Tibial Plateau Fractures: Comprehensive Guide to Epidemiology, Classification & Biomechanics
Key Takeaway
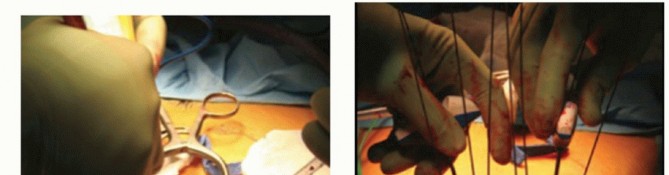
Tibial plateau fractures are complex intra-articular injuries of the proximal tibia, critical for knee function. They arise from high- or low-energy trauma, often involving associated soft tissue damage. Classification systems like Schatzker and AO/OTA categorize patterns to guide treatment, focusing on restoring articular congruity and stability to prevent osteoarthritis.
Plateau Fracture Tibial: Your Guide to Symptoms & Treatment
Introduction & Epidemiology
Tibial plateau fractures represent a spectrum of complex intra-articular injuries involving the proximal tibia, crucial for knee joint function and stability. These fractures typically result from high-energy mechanisms in younger individuals, such as motor vehicle collisions or falls from height, or low-energy mechanisms in osteoporotic elderly patients. The hallmark of these injuries is disruption of the articular surface, often compounded by metaphyseal comminution and associated soft tissue injuries, including meniscal tears, ligamentous laxity (cruciate and collateral ligaments), and neurovascular compromise.
The incidence of tibial plateau fractures is estimated to be approximately 10-15 per 100,000 person-years, with a bimodal distribution. Younger, active individuals tend to sustain high-energy fractures, often Schatzker types V and VI, while older patients with compromised bone quality typically present with Schatzker types I and II from lower-energy mechanisms. Associated injuries are common, with meniscal tears reported in 50-70% of cases, ligamentous injuries in 20-40%, and neurovascular compromise in up to 10%. Compartment syndrome, particularly in high-energy bicondylar fractures, is a critical concern, necessitating prompt recognition and management.
Accurate classification is paramount for guiding treatment. The Schatzker classification, though limited by its two-dimensional nature on plain radiographs, remains widely utilized due to its clinical applicability and correlation with prognosis. It categorizes fractures from I to VI based on fracture pattern, displacement, and comminution:
*
Schatzker Type I:
Isolated lateral tibial plateau wedge fracture.
*
Schatzker Type II:
Lateral tibial plateau split depression fracture.
*
Schatzker Type III:
Lateral tibial plateau pure depression fracture.
*
Schatzker Type IV:
Medial tibial plateau fracture (split or depressed).
*
Schatzker Type V:
Bicondylar fracture with intact diaphyseal-metaphyseal dissociation.
*
Schatzker Type VI:
Bicondylar fracture with metaphyseal-diaphyseal dissociation.
The AO/OTA classification offers a more detailed, alphanumeric system that accounts for articular involvement (partial or complete) and metaphyseal-diaphyseal extension. While more comprehensive, its complexity often leads to Schatzker remaining the primary descriptive system in clinical practice. The overarching goal of treatment, whether operative or non-operative, is the restoration of articular congruity, mechanical axis alignment, and knee stability, thereby minimizing the long-term risk of post-traumatic osteoarthritis and chronic pain.
Surgical Anatomy & Biomechanics
A thorough understanding of the surgical anatomy and biomechanics of the proximal tibia and surrounding knee joint is fundamental for successful management of tibial plateau fractures.
The proximal tibia comprises the medial and lateral tibial condyles, separated by the intercondylar eminence. The articular surface, covered by hyaline cartilage, includes the medial and lateral tibial plateaus, which articulate with the corresponding femoral condyles. The medial plateau is larger, concave, and typically bears more weight, while the lateral plateau is smaller, convex, and more prone to depression fractures due to its inherent weaker bony support. The subchondral bone, underlying the articular cartilage, is dense, providing crucial support. The metaphyseal region inferior to the plateau flares outwards, forming the bony buttress for the articular surface.
Key soft tissue structures contributing to knee stability and often involved in these injuries include:
*
Menisci:
The medial and lateral menisci are C-shaped fibrocartilaginous structures that deepen the articular fossae, distribute load, and provide secondary stability. They are frequently torn or entrapped within fracture fragments, particularly in split depression patterns.
*
Collateral Ligaments:
The medial collateral ligament (MCL) resists valgus stress and is often injured in lateral plateau fractures. The lateral collateral ligament (LCL) resists varus stress, and posterolateral corner injuries are critical to assess, especially in medial plateau fractures.
*
Cruciate Ligaments:
The anterior cruciate ligament (ACL) and posterior cruciate ligament (PCL) are intra-articular stabilizers. Their integrity is crucial for sagittal stability and often assessed post-reduction.
*
Neurovascular Structures:
The popliteal artery and vein are situated posteriorly, making them vulnerable in high-energy or posteriorly displaced fractures. The common peroneal nerve courses around the fibular neck, making it susceptible to injury, particularly with lateral surgical approaches or external fixation pin placement.
Biomechanically, the knee joint is designed to transmit axial loads from the femur to the tibia, with the menisci playing a critical role in load distribution. Valgus and varus forces, often combined with axial compression, are the primary mechanisms of tibial plateau fractures.
*
Valgus Compression:
Typically leads to lateral tibial plateau fractures (Schatzker types I, II, III). The lateral femoral condyle acts as a wedge, driving into the weaker lateral plateau.
*
Varus Compression:
More commonly results in medial tibial plateau fractures (Schatzker type IV). These are less common but often associated with higher energy and worse prognosis due to the stronger medial column requiring greater force to fracture.
*
Axial Compression:
High-energy axial loads, often combined with valgus or varus forces, can lead to bicondylar fractures (Schatzker types V, VI) with significant comminution and metaphyseal-diaphyseal dissociation.
The integrity of the articular surface and the underlying metaphyseal bone is critical for load bearing. Articular depression creates incongruity, leading to stress concentrations and premature cartilage degeneration. Metaphyseal bone loss or comminution compromises the foundation for the articular surface, requiring structural support (e.g., bone grafting) to restore plateau height and alignment. Understanding these structural and mechanical principles guides surgical decision-making regarding reduction techniques, fixation constructs, and the need for bone augmentation.

Indications & Contraindications
The decision for operative versus non-operative management of tibial plateau fractures is multifaceted, balancing fracture characteristics, patient comorbidities, and surgeon expertise. The primary goals of operative intervention are anatomic restoration of the articular surface, stable fixation to allow early motion, and accurate mechanical axis alignment to prevent post-traumatic arthritis and chronic instability.
Indications for Operative Management
- Articular Step-off: Greater than 2-3 mm, as measured on CT scans. This threshold is critical for preventing accelerated cartilage wear and subsequent osteoarthritis.
- Condylar Widening: Greater than 5 mm (often 10 mm in some literature) of the metaphyseal bone, leading to instability and malalignment.
- Meniscal Entrapment: When a meniscus is incarcerated within the fracture site, preventing reduction or leading to persistent pain and mechanical symptoms.
- Neurovascular Compromise: Acute neurovascular injury requiring exploration and repair.
- Compartment Syndrome: Clinical diagnosis requiring emergent fasciotomy. While not directly treating the fracture, it's an emergent condition often associated with severe tibial plateau fractures that necessitates surgery.
- Open Fractures: Gustilo-Anderson types I-III require urgent debridement, irrigation, and stabilization.
- Associated Ligamentous Instability: When significant instability persists after fracture reduction, particularly involving multiple ligaments, leading to a grossly unstable knee.
- Bicondylar Fractures (Schatzker V, VI): These complex patterns almost universally require operative stabilization due to inherent instability and significant articular disruption.
- Medial Tibial Plateau Fractures (Schatzker IV): Often associated with higher energy and instability, frequently necessitating surgical intervention.
- Failure of Non-Operative Treatment: Progressive displacement or loss of reduction during conservative management.
Indications for Non-Operative Management
- Non-Displaced or Minimally Displaced Fractures: Articular step-off less than 2-3 mm and condylar widening less than 5 mm, often confirmed on CT.
- Stable Fractures: Fractures that demonstrate stability to varus/valgus stress testing under fluoroscopic guidance (if applicable) or on plain radiographs.
- Non-Articular Involvement: Certain extra-articular proximal tibia fractures (though technically not plateau fractures) or purely metaphyseal fractures without articular disruption.
- Severe Medical Comorbidities: Patients with significant comorbidities (e.g., severe cardiac, pulmonary, renal disease, coagulopathy) that preclude safe anesthesia and surgery. The risks of surgery must outweigh the potential benefits.
- Non-Ambulatory or Limited Demand Patients: Patients with limited functional demands where the potential benefits of surgical reconstruction may not justify the risks.
Contraindications for Operative Management
-
Absolute Contraindications:
- Active Infection: Cellulitis or osteomyelitis at the surgical site.
- Severe Systemic Instability: Patient medically unstable to tolerate anesthesia and surgery (e.g., acute MI, uncontrolled sepsis).
- Non-Viable Soft Tissues: Extremely poor soft tissue envelope (e.g., severe crush injury, degloving) where surgical wound closure and healing are impossible. This often necessitates external fixation with delayed definitive fixation or amputation.
-
Relative Contraindications:
- Extensive Comminution with Osteoporosis: Severe osteoporosis making stable fixation difficult to achieve and maintain.
- Extremely Poor Soft Tissue Condition: Significant swelling, fracture blisters, or impending skin necrosis. These often mandate temporization with external fixation until the soft tissue envelope improves ("fix and flail").
- Patient Non-Compliance: Unreliable patient who will not adhere to post-operative weight-bearing restrictions or rehabilitation protocols.
Operative vs. Non-Operative Indications
| Indication Feature | Operative Management (Usually) | Non-Operative Management (Usually) |
|---|---|---|
| Articular Step-off | ≥ 2-3 mm | < 2-3 mm |
| Condylar Widening | ≥ 5-10 mm | < 5 mm |
| Fracture Stability | Unstable (gross laxity, displacement under stress) | Stable (no significant displacement under stress) |
| Meniscal Entrapment | Present | Absent |
| Neurovascular Injury | Present (requiring repair/decompression) | Absent |
| Compartment Syndrome | Present (requiring fasciotomy) | Absent |
| Open Fracture | All Gustilo-Anderson types | Closed fractures only |
| Fracture Type | Bicondylar (Schatzker V, VI), Medial (Schatzker IV), high-energy | Non-displaced Schatzker I, II, III (low energy) |
| Soft Tissue | Optimal envelope, minimal swelling | Severe swelling, fracture blisters (may require temporization) |
| Patient Health | Medically stable, compliant | Severe comorbidities precluding surgery, non-ambulatory, non-compliant |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is the cornerstone of successful tibial plateau fracture management, minimizing intra-operative complications and optimizing outcomes.
Pre-Operative Planning Steps
-
Clinical Assessment:
- History: Mechanism of injury, associated pain, prior knee pathology.
- Physical Exam: Thorough neurovascular assessment (popliteal pulses, peroneal nerve function), soft tissue evaluation (swelling, fracture blisters, open wounds), assessment for compartment syndrome, and ligamentous stability testing (if pain allows and fracture is stable enough).
-
Imaging Review:
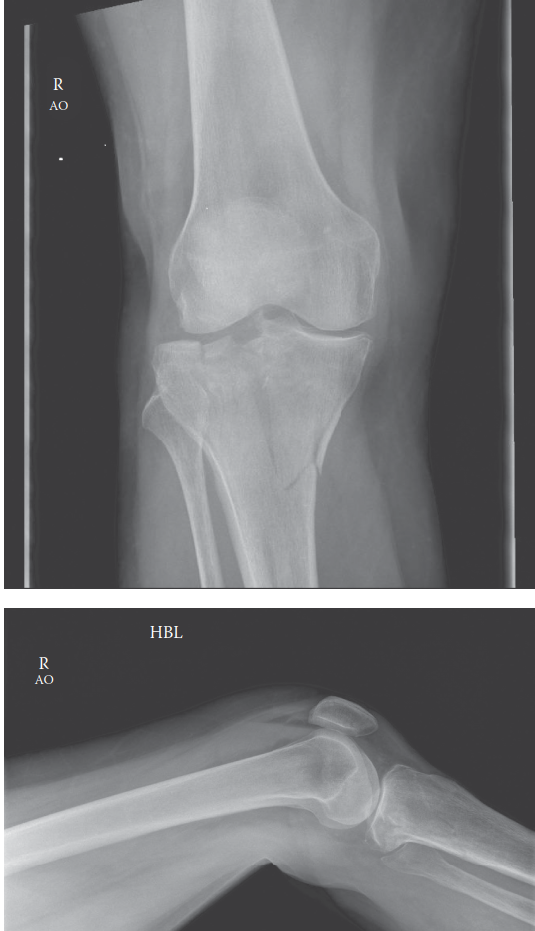
- Plain Radiographs: AP, lateral, and oblique views of the knee are initial imaging. Full-length leg films are crucial for assessing the mechanical axis.
-
Computed Tomography (CT) Scan:
Essential.
This is the definitive imaging modality for tibial plateau fractures. It provides detailed information on:
- Articular step-off and depression (accurate quantification).
- Extent of metaphyseal comminution and bone loss.
- Coronal and sagittal plane fracture lines.
- Posterior column involvement (critical for surgical approach).
- 3D reconstructions are invaluable for understanding fracture morphology and planning reduction.
- Magnetic Resonance Imaging (MRI): Indicated if significant meniscal, collateral ligament, or cruciate ligament injuries are suspected. This can alter the surgical plan significantly (e.g., meniscal repair, concomitant ligamentous reconstruction).
- CT Angiogram: If arterial injury is suspected (e.g., diminished pulses, expanding hematoma).
-
Classification & Surgical Strategy:
- Fracture Classification: Utilize Schatzker and AO/OTA to thoroughly characterize the fracture. Identify key fragments, areas of depression, and comminution.
-
Approach Selection:
Based on fracture pattern, determine the optimal surgical approach(es) to visualize, reduce, and fix all critical fragments. For example:
- Isolated lateral plateau: Anterolateral.
- Isolated medial plateau: Anteromedial.
- Bicondylar (Schatzker V, VI): Dual approaches (e.g., anterolateral and posteromedial, or direct lateral and direct medial), often staged.
- Posterior column involvement: Posteromedial, direct posterior.
- Implant Selection: Determine the necessary hardware (e.g., specific plates like lateral locking plates, medial buttress plates, posteromedial plates, small fragment plates, cannulated screws, rafting screws). Consider bone graft materials (autograft, allograft, synthetic) for metaphyseal defects.
- Contingency Planning: Plan for potential challenges (e.g., unachievable reduction, persistent instability, soft tissue issues).
-
Timing of Surgery:
- "Wrinkle Sign": Delay definitive internal fixation until the soft tissue swelling has subsided, typically indicated by the presence of skin wrinkles over the knee. This often means delaying surgery for 7-14 days.
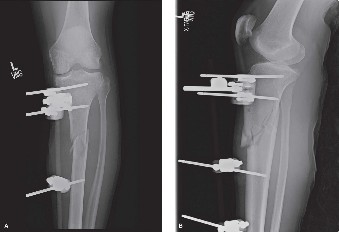
- Temporization: For unstable fractures with poor soft tissues, apply a temporary spanning external fixator across the knee to provide stability, perform ligamentotaxis, and allow soft tissue recovery. This is critical in high-energy injuries to prevent further soft tissue damage and reduce compartment syndrome risk.
- Emergent Surgery: Open fractures, compartment syndrome, or acute neurovascular compromise require immediate surgical intervention, irrespective of soft tissue status.
Patient Positioning
The goal of patient positioning is to allow unobstructed surgical access, facilitate radiographic imaging, and maintain patient safety.
-
Supine Position:
This is the most common position for the majority of tibial plateau fractures.
- Table: Utilize a radiolucent operating table that allows for easy C-arm access in both AP and lateral planes.
- Leg Prep: The entire affected limb, from hip to ankle, is prepped and draped to allow for manipulation and full visualization, as well as potential for distal extension of incisions or fibular head osteotomy if needed.
- Tourniquet: A pneumatic thigh tourniquet is almost always used to provide a bloodless field, typically inflated after exsanguination.
- Leg Holders/Pillows: A bump or bolster under the ipsilateral hip elevates it to prevent external rotation of the limb. A towel roll or small bolster under the distal femur or proximal tibia can help flex the knee slightly for improved access.
- C-arm Placement: Position the C-arm to allow for both AP and true lateral fluoroscopic views without repositioning the patient or the limb. This is crucial for real-time assessment of reduction and hardware placement.
- Consider a Distraction Tower: For complex cases, an ankle traction tower can be utilized to aid indirect reduction via ligamentotaxis, particularly for articular depression.
-
Lateral Decubitus Position:
- Indication: May be considered for specific posterior approaches (e.g., direct posterior approach for isolated posterior column fractures) to optimize exposure. However, the supine position with specific modifications (e.g., rolling the patient slightly, flexing the hip and knee) often suffices.
- Pillows/Rolls: Support the patient appropriately to maintain stability and prevent nerve compression.
- Well-padded: Ensure all bony prominences (heels, sacrum, contralateral limb) are well-padded to prevent pressure sores or nerve palsies.
Detailed Surgical Approach / Technique
The surgical technique for tibial plateau fractures is dictated by the specific fracture pattern, degree of articular depression, metaphyseal comminution, and associated soft tissue injuries. The overarching principles are:
1.
Anatomic Reduction:
Restore articular congruity and overall mechanical axis.
2.
Stable Internal Fixation:
Provide a construct robust enough to withstand early rehabilitation.
3.
Preservation of Soft Tissues:
Minimize iatrogenic damage to skin, muscle, and neurovascular structures.
General Principles
- Timing: As discussed, definitive fixation often occurs after the "wrinkle sign" appears.
- Antibiotics: Prophylactic antibiotics are administered.
- Tourniquet: Use of a thigh tourniquet is standard to achieve a bloodless field.
- Fluoroscopy: Essential for real-time assessment of reduction and hardware placement.
Step-by-Step Surgical Approach / Technique
1. Incision and Exposure
The chosen incision(s) should provide adequate visualization of the fracture while minimizing soft tissue stripping.
-
Anterolateral Approach (Common for Schatzker I, II, III, and lateral component of V, VI):
- Incision: Longitudinal incision centered over the lateral tibial plateau, slightly posterior to the Gerdy's tubercle. Extend proximally beyond the fracture and distally to allow plate placement.
- Internervous Plane: Dissect between the iliotibial band (ITB) anteriorly and the biceps femoris tendon posteriorly. The common peroneal nerve is found posteriorly, superficial to the biceps femoris, and must be carefully protected.
- Deep Dissection: Incise the ITB longitudinally or detach it from Gerdy's tubercle. Subperiosteal dissection anteriorly elevates the tibialis anterior and other anterior compartment muscles. Posteriorly, the lateral head of the gastrocnemius is retracted.
- Meniscal Preservation: Perform an arthrotomy, typically submeniscal (just inferior to the lateral meniscus) or via a longitudinal incision in the capsule/meniscotibial ligament, to visualize the articular surface. The lateral meniscus should be carefully assessed for tears and its attachment preserved or repaired.
- Visualization: Retract the meniscus superiorly to directly visualize the depressed articular fragments.
-

-
Anteromedial Approach (Common for Schatzker IV, and medial component of V, VI):
- Incision: Longitudinal incision over the medial tibial plateau, posterior to the saphenous nerve and vein.
- Internervous Plane: Dissect between the sartorius muscle (anteriorly) and the semitendinosus/gracilis tendons (posteriorly). The saphenous nerve and vein are anterior to the sartorius and must be protected.
- Deep Dissection: Detach the superficial MCL from the tibia or incise longitudinally posterior to its anterior fibers. The deep MCL can be incised carefully or elevated with a small cuff of bone.
- Arthrotomy: Submeniscal arthrotomy or through the meniscotibial ligament to visualize the medial articular surface. The medial meniscus needs careful evaluation.
-
Posteromedial Approach (For posterior column involvement, e.g., modified posteromedial by Lobenhoffer, or for bicondylar Schatzker VI):
- Incision: Longitudinal incision along the posteromedial border of the tibia.
- Internervous Plane: Between the posterior margin of the superficial MCL (anteriorly) and the medial head of the gastrocnemius (posteriorly). The popliteal neurovascular bundle is lateral to the gastrocnemius and must be protected.
- Deep Dissection: Elevate the pes anserinus tendons and the sartorius muscle anteriorly. Retract the medial head of the gastrocnemius posteriorly. Identify and protect the saphenous nerve and vein. The neurovascular bundle is deep in this plane.
- Visualization: This approach provides direct access to the posteromedial column and often allows for a relatively wide plate placement.
- Dual Incisions: For bicondylar fractures (Schatzker V, VI), often a combination of anterolateral and posteromedial incisions is used. Staged procedures (e.g., lateral first, then medial, or vice versa) can reduce soft tissue compromise.
2. Fracture Reduction
This is the most critical step, focusing on articular reconstruction.
- Indirect Reduction (Ligamentotaxis): For depressed articular fragments, apply longitudinal traction, often with an external fixator or traction tower. This helps restore overall length and width, bringing large fragments into alignment.
-
Direct Reduction:
- Articular Fragment Elevation: Use elevators (e.g., periosteal, Tamp, Hohmann retractors) to elevate depressed articular fragments from below (through a cortical window in the metaphysis) or from above (direct manipulation through the arthrotomy). K-wires can be used to temporarily hold fragments.
-
Metaphyseal Void Filling:
Once the articular surface is elevated, the underlying metaphyseal void must be filled to prevent re-collapse.
- Autograft: Iliac crest bone graft (cancellous or corticocancellous). Gold standard.
- Allograft: Cancellous chips or structural grafts.
- Bone Graft Substitutes: Calcium phosphate, calcium sulfate, demineralized bone matrix (DBM).
- Reduction of Main Fragments: Use reduction clamps (e.g., large fragment, Verbrugge, pointed reduction clamps), K-wires, and manual manipulation to restore the overall shape of the proximal tibia and the mechanical axis. Use fluoroscopy (AP and lateral views, often a 0° and 10° or 15° "knee-up" view for true lateral of the plateau) to confirm articular congruity and overall alignment.
- Meniscal Management: Assess meniscal integrity. If torn or unstable, perform repair or meniscectomy as indicated. Ensure no meniscal incarceration at the fracture site.
3. Internal Fixation
Choose a fixation construct that provides adequate stability for early motion while protecting soft tissues.
-
Plate Osteosynthesis:
- Lateral Locking Plates: For lateral column fractures (Schatzker I, II, III) and bicondylar patterns. These plates provide angular stable fixation, protecting the reduced articular fragments. Positioning the plate appropriately (e.g., slightly anterior or posterior to Gerdy's tubercle) is important.
- Medial Buttress Plates: For medial column fractures (Schatzker IV) and bicondylar patterns. These plates provide robust medial column support.
- Posterior Plates: For posteromedial or posterolateral fragments. Low-profile plates are often preferred.
- Rafting Screws: Small, cancellous, non-locked screws placed directly under the articular surface to "raft" or support the subchondral bone, preventing collapse. These are critical in depression fractures.
- Lag Screws: For large, reducible split fragments, lag screws provide interfragmentary compression.
- External Fixation (for definitive management): In select cases, particularly open fractures with significant contamination or comminution, a hybrid external fixator can be used for definitive fixation, preserving soft tissue integrity.
-
Hardware Placement:
- Ensure proper plate length and contouring.
- Place screws strategically to engage good bone stock, avoiding joint penetration. Use fluoroscopy for every screw to confirm length and position.
- In bicondylar fractures, ensure the lateral and medial plates do not interfere with each other or with potential screw placement from the opposing side. This often requires careful pre-operative templating.
- Fixation Sequence: Typically, large main fragments are reduced and temporarily fixed with K-wires. The articular surface is reconstructed first, followed by metaphyseal reduction and plate application.
4. Soft Tissue Repair and Closure
- Meniscal Repair: If a meniscal tear is amenable to repair, perform it at this stage.
- Ligamentous Repair: Repair any identified collateral ligament avulsions or significant tears. Cruciate ligament injuries are often addressed in a delayed fashion if symptomatic after fracture healing.
- Wound Irrigation: Thoroughly irrigate the surgical site to remove bone debris and blood.
- Drain Placement: Consider placing a negative pressure drain (e.g., Hemovac) in large wounds or if significant bleeding is anticipated, particularly in bicondylar fractures.
- Layered Closure: Close the deep fascia, subcutaneous tissue, and skin meticulously. Pay careful attention to subcutaneous closure to eliminate dead space and prevent hematoma formation. Skin closure should be tension-free to prevent wound dehiscence.
Complications & Management
Despite meticulous surgical technique, tibial plateau fractures are prone to a range of complications, both intra-operative and post-operative, necessitating vigilance and a systematic approach to management.
Common Complications & Management Strategies
| Complication | Incidence | Etiology & Presentation | Management Strategies |
|---|---|---|---|
| Intra-operative Nerve Injury | 1-5% (peroneal) |
Common Peroneal Nerve:
Vulnerable during lateral approaches, particularly with excessive retraction, direct injury from drills/screws, or fibular head osteotomy. Presents as foot drop (weak dorsiflexion/eversion), numbness over dorsal foot/lateral calf.
Popliteal Artery/Vein: Rare but devastating. Direct laceration, contusion. Leads to acute ischemia (pallor, pulselessness, pain, paresthesias, paralysis). |
Immediate Recognition: Stop surgical procedure. Explore and protect nerve. For suspected arterial injury, obtain intra-op angiogram or consult vascular surgery for repair. Post-op, manage nerve palsies expectantly for up to 6-12 months. Foot drop splint. If no recovery, consider nerve graft, tendon transfer. For popliteal artery injury, emergent vascular repair is paramount to limb salvage. |
| Compartment Syndrome | 5-15% | Often associated with high-energy injuries or delayed presentation of swelling. Increased pressure within muscle compartments leads to tissue ischemia. Presents with disproportionate pain, pain on passive stretch, tense compartment, paresthesias. | Emergent Fasciotomy: Measure compartment pressures (anterior, lateral, deep posterior, superficial posterior). If ΔP (DBP-compartment pressure) < 30 mmHg or absolute pressure > 30-40 mmHg, perform four-compartment fasciotomy immediately. Defer definitive fracture fixation until fasciotomy wounds can be closed or skin grafted. |
| Infection (Superficial/Deep) | 2-10% |
Superficial:
Wound cellulitis, erythema, warmth, drainage.
Deep: Periprosthetic joint infection (PJI). Persistent pain, fever, swelling, purulent drainage, systemic signs. Higher risk with open fractures, prolonged surgery, compromised soft tissues, diabetes, smoking. |
Superficial:
Oral or IV antibiotics based on culture. Local wound care.
Deep: Urgent surgical debridement and irrigation, cultures (aerobic, anaerobic, fungal, atypical), hardware retention vs. removal (depending on stability, chronicity, organism), exchange of mobile components (if applicable), prolonged targeted IV antibiotics. If hardware must be removed, plan for staged reconstruction (e.g., external fixator followed by revision ORIF or arthroplasty). |
| Wound Healing Complications | 10-25% | Dehiscence, necrosis, skin blistering, hematoma. Related to soft tissue stripping, excessive tension, poor planning for swelling, smoking, diabetes. |
Prevention:
Meticulous soft tissue handling, delayed surgery ("wrinkle sign"), appropriate incisions, tension-free closure.
Management: Local wound care, serial debridements, negative pressure wound therapy (NPWT), skin grafting, local flap coverage. Revision closure. Address underlying patient factors (smoking cessation, glycemic control). |
| Loss of Reduction/Malunion | 5-15% | Inadequate fixation, premature weight-bearing, poor bone quality, technical error. Leads to persistent articular step-off, joint widening, angular deformity (varus/valgus), limb length discrepancy. |
Early Detection:
Close radiographic follow-up.
Management: If significant and early, revision ORIF. If established malunion and symptomatic, corrective osteotomy with internal fixation to restore alignment. For severe articular incongruity, consider arthrodesis or total knee arthroplasty (TKA) in older patients. |
| Nonunion | 2-5% | Failure of bone to heal after 6-9 months. Related to inadequate fixation, biological factors (smoking, poor nutrition), infection, excessive gap. Presents with persistent pain, instability, imaging showing lack of bridging callus. | Management: Address underlying cause (infection, instability). Surgical revision with debridement, stable internal fixation, and bone grafting (autograft preferred). Bone stimulators (electrical, ultrasound) may be considered as adjuncts. |
| Post-Traumatic Osteoarthritis (PTOA) | 20-50% (long-term) | Inevitable consequence of intra-articular injury, even with anatomic reduction. Related to articular cartilage damage at time of injury, residual articular incongruity, axial malalignment, meniscal loss. Presents as chronic pain, stiffness, swelling, crepitus, functional limitation. |
Prevention:
Anatomic reduction and stable fixation are paramount.
Management: Conservative (NSAIDs, PT, activity modification, injections). If severe and symptomatic, consider arthroscopic debridement, osteotomy (for malalignment), partial or total knee arthroplasty (TKA), or arthrodesis for end-stage arthritis. |
| Knee Stiffness / Arthrofibrosis | 10-30% | Scar tissue formation within the joint or surrounding soft tissues. Related to prolonged immobilization, insufficient early motion, high-energy injury, infection. Presents as restricted range of motion. |
Prevention:
Early, controlled range of motion (CPM, physical therapy) is critical.
Management: Aggressive physical therapy. If conservative measures fail, consider manipulation under anesthesia (MUA) or arthroscopic/open arthrolysis to release adhesions. |
| Hardware Prominence / Pain | Up to 20% | Plates or screws are palpable or irritate overlying soft tissues. More common with thin patients or superficial hardware placement. | Management: If symptomatic after fracture healing (usually 12-18 months post-op), elective hardware removal. Prior to hardware removal, ensure fracture is fully healed radiographically. |
| DVT/PE | 1-5% (clinical) | Venous stasis from immobilization, hypercoagulability from trauma/surgery, endothelial injury. Deep vein thrombosis (DVT) in calf/thigh, potentially leading to pulmonary embolism (PE). Symptoms: leg swelling, pain (DVT); dyspnea, chest pain, hypoxia (PE). |
Prevention:
Pharmacological prophylaxis (LMWH, DOACs, aspirin) and mechanical prophylaxis (compression stockings, IPCs). Early mobilization.
Management: Anticoagulation (therapeutic dose) for DVT/PE. Monitor for bleeding complications. For PE, consider IVC filter in select cases. |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is a critical determinant of functional outcome following tibial plateau fracture fixation. Protocols are individualized based on fracture stability, quality of fixation, patient compliance, and associated soft tissue injuries. The core tenets involve protecting the healing fracture, gradually restoring knee range of motion (ROM), progressive weight-bearing, and muscle strengthening.
Phase 1: Acute Protection & Early Motion (Weeks 0-6)
- Goals: Protect surgical repair, minimize swelling and pain, initiate early controlled ROM, maintain muscle tone.
- Weight-Bearing (WB): Non-Weight Bearing (NWB) or Toe-Touch Weight Bearing (TTWB) on the operative leg. Crutches or a walker are used. This is crucial for preventing collapse of the articular surface and loss of reduction.
-
Immobilization/Bracing:
A hinged knee brace is typically applied post-operatively.
- Initially locked in extension for transfers and protection.
- Gradually adjust ROM limits (e.g., 0-30° initially, progressing to 0-90° by week 6).
- Removed for exercises and hygiene.
-
Range of Motion:
- CPM Machine: Often initiated immediately post-op, typically for 4-8 hours daily, increasing flexion as tolerated (e.g., 0-30° to 0-90°). Evidence for universal benefit is mixed, but often used to reduce stiffness.
- Active-Assisted & Gentle Passive ROM: Within protected limits. Focus on quadriceps sets, hamstring sets, ankle pumps.
- Patellar Mobilization: Gentle superior/inferior and medial/lateral glides to prevent patellar infera.
- Edema Control: Elevation, cryotherapy, compression stockings.
- Muscle Activation: Isometric quadriceps (quad sets), hamstring sets, gluteal sets. Ankle pumps to prevent DVT.
- Wound Care: Monitor incision for signs of infection or dehiscence.
Phase 2: Progressive Loading & Strengthening (Weeks 6-12)
- Goals: Gradually increase weight-bearing, improve ROM, begin light strengthening, and enhance proprioception.
-
Weight-Bearing (WB):
- Partial Weight Bearing (PWB): Typically initiated around 6-8 weeks, progressing from 25% to 50% to 75% body weight, based on radiographic signs of healing and fracture stability. Use crutches/walker for support.
- Progression: Guided by surgeon assessment, pain levels, and physical therapist evaluation.
-
Range of Motion:
- Continue to increase active and passive ROM. Aim for near full flexion and extension by 12 weeks.
- Scar tissue massage and mobilization.
-
Strengthening:
- Closed Chain Exercises: Wall squats (partial), mini-squats, leg presses (light resistance), calf raises (bilateral progressing to unilateral).
- Open Chain Exercises (Controlled): Straight leg raises (SLR), knee extension (controlled range, low resistance), hamstring curls. Avoid high-resistance knee extension in early phases to protect fixation.
- Balance & Proprioception: Single leg stance (with support), balance board exercises.
- Cardiovascular: Non-impact activities like swimming (once wounds healed), stationary cycling (high seat, low resistance).
Phase 3: Advanced Strengthening & Return to Function (Weeks 12+)
- Goals: Restore full strength, endurance, power, agility, and prepare for return to desired activities.
- Weight-Bearing (WB): Full Weight Bearing (FWB) typically by 12 weeks, as tolerated and confirmed by radiographic healing. Discontinue assistive devices.
- Range of Motion: Achieve full, pain-free ROM.
-
Strengthening:
- Progressive Resistance: Increase intensity and load for all exercises.
- Functional Exercises: Lunges, step-ups, box jumps (later phase), agility drills (cutting, pivoting).
- Plyometrics: Begin with low-impact drills, gradually progressing.
- Sport-Specific Training: Tailored exercises to prepare for specific athletic demands.
-
Return to Activity:
- Low-Impact Activities: Walking, swimming, cycling often first.
- High-Impact/Sport: Gradual return, typically after 6-12 months, contingent on full strength, stability, and absence of pain. Clearance from the surgeon is essential.
- Monitoring: Continued monitoring for signs of post-traumatic arthritis, pain, or instability. Hardware removal may be considered after 12-18 months if symptomatic.
Key Considerations:
- Individualization: Protocols must be tailored to each patient's specific injury, healing progression, and personal goals.
- Pain Management: Adequate pain control is crucial to facilitate participation in physical therapy.
- Patient Education: Patients must be educated on the importance of adherence to restrictions and exercises.
- Radiographic Follow-up: Regular X-rays (e.g., at 2, 6, 12 weeks, then 3, 6, 12 months) are essential to monitor fracture healing and maintenance of reduction.
- Associated Injuries: Rehabilitation needs to address concurrent meniscal repairs or ligamentous reconstructions.
Summary of Key Literature / Guidelines
The management of tibial plateau fractures continues to evolve, with ongoing research refining surgical techniques, implant design, and rehabilitation protocols. A critical review of the literature highlights several key principles and emerging trends.
Classification Systems and Imaging
- The Schatzker classification remains the most clinically utilized system due to its simplicity and prognostic value, despite limitations in characterizing posterior column involvement and multi-fragmentary injuries.
- The AO/OTA classification provides greater detail but is more complex.
- CT imaging with 3D reconstructions is universally acknowledged as indispensable for pre-operative planning, offering superior assessment of articular depression, comminution, and fragment orientation compared to plain radiographs. MRI is increasingly used to identify associated soft tissue injuries (meniscus, ligaments) that significantly impact surgical strategy and prognosis.
Surgical Timing and Soft Tissue Management
- A consensus supports delayed definitive internal fixation until the "wrinkle sign" appears and the soft tissue envelope has recovered, particularly for high-energy injuries. This strategy significantly reduces the incidence of wound complications.
- Temporizing external fixation is a well-established practice for unstable fractures with compromised soft tissues, allowing for soft tissue rest, ligamentotaxis, and reduction of swelling before definitive internal fixation. This staged approach is superior to immediate open reduction in reducing infection and wound complications in many complex cases.
Surgical Approaches and Fixation
- Dual surgical approaches (e.g., anterolateral and posteromedial) are increasingly favored for bicondylar fractures (Schatzker V, VI) to allow direct visualization and reduction of both columns. This minimizes extensive soft tissue stripping associated with single large incisions.
- The importance of addressing the posteromedial column as a distinct entity has gained recognition, with specific posteromedial approaches and plating strategies improving stability and preventing malreduction.
- Anatomic reduction of the articular surface (step-off <2mm) and restoration of the mechanical axis are paramount goals, correlating strongly with long-term outcomes and reduced rates of post-traumatic osteoarthritis.
- Stable internal fixation using modern locking plate technology provides angular stability, allowing for early mobilization. Rafting screws are critical for supporting depressed articular fragments.
- Bone grafting (autograft, allograft, or synthetics) for metaphyseal voids is a standard practice to prevent articular collapse, though the superiority of one graft type over others remains debated.
Rehabilitation and Outcomes
- Early, controlled range of motion is emphasized to prevent stiffness and optimize cartilage nutrition.
- Gradual, protected weight-bearing is fundamental, with specific timelines dictated by fracture stability, quality of fixation, and patient compliance. Premature weight-bearing can lead to loss of reduction or fixation failure.
- Long-term studies consistently demonstrate a significant risk of post-traumatic osteoarthritis (PTOA) , even with anatomically reduced and stably fixed fractures, highlighting the impact of initial cartilage damage. Factors like persistent articular incongruity, meniscal damage, and axial malalignment significantly accelerate PTOA progression.
- Functional outcomes are often good to excellent in simple fractures, but more complex bicondylar patterns are associated with higher rates of complications and less predictable outcomes, often leading to chronic pain and functional limitations.
Evolving Concepts
- Minimally Invasive Plate Osteosynthesis (MIPO): While promising for diaphyseal and metaphyseal fractures, its application to complex intra-articular tibial plateau fractures is technically demanding and limited by the need for direct articular visualization and reduction. Percutaneous screw fixation or limited open approaches combined with arthroscopy are explored.
- Arthroscopy-Assisted Reduction: Offers direct visualization of the articular surface and menisci, facilitating reduction and meniscal repair, especially for less complex depression fractures. However, it can prolong surgical time and adds technical complexity.
- Patient-Specific Instrumentation/3D Printing: Emerging technologies for complex reconstructive challenges, allowing for highly individualized pre-operative planning and potentially guiding intra-operative reduction and fixation.
The consensus from major orthopedic organizations like the AO Foundation and AAOS emphasizes a comprehensive, individualized approach, integrating advanced imaging, meticulous surgical technique, and a structured rehabilitation program to optimize outcomes for patients with tibial plateau fractures. Continued research focusing on cartilage protection strategies and biologics for cartilage repair remains a significant area of interest to mitigate the long-term burden of PTOA.
You Might Also Like