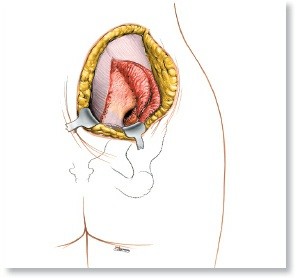
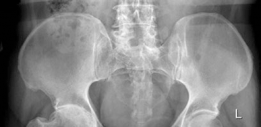
Chronic Ankle Arthritis: A Detailed Clinical Case Study & Diagnostic Approach
Key Takeaway
Severe chronic ankle arthritis diagnosis involves patient history noting chronic pain and painful plantarflexion. Clinical exam reveals restricted range of motion. Weight-bearing radiographs confirm significant tibiotalar joint space narrowing, subchondral sclerosis, and prominent osteophytes, particularly posterior, which correlate with symptoms and guide treatment.
Patient Presentation & History
A 62-year-old male presented with a chief complaint of chronic, progressive left ankle pain spanning approximately eight years. The patient described the pain as deep-seated, aching, and significantly exacerbated by weight-bearing activities, prolonged standing, and notably, by forceful plantarflexion of the ankle. He reported a particular functional limitation in negotiating stairs, pushing off during ambulation, and participating in recreational walking, activities that consistently provoked his symptoms. The pain was often rated 7/10 on a visual analogue scale (VAS) during exacerbations, improving to 4/10 with rest. Nocturnal pain was also a significant complaint, disrupting sleep.
His medical history is significant for a remote (approximately 15 years prior) severe left ankle sprain, which was initially managed non-operatively. There was no documented ankle fracture at that time. He is otherwise healthy, with well-controlled hypertension and no history of inflammatory arthropathy, diabetes, or other systemic conditions that might predispose to widespread arthropathy. He is a non-smoker and consumes alcohol socially. He works in a supervisory role that requires moderate ambulation and standing.
Conservative management over the preceding five years included:
* Serial non-steroidal anti-inflammatory drugs (NSAIDs).
* Activity modification.
* Custom orthotics and ankle bracing.
* Multiple courses of physical therapy, focusing on strengthening, proprioception, and range of motion, which provided only transient, minimal relief.
* Two intra-articular corticosteroid injections, providing symptomatic relief for approximately 3-4 weeks each, with diminishing returns.
The patient’s primary goal was to regain the ability to walk for extended periods without debilitating pain and to return to his recreational activities. The specific emphasis on "painful plantar flexion hindfoot" in his presentation suggested a significant degenerative process within the tibiotalar articulation, potentially with concomitant posterior impingement or secondary subtalar involvement.
Clinical Examination
Inspection
On inspection, the left ankle presented with mild effacement of the anterior gutters, indicative of a subtle effusion. There was no obvious erythema, warmth, or gross deformity such in varus or valgus alignment when standing. Mild swelling was noted diffusely around the joint. The skin integrity was intact, with no signs of trophic changes or prior surgical scars. Muscle atrophy of the calf was not pronounced, though subtle disuse atrophy could be appreciated compared to the contralateral limb. Gait analysis revealed an antalgic gait pattern, with a shortened stance phase on the left, and a noticeable avoidance of push-off.
Palpation
Palpation elicited tenderness primarily along the anterior tibiotalar joint line, as well as diffuse tenderness over the anterior aspect of the ankle. Posterior palpation, especially when the ankle was forcefully plantarflexed, reproduced the patient's characteristic pain, suggesting posterior impingement or osteophyte formation. There was no significant tenderness along the medial or lateral collateral ligaments, suggesting primary ligamentous stability. The subtalar joint was also assessed for tenderness, and moderate discomfort was noted with palpation directly over the sinus tarsi and posteromedial to the talus, indicating possible secondary involvement.
Range of Motion (ROM)
Active and passive range of motion of the left ankle was significantly restricted and painful.
*
Dorsiflexion:
Limited to 0 degrees (neutral position being 0), with a firm endpoint and elicitation of significant pain at the end range. Compared to the contralateral limb's 15-20 degrees.
*
Plantarflexion:
Limited to 20 degrees (compared to 45-50 degrees contralaterally), again with a painful, firm endpoint. The patient specifically reported increased pain in the posterior hindfoot with attempts at full plantarflexion.
*
Subtalar Inversion/Eversion:
Active and passive subtalar motion was also restricted and painful, particularly inversion, limited to approximately 5 degrees (normal 20-30 degrees) and eversion to 5 degrees (normal 10-20 degrees). This suggested secondary involvement of the subtalar joint.
*
Midfoot/Forefoot:
Motion in the midfoot and forefoot was preserved, with no significant pain or restriction.
Neurological and Vascular Assessment
Neurological examination revealed intact sensation to light touch in all dermatomes of the foot (L4, L5, S1, S2). Motor strength was 5/5 for all major muscle groups (tibialis anterior, gastrocnemius-soleus complex, extensor hallucis longus, fibularis longus/brevis, tibialis posterior). Deep tendon reflexes (Achilles, patellar) were 2+ bilaterally and symmetrical.
Vascular assessment demonstrated palpable dorsalis pedis and posterior tibial pulses bilaterally, 2+ and symmetrical. Capillary refill was brisk (<2 seconds) in all digits. No signs of peripheral vascular disease were noted.
Imaging & Diagnostics
Radiographs
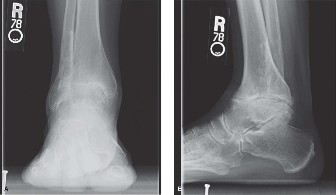
Weight-bearing radiographs (anteroposterior, lateral, and mortise views) of the left ankle were obtained.
*
Anteroposterior (AP) view:
Demonstrated significant narrowing of the tibiotalar joint space, particularly medially. There was diffuse subchondral sclerosis on both the distal tibia and talar dome. Mild varus alignment of the ankle joint was observed.
*
Lateral view:
Revealed severe loss of joint space, more pronounced anteriorly and posteriorly. Large anterior and posterior tibiotalar osteophytes were clearly visible. The posterior osteophyte was particularly prominent, consistent with the patient's complaints of painful plantarflexion and posterior impingement. There was also evidence of subchondral cyst formation within the talar body. The overall sagittal alignment showed a mild procurvatum of the distal tibia.
*
Mortise view:
Confirmed severe narrowing of the tibiotalar joint space, with loss of the normal mortise congruity. Medial clear space was reduced, and lateral clear space appeared relatively preserved, reiterating the mild varus deformity.
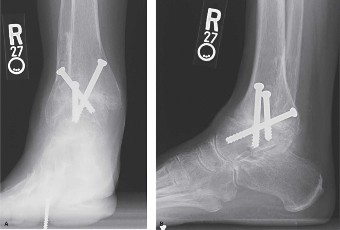
Figure 1: Pre-operative weight-bearing anteroposterior radiograph demonstrating severe tibiotalar joint space narrowing, subchondral sclerosis, and osteophyte formation, with a mild varus alignment.
Computed Tomography (CT)
A non-contrast CT scan of the left ankle was performed to further characterize the extent of the degenerative changes, assess bone stock, and aid in pre-operative planning, especially concerning osteophyte morphology and subchondral cyst size.
*
Findings:
Confirmed severe pan-tibiotalar arthritis with significant cartilage loss across the entire articular surface. The CT clearly delineated large anterior and posterior osteophytes, with the posterior osteophyte measuring approximately 1.5 cm in size, impinging into the posterior joint space during simulated plantarflexion. Extensive subchondral sclerosis and multiple subchondral cysts were evident in the distal tibia and talus, particularly a large cyst (1.2 cm) in the central talar dome. The overall alignment was consistent with mild varus. The subtalar joint showed moderate degenerative changes with mild joint space narrowing and subchondral sclerosis, suggesting secondary involvement or concomitant wear. The integrity of the distal tibiofibular syndesmosis appeared maintained.
Magnetic Resonance Imaging (MRI)
An MRI was not deemed strictly necessary given the clear radiographic and CT findings of advanced arthrosis. However, an MRI could be considered in cases of unclear etiology, suspicion of avascular necrosis (AVN) of the talus, occult osteochondral lesions not well visualized on CT, or significant soft tissue pathology, such as tendinopathy or occult stress fractures. In this patient, the clinical picture and CT findings were sufficient for surgical planning.
Templating
Pre-operative templating for Total Ankle Arthroplasty (TAA) was performed using the CT images. This involved selecting the appropriate implant size (tibial and talar components), determining the ideal resection levels for both the distal tibia and talus to restore mechanical axis alignment, and assessing the need for soft tissue balancing. The presence of significant posterior osteophytes and the patient's plantarflexion pain indicated a need for comprehensive debridement and restoration of joint mechanics.
Differential Diagnosis
The patient's presentation of chronic, progressive ankle pain exacerbated by weight-bearing and plantarflexion, along with the imaging findings, pointed strongly towards advanced tibiotalar arthritis. However, a comprehensive differential diagnosis includes other conditions that can cause similar symptoms, particularly those affecting the posterior hindfoot.
| Feature | Ankle Arthritis (Post-traumatic) | Posterior Ankle Impingement Syndrome (PAIS) | Subtalar Arthritis |
|---|---|---|---|
| Pathology | Degeneration of tibiotalar articular cartilage, subchondral bone changes. Typically post-traumatic. | Soft tissue (e.g., synovitis, scar tissue) or bony (e.g., os trigonum, posterior talar/tibial osteophytes) compression in posterior ankle. | Degeneration of subtalar joint articular cartilage and subchondral bone. Often secondary to ankle malalignment or prior trauma. |
| Mechanism | Prior fracture, severe sprain, chronic instability leading to altered biomechanics & cartilage breakdown. | Repetitive forced plantarflexion (e.g., ballet dancers, athletes) causing impingement. | Prior calcaneal or talar fracture, ankle malalignment, idiopathic. |
| Primary Symptom | Diffuse ankle pain, stiffness, swelling, crepitus. Worsens with activity. | Pain specifically with forced plantarflexion, often localized posteriorly. Clicking/catching sensation. | Pain in sinus tarsi, under lateral malleolus, or diffuse hindfoot. Worsens with uneven ground, walking. Restricted inversion/eversion. |
| Physical Exam Findings | Restricted, painful ROM (dorsiflexion & plantarflexion). Tenderness along joint lines. Deformity (varus/valgus) may be present. | Tenderness posteriorly, positive plantarflexion impingement test. Normal or near-normal dorsiflexion. | Restricted, painful subtalar inversion/eversion. Tenderness over sinus tarsi or posterior subtalar joint. |
| Radiographic Findings | Joint space narrowing, osteophytes, subchondral sclerosis/cysts. May show malalignment. | May show os trigonum, posterior talar osteophyte, posterior tibial osteophyte. Joint space often preserved. | Joint space narrowing of subtalar joint, sclerosis, osteophytes. May show talocalcaneal coalition. |
| CT Scan Utility | Definitive assessment of bone morphology, extent of cartilage loss, subchondral cysts, malalignment, and bone stock. | Clearly identifies bony impingers (os trigonum, osteophytes), but soft tissue impingement may be missed. | Detailed assessment of subtalar joint space, facets, and bone morphology. |
| MRI Scan Utility | Assess cartilage integrity (early arthritis), osteochondral defects, AVN of talus, soft tissue pathology (e.g., synovitis, tendinopathy). | Excellent for soft tissue impingement (synovitis, scar tissue) and bony lesions (marrow edema, stress fracture). | Assess cartilage, synovitis, and bone marrow edema in subtalar joint. |
| Treatment | Conservative (NSAIDs, orthotics, PT, injections). Operative (arthrodesis, total ankle arthroplasty, osteotomy). | Conservative (rest, NSAIDs, PT). Operative (arthroscopic or open debridement of impingers). | Conservative (NSAIDs, orthotics, PT, injections). Operative (subtalar fusion, subtalar arthrodesis, arthroscopy). |
In this patient, the combination of diffuse ankle pain, severe restriction in both dorsiflexion and plantarflexion, extensive radiographic changes of joint space narrowing, subchondral sclerosis, and prominent osteophytes across the tibiotalar joint clearly established post-traumatic ankle arthritis as the primary diagnosis. The additional finding of a large posterior osteophyte and pain with forced plantarflexion indicates a significant component of posterior ankle impingement syndrome as part of the overall arthritic pathology. The secondary subtalar changes also point to concomitant subtalar arthritis . Given the severity, all three aspects contributed to the patient’s debilitating symptoms, necessitating a comprehensive surgical approach.
Surgical Decision Making & Classification
The decision for operative intervention was based on several factors:
1.
Failure of exhaustive conservative management:
The patient had undergone a prolonged course of non-operative treatments with no sustained relief.
2.
Severity of pain and functional impairment:
Chronic pain rated 7/10 VAS and significant limitations in daily activities and recreational pursuits.
3.
Radiographic evidence of advanced arthrosis:
Kellgren-Lawrence grade IV equivalent tibiotalar arthritis with significant joint space narrowing, osteophytes, and subchondral changes.
4.
Patient's age and activity level:
A 62-year-old active non-smoker with reasonable bone quality, making him a suitable candidate for joint-preserving surgery if possible.
5.
Specific complaint of "painful plantar flexion hindfoot":
This indicated a need to address not only the overall arthritic process but also the specific posterior impingement component.
The primary surgical options for end-stage ankle arthritis include:
*
Ankle Arthrodesis (Fusion):
Gold standard for pain relief, but sacrifices motion. Indicated for severe deformity, poor bone stock, chronic infection, or failed total ankle arthroplasty.
*
Total Ankle Arthroplasty (TAA):
Aims to preserve motion while alleviating pain. Indicated for less severe deformity, adequate bone stock, and a desire to maintain mobility.
After detailed discussion with the patient regarding the pros and cons of both arthrodesis and TAA, including potential complications, rehabilitation, and long-term outcomes, the patient opted for Total Ankle Arthroplasty . The patient's desire to maintain ankle motion and his relatively active lifestyle, combined with favorable bone quality and alignment (mild varus correctable with TAA), made him an appropriate candidate for TAA. The presence of a significant posterior osteophyte and secondary subtalar arthritis required a nuanced approach, but a well-executed TAA, potentially with posterior debridement, could effectively address these issues while maintaining a functional range of motion.
Classification Systems:
While specific classification systems for ankle arthritis (like the Kellgren-Lawrence system for knee/hip arthritis) are not universally applied, the severity is often described by radiographic features. For surgical planning, the morphology of the ankle deformity is crucial:
*
Alignment:
Varus, valgus, or neutral. This patient presented with a mild varus alignment (approximately 5-7 degrees on weight-bearing radiographs).
*
Bone Stock:
Assessed via CT for quality and quantity, especially important for implant seating.
*
Osteophyte Burden:
Crucial for planning debridement and ensuring adequate exposure.
For TAA, the
Hintermann Classification
for TAA indications is often considered, although it's more of a surgical philosophy than a strict classification:
* Type 1: Concentric arthritis with minor deformity, good bone stock.
* Type 2: Varus or valgus deformity with moderate bone loss.
* Type 3: Major deformity with significant bone loss or revision cases.
Our patient broadly fit into a Type 1-2 category, with a correctable varus deformity and adequate bone stock. The presence of significant posterior osteophytes required specific attention during the TAA procedure.
Surgical Technique / Intervention: Total Ankle Arthroplasty (TAA)
The procedure performed was a right Total Ankle Arthroplasty with concomitant posterior ankle arthroscopy for osteophyte debridement.
Patient Positioning and Preparation
The patient was positioned supine on the operating table. A pneumatic tourniquet was applied to the proximal thigh. All bony prominences were meticulously padded. A bump was placed under the ipsilateral hip to allow for neutral alignment of the lower extremity. Standard sterile preparation and draping were performed, ensuring adequate exposure for both anterior and posterior approaches if necessary. A prophylactic single dose of broad-spectrum intravenous antibiotic was administered pre-incision.
Anterior Approach for TAA
- Incision: A straight anterior longitudinal incision, approximately 12-14 cm in length, was made midway between the medial and lateral malleoli, centered over the tibiotalar joint. The incision extended from approximately 2 cm proximal to the joint line to just distal to the talonavicular joint.
- Dissection: The incision was carried down through the skin and subcutaneous tissue. The superficial peroneal nerve branches were identified and carefully protected and retracted, typically laterally. The deep fascia was incised. The interval between the tibialis anterior tendon medially and the extensor hallucis longus (EHL) tendon laterally was identified. The neurovascular bundle (deep peroneal nerve and dorsalis pedis artery) lies between the EHL and the extensor digitorum longus (EDL) tendons, and was carefully retracted laterally along with the EHL and EDL.
- Capsulotomy: A longitudinal capsulotomy was performed directly over the anterior aspect of the tibiotalar joint.
- Osteophyte Resection and Synovectomy: Significant anterior osteophytes from the distal tibia and talar neck were resected using osteotomes and rongeurs to improve exposure and facilitate instrumentation. A thorough synovectomy was performed to remove hypertrophic synovium and any loose bodies.
- Distal Tibial Resection: Specialized jigs and guides (using the STAR™ Ankle System, for example) were utilized. The appropriate distal tibial cut was determined to restore the mechanical axis, typically with 0-3 degrees of valgus and 0-5 degrees of posterior slope. Fluoroscopy or navigation was used to confirm accurate resection. The amount of bone removed was precisely controlled to match the implant design.
- Talar Resection: After temporary distraction of the joint, the talar cutting guide was inserted. The talar dome was resected to achieve appropriate alignment and rotation, ensuring the component was perpendicular to the mechanical axis of the tibia. Care was taken to avoid over-resection, particularly laterally, and to preserve bone stock. The central talar cyst identified on CT was debrided.
- Trial Reduction and Component Sizing: Trial tibial and talar components were inserted. The ankle was taken through a full range of motion to assess stability, impingement, and ligamentous balancing. Appropriate soft tissue releases (e.g., medial gutter release for varus deformity, lateral lengthening for valgus) were performed as needed to achieve neutral alignment and balanced tension. Dorsiflexion and plantarflexion were assessed, and the height of the polyethylene insert was selected. The goal was 0 degrees of dorsiflexion past neutral and approximately 20-25 degrees of plantarflexion.
- Definitive Component Implantation: The definitive tibial component (cementless, porous coated) was impacted onto the resected distal tibia. The talar component was similarly impacted onto the resected talus. A polyethylene insert of the chosen thickness was then placed between the metal components, ensuring secure locking mechanisms.
- Wound Closure: The wound was copiously irrigated. The capsule was closed loosely. The deep fascia was repaired. Subcutaneous tissues were approximated, and the skin was closed with appropriate sutures. A sterile dressing was applied.
Posterior Ankle Arthroscopy (for Posterior Impingement)
Given the patient's prominent posterior osteophyte and pain with plantarflexion, a posterior ankle arthroscopy was performed concurrently.
1.
Positioning:
The patient's position was adjusted to prone or lateral decubitus, or a specific setup for posterior arthroscopy in supine. In this case, supine with the heel off the table allowed for easier access post-TAA.
2.
Portals:
Standard posterolateral and posteromedial portals were established using an 8-gauge spinal needle for localization. The posterolateral portal was established first, approximately 1 cm lateral to the Achilles tendon and 1.5 cm superior to the calcaneal tuberosity. The posteromedial portal was then established, similarly medial to the Achilles. Care was taken to protect the sural nerve laterally and the posterior tibial neurovascular bundle medially.
3.
Debridement:
A 2.7 mm 30-degree arthroscope was inserted. Gross visualization confirmed the significant posterior talar osteophyte and a smaller posterior tibial osteophyte. Using a motorized shaver and a burr, these osteophytes were carefully resected. The os trigonum, if present and symptomatic, would also be resected at this stage. Any hypertrophic synovium or scar tissue in the posterior gutter was debrided.
4.
Assessment:
After debridement, the ankle was passively plantarflexed to confirm full clearance and absence of impingement. The increase in pain-free plantarflexion was immediately noticeable.
5.
Closure:
Portals were closed with single sutures, and sterile dressings applied.

Figure 2: Intra-operative view during Total Ankle Arthroplasty (example image showing bone cuts or implant in situ). Demonstrates the precision required for component placement after bone resection.
Post-Operative Protocol & Rehabilitation
Immediate Post-Operative (Day 0-14)
- Immobilization: A well-padded posterior splint or a removable CAM walker boot in a neutral position (0 degrees dorsiflexion/plantarflexion) was applied immediately post-operatively.
- Weight-Bearing: Non-weight-bearing (NWB) with crutches or a walker.
- Pain Management: Multimodal analgesia including NSAIDs, acetaminophen, and opioid analgesics as needed.
- Elevation: Strict elevation of the limb above the heart to reduce swelling.
- Cryotherapy: Continuous cold therapy device applied to the ankle.
- DVT Prophylaxis: Low molecular weight heparin (LMWH) for 2-4 weeks.
- Wound Care: Daily wound checks, dressing changes as per protocol. Staples/sutures removed at 14 days post-op.
Early Rehabilitation (Weeks 2-6)
- Weight-Bearing: Progression to partial weight-bearing (PWB) in the CAM walker boot. Initially 25% body weight, gradually increasing to 50-75% over weeks 4-6, as tolerated and based on radiographic healing.
-
Range of Motion (ROM):
- Initiate gentle active-assisted and passive ankle dorsiflexion/plantarflexion, inversion/eversion within a pain-free range, starting out of the boot.
- Focus on restoring plantigrade foot position and preventing equinus contracture.
- Subtalar mobility exercises to prevent stiffness.
- Strengthening: Gentle isometric exercises for ankle musculature (dorsiflexors, plantarflexors, invertors, evertors).
- Manual Therapy: Soft tissue mobilization to address swelling and scar tissue.
Intermediate Rehabilitation (Weeks 6-12)
- Weight-Bearing: Full weight-bearing (FWB) in the CAM walker boot or a supportive shoe. Transition out of the boot as pain allows and strength improves.
- ROM: Continue to work on restoring full pain-free ankle ROM. Focus on terminal dorsiflexion and plantarflexion.
- Strengthening: Progressive resisted exercises using resistance bands or light weights for all ankle and lower leg muscle groups. Proprioceptive exercises (e.g., wobble board, single leg balance).
- Gait Training: Focus on normal heel-to-toe gait pattern, with emphasis on push-off.
- Scar Management: Continued massage and desensitization.
Advanced Rehabilitation (Months 3-6)
- Functional Progression: Gradual return to activities of daily living and work.
- Strengthening: Advanced strengthening exercises including calf raises (bilateral then unilateral), plyometrics (low impact initially), and sport-specific drills if applicable.
- Proprioception: Advanced balance and agility drills.
- Impact Activities: Low-impact activities such as swimming, cycling, elliptical allowed. High-impact activities (running, jumping sports) are generally discouraged long-term after TAA to minimize implant wear and loosening.
- Patient Education: Emphasize joint protection strategies, footwear modifications, and avoidance of high-impact activities.
Long-Term Follow-up
Regular clinical and radiographic follow-up is essential to monitor implant integrity, alignment, and detect any signs of loosening, osteolysis, or progressive arthritis in adjacent joints.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls
- Patient Selection is Paramount for TAA: Not all ankle arthritis is suitable for arthroplasty. Ideal candidates are typically older, lower demand, with correctable deformity (<15-20 degrees varus/valgus), adequate bone stock, and no active infection or severe neuropathy. Younger, higher-demand patients, or those with significant malalignment, often do better with arthrodesis.
- Pre-operative Imaging is Critical: Weight-bearing radiographs for alignment, and a CT scan for bone morphology, osteophyte burden, and precise templating are indispensable. MRI is useful for soft tissue assessment, AVN, or occult OCLs.
- Achieve Plantigrade Foot: The primary goal of TAA is to establish a pain-free, stable, and plantigrade foot with restored alignment. This is more important than absolute range of motion.
- Soft Tissue Balancing: Crucial for implant longevity and preventing loosening. This involves careful release of contracted structures (e.g., deltoid ligament for varus, spring ligament for valgus) and ensuring balanced tension throughout the range of motion.
- Address Concomitant Pathology: As demonstrated in this case, a posterior osteophyte causing impingement, or secondary subtalar arthritis, must be addressed. This may involve arthroscopic or open debridement of impingers, or even concomitant subtalar fusion in select cases (though not for this case).
- Neurovascular Protection: Meticulous dissection and careful retraction of the superficial peroneal nerve, deep peroneal nerve, and dorsalis pedis artery are vital to prevent iatrogenic injury.
- Appropriate Resection and Alignment: Accurate bone cuts are fundamental. Over-resection can compromise bone stock, while under-resection or malalignment can lead to early implant failure. Utilize intraoperative fluoroscopy or navigation.
- Multimodal Pain Management: Essential for early mobilization and patient comfort.
- Graduated Rehabilitation: A structured and progressive rehabilitation protocol is crucial for achieving optimal functional outcomes and protecting the implant during the initial healing phases.
Pitfalls
- Improper Patient Selection: Performing TAA in patients with severe deformity, poor bone quality, or high activity levels can lead to early failure (loosening, subsidence).
- Malalignment: Inadequate correction of coronal or sagittal plane deformity is a leading cause of aseptic loosening and polyethylene wear. Varus malalignment places excessive stress on the medial aspect of the implant.
- Neurovascular Injury: Injury to the superficial or deep peroneal nerves can cause foot drop or chronic pain/dyskinesia. Dorsalis pedis artery injury can lead to compromise of foot perfusion.
- Infection: Despite prophylactic antibiotics, TAA, like any arthroplasty, carries a risk of deep infection, which is devastating and often necessitates implant removal and fusion.
- Aseptic Loosening/Osteolysis: Long-term complication due to stress shielding, micromotion, or particulate wear debris. Regular radiographic surveillance is critical.
- Subsidence: Especially with cementless implants, poor bone stock or aggressive weight-bearing can lead to implant subsidence.
- Tibiofibular Synostosis/Heterotopic Ossification: Can restrict motion and cause pain.
- Persistent Pain/Stiffness: Despite a technically perfect TAA, some patients may experience ongoing pain or stiffness, which can be multifactorial (e.g., undiagnosed adjacent joint pathology, tendinopathy, or residual impingement).
- Failure to Address Impingement: If posterior osteophytes or soft tissue impingement are not adequately addressed, painful plantarflexion may persist post-TAA, negating one of the primary goals of the surgery.
- Early Return to High-Impact Activities: Can accelerate implant wear and lead to early failure. Patient education is key here.
Clinical & Radiographic Imaging

You Might Also Like