Débridement & Glenoidplasty: Treating Degenerative Joint Disease
Key Takeaway
Your ultimate guide to Débridement & Glenoidplasty: Treating Degenerative Joint Disease starts here. Arthroscopic débridement and glenoidplasty are surgical options for shoulder degenerative joint disease when conservative methods fail and joint replacement is not desired. This approach aims to provide symptomatic relief, not reverse osteoarthritis, by removing loose bodies, resecting osteophytes, and addressing other coexisting pathologies. It is considered for patients with early to severe arthritis.
Introduction and Epidemiology
Osteoarthritis (OA) of the glenohumeral joint is a progressive, degenerative disorder of synovial joints characterized by the focal loss of articular cartilage, with concomitant reactive changes in the subchondral and marginal bone, synovium, and para-articular soft tissues. Patients presenting with degenerative joint disease (DJD) of the shoulder frequently exhibit a complex constellation of coexisting intra-articular and extra-articular pathology. This typically includes chronic bursitis, hypertrophic synovitis, intra-articular loose bodies, degenerative labral tears, peripheral osteophyte formation, and varying grades of articular cartilage defects.
While total shoulder arthroplasty (TSA) remains the gold standard for end-stage glenohumeral osteoarthritis in older, lower-demand populations, a significant therapeutic dilemma exists for young, active, or high-demand patients. Individuals under the age of 55, heavy laborers, and elite athletes who subject their upper extremities to high axial loads or repetitive impact are generally considered poor candidates for conventional arthroplasty due to the high risks of premature component wear, aseptic loosening, and the necessity for complex revision surgeries.
For this specific demographic, joint-preserving techniques such as comprehensive arthroscopic management (CAM)—which encompasses arthroscopic débridement, capsular release, and glenoidplasty—have emerged as highly valuable interventions. Arthroscopic débridement serves as a viable, less invasive treatment option when conservative modalities (e.g., physical therapy, nonsteroidal anti-inflammatory drugs, intra-articular corticosteroid or biologic injections) have failed, and when the patient wishes to delay arthroplasty. Historically, optimal candidates for arthroscopic joint preservation are those with early-stage osteoarthritis who maintain a concentric glenohumeral articulation and possess a visible, preserved joint space on an axillary lateral radiograph. It is paramount that the surgeon sets appropriate preoperative expectations; the primary objective of arthroscopic débridement and glenoidplasty is to provide a durable period of symptomatic relief and functional improvement, rather than to reverse or permanently halt the natural progression of the degenerative joint disease.
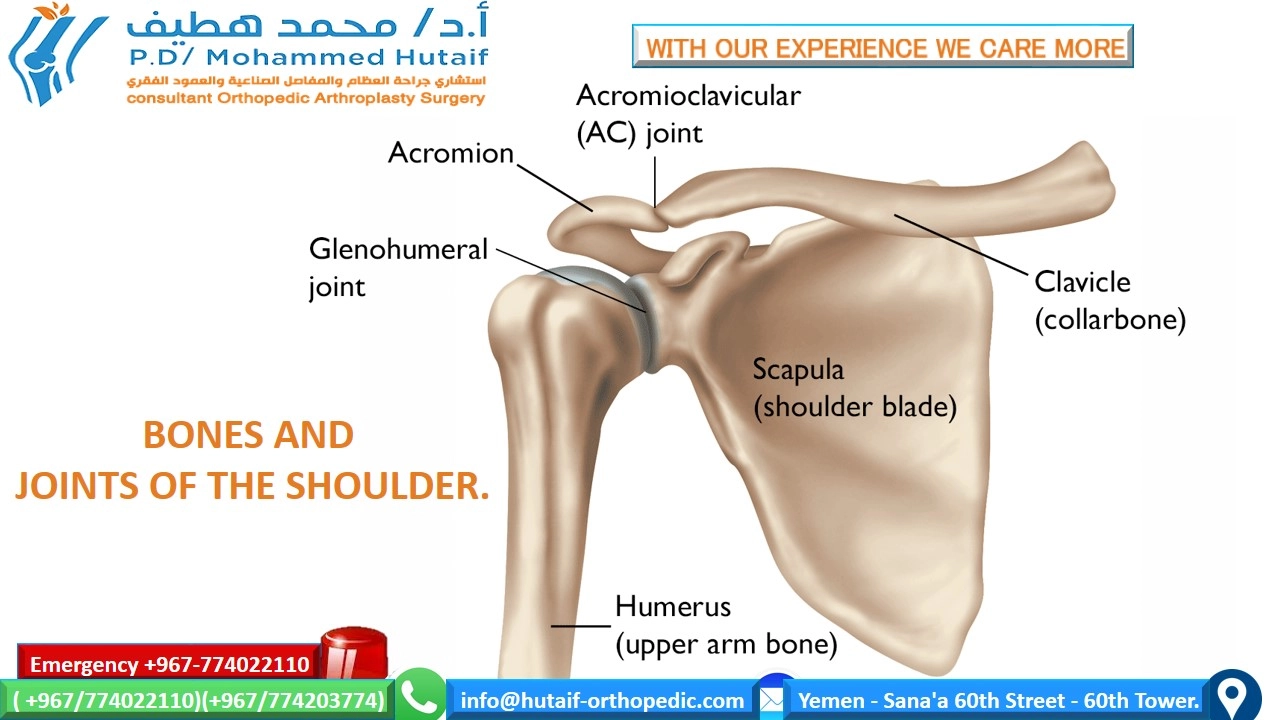
Surgical Anatomy and Biomechanics
A profound understanding of glenohumeral osteology, capsuloligamentous anatomy, and joint biomechanics is essential for executing safe and effective arthroscopic joint preservation.
Osteology and Articular Geometry
The normal proximal humeral anatomy is characterized by a head-shaft angle of approximately 130 degrees and an average retroversion of 30 degrees relative to the epicondylar axis of the distal humerus. The articular surface area of the humeral head is significantly larger than the corresponding articular surface of the glenoid, a mismatch that permits the shoulder's characteristically large, global range of motion at the expense of inherent bony stability.
Glenoid version, defined as the angle formed between the center of the glenoid articular surface and the longitudinal axis of the scapular body, averages approximately 3 degrees of retroversion. This orientation is critical for maintaining dynamic stability. The glenoid fossa itself provides a remarkably shallow socket.

The Glenoid Labrum
The native bony glenoid is deepened and stabilized by the glenoid labrum, a wedge-shaped, fibrocartilaginous structure that circumferentially surrounds the periphery of the glenoid rim. The labrum effectively increases the depth of the glenohumeral concavity by 50%, providing an average depth of 9 mm in the superoinferior plane and 5 mm in the anteroposterior plane. This deepening is critical for the "concavity compression" mechanism, wherein the rotator cuff musculature compresses the humeral head into the glenoid socket to maintain dynamic stability during motion. In the setting of DJD, the labrum frequently undergoes degenerative tearing, fraying, and calcification, compromising its stabilizing function and acting as a mechanical irritant.
Capsuloligamentous Structures
The capsuloligamentous complex provides the primary static stabilization for the glenohumeral joint. Within the broader joint capsule exist three distinct, biomechanically significant thickenings:
1. Superior Glenohumeral Ligament (SGHL): Restrains inferior translation at 0 degrees of abduction.
2. Middle Glenohumeral Ligament (MGHL): Restrains anterior translation at 45 degrees of abduction.
3. Inferior Glenohumeral Ligament (IGHL) Complex: Composed of an anterior band, a posterior band, and an axillary pouch. It is the primary restraint to anterior, posterior, and inferior translation at 90 degrees of abduction.

In the osteoarthritic shoulder, these capsular structures frequently become fibrotic, thickened, and contracted, leading to the profound loss of external and internal rotation characteristic of glenohumeral DJD.
Pathogenesis and Pathoanatomy
Osteoarthritis is broadly classified as primary (idiopathic) or secondary (arising from a predisposing condition such as trauma, instability, avascular necrosis, or inflammatory arthropathy). The pathoanatomy of glenohumeral OA involves a predictable cascade of structural changes.

As articular cartilage degrades, the joint experiences altered contact mechanics. This leads to the formation of marginal osteophytes, most notably the large inferior humeral osteophyte (often termed a "goat's beard") and posterior glenoid osteophytes. These osteophytes physically impinge on surrounding soft tissues, restrict range of motion, and can cause extrinsic compression of the axillary nerve within the quadrangular space.
Indications and Contraindications
Patient selection is the single most critical determinant of success in arthroscopic management of shoulder DJD. The ideal candidate is a physiologically young, high-demand patient with intractable pain, mechanical symptoms (catching/locking), and stiffness, who maintains a concentric joint space.
Summary of Indications and Contraindications
| Parameter | Operative Indications (Arthroscopic CAM) | Contraindications to Arthroscopy (Favor Arthroplasty or Non-Op) |
|---|---|---|
| Patient Age/Demand | Young (< 55 years), heavy laborers, elite athletes | Elderly (> 65 years), low physical demand |
| Joint Morphology | Concentric joint, early to moderate OA (Walch A1, early B1) | Bone-on-bone articulation, severe posterior wear (Walch B2/B3, C) |
| Radiographic Findings | Visible joint space on axillary lateral, loose bodies, focal osteophytes | Complete obliteration of joint space, severe humeral head flattening |
| Clinical Presentation | Mechanical symptoms, pain out of proportion to radiographic OA, refractory stiffness | Inflammatory arthropathy, neuropathic joint (Charcot), active infection |
| Rotator Cuff Status | Intact or repairable rotator cuff | Massive, irreparable rotator cuff tear (favor Reverse TSA) |
Pre Operative Planning and Patient Positioning
Thorough preoperative evaluation dictates the specific sequence of the arthroscopic intervention.
Clinical Evaluation and Imaging
Physical examination must meticulously document active and passive range of motion, noting specific deficits in external rotation (indicative of anterior capsular contracture and coracohumeral ligament thickening) and internal rotation (indicative of posterior capsular contracture). Posterior or lateral shoulder pain radiating down the arm may suggest axillary nerve compression secondary to inferior osteophytosis.

Standard radiographic series include a true anteroposterior (Grashey) view, an axillary lateral view, and a scapular Y view. The axillary view is paramount for assessing joint concentricity and estimating glenoid version and wear patterns (Walch classification). Advanced imaging with Magnetic Resonance Imaging (MRI) or MR Arthrography is highly recommended to evaluate the integrity of the rotator cuff, quantify articular cartilage loss, identify subchondral cysts, and assess for axillary nerve encroachment by inferior humeral osteophytes. Computed Tomography (CT) without contrast is an excellent adjunct for precise 3D mapping of complex osteophytes prior to glenoidplasty.
Patient Positioning and Anesthesia
Arthroscopic shoulder procedures for DJD can be performed in either the lateral decubitus or the beach chair position, largely dependent on surgeon preference and training. Regional anesthesia (interscalene nerve block) combined with general anesthesia is standard to ensure profound muscle relaxation and postoperative pain control.

Lateral Decubitus Position:
* Provides excellent visualization of the glenohumeral joint due to longitudinal traction.
* Facilitates access to the inferior capsule and axillary recess, which is advantageous for inferior capsular release and axillary nerve decompression.
* Requires careful padding of all bony prominences and strict adherence to traction weight limits (typically 10-15 lbs) to prevent neurapraxia.
Beach Chair Position:
* Allows the arm to be manipulated freely through a full range of motion, facilitating dynamic assessment of impingement and osteophyte clearance.
* Provides a more anatomic orientation for subacromial work and biceps tenodesis.
* Requires meticulous attention to cerebral perfusion pressure to mitigate the risk of cerebral hypoperfusion events.
Detailed Surgical Approach and Technique
The comprehensive arthroscopic management (CAM) of shoulder DJD is not a single procedure, but a highly customizable menu of interventions. There are six primary surgical options; the selection depends on the severity of the pathology and the specific anatomical pain generators identified preoperatively and intraoperatively.
Portal Placement and Diagnostic Arthroscopy
Standard posterior, anterior, and lateral portals are established. An accessory posterolateral or posteroinferior portal may be required for optimal trajectory during axillary nerve decompression.

A thorough diagnostic arthroscopy is performed systematically, evaluating the biceps tendon, labrum, articular surfaces, capsular recesses, and rotator cuff.
Glenohumeral Joint Débridement and Chondroplasty
The initial phase involves the meticulous removal of all intra-articular loose bodies, which frequently aggregate in the axillary pouch and subscapularis recess.

Hypertrophic, inflamed synovium is resected using a motorized shaver and radiofrequency ablation wand to reduce cytokine-mediated pain and improve visualization. Unstable, delaminated flaps of articular cartilage are carefully débrided to stable, vertical margins (chondroplasty). Care must be taken to avoid violating the subchondral bone plate, which can incite further inflammatory cascades, unless a specific microfracture technique is planned for focal grade IV defects. Degenerative, unstable portions of the labrum that catch within the articulation are excised, preserving as much stable labral tissue as possible to maintain the concavity compression effect.
Capsular Release
To address the profound stiffness associated with shoulder OA, a sequential, 270-degree to 360-degree capsular release is often necessary.

The release typically begins at the rotator interval, resecting the thickened coracohumeral ligament to restore external rotation with the arm at the side. Using electrocautery, the anterior capsule and superior glenohumeral ligament (SGHL) are released just lateral to the glenoid rim to protect the subscapularis. The release proceeds inferiorly through the middle glenohumeral ligament (MGHL) and the anterior band of the IGHL. When releasing the inferior capsule (axillary pouch), the surgeon must remain meticulously close to the glenoid rim (within 1-2 mm) to avoid iatrogenic injury to the axillary nerve, which lies in close proximity (average 12-14 mm) to the inferior glenoid. The release is then carried posteriorly up to the level of the biceps anchor to restore internal rotation.
Subacromial Decompression
Although the primary pathology is intra-articular, secondary subacromial impingement is common due to altered glenohumeral kinematics.

The arthroscope is redirected into the subacromial space. A thorough bursectomy is performed. If a type III hooked acromion or significant subacromial spurring is present and contributing to bursal-sided cuff fraying, a judicious acromioplasty is executed using a high-speed burr, flattening the undersurface of the anterior acromion and releasing the coracoacromial ligament.
Biceps Tenodesis
The long head of the biceps tendon is a notorious pain generator in the osteoarthritic shoulder. It is frequently flattened, frayed, or subluxated due to concomitant pulley lesions.

Simple tenotomy may be acceptable in older, low-demand patients, but in the younger, active demographic targeted for this procedure, an arthroscopic or subpectoral biceps tenodesis is highly recommended to maintain supination strength and prevent aesthetic deformity (Popeye sign). The tendon is released from its superior labral anchor, and the stump is stabilized via suture anchors or interference screws in the bicipital groove or subpectoral space.
Glenoidplasty and Osteophyte Resection
Glenoidplasty involves the strategic recontouring of the glenoid architecture and the resection of mechanical blocks to motion.

Peripheral marginal osteophytes effectively deepen the glenoid socket pathologically, creating a "pincer" effect that limits rotation and elevation. Using a shielded arthroscopic burr, these osteophytes are resected flush with the native articular margin. Posterior glenoid osteophytes are common and must be removed to restore smooth articulation. In cases of early eccentric wear (e.g., transition toward a B2 biconcave glenoid), the central ridge between the paleoglenoid and neoglenoid can be gently smoothed to reduce mechanical catching, though aggressive reaming should be avoided to preserve subchondral bone stock for future arthroplasty.
Axillary Nerve Decompression
Recent advancements by Millett et al. have highlighted the role of the inferior humeral osteophyte in compressing the axillary nerve within the quadrangular space.

If the patient exhibits posterior/lateral shoulder pain, or if MRI or intraoperative assessment reveals axillary nerve encroachment, a targeted decompression is indicated. Viewing from the anterior-superior portal, an accessory posteroinferior portal is established. The axillary nerve is carefully identified as it traverses inferior to the joint capsule. A blunt switching stick or specialized retractor is placed to gently retract and protect the nerve inferiorly. An arthroscopic burr is then introduced to resect the inferior humeral "goat's beard" osteophyte until a minimum of 5 mm of clearance is achieved between the nerve and the bony contour throughout a full range of motion.
Complications and Management
While generally safe, the comprehensive arthroscopic management of DJD carries specific risks, particularly given the extensive capsular releases and bone resections involved.

Table of Complications and Salvage Strategies
| Complication | Estimated Incidence | Etiology / Risk Factors | Management and Salvage Strategies |
|---|---|---|---|
| Recurrent Pain / OA Progression | 15-30% (at 5 years) | Natural history of DJD, inadequate osteophyte resection, advanced initial Walch grade | Non-operative modalities; eventual conversion to Total or Reverse Shoulder Arthroplasty. |
| Axillary Nerve Injury | < 1% | Straying >2mm from inferior glenoid rim during capsular release; thermal injury; direct burr trauma | Prevention via meticulous technique and protective retractors. Observation for neuropraxia; nerve exploration/grafting if neurotmesis suspected. |
| Postoperative Stiffness | 5-10% | Inadequate initial release, poor rehabilitation compliance, excessive postoperative immobilization | Aggressive physical therapy, intra-articular corticosteroids. Manipulation under anesthesia or revision arthroscopic lysis of adhesions. |
| Chondrolysis | Rare | Use of intra-articular pain pumps (bupivacaine), excessive thermal energy (radiofrequency) | Avoid intra-articular pain pumps. Salvage relies on arthroplasty once bone stock allows. |
| Fluid Extravasation | 1-3% | Prolonged surgical time, high pump pressures, extensive capsulotomy | Monitor airway and compartment pressures. Usually resolves spontaneously within 12-24 hours. Diuretics if severe. |
Post Operative Rehabilitation Protocols
The success of a capsular release and glenoidplasty relies heavily on immediate, structured postoperative rehabilitation to prevent the recurrence of adhesive capsulitis and maintain the surgically achieved range of motion.

Phase I: Immediate Motion (Weeks 0-2)
* Immobilization: Sling usage is strictly minimized to comfort only. Patients are encouraged to discontinue the sling within the first 48-72 hours.
* Range of Motion: Immediate initiation of passive range of motion (PROM) and active-assisted range of motion (AAROM) in all planes. Forward elevation, external rotation at the side, and internal rotation are prioritized to preserve the capsular release.
* Analgesia: Aggressive multimodal pain management is critical to allow patient compliance with early motion.
Phase II: Active Motion and Early Strengthening (Weeks 2-6)
* Range of Motion: Transition to full active range of motion (AROM). Terminal stretching is instituted to maintain capsular compliance.
* Strengthening: Initiation of submaximal isometric exercises for the rotator cuff and periscapular stabilizers.
* Precautions: If a biceps tenodesis was performed, resisted elbow flexion and supination are restricted for the first 4-6 weeks to protect the repair.
Phase III: Advanced Strengthening (Weeks 6-12)
* Strengthening: Progression to isotonic strengthening, focusing on the dynamic stabilizers of the glenohumeral joint. Scapulothoracic rhythm must be optimized to prevent secondary impingement.
* Functional Training: Introduction of closed kinetic chain exercises and proprioceptive training.
Phase IV: Return to Activity (Months 3-6)
* Gradual return to heavy lifting, manual labor, or sports-specific activities. Return to play is dictated by the restoration of symmetric strength and pain-free full range of motion.
Summary of Key Literature and Guidelines
The literature supporting comprehensive arthroscopic management (CAM) for glenohumeral osteoarthritis demonstrates its efficacy as a bridging procedure for young, active patients.
Millett et al. have published extensively on the CAM procedure, reporting significant improvements in American Shoulder and Elbow Surgeons (ASES) scores and visual analog scale (
Clinical & Radiographic Imaging














You Might Also Like