Management of Tibial, Malleolar, and Metatarsal Nonunions
Key Takeaway
Nonunions of the tibia, medial malleolus, and metatarsals present complex reconstructive challenges requiring meticulous surgical planning. Successful management demands a thorough understanding of local biomechanics, optimization of host biology, and rigid mechanical stabilization. This guide details evidence-based surgical approaches, including autogenous bone grafting, internal fixation techniques, and fragment excision protocols, to restore functional anatomy and promote definitive osseous union in recalcitrant lower extremity fractures.
INTRODUCTION TO LOWER EXTREMITY NONUNIONS
The failure of a fracture to unite—defined clinically as a cessation of osteogenic activity at the fracture site without the potential for healing in the absence of intervention—presents a formidable challenge in orthopedic traumatology. In the lower extremity, nonunions profoundly impact patient mobility, quality of life, and socioeconomic productivity. The etiology of nonunion is multifactorial, encompassing mechanical instability, biological compromise, and occult infection. Successful management requires a systematic approach to identify the underlying cause, optimize host biology, and execute precise surgical reconstruction. This masterclass details the evidence-based management of nonunions specific to the metatarsals, the tibial diaphysis, and the medial malleolus.
NONUNION OF THE METATARSALS
Epidemiology and Pathoanatomy
Nonunions of the metatarsals are relatively uncommon in routine orthopedic practice. When they do occur, they are predominantly localized to the distal third of the bone. The primary etiologic factors contributing to metatarsal nonunion include poor apposition of the fracture fragments (often due to inadequate initial reduction or loss of fixation) and localized infection.
The distal third of the metatarsal is particularly vulnerable due to its unique biomechanical environment and tenuous vascular supply. During the terminal stance phase of the gait cycle, the distal metatarsals are subjected to immense cantilever bending and shear forces. If mechanical stabilization is insufficient, these micro-motions disrupt the delicate process of endochondral ossification, leading to a hypertrophic or oligotrophic nonunion. Conversely, severe soft tissue stripping from the initial trauma or iatrogenic injury during primary surgery can devascularize the fragments, resulting in an atrophic nonunion.
Clinical Evaluation
Patients typically present with chronic, localized forefoot pain exacerbated by weight-bearing, particularly during toe-off. Clinical examination may reveal palpable hardware, localized edema, and point tenderness over the affected metatarsal.
Clinical Pearl: Always evaluate the adjacent metatarsals. A nonunion in one metatarsal alters the load distribution across the forefoot, frequently leading to transfer metatarsalgia or stress fractures in adjacent rays.
Surgical Management
The treatment of metatarsal nonunions is dictated by the biological viability of the fracture ends and the presence of deformity.
- Preoperative Planning: High-resolution radiographs (weight-bearing AP, lateral, and oblique views) are mandatory. A CT scan may be utilized to assess the exact volume of bone loss and the presence of cystic changes.
- Surgical Approach: A dorsal longitudinal incision is typically employed. Care must be taken to protect the dorsal cutaneous nerves and the extensor tendons, which are retracted gently to expose the nonunion site.
- Debridement and Preparation: The nonunion site is aggressively debrided of all intervening fibrous tissue until punctate bleeding bone (the "paprika sign") is encountered. The medullary canals of both the proximal and distal fragments must be opened using a small drill or curette to restore endosteal blood flow.
- Bone Grafting: For atrophic nonunions or those with structural defects, autogenous cancellous bone graft (frequently harvested from the proximal tibia or iliac crest) is packed into the defect.
- Internal Fixation: Rigid internal fixation is paramount. While intramedullary Kirschner wires may suffice for highly distal lesions, low-profile mini-fragment locking plates (2.0 mm or 2.4 mm systems) applied dorsally provide superior biomechanical stability, neutralizing bending moments and allowing for earlier mobilization.
NONUNION OF THE TIBIA
Epidemiology and Risk Factors
The tibia is the most commonly fractured long bone, and consequently, it represents the most frequent site of long bone nonunion. Epidemiological data estimates that nonunions occur after 2% to 15% of all tibial fractures. The development of a tibial nonunion is intimately related to the mechanism, type, and severity of the initial injury.
Several critical factors play a role in the pathogenesis of tibial nonunions:
* Fracture Characteristics: High-energy mechanisms resulting in severe comminution, segmental bone loss, or open fractures significantly increase the risk.
* Soft Tissue Envelope: The anteromedial surface of the tibia is subcutaneous. Severe soft tissue injury (Tscherne classification) or extensive periosteal stripping compromises the extrinsic blood supply, leading to atrophic nonunion.
* Infection: Infection is a catastrophic complication that arrests bone healing. Infection rates as high as 24% have been reported in severe open tibial fractures (Gustilo-Anderson Type III).
* Host Factors: Medical comorbidities (e.g., diabetes mellitus, peripheral vascular disease), poor nutritional status, and specific medications (e.g., NSAIDs, corticosteroids) impair osteogenesis.
* Patient Lifestyle: Tobacco use is one of the most profound modifiable risk factors, causing microvascular vasoconstriction and inhibiting cellular proliferation.
* Subsequent Complications: The development of compartment syndrome and the necessity for fasciotomies further compromise the local vascularity and soft tissue envelope.
Surgical Strategies for Tibial Nonunion
The management of a tibial nonunion requires a comprehensive strategy addressing both mechanical and biological deficiencies.
1. Exchange Intramedullary Nailing
For aseptic diaphyseal nonunions previously treated with an intramedullary nail, exchange nailing is the gold standard.
* Mechanism: The procedure involves the removal of the existing nail, sequential over-reaming of the medullary canal (typically 1 to 2 mm larger than the previous nail), and insertion of a larger diameter nail.
* Biological Benefit: Reaming generates autogenous bone graft that is deposited at the nonunion site, stimulating a robust osteogenic response.
* Mechanical Benefit: A larger nail increases the working length stiffness and provides enhanced rotational and angular stability.
Surgical Warning: If the fibula has healed solidly, it may act as a strut, holding the tibial nonunion in distraction. In such cases, a partial fibulectomy (resection of a 1-2 cm segment of the fibula) is mandatory to allow dynamic compression of the tibial nonunion site upon weight-bearing.
2. Augmentative Plating
In cases where an intramedullary nail provides insufficient rotational stability (particularly in distal metaphyseal-diaphyseal junction nonunions), leaving the nail in situ and applying a supplementary compression plate with autogenous bone grafting can yield excellent union rates.
3. Management of Infected Nonunions
Infected tibial nonunions require a staged approach:
* Stage 1: Radical debridement of all necrotic bone and soft tissue, removal of all hardware, and placement of an antibiotic-impregnated polymethylmethacrylate (PMMA) spacer (the Masquelet technique) or application of a circular external fixator (Ilizarov frame).
* Stage 2: Once the infection is definitively eradicated (confirmed by normalized inflammatory markers and negative intraoperative cultures), the PMMA spacer is removed, and the induced biomembrane is filled with copious autogenous bone graft, followed by definitive internal fixation.
NONUNION OF THE MEDIAL MALLEOLUS
Pathoanatomy and Indications for Surgery
A fracture of the medial malleolus occasionally fails to unite, a complication seen most frequently following nonoperative (closed) treatment. The failure of union is typically driven by the interposition of periosteum or the posterior tibial tendon into the fracture site, or by the continuous sheer forces exerted by the robust deltoid ligament during ankle motion. Furthermore, synovial fluid from the ankle joint can infiltrate the fracture gap, washing away the fracture hematoma and inhibiting the formation of a provisional callus.
Surgery is generally indicated for the subset of nonunions in which other serious complications of the fracture—most notably, advanced post-traumatic osteoarthritis—are not yet evident on radiographs, and ideally if the injury is less than 2 years old.
Treatment Algorithms
When a medial malleolar nonunion is symptomatic and painful, it can be managed via one of three distinct pathways, depending on the size of the fragment, the patient's functional demands, and the integrity of the ankle mortise:
1. Conservative Management
When the ununited fragment is small, the ankle mortise remains radiographically stable, and the patient’s occupation or lifestyle is primarily sedentary, conservative treatment is a viable option. This typically involves the use of a custom-molded ankle corset, an ankle-foot orthosis (AFO), or a rigid lace-up brace to restrict inversion/eversion and mitigate pain.
2. Open Reduction and Internal Fixation (ORIF) with Bone Grafting
For larger fragments that are critical to the stability of the medial ankle mortise, joint preservation through ORIF is the treatment of choice.
* Technique: The surgical approach involves a standard medial incision. The nonunion site is meticulously taken down, and all fibrous tissue is excised using a curette until healthy, bleeding subchondral bone is exposed.
* Grafting: Autogenous cancellous bone graft (often harvested locally from the distal tibial metaphysis) is packed into the defect to stimulate osteogenesis.
* Fixation: Internal fixation is achieved using two partially threaded cancellous lag screws or a tension band wiring construct to provide absolute stability and interfragmentary compression.
3. Excision of the Nonunion Fragment
In cases where the nonunion fragment is too small or osteopenic to accommodate internal fixation, but conservative management has failed, excision of the fragment is indicated.
Surgical Warning: The deep deltoid ligament originates from the medial malleolus and is the primary restraint against lateral talar shift. When excising a medial malleolar fragment, the surgeon must meticulously preserve the deep deltoid ligament's attachment to the remaining intact medial malleolus, or perform a primary ligamentous repair to the distal tibia using suture anchors. Excessive resection will inevitably lead to valgus instability and rapid joint degeneration.
Clinical Case: Grafting vs. Resection
The following radiographic sequence illustrates the complex decision-making process in managing a recalcitrant medial malleolar nonunion.
Figure A: Demonstrates the ankle one month after an intraosseous autogenous bone grafting procedure was attempted for a chronic nonunion of the medial malleolus. Despite the intervention, the fracture line remains clearly visible, and the biological response is blunted.

FIGURE 59-17 A, One month after intraosseous graft for nonunion of fracture of medial malleolus.
Figure B: Illustrates the ultimate failure of the grafting procedure. Due to persistent pain and lack of osseous integration, the decision was made to proceed with surgical resection. The ununited medial malleolar fragment was carefully excised, ensuring that the deep deltoid ligament was reattached to the remaining stable tibial metaphysis to prevent lateral talar subluxation.
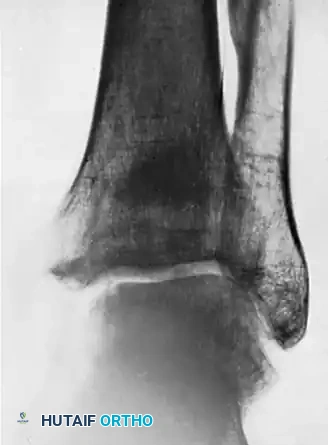
FIGURE 59-17 B, Failure of grafting procedure. Medial malleolus was resected.
Figure C: Represents the long-term follow-up, seven years post-resection. The ankle mortise remains remarkably stable without evidence of talar shift. While mild arthritic changes (joint space narrowing and subchondral sclerosis) are becoming evident, the patient maintains functional mobility. This radiograph highlights a critical biomechanical threshold: this represents the maximal amount of the medial malleolus that can be safely removed while still preserving the intrinsic stability of the ankle joint.
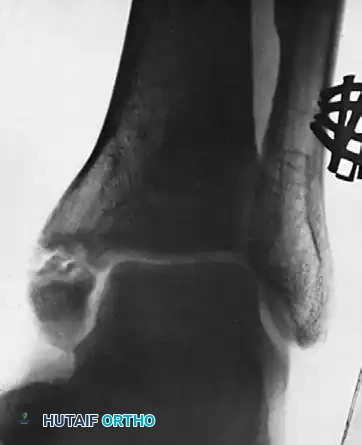
FIGURE 59-17 C, Seven years after resection, ankle is stable, although mild arthritic changes are becoming evident. This is maximal amount of medial malleolus that can be removed if stability of ankle is to be preserved.
POSTOPERATIVE REHABILITATION PROTOCOLS
The postoperative management of lower extremity nonunions is as critical as the surgical execution. Protocols must be tailored to the specific bone, the rigidity of the fixation, and the biological quality of the host tissue.
Metatarsal Nonunions
- Phase 1 (0-2 weeks): Strict non-weight-bearing in a well-padded posterior splint. Elevation is critical to manage forefoot edema.
- Phase 2 (2-6 weeks): Transition to a rigid controlled ankle motion (CAM) boot. Heel-touch weight-bearing is permitted. Active range of motion (ROM) of the metatarsophalangeal (MTP) joints is initiated to prevent stiffness.
- Phase 3 (6-12 weeks): Progressive weight-bearing as tolerated in a stiff-soled shoe, guided by radiographic evidence of bridging callus.
Tibial Nonunions
- Phase 1 (0-4 weeks): For exchange nailing, patients are typically allowed touch-down weight-bearing (TDWB) to stimulate the mechanoreceptors and promote early callus formation, provided the fixation is rotationally stable.
- Phase 2 (4-8 weeks): Progression to partial weight-bearing. Physical therapy focuses on restoring full knee and ankle ROM and preventing quadriceps atrophy.
- Phase 3 (8+ weeks): Advancement to full weight-bearing is contingent upon the visualization of bridging callus on at least three out of four cortices on orthogonal radiographs.
Medial Malleolar Nonunions
- Phase 1 (0-2 weeks): Immobilization in a short-leg cast or rigid splint. Strict non-weight-bearing to protect the articular surface and the delicate deltoid ligament repair (if excision was performed).
- Phase 2 (2-6 weeks): Transition to a CAM boot. Gentle active ROM exercises (dorsiflexion and plantarflexion) are initiated. Inversion and eversion are strictly prohibited to protect the medial structures.
- Phase 3 (6-12 weeks): Gradual progression to full weight-bearing. Proprioceptive training and peroneal strengthening are emphasized to restore dynamic ankle stability.
CONCLUSION
The surgical management of nonunions in the lower extremity demands a profound respect for both biomechanics and biology. Whether addressing the high-stress environment of the metatarsals, the precarious vascularity of the tibial diaphysis, or the complex articular mechanics of the medial malleolus, the surgeon must meticulously balance rigid mechanical fixation with the optimization of the local biological envelope. Through precise preoperative planning, meticulous surgical technique, and structured postoperative rehabilitation, orthopedic surgeons can successfully navigate these complex reconstructive challenges, ultimately restoring function and mobility to the patient.
You Might Also Like