End Your Pain: Hallux IPJ Arthrodesis for Cockup Toe Deformity
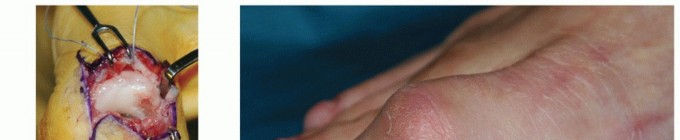
Key Takeaway
This article provides essential research regarding End Your Pain: Hallux IPJ Arthrodesis for Cockup Toe Deformity. A cockup toe deformity typically arises from chronic untreated turf toe injuries or inadequate repair after sesamoid excision. It presents with hyperextension of the metatarsophalangeal (MTP) joint and flexion of the hallux interphalangeal (IP) joint. This leads to dorsal IPJ and distal toe pressure, often causing pain and requiring treatment like IPJ arthrodesis.
Introduction and Epidemiology
Multiple potentially disabling disorders affect the hallux interphalangeal joint. Symptomatic hallux interphalangeal joint arthritis and deformity may be effectively treated with hallux interphalangeal joint arthrodesis. The goal of hallux interphalangeal joint arthrodesis is to relieve intra-articular pain, dorsal interphalangeal joint and distal toe pressure due to flexion contracture, and resultant sesamoid pain due to chronic hallux metatarsophalangeal joint extension and interphalangeal joint flexion contracture.
Intra-articular fractures are often due to direct axial load or impact to the hallux. Treatment with rest and a period of immobilization may relieve symptoms in the acute setting for nondisplaced fractures. Patients with displaced intra-articular fractures may require open reduction and internal fixation versus primary interphalangeal joint arthrodesis. Degenerative hallux interphalangeal joint arthritis is often attributed to trauma or chronic biomechanical overload.

Osteochondritis dissecans of the hallux interphalangeal joint is rare compared to that of the knee or talus. Case series of athletes with interphalangeal joint osteochondral fragments have been published. Débridement and temporary Kirschner wire fixation have produced short-term symptomatic improvement of symptoms; however, long-term data remain sparse regarding joint preservation in advanced disease.
Claw hallux deformity etiology comprises compartment syndrome of the foot, Charcot-Marie-Tooth disease, cerebral palsy, spina bifida, and other static or progressive neuromuscular diseases. The soft tissue imbalance produces hyperextension of the metatarsophalangeal joint and flexion of the hallux interphalangeal joint. Cock-up toe deformity develops from chronic untreated turf toe or plantar plate injuries. Likewise, when both the medial and lateral sesamoids are excised with inadequate repair of the residual flexor mechanism, a cock-up toe deformity may rapidly develop.

Inflammatory arthritis represents another distinct cohort. In select cases, inflamed synovitis and progressive periarticular joint destruction of an inflammatory arthropathy may occur in the hallux interphalangeal joint, necessitating arthrodesis to restore a plantigrade, painless digit.

Surgical Anatomy and Biomechanics
The hallux consists of two phalanges, proximal and distal. The hallux interphalangeal joint is the articulation of the proximal phalangeal head and the distal phalangeal base. This simple and stable hinge joint allows for motion up to 11.9 degrees of active extension and 46 degrees of flexion.
The osteology of the proximal phalangeal head has been described as a large trochlear groove that is wider and more concave on the plantar side. The phalangeal head topography is congruently matched by the distal phalangeal base.

Static stability is primarily created by the collateral ligaments originating from the superolateral aspect of the phalangeal head and inserting into the dorsal tubercle of the distal phalanx. This static restraint is augmented by the circumferential joint capsule that includes the plantar flexor plate.

Dynamic support arises from the extensor hallucis longus and flexor hallucis longus tendons that cross the joint. The flexor hallucis longus inserts at the plantar base of the distal phalanx and provides the primary plantarflexion force during the terminal stance phase of gait. When the metatarsophalangeal joint is hyperextended, the flexor hallucis longus becomes functionally lengthened or mechanically disadvantaged depending on the integrity of the plantar plate, exacerbating interphalangeal joint flexion contractures.

Indications and Contraindications
Patient History and Physical Findings
Occasionally, the patient recalls a traumatic inciting event such as stubbing of the great toe. However, the patient typically presents with an activity-related ache or pain in the hallux interphalangeal joint. Careful history should be directed to explore the possible etiology of the pain or deformity, particularly screening for progressive neuromuscular disorders.
The patient may have an obvious deformity such as claw hallux, hyperextension, or hallux valgus interphalangeus. The clinician should examine the skin for associated soft tissue corns, plantar callosities, or even open ulcers in patients with severe deformities. Tenderness is usually localized to the dorsal or plantar aspect of the interphalangeal joint, often exacerbated by forced flexion or extension during the clinical examination.

Operative Rationale
Arthrodesis is the definitive management for end-stage pathology of the hallux interphalangeal joint when conservative measures, such as shoe modifications, rigid insoles, and taping, have failed.

| Indication Category | Operative Indications | Non Operative Indications |
|---|---|---|
| Degenerative | End-stage osteoarthritis with intractable pain, failed conservative therapy | Mild to moderate osteoarthritis responsive to stiff-soled shoes or NSAIDs |
| Deformity | Rigid claw toe, severe hallux valgus interphalangeus, cock-up toe | Flexible deformities correctable with taping or orthotics |
| Neuromuscular | Charcot-Marie-Tooth, cerebral palsy with fixed contracture | Non-ambulatory patients without skin breakdown risk |
| Trauma | Chronic painful nonunion, severe intra-articular comminution | Acute, nondisplaced intra-articular fractures |
| Inflammatory | Rheumatoid arthritis with joint destruction and instability | Medically managed inflammatory arthropathy with preserved joint space |
Contraindications to surgical intervention include active local or systemic infection, severe peripheral vascular disease precluding wound healing, and inadequate dorsal soft tissue coverage. A thorough vascular assessment, including ankle-brachial indices or toe pressures, is mandatory in patients with a history of diabetes or peripheral arterial disease.
Pre Operative Planning and Patient Positioning
Radiographic Evaluation and Templating
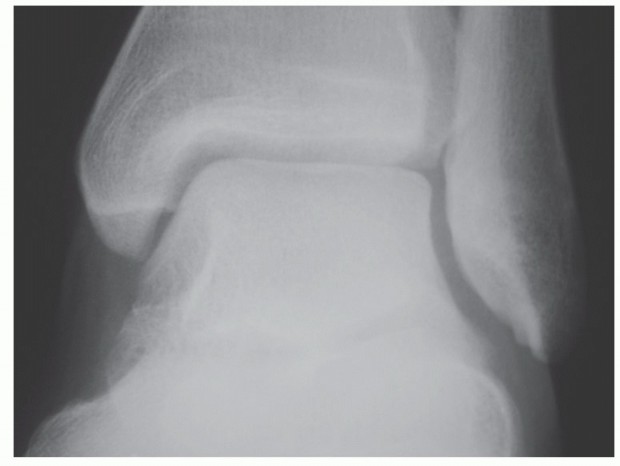
Standard weight-bearing anteroposterior, lateral, and oblique radiographs of the foot are required. The anteroposterior view allows assessment of the hallux valgus interphalangeus angle, while the lateral view is critical for evaluating the extent of flexion contracture and joint space narrowing.

Templating is performed to determine the optimal length and diameter of the fixation device. The current gold standard utilizes a fully threaded, headless compression screw (typically 3.0 mm to 4.0 mm in diameter). The screw must be long enough to bypass the interphalangeal joint and achieve purchase in the diaphyseal or metaphyseal bone of the proximal phalanx without penetrating the metatarsophalangeal joint.
Patient Positioning and Anesthesia
The procedure is typically performed on an outpatient basis under regional anesthesia (ankle block or popliteal block) combined with monitored anesthesia care. The patient is positioned supine on the operating table. A bump may be placed under the ipsilateral hip to correct natural external rotation of the lower extremity, ensuring the hallux faces directly toward the ceiling for orthogonal fluoroscopic imaging. A calf or ankle tourniquet is utilized to provide a bloodless surgical field.

Detailed Surgical Approach and Technique
Incision and Exposure
Several incisions can be utilized, including a dorsal transverse, dorsal longitudinal, or an elliptical incision if redundant skin needs excision. The dorsal longitudinal incision is most commonly employed as it provides excellent extensile exposure and minimizes the risk of vascular compromise to the dorsal skin flaps.

The incision is carried sharply through the dermis. Subcutaneous dissection is performed meticulously to identify and protect the dorsal medial and dorsal lateral proper digital nerves. The extensor hallucis longus tendon is identified. Depending on surgeon preference and the presence of a contracture, the extensor hallucis longus can be longitudinally split, Z-lengthened, or retracted laterally to expose the dorsal joint capsule.

Joint Preparation
A transverse capsulotomy is performed. The collateral ligaments must be completely excised from their origins on the proximal phalangeal head to allow for adequate plantarflexion and exposure of the articular surfaces. If a severe flexion contracture is present, a formal release of the plantar plate from the proximal phalanx may be required to achieve neutral alignment.

Preparation of the articular surfaces can be performed using flat cuts with an oscillating saw or by utilizing cup-and-cone reamers. The cup-and-cone technique is frequently preferred as it preserves digital length, maximizes cancellous bone contact area, and allows for multi-planar adjustment of the arthrodesis position prior to fixation.

The cartilage is completely denuded down to bleeding subchondral bone. A 2.0 mm drill bit or K-wire is often used to fenestrate the sclerotic subchondral bone, promoting marrow egress and enhancing the biologic environment for fusion.

Reduction and Alignment
Optimal positioning of the hallux interphalangeal joint arthrodesis is critical for postoperative function and shoe wear. The joint should be fused in neutral to 5 degrees of plantarflexion, neutral rotation, and neutral to slight valgus (matching the contralateral digit). Excessive plantarflexion leads to distal tip pressure and ulceration, while excessive extension leads to dorsal shoe impingement.

Once the desired alignment is achieved, provisional fixation is obtained using a 0.045-inch or 0.062-inch Kirschner wire driven from distal to proximal.
Fixation Technique
For retrograde screw fixation, a guide wire is introduced at the distal tip of the distal phalanx, taking care to position it 2 to 3 mm plantar to the nail matrix to avoid iatrogenic nail dystrophy. The wire is advanced across the interphalangeal joint and into the proximal phalanx under fluoroscopic guidance.

The trajectory should aim slightly dorsal to plantar to engage the robust plantar cortical bone of the proximal phalanx, maximizing thread purchase.

Once wire position is confirmed, the length is measured. The distal phalanx is drilled and countersunk to allow the trailing edge of the headless compression screw to sit flush or slightly recessed within the distal phalangeal tuft. The selected screw is then inserted over the wire.

Compression across the arthrodesis site is verified both visually and fluoroscopically. If rotational instability is noted despite the compression screw, a supplemental derotational K-wire may be placed, though this is rarely necessary with modern cup-and-cone preparation and adequate compression.

Closure
The wound is thoroughly irrigated. The extensor hallucis longus tendon is reapproximated if it was split. The subcutaneous tissue is closed with absorbable sutures, and the skin is closed with non-absorbable monofilament sutures. A sterile, compressive dressing is applied.

Complications and Management
While hallux interphalangeal joint arthrodesis is generally highly successful, complications can occur and must be managed promptly to prevent long-term morbidity.
| Complication | Estimated Incidence | Etiology and Salvage Strategies |
|---|---|---|
| Nonunion (Pseudoarthrosis) | 5% - 10% | Caused by inadequate joint preparation, poor compression, or patient non-compliance. Asymptomatic nonunions require no treatment. Symptomatic nonunions require revision arthrodesis with bone grafting and robust fixation. |
| Malunion | 2% - 5% | Usually due to intraoperative technical error. Excessive plantarflexion causes distal tip ulcers; excessive extension causes dorsal shoe wear issues. Treated with closing wedge osteotomy and revision internal fixation. |
| Hardware Prominence | 5% - 15% | Occurs if the distal screw head is not adequately countersunk. Can cause distal tip pain. Managed by hardware removal after clinical and radiographic union is achieved. |
| Infection | 1% - 3% | Superficial infections managed with oral antibiotics. Deep space infections require hardware removal, aggressive surgical débridement, and culture-directed intravenous antibiotics. |
| Nerve Injury | 2% - 4% | Iatrogenic injury to dorsal proper digital nerves. Can lead to painful neuroma. Managed with gabapentinoids, local injections, or surgical neuroma excision and capping. |
Symptomatic nonunion is the most challenging complication. It often presents with persistent swelling, pain with weight-bearing, and radiographic evidence of a persistent radiolucent line or hardware failure (screw breakage or back-out).

Revision surgery for nonunion requires careful removal of broken hardware, aggressive takedown of the fibrous pseudoarthrosis, and often the use of structural allograft or autograft to restore length if significant bone resorption has occurred.
Post Operative Rehabilitation Protocols
The postoperative rehabilitation protocol is designed to protect the arthrodesis site while allowing for early mobilization of adjacent joints to prevent stiffness.
Phase 1: 0 to 2 Weeks Postoperative
The patient is placed in a rigid postoperative shoe or controlled ankle motion boot. Weight-bearing is restricted to heel-touch or flat-foot weight-bearing only, strictly avoiding toe-off mechanics. Elevation and icing are emphasized to control edema. Sutures are removed at 10 to 14 days once the incision is completely healed.
Phase 2: 2 to 6 Weeks Postoperative
The patient continues to wear the rigid postoperative shoe or boot. Progressive weight-bearing to tolerance is permitted, but the rigid sole is mandatory to prevent bending forces across the interphalangeal joint. Active and passive range of motion exercises for the metatarsophalangeal joint and ankle are initiated to prevent secondary stiffness.
Phase 3: 6 to 12 Weeks Postoperative
At 6 weeks, weight-bearing radiographs are obtained to assess for bridging trabecular bone. If clinical and radiographic union is progressing appropriately, the patient is transitioned to a stiff-soled athletic shoe. High-impact activities and running are generally restricted until 10 to 12 weeks postoperative, or until complete radiographic consolidation is evident.
Summary of Key Literature and Guidelines
The literature strongly supports hallux interphalangeal joint arthrodesis as a durable, reliable procedure for alleviating pain and correcting deformity. Biomechanical studies have consistently demonstrated that fully threaded, headless compression screws provide superior compression and torsional stability compared to crossed Kirschner wires or interosseous wiring techniques.
Clinical outcomes research highlights that the cup-and-cone joint preparation technique yields union rates exceeding 90%, largely due to the maximization of cancellous bone contact and the intrinsic stability of the contoured surfaces. Furthermore, literature emphasizes that patient satisfaction is intimately tied to the final sagittal plane alignment; fusions left in excessive plantarflexion are highly correlated with poor functional outcome scores due to terminal stance pain.
Current academic consensus dictates that meticulous soft tissue handling, precise joint contouring, and rigid internal fixation are the triad of requirements for minimizing complications and achieving a successful hallux interphalangeal joint arthrodesis.
Clinical & Radiographic Imaging






















You Might Also Like