Unlock Stable Arthrodesis with Blade Plate Fixation
Key Takeaway
This topic focuses on Unlock Stable Arthrodesis with Blade Plate Fixation, Tibiotalocalcaneal arthritis involves cartilage loss in both the ankle and subtalar joints, causing significant pain and disability. Tibiotalocalcaneal arthrodesis is performed to achieve a stable, pain-free foot. In cases with osteopenic bone where stable fixation is challenging, blade plate fixation demonstrates higher initial and final stiffness for effective joint fusion, as shown in biomechanical studies.
Introduction and Epidemiology
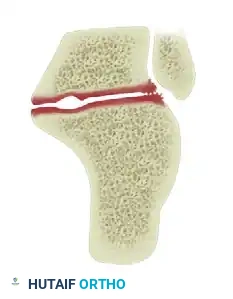
Tibiotalocalcaneal arthritis is formally defined as the progressive loss of articular cartilage from both the tibiotalar (ankle) and the talocalcaneal (subtalar) joints. This dual-joint arthropathy presents a complex reconstructive challenge, as the natural history of hindfoot arthritis is characterized by progressive deformity, severe pain, and profound functional limitation. Epidemiological data indicates that end-stage ankle and hindfoot arthritis produces a degree of physical disability equivalent to that of end-stage hip or knee osteoarthritis.

The etiology of tibiotalocalcaneal arthritis is diverse, encompassing primary osteoarthritis, post-traumatic arthrosis, neuroarthropathy (Charcot), chronic infection, avascular necrosis of the talus, inflammatory arthropathies, and failed prior surgical interventions such as total ankle arthroplasty. Among these, post-traumatic arthritis remains the most prevalent, frequently resulting from pilon fractures, severe rotational ankle fractures, or talar body and neck fractures where articular congruency could not be anatomically restored.

Nonoperative treatment modalities, including the utilization of an ankle-foot orthosis or rigid custom bracing, are inherently limited. While these conservative measures may partially mitigate pain by restricting motion, they do not arrest the progression of the disease and are generally ineffective in correcting progressive structural deformity. Consequently, surgical intervention is frequently mandated.

The primary objective of tibiotalocalcaneal arthrodesis is the creation of a stable, plantigrade, and pain-free foot and ankle complex. Achieving rigid intraoperative fixation is paramount to obtaining a solid osseous union, a task that becomes exceedingly difficult in the presence of osteopenic bone, massive bone loss, or neuropathic conditions. Biomechanical investigations have demonstrated that blade plate fixation of the tibiotalocalcaneal joint offers superior initial and final construct stiffness compared to traditional intramedullary nailing in specific clinical scenarios, particularly when the lateral tension band principle is effectively applied.
Surgical Anatomy and Biomechanics
A profound understanding of the osseous architecture, vascular supply, and neuroanatomy of the hindfoot is essential for executing a successful tibiotalocalcaneal arthrodesis.
Osseous Architecture
The ankle joint is a highly congruent hinge joint comprising the talus articulating within the mortise created by the distal tibia and fibula. The body of the talus is saddle-shaped dorsally, exhibiting a wider anterior dimension and narrowing posteriorly. This trapezoidal geometry accommodates the necessary internal and external rotation coupled with ankle dorsiflexion and plantarflexion.

The subtalar joint is anatomically complex, consisting of the talus and the calcaneus articulating through three distinct facets: anterior, middle, and posterior. The posterior facet is the largest and bears the majority of the load, making it a critical target for meticulous preparation during arthrodesis.

The talus itself is structurally divided into the head, neck, and body. Uniquely, approximately 70 percent of the talar surface is covered with articular cartilage, and it is devoid of any direct muscular or tendinous attachments.

Vascular Supply and Innervation
The precarious vascularity of the talus dictates surgical decision-making. The primary blood supply to the talar body enters in a retrograde fashion through the vascular foramina in the talar neck, predominantly via the artery of the tarsal canal (a branch of the posterior tibial artery) and the deltoid branch. This retrograde flow renders the talar body highly susceptible to avascular necrosis following displaced talar neck fractures or extensive surgical dissection.

Neurologically, the lateral aspect of the foot and ankle, which is the primary surgical corridor for blade plate application, is innervated by the superficial peroneal and sural nerves. The superficial peroneal nerve typically pierces the crural fascia 10 to 12 cm proximal to the tip of the lateral malleolus, coursing anteriorly to supply sensation to the dorsal foot. The sural nerve, formed by contributions from the tibial and common peroneal nerves, courses distally along the posterolateral calf, adjacent to the Achilles tendon, and is consistently located approximately 1 cm distal and posterior to the tip of the fibula.

Biomechanical Principles of Blade Plate Fixation
Blade plate fixation utilizes a lateral approach, capitalizing on the tension band principle. By placing a rigid, fixed-angle construct on the lateral aspect of the tibia, talus, and calcaneus, the plate converts physiological varus bending moments into compressive forces across the arthrodesis sites.

The geometry of the blade allows for broad purchase within the dense trabecular bone of the calcaneal tuberosity. When combined with dynamic compression applied through the vertical limb of the plate on the tibial shaft, the construct achieves exceptional resistance to torsional, bending, and shear forces, which is particularly beneficial in patients with compromised bone density or massive talar defects.
Indications and Contraindications
The decision to proceed with tibiotalocalcaneal arthrodesis utilizing a blade plate must be carefully weighed against the patient's physiological status, bone quality, and soft tissue envelope.

Primary indications include severe, symptomatic tibiotalar and subtalar arthritis that has failed exhaustive nonoperative management. It is particularly advantageous in scenarios where intramedullary nailing is contraindicated or mechanically unfavorable. Examples include significant extra-articular distal tibial deformity that precludes straight nail passage, obliteration of the tibial medullary canal, or the presence of a retained total knee arthroplasty with a long intramedullary stem.

Blade plate fixation is also highly indicated in salvage procedures for failed total ankle arthroplasty, where massive bone voids require structural allograft interposition, as the plate can bridge the defect and provide rigid lateral support.

Contraindications are primarily related to active infection, severe peripheral arterial disease, and inadequate soft tissue coverage over the lateral hindfoot.
| Clinical Scenario | Operative Indication | Non Operative Indication |
|---|---|---|
| End Stage Primary Osteoarthritis | Refractory pain, progressive structural deformity | Mild symptoms, high surgical risk |
| Charcot Neuroarthropathy | Unstable plantigrade foot, impending ulceration | Stable, braceable deformity without ulceration |
| Failed Total Ankle Arthroplasty | Aseptic loosening, severe subsidence, bone loss | Asymptomatic radiolucency (surveillance) |
| Talar Avascular Necrosis | Collapse of the talar dome, intractable pain | Pre-collapse (variable management) |
| Active Deep Infection | Contraindicated (requires staged eradication first) | Suppressive antibiotics if poor surgical candidate |
| Severe Peripheral Vascular Disease | Contraindicated (high risk of amputation) | Bracing, vascular surgery consultation |
Pre Operative Planning and Patient Positioning
Comprehensive preoperative planning begins with a meticulous clinical evaluation. Gait analysis requires observing the patient in both the coronal and sagittal planes to document antalgia and the reliance on assistive devices. Hindfoot alignment must be assessed from a posterior viewpoint to quantify varus or valgus malalignment. Active and passive sagittal plane motion of the tibiotalar joint, as well as inversion and eversion of the subtalar joint, must be documented.

Radiographic evaluation is critical. Standard weight-bearing anteroposterior, lateral, and mortise views of the ankle, along with weight-bearing views of the foot, are mandatory. Advanced imaging, such as Computed Tomography, is highly recommended to assess the precise extent of articular degeneration, evaluate subchondral cysts, and quantify available bone stock for hardware purchase. Magnetic Resonance Imaging may be utilized if avascular necrosis of the talus is suspected but not definitively seen on plain radiographs.

Preoperative templating is essential to determine the appropriate blade length and plate length. The surgeon must calculate the angle of insertion to ensure the blade resides centrally within the calcaneal tuberosity without breaching the medial cortex or the plantar aspect of the calcaneus.

Patient Positioning and Setup
The patient is typically placed in the lateral decubitus position to provide unhindered access to the lateral aspect of the distal tibia, fibula, and hindfoot. A beanbag is utilized to secure the torso, and all bony prominences are meticulously padded. Alternatively, a supine position with a large ipsilateral hip bump can be utilized if concurrent access to the medial side or the iliac crest (for autograft harvest) is anticipated.

A radiolucent table is mandatory to facilitate unobstructed intraoperative fluoroscopy. The C-arm should be positioned to easily obtain true anteroposterior, lateral, and axial views of the hindfoot. A pneumatic tourniquet is applied to the proximal thigh to ensure a bloodless surgical field during the critical stages of joint preparation.

Detailed Surgical Approach and Technique
The transfibular approach is the gold standard for lateral blade plate application, providing excellent exposure of both the tibiotalar and subtalar joints while allowing for the utilization of the resected fibula as an autogenous bone graft.
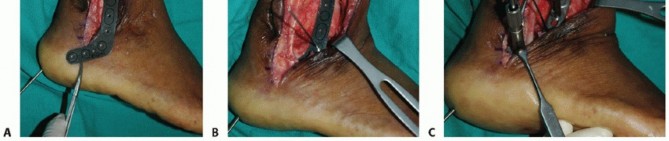
Incision and Superficial Dissection
A longitudinal incision is made over the posterolateral aspect of the distal fibula, extending from approximately 10 to 15 cm proximal to the tip of the lateral malleolus, curving slightly anteriorly toward the base of the fourth metatarsal.

Full-thickness fasciocutaneous flaps are elevated to preserve the delicate subdermal vascular plexus. The sural nerve and the lesser saphenous vein are identified in the distal aspect of the incision, carefully mobilized, and protected with vessel loops. Retraction of these structures should be gentle to prevent neuropraxia.

Fibular Osteotomy and Joint Preparation
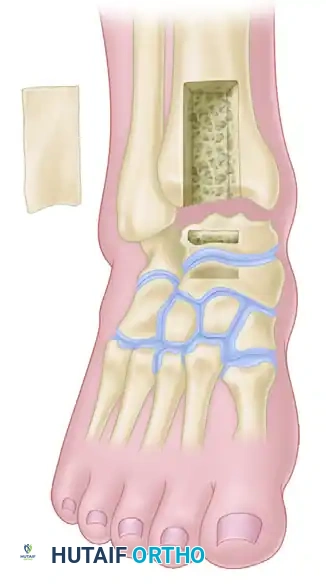
The periosteum over the distal fibula is incised longitudinally. An oscillating saw is used to perform a transverse or oblique fibular osteotomy approximately 2 to 3 cm proximal to the level of the tibial plafond.

The distal fibular segment is carefully excised by sharply dissecting the anterior and posterior tibiofibular ligaments, the calcaneofibular ligament, and the anterior talofibular ligament. This resected fibula is passed to the back table to be morselized for later use as autograft.

With the lateral hindfoot exposed, the tibiotalar and subtalar joints are systematically distracted using a lamina spreader or a specialized joint distractor. All residual articular cartilage is meticulously resected using a combination of sharp osteotomes, ring curettes, and high-speed burrs.

The subchondral bone must be aggressively denuded to expose bleeding, healthy cancellous bone. The surfaces are then repeatedly shingled or feathered with a narrow osteotome to maximize the surface area for osteogenesis and facilitate vascular ingrowth across the arthrodesis sites.

Deformity Correction and Provisional Fixation
Optimal alignment is the most critical determinant of long-term functional success. The foot must be positioned in neutral dorsiflexion (0 degrees), approximately 5 degrees of hindfoot valgus, and 5 to 10 degrees of external rotation (matching the contralateral extremity). Furthermore, the talus should be translated slightly posteriorly beneath the tibia to optimize the biomechanical lever arm of the Achilles tendon.

Once ideal alignment is achieved, provisional fixation is secured using multiple heavy, threaded Kirschner wires or Steinmann pins driven from the plantar aspect of the calcaneus, through the talus, and into the distal tibia. Alignment is rigorously verified in multiple planes using intraoperative fluoroscopy.

Blade Plate Preparation and Insertion
A 90-degree cannulated blade plate is typically selected. The starting point for the blade is identified on the lateral aspect of the calcaneus, taking care to avoid the subtalar joint superiorly and the plantar cortex inferiorly.

A guide wire is inserted from lateral to medial into the calcaneal tuberosity, parallel to the plantar surface of the foot and perpendicular to the long axis of the calcaneus in the axial plane. Fluoroscopy confirms wire placement. The lateral cortex is opened with a cannulated drill, and the seating chisel is subsequently driven over the wire to create the precise track for the blade.

The chisel is removed, and the blade plate is inserted into the prepared track. As the blade is seated, the vertical limb of the plate is aligned with the lateral cortex of the tibia.

An articulated tensioning device is attached to the proximal aspect of the plate on the tibia. Compression is applied across both the subtalar and tibiotalar joints simultaneously.

Once maximum compression is achieved, the plate is secured to the tibia with multiple bicortical screws. Additional fixation can be obtained by placing screws through the plate directly into the talus, further increasing construct rigidity.

Bone Grafting and Closure
The previously harvested fibular autograft, supplemented with allograft or demineralized bone matrix if necessary, is packed tightly into any remaining voids within the sinus tarsi, the lateral gutters, and the arthrodesis interfaces.

A closed suction drain may be placed depending on the degree of oozing. The deep fascia is meticulously closed over the plate to the extent possible, followed by layered closure of the subcutaneous tissues and skin. A sterile dressing and a well-padded, short-leg posterior splint in neutral alignment are applied.
Complications and Management
Tibiotalocalcaneal arthrodesis is a major reconstructive procedure associated with a significant complication profile, particularly in patients with multiple medical comorbidities.
| Complication | Estimated Incidence | Prevention and Salvage Strategies |
|---|---|---|
| Nonunion (Pseudoarthrosis) | 10% - 15% | Prevention: Meticulous joint preparation, rigid compression, smoking cessation. Salvage: Revision arthrodesis with structural grafting, bone stimulators, modification of fixation construct. |
| Wound Dehiscence / Infection | 5% - 10% | Prevention: Respect soft tissue envelopes, optimize glycemic control, precise flap handling. Salvage: Aggressive serial debridement, targeted intravenous antibiotics, negative pressure wound therapy, potential hardware removal once fused. |
| Malunion | 5% - 8% | Prevention: Rigorous intraoperative fluoroscopic checks, precise provisional pinning. Salvage: Corrective osteotomy if symptomatic, custom orthotic accommodation. |
| Sural Nerve Injury | 3% - 5% | Prevention: Careful superficial dissection, avoidance of excessive retraction. Salvage: Neuromodulating medications, surgical excision and burying of neuroma into muscle or bone. |
| Symptomatic Prominent Hardware | 10% - 20% | Prevention: Adequate soft tissue coverage, accurate plate templating. Salvage: Hardware removal after definitive radiographic and clinical confirmation of solid osseous union |
Clinical & Radiographic Imaging































You Might Also Like