Salvage Your Scapular Winging: Understanding Scapulothoracic Arthrodesis
Key Takeaway
We review everything you need to understand about Salvage Your Scapular Winging: Understanding Scapulothoracic Arthrodesis. Scapulothoracic arthrodesis is a surgical intervention for severe, refractory disorders of the scapulothoracic articulation, often presenting as debilitating pain and scapular winging. This procedure is the treatment of choice following failed muscle transfers or for significant, irreducible scapular winging. It functions as a successful salvage operation to stabilize the scapula and restore function.
Introduction and Epidemiology
Refractory disorders of the scapulothoracic articulation represent a complex and challenging subset of shoulder pathology. These conditions frequently result in debilitating pain, profound upper extremity dysfunction, and significant cosmetic deformity that ultimately require surgical management. The most common clinical presentation of scapulothoracic dysfunction is scapular winging, a phenomenon first described in the published medical literature in 1723. Since that initial documentation, a broad spectrum of etiologies responsible for scapular dyskinesia and winging has been elucidated.

Traumatic injuries to the serratus anterior muscle or its innervation, the long thoracic nerve, are frequently cited causes of symptomatic medial winging. Conversely, injury to the spinal accessory nerve results in trapezius paralysis and lateral winging. Atraumatic etiologies also account for a significant proportion of cases. Conditions such as neuralgic amyotrophy (Parsonage-Turner syndrome), poliomyelitis, and muscular dystrophies—most notably facioscapulohumeral dystrophy (FSHD)—can produce disabling, progressive scapular winging.

Historically, soft tissue operations, such as the Eden-Lange procedure for trapezius palsy or pectoralis major tendon transfers for serratus anterior palsy, have demonstrated success in stabilizing the dyskinetic scapula in appropriately selected patients. However, despite successful initial clinical outcomes, a distinct population of patients experiences recurrent, highly symptomatic scapular winging even after technically sound muscle transfers. Furthermore, patients with progressive myopathies such as FSHD are often poor candidates for dynamic tendon transfers due to the global nature of their muscle weakness.
For these challenging clinical scenarios—including failed pectoralis major transfers, significant irreducible fixed winging, and progressive muscular dystrophies—scapulothoracic arthrodesis remains the definitive salvage operation. When executed with meticulous surgical technique, arthrodesis successfully restores the stable fulcrum necessary for glenohumeral elevation, thereby significantly improving functional capacity and alleviating debilitating scapulothoracic pain.
Surgical Anatomy and Biomechanics
A profound understanding of scapulothoracic anatomy and biomechanics is paramount when undertaking an arthrodesis, as the procedure fundamentally alters the kinetic chain of the upper extremity.
Osseous Architecture and Articulation
The scapula is a flat, triangular bone positioned over the posterolateral aspect of the thoracic cage, typically overlying ribs one through seven in its resting anatomical position. It is suspended from the axial skeleton anteriorly by the clavicle via the acromioclavicular and sternoclavicular joints. The lateral aspect of the scapula features the glenoid fossa, which articulates with the humeral head to form the glenohumeral joint.

Unlike true diarthrodial joints, the scapulothoracic articulation lacks a true joint capsule or articular cartilage. Instead, it functions as a physiological joint where the concave anterior surface of the scapula glides over the convex posterior thoracic wall. A thin, specialized bursal layer—comprising the supraserratus and infraserratus bursae—separates the scapula from the underlying ribs, facilitating smooth, frictionless motion during upper extremity kinematics.

Muscular and Neural Anatomy
The scapula serves as the origin or insertion site for 16 distinct muscles, which act in highly coordinated force couples to maintain functional positioning and dynamic stability. The primary stabilizers include the trapezius (innervated by the spinal accessory nerve, cranial nerve XI), the serratus anterior (innervated by the long thoracic nerve, C5-C7), the rhomboids, and the levator scapulae (innervated by the dorsal scapular nerve, C5).

Dysfunction in any of these critical stabilizers disrupts the delicate balance of forces. For instance, serratus anterior paralysis leads to unopposed action of the trapezius and rhomboids, resulting in medial translation and prominent medial winging of the scapula. Trapezius paralysis results in lateral winging and drooping of the shoulder girdle.

Biomechanics of Scapulohumeral Rhythm
Normal shoulder elevation relies on synchronous motion between the glenohumeral and scapulothoracic joints, classically described as a 2 to 1 ratio. For every 3 degrees of overall shoulder elevation, 2 degrees occur at the glenohumeral joint and 1 degree occurs at the scapulothoracic articulation. The scapula must upwardly rotate, posteriorly tilt, and externally rotate to clear the acromion from the greater tuberosity, thereby preventing subacromial impingement and maximizing the mechanical advantage of the deltoid and rotator cuff.
When scapulothoracic arthrodesis is performed, this dynamic rhythm is intentionally obliterated. The scapula is fixed to the thoracic cage, meaning all subsequent shoulder elevation must occur strictly through the glenohumeral joint. Consequently, maximum postoperative elevation is typically limited to 90 to 110 degrees. The precise intraoperative positioning of the fused scapula is therefore the most critical determinant of postoperative function.
Indications and Contraindications
Patient selection is the cornerstone of successful scapulothoracic arthrodesis. Most patients presenting with symptomatic scapular winging, scapulothoracic pain, or crepitus respond favorably to nonoperative measures, including targeted physical therapy focusing on periscapular strengthening, postural re-education, and judicious use of anti-inflammatory modalities. Arthrodesis is strictly reserved for the subset of patients who experience complex dysfunction or pain entirely refractory to conservative management and who are not candidates for dynamic reconstruction.

Primary Indications
The classic indication for primary scapulothoracic arthrodesis is facioscapulohumeral dystrophy (FSHD). In these patients, the periscapular musculature undergoes progressive fatty infiltration and atrophy, rendering dynamic tendon transfers futile. Fixing the scapula to the thorax provides a stable base, allowing the often-preserved deltoid muscle to effectively elevate the arm.

Arthrodesis is also indicated as a salvage procedure for failed soft tissue operations, such as a failed pectoralis major transfer for serratus anterior palsy or a failed Eden-Lange procedure for trapezius palsy. Additional indications include severe, irreducible fixed winging secondary to malunited scapular fractures, extensive muscle avulsions, or severe brachial plexus injuries where regional muscle donors are unavailable.

Contraindications
Absolute contraindications include active surgical site infection, profound medical comorbidities precluding general anesthesia, and the absence of a functional glenohumeral joint (e.g., severe rotator cuff arthropathy or glenohumeral osteoarthritis), as fixing the scapula in the setting of a stiff or painful glenohumeral joint will result in a completely non-functional extremity.
| Parameter | Operative Indications for Arthrodesis | Non-Operative / Contraindications |
|---|---|---|
| Primary Pathology | Facioscapulohumeral dystrophy (FSHD) | Early, acute nerve palsy (e.g., Parsonage-Turner) |
| Previous Surgery | Failed dynamic tendon transfers | Intact, functional dynamic transfer options |
| Glenohumeral Status | Functional deltoid and rotator cuff | Severe glenohumeral arthritis or cuff tear arthropathy |
| Bone Quality | Adequate scapular and rib bone stock | Severe osteopenia or prior extensive rib resections |
| Patient Factors | Intractable pain, severe functional deficit | Medical instability, inability to comply with strict rehab |
Pre Operative Planning and Patient Positioning
Thorough preoperative evaluation includes a comprehensive physical examination focusing on the resting posture of the scapula and its dynamic position. Both scapulae must be observed and palpated while the arms are elevated or while the patient performs a wall push-up to assess the degree of dyskinesia.
Advanced Imaging and Diagnostics
Standard radiographic evaluation includes true anteroposterior, scapular Y, and axillary lateral views of the shoulder, as well as orthogonal views of the thoracic cage. A fine-cut computed tomography (CT) scan is essential for assessing the bone stock of the medial scapular border and the underlying ribs, particularly in patients with prior trauma or congenital anomalies.

Electromyography (EMG) and nerve conduction studies (NCS) are frequently utilized to objectively map the extent of neurologic deficits or myopathic progression, ensuring that the deltoid and rotator cuff musculature—which will be solely responsible for postoperative arm elevation—remain adequately innervated and functional.

Patient Positioning and Setup
The procedure is typically performed with the patient under general endotracheal anesthesia. The patient is placed in the prone position on a specialized radiolucent table (e.g., Jackson table) with chest rolls to allow for unencumbered respiratory excursion. The operative extremity must be prepped and draped entirely free to allow for intraoperative manipulation of the shoulder girdle and assessment of the scapular position relative to the thoracic cage.

Careful attention must be paid to padding all bony prominences. The head is secured in a neutral position, often using a Mayfield headrest or a specialized prone foam mask, to avoid excessive cervical extension or rotation. Intraoperative fluoroscopy should be positioned to allow for orthogonal views of the scapula and thorax without compromising the sterile field.

Detailed Surgical Approach and Technique
The surgical technique for scapulothoracic arthrodesis requires meticulous soft tissue handling, precise preparation of the osseous surfaces, and rigid internal fixation to achieve a successful union.
Incision and Superficial Dissection
A longitudinal parasagittal incision is made approximately 2 to 3 centimeters medial to the medial border of the scapula, extending from the superior angle to the inferior angle. The subcutaneous tissues are divided to expose the underlying trapezius muscle. Depending on the remaining functional status of the trapezius, the muscle fibers are either split longitudinally in line with their orientation or, if atrophic (as in FSHD), mobilized as a full-thickness flap.

Deep Dissection and Scapular Preparation
The rhomboid major and minor muscles are identified inserting onto the medial border of the scapula. These are detached subperiosteally to expose the anterior (costal) surface of the scapula. The subscapularis and serratus anterior muscle bellies are elevated from the medial aspect of the scapular body.

Using a high-speed burr, osteotomes, and curettes, the cortical bone on the undersurface of the medial scapula is aggressively decorticated to expose bleeding cancellous bone. This decortication typically spans from the superior angle to the inferior angle, encompassing a width of approximately 2 to 3 centimeters.

Rib Exposure and Preparation
Attention is then directed to the thoracic cage. The scapula is retracted laterally to expose the underlying ribs. Arthrodesis is most commonly performed incorporating ribs three, four, and five, though ribs two through six may be utilized depending on the patient's anatomy and the planned fixation construct.

The periosteum of the selected ribs is carefully incised and elevated. Meticulous subperiosteal dissection is critical during this phase to avoid breaching the parietal pleura, which lies immediately deep to the inner rib cortex and intercostal musculature. The outer cortices of the selected ribs are then decorticated to match the prepared bed on the undersurface of the scapula.

Bone Grafting and Scapular Positioning
To maximize the probability of osseous union, autogenous bone graft (typically harvested from the posterior superior iliac spine) or structural allograft is packed into the interfaces between the decorticated ribs and the scapula.

The most critical step of the procedure is establishing the optimal position of the scapula prior to fixation. The consensus in the orthopedic literature recommends positioning the scapula in:
1. 15 to 20 degrees of external rotation (upward rotation of the glenoid).
2. 10 to 15 degrees of forward flexion (internal rotation relative to the thorax).
3. Neutral elevation relative to the contralateral, normal scapula.
This specific orientation maximizes the functional arc of motion of the glenohumeral joint, allowing the patient to reach their face and mouth while avoiding excessive winging or impingement.

Fixation Strategies
Historically, fixation was achieved using heavy non-absorbable sutures or fascial slings. Modern techniques predominantly utilize robust metallic fixation to provide the rigid stability required for arthrodesis.

Cerclage wiring or heavy multifilament cables can be passed circumferentially around the prepared ribs and through drill holes in the medial border of the scapula. Alternatively, custom-contoured reconstruction plates can be applied along the medial border of the scapula, with screws directed through the plate, through the scapula, and into the underlying ribs. Some surgeons advocate for a hybrid approach utilizing both plates and cerclage cables to maximize biomechanical stability and prevent construct failure during the prolonged healing phase.

Following rigid fixation, the surgical site is copiously irrigated. A closed suction drain is placed deep to the muscle layers. The rhomboids and trapezius are meticulously repaired over the hardware to provide robust soft tissue coverage, and the skin is closed in a layered fashion.
Complications and Management
Scapulothoracic arthrodesis is a major structural alteration of the thoracic wall and shoulder girdle, carrying a significant complication profile. Surgeons must be prepared to identify and manage these intraoperative and postoperative challenges.

Pleural Breach and Pneumothorax
The most immediate intraoperative risk is a breach of the parietal pleura during rib exposure or drilling, leading to a pneumothorax. If a pleural tear is identified intraoperatively, it should be repaired primarily if possible, and a small red rubber catheter can be used to evacuate air from the pleural space prior to tying the final suture. A postoperative chest radiograph in the recovery room is mandatory for all patients. Significant pneumothoraces require the insertion of a thoracostomy tube.

Nonunion and Hardware Failure
Nonunion (pseudoarthrosis) is a devastating complication that typically presents with recurrent pain, recurrent winging, and hardware breakage. The risk of nonunion is highest in patients with poor bone quality, inadequate decortication, or insufficient rigid fixation. Management of a symptomatic nonunion requires revision surgery with hardware removal, repeat aggressive decortication, copious structural bone grafting, and application of a more rigid fixation construct.

Hardware Prominence
Due to the relatively thin soft tissue envelope over the medial scapula, hardware prominence is a frequent source of late postoperative pain. Once solid osseous union is confirmed via CT scan (typically 6 to 12 months postoperatively), symptomatic hardware can be safely removed without compromising the arthrodesis.
| Complication | Estimated Incidence | Prevention and Salvage Strategy |
|---|---|---|
| Pneumothorax | 5% - 10% | Meticulous subperiosteal rib dissection; post-op CXR; Chest tube if >20% or symptomatic. |
| Nonunion / Pseudoarthrosis | 10% - 15% | Aggressive decortication, robust bone grafting, rigid multi-point fixation; Revision grafting and plating. |
| Hardware Prominence | 20% - 30% | Low-profile implants, robust muscular closure; Hardware removal after confirmed radiographic union. |
| Pulmonary Restriction | Variable | Avoid fusing >3-4 ribs; Preoperative pulmonary function testing in myopathic patients. |
| Persistent Pain | 10% - 20% | Ensure optimal intraoperative scapular positioning; Rule out nonunion or cervical spine pathology. |
Post Operative Rehabilitation Protocols
The success of a scapulothoracic arthrodesis is heavily dependent on strict adherence to a rigorous postoperative rehabilitation protocol. The primary goal in the initial postoperative phase is the protection of the surgical construct to allow for osseous union.
Immediately following surgery, the patient is placed in a custom-molded thoraco-brachial orthosis or a rigid abduction sling. The arm is typically immobilized in 30 to 45 degrees of abduction and neutral rotation to relieve tension on the fixation construct and soft tissue repair.
Strict immobilization is maintained for a minimum of 6 to 8 weeks. During this period, only passive range of motion of the elbow, wrist, and hand is permitted. Glenohumeral motion is strictly prohibited to prevent micromotion at the arthrodesis site, which could lead to hardware failure and nonunion.
At 6 to 8 weeks, clinical and radiographic evaluations are performed. If early bridging callus is evident, the patient may begin gentle, therapist-assisted passive range of motion of the glenohumeral joint. Active elevation and progressive strengthening are typically delayed until definitive osseous union is confirmed on plain radiographs or CT scan, usually between 12 and 16 weeks postoperatively. Full functional recovery and maximal medical improvement may take up to 12 to 18 months.
Summary of Key Literature and Guidelines
The academic literature consistently supports scapulothoracic arthrodesis as a highly effective salvage procedure for specific indications, though it emphasizes the technical demands and complication risks.
Classic studies by Letournel and later modifications by Cofield established the biomechanical necessity of specific scapular positioning (15-20 degrees of upward rotation) to maximize postoperative glenohumeral elevation. Modern retrospective cohorts evaluating wire versus plate fixation have demonstrated that while both techniques can achieve union, rigid plate fixation combined with robust autogenous bone grafting yields the lowest rates of pseudoarthrosis.
In the context of facioscapulohumeral dystrophy (FSHD), literature reviews indicate a high rate of patient satisfaction and significant improvements in activities of daily living following arthrodesis, provided the deltoid remains functional. For patients undergoing arthrodesis as a salvage for failed dynamic transfers (e.g., failed pectoralis major transfer), outcomes are generally favorable regarding pain relief, though functional gains in active elevation may be more modest compared to the primary FSHD cohort.
Ultimately, surgical guidelines dictate that scapulothoracic arthrodesis should be performed by experienced shoulder surgeons in centers equipped to handle the complex perioperative and rehabilitative demands of the procedure. When executed with precision and appropriate patient selection, it remains an indispensable tool in the orthopedic surgeon's armamentarium for salvaging the severely dyskinetic shoulder.
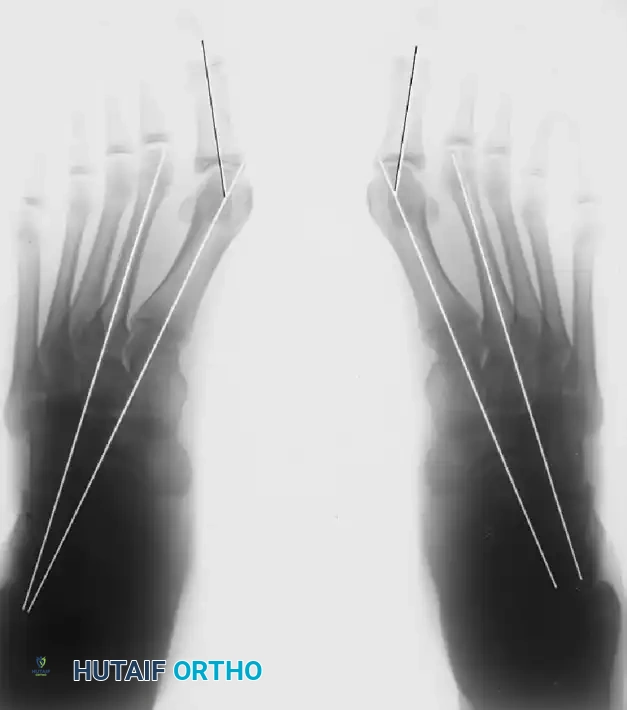
Clinical & Radiographic Imaging

























You Might Also Like