RUPTURE OF THE GASTROCNEMIUS MUSCLE (TENNIS LEG)
Musculotendinous rupture of the gastrocnemius muscle—colloquially referred to as "tennis leg"—is a frequent source of acute calf pain in the athletic and active middle-aged population. The injury predominantly involves the medial head of the gastrocnemius at its insertion into the soleus aponeurosis.
Pathoanatomy and Biomechanics
The gastrocnemius is a biarticular muscle, crossing both the knee and the ankle joints, which places it at a mechanical disadvantage during simultaneous knee extension and ankle dorsiflexion. Ruptures most commonly occur during an acute eccentric overload. In middle-aged male athletes, this typically manifests during sports requiring sudden acceleration or directional changes, such as tennis, squash, or jogging. The medial head is significantly more susceptible to rupture than the lateral head due to its larger cross-sectional area, greater contribution to plantarflexion force, and more distal extension along the aponeurosis.
Clinical Presentation and Differential Diagnosis
Patients classically report an acute, sharp pain in the posterior calf, often accompanied by an audible "pop" or the sensation of being struck in the back of the leg by an object.
Physical examination reveals:
* Acute tenderness localized to the medial musculotendinous junction.
* A visible or palpable defect in the medial gastrocnemius muscle belly.
* Progressive ecchymosis and edema that may track distally to the foot and ankle over subsequent days.
* Pain exacerbated by passive ankle dorsiflexion and active plantarflexion.
Clinical Pitfall: The differential diagnosis for acute calf pain is critical. Gastrocnemius rupture must be distinguished from Achilles tendon rupture, plantaris tendon rupture, ruptured popliteal (Baker's) cyst, and, most importantly, deep vein thrombosis (DVT).
Misdiagnosing a gastrocnemius tear as a DVT can lead to the erroneous administration of systemic anticoagulants. This iatrogenic error exacerbates intramuscular hemorrhage, potentially precipitating acute compartment syndrome of the superficial posterior compartment. Conversely, missing a DVT can be fatal. If the clinical picture is ambiguous, advanced imaging is mandatory.
Diagnostic Imaging
While the diagnosis is primarily clinical, imaging is invaluable in equivocal cases:
* Ultrasonography (US): The first-line modality due to its dynamic capabilities, low cost, and lack of radiation. It effectively visualizes the disruption of muscle fibers, hematoma formation between the gastrocnemius and soleus aponeurosis, and can simultaneously rule out a DVT via Doppler evaluation.
* Magnetic Resonance Imaging (MRI): The gold standard for complex cases. MRI provides superior soft-tissue contrast, accurately delineating the extent of the musculotendinous disruption, the size of the hematoma, and the presence of any concomitant pathology.
Evidence-Based Management Protocol
Operative intervention is virtually never indicated for isolated gastrocnemius muscle ruptures. The foundation of treatment is conservative, focusing on protecting the healing tissue while preventing contracture.
Phase 1: Acute Management (Days 1–7)
* RICE Protocol: Relative rest, ice, compression (tubigrip or compression stocking), and elevation.
* Weight-Bearing: Early weight-bearing as tolerated is encouraged. Crutches may be used initially for pain control.
* Immobilization: The use of a controlled ankle motion (CAM) boot or ankle bracing that holds the ankle in maximal tolerable dorsiflexion has been shown to optimize the length-tension relationship of the healing muscle fibers, accelerating recovery. Heel lifts (1-2 cm) can be temporarily utilized to offload the musculotendinous junction if dorsiflexion is poorly tolerated.
Phase 2: Rehabilitation and Return to Play (Weeks 2–12)
* Physical Therapy: Initiated once acute pain subsides. The focus shifts to restoring full, symmetrical range of motion (ROM) and progressive strengthening.
* Strengthening: Transition from isometric to concentric, and finally to eccentric loading of the gastroc-soleus complex.
* Return to Sport: Sport-specific agility and plyometric exercises are introduced once the patient is pain-free with full strength. Depending on the severity of the tear (Grade I vs. Grade III), return to play ranges from 1 to 12 weeks.
TENDINOSIS OF THE EXTENSOR MECHANISM OF THE KNEE (JUMPER’S KNEE)
Tendinosis of the extensor mechanism, widely known as "jumper's knee," is a chronic, degenerative overuse injury. It is overwhelmingly prevalent in elite athletes participating in jumping sports, with an estimated prevalence of 40% to 50% in high-level volleyball players and 35% to 40% in elite basketball players.
Pathophysiology: Angiofibroblastic Tendinosis
The pathology typically localizes to the tendoosseous junction at the inferior pole of the patella. The term "tendinitis" is a misnomer; histological analysis rarely reveals acute inflammatory cells. Instead, repetitive traction and eccentric overload induce microtrauma that outpaces the tendon's healing capacity.
This leads to angiofibroblastic tendinosis, characterized by:
* Focal mucoid degeneration.
* Fraying and microtearing of collagen fibrils.
* A pathological shift from organized Type I collagen to disorganized, mechanically inferior Type III collagen.
* Neovascularization and nerve ingrowth (substance P and glutamate), which are the primary drivers of nociception.
While chronic repetitive microtrauma is the standard etiology, a single episode of massive eccentric overload or a direct blow can occasionally precipitate symptoms.
Clinical Evaluation
Patients present with insidious onset, anterior knee pain localized precisely to the inferior patellar pole.
* Palpation: Exquisite tenderness at the inferior pole, which is characteristically worse when the knee is in full extension (Basset's sign) compared to 90 degrees of flexion (where the tendon is under tension and the pathological lesion is shielded by the patella).
* Associated Findings: Evaluation must rule out or identify concomitant patellar maltracking, chondromalacia patellae, Osgood-Schlatter disease, or mechanical malalignment (e.g., increased Q-angle, femoral anteversion).
Classification Systems
Clinical staging is essential for guiding treatment. The two most widely utilized systems are the Blazina classification and the modified Ferretti staging.
Blazina et al. Classification:
* Phase 1: Pain only after sports activity.
* Phase 2: Pain during and after activity, but no significant functional impairment.
* Phase 3: Pain during and after activities with progressive difficulty in satisfactory performance.
* Phase 4: End-stage disease with stress fracture through the patella or complete disruption of the extensor mechanism.
Ferretti et al. Classification (Table 48-4 Modified):
* Stage 0: No pain.
* Stage 1: Pain only after intense sports activity; no undue functional impairment.
* Stage 2: Pain at the beginning and after sports activity; still able to perform at a satisfactory level.
* Stage 3: Pain during sports activity; increasing difficulty in performing at a satisfactory level.
* Stage 4: Pain during sports activity; unable to participate in sport at a satisfactory level.
* Stage 5: Pain during daily activity; unable to participate in sport at any level.
Radiographic and Advanced Imaging
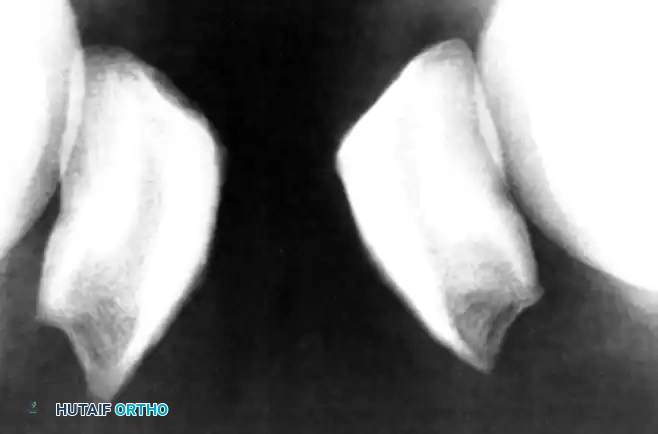
- Radiographs: Anteroposterior, lateral, and tangential (Merchant) views are standard. Early in the disease process, radiolucency at the inferior pole may be noted. With chronic, prolonged symptoms, the inferior pole may become hypertrophied and elongated. A periosteal reaction on the anterior patellar surface (the "tooth sign") and intratendinous calcifications may also be evident.

FIGURE 48-27: Elongation of the lower pole of the patella in an athlete with a long history of patellar tendinosis. Note the structural remodeling secondary to chronic traction.
- Magnetic Resonance Imaging (MRI): MRI is highly sensitive. It typically demonstrates focal thickening of the proximal patellar tendon (usually medial) and increased signal intensity on T1 and T2-weighted images, representing mucoid degeneration.
- Ultrasonography (US): Advances in high-resolution US, particularly with color Doppler, allow for the visualization of hypoechoic regions, tendon thickening, and pathological neovascularization. It is highly effective for guiding therapeutic injections.
Nonoperative Management Strategies
Conservative management is the mainstay of treatment for Phase 1 and Phase 2 symptoms, and the initial approach for Phase 3.
- Activity Modification and Rehabilitation: Relative rest and cessation of jumping/plyometric activities.
- Eccentric Exercise: The cornerstone of tendinosis rehabilitation. Heavy, slow eccentric loading (e.g., decline squat protocols) stimulates collagen synthesis and realignment. While some studies show conflicting results, it remains a first-line recommendation.
- Pharmacotherapy: NSAIDs may provide short-term analgesic relief but do not alter the underlying degenerative pathology.
> Surgical Warning: Corticosteroid injections into or around the patellar tendon are strictly contraindicated. They induce collagen necrosis, significantly increasing the risk of catastrophic tendon rupture. - Orthobiologics and Advanced Modalities:
- Platelet-Rich Plasma (PRP): Leukocyte-rich PRP injections have demonstrated statistically significant improvements in pain and function by delivering concentrated growth factors (PDGF, TGF-β) to the hypovascular degenerative lesion.
- Sclerosing Injections: Ultrasound-guided injection of polidocanol targets the pathological neovessels and accompanying sensory nerves on the dorsal aspect of the tendon, effectively denervating the painful lesion.
- Extracorporeal Shockwave Therapy (ESWT): ESWT induces microtrauma to stimulate a healing response. Studies report satisfactory results in up to 74% of patients, facilitating return to sport in an average of 6 weeks.
- Cell Therapy: Emerging randomized trials comparing ultrasound-guided injection of autologous skin-derived tendon-like cells versus plasma alone have shown faster responses and superior functional outcomes with cell therapy.
Surgical Management of Chronic Tendinosis
Operative intervention is indicated for patients with Phase 3 symptoms that remain recalcitrant after 3 to 6 months of comprehensive nonoperative management, or immediately for Phase 4 (rupture).
Arthroscopic vs. Open Debridement
Historically, open patellar tenotomy and excision of the degenerative tissue was the gold standard. However, arthroscopic shaving of the dorsal aspect of the tendon and the inferior patellar pole has gained prominence. Randomized controlled trials comparing arthroscopic shaving to sclerosing injections have shown that arthroscopic debridement yields less pain, higher patient satisfaction, and a faster return to sport.
Surgical Technique: Open Debridement of the Patellar Tendon
Positioning and Setup:
1. The patient is placed supine on the operating table.
2. A well-padded tourniquet is applied to the proximal thigh.
3. The knee is positioned with a bump to maintain 30 degrees of flexion, placing the extensor mechanism under mild tension.
Surgical Approach:
1. A longitudinal midline or paratendinous incision is made over the inferior pole of the patella extending distally over the proximal tendon.
2. The paratenon is carefully incised longitudinally and preserved for later closure.
Debridement and Repair:
1. A longitudinal tenotomy is performed in line with the tendon fibers, typically in the central or medial third where the pathology is concentrated.
2. The degenerative tissue is identified; it classically appears gray, friable, and lacks the normal glistening, fibrillar structure of healthy tendon.
3. An elliptical excision of the angiofibroblastic tissue is performed.
4. The inferior pole of the patella is debrided of any prominent osteophytes or "tooth sign" bone.
5. Microfracture or drilling of the inferior pole may be performed to stimulate a marrow-derived healing response (bleeding bone bed).
6. If the remaining tendon defect is large, side-to-side closure of the healthy tendon fibers is performed using non-absorbable sutures.
7. The paratenon is meticulously closed to prevent adhesions.
Postoperative Protocol:
* Weeks 0-2: The knee is locked in extension in a hinged brace. Weight-bearing is permitted as tolerated with crutches.
* Weeks 2-6: Progressive passive and active-assisted ROM is initiated.
* Weeks 6-12: Transition to closed-chain strengthening and eccentric loading.
* Months 3-6: Gradual return to sport-specific activities.
Management of Extensor Mechanism Disruption (Phase 4)
End-stage disease can result in complete disruption of the patellar tendon. Acute repair is mandatory.
Surgical Pitfall: Delays in operative treatment of extensor mechanism ruptures (greater than 2 to 8 weeks) result in profound quadriceps retraction. Retraction of up to 5 cm may occur, precluding primary end-to-end repair and necessitating complex reconstructive procedures such as quadriceps lengthening (V-Y plasty), hamstring tendon autograft augmentation, or allograft reconstruction.
For acute ruptures, primary repair is achieved via transosseous tunnels drilled through the patella or the use of heavy suture anchors at the inferior pole. Krackow or locking whipstitches are placed in the tendon stump, passed through the tunnels, and tied over the superior pole of the patella. Augmentation with a cerclage wire or heavy suture tape (e.g., FiberTape) through the tibial tubercle and around the patella may be utilized to protect the repair during early rehabilitation.
STRESS FRACTURE THROUGH THE PATELLA
The identical repetitive eccentric loading forces that precipitate patellar tendinosis can, alternatively, result in a stress fracture of the patella. This entity is most frequently observed in young, skeletally immature athletes or young adults.
Pathomechanics and Management
The mechanical stress concentrates at the junction of the middle and distal thirds of the patella, precisely where the converging fibers of the distal quadriceps tendon and the proximal patellar tendon merge and insert into the osseous architecture.
- Early Stage (Stress Reaction): Initially, the pathology manifests as a stress reaction with low-grade, aching anterior knee pain. If recognized early via MRI (showing bone marrow edema without a distinct fracture line), it responds excellently to conservative management. Strict activity restriction and immobilization for 4 to 6 weeks typically result in complete resolution.
- Late Stage (Stress Fracture): If the athlete continues to train through the pain, a frank stress fracture develops. Non-displaced fractures can be managed with prolonged immobilization in a cylinder cast or locked brace. Displaced stress fractures compromise the extensor mechanism and require open reduction and internal fixation (ORIF), typically utilizing tension-band wiring techniques to convert the tensile forces on the anterior patella into compressive forces at the articular surface.
📚 Medical References
- : a follow-up study of surgical treatment, J Bone Joint Surg 84A:2179, 2002.
- Fischer WR, Shepanek LA: Avulsion of the insertion of the biceps brachii: report of a case, J Bone Joint Surg 38A:158, 1956.
- Foxworthy M, Kinninmonth AWG: Median nerve compression in the proximal forearm as a complication of partial rupture of the distal biceps brachii tendon, J Hand Surg 17B:515, 1992.
- Frazier CH: Tendon repairs with Dacron vascular graft suture: a follow-up report, Orthopedics 4:539, 1981.
- Friedmann E: Rupture of the distal biceps brachii tendon: report of 13 cases, JAMA 184:60, 1963.
- Froimson AI, Oh I: Keyhole tenodesis of biceps origin at the shoulder, Clin Orthop Relat Res 112:245, 1975.
- Garrett WE Jr: Injuries to the muscle-tendon unit, Instr Course Lect 37:275, 1988.
- Garrett WE Jr, Califf JC, Bassett FH III: Histochemical correlates of hamstring ruptures, Am J Sports Med 12:98, 1984.
- Gilcreest EL: The common syndrome of rupture, dislocation and elongation of the long head of the biceps brachii, Surg Gynecol Obstet 58:322, 1934.
- Gilcreest EL: Dislocation and elongation of the long head of the biceps brachii, Ann Surg 104:118, 1936.
- Gilcreest EL, Albi P: Unusual lesions of muscles and tendons of the shoulder girdle and upper arm, Surg Gynecol Obstet 68:903, 1939.
- Goren D, Ayalon M, Nyska M: Isokinetic strength and endurance after percutaneous and open surgical repair of Achilles tendon ruptures, Foot Ankle Int 26:286, 2005.
- Gorschewsky O, Pitzi M, Putz A, et al: Percutaneous repair of acute Achilles tendon rupture, Foot Ankle Int 25:219, 2004.
- Greenberg JA, Fernandez JJ, Wang T, et al: EndoButton-assisted repair of distal biceps tendon ruptures, J Shoulder Elbow Surg 12:484, 2003.
- Greis PE, Holmstrom MC, Lahav A: Surgical treatment options for patella tendon supture, part I: acute, Orthopedics 28:672, 2005.
- Greis PE, Lahav A, Holmstrom MC: Surgical treatment options for patella tendon rupture, part II: chronic, Orthopedics 28:765, 2005.
- Hang DW, Bach BR, Bojchuk J: Repair of chronic distal biceps brachii tendon rupture using free autogenous semitendinosus tendon, Clin Orthop Relat Res 323:188, 1996.
- Hardy J, Chimutengwende-Gordon M, Bakar I: Rupture of the quadriceps tendon: an association with a patellar spur, J Bone Joint Surg 87B:1361, 2005.
- Hitchcock HH, Bechtol CO: Painful shoulder: observations on the role of the tendon of the long head of the biceps brachii in its causation, J Bone Joint Surg 30A:263, 1948.
- Hoksrud A, Ohberg L, Alfredson H, et al: Ultrasound-guided sclerosis of neovessels in painful chronic patellar tendinopathy: a randomized controlled trial, Am J Sports Med 34:1738, 2006.
- Ilan DI, Tejwani N, Keschner M, et al: Quadriceps tendon rupture, J Am Acad Orthop Surg 11:192, 2003.
- Inglis AE, Scott WN, Sculco TP, et al: Ruptures of the tendo Achillis: an objective assessment of surgical and non-surgical management, J Bone Joint Surg 58A:990, 1976.
- Inglis AE, Sculco TP: Surgical repair of ruptures of the tendo Achillis, Clin Orthop Relat Res 156:160, 1981.
- Jacobs D, Martens M, Van Audekercke R, et al: Comparison of conservative and operative treatment of Achilles tendon rupture, Am J Sports Med 6:107, 1978.
- Jobe MT, Azar FM, Calandruccio JH, et al: Surgical repair of ruptures of the distal biceps, Orthop Trans 19:783, 1996.
- John CK, Field LD, Weiss KS, et al: Single-incision repair of acute distal biceps ruptures by use of suture anchors, J Shoulder Elbow Surg 16:78, 2007.
- Kangas J, Pajala A, Siira P, et al: Early functional treatment versus early immobilization in tension of the musculoskeletal unit after Achilles tendon repair: a prospective, randomized clinical study, J Trauma 54:1171, 2003.
- Kaplan FT, Rokito AS, Birdzell MG, et al: Reconstruction of chronic distal biceps tendon supture with the use of fascia lata combined with a ligament augmentation device: a report of 3 cases, J Shoulder Elbow Surg 11:633, 2002.
- Kawashima M, Sato M, Torisu T, et al: Rupture of the pectoralis major: report of two cases, Clin Orthop Relat Res 109:115, 1975.
- Kelikian H, Riashi E, Gleason J: Restoration of quadriceps function in neglected tear of the patellar tendon, Surg Gynecol Obstet 104:200, 1957.
- Kellam JF, Hunter GA, McElwain JP: Review of the operative treatment of Achilles tendon rupture, Clin Orthop Relat Res 201:80, 1985.
- Kelly DW, Carter VS, Jobe FW, et al: Patellar and quadriceps tendon ruptures—jumper’s knee, Am J Sports Med 12:375, 1984.
- Kelly DW, Godfrey KD, Johanson PH, et al: Quadriceps rupture in association with the radiographic “tooth” sign: a case report, Orthopedics 3:1207, 1980.
- Kelly EW, Steinmann S, O’Driscoll SW: Surgical treatment of partial distal biceps tendon ruptures through a single posterior incision, J Shoulder Elbow Surg 12:456, 2003.
- Kettunen JA, Kvist M, Alanen E, et al: Long-term prognosis for jumper’s knee in male athletes: a prospective follow-up study, Am J Sports Med 30:689, 2002.
- Khan RJ, Fick D, Keogh A, et al: Treatment of acute Achilles tendon ruptures: a meta-analysis of randomized, controlled trials, J Bone Joint Surg 87A:2202, 2005.
- Klonz A, Loitz D, Wohler P, et al: Rupture of the distal biceps brachii tendon: isokinetic power analysis and complications after anatomic reinsertion compared with fi xation to the brachialis muscle, J Shoulder Elbow Surg 12:607, 2003.
- Kocher MS, Bishop J, Marshall R, et al: Operative versus nonoperative management of acute Achilles tendon rupture: expected-value decision analysis, Am J Sports Med 30:783, 2002.
- Krackow KA, Thomas SC, Jones LC: A new stitch for ligamenttendon fi xation, J Bone Joint Surg 68A:764, 1986.
- Krushinski EM, Brown JA, Murthi AM: Distal biceps tendon rupture: biomechanical analysis of repair strength of the BioTenodesis screw versus suture anchors, J Shoulder Elbow Surg 16:218, 2007.
- Lansdaal JR, Goslings JC, Reichart M, et al: The results of 163 Achilles tendon ruptures treated by a minimally invasive surgical technique and functional aftertreatment, Injury 38:839, 2007.
- Lea RB, Smith L: Non-surgical treatment of tendo Achillis rupture, J Bone Joint Surg 54A:1398, 1972.
- Le Huec JC, Moinard M, Liquois F, et al: Distal rupture of the tendon of biceps brachii, J Bone Joint Surg 78B:767, 1996.
- Leighton MM, Bush-Joseph CA, Bach BR Jr: Distal biceps brachii repair: results in dominant and nondominant extremities, Clin Orthop Relat Res 317:114, 1995.
- Leslie HD, Edwards WH: Neglected ruptures of the Achilles tendon, Foot Ankle Clin 10:357, 2005.
- Levin PD: Reconstruction of the patellar tendon using a Dacron graft: a case report, Clin Orthop Relat Res 118:70, 1976.
- Levy M: Brief report: repair of triceps tendon avulsions or ruptures, J Bone Joint Surg 69B:115, 1987.
- Levy M, Velkes S, Goldstein J, et al: A method of repair for Achilles tendon ruptures without cast immobilization: preliminary report, Clin Orthop Relat Res 187:199, 1984.
- Lian OB, Engebretsen L, Bahr R: Prevalence of jumper’s knee among elite athletes from different sports: a cross-sectional study, Am J Sports Med 33:561, 2005.
- Lieberman JR, Lozman J, Czajka J, et al: Repair of Achilles tendon ruptures with Dacron vascular graft, Clin Orthop Relat Res 234:204, 1988.
- Lim J, Dalal R, Waseem M: Percutaneous vs. open repair of the ruptured Achilled tendon—a prospective randomized controlled study, Foot Ankle Int 22:559, 2001.
- Lindholm A: A new method of operation in subcutaneous rupture of the Achilles tendon, Acta Chir Scand 117:261, 1959.
- Lynn TA: Repair of the torn Achilles tendon, using the plantaris tendon as a reinforcing membrane, J Bone Joint Surg 48A:268, 1966.
- Ma GWC, Griffi th TG: Percutaneous repair of acute closed ruptured Achilles tendon, Clin Orthop Relat Res 128:247, 1977.
- Mair SD, Isbell WM, Gill TJ, et al: Triceps tendon ruptures in professional football players, Am J Sports Med 32:431, 2004.
- Mandelbaum BR, Bartolozzi A, Carney B: A systematic approach to reconstruction of neglected tears of the patellar tendon: a case report, Clin Orthop Relat Res 235:268, 1988.
- Mandelbaum BR, Myerson MS, Forster R: Achilles tendon ruptures: a new method of repair, early range of motion, and functional rehabilitation, Am J Sports Med 23:392, 1995.
- Marder RA, Timmerman LA: Primary repair of patellar tendon rupture without augmentation, Am J Sports Med 27:304, 1999.
- Mariani EM, Cofi eld RH, Askew LJ, et al: Rupture of the tendon of the long head of the biceps brachii: surgical versus nonsurgical treatment, Clin Orthop Relat Res 228:233, 1988.
- Martens M, Wouters P, Burssens A, et al: Patellar tendinitis: pathology and results of treatment, Acta Orthop Scand 53:445, 1982.
- Matava MJ: Patellar tendon ruptures, J Am Acad Orthop Surg 4:287, 1996.
- McClure JG: Gastrocnemius musculotendinous rupture: a condition confused with thrombophlebitis, South Med J 77:1143, 1984.
- McKee MD, Hirji R, Schemitsch EH, et al: Patient-oriented functional outcome after repair of distal biceps tendon ruptures using a single-incision technique, J Shoulder Elbow Surg 14:302, 2005.
- McLaughlin HL, Francis KC: Operative repair of injuries to the quadriceps extensor mechanism, Am J Surg 91:651, 1956.
- McMaster PE: Tendon and muscle ruptures, J Bone Joint Surg 15:705, 1933.
- McReynolds IS: Avulsion of the insertion of the biceps brachii tendon, a method of surgical repair. Personal communication, Oct 1944.
- Meherin JM, Kilgore ES Jr: The treatment of ruptures of the distal biceps brachii tendon, Am J Surg 99:636, 1960.
- Moller M, Movin T, Granhed H, et al: Acute rupture of tendon Achilles: a prospective randomised study of comparison between surgical and non-surgical treatment, J Bone Joint Surg 84B:843, 2001.
- Morrey BF, Askew LJ, An K, et al: Rupture of the distal tendon of the biceps brachii: a biomechanical study, J Bone Joint Surg 67A:418, 1985.
- Neer CS II, Bigliani LU, Hawkins RJ: Rupture of the long head of the biceps related to subacromial impingement, Orthop Trans 1:111, 1977 (abstract). Neer CS II, Craig EV, Fukuda H: Cuff-tear arthropathy, J Bone Joint Surg 65A:1232, 1983.
- Neer CS II, Welsh RP: The shoulder in sports, Orthop Clin North Am 8:583, 1977.
- Neviaser TJ: The role of the biceps tendon in the
Detailed Chapters & Topics
Dive deeper into specialized chapters regarding rupture-of-gastrocnemius-muscle
