Advanced Operative Orthopaedics: Hip Instability, Tibial Realignment, and Sternoclavicular Reconstruction
Key Takeaway
The evolution of advanced imaging and arthroscopy has revolutionized the management of joint instability. This comprehensive guide details the diagnostic maneuvers for anterior hip instability, including the Ganz and dial tests. Furthermore, it outlines the precise surgical techniques and postoperative protocols for tibial osteotomies and complex shoulder reconstructions, emphasizing biomechanical restoration and strict complication avoidance in orthopedic practice.
Advanced Concepts in Hip Instability and Labral Pathology
With the rapid evolution of hip arthroscopy and high-resolution magnetic resonance (MR) arthrography, the orthopedic community’s understanding of hip joint kinematics, microinstability, and labral pathology has expanded exponentially. Historically underdiagnosed, hip instability is now recognized as a primary generator of chondral damage and early-onset osteoarthritis if left untreated. The diagnosis and treatment of hip instability require a meticulous understanding of the capsulolabral complex, osseous morphology, and dynamic biomechanics.
Pathoanatomy and Biomechanics of the Hip
The stability of the hip joint is dictated by a complex interplay between the bony architecture (acetabular coverage and femoral version), the static soft-tissue stabilizers (the labrum, capsule, and the robust iliofemoral, pubofemoral, and ischiofemoral ligaments), and the dynamic musculotendinous units. The acetabular labrum serves a critical biomechanical role by deepening the socket and creating a fluid "suction seal" that maintains synovial fluid pressurization, thereby protecting the articular cartilage from excessive contact stresses.
When this suction seal is compromised—either through an acute traumatic tear or chronic repetitive microtrauma—the hip is subjected to microinstability. This is frequently observed in athletes participating in sports requiring repetitive axial loading and rotational torque.
Clinical Evaluation and Diagnostic Maneuvers
The clinical presentation of hip instability is often insidious. Patients typically report a recurrent sensation of "giving way," deep groin pain, or mechanical popping. These symptoms are classically exacerbated by hip extension and external rotation, which places maximal tension on the anterior capsule and the iliofemoral ligament (the Y-ligament of Bigelow). Activities such as pivoting maneuvers during sports, kicking, or even the simple act of getting out of a car can provoke profound discomfort.
A comprehensive physical examination must begin with an assessment of generalized ligamentous laxity. The Beighton score should be calculated, and the uninvolved hip must be examined to establish the patient's baseline physiologic laxity.
Specific provocative tests are essential for isolating pathologic laxity and labral dysfunction:
- The Dial Test: Performed with the patient supine, the lower extremity is internally rotated and then released. Passive external rotation of more than 45 degrees—particularly if it lacks a firm endpoint or reproduces the patient's symptoms—is highly indicative of anterior capsular laxity and iliofemoral ligament incompetence.
- The Ganz Test (Anterior Apprehension Test): The patient is positioned supine with the pelvis stabilized. The examiner passively moves the hip into hyperextension and external rotation. The reproduction of anterior capsular pain or a subjective feeling of apprehension strongly suggests anterior instability.
- Axial Traction: Direct, manual axial traction applied to the lower extremity may produce apprehension or a palpable subluxation in the setting of gross capsular incompetence.
- Dynamic Labral Shear Test (FABER to FADIR/EADIR): Moving the hip dynamically from a position of Flexion, Abduction, and External Rotation (FABER) into Extension, Adduction, and Internal Rotation (EADIR) places shear stress across the anterosuperior labrum. This maneuver frequently re-creates the catching, clicking, or popping associated with labral tears and chondral delamination.
Clinical Pearl: Always differentiate between intra-articular pathology and extra-articular snapping hip syndromes (e.g., iliopsoas tendon snapping over the iliopectineal eminence). While extra-articular snapping is often visible and palpable, intra-articular popping associated with labral tears is typically felt deep within the groin and is highly correlated with the dynamic shear test.
Imaging and Surgical Indications
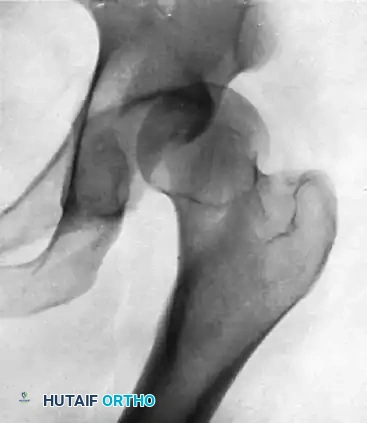
Standard weight-bearing anteroposterior (AP) pelvis, false-profile, and Dunn lateral radiographs are mandatory to assess for dysplasia (e.g., lateral center-edge angle < 25 degrees) or femoroacetabular impingement (FAI) morphology. However, MR arthrography remains the gold standard for evaluating the labrum and capsular integrity. Extravasation of contrast into the perilabral recess or through the capsule confirms the loss of the suction seal.
Surgical intervention—typically via hip arthroscopy—is indicated for symptomatic patients who have failed conservative management (core strengthening, pelvic floor physical therapy, and NSAIDs). The surgical objective is to restore the native biomechanics through anatomic labral repair and, critically, capsular plication to eliminate redundant capsular volume and restore the tension of the iliofemoral ligament.
Tibial Osteotomy and Tubercle Realignment Techniques
In the management of complex patellofemoral instability, torsional malalignment, or unicompartmental overload, tibial osteotomies—including High Tibial Osteotomy (HTO) and Tibial Tubercle Osteotomy (TTO)—are powerful joint-preserving procedures. Precise execution of the osteotomy and rigid internal fixation are paramount to achieving optimal biomechanical realignment and preventing nonunion.
Preoperative Planning and Biomechanical Goals
The primary goal of a derotational or tubercle realignment osteotomy is to normalize the extensor mechanism vector. A critical intraoperative metric is the tubercle-sulcus angle. The surgical objective is to achieve a tubercle-sulcus angle of exactly 0 degrees after the rotation and fixation of the distal tibia (or the tubercle fragment) are completed. This ensures that the patellar tendon vector is perfectly aligned with the trochlear groove during dynamic knee extension, thereby eliminating lateral patellar tracking and sheer forces.
Operative Technique and Fixation
Meticulous surgical technique is required to prevent iatrogenic fractures and ensure stable fixation.
- Osteotomy Execution: Following the planned osteotomy cuts (whether a medial opening wedge, lateral closing wedge, or an anteromedialization of the tubercle), the bone segments are mobilized.
- Fluoroscopic Verification: Once the proper position of the tibia is achieved, it must be rigorously verified with multi-planar fluoroscopy. The mechanical axis must be confirmed, and the tubercle-sulcus angle must be assessed dynamically.
- Staple and Screw Fixation: Fix the proximal and distal tibial sections utilizing one or two lateral compression staples. These must be placed strictly perpendicular to the tibial shaft and the osteotomy cut to maximize compression across the osteotomy site.
- Orthogonal Fixation: To prevent rotational displacement and enhance construct rigidity, place a third staple (or cortical lag screw) directed from anterior to posterior, perpendicular to the lateral staples. This orthogonal fixation strategy neutralizes multi-planar deforming forces.
- Closure: The surgical site is copiously irrigated, and the periosteal and fascial layers are meticulously closed with heavy absorbable sutures to prevent hematoma formation and optimize soft-tissue healing.
Surgical Warning: Over-medialization of the tibial tubercle can lead to catastrophic medial patellar subluxation and accelerated medial compartment arthrosis. Always respect the anatomic limits of transfer (typically 10-15 mm) and verify tracking intraoperatively before final fixation.
Postoperative Care and Rehabilitation Protocol
The postoperative rehabilitation following a tibial osteotomy is phased, protecting the bone healing while preventing arthrofibrosis.
- Phase I: Protection (Weeks 0-4): A postoperative locked hinged brace is applied immediately in the operating room with the knee locked in 20 degrees of flexion to minimize tension on the extensor mechanism. Crutches are mandatory, with the patient restricted to toe-touch weight bearing (TTWB) for 4 to 6 weeks, or until postoperative swelling significantly subsides. Straight-leg raises, isometric quadriceps contractions, and neuromuscular electrical stimulation (NMES) are initiated on postoperative day one to prevent profound quadriceps atrophy.
- Phase II: Early Range of Motion (Weeks 2-6): Passive range-of-motion (PROM) exercises are introduced in the second postoperative week. Active extension is strictly delayed until the fourth week to protect the osteotomy fixation. Flexion is increased incrementally each week as tolerated by the patient and the soft tissues. Aquatic therapy exercises are highly beneficial and are begun in the third week once the incisions are fully healed.
- Phase III: Intermediate Rehabilitation (Weeks 6-12): Stationary cycling exercises are initiated as soon as the knee has obtained 110 degrees of flexion. Weight-bearing is progressively advanced based on radiographic evidence of early callus formation.
- Phase IV: Advanced Strengthening and Return to Play (Months 3-6): Unrestricted closed kinetic chain (CKC) exercises (e.g., leg presses, squats) are begun by 12 weeks. Running, plyometrics, and a return to full athletic activities are usually permitted by 6 months, contingent upon symmetric quadriceps strength and radiographic union. A soft lateral-buttress brace is highly recommended during sports activities for the first year after surgery to provide proprioceptive feedback and dynamic support.
Sternoclavicular Joint and Complex Shoulder Reconstruction
Instability of the sternoclavicular (SC) joint and complex posterior shoulder girdle represents one of the most challenging pathologies in orthopedic surgery. The SC joint is the sole true synovial articulation between the axial skeleton and the upper extremity. Because of its proximity to the mediastinum, surgical interventions in this region carry a risk of catastrophic, life-threatening complications.
Surgical Anatomy and Indications for Reconstruction
The SC joint is inherently unstable due to the incongruence of the medial clavicle and the sternal manubrium. Stability is almost entirely dependent on the surrounding ligamentous complex, primarily the anterior and posterior sternoclavicular ligaments, and the costoclavicular (rhomboid) ligament.
Posterior SC joint dislocations are orthopedic emergencies due to the risk of compression or laceration of the great vessels, trachea, and esophagus. While anterior dislocations are more common, they are often managed non-operatively unless they become chronically painful and functionally limiting. When reconstruction is indicated, it must be reinforced with robust local tissue repair or autograft reconstruction (e.g., figure-of-eight semitendinosus graft).
Surgical Warning: The posterior capsular tissue is the most critical stabilizer of the SC joint. During any reconstruction, meticulous repair and augmentation of the posterior capsule are mandatory to prevent recurrent posterior translation.
Operative Execution and Catastrophic Risk Mitigation
The surgical approach to the SC joint requires a profound respect for the underlying visceral anatomy.
- Multidisciplinary Approach: It is an absolute requirement to have a thoracic surgeon available (or on immediate standby) for the procedure. The potential complications associated with drilling, dissecting, or passing grafts near the brachiocephalic trunk and superior vena cava cannot be overstated.
- Hardware Selection: Historically, Kirschner wires (K-wires) and Steinmann pins were used to stabilize the SC and acromioclavicular (AC) joints. This practice is now universally condemned. Because of the high probability of pin migration—driven by the continuous respiratory and upper extremity motion—and the potentially severe, fatal complications of hardware migrating into the heart, aorta, or lungs, pins or wires should never be placed across the joint. Modern reconstructions rely exclusively on heavy non-absorbable sutures, tendon autografts, and specialized suspensory fixation buttons.
Postoperative Care and Functional Recovery
The rehabilitation following a complex SC joint or shoulder girdle reconstruction requires strict adherence to immobilization protocols to allow for ligamentous healing.
- Immobilization Phase (Weeks 0-6): After reconstruction, the shoulder is strictly immobilized in a sling for 6 weeks. This prolonged immobilization is necessary because the upper extremity acts as a massive lever arm that can easily disrupt the delicate reconstruction at the sternum.
- Early Motion (Days 2 to Week 6): On the second postoperative day, the patient is allowed to perform gentle, gravity-assisted pendulum exercises to prevent glenohumeral adhesive capsulitis. However, the patient is strictly cautioned against any active flexion or abduction of the shoulder above 90 degrees, as this places immense rotational stress on the clavicle.
- Protection Phase (Months 1-3): All pushing, pulling, and heavy lifting are strictly avoided for a minimum of 3 months. The graft requires this time to undergo preliminary ligamentization and integration into the osseous tunnels.
- Strengthening and Return to Labor (Weeks 8-12+): Progressive isometric and isotonic strengthening exercises for the periscapular stabilizers and rotator cuff are started at 8 to 12 weeks. The patient is restricted from returning to strenuous manual labor, heavy overhead lifting, or contact sports for a minimum of 3 to 6 months, depending on the intraoperative stability achieved and the patient's clinical progression.
📚 Medical References
- joint instability, Acta Orthop Scand 59:168, 1988.
- Leith J, McConkey JP, Li D, et al: Valgus stress radiography in normal ankles, Foot Ankle Int 18:654, 1997.
- Lektrakul N, Chung CB, Lai YM, et al: Tarsal sinus: arthrographic, MR imaging, MR arthrographic, and pathologic fi ndings in cadavers and retrospective study data in patients with sinus tarsi syndrome, Radiology 219:802, 2001.
- Lindstrand A: New aspects in the diagnosis of lateral ankle sprains, Orthop Clin North Am 7:247, 1976.
- Liu SH, Baker CL: Comparison of lateral ankle ligamentous reconstruction procedures, Am J Sports Med 22:313, 1994.
- Liu SH, Jacobson KE: A new operation for chronic lateral ankle instability, J Bone Joint Surg 77B:55:1995.
- Loomer R, Fisher C, Lloyd-Smith R, et al: Osteochondral lesions of the talus, Am J Sports Med 21:13, 1993.
- Lynch SA, Renstrom PA: Treatment of acute lateral ankle ligament rupture in the athlete: conservative versus surgical treatment, Sports Med 27:61, 1999.
- Maiotti M, Massoni C, Tarantino U: The use of arthroscopic thermal shrinkage to treat chronic lateral ankle instability in young athletes, Arthroscopy 21:751, 2005.
- Marder RA: Current methods for evaluation of
You Might Also Like