its anterior and posterior divisions. This detail is crucial for precise division during neurectomy.
6. Psoas Release (for DDH)
- The psoas tendon lies deep and lateral to the adductor origins, running over the anterior capsule of the hip joint.
- It is identified as a taut band passing over the inferior femoral neck/capsule.
- The tendon can be released either intra-articularly (from its insertion on the lesser trochanter) or extra-articularly (elongation or tenotomy near the femoral head). The extra-articular release is often preferred to preserve hip flexor strength.
- Care is taken to protect the femoral neurovascular bundle, which lies lateral to the psoas.
7. Capsulotomy and Hip Reduction (for DDH)
- After adductor and psoas release, the anterior and inferior hip capsule is exposed.
- A T-shaped or inverted T-shaped capsulotomy is performed to fully expose the femoral head and acetabulum.
- Intra-articular impediments such as the pulvinar (hypertrophied fat pad), ligamentum teres, or an inverted labrum are identified and excised or reduced.
- With the hip maximally flexed, abducted, and externally rotated, reduction is attempted by gently applying traction and internal rotation. The femoral head should seat concentrically into the acetabulum.
- Stability of reduction is assessed by bringing the hip through a gentle range of motion. The hip should remain reduced in approximately 90 degrees of flexion, 45 degrees of abduction, and neutral rotation.

Illustrates the hip joint after soft tissue release and capsulotomy, demonstrating the reduction of the femoral head into the acetabulum. Note the direct visualization of the hip joint components.
8. Closure
- The hip joint capsule (if opened) is typically repaired, leaving a portion of the inferior capsule open to prevent impingement in abduction, particularly for DDH.
- Meticulous hemostasis is ensured.
- The layers are closed with absorbable sutures: fascia, subcutaneous tissue, and skin.
- A drain is rarely necessary.
- For DDH, the hip is immobilized in a spica cast in the position of stability (typically 90 degrees flexion, 45 degrees abduction, mild internal rotation).
Complications & Management
While the medial hip approach is effective for its indications, surgeons must be aware of potential complications and have strategies for their management.
Common Complications and Management Strategies
| Complication | Incidence | Etiology | Salvage/Management Strategy |
|---|---|---|---|
| Hemorrhage | Low-Moderate | Injury to femoral or obturator vessels, muscle bleeding. | Meticulous hemostasis throughout dissection. Pre-operative planning for potential vascular anomalies. Direct pressure, ligation of identified bleeders. In severe cases, vascular surgery consultation. |
| Nerve Injury (Obturator) | Low (transient > permanent) | Direct laceration, stretch, thermal injury during neurectomy or retraction. | Prevention : Careful anatomical dissection, use of nerve stimulator, blunt dissection. Management : For transient neuropraxia, observation and supportive care. For complete transection, primary repair may be considered if identified immediately, but often functional deficits are managed with rehabilitation or further selective neurectomy (if incomplete initially). |
| Nerve Injury (Femoral/Saphenous) | Very Low | Lateral retraction injury, thermal injury. | Prevention : Meticulous lateral retraction, clear identification of femoral neurovascular bundle. Management : Observation, physiotherapy for motor deficits. For sensory deficits (saphenous), symptomatic management. |
| Incomplete Soft Tissue Release | Moderate | Inadequate division of adductors, psoas, or capsular structures (DDH). | Prevention : Intraoperative assessment of hip reduction/abduction after release. Management : For DDH, often requires repeat open reduction. For spasticity, recurrence of contracture may necessitate revision tenotomy, further obturator neurectomy (if initial was partial), or alternative treatments (e.g., botulinum toxin, intrathecal baclofen). |
| Recurrent Adductor Spasticity/Contracture | Low-Moderate | Incomplete neurectomy, nerve regeneration, development of compensatory spasticity in other muscles. | Prevention : Complete division of both anterior and posterior obturator nerve branches, excising a segment. Consider accessory obturator nerve. Management : Physiotherapy, serial casting, botulinum toxin injections. For persistent severe recurrence, revision neurectomy or tenotomy, or alternative spasticity management (e.g., intrathecal baclofen, dorsal rhizotomy). |
| Avascular Necrosis (AVN) of Femoral Head (DDH) | Low-Moderate | Aggressive positioning (excessive abduction), damage to medial circumflex femoral artery during reduction/capsulotomy. | Prevention : Gentle reduction, avoidance of extreme abduction post-reduction (avoiding the "frog-leg" cast), careful capsular repair, preservation of retinacular vessels. Management : Non-weight-bearing, observation for revascularization. Progressive collapse may require osteotomy (e.g., varus derotational) or, in severe cases, hip arthroplasty later in life. |
| Redislocation/Subluxation (DDH) | Low | Inadequate reduction, insufficient soft tissue release, improper cast application, unstable hip. | Prevention : Confirm concentric reduction and stability intraoperatively, proper cast application in a stable position. Management : Prompt recognition via imaging. Requires cast change, repeat closed reduction, or revision open reduction. |
| Wound Complications | Low | Hematoma, infection, dehiscence. | Prevention : Meticulous hemostasis, aseptic technique, layered closure. Management : Hematoma evacuation, antibiotics for infection (with debridement if needed), wound care, secondary closure. |
| Heterotopic Ossification | Low | Excessive periosteal stripping during adductor release. | Prevention : Limited periosteal stripping, gentle handling of soft tissues. Management : Prophylaxis with NSAIDs (e.g., indomethacin) or radiation in high-risk patients. For symptomatic ossification, surgical excision after maturation, combined with prophylaxis. |
| Gait Disturbance | Low-Moderate | Overcorrection of adduction leading to excessive abduction, unmasking of other gait issues. | Prevention : Judicious assessment of the degree of adductor spasticity and planning for selective neurectomy. Management : Intensive gait training, physiotherapy, use of assistive devices. Addressing other underlying neuromuscular imbalances. |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation following a medial hip approach is tailored to the specific indication and extent of the surgical intervention. The primary goals are to protect the repair/reduction, prevent recurrence of deformity, restore range of motion, and optimize functional outcomes.
For Developmental Dysplasia of the Hip (DDH)
-
Immobilization Phase (0-6 weeks)
:
- Spica Cast : The hip is typically immobilized in a custom-molded spica cast in a stable position (e.g., 90 degrees flexion, 45 degrees abduction, neutral-to-mild internal rotation).
- Cast Care : Parents/caregivers are educated on cast care, hygiene, skin checks, and signs of complications (e.g., neurovascular compromise, infection).
- Activity : Non-weight-bearing on the affected side. Age-appropriate activity is encouraged within the confines of the cast.
- Monitoring : Regular clinical and radiographic follow-up to confirm cast integrity and hip reduction.
-
Early Mobilization Phase (6-12 weeks, post-cast removal)
:
- Radiographic Assessment : Confirm stable reduction before initiating mobilization.
- Gentle Range of Motion (ROM) : Begin passive and active-assisted ROM exercises within pain-free limits. Focus on restoring flexion and carefully increasing abduction. Avoid aggressive stretching or forced movements.
- Weight-Bearing : Gradual progression to partial weight-bearing with assistive devices (walker, crutches) as tolerated, once radiographic stability is confirmed.
- Strengthening : Initiate isometric exercises for hip flexors, extensors, and abductors.
- Physical Therapy : Formal physical therapy sessions several times a week to guide ROM, strengthening, and gait training.
-
Advanced Rehabilitation Phase (12 weeks onwards)
:
- Progressive Strengthening : Advance to dynamic strengthening exercises for all hip muscle groups, emphasizing hip abductor and extensor strength.
- Gait Training : Progress to full weight-bearing, normalize gait pattern, and discontinue assistive devices as appropriate.
- Balance and Proprioception : Incorporate exercises to improve balance and coordination.
- Return to Activity : Gradual return to age-appropriate activities and sports, avoiding high-impact activities for several months.
- Long-term Follow-up : Continued monitoring for potential complications like AVN or redislocation, often extending into skeletal maturity.
For Adductor Release and Obturator Neurectomy (for Spasticity)
-
Immediate Post-Operative (Day 0-3)
:
- Pain Management : Aggressive pain control to facilitate early mobilization.
- Positioning : Maintain the hip in a moderately abducted position using pillows or an abduction brace to stretch the released adductors and prevent immediate re-contracture.
- Wound Care : Standard wound care protocols.
-
Early Mobilization Phase (Day 3 - 6 weeks)
:
- Continuous Passive Motion (CPM) : If tolerated and available, CPM may be used to gently maintain hip ROM.
- Passive and Active-Assisted ROM : Begin gentle passive stretching and active-assisted ROM exercises for hip abduction and extension, several times daily. Avoid forceful, ballistic stretching.
- Weight-Bearing : Early weight-bearing and ambulation with appropriate assistive devices (walker, crutches) are encouraged to restore functional movement patterns.
- Strengthening : Initiate strengthening of hip abductors and extensors to counteract the previous adductor dominance and improve hip stability.
- Functional Training : Physical therapy focuses on improving gait, transfers, and activities of daily living. Address any pre-existing compensatory patterns.
-
Intermediate Phase (6 weeks - 3 months)
:
- Progressive Stretching : Continue and progress static and dynamic stretching exercises, focusing on maintaining the gains in abduction.
- Advanced Strengthening : Progress to more challenging resistance exercises, core strengthening, and balance activities.
- Gait Re-education : Intensive gait analysis and training to refine walking patterns, reduce scissoring, and improve efficiency.
- Splinting/Bracing : Consider night-time abduction bracing or serial casting if there is a risk of recurrence of contracture.
-
Long-Term Management (3 months onwards)
:
- Home Exercise Program : Transition to an independent home exercise program to maintain ROM and strength.
- Monitoring for Recurrence : Regular follow-up to assess for recurrence of spasticity or contracture, which may require further intervention (e.g., botulinum toxin injections, repeat surgery).
- Multidisciplinary Approach : Continue collaboration with neurologists, physiatrists, and occupational therapists to manage overall spasticity and optimize long-term function.
Summary of Key Literature / Guidelines
The medial approach to the hip, while less common for primary hip arthroplasty, holds a critical and well-established role in specific areas of orthopedic surgery, particularly in pediatric hip reconstruction and spasticity management.
1. Developmental Dysplasia of the Hip (DDH):
*
Ludloff's Legacy (1908)
: The medial approach was initially popularized by Ludloff for open reduction of CDH, emphasizing the direct visualization of soft tissue impediments. Early series demonstrated good reduction rates with meticulous technique.
*
Contemporary Pediatric Orthopedics
: Modern guidelines from organizations like the Pediatric Orthopaedic Society of North America (POSNA) acknowledge the medial approach as a viable option for open reduction of DDH, particularly in infants and toddlers (generally <18-24 months) where soft tissue interposition is a primary block to reduction.
* Literature consistently reports high success rates for reduction (often >90%) and stable fixation.
* However, concerns regarding
avascular necrosis (AVN) of the femoral head
remain a significant consideration. Studies have reported variable rates of AVN (ranging from 0% to over 30%), influenced by factors such as patient age, severity of dislocation, surgical technique, and post-operative immobilization protocol. Gentle handling of tissues, meticulous capsular repair (avoiding excessive tension), and careful post-operative positioning are critical to minimizing AVN risk.
* Compared to the anterior (Smith-Petersen) or anterolateral approaches, the medial approach offers superior access to the inferior capsule, psoas tendon, and adductors, often leading to a more complete soft tissue release.
*
Long-Term Outcomes
: Long-term studies indicate that satisfactory hip function and radiographic outcomes are achievable, though a proportion of patients may still require further intervention (e.g., osteotomy, hip arthroplasty) later in life due to residual dysplasia or premature degenerative changes.
2. Obturator Neurectomy and Adductor Release for Spasticity:
*
Historical Context
: Adductor tenotomy and obturator neurectomy have been performed since the mid-20th century to manage severe adductor spasticity.
*
Effectiveness
: Current literature supports the efficacy of obturator neurectomy (often combined with adductor tenotomy) in improving hip abduction, facilitating hygiene, alleviating pain, and improving gait mechanics in patients with cerebral palsy, stroke, and spinal cord injury.
* Studies demonstrate significant improvements in functional scores (e.g., Gross Motor Function Measure in CP) and reduced caregiver burden.
*
Selective Neurectomy
: The ability to selectively denervate specific adductor muscles by dividing only the anterior or posterior divisions of the obturator nerve (or both) allows for tailored interventions based on individual patient assessment and spasticity patterns.
*
Recurrence
: Recurrence of spasticity or contracture can occur due to nerve regeneration or compensatory muscle activity. Reported recurrence rates vary but highlight the importance of thorough initial neurectomy (e.g., excising a nerve segment) and a robust post-operative rehabilitation program.
*
Role in Multidisciplinary Care
: Obturator neurectomy is often part of a broader spasticity management strategy, which may include oral medications, botulinum toxin injections, intrathecal baclofen, and intensive physical therapy. The decision for surgical intervention is typically made by a multidisciplinary team.
*
Complications
: While generally safe, potential complications include incomplete denervation, hemorrhage, and, rarely, injury to the femoral nerve or artery. The risk of motor weakness in other hip muscles is minimal if precise selective neurectomy is performed.
3. Tumor Access:
* While less extensively studied in large series, the medial approach offers a direct and often less morbid route for biopsy and resection of tumors localized to the inferior femoral neck and medial proximal femur. Its utility is in avoiding more extensive muscle detachment or neurovascular manipulation required by other approaches for these specific locations.
In conclusion, the medial hip approach, particularly when focused on obturator division, remains a valuable surgical technique. Its successful application relies on a profound understanding of surgical anatomy, meticulous technique, and a patient-centered approach to rehabilitation. Continuous evaluation of outcomes and adherence to evidence-based practices are essential for optimizing patient care.
Clinical & Radiographic Imaging
You Might Also Like