Management of Inflammatory Hand Pathologies: Synovitis, Nodules, and Surgical Staging
Key Takeaway
The management of the rheumatoid and inflammatory hand requires a meticulous balance of nonoperative modalities and precisely staged surgical interventions. Persistent synovitis often responds to targeted corticosteroid injections, though refractory cases necessitate synovectomy. When surgical reconstruction is indicated, prioritizing pain relief and functional restoration is paramount. This involves strategic staging of procedures, addressing the wrist as the foundational keystone, and employing specialized fixation techniques tailored to osteopenic bone.
NONOPERATIVE TREATMENT FOR SYNOVITIS AND TENOSYNOVITIS
The management of inflammatory arthropathies and tenosynovitis in the hand requires a highly structured, evidence-based approach. Persistent tenosynovitis or joint synovitis characterized by obvious, boggy swelling that remains refractory to several weeks of systemic medical management (including nonsteroidal anti-inflammatory drugs [NSAIDs] and disease-modifying antirheumatic drugs [DMARDs]) warrants localized intervention.
Indications and Efficacy of Corticosteroid Injections
Local injections of a corticosteroid preparation combined with a local anesthetic serve as the first-line localized treatment for persistent inflammatory swelling. In many instances, this technique provides profound pain relief, reduces tenosynovial volume, and effectively delays the need for surgical intervention.
This nonoperative modality is particularly efficacious for:
* Stenosing Tenosynovitis (Trigger Fingers): Reduces the volume of the A1 pulley and the inflamed flexor tendon sheath.
* Carpal Tunnel Syndrome: Decreases flexor tenosynovitis within the rigid confines of the carpal canal, thereby relieving median nerve compression.
* Osteoarthritis (OA) of the Trapeziometacarpal (CMC) Joint: Provides symptomatic relief in early-stage basal joint arthritis.
* Distal Interphalangeal (DIP) Joint OA and Proximal Interphalangeal (PIP) Joint Rheumatoid Arthritis (RA): Yields favorable, albeit temporary, symptomatic improvement.
Clinical Pearl: While initial corticosteroid injections often yield dramatic results, the efficacy of repeated injections diminishes over time. Furthermore, repeated intratendinous or peritendinous injections carry a well-documented risk of tendon attenuation and spontaneous rupture, particularly in the rheumatoid patient where enzymatic degradation of the tendon is already occurring.
Transitioning to Surgical Intervention
The window for nonoperative management is finite. If florid synovitis and tenosynovitis persist after 4 to 6 months of adequate medical and localized injection therapy, surgical intervention must be strongly considered. Prolonged tenosynovitis inevitably leads to invasive pannus formation, which enzymatically destroys the tendon substance and articular cartilage.
Prophylactic synovectomy or tenosynovectomy is indicated to prevent catastrophic complications such as Vaughan-Jackson syndrome (attritional rupture of the extensor tendons) or flexor tendon ruptures within the carpal tunnel or digital sheaths.
SURGICAL MANAGEMENT OF RHEUMATOID NODULES
Rheumatoid subcutaneous nodules are a hallmark of seropositive rheumatoid arthritis, occurring in approximately 20% to 30% of patients. Histologically, they are characterized by a central zone of fibrinoid necrosis surrounded by palisading histiocytes and a peripheral layer of chronic inflammatory cells.
Anatomic Distribution and Clinical Presentation
These nodules typically manifest in areas subjected to repeated mechanical pressure or friction. Common locations include:
* The dorsal aspect of the hand and metacarpophalangeal (MCP) joints.
* The palmar surface of the fingers (often interfering with grip).
* The subcutaneous border of the proximal ulna.
* The olecranon bursa.
While often asymptomatic, these masses can grow to a size where they severely interfere with digital motion, cause significant discomfort during activities of daily living (ADLs), and pose a high risk for skin breakdown, ulceration, and subsequent secondary infection.
Surgical Excision Technique
If rheumatoid nodules cause sufficient mechanical symptoms or threaten skin integrity, surgical excision is indicated.
- Incision and Approach: A meticulously planned incision (often a lazy-S or longitudinal incision avoiding the apex of the nodule) is utilized. The overlying skin in rheumatoid patients is notoriously thin, fragile, and ischemic.
- Neurovascular Protection: Careful blunt and sharp dissection is mandatory. On the palmar aspect of the digits, the neurovascular bundles are frequently displaced, splayed, or densely adherent to the pseudocapsule of larger nodular masses. Magnification loupes should be used to meticulously separate the digital nerves from the nodule.
- Soft Tissue Coverage: Because the expanding nodule often causes pressure necrosis of the overlying dermis, primary closure may result in excessive tension. The surgeon must be prepared to utilize full-thickness or split-thickness skin grafts to achieve tension-free closure and prevent postoperative wound dehiscence.
Surgical Warning: Incomplete excision of the nodule's base or failure to address the underlying bony prominence (such as an osteophyte or prominent ulnar styloid) will result in a high rate of local recurrence.
STAGING OF OPERATIONS IN THE INFLAMMATORY HAND
When evaluating a patient with rheumatoid arthritis or systemic connective tissue disease for surgical reconstruction, the surgeon must adopt a holistic view of the patient's entire musculoskeletal involvement. The rheumatoid hand is rarely an isolated problem; it is part of a systemic biomechanical collapse.
Prioritization: Pain vs. Function
The primary indication for surgery in the rheumatoid hand is pain that limits function. Esthetics, while important to the patient, are secondary. Patients who function well despite significant, visually striking deformities may be less inclined—and are generally poorer candidates—for surgical intervention than patients whose activities are severely restricted by pain.
Souter’s Hierarchy of Operative Procedures
To optimize outcomes, Souter recommended a strategic staging protocol, beginning with procedures that carry the highest probability of success and the lowest morbidity, typically starting on the least involved hand to maintain patient independence. He grouped hand procedures from the most effective (Group I) to the least effective (Group V):
- Group I (Highly Predictable/Effective): Carpal tunnel release, trigger finger release, dorsal tenosynovectomy, and distal radioulnar joint (DRUJ) reconstruction (e.g., Darrach or Sauvé-Kapandji procedures).
- Group II: Arthrodesis of the thumb MCP or interphalangeal joints, and PIP joint arthrodesis.
- Group III: MCP joint arthroplasty (silicone elastomer implants) and wrist arthrodesis.
- Group IV & V (Less Predictable/Salvage): Complex tendon transfers for multiple ruptures, PIP joint arthroplasties, and complex soft-tissue realignments.
The Wrist as the Keystone of Hand Function
The position and stability of the wrist dictate the biomechanical balance of the digital flexor and extensor tendons. In rheumatoid arthritis, the typical collapse pattern involves carpal supination, ulnar translation of the carpus, and radial deviation of the metacarpals. This radial deviation of the metacarpals creates a secondary, zigzag biomechanical force that exacerbates the ulnar drift of the digits at the MCP joints.
Therefore, wrist reconstruction (arthrodesis or arthroplasty) must precede or be performed concurrently with digital realignment. Correcting MCP ulnar drift without first stabilizing the wrist will inevitably lead to rapid recurrence of the digital deformity.
At the time of wrist surgery, an additional, highly reliable procedure—such as arthrodesis of the MCP joint of the thumb—may be performed simultaneously. However, more extensive, multi-level surgeries should generally be delayed to prevent overwhelming the patient's rehabilitation capacity.
Managing Complex Connective Tissue Deformities
Systemic conditions like scleroderma present unique staging challenges due to severe soft-tissue contractures and microvascular compromise.

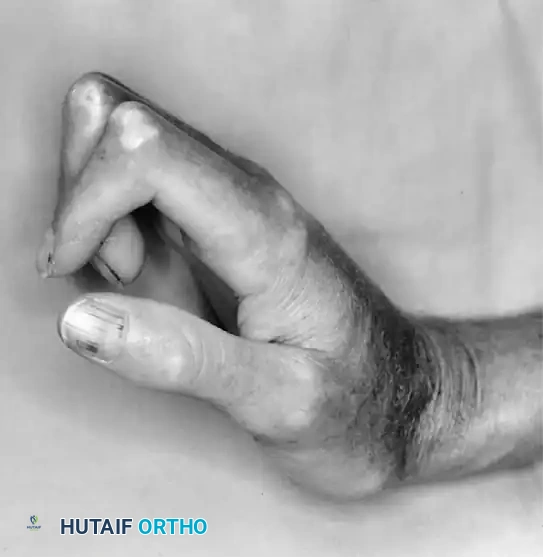
As illustrated in the systemic scleroderma patient, the classic presentation involves rigid flexion contractures of the interphalangeal joints, extension contractures of the MCP joints, and a severe adduction contracture of the thumb. In such cases, reconstructive surgery must be staged to first release the first web space (restoring thumb opposition) before addressing the digital contractures, always prioritizing the preservation of the precarious vascular supply.
Logistical Considerations for Bilateral Disease
When multiple small joint procedures (e.g., all four MCP arthroplasties or multiple PIP joint fusions) are indicated, they should be performed concurrently on the same hand to minimize the total number of surgical events and anesthetic exposures.
Frequently, the rheumatoid patient requires surgical intervention not only on the opposite hand but also on weight-bearing joints (hips, knees, feet). Crucial Rule of Staging: Surgery is almost universally performed on only one hand at a given time. The patient must retain the use of one hand for daily independent living, personal hygiene, and feeding.
Furthermore, if the patient's lower extremity involvement requires the use of external walking aids (canes, crutches, or walkers), standard grip devices will be impossible to use during the hand's postoperative recovery. In these instances, a platform walker or forearm crutch must be provided to allow weight-bearing through the forearms rather than the healing hand.
USE OF KIRSCHNER WIRES IN THE RHEUMATOID HAND
Kirschner wires (K-wires) remain a fundamental tool for osseous fixation in rheumatoid hand surgery, particularly for arthrodesis of the PIP, DIP, and thumb MCP joints. However, the rheumatoid patient presents unique biomechanical and biological challenges, primarily severe periarticular osteopenia and chronic immunosuppression.
Biomechanics and Bone Healing
In the rheumatoid hand, the osteopenic nature of the bone means that most K-wires will eventually loosen due to micro-motion at the pin-bone interface. Fortunately, because rheumatoid bone is often highly vascularized due to chronic inflammation, osseous fusion occurs remarkably rapidly after joint preparation and arthrodesis. The primary role of the K-wire is to provide temporary alignment rather than rigid, long-term biomechanical stability.
Surgical Technique and Pin Placement
The trajectory and final resting position of the K-wires are critical to preventing severe postoperative morbidity.
- Subcutaneous vs. Percutaneous: K-wires are usually cut beneath the skin at a level that makes them easily recoverable once fusion is achieved. In some instances, particularly at the PIP joints, they may be left protruding through the skin to facilitate easy removal in the clinic. If left protruding, meticulous pin-site care is required, and the postoperative dressing is applied directly over the wires to prevent catching or accidental extraction.
- Avoiding the Volar Pulp: Under no circumstances should K-wires be left embedded in the tactile pulp of the fingers or near the palmar aspect of the MCP joint of the thumb. The volar skin is highly innervated, and a prominent wire in these areas will cause excruciating pain during pinch and grasp, completely negating the functional benefits of the surgery.
- Dorsal Insertion: To avoid volar pain, wires in these regions must always be inserted or driven so that the end nearest the skin rests on the dorsal surface of the digit or hand, where the soft tissue is more forgiving and less involved in tactile interaction.
Postoperative Protocol and Removal
Because of the rapid fusion rates and the tendency for wires to loosen in osteopenic bone, prolonged retention of K-wires is rarely necessary or advised. Once clinical and radiographic evidence of early consolidation is present (typically 4 to 6 weeks), the wires should be extracted.
Most percutaneous or superficially buried K-wires can be easily removed in the outpatient office setting using a local anesthetic. Prompt removal minimizes the risk of deep pin-tract infections, which can be devastating in the immunocompromised rheumatoid patient. Following removal, the limb is typically protected in a custom orthosis until final, robust osseous union is achieved.
You Might Also Like