Proximal Humerus Malunion: Evaluation and Surgical Management
Key Takeaway
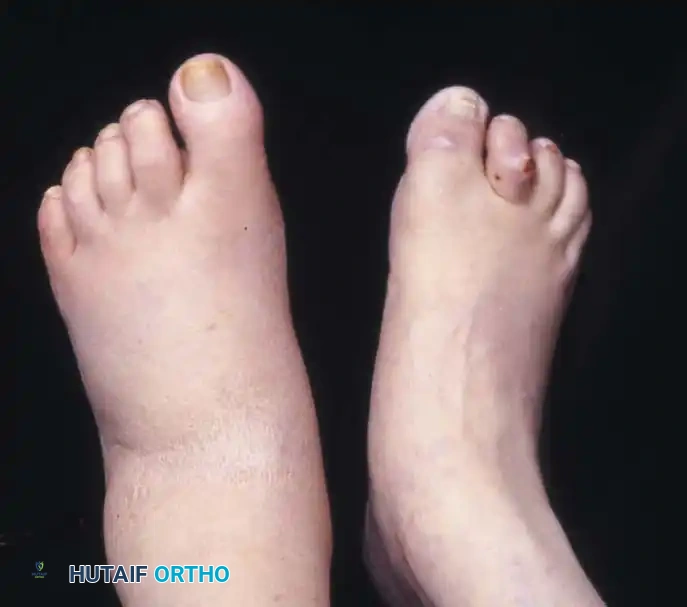
Malunion of the proximal humerus presents a complex reconstructive challenge, often resulting from inadequate reduction or conservative management of displaced fractures. This condition severely impairs shoulder biomechanics, causing pain, stiffness, and rotator cuff dysfunction. Successful management requires meticulous clinical evaluation, advanced cross-sectional imaging, and precise surgical execution. Corrective strategies range from tuberosity osteotomies to arthroplasty, depending on articular congruity, bone stock, and the presence of osteonecrosis.
INTRODUCTION AND PATHOANATOMY
Malunion of a fracture of the proximal humerus typically results from inadequate operative reduction, secondary loss of operative reduction, or the nonoperative treatment of a significantly displaced fracture. The proximal humerus relies on a delicate balance of force couples generated by the rotator cuff musculature. Disruption of the normal anatomical relationships between the articular segment, the tuberosities, and the humeral shaft profoundly alters glenohumeral kinematics.
Deformities of this kind can cause severe functional impairment, primarily characterized by a debilitating loss of abduction and rotation. The specific pathoanatomy is dictated by the original fracture pattern and the unopposed pull of the attached musculature:
* Three-Part Fractures: Malunions involving the lesser tuberosity and surgical neck are characterized by external rotation and abduction of the articular segment. This occurs because of the unopposed pull of the posterior rotator cuff muscles (infraspinatus and teres minor) on the intact greater tuberosity. A malunion in this position causes chronic pain and severe limitation of motion, especially internal rotation. These malunions are notoriously difficult to treat because they are frequently complicated by severe contractures of the deforming muscles, glenohumeral subluxation, posttraumatic arthritis, or osteonecrosis (avascular necrosis).
* Four-Part Fractures and Fracture-Dislocations: Malunions in this category are exceptionally challenging. They are complicated by the frequent presence of articular incongruity, profound muscular contractures, dense intra-articular and extra-articular adhesions, osteonecrosis of the articular head, and, occasionally, concomitant neurological injury.
CLASSIFICATION OF PROXIMAL HUMERAL MALUNIONS
Currently, there is no universally accepted, comprehensive classification system for proximal humeral malunions. However, the system proposed by Beredjiklian et al. is highly regarded in academic orthopaedics. This classification categorizes malunions based on specific osseous and soft tissue abnormalities, guiding surgical decision-making.
The Beredjiklian Classification
- Type I: Malposition of the greater or lesser tuberosity of more than 1 cm. This alters the resting length and tension of the rotator cuff, leading to weakness and mechanical impingement.
- Type II: Intra-articular incongruity or a step-off of the articular surface of more than 5 mm. This inevitably leads to rapid posttraumatic glenohumeral arthropathy.
- Type III: Rotational malalignment of the articular segment by more than 45 degrees in the coronal, sagittal, or axial plane.
Soft Tissue Considerations:
In the Beredjiklian system, soft tissue abnormalities are categorized as soft tissue contracture, rotator cuff tear, and subacromial/coracoid impingement. The importance of soft tissue evaluation cannot be overstated; in their seminal study of 39 patients, only eight (21%) had malunions without any associated soft tissue abnormality.
CLINICAL EVALUATION
A thorough history and a meticulous physical examination are essential in the evaluation of a patient presenting with a proximal humeral malunion.
History and Initial Assessment
Determining the mechanism of injury, associated injuries, and the exact treatment of the initial fracture is paramount. If the patient underwent previous internal fixation, identifying the specific type of hardware used is critical so that the appropriate extraction equipment (e.g., specific screwdrivers, broken screw removal sets) is available in the operating theater.
Range of Motion and Soft Tissue Assessment
Range-of-motion (ROM) evaluation, particularly passive ROM, is the cornerstone of assessing soft tissue contractures. Active and passive ROM must be measured in all planes of movement (forward elevation, abduction, internal rotation, external rotation).
Potential causes of decreased ROM include:
* Capsular contracture
* Extracapsular contracture (adhesions)
* Mechanical osseous impingement
* Pain-induced guarding
* Rotator cuff tears or dysfunction
Limited passive ROM almost universally indicates a soft tissue contracture or a mechanical bony block. External rotation should be checked with the arm resting at the side and at 90 degrees of abduction.
CLINICAL PEARL: A classic, though not strictly pathognomonic, sign of a greater tuberosity malunion is the profound absence of external rotation when the arm is maximally abducted. This occurs due to the malunited tuberosity mechanically impinging against the posterior superior glenoid or the acromion.
Rotator Cuff and Stability Testing
The integrity of the rotator cuff musculature must be systematically determined:
* Infraspinatus and Teres Minor: Evaluated by testing external rotation strength against resistance.
* Subscapularis: Evaluated using the Gerber lift-off test, the belly-press test, or the bear-hug test.
* Supraspinatus: Evaluated via opposed abduction at 90 degrees in the scapular plane (Jobe's test).
Instability is evaluated using provocative maneuvers, including the anterior and posterior drawer tests, the shift test, the load-and-shift test, the anterior apprehension test, the posterior stress test, and the sulcus sign. While instability may be elicited by these provocative tests, in most patients with chronic malunions, profound stiffness limits their diagnostic effectiveness.
SURGICAL WARNING: The exact nature of a soft tissue pathological process is notoriously difficult to determine purely clinically. Intraoperative assessment and sequential release of the soft tissues are mandatory if joint-preserving surgery is chosen.
Neurological Evaluation
Because many patients with proximal humeral malunions (especially those following high-energy fracture-dislocations) have underlying neurological deficits, the function of the axillary, suprascapular, and musculocutaneous nerves must be meticulously documented preoperatively. Electromyography (EMG) and nerve conduction studies (NCS) may be highly helpful to determine the exact pattern of nerve injury, the degree of denervation, and the likelihood of spontaneous recovery of nerve function.
RADIOGRAPHIC AND IMAGING EVALUATION
Advanced imaging is mandatory for preoperative planning, as plain radiographs often underestimate the complexity of the three-dimensional deformity.
- Plain Radiography: A standard trauma series should include true anteroposterior (Grashey), lateral (scapular Y), and axillary views. Supplemental internal and external rotational AP views can provide additional information regarding tuberosity position and hardware status.
- Computed Tomography (CT): CT with 3D reconstructions is the gold standard. It helps determine the precise three-dimensional spatial relationships between the malunited tuberosities, the articular head, and the shaft fragments. Because it provides a clear, unobstructed image of the glenohumeral articular surface, CT is invaluable for evaluating articular congruity and planning osteotomy trajectories.
- Magnetic Resonance Imaging (MRI): MRI provides critical information about the integrity of the rotator cuff tendons, the degree of fatty infiltration/muscle atrophy (Goutallier classification), and the presence of early osteonecrosis of the humeral head.
SURGICAL MANAGEMENT: OPERATIVE TECHNIQUES
Surgical intervention for proximal humeral malunions is technically demanding. The choice between corrective osteotomy and arthroplasty (anatomic or reverse total shoulder arthroplasty) depends on the patient's age, functional demands, articular congruity, bone stock, and rotator cuff integrity.
In cases of complex shoulder girdle trauma, proximal humerus malunions may present concomitantly with clavicular malunions (the "floating shoulder" variant). The following sections detail the operative steps for addressing these complex deformities.
Technique 1: Corrective Osteotomy for Proximal Humerus Tuberosity Malunion
For Beredjiklian Type I malunions in young, active patients with preserved articular cartilage, a corrective tuberosity osteotomy is indicated.
- Positioning and Approach: Place the patient in the beach-chair position. Utilize a standard deltopectoral approach. Identify and protect the cephalic vein.
- Soft Tissue Release: Perform a meticulous tenolysis and capsular release. Identify the axillary nerve inferiorly and protect it throughout the procedure.
- Osteotomy: Under fluoroscopic guidance, identify the malunited greater tuberosity. Using a fine osteotome or an oscillating saw, perform the osteotomy along the original fracture line. Take extreme care not to violate the underlying articular surface of the humeral head.
- Mobilization: Mobilize the tuberosity fragment along with its attached rotator cuff. This often requires extensive subacromial, subdeltoid, and intra-articular releases.
- Reduction and Fixation: Reduce the tuberosity to its anatomical footprint (lateral to the bicipital groove and inferior to the articular margin). Fixation is typically achieved using heavy non-absorbable sutures passed through drill holes in the shaft, or via a low-profile locking plate, depending on bone quality.
Technique 2: Intramedullary Correction of Associated Clavicular Malunion
In cases where a concomitant clavicular malunion contributes to shoulder girdle dysfunction, corrective osteotomy and intramedullary fixation using a Titanium Elastic Nail (TEN) may be indicated.
- Exposure: Incise the periosteum sharply over the clavicular deformity. Separate the deltotrapezial muscle attachment subperiosteally as a single, intact layer to preserve the vascular supply. Expose the deformity over a distance of approximately 5 cm.
- Osteotomy: Determine the optimal osteotomy plane under direct fluoroscopic control. Using a fine-bladed oscillating saw, perform the osteotomy, carefully separating the two main original fracture fragments.
- Canal Preparation: Hold the proximal and distal fracture fragments with pointed reduction clamps. Reopen the sclerotic medullary canal on both sides using a 2.7-mm drill under continuous fluoroscopic guidance.
- Nail Insertion: Make a small, separate skin incision (1-2 cm) just above the sternal end of the clavicle. Open the anterior cortex with a 2.7-mm drill and insert a 2.5-mm titanium elastic nail (TEN, Synthes, West Chester, PA).
- Reduction and Advancement: The distal clavicular fragment is almost always displaced caudally and malrotated, with its superior surface facing anteriorly. Realign the clavicle by lifting and derotating the distal fragment. Freshen the osseous surfaces with a rongeur or curette. Advance and insert the nail into the lateral fragment under fluoroscopic control.
> SURGICAL WARNING: Precise fluoroscopic monitoring during lateral advancement is critical to prevent inadvertent perforation of the thin posterior or superior cortex of the distal fragment. - Closure: Cut the inserted nail back to the medial insertion point, leaving it as short as possible to prevent medial skin irritation and hardware prominence. Smooth the bone ends at the osteotomy site with a rongeur, and meticulously suture the periosteal and deltotrapezial layers to ensure a robust soft-tissue envelope.
POSTOPERATIVE PROTOCOL AND REHABILITATION
The rehabilitation following surgical correction of a proximal humerus malunion is prolonged and requires strict adherence to a phased protocol to balance tissue healing with the prevention of recurrent stiffness.
Phase I: Maximum Protection (Weeks 0-6)
- The shoulder is immobilized in a sling or an abduction orthosis, depending on the tension of the rotator cuff repair and the stability of the osteotomy.
- Immediate active range of motion of the elbow, wrist, and hand is encouraged.
- Passive range of motion (PROM) of the shoulder is initiated within the "safe zone" determined intraoperatively. External rotation is typically limited to neutral or 20 degrees to protect the tuberosity fixation.
Phase II: Active Motion and Early Strengthening (Weeks 6-12)
- Radiographic evaluation is performed at 6 weeks to confirm early osseous union.
- Once clinical and radiographic signs of healing are present, the sling is discontinued.
- Active-assisted and active range of motion (AROM) exercises are initiated.
- Gentle isometric strengthening of the rotator cuff and periscapular stabilizers begins.
Phase III: Advanced Strengthening (Months 3-6)
- Progressive resistive exercises are introduced.
- Focus shifts to restoring the dynamic force couples of the glenohumeral joint and optimizing scapulothoracic rhythm.
- Return to heavy manual labor or high-impact sports is generally delayed until 6 to 9 months postoperatively, contingent upon complete radiographic union and the restoration of near-normal strength.
COMPLICATIONS
Surgical management of proximal humerus malunions carries a high complication profile due to the compromised local biology and altered anatomy.
* Osteonecrosis (AVN): The risk of AVN is significant, particularly following extensive soft tissue stripping required to mobilize malunited fragments. If symptomatic AVN develops and leads to hardware penetration or joint collapse, conversion to a total shoulder arthroplasty or reverse total shoulder arthroplasty (RTSA) is required.
* Nonunion: Failure of the osteotomy site to heal can occur due to poor bone stock or inadequate fixation.
* Hardware Failure/Impingement: Prominent hardware, especially in the subacromial space, may necessitate a secondary procedure for removal once union is achieved.
* Persistent Stiffness: Despite meticulous surgical release and aggressive rehabilitation, some degree of permanent ROM deficit is common. Managing patient expectations preoperatively is a critical component of the treatment algorithm.
You Might Also Like