Osteoarthritis of the Wrist: SLAC Wrist Pathoanatomy and Surgical Management
Key Takeaway
Scapholunate advanced collapse (SLAC) is the most common pattern of degenerative wrist arthritis, driven by untreated scapholunate ligament injuries. This predictable progression of articular wear begins at the radioscaphoid joint and advances to the midcarpal joint, characteristically sparing the radiolunate articulation. Surgical management depends on the stage of degeneration and includes motion-preserving procedures such as proximal row carpectomy (PRC) or four-corner arthrodesis with scaphoid excision to alleviate pain while maintaining functional wrist kinematics.
OSTEOARTHRITIS OF THE WRIST: SCAPHOLUNATE ADVANCED COLLAPSE (SLAC)
Degenerative arthritis developing in the wrist is most frequently the result of altered carpal kinematics, classically presenting as Scapholunate Advanced Collapse (SLAC). The SLAC wrist is a highly predictable pattern of progressive articular degeneration related to chronic instability around the scaphoid. While primary degenerative changes or crystalline arthropathies can occasionally manifest in the carpus, the vast majority of SLAC wrists are the direct sequelae of posttraumatic changes—specifically, an untreated or unrecognized rupture of the scapholunate interosseous ligament (SLIL) or a chronic scaphoid nonunion (which leads to a similar pattern known as Scaphoid Nonunion Advanced Collapse, or SNAC).
Biomechanics and Pathoanatomy
The scaphoid functions as the critical mechanical bridge between the proximal and distal carpal rows. Normal wrist kinematics rely on the intact scapholunate ligament to couple the flexion tendency of the scaphoid with the extension tendency of the lunate. When the scapholunate ligament is disrupted, this vital linkage is lost.
The scaphoid subsequently flexes and pronates, while the lunate, now tethered only to the triquetrum via the intact lunotriquetral ligament, extends. This uncoupling results in a Dorsal Intercalated Segment Instability (DISI) deformity. The end result is a wrist with profound biomechanical derangement:
* Widening of the scapholunate gap: The classic "Terry Thomas" sign on anteroposterior radiographs.
* Radioscaphoid joint incongruency: The flexed scaphoid shifts its contact area dorsally on the radial styloid, drastically reducing the contact surface area and exponentially increasing focal articular contact stresses.
* Midcarpal instability: The capitate migrates proximally into the widened scapholunate interval, leading to narrowing and degeneration of the capitolunate joint.
* Radiolunate preservation: Remarkably, the radiolunate joint is almost universally spared. The lunate fossa of the distal radius and the proximal articular surface of the lunate share a concentrically spherical relationship. Even in the extended position of a DISI deformity, the radiolunate joint maintains a congruent, load-sharing articulation without the pathological shear forces seen in the radioscaphoid compartment.
Clinical Pearl: The absolute preservation of the radiolunate joint is the cornerstone of modern salvage procedures for the SLAC wrist. If the radiolunate joint exhibits degenerative changes, motion-preserving procedures like Proximal Row Carpectomy (PRC) or Four-Corner Fusion (4CF) are contraindicated, and a total wrist arthrodesis must be considered.
RADIOGRAPHIC STAGING OF SLAC WRIST
The progression of SLAC wrist osteoarthritis follows a strict, sequential pattern originally described by Watson and Ballet. Understanding these stages is critical for preoperative planning and surgical decision-making.
Stage I SLAC Wrist
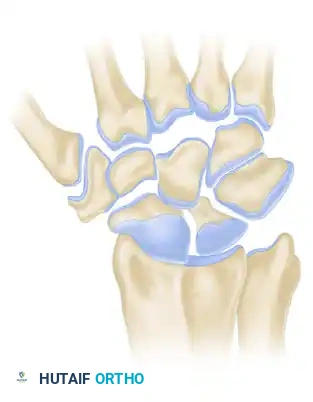
In Stage I, the degenerative changes are strictly localized to the articulation between the radial styloid and the distal pole of the scaphoid. The flexed posture of the scaphoid causes abnormal point-loading against the radial styloid, leading to localized joint space narrowing, subchondral sclerosis, and osteophyte formation.

Stage II SLAC Wrist
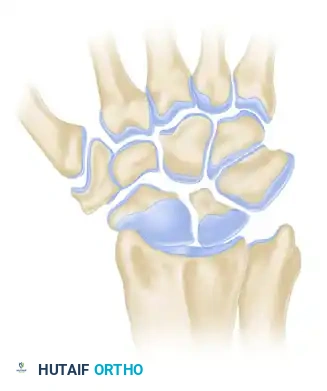
As the instability persists, the degenerative process extends proximally to involve the entire radioscaphoid fossa. The scaphoid continues to articulate abnormally with the elliptical scaphoid fossa of the distal radius, leading to complete loss of the radioscaphoid articular cartilage. The capitolunate and radiolunate joints remain preserved at this stage.
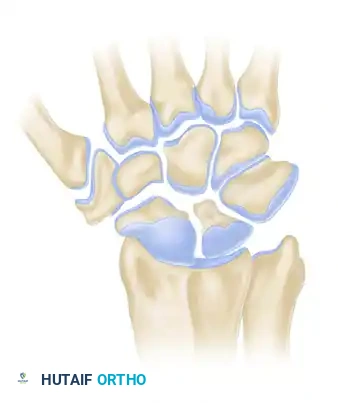
Stage III SLAC Wrist
In Stage III, the capitate subluxates proximally into the widened scapholunate interval. This proximal migration alters the kinematics of the midcarpal joint, leading to narrowing, sclerosis, and osteophyte formation at the capitolunate joint. Despite this extensive midcarpal and radioscaphoid destruction, the radiolunate joint remains remarkably preserved.
SURGICAL MANAGEMENT STRATEGIES
The surgical treatment of the SLAC wrist is dictated by the stage of arthritis, the patient's age, functional demands, and the status of the radiolunate and proximal capitate articular surfaces. The primary goal is pain relief, with a secondary goal of preserving a functional arc of motion and grip strength.
Historical Context: Silastic Implants
Historically, the surgical treatment of this problem involved limited intercarpal arthrodesis (such as capitohamate and triquetrolunate fusions) combined with scaphoid excision and Silastic (silicone) scaphoid replacement. The rationale was to maintain carpal height and kinematics. However, because of the high tendency for patients to develop "silicone synovitis"—a destructive, foreign-body giant cell reaction to particulate silicone wear debris—this practice has been largely abandoned.
Today, many surgeons prefer the use of biological spacers, such as rolled tendon (e.g., palmaris longus) or fascia, and some use no spacer at all following scaphoid excision. More definitively, contemporary reports and long-term outcomes suggest that other motion-preserving procedures—specifically Proximal Row Carpectomy (PRC) or Capitate-Hamate-Triquetrum-Lunate (Four-Corner) fusion with scaphoid excision—are the most satisfactory methods for dealing with this troublesome problem.
Proximal Row Carpectomy (PRC)
PRC involves the excision of the scaphoid, lunate, and triquetrum, allowing the capitate to articulate directly within the lunate fossa of the distal radius.
* Indications: Stage I or II SLAC wrist.
* Contraindications: Stage III SLAC wrist (capitolunate arthritis precludes PRC because the proximal capitate cartilage is degraded and cannot serve as a smooth articular surface against the radius).
* Advantages: Technically simpler than 4CF, requires no bone grafting, eliminates the risk of nonunion, and requires a shorter period of postoperative immobilization.
Four-Corner Fusion (4CF) with Scaphoid Excision
Four-corner fusion involves the excision of the entire scaphoid and the decortication and arthrodesis of the capitate, hamate, lunate, and triquetrum. The lunate is reduced out of its DISI posture prior to fixation.
* Indications: Stage II or Stage III SLAC wrist. Because the midcarpal joint is fused, pre-existing capitolunate arthritis (Stage III) is addressed and neutralized.
* Advantages: Preserves carpal height better than PRC and is highly durable for heavy laborers.
Surgical Warning: A successful 4CF relies entirely on a pristine radiolunate joint. If intraoperative inspection reveals full-thickness cartilage loss in the lunate fossa, the surgeon must be prepared to convert to a total wrist arthrodesis.
STEP-BY-STEP SURGICAL TECHNIQUE: LIMITED INTERCARPAL ARTHRODESIS & FIXATION
The following details the operative steps for limited intercarpal arthrodesis (such as lunotriquetral or four-corner fusions) utilizing bone grafting and rigid fixation.
1. Patient Positioning and Approach
- Place the patient supine with the operative arm extended on a radiolucent hand table.
- Apply a well-padded proximal arm tourniquet.
- Make a dorsal longitudinal incision centered over the radiocarpal joint, typically in line with Lister's tubercle and the third metacarpal.
- Incise the extensor retinaculum over the third dorsal compartment. Transpose the extensor pollicis longus (EPL) tendon radially.
- Elevate the second and fourth dorsal compartments subperiosteally to expose the dorsal wrist capsule.
- Perform a ligament-sparing dorsal capsulotomy (e.g., Berger's flap) to expose the radiocarpal and midcarpal joints.
2. Joint Preparation and Scaphoid Excision
- Inspect the articular surfaces to confirm the preoperative staging. Verify that the radiolunate joint is intact to maintain joint alignment and to hold the graft in place.
- Excise the scaphoid piecemeal using a rongeur or osteotome, taking care not to damage the volar radiocarpal ligaments (radioscaphocapitate ligament).
- Using a high-speed burr or sharp curettes, meticulously denude the articular cartilage down to bleeding subchondral bone at the target fusion sites (e.g., capitohamate, triquetrolunate, and capitolunate joints for a 4CF).
- Correct the DISI deformity by placing a joystick (Kirschner wire) into the lunate and flexing it into a neutral position relative to the radius.
3. Bone Grafting
- Obtain cancellous bone graft to promote robust osteogenesis. This can be harvested locally from the distal radius (e.g., from Lister's tubercle or the scaphoid fossa) or from the iliac crest if the distal radius has been used as a bone graft donor previously or if a larger volume is required.
- Tightly pack the cancellous bone graft into the prepared intercarpal spaces (e.g., the lunotriquetral and capitolunate gaps).
4. Fixation Techniques
Rigid fixation is paramount to prevent nonunion. While modern circular plates are popular, traditional methods remain highly effective and biomechanically sound.
* Kirschner Wire Fixation: Use multiple Kirschner wires (0.045 or 0.062 inch) for lunotriquetral and midcarpal fixation. Drive the wires percutaneously or directly across the joints while maintaining the reduced carpal alignment.
* Screw Fixation: A Herbert screw or other headless compression lag screw can be used for superior biomechanical compression. If a screw is to be used for lunotriquetral fixation, make another small incision over the ulnar margin of the triquetrum to allow the proper trajectory for placement of the screw across the triquetrum and into the lunate.
* After fixation and packing of the bone graft, obtain intraoperative fluoroscopic radiographs in multiple planes (PA, Lateral, Oblique) to ascertain satisfactory position of the carpal bones, correction of the DISI deformity, and appropriate length and placement of the fixation hardware.
5. Closure
- Irrigate the wound thoroughly to remove any bone debris.
- Meticulously close the dorsal capsule to prevent extensor tendon bowstringing and to provide a smooth gliding surface.
- Repair the extensor retinaculum, leaving the EPL transposed in the subcutaneous tissues.
- Close the skin with non-absorbable sutures.
- Apply a sterile, nonadherent dressing and a well-padded short-arm volar splint, placing the wrist in slight extension.
POSTOPERATIVE CARE AND REHABILITATION
The postoperative protocol must balance the need for rigid immobilization to achieve bony union with the need to initiate motion to prevent debilitating wrist stiffness.
- 0 to 2 Weeks: The patient remains in the initial postoperative splint. Elevation and digital range of motion are encouraged immediately to reduce edema and prevent tendon adhesions. The skin sutures are removed about 2 weeks after surgery.
- 2 to 8 Weeks: Following suture removal, the patient is transitioned to a short-arm cast or a rigid custom thermoplastic splint. Protective splinting is continued for about 12 weeks total.
- 8 Weeks: Protected motion exercises are allowed at about 8 weeks. The patient may remove the splint for therapist-guided active and active-assisted range of motion exercises, focusing on wrist flexion, extension, pronation, and supination.
- 8 to 12 Weeks: The Kirschner wires (if left protruding or symptomatic) are removed after clinical and radiographic union is shown, usually at 8 to 12 weeks.
- 3 Months: Strengthening exercises are begun at about 3 months after the operation, once solid arthrodesis is confirmed on radiographs.
- 4+ Months: Return to unrestricted activities is gradual. Sports, heavy lifting, and impact loading should be avoided for at least 4 months to protect the maturing fusion mass.
Pitfall: Premature initiation of aggressive passive stretching or heavy lifting before radiographic union is confirmed is the leading cause of hardware failure and nonunion in intercarpal arthrodesis. Always correlate clinical lack of tenderness with bridging trabeculae on radiographs before advancing the rehabilitation protocol.
COMPLICATIONS
While motion-preserving salvage procedures for SLAC wrist are generally highly successful in alleviating pain, surgeons must counsel patients on potential complications:
1. Nonunion: The most common complication of 4CF, particularly at the capitolunate articulation. Smoking, inadequate decortication, and insufficient rigid fixation increase this risk.
2. Hardware Impingement: Dorsal hardware prominence can cause extensor tendon irritation or rupture. Headless compression screws or low-profile dorsal circular plates mitigate this risk.
3. Decreased Range of Motion: Patients should expect to lose approximately 40-50% of their normal radiocarpal flexion-extension arc following either PRC or 4CF. Setting realistic preoperative expectations is crucial.
4. Progressive Degeneration: In PRC, radiocapitate arthritis can develop over time. In 4CF, radiolunate arthritis may occur if the lunate was not properly reduced out of its extended DISI posture during fixation, leading to abnormal point loading.
You Might Also Like
