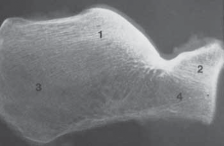
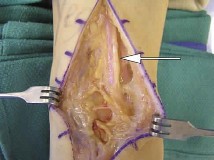
Advanced Surgical Management of Pelvic & Acetabular Fractures: Anatomy & Approaches
Key Takeaway
Pelvic and acetabular fractures are complex orthopedic injuries. Effective surgical management requires mastering their epidemiology, classifications (Judet-Letournel, Tile), and intricate surgical anatomy. Understanding the pelvic ring, acetabular columns, and critical neurovascular structures ensures precise approaches, stable fixation, and optimal patient outcomes.
Introduction & Epidemiology
Pelvic and acetabular fractures represent a formidable challenge in orthopedic trauma surgery, often associated with high-energy mechanisms, significant physiological derangement, and substantial morbidity. Mastering the diverse surgical approaches to these complex anatomical regions is paramount for achieving optimal patient outcomes, including anatomical reduction, stable fixation, and restoration of function. These injuries frequently occur in younger, economically active individuals involved in motor vehicle collisions, falls from height, or industrial accidents, resulting in considerable societal and economic burden. There is a bimodal distribution, with high-energy trauma affecting younger patients and low-energy falls contributing to fragility fractures in the elderly, particularly those with osteopenia or osteoporosis.
Pelvic ring injuries are classified by various systems, notably the Young-Burgess classification based on mechanism (Anterior-Posterior Compression, Lateral Compression, Vertical Shear, Combined Mechanical) and the Tile classification based on stability (A: Stable, B: Rotationally unstable, C: Rotationally and Vertically unstable). Acetabular fractures are classically categorized by Judet and Letournel into five elementary patterns (posterior wall, posterior column, anterior wall, anterior column, transverse) and five associated patterns (posterior column and posterior wall, transverse and posterior wall, anterior column and posterior hemitransverse, T-type, both column). The incidence of pelvic fractures ranges from 16 to 37 per 100,000 person-years, with acetabular fractures comprising approximately 3-8% of all adult fractures. Associated injuries, including head trauma, thoracic trauma, abdominal visceral injuries, and genitourinary trauma, are prevalent, necessitating a multidisciplinary approach grounded in Advanced Trauma Life Support (ATLS) principles. Early recognition, precise classification, and judicious application of surgical principles are critical determinants of long-term functional recovery and the prevention of disabling complications such as post-traumatic arthritis, chronic pain, and neurological deficits.
Surgical Anatomy & Biomechanics
A thorough understanding of the intricate surgical anatomy and biomechanics of the pelvis and acetabulum is fundamental to safe and effective surgical intervention.
Pelvic Ring Anatomy
The pelvic ring is a closed osteoligamentous structure composed of the sacrum, two innominate bones (ilium, ischium, pubis), and their strong ligamentous connections. Stability is provided by:
*
Anterior Structures:
Pubic symphysis, arcuate ligament.
*
Posterior Structures:
Sacroiliac joints, anterior and posterior sacroiliac ligaments, sacrotuberous ligaments, sacrospinous ligaments. These posterior ligamentous complexes are crucial for vertical and rotational stability.
*
Bony Anatomy:
The iliac crest serves as an important landmark and donor site for bone graft. The sacrum, a keystone in pelvic stability, articulates with the ilium at the sacroiliac joints. The pubic rami form the anterior arch.
Acetabular Anatomy
The acetabulum is a hemispherical socket forming the articulation with the femoral head. It comprises two columns and a quadrilateral plate:
*
Anterior Column:
Extends from the anterior superior iliac spine, through the anterior wall, to the pubic ramus.
*
Posterior Column:
Extends from the posterior ilium, through the posterior wall, to the ischial tuberosity.
*
Quadrilateral Plate:
The medial wall of the acetabulum, providing significant support to the femoral head.
*
Weight-Bearing Dome:
The superior articular surface.
Neurovascular Structures of Concern
Understanding the proximity of critical neurovascular structures is paramount to minimizing iatrogenic injury during surgical dissection and fixation.
*
Major Arteries:
*
External Iliac Artery/Vein:
Located anteriorly, along the pelvic brim, vulnerable during ilioinguinal approaches.
*
Internal Iliac Artery/Vein:
Branches supply the gluteal regions and pelvic viscera.
*
Superior Gluteal Artery/Vein:
Exits the greater sciatic notch, susceptible during posterior approaches or superior gluteal screw placement.
*
Inferior Gluteal Artery/Vein:
Exits the greater sciatic notch inferior to the piriformis.
*
Obturator Artery/Vein:
Courses along the obturator canal, often forms the "corona mortis" anastomosis with the external iliac or inferior epigastric artery, a crucial structure to be aware of during approaches to the pubic symphysis or medial quadrilateral plate.
*
Major Nerves:
*
Sciatic Nerve:
Exits the greater sciatic notch, courses posterior to the hip joint, highly vulnerable in posterior acetabular and pelvic approaches.
*
Femoral Nerve:
Lies lateral to the femoral artery in the femoral triangle, at risk during anterior dissection of the iliac fossa.
*
Obturator Nerve:
Passes through the obturator foramen, vulnerable during medial dissection.
*
Superior Gluteal Nerve:
Accompanies the superior gluteal vessels, innervates gluteus medius and minimus, at risk with lateral iliac wing dissection or superior gluteal screw placement.
*
Lateral Femoral Cutaneous Nerve:
Crosses the iliac crest near the ASIS, susceptible to injury or entrapment during anterior iliac crest approaches.
Biomechanics
- Pelvic Ring: Functions as a robust load-bearing structure transferring forces between the axial skeleton and lower limbs. Stability is maintained by a combination of bony congruity and strong ligamentous complexes. Disruption of these complexes leads to instability and potential for significant hemorrhage.
- Acetabulum: The spherical articulation provides a wide range of motion while withstanding immense compressive and shear forces. Fractures disrupt articular congruity, impair load distribution, and lead to post-traumatic arthritis if not anatomically reduced and stably fixed. The anterior and posterior columns function as distinct load-bearing units, and their disruption significantly compromises hip joint stability.
Figure 1: Illustration demonstrating key anatomical relationships relevant to pelvic and acetabular surgery.
Indications & Contraindications
The decision-making process for operative versus non-operative management of pelvic and acetabular fractures is complex, relying on fracture stability, displacement, articular congruity, patient physiological status, and associated injuries.
Indications for Operative Management
-
Pelvic Ring Fractures:
- Mechanical Instability: Tile B (rotationally unstable) and Tile C (rotationally and vertically unstable) fractures, including APC II/III, LC II/III, and Vertical Shear patterns.
- Significant Displacement: Especially in the posterior pelvic ring (sacrum, SI joint), indicating ligamentous disruption.
- Open Pelvic Fractures: Require urgent debridement and stabilization to prevent infection.
- Neurological Deficits: Associated with sacral fractures, especially cauda equina syndrome, warranting decompression and stabilization.
- Vascular Injury: Requiring angiography and embolization, often followed by stabilization.
- Gross Malreduction: After external fixation or initial stabilization that does not adequately restore pelvic stability.
- Fracture-Dislocations: Of the pubic symphysis or sacroiliac joint.
-
Acetabular Fractures:
- Displaced Articular Fractures: Incongruity of the articular surface >2mm.
- Marginal Impaction: Of the weight-bearing dome.
- Intra-articular Loose Bodies: Causing mechanical block or damage to articular cartilage.
- Femoral Head Subluxation or Dislocation: Persisting after reduction or unstable after closed reduction.
- Posterior Wall Fractures: With instability on stress views (e.g., obturator oblique with internal rotation of the hip).
- Irreducible Fractures: Where closed reduction is impossible or unsatisfactory.
- Anterior Column/Wall Fractures: With significant displacement and potential for future impingement or arthritis.
- Associated Fractures: e.g., femoral neck fracture, requiring simultaneous management.
Contraindications for Operative Management
-
Absolute Contraindications:
- Patient Instability: Unresuscitatable shock, severe systemic comorbidities that prohibit anesthesia or prolonged surgery (e.g., severe cardiac or pulmonary disease, uncontrolled sepsis).
- Severe Local Contamination/Infection: Of the surgical field (relative, as open fractures require debridement, but definitive fixation may be delayed).
-
Relative Contraindications:
- Stable Fracture Patterns: Minimally displaced, stable pelvic ring or acetabular fractures that are unlikely to benefit from surgical intervention compared to non-operative treatment.
- Extensive Soft Tissue Injury/Degloving: Requiring delay for soft tissue recovery.
- Chronic, Untreated Infection: In the vicinity of the planned surgical approach.
- Delay in Presentation: Extremely late presentation of certain fracture types, where callus formation makes reduction impossible, and surgical goals shift towards salvage.
Table: Operative vs. Non-Operative Indications
| Feature | Operative Indications | Non-Operative Indications |
|---|---|---|
| Pelvic Ring | Tile B/C instability (rotational/vertical shear) | Tile A stability (APCI, LC I, isolated pubic rami) |
| Pubic symphysis diastasis >2.5 cm | Minimally displaced fractures | |
| Open fractures | Medically unstable patient (initial management often non-op) | |
| Neurological compromise (e.g., cauda equina from sacral fx) | Extensive degloving injury (delay definitive fixation) | |
| Acetabulum | Articular incongruity >2 mm | Concentrically reduced femoral head (post-reduction) |
| Femoral head subluxation/dislocation (unstable) | Minimally displaced (e.g., posterior wall <2mm) | |
| Marginal impaction of weight-bearing dome | Medically unstable patient | |
| Intra-articular loose bodies | Elderly with stable fracture pattern and low demand | |
| Irreducible fractures |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is the cornerstone of successful pelvic and acetabular surgery, enabling the surgeon to anticipate challenges and optimize outcomes.
Pre-Operative Planning
-
Imaging Review:
- Standard Radiographs: AP pelvis, inlet, and outlet views for pelvic ring injuries. Judet views (obturator oblique, iliac oblique) for acetabular fractures.
- Computed Tomography (CT) Scan: Essential for both pelvic and acetabular fractures. Thin-cut axial images with 2D and 3D reconstructions are critical for delineating fracture patterns, displacement, comminution, articular involvement, and identifying associated injuries. 3D reconstructions aid in understanding complex fracture morphology and planning screw trajectories.
- Magnetic Resonance Imaging (MRI): Useful for assessing ligamentous injuries (e.g., posterior sacroiliac complex, pubic symphysis) in stable pelvic ring injuries where plain radiographs and CT may underestimate instability, and for evaluating soft tissue injuries or hematomas.
- Fracture Classification: Utilize standard classification systems (Young-Burgess/Tile for pelvis, Judet-Letournel for acetabulum) to guide treatment strategy.
- Surgical Approach Selection: Based on fracture pattern, displacement, and surgeon familiarity. The goal is to obtain adequate exposure for anatomical reduction and stable fixation with minimal iatrogenic damage.
- Hardware Planning: Template plates and screws using actual hardware or digital templating software. Pre-bend plates to approximate normal anatomy using cadaveric models or 3D prints if available.
-
Patient Optimization:
- Resuscitation: Ensure hemodynamic stability. Address associated injuries.
- Blood Management: Type and cross-match blood, consider cell saver, massive transfusion protocols.
- DVT Prophylaxis: Initiate pre-operatively, continue post-operatively.
- Antibiotic Prophylaxis: Standard broad-spectrum antibiotics, often extended for open fractures.
- Heterotopic Ossification (HO) Prophylaxis: Consider NSAIDs (e.g., indomethacin) or low-dose radiation post-operatively, especially for high-risk patients (e.g., TBI, significant soft tissue injury, posterior approaches to acetabulum).
Patient Positioning
Appropriate patient positioning is crucial for exposure, fluoroscopic access, and preventing iatrogenic injury.
1.
Supine Position:
*
Indications:
Ilioinguinal, Stoppa, anterior pelvic approaches (pubic symphysis, anterior SI joint).
*
Setup:
Patient flat on the operating table. A bump under the ipsilateral hip may facilitate exposure of the posterior aspect of the iliac crest for bone graft. Fluoroscopy unit placed for AP, inlet, and outlet views. Traction table often used for acetabular fractures for provisional reduction.
2.
Lateral Decubitus Position:
*
Indications:
Kocher-Langenbeck approach, some posterior iliac crest bone graft harvests, extended iliofemoral approach.
*
Setup:
Patient positioned with the injured side up. Pillows or beanbag for support. Axillary roll. Sacral and peroneal nerve padding. Free draping of the operative leg allows for range of motion and traction. Fluoroscopy for Judet views.
3.
Prone Position:
*
Indications:
Posterior pelvic ring fixation (sacral fractures, posterior SI joint fixation), posterior iliac crest bone graft.
*
Setup:
Patient prone on a radiolucent table or bolsters to allow abdomen to hang freely, minimizing venous congestion. Padding of face, chest, iliac crests, and knees. Fluoroscopy for sacral and SI views.
4.
Considerations:
*
Operating Table:
Radiolucent table compatible with fluoroscopy is essential.
*
Traction Table:
Often used for acetabular fractures to achieve preliminary reduction via ligamentotaxis. Requires careful setup to avoid traction neurapraxia.
*
Fluoroscopy:
C-arm must have unrestricted access for all necessary views (AP pelvis, inlet, outlet, Judet views, sacral views).
*
Neuro-Monitoring:
Consider for complex sacral fractures or cases with pre-existing neurological deficits.
Detailed Surgical Approach / Technique
The choice of surgical approach depends on the fracture pattern, displacement, and the specific anatomical structures requiring access for reduction and fixation. A combination of approaches may be necessary for complex injuries.
Pelvic Approaches
1. Anterior Approach to the Iliac Crest for Bone Graft
- Indications: Harvest of cancellous bone graft, access to the anterior ilium.
- Positioning: Supine.
- Incision: Curvilinear incision just posterior and inferior to the anterior superior iliac spine (ASIS), following the iliac crest for approximately 5-8 cm.
-
Dissection:
- Incise skin and subcutaneous tissue.
- Identify and protect the lateral femoral cutaneous nerve as it crosses the iliac crest medially to the ASIS.
- Incise the fascia over the iliac crest. Subperiosteal elevation of the origin of the abdominal wall musculature (external and internal obliques, transversus abdominis) from the lateral aspect of the ilium.
- Subperiosteal elevation of the iliacus muscle from the medial aspect of the ilium.
- Bone Graft Harvest: Create an osteotomy window in the outer table of the ilium. Harvest cancellous bone from the inner table. Close periosteum meticulously to prevent hernia.
- Closure: Layered closure.
2. Posterior Approach to the Iliac Crest for Bone Graft
- Indications: Harvest of cancellous and cortical bone graft, access to the posterior ilium.
- Positioning: Prone or lateral decubitus.
- Incision: Curvilinear incision centered over the posterior superior iliac spine (PSIS), extending laterally along the iliac crest.
-
Dissection:
- Incise skin and subcutaneous tissue.
- Incise the lumbodorsal fascia overlying the gluteus maximus.
- Subperiosteal elevation of the gluteus maximus and paraspinal muscles from the iliac crest.
- Caution: Avoid excessive stripping posteriorly near the PSIS to protect the superior cluneal nerves, which cross the crest.
- Bone Graft Harvest: Harvest cancellous bone from the inner table or cortical-cancellous strips from the crest.
- Closure: Layered closure.
3. Anterior Approach to the Pubic Symphysis (Pfannenstiel)
- Indications: Fixation of pubic symphysis diastasis, displaced pubic rami fractures.
- Positioning: Supine.
- Incision: Transverse Pfannenstiel incision approximately 2 cm superior to the pubic symphysis.
-
Dissection:
- Incise skin and subcutaneous tissue.
- Incise the anterior rectus sheath transversely.
- Separate the rectus abdominis muscles in the midline.
- Retract the rectus abdominis muscles superiorly to expose the space of Retzius (preperitoneal space).
- Caution: Identify and ligate or cauterize the "corona mortis" (anastomosis between obturator and inferior epigastric arteries/veins), which can be a significant source of bleeding, found inferior to the pubic bone.
- Expose the pubic symphysis and superior pubic rami subperiosteally.
- Reduction & Fixation: Reduce symphysis diastasis with reduction clamps. Fixation typically involves a precontoured plate (e.g., 3.5mm symphyseal plate) applied to the superior aspect of the pubic bones. For pubic rami, consider anterior plating or retrograde pubic ramus screws.
- Closure: Reapproximate rectus abdominis muscle origins, close rectus sheath, then subcutaneous tissue and skin.
4. Anterior Approach to the Sacroiliac Joint (for Pelvic Ring Fixation)
- Indications: Anterior plate fixation of unstable sacroiliac joint disruptions or sacral fractures, often in conjunction with symphyseal plating.
- Positioning: Supine, often with a traction table to aid reduction.
- Incision: Oblique incision originating just medial to the ASIS, extending superomedially toward the umbilicus (similar to a lower abdominal wall approach, or part of an ilioinguinal approach).
-
Dissection:
- Incise skin and subcutaneous tissue.
- Split the external oblique fascia, then internal oblique and transversus abdominis muscles in line with their fibers.
- Retract the peritoneum and its contents medially to enter the retroperitoneal space.
- Carefully identify and protect the external iliac vessels and ureter.
- Subperiosteal dissection along the inner aspect of the iliac wing, posterior to the psoas muscle, to expose the anterior aspect of the sacroiliac joint.
- Caution: Lumbar plexus nerves (femoral, obturator, lateral femoral cutaneous) lie within the psoas muscle or on its surface, protect them.
- Reduction & Fixation: Reduce SI joint displacement. Apply a pelvic reconstruction plate (e.g., 3.5mm) across the anterior aspect of the SI joint, securing it to the ilium and sacral ala.
- Closure: Layered closure, reapproximating muscle layers and fascia.
5. Posterior Approach to the Sacroiliac Joint (for Percutaneous Fixation)
- Indications: Percutaneous iliosacral screw fixation for unstable SI joint disruptions or sacral fractures (most common method).
- Positioning: Prone.
- Incision: Small skin incisions (stab wounds) for guide wire and cannulated screw insertion, guided by fluoroscopy.
- Dissection: Minimal, primarily involves blunt dissection through muscle and fascia to bone.
-
Reduction & Fixation:
- Closed reduction of SI joint/sacral displacement using external rotation forces, pelvic clamp, or temporary external fixator.
- Using fluoroscopy (inlet, outlet, lateral sacral views), carefully place guide wires into the S1 and/or S2 sacral bodies, ensuring they are contained within the bone and clear of neural foramina.
- Caution: The superior gluteal neurovascular bundle exits the greater sciatic notch superior to the piriformis and is at risk with improper or laterally placed S1 screws. Use the lateral sacral view to ensure screws are not breaching the anterior cortex of the sacrum.
- Measure length and insert cannulated screws.
- Closure: Skin closure.
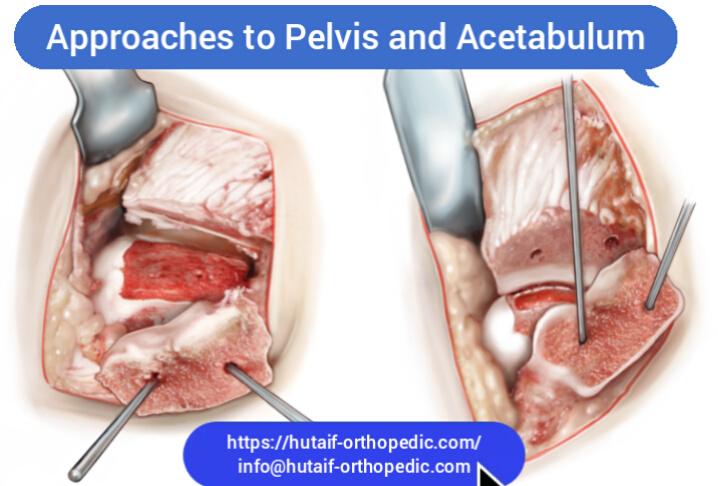
Acetabular Approaches
1. Kocher-Langenbeck Approach (Posterior)
- Indications: Posterior wall, posterior column, transverse, and T-type fractures, especially when the main displacement is posterior.
- Positioning: Lateral decubitus, injured side up. Free draping of the leg.
- Incision: Curvilinear incision starting 5 cm distal to the PSIS, curving laterally over the greater trochanter, and extending distally along the posterior femoral shaft for 10-15 cm.
-
Dissection:
- Incise skin and subcutaneous tissue.
- Incise the fascia lata.
- Split the gluteus maximus fibers in line with their orientation.
- Identify the sciatic nerve lying deep to the gluteus maximus and inferior to the piriformis. Carefully mobilize and protect the nerve throughout the procedure. It is the most critical structure to protect.
- Release the short external rotators (piriformis, superior gemellus, obturator internus, inferior gemellus, quadratus femoris) from their insertions on the greater trochanter. Tag these muscles with sutures for later repair.
- Capsulotomy of the hip joint if needed for articular inspection.
- Exposure: This approach exposes the posterior column, posterior wall, posterior roof, and greater sciatic notch.
- Reduction & Fixation: Use reduction clamps, levers, and hooks. Apply buttress plates to the posterior column and/or posterior wall. Lag screws for articular fragments.
- Closure: Repair the short external rotators to the greater trochanter. Repair gluteus maximus fascia. Layered closure.
2. Ilioinguinal Approach (Anterior)
- Indications: Anterior column, anterior wall, both column, transverse, and T-type fractures, and fractures of the quadrilateral plate.
- Positioning: Supine, with a bump under the ipsilateral hip for slight external rotation if desired, or on a traction table.
- Incision: Classic "bikini" or "Pfannenstiel" type incision, approximately 12-15 cm long, starting 2 cm medial to the ASIS and extending toward the contralateral side, crossing the midline 1-2 cm superior to the pubic symphysis. The skin incision may be extended superiorly and laterally from the ASIS along the iliac crest for more proximal exposure.
-
Dissection (Three Windows):
-
Window 1 (Lateral):
Located lateral to the external iliac vessels.
- After incising skin and subcutaneous tissue, incise the external oblique aponeurosis lateral to the inguinal ligament.
- Mobilize and retract the spermatic cord (male) or round ligament (female) inferiorly.
- Identify and incise the internal oblique and transversus abdominis muscles, entering the retroperitoneal space.
- Retract the iliopsoas muscle and femoral nerve laterally.
- This window exposes the inner wall of the ilium, sacroiliac joint, and greater sciatic notch region (posterior aspect of the iliac wing).
-
Window 2 (Middle):
Between the external iliac artery and vein.
- Medial to Window 1, separate the external iliac artery and vein from the psoas muscle.
- Carefully dissect between the artery and vein (vascular loop often required for retraction).
- This window exposes the anterior column, quadrilateral plate, and dome.
-
Window 3 (Medial):
Medial to the external iliac vein.
- Retract the external iliac vein laterally.
- Expose the superior pubic ramus, pubic symphysis, and medial portion of the quadrilateral plate.
- Caution: Be aware of the corona mortis. Retract the bladder medially.
-
Window 1 (Lateral):
Located lateral to the external iliac vessels.
- Reduction & Fixation: Use reduction clamps and bone hooks. Apply reconstruction plates along the iliac crest, anterior column, and superior pubic ramus. Screws directed into the anterior column, pubic body, and potentially the quadrilateral plate.
- Closure: Repair the inguinal ligament/external oblique aponeurosis. Layered closure.
3. Stoppa Approach (Pararectus)
- Indications: Primarily for fractures involving the quadrilateral plate and anterior column, especially when direct visualization of the quadrilateral surface is desired, or when the external iliac vessels prevent adequate access with the ilioinguinal approach.
- Positioning: Supine, with the ipsilateral side slightly elevated.
- Incision: Longitudinal paramedian incision, approximately 10-15 cm, starting 2 cm superior to the pubic symphysis, parallel to the rectus abdominis muscle, and 2-3 cm lateral to the midline.
-
Dissection:
- Incise skin and subcutaneous tissue.
- Incise the anterior rectus sheath laterally to the rectus abdominis muscle.
- Retract the rectus abdominis muscle medially.
- Incise the posterior rectus sheath (transversalis fascia) and peritoneum laterally, entering the retroperitoneal space.
- Caution: Identify and protect the inferior epigastric vessels and the corona mortis. Mobilize the bladder medially.
- This approach offers direct access to the quadrilateral plate, superior pubic ramus, and anterior column, medial to the external iliac vessels and nerves.
- Reduction & Fixation: Facilitates direct reduction and plating of the quadrilateral surface with buttress or spring plates.
- Closure: Repair posterior rectus sheath and anterior rectus sheath. Layered closure.
4. Extended Iliofemoral Approach
- Indications: Highly complex both-column fractures, severe comminution, or for revision surgery where extensive exposure is required. This is a salvage approach due to significant morbidity.
- Positioning: Lateral decubitus, injured side up.
- Incision: Long, curvilinear incision from the posterior iliac crest, along the iliac crest to the ASIS, then continuing along the lateral aspect of the thigh to the mid-femur.
-
Dissection:
- Extensive subperiosteal elevation of all muscles from the outer table of the ilium (gluteus maximus, medius, minimus, tensor fascia lata).
- Often involves a trochanteric osteotomy (e.g., greater trochanter) for better exposure and access to the joint.
- Caution: Significant soft tissue devascularization. Risk of superior gluteal neurovascular injury and lateral femoral cutaneous nerve injury.
- Exposure: Provides extensive visualization of both anterior and posterior columns.
- Reduction & Fixation: Allows for direct reduction of complex fracture patterns.
- Closure: Reattach trochanteric osteotomy. Reattach gluteal muscles. Layered closure.
General Principles of Reduction and Fixation
- Anatomical Reduction: For articular fractures, anatomical reduction is paramount to minimize post-traumatic arthritis.
- Indirect Reduction: Ligamentotaxis using traction or external fixators can provide preliminary reduction.
- Direct Reduction: Use of specialized instruments (reduction clamps, pointed reduction forceps, bone hooks, ball-spikes, periosteal elevators) to manipulate fragments.
- Temporary Fixation: K-wires or small wires to hold reduced fragments.
- Definitive Fixation: Reconstruction plates (3.5 mm) are commonly used for acetabular fractures, contoured to the complex anatomy. Lag screws provide interfragmentary compression. Buttress plates support articular segments. Locking plates may be used in osteoporotic bone.
- Fluoroscopic Control: Essential throughout the procedure to confirm reduction and hardware placement.
Complications & Management
Surgical intervention for pelvic and acetabular fractures carries a significant risk of complications, reflecting the severity of the trauma, the complexity of the anatomy, and the extensive nature of the surgery.
General Complications
- Hemorrhage: Significant intraoperative blood loss is common, requiring meticulous hemostasis, often cell saver, and liberal transfusion. Pelvic packing or angiography with embolization may be necessary for uncontrolled bleeding.
- Infection: Surgical site infection (SSI) can range from superficial to deep. Rates vary but can be up to 5-10%. Management involves debridement, antibiotics, and possible hardware removal in chronic cases.
- Deep Venous Thrombosis (DVT) and Pulmonary Embolism (PE): High incidence due to prolonged immobilization, hypercoagulability, and extensive surgery. Prophylaxis (mechanical and chemical) is critical.
- Malunion/Nonunion: Failure to achieve or maintain anatomical reduction and stable fixation can lead to malunion or nonunion, potentially requiring revision surgery.
- Heterotopic Ossification (HO): Ectopic bone formation in soft tissues. Particularly common after posterior acetabular approaches (Kocher-Langenbeck) and in patients with associated TBI. Prophylaxis with NSAIDs or radiation therapy is often indicated.
- Post-Traumatic Arthritis: The most common long-term complication of acetabular fractures, even with anatomical reduction, due to cartilage damage at the time of injury. May necessitate hip arthroplasty in the future.
-
Nerve Palsy:
- Sciatic nerve: Most common with posterior acetabular approaches (Kocher-Langenbeck), incidence 5-20%. Often neuropraxia, but can be complete transection.
- Femoral nerve: Rare, associated with anterior approaches (ilioinguinal).
- Obturator nerve: Rare, associated with medial dissection.
- Lateral femoral cutaneous nerve: Sensory nerve, common with anterior iliac approaches (ilioinguinal, bone graft harvest), usually resolves or is managed symptomatically.
- Superior gluteal nerve: Associated with high iliac wing approaches or misplaced screws in the superior ilium/sacrum.
- Vascular Injury: Direct injury to external iliac, internal iliac, obturator, or gluteal vessels. The corona mortis is a common source of anterior pelvic hemorrhage. May require immediate repair, ligation, or embolization.
- Hardware Complications: Screw pullout, plate breakage, prominence requiring removal.
Table: Common Complications, Incidence, and Salvage Strategies
| Complication | Incidence | Salvage / Management Strategies |
|---|---|---|
| Hemorrhage | High (variable) | Pre-op planning, cell saver, MTP, judicious use of hypotensive anesthesia, angiography/embolization, pelvic packing |
| Deep Infection | 2-10% | Debridement, irrigation, IV antibiotics, implant retention (if stable) or removal (if unstable/chronic), negative pressure wound therapy |
| DVT/PE | High (10-60% DVT, 1-5% PE) | Mechanical prophylaxis (SCDs), chemical prophylaxis (LMWH), early mobilization, IVC filter (select high-risk) |
| Heterotopic Ossification | 10-30% (clinical), higher radiographically | Prophylaxis (Indomethacin, radiation), surgical excision if symptomatic and mature HO |
| Sciatic Nerve Palsy | 5-20% (K-L approach) | Meticulous dissection, protection, early diagnosis, neurolysis if persistent, bracing, rehabilitation |
| Femoral Nerve Palsy | <1% (Ilioinguinal) | Meticulous dissection, protection, early diagnosis, neurolysis, bracing, rehabilitation |
| Vascular Injury (major) | <5% | Immediate repair by vascular surgeon, ligation if small and non-critical, embolization, tamponade |
| Post-Traumatic Arthritis | 20-50% (long-term) | Optimize initial reduction/fixation, activity modification, NSAIDs, eventual total hip arthroplasty (THA) |
| Malunion/Nonunion | 5-15% | Revision ORIF, osteotomy, bone grafting, salvage arthrodesis or THA |
| Hardware Prominence/Failure | 10-20% | Hardware removal after fracture healing, revision fixation for failure |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is a critical component of treatment, aiming to restore strength, range of motion, and functional independence while protecting the surgical repair. Protocols vary significantly based on the fracture pattern, stability of fixation, and individual patient factors.
General Principles
- Pain Management: Multimodal analgesia to facilitate early mobilization and participation in therapy.
-
Weight-Bearing (WB):
- Non-Weight-Bearing (NWB): For 8-12 weeks is common for unstable pelvic ring injuries or complex acetabular fractures with tenuous fixation or comminution.
- Touch-Down Weight-Bearing (TDWB) / Partial Weight-Bearing (PWB): Often initiated between 6-12 weeks, gradually progressing to full weight-bearing based on radiographic healing and clinical stability.
- Weight-Bearing as Tolerated (WBAT): May be allowed earlier for stable pelvic ring injuries (e.g., APC I, LC I) or highly stable fixation constructs.
-
Range of Motion (ROM):
- Early Gentle ROM: Often initiated within the first few days, avoiding provocative movements or extremes of motion that could stress the repair.
-
Acetabular Fractures:
- Posterior approaches (Kocher-Langenbeck): Avoid hip flexion >90 degrees, adduction, and internal rotation to prevent posterior dislocation.
- Anterior approaches (Ilioinguinal, Stoppa): Avoid hip extension and external rotation.
- Pelvic Fractures: Emphasize core stability and pain-free motion.
-
Strengthening:
- Isometric Exercises: Initiate early for gluteal, quadriceps, and hamstring muscles.
- Progressive Strengthening: Advance as tolerated, initially non-weight-bearing, then closed kinetic chain exercises. Focus on hip abductors, extensors, and core musculature.
-
Functional Progression:
- Transfers: Bed mobility, chair transfers.
- Gait Training: With appropriate assistive devices (walker, crutches) according to weight-bearing status.
- Activities of Daily Living (ADLs): Progress toward independence in self-care.
- Patient Education: Crucial for adherence to activity restrictions, understanding the healing process, and recognizing signs of complications.
Example Phased Protocol (Highly Variable)
Phase 1: Immediate Post-Op (Weeks 0-6)
- Goals: Pain control, protect fixation, prevent complications, initiate gentle ROM.
- Weight-Bearing: NWB or TDWB (e.g., 10-15 kg).
-
Exercises:
- Ankle pumps, quadriceps sets, gluteal sets.
- Gentle, supervised active/passive ROM within precautions.
- Upper extremity conditioning.
- Mobilization: Bed to chair transfers, gait training with assistive devices.
Phase 2: Early Healing (Weeks 6-12)
- Goals: Increase ROM, begin strength, progress weight-bearing.
- Weight-Bearing: Progress from TDWB/PWB to WBAT as tolerated, guided by radiographs and pain.
-
Exercises:
- Increased intensity of ROM exercises.
- Initiate light resistance exercises (e.g., elastic bands) for hip and core.
- Pool therapy may be beneficial.
- Mobilization: Continue gait training, reduce assistive device reliance.
Phase 3: Advanced Healing & Strengthening (Weeks 12-24)
- Goals: Full weight-bearing, restore strength and endurance, improve proprioception.
- Weight-Bearing: Full weight-bearing.
-
Exercises:
- Progressive resistive exercises for all major hip muscle groups.
- Balance and proprioception training.
- Light aerobic activities (e.g., stationary bike, elliptical).
- Transition to functional exercises specific to patient's activities.
Phase 4: Return to Activity (Months 6+)
- Goals: Return to pre-injury activity levels, sports-specific training.
- Exercises: High-level strengthening, plyometrics, agility drills, sport-specific training.
- Monitoring: Continued monitoring for pain, weakness, or residual functional deficits.
Summary of Key Literature / Guidelines
The management of pelvic and acetabular fractures is constantly evolving, guided by robust clinical research, technological advancements, and expert consensus. Key literature and guidelines underpin current best practices.
-
Classification Systems:
- Judet and Letournel (1964, 1974): Seminal work categorizing acetabular fractures into 10 patterns (5 elementary, 5 associated) remains the gold standard for diagnosis, surgical planning, and prognosis. Their detailed descriptions of surgical approaches are foundational.
- Tile (1988): Classification of pelvic ring injuries based on mechanical stability (Type A: Stable, Type B: Rotationally unstable, Type C: Rotationally and vertically unstable).
- Young and Burgess (1990): Classification of pelvic ring injuries based on mechanism of injury (Anterior-Posterior Compression, Lateral Compression, Vertical Shear), providing insights into injury patterns and associated visceral damage.
- AO/OTA Classification: Comprehensive fracture classification system widely used for both pelvic and acetabular injuries, providing a standardized language for research and communication.
-
Timing of Surgery:
- Consensus generally favors early definitive fixation of unstable pelvic and displaced acetabular fractures once the patient is physiologically optimized ("damage control orthopedics"). Delayed surgery (e.g., >2-3 weeks for acetabulum) is associated with increased difficulty of reduction and poorer outcomes.
- Damage Control: For polytraumatized patients, initial stabilization may involve external fixation or pelvic binders, followed by definitive internal fixation once systemic inflammatory response syndrome (SIRS) resolves.
-
Choice of Surgical Approach:
- Letournel's Principles: The choice of approach is dictated by the fracture anatomy (Judet-Letournel classification), the displacement, and the need for direct visualization for reduction and fixation.
- Multimodal Imaging: High-resolution CT with 3D reconstructions is indispensable for pre-operative planning, confirming fracture patterns, assessing fragment rotation, and guiding approach selection.
- Minimally Invasive Techniques: Percutaneous iliosacral screw fixation is the standard for many posterior pelvic ring injuries, minimizing soft tissue stripping and complications. Recent advancements include robotic assistance for screw placement accuracy.
-
Heterotopic Ossification (HO) Prophylaxis:
- Evidence supports the use of NSAIDs (e.g., Indomethacin 25 mg TID for 6 weeks) or a single dose of post-operative radiation therapy (e.g., 700-800 cGy) for high-risk patients, particularly after posterior acetabular approaches (Kocher-Langenbeck).
-
Thromboembolism Prophylaxis:
- Guidelines from organizations like the American Academy of Orthopaedic Surgeons (AAOS) and American College of Chest Physicians (ACCP) recommend both mechanical (intermittent pneumatic compression) and pharmacological (low molecular weight heparin or direct oral anticoagulants) prophylaxis for patients with pelvic and acetabular fractures, given their high risk of DVT/PE.
-
Outcomes and Prognosis:
- Long-term outcomes for acetabular fractures are primarily linked to the quality of anatomical reduction, residual articular step-off or gap, and the development of post-traumatic arthritis.
- For pelvic ring injuries, stability restoration, neurological recovery, and functional independence are key metrics.
- Advanced surgical techniques, improved imaging, and refined perioperative care have significantly improved outcomes, yet these injuries remain challenging with a potential for long-term disability.
Mastering surgical approaches to the pelvis and acetabulum is a demanding yet highly rewarding endeavor. It requires not only a deep understanding of anatomy and biomechanics but also meticulous pre-operative planning, precise surgical execution, and thoughtful post-operative management, all underpinned by continuous learning and adherence to evidence-based guidelines.
You Might Also Like