Orthopedic Gunshot Wounds: Ballistics, Energy Transfer & Injury Biomechanics
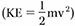
Key Takeaway
Orthopedic gunshot wound severity is primarily dictated by kinetic energy transferred from the projectile to tissue, predominantly influenced by projectile velocity. High-velocity rounds create destructive temporary cavitation. Low-velocity rounds cause direct crushing. Shotgun wounds vary based on choke, load, and range, all impacting musculoskeletal trauma extent.
Introduction & Epidemiology
Gunshot wounds (GSWs) represent a significant and escalating public health crisis globally, presenting complex challenges for the orthopedic surgeon. The increasing incidence of both civilian and combat-related ballistic trauma necessitates a profound understanding of the underlying principles of injury mechanics to optimize patient outcomes. Ballistic injuries are characterized by their unique biomechanical profile, distinct from blunt or penetrating trauma, often resulting in extensive soft tissue and osseous destruction that extends far beyond the apparent entry and exit wounds.
Orthopedic surgeons frequently manage GSWs affecting the musculoskeletal system, ranging from simple soft tissue injuries to devastating fractures, joint disruptions, and complex neurovascular deficits. The morbidity associated with these injuries is substantial, often leading to prolonged hospitalization, multiple surgical procedures, significant functional impairment, and socioeconomic burden. A thorough grasp of ballistics, energy transfer, and tissue response is paramount for accurate injury assessment, appropriate surgical planning, and effective post-operative management.
Surgical Anatomy & Biomechanics
Understanding the biomechanics of GSWs requires a comprehensive analysis of the projectile's characteristics, its interaction with biological tissues, and the resulting energy transfer. This interaction dictates the extent and pattern of tissue damage.
Ballistics
Ballistics, the science of projectile motion, is categorized based on projectile velocity, which directly correlates with kinetic energy transfer and, consequently, wounding potential.
Low Velocity Projectiles
Low velocity projectiles, defined as those traveling at less than 610 meters per second (2,000 ft/sec), primarily include rounds fired from all handguns and some shotguns at extended ranges. The primary mechanism of injury with low-velocity projectiles is direct crushing and tearing of tissue along the missile path. While temporary cavitation is still present, its magnitude is significantly less destructive compared to high-velocity impacts. Fractures caused by low-velocity projectiles are typically direct, often comminuted at the site of impact but with less widespread fragmentation than high-velocity injuries. The kinetic energy deposited is generally localized.
High Velocity Projectiles
High velocity projectiles, characterized by velocities exceeding 610 meters per second (2,000 ft/sec), encompass rounds from all military rifles and most hunting rifles. These projectiles possess significantly greater kinetic energy, leading to a vastly different injury pattern. The critical distinction lies in the phenomenon of temporary cavitation . As a high-velocity projectile traverses tissue, it creates an enormous pressure wave, displacing tissue radially away from the missile path. This displacement creates a temporary cavity many times larger than the projectile's diameter, which then collapses. The rapid expansion and collapse stretch and tear tissues, disrupt vascular supply, and cause damage to structures far from the direct bullet path. This effect is particularly devastating in dense tissues with low elasticity. Bone fractures are often highly comminuted, with significant energy transfer leading to extensive periosteal stripping and devitalization.
Shotgun Wounding Potential
The wounding potential of shotgun injuries is uniquely dependent on several factors:
1.
Choke (shot pattern):
The choke restricts the barrel's diameter at the muzzle, controlling the spread of the pellets. A tighter choke results in a denser pattern, concentrating energy over a smaller area, increasing injury severity at closer ranges.
2.
Load (size of the individual pellet):
Larger pellets (e.g., buckshot) carry more individual kinetic energy and mass, penetrating deeper and creating larger permanent tissue defects. Smaller pellets (e.g., birdshot) disperse more widely, resulting in a broader but shallower wound profile.
3.
Distance from the target:
This is a crucial determinant. At close range (<5-7 meters), shotgun wounds are highly destructive, often behaving like high-velocity single projectile injuries due to the concentrated mass of pellets. The combined kinetic energy of the clustered pellets is delivered over a small area, leading to massive tissue destruction and extensive comminution. At intermediate ranges, the pattern spreads, causing multiple individual penetrations. At extended ranges, the energy of individual pellets diminishes, and injuries may be superficial.
Energy Transfer
The extent of tissue damage from a GSW is primarily determined by the amount of kinetic energy transferred from the projectile to the tissue.
The kinetic energy (KE) of any moving object is directly proportional to its mass (m) and the square of its velocity (v²) and is defined by the equation:
KE = 1/2 mv²

This fundamental principle explains why velocity is a far more critical determinant of wounding potential than mass. A small increase in velocity results in a disproportionately large increase in kinetic energy.
The energy delivered by a missile to a target is dependent on:
1.
The energy of the missile on impact (striking energy):
This is the kinetic energy of the projectile immediately prior to striking the tissue.
2.
The energy of the missile on exiting the tissue (exit energy):
If the projectile exits, it retains some kinetic energy. The difference between striking and exit energy represents the energy transferred to the tissue. If the projectile is retained, all its striking energy is transferred (minus any energy lost to air resistance or fragmentation).
3.
The behavior of the missile while traversing the target:
This is critical and encompasses several phenomena:
*
Tumbling (Yaw):
Projectiles are designed for aerodynamic stability in flight. Upon entering a denser medium like tissue, they become unstable, often yawing (rotating about their transverse axis) and then tumbling (a complete end-over-end rotation). Tumbling presents a larger surface area to the tissue, increasing drag and thus maximizing energy transfer.
*
Deformation:
Soft-nosed or hollow-point bullets are designed to deform or mushroom upon impact, increasing their frontal surface area. This significantly increases drag and energy transfer, leading to larger permanent cavities.
*
Fragmentation:
Some projectiles are designed to fragment into multiple smaller pieces. Each fragment acts as a secondary projectile, creating multiple wound tracts and further increasing tissue damage and energy deposition. Military full metal jacket (FMJ) rounds may also fragment upon impact with bone.

Figure: Illustration of projectile deformation and fragmentation patterns, demonstrating how missile behavior directly influences energy transfer and wound creation.
Tissue Parameters
The wounding potential of a bullet depends not only on the missile parameters, including caliber, mass, velocity, range, composition, and design, but also on the characteristics of the target tissue itself.
The degree of injury created by the missile is generally dependent on the specific gravity (density) and elasticity of the traversed tissue: higher specific gravity and lower elasticity equate to greater tissue damage.
*
Bone:
With high specific gravity and low elasticity, bone sustains severe damage, often leading to extensive comminution and fragmentation. Bone fragments can act as secondary projectiles, further extending injury.
*
Muscle:
Dense but relatively elastic, muscle tissue tolerates temporary cavitation somewhat better than bone, but muscle cells are highly sensitive to ischemia and mechanical disruption.
*
Solid Organs (Liver, Spleen):
High specific gravity and low elasticity lead to massive damage and hemorrhage.
*
Hollow Organs (Intestine):
More resilient to temporary cavitation due to elasticity, but direct perforation can lead to contamination.
*
Connective Tissue (Fascia, Tendon):
Can be avulsed or lacerated.
*
Neurovascular Structures:
Highly susceptible to direct injury, stretching, or contusion from temporary cavitation, leading to severe functional deficits.
A missile projectile achieves a high kinetic energy because of its relatively high velocity. The impact area is relatively small, resulting in a small area of entry with a momentary expansion of the tissue creating a temporary cavity. This temporary cavitation is followed by tissue collapse. The destructive force generated can devitalize tissue far from the actual projectile path, creating a larger zone of injury than initially apparent. The permanent cavity is the actual tissue defect caused by the crushing and lacerating action of the projectile and its fragments. The surrounding zone of injury, characterized by cellular damage, edema, and microvascular disruption, is often more extensive, especially with high-velocity impacts.

Figure: Depiction of temporary and permanent cavitation. The permanent cavity represents the actual tissue destruction, while the larger, transient temporary cavity causes significant stretching, tearing, and microvascular damage in the surrounding tissues.

Figure: Cross-sectional view illustrating the wound tract with zones of injury: the permanent cavity (direct tissue destruction), the zone of contusion and devitalization, and the surrounding zone of edema and inflammation.
Indications & Contraindications
The management of GSWs, particularly those involving the musculoskeletal system, often necessitates surgical intervention. The decision-making process is guided by the extent of tissue damage, presence of complications, and potential for functional compromise.
Operative Indications
-
Open Fractures (Gustilo Type I-IIIC):
All open fractures secondary to GSWs typically require surgical debridement and stabilization. The Gustilo-Anderson classification is commonly employed, though GSWs often defy strict categorization due to extensive soft tissue injury and contamination.
- Gustilo I/II: Minimal soft tissue damage, but requires thorough debridement.
- Gustilo III: Extensive soft tissue damage, periosteal stripping, vascular/nerve injury, or gross contamination. These always require aggressive debridement and often staged reconstruction.
- Neurovascular Compromise: Any evidence of vascular insufficiency (e.g., absent pulses, pallor, paresthesias, paralysis, poikilothermia) or progressive neurological deficit necessitates emergent exploration. Angiography may be performed pre-operatively if the patient is stable.
- Compartment Syndrome: Clinical suspicion or documented elevated intracompartmental pressures mandate emergent fasciotomy. High-velocity GSWs, especially in the forearm or leg, carry a high risk due to massive tissue swelling.
- Joint Involvement: Intra-articular fractures, particularly those with retained foreign bodies, require arthrotomy, debridement, and often internal fixation to restore joint congruity and prevent post-traumatic arthritis.
- Significant Soft Tissue Contamination/Devitalization: While all GSWs are considered contaminated, gross contamination (e.g., clothing, dirt, heavy metal fragments) or extensive necrotic tissue requires aggressive debridement.
- Unstable Fractures: Fractures that cannot be managed non-operatively due to instability, shortening, or unacceptable angulation often require fixation.
-
Retained Foreign Bodies:
- Intra-articular projectiles (risk of lead arthropathy, synovial reaction).
- Projectiles impinging on nerves or vessels.
- Projectiles in critical locations (e.g., spinal canal, skull base, near major visceral structures where migration could be catastrophic).
- Large, accessible fragments causing pain or mechanical irritation.
- Wound Ballistics Indicating High-Energy Transfer: Even with a relatively small entry/exit, high-velocity wounds may warrant exploration and debridement due to unseen deep tissue damage.
Non-Operative Indications
- Stable Fractures: Nondisplaced or minimally displaced fractures that can be adequately managed with immobilization (e.g., splinting, casting) without compromising function or stability.
- Tangential Wounds: Injuries where the projectile traverses superficial soft tissues without violating critical structures or causing significant deep tissue destruction.
-
Retained Projectiles:
- Small, deeply embedded, asymptomatic fragments located in non-critical areas (e.g., muscle, subcutaneous tissue) where removal would necessitate extensive dissection and potentially cause more harm than leaving them.
- Projectiles in close proximity to major neurovascular structures where surgical exploration carries a high iatrogenic risk.
- Projectiles in cancellous bone without joint involvement or impending neurovascular compromise.
- Absence of Neurovascular Injury, Compartment Syndrome, or Significant Contamination: In these specific low-energy scenarios, non-operative management may be considered for soft tissue wounds or stable fractures.
Operative vs. Non-Operative Indications for GSWs
| Indication Category | Operative Management | Non-Operative Management |
|---|---|---|
| Fracture Type | Open fractures (Gustilo I-IIIC), unstable fractures, intra-articular fractures, fractures with significant bone loss, segmental fractures. | Stable, nondisplaced or minimally displaced fractures without joint involvement or neurovascular compromise (e.g., hairline fractures, stable avulsion fractures). |
| Neurovascular Status | Documented neurovascular compromise (ischemia, progressive deficit), impending compartment syndrome, pulsatile hematoma, active hemorrhage. | Intact neurovascular status, no signs of compartment syndrome, stable hematoma without active bleeding. |
| Soft Tissue Injury | Extensive soft tissue devitalization, gross contamination, impending skin necrosis, wound dehiscence requiring secondary closure, infected wounds. | Superficial tangential wounds, small entry/exit wounds with minimal surrounding tissue damage, clean wounds without devitalized tissue (after initial assessment). |
| Foreign Bodies | Intra-articular projectiles, projectiles impinging on nerves/vessels, projectiles in critical anatomical locations (e.g., spinal canal, CNS, major visceral proximity), symptomatic superficial fragments, large fragments causing chronic pain or infection. | Small, deeply embedded, asymptomatic fragments in non-critical soft tissue or cancellous bone, where removal carries greater risk than retention, or projectiles near vital structures where dissection poses iatrogenic risk. |
| Infection Risk | Wounds with high suspicion of infection (delayed presentation, signs of cellulitis, purulence), established osteomyelitis. | Prophylactic antibiotics for all GSWs (standard), no signs of acute infection on presentation for select superficial wounds. |
| Functional Impairment | Injuries requiring stabilization for early mobilization or functional restoration (e.g., major joint fractures, weight-bearing bone fractures), amputations. | Injuries where function can be restored with non-operative immobilization or bracing without significant long-term disability. |
| Patient Stability | Hemodynamically stable patients amenable to definitive surgical intervention. | Patients who are hemodynamically unstable, where surgery would be life-threatening (may require temporizing measures like external fixation, then definitive surgery once stable). |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is critical for optimizing outcomes in GSWs, given their inherent complexity and potential for severe complications.
Initial Assessment and Resuscitation
- ATLS Protocol: Adherence to Advanced Trauma Life Support (ATLS) guidelines is paramount. Primary survey (Airway, Breathing, Circulation, Disability, Exposure) takes precedence. Hemodynamic stabilization, control of hemorrhage, and assessment for life-threatening injuries are the initial priorities.
-
Imaging:
- Plain Radiographs: Essential to localize the projectile, identify fracture patterns, assess fragmentation, and determine entry/exit points (when present). Obtain two orthogonal views. For shotgun wounds, radiographs help delineate pellet distribution.
- Computed Tomography (CT): Crucial for complex fractures (especially periarticular or involving the spine/pelvis), assessing bone loss, identifying retained fragments, and evaluating soft tissue damage and missile tracts. CT angiography (CTA) is indicated for suspected vascular injury.
- Angiography: Gold standard for vascular injury assessment when CTA is inconclusive or for pre-operative planning of complex vascular repairs.
- Ultrasound: May be used in the emergency department for rapid assessment of fluid collections or vascular integrity.
- Antibiotic Prophylaxis: Broad-spectrum intravenous antibiotics (e.g., a cephalosporin with an aminoglycoside, or penicillin if clostridial infection is a concern) should be administered as soon as possible, ideally within 3 hours of injury. The duration typically extends for 24-72 hours post-debridement, depending on contamination and tissue loss. Tetanus prophylaxis must also be updated.
- Tourniquet Placement: Prophylactic tourniquet placement proximal to the injury may be prudent, particularly for extremity GSWs, to facilitate a bloodless field during debridement and fracture fixation. It should be inflated only when needed and for the shortest duration possible.
Pre-operative Surgical Considerations
- Debridement Strategy: Plan for aggressive debridement of all devitalized tissue. This is often the most critical step in preventing infection. Determine the likely extent of devitalization based on ballistic characteristics.
- Fracture Fixation Strategy: Determine whether internal fixation (plates, screws, intramedullary nails) or external fixation is appropriate. External fixation is often preferred for initial stabilization in highly contaminated or comminuted open fractures, allowing for serial debridements and soft tissue healing prior to definitive internal fixation.
- Soft Tissue Coverage: Anticipate the need for delayed wound closure, local flaps, or free tissue transfer. Early consultation with plastic surgery may be beneficial for extensive defects.
- Foreign Body Management: Identify the location of retained fragments. Plan for selective removal of symptomatic or critically located projectiles.
- Sequential Surgical Planning: GSWs often require staged procedures, starting with initial stabilization and debridement, followed by definitive fracture fixation and soft tissue reconstruction.
Patient Positioning
Patient positioning must allow complete access to the injury site, potential donor sites for grafts/flaps, and for intraoperative imaging.
*
Versatility:
The position should allow for extension of incisions, exploration of adjacent compartments, and management of entry and exit wounds.
*
Hemodynamic Stability:
Ensure safe padding of all pressure points, access for anesthesiology, and protection of neurovascular structures.
*
Image Intensifier Access:
Position the patient and equipment to allow for unobstructed fluoroscopic imaging from multiple angles. For example, a supine position with an arm board for an upper extremity injury, or a fracture table for lower extremity long bone fractures.
Detailed Surgical Approach / Technique
The surgical management of GSWs, particularly those involving orthopedic structures, is guided by principles of open fracture care, with a strong emphasis on radical debridement, stabilization, and infection prevention.
1. Initial Wound Exploration & Debridement
- Extension of Wounds: The skin incision should be extended proximally and distally along the axis of the limb or body segment to adequately expose the wound tract and allow for thorough debridement. Avoid extensive transverse incisions which may compromise vascularity. The trajectory of the projectile, often assessed by entry and exit wounds or imaging, guides the surgical approach.
-
Serial Debridement:
This is the cornerstone of GSW management.
- Skin: Excise obviously devitalized skin edges. The skin is remarkably resilient, but areas of tension necrosis or avulsion require careful assessment.
- Subcutaneous Tissue: Remove bruised or necrotic subcutaneous tissue.
- Fascia: Fasciotomy of all affected compartments, particularly in high-velocity injuries, is often indicated to prevent compartment syndrome and allow for complete decompression and debridement of underlying muscle. Release all fascial compartments involved.
- Muscle: This is the most critical component of debridement. Devitalized muscle (characterized by its lack of contractility, non-bleeding upon incision, dull color, and inability to react to electrocautery) must be aggressively excised. Use sharp dissection to remove all necrotic muscle, preserving viable tissue as much as possible. This may require multiple passes over the course of serial debridements.
- Bone: Remove free, non-articular bone fragments that are devascularized or heavily contaminated. Large, cortical fragments that retain soft tissue attachments and contribute to mechanical stability, even if partially devascularized, may be preserved and incorporated into the reconstruction if thoroughly cleaned and reduced. Intra-articular fragments should be removed if severely comminuted or if they impede reduction or joint mechanics.
- Irrigation: Copious lavage with normal saline (often 6-9 liters or more for Gustilo III injuries) using low-pressure irrigation (syringe and needle or pulsatile lavage at ~30 psi) is essential to remove gross contaminants and small foreign bodies. High-pressure lavage may drive contaminants deeper into tissues.
- Assessment of Neurovascular Structures: Carefully inspect and protect all neurovascular bundles. Any transected or significantly injured vessels require repair or ligation. Nerves should be tagged for potential delayed repair if transected.
2. Fracture Management
- Reduction: Principles of open reduction and internal fixation (ORIF) are applied, but often modified due to tissue damage and contamination. Indirect reduction techniques (e.g., using distraction or ligamentotaxis) are often preferred to minimize further soft tissue stripping.
-
Stabilization Options:
- External Fixation: The primary method for initial stabilization of severely contaminated or comminuted open fractures. It is rapidly applied, allows access for serial debridements and soft tissue care, and provides stability with minimal additional tissue dissection. Pin placement must respect potential future definitive fixation plans.
- Internal Fixation (Plates, Screws, Intramedullary Nailing): Generally reserved for definitive fixation once the soft tissue envelope has stabilized and the risk of infection is minimized. This may be a delayed procedure (5-14 days post-injury) after serial debridements. Intramedullary nailing can be considered for selected long bone fractures, particularly in Gustilo I/II injuries with minimal soft tissue loss, but the canal must be debrided, and reaming should be performed cautiously in contaminated fields. Bridge plating techniques are often preferred over absolute stability plating to respect the soft tissue envelope.
- Bone Grafting: For significant bone defects, bone grafting (autograft or allograft) is typically delayed until the soft tissues are healthy and the infection risk is low, usually weeks to months after the initial injury.
3. Soft Tissue Coverage
- Delayed Primary Closure: Most GSWs are left open after initial debridement and managed with sterile dressings, vacuum-assisted closure (VAC) devices, or wet-to-dry dressings. This allows for ongoing drainage and reassessment of tissue viability.
- Second-Look Procedures: Mandatory in high-velocity GSWs and heavily contaminated wounds. These involve repeat debridement every 24-48 hours until all devitalized tissue is removed.
-
Definitive Closure:
Achieved when the wound bed is healthy and free of necrotic tissue. This may involve:
- Primary Closure: If minimal tissue loss and tension-free.
- Skin Grafts: For large superficial defects.
- Local or Regional Flaps: For moderate defects with exposed bone or hardware.
- Free Tissue Transfer: For extensive soft tissue defects or composite defects requiring significant volume replacement, often performed in conjunction with plastic surgeons.
4. Foreign Body Removal
-
Selective Removal:
Not all retained projectiles or fragments need to be removed. Indications for removal include:
- Intra-articular location.
- Impacting or adjacent to major nerves or vessels.
- Causing symptoms (pain, mechanical irritation).
- Significant lead contamination (e.g., large fragments in joints, or in patients with renal failure, which can lead to lead toxicity).
- Superficial and easily accessible.
- Non-removal: Deep, asymptomatic fragments in muscle or cancellous bone are often left in situ, as the risk of extensive dissection and iatrogenic injury often outweighs the potential benefits of removal.
Complications & Management
Gunshot wounds are associated with a high rate of complications due to the severity of initial tissue damage, contamination, and the complex healing environment. Proactive recognition and aggressive management are essential.
Common Complications & Salvage Strategies
| Complication | Incidence (Variable, dependent on GSW severity) | Salvage Strategies |
|
Infection
| ~20-40% for severe open fractures (Gustilo III) | Aggressive debridement (serial), broad-spectrum antibiotic regimen guided by cultures, negative pressure wound therapy (NPWT), planned definitive wound coverage (flaps), removal of infected hardware (if secondary to infection and not critical for stability), bone infection management (e.g., debridement, antibiotic cement, systemic antibiotics). |
|
Nonunion / Malunion
| ~10-30% for high-energy fractures | Nonunion: Revision surgery with stable fixation, bone grafting (autograft/allograft), osteogenic stimulants (e.g., bone morphogenetic protein, pulsed electromagnetic fields). Malunion: Corrective osteotomy and internal fixation after fracture healing, often involving complex planning with 3D models. |
|
Neurovascular Injury
| ~5-20% (direct injury or secondary contusion) | Vascular: Emergent surgical exploration, primary repair (end-to-end anastomosis), interposition vein graft, ligation (if limb not viable or collateral flow adequate). Nerve: Observation for neurapraxia/axonotmesis, neurolysis, primary repair (if sharp transection), nerve grafting (for gaps), tendon transfers or functional bracing for irreversible deficits. |
|
Compartment Syndrome
| ~5-15% (especially high-velocity extremity GSWs) | Emergent four-compartment fasciotomy (limb), or other appropriate fascial release (e.g., gluteal). |
|
* |
*
Average
Incidence
|
Management Strategies
|
|
Overall
incidence
|
Overall average
:
5-10% (from lowest for tangential to highest for major GSWs)
|
Proactive strategies:
Rigorous adherence to principles of GSW management from the start.
|
|
Amputation
| Rare as primary procedure; often secondary to severe limb-threatening complications or irreversible damage. | Initial assessment for replantation potential (if suitable for replantation based on limb ischemia time, level of injury, patient factors). If not replantable or limb non-salvageable, definitive amputation with consideration of prosthetic fitting and rehabilitation. |
|
Post-Traumatic Arthritis
| High (especially intra-articular fractures) | Early, accurate anatomical reduction and stable fixation of intra-articular fractures, aggressive rehabilitation. If severe, arthroplasty (total joint replacement) or arthrodesis may be required. |
|
Residual Disability
| Common (loss of function, chronic pain) | Multidisciplinary rehabilitation (physical therapy, occupational therapy, psychological support, pain management), surgical reconstruction for functional restoration (e.g., arthroplasty, tendon transfers, corrective osteotomies), appropriate bracing or orthotics, vocational rehabilitation. |
|
Amputation
| ~1-5% (as primary procedure if unsalvageable) | Replantation attempt (if appropriate criteria met: clean transection, short ischemia time, minimal tissue damage). Definitive amputation with consideration of prosthetic fitting and rehabilitation. |
Specific Orthopedic Complications
-
Segmental Bone Loss:
GSWs frequently result in significant osseous defects. Management involves:
- Bone Transport: Using external fixators (e.g., Ilizarov, Taylor spatial frame) to induce osteogenesis and gradually transport a bone segment to fill the defect.
- Masquelet Technique (Induced Membrane): Staged procedure involving placement of a cement spacer in the defect, removal after 6-8 weeks, and subsequent filling with cancellous autograft within the induced membrane.
- Vascularized Fibula Graft: For large, critical defects, particularly in the lower extremity.
-
Soft Tissue Coverage Deficiencies:
Large wounds often struggle to heal or cover exposed hardware. Strategies include:
- NPWT: Facilitates granulation tissue formation and reduces wound size.
- Local/Regional Flaps: Transposition of adjacent healthy tissue.
- Free Flaps: Microvascular transfer of tissue from a distant site.
- Lead Toxicity: Retained lead fragments in certain anatomical locations (e.g., joints, bursae, or near large fluid collections) can lead to systemic lead poisoning, especially in patients with acidic body fluids or those with impaired renal function. Monitoring of lead levels and chelation therapy may be necessary. Symptomatic lead fragments should be removed.
- Heterotopic Ossification (HO): Particularly common in blast injuries and high-energy GSWs, especially involving large muscle groups. Prophylaxis with NSAIDs (e.g., indomethacin) or radiation therapy may be considered for high-risk patients. Excision is performed once mature.
- Complex Regional Pain Syndrome (CRPS): A debilitating neuropathic pain condition that can follow extremity trauma. Early recognition and multidisciplinary pain management are crucial.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is a critical, integrated component of GSW management, aiming to restore function, prevent stiffness, and minimize long-term disability. Protocols are tailored to the specific injury, surgical intervention, and patient's general condition.
Early Post-Operative Phase (Weeks 0-6)
- Pain Management: Multimodal approach including analgesics, nerve blocks, and non-pharmacological methods.
- Wound Care: Meticulous wound care, often involving dressing changes, NPWT management, and monitoring for signs of infection.
-
Immobilization vs. Early Mobilization:
- Stable Fixation: For fractures with stable internal fixation and good soft tissue coverage, early protected range of motion (PROM) and active range of motion (AROM) exercises can be initiated to prevent stiffness and promote joint health.
- External Fixation / Unstable Fixation: Immobilization is maintained, or a strictly protected range of motion is allowed. The external fixator itself may be used for controlled articulation (e.g., hinged knee fixators).
- Edema Control: Elevation, compression, and gentle muscle pumping exercises.
- Weight-Bearing (Lower Extremity): Non-weight bearing or protected weight-bearing (e.g., touch-down weight-bearing) is maintained until fracture healing shows progress, and stability is confirmed by imaging.
- Upper Extremity: Strict lifting and carrying restrictions.
- Functional Activities of Daily Living (ADLs): Training for independence in basic ADLs, often with assistive devices.
Intermediate Phase (Weeks 6-12)
- Progressive Range of Motion: Gradually increase joint range of motion, advancing from passive to active assisted, then full active. Address any developing contractures.
- Strengthening: Initiate isometric and then progressive isotonic strengthening exercises for muscle groups surrounding the injured area. Focus on core stability and proximal strength for overall functional recovery.
- Scar Management: Gentle massage, stretching, and silicone sheeting to minimize scar contracture and improve skin pliability.
- Proprioception and Balance (Lower Extremity): Incorporate balance exercises as weight-bearing status improves.
- Weight-Bearing Progression (Lower Extremity): Gradually increase weight-bearing as determined by clinical and radiographic signs of healing.
Advanced Phase (Weeks 12+)
- Full Strength and Endurance Training: Advance to higher resistance and longer duration exercises. Focus on sport-specific or occupation-specific activities.
- Return to Activity: Gradual return to work, recreational activities, and sports, guided by functional assessments and physician clearance.
- Addressing Residual Deficits: Continual assessment for any persistent pain, weakness, or functional limitations. This may require further interventions such as bracing, orthotics, or additional surgical procedures (e.g., for nonunion, malunion, or nerve injury).
- Psychological Support: Many GSW patients experience significant psychological distress, including PTSD, depression, and anxiety. Integration of psychological counseling and support groups is essential for holistic recovery.
Summary of Key Literature / Guidelines
The management of GSWs, particularly those involving the musculoskeletal system, is continuously refined by clinical experience and research. Key guidelines and literature provide the framework for optimal practice.
Trauma Management Protocols
- Advanced Trauma Life Support (ATLS): Remains the foundational standard for initial assessment and resuscitation of trauma patients, including those with GSWs. Emphasizes systematic evaluation and stabilization.
- Damage Control Orthopedics (DCO): For severely injured, unstable patients, DCO principles advocate for immediate life-saving interventions (e.g., external fixation for open fractures, wound packing) with definitive orthopedic procedures deferred until the patient is physiologically stable. This approach has significantly improved outcomes in polytrauma patients.
Wound Management & Infection Prevention
- Gustilo-Anderson Classification: While originally developed for blunt trauma open fractures, it is broadly applied to GSW open fractures to guide management, particularly regarding debridement and antibiotic selection. However, the unique energy transfer of GSWs often means Gustilo grades may underestimate the true extent of deep tissue damage.
- Antibiotic Prophylaxis: Consensus guidelines recommend broad-spectrum intravenous antibiotics initiated as early as possible (within 3 hours) and continued for 24-72 hours post-debridement. Prolonged antibiotic courses are not routinely recommended unless there is established infection or significant ongoing contamination. The choice of antibiotics should cover common skin flora and environmental contaminants.
- Debridement Principles: The critical role of aggressive, serial surgical debridement of all devitalized tissue is consistently supported by literature as the primary means of infection prevention and wound healing promotion. The concept of the "zone of injury" extending beyond the visible wound is central to this.
- Negative Pressure Wound Therapy (NPWT): Evidence supports the use of NPWT for temporary wound coverage following debridement of complex GSWs. It promotes granulation tissue formation, reduces edema, and prepares the wound bed for definitive closure.
Fracture Fixation in Contaminated Wounds
- External Fixation: Widely recognized as the preferred initial method for stabilizing GSW-related open fractures, especially Gustilo II and III injuries, due to its minimally invasive nature, adaptability for serial debridements, and effectiveness in maintaining alignment in contaminated fields.
- Internal Fixation: While internal fixation can be performed, it is often delayed after serial debridements and when the wound is deemed clean and has a healthy soft tissue envelope. The use of intramedullary nails in Gustilo III GSWs remains a topic of debate, with many surgeons preferring external fixation followed by conversion to internal fixation or plate fixation.
Foreign Body Management
- Selective Removal: Current literature generally supports a selective approach to retained GSW fragments. Removal is indicated for intra-articular fragments, those causing neurovascular impingement, symptomatic superficial fragments, or those associated with significant lead toxicity. Deep, asymptomatic fragments in non-critical locations are often safely left in situ. Close observation and patient education regarding potential long-term issues are important.
Lead Toxicity
- The risk of lead toxicity from retained projectiles, particularly intra-articular lead or high-surface-area fragments, is a recognized concern. Monitoring blood lead levels and considering removal or chelation for symptomatic patients or those with elevated levels, especially in specific anatomical locations or patient cohorts (e.g., renal impairment), is recommended.
Emerging Concepts
- Biofilms: The role of bacterial biofilms in persistent GSW infections and osteomyelitis is gaining recognition, influencing antibiotic strategies and debridement techniques.
- Advanced Soft Tissue Reconstruction: Microvascular free tissue transfer and bioengineered matrices continue to evolve, offering improved solutions for complex soft tissue and composite defects.
- Personalized Medicine: Future directions may include advanced genetic profiling to predict infection risk or optimize healing, though these are still largely research-based.
In conclusion, the effective management of gunshot wounds demands a nuanced understanding of ballistic principles, energy transfer, and tissue response, coupled with adherence to established surgical principles and continuous adaptation to emerging evidence. The orthopedic surgeon plays a pivotal role in restoring function and minimizing the devastating long-term consequences of these severe injuries.
Clinical & Radiographic Imaging

You Might Also Like