Distal Chevron Metatarsal Osteotomy: Comprehensive Surgical Guide
Key Takeaway
The distal chevron metatarsal osteotomy is a highly effective, inherently stable intracapsular procedure utilized for the correction of mild-to-moderate hallux valgus deformities. By creating a V-shaped osteotomy through the cancellous bone of the first metatarsal head, surgeons can achieve precise lateral translation of the capital fragment. This guide details the biomechanical principles, strict indications, and step-by-step surgical execution required to optimize patient outcomes and minimize avascular necrosis risk.
INTRODUCTION TO THE DISTAL CHEVRON METATARSAL OSTEOTOMY
The distal chevron intracapsular osteotomy remains one of the most popular and reliable surgical interventions for the correction of mild-to-moderate hallux valgus associated with metatarsus primus varus. Originally described by Corless in 1976 as a modification of the Mitchell procedure, the chevron osteotomy was designed to address the biomechanical deficiencies of earlier techniques by providing superior inherent stability and maximizing cancellous bone contact.
The procedure fundamentally consists of two synergistic components:
1. Osseous Correction: A V-shaped osteotomy in the transverse plane through the metatarsal head and neck, allowing for lateral translation of the capital fragment to reduce the intermetatarsal angle (IMA).
2. Soft Tissue Realignment: Correction of the hallux valgus angle (HVA) via a meticulous medial capsulorrhaphy, often combined with the release of the adductor hallucis tendon in more pronounced deformities.
Extensive clinical series with long-term follow-up consistently report good-to-excellent outcomes in 85% to 95% of patients. While historically reserved for patients under 50 years of age, contemporary evidence supports its efficacy in older populations, provided bone quality is adequate and strict indications are met.
INDICATIONS AND PATIENT SELECTION
Patient selection is the most critical determinant of success in distal metatarsal osteotomies. The chevron osteotomy is highly effective for narrowing the forefoot, restoring cosmetically acceptable valgus, and maintaining adequate dorsiflexion of the first metatarsophalangeal (MTP) joint.
Ideal Radiographic Parameters
- Hallux Valgus Angle (HVA): Less than 30° to 40°. Deformities with an HVA > 35° frequently exhibit significant hallux pronation, which cannot be adequately corrected by medial capsulorrhaphy or a simple uniplanar osteotomy.
- Intermetatarsal Angle (IMA): Less than 13° to 20°. Standard lateral translation of the capital fragment (typically 4 to 5 mm) is mathematically insufficient to correct an IMA greater than 15° without risking severe loss of bone apposition.
Contraindications
- Severe Deformity: HVA > 40° or IMA > 20°.
- Degenerative Joint Disease: Moderate-to-severe osteoarthritis of the first MTP joint (hallux rigidus).
- First Ray Hypermobility: Significant instability at the first tarsometatarsal (TMT) joint, which may necessitate a Lapidus arthrodesis.
- Inadequate Bone Stock: Severe osteopenia or cystic changes in the metatarsal head that would compromise fixation and stability.
Clinical Pearl: A hallux valgus angle exceeding 30° is notoriously difficult to correct to a cosmetically acceptable angle (10° to 20°) using a chevron osteotomy alone, particularly if the IMA exceeds 12°. In such cases, consider a diaphyseal (Scarf) or proximal osteotomy.
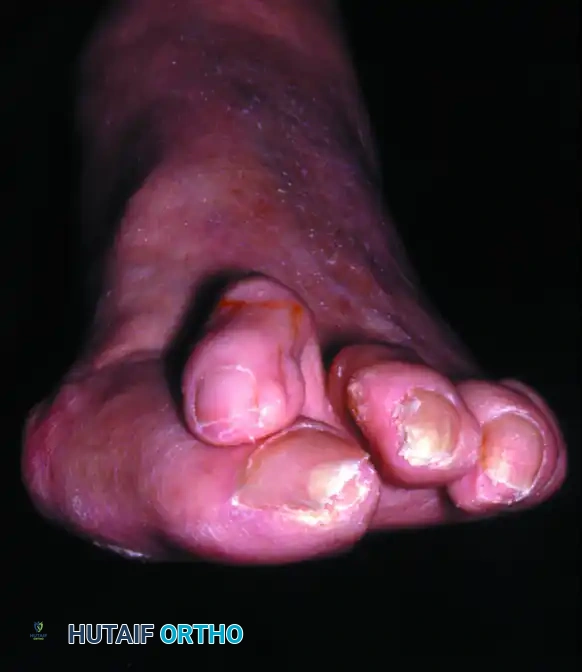
Figure 1: Clinical presentation of a severe hallux valgus deformity with an overriding second toe. This degree of deformity is exceedingly difficult to correct with a standard distal chevron osteotomy where the apex is at the subchondral bone of the capital fragment. Proximal osteotomies or fusion should be considered.
PREOPERATIVE PLANNING AND IMAGING
Standard weight-bearing anteroposterior (AP), lateral, and sesamoid axial radiographs are mandatory. The AP view is utilized to measure the HVA, IMA, and distal metatarsal articular angle (DMAA). The sesamoid axial view assesses the degree of sesamoid subluxation and frontal plane rotation (pronation) of the first metatarsal.
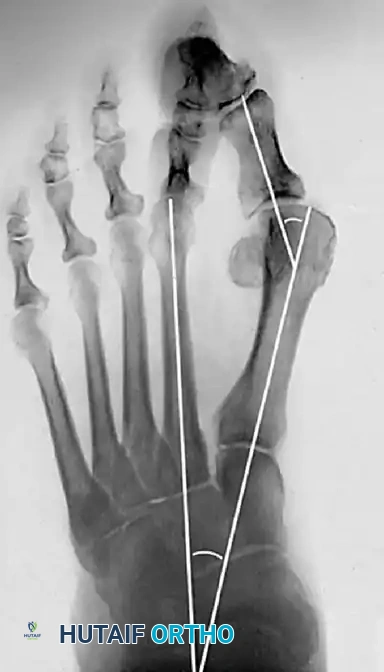
Figure 2: Preoperative weight-bearing AP radiograph demonstrating a moderate hallux valgus deformity. The HVA is measured at 38° and the IMA at 17°. While pushing the upper limits of standard indications, modifications to the chevron technique can accommodate this pathology.
Modifications of the Standard Chevron
To expand the utility of the chevron osteotomy, several modifications have been developed:
* Angle Modification: Placing the arms of the V-shaped osteotomy at a 90-degree angle rather than the traditional 60-degree angle to alter stability profiles.
* Apex Marker: Using a 2-mm drill hole at the intended apex to prevent stress risers and propagation of the osteotomy into the articular surface (Horne et al.).
* Biplanar Correction: Placing the bone wedge harvested from the medial eminence into the dorsal limb of the osteotomy to supinate, plantarflex, and distract the metatarsal (Borton and Stephens).
* Extended Lateral Displacement: Shifting the osteotomy more than 50% of the metatarsal width to address IMAs up to 18° (Murawski and Beskin).
* Proximal Extension: Utilizing an intracapsular-to-extracapsular extension with the apex slightly proximal to the center of the metatarsal head. This allows for greater correction of excessive valgus of the articular surface, though it sacrifices some inherent stability and mandates rigid internal fixation.
SURGICAL ANATOMY AND VASCULAR CONSIDERATIONS
The most devastating complication of a distal metatarsal osteotomy is avascular necrosis (AVN) of the capital fragment. The primary blood supply to the first metatarsal head is derived from the first dorsal metatarsal artery and the first plantar metatarsal artery, which form an extracapsular arterial ring.
Surgical Warning: The capsular attachments on the dorsolateral and lateral aspects of the metatarsal head and neck must be meticulously preserved. Aggressive lateral soft tissue stripping combined with the intracapsular osteotomy severs the intraosseous blood supply, exponentially increasing the risk of AVN.
STEP-BY-STEP SURGICAL TECHNIQUE (JOHNSON; CORLESS)
1. Positioning and Anesthesia
The patient is placed supine on the operating table. The procedure can be performed under general anesthesia, spinal anesthesia, or a regional ankle block. A pneumatic calf or thigh tourniquet is applied to ensure a bloodless surgical field.
2. Skin Incision and Superficial Dissection
- Begin a straight midline medial incision (or a dorsomedial incision starting at the midportion of the proximal phalanx, curving gently over the medial eminence, and ending 2 cm proximal to the eminence along the medial subcutaneous shaft).
- Raise the skin flap with meticulous atraumatic technique.
- Nerve Protection: Identify and retract the terminal branches of the medial division of the superficial peroneal nerve, which supply sensation to the dorsomedial hallux.
- Vein Preservation: Protect as many branches of the superficial venous system as possible to minimize postoperative edema and optimize wound healing.
- Carefully coagulate small vessels encountered during this exposure.
3. Capsulotomy and Joint Exposure
- Make a longitudinal capsular incision in the midline of the medial eminence. Extend it distally along the shaft of the proximal phalanx and proximally along the metatarsal shaft until the medial eminence is fully exposed. (An alternative is a Y-shaped or L-shaped capsular incision).
- By sharp dissection, raise the capsular flap, which is based distally on the base of the proximal phalanx.
- Inspect the joint by applying valgus posturing to the hallux.
- Critical Step: As the flap is raised from proximal to distal, do not release all proximal capsular attachments on the metatarsal neck. These remnants are essential for the subsequent capsulorrhaphy. Furthermore, strictly avoid stripping the capsule from the dorsolateral and lateral aspects of the metatarsal head to preserve vascularity.
4. Medial Eminence Removal (Exostectomy)
- Identify the parasagittal groove (the sagittal sulcus) and the junction of the medial eminence with the metatarsal shaft.
- Score the bone at this junction with a sharp osteotome or saw blade.
- Using a power saw with a 9-mm or 10-mm blade, begin resecting the eminence at the dorsal lip of the parasagittal groove.
- Direct the blade proximally, plantarward, and slightly medially toward the scored bone. This trajectory minimizes the risk of inadvertently splitting the metatarsal shaft.
- Pitfall Avoidance: If using a narrow blade (e.g., 4 mm), ensure you do not scoop out cancellous bone from the metatarsal head, as this will decrease the surface contact area for the osteotomy and delay union.
5. The V-Shaped Osteotomy
- Apex Placement: The apex of the osteotomy should be located in the center of the metatarsal head, approximately 3 to 4 mm proximal to the medial edge of the articular cartilage.
- Dorsal Arm: Using a 9-mm-wide saw blade, begin the dorsal arm of the osteotomy near the subchondral bone. Angle the blade dorsally approximately 30 degrees from the longitudinal axis of the metatarsal.
- Plantar Arm: Angle the plantar arm 30 degrees plantarward from the longitudinal axis.
- Geometry: The angle between the two limbs should be 60 to 70 degrees. This specific geometry maximizes metaphyseal cancellous bone contact while maintaining inherent stability upon displacement. An angle less than 50 degrees places the proximal ends of the cuts into the cortical bone of the diaphyseal neck, delaying healing. An angle greater than 70 degrees severely compromises stability.
- Execution: Ensure the saw blade remains perfectly perpendicular to the medial border of the metatarsal. Avoid diverging or converging the blade during the second cut, as non-parallel cuts will lock the fragments and prevent smooth lateral translation.
- Do not overpenetrate the lateral cortex excessively, as this endangers the lateral soft tissues and the vascular supply.
6. Lateral Shift of the Capital Fragment
- Stabilize the proximal metatarsal shaft manually or with a towel clip.
- Apply direct thumb pressure to the capital fragment to shift it laterally.
- The displacement should typically be 4 to 5 mm, and strictly no more than 40% to 50% of the total width of the metatarsal head. Shifting beyond 5 to 6 mm results in critical loss of bone apposition and risks catastrophic instability or nonunion.
- Warning: Never use an instrument to lever the osteotomy open to facilitate displacement, as this crushes the delicate cancellous bone and renders the osteotomy highly unstable.
7. Fixation of the Osteotomy
While the classic chevron osteotomy is inherently stable, modern orthopedic practice heavily favors internal fixation to prevent displacement, allow for earlier mobilization, and maintain precise alignment.
* Insert one or two smooth Kirschner wires (K-wires), a 2.5 mm or 3.0 mm headless compression screw, or a biodegradable pin across the osteotomy site.
* If using a screw, direct it from dorsal-proximal to plantar-distal, ensuring the threads fully bypass the osteotomy line to achieve compression without penetrating the articular surface.
8. Removal of the Medial Metatarsal Projection
- Following lateral displacement, a sharp medial projection of the proximal metatarsal shaft will remain prominent.
- Shape this projection to match the new contour of the metatarsal neck. Begin a saw cut dorsomedially and direct it medially and proximally, parallel to the medial border of the foot.
- Use a small rongeur (taking small bites with the beveled side) or a rasp to meticulously smooth the medial surface, preventing postoperative bursa formation or skin irritation.
9. Medial Capsulorrhaphy and Soft Tissue Balancing
- Bring the hallux into approximately 5 degrees of valgus and inspect the osteotomy stability.
- If the HVA was 30 degrees or more preoperatively, a transarticular lateral release of the adductor hallucis tendon is highly recommended prior to capsular closure.
- Perform the capsulorrhaphy to hold the hallux in 5 to 10 degrees of valgus.
- Pants-Over-Vest Technique: This is the preferred method due to its superior biomechanical strength. The plantar flap is pulled dorsally over the dorsal flap. This specific vector not only tightens the medial capsule but also assists in derotating the hallux and repositioning the sesamoid apparatus under the metatarsal head.
- Alternatively, excising an elliptical portion of the redundant dorsal capsule and closing it side-to-side is acceptable.
POSTOPERATIVE CARE AND REHABILITATION
Meticulous postoperative care is essential to maintain the correction and ensure osseous union.
- Immediate Post-Op: A bulky, compressive soft dressing is applied in the operating room to hold the toe in the corrected alignment and control edema.
- Days 1-3: Elevation is strictly enforced.
- Day 3 to Week 6: The bulky dressing is removed. A smaller, sterile dressing is applied, and the patient is placed in a short-leg walking cast or a rigid postoperative shoe with dorsal and plantar toe plates.
- Weight Bearing: Touch-down to heel-weight bearing is permitted with crutches. Full weight-bearing on the forefoot is restricted until radiographic evidence of bridging trabecular bone is observed, typically between 6 to 8 weeks.
- Physical Therapy: Once clinical and radiographic union is achieved, aggressive active and passive range-of-motion exercises for the first MTP joint are initiated to prevent arthrofibrosis.
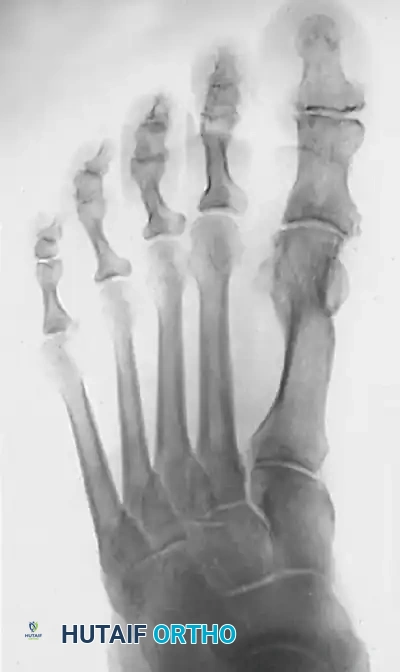
Figure 3: Standing AP radiograph 1 year postoperatively. The patient underwent a chevron osteotomy, release of the adductor hallucis, an Akin osteotomy of the proximal phalanx, and correction of the second hammer toe. Note the excellent consolidation of the osteotomy, restoration of the IMA, and congruent first MTP joint.
COMPLICATIONS AND PITFALLS
While highly successful, the distal chevron osteotomy carries specific risks that the surgeon must actively mitigate:
1. Avascular Necrosis (AVN): The most feared complication. Prevented by preserving the lateral capsular attachments and avoiding excessive stripping of the metatarsal neck.
2. Undercorrection / Recurrence: Often due to poor patient selection (IMA > 15°), inadequate lateral translation, or failure to perform an adequate lateral soft tissue release.
3. Overcorrection (Hallux Varus): Results from excessive resection of the medial eminence (violating the sagittal sulcus), over-tightening of the medial capsule, or aggressive complete release of the lateral collateral ligament.
4. Malunion / Dorsal Elevation: If the osteotomy is not properly fixated, the capital fragment may displace dorsally under the load of weight-bearing, leading to transfer metatarsalgia beneath the second metatarsal head.
5. Intra-articular Fracture: Caused by placing the apex of the V-cut too far distally or failing to use a drill hole to dissipate stress at the apex.
By adhering to strict biomechanical principles, respecting the delicate vascular anatomy, and executing precise osseous cuts, the orthopedic surgeon can utilize the distal chevron metatarsal osteotomy to achieve reproducible, excellent, and long-lasting functional outcomes for patients with hallux valgus.
You Might Also Like
