Operative Management and Stabilization of the Distal Radioulnar Joint
Key Takeaway
Distal radioulnar joint (DRUJ) instability frequently results from distal radius malunions, ulnar styloid nonunions, or triangular fibrocartilage complex (TFCC) tears. Surgical management requires a meticulous approach, ranging from corrective radial osteotomies to complex soft-tissue reconstructions. Anatomical reconstruction of the distal radioulnar ligaments, such as the Adams-Berger technique, provides robust stabilization while preserving rotational kinematics. This guide details the biomechanics, indications, and step-by-step surgical techniques for restoring DRUJ stability.
INTRODUCTION TO DRUJ INSTABILITY
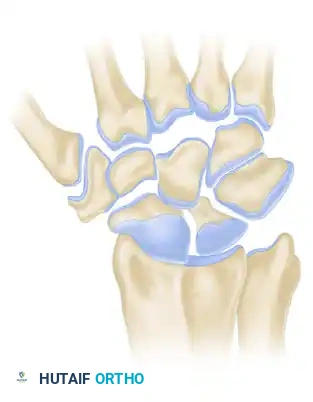
The distal radioulnar joint (DRUJ) is a highly complex trochoid articulation that, in conjunction with the proximal radioulnar joint (PRUJ) and the interosseous membrane (IOM), facilitates pronation and supination of the forearm. Stability of the DRUJ is conferred by a delicate interplay between the bony architecture of the sigmoid notch and the dynamic and static soft-tissue restraints, most notably the triangular fibrocartilage complex (TFCC).
Chronic DRUJ instability is a debilitating condition characterized by ulnar-sided wrist pain, weakness, and a mechanical sensation of subluxation or clunking during forearm rotation. It frequently arises as a sequela of distal radius fractures, isolated TFCC tears, or Essex-Lopresti injuries. The management of DRUJ instability demands a rigorous understanding of wrist biomechanics, as the surgeon must differentiate between bony incongruity and soft-tissue incompetence to select the appropriate reconstructive procedure.
Clinical Pearl: The DRUJ is inherently unstable from a bony perspective. The radius of curvature of the sigmoid notch is substantially larger than that of the ulnar head, meaning bony congruity provides minimal constraint. The joint relies almost entirely on the TFCC—specifically the volar and dorsal radioulnar ligaments—for stability.
BONY PROCEDURES FOR DRUJ STABILIZATION
Before embarking on complex soft-tissue reconstructions, the surgeon must critically evaluate the bony architecture of the distal radius and ulna. Soft-tissue reconstruction in the presence of uncorrected bony deformity is destined to fail due to altered joint kinematics and excessive strain on the reconstructed ligaments.
Distal Radial Osteotomy
DRUJ instability related to malunited distal radial fractures is a common clinical scenario. A malunion characterized by radial shortening, loss of volar tilt, or significant articular step-off alters the spatial relationship between the sigmoid notch and the ulnar head.
* Biomechanics of Malunion: Dorsal angulation of the distal radius shifts the load-bearing axis and subluxates the ulnar head volarly relative to the sigmoid notch. Radial shortening leads to ulnocarpal impaction and distorts the tension of the interosseous membrane and TFCC.
* Surgical Correction: Corrective distal radial osteotomy, supplemented with structural bone grafting (autograft or allograft) and rigid volar locking plate fixation, is the treatment of choice. By restoring anatomical radial length, inclination, and volar tilt, the DRUJ is anatomically realigned. In many cases, restoring the bony anatomy spontaneously resolves the DRUJ instability without the need for direct soft-tissue intervention.
Open Reduction and Internal Fixation of the Ulnar Styloid
The ulnar styloid serves as the critical anchor point for the superficial and deep (foveal) fibers of the TFCC.
* Indications: Ununited, displaced ulnar styloid base fractures that are associated with demonstrable DRUJ instability should be treated with open reduction and internal fixation (ORIF). Tip fractures generally do not compromise the foveal attachment and rarely require fixation.
* Technique: Fixation can be achieved using a tension band wiring construct, a headless compression screw, or a dedicated ulnar styloid plate. Restoring the ulnar styloid anatomically re-tensions the TFCC and stabilizes the DRUJ.
SOFT TISSUE RECONSTRUCTION TECHNIQUES
When the bony architecture is intact or has been surgically restored, yet DRUJ instability persists, soft-tissue reconstruction is indicated. Historically, a myriad of soft-tissue techniques have been proposed to stabilize the DRUJ and the unstable distal ulna. The evolution of these procedures reflects a growing understanding of DRUJ kinematics.
Direct TFCC Repair
Bowers emphasized the paramount importance of repairing or reconstructing the TFCC in the unstable wrist. While acute tears are highly amenable to arthroscopic or open repair, late repair of the TFCC may still be possible depending on tissue quality.
* Minimal Subluxation: Hermansdorfer and Kleinman found that direct reattachment of the TFCC to the fovea is highly effective for patients presenting with minimal subluxation and good tissue integrity.
* Technique: This is typically performed via an open ulnar approach or arthroscopically assisted transosseous suturing, anchoring the deep fibers of the TFCC back to the fovea using suture anchors or drill holes.
Adams' Classification of Soft Tissue Reconstructions
If the TFCC is irreparably damaged or attenuated, but the articular surfaces are in good condition and the sigmoid notch is competent, reconstruction of the ligaments around the DRUJ is required to stabilize the joint satisfactorily. Adams identified three distinct categories of soft tissue reconstruction for chronic DRUJ instability:
1. Distal Ulnar Tenodesis
This category utilizes local tendons, typically the extensor carpi ulnaris (ECU) or flexor carpi ulnaris (FCU), to create a dynamic or static sling around the distal ulna.
* Bach’s Augmentation: Bach et al. described a technique utilizing tenodesis augmentation of a TFCC repair with a distally based slip of the ECU tendon. This sling helps to depress the ulnar head and prevent dorsal subluxation during pronation.
* Limitations: While historically popular, simple tenodesis procedures often fail to control the complex rotational forces of the DRUJ and may stretch out over time, leading to recurrent instability.
2. Ulnocarpal Tether
These techniques aim to stabilize the distal ulna by tethering it to the carpus.
* Historical Techniques: The ulnocarpal techniques described by Hui and Linscheid, as well as by Boyes and Bunnell, utilize tendon grafts to create a suspension system between the ulna and the carpal bones.
* Modern Biomechanical Insights: Although these procedures may be effective in select cases, a landmark cadaveric study by Gupta et al. suggested that the ulnocarpal ligaments may not require reconstruction in all patients with DRUJ instability. The primary stabilizers are the radioulnar ligaments; over-constraining the ulnocarpal joint can lead to severe stiffness and loss of wrist flexion/extension.
3. Radioulnar Tether (Anatomical Reconstruction)
The difficulty of restoring a smooth carpal articulation, a flexible rotational radioulnar tether, an ulnocarpal suspension from the radius, an ulnocarpal cushion, and an ulnar shaft to the ulnar carpal connection is widely recognized. Consequently, many complex radioulnar tethering procedures proximal to the radioulnar joint have been described.
* Scheker’s Technique: Scheker et al. suggested that tendon graft reconstruction passed through radioulnar drill holes helped to stabilize the DRUJ by directly mimicking the mechanical restraint of the native ligaments.
* The Adams-Berger Procedure: Adams emphasized the critical importance of reconstructing the distal radioulnar ligaments to restore DRUJ stability while preserving DRUJ motion. In patients with posttraumatic DRUJ instability, Adams and Berger found that anatomical reconstruction of the distal radioulnar ligaments restored stability, preserved motion, and relieved pain in 12 of 14 patients. This has become the gold standard for chronic, irreparable DRUJ instability.
Surgical Warning: Non-anatomical reconstructions (such as ECU tenodesis) often result in a trade-off: they either fail to provide adequate stability or they over-constrain the joint, leading to a profound loss of pronation and supination. Anatomical reconstruction via radioulnar tethering is strongly preferred.
SURGICAL TECHNIQUE: THE ADAMS-BERGER ANATOMICAL RECONSTRUCTION
The Adams-Berger procedure utilizes a free tendon graft (typically the palmaris longus or a plantaris allograft) to anatomically reconstruct the volar and dorsal radioulnar ligaments.
Preoperative Planning and Indications
- Indications: Chronic DRUJ instability, irreparable TFCC, competent sigmoid notch, and preserved articular cartilage (no severe osteoarthritis).
- Contraindications: Advanced DRUJ arthritis (which would require a salvage procedure such as a Darrach, Sauvé-Kapandji, or DRUJ arthroplasty), fixed bony deformity of the radius.
Step 1: Patient Positioning and Approach
- The patient is placed supine with the operative arm on a radiolucent hand table. A proximal arm tourniquet is applied.
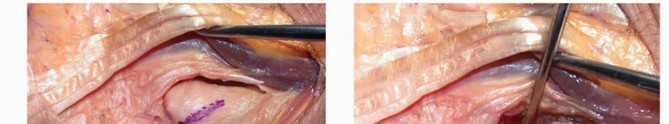
- A dorsal longitudinal incision is made over the 5th extensor compartment, extending from the distal third of the ulna to the mid-carpus.
- The extensor retinaculum is incised, and the extensor digiti minimi (EDM) is retracted radially. The ECU subsheath is carefully preserved.
- The DRUJ capsule is exposed and opened longitudinally to inspect the joint surfaces and clear any fibrotic remnants of the TFCC.
Step 2: Preparation of the Radius and Ulna
- Radial Drill Hole: A guide pin is placed at the dorsal margin of the sigmoid notch, approximately 5 mm proximal to the articular surface. It is directed volarly, exiting at the volar margin of the sigmoid notch. A 3.2 mm cannulated drill is used to create the radial tunnel.
- Ulnar Drill Hole: The fovea of the ulnar head is identified. A guide pin is inserted into the fovea and directed proximally and ulnarly, exiting at the ulnar neck. A 3.2 mm drill is used to create the ulnar tunnel.
Pitfall: Improper placement of the radial drill hole is a common cause of failure. If the hole is placed too proximally, the graft will not replicate the anatomical vector of the radioulnar ligaments, resulting in altered kinematics and restricted rotation.
Step 3: Graft Harvest and Passage
- A palmaris longus autograft is harvested using standard minimally invasive tendon strippers. If absent, a strip of flexor carpi radialis (FCR) or an allograft may be utilized.
- The graft is passed through the ulnar tunnel from proximal to distal, exiting at the fovea.
- The two limbs of the graft (now exiting the fovea) are passed across the DRUJ. One limb is passed dorsally over the ulnar head, and the other is passed volarly.
- Both limbs are then passed through the radial tunnel from their respective sides (volar to dorsal, and dorsal to volar), creating a figure-of-eight configuration that perfectly mimics the native volar and dorsal radioulnar ligaments.
Step 4: Tensioning and Fixation
- The forearm is placed in neutral rotation.
- The DRUJ is manually compressed to ensure the ulnar head is seated concentrically within the sigmoid notch.
- The graft limbs are tensioned simultaneously. Over-tensioning must be avoided, as it will severely restrict forearm rotation.
- The graft is secured to the radius. This can be achieved by tying the two limbs of the graft over the dorsal bony bridge of the radius, or by utilizing a tenodesis screw or suture anchors.
- The capsule and extensor retinaculum are meticulously repaired.
POSTOPERATIVE PROTOCOL AND REHABILITATION
The success of an anatomical DRUJ reconstruction relies as much on disciplined postoperative rehabilitation as it does on surgical execution.
- Phase I (0-4 Weeks): The patient is placed in a long-arm Muenster cast or a sugar-tong splint with the forearm in neutral rotation. Absolute immobilization of the DRUJ is required to allow for graft incorporation. Finger and thumb range of motion (ROM) exercises are initiated immediately to prevent tendon adhesions.
- Phase II (4-8 Weeks): The cast is transitioned to a custom short-arm splint that controls rotation. Active and active-assisted forearm pronation and supination are initiated under the strict guidance of a specialized hand therapist. Passive stretching is strictly avoided during this phase to prevent stretching the graft.
- Phase III (8-12 Weeks): The splint is gradually weaned. Progressive strengthening exercises for the forearm and wrist are introduced.
- Phase IV (3-6 Months): Return to heavy manual labor or contact sports is generally permitted after 4 to 6 months, provided the patient has regained functional ROM and demonstrates no clinical signs of recurrent instability.
COMPLICATIONS AND MANAGEMENT
While anatomical reconstruction yields excellent outcomes, surgeons must be prepared to manage potential complications:
* Postoperative Stiffness: The most common complication. A mild loss of terminal pronation or supination (10-15 degrees) is expected and generally well-tolerated. Severe stiffness usually results from over-tensioning the graft or prolonged immobilization.
* Recurrent Instability: Can occur due to graft rupture, failure of fixation, or failure to address an underlying bony malunion prior to soft-tissue reconstruction. Revision surgery may require a salvage procedure.
* Hardware Irritation: If interference screws or anchors are used dorsally on the radius, they may irritate the extensor tendons, necessitating hardware removal after graft healing.
CONCLUSION
The stabilization of the distal radioulnar joint is a complex surgical challenge that requires a thorough appreciation of wrist kinematics. While bony deformities must be addressed with corrective osteotomies, isolated soft-tissue incompetence is best managed through anatomical reconstruction. As demonstrated by Adams and Berger, recreating the precise vectors of the volar and dorsal radioulnar ligaments provides the most reliable means of restoring stability, relieving pain, and preserving the vital rotational capacity of the forearm.
You Might Also Like