Gastrocnemius Fascia Lengthening: An Intraoperative Masterclass for Equinus Deformity
Key Takeaway
Join us in the OR for a detailed masterclass on gastrocnemius fascia lengthening, a critical procedure for equinus deformities. We'll meticulously cover surgical anatomy, preoperative planning, precise intraoperative execution of Strayer, Baker, and Vulpius techniques, essential pearls and pitfalls, and comprehensive postoperative management to optimize patient outcomes and prevent recurrence.
Introduction and Epidemiology
Equinus deformity represents one of the most frequently encountered musculoskeletal pathologies in both pediatric and adult orthopedic surgery. Defined biomechanically as a fixed or dynamic plantarflexion contracture of the ankle joint, equinus prevents normal dorsiflexion during the stance phase of gait. Lengthening of the gastrocnemius fascia, often referred to as a gastrocnemius recession, is a foundational surgical intervention designed to restore normal ankle kinematics in patients where the equinus is primarily driven by an isolated contracture of the gastrocnemius muscle complex.

The most common etiology necessitating gastrocnemius fascia lengthening is cerebral palsy (CP). In the CP population, an upper motor neuron lesion leads to spasticity, which over time transitions from a dynamic muscular overactivity to a fixed myostatic contracture. However, the procedure is broadly applicable across a diverse array of pathologies. Idiopathic toe walking, post-traumatic tethering, iatrogenic contractures following prolonged plantarflexed immobilization, and neuromuscular dystrophies (such as Duchenne muscular dystrophy) frequently culminate in functionally limiting equinus.
It is paramount to distinguish true ankle equinus from apparent equinus. In patients with hereditary motor sensory neuropathies, such as Charcot-Marie-Tooth (CMT) disease, the forefoot is often severely plantarflexed relative to the hindfoot (anterior cavus). This creates an illusion of ankle equinus, whereas the true deformity lies within the midfoot. Inappropriate lengthening of the triceps surae in a patient with an isolated midfoot cavus deformity will precipitate a devastating calcaneal gait.

Natural History of Equinus Deformity
The natural history of equinus is highly dependent on the underlying etiology. In the spastic cerebral palsy patient, the deformity is progressive. It begins as a dynamic, tone-driven posturing of the foot during gait. Without intervention, this constant hypertonicity leads to structural shortening of the muscle-tendon unit, decreasing the number of in-series sarcomeres. Eventually, this soft-tissue contracture places abnormal compressive forces across the anterior tibiotalar joint, leading to secondary bony deformity, flattening of the talar dome, and joint incongruity. Conversely, idiopathic toe walking often presents early in childhood and may spontaneously resolve or improve as the patient matures, though a subset will develop persistent, fixed contractures requiring surgical release.
Surgical Anatomy and Biomechanics
A rigorous understanding of the triceps surae complex is mandatory for precise surgical execution and the avoidance of iatrogenic complications. The triceps surae comprises three distinct muscular units: the medial gastrocnemius, the lateral gastrocnemius, and the soleus, augmented by the vestigial plantaris muscle.

The Gastrocnemius Muscle
The gastrocnemius is a biarticular muscle, crossing both the knee and the ankle joints. The larger medial head originates from the popliteal surface of the femur, proximal to the medial femoral condyle. The lateral head originates from the superolateral surface of the lateral femoral condyle. Because it spans two joints, the gastrocnemius functions as both a knee flexor and an ankle plantarflexor.
Histologically, the gastrocnemius is predominantly composed of fast-twitch (Type II) muscle fibers. This physiological composition equips the muscle for short, explosive bursts of kinetic energy, essential for activities such as sprinting and jumping.
The medial and lateral muscle bellies converge distally into a midline tendinous raphe. This raphe broadens into the distinct aponeurosis of the gastrocnemius at the mid-calf level. Understanding this aponeurotic confluence is the cornerstone of the gastrocnemius recession, as the surgical objective is to selectively transect this fascial layer while preserving the underlying soleus fascia and muscle fibers.

The Soleus and Plantaris Muscles
The soleus lies anterior (deep) to the gastrocnemius. It is a uniarticular muscle, originating from the posterior aspect of the proximal tibia, fibula, and the interosseous membrane. It does not cross the knee joint; therefore, its solitary function is ankle plantarflexion. Unlike the gastrocnemius, the soleus is composed primarily of slow-twitch (Type I) muscle fibers, reflecting its critical role in sustained postural control and the maintenance of upright bipedal stance. Distally, the soleus aponeurosis merges with the gastrocnemius aponeurosis to form the conjoined tendo Achilles, which inserts into the posterior calcaneal tuberosity.
The plantaris is a small, largely vestigial muscle that originates superior to the lateral head of the gastrocnemius. Its long, slender tendon courses obliquely between the gastrocnemius and soleus to insert on the medial aspect of the calcaneus. During a gastrocnemius recession, the plantaris tendon is frequently encountered and must be selectively released to prevent residual tethering.

Biomechanical Evaluation The Silfverskiold Test
The anatomical differentiation between the biarticular gastrocnemius and the uniarticular soleus forms the biomechanical basis for the Silfverskiöld test. This clinical maneuver isolates the specific anatomical locus of the equinus contracture.
The ankle is passively dorsiflexed with the knee fully extended, and then the measurement is repeated with the knee flexed to 90 degrees.
1. If ankle dorsiflexion improves significantly when the knee is flexed, the contracture is isolated to the gastrocnemius (which is placed on slack by knee flexion). This indicates a gastrocnemius recession.
2. If ankle dorsiflexion remains equally restricted regardless of knee position, the contracture involves the soleus and/or the posterior ankle capsule, necessitating a more distal tendo Achilles lengthening (TAL) or capsular release.
Indications and Contraindications
The decision to proceed with a gastrocnemius fascia lengthening hinges upon precise clinical and kinematic indications. The primary goal is to restore plantigrade foot positioning during the stance phase of gait without compromising the plantarflexion power required for push-off.

Operative vs Non Operative Management
| Modality | Indications | Contraindications / Limitations |
|---|---|---|
| Non-Operative (Physical Therapy) | Mild dynamic equinus, early CP, reducible deformity, idiopathic toe walking in young children. | Fixed myostatic contracture, severe bony deformity, failure to progress. |
| Non-Operative (Botulinum Toxin) | Dynamic spasticity without fixed contracture, diagnostic tool to simulate surgical release. | Fixed contracture (muscle structurally shortened), neutralizing antibodies. |
| Non-Operative (Serial Casting) | Moderate fixed contracture, adjunct to Botulinum toxin, idiopathic toe walking. | Severe fixed contracture, sensory neuropathies, rigid midfoot break. |
| Operative (Gastrocnemius Recession) | Positive Silfverskiöld test, fixed gastrocnemius contracture, failure of conservative therapy, part of single-event multilevel surgery (SEMLS). | Negative Silfverskiöld test (requires TAL), fixed bony block at the ankle joint, pre-existing calcaneal gait. |
| Operative (Tendo Achilles Lengthening) | Combined gastrocnemius-soleus contracture (negative Silfverskiöld test), severe rigid equinus. | Isolated gastrocnemius contracture, high risk of over-lengthening (crouch gait). |
Over-lengthening of the triceps surae is a catastrophic complication, particularly in the cerebral palsy population. Weakening the soleus excessively leads to an inability to control tibial advancement over the plantigrade foot during stance. This results in a progressive calcaneal stance, compensatory knee flexion, and ultimately, an energy-inefficient and debilitating crouch gait. Therefore, isolated gastrocnemius recession is highly preferred over TAL whenever the Silfverskiöld test permits, as it preserves soleus strength for postural control.
Pre Operative Planning and Patient Positioning
Thorough preoperative evaluation is required to ensure the correct procedure is selected and to plan for any concomitant interventions. In patients with complex neuromuscular disorders, isolated equinus is rare; it is frequently accompanied by hamstring tightness, hip flexion contractures, or foot deformities (e.g., pes planovalgus).

Clinical and Radiographic Assessment
Clinical examination must include a meticulous Silfverskiöld test, assessment of torsional profiles, and evaluation of hindfoot varus or valgus. In the setting of a tight Achilles tendon, the foot will often pronate through the transverse tarsal joint to achieve apparent dorsiflexion, leading to a midfoot break.
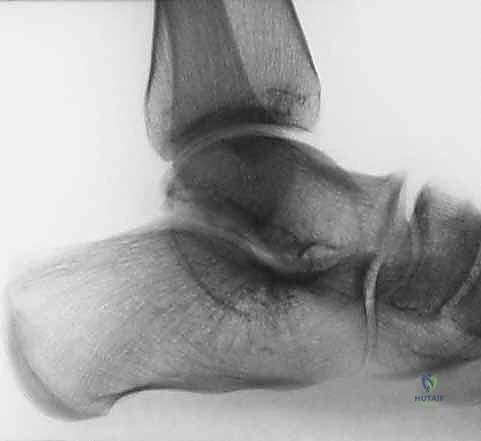
Weight-bearing anteroposterior and lateral radiographs of the foot and ankle are mandatory. The lateral view should be scrutinized for a flattened talar dome, which may indicate a bony block to dorsiflexion that soft-tissue lengthening cannot overcome. The lateral view also assesses the calcaneal pitch and the talonavicular alignment to rule out a midfoot break or occult cavus.
Computerized 3D gait analysis (kinematics and kinetics) is considered the gold standard for preoperative planning in ambulatory patients with cerebral palsy. Gait analysis differentiates between dynamic spasticity and fixed contracture during the dynamic phases of walking, providing objective data to guide single-event multilevel surgery (SEMLS).

Patient Positioning and Anesthesia
Patient positioning is dictated by the scope of the planned surgical intervention.
1. Prone Position: Ideal for isolated gastrocnemius recession or combined posterior procedures (e.g., hamstring lengthenings). It provides excellent, direct visualization of the posterior calf and the sural nerve.
2. Supine Position (Frog-Leg): Frequently utilized when the gastrocnemius recession is part of a larger SEMLS involving anterior procedures (e.g., hip adductor releases, femoral derotational osteotomies, or foot reconstructions). The hip is externally rotated, and the knee is flexed to expose the medial and posterior aspects of the calf.
A thigh tourniquet is typically applied to provide a bloodless surgical field. General anesthesia is standard, often supplemented with regional anesthesia (e.g., popliteal block) for postoperative pain management.
Detailed Surgical Approach and Technique
Several surgical techniques have been described for lengthening the gastrocnemius fascia. The choice of technique depends on the surgeon's preference and the exact anatomical level of the contracture. The most common techniques include the Strayer procedure, the Vulpius procedure, and the Baumann procedure.

Surgical Techniques Overview
- Strayer Procedure: Transection of the gastrocnemius aponeurosis proximal to its junction with the soleus aponeurosis. The underlying soleus muscle is left intact.
- Vulpius Procedure: An inverted V-shaped incision through the combined gastrocnemius and superficial soleus aponeurosis, leaving the underlying soleus muscle fibers intact.
- Baumann Procedure: Intramuscular lengthening of the gastrocnemius aponeurosis via one or more transverse incisions in the deep fascia of the gastrocnemius, performed in the proximal third of the calf.
- Baker Procedure: A tongue-in-groove (U-shaped) lengthening of the gastrocnemius aponeurosis, allowing for controlled lengthening and direct suturing of the lengthened fascia.

Step by Step Classical Strayer Approach
The classical Strayer procedure remains the workhorse for isolated gastrocnemius contractures.
Step 1: Incision and Dissection
A 3 to 5 cm longitudinal incision is made over the posteromedial aspect of the calf, approximately 2 cm medial to the midline, at the junction of the middle and distal thirds of the leg. This location corresponds to the transition zone where the gastrocnemius muscle bellies terminate into the aponeurosis. Subcutaneous tissues are bluntly dissected.
Step 2: Sural Nerve Identification and Protection
The sural nerve is the most critical structure at risk during this approach. It courses superficially down the posterior midline of the calf, often accompanied by the lesser saphenous vein. The nerve must be definitively identified, mobilized, and protected with a vessel loop or gentle retraction laterally.

Step 3: Exposure of the Aponeurosis
The paratenon over the gastrocnemius aponeurosis is incised longitudinally. The interval between the gastrocnemius aponeurosis and the underlying soleus muscle is developed. This internervous/intermuscular plane is usually easily established with blunt finger dissection or a right-angle clamp.
Step 4: Transection of the Gastrocnemius Fascia
With the plane between the gastrocnemius and soleus clearly defined, the gastrocnemius aponeurosis is sharply transected transversely from medial to lateral. It is imperative to ensure that the release extends completely across the lateral border of the aponeurosis. The plantaris tendon, typically found at the medial border of the interval, should be identified and transected to prevent residual tethering.

Step 5: Assessment of Correction
Following the fascial release, the knee is maintained in full extension, and the ankle is forcefully dorsiflexed. The surgeon should observe a distinct separation (gap) of the transected aponeurotic ends, typically measuring 1.5 to 3 cm. The ankle should now easily reach 10 to 15 degrees of dorsiflexion with the knee extended. If residual tightness persists, the surgeon must re-evaluate for incomplete lateral fascial release or unrecognized soleus contracture.
Step 6: Closure
The paratenon is approximated if possible, followed by meticulous closure of the subcutaneous layer to prevent dead space and tethering of the skin to the underlying fascia. The skin is closed with a running subcuticular absorbable suture.
Complications and Management
While gastrocnemius fascia lengthening is generally considered a safe and highly effective procedure, complications can arise, ranging from minor wound issues to severe biomechanical derangements.

Summary of Complications and Salvage Strategies
| Complication | Estimated Incidence | Pathophysiology | Salvage Strategy / Management |
|---|---|---|---|
| Over-lengthening (Crouch Gait) | 2% - 5% | Excessive lengthening of the triceps surae complex, leading to loss of plantarflexion power and uncontrolled tibial advancement. | Prolonged use of solid AFOs. In severe, refractory cases, complex reconstruction including Achilles shortening and distal femoral extension osteotomies may be required. |
| Under-correction / Recurrence | 10% - 15% | Incomplete release of the lateral fascia, failure to release plantaris, or progressive spasticity in a growing child. | Aggressive postoperative bracing. Revision surgery (repeat gastroc recession or TAL) if fixed contracture recurs. |
| Sural Nerve Neuroma / Injury | 1% - 3% | Direct transection, traction injury, or entrapment in scar tissue during closure. | Conservative management with gabapentinoids/desensitization. Surgical exploration, neuroma excision, and nerve burying into deep muscle belly for refractory pain. |
| Wound Dehiscence / Infection | < 2% | Poor vascular supply to the posterior calf skin, excessive tension on closure, or hematoma formation. | Local wound care, oral antibiotics. Rarely requires surgical debridement or flap coverage unless deep infection occurs. |
| Midfoot Break | Variable | Forcing dorsiflexion through the transverse tarsal joint rather than the ankle joint during casting or bracing. | Ensure proper casting technique molding the longitudinal arch. May require midfoot stabilization (e.g., calcaneocuboid lengthening) if severe. |
The most critical intraoperative error is the failure to recognize a combined gastrocnemius-soleus contracture. Performing an isolated gastrocnemius recession in a patient who actually requires a TAL will result in immediate under-correction. Conversely, performing a TAL when only a gastrocnemius recession is indicated risks catastrophic over-lengthening.
Post Operative Rehabilitation Protocols
The success of a gastrocnemius recession is inextricably linked to the postoperative rehabilitation protocol. Surgical lengthening provides the anatomical potential for normal kinematics, but extensive physical therapy is required to integrate this new range of motion into functional gait.

Immobilization Phase
Immediately following surgery, the lower extremity is typically immobilized to protect the surgical release and allow the soft tissues to heal in their new, lengthened position.
1. Short Leg Cast: A fiberglass short leg cast is applied with the ankle in neutral to 5 degrees of dorsiflexion. The knee is left free to allow immediate mobilization. The cast is generally maintained for 3 to 4 weeks.
2. Weight-Bearing Status: Most protocols allow for immediate weight-bearing as tolerated in the cast. Weight-bearing actually assists in maintaining the stretch on the triceps surae complex and prevents disuse osteopenia.
Mobilization and Bracing Phase
Upon removal of the cast at 3 to 4 weeks, the patient transitions into a custom-molded Ankle-Foot Orthosis (AFO).
1. Daytime Bracing: Articulating AFOs with a plantarflexion stop are frequently utilized to allow active dorsiflexion while preventing recurrence of the equinus contracture.
2. Nighttime Bracing: Solid AFOs or resting splints are worn at night for a minimum of 6 to 12 months postoperatively to counteract the nocturnal return of spasticity and prevent contracture recurrence.
Physical Therapy
Formal physical therapy commences immediately after cast removal. The protocol focuses on:
* Active and Passive Range of Motion: Gentle stretching of the Achilles tendon and gastrocnemius.
* Strengthening: Particular emphasis is placed on strengthening the antagonist muscles, specifically the tibialis anterior, to improve active dorsiflexion during the swing phase of gait.
* Gait Training: Retraining the neuromuscular system to utilize the newly acquired heel strike and smooth tibial progression during stance phase.
Summary of Key Literature and Guidelines
The academic consensus regarding the management of equinus deformity heavily favors gastrocnemius recession over tendo-Achilles lengthening whenever anatomically appropriate, particularly in patients with cerebral palsy.

Seminal work by Gage and Novacheck on computerized gait analysis has demonstrated that isolated gastrocnemius recession effectively restores the first rocker (heel strike) and second rocker (tibial advancement) of gait without sacrificing the vital push-off power generated by the soleus during the third rocker.
Furthermore, long-term outcome studies stratified by the Gross Motor Function Classification System (GMFCS) indicate that ambulatory patients (GMFCS Levels I-III) who undergo selective gastrocnemius lengthening maintain their functional ambulation status significantly better than those who undergo non-selective TAL, who are at a demonstrably higher risk for iatrogenic crouch gait.
Comparative literature between the various techniques (Strayer vs. Vulpius vs. Baumann) shows no significant difference in long-term kinematic outcomes, provided the correct anatomical layer is released. The Baumann procedure has gained popularity in recent years due to its ability to be performed through multiple smaller incisions, potentially reducing the risk of sural nerve injury and allowing for a more titratable lengthening of the aponeurosis.
In conclusion, gastrocnemius fascia lengthening is a highly effective, targeted surgical intervention for equinus deformity. Rigorous preoperative evaluation utilizing the Silfverskiöld test and gait analysis, combined with meticulous surgical technique to protect the sural nerve and preserve the soleus, ensures optimal restoration of ankle kinematics and long-term functional outcomes.
Clinical & Radiographic Imaging















You Might Also Like