Posterior Subtalar Arthrodesis: The Gallie Technique and Modern Academic Perspectives
Key Takeaway
The Gallie posterior subtalar arthrodesis is a specialized surgical technique indicated for isolated subtalar arthritis without significant coronal plane deformity. By utilizing a posterior approach lateral to the Achilles tendon, surgeons can achieve solid fusion through a posterior mortise and bone grafting. This approach is contraindicated in varus deformities due to the risk of lateral column overload.
INTRODUCTION TO POSTERIOR SUBTALAR ARTHRODESIS
Subtalar arthrodesis remains the gold standard surgical intervention for end-stage, isolated arthritis of the talocalcaneal joint. While the lateral approach to the subtalar joint via the sinus tarsi is the most commonly utilized contemporary method, the posterior approach, originally championed by William E. Gallie, offers a unique, simplified trajectory to the posterior facet.
Gallie advised arthrodesis of the subtalar joint from the posterior aspect primarily because the procedure is technically simpler and avoids the extensive lateral soft tissue dissection required in standard approaches. By accessing the joint posteriorly, the surgeon directly visualizes the posterior facet—the largest and most critical weight-bearing surface of the subtalar complex. However, this historical technique carries highly specific indications and strict biomechanical limitations that the modern orthopedic surgeon must thoroughly understand before implementation.
BIOMECHANICS AND DEFORMITY CONSIDERATIONS
To master the Gallie posterior subtalar arthrodesis, one must first understand the intricate biomechanics of the hindfoot and the profound limitations of this specific surgical approach.
The Subtalar Axis and Hindfoot Alignment
The subtalar joint functions as a complex, single-axis hinge that dictates the inversion and eversion of the hindfoot. This motion is inextricably linked to the transverse tarsal joint (talonavicular and calcaneocuboid joints). When the calcaneus is in valgus (eversion), the axes of the transverse tarsal joints become parallel, unlocking the midfoot and allowing for shock absorption during the heel-strike phase of gait. Conversely, when the calcaneus is in varus (inversion), these axes diverge, locking the midfoot to provide a rigid lever arm for toe-off.
The Limitation of the Posterior Approach
The critical limitation of the Gallie posterior approach is that it does not allow for the correction of varus or valgus malalignment of the calcaneus, nor does it permit the correction of complex multiplanar foot deformities. The posterior mortise technique locks the calcaneus in its in situ position.
Surgical Warning: The Gallie operation is strictly contraindicated if the primary deformity is one of varus. Fusing the subtalar joint in a varus position locks the transverse tarsal joint, creating a rigid, inflexible midfoot. Consequently, excessive weight-bearing forces are abnormally distributed to the lateral column, specifically concentrating on the head of the fifth metatarsal. This inevitably leads to the formation of a painful, intractable plantar keratosis (callus) and potential stress fractures of the fifth metatarsal.
According to Gallie, a mild valgus position of the heel (up to 5 degrees) is physiologically acceptable and can usually be disregarded, as it maintains the flexibility of the transverse tarsal joint and mimics the natural resting posture of the hindfoot.
INDICATIONS AND CONTRAINDICATIONS
Indications
The posterior subtalar arthrodesis is indicated in a highly select group of patients:
* Isolated Subtalar Osteoarthritis: Secondary to prior trauma (e.g., calcaneus fractures) where the overall height and alignment of the calcaneus have been preserved.
* Primary Osteoarthritis: Confined strictly to the posterior facet of the subtalar joint.
* Inflammatory Arthritis: Such as rheumatoid arthritis, provided there is no significant hindfoot collapse or valgus drift.
* Talocalcaneal Coalition: In mature patients where resection has failed or is not feasible, and the hindfoot alignment is neutral or in mild, acceptable valgus.
Absolute Contraindications
- Varus Deformity: As previously detailed, fusing the hindfoot in varus is a catastrophic biomechanical error.
- Severe Valgus Deformity: Requires a lateral or medial approach to perform corrective osteotomies or structural bone grafting to restore the calcaneal pitch and medial longitudinal arch.
- Active Infection: Local or systemic.
- Compromised Posterior Soft Tissue Envelope: Poor skin quality over the Achilles tendon or posterior heel.
PREOPERATIVE PLANNING
Meticulous preoperative planning is mandatory to ensure the patient is an appropriate candidate for an in situ posterior fusion.
Clinical Evaluation
Assess the resting posture of the hindfoot with the patient standing. Observe the heel from behind to quantify the degree of varus or valgus. Evaluate the flexibility of the transverse tarsal joint and the presence of any lateral column overload (callosities under the 5th metatarsal head). Assess the vascular status and the integrity of the posterior skin.
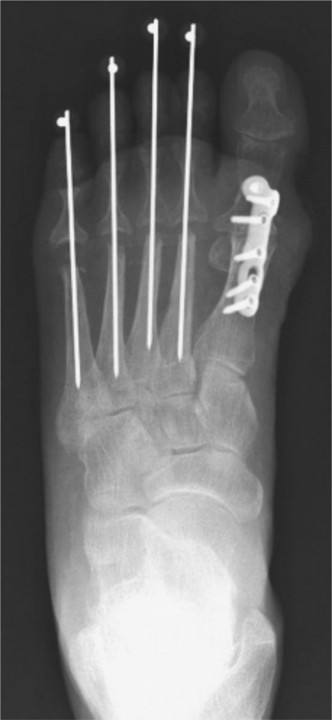
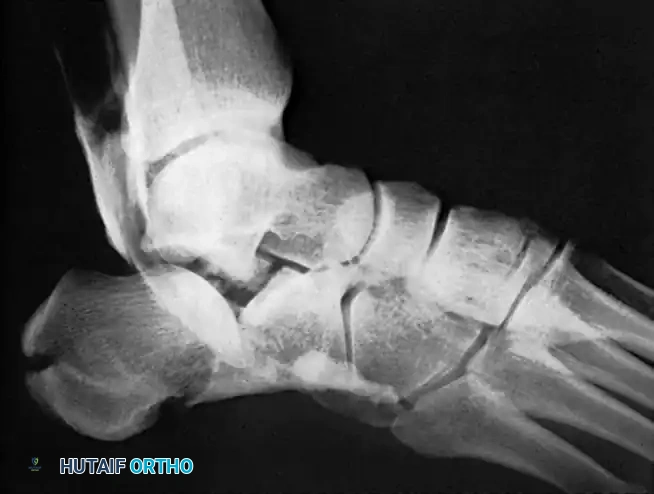
Radiographic Assessment
- Weight-Bearing Radiographs: AP, lateral, and mortise views of the ankle and foot. The lateral view is critical for assessing the posterior facet and the presence of arthritis.
- Harris Heel View: Essential for evaluating the coronal plane alignment of the calcaneus relative to the tibia.
- Computed Tomography (CT): A non-contrast CT scan with sagittal and coronal reconstructions is the gold standard for evaluating the extent of subtalar arthritis, the presence of subchondral cysts, and the exact morphology of the posterior facet.
SURGICAL ANATOMY AND DANGER ZONES
When approaching the subtalar joint posteriorly, the surgeon must navigate several critical anatomical structures:
- The Achilles Tendon: Forms the medial boundary of the surgical approach.
- The Sural Nerve and Lesser Saphenous Vein: Course along the posterolateral aspect of the ankle. The sural nerve is at high risk during the initial incision and superficial dissection.
- The Flexor Hallucis Longus (FHL): Located posteromedially. While the approach is lateral to the Achilles, over-penetration medially during joint preparation can endanger the FHL tendon and the adjacent posteromedial neurovascular bundle (tibial nerve and posterior tibial artery).
SURGICAL TECHNIQUE: THE GALLIE PROCEDURE
The following details the classic Gallie technique, augmented with modern academic insights for safety and efficacy.
Patient Positioning and Anesthesia
- Anesthesia: General anesthesia or regional spinal anesthesia is utilized, supplemented with a popliteal nerve block for postoperative pain control.
- Positioning: The patient is placed in the prone position. Ensure all bony prominences are meticulously padded. The feet should extend just over the edge of the operating table to allow for intraoperative manipulation of the ankle and hindfoot.
- Tourniquet: A well-padded pneumatic tourniquet is applied to the proximal thigh or proximal calf, depending on surgeon preference.
Incision and Superficial Dissection
- Make a longitudinal incision, approximately 6 to 8 cm in length, along the lateral border of the Achilles tendon.
- Deepen the incision through the subcutaneous tissue.
Clinical Pearl: Meticulous hemostasis and blunt dissection in the subcutaneous layer are critical to identify and protect the sural nerve, which typically crosses the lateral border of the Achilles tendon in the distal third of the leg. Retract the nerve laterally.
Capsulotomy and Joint Exposure
- Retract the Achilles tendon medially.
- Identify the posterior capsule of the ankle joint (superiorly) and the subtalar joint (inferiorly).
- Incise the posterior capsule transversely to expose both the posterior aspect of the talus and the superior aspect of the calcaneus.
Pitfall: Do not mistake the posterior ankle joint for the subtalar joint. The subtalar joint lies inferior to the posterior process of the talus.
- Locate the Subtalar Joint: Confirm the location of the subtalar joint by applying medial and lateral (inversion/eversion) motions to the calcaneus. The articulation of the posterior facet will become clearly visible.
- Probe the subtalar joint with a blunt elevator or Freer to determine its general direction, which slopes anteriorly and inferiorly toward the sinus tarsi.
Joint Preparation and Mortise Creation
The hallmark of the Gallie technique is the creation of a posterior mortise to accept a structural bone graft.
- Using a sharp osteotome or a high-speed burr, cut a rectangular mortise centered over the posterior facet, incorporating both the inferior aspect of the talus and the superior aspect of the calcaneus.
- Dimensions: The mortise should be approximately 1.3 cm wide and 0.6 cm deep.
- Depth: Extend the mortise anteriorly and distally, following the trajectory of the posterior facet, reaching as far distally as the sinus tarsi.
- Ensure all remaining articular cartilage within the mortise and the adjacent posterior facet is meticulously denuded down to bleeding subchondral bone to maximize the osteogenic environment.
Bone Grafting Strategies
The Classic Gallie Tibial Graft
Gallie originally described using a structural autograft harvested from the tibia to provide both osteogenic material and mechanical stability via a press-fit mechanism.
1. Flex the patient's knee.
2. Through a separate incision, remove a cortical-cancellous bone graft measuring 6.2 cm long by 1.3 cm wide from the anteromedial surface of the proximal tibia.
3. Divide the harvested graft into two equal parts.
4. Bevel one end of each graft to facilitate insertion.
5. Pack the deepest portion of the subtalar mortise with residual cancellous bone.
6. With their cortical surfaces apposed (facing each other), drive the two tibial grafts into the mortise.
7. If sized correctly, the cancellous surfaces of the grafts will press snugly against the lateral and medial cancellous walls of the calcaneal and talar mortise, providing immediate structural stability.
Modern Evolution: Iliac Crest or Allograft
While Gallie's mechanical concept is sound, harvesting a massive 6.2 cm cortical window from the proximal tibia carries significant donor site morbidity, including a risk of tibial stress fractures.
Modern Academic Perspective: Today, strips of cancellous bone harvested from the posterior or anterior iliac crest are highly preferable to the structural tibial grafts used by Gallie. Cancellous bone provides superior osteoinductive and osteoconductive properties. The mortise is packed tightly with this cancellous autograft. If structural stability is required, modern surgeons will supplement the cancellous graft with rigid internal fixation (e.g., a large cannulated compression screw placed from the posterior calcaneus into the talar dome), rather than relying solely on a press-fit cortical graft.
Closure
- Irrigate the wound copiously with sterile saline.
- Place a closed-suction drain deep within the wound to prevent postoperative hematoma formation, which can compromise the posterior skin envelope.
- Close the subcutaneous tissue with absorbable sutures.
- Close the skin with non-absorbable sutures or surgical staples, ensuring no tension is placed on the skin edges.
POSTOPERATIVE PROTOCOL
Successful arthrodesis relies as much on strict postoperative management as it does on meticulous surgical technique.
Phase I: Immediate Postoperative (Weeks 0-2)
- Immobilization: Apply a bulky, well-padded compressive dressing supported by a posterior splint or a short-leg cast in neutral dorsiflexion.
- Weight-Bearing: Strictly non-weight-bearing (NWB).
- Elevation: The operative limb must be elevated strictly above heart level for the first 48 to 72 hours to minimize edema and protect the posterior skin incision.
- Follow-up: At 2 weeks, the cast is removed, the wound is inspected, and sutures are removed.
Phase II: Intermediate Healing (Weeks 2-6)
- Immobilization: The patient is transitioned into a rigid fiberglass short-leg cast.
- Weight-Bearing: Continued strict non-weight-bearing.
- DVT Prophylaxis: Depending on patient risk factors, chemical prophylaxis may be continued during the period of immobility.
Phase III: Progressive Weight-Bearing (Weeks 6-12)
- Clinical Assessment: At 6 weeks, radiographs are obtained to assess early trabecular bridging across the arthrodesis site.
- Immobilization: If radiographic healing is progressing, the patient is transitioned to a controlled ankle motion (CAM) boot.
- Weight-Bearing: Progressive partial weight-bearing is initiated, advancing to full weight-bearing as tolerated by week 8 to 10.
- Physical Therapy: Gentle active range of motion of the ankle (tibiotalar joint) and midfoot is encouraged to prevent secondary stiffness.
COMPLICATIONS AND PITFALLS
Despite its relative simplicity, the posterior subtalar arthrodesis carries specific risks:
- Malunion (Varus Deformity): The most devastating complication. If the joint is fused in varus, the patient will develop lateral column pain and midfoot rigidity. This underscores the importance of strict patient selection.
- Nonunion (Pseudarthrosis): Subtalar nonunion rates range from 5% to 15%. Risk factors include smoking, diabetes, inadequate joint debridement, and failure to achieve a tight press-fit with the bone graft. Treatment requires revision arthrodesis, often with supplemental internal fixation and orthobiologics.
- Sural Nerve Injury: Neuroma formation or numbness along the lateral border of the foot can occur if the sural nerve is lacerated or aggressively retracted during the initial approach.
- Wound Dehiscence: The posterior skin over the Achilles tendon has a tenuous blood supply. Excessive retraction, postoperative hematoma, or premature dependency of the limb can lead to wound breakdown and deep infection.
CONCLUSION
The Gallie posterior subtalar arthrodesis is a historically significant procedure that retains utility in the modern orthopedic armamentarium for a highly specific subset of patients. By offering a direct route to the posterior facet, it simplifies joint preparation and avoids lateral soft tissue stripping. However, the surgeon must respect its biomechanical limitations—specifically its inability to correct deformity—and strictly avoid its use in patients with varus hindfoot alignment. When executed with precision, utilizing modern grafting principles and meticulous soft tissue handling, the posterior approach yields a robust, durable fusion for isolated subtalar arthritis.
You Might Also Like