Orthopedics Hyperguide Review | Dr Hutaif General Ortho -...
14 Apr 2026
48 min read
89 Views
Key Takeaway
This interactive board review contains 100 randomly selected orthopedic surgery questions with clinical images, immediate feedback, and detailed references.
Orthopedics Hyperguide Review | Dr Hutaif Gen...
00:00
Start Quiz
Question 1High Yield
The Lisfranc ligament extends from the
Explanation
- medial cuneiform to the second metatarsal bone.
Question 2High Yield
Which of the following organisms is most often found in a late (> 3 months) infection of a total hip arthroplasty?

Explanation
DISCUSSION: Staphylococcus epidermidis is the most common organism found in an infected total hip arthroplasty greater than 3 months from the origional surgery. Staphylococcus aureus is more common in acute postoperative infections, and E. coli is associated with infections of the urinary tract. Streptococcus species are less common.
REFERENCE: Barrack RL, Booth RE Jr, Lonner JH, et al (eds): Orthopaedic Knowledge Update: Hip and Knee Reconstruction 3. Rosemont, IL American Academy of Orthopedic Surgeons, 2006, pp 475-503.
Figure 82
REFERENCE: Barrack RL, Booth RE Jr, Lonner JH, et al (eds): Orthopaedic Knowledge Update: Hip and Knee Reconstruction 3. Rosemont, IL American Academy of Orthopedic Surgeons, 2006, pp 475-503.
Figure 82
Question 3High Yield
..Numbness after his first dislocation was related to
Explanation
- His activity levels after surgery
PREFERRED RESPONSE: 4- sensory axillary nerve palsy from his dislocation.
PREFERRED RESPONSE: 4- sensory axillary nerve palsy from his dislocation.
Question 4High Yield
At the time of revision total knee arthroplasty, the surgeon is trialing the knee and finds that it extends fully and is stable in flexion with a 23-mm trial spacer; however, the patella is impinging on the polyethylene spacer. No augments were used on the femur or the tibia because the components fit well without them. What is the most appropriate action at this time?
Explanation
DISCUSSION: The surgeon in this case is faced with a common scenario at the time of revision total knee arthroplasty and the tendency is to elevate the joint line. Elevation of the joint line is associated with deleterious effects including anterior knee pain, restricted knee flexion, and instability. The error that has been made is resting the femoral component on the bone that is left behind after removal of the prior component; this typically leads to a femoral component that is too small (leading to an enlarged flexion gap) and proximal to where it should be (enlarging the extension gap). Although the flexion and extension gaps are equivalent, joint line elevation has occurred. To correct this problem, the femoral component size should be increased or offset posteriorly (to decrease the size of the flexion gap) and distal femoral augments should be used to decrease the size of the extension gap and restore the joint line to the appropriate level.
REFERENCES: Laskin RS: Joint line position restoration during revision total knee replacement. Clin Orthop Relat Res 2002;404:169-171.
Yoshii I, Whiteside LA, White SE, et al: Influence of prosthetic joint line position on knee kinematics and patellar position. J Arthroplasty 1991;6:169-177.
Barrack RL, Booth RE Jr, Lonner JH, et al (eds): Orthopaedic Knowledge Update: Hip and Knee Reconstruction
3. ### Rosemont, IL, American Academy of Orthopaedic Surgeons, 2006, pp 123-145. Question 100
A 68-year-old woman is undergoing a cementless medial/lateral tapered femoral placement during a total hip arthroplasty and the surgeon notices a small crack forming in the anteromedial femoral neck with final implant insertion. The most appropriate management should include which of the following?
1. ### Placement of a cerclage cable around the femoral neck above the lesser trochanter
2. ### Removal of the implant, placement of a cable around the femoral neck above the lesser trochanter, and reinsertion of the implant
3. ### Removal of the press-fit implant and cementing of the same femoral stem
4. ### Final seating of the cementless femoral component without additional measures
5. ### Removal of the cementless femoral component and placement of a revision modular taper- fluted femoral stem
PREFERRED RESPONSE: 2
DISCUSSION: The recognized treatment of the proximal periprosthetic fracture is first to identify its extent and then to optimize the correction. Removing the implant seems logical to accomplish the identification. Several studies indicate that proximal cerclage wiring is adequate to create a “barrel hoop” stability of the proxima l femur. The postoperative management may also include protected weight bearing and periodic radiographs.
REFERENCES: Barrack RL, Booth RE Jr, Lonner JH, et al (eds): Orthopaedic Knowledge Update: Hip and Knee Reconstruction 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2006, pp 475503.
Warren PJ, Thompson P, Fletcher MD: Transfemoral implantation of the Wagner SL stem: The abolition of
subsidence and enhancement of osteotomy union rate using Dall-Miles cables. Arch Orthop Trauma Surg 2002;122:557-560.
_Your Source for Lifelong Orthopaedic Learning_
DISCUSSION: The surgeon in this case is faced with a common scenario at the time of revision total knee arthroplasty and the tendency is to elevate the joint line. Elevation of the joint line is associated with deleterious effects including anterior knee pain, restricted knee flexion, and instability. The error that has been made is resting the femoral component on the bone that is left behind after removal of the prior component; this typically leads to a femoral component that is too small (leading to an enlarged flexion gap) and proximal to where it should be (enlarging the extension gap). Although the flexion and extension gaps are equivalent, joint line elevation has occurred. To correct this problem, the femoral component size should be increased or offset posteriorly (to decrease the size of the flexion gap) and distal femoral augments should be used to decrease the size of the extension gap and restore the joint line to the appropriate level.
REFERENCES: Laskin RS: Joint line position restoration during revision total knee replacement. Clin Orthop Relat Res 2002;404:169-171.
Yoshii I, Whiteside LA, White SE, et al: Influence of prosthetic joint line position on knee kinematics and patellar position. J Arthroplasty 1991;6:169-177.
Barrack RL, Booth RE Jr, Lonner JH, et al (eds): Orthopaedic Knowledge Update: Hip and Knee Reconstruction
3. ### Rosemont, IL, American Academy of Orthopaedic Surgeons, 2006, pp 123-145. Question 100
A 68-year-old woman is undergoing a cementless medial/lateral tapered femoral placement during a total hip arthroplasty and the surgeon notices a small crack forming in the anteromedial femoral neck with final implant insertion. The most appropriate management should include which of the following?
1. ### Placement of a cerclage cable around the femoral neck above the lesser trochanter
2. ### Removal of the implant, placement of a cable around the femoral neck above the lesser trochanter, and reinsertion of the implant
3. ### Removal of the press-fit implant and cementing of the same femoral stem
4. ### Final seating of the cementless femoral component without additional measures
5. ### Removal of the cementless femoral component and placement of a revision modular taper- fluted femoral stem
PREFERRED RESPONSE: 2
DISCUSSION: The recognized treatment of the proximal periprosthetic fracture is first to identify its extent and then to optimize the correction. Removing the implant seems logical to accomplish the identification. Several studies indicate that proximal cerclage wiring is adequate to create a “barrel hoop” stability of the proxima l femur. The postoperative management may also include protected weight bearing and periodic radiographs.
REFERENCES: Barrack RL, Booth RE Jr, Lonner JH, et al (eds): Orthopaedic Knowledge Update: Hip and Knee Reconstruction 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2006, pp 475503.
Warren PJ, Thompson P, Fletcher MD: Transfemoral implantation of the Wagner SL stem: The abolition of
subsidence and enhancement of osteotomy union rate using Dall-Miles cables. Arch Orthop Trauma Surg 2002;122:557-560.
_Your Source for Lifelong Orthopaedic Learning_
Question 5High Yield
Which of the following has been shown to have similar biochemical and clinical characteristics as iliac crest autograft?
Explanation
In multiple studies, femoral intramedullary reaming debris has been shown to have similar biochemical characteristics as iliac crest autograft. Intramedullary reaming products have osteogenic potential with viable cells while BMP's are osteoinductive cytokines.
Hoegel et al found that the reamings had alkaline phospatase activity, indicating living osteoblasts. The amount of activity was independent of the reamer sizes and reamer design.
Frolke et al concluded that reaming debris supports callus building (healing) as much as conventional iliac crest bone grafting in an animal fracture gap model.
The video shows a retrograde femoral autograft harvest using the RIA system.
Hoegel et al found that the reamings had alkaline phospatase activity, indicating living osteoblasts. The amount of activity was independent of the reamer sizes and reamer design.
Frolke et al concluded that reaming debris supports callus building (healing) as much as conventional iliac crest bone grafting in an animal fracture gap model.
The video shows a retrograde femoral autograft harvest using the RIA system.
Question 6High Yield
A 24-year-old man presents for treatment of a painful fifth toe deformity. He had the deformity for 10 years and notes that it is getting progressively worse. On examination, a claw toe deformity is present. There is 90° of fixed hyperextension of the metatarsophalangeal joint, 70° of flexion at the interphalangeal joint, and a painful corn on the distal tip of the phalanx. The patient would like surgical correction. Which procedure is most likely to give him relief of pain and correction of deformity:
Explanation
C orrection of a fixed claw fifth toe deformity is not an easy procedure. The customary procedures used for correction of other lesser toe deformities are not always successful. In this patient, PIP arthroplasty or arthrodesis alone will not correct this deformity. The deformity requires a subtotal or complete proximal phalangectomy. Although this procedure corrects the deformity, patients must know that they will inevitably have a floppy fifth toe.
Question 7High Yield
Which level has the smallest pedicle diameter?
Explanation
_
From proximal to distal, pedicle sizes decrease from T1 to roughly the T4-T6 level, and then pedicle size increases in diameter. L1 is typically smaller than T12. The diameter, however, continues to increase in the lumbar spine and the sacrum.
RECOMMENDED READINGS
26. [Scoles PV, Linton AE, Latimer B, Levy ME, Digiovanni BF. Vertebral body and posterior element morphology: the normal spine in middle life. Spine (Phila Pa 1976). 1988 Oct;13(10):1082-6. PubMed PMID: 3206263. ](http://www.ncbi.nlm.nih.gov/pubmed/3206263)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/3206263)
27. [Ofiram E, Polly DW, Gilbert TJ Jr, Choma TJ. Is it safer to place pedicle screws in the lower thoracic spine than in the upper lumbar spine? Spine (Phila Pa 1976). 2007 Jan 1;32(1):49-54. PubMed PMID: 17202892. ](http://www.ncbi.nlm.nih.gov/pubmed/17202892)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/17202892)
28. [Christodoulou AG, Apostolou T, Ploumis A, Terzidis I, Hantzokos I, Pournaras J. Pedicle dimensions of the thoracic and lumbar vertebrae in the Greek population. Clin Anat. 2005 Sep;18(6):404-8. PubMed PMID: 16015613. ](http://www.ncbi.nlm.nih.gov/pubmed/16015613)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/16015613)
RESPONSES FOR QUESTIONS 80 THROUGH 86
1. Well-fixed cemented stem
2. Well-fixed uncemented stem
3. Well-fixed uncemented stem with femoral osteolysis
4. Well-fixed uncemented stem with stress shielding
5. Loose cemented stem
6. Loose uncemented stem
For each image below, select the above response that best describes the femoral component.
From proximal to distal, pedicle sizes decrease from T1 to roughly the T4-T6 level, and then pedicle size increases in diameter. L1 is typically smaller than T12. The diameter, however, continues to increase in the lumbar spine and the sacrum.
RECOMMENDED READINGS
26. [Scoles PV, Linton AE, Latimer B, Levy ME, Digiovanni BF. Vertebral body and posterior element morphology: the normal spine in middle life. Spine (Phila Pa 1976). 1988 Oct;13(10):1082-6. PubMed PMID: 3206263. ](http://www.ncbi.nlm.nih.gov/pubmed/3206263)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/3206263)
27. [Ofiram E, Polly DW, Gilbert TJ Jr, Choma TJ. Is it safer to place pedicle screws in the lower thoracic spine than in the upper lumbar spine? Spine (Phila Pa 1976). 2007 Jan 1;32(1):49-54. PubMed PMID: 17202892. ](http://www.ncbi.nlm.nih.gov/pubmed/17202892)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/17202892)
28. [Christodoulou AG, Apostolou T, Ploumis A, Terzidis I, Hantzokos I, Pournaras J. Pedicle dimensions of the thoracic and lumbar vertebrae in the Greek population. Clin Anat. 2005 Sep;18(6):404-8. PubMed PMID: 16015613. ](http://www.ncbi.nlm.nih.gov/pubmed/16015613)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/16015613)
RESPONSES FOR QUESTIONS 80 THROUGH 86
1. Well-fixed cemented stem
2. Well-fixed uncemented stem
3. Well-fixed uncemented stem with femoral osteolysis
4. Well-fixed uncemented stem with stress shielding
5. Loose cemented stem
6. Loose uncemented stem
For each image below, select the above response that best describes the femoral component.
Question 8High Yield
Slide 1 Slide 2
The following image (Slide 1) depicts:
The following image (Slide 1) depicts:
Explanation
The image depicts the harvesting of a vascularized fibula from the contralateral leg, which is then used to move a defect in congenital pseudoarthrosis of the tibia on the opposite side. The following image (Slide 2) shows clinical union 3.5 years later
Question 9High Yield
Posterior lumbar spine arthrodesis may be associated with adjacent segment degeneration cephalad or caudad to the fusion segment. Which of the following is the predicted rate of symptomatic degeneration at an adjacent segment warranting either decompression and/or arthrodesis at 5 to 10 years after lumbar fusion?
Explanation
Ghiselli and associates described a rate of symptomatic degeneration at an adjacent segment warranting either decompression or arthrodesis to be 16.5% at 5 years and 36.1% at 10 years based on a Kaplan-Meier analysis.
Question 49 Halo treatment for preadolescent children typically requires the use of which of the following?
1. # 4 to 6 pins with an insertional torque of 1 to 5 in-lb
2. # 4 to 6 pins with an insertional torque of 4 to 6 in-lb
3. # 4 to 6 pins with an insertional torque of 6 to 8 in-lb
4. # 8 to 12 pins with an insertional torque of 1 to 5 in-lb
5. # 8 to 12 pins with an insertional torque of 4 to 6 in-lb
DISCUSSION: The complication rate with halo vest treatment in children is reported to be as high as 68% in contrast to a 36% complication rate in adults. These complications include not only pin tract infections,but also skull penetration. Multiple pins allow for the early removal of pins without fixation consequences should pin site infections begin to develop. Moreover, there is significant variability in the insertional torque applied by a variety halo pin torque wrenches, including those from the same manufacturer.
Consequently, the use of a large number of pins (8 to 12) placed a very low insertional torque (1 to 5 in-lb) in children is recommended. A CT scan of the head should also be considered to assess for the thickest areas of the skull suitable for pin application. PR: 4
Question 49 Halo treatment for preadolescent children typically requires the use of which of the following?
1. # 4 to 6 pins with an insertional torque of 1 to 5 in-lb
2. # 4 to 6 pins with an insertional torque of 4 to 6 in-lb
3. # 4 to 6 pins with an insertional torque of 6 to 8 in-lb
4. # 8 to 12 pins with an insertional torque of 1 to 5 in-lb
5. # 8 to 12 pins with an insertional torque of 4 to 6 in-lb
DISCUSSION: The complication rate with halo vest treatment in children is reported to be as high as 68% in contrast to a 36% complication rate in adults. These complications include not only pin tract infections,but also skull penetration. Multiple pins allow for the early removal of pins without fixation consequences should pin site infections begin to develop. Moreover, there is significant variability in the insertional torque applied by a variety halo pin torque wrenches, including those from the same manufacturer.
Consequently, the use of a large number of pins (8 to 12) placed a very low insertional torque (1 to 5 in-lb) in children is recommended. A CT scan of the head should also be considered to assess for the thickest areas of the skull suitable for pin application. PR: 4
Question 10High Yield
Which surgical approach will provide the most exposure and pose the lowest risk?
Explanation
- Lateral and medial approach with a medial malleolar osteotomy, if needed_
Question 11High Yield
Intra-articular steroids change synovial fluid characteristincs by:
Explanation
Intra-articular steroids change synovial fluid characteristics by increasing hyaluroniCacid concentration
Question 12High Yield
A 26-year-old weightlifter has increasing pain in his left shoulder for 4 months. Nonsurgical treatment
consisting of anti-inflammatory medication, corticosteroid injections, and rest fails to alleviate his symptoms. He undergoes an arthroscopic distal clavicle resection with excision of the distal 8 mm of clavicle (Mumford procedure). Three months after surgery, he reports mild pain and popping by his clavicle. His clavicle demonstrates mild posterior instability on examination without any obvious deformity on his radiographs. What structures were compromised during his excision?
consisting of anti-inflammatory medication, corticosteroid injections, and rest fails to alleviate his symptoms. He undergoes an arthroscopic distal clavicle resection with excision of the distal 8 mm of clavicle (Mumford procedure). Three months after surgery, he reports mild pain and popping by his clavicle. His clavicle demonstrates mild posterior instability on examination without any obvious deformity on his radiographs. What structures were compromised during his excision?
Explanation
The posterior and superior acromioclavicular ligaments provide the most restraint to posterior translation of the acromioclavicular joint and must be preserved during a Mumford procedure. Anterior and superior acromioclavicular joint ligaments are the opposite of the preferred response and prevent anterior translation of the clavicle. Injuries to the conoid and trapezoid ligaments are more pronounced with grade III or higher acromioclavicular separations, with superior migration of the clavicle relative to the acromion.
Question 13High Yield
Figures 35a and 35b show the radiographs of a 20-year-old man who is unable to rotate his dominant forearm. Examination reveals that the arm is fixed in supination. To regain motion, management should consist of
Explanation
The patient has a proximal synostosis; therefore, resection of the synostosis is considered the best option to regain motion. While forearm osteotomy can place the hand in a more functional position, rotation will not be restored. Proximal radial excision can provide forearm rotation; however, this procedure is reserved for patients who have a proximal radioulnar synostosis that is too extensive to allow a safe resection, involves the articular surface, and is associated with an anatomic deformity. Motion will not be restored with dynamic splinting.
REFERENCES: Kamineni S, Maritz NG, Morrey BF: Proximal radial resection for posttraumatic radioulnar synostosis: A new technique to improve forearm rotation. J Bone Joint Surg Am 2002;84:745-751.
Jupiter JB, Ring D: Operative treatment of post-traumatic proximal radioulnar synostosis.
J Bone Joint Surg Am 1998;80:248-257.
REFERENCES: Kamineni S, Maritz NG, Morrey BF: Proximal radial resection for posttraumatic radioulnar synostosis: A new technique to improve forearm rotation. J Bone Joint Surg Am 2002;84:745-751.
Jupiter JB, Ring D: Operative treatment of post-traumatic proximal radioulnar synostosis.
J Bone Joint Surg Am 1998;80:248-257.
Question 14High Yield
Following palmar fasciectomy for Dupuytren contracture performed under general anesthesia, the tourniquet is released and the surgical finger remains pale and cool to touch. The next appropriate steps are to flex the digit, warm the digit, and
Explanation
- apply topical lidocaine._
Question 15High Yield
Which subtype of Ehlers-Danlos syndrome (EDS) is caused by lysyl hydroxylase deficiency:
Explanation
Many of the mutations responsible for the differing subtypes of Ehlers-Danlos syndrome (EDS) have not been identified (EDS types I, II, and III). Lysyl hydroxylase deficiency has been identified as the cause of type IV. A mutation in type I collagen has been identified as the cause of EDS VII.
Question 16High Yield
A 50-year-old man who underwent an arthroscopic rotator cuff repair 5 days ago now returns for an early postoperative follow-up because of increasing pain in his shoulder. He reports increasing malaise and has a low-grade fever. Examination reveals no redness or swelling, but he has scant serous drainage from the posterior portal. An emergent Gram stain is positive for gram-positive cocci. The next most appropriate step in management should consist of
Explanation
An infection of the shoulder is considered a surgical emergency unless there are medical reasons that a patient cannot be taken to the operating room. If cultures of wound drainage are in question, then an aspiration should be done emergently, not several days later. The hallmark of infection in any major joint is increasing pain out of proportion to what is expected. Drainage occurring 1 to 2 days after an arthroscopic procedure is not normal, and it should be aggressively treated. Delay in diagnosis can result in sepsis and on a delayed basis, postinfectious arthritis. Both the glenohumeral joint and the subacromial space require debridement and irrigation, followed by antibiotics after both areas are cultured.
REFERENCES: Mansat P, Cofield RH, Kersten TE, Rowland CM: Complications of rotator cuff repair. Orthop Clin North Am 1997;28:205-213.
Settecerri JJ, Pitner MA, Rock MG, Hanssen AD, Cofield RH: Infection after rotator cuff repair. J Shoulder Elbow Surg 1999;8:1-5.
Ward WG, Eckardt JJ: Subacromial/subdeltoid bursa abscesses: An overlooked diagnosis. Clin Orthop 1993;288:189-194.
Ward WG, Goldner RD: Shoulder pyarthrosis: A concomittant process. Orthopedics 1994;17:591-595.
REFERENCES: Mansat P, Cofield RH, Kersten TE, Rowland CM: Complications of rotator cuff repair. Orthop Clin North Am 1997;28:205-213.
Settecerri JJ, Pitner MA, Rock MG, Hanssen AD, Cofield RH: Infection after rotator cuff repair. J Shoulder Elbow Surg 1999;8:1-5.
Ward WG, Eckardt JJ: Subacromial/subdeltoid bursa abscesses: An overlooked diagnosis. Clin Orthop 1993;288:189-194.
Ward WG, Goldner RD: Shoulder pyarthrosis: A concomittant process. Orthopedics 1994;17:591-595.
Question 17High Yield
What is the most appropriate treatment?
Explanation
- Total-contact casting
Question 18High Yield
Internal impingement is characterized by which of the following anatomic lesions?

Explanation
DISCUSSION: Internal impingement is characterized by articular-sided partial-thickness rotator cuff tears and superior glenoid labral tears. The capsule is characterized by laxity anteriorly and tightness posteriorly.
Scientific References
- : Garrick JG (ed): Orthopaedic Knowledge Update: Sports Medicine 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2004, p 82.
Burkhart SS, Morgan CD, Kibler WB: The disabled throwing shoulder: Spectrum of pathology. Part I:
Pathoanatomy and biomechanics. Arthroscopy 2003;19:404-420.
Figure 27
Question 19High Yield
The mean C obb measurement for idiopathic scoliosis curves with a 7° angle of trunk rotation (ATR) is:
Explanation
Although the angle of trunk rotation (ATR) does not convert directly to a C obb angle, there are population-based figures for mean curve at each ATR. The mean C obb angle for curves having a 7° ATR is 20°.
Question 20High Yield
In an asymptomatic athlete, what condition represents an absolute contraindication to returning to contact or collision sports?
Explanation
The one overriding principle regarding the return to any collision sport, as Torg and associates has described, is that the athlete be "neurologically intact, asymptomatic, and pain-free and have full strength and full cervical range of motion". Forces exerted on the cervical spine can be absorbed by the "elasticity of the intervertebral disk, the mobility of the spine itself, and the impact of absorbing capabilities of the cervical paravertebral musculature". The C1 and C2 levels (atlanto-occipital level) control movement of the skull and articulate the large motion movements. Specifically, partial or complete 56
congenital fusion of the atlas to the base of the occiput results in progressive cord compression by the posterior lip of the foramen magnum. It can result in sudden death.
A cervical disk herniation that was previously treated nonsurgically and is not causing cord compression in the currently asymptomatic patient is not a contraindication to return to collision sports. Spina bifida occulta is common (10-20% of healthy individuals). It is typically an incidental finding and does not result in neurologic problems. If individuals have a healed anterior, lateral or posterior disk herniation that is treated nonsurgically and they are currently asymptomatic, then there is no contraindication to participation in contact sports. If they require a diskectomy and fusion and they have a solid/healed fusion, are asymptomatic and neurologically intact with full and pain-free range of motion, then there is no contraindication to return to collision sports. An acute disk herniation, a disk herniation with associated pain or neurologic symptoms, or the presence of cord compression or loss of normal lordosis are all contraindications.
congenital fusion of the atlas to the base of the occiput results in progressive cord compression by the posterior lip of the foramen magnum. It can result in sudden death.
A cervical disk herniation that was previously treated nonsurgically and is not causing cord compression in the currently asymptomatic patient is not a contraindication to return to collision sports. Spina bifida occulta is common (10-20% of healthy individuals). It is typically an incidental finding and does not result in neurologic problems. If individuals have a healed anterior, lateral or posterior disk herniation that is treated nonsurgically and they are currently asymptomatic, then there is no contraindication to participation in contact sports. If they require a diskectomy and fusion and they have a solid/healed fusion, are asymptomatic and neurologically intact with full and pain-free range of motion, then there is no contraindication to return to collision sports. An acute disk herniation, a disk herniation with associated pain or neurologic symptoms, or the presence of cord compression or loss of normal lordosis are all contraindications.
Question 21High Yield
Figure 2 shows the radiograph of a 26-year-old auto mechanic who injured his right dominant elbow in a fall during a motocross race. Examination reveals pain and catching that limits his range of motion to 45 degrees of supination and 20 degrees of pronation. The interosseous space and distal radioulnar joint are stable. Management should
consist of
consist of
Explanation
The radial head is an important secondary stabilizer of the elbow, helping to resist valgus forces. There has been a movement toward open reduction and internal fixation of the radial head when technically feasible, especially in a relatively high-demand athlete or laborer. The examination and radiograph suggest that displacement of the fragment is great enough to create a mechanical block. Extended splinting would only serve to encourage arthrofibrosis. Early range of motion is appropriate if there is minimal displacement of the radial head fragement, it is stable, and there is no mechanical block to motion. Fragments larger than one third of the joint surface should be excised only if it is not possible to reduce and repair the fragment. Primary excision of the radial head should be avoided if possible. Complications after excision of the radial head include muscle weakness, wrist pain, valgus elbow instability, heterotopic ossification, and arthritis.
REFERENCES: Hotchkiss RN: Displaced fractures of the radial head: Internal fixation or excision? J Am Acad Orthop Surg 1997;5:1-10.
Esser RD, Davis S, Taavao T: Fractures of the radial head treated by internal fixation: Late results in 26 cases. J Orthop Trauma 1995;9:318-323.
REFERENCES: Hotchkiss RN: Displaced fractures of the radial head: Internal fixation or excision? J Am Acad Orthop Surg 1997;5:1-10.
Esser RD, Davis S, Taavao T: Fractures of the radial head treated by internal fixation: Late results in 26 cases. J Orthop Trauma 1995;9:318-323.
Question 22High Yield
What are the five major compartments of the foot?
Explanation
The five major compartments of the foot are medial, lateral, central, interosseous, and calcaneal. There is no dorsal compartment in the foot.
REFERENCES: Mizel MS, Miller RA, Scioli MW (eds): Orthopaedic Knowledge Update: Foot and Ankle 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1998, pp 262-264.
Shereff MJ: Compartment syndromes of the foot. Instr Course Lect 1990;39:127-132.
REFERENCES: Mizel MS, Miller RA, Scioli MW (eds): Orthopaedic Knowledge Update: Foot and Ankle 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1998, pp 262-264.
Shereff MJ: Compartment syndromes of the foot. Instr Course Lect 1990;39:127-132.
Question 23High Yield
When performing capsular releases during shoulder arthroplasty for the treatment of glenohumeral joint osteoarthritis, what anatomic landmark indicates the location of the axillary nerve as it begins to travel from anterior to posterior?
Explanation
The axillary nerve originates from the posterior cord of the brachial plexus. It passes down the anteroinferior aspect of the subscapularis, courses posteriorly beneath the glenoid and inferior capsule, then wraps around the humerus from posterior to anterior on the deep surface of the deltoid. In the setting of glenoid and humeral head deformity, the inferior border of the subscapularis can be a useful landmark to ensure the nerve is appropriately protected intraoperatively.
Question 24High Yield
Figures 1 through 3 are the radiographs of a 55-year-old woman who fell on her outstretched right arm, resulting in acute elbow pain and swelling. On examination, she has lateral elbow bruising and tenderness, with a mechanical block to forearm supination and pronation. She has no medial tenderness. During surgery through a direct lateral approach, the surgeon observes a completely bare lateral epicondyle and surgical repair is performed, resulting in a stable and congruent joint. Initial postoperative rehabilitation should include
Explanation
Radial head fractures are thought to occur as a result of valgus posterolateral rotary load across the elbow, although the mechanism can certainly vary. Minimally or nondisplaced fractures without any clinical instability or block to motion can often be successfully managed non-surgically. Fractures with >2 mm of displacement or fragments that block motion require surgical repair. A critical aspect during surgery is identifying concomitant injury to the lateral collateral ligament complex (LCL). When encountered, the LCL is most often avulsed from its origin at the lateral epicondyle, resulting in a bare area. After the radial head is either repaired or replaced (Figures 4 and 5), the LCL should
16
be repaired back to its anatomic origin. Postoperatively, the surgeon must communicate to the therapist that elbow extension exercises should be performed with the forearm in pronation as a result of the compromised LCL, as this position places the least stress on the ligamentous repair. Elbow extension exercises in supination or neutral are recommended for compromise of the medial collateral ligament, or combined medial and lateral ligament injury, respectively. Without any medial elbow bruising, swelling, or tenderness, it is unlikely that the patient has an injury to the medial collateral ligament.
16
be repaired back to its anatomic origin. Postoperatively, the surgeon must communicate to the therapist that elbow extension exercises should be performed with the forearm in pronation as a result of the compromised LCL, as this position places the least stress on the ligamentous repair. Elbow extension exercises in supination or neutral are recommended for compromise of the medial collateral ligament, or combined medial and lateral ligament injury, respectively. Without any medial elbow bruising, swelling, or tenderness, it is unlikely that the patient has an injury to the medial collateral ligament.
Question 25High Yield
A 26-year-old man underwent excision of a ganglion cyst of the tibiofibular joint 1 year ago. It has now recurred and is extremely symptomatic. Nonsurgical management has failed to provide relief. What type of surgery provides the most predictable results for this patient?
Explanation
DISCUSSION: Recurrence of a ganglion cyst of the tibiofibular joint is most successfully treated by proximal tibiofibular joint fusion. A repeat excision will most likely result in recurrence of the cyst. Total or partial excision may lead to instability of the posterolateral structures of the knee. Interpositional arthroplasty has not been proven to be effective for the treatment of recurrent ganglion cysts of the proximal tibiofibular joint.
REFERENCES: Miskovsky S, Kaeding C, Weis L: Proximal tibiofibular joint ganglion cysts: Excision, recurrence, and joint arthrodesis. Am J Sports Med 2004;32:1022-1028.
Vatansever A, Bal E, Okcu G: Ganglion cysts of the proximal tibiofibular joint review of literature with three case reports. Arch Orthop Trauma Surg 2006;126:637-640.
REFERENCES: Miskovsky S, Kaeding C, Weis L: Proximal tibiofibular joint ganglion cysts: Excision, recurrence, and joint arthrodesis. Am J Sports Med 2004;32:1022-1028.
Vatansever A, Bal E, Okcu G: Ganglion cysts of the proximal tibiofibular joint review of literature with three case reports. Arch Orthop Trauma Surg 2006;126:637-640.
Question 26High Yield
A 21-year-old collegiate female cross-country athlete reports right hip pain that begins about 12 miles into a run, followed by pain resolution when she discontinues running. However, each time she tries to resume a running program, she experiences recurrence of pain deep in the anterior groin. A plain radiograph and MRI scan are shown in Figures 8a and 8b. Management should consist of
Explanation
The history is consistent with a stress fracture. Findings on the plain radiograph are marginal, but the MRI scan shows evidence of stress reaction in the medial neck of the femur (compression side). A lesion on the compression side is not normally at risk for displacement and usually can be managed nonsurgically. A bone scan would further identify the lesion but is not necessary. A skeletal survey and chest radiograph are used in staging a tumor. Radioisotope injection and guided biopsy are sometimes used for osteoid osteomas.
REFERENCES: Boden BP, Osbahr DC: High-risk stress fractures: Evaluation and treatment. J Am Acad Orthop Surg 2000;8:344-353.
Lynch SA, Renstrom PA: Groin injuries in sport: Treatment strategies. Sports Med 1999;28:137-144.
REFERENCES: Boden BP, Osbahr DC: High-risk stress fractures: Evaluation and treatment. J Am Acad Orthop Surg 2000;8:344-353.
Lynch SA, Renstrom PA: Groin injuries in sport: Treatment strategies. Sports Med 1999;28:137-144.
Question 27High Yield
Which of the following lesions would display a low to moderate signal on T1 weighted images and high signal on T2 weighted images:
Explanation
All soft tissue sarcomas have the same signal sequence - low on T1 weighted images and high on T2 weighted images.
| Tissue | T1 weighted | T2 weighted |
|---|---|---|
| Fat | High | Moderate |
| Tendons | Low | Low |
| Ligaments | Low | Low |
| Fascial layers | Low | Low |
| Cortical bone | Low | Low |
| Muscle | Moderate | Moderate |
| Normal marrow | High | Moderate |
| Soft tissue sarcomas | Low | High |
| Fluid (ganglions, effusions) | Low | High |
| Pigmented villonodular synovitis* | Very low | Very low |
Question 28High Yield
The underlying cause of the neoplasm is
Explanation
The bone scan reveals multiple bone lesions, which does not rule out any of the responses. The radiographs reveal dysplastic bone with a “ground glass” appearance, suggesting fibrous dysplasia as the preferred response. Multiple myeloma typically demonstrates purely lytic, “punched out” lesions and would be highly unusual in a 23-year-old woman. Multiple hereditary exostosis would demonstrate more expansile lesions concentrated in the metaphysis. Metastatic carcinoma could have a lytic or blastic appearance but is less likely to occur in a 23-year-old woman.
McCune-Albright syndrome in polyostotic fibrous dysplasia is present in as many as 50% of patients and should be evaluated for during an endocrine consultation. Adrenal, pituitary, parathyroid, and thyroid endocrinopathies may be present. Untreated hyperthyroidism can be life threatening during a surgical procedure. There is no indication to repeat the nuclear bone scan. Although phosphate wasting and, rarely, oncogenic osteomalacia have been reported in polyostotic fibrous dysplasia, an endocrinology consultation always should be sought.
Café au lait macules are the most common extraskeletal manifestation of fibrous dysplasia, often referred to as “coast of Maine” in appearance because of their irregular borders (in comparison to the “Coast of California” with smooth borders as seen in neurofibromatosis). Multiple myeloma would not ordinarily appear with increased uptake on a bone scan unless a pathologic fracture of some duration were present. A long area of bone involvement would not appear in patients with metastatic lung adenocarcinoma.
An ALK rearrangement occurs in nonsmall-cell lung cancer. The translocation t(11;14)(q13;q32) should be recognized as a poor prognosticator in multiple myeloma. The germline alteration in EXT1 and EXT2 occurs in multiple hereditary exostosis.
All forms of fibrous dysplasia are caused by a nongerm-cell mutation that occurs during early embryogenesis. A missense mutation of the GNAS1 gene, which encodes the alpha subunit of the stimulatory G-protein-couple-receptor, Gs alpha, results in G-protein activation and the production of cyclic adenosine monophosphate affecting melanocytes, endocrine cells, and osteoprogenitor cells.
RECOMMENDED READINGS
1. [DiCaprio MR, Enneking WF. Fibrous dysplasia. Pathophysiology, evaluation, and treatment. J Bone Joint Surg Am. 2005 Aug;87(8):1848-64. Review.](http://www.ncbi.nlm.nih.gov/pubmed/16085630)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/16085630)
2. [Parekh SG, Donthineni-Rao R, Ricchetti E, Lackman RD. Fibrous dysplasia. J Am Acad Orthop Surg. 2004 Sep-Oct;12(5):305-13. Review. PubMed PMID: 15469225. ](http://www.ncbi.nlm.nih.gov/pubmed/15469225)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/15469225)
3. [Shin HJ, Kim K, Lee JJ, Song MK, Lee EY, Park SH, Kim SH, Jang MA, Kim SJ, Chung JS. The t(11;14)(q13;q32) translocation as a poor prognostic parameter for autologous stem cell transplantation in myeloma patients with extramedullary plasmacytoma. Clin Lymphoma Myeloma Leuk. 2015 Apr;15(4):227-35. doi: 10.1016/j.clml.2014.12.007. Epub 2014 Dec 12.](http://www.ncbi.nlm.nih.gov/pubmed/25812994)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/25812994)
4. [Esfahani K, Agulnik JS, Cohen V. A Systemic Review of Resistance Mechanisms and Ongoing Clinical Trials in ALK-Rearranged Non-Small Cell Lung Cancer. Front Oncol. 2014 Jul 21;4:174. doi: 10.3389/fonc.2014.00174. eCollection 2014. Review. PubMed PMID: 25101240. ](http://www.ncbi.nlm.nih.gov/pubmed/25101240)[View Abstract at](http://www.ncbi.nlm.nih.gov/pubmed/25101240)[ ](http://www.ncbi.nlm.nih.gov/pubmed/25101240)[PubMed](http://www.ncbi.nlm.nih.gov/pubmed/25101240)
McCune-Albright syndrome in polyostotic fibrous dysplasia is present in as many as 50% of patients and should be evaluated for during an endocrine consultation. Adrenal, pituitary, parathyroid, and thyroid endocrinopathies may be present. Untreated hyperthyroidism can be life threatening during a surgical procedure. There is no indication to repeat the nuclear bone scan. Although phosphate wasting and, rarely, oncogenic osteomalacia have been reported in polyostotic fibrous dysplasia, an endocrinology consultation always should be sought.
Café au lait macules are the most common extraskeletal manifestation of fibrous dysplasia, often referred to as “coast of Maine” in appearance because of their irregular borders (in comparison to the “Coast of California” with smooth borders as seen in neurofibromatosis). Multiple myeloma would not ordinarily appear with increased uptake on a bone scan unless a pathologic fracture of some duration were present. A long area of bone involvement would not appear in patients with metastatic lung adenocarcinoma.
An ALK rearrangement occurs in nonsmall-cell lung cancer. The translocation t(11;14)(q13;q32) should be recognized as a poor prognosticator in multiple myeloma. The germline alteration in EXT1 and EXT2 occurs in multiple hereditary exostosis.
All forms of fibrous dysplasia are caused by a nongerm-cell mutation that occurs during early embryogenesis. A missense mutation of the GNAS1 gene, which encodes the alpha subunit of the stimulatory G-protein-couple-receptor, Gs alpha, results in G-protein activation and the production of cyclic adenosine monophosphate affecting melanocytes, endocrine cells, and osteoprogenitor cells.
RECOMMENDED READINGS
1. [DiCaprio MR, Enneking WF. Fibrous dysplasia. Pathophysiology, evaluation, and treatment. J Bone Joint Surg Am. 2005 Aug;87(8):1848-64. Review.](http://www.ncbi.nlm.nih.gov/pubmed/16085630)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/16085630)
2. [Parekh SG, Donthineni-Rao R, Ricchetti E, Lackman RD. Fibrous dysplasia. J Am Acad Orthop Surg. 2004 Sep-Oct;12(5):305-13. Review. PubMed PMID: 15469225. ](http://www.ncbi.nlm.nih.gov/pubmed/15469225)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/15469225)
3. [Shin HJ, Kim K, Lee JJ, Song MK, Lee EY, Park SH, Kim SH, Jang MA, Kim SJ, Chung JS. The t(11;14)(q13;q32) translocation as a poor prognostic parameter for autologous stem cell transplantation in myeloma patients with extramedullary plasmacytoma. Clin Lymphoma Myeloma Leuk. 2015 Apr;15(4):227-35. doi: 10.1016/j.clml.2014.12.007. Epub 2014 Dec 12.](http://www.ncbi.nlm.nih.gov/pubmed/25812994)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/25812994)
4. [Esfahani K, Agulnik JS, Cohen V. A Systemic Review of Resistance Mechanisms and Ongoing Clinical Trials in ALK-Rearranged Non-Small Cell Lung Cancer. Front Oncol. 2014 Jul 21;4:174. doi: 10.3389/fonc.2014.00174. eCollection 2014. Review. PubMed PMID: 25101240. ](http://www.ncbi.nlm.nih.gov/pubmed/25101240)[View Abstract at](http://www.ncbi.nlm.nih.gov/pubmed/25101240)[ ](http://www.ncbi.nlm.nih.gov/pubmed/25101240)[PubMed](http://www.ncbi.nlm.nih.gov/pubmed/25101240)
Question 29High Yield
..A 42-year-old woman has a posterior elbow dislocation. Closed reduction is performed, and the elbow appears stable under fluoroscopic examination. Further treatment should consist of
Explanation
- early mobilization only.
RESPONSES FOR QUESTIONS 12 THROUGH 16
RESPONSES FOR QUESTIONS 12 THROUGH 16
Question 30High Yield
A 30-year-old patient sustains a comminuted tibia fracture and is treated with minimally invasive plating, shown in Figure A. The patient returns to the office 2 weeks after the surgery and reports persistent numbness over most of the dorsum of the foot, but motor exam is normal. What is the most likely explanation?
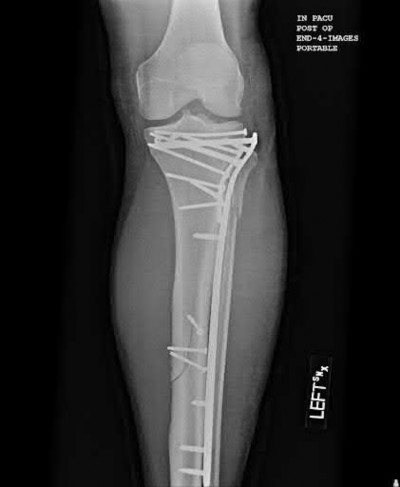
Explanation
Superficial peroneal nerve (SPN) injury is a known complication of percutaneous plating of proximal tibial fractures with the LISS system as seen in Figure A.
The Less Invasive Stabilization System (LISS) is a minimally invasive implant that uses indirect fracture reduction techniques. When using the LISS system, percutaneous screw placement increases the risk of injury to nearby structures because they are not necessarily visualized. The superficial peroneal nerve exits the superficial fascia of the leg approximately 8 cm above the tip of the
lateral malleolus. The nerve then travels from posterior to anterior in the vicinity of the distal aspect of the 13-hole proximal tibia LISS plate (near holes 11-13). In a patient of shorter stature, the nerve could cross the distal portion of a 9-hole plate.
Deangelis et al. performed a cadaveric study using Less Invasive Stabilization System (LISS) plates and found that the average distance from the SPN to the center of holes 11, 12, and 13 was 10.0 mm, 6.8 mm, and 2.7 mm respectively. They recommended using a larger incision and careful dissection down to the plate in this region to minimize the risk of damage to the nerve.
Cole et al. retrospectively reviewed 77 tibia fractures treated with LISS and found that 91% healed without complication. In their cohort, there were no superficial peroneal nerve palsies and one deep peroneal nerve palsy.
Figure A demonstrates AP and lateral x-rays of a tibial shaft fracture treated with a LISS plate.
Incorrect Answers:
A: compartment syndrome would have demonstrated pain out of proportion which the patient never complains of
B, D, and E are all less likely to be injured with LISS plate application than the superficial peroneal nerve.
The Less Invasive Stabilization System (LISS) is a minimally invasive implant that uses indirect fracture reduction techniques. When using the LISS system, percutaneous screw placement increases the risk of injury to nearby structures because they are not necessarily visualized. The superficial peroneal nerve exits the superficial fascia of the leg approximately 8 cm above the tip of the
lateral malleolus. The nerve then travels from posterior to anterior in the vicinity of the distal aspect of the 13-hole proximal tibia LISS plate (near holes 11-13). In a patient of shorter stature, the nerve could cross the distal portion of a 9-hole plate.
Deangelis et al. performed a cadaveric study using Less Invasive Stabilization System (LISS) plates and found that the average distance from the SPN to the center of holes 11, 12, and 13 was 10.0 mm, 6.8 mm, and 2.7 mm respectively. They recommended using a larger incision and careful dissection down to the plate in this region to minimize the risk of damage to the nerve.
Cole et al. retrospectively reviewed 77 tibia fractures treated with LISS and found that 91% healed without complication. In their cohort, there were no superficial peroneal nerve palsies and one deep peroneal nerve palsy.
Figure A demonstrates AP and lateral x-rays of a tibial shaft fracture treated with a LISS plate.
Incorrect Answers:
A: compartment syndrome would have demonstrated pain out of proportion which the patient never complains of
B, D, and E are all less likely to be injured with LISS plate application than the superficial peroneal nerve.
Question 31High Yield
An 80-year-old patient presents 8 months postoperatively with right groin pain. Examination reveals a leg length discrepancy of
1.5cm. Recent radiographs are seen in Figures A and B. What is the most appropriate treatment plan?
1.5cm. Recent radiographs are seen in Figures A and B. What is the most appropriate treatment plan?
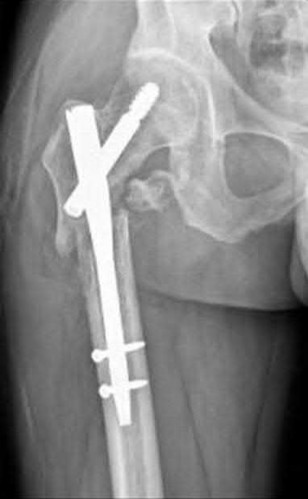
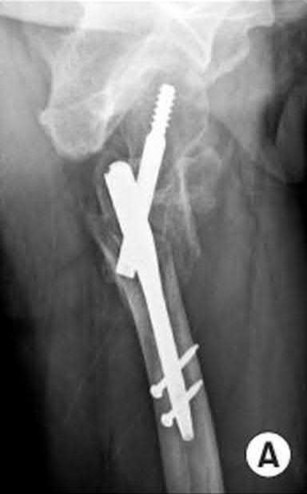
Explanation
This patient has atrophic non-union (NU) and varus collapse following cephalomedullary nailing of a subtrochanteric fracture. The ideal treatment involves nail removal, correction of alignment, fracture fixation, and bone grafting. Fixation can be achieved with a nail or plate.
Subtrochanteric fractures can be treated with cephalomedullary nailing or fixed angle plates. Nailing of these fractures is technically challenging because the fracture must be reduced prior to nail passage. Failure to do so leads to varus and procurvatum malreduction.
Bellabarba et al. reviewed plating of femoral nonunions after intramedullary nailing. Of 23 nonunions, 21 healed at an average of 12 weeks. The remaining 2 cases required repeat plating (at 2 and 8 weeks) for hardware breakage because of noncompliance with weightbearing restrictions. They advocate plating because it allows for correction of malalignment and provides a biomechanically superior tension band construct.
Incorrect Answers:
Answer 1:Dynamization is less effective in femoral NU compared with tibial NU. It is suitable for NU of axially stable fractures without significant angular deformity, particularly if statically locked in distraction. It is not suitable in this case because of varus collapse and shortening.
Answer 2: The use of tensioned wire fixators is poorly tolerated in the femur and has a high complication rate.
Answer 3: Reamed exchange nailing is the procedure of choice after IM nailing in the ABSENCE of femoral deformity. It is less effective in this case of varus collapse and shortening. Exchange unreamed nailing is not useful because (1) the new nail follows the same path as the old, making deformity correction impossible, and (2) the new nail cannot be larger than the old nail. A larger implant is only possible following reaming, especially if the isthmus is to be crossed.
Answer 4: Plating around a nail is inadvisable in this case because the existing hardware precludes deformity correction.
Subtrochanteric fractures can be treated with cephalomedullary nailing or fixed angle plates. Nailing of these fractures is technically challenging because the fracture must be reduced prior to nail passage. Failure to do so leads to varus and procurvatum malreduction.
Bellabarba et al. reviewed plating of femoral nonunions after intramedullary nailing. Of 23 nonunions, 21 healed at an average of 12 weeks. The remaining 2 cases required repeat plating (at 2 and 8 weeks) for hardware breakage because of noncompliance with weightbearing restrictions. They advocate plating because it allows for correction of malalignment and provides a biomechanically superior tension band construct.
Incorrect Answers:
Answer 1:Dynamization is less effective in femoral NU compared with tibial NU. It is suitable for NU of axially stable fractures without significant angular deformity, particularly if statically locked in distraction. It is not suitable in this case because of varus collapse and shortening.
Answer 2: The use of tensioned wire fixators is poorly tolerated in the femur and has a high complication rate.
Answer 3: Reamed exchange nailing is the procedure of choice after IM nailing in the ABSENCE of femoral deformity. It is less effective in this case of varus collapse and shortening. Exchange unreamed nailing is not useful because (1) the new nail follows the same path as the old, making deformity correction impossible, and (2) the new nail cannot be larger than the old nail. A larger implant is only possible following reaming, especially if the isthmus is to be crossed.
Answer 4: Plating around a nail is inadvisable in this case because the existing hardware precludes deformity correction.
Question 32High Yield
Noncemented femoral components must be able to resist translation and rotation in all of the following except:
Explanation
Implants must resist translation in the axial, medial-lateral, and anteroposterior planes, as well as resisting rotation in the parasagittal, transverse, and coronal planes
Question 33High Yield
A 6-year-old boy presents with a Salter-Harris II distal radius fracture 3 weeks after injury. He is nontender and neurologically intact. On radiographs, he has a 35º dorsal angulation. The appropriate course of treatment is:
Explanation
For a patient with delayed presentation of a distal radius fracture, appropriate management includes casting and observation for at least 2 years to assess physeal damage and remodeling. The patient may require osteotomy if remodeling does not occur.
Question 34High Yield
In either a ceramic-on-highly-cross-linked polyethylene (HXPE) or metal- on-HXPE component, increasing the ball head size leads to
Explanation
Increasing the size of the ball head increases the primary arc of motion prior to impingement and the jump distance prior to dislocation, assuming an acetabular component abduction of less than 90 degrees. Although HXPE has demonstrated decreases in linear wear rates even with ball head sizes larger than 28 mm, volumetric wear remains a concern. A larger ball head size does not significantly change offset, and larger metal ball heads are not associated with decreased risk for corrosion.
3
3
Question 35High Yield
Which characteristic of complex regional pain syndrome (CRPS) type 2 differentiates it from CRPS 1?
Explanation
CRPS 2 develops after nerve injury, whereas CRPS 1 occurs without nerve injury. The diagnostic criteria are otherwise the same for the 2 conditions. A 3-phase bone scan can be helpful; a pattern of increased uptake in all 3 phases, and particularly diffuse periarticular uptake in and around the joints of the affected extremity during the delayed phase, is considered typical of CRPS, especially during the first 6 months; however, it is not specific enough to be used as a diagnostic criteria. Unfortunately, the pathophysiological mechanisms underlying CRPS remain unclear, and, as such, no standard diagnostic test for CRPS exists. There are 3 major sets of diagnostic criteria for CRPS: the International Association for the Study of Pain (IASP) criteria, the Budapest Research Criteria, and the Veldman criteria. According to IASP, CRPS type
1 involves an initiating noxious event or a cause of immobilization; continuing pain/allodynia/hyperalgesia for which the pain is disproportionate to any known inciting event; evidence of edema, changes in skin blood flow, or abnormal pseudomotor activity in the region of pain; and exclusion of the diagnosis by the existence of other conditions that would otherwise account for the degree of pain and dysfunction. CRPS type 2 is a syndrome that develops after nerve injury, contends IASP. Spontaneous pain or allodynia/hyperalgesia occurs and is not necessarily limited to the territory of the injured nerve; there is or has been evidence of edema, a skin blood flow abnormality, or abnormal sudomotor activity in the region of pain since the inciting event; and the diagnosis is excluded by the existence of conditions that would otherwise account for the degree of pain and dysfunction.
1 involves an initiating noxious event or a cause of immobilization; continuing pain/allodynia/hyperalgesia for which the pain is disproportionate to any known inciting event; evidence of edema, changes in skin blood flow, or abnormal pseudomotor activity in the region of pain; and exclusion of the diagnosis by the existence of other conditions that would otherwise account for the degree of pain and dysfunction. CRPS type 2 is a syndrome that develops after nerve injury, contends IASP. Spontaneous pain or allodynia/hyperalgesia occurs and is not necessarily limited to the territory of the injured nerve; there is or has been evidence of edema, a skin blood flow abnormality, or abnormal sudomotor activity in the region of pain since the inciting event; and the diagnosis is excluded by the existence of conditions that would otherwise account for the degree of pain and dysfunction.
Question 36High Yield
-Decreased sun exposure leads to decreased bone health via what mechanism?
Explanation
No detailed explanation provided for this question.
Question 37High Yield
What is the most important factor in determining recovery after surgical repair of a complete laceration of a nerve at the wrist?
Explanation
All other factors being equal, a patient’s age is the most important factor in determining outcome after peripheral nerve injury. Repair of a nerve laceration within the first 2 weeks is generally considered appropriate. Fascicular repair may be of benefit in larger proximal nerves to reapproximate appropriate nerve bundles; distally perineural or epineural repair is sufficient. Use of a fibrin tissue sealant for nerve repair does not result in improved outcomes over suture repair. Nerve conduits have shown promise in digital nerves but do not have proven benefit in larger caliber nerves.
REFERENCES: Sunderland S: Nerve Injuries and Their Repair: A Critical Appraisal. New York, NY, Churchill Livingstone, 1991.
Wilgis ES, Brushart TM: Nerve repair and grafting, in Green DP, Hotchkiss RN (eds): Operative Hand Surgery, ed 3. New York, NY, Churchill Livingstone, 1993, p 1325.
Narakas A: The use of fibrin glue in repair of peripheral nerves. Orthop Clin North Am 1988;19:187-199.
Weber RA, Breidenbach WC, Brown RE, et al: A randomized prospective study of
polyglycolic acid conduits for digital nerve reconstruction in humans. Plast Reconstr Surg 2000;106:1036-1045.
REFERENCES: Sunderland S: Nerve Injuries and Their Repair: A Critical Appraisal. New York, NY, Churchill Livingstone, 1991.
Wilgis ES, Brushart TM: Nerve repair and grafting, in Green DP, Hotchkiss RN (eds): Operative Hand Surgery, ed 3. New York, NY, Churchill Livingstone, 1993, p 1325.
Narakas A: The use of fibrin glue in repair of peripheral nerves. Orthop Clin North Am 1988;19:187-199.
Weber RA, Breidenbach WC, Brown RE, et al: A randomized prospective study of
polyglycolic acid conduits for digital nerve reconstruction in humans. Plast Reconstr Surg 2000;106:1036-1045.
Question 38High Yield
A 55-year-old patient has ongoing right-hand pain despite having 4 months of treatment that included splinting, activity modification, and nonsteroidal anti-inflammatory drugs. She reports loss of dexterity and worsening hand writing during the last year. She has cramping of her affected hand, particularly in the first web space. Her symptoms are often worse at night. She has difficulty adducting her small finger and notes decreased sensation on the dorsum of her hand, particularly ulnarly. Division of which anatomical structure can most likely alleviate her symptoms?
Explanation
Cubital tunnel syndrome is the second-most-common compressive peripheral neuropathy after carpal tunnel syndrome. The diagnosis is typically established through a combination of a supportive history, positive clinical signs, and electrodiagnostic studies. Patients often experience hand paresthesias and/or numbness and hand pain (and less commonly medial elbow pain). Numbness usually affects the small finger, the ulnar aspect of the ring finger, and the dorsum of the hand (via the dorsal cutaneous branch of the ulnar nerve). When symptoms affect motor function, patients will have weakness of the hand intrinsics muscles and may exhibit atrophy. The Wartenberg sign is the observation of an abducted posture of the small finger in an affected hand attributable to an imbalance caused by an intact extensor digiti minimi and functional impairment of the affected third volar interosseous muscle attributable to atrophy and weakness. There are many surgical options for cubital tunnel syndrome, but all share division of the Osborne ligament because the nerve passes anterior to the olecranon and posterior to the medial epicondyle at the elbow.
Division of the transverse carpal ligament will decompress the median nerve and alleviate symptoms involving the thumb, index, and long fingers. Release of the lacertus fibrosus will not affect symptoms secondary to ulnar nerve compression. Ulnar nerve compression at Guyon’s canal will cause numbness to the small finger and intrinsic muscle weakness but not numbness to the
dorsum of the hand because the dorsal ulnar sensory nerve branches from the ulnar nerve prior to Guyon’s canal.
RECOMMENDED READINGS
5. Palmer BA, Hughes TB. Cubital tunnel syndrome. J Hand Surg Am. 2010 Jan;35(1):153-63. doi: 10.1016/j.jhsa.2009.11.004. Review. PubMed PMID: 20117320.
6. Soltani AM, Best MJ, Francis CS, Allan BJ, Panthaki ZJ. Trends in the surgical treatment of cubital tunnel syndrome: an analysis of the national survey of ambulatory surgery database. J Hand Surg Am. 2013 Aug;38(8):1551-6. doi: 10.1016/j.jhsa.2013.04.044. Epub 2013 Jul 3. PubMed PMID: 23830676.
Division of the transverse carpal ligament will decompress the median nerve and alleviate symptoms involving the thumb, index, and long fingers. Release of the lacertus fibrosus will not affect symptoms secondary to ulnar nerve compression. Ulnar nerve compression at Guyon’s canal will cause numbness to the small finger and intrinsic muscle weakness but not numbness to the
dorsum of the hand because the dorsal ulnar sensory nerve branches from the ulnar nerve prior to Guyon’s canal.
RECOMMENDED READINGS
5. Palmer BA, Hughes TB. Cubital tunnel syndrome. J Hand Surg Am. 2010 Jan;35(1):153-63. doi: 10.1016/j.jhsa.2009.11.004. Review. PubMed PMID: 20117320.
6. Soltani AM, Best MJ, Francis CS, Allan BJ, Panthaki ZJ. Trends in the surgical treatment of cubital tunnel syndrome: an analysis of the national survey of ambulatory surgery database. J Hand Surg Am. 2013 Aug;38(8):1551-6. doi: 10.1016/j.jhsa.2013.04.044. Epub 2013 Jul 3. PubMed PMID: 23830676.
Question 39High Yield
An otherwise healthy 35-year-old woman reports dorsal wrist pain and has trouble extending her thumb after sustaining a minimally displaced fracture of the distal radius 3 months ago. What is the next most appropriate step in management?
Explanation
Extensor pollicis longus tendon rupture can occur after a fracture of the distal radius, even a minimally displaced one. Poor vascularity of the tendon within the third dorsal compartment is the suspected etiology, not the displaced fracture fragments. Tendon transfer will suitably restore active extension of the thumb interphalangeal joint.
REFERENCES: Christophe K: Rupture of the extensor pollicis longus tendon following Colles fracture. J Bone Joint Surg Am 1953;35:1003-1005.
Hove LM: Delayed rupture of the thumb extensor tendon: A 5-year study of 18 consecutive cases. Acta Orthop Scand 1994;65:199-203.
REFERENCES: Christophe K: Rupture of the extensor pollicis longus tendon following Colles fracture. J Bone Joint Surg Am 1953;35:1003-1005.
Hove LM: Delayed rupture of the thumb extensor tendon: A 5-year study of 18 consecutive cases. Acta Orthop Scand 1994;65:199-203.
Question 40High Yield
A 14-year-old boy sustains a twisting injury to his right shoulder and recalls feeling a snap during a wrestling match. Examination shows hesitancy to raise the arm away from the side, diffuse tenderness and swelling of the upper arm, and no evidence of neurovascular compromise. Figures 6a and 6b show an AP radiograph and MRI scan. What is the most likely diagnosis?
Explanation
While difficult to appreciate on the AP radiograph of the shoulder, the increased physeal signal demonstrated on the axial MRI scan is consistent with a nondisplaced growth plate fracture. A comparison radiograph of the left shoulder also could be considered and the injured shoulder evaluated for physeal widening.
Proximal humeral fractures in children are somewhat unusual, representing less than 1% of all fractures seen in children and only 3% to 6% of all epiphyseal fractures. Physeal injuries are classified according to the Salter-Harris classification scheme. Salter-Harris type I fractures represent approximately 25% of physeal injuries to the proximal humerus in adolescents.
The proximal humeral physis is responsible for 80% of the longitudinal growth of the humerus; therefore, there is tremendous potential for remodeling of fractures in this region. Management for nondisplaced Salter-Harris type I fractures is limited to a short period of immobilization followed by a gradual return to activities as clinical symptoms resolve.
REFERENCES: Curtis RJ, Rockwood CA Jr: Fractures and dislocations of the shoulder in children, in Rockwood CA Jr, Matsen FA III (eds): The Shoulder. Philadelphia, PA, WB Saunders, 1990, pp 991-1007.
Salter RB, Harris WR: Injuries involving the epiphyseal plate. J Bone Joint Surg Am 1963;45:587-622.
Proximal humeral fractures in children are somewhat unusual, representing less than 1% of all fractures seen in children and only 3% to 6% of all epiphyseal fractures. Physeal injuries are classified according to the Salter-Harris classification scheme. Salter-Harris type I fractures represent approximately 25% of physeal injuries to the proximal humerus in adolescents.
The proximal humeral physis is responsible for 80% of the longitudinal growth of the humerus; therefore, there is tremendous potential for remodeling of fractures in this region. Management for nondisplaced Salter-Harris type I fractures is limited to a short period of immobilization followed by a gradual return to activities as clinical symptoms resolve.
REFERENCES: Curtis RJ, Rockwood CA Jr: Fractures and dislocations of the shoulder in children, in Rockwood CA Jr, Matsen FA III (eds): The Shoulder. Philadelphia, PA, WB Saunders, 1990, pp 991-1007.
Salter RB, Harris WR: Injuries involving the epiphyseal plate. J Bone Joint Surg Am 1963;45:587-622.
Question 41High Yield
Which radiographic abnormality most accurately serves as a predictor of ankle syndesmosis disruption?
Explanation
Normal syndesmotic relationships include a tibiofibular clear space smaller than 6 mm on both AP and mortise views. In a 1989 cadaveric study by Harper and Keller, a tibiofibular clear space exceeding 6 mm on both the AP and mortise views was the most reliable predictor of early syndesmotic widening. Tibiofibular overlap is measured 1 cm proximal to the plafond. Normal values exceed 6 mm or 42% of the width of the fibula on the AP view, or 1 mm on the mortise view. Proximal fibula fracture can occur in isolation without syndesmotic injury, frequently after direct trauma. The medial clear space is the distance between the lateral border of the medial malleolus and the medial border of the talus and is measured at the level of the talar dome. In the mortise view with the ankle in neutral dorsiflexion, the medial clear space should be equal to or smaller than the superior clear space between the talar dome and the tibial plafond. ?A normal medial clear space may be present with syndesmotic injury and consequently lacks sensitivity and specificity.
RECOMMENDED READINGS
[Zalavras C, Thordarson D. Ankle syndesmotic injury. J Am Acad Orthop Surg. 2007 Jun;15(6):330-9. Review. PubMed PMID: 17548882. ](http://www.ncbi.nlm.nih.gov/pubmed/17548882)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/17548882)
[Wuest TK. Injuries to the Distal Lower Extremity Syndesmosis. J Am Acad Orthop Surg. 1997 May;5(3):172-181. PubMed PMID: 10797219. ](http://www.ncbi.nlm.nih.gov/pubmed/10797219)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/10797219)
[Harper MC, Keller TS. A radiographic evaluation of the tibiofibular syndesmosis. Foot Ankle. 1989 Dec;10(3):156-60. PubMed PMID: 2613128. ](http://www.ncbi.nlm.nih.gov/pubmed/2613128)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/2613128)
CLINICAL SITUATION FOR QUESTIONS 37 THROUGH 40
A 41-year-old man sustained a twisting injury while running up stairs 4 weeks ago. He was treated in an ankle brace and has been bearing weight since the injury occurred. He has no history of ankle problems, but he now has ankle pain, swelling, and instability. The pain is aggravated by stairs, and the instability is worse on unlevel ground. Radiographs do not show a fracture.
RECOMMENDED READINGS
[Zalavras C, Thordarson D. Ankle syndesmotic injury. J Am Acad Orthop Surg. 2007 Jun;15(6):330-9. Review. PubMed PMID: 17548882. ](http://www.ncbi.nlm.nih.gov/pubmed/17548882)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/17548882)
[Wuest TK. Injuries to the Distal Lower Extremity Syndesmosis. J Am Acad Orthop Surg. 1997 May;5(3):172-181. PubMed PMID: 10797219. ](http://www.ncbi.nlm.nih.gov/pubmed/10797219)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/10797219)
[Harper MC, Keller TS. A radiographic evaluation of the tibiofibular syndesmosis. Foot Ankle. 1989 Dec;10(3):156-60. PubMed PMID: 2613128. ](http://www.ncbi.nlm.nih.gov/pubmed/2613128)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/2613128)
CLINICAL SITUATION FOR QUESTIONS 37 THROUGH 40
A 41-year-old man sustained a twisting injury while running up stairs 4 weeks ago. He was treated in an ankle brace and has been bearing weight since the injury occurred. He has no history of ankle problems, but he now has ankle pain, swelling, and instability. The pain is aggravated by stairs, and the instability is worse on unlevel ground. Radiographs do not show a fracture.
Question 42High Yield
What is the origin of this patient's pathology?
Explanation
- Genetic
Question 43High Yield
Which treatment will most likely improve this patient’s condition?
Explanation
- Resuscitation and oxygen_
Question 44High Yield
A 15-year-old white boy presents to your office with inability to elevate his right shoulder and flex his elbow. He sustained a fall from an all-terrain vehicle 8 weeks ago. He landed on the right shoulder and says his neck was twisted away at the time of fall. He was seen at the local emergency department; skull, chest, cervical and thoracic spine, and shoulder x-rays showed no damage. There was no loss of consciousness and he has no chest pain or breathing difficulties. He was observed in the hospital until stable and was referred to follow up in the hand clinic at 4 weeks and scheduled for an electromyogram.
C linical examination reveals weakness of deltoid, supraspinatus, infraspinatus, teres minor, biceps, brachialis, brachioradialis, and extensor carpi radialis longus. The remainder of his forearm musculature is preserved and he can grasp and release and pinch. Sensations are decreased along the distribution of axillary nerve. There is 3 cm wasting of his arm and 2 cm of his forearm. Tinel sign is positive around the clavicle. Horner signs are absent and his arm lies against the body. The EMG report shows fibrillation potentials in the weak muscles. The parents are concerned and say they have not seen any improvement. The boy reports that he is now able to flex his elbow. When asked to demonstrate you notice that he flexes his wrist and pronates his forearm to âswingâ his elbow into flexion.
The plan of management in this boy 5 months after injury with no clinical improvement should be:
C linical examination reveals weakness of deltoid, supraspinatus, infraspinatus, teres minor, biceps, brachialis, brachioradialis, and extensor carpi radialis longus. The remainder of his forearm musculature is preserved and he can grasp and release and pinch. Sensations are decreased along the distribution of axillary nerve. There is 3 cm wasting of his arm and 2 cm of his forearm. Tinel sign is positive around the clavicle. Horner signs are absent and his arm lies against the body. The EMG report shows fibrillation potentials in the weak muscles. The parents are concerned and say they have not seen any improvement. The boy reports that he is now able to flex his elbow. When asked to demonstrate you notice that he flexes his wrist and pronates his forearm to âswingâ his elbow into flexion.
The plan of management in this boy 5 months after injury with no clinical improvement should be:
Explanation
Neurotization is appropriate in preganglionic lesions. Around 6 months with no evidence of recovery is ideal time for plexus exploration. Further observation will not change the picture and tendon transfers are reconstructive procedures, which are done at a later stage.
Question 45High Yield
Posterior cruciate-retaining total knee arthroplasty has been studied by numerous methods including kinematic video fluoroscopy. Which of the following is the best description of typical kinematic behavior?

Explanation
DISCUSSION: In vivo fluoroscopic studies have enlightened orthopaedic surgeons as to the actual kinematic performance of the total knee implants. Importantly, many technical factors combine to result in abnormal kinematics after total knee arthroplasty. The typical kinematics of the normal knee are negated by osteoarthritis and the various changes created by the surgeon’s technique. Dennis and associates observed that anterior femoral condylar translation during deep knee flexion was most commonly observed in posterior cruciate-retaining knees.
REFERENCES: Dennis DA, Komistek RD, Mahfouz MR, et al: Multicenter determination of in vivo kinematics after total knee arthroplasty. Clin Orthop Relat Res 2003;416:37-57.
Freeman MA, Pinskerova V: The movement of the normal tibio-femoral joint. J Biomech 2005-38'197- 208.
**42 • American Academy of Orthopaedic Surgeons**
Figure 52
REFERENCES: Dennis DA, Komistek RD, Mahfouz MR, et al: Multicenter determination of in vivo kinematics after total knee arthroplasty. Clin Orthop Relat Res 2003;416:37-57.
Freeman MA, Pinskerova V: The movement of the normal tibio-femoral joint. J Biomech 2005-38'197- 208.
**42 • American Academy of Orthopaedic Surgeons**
Figure 52
Question 46High Yield
A 75-year-old man sustains an anterior dislocation of his reverse total shoulder arthroplasty. What activity places the arm in the position most commonly associated with reverse total shoulder dislocation?
Explanation
DISCUSSION
Proper soft-tissue tension is critical to prevent instability of a reverse total shoulder implanted with the deltopectoral approach; dislocation of the prosthesis is exceedingly rare if the superior approach is employed. The arm position implicated in reverse total shoulder instability is extension, adduction, and internal rotation,
such as pushing out of a chair. The other positions described do not involve extension of the shoulder.
DISCUSSION
Proper soft-tissue tension is critical to prevent instability of a reverse total shoulder implanted with the deltopectoral approach; dislocation of the prosthesis is exceedingly rare if the superior approach is employed. The arm position implicated in reverse total shoulder instability is extension, adduction, and internal rotation,
such as pushing out of a chair. The other positions described do not involve extension of the shoulder.
Question 47High Yield
The ideal range of micromotion to stimulate bone ingrowth into cementless implants is:
Explanation
Ideal values of micromotion that stimulate bone ingrowth are 28 microns to 150 microns. Values greater than 150 microns are associated with fibrous ingrowth
Question 48High Yield
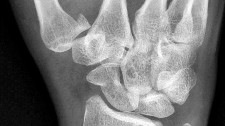
Figure 1 is the radiograph of an 18-year-old, right hand-dominant man who has right side thumb pain after a tackle during a rugby game. Examination shows ecchymosis and swelling of the right thumb along with tenderness to palpation about the thumb CMC joint and metacarpal base. What ligament is holding the small fracture fragment in anatomical location to the trapezium?
---
---
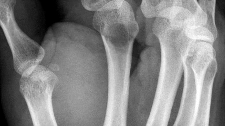
Explanation
Bennett fractures are defined as intra-articular thumb metacarpal base fractures. The fracture is often caused by axial loading, and concomitant injuries to the thumb MCP joint and trapezium are common. The palmar ulnar aspect of the base of the metacarpal stays in place through its attachment to the trapezium by way of the anterior oblique ligament. The metacarpal shaft is displaced dorsally, proximally, and radially by the pull of the abductor pollicis longus, extensor pollicis brevis, extensor pollicis longus, and adductor pollicis brevis. These fractures are often considered unstable and are treated surgically.
Question 49High Yield
Figure 1 is the MRI scan of a high school hockey player who is checked from behind and falls forward to the ice onto his flexed knees. He complains of swelling and posterior knee pain. Nonoperative treatment of the injured structure will most likely result in increased risk of degenerative change in
Explanation
The injury mechanism and MRI scans demonstrate an isolated posterior cruciate ligament (PCL) tear. PCL injury may result in posterior translational macro-instability of the knee, but may
also result in more subtle and subclinical increases in varus and posterior tibial translation during normal gait and other activities of daily living. These changes result in increased contact stresses in the medial (due to varus forces) and patellofemoral (due to posterior forces) compartments, leading to an increased risk of degenerative chondrosis in these areas.
5
also result in more subtle and subclinical increases in varus and posterior tibial translation during normal gait and other activities of daily living. These changes result in increased contact stresses in the medial (due to varus forces) and patellofemoral (due to posterior forces) compartments, leading to an increased risk of degenerative chondrosis in these areas.
5
Question 50High Yield
Which of the following proteins or vitamins controls the amount of receptor activator of nuclear factor âkB ligand (RANKL)
produced by osteoblasts:
produced by osteoblasts:
Explanation
The active from of vitamin D (1,25 dihydroxyvitamin D3) regulates the control of RANKL production by the osteoblast.
The activation of osteoclasts is a complex process. Surface receptors on the osteoclast precursor cells are called RANK. Receptor activator of nuclear factor âkB ligand (RANKL) is expressed on the surface of osteoblasts/stromal cells. The RANKL proteins leave the osteoblast and attach to the RANK receptor on the osteoclast precursor. Macrophage colony stimulating factor then facilitates the production of active osteoclasts from the osteoclast precursor
The activation of osteoclasts is a complex process. Surface receptors on the osteoclast precursor cells are called RANK. Receptor activator of nuclear factor âkB ligand (RANKL) is expressed on the surface of osteoblasts/stromal cells. The RANKL proteins leave the osteoblast and attach to the RANK receptor on the osteoclast precursor. Macrophage colony stimulating factor then facilitates the production of active osteoclasts from the osteoclast precursor
You Might Also Like

Medically Verified Content by
Prof. Dr. Mohammed Hutaif
Consultant Orthopedic & Spine Surgeon

