Double First Metatarsal Osteotomies: A Comprehensive Surgical Guide
Key Takeaway
The double first metatarsal osteotomy is a powerful surgical technique reserved for severe hallux valgus and metatarsus primus varus deformities. By combining a distal closing wedge with a proximal opening wedge osteotomy, surgeons can achieve multiplanar correction without sacrificing joint congruity. This comprehensive guide details the biomechanical rationale, precise surgical steps, and postoperative protocols necessary to optimize patient outcomes and minimize complications such as transfer metatarsalgia and malunion.
INTRODUCTION TO DOUBLE FIRST METATARSAL OSTEOTOMIES
The management of severe hallux valgus associated with a high intermetatarsal angle (metatarsus primus varus) and an abnormal distal metatarsal articular angle (DMAA) presents a complex biomechanical challenge for the orthopedic surgeon. While single osteotomies (such as the chevron, scarf, or proximal crescentic osteotomies) are sufficient for mild to moderate deformities, severe multiplanar deformities often require a more robust reconstructive approach.
The Double First Metatarsal Osteotomy, popularized by Peterson and Newman, is a highly effective, joint-sparing procedure designed to address both proximal varus angulation and distal articular malorientation simultaneously. By performing a distal closing wedge osteotomy and utilizing the resected bone as an autograft for a proximal opening wedge osteotomy, the surgeon can achieve profound correction of the first ray axis while maintaining metatarsal length and joint congruity.
This comprehensive guide explores the pathoanatomy, biomechanical rationale, preoperative planning, and step-by-step surgical execution of the double first metatarsal osteotomy, providing orthopedic residents, fellows, and practicing consultants with an evidence-based framework for mastering this complex procedure.
BIOMECHANICS AND PATHOANATOMY
Understanding the pathoanatomy of the hallux valgus complex is critical for selecting the appropriate surgical intervention. The deformity is rarely isolated to the metatarsophalangeal (MTP) joint; it typically involves a cascade of biomechanical failures across the first ray.
The Hallux Valgus Complex
In severe hallux valgus, the first metatarsal deviates medially (metatarsus primus varus), while the proximal phalanx deviates laterally. This subluxation alters the pull of the extrinsic tendons (extensor hallucis longus and flexor hallucis longus), converting them into deforming forces that exacerbate the valgus drift and induce pronation of the great toe.
The Role of the Double Osteotomy
A single proximal osteotomy can correct the intermetatarsal angle (IMA) but may inadvertently increase the DMAA, leading to a laterally facing articular surface and subsequent joint incongruity or hallux valgus recurrence. Conversely, a single distal osteotomy cannot adequately correct a severe IMA without risking lateral translation beyond the mechanical limits of the metaphysis.
The double osteotomy addresses both centers of rotation of angulation (CORA):
1. Proximal Opening Wedge: Corrects the severe metatarsus primus varus (reduces the 1-2 IMA).
2. Distal Closing Wedge: Corrects the DMAA, realigning the articular cartilage to a neutral position relative to the longitudinal axis of the first metatarsal.
Clinical Pearl: The double osteotomy is particularly advantageous in adolescent hallux valgus, where the deformity is often driven by a widened IMA and a highly abnormal DMAA, rather than degenerative joint changes.
PREOPERATIVE EVALUATION AND INDICATIONS
Clinical Assessment
A thorough clinical examination must evaluate:
* First ray hypermobility (assessing the first tarsometatarsal joint).
* Achilles tendon or gastrocnemius contracture (Silfverskiöld test).
* Presence of transfer metatarsalgia under the lesser metatarsal heads.
* Pronation and valgus deformity of the distal hallux.
If the deformity at the interphalangeal (IP) joint remains prominent even after the metatarsus primus varus and hallux valgus have been simulated as corrected, a concomitant proximal phalangeal osteotomy (Akin procedure) may be required.
Surgical Warning: The patient and their family must be informed during the informed consent process that two (or potentially three, if an Akin is needed) separate osteotomies may be required to achieve full clinical correction.
Radiographic Parameters
Standard weight-bearing anteroposterior (AP), lateral, and sesamoid axial radiographs are mandatory. Key parameters include:
* Hallux Valgus Angle (HVA): Typically > 40 degrees in severe cases.
* Intermetatarsal Angle (IMA): Typically > 15 degrees.
* Distal Metatarsal Articular Angle (DMAA): > 15 degrees indicates the need for a distal articular realignment.
* Joint Congruity: The MTP joint must be evaluated for arthritic changes, which would contraindicate a joint-sparing osteotomy.
ALTERNATIVES: THE LAPIDUS PROCEDURE (FIRST TMT ARTHRODESIS)
Historically, the rationale for arthrodesis of the first metatarsocuneiform articulation (the Lapidus procedure) was based on the assumption that developmental varus posture and hypermobility of the first metatarsal were the prime offenders in the hallux valgus complex. Currently, the Lapidus procedure is generally reserved for severe deformity with documented first ray hypermobility or TMT arthritis.
While good or excellent results have been reported in approximately 75% of patients undergoing a Lapidus procedure, it carries a distinct complication profile that makes the double osteotomy a preferable alternative in select patients (particularly those without TMT arthritis).
Complications of First TMT Arthrodesis
- Nonunion: Occurs in approximately 10% of cases.
- Malunion (Dorsal Bunion): Dorsiflexion of the first metatarsal resulting from malunion at the arthrodesis site severely limits first MTP motion and causes a dorsal bunion.
- Transfer Metatarsalgia: Occurs due to decreased weight-bearing on the elevated first ray, shifting loads to the lesser metatarsals.
- Iatrogenic Hallux Varus.
- Traumatic Cutaneous Neuromas.
To mitigate these risks during a Lapidus, technical aspects reported to improve results include:
1. The use of bone grafts to preserve metatarsal length.
2. Rigid fixation utilizing a two-screw or plate-and-screw construct.
3. Avoidance of dorsiflexion by placing the first metatarsal in approximately 5 degrees of plantar flexion compared with the preoperative weight-bearing angle of inclination.
SURGICAL ANATOMY AND VASCULAR CONSIDERATIONS
The success of a double osteotomy relies heavily on preserving the vascular supply to the intervening diaphyseal segment of the first metatarsal.
- Arterial Supply: The first metatarsal is supplied by the first dorsal metatarsal artery, the first plantar metatarsal artery, and the superficial branch of the medial plantar artery.
- Nutrient Artery: Enters the lateral aspect of the middle third of the diaphysis.
- Capsular Network: The distal metaphysis and head are supplied by an extensive capsular network.
Surgical Warning: Aggressive bilateral periosteal stripping combined with a double osteotomy significantly increases the risk of avascular necrosis (AVN) of the metatarsal head or diaphyseal segment. The lateral periosteum and lateral capsular attachments must remain intact.
SURGICAL TECHNIQUE: DOUBLE FIRST METATARSAL OSTEOTOMY (PETERSON AND NEWMAN)
The following technique details the precise execution of Surgical Technique 81-22.
Step 1: Positioning and Incision
- Place the patient supine on the operating table. A calf or thigh tourniquet is applied following exsanguination.
- Begin a longitudinal incision over the medial side of the first metatarsal.
- Curve the incision dorsally over the metatarsophalangeal joint and extend it onto the medial side of the base of the proximal phalanx.
- Carefully dissect through the subcutaneous tissues, protecting the terminal branches of the superficial peroneal nerve dorsally and the proper plantar digital nerve medially.
Step 2: Capsular Exposure and Flap Creation
- Incise the periosteum and joint capsule in the midline longitudinally.
- Create a distally based, Y-shaped capsular flap. Carefully elevate and retract this flap distally to expose the medial eminence and the MTP joint.
- Expose the metatarsal diaphysis and both metaphyses subperiosteally on the dorsal, medial, and volar surfaces only.
- CRITICAL: Leave the periosteum intact laterally. Only three-fourths of the circumference of the metatarsal should be exposed to preserve the vascular supply.
Step 3: Medial Eminence Resection
- Identify the medial eminence (bunion).
- Using a microsagittal saw, excise the medial eminence. Ensure the cut is parallel to the medial border of the foot, preserving the medial sulcus if present.
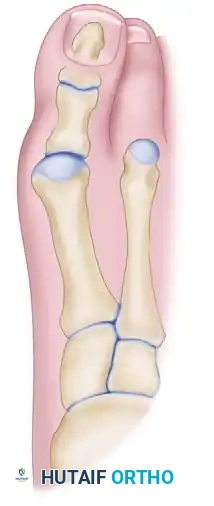
Figure 81-67A: Preoperative deformity demonstrating severe metatarsus primus varus and an abnormal DMAA. The medial eminence is exposed for resection.
Step 4: The Distal Closing Wedge Osteotomy
- Plan a transverse closing wedge osteotomy at the junction of the head and neck of the first metatarsal.
- The base of the wedge must be medial. The width of the medial base is typically 5 to 8 mm, depending on the size of the bone and the amount of DMAA correction desired. (Note: In adolescent patients, bone size varies minimally, though males generally present with slightly larger dimensions).
- The angle of the apex varies with the degree of deformity but is usually approximately 20 degrees.
- Measurement: The angle must be measured meticulously using a sterile goniometer.
- Execute the osteotomy using a fine saw blade, ensuring the lateral cortex acts as a hinge or is cut cleanly without violating the lateral soft tissues.
- Carefully extract the intact 20-degree wedge of bone and preserve it in a moist sponge; this will serve as the autograft for the proximal osteotomy.
- Close the distal osteotomy. This maneuver allows the entire head of the metatarsal, the articular surfaces, and the great toe to angle medially to a neutral position, placing the phalanges in line with the first metatarsal shaft without disturbing the capsular relationships.
- At this stage, any malrotation (pronation) of the toe can be manually corrected. Do not apply internal fixation to the distal osteotomy yet.
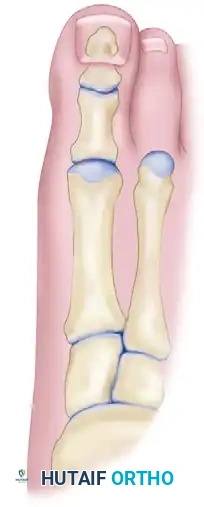
Figure 81-67B: The distal closing wedge osteotomy has been executed, correcting the articular orientation. The proximal osteotomy is planned.
Step 5: The Proximal Opening Wedge Osteotomy
- Hold the diaphysis of the metatarsal securely with a bone clamp.
- Make a second transverse osteotomy perpendicular to the metatarsal shaft, approximately 1.5 cm distal to the proximal articular surface of the first metatarsal.
- Gently open this proximal osteotomy on the medial side.
- Insert the 20-degree bone wedge (harvested from the distal metaphysis) into this proximal opening wedge osteotomy. This maneuver lateralizes the metatarsal shaft, correcting the abnormally wide first-to-second intermetatarsal angle.
Step 6: Intramedullary Fixation
- Obtain a 3/16-inch smooth Steinmann pin.
- Under direct vision, begin insertion at the tip of the great toe, exactly 2 or 3 mm below the distal end of the nail bed at its midpoint.
- Drive the pin retrograde through the distal phalanx and the proximal phalanx.
- Continue driving the pin across the MTP joint and into the metatarsal head. As the pin traverses the distal closing wedge osteotomy, its position can be visually confirmed.
- Ensure the distal osteotomy is perfectly closed and aligned, then drill the pin down the longitudinal axis of the metatarsal diaphysis.
- As the pin approaches the proximal osteotomy, visually confirm its trajectory.
- Ensure the bone graft is securely seated in the proximal opening wedge. Drive the pin through the graft and into the proximal metatarsal fragment (base) to provide rigid, continuous intramedullary fixation across all four bone segments.
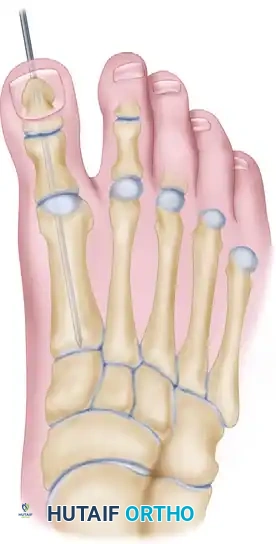
Figure 81-68: Intramedullary fixation with a Steinmann pin secures the longitudinal alignment of the metatarsal segments, the bone graft, and both phalanges.
Step 7: Rotational Control and Closure
Clinical Pearl: The intramedullary Steinmann pin provides excellent fixation in the sagittal and axial planes, preventing malunion in these vectors. However, a smooth pin does not control rotation in the frontal (coronal) plane.
- To prevent rotation of the metatarsal fragments and the hallux, the hallux must be held strictly in neutral rotation by the surgical assistant.
- While maintaining neutral rotation, resuture the Y-shaped capsular flap under appropriate tension. If the soft tissues are insufficient, the capsule may be anchored directly into the bone using suture anchors or transosseous tunnels.
- If a prominent interphalangeal deformity persists despite the metatarsal corrections, perform a proximal phalangeal (Akin) osteotomy at this stage. If the physis is closed, perform it near the base; if open, perform it at the neck.
- Close the subcutaneous tissues and skin in a standard layered fashion.
- Apply a meticulously molded, bulky compression bandage. The forefoot dressing is a critical structural component that helps control coronal rotation postoperatively.
COMPLICATIONS AND PITFALLS
While the double first metatarsal osteotomy is a powerful corrective tool, it is technically demanding. Surgeons must be vigilant regarding the following complications:
1. Avascular Necrosis (AVN)
Performing two osteotomies on a single bone significantly disrupts its intraosseous blood supply. Preservation of the lateral periosteum and lateral capsular attachments is non-negotiable. If AVN occurs, it typically affects the metatarsal head, leading to joint collapse and severe secondary osteoarthritis.
2. Malunion and Nonunion
Nonunion is rare with adequate intramedullary fixation but can occur at the proximal opening wedge site if the graft is poorly contoured or lacks compression. Malunion, particularly in dorsiflexion, will result in a dorsal bunion and transfer metatarsalgia. The Steinmann pin must be driven centrally into the proximal fragment to maintain a neutral or slightly plantarflexed sagittal alignment.
3. Loss of Fixation / Pin Tract Infection
Because the Steinmann pin exits the tip of the toe, it is susceptible to micro-motion and colonization. Meticulous pin care is required. If the pin migrates or becomes infected, early removal may be necessary, which compromises the stability of the osteotomies.
POSTOPERATIVE CARE AND REHABILITATION
Strict adherence to the postoperative protocol is essential to ensure graft incorporation and prevent hardware failure or loss of correction.
Phase 1: Immediate Postoperative Period (Weeks 0-1)
- The patient is placed in a bulky compression bandage immediately post-surgery.
- Strict elevation is mandated to control edema.
- A few days after surgery, once initial swelling subsides, the bulky dressing is converted to a short-leg, non-weight-bearing (NWB) cast.
Phase 2: Intermediate Healing (Weeks 1-6)
- The patient remains strictly non-weight-bearing in the short-leg cast.
- At exactly 6 weeks postoperatively, the patient returns to the clinic.
- The cast is bivalved and removed.
- The intramedullary Steinmann pin is extracted in the clinic (this is typically performed without anesthesia, using sterile pliers and a smooth, continuous pulling motion).
- Radiographs are obtained to confirm interval healing of both osteotomy sites and incorporation of the proximal graft.
Phase 3: Weight-Bearing and Functional Recovery (Weeks 6-11)
- Following pin removal, a short-leg walking cast (or rigid controlled ankle motion [CAM] boot, depending on surgeon preference and patient compliance) is applied.
- The patient is permitted to begin progressive weight-bearing.
- This walking cast is worn for an additional 5 weeks (until approximately 11 weeks postoperatively).
- After cast removal, physical therapy is initiated to restore first MTP joint range of motion, strengthen the intrinsic foot musculature, and normalize the gait cycle.
CONCLUSION
The double first metatarsal osteotomy remains a masterclass technique in the armamentarium of the foot and ankle surgeon. By adhering to strict biomechanical principles—meticulous measurement of the distal wedge, preservation of lateral vascularity, and rigid intramedullary stabilization—surgeons can achieve excellent, long-lasting correction of severe hallux valgus deformities while avoiding the joint-sacrificing limitations of arthrodesis. Proper patient selection, precise surgical execution, and rigorous postoperative management are the cornerstones of success in this complex reconstructive procedure.
You Might Also Like